Abstract
Concepts like race, migration background, or ethnic group are more and more being investigated in health research. It should be noted that those concepts themselves are very heterogeneous. They are, for example, endowed with different rights (e.g., cosmopolitan migrants from the global north, refugees from the global south) (Ambrosini & van der Leun, 2015) or have to deal with racism or discrimination (Nazroo, 2003). A challenge and a recurrent difficulty in research on the health of migrants is the operationalization of studies due to the heterogeneity of the group. On the one hand, it is unclear which criteria—nationality, mother tongue, ethnicity of grandparents, race, place of birth, place of migration as well as migration regime—are used to determine “migrants,” which makes comparability of the studies difficult (Sheldon & Parker, 1992). On the other hand, the group of people with a history of migration is very heterogeneous with regard to other lines of difference, such as social milieu/class and gender, but also country of origin and reason and time of migration. This makes the health situation of the so-called migrants very different, and it cannot be described in a generalized way. Research shows that social integration and social support can play a big role in the health status of migrants. It can provide information to the healthcare system, provide emotional support, or simply make someone feel like they are not alone. Social networks also play a big role for people with a so-called migration background or with a so-called different ethnic background (Johnson et al., 2017). In this chapter, we explore the link between health, migration, and networks. In doing so, we will try to minimize the uncertainty of the heterogeneity of the group as much as possible.
You have full access to this open access chapter, Download chapter PDF
Similar content being viewed by others
-
Ethnic and migration-related differences are increasingly being researched as a determinant of health inequalities, but empirical results in this regard are sometimes contradictory.
-
Studies on “Migration and health or health inequalities” and on “Migration and networks” are available.
-
Studies that cover all three areas together are very rare and almost always only consider a population group without additionally broadening the view to vertical dimensions of inequality, such as income or education.
-
Most studies use the term “network” as a metaphor or synonym for group or social capital, or they exclusively investigate social support as a central function of social networks.
-
The extent to which the phenomena associated with the concept of migration are actually migration-specific—for example, linked to a concrete migration process—or whether other social group memberships, such as class or gender, have (higher) explanatory power for health inequalities, in the sense of intersectionality, remains to be studied.
1 Introduction
Concepts like race, migration background, or ethnic group are more and more being investigated in health research. It should be noted that those concepts themselves are very heterogeneous. They are, for example, endowed with different rights (e.g., cosmopolitan migrants from the global north, refugees from the global south) (Ambrosini & van der Leun, 2015) or have to deal with racism or discrimination (Nazroo, 2003). A challenge and a recurrent difficulty in research on the health of migrants is the operationalization of studies due to the heterogeneity of the group. On the one hand, it is unclear which criteria—nationality, mother tongue, ethnicity of grandparents, race, place of birth, place of migration as well as migration regime—are used to determine “migrants,” which makes comparability of the studies difficult (Sheldon & Parker, 1992). On the other hand, the group of people with a history of migration is very heterogeneous with regard to other lines of difference, such as social milieu/class and gender, but also country of origin and reason and time of migration. This makes the health situation of the so-called migrants very different, and it cannot be described in a generalized way. Research shows that social integration and social support can play a big role in the health status of migrants. It can provide information to the healthcare system, provide emotional support, or simply make someone feel like they are not alone. Social networks also play a big role for people with a so-called migration background or with a so-called different ethnic background (Johnson et al., 2017). In this chapter, we explore the link between health, migration, and networks. In doing so, we will try to minimize the uncertainty of the heterogeneity of the group as much as possible.
2 The Health of Migrants: Study Results to Migration and Health
First, we will present research on health and migration.Footnote 1 We will show research results on the physical and mental health status of migrants as well as outcomes on subjective well-being and health behavior. The focus will be on research on physical as well as psychological factors. In addition, we give a short summary of current study results addressing COVID-19 and migration. Finally, we shortly sum up different explanation models for the health status of migrants. In several parts of this chapter, we would like to distinguish between migrants (e.g., migrant workers) and refugees.
2.1 Physical and Mental Health of Migrants
2.1.1 Mortality
Researchers studying mortality among migrants have found evidence that this “group” tends to show lower mortality than the non-migrant population of host countries in the global north. For example studies in Australia illustrate a lower mortality over different migrant groups (Kouris-Blazos, 2002; Anikeeva et al., 2010, 2015). The same results can be found in New Zealand (Hajat et al., 2010). Research on immigrants in the United States showed a lower risk of overall mortality than persons who were born there (Singh & Siahpush, 2001). One big focus is on the Hispanic mortality paradox. A meta-analysis of the published longitudinal literature on Hispanic populations shows that 17.5% have a lower risk of mortality compared with other ethnic groups. The results differed by age, preexisting health conditions, and racial group: Hispanics had a lower overall risk of mortality than non-Hispanic Blacks and non-Hispanic Whites, nevertheless an overall higher risk than Asian-Americans (Ruiz et al., 2013). Shiels et al. (2017) note that between 2011 and 2014, Native Americans and native peoples of Alaska had the highest premature mortality followed by black people. Newbold used the data of Canada’s longitudinal National Population Health Survey to explore the self-assessed health of Canada’s immigrant population. He focused on the health between the native-born populations and immigrants, the factors that contribute to immigrant self-assessed health, and the factors associated with declining self-assessed health status. According to Newbold (2005, p. 1359), “Results indicate mixed support for the Healthy Immigrant Effect, with the native- and foreign-born neither more nor less likely to rank their health as fair or poor. However, results from the proportional hazards model indicated that the native-born were at lower risk to transition to poor health.” Setia et al. (2011) emphasize that women from countries with a lower development index appear at greater risk of poor self-assessed health.
The migrants mortality paradox is also being explored in Europe (Khlat & Darmon, 2003). Research conducted by Razum et al. (1998) shows that the age-adjusted mortality rate of Turkish males and females aged 25–65 years residing in Germany was, consistently half that of the German population in 1980 and 1990 (Razum et al., 1998). Similar results are found for German immigrants from the Former Soviet Union (Ronellenfitsch et al., 2006). In contrast, a study by Kibele et al. (2008) assumes an underestimation of the mortality of migrants over 65 years using the data of the German Pension Scheme. They argue that: “Mortality re-estimation reveals two-fold underestimation of mortality of foreigners due to biased death numerator and population denominator” (Kibele et al., 2008, p. 389). In Belgium, the research data points to the migrant mortality paradox (Deboosere & Gadeyne, 2005; Vandenheede et al., 2015). However, according to Vanthomme and Vandenheede, “Adjusting for socioeconomic position generally increased the migrant mortality advantage, however with large differences by gender, migrant origin, socioeconomic position indicator and causes of death” (Vanthomme & Vandenheede, 2019, p. 96). Similar results are also observed in the United Kingdom (Scott & Timæus, 2013; Wallace & Kulu, 2014a, 2014b), Switzerland (Tarnutzer et al., 2012), and France (Wallace et al., 2019).
Other studies look at the mortality of migrants in the host countries and compare it with the mortality of people in countries of origin (Wallace & Wilson, 2019). Wallace and Wilson (2019) find that the “migrant mortality advantage” relative to the origin country is present in nearly all groups, but its size depends on the development level in the origin country. Migrants originating from countries that neighbor England and Wales or feature similar levels of development, including Canada, Hong Kong, and Ireland, do not have lower death rates than those who remain in the origin country. In general, the lower the development level is in the origin country, the greater the size of the advantage of migrants in the destination country. Advantages were often largest in young adulthood (just after many migrants tend to arrive) and diminished with age and length of stay. Wallace and Wilson (2019) also find a persistent educational advantage for almost all migrant groups, which may help to explain their mortality advantage. Still others compare immigrant migrants with migrants born in the host countries. Stanaway et al. (2020) found a lower mortality rate in Italian-born men compared with Australian-born men.
An international study, which compared data from France, the United Kingdom, and the United States, shows that the migrant mortality advantage varies with the age. They found a U-shape pattern: “[…] at the aggregate level, migrants often experience excess mortality at young ages, then exhibit a large advantage at adult ages (with the largest advantage around age 45), and finally experience mortality convergence with natives at older ages” (Guillot et al., 2018, p. 14). The meta-study by Aldridge et al. (2018) analyzed 5464 studies with more than 15.2 million migrants: 5327 studies (97%) were from high-income states, 115 (2%) were from middle-income countries, and 22 (<1%) were from low-income states. The study shows that international migrants have a mortality advantage compared with general populations. They have a mortality advantage across the following categories: circulatory, digestive, endocrine, injuries, mental and behavioral, neoplasms, nervous, and respiratory. “The mortality advantage identified will be representative of international migrants in high-income countries who are studying, working, or have joined family members in these countries” (Aldridge et al., 2018, p. 2553).
Many refugees were from countries that do not have a well-developed healthcare system, economic resources, or the capacity for a good psychological care. This can lead to high mortality rates, particularly in the refugee camps in countries of the global south (Médecins Sans Frontières, 1997). In contrast, just a few studies on refugees in western countries show a mortality advantage for refugees but not for asylum seekers (Aldridge et al., 2018).
Most of the international and national studies in the global north on mortality find that migrants illustrate a lower mortality than the non-migrant population of host countries. As Deboosere and Gadeyne (2005, p. 691) note: “[…] lower mortality does not necessarily imply better health.”
2.1.2 Disease, Illness, and Migration
In this section, we highlight some of the diseases associated with migration. It is not possible for us to shed light on every disease. Therefore, we decided to present some research results on selected diseases and focused on recent studies.
Studies about heart diseases show different results. A higher prevalence of cardiovascular diseases was found among Middle Eastern, South Asian, and some European immigrants in Australia, and a higher frequency of CVD (cardiovascular disease) risk factors was found among Middle Eastern and Southern European immigrants (Dassanayake et al., 2009). In Western Europe, most migrant groups were at a similar or higher risk of ischemic heart disease and stroke compared with the host population (Sohail et al., 2015; Cainzos-Achirica et al., 2019). In the United States, foreign-born adults had a lower prevalence of coronary heart disease and stroke than US-born adults (Fang et al., 2018).
The analysis of the 2010–2016 National Health Interview Survey in the United States showed that migrants from Mexico, Central America, the Caribbean, and the Indian subcontinent have the highest burden of obesity and diabetes, while those from Southeast Asia and Russia bore the highest burden of hypertension (Commodore-Mensah et al., 2018). Similar results can be found by Oza-Frank et al. (2010) and Engelman and Ye (2019). A higher risk of diabetes for different ethnic groups is found in the United States (Engelman & Ye, 2019; Commodore-Mensah et al., 2018). This also seems to be the case for immigrants groups in Northern Europe (Uitewaal et al., 2004). Results in the United States show considerable heterogeneity in the prevalence of diagnosed hypertension among immigrants (e.g., immigrants from Russia and Southeast Asia have a high hypertension prevalence) (Commodore-Mensah et al., 2018). Studies on blood pressure in Europe show similar results (Lane et al., 2002; Nilsson et al., 2017). Hepatitis B and C are estimated to be higher among immigrants than the general population (Rossi et al., 2012; Hahné et al., 2013; Seedat et al., 2018). Reviews studies show that tuberculosis in migrant populations remains higher in most of the world regions (Kärki et al., 2014; Seedat et al., 2018; World Health Organization, 2020). It seems that most migrant groups in Europe faced higher mortality due to infectious diseases and homicide, but lower mortality due to cancer and suicide (Ikram et al., 2016).
2.1.3 Mental Health
Three cycles of the Canadian Health Measures Survey were analyzed. The results show that within 5 years migrants described better self-perceived mental health, but after immigration, this effect disappeared over time. Other predictors were older age, higher income, a better sense of community belonging, and employment. Equally, diagnosis of mood disorders was less likely to be reported in recent migrants. The migration status per se was not associated with self-reported well-being but was associated with reduced odds of being diagnosed with a mood disorder as compared with Canadians (Salami et al., 2017). Studies in the United States show that there is a high need for mental health services for Hispanics immigrants there. Higher rates of depression, anxiety, and substance use disorders were found (Bridges et al., 2012; Alegría et al., 2007).
A study on White, Black-Caribbean, Indian, Pakistani, and Bangladeshi ethnic groups in the United Kingdom evaluated mental disorders between different ethnic groups. The propensity-matched analysis sample assessed 766 (23.8%) as having a common mental disorder, which is a similar percentage as the current population in the United Kingdom. In the propensity-matched analysis, immigrants were significantly associated with a lower risk of common mental disorders than non-immigrants (Dhadda & Greene, 2018). In contrast, studies about South Asian immigrants in the United Kingdom show higher rates of depression and anxiety (Gater et al., 2009; Taylor et al., 2013). A systematic review on schizophrenia in the United Kingdom shows increased rates, especially in Caribbean migrants (Hutchinson & Haasen, 2004). In Denmark, a researcher found an increased risk for schizophrenia (Cantor-Graae et al., 2003). Similar results on mental health were found in Sweden (Gilliver et al., 2014), Norway (Abebe et al., 2014), the Netherlands (Veling et al., 2006), and Spain (Robert et al., 2014). In Germany, studies show that a so-called migration background is a significant predictor of worse mental health outcomes (Nesterko et al., 2019a, 2019b; Janssen-Kallenberg et al., 2017). Despite anti-discrimination laws, the health of immigrants in Germany is negatively predicted by perceived discrimination (Schunck et al., 2015) and by older age, low socioeconomic status, and acculturation pressures (Janssen-Kallenberg et al., 2017).
A look at international meta-analysis or scoping studies presents the following picture. A scoping review by Patel et al. from 2017 revealed that: “[…] whilst migrants can be at an increased risk of developing psychotic disorders and suicide mortality, they are less likely to use psychotropic medication and mental health-related services” (Patel et al., 2017, p. 1). Another international meta-analysis of 21 studies found that migrants experience higher rates of mental health problems than non-migrants (Bourque et al., 2011). Similar results were seen with cases of schizophrenia and related psychotic disorders (Cantor-Graae & Selten, 2005; Henssler et al., 2020).
Refugees have a higher risk of some psychiatric disorders, such as psychosis, trauma- and stress-related disorders, and insomnia compared with other non-refugee migrants and the general population (Richter et al., 2018; Lindert et al., 2018; Bogic et al., 2015; Hollander et al., 2016).
Most findings show an increased rate of mental illness for so-called migrants in western states compared with non-migrants, especially for refugees and asylum seekers. It is important to consider variables like age, gender, and socioeconomic determinants, such as low income, unemployment, and a poor sense of community belonging, which influence the health outcomes of migrants (Salami et al., 2017). Refugees especially suffer from mental illness compared with non-migrants (Lindert et al., 2018) as well as labor migrants (Lindert et al., 2009).
2.1.4 Summary
According to Rechel et al. (2013, p. 1235): “Although migrants are often, at least initially, relatively healthy compared with the non-migrant population in the host country, available data suggest that they tend to be more vulnerable to certain communicable diseases, occupational health hazards, injuries, poor mental health, diabetes mellitus, and maternal and child health problems.” Information systems should implement an improved data collection system to get a deeper look at health differences between immigrants and non-migrants. Therefore, it is significant to combine the data with variables like gender, socioeconomic status, age, income, unemployment, social integration, and racism and discrimination.
2.2 Health Behavior and Migration
2.2.1 HIV and Obesity
While a high prevalence of overweight and obese people was found among the first generation of migrants from Turkey and Morocco (Dijkshoorn et al., 2008), this is no longer true for the second generation in the Netherlands compared with the Dutch host population (Dijkshoorn et al., 2014). A study in the United Kingdom found evidence of weight increases in immigrants during their time there (Averett et al., 2012). A higher BMI for children is found in Switzerland (Eiholzer et al., 2021) and Germany (Santos-Hövener et al., 2019), while in Italy overweight and obese immigrants have the same dimensions as Italians. In Australia, evidence shows that so-called ethnic differences have an influence on obesity, especially for male immigrants from North Africa, the Middle East, and Oceania. This study suggests that greater acculturation may have a negative impact on immigrants (Menigoz et al., 2016). A systematic review shows weight gain in the immigrant population and greater risk of obesity over time (10–15 years after migration) compared with the native populations (Murphy et al., 2017). Another review evaluates a positive correlation between acculturation and obesity in populations migrating to high-income countries from low- to middle-income countries (Delavari et al., 2013). It seems that living in the global north increases the likelihood of being overweight or obese over the years.
A systematic search of 35 studies by Alidu and Grunfeld (2018), predominantly undertaken in the United States, Canada, Australia, and the United Kingdom, showed that acculturation is associated with weight gain and obesity amongst migrants in most studies. “However, current literature and measures are not exhaustive and lack a detailed focus on the role of extraneous and social sources (including the media, family units, wider social networks) and the role of neighborhood or work-related influences” (Alidu & Grunfeld, 2018, p. 739). A small study from Khafaie et al. (2016) with Iranian students who migrated to India found that migration changed the lifestyles of students in an unfavorable way. Prevalence of smoking, no exercise, and low intakes of whole-grain bread as well as fruits and vegetables increased. After their resettlement in developed countries, even refugee children (2–16 years old) are likely to eat unhealthier and become less active (Alsubhi et al., 2020). Other factors that influence health behaviors include acculturation, environmental, socioeconomic status, cognition, and family (Alsubhi et al., 2020).
The systematic review (n = 24) by Michalopoulos et al. (2016) demonstrated an overall relationship between trauma and HIV risk behaviors among both forced and unforced migrant populations from low and middle income countries (LMIC). “More specifically, sexual violence was consistently associated with HIV sexual risk behaviors and HIV infection across the studies” (Michalopoulos et al., 2016, p. 257).
Men who have sex with men (MSM) bear a disproportionate burden of HIV in North American and European countries. The systematic review by Lewis and Wilson (2017) revealed high rates of HIV, unprotected sex, and stimulant use in foreign-born Latino samples. They also found evidence of high rates of alcohol and club drug use among foreign-born Asian Pacific Islanders, which provide baseline evidence for the theory of migration and HIV risk as syndemics within ethnic minority populations in North American and European countries (Lewis & Wilson, 2017).
2.2.2 Alcohol and/or Substance Abuse
Harris et al. (2019) used the longitudinal Swedish register data from Psychiatry SwedenFootnote 2 to show that there were initially fewer detectable dependency disorders among migrants (alcohol and polydrug use disorders). “The incidence rate of any substance use disorder, including alcohol and polydrug use disorders, was between 48% and 54% lower in refugees and non-refugee migrants from similar regions of origin than the Swedish-born population, who had particularly high rates of alcohol use disorders” (Harris et al., 2019). However, this difference disappears over time—with the exception of cannabis use—and the incidence of dependency disorders among immigrants and the Swedish-born population is leveling out. “For all outcomes, rates in migrants converged to the Swedish-born rate over time, indicated by earlier age at migration or longer time lived in Sweden” (Harris et al., 2019, p. 2).
Patel et al. (2017) found—with the help of their scoping review on the use of registry and record-linkage—that migrants are less likely to use psychotropic medication and mental health-related services. Likewise, Horyniak et al. (2016) found forced migrants less likely to report alcohol or drug use compared to non-forced migrants. They systematically reviewed the literature and examined substance use among forced migrantsFootnote 3 (Horyniak et al., 2016). At the same time, there seem to be differences regarding female refugees. Based on a cross-sectional, population-based study in Sweden, female (but not male) refugees from low-income countries had a higher likelihood of purchasing psychotropic drugs than non-refugees (in this case often family members of refugees). They seem to be a risk group among immigrant women, whereas male refugee and non-refugee immigrants had the same risk patterns (Hollander et al., 2011).
A systematic review shows that young migrants from non-European countries and/or with a Muslim background (11–29 years old) consume less alcohol than native-born adolescents/young adults in European countries. The findings were mixed for tobacco and illicit drug use (van Dorp et al., 2021). For young migrants up to 18 years of age another review found decreased prevalence of some harmful health practices such as alcohol consumption, cannabis use, or use of stimulants/sedative hypnotics when compared with the majority population (Curtis et al., 2018).
2.2.3 Help Seeking Behavior
After reviewing 77 papers from nine European countries, Lebano et al. (2020) found evidence of persistent inequalities between migrants and non-migrants for access to healthcare services. There are unmet healthcare needs (especially mental and dental care) and legal barriers in accessing healthcare (Lebano et al., 2020). Lindert et al. (2008) assert that mental health and access to care facilities is shaped by migrants used patterns of help-seeking and by the legal frame of the host country. Other barriers described are language and communication barriers, overuse of emergency services, and underuse of primary healthcare services as well as discrimination (Lindert et al., 2008).
Ismayilova et al. (2014) found that labor migrants in Kazakhstan often do not see a doctor when needed (almost half of the participants). Female migrants and migrants with high mobility (additional trips to see family or friends) were at even higher risk of underutilization. Help seeking by non-English speaking migrant families with a newborn/young child seems to be mainly affected by (a lack of) cultural sensitivity/understanding of cultural practice differences on the supply side and difficulty accessing interpreters (Dougherty et al., 2020). Even migrant children show high levels of unmet healthcare needs (Curtis et al., 2018).
The systematic review of Selkirk et al. (2014) shows that three major barriers are associated with attitudes toward seeking psychological help: logistical barriers, cultural mismatch between service providers and participants, and preferences for other sources of assistance. Those who had a stronger identification with the host country’s culture than their own cultural heritage, fluency in the host country language, psychological attributions of distress, higher educational levels, higher socioeconomic status, were female and were of older age enjoyed better access (Selkirk et al., 2014). Byrow et al. (2020) showed cultural barriers, including mental health stigma and knowledge of dominant models of mental health, as one of three main barriers to help seeking. “(S)tructural barriers, including financial strain, language proficiency, unstable accommodation, and a lack of understanding of how to access services, and (c) barriers specific to the refugee experience, including immigration status, a lack of trust in authority figures and concerns about confidentiality” (Byrow et al., 2020, p. 1).
An overview of nine systematic reviews by Parajuli and Horey (2020) to identify barriers and facilitators to health service utilization by refugees in resettlement countries found three main barriers as well. Those issues were related to refugees (e.g., sociocultural factors, effects of previous experiences), health services (e.g., knowledge and skills of health professionals), and the resettlement context (including policies and practical issues). In contrast, behaviors of health professionals, health service responses, and approaches to care can facilitate help seeking. Even so, more research is needed to evaluate facilitators (Parajuli & Horey, 2020).
2.2.4 Summary
On the one hand, in most studies, so-called migrants seem to have a greater obesity risk over time. It seems that being in the global north and, especially, acculturation processes increase the likelihood of being overweight over the years. Studies also found baseline evidence for the theory of migration and HIV risk as syndemics within ethnic minorities. On the other hand, there seem to be fewer dependency disorders among migrants in contrast to people born in the host countries, but difference disappears over time. Female refugees could have special risks. Findings for young migrants, up to 18 years old, are mixed. Different studies concerning help seeking behavior found inequalities between migrants and non-migrants in access to healthcare services. Female migrants and migrants with high mobility were at even higher risk of underutilization. Barriers seem to be manifold.
2.3 Excursus: COVID-19 and Migration
In the United States, so-called ethnic minorities seem to be “at increased risk of acquiring COVID-19 and experiencing greater severity of infection and are at excess risk of death” (Abuelezam, 2020, p. 455). With the help of a systematic review and meta-analysis, Sze et al. (2020) found that in the United Kingdom and the United States individuals from Black and Asian ethnicities had a higher risk of COVID-19 infection compared with White individuals. Those of Black ethnicity were twice as likely to become infected with SARS-CoV-2 compared with White individuals. Although the relationship between COVID-19, ethnicity, and specific clinical outcomes is unclear in this research study, the authors assume that overcrowding, working conditions, racism, and structural discrimination (see also Wang et al., 2021) are the reasons for inequities in the delivery of care (Sze et al., 2020). Especially for Arab Americans Abuelezam (2020) assumes that higher infection and complication rates could also be influenced by “xenophobia and stigma, pre-existing conditions, crowded living conditions, lack of social support for new immigrants, and poor adoption of prevention behavior” (Abuelezam, 2020, p. 455). Underlying health conditions, such as diabetes and hypertension, which are known risk factors for increased severity of COVID-19 and death, are more prevalent in Arab Americans than among white populations in the United States. Ayoubkhani et al. (2021) make similar considerations. With the help of a census-based data set, they investigated firstly an ethnicity-specific substantially elevated mortality risk during the pandemic in England and Wales. “Secondly, this elevated risk was largely attenuated by location, living circumstances, socioeconomic factors, occupational exposure and self-reported health status” (Ayoubkhani et al., 2021, p. 1957). Particularly for males and during the pre-lockdown period some residual differences in risk remained. To understand the causal mechanisms further research is needed (Ayoubkhani et al., 2021, p. 1957). Suhardiman et al. (2021) video-interviewed 44 international and domestic labor migrants from Bangladesh, India, Laos, and Myanmar working in Laos, Myanmar, China, Singapore, and Thailand to understand how COVID-19 and ensuing policy responses shaped their mobility, evolving livelihoods, and well-being. They found that: “informal migrants faced heightened exposure to the virus under conditions of forced evictions, food shortages, job losses without any compensation payment, quarantining in cramped and unhygienic conditions, limited access to health care, and chaotic border-crossing areas” (Suhardiman et al., 2021, p. 102).
Refugee communities have been affected in various ways by the impact of COVID-19 and political reactions. Migration routes and therefore movement had been blocked. Also, refugees live in remote and isolated camps or in urban settings under precarious conditions that promote contagion with COVID-19.
When looking at Syrian refugees in Lebanon, Fouad et al. (2021) found vulnerability factors that directly impact important parameters of transmission dynamics, namely the physical environment in which refugees reside, especially the high levels of crowding, where physical distancing is virtually impossible. Inadequate access to clean water for hand and face washing complicates prevention. Limited use of masks, due to inadequate access and low levels of awareness, puts refugees at higher risk of contracting the infection. Inadequate access to healthcare (see above) and lack of awareness of symptoms and recommended course of action are also factors that may impact RFootnote 4 by increasing the duration of infectiousness (Fouad et al., 2021).
An online survey of Bhutanese and Burmese refugees in the United States (n = 218) shows the following risk factors for a COVID-19–infection: being an essential worker during the pandemic (e.g., in food supply chain industries, working at packing plants), having an infected family member (in multigenerational households), and being female (as females are more likely to care for family members with COVID-19) (Zhang et al., 2021).
2.4 Explanation Models for the Health Status of Migrants
How can these health differences be explained? There are diverse approaches that describe the positive as well as negative effects on the health and mortality on migrants. These factors can differ in the migration phase: premigration risk factors, migration (in transit) risk factors, and postmigration risk factors (Priebe et al., 2016). The influence of different factors depend on age, gender, socioeconomic status, unemployment, and social networks (Salami et al., 2017). Below we briefly present the most important effects.
2.4.1 Migration and Stress: Migration Stress Hypothesis
Migration can be described as a critical life event, which goes hand in hand with other great challenges. Migration and acculturation processes are often correlated to a special stress situation—even without the presence of a flight history or even traumatization—and can thus influence mental health and the emergence of mental and physical illnesses. Torres and Wallace (2013) argue that there is a significant relationship between premigration circumstances and postmigration psychological and physical health. Different stressors, like insecure living conditions/housing, legal residence rights, chronic occupational stress, (threatening) unemployment, isolation due to persistent separation and changing network relationships, marital problems, and intergenerational conflicts of norms and roles are recognized.
2.4.2 Economic and Occupational Stress as a Structural Effect: Theory of Underprivileged
Another negative effect is correlated to the theory of underprivileged status of migrants. Meta-reviews show that race, socioeconomic status, and gender do have an influence on health separately as well as combined (Williams et al., 2010). Migrants are frequently socially disadvantaged compared with non-migrants in areas like education and employment (Nazroo et al., 2020). Refugees and asylum seekers especially seem to be particularly affected (Richter et al., 2018). Socioeconomic status before crisis and migration provides limited protection (Bauer et al., 2020).
2.4.3 Healthy Immigrant Effect and Their Explanations
A systematic review in Canada shows a healthy immigrant effect. It appears to be strongest during adulthood but less during childhood or adolescence and late in life. A foreign-born health benefit is likewise more robust for mortality but less so for morbidity (Vang et al., 2017). This Healthy Immigrant (or Migrant) Effect for mortality is explained in different ways. The positive outcome is explained by a healthy, strong, and young effect, by a healthy lifestyle effect based on, for instance, religious reasons (e.g., alcohol and drugs are not allowed in religious communities), and by the healthcare systems effect in the host countries. It is argued that migrants do combine advantages and have been confronted with different circumstances in the country of origin and host country (Vanthomme & Vandenheede, 2019).
2.4.4 Use of Health Services: Barriers to Entry
In the United States, the identified barriers to receiving services were cost, lack of health insurance, and language (Bridges et al., 2012). An international review shows barriers encountered by refugees, asylum seekers, and irregular migrants in accessing mental healthcare. Those barriers include a lack of knowledge regarding their healthcare entitlements and of the healthcare systems in the host country, poor language expertise in the host country, belief systems and cultural expectations for healthcare, and a lack of trust in professionals and authorities in the official healthcare system (Priebe et al., 2016; Lebano et al., 2020).
2.4.5 Racism and Exclusion
Discrimination and social exclusion have negative effects on health (Henssler et al., 2020). A correlation between perceived ethnic discrimination and well-being in ethnic minority groups can be found. “As such, ethnic inequalities in depression could be reduced substantially if ethnic minority groups would not perceive any ethnic discrimination” (Ikram et al., 2015, p. 243).
3 Social Networks of Migrants: The Role of Social Networks in the Migration Process
While the concept of social networks has played a role in migration research at a very early stage (e.g., chain migration) (Boyd, 1989; Jedlicka, 1978), methods of network analysis have only been used more recently (Lubbers et al., 2010; Gamper & Reschke, 2010). It is striking, however, that network analysis is mainly related to social capital theory (Gamper, 2015) and the support provided by migrant networks is examined (Portes, 1995; Pohjola, 1991). Against this background, the studies can be distinguished between structure-describing and resource-oriented research perspectives.
From a structure-describing research perspective, the relationships and the network structure of migrants and their individual embedding in the social environment are examined (Lubbers et al., 2010; Gamper et al., 2013). There is often a strong reference to network analysis, but it also includes other methodological approaches. Resource-oriented approaches tend to focus more on the support services available (e.g., monetary loans, emotional support) (Bashi, 2007). Even though some of these approaches refer to networks, network analysis in the narrower sense of the term is rarely used.
In addition to the preceding methodological distinction, networks can theoretically play an important role in three different phases of migration: Firstly in the decision to emigrate, secondly within the migration or migration process, and thirdly after arrival in the destination country. These three processes can repeat in the life course. In this context, research focuses on different aspects.
3.1 Decision-Making on Migration
As early as 1964, MacDonald and MacDonald introduced the concept of chain migration. They assume that pioneer migrants influence the actors in their network by providing support and information. It is argued that pioneer migrants are exposed to high migration costs and risks, while subsequent migrants have to make less effort, as they can mobilize their network resources—those who migrated before them—to find work or housing and to get help in obtaining or filling in official documents (Fussell & Massey, 2004).
Studies have shown that, regardless of the previous migration experience of the interviewees, the probability of migration increases if they make contact with actors in the country of arrival (e.g., good friends, family) (Massey et al., 1993; Palloni et al., 2001). With the help of simulations, Teteryatnikova (2013) was able to illustrate that even a small increase in personal contacts with people in a destination country can significantly increase the migration rate. In some cases, experienced migrants even explicitly look for newcomers, carefully selecting which actors support them (Bashi, 2007).
However, the influence of social networks on decision-making should not be seen as exclusively positive. There are three arguments regarding this. Networks can (1) limit the selection of emigration destinations through so-called “migration corridors.” Certain migration groups focus on certain destination countries, which can lead to dependency (e.g., costs for smugglers) (De Haas, 2007; Parsons et al., 2007). Although the effects of network structures have not yet been researched in detail, researchers assume that (2) dense networks and strong, supportive connections in the country of departure (e.g., through close emotional ties) can also prevent migration (Haug, 2008). Finally, (3) network-based migration can lead to dependency on both individuals and entire economies, for example by making countries dependent on remittances (Boyd, 1989).
3.2 Migrant Networks in the Transit or Border Crossing Phase
Another line of research sheds light on the role of social networks during migration along the different migration routes. Recent ethnographies (e.g., Andersson, 2014) describe the physical dangers, violence, and exploitation migrants often face on south to north routes. The few studies dealing with the role of social networks in this phase argue that personal ties facilitate border crossing. For example, personal connections provide valuable information on how to find helpers or smugglers to cross national borders (Bilecen, 2012; Garip, 2016). Koser (1997) argues that the social network approach is crucial for understanding the asylum process. Koser and Pinkerton (2002) further argue that social networks influence the when and where of migration. Recent findings among Syrian refugees in Jordan also point out that the increasingly restrictive entry policy of Jordanian migrants forces them to resort to weaker ties—professional actors and smugglers who, in turn, influence the migrants’ travel plans and provide coping strategies (Lagarde & Doraï, 2016). Against this background, network analysis as well as other methods for the description of relations will be used.
3.3 Migrant Networks in the Post-migration Phase
The majority of migration studies on social networks focus on the post-migration phase. These studies primarily focus on egocentric networks and often relate them to controversial concepts such as social integration or social assimilation. To this end, the research analyzes general characteristics of the network, such as the size and composition of the network in relation to the number of the “native population,” “compatriots,” and “other migrants.” Other factors are, for example, the role of the alteri (e.g., work colleagues, friends) or the strength and duration of the bond (e.g., Bashi, 2007; Brandes et al., 2008, 2010; Kindler et al., 2015). The main assumption of this research is that the more ties migrants have with the native population in the country of immigration, the higher is their social integration (Eisenstadt, 1952; Gordon, 1964; Nauck, 1989; Facchini et al., 2014). Studies show that migrants depend heavily on contacts with their compatriots in their new country of residence in the first arrival phase (e.g., Bashi, 2007; Bauer et al., 2009), but then the networks become more and more heterogeneous over time (Facchini et al., 2014).
In addition to describing personal networks in terms of their size, composition, and structure, researchers have analyzed the social support services in networks. They focus on the support provided by local, international, and transnational relationships (e.g., Bilecen, 2016; Herz, 2015; Schweizer et al., 1998; Olbermann, 2003). Although research generally assumes a positive relationship between perceived stress or health and networks, it is usually not analyzed through network analysis.
Social capital research also focuses on the exchange of resources in migrant networks. Theories of social capital tend to combine concepts of support and social integration. The focus here is primarily on “integration” into the labor market (Sommer & Gamper, 2018). The studies available to date show that integration into the labor market depends not only on networks but especially on the respective context conditions. On the basis of the Migrations between Africa and Europe Project (MAFE), a recent network study by Toma (2015) showed that the connection to former migrant women on arrival has positive effects on the economic situation of Senegalese men in France. France’s Senegalese community is socioeconomically diverse and thus offers many points of contact. Such a network effect is not found in Spain or Italy. Here the networks are usually concentrated only in the low-wage sector. These findings suggest that the functioning of personal networks and their results also depend strongly on the legal, economic, and cultural context in which these networks operate (e.g., Sommer & Gamper, 2021; Lubbers et al., 2020).
While the classical migration research presented above understands the migration process as a “one-way street,” there are research projects that can be subsumed under the term transmigration (Bilecen et al., 2018). Here, social networks of relationships are of particular importance. The concepts of “transnationalism” (Pries, 2008), “transstate spaces” (Faist, 2007), and “social fields” (Levitt & Glick Schiller, 2007) should be mentioned here. These studies focus on the network of relationships of (trans-)migrants (Lutz, 2008), who are usually both spatially and socially mobile, who span their social network globally and often commute between several states. “Trans-” describes the social, economic, political, and cultural cross-border relations of migrants and the active shaping of these constructed border spaces. Qualitative as well as quantitative network research examines, for example, the nature of relationships, social benefits, and the role of the Alteri in these transnational networks (Lubbers et al., 2020; Dahinden & Ryan, 2021).
4 Migration, Social Networks, and Health
While there are numerous studies on the topics of “migration and health or health inequalities” and “migration and social networks,” research that covers all three areas together is very rare and almost always looks at only one population group—exclusively migrants without comparison groups—without additionally broadening the view to vertical dimensions of inequality such as income or education. Most studies also use the concept of the network as a metaphor, a synonym for group or social capital. Or else, they exclusively investigate social support as a central function of social networks. Particularly with reference to the migration stress hypothesis mentioned in Sect. 2.4.1 and the resource-oriented research perspective mentioned in Sect. 3, social support from social networks as a buffer against migration-related stress is then examined alongside personal resources (e.g., beneficial control convictions, optimism, material resources). The connection between social support and the psychological well-being of migrants has been proven in many cases (Jasinskaja-Lahti et al., 2006). For example, an adequate social support system reduces the probability of manifested psychiatric disorders (Jasinskaja-Lahti et al., 2006), and effective social support reduces many developmental risks for migrants (Ralston & Escandell, 2012).
Below we present research that attempts to link all three areas—migration, health, and social networks. We use a very broad concept of “migration” and also list studies that work with the terms “race” or “ethnicity” or examine internal migration (e.g., from rural to urban areas). The presentation is divided thematically into studies on physical health and healthcare, coping with health problems, pregnancy, contraception, infant health, and mental health and quality of life. As mentioned above, the studies were made without comparison groups.
4.1 Physical Health (Transplantation, Cancer, Coronary Heart Disease) and Healthcare
Cetingok et al. (2008) examined the effects of social support on the mental and physical health of 258 transplant recipients. For this purpose, the authors used network cards in which the subjects could mark their relationships with friends, acquaintances, and family members. Measures such as network size and form of support were then statistically evaluated. The authors interviewed persons who were differentiated according to their gender, social class, and “race.” Close and other family members provide the most support. The authors also point out: “African Americans reported a higher frequency and longer duration of social support than did whites […]. Social and nursing intervention may improve the network closeness in males and may also augment support frequency and duration for whites” (Cetingok et al., 2008, p. 87).
Another study uses so-called resource generators in order to investigate the social support of Chinese people with cancer living in Hong Kong. Different types of support were surveyed, the role of the age group was investigated, and the size of the support network was included in the statistical calculation. The results support the connection between social support and coping successfully after being diagnosed with cancer. During the postoperative phase, material and informational support seems to be more relevant for effective coping than emotional support. In addition, the involvement of family members in patient care is crucial (Chan et al., 2004).
Pollard et al. (2003) looked into the influence that (the lack of) social support could have. They compared 684 South AsiansFootnote 5 and 825 EuropeansFootnote 6 in Newcastle upon Tyne (Britain) concerning the influence of social network size for having coronary heart disease risk factors (health behaviors such as smoking and being overweight, blood pressure, serum lipid profile). Social network size is composed of marital status, household size, contact with friends and relatives, and attendance at worship gatherings. The only significant relationship found in this study was that Europeans, but not South Asians, with larger social networks were significantly less likely to smoke. However, they found that: “South Asians, as a whole, had smaller networks of relatives and friends outside the household, but bigger household networks, and more contact with others at places of worship” (Pollard et al., 2003, p. 273). Overall, “there was no clear evidence of a protective effect of larger social networks for abdominal obesity, blood pressure or serum lipid profile” (Pollard et al., 2003, p. 274). The secondary evaluation of the Mexican Migration Project (MMP) by Ralston and Escandell (2012) studied 1776 Mexican men between 17 and 89 years of age (interviewed between 1998 and 2009). The influence of social networks on the use of hospital care by Mexicans in the United States was examined. Network relationships are surveyed via closed questions, such as whether the mother, father, or siblings lived in the United States during one of their last migration stays (0–6, close family contact), so that social networks as the respondent’s family and friends’ past and current migration experience to the United States is conceptualized (Ralston & Escandell, 2012, p. 327). The Mexican Migration Project shows the importance of (especially close) family social networks of migrants as mediators in the healthcare system. Migrants with a higher number of family members who have migrated themselves are also more likely to use hospital care. Friendship networks did not show any significant influence. “Mexican migrants likely rely on family members for information about healthcare alternatives because close family networks facilitate higher levels of trust and obligation” (Ralston & Escandell, 2012, p. 333).
Another qualitative network study (48 in-depth interviews) analyzed the role of social networks on the health behaviors of Sri Lankans and Anglo-Australians. The study shows that the decision-making process involved in seeking help for depression is highly correlated to interactions with actors in the social network. Social networks have a great influence over the care trajectory of people living with depression. Strong ties (e.g., parents) especially have influence and provide emotional and practical support. According to the authors: “[…] the role of social networks is pivotal in uptake of formal care, and engaging with communities to improve responses of social networks to mental illnesses may provide a bottom-up avenue for improving uptake of mental health services in migrant communities” (Antoniades et al., 2018, p. 1376).
4.2 Tackling Health Problems
The explorative research work of Li and Wu (2010) based on case studies investigate the role of social networks for Chinese people migrating from rural regions to the urban region of Beijing in coping with health problems. For this purpose, the authors conducted semi-structured interviews with 36 migrants (16 women and 20 men, 18–50 years old), which were evaluated using the Grounded Theory. The network size and composition were determined on the basis of with whom the respondents feel closely connected or with whom they have regular contact. In the interviews, social and especially family network members were seen as a great support for critical life events. In times of financial need, siblings and nephews, but also friends with the same migration history, are approached for help. Emotional support also comes primarily from the above-mentioned support sources. However, the strong reference to so-called strong ties who do not live at the place of arrival and lose contacts outside the family networks prevent the interviewees from turning to people in their environment in emotionally stressful situations (loneliness, lack of sleep) of migration. Restricted and missing social networks at the place of arrival thus have a negative impact on the state of health as well as access to healthcare. According to the authors: “However, due to the limited social networks of migrants in urban areas, it is difficult for them to obtain useful health information or information sources at the right time” (Li & Wu, 2010, p. 375).
In the early, representative research work of Chatters et al. (1985), informal helpers’ networks of 581 older “blacks” were surveyed, and their structure as a dependent variable (network size and composition) of health factors was investigated. The network survey was conducted on the question of who would help with illness and health restrictions (e.g., physical disability). A list of 12 persons (partner, son, sister, friend, neighbor, etc.) was presented, and they were grouped into categories. Unmarried, childless respondents had smaller networks, and women indicated more supporters than men. However, the experience of health restrictions, disabilities, and health problems, and the satisfaction or dissatisfaction with one’s own health status (as health factors), had no significant influence on the network size and composition (kin/non-kin/mixed).
4.3 Pregnancy, Contraception, and Child Health
The qualitative study by Chakrabarti (2010) aims to show the importance of social networks for the healthy pregnancy of Bengali women in New York. On the basis of 40 in-depth interviews, the author proved that local relationships are helpful, but transnational relationships also play an important role. Material and “virtual” support from personal face-to-face contacts such as telephone conversations seemed significant. Advice on healthy pregnancy, healthy nutrition, and food preparation, but also therapeutic conversations, proved to be important forms of support through “therapeutic networks.”
Wakeel et al. (2013) also examine the connection between pregnancy and available personal capital. They ask to what extent belonging to different ethnicities (Hispanic, Black, White, Asian/Pacific Islander, extracted from the birth register) influences the personal capital available during pregnancy and what role the socio-demographic characteristics of the 3716 mothers surveyed and their acculturation factors (origin, language spoken at home) play in this context. Personal capital was recorded as a scale of 30 items weighted by groups, consisting of individual resources (e.g., self-esteem, seven items), partnership support (Fragile Families Study, six items), family and friendship support (Pregnancy Risk Assessment Monitoring System, seven items), and neighbor support (Project on Human Development in Chicago Neighborhoods, ten items). The calculations were initially based on one-way ANOVA tests and then on multivariate, generalized linear models to understand the relationship between personal capital and socio-demographic data as well as acculturation factors. In this context, existing differences in available personal capital between Black-White and Hispanic-White were elucidated by socio-demographic characteristics such as income, education, and marital status. Thus, low socioeconomic status, single parenting, and low acculturation are mainly decisive for lower personal and social resources (capital), which in turn can influence maternal and child health. All in all, the study provides group comparisons, but the focus on health is pushed into the background—only the choice of mothers as interviewees and the view on the future health of mother and child, possibly influenced by the social network, are considered.
Similarly, Blackstock et al. (2010) examine the influence of social networks and primary healthcare (such as family doctors) on family planning and contraceptive use. The starting point is the increasing number of unplanned pregnancies, especially among African-American women, from the lower social strata in urban areas. Unplanned pregnancies are often associated with poorer health of mothers and newborns. In the 20 semi-structured interviews, the women revealed the importance of female network members, particularly for (first-time) information on contraceptives (often from female relatives) and the development of attitudes and subjective norms regarding their own family planning.
Using data from the Health and Migration Survey (HMS), Donato and Duncan (2011) explore the impact of parental migration on child health by comparing a total of 804 children of parents who have migrated from Mexico to the United States, remigrated, or never migrated, in terms of their mother’s assessment of their health. Family network resources (as an independent variable), network size, frequency of contact, and residence were surveyed by closed questions about relationships and interactions and support of family members (parents, siblings, cousins, uncles/aunts, grandparents, in-laws) and an open question about other, unmentioned network relationships. Where children in the United States have better health than children in Mexico, especially compared with children of remigrated parents, social networks have no (buffering) influence on the health of remigrated children. In some cases, close network members of remigrated families may be disappointed by the lack of financial support, or their absence due to migration may have weakened family relationships. In contrast, social networks (as weekly meetings with friends and family, along with the mother’s health and education) have a positive influence on the health of children living in the United States.
4.4 Mental Health and Quality of Life
The work of Vega et al. (1991) questions the influence of social networks (role relationships, frequency of contact, satisfaction) and the social support for 679 Mexican migrant women suffering from depression in the United States. “Family support and family income are the best predictors of low depression scores for immigrant Mexican women. In contrast, interaction contact frequency with friends and family is not correlated with depression” (Vega et al., 1991, p. 159). The significant role of (new) support networks in the country of arrival could explain why Mexican migrant women—despite great challenges—are not exposed to a higher risk of disease.
The research by Teodorescu et al. (2012) also focuses on mental health. For 55 adult refugees in psychiatric care in Norway, they show a strong association between post-traumatic stress and depressive/psychopathological symptoms with weak social integration and small friendship networks, whereas larger networks are more likely to be associated with post-traumatic growth. As a measure of social networking, the question: “How many good friends do you have? Count those with whom you can talk in confidence and who can help you if necessary,” (Teodorescu et al., 2012, p. 319) the size of the friendship network was chosen as a measure of social network. Social integration, meant as integration into Norwegian society, was measured by four items: language, reading Norwegian newspapers, Norwegian visitors, and help received from Norwegians.
Another study by Chandra and Batada (2006) investigates the perception of stress, social support, and coping strategies of 26 young African-Americans in ninth grade using a triangulative research design that includes ego-centered network cards to survey support networks. Depending on the topic—stress in the partnership or conflicts in school or family—different sources of support (partnership—friends, school—family) were requested. In addition, African-American girls report about active requests for help more often than boys.
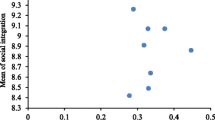
Finally, Baxter et al. (2015) surveyed 1039 Hispanics and non-Hispanic Whites over 60 years of age in the United States on the influence of network size (“How many close friends/relatives do you have?”) and contact frequency on the subjectively perceived quality of life. Regardless of “race” and “ethnicity” (which remain unclear as terms), a larger number of close friends and relatives and frequent contact with them have positive influence on the subjectively perceived quality of life, although this effect is more pronounced for non-Hispanic whites.
We ultimately found that transnational networks have a strong positive effect on how ageing migrants perceive their health (Cela & Di Barbiano Belgiojoso, 2019).
5 Conclusion and Desiderata
5.1 Desiderata on Migration and Health
The research field about migration and health is wide and quite heterogeneous. The studies give a good view of the issue but there is still some work to be done to study the link between migration and health, which has been documented for certain groups. To determine the influences of the majority society/dominant culture on the health of migrants, for example, comparative studies within different host countries would be needed. Although research shows that, for example, race, class, and gender are interrelated, more research is needed that is intersectionally designed to explain the interaction of multiple variables in more detail (Malmusi et al., 2010). Therefore, it is significant to combine the data with variables like gender, socioeconomic status, age, income, unemployment, social integration, and racism and discrimination. The data collection system should be improved and internationalized, in cooperation with countries of the global south especially, to get a deeper look at health differences.
Also, it is important to remember that migration is not a disease and is not pathological. In some cases, migration can be linked to different disease phenomena, but the correlation has to be discussed carefully. Many good quantitative studies can significantly draw correlations. However, there is a lack of qualitative research that traces the subjective view of those affected and attempts to better understand the links between migration and health.
It remains to be asked to what extent the phenomena associated with the concept of migration are actually migration-specific—whether, for example, there is a link to a concrete migration process or whether other social group affiliations have (higher) explanatory power for health inequalities like class and, therefore, income or educational status (Sheldon & Parker, 1992).
5.2 Desiderata on Migration and Social Networks
As the studies presented in Sect. 3 have shown, social relations play a major role in the migration process. However, we have to point out that although many of these studies examine relationships, a deep structural analysis (e.g., ERGMs) usually does not take place. With such an analysis, significant relationships between personal attributes (e.g., age, migration background) and relational aspects (e.g., density) could be identified. For example, measures such as network size and network roles (e.g., family, friends) are used as variables, but the analyses hardly go beyond that. Furthermore, the term “network” is often used as a synonym for group, social capital, or social support. The few network studies that do exist can be assigned to the ego-centered network analysis and focus mainly on the aspects of social integration or assimilation of migrants in the “host society.” Negative relationships (see chapter “Negative Ties and Inequalities in Health”) such as racist attacks or hostility are a desideratum so far. Studies on networks in the transit situation are also scarcely found.
5.3 Desiderata on Health, Migration, and Social Networks
Research linking health, networks, and migration is scarce. The few internationally available research works—primarily in the case of illness (transplant recipients, cancer, health problems in general)—relate to health behavior, health, and the use of healthcare and the support of networks. There are also studies with a preventive focus on quality of life, stress management mechanisms, or the handling of special life situations, such as pregnancy. Social networks are almost exclusively the independent variable.
In the studies presented, it becomes clear that social support can be very helpful. Support from the family, ongoing support in case of illness, and social integration through regular contacts play a central role. It is also striking that studies comparing “ethnic groups” are very rare. The focus here is usually on a specific migration group, such as Chinese women in Hong Kong.
However, beyond the size and the distinction between strong and weak relationships, which are often not discussed theoretically in the available studies, structural analyses are hardly found. In Sect. 3, “Social networks of migrants,” it becomes clear here that there is a deficit in the analysis of social networks. In addition, there is a lack of longitudinal studies that take into account the changes in networks or that investigate the direction of the context: In other words, whether networks influence health or health behavior or whether health or health behavior influences the networks (e.g., homophilia).
In addition, we have quoted studies that question people who have migrated and changed their place of residence (which, with regard to transmigration phenomena, occurs several times in commuting movements) and who are exposed to other contexts of belonging and possibly other influences on their health because of their ethnicity or simply because of their “skin color.” We consider it necessary to differentiate between these factors and plead for studies that, especially in German-speaking countries, question particularly vulnerable target groups (e.g., refugees, unemployed migrants) in a differentiated way.
6 Outlook
Before we give an outlook on possible future research we want to frame the studies mentioned above: studies with a so-called migrant focus on the global south and on migration routes from south to north. We rarely have information about the health of migrants traveling from north to south.
What should future studies look for in order to fill the research gaps we have identified? Against the background of the lack of overall network analyses, an attempt should be made to find fields of research (e.g., school classes, retirement homes) in which overall network measures can be used for the analysis. Here, new insights could be gained that take structural aspects in particular into account even better and reveal new connections beyond individual attributes (e.g., age, role). In ego-centered network analysis, it would be empirically important to include name generators and age-age relationships even more strongly in order to be able to calculate further structural measures here as well. Density or even clique formations would be attributes that could provide new insights, for example. Also, an extension of the network studies, which have so far been strongly focused on support, to other functions and mechanisms of action realized in social networks, such as social inclusion, influence, infection, or burden (see chapters “Social Network Mechanisms” and “Negative Ties and Inequalities in Health”), would in our opinion be useful. In general, it would be logical to link health, migration, and network variables even more closely, without directly considering certain phenomena as typical for migration, but always including the concept of intersectionality (e.g., gender, class) in one’s own research. Finally, as indicated in the dissertation by Olbermann (2003) on social networks of older migrants (n = 99), it would be important to take into account the life-specific characteristics of migrants and to consider social relationships as a dependent variable. In the study mentioned above, for example, older, unemployed, or early-retired migrants lacked financial resources to maintain social network relationships, which means that the health-related reduction of their social networks observed among very old people is likely to occur earlier among migrants (Olbermann, 2003, p. 144).
Reading Recommendations
-
Cetingok, M., Winsett, R. P., Russell, C. L., & Hathaway, D. K. (2008). Relationships between sex, race, and social class and social support networks in kidney, liver, and pancreas transplant recipients. Progress in Transplantation, 18(2), 80–88. An exploratory-descriptive analysis focused on social support, examining mental as well as physical health by socio-demographic and ethnic characteristics.
-
Donato, K. M., & Duncan, E. M. (2011). Migration, social networks, and child health in Mexican families. Journal of Marriage and Family, 73(4), 713–728. A quantitative comparative study between migrant, non-migrant, and remigrated families. The results are exciting, but the calculated network measures are not in focus.
Data Sets/Overview
-
The Socio-Economic Panel (SOEP) of the German Institute for Economic Research (DIW) has included a sample of people with a so-called migrant background (immigrant sample) and items to depict egocentric networks since 1994/95; see https://www.diw.de/soep/
Notes
- 1.
We could only consider literature published in English and German. This may lead to a concentration on the global north.
- 2.
Initial cohort of 1,345,320 people born between 1984 and 1997, of refugees, non-refugee migrants, and Swedish-born.
- 3.
Refugees, internally displaced people (IDPs), asylum seekers, people displaced by disasters, and deportees.
- 4.
Average number of infections generated by one infected individual.
- 5.
Newcastle residents with ancestral origins in India, Pakistan, or Bangladesh who had at least three grandparents born in those countries.
- 6.
Newcastle residents with ancestral origins in European countries.
References
Abebe, D. S., Lien, L., & Hjelde, K. H. (2014). What we know and don’t know about mental health problems among immigrants in Norway. Journal of Immigrant and Minority Health, 16(1), 60–67.
Abuelezam, N. N. (2020). Health equity during COVID-19: The case of Arab Americans. American Journal of Preventive Medicine, 59(3), 455–457.
Aldridge, R. W., Nellums, L. B., Bartlett, S., Barr, A. L., Patel, P., Burns, R., Hargreaves, S., Miranda, J. J., Tollman, S., Friedland, J. S., & Abubakar, I. (2018). Global patterns of mortality in international migrants: A systematic review and meta-analysis. Lancet, 392(10164), 2553–2566.
Alegría, M., Mulvaney-Day, N., Torres, M., Polo, A., Cao, Z., & Canino, G. (2007). Prevalence of psychiatric disorders across Latino subgroups in the United States. American Journal of Public Health, 97(1), 68–75.
Alidu, L., & Grunfeld, E. A. (2018). A systematic review of acculturation, obesity and health behaviours among migrants to high-income countries. Psychology and Health, 33(6), 724–745.
Alsubhi, M., Goldthorpe, J., Epton, T., Khanom, S., & Peters, S. (2020). What factors are associated with obesity-related health behaviours among child refugees following resettlement in developed countries? A systematic review and synthesis of qualitative and quantitative evidence. Obesity Reviews, 21(11), e13058.
Ambrosini, M., & van der Leun, J. (2015). Introduction to the special issue: Implementing human rights: Civil society and migration policies. Journal of Immigrant and Refugee Studies, 13(2), 103–115.
Andersson, R. (2014). Illegality.inc: Clandestine migration and the business of bordering Europe. California University Press.
Anikeeva, O., Bi, P., Hiller, J. E., Ryan, P., Roder, D., & Han, G.-S. (2010). The health status of migrants in Australia: A review. Asia-Pacific Journal of Public Health, 22(2), 159–193.
Anikeeva, O., Bi, P., Hiller, J. E., Ryan, P., Roder, D., & Han, G.-S. (2015). Trends in migrant mortality rates in Australia 1981–2007: A focus on the National Health Priority Areas other than cancer. Ethnicity and Health, 20(1), 29–48.
Antoniades, J., Mazza, D., & Brijnath, B. (2018). Agency, activation and compatriots: The influence of social networks on health-seeking behaviours among Sri Lankan migrants and Anglo-Australians with depression. Sociology of Health and Illness, 40(8), 1376–1390.
Averett, S. L., Argys, L. M., & Kohn, J. L. (2012). Immigration, obesity and labor market outcomes in the UK. IZA Journal of Migration, 1(1), 1–19.
Ayoubkhani, D., Nafilyan, V., White, C., Goldblatt, P., Gaughan, C., Blackwell, L., Rogers, N., Banerjee, A., Khunti, K., Glickman, M., Humberstone, B., & Diamond, I. (2021). Ethnic-minority groups in England and Wales-factors associated with the size and timing of elevated COVID-19 mortality: A retrospective cohort study linking census and death records. International Journal of Epidemiology, 49(6), 1951–1962.
Bashi, V. (2007). Survival of the knitted. Immigrant social networks in a stratified world. Stanford University Press.
Bauer, T., Epstein, G. S., & Gang, I. N. (2009). Measuring ethnic linkages among migrants. International Journal of Manpower, 30(1/2), 56–69.
Bauer, J. M., Brand, T., & Zeeb, H. (2020). Pre-migration socioeconomic status and post-migration health satisfaction among Syrian refugees in Germany: A cross-sectional analysis. PLoS Medicine, 17(3), e1003093.
Baxter, J., Shetterly, M., Eby, C., Mason, L., Cortese, C. F., & Hamman, R. F. (2015). Social networks factors associates with perceived quality of life. Journal of Aging and Health, 10(3), 287–310.
Bilecen, B. (2012). How to cross? Migrant perspectives. In A. Icduygu & D. Sert (Eds.), Borders under stress: The cases of Turkey-EU and Mexico-USA borders (pp. 167–182). ISIS.
Bilecen, B. (2016). A mixed-methods design of social network analysis to investigate transnational social protection. International Review of Social Research, 6(4), 233–244.
Bilecen, B., Gamper, M., & Lubbers, M. J. (2018). The missing link: Social network analysis in migration and transnationalism. Social Networks, 53, 1–3.
Blackstock, O. J., Mba-Jonas, A., & Sacajiu, G. M. (2010). Family planning knowledge: The role of social networks and primary care providers as information sources for African American women. American Journal of Sexuality Education, 5(2), 128–143.
Bogic, M., Njoku, A., & Priebe, S. (2015). Long-term mental health of war-refugees: A systematic literature review. BMC International Health and Human Rights, 15(1), 29.
Bourque, F., van der Ven, E., & Malla, A. (2011). A meta-analysis of the risk for psychotic disorders among first- and second-generation immigrants. Psychological medicine, 41(5), 897–910.
Boyd, M. (1989). Family and personal networks in international migration: Recent developments and new agendas. International Migration Review, 23(3), 638–670.
Brandes, U., Lerner, J., Lubbers, M., McCarty, C., & Molina, J. L. (2008). Visual statistics for collections of clustered graphs. In Proceedings of the 2008 IEEE Pacific Visualization Symposium, pp. 47–54.
Brandes, U., Lerner, J., Lubbers, M. J., McCarty, C., Molina, J. L., & Nagel, U. (2010). Recognizing modes of acculturation in personal networks of migrants. Procedia—Social and Behavioral Sciences, 4, 4–13.
Bridges, A. J., Andrews, A. R., & Deen, T. L. (2012). Mental health needs and service utilization by Hispanic immigrants residing in mid-southern United States. Journal of Transcultural Nursing: Official Journal of the Transcultural Nursing Society, 23(4), 359–368.
Byrow, Y., Pajak, R., Specker, P., & Nickerson, A. (2020). Perceptions of mental health and perceived barriers to mental health help-seeking amongst refugees: A systematic review. Clinical Psychology Review, 75(101), 812.
Cainzos-Achirica, M., Vela, E., Cleries, M., Bilal, U., Mauri, J., Pueyo, M. J., Rosas, A., Enjuanes, C., Blaha, M. J., Kanaya, A. M., & Comin-Colet, J. (2019). Cardiovascular risk factors and disease among non-European immigrants living in Catalonia. Heart (British Cardiac Society), 105(15), 1168–1174.
Cantor-Graae, E., & Selten, J. (2005). Schizophrenia and migration: A meta-analysis and review. The American Journal of Psychiatry, 162(1), 12–24.
Cantor-Graae, E., Pedersen, C. B., McNeil, T. F., & Mortensen, P. B. (2003). Migration as a risk factor for schizophrenia: A Danish population-based cohort study. The British Journal of Psychiatry, 182(2), 117–122.
Cela, E., & Di Barbiano Belgiojoso, E. (2019). Ageing in a foreign country: Determinants of self-rated health among older migrants in Italy. Journal of Ethnic and Migration Studies, 15, 1–23.
Cetingok, M., Winsett, R. P., Russell, C. L., & Hathaway, D. K. (2008). Relationships between sex, race, and social class and social support networks in kidney, liver, and pancreas transplant recipients. Progress in Transplantation, 18(2), 80–88.
Chakrabarti, R. (2010). Therapeutic networks of pregnancy care: Bengali immigrant women in New York City. Social Science and Medicine, 71(2), 362–369.
Chan, C. W., Hon, H. C., Chien, W. T., & Lopez, V. (2004). Social support and coping in Chinese patients undergoing cancer surgery. Cancer Nursing, 27(3), 230–236.
Chandra, A., & Batada, A. (2006). Exploring stress and coping among urban African American adolescents: The Shifting the Lens Study. Preventing Chronic Disease. Public Health Research, Practice, and Policy, 3(2), 1–10.
Chatters, L. M., Taylor, R. J., & Jackson, J. S. (1985). Size and composition of the informal helper networks of elderly blacks. Journal of Gerontology, 40(5), 605–614.
Commodore-Mensah, Y., Selvin, E., Aboagye, J., Turkson-Ocran, R. A., Li, X., Himmelfarb, C. D., Ahima, R. S., & Cooper, L. A. (2018). Hypertension, overweight/obesity, and diabetes among immigrants in the United States: An analysis of the 2010–2016 National Health Interview Survey. BMC Public Health, 18(1), 773.
Curtis, P., Thompson, J., & Fairbrother, H. (2018). Migrant children within Europe: A systematic review of children’s perspectives on their health experiences. Public Health, 158, 71–85.
Dahinden, J., & Ryan, L. (Eds.). (2021). Special issue: How qualitative Social Network analysis can offer new opportunities in transnational migration research. Global Network, 22(3), 455–625.
Dassanayake, J., Dharmage, S. C., Gurrin, L., Sundararajan, V., & Payne, W. R. (2009). Are immigrants at risk of heart disease in Australia? A systematic review. Australian Health Review, 33(3), 479–491.
De Haas, H. (2007). Morocco’s migration experience: A transitional perspective. International Migration, 54(4), 39–70.
Deboosere, P., & Gadeyne, S. (2005). Adult migrant mortality advantage in Belgium: Evidence using census and register data. Population, 60(5), 655–698.
Delavari, M., Sønderlund, A. L., Swinburn, B., Mellor, D., & Renzaho, A. (2013). Acculturation and obesity among migrant populations in high income countries—a systematic review. BMC Public Health, 13, 458.
Dhadda, A., & Greene, G. (2018). ‘The healthy migrant effect’ for mental health in England: Propensity-score matched analysis using the EMPIRIC survey. Journal of Immigrant and Minority Health, 20(4), 799–808.
Dijkshoorn, H., Nierkens, V., & Nicolaou, M. (2008). Risk groups for overweight and obesity among Turkish and Moroccan migrants in The Netherlands. Public Health, 122(6), 625–630.
Dijkshoorn, H., Nicolaou, M., Ujcic-Voortman, J. K., Schouten, G. M., Bouwman-Notenboom, A. J., Berns, M. P. H., & Verhoeff, A. P. (2014). Overweight and obesity in young Turkish, Moroccan and Surinamese migrants of the second generation in the Netherlands. Public Health Nutrition, 17(9), 2037–2044.
Donato, K. M., & Duncan, E. M. (2011). Migration, social networks, and child health in Mexican families. Journal of Marriage and Family, 73(4), 713–728.
Dougherty, L., Lloyd, J., Harris, E., Caffrey, P., & Harris, M. (2020). Access to appropriate health care for non-English speaking migrant families with a newborn/young child: A systematic scoping literature review. BMC Health Services Research, 20(1), 1–12.
Eiholzer, U., Fritz, C., & Stephan, A. (2021). The increase in child obesity in Switzerland is mainly due to migration from Southern Europe–a cross-sectional study. BMC Public Health, 21(1), 1–11.
Eisenstadt, N. (1952). The process of absorption of new immigrants in Israel. Human Relations, 5, 223–246.
Engelman, M., & Ye, L. Z. (2019). The immigrant health differential in the context of racial and ethnic disparities: The case of diabetes. Advances in Medical Sociology, 19, 147–171.
Facchini, G., Patacchini, E., & Steinhardt, M. F. (2014). Migration, friendship ties and cultural assimilation. IZA Discussion Paper Series 7881. https://onlinelibrary.wiley.com/doi/epdf/10.1111/sjoe.12096
Faist, T. (2007). Transstate social spaces and development: Exploring the changing balance between communities, states and markets, international institute for labour studies. Discussion paper DP/169/2007 Decent Work Research Programme. ILO.
Fang, J., Yuan, K., Gindi, R. M., Ward, B. W., Ayala, C., & Loustalot, F. (2018). Association of birthplace and coronary heart disease and stroke among US adults: National health interview survey, 2006 to 2014. Journal of the American Heart Association, 7(7), e008153.
Fouad, F. M., McCall, S. J., Ayoub, H., Abu-Raddad, L. J., & Mumtaz, G. R. (2021). Vulnerability of Syrian refugees in Lebanon to COVID-19: Quantitative insights. Conflict and Health, 15(1), 13.
Fussell, E., & Massey, D. S. (2004). The limits of cumulative causation: International migration from Mexican urban areas. Demography, 41(1), 151–171.
Gamper, M. (2015). Die Sozialkapital-Theorie Bourdieus und ihre Bedeutung für die Migrationsforschung [=Bourdieu’s social capital theory and its relevance for migration research]. In J. Reuter & P. Mecheril (Eds.), Schlüsselwerke der Migrationsforschung – Pionierstudien und Referenztheorien (pp. 343–360). Springer VS.
Gamper, M., & Reschke, L. (Eds.). (2010). Knoten und Kanten: Soziale Netzwerkanalyse in Wirtschafts-und Migrationsforschung [=Nodes and edges: Social network analysis in economic and migration research]. Transcript.
Gamper, M., Fenicia, T., & Schönhuth, M. (2013). Transnationale Netzwerke, Sozialkapital und Migration – Eine triangulative Studie über die Vernetzung von Aussiedlern aus der ehemaligen Sowjetunion [=Transnational networks, social capital and migration - A triangulative study on the networking of repatriates from the former Soviet Union]. In A. Herz & C. Olivier (Eds.), Transmigration und Soziale Arbeit. Theoretische Herausforderungen und gesellschaftliche Praxis (pp. 249–272). Schneider.
Garip, F. (2016). On the move. Changing mechanisms of Mexico-US migration. Princeton University Press.
Gater, R., Tomenson, B., Percival, C., Chaudhry, N., Waheed, W., Dunn, G., Macfarlane, G., & Creed, F. (2009). Persistent depressive disorders and social stress in people of Pakistani origin and white Europeans in UK. Social Psychiatry and Psychiatric Epidemiology, 44(3), 198–207.
Gilliver, S. C., Sundquist, J., Li, X., & Sundquist, K. (2014). Recent research on the mental health of immigrants to Sweden: A literature review. The European Journal of Public Health, 24(suppl_1), 72–79.
Gordon, M. (1964). Assimilation and American life: The role of race, religion and national origins. Oxford University Press.
Guillot, M., Khlat, M., Elo, I., Solignac, M., & Wallace, M. (2018). Understanding age variations in the migrant mortality advantage: An international comparative perspective. PLoS One, 13(6), e0199669.
Hahné, S. J. M., Veldhuijzen, I. K., Wiessing, L., Lim, T.-A., Salminen, M., & van de Laar, M. (2013). Infection with hepatitis B and C virus in Europe: A systematic review of prevalence and cost-effectiveness of screening. BMC Infectious Diseases, 13(1), 181.
Hajat, A., Blakely, T., Dayal, S., & Jatrana, S. (2010). Do New Zealand’s immigrants have a mortality advantage? Evidence from the New Zealand census-mortality study. Ethnicity and Health, 15(5), 531–547.
Harris, S., Dykxhoorn, J., Hollander, A., Dalman, C., & Kirkbride, J. B. (2019). Substance use disorders in refugee and migrant groups in Sweden: A nationwide cohort study of 1.2 million people. PLoS Medicine, 16(11), e1002944.
Haug, S. (2008). Migration networks and migration decision-making. Journal of Ethnic and Migration Studies, 34(4), 585–605.
Henssler, J., Brandt, L., Müller, M., Liu, S., Montag, C., Sterzer, P., & Heinz, A. (2020). Migration and schizophrenia: Meta-analysis and explanatory framework. European Archives of Psychiatry and Clinical Neuroscience, 270(3), 325–335.
Herz, A. (2015). Relational constitution of social support in migrants’ transnational personal communities. Social Networks, 40, 64–74.
Hollander, A., Bruce, D., Burström, B., & Ekblad, S. (2011). Gender-related mental health differences between refugees and non-refugee immigrants—A cross-sectional register-based study. BMC Public Health, 11, 1–8.
Hollander, A., Dal, H., Lewis, G., Magnusson, C., Kirkbride, J. B., & Dalman, C. (2016). Refugee migration and risk of schizophrenia and other non-affective psychoses: Cohort study of 1.3 million people in Sweden. BMJ (Clinical research ed.), 352, i1030.
Horyniak, D., Melo, J. S., Farrell, R. M., Ojeda, V. D., & Strathdee, S. A. (2016). Epidemiology of substance use among forced migrants: A global systematic review. PLoS One, 11(7), e0159134.
Hutchinson, G., & Haasen, C. (2004). Migration and schizophrenia. Social Psychiatry and Psychiatric Epidemiology, 39(5), 350–357.
Ikram, U. Z., Snijder, M. B., Fassaert, T. J. L., Schene, A. H., Kunst, A. E., & Stronks, K. (2015). The contribution of perceived ethnic discrimination to the prevalence of depression. European Journal of Public Health, 25(2), 243–248.
Ikram, U. Z., Mackenbach, J. P., Harding, S., Rey, G., Bhopal, R. S., Regidor, E., Rosato, M., Juel, K., Stronks, K., & Kunst, A. E. (2016). All-cause and cause-specific mortality of different migrant populations in Europe. European Journal of Epidemiology, 31(7), 655–665.
Ismayilova, L., Lee, H. N., Shaw, S., El-Bassel, N., Gilbert, L., Terlikbayeva, A., & Rozental, Y. (2014). Mental health and migration: Depression, alcohol abuse, and access to health care among migrants in Central Asia. Journal of Immigrant and Minority Health, 16(6), 1138–1148.
Janssen-Kallenberg, H., Schulz, H., Kluge, U., Strehle, J., Wittchen, H.-U., Wolfradt, U., Koch-Gromus, U., Heinz, A., Mösko, M., & Dingoyan, D. (2017). Acculturation and other risk factors of depressive disorders in individuals with Turkish migration backgrounds. BMC Psychiatry, 17(1).
Jasinskaja-Lahti, I., Liebkind, K., Jaakkola, M., & Reuter, A. (2006). Perceived discrimination, social support networks, and psychological well-being among three immigrant groups. Journal of Cross-Cultural Psychology, 37(3), 293–311.
Jedlicka, D. (1978). Opportunities, information networks and international migration streams. Social Networks, 1(3), 277–284.
Johnson, C. M., Rostila, M., Svensson, A. C., & Engström, K. (2017). The role of social capital in explaining mental health inequalities between immigrants and Swedish-born: A population-based cross-sectional study. BMC Public Health, 17(1), 1–15.
Kärki, T., Napoli, C., Riccardo, F., Fabiani, M., Dente, M. G., Carballo, M., Noori, T., & Declich, S. (2014). Screening for infectious diseases among newly arrived migrants in EU/EEA countries—Varying practices but consensus on the utility of screening. International Journal of Environmental Research and Public Health, 11(10), 11004–11014.
Khafaie, M. A., Khafaie, B., Salmanzadeh, S., & Radkar, A. (2016). Health behavior of Iranian students in India-impact from migration. International Journal of Pharmaceutical Research and Allied Sciences, 5(2), 26–31.
Khlat, M., & Darmon, N. (2003). Is there a Mediterranean migrants mortality paradox in Europe? International Journal of Epidemiology, 32(6), 1115–1118.
Kibele, E., Scholz, R., & Shkolnikov, V. M. (2008). Low migrant mortality in Germany for men aged 65 and older: Fact or artifact? European Journal of Epidemiology, 23(6), 389.
Kindler, M., Ratcheva, V., & Piechowska, M. (2015). Social networks, social capital and migrant integration at local level. European literature review. Iris Working Paper Series No. 6/2015. Institute for Research into Superdiversity.
Koser, K. (1997). Social networks and the asylum cycle: The case of Iranians in the Netherlands. International Migration Review, 31(3), 591–611.
Koser, K., & Pinkerton, C. (2002). The social networks of asylum seekers and the dissemination of information about countries of asylum. http://www.urbanlab.org/articles/Koser_2002_SocialNetworksOfAsylumSeekers.pdf
Kouris-Blazos, A. (2002). Morbidity mortality paradox of 1st generation Greek Australians. Asia Pacific Journal of Clinical Nutrition, 11, S569–S575.
Lagarde, D., & Doraï, K. (2016). Host state policies and the changing role of social networks for Syrian refugees in Jordan. In XIII Annual Conference of the Italian Society of the Italian Society for Middle Eastern Studies (SeSaMO), March 2016, Catane.
Lane, D., Beevers, D. G., & Lip, G. Y. H. (2002). Ethnic differences in blood pressure and the prevalence of hypertension in England. Journal of Human Hypertension, 16(4), 267–273.
Lebano, A., Hamed, S., Bradby, H., Gil-Salmerón, A., Durá-Ferrandis, E., Garcés-Ferrer, J., Azzedine, F., Riza, E., Karnaki, P., Zota, D., & Linos, A. (2020). Migrants’ and refugees’ health status and healthcare in Europe: A scoping literature review. BMC Public Health, 20(1), 1039.
Levitt, P., & Glick Schiller, N. (2007). Conceptualizing simultaneity: A transnational social field perspective on society. In A. Portes & J. DeWind (Eds.), Rethinking migration. New theoretical and empirical perspectives (pp. 181–219). Berghahn.
Lewis, N. M., & Wilson, K. (2017). HIV risk behaviours among immigrant and ethnic minority gay and bisexual men in North America and Europe: A systematic review. Social Science and Medicine, 179, 115–128.
Li, Y., & Wu, S. (2010). Social networks and health among rural–urban migrants in China: A channel or a constraint? Health Promotion International, 25(3), 371–380.
Lindert, J., Schouler-Ocak, M., Heinz, A., & Priebe, S. (2008). Mental health, health care utilisation of migrants in Europe. European Psychiatry, 23(S1), s114–ss20.
Lindert, J., Ehrenstein, O. S., Priebe, S., Mielck, A., & Brähler, E. (2009). Depression and anxiety in labor migrants and refugees—A systematic review and meta-analysis. Social Science and Medicine (1982), 69(2), 246–257.
Lindert, J., von Ehrenstein, O. S., Wehrwein, A., Brähler, E., & Schäfer, I. (2018). Angst, Depressionen und posttraumatische Belastungsstörungen bei Flüchtlingen – eine Bestandsaufnahme [=Anxiety, depression, and post-traumatic stress disorder in refugees - a review]. Psychotherapie, Psychosomatik, medizinische Psychologie, 68(1), 22–29.
Lubbers, M. J., Molina, J. L., Lerner, J., Brandes, U., Ávila, J., & McCarty, C. (2010). Longitudinal analysis of personal networks. The case of Argentinean migrants in Spain. Social Networks, 32(1), 91–104.
Lubbers, M. J., Verdery, A. M., & Molina, J. L. (2020). Social networks and transnational social fields: A review of quantitative and mixed-methods approaches. International Migration Review, 54(1), 177–204.
Lutz, H. (2008). From the world market to the private household. The new maids in the age of globalization. Barbara Budrich.
MacDonald, J. S., & MacDonald, L. D. (1964). Chain migration, ethnic neighborhood formation, and social networks. Milbank Memorial Fund Quarterly, 42, 82–94.
Malmusi, D., Borrell, C., & Benach, J. (2010). Migration-related health inequalities: Showing the complex interactions between gender, social class and place of origin. Social Science and Medicine (1982), 71(9), 1610–1619.
Massey, D. S., Arango, J., Hugo, G., Kouaouci, A., Pellegrino, A., & Taylor, E. J. (1993). Theories of international migration: A review and appraisal. Population and Development Review, 19(3), 431–466.
Médecins Sans Frontières. (1997). Refugee health. An approach to emergency situations. Retrieved from http://ispeed.org/docs/1_Sante/Refugee.Health.An.Approach.to.Emergency.Situations_by_MSF.pdf
Menigoz, K., Nathan, A., & Turrell, G. (2016). Ethnic differences in overweight and obesity and the influence of acculturation on immigrant bodyweight: Evidence from a national sample of Australian adults. BMC Public Health, 16(1), 1–13.
Michalopoulos, L. M., Aifah, A., & El-Bassel, N. (2016). A systematic review of HIV Risk behaviors and trauma among forced and unforced migrant populations from low and middle-income countries: State of the literature and future directions. AIDS and Behavior, 20(2), 243–261.
Murphy, M., Robertson, W., & Oyebode, O. (2017). Erratum to: Obesity in international migrant populations. Current Obesity Reports, 6(4), 438.
Nauck, B. (1989). Assimilation process and group integration of migrant families. International Migration, 27(1), 27–48.
Nazroo, J. Y. (2003). The structuring of ethnic inequalities in health: Economic position, racial discrimination, and racism. American Journal of Public Health, 93(2), 277–284.
Nazroo, J. Y., Bhui, K. S., & Rhodes, J. (2020). Where next for understanding race/ethnic inequalities in severe mental illness? Structural, interpersonal and institutional racism. Sociology of Health & Illness, 42(2), 262–276.
Nesterko, Y., Friedrich, M., Brähler, E., Hinz, A., & Glaesmer, H. (2019a). Mental health among immigrants in Germany—The impact of self-attribution and attribution by others as an immigrant. BMC Public Health, 19(1), 1–8.
Nesterko, Y., Turrión, C. M., Friedrich, M., & Glaesmer, H. (2019b). Trajectories of health-related quality of life in immigrants and non-immigrants in Germany: A population-based longitudinal study. International Journal of Public Health, 64(1), 49–58.
Newbold, K. B. (2005). Self-rated health within the Canadian immigrant population: Risk and the healthy immigrant effect. Social Science and Medicine, 60(6), 1359–1370.
Nilsson, C., Christensson, A., Nilsson, P. M., & Bennet, L. (2017). Renal function and its association with blood pressure in Middle Eastern immigrants and native Swedes. Journal of Hypertension, 35(12), 2493–2500.
Olbermann, E. (2003). Soziale Netzwerke, Alter und Migration: Theoretische und empirische Explorationen zur sozialen Unterstützung älterer Migranten [=Social networks, age and migration: Theoretical and empirical explorations of social support for older migrants]. Dissertation, University of Dortmund. https://core.ac.uk/download/pdf/46902123.pdf%20.%20
Oza-Frank, R., Narayan, K., & Venkat, M. (2010). Overweight and diabetes prevalence among US immigrants. American Journal of Public Health, 100(4), 661–668.
Palloni, A., Massey, D. S., Ceballos, M., Espinosa, K., & Spittel, M. (2001). Social capital and international migration: A test using information on family networks. American Journal of Sociology, 106(5), 1262–1298.
Parajuli, J., & Horey, D. (2020). Barriers to and facilitators of health services utilisation by refugees in resettlement countries: An overview of systematic reviews. Australian Health Review, 44(1), 132–142.
Parsons, C. R., Skeldon, R., Walmsley, T. R., & Winters, A. L. (2007). Quantifying international migration: A database of bilateral migrant stocks. World Bank Policy Research Working Paper 4165. https://ssrn.com/abstract=969242
Patel, K., Kouvonen, A., Close, C., Väänänen, A., O’Reilly, D., & Donnelly, M. (2017). What do register-based studies tell us about migrant mental health? A scoping review. Systematic Reviews, 6(1), 1–11.
Pohjola, A. (1991). Social networks: Help or hindrance to the migrant? International Migration, 29(3), 435–444.
Pollard, T. M., Carlin, L. E., Bhopal, R., Unwin, N., White, M., & Fischbacher, C. (2003). Social networks and coronary heart disease risk factors in South Asians and Europeans in the UK. Ethnicity and Health, 8(3), 263–275.
Portes, A. (1995). Economic sociology and the sociology of immigration: A conceptual overview. In A. Portes (Ed.), The economic sociology of immigration (pp. 1–41). Russel Sage Foundation.
Priebe, S., Giacco, D., & El-Nagib, R. (2016). Public health aspects of mental health among migrants and refugees. A review of the evidence on mental health care for refugees, asylum seekers, and irregular migrants in the WHO European region. Health Evidence Network; World Health Organization, Regional Office for Europe (Health Evidence Network synthesis report, 47).
Pries, L. (Ed.). (2008). Rethinking transnationalism: The meso-link of organisations. Routledge.
Ralston, M. L., & Escandell, X. (2012). Networks matter: Male Mexican migrants’ use of hospitals. Population Research and Policy Review, 31, 321–337.
Razum, O., Zeeb, H., Akgün, H. S., & Yilmaz, S. (1998). Low overall mortality of Turkish residents in Germany persists and extends into a second generation: Merely a healthy migrant effect? Tropical Medicine and International Health, 3(4), 297–303.
Rechel, B., Mladovsky, P., Ingleby, D., Mackenbach, J. P., & McKee, M. (2013). Migration and health in an increasingly diverse Europe. The Lancet, 381(9873), 1235–1245.
Richter, K., Peter, L., Lehfeld, H., Zäske, H., Brar-Reissinger, S., & Niklewski, G. (2018). Prevalence of psychiatric diagnoses in asylum seekers with follow-up. BMC Psychiatry, 18(1), 206.
Robert, G., Martínez, J. M., García, A. M., Benavides, F. G., & Ronda, E. (2014). From the boom to the crisis: Changes in employment conditions of immigrants in Spain and their effects on mental health. The European Journal of Public Health, 24(3), 404–409.
Ronellenfitsch, U., Kyobutungi, C., Becher, H., & Razum, O. (2006). All-cause and cardiovascular mortality among ethnic German immigrants from the Former Soviet Union: A cohort study. BMC Public Health, 6(1), 16.
Rossi, C., Shrier, I., Marshall, L., Cnossen, S., Schwartzman, K., Klein, M. B., Schwarzer, G., & Greenaway, C. (2012). Seroprevalence of chronic hepatitis B virus infection and prior immunity in immigrants and refugees: A systematic review and meta-analysis. PLoS One, 7(9), e44611.
Ruiz, J. M., Steffen, P., & Smith, T. B. (2013). Hispanic mortality paradox: A systematic review and meta-analysis of the longitudinal literature. American Journal of Public Health, 103(3), e52–e60.
Salami, B., Yaskina, M., Hegadoren, K., Diaz, E., Meherali, S., Rammohan, A., & Ben-Shlomo, Y. (2017). Migration and social determinants of mental health: Results from the Canadian Health Measures Survey. Canadian Journal of Public Health. Revue Canadienne de Sante Publique, 108(4), e362–e367.
Santos-Hövener, C., Kuntz, B., Frank, L., Koschollek, C., Ellert, U., & Hölling, H. (2019). Zur gesundheitlichen Lage von Kindern und Jugendlichen mit Migrationshintergrund in Deutschland [=On the health situation of children and adolescents with migration background in Germany]. Bundesgesundheitsblatt-Gesundheitsforschung-Gesundheitsschutz, 62(10), 1253–1262.
Schunck, R., Reiss, K., & Razum, O. (2015). Pathways between perceived discrimination and health among immigrants: Evidence from a large national panel survey in Germany. Ethnicity and Health, 20(5), 493–510.
Schweizer, T., Schnegg, M., & Berzbon, S. (1998). Personal networks and social support in a multiethnic community of Southern California. Social Networks, 20, 1–21.
Scott, A. P., & Timæus, I. M. (2013). Mortality differentials 1991–2005 by self-reported ethnicity: Findings from the ONS Longitudinal Study. Journal of Epidemiology Community Health, 67(9), 743–750.
Seedat, F., Hargreaves, S., Nellums, L. B., Ouyang, J., Brown, M., & Friedland, J. S. (2018). How effective are approaches to migrant screening for infectious diseases in Europe? A systematic review. The Lancet Infectious Diseases, 18(9), e259–e271.
Selkirk, M., Quayle, E., & Rothwell, N. (2014). A systematic review of factors affecting migrant attitudes towards seeking psychological help. Journal of Health Care for the Poor and Underserved, 25(1), 94–127.
Setia, M. S., Lynch, J., Abrahamowicz, M., Tousignant, P., & Quesnel-Vallee, A. (2011). Self-rated health in Canadian immigrants: Analysis of the Longitudinal Survey of Immigrants to Canada. Health and Place, 17(2), 658–670.
Sheldon, T. A., & Parker, H. (1992). Race and ethnicity in health research. Journal of Public Health, 14(2), 104–110.
Shiels, M. S., Chernyavskiy, P., Anderson, W. F., Best, A. F., Haozous, E. A., Hartge, P., Rosenberg, P. S., Thomas, D., Freedman, N. D., & Berrington de Gonzalez, A. (2017). Trends in premature mortality in the USA by sex, race, and ethnicity from 1999 to 2014: An analysis of death certificate data. Lancet (London, England), 389(10073), 1043–1054.
Singh, G. K., & Siahpush, M. (2001). All-cause and cause-specific mortality of immigrants and native born in the United States. American Journal of Public Health, 91(3), 392–399.
Sohail, Q. Z., Chu, A., Rezai, M. R., Donovan, L. R., Ko, D. T., & Tu, J. V. (2015). The risk of ischemic heart disease and stroke among immigrant populations: A systematic review. The Canadian Journal of Cardiology, 31(9), 1160–1168.
Sommer, E., & Gamper, M. (2018). Transnational entrepreneurial activities: A qualitative network study of self-employed migrants from the former Soviet Union in Germany. Social Networks, 53, 136–147.
Sommer, E., & Gamper, M. (2021). Beyond structural determinism: Advantages and challenges of qualitative social network analysis for studying social capital of migrants. Global Networks, 21(3), 608–625.
Stanaway, F. F., Blyth, F. M., Naganathan, V., Le Couteur, D. G., Ribeiro, R., Hirani, V., Waite, L. M., Handelsman, D. J., Seibel, M. J., & Cumming, R. G. (2020). Mortality paradox of older Italian-born men in Australia: The concord health and ageing in men project. Journal of Immigrant and Minority Health, 22(1), 102–109.
Suhardiman, D., Rigg, J., Bandur, M., Marschke, M., Miller, M. A., Pheuangsavanh, N., Sayatham, M., & Taylor, D. (2021). On the Coattails of globalization: Migration, migrants and COVID-19 in Asia. Journal of Ethnic and Migration Studies, 47(1), 88–109.
Sze, S., Pan, D., Nevill, C. R., Gray, L. J., Martin, C. A., Nazareth, J., Minhas, J. S., Divall, P., Khunti, K., Abrams, K. R., Nellums, L. B., & Pareek, M. (2020). Ethnicity and clinical outcomes in COVID-19: A systematic review and meta-analysis. EClinicalMedicine, 29(100630), 100,630.
Tarnutzer, S., Bopp, M., & SNC Study Group. (2012). Healthy migrants but unhealthy offspring? A retrospective cohort study among Italians in Switzerland. BMC Public Health, 12(1), 1104.
Taylor, R., Brown, J. S. L., & Weinman, J. (2013). A comparison of the illness perceptions of North Indian and white British women. Journal of mental health (Abingdon, England), 22(1), 22–32.
Teodorescu, D.-S., Siqveland, J., Heir, T., Hauff, E., Wentzel-Larsen, T., & Lien, L. (2012). Posttraumatic growth, depressive symptoms, posttraumatic stress symptoms, post-migration stressors and quality of life in multi-traumatized psychiatric outpatients with a refugee background in Norway. Health and Quality of Life Outcomes, 10(84), 1–16.
Teteryatnikova, M. (2013). A model of social networks and migration decisions. University of Vienna.
Toma, S. (2015). The role of migrant networks in the labour market outcomes of Senegalese men: How destination contexts matter. Ethnic and Racial Studies, 39(4), 593–613.
Torres, J. M., & Wallace, S. P. (2013). Migration circumstances, psychological distress, and self-rated physical health for Latino immigrants in the United States. American Journal of Public Health, 103(9), 1619–1627.
Uitewaal, P. J. M., Manna, D. R., Bruijnzeels, M. A., Hoes, A. W., & Thomas, S. (2004). Prevalence of type 2 diabetes mellitus, other cardiovascular risk factors, and cardiovascular disease in Turkish and Moroccan immigrants in North West Europe: A systematic review. Preventive Medicine, 39(6), 1068–1076.
van Dorp, M., Boon, A., Spijkerman, R., & Los, L. (2021). Substance use prevalence rates among migrant and native adolescents in Europe: A systematic review. Drug and Alcohol Review, 40(2), 325–339.
Vandenheede, H., Willaert, D., Grande, H., Simoens, S., & Vanroelen, C. (2015). Mortality in adult immigrants in the 2000s in Belgium: A test of the ‘healthy-migrant’ and the ‘migration-as-rapid-health-transition’ hypotheses. Tropical Medicine and International Health, 20(12), 1832–1845.
Vang, Z. M., Sigouin, J., Flenon, A., & Gagnon, A. (2017). Are immigrants healthier than native-born Canadians? A systematic review of the healthy immigrant effect in Canada. Ethnicity and Health, 22(3), 209–241.
Vanthomme, K., & Vandenheede, H. (2019). Migrant mortality differences in the 2000s in Belgium: Interaction with gender and the role of socioeconomic position. International Journal for Equity in Health, 18(1), 96–110.
Vega, W. A., Kolody, B., Valle, R., & Weir, J. (1991). Social networks, social support, and their relationship to depression among immigrant Mexican women. Human Organization, 50(2), 154–162.
Veling, W., Selten, J.-P., Veen, N., Laan, W., Blom, J. D., & Hoek, H. W. (2006). Incidence of schizophrenia among ethnic minorities in the Netherlands: A four-year first-contact study. Schizophrenia Research, 86(1–3), 189–193.
Wakeel, F., Witt, W., Wisk, L. E., Lu, M. C., & Chao, M. (2013). Racial and ethnic disparities in personal capital during pregnancy: Findings from the 2007 Los Angeles Mommy and Baby (LAMB) Study. Maternal and Child Health Journal, 18(1), 209–222.
Wallace, M., & Kulu, H. (2014a). Low immigrant mortality in England and Wales: A data artefact? Social Science and Medicine, 120, 100–109.
Wallace, M., & Kulu, H. (2014b). Migration and health in England and Scotland: A study of migrant selectivity and salmon bias. Population, Space and Place, 20(8), 694–708.
Wallace, M., & Wilson, B. (2019). Migrant mortality advantage versus origin and the selection hypothesis. Population and Development Review, 45(4), 767–794.
Wallace, M., Khlat, M., & Guillot, M. (2019). Mortality advantage among migrants according to duration of stay in France, 2004–2014. BMC Public Health, 19(1), 1–9.
Wang, S., Chen, X., Li, Y., Luu, C., Yan, R., & Madrisotti, F. (2021). ‘I’m more afraid of racism than of the virus!’: Racism awareness and resistance among Chinese migrants and their descendants in France during the Covid-19 pandemic. European Societies, 23(sup1), S721–S742.
Williams, D. R., Mohammed, S. A., Leavell, J., & Collins, C. (2010). Race, socioeconomic status, and health: Complexities, ongoing challenges, and research opportunities: Race, SES, and health. Annals of the New York Academy of Sciences, 1186(1), 69–101.
World Health Organization. (2020). Tuberculosis surveillance and monitoring in Europe 2020: 2018 data. 92890549.
Zhang, M., Gurung, A., Anglewicz, P., & Yun, K. (2021). COVID-19 and immigrant essential workers: Bhutanese and Burmese refugees in the United States. Public Health Reports (Washington, D.C.: 1974), 136(1), 117–123.
Author information
Authors and Affiliations
Corresponding author
Editor information
Editors and Affiliations
Rights and permissions
Open Access This chapter is licensed under the terms of the Creative Commons Attribution 4.0 International License (http://creativecommons.org/licenses/by/4.0/), which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons license and indicate if changes were made.
The images or other third party material in this chapter are included in the chapter's Creative Commons license, unless indicated otherwise in a credit line to the material. If material is not included in the chapter's Creative Commons license and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder.
Copyright information
© 2022 The Author(s)
About this chapter
Cite this chapter
Gamper, M., Kupfer, A. (2022). Migration as a Health Inequality Dimension? Natio-Ethno-Cultural Affiliation, Health, and Social Networks. In: Klärner, A., Gamper, M., Keim-Klärner, S., Moor, I., von der Lippe, H., Vonneilich, N. (eds) Social Networks and Health Inequalities. Springer, Cham. https://doi.org/10.1007/978-3-030-97722-1_16
Download citation
DOI: https://doi.org/10.1007/978-3-030-97722-1_16
Published:
Publisher Name: Springer, Cham
Print ISBN: 978-3-030-97721-4
Online ISBN: 978-3-030-97722-1
eBook Packages: Social SciencesSocial Sciences (R0)