Abstract
Improved protection of urinary stents against infections is a significant current challenge because of the increasing microbial resistance to the conventional antibiotics and negative issues for the patients. Formation of crystalline biofilms of pathogenic microbial cells is the leading cause of urinary stent associated infections. A lot of approaches, antimicrobial agents and techniques are under a study to mitigate the problem by creation of contact killing; releasing or low adhesive surfaces do not allow attachment of microbial cells. The plasma treatment has a number of advantages that make it preferable in many strategies for the development of antimicrobial biomaterials. The control over the plasma processing parameters allows control over the surface chemistry, charge, structure, morphology, hydrophilic/hydrophobic balance, etc. Due to a variety of biomaterials and bacteria, causing urinary tract infections, plasma assisted antibacterial strategies need in tailoring to each specific surface. Plasma treatment of polymers under corresponding operation conditions allows deposition of contact killing, releasing (including controlled release) or low-adhesive antimicrobial coatings, as well as polymer surface functionalization and durable immobilization of antimicrobial molecules. Most of the plasma technologies are developed in laboratory and the surface engineered biomaterials are tested in vitro.
You have full access to this open access chapter, Download chapter PDF
Similar content being viewed by others
Keywords
- Polymer surfaces
- Antimicrobial protection
- Cold plasma
- Surface activation
- Coatings deposition
- Antimicrobial agents grafting
1 Introduction
Improved protection of urinary stents against infections is a significant current challenge because of the increasing microbial resistance to the conventional antibiotics and negative issues for the patients. Formation of crystalline biofilms of pathogenic microbial cells is the leading cause of urinary stent associated infections.
On many parameters polymeric materials satisfy the basic requirements and are widely used for the fabrication of urinary stents, silicones and polyurethanes being preferable ones currently [1]; and biodegradables attracting interest lately. However, the nonsufficient microbial resistance, biofilm formation and encrustation are their common gap.
A lot of approaches, antimicrobial agents and techniques are under a study to mitigate the problem by creation of contact killing, releasing or low adhesive surfaces do not allowing attachment of microbial cells [2,3,4].
The plasma treatment has a number of advantages that make it preferable in many strategies for the development of antimicrobial biomaterials. The control over the plasma processing parameters allows control over the surface chemistry, charge, structure, morphology, hydrophilic/hydrophobic balance, etc. Due to a variety of biomaterials and bacteria, causing urinary tract infections, plasma assisted antibacterial strategies need in tailoring to each specific surface [5,6,7,8].
2 Physical Plasma and Plasma Processes
Plasma is a multicomponent system obtained by a partial ionization of gas. The plasma consists of positively and negatively charged ions, negatively charged electrons, radicals, neutral and excited atoms, highly energetic molecules and molecular fragments [8,9,10,11,12]. According to the temperature of the ions, the plasma refers to low temperature (cold) or high temperature plasma [13].
Surface modification of polymeric biomaterials is performed in low temperature plasma created by ionization of inert (Ar, Ne, He) or reactive (O2, N2, NH3, CO2) gases or volatile monomers at low (RF) or atmospheric pressure by applying energy in the form of heat, direct or alternating electric current, radiation or laser light [8, 12].
Depending on the mode of plasma treatment, four types modification processes happen on the polymer surface: sputtering, etching, ion implantation and plasma polymer deposition [12].
Plasma sputtering is the plasma physical degradation, limited to the outermost layer of the polymeric biomaterial, as it simplified presented in Fig. 1.
Plasma sputtering is used for sterilization of sensitive to temperature or radiation biomaterials, removal of surface contaminations and deposition of sputtered thin coatings [12, 14].
Plasma etching (Fig. 2) is a process at which the loss of the exposed polymeric material is deeper and the adsorption of energetic species is followed by a product formation, prior to a product desorption.
Plasma etching is aimed at: removal of impurities, surface nanopatterning, cross-linking of surface polymer chains and generation of surface functional groups [11, 15].
Plasma ion implantation is a process at which the presenting in the plasma excited species react directly with the polymer surface and induce grafting of new chemical groups (amine, hydroxyl and others), Fig. 3 [11, 15].
Plasma polymer deposition (PPD) is a process in which a thin polymer-like film is formed over the surface of the substrate polymer (Fig. 4).
PPD happens inside the plasma reactor but outside the plasma zone where activated gas species polymerize onto the cold substrate. The generated films are commonly referred as plasma polymers although they do not be formally classified as polymers because they do not consist of repeating monomer units [10, 15]. Using plasma of different gaseous substances: allylamine, octadiene, aldehydes, ethanol, acrylic acid, perfluorooctane, etc.) and optimizing the operation conditions it is possible to create thin coatings with different functional groups and varied properties (hydrophilic/hydrophobic, positively/negatively charged or non-charged, soft or hard, etc.), as it is evident from Fig. 5.
Chemical composition (based on results from XPS) of RF vacuum plasma deposited films of different monomers: diaminocyclohexane (DACH), hydroxyethylmethacrylate (HEMA), hexamethyldisiloxane (HMDS), acrylic acid (AA), methane (CH4) and polyethylene oxide (PEO) (from. T. Vladkova, Surface Engineering of Polymeric Biomaterials, Smithers Rapra, UK, 2013)
Plasma-enhanced chemical vapor deposition (PECVD) is the most common plasma polymerization technique. Magnetron sputtering, liquid-assisted deposition, plasma-assisted thermal evaporation, etc. are other technics to polymer surface modification [11, 15,16,17]. Ion beam processing includes: ion implantation; ion beam texturing and sputtering, etc. The ion-beam modification is durable and no surface “reconstruction” happens in contrary to the plasma treated surface. Plasma immersion ion implantation and ion treatment by plasma exposure are two relative new possibilities. The above methods could be utilized in antimicrobial approaches to the creation of functionalized, or low adhesive surfaces with controlled topography and surface energy [11, 18]. Some examples of plasma treatments are: ion-plasma modification of polyvinylchloride microfiltration membranes [19]; treatment of polyacrylonitrile membranes in DBD discharge in air (including magnet stimulated), [20,21,22]; electron beam cross-linking of silicone rubber [23], plasma pre-treatment of collagen and keratin base materials [24]; generation of self-organized patterns in cold atmospheric plasma-activated liquids [25] etc.
3 Plasma Approaches to Antimicrobial Surfaces Development
Polymer surfaces with antimicrobial properties can be developed either by coating deposition, antimicrobial agent grafting or affecting the surface topography and free energy. These approaches act through distinct mechanisms: contact killing, killing in solution or stimuli responsive killing and bacterial repellence [3, 4, 26]. Plasma strategies for developing of such surfaces are in the focus of many current investigations [27]. They could be referred to the following main groups: deposition of antimicrobial plasma coatings, plasma based surface functionalization and covalent immobilization of antimicrobial molecules.
3.1 Deposition of Antimicrobial Plasma Coatings
Deposition of plasma coatings decreasing the microbial adhesion, contact killing or releasing antimicrobial agent (passively or in response of external stimuli) is accepted now as a promising strategy to creation of antimicrobial surfaces [4, 8].
Plasma deposition of nanocomposite coatings, containing metal or metal oxides nanoparticles (Ag, Cu, Ti, TiO2, etc.), is becoming an important step in the manufacturing of antimicrobial polymeric biomaterials [8]. Silver is one of the most utilized antibacterial components of plasma coatings. It is included in different forms: as phospholipid encapsulated nanoparticles [28]; hybrid silver-poly(l-lactide) nanoparticles [29]; polyvinyl-sulphonate-stabilized nanoparticles [30]; as Ag/SiO(x)C(y) plasma polymer [31]; as (AgNPs)-loaded coatings with a second n-heptylamine layer [32]; plasma-sprayed silver-doped hydroxyapatite coating [33, 34]; silver-doped diamond-like carbon coatings deposited via a hybrid plasma process [35]; Ag clusters incorporated in a:C (Ag/a:C) matrix produced by plasma gas condensation process [36]; silver/montmorillonite biocomposite multilayers [37], hexamethyldisiloxane nanocomposites [38]; as plasma coated AgNPs [39]; etc. Piszek and Radtke [40] discuss chemical vapor deposition (CVD) and atomic layer deposition (ALD) as a tools for fabrication of silver layers, nanoparticles, and nanocomposites together with the release of silver ions from nanoparticles or nanolayers as well as the antimicrobial activity of these materials.
Vladkova et al. [41] developed new functional coatings for medical devices, employing magnetron co-sputtering to deposit triple TiO2/SiO2/Ag nanocomposite thin films. Combining the antimicrobial activity of the TiO2 and Ag with the dispersing effect of the SiO2 these coatings demonstrate strong inhibitory effect toward E. coli and P. aeruginosa growth. Direct contact and eluted silver mediated killing were experimentally demonstrated as mechanism of antibacterial action of these coatings [41]. Kredl et al. [42] use DC plasma air jet to deposit Cu coating on PDMS and acrylonitrile butadiene styrene ABS triple co-polymer surfaces. Good antimicrobial activity against Gram-negative and Gram-positive test bacteria with clinical significance was found by Stoyanova et al. [43] for RF magnetron co-sputtered Ag and Cu doped TiO2 coatings. Woskowicz et al. [44] just reported MS-PVD plasma treatment of polypropylene surface utilizing sputtering of Ag, Cu and their oxides in order to impart antimicrobial activity [44].
Deposition of plasma coatings releasing antimicrobial agents either passively or in response to external stimuli is another option to limit bacterial colonization. Releasing metal nanoparticles (silver, coper or tin), amino-hydrocarbon coatings, prepared by plasma immersion ion implantation are an example discussed as alternative of the antibiotics releasing ones [12].
Plasma coatings that release antimicrobials in response to external stimuli are produced by ‘sandwiching’ of antimicrobials between two plasma polymer layers, plasma polymer over coating or nano-templating for creation of antimicrobial reservoirs [45,46,47]. A novel approach to generate hydrogel coatings through atmospheric-pressure plasma polymerization includes: plasma pre-treatment of the substrate leaving reactive surface radicals; plasma-induced polymerization of the monomer units and cross-linking the polymer chains into a polymer network [48].
Plasma coatings inhibiting bacterial adhesion are based on the idea for creation of surfaces decreasing microbial adhesion down to levels do not allowing attachment or allowing easy detachment of microbial cells. Non-toxicity is the main advantage of this strategy together with some others. Ykada et al. [49] proved that the work of adhesion in aqueous media, W1,2w approaches to zero when the water contact angle (WCA) or surface tension, γc approaches to zero, i.e. low adhesive are strong hydrophilic or strong hydrophobic surfaces. Surface enrichment of relevant functional groups and topographical modifications are main ways to creation of such by plasma treatment [4, 11]. When plasma processes are combined with nanotexturing, remarkable wetting states such as superhydrophobicity and superhydrophilicity can be achieved [50,51,52]. Nwankire et al. [53] deposited superhydrophobic (WCA above 150°) siloxane coatings using atmospheric pressure plasma jet system and hexamethyldisiloxane (HMDSO), tetramethyl cyclotetrasiloxane (Tomcats) or a mixture of Tomcats and fluorosiloxane as liquid precursors [53].
Diamond like carbon (DLC) plasma coatings are also used for creation of low adhesive polymer surfaces. A fluid precursor, generally used for production of DLC is hydrocarbon (methane) or silicone. The hydrogen to carbon ratio has a dramatic influence on the characteristics of the DLC coatings. But overall they characterize by excellent biocompatibility and low friction coefficient [11, 54]. In 2007, Laube et al. [55] discuss DLC coatings as a new strategy for decreasing the formation of crystalline bacterial biofilms on ureteral stents. A preliminary study with ten patients having indwelled DLC coated stent demonstrates quite promising results: significantly decreased friction, encrustation and biofilm formation. It was concluded that further investigation in larger patient groups is necessary for their confirmation. Unfortunately, no reports were found about that [55]. The doping with antimicrobial metals (copper, silver, and other) or elements increasing the hydrophobicity are conventional tools to improve the DLC coatings resistance to bacterial biofilms formation. Ren [56] reports increased resistance to bacterial colonization of anti-adhesive Si-and F-Doped DLC coatings and micro-nanostructured surfaces than non-doped DLC coatings.
Another promising candidate for antimicrobial protection of biomaterial are oxazoline-derived plasma polymer (PPOx) coatings. Bacteria may attach in small numbers to the deposited under appropriate conditions PPOx coatings but would not proliferate to form biofilms, that is very interesting for development of low fouling coatings to indwelling medical devices [57, 58]. A simple and efficient strategy for preparation of poly(2-oxazoline)-based coatings on polytetrafluoroethylene (PTFE) substrate, using diffuse coplanar surface barrier discharge (DCSBD) as a cold plasma source was just reported [59].
3.2 Plasma-Based Surface Functionalization and Antimicrobial Agents’ Immobilization
Plasma deposited antimicrobial coatings improve the antibacterial activity but the effect is not enough durable for some applications and toxicity concerns remain. Covalent grafting of antimicrobial agents is a subject of many investigations aimed at a long-lasting efficacy and a reduced toxicity [5]. Plasma treatment is an easy way to creation of functionalized surfaces with antimicrobial activity or such that can be utilized for covalent immobilization of antimicrobial agents including on nanoscale topographies [4, 60].
Conventionally, an antimicrobial agent immobilization is carried out in two steps: enriching the topmost polymer surface with reactive functional groups by cold plasma treatment (RF or atmospheric pressure plasma, lately preferable) followed by covalent binding using known chemical reactions [4, 60].
The oxygen-rich surfaces, containing hydroxyl, carboxyl and carbonyl groups promote the cellular attachment because of ionic interactions with molecules, mediating the cell adhesion [61]. The amine-rich polymer surfaces created by plasma treatment, using allylamine, ethylendiamine, propylamine, butlyamine or heptylamine as starting monomer are positively charged and facilitate the electrostatic adsorption of negatively charged proteins, that maybe confer their biocompatibility [62].
Plasma deposition of ring opening monomers (oxazolines, pyrrole, furfuryl, thiophene, aniline, etc.) generates surface chemistries that are not achievable via other ways. Careful tuning the plasma deposition condition is very important to tailor the amount of functionality suit for any specific application and to ensure that film reactivity can be maintained for relevant time [57, 63,64,65,66,67]. Plasma deposited polyoxazolines (POx) contain isocyanate-, nitrile groups and intact oxazoline rings. This provides unique opportunities to carry out binding reactions with biomolecules, nanoparticles and various ligands that contain carboxyl groups in their structures [57, 68]. Plasma-assisted processing and catechol chemistry as well as the use of natural antimicrobial agents to produce synthetic antibiotic-free antibacterial surfaces are a particularly hot topic discussed now [69].
Immobilization of biologically active molecules (antibiotics and other antimicrobial agents) to polymer surfaces is for a long time studied [4].
Examples of plasma assisted attachment of antibiotics are grafting of triclosan and bronopol on oxygen plasma pre-treated polyvinylchloride; grafting of gentamycin to polyvinylidene fluoride after plasma-induced graft polymerization of acrylic acid; etc. [27]. The efficacy of cold plasma for direct deposition of antibiotics is discussed lately as a novel approach for localized delivery and retention of the effect. Ampicillin and gentamicin, deposited onto two types of surfaces: polystyrene micro-titer plates and stainless steel coupons confirmed that the plasma process bonds the antibiotics to the surfaces and ensures localized retention of the antibiotic activity against planktonic and sessile E. coli and P. aeruginosa [70].
Plasma treated polymer surfaces, enriched with reactive functional groups are utilized in other bioactive molecules immobilization such as peptides, proteins, quaternary ammonium compounds, etc. via corresponding chemical reactions [11, 60]: Plasma pre-treated expanded poly(tetra fluoro ethylene) (PTFE) was peptide immobilised after acrylic acid (AA) grafting and diNH2PEG coupling [71]; RF acrylic acid plasma treated silicone surface was immobilized with avidin protein [72].
Plasma treatments, opening a way to biofunctionalization of chemically inert polymers (such as PDMS is) are of especial interest. Trying to combine some advantages of both: ion-beam and plasma treatment, namely the durability of the modifying effect of the ion-beam with the simplicity of the plasma as compared to ion-beam equipment, we developed a special irradiation technique, plasma based Ar+ beam, to activate the PDMS surface for further hybrid functionalization [18, 73, 74]. Assuming that the existence of an ion-flow in the plasma volume could strength the surface modifying effect including its durability, a parallel plate reactor equipped with a serial capacitance (Fig. 6) was employed to obtain an ion flow in the plasma volume. The vary of the discharge power ensures varied density of the ion flow [10].
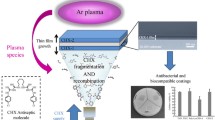
Plasma based Ar+ beam can initiate multistep surface modification procedure including antimicrobial agent (peptide/protein) immobilization via flexible spacer. The principle scheme of this experimental approach is presented in Fig. 7.
This multistep procedure opens a new way to obtain four types modified PDMS surfaces: (1) partially mineralised (moderate hydrophilic, with O-containing groups and free radicals); (2) chemically grafted with AA (moderate hydrophilic, with –COOH functional groups); (3) diNH2PEG-coupled (strong hydrophilic, with –NH2 functional groups; PEG acting as flexible spacer); and (4) biomolecules immobilized (collagen, antimicrobial peptide, or other). The chemical composition, surface topography and roughness as well as the surface hydrophilic/hydrophobic balance, surface free energy, its components and polarity were controlled on every stage of the modification procedure by means of XPS, AFM, SEM and equilibrium contact angle measurements.
Figure 8 demonstrates the cascade process of partial mineralization and functionalization of cross-linked PDMS. It is evident where and how appear a number of active centres such as free radicals and oxygen-containing gropes that could be utilised in further chemical grafting of desired functionalities.
The partially mineralized surface layer was similar to that obtained after a conventional ion-beam. The PDMS surface hydrophilisation was due to surface polarity increase as a result of polar groups’ accumulation, this effect depending on the discharge power. The above presented multi-step procedure has a potential to be used whenever need arises to control chemical activity, hydrophilic/hydrophobic balance and biocontact properties of chemically inert polymers for application as antimicrobial biomaterials for cells culture, processing of biosensors, indwelling medical devices, etc.
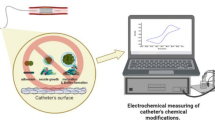
In 2019, Tran et al. [75] develop a single step plasma process for covalent binding of antimicrobial peptides on catheters to suppress bacterial adhesion. Plasma immersion ion implantation (PIII) was demonstrated as a single step treatment leading to covalent coupling of antimicrobial peptides to both internal and external surfaces of PVC catheter tubing, reducing 99% of bacterial adhesion. Ye et al. [76] created self-sterilizing surfaces using a single-step solvent less grafting method. A grafting process was conducted by vapor deposition of a crosslinked poly(dimethylaminomethyl styrene-co-ethylene glycol diacrylate) (P(DMAMS-co-EGDA)) prime layer, followed by in situ grafting of poly(dimethylaminomethyl styrene) (PDMAMS) from the reactive sites of the prime layer. This hybrid coating demonstrates more than 99% bacterial killing against both Gram-negative E. coli and Gram-positive B. subtilis [76]. Surface-grafted polymers, known as polymer brushes, become an important tool for surface modification and functionalization. Wang et al. [77] review the recent progress in the surface-grafting of polymers, including their formation and utilization in functional materials for electronics, medical devices, etc. O2-functional groups, introduced by oxygen-plasma treatment, on plasma polymerized HMDSO surface, are utilized in binding of pharmaceuticals and anti-microbial peptides inhibiting the biofilms accumulation [78, 79]. The plasma treatment effectiveness as a tool to direct PET surface modification or to surface functionalization prior to immobilization of chitosan was evaluated using different discharge types: DC-discharge (at the cathode or at the anode) or AC-discharge [80]. The use of cold RF- and atmospheric pressure plasma-assisted polymerization for subsequently immobilization of various biomolecules for biomedical applications is discussed lately [81].
4 Concluding Remarks
Plasma treatment of polymers under corresponding operation conditions allows deposition of contact killing, releasing (including controlled release) or low-adhesive antimicrobial coatings, as well as polymer surface functionalization and durable immobilization of antimicrobial molecules. Most of the plasma technologies are developed in laboratory conditions and the surface engineered biomaterials are tested in vitro.
The use of plasmas facilitates modifications which are difficult or unable to achieve by conventional physical or chemical methods, like for example the stable attachment of biologically active molecules onto chemically inert polymer surfaces.
For the step “from laboratory into clinical practice” it is essential to examine the in vivo antimicrobial action by using appropriate animal models and human groups.
References
Gadzhiev N, Gorelov D, Malkhasyan V, Akopyan G, Harchelava R, Mazurenko D, et al. Comparison of silicone versus polyurethane ureteral stents: a prospective controlled study. BMC Urol. 2020;20(1):10.
Mosayyebi A, Vijayakumar A, Yue QY, Bres-Niewada E, Manes C, Carugo D, et al. Engineering solutions to ureteral stents: material, coating and design. Cent Eur J Urol. 2017;70(3):270–4.
Zhang Z, Wagner VE. Antimicrobial coatings and modifications on medical device. Cham: Springer; 2017.
Vladkova TG, Staneva AD, Gospodinova DN. Surface engineered biomaterials and ureteral stents inhibiting biofilm formation and encrustation. Surf Coat Technol. 2020;404:126424.
Vasilev K, Griesser SS, Griesser HJ. Antibacterial surfaces and coatings produced by plasma techniques. Plasma Process Polym. 2011;8(11):1010–23.
Cvrček L, Horáková M. Plasma modified polymeric materials for implant applications. In Non-thermal plasma technology for polymeric materials. Amsterdam: Elsevier; 2019.
Múgica-Vidal R, Sainz-García E, Álvarez-Ordóñez A, Prieto M, González-Raurich M, López M, et al. Production of antibacterial coatings through atmospheric pressure plasma: a promising alternative for combatting biofilms in the food industry. Food Bioprocess Technol. 2019;12(8):1251–63.
Nikiforov A, Deng X, Xiong Q, Cvelbar U, Degeyter N, Morent R, et al. Non-thermal plasma technology for the development of antimicrobial surfaces: a review. J Phys D Appl Phys. 2016;49(20):204002.
Wikipedia. Plasma [Internet]. Plasma. https://bg.wikipedia.org/wiki/Плазма.
Hippler R, Pfau S, Schmidt M, Schoenbach KH. Low temperature plasma physics: fundamental aspects and applications. 2nd ed. New York: Wiley-VCH; 2008. p. 945. https://www.amazon.com/Low-Temperature-Plasmas-Fundamentals-Technologies-dp-3527406735/dp/3527406735/ref=dp_ob_image_bk.
Vladkova TG. Surface engineering of polymeric biomaterials. Shawbury: Smithers Rapra Technology; 2013. p. 590. https://www.amazon.co.uk/Surface-Engineering-Polymeric-Biomaterials-Vladkova/dp/1847356591.
Walschusр U, Schlosser K, Schroder M, Finke K, Nebe B, Meichsner B, et al. Application of low-temperature plasma processes for biomaterials. In Biomaterials applications for nanomedicine. London: IntechOpen; 2011.
Knowledge Computing. Plasma classification (types of plasma). https://www.plasma-universe.com/plasma-classification-types-of-plasma/.
Glow CB. Discharge processes: sputtering and plasma etching. 1st ed. New York: Wiley-Interscience; 1980. p. 432. https://www.wiley.com/en-bg/Glow+Discharge+Processes:+Sputtering+and+Plasma+Etching-p-9780471078289.
Yasuda H. Plasma polymerization. New York: Academic Press; 2012. p. 442. https://www.amazon.com/Plasma-Polymerization-H-Yasuda/dp/0123960916.
Hegemann D, Nisol B, Watson S, Wertheimer MR. Energy conversion efficiency in plasma polymerization—a comparison of low- and atmospheric-pressure processes. Plasma Process Polym. 2016;13(8):834–42. https://doi.org/10.1002/ppap.201500224.
Friedrich J. Mechanisms of plasma polymerization—reviewed from a chemical point of view. Plasma Process Polym. 2011;8(9):783–802. https://doi.org/10.1002/ppap.201100038.
Vladkova TG, Keranov IL, Dineff PD, Youroukov SY, Avramova IA, Krasteva N, et al. Plasma based Ar+ beam assisted poly(dimethylsiloxane) surface modification. Nucl Instrum Methods Phys Res Sect B Beam Interact Mater Atoms. 2005;236(1):552–62.
Vladkova TG, Dineff P, Stojcheva R, Tomerova B. Ion-plasma modification of polyvinylchloride microfiltration membranes. J Appl Polym Sci. 2003;90(9):2433–40. https://doi.org/10.1002/app.12912.
Petrov S, Atanasova P, Dineff P, Vladkova T. Surface modification of polymeric ultrafiltration membranes I. Effect of atmospheric pressure barrier discharge in air onto some characteristics of polyacrylonitrile ultrafiltration membranes. High Energy Chem. 2012;46(4):283–91. https://doi.org/10.1134/S0018143912040145.
Atanasova P, Petrov S, Dineff P, Vladkova T. Surface modification of polymeric ultrafiltration membranes II. Effect of magnet stimulated atmospheric pressure barrier discharge in air onto some characteristics of polyacrylonitrile ultrafiltration membranes. High Energy Chem. 2012;46(5):1–8.
Vladkova T, Atanasova P, Petrov S, Dineff P. Surface modification of polymeric ultrafiltration membranes: III. Effect of plasma-chemical surface modification onto some characteristics of polyacrylonitrile ultrafiltration membranes. High Energy Chem. 2013;47(6):346–52. https://doi.org/10.1134/S0018143913060118.
Stelescu M, Manaila E, Vladkova T, Georgescu M. The influence of polyfunctional monomers on the mechanical properties of the silicone rubber cross-linked by irradiation with electron beam. Ecol Saf. 2012;6(1):323–9. https://www.scientific-publications.net/download/ecology-and-safety-2012-1.pdf.
Gaidau C, Petica A, Micutz M, Danciu M, Vladkova T. Progresses in treatment of collagen and keratin-based materials with silver nanoparticles. Open Chem. 2013;11(6):901–11. https://www.degruyter.com/view/journals/chem/11/6/article-p901.xml.
Chen Z, Xu RG, Chen P, Wang Q. Potential agricultural and biomedical applications of cold atmospheric plasma-activated liquids with self-organized patterns formed at the interface. IEEE Trans Plasma Sci. 2020;48(10):3455–71.
Singha P, Locklin J, Handa H. A review of the recent advances in antimicrobial coatings for urinary catheters. Acta Biomater. 2017;50:20–40.
Sardella E, Palumbo F, Camporeale G, Favia P. Non-equilibrium plasma processing for the preparation of antibacterial surfaces. Materials. 2016;9:515.
Taheri S, Cavallaro A, Christo SN, Majewski P, Barton M, Hayball JD, et al. Antibacterial plasma polymer films conjugated with phospholipid encapsulated silver nanoparticles. ACS Biomater Sci Eng. 2015;12:1278–86. https://doi.org/10.1021/acsbiomaterials.5b00338.
Taheri S, Baier G, Majewski P, Barton M, Förch R, Landfester K, et al. Synthesis and surface immobilization of antibacterial hybrid silver-poly(l-lactide) nanoparticles. Nanotechnology. 2014;25(30):305102. https://doi.org/10.1088/0957-4484/25/30/305102.
Vasilev K, Sah VR, Goreham RV, Ndi C, Short RD, Griesser HJ. Antibacterial surfaces by adsorptive binding of polyvinyl-sulphonate-stabilized silver nanoparticles. Nanotechnology. 2010;21(21):215102. https://doi.org/10.1088/0957-4484/21/21/215102.
Khalilpour P, Lampe K, Wagener M, Stigler B, Heiss C, Ullrich MS, et al. Ag/SiOxCy plasma polymer coating for antimicrobial protection of fracture fixation devices. J Biomed Mater Res Part B Appl Biomater. 2010;94(1):196–202. https://doi.org/10.1002/jbm.b.31641.
Ploux L, Mateescu M, Anselme K, Vasilev K. Antibacterial properties of silver-loaded plasma polymer coatings. J Nanomater. 2012;2012:674145. https://doi.org/10.1155/2012/674145.
Carmona VO, Martínez Pérez C, de Lima R, Fraceto LF, Romero García J, Ledezma Pérez A, et al. Effect of silver nanoparticles in a hydroxyapatite coating applied by atmospheric plasma spray. Int J Electrochem Sci. 2014;9:7471–94. http://www.electrochemsci.org/papers/vol9/91207471.pdf.
Roy M, Fielding GA, Beyenal H, Bandyopadhyay A, Bose S. Mechanical, in vitro antimicrobial, and biological properties of plasma-sprayed silver-doped hydroxyapatite coating. ACS Appl Mater Interfaces. 2012;4(3):1341–9. https://doi.org/10.1021/am201610q.
Cloutier M, Tolouei R, Lesage O, Lévesque L, Turgeon S, Tatoulian M, et al. On the long term antibacterial features of silver-doped diamondlike carbon coatings deposited via a hybrid plasma process. Biointerphases. 2014;9(2):29013. https://doi.org/10.1116/1.4871435.
Carvalho I, Faraji M, Ramalho A, Carvalho AP, Carvalho S, Cavaleiro A. Ex-vivo studies on friction behaviour of ureteral stent coated with Ag clusters incorporated in a: C matrix. Diam Relat Mater. 2018;86:1–7.
Iconaru SL, Groza A, Stan GE, Predoi D, Gaiaschi S, Trusca R, et al. Preparations of silver/montmorillonite biocomposite multilayers and their antifungal activity. Coatings. 2019;9:817.
Ionita MD, Ionita ER, Satulu V, De Vrieze M, Zille A, Modic M, et al. Antibacterial nanocomposites based on Ag NPs and HMDSO deposited by atmospheric pressure plasma. In: 23rd International symposium on plasma chemistry [Internet]. Montréal, Canada; 2014. http://repositorium.sdum.uminho.pt/handle/1822/57250.
Brobbey KJ, Haapanen J, Mäkelä JM, Gunell M, Eerola E, Rosqvist E, et al. Effect of plasma coating on antibacterial activity of silver nanoparticles. Thin Solid Films. 2019;672:75–82.
Piszczek P, Radtke A. Silver nanoparticles fabricated using chemical vapor deposition and atomic layer deposition techniques: properties, applications and perspectives: review. In: Seehra MS, Bristow AD, editors. Noble and precious metals-properties, nanoscale effects and applications. London: IntechOpen; 2018.
Vladkova T, Angelov O, Stoyanova D, Gospodinova D, Gomes L, Soares A, et al. Magnetron co-sputtered TiO2/SiO2/Ag nanocomposite thin coatings inhibiting bacterial adhesion and biofilm formation. Surf Coat Technol. 2020;384:125322.
Kredl J, Quade A, Mueller S, Peglow S, Polak M, Kolb JF, et al. Antimicrobial copper-coatings on temperature labile surfaces deposited with a DC plasma jet operated with air. 2014.
Stoyanova DS, Ivanova IA, Angelov OI, Vladkova TG. Antibacterial activity of thin films TiO2 doped with Ag and Cu on gracilicutes and firmicutes bacteria. Biodiscovery. 2017;20:e15076. https://doi.org/10.3897/biodiscovery.20.e15076.
Woskowicz E, Łożynska M, Kowalik-Klimczak A, Kacprzyńska-Gołacka J, Osuch-Słomka E, Piasek A, et al. Plasma deposition of antimicrobial coatings based on silver and copper on polypropylene. Polimery. 2020;65(1):33–43. http://repo.bg.pw.edu.pl/index.php/en/r#/info/article/WUT7d3f00caa77d4cb1a07f2503c91147fe/Plasma+deposition+of+antimicrobial+coatings+based+on+silver+and+copper+on+polypropylene%23.X7pIVlUzaUk.
Simovic S, Losic D, Vasilev K. Controlled release from drug delivery systems based on porous platforms. Pharm Technol. 2011;35:68–71.
Vasilev K, Poulter N, Martinek P, Griesser HJ. Controlled release of levofloxacin sandwiched between two plasma polymerized layers on a solid carrier. ACS Appl Mater Interfaces. 2011;3(12):4831–6. https://doi.org/10.1021/am201320a.
Simovic S, Losic D, Vasilev K. Controlled drug release from porous materials by plasma polymer deposition. Chem Commun. 2010;46(8):1317–9. https://doi.org/10.1039/B919840G.
Levien M, Fricke K. Fabrication of hydrogel coatings by atmospheric-pressure plasma polymerization: function by structure and chemistry. Mater Today. 2020;41:316–7.
Ikada Y, Suzuki M, Tamada Y. Polymer surfaces possessing minimal interaction with blood components. In: Shalaby SW, Hoffman AS, Ratner BD, Horbett TA, editors. BT-Polymers as biomaterials. Boston: Springer; 1984. p. 135–47. https://doi.org/10.1007/978-1-4613-2433-1_10.
Choukourov A, Kylián O, Petr M, Vaidulych M, Nikitin D, Hanuš J, et al. RMS roughness-independent tuning of surface wettability by tailoring silver nanoparticles with a fluorocarbon plasma polymer. Nanoscale. 2017;9(7):2616–25. https://doi.org/10.1039/C6NR08428A.
Kuzminova A, Shelemin A, Kylián O, Petr M, Kratochvíl J, Solař P, et al. From super-hydrophilic to super-hydrophobic surfaces using plasma polymerization combined with gas aggregation source of nanoparticles. Vacuum. 2014;110:58–61.
Ramiasa-MacGregor M, Mierczynska A, Sedev R, Vasilev K. Tuning and predicting the wetting of nanoengineered material surface. Nanoscale. 2016;8(8):4635–42. https://doi.org/10.1039/C5NR08329J.
Nwankire CE, Favaro G, Duong Q-H, Dowling DP. Enhancing the mechanical properties of superhydrophobic atmospheric pressure plasma deposited siloxane coatings. Plasma Process Polym. 2011;8(4):305–15. https://doi.org/10.1002/ppap.201000069.
Vladkova TG. Surface engineered polymeric biomaterials with improved biocontact properties. Int J Polym Sci. 2010;2010:296094.
Laube N, Kleinen L, Bradenahl J, Meissner A. Diamond-like carbon coatings on ureteral stents—a new strategy for decreasing the formation of crystalline bacterial biofilms? J Urol. 2007;177(5):1923–7. https://doi.org/10.1016/j.juro.2007.01.016.
Ren D. Anti-adhesive Si-and F-doped DLC coatings and micro-nanostructured surfaces for medical implants. Dundee: University of Dundee; 2015. https://discovery.dundee.ac.uk/en/studentTheses/anti-adhesive-si-and-f-doped-dlc-coatings-and-micro-nanostructure.
Ramiasa MN, Cavallaro AA, Mierczynska A, Christo SN, Gleadle JM, Hayball JD, et al. Plasma polymerised polyoxazoline thin films for biomedical applications. Chem Commun. 2015;51(20):4279–82. https://doi.org/10.1039/C5CC00260E.
Visalakshan RM, Cavallaro A, Smith LE, MacGregor-Ramiasa M, Hayball J, Vasilev K. Downstream influences of oxazoline plasma polymerisation conditions on chemical and biological interactions. In CHEMECA 2016: Chemical engineering-regeneration, recovery and reinvention. Adelaide: CHEMECA; 2016. p. 840–8. https://search.informit.com.au/documentSummary;dn=410967258296456;res=IELENG;type=pdf.
Šrámková P, Zahoranová A, Kelar J, Kelar Tučeková Z, Stupavská M, Krumpolec R, et al. Cold atmospheric pressure plasma: simple and efficient strategy for preparation of poly(2-oxazoline)-based coatings designed for biomedical applications. Sci Rep. 2020;10(1):9478. https://doi.org/10.1038/s41598-020-66423-w.
Hermanson GT. Chapter 4-Zero-length crosslinkers. 3rd ed. Boston: Academic Press; 2013. p. 259–73.
Ruiz J-C, Girard-Lauriault P-L, Wertheimer MR. Fabrication, characterization, and comparison of oxygen-rich organic films deposited by plasma- and vacuum-ultraviolet (VUV) photo-polymerization. Plasma Process Polym. 2015;12(3):225–36. https://doi.org/10.1002/ppap.201400146.
Lerouge S, Barrette J, Ruiz J-C, Sbai M, Savoji H, Saoudi B, et al. Nitrogen-rich plasma polymer coatings for biomedical applications: stability, mechanical properties and adhesion under dry and wet conditions. Plasma Process Polym. 2015;12(9):882–95. https://doi.org/10.1002/ppap.201400210.
Saboohi S, Al-Bataineh SA, Safizadeh Shirazi H, Michelmore A, Whittle JD. Continuous‐wave RF plasma polymerization of furfuryl methacrylate: correlation between plasma and surface chemistry. Plasma Process Polym. 2017;14(3):1600054. https://doi.org/10.1002/ppap.201600054.
Kumar SD, Yoshida Y. Dielectric properties of plasma polymerized pyrrole thin film capacitors. Surf Coat Technol. 2003;169:600–3.
Silverstein MS, Visoly-Fisher I. Plasma polymerized thiophene: molecular structure and electrical properties. Polymer (Guildf). 2002;43(1):11–20.
Morales J, Olayo MG, Cruz GJ, Castillo-Ortega MM, Olayo R. Electronic conductivity of pyrrole and aniline thin films polymerized by plasma. J Polym Sci Part B Polym Phys. 2000;38(24):3247–55. https://doi.org/10.1002/1099-0488(20001215)38:24%3C3247::AID-POLB60%3E3.0.CO.
Jacob MV, Easton CD, Anderson LJ, Bazaka K. RF plasma polymerised thin films from natural resources. Int J Mod Phys Conf Ser. 2014;32:1460319. https://doi.org/10.1142/S2010194514603196.
Macgregor-Ramiasa MN, Cavallaro AA, Vasilev K. Properties and reactivity of polyoxazoline plasma polymer films. J Mater Chem B. 2015;3(30):6327–37. https://doi.org/10.1039/C5TB00901D.
Bazaka K, Jacob MV, Chrzanowski W, Ostrikov K. Anti-bacterial surfaces: natural agents, mechanisms of action, and plasma surface modification. RSC Adv. 2015;5(60):48739–59.
Los A, Ziuzina D, Boehm D, Han L, O’Sullivan D, O’Neill L, et al. Efficacy of cold plasma for direct deposition of antibiotics as a novel approach for localized delivery and retention of effect. Front Cell Infect Microbiol. 2019;9:428. https://doi.org/10.3389/fcimb.2019.00428.
Baquey C, Palumbo F, Porte-Durrieu MC, Legeay G, Tressaud A, d’Agostino R. Plasma treatment of expanded PTFE offers a way to a biofunctionalization of its surface. Nucl Instrum Methods Phys Res Sect B Beam Interact Mater Atoms. 1999;151(1):255–62. http://www.sciencedirect.com/science/article/pii/S0168583X99001068.
Costa LT, Vilani C, Peripolli S, Stavale F, Legnani C, Achete CA. Direct immobilization of avidin protein on AFM tip functionalized by acrylic acid vapor at RF plasma. J Mol Recognit. 2012;25(5):256–61. https://doi.org/10.1002/jmr.2189.
Keranov I, Vladkova TG, Minchev M, Kostadinova A, Altankov G, Dineff P. Topography characterization and initial cellular interaction of plasma-based Ar+ beam-treated PDMS surfaces. J Appl Polym Sci. 2009;111(5):2637–46. https://doi.org/10.1002/app.29185.
Keranov I, Vladkova T, Minchev M, Kostadinova A, Altankov G. Preparation, characterization, and cellular interactions of collagen-immobilized PDMS surfaces. J Appl Polym Sci. 2008;110(1):321–30. https://doi.org/10.1002/app.28630.
Tran C, Yasir M, Dutta D, Eswaramoorthy N, Suchowerska N, Willcox M, et al. Single step plasma process for covalent binding of antimicrobial peptides on catheters to suppress bacterial adhesion. ACS Appl Biol Mater. 2019;2(12):5739–48. https://doi.org/10.1021/acsabm.9b00776.
Ye Y, Song Q, Mao Y. Solventless hybrid grafting of antimicrobial polymers for self-sterilizing surfaces. J Mater Chem. 2011;21(35):13188–94. https://doi.org/10.1039/C1JM12050F.
Wang S, Wang Z, Li J, Li L, Hu W. Surface-grafting polymers: from chemistry to organic electronics. Mater Chem Front. 2020;4(3):692–714. https://doi.org/10.1039/C9QM00450E.
Yoshinari M, Matsuzaka K, Inoue T. Surface modification by cold-plasma technique for dental implants—bio-functionalization with binding pharmaceuticals. Jpn Dent Sci Rev. 2011;47(2):89–101. http://www.sciencedirect.com/science/article/pii/S1882761611000287.
Mon H, Chang Y-R, Ritter AL, Falkinham JO, Ducker WA. Effects of colloidal crystals, antibiotics, and surface-bound antimicrobials on Pseudomonas aeruginosa surface density. ACS Biomater Sci Eng. 2018;4(1):257–65. https://doi.org/10.1021/acsbiomaterials.7b00799.
Demina TS, Piskarev MS, Romanova OA, Gatin AK, Senatulin BR, Skryleva EA, et al. Plasma treatment of poly(ethylene terephthalate) films and chitosan deposition: DC- vs. AC-discharge. Materials (Basel, Switzerland). 2020;13(3):508.
Ramkumar MC, Trimukhe AM, Deshmukh RR, Tripathi A, Melo JS, Navaneetha PK. Immobilization of biomolecules on plasma-functionalized surfaces for biomedical applications. In: Tripathi A, Melo JS, editors. BT-immobilization strategies: biomedical, bioengineering and environmental applications. Singapore: Springer; 2021. p. 305–33. https://doi.org/10.1007/978-981-15-7998-1_8.
Author information
Authors and Affiliations
Corresponding author
Editor information
Editors and Affiliations
Rights and permissions
Open Access This chapter is licensed under the terms of the Creative Commons Attribution 4.0 International License (http://creativecommons.org/licenses/by/4.0/), which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons license and indicate if changes were made.
The images or other third party material in this chapter are included in the chapter's Creative Commons license, unless indicated otherwise in a credit line to the material. If material is not included in the chapter's Creative Commons license and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder.
Copyright information
© 2022 The Author(s)
About this chapter
Cite this chapter
Vladkova, T.G., Gospodinova, D.N. (2022). Plasma Based Approaches for Deposition and Grafting of Antimicrobial Agents to Polymer Surfaces. In: Soria, F., Rako, D., de Graaf, P. (eds) Urinary Stents. Springer, Cham. https://doi.org/10.1007/978-3-031-04484-7_22
Download citation
DOI: https://doi.org/10.1007/978-3-031-04484-7_22
Published:
Publisher Name: Springer, Cham
Print ISBN: 978-3-031-04483-0
Online ISBN: 978-3-031-04484-7
eBook Packages: MedicineMedicine (R0)