Abstract
Parkinson’s disease (PD) is the second most common neurodegenerative disease, and its hallmark pathological features are the loss of dopaminergic (DA) neurons in the midbrain substantia nigra pars compacta (SNpc) and the accumulation of alpha-synuclein (α-syn). It has been shown that the integrity of the blood-brain barrier (BBB) is damaged in PD patients, and a large number of infiltrating T cells and inflammatory cytokines have been detected in the cerebrospinal fluid (CSF) and brain parenchyma of PD patients and PD animal models, including significant change in the number and proportion of different CD4+ T cell subsets. This suggests that the neuroinflammatory response caused by CD4+ T cells is an important risk factor for the development of PD. Here, we systematically review the differentiation of CD4+ T cell subsets, and focus on describing the functions and mechanisms of different CD4+ T cell subsets and their secreted cytokines in PD. We also summarize the current immunotherapy targeting CD4+ T cells with a view to providing assistance in the diagnosis and treatment of PD.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Parkinson’s disease (PD) is the second most common neurodegenerative disease and the fastest growing neurological disorder in world, with 12.9 million patients predicted worldwide by 2040 [1]. The hallmark pathological features of PD include the loss of dopaminergic (DA) neurons in the midbrain substantia nigra pars compacta (SNpc) and the formation of Lewy bodies, which are composed of alpha-synuclein (α-syn) [2]. Patients with PD present with motor symptoms, including bradykinesia, stiffness, resting tremor, and postural instability, as well as a variety of non-motor symptoms, such as depression, autonomic disorders, and cognitive impairment, which lead to a dramatic decline in the quality of life of patients and increase the financial burden on patients and the healthcare system [3,4,5]. The occurrence of PD is associated with various risk factors, including gene mutations [6], environmental risks [7], gut microbiota disturbances [8] and unhealthy lifestyles [9]. Recent studies have shown that the dysregulation of the immune system also plays a crucial role in the pathogenesis of PD [10,11,12].
Specific factors, such as viruses, heavy metals, and some severe brain injuries, drive the activation of neuroinflammation [13]. Neuroinflammation is an inflammatory response of the central nervous system (CNS) in response to factors that interfere with homeostasis. This response entails a concerted effort from resident glial cells in the CNS, such as microglia, oligodendrocytes, and astrocytes, alongside non-glial resident bone marrow cells including macrophages and dendritic cells (DCs) and peripheral white blood cells [14]. Recent evidence has revealed that neuroinflammation plays an important role in the occurrence and development of neurodegenerative diseases, such as PD, Alzheimer’s disease (AD), amyotrophic lateral sclerosis (ALS) and Huntington’s disease (HD) [15].
Many studies have shown that the proportion of different subsets of T cells changes significantly in the peripheral blood of PD patients. Wang et al. compared the proportion of CD4+ T cells and CD8+ T cells in the peripheral blood of PD patients and healthy controls and found that the proportion of CD8+ T cells in PD patients increased significantly compared with healthy controls, while the proportion of CD4+ T cells decreased significantly. This resulted in a significantly lower overall CD4/CD8 ratio in PD patients, indicating that PD patients may have immune disorders [16]. However, Chen et al. found that the proportion of CD3+ T and CD4+ T cells in the peripheral blood of PD patients was higher than in healthy controls, while the proportion of CD8+ T cells did not change significantly, resulting in a significant increase in the CD4/CD8 ratio of PD patients [17]. Therefore, the proportion of T cells in the peripheral blood of PD patients is not consistent, which may be due to different PD samples [17].
Notably, Brochard et al.‘s study suggests that CD4+ T cells have a stronger correlation than CD8+ T cells in mouse models of PD. Specifically, the lacking of CD4+ but not CD8+ T cells in mice significantly reduced 1-methyl-4-phenyl-1,2,3,6-tetrahydropyridine (MPTP)-induced dopamine-containing neurons (DNs) cell death in the SNpc [18]. Furthermore, Williams et al. observed that overexpression of α-syn enhanced the infiltration of both CD4+ and CD8+ T cells into the CNS parenchyma in mice [19]. Conversely, the knockout (KO) or pharmacological inhibition of T cells, particularly CD4+ T cells, protected against the loss of tyrosine hydroxylase-positive (TH+) neurons in the SNpc [19]. These findings suggest a potentially critical role of neuroinflammation, specifically CD4+ T cells, in the pathogenesis and progression of PD.
In this review, we systematically summarize the differentiation of different subsets of CD4+ T cells, focus on the mechanism of different subsets and their secreted cytokines in the development of PD, and finally elaborate the immunotherapy targeting CD4+ T cell for PD to provide further evidence for the diagnosis and treatment of PD.
Differentiation of CD4+ T cell subsets
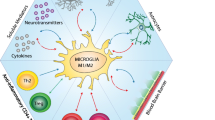
T lymphocytes originate from the bone marrow, then migrate to the thymus for maturation, and ultimately export to the periphery, where they play important roles in the peripheral tissues and various lymphatic organs. Progenitor cells lacking CD4+ and CD8+ receptors in the bone marrow generate CD4+CD8+ double-positive (DP) thymocytes via T cell receptor (TCR) rearrangement. DP cells undergo selection to produce either CD4+ or CD8+ single-positive (SP) thymocytes, which subsequently enter the periphery as naïve T cells [20, 21]. Recognition of major histocompatibility complex class II (MHC-II) on antigen-presenting cells (APCs), such as DCs, is a prerequisite for activating CD4+ T cells. Subsequently, under the combined stimulation from TCR signaling, APCs, and cytokines, the naïve CD4+ T cells are fully activated and differentiated into distinct cell subsets, including T helper (Th) 1 cells, Th2 cells, Th9 cells, Th17 cells, regulatory T cells (Tregs) and T follicular helper (Tfh) cells [22, 23]. Notably, the expression of specific transcription factors is required for T cell differentiation (Fig. 1) [24].
Cytokines and master transcription factors in CD4+ T cell subsets. Under the regulation of specific cytokines, the naïve CD4+ T cells differentiate into different cell subsets, which play an important role in the immune response. Key transcription factors such as T-bet, GATA-3, PU.1, ROR-γt, FOXP3, and Bcl-6 are also essential for the differentiation and maintenance of CD4+ T cells. Th1 cells mainly release cytokines such as IL-2, TNF-α and IFN-γ, while Th2 cells secrete cytokines such as IL-4, IL-5 and IL-13. Th9 cells mainly secrete IL-9. Th17 cells perform pro-inflammatory function by releasing IL-17, IL-21, and IL-22. In contrast, the anti-inflammatory function of Tregs cells is mainly mediated by cytokines such as IL-10, IL-35 and TGF-β. IL-4, IL-10, and IFN-γ are produced by Tfh cells
Th1 cells
Th1 cells primarily mediate immune responses against extracellular pathogens [25]. Interleukin 12 (IL-12) and interferon gamma (IFN-γ) are key cytokines that initiate the differentiation of CD4+ T cells into Th1 cells [26]. APCs, upon activation, release high levels of IL-12, which stimulates natural killer (NK) cells to produce IFN-γ [27]. In turn, IL-12 secreted by APCs and IFN-γ produced by NK cells activate the transcription factors signal transducer and activator of transcription 4 (STAT4) and STAT1, respectively, which further induce T-box expressed in T cells (T-bet) expression, thereby promoting Th1 cell polarization [28, 29] (Fig. 2a). In addition, IL-18 and IL-27 also promote Th1 differentiation and the production of IFN-γ [30,31,32]. T-bet, the main transcription factor of Th1 cells, is specifically expressed in Th1 cell subset and induces the production of IFN-γ, which plays a decisive role in Th1 cell differentiation [33]. T-bet also plays important roles in Th1 cell polarization by regulating the expressions of other transcription factors. For example, T-bet induces Runt-associated transcription factor 3 (RUNX3) expression, which then co-binds to the IFN-γ promoter to promote Th1 cell differentiation [34, 35].
The regulation networks of CD4+ T cell subsets. IL-12 and IFN-γ are key cytokines that initiate the differentiation of CD4+ T cells into Th1 cells. They activate the transcription factors STAT4 and STAT1, respectively, and then induce the expression of T-bet and the polarization of Th1 cells (a). The main transcription factor involved in Th2 subset differentiation is GATA-3, which is regulated by IL4-induced STAT6 (b). Th9 cells are derived from naïve CD4+ T cells induced by TGF-β and IL-4 and mainly secrete IL-9. In addition, cytokines such as IL-1, IL-25 and IL-33 also promote the differentiation of Th9 cells and the production of IL-9. Downstream transcription factors of IL-4 and TGF-β, such as STAT6, IRF4, SMAD3, etc., are also necessary for Th9 cell differentiation (c). IL-6 and TGF-β are the main cytokines involved in Th17 cell differentiation, which promote the transcription of ROR-γt by up-regulating the expression of STAT3 and SMAD. In addition, Th17 cell differentiation is also regulated by IL-23 and IL-1β (d). FOXP3 and Bcl-6 are transcription factors that play dominant roles in the differentiation of Tregs (e) and Tfh cells (f), respectively, and their expression is regulated by cytokines such as IL-2 and TGF-β, and IL-6, IL-21 and IL-27
Th2 cells
Th2 cells primarily mediate host defense against large extracellular pathogens, including parasites [25]. IL-4 and IL-2 are the main regulators of Th2 differentiation. The main transcription factor involved in Th2 subset differentiation is GATA binding protein 3 (GATA-3), which is regulated by IL4-induced STAT6 [36, 37]. GATA-3 activates the expression of Th2 cytokines (IL-4, IL-5, and IL-13) by directly binding to different regions of gene loci, thereby promoting Th2 cell differentiation [38] (Fig. 2b). Interestingly, although IL-4 and IL-2 are required for Th2 cell differentiation in vitro, normal Th2 cell development is still observed in IL-4 and STAT6-deficient mice, suggesting that Th2 cells can differentiate independently on IL-4-STAT6 signaling in vivo [39]. Additionally, GATA-3 also inhibits the expression of transcription factors related to other T cell subsets, such as STAT4, T-bet and retinoic acid receptor-related orphan receptor gamma t (ROR-γt) [38, 40,41,42,43,44,45], and thus inhibits differentiation into other cell subsets.
Th9 cells
Th9 cells are a new subset of CD4+ T cells differentiated from naïve CD4+ T induced by transforming growth factor β (TGF-β) and IL-4, and mainly secrete IL-9 [46]. Studies have shown that Th9 cells play an important role in the immune response to diseases such as autoimmune diseases [47, 48] and cancers [49, 50]. IL-4 is the key cytokine involved in the differentiation of Th9 cells. Interestingly, IL-4 alone induces Th2 differentiation, but in the presence of TGF-β, it converts the Th2 cell phenotype to the Th9 cell phenotype [51]. Other cytokines, including IL-1 [52], IL-2 [53], IL-10 [54], IL-21 [55], IL-25 [56], IL-33 [57], and tumor necrosis factor-α (TNF-α) [58], have also been shown to promote the differentiation of Th9 cells and the production of IL-9. However, IFN-γ and IL-27 have been found to inhibit the production of IL-9 [59]. Downstream transcription factors of IL-4 and TGF-β, such as STAT6 [60], GATA-3 [61, 62], interferon regulatory factor 4 (IRF4) [63], and small mother against decapentaplegic (SMAD)3 [64], are also required for Th9 cell differentiation. Additionally, TGF-β induces the expression of the signature transcription factor PU.1 in Th9 cells, which promotes their differentiation by interfering with GATA-3 expression [65] or affecting chromatin modification through binding to the IL-9 promoter [66], as well as inhibits Th2 cells differentiation (Fig. 2c) [67].
Th17 cells
Th17 cells are a newly discovered CD4+ T cell subset that mainly mediate the host’s immune response to extracellular bacterial and fungal infections through the secretion of IL-17 and other inflammatory cytokines [68,69,70,71,72]. IL-6 and TGF-β are the main cytokines involved in Th17 cell differentiation and induce mouse naïve T cells to differentiate into Th17 cells in vitro and in vivo [73,74,75]. In the absence of IL-6, IL-21 is combined with TGF-β to induce the expression of ROR-γt during T cell differentiation, suggesting that IL-21 combined with TGF-β can induce Th17 cells differentiation independently on IL-6, although the efficiency is lower than that of the combination of IL-6 and TGF-β [76]. In addition, the differentiation of Th17 cells is also regulated by IL-23 [74] and IL-1β [77] (Fig. 2d).
As the most important transcription factor of Th17 cells, ROR-γt induces IL-17A/F expression and Th17 cells differentiation in antigen-stimulated naïve CD4+ T cells [78]. The expression of ROR-γt is positively regulated by IL-6/21/23, TGF-β, and some transcription factors, such as STAT3, IRF4, eomesodermin (Eomes), RUNX1, c-Rel, and induces the differentiation of naïve CD4+ T cells into Th17 cells [79]. Yang et al. also found that ROR-γt and RORα, another orphan nuclear receptor, co-expression synergistically promoted Th17 differentiation in vitro [80].
Tregs
Tregs play an important role in preventing autoimmune diseases and maintaining immune homeostasis as inhibitors of inflammatory response [81, 82]. Tregs are induced in vitro by naïve CD4+ T cells in the presence of specific factors such as TGF-β and IL-2 [83]. FOXP3 is a transcription factor that plays a dominant role in the differentiation of Tregs. Studies have shown that FOXP3 locus contains multiple conserved regulatory sequences [84] of many factors, such as STAT5 [85], SMADs [86], c-Rel [87], special AT-rich sequence-binding protein 1 (SATB1) [88], NFAT [89] and nuclear receptor 4 A (NR4A) [90], which bind to FOXP3 promoter or other regulatory regions to promote its transcription and induce the differentiation of Tregs (Fig. 2e). In addition, cytokines, especially IL-7 [91] and IL-15 [92], and other transcription factors, such as RUNX1 [93], FOXO1 [94] and Helios [95], also play a very important role in the differentiation and maintenance of Tregs.
Tfh cells
Tfh cells are a subset of CD4+ T cells first identified in human tonsil [96, 97], which help the formation of germinal centres (GCs), and promote the generation of high-affinity antibodies and the development of memory B cells [98,99,100]. Tfh cells play an important role in allergic reactions [101], systemic autoimmune diseases [102, 103] and chronic inflammation [104].
Like other T cell subsets, Tfh cell differentiation is also regulated by a variety of cytokines and transcription factors [98, 105, 106]. Briefly, cytokines such as IL-6 [107, 108], IL-12 [109], IL-21 [110], and IL-27 [111] promote Tfh cell differentiation, while IL-2 [112], IL-10 [113], and programmed death 1 (PD-1) [114] inhibit Tfh cell differentiation. B cell lymphoma 6 (Bcl-6) is a key transcription factor regulating Tfh cell differentiation, and it is crucial for the expression of Tfh cell-related factors and the development of Tfh cells [115, 116]. Transcription factors such as STAT1/3/4 [107, 117, 118], IRF4 [119] and basic leucine zipper transcription factor (BATF) [120] also play an active role in promoting the expression of Bcl-6 and the differentiation of Tfh cells (Fig. 2f).
CD4+ T cells and PD
The blood-brain barrier (BBB) is an important tissue to maintain the balance of the brain microenvironment, which can effectively prevent peripheral immune cells and other neurotoxic substances from entering the brain from the blood [121]. Therefore, CNS was once thought to be an “immunologically privileged” site where surrounding immune cells could not or rarely enter [122]. However, studies have shown that dysregulation of neuroinflammation disrupts the integrity of the BBB, which provides the possibility for peripheral immune cells to infiltrate the brain parenchyma [123]. As expected, increasing evidence proves that infiltrating T cells and inflammatory cytokines existed in the post-mortem brain tissues of PD patients and PD animal models, implicating T lymphocytes immune response happened in PD [124,125,126].
Brochard et al. [18] found that in a mouse model of PD, CD8+ and CD4+ T cells but not B cells invaded the brain. Further studies found that mice lacking CD4+ T cells attenuated MPTP-induced DA neuronal death, but not mice lacking CD8+ T cell. These results suggest that CD4+ T cells play a more important role in the development of PD. Similarly, many studies have shown disturbances in the peripheral immune cells and brain parenchyma of PD patients with CD4+ T cell subsets [17, 18, 127, 128]. Magistrelli et al. also found that peripheral CD4+ T cells were associated with cognitive dysfunction in patients with PD. Patients with cognitive impairment had more circulating CD4+ T cells than patients with normal cognitive function [129]. During the pathological development of PD, the abnormally accumulated α-syn binds to Toll-like receptors (TLR) to activate microglia, thereby inducing the release of pro-inflammatory cytokines (mainly IFN-γ and TNF-α) and promoting the differentiation of CD4+ T cells into Th1 and Th17 cells [130]. More importantly, a growing number of studies have shown that Th1 and Th17 aggravate the damage of DA neurons, while Th2 and Tregs have neuroprotective effects [131, 132]. Although there is currently no clear evidence to prove the function of Th9 cells and Tfh cells in PD, the cytokines secreted from these cells regulate neuronal survival. In addition, dysregulation of CD4+ T cell-related transcription factors is receiving attention since it is a special molecular feature of idiopathic rapid eye movement (REM) sleep behavior disorder patients and PD patients, and used to identify motor complications [133, 134]. Therefore, understanding the roles of CD4+ T cells and related cytokines in PD is crucial for the diagnosis and treatment of PD.
Th1 cell-associated cytokines in PD
Th1 cells are thought to have a pro-inflammatory phenotype and promote neuronal loss in neurodegenerative diseases such as PD. Compared with healthy controls, the number and frequency of Th1 cells in the peripheral blood of PD patients were significantly increased [135,136,137], and it was positively correlated with UPDRS-I score (Unified Parkinson’s Disease Rating Scale I score) and negatively correlated with MMSE score (Mini-Mental State Examination) [138, 139]. Kustrimovic et al. found that although the absolute number of Th1 cells in PD patients was similar to that in healthy controls, an increased proportion of Th1 cells was observed, which led to a Th1 bias [136]. As a result, Th1 cells significantly increased production of cytokines such as IFN-γ and TNF-α, which affect neuronal survival [140,141,142,143,144]. In PD animal models, increased Th1 cells were also found in the brain tissues of MPTP-treated PD mice, and adoptive transfer of Th1 cells increased neurodegeneration (Fig. 3) [145, 146].
IL-2
IL-2 is an immune cytokine that plays an important role in immune cell survival and anti-infection immunity. Benveniste and Saneto et al. first reported in 1986 that IL-2 inhibited the growth of glial cells, especially the proliferation and differentiation of oligodendrocytes [147, 148]. Later study found that IL-2 played a role by regulating the phagocytosis activity and the production of reactive oxygen species (ROS) in stimulated microglia-like cells [149]. In addition, IL-2 has been shown to be a potent regulator of DA neuron activity in the mesocortex limbic and mesocortex striatal systems, and plays a key role in inducing endogenous changes in the CNS and the homing of T cells into the brain [150, 151]. These results suggest that IL-2 plays an important role in neurological diseases, including PD.
Although a small number of studies are controversial [152, 153], more and more studies confirm that IL-2 level is significantly increased in peripheral blood [154,155,156,157] and cerebrospinal fluid (CSF) [158] of PD patients compared with healthy controls, and is negatively correlated with cognitive performance of early PD patients [159]. Similarly, IL-2 level was also found to be significantly increased in mouse PD models treated with MPTP or 6-hydroxydopamine (6-OHDA) [160,161,162]. Besides, α-syn overexpression also promoted the increase of IL-2 mRNA level in the cerebral cortex of mice [163].
TNF-α
In the CNS, TNF-α is mainly produced by glial cells and neurons in response to intracellular and extracellular stimuli and is considered to be the primary mediator of neuroinflammation [164]. TNF-α performs its biological function by binding to two cell surface receptors, TNFR1 (p55) and TNFR2 (p75). Although TNFR1 is expressed in most cell types, TNFR2 is mainly expressed by microglia and endothelial cells [165, 166].
A large number of studies have found that TNF-α is closely related to the pathological process of PD patients. The level of TNF-α in peripheral blood [157, 167, 168], CSF [158, 169] and brain [170, 171] of PD patients is significantly increased compared with healthy controls. Clinical studies have found that TNF-α (-308) gene polymorphisms increase the risk of PD [172]. In addition, the level of TNF-α in peripheral blood of PD patients is closely related to the severity of the symptoms, such as fatigue [173,174,175]. Therefore, TNF-α level may be an important biomarker for early diagnosis in PD patients.
TNF-α exacerbates the death of DA neurons in animal models of PD. Carvey et al. found that injection of TNF-α into the forebrain of mice resulted in the loss of DA neurons in the SN, providing direct evidence that TNF-α alone can induce the death of DA neurons [176]. In MPTP-treated PD mouse models, the number of activated microglia and pro-inflammatory cytokines were significantly reduced in TNF-α KO mice compared to WT mice, and MPTP-induced BBB destruction was also mitigated [177]. Similarly, in 6-OHDA-induced mouse or rat models, low expression of TNF-α in the SN significantly reduces the microglia activation and loss of SN neurons [178, 179]. In addition, mice lacking both TNFRs had a protective effect against MPTP-induced DA neuron loss [180, 181]. Using in vitro experiments, Takeuchi et al. found that TNF-α-induced neurotoxicity was caused by glutamate released from microglia [182]. Other studies have suggested that TNF-α released by activated microglia causes mitochondrial dysfunction, which in turn induces apoptosis of neurons or neural precursor cells [183, 184]. Interestingly, the accumulation of α-syn in PD patients is also thought to be associated with abnormal expression of TNF-α. Wang et al. demonstrated that a subtoxic dose of TNF-α impaired autophagy flux and disrupted α-syn degradation by reducing lysosomal acidification, leading to accumulation of α-syn in midbrain neurons [185]. Another study suggests that TNF-α-treated neurons promote the acquisition of a senescence-associated secretory phenotype (SASP), while α-syn secretion increases significantly in aging neurons [186].
Conversely, there is evidence that TNF-α also has a neuroprotective function. In 6-OHDA-treated PD mouse models, low levels of TNF-α reduced nigrostriatal neurodegeneration, while high levels increased neuronal loss [178]. This suggests that low levels of TNF-α may play a neuroprotective role in the development of PD. In addition, the timing of TNF-α expression, brain regions, and factors that stimulate TNF-α signaling may determine the role of TNF-α in neuroinflammation [187].
IFN-γ
IFN-γ is an important inflammatory cytokine, which mainly promotes the activation and proliferation of microglia, induces the expression of T-cell-related chemokines and plays an important role in microglia-mediated neurodegeneration [141, 188, 189]. Under pathological conditions, IFN-γ can enter the brain parenchyma through the BBB, then inhibits the proliferation of neural stem cells and precursor cells, finally induces the death of neurons [190, 191]. In addition, Hashioka et al. found that supernatants produced by IFN-γ-activated astrocytes reduced SH-SY5Y cell viability, suggesting that activated astrocytes generated neurotoxicity when stimulated by IFN-γ [192].
A large number of studies have found that IFN-γ in the peripheral blood of PD patients is significantly increased [156, 157, 193], however, there are also studies to prove that the level of IFN-γ in the peripheral blood of PD patients is unchanged or even decreased compared with healthy controls [153, 167, 194], and lower level of IFN-γ is associated with more severe tremor in PD patients [195]. Interestingly, unlike in patients with PD, IFN-γ level was significantly increased in multiple PD animal models [141, 161, 162, 168, 196,197,198]. In the CNS of IFN-γ transgenic mice, the proliferation of microglia and astrocytes was accelerated, accompanied by the degeneration of the SNpc and the reduction of TH+ neurons in the dense region of the SNpc. Moreover, the transgenic mice showed symptoms similar to frozen of gait, suggesting that IFN-γ has the potential to induce PD [199]. In MPTP-treated monkey PD models, microglia were extensively activated and IFN-γ immunoreactivity was observed, and expression level of IFN-γ was strongly correlated with motor impairment and DA cell death [141]. In addition, Xue et al. demonstrated that lipopolysaccharide (LPS) + IFN-γ treatment significantly increased the expression of IL-1β, TNF-α, and IL-6 in BV2 cells, and up-regulated the caspase3 level while down-regulated the Bcl-2 expression, suggesting that IFN-γ may induce neuronal apoptosis by increasing the expression of inflammatory factors [200]. Leucine-Rich Repeat Kinase 2 (LRRK2) is a PD-associated kinase, which mutations are significantly associated with an increased risk of PD [201]. It has been found that LRRK2 is induced by IFN-γ via extracellular signal-regulated kinase 5 (ERK5) [202], and their synergistic activation plays a potentially important role in inflammation and neurodegeneration in PD [203]. These studies suggest that the proinflammatory effects of IFN-γ play an important role in the pathological development of PD.
Th2-associated cytokines in PD
Contrary to Th1 cells, multiple studies have shown that Th2 cells are significantly reduced in PD patients, and the ratio of Th1/Th2 is significantly increased, and the ratio increases with the deterioration of the disease [135, 136, 138, 139, 204]. Studies have shown that α-syn plays an important role in the development and function of T lymphocytes. Shameli et al. found defective Th2 differentiation and significantly reduced IL-4 secretion in α-syn KO mice, which possibly due to the altered affinity of TCR interactions in the absence of α-syn [205]. The cytokines produced by Th2 cells (IL-4 and IL-13) are also involved in cognitive function by activating astrocytes, and these results are important for the prevention and treatment of neurodegenerative diseases such as PD (Fig. 3) [206,207,208].
The regulation mechanisms of Th1 and Th2 cells in PD. In PD animal models, inflammatory factors such as TNF-α, IFN-γ, and IL-2 secreted by Th1 cells enter the brain parenchyma through the BBB and promote neuroinflammatory response. TNF-α performs its biological function by binding to the cell surface receptor TNFR1. TNF-α significantly activates microglia and induces neuronal death. This neurotoxicity may be caused by glutamate released by microglia, mitochondrial dysfunction, and the acquisition of SASP. In addition, IFN-γ and IL-2 levels are also significantly elevated in PD models and have been shown to be effective regulators of DA neuronal activity. In contrast to Th1 cells, the secretion of IL-4 and other anti-inflammatory factors by Th2 cells in PD patients is significantly reduced. Microglia-derived IL-4 promotes neuroprotection by regulating the secretion of neuroprotective factors such as IGF-1
IL-4/13
IL-4 and IL-13 are two cytokines mainly secreted by Th2 cells, in addition, Tfh and group 2 innate lymphoid cells (ILC2s) have also been found to be important sources of IL-4 and IL-13, respectively [209]. IL-4 and IL-13 genes are located in the same vicinity on chromosome 5, and they share 20–25% homology at amino acid level [210]. Additionally, IL-4 and IL-13 partially share a same receptor, the IL-13 receptor alpha 1 chain (IL-13Rα1) [211]. Therefore, they may have similar biological functions.
In most studies, IL-4 and IL-13 have been shown to have a neuroprotective effect on the CNS by reducing the inflammatory response. IL4 and IL-13 induced the death of microglia treated with neurotoxins such as LPS and ganglioside mixture (Gmix) in vitro, thereby increasing neuronal survival [212]. IL-13 promoted cognitive function by stimulating the production of brain-derived neurotrophic factors (BDNF) by primary astrocytes [208]. In a mouse model of permanent middle cerebral artery occlusion (pMCAo), IL-13 treatment significantly increased the M2-type microglia/macrophage ratio in ischemic areas of brain and the anti-inflammatory cytokines IL-6 and IL-10 levels in the plasma [213]. IL-13 also produced long-term neuroprotection in mice with transient middle cerebral artery occlusion (tMCAO) by inhibiting STAT3 activation in microglia [214]. On the other hand, IL-4 and IL-13 accelerate the loss of neurons under inflammatory conditions. Studies find that the levels of IL-4 and IL-13 are increased significantly with the treatment of neurotoxins [215,216,217]. In addition, IL-13Rα1 increases the susceptibility to LPS-induced oxidative damage of DA neurons [218], and deficiency of IL-13Rα1 delays the loss of DA neurons during chronic stress [219].
Clinical studies have found that two single nucleotide polymorphisms of IL-13 and IL13-RA1 (rs148077750 and rs145868092) increase the risk of PD [220], suggesting that IL-4 and IL-13 play an important role in the development of PD. However, the expression of IL-4 and IL-13 in PD patients and PD animal models is controversial. Some studies suggest that IL-4 expression is significantly increased in PD patients [157, 167, 221,222,223], and higher level of IL-4 is significantly correlated with the severity of tremors in PD patients [195]. IL-13 level is also significantly higher in plasma of PD patients compared with healthy controls [156, 193, 224]. However, other studies show quite different results [194, 225, 226]. Hühner et al. found that exogenous IL-4 protected mDA neurons from 1-methyl-4-phenylpyridinium (MPP+) induced loss in the presence of glial cells in vitro, and that primary microglia-derived IL-4 promoted neuroprotection by modulating the secretion of neuroprotective factors such as insulin growth factor-1(IGF-1). In vivo experiments demonstrated that the loss of IL-4 did not affect the susceptibility of mDA neurons to MPTP-induced damage, and nigrostriatal development was not impaired in IL-4 deficient mice [227, 228]. Interestingly, another study found that IL-4 was involved in LPS-induced SN neurodegeneration and microglial activation in vivo, which was related to upregulation of the pro-inflammatory cytokine IL-1β and disruption of the BBB and astrocytes [229]. The different effects of IL-4 in the two studies may be due to different drug administration and different cells.
IL-5
IL-5 is a type of cytokine secreted mainly by Th2 cells and ILC2s [230], and plays a key role in the development, differentiation and survival of eosinophils. IL-5 and its receptors have now become important targets for treating diseases such as asthma [231], chronic sinusitis [232], and hypereosinophilic syndrome [233]. The expression level of IL-5 in PD is different in different research groups. Di Lazzaro et al. [234]. and Hasan Kadhum al-Huchaimi et al. [235]. found that IL-5 was significantly reduced in PD patients compared with healthy controls, while Walker et al. found that the expression of IL-5 in protein level in SN of PD patients was higher than that in healthy controls or incidental Lewy body disease (ILBD) patients, and ROC curve analysis had significant predictive value [236]. It has been demonstrated that IL-5 promotes the proliferation and activation of microglia [237, 238], but how IL-5 affects the death of PD-related neurons is still unknown.
Th9-associated cytokines in PD
Although the function of Th9 cells in PD is unclear, its main cytokine IL-9 has potential pro-inflammatory effects. IL-9 is a multifunctional cytokine that is mainly produced by Th9 cells [239], but also secreted in small amounts by Th17 cells [240]. Studies have shown that IL-9 level is elevated in a variety of inflammation-related diseases, such as mild traumatic brain injury (mTBI) [241] and AD [242, 243], and has effects on the development of the diseases. In a mouse model of experimental autoimmune encephalomyelitis (EAE), Li et al. found that the KO of IL-9 reduced inflammatory cell invasion to the CNS, which downregulated IL-17, IFN-γ, TNF-α, and IL-12p70, and inhibited chemokine receptors CCR2, CCR5, and CCR6. Furthermore, IL-9 mediated Th17 cell differentiation was regulated by STAT1 and STAT3 [244]. Interestingly, another study showed that IL-9R KO increased granulocyte-macrophage colony-stimulating factor (GM-CSF) levels and the number of DCs, resulting in a more severe EAE phenotype [245]. Donninelli et al. also found that IL-9 played an anti-inflammatory role in multiple sclerosis (MS) by decreasing the activation of human macrophages and increasing the secretion of the anti-inflammatory cytokine TGF-β [246]. The contradictions in these results reflect the complexity of IL-9 functions, as IL-9 has been shown to promote the differentiation of Th17 cells and Tregs in different cellular environments [247]. Thus, IL-9 plays an anti-inflammatory role in PD, studies have found that the level of IL-9 in the CSF [158] and serum [248] of PD patients is significantly reduced compared with healthy controls, however, the mechanism of IL-9 in PD remains unclear.
Th17-associated cytokines in PD
Numerous studies have reported significant variations regarding level of Th17 cells among individuals with PD. Some studies indicate marked increases in the peripheral blood of PD patients while others suggest no change or even decreases. These discrepancies may be resulted from differences in assessing Th17 cell populations [249]. In animal models, MPTP-treated mice show a BBB disruption, resulting in a significant increase in Th17 cells and IL-17A in the SN [146, 250, 251]. Furthermore, adoptive transfer of nitrated α-syn (N-α-syn)-treated Th17 cells significantly enhanced MPTP-induced neurotoxicity [146]. Liu et al. have also demonstrated that Th17 cells exacerbate the loss of neurons in vitro [250]. All these provide direct evidence for the neurotoxic effects of Th17 cells. Additionally, Sommer et al. found that Th17 cells accelerated the death of midbrain neurons (MBNs) induced by PD patient-derived induced pluripotent stem cells (iPSCs). This may be due to the secretion of pro-inflammatory cytokines, such as IL-17, TNF-α, IL-1β, and IL-6 [252]. Studies in animal models have also shown that direct association between Th17 cells and neurons is mediated by the leukocyte function-associated antigen (LFA-1)/intercellular adhesion molecule (ICAM)-1 system, which leading to neuronal apoptosis [250]. Taken together, these findings suggest that Th17 cells and related inflammatory factors play a significant role in the pathology of PD (Fig. 4).
IL-17A/F
The IL-17 family is composed of six members (IL-17A-17F) that play essential roles in important processes such as host immune defense, autoimmune diseases, and cancer progression [253]. IL-17A is considered the hallmark cytokine of Th17 cells [254], and while its role in neurodegenerative diseases is still controversial, there is a study showing that IL-17A is involved in neuroinflammation and cognitive impairment in aged rats by activating microglia [255]. Both IL-17A and IL-17F bind to a heterodimer consisting of IL-17 receptor A (IL-17RA) and IL-17RC [256]. Similar to IL-17A, IL-17F also plays an important driving role in the inflammatory response [257].
Kebir et al. found that IL-17 and IL-22 disrupted the integrity of the BBB and promoted CD4+ lymphocyte migration [258]. This finding is supported by the observation of increased levels of IL-17 and IL-17-producing Th17 cells in both PD patients [157, 221] and PD animal models [196, 251, 259]. Additionally, Gate et al. demonstrated that α-syn stimulation promoted the expression of IL-17A in T cells of LBD patients, providing a possible explanation for the elevated level of IL-17 in PD patients [260]. Further clinical studies have also found that IL-17 is associated with non-motor symptoms in PD patients, including anxiety, depression, and cognitive impairment [261, 262]. However, some studies have reported significantly lower level of IL-17 in PD patients compared to healthy controls, reflecting the high heterogeneity of IL-17 in PD [194, 234].
In MPTP-treated mice, increased IL-17A activates microglia and aggravates the loss of DA neurons. This may be due to an increase in TNF-α, which is present in higher concentrations in IL-17A-treated microglia. However, this neurotoxicity is mitigated by TNF-α-neutralizing antibodies [251]. Sommer et al. have shown that Th17 cells from PD patients or IL-17 induces MBNs death through upregulation of IL-17R and activation of downstream nuclear factor κB (NF-κB). Blocking IL-17/17R or adding an FDA-approved anti-IL-17 antibody, secukinumab, reduces neuronal death [252]. Another study has also demonstrated that secukinuma reduces neuroinflammation in PD rats by blocking the interaction between IL-17A and IL-17RA [259]. Moreover, IL-17A and IL-17F also play pro-inflammatory roles by inducing the expression of other cytokines and chemokines, such as IL-1β, IL-6, TNF-α, granulocyte colony-stimulating factor (G-CSF), CXCL1, CXCL2, CXCL8, and CCL10 [72, 263]. In addition, IL-17A has been found to be helpful in maintaining intestinal homeostasis [264], and the intestinal microbiota has the ability to induce Th17 differentiation [265]. These findings will provide new insights for studying the relationship between PD patients and intestinal microbes.
IL-21
IL-21 is an inflammatory factor that is mainly produced by Th17 cells and Tfh cells. During chronic viral infections, IL-21 produced by CD4+ T cells directly or indirectly maintains the normal activity and function of CD8+ T cells by preventing CD8+ T cell exhaustion [266, 267] and reducing Tregs cell activity [268]. IL-21 also plays an important role in immune regulation in various neurodegenerative diseases, such as ALS [269] and AD. For instance, Agrawal et al. found that IL-21 contributed to neuroinflammation in AD mouse models by activating microglia and increasing the production of inflammatory cytokines such as TNF-α, IL-18, and IL-6 [270]. However, the function and mechanism of IL-21 in PD remain unclear.
IL-22
IL-22 is also a member of the IL-10 family, and its receptor, IL-22R, is a heterodimer composed of IL-22rα and IL-10Rβ subunits [271]. IL-22 is mainly produced by activated T cells, NK cells, ILCs, and neutrophils [272, 273], with Th17 cells being the main source [274]. IL-22 has been detected in various of tissues, including the gut, skin, lungs, liver, and eyes [275]. In addition, IL-22 is also expressed in human brain tissue, suggesting a potential role in the CNS diseases [276]. IL-22 has different anti-inflammatory or pro-inflammatory functions in different tissues, which depends on the environment and cytokines in which it is located [277].
IL-22 expression level is also significantly elevated in AD and PD patients or animal models [242, 278,279,280]. Mechanically, both IL-22 and IL-17 disrupt the BBB permeability, as demonstrated in EAE models [258]. In vitro studies have shown that IL-22 may improve the survival rate of human astrocytes through the anti-apoptotic pathway [276, 281]. Additionally, IL-22 activates microglia to produce more inflammatory factors, leading to neuronal death, which may be the main cause of neurodegeneration [277]. Furthermore, Lee et al. found that the interaction between IL-22 and IL-22Rα induced the production of pro-inflammatory factors TNF-α and IL-6 in BV2 and HT22 cells, and the c-jun N-terminal kinase (JNK) and STAT3 signaling pathways played an important role in this process [282]. However, IL-22 also plays an important role in inhibiting the inflammatory response. Gao et al. found that troxerutin, a clinical anticoagulant that acts as an IL-22 enhancer, increased IL-22 level in rats and activated the microglial IL-22R1/IRF3 system, promoting microglial M2 polarization. This leads to an increase in the anti-inflammatory factor IL-10 and a decrease in the pro-inflammatory factors IL-1β, TNF-α and IL-6 [283]. Therefore, a comprehensive understanding of the functions and mechanisms of IL-22 in neuroinflammation is very important for the treatment of neurodegenerative diseases.
Treg-associated cytokines in PD
Compared to healthy controls, the number of Tregs in the peripheral blood of PD patients is significantly reduced, and the proportion of Tregs is negatively correlated with the severity of motor symptoms, as measured by UPDRS-III scores [128, 284, 285]. This reduction of Tregs is also observed in animal models of PD. MPTP-treated PD mice exhibits fewer Tregs, and the adoptive transfer of Tregs reduces the brain’s inflammatory response and alleviated neuronal death [146, 286]. There is growing evidence suggesting that Tregs reduce neuroinflammation and promote neuronal survival by inhibiting glial cell activation [18, 146, 286,287,288,289,290]. Reynolds et al. demonstrated that the adoptive transfer of Tregs significantly reduced the inflammatory response of microglia, up-regulated the expression of BDNF and glial cell-derived neurotrophic factor (GDNF), and down-regulated the pro-inflammatory cytokines and oxidative stress, ultimately providing a protective effect on the nigrostriatum in MPTP-treated mice [146, 286, 287]. Furthermore, Tregs have been shown to protect neurons through a cell-contact dependent manner. Huang et al. revealed the protective function of Tregs on MN9D cells, a mDA neuronal cell line, and ventral mesencephalic neurons in vitro through the interactions of CD45-galectin-1 and CD47-SIRPA, respectively [291, 292]. These experimental data provide strong support for the role of Tregs in neuroprotection. (Fig. 4)
IL-10
IL-10, an anti-inflammatory and immunosuppressive cytokine produced by both innate and adaptive immune cells, plays an important role in the development of numerous chronic human diseases associated with inflammation [293]. Recent studies have demonstrated that IL-10 also plays a role in neuroinflammation-related neurodegeneration such as MS, traumatic brain injury, amyotrophic lateral sclerosis, AD, and PD, and is now a potential target for the treatment of neurodegenerative diseases [294].
As an anti-inflammatory factor, the expression level of IL-10 in the PD peripheral blood is significantly lower than that in healthy controls [194, 234], and it is negatively correlated with the severity of patients [295] and non-motor symptoms such as PD-related pain [296] and gastrointestinal symptoms [155]. IL-10 level is also significantly reduced in animal models of PD [161, 297, 298]. Mechanistically, IL-10 inhibits glial cell activation and neuronal loss by down-regulating pro-inflammatory mediators, TNF-α, IL-1β, inducible nitric oxide synthase (iNOS), and cyclooxygenase-2 (COX-2) and up-regulating anti-inflammatory factors, such as BDNF, insulin-like growth factor-1, TGF-β and GDNF [299,300,301,302]. Zhu et al. found that IL-10 reduced LPS-induced neuronal loss, while silencing of IL-10 receptor and blocking of Janus kinase (JAK)-STAT3 pathway abolished IL-10 mediated neuroprotective effect [303]. IL-10 also inhibited the synthesis, activation and cleavage of NLRP3, pro-caspase-1 and pro-IL-1β by inhibiting the production of LPS-induced intracellular ROS in vitro. Through this mechanism, IL-10 reduces the occurrence of neuroinflammation [304]. In addition, IL-10 can be regulated by other regulatory factors. For example, the transcription factor myocyte enhancer factor 2D (MEF2D) binds to the promoter of IL-10 and promotes its transcription, thereby inhibiting microglia-mediated cellular inflammation [305].
However, some other studies have found that the expression level of IL-10 in PD patients is significantly increased [154, 167, 222], which reflects the dual function of IL-10 in inflammatory response. Cockey et al. demonstrated that IL-10 and its anti-inflammatory variant I87A variant (v)-IL-10 resulted in shortened lifespan, accelerated α-syn pathology, microglial proliferation and increased apoptosis in A53T PD mice [306]. Therefore, a comprehensive understanding of the mechanisms of IL-10 is essential for the diagnosis and treatment of PD.
IL-35
IL-35 is a newly discovered member of the IL-12 family, consisting of IL-27β chain Ebi3 and interleukin-α chain p35 [307]. IL-35 is an anti-inflammatory cytokine secreted mainly by Tregs and B cells [307, 308]. Recent studies have revealed abnormal expression and function of IL-35 in autoimmune diseases such as systemic lupus erythematosus, rheumatoid arthritis (RA), EAE and MS [309, 310]. Although the role of IL-35 in PD is not well understood, studies have shown that levels of Tregs and their related cytokines IL-35 and TGF-β are correlated with cognitive impairment in AD patients [311]. In addition, Lin et al. have demonstrated that IL-35 has an anti-pyroptosis effect in primary microglia stimulated by LPS and adenosine triphosphate (ATP) [312]. Therefore, it is important to further explore the mechanisms of IL-35 in neurodegenerative diseases, including PD.
TGF-β
Currently, three highly conserved subtypes of TGF-β, named TGF-β1, TGF-β2, and TGF-β3, have been identified in mammals with similar sequence homology [313]. Increasing studies have shown that TGF-β is a negative regulator of inflammation and plays an important role in neuroprotection. TGF-β is essential for the growth and survival of neurons. The double KO of TGF-β2 and TGF-β3 in the embryonic stage results in a significant reduction of DA neurons in the midbrain of mice [314]. Reduced TGF-β signaling in mature neurons also leads to motor deficits and degeneration of the nigrostriatum in mice. By increasing TGF-β signaling in the SN, MPTP-induced DA neuron loss and motor deficits can be significantly reduced [315]. In addition, TGF-β also regulates the differentiation and development of neuronal axons both in vivo and in vitro [316]. Roussa et al. [317]. found that TGF-β, together with Shh and FGF-8 (two factors necessary for the development of mDA neurons), promoted the survival of mDA neurons, while loss of TGF-β1 led to neuronal apoptosis, and neutralization of TGF-βs reduced neuronal death [318, 319]. The protective effect of TGF-β1 on DA neurons results from its ability to block IFNγ-induced microglial activation by inhibiting STAT1 phosphorylation and IFNγRα expression, thereby improving neuronal survival [320]. Studies have also found that TGF-β plays a key role in regulating astrocytes [321]. Removal of TGF-β3 from the medium significantly increased the expression of astrocyte associated markers (GFAP and S100B), while decreasing the expression of DA phenotype-associated markers such as FOXA2 and TH [322].
The anti-inflammatory and neuroprotective properties of TGF-β indicate that it may play an important role in neurodegenerative diseases such as PD. Indeed, higher level of TGF-β has been found in the serum [323] and CSF [324] of PD patients, which may be related to the accumulation of α-syn. Diniz et al. demonstrated that α-syn oligomers (αSO), the most toxic components in PD pathology [325], induced the secretion of TGF-β1 by astrocytes, which promoted the formation of glutamatergic synapses and protected neurons from damage [326]. In in vitro experiment, TGF-β1 treatment significantly inhibits the expression of inflammatory factors in microglia induced by MPP+, and reduced the loss of DA neurons by activating TGF-β receptor (TβR)-I and its downstream p38 mitogen-activated protein kinase (MAPK) and phosphoinositide 3-kinase (PI3K)/Akt signaling pathways in microglia [327]. In a mouse model of PD, intraventricular administration of TGF-β1 improved MPP+-induced microglial activation and inflammatory cytokine production, and alleviated MPP+-induced dyskinesia and behavioral changes [328]. However, it is worth noting that while TGF-β1 has a neuroprotective effect, long-term exposure to it can also have negative effects on neurons. Martinez-Canabal et al. found that transgenic mice overexpressing TGF-β1 in astrocytes had changes in brain structure, especially a significant increase in the hippocampus volume. This led to an increase in the number of granulosa cells within the dentate gyrus (DG) of the hippocampus and ultimately resulted in spatial learning deficits [329]. In addition to TGF-βs, other members of the TGF-β superfamily, such as activins [330], growth and differentiation factors (GDFs) [331], and bone morphogenetic proteins (BMPs) [332], also play vital roles in the regulation of neuroinflammation and the development of PD.
The regulation mechanisms of Th17 and Tregs cells in PD. In animal models of PD, disruption of the BBB results in a significant increase of Th17 cells and cytokines in the SN. Studies have shown that Th17 cells come into direct contact with neurons via the LFA-1/ICAM-1 system in vitro, which leads to neuronal death. Tregs are a subset of anti-inflammatory cells that reduce neuroinflammation and promote neuronal survival by inhibiting the activation of glial cells. Tregs protect neurons through CD47-SIRPA interaction in vitro
Tfh-associated cytokines in PD
Zhao et al. discovered a significant increase in the proportion of peripheral Tfh cells in PD patients compared to healthy controls [333]. In contrast, Li et al. observed a decrease in the number of Tfh cells in PD patients, which was associated with a decrease in Ki-67+ B cells [334]. At present, there are no studies on the mechanism of Tfh cells in PD. The functions of Tfh cytokines IL-4, IL-10 and IFN-γ in PD are discussed in detail in Sect. 3.2.1, 3.1.3 and 3.5.1, respectively.
Immunotherapy for PD
As the global population ages, the risk of developing neurodegenerative diseases such as PD is on the rise. Currently, there are no pharmacological treatments available to completely stop or reverse the progression of PD. Therefore, it is imperative to identify an effective treatment. While current PD treatments primarily involve levodopa or dopamine receptor agonists, these medications provide symptomatic benefits only and do not halt disease progression, may not adequately treat all the symptoms of PD especially non-motor symptoms, and can cause adverse side effects [335]. Given the important role of neuroinflammation in the pathological development of PD, immunotherapy has become a potential approach to alleviate PD disease. At present, immunotherapies targeting CD4+ T cells have become an important means of treating PD. This section provides a summary of clinical trials targeting CD4+ T cells in PD.
Immunotherapy targeting CD4+ T cell-related cytokines
Given the important role of inflammatory response in PD, small molecule drugs targeting inflammatory cytokines, especially antagonists of pro-inflammatory factors, have become a potential treatment for PD (Table 1).
TNF-α inhibitors
Currently, TNF-α inhibitors worldwide mainly include infliximab, adalimumab, certolizumab, golimumab, and etanercept, which provide effective treatment options for a variety of inflammatory diseases. Infliximab [336], adalimumab [337], certolizumab [338], and golimumab [339] are anti-TNF-α monoclonal antibodies, and play important roles in anti-inflammation. In a clinical study, Peter et al. observed that IBD patients who received anti-TNF therapy (infliximab, certolizumab, adalimumab and golimumab) had a significantly lower incidence of PD compared to IBD patients who did not receive anti-TNF therapy. This study suggests that these anti-TNF drugs have the potential to treat PD [340]. Etanercept is a fully humanized soluble recombinant TNF receptor fusion protein [341], which is now used to treat a variety of diseases such as RA [342], psoriasis [343], psoriatic arthritis [344] and ankylosing spondylitis [345]. In in vivo assay, etanercept mitigated the LPS-induced inflammatory response and the microgliosis and astrocytosis in rats, attenuating systemic and local inflammation [346].
IL-1 receptor antagonist
Anakinra (Kineret) is a recombinant human IL-1 receptor antagonist that inhibits IL-1 by binding to IL-1 type 1 receptors. Anakinra is the first biological agent approved to block the pro-inflammatory effects of IL-1 in patients with RA [347]. In addition, anakinra has also achieved good results in clinical trials for diseases such as type 2 diabetes [348], coronavirus disease (COVID-19) [349], intracerebral haemorrhage [350], gout [351], and elevated myocardial infarction [352]. In 6-OHDA-induced rat models of PD, anakinra significantly reduces levels of TNF-α and IFN-γ, and mitigates the loss of DA neurons [353].
IL-17A/IL-17RA inhibitors
There are currently five IL-17A/IL-17RA inhibitors in various stages of clinical development: secukinumab, ixekizumab, brodalumab, netakimab, and bimekizumab [354]. However, only secukinumab has been demonstrated to have neuroprotective properties. Secukinumab selectively targets IL-17A and inhibits its interaction with the IL-17 receptor, thereby inhibiting the release of pro-inflammatory cytokines and chemokines [355]. In rotenone-induced PD rat models, secukinumab exerts neuroprotective effects by inhibiting IL-17A/IL-17RA interaction and activation of TLR-4 and its downstream signaling pathway, as well as activating the TrKB/Akt/CREB/BDNF axis [259]. Additionally, secukinumab rescued neuronal death in vitro [252].
ROR-γt inhibitors
As an important transcription factor, ROR-γt promotes the differentiation of Th17 cell and the expression of IL-17, which plays a pivotal role in the neuroinflammation of PD [78]. Thus, drugs targeting ROR-γt interferes with Th17 differentiation and inhibits the production of multiple inflammatory cytokines, thereby reducing the inflammatory response. Li et al. discovered that the ROR-γt inhibitor GSK805 hindered the increase of Th17 cells, the decrease of Tregs, and the apoptosis of DA in MPTP-treated mice [284].
Tregs inducers
Tregs are indispensable for maintaining normal immune tolerance due to their powerful anti-inflammatory function. A recent study demonstrated that Tregs autologous co-transplantation effectively reduced the needle-trauma-induced death of mDA neurons during cell therapy [356]. Drug-induced enhancement of Tregs function also has been shown to provide neuroprotection for DA neurons and improve clinical scores and prognostic outcomes in PD patients. Currently, Tregs inducers in animal studies or clinical trials mainly include GM-CSF and vasoactive intestinal peptide (VIP). GM-CSF, an inflammatory cytokine, exerts its anti-inflammatory activity primarily by regulating the differentiation of tolerant DCs, leading to an increase in the number and function of Tregs [357]. At present, GM-CSF is undergoing evaluation in clinical studies. In a randomized, double-blind phase 1 clinical PD trial, after 2 months of daily administration of sargramostim (a recombinant human GM-CSF), cortical motor activities, Tregs numbers and function improved in PD patients [358]. VIP is another promising immunomodulatory agent that plays a neuroprotective role by increasing the number and function of Tregs while reducing microglial inflammatory response [146]. In particular, VIP receptor 2 (VIPR2) agonist LBT-3627 increases Tregs activity, inhibits astrocyte proliferation, and reduces neuroinflammation, providing a basis for follow-up immunotherapy in PD patients [359, 360]. Additionally, histone deacetylase (HDAC) inhibitors [361] and RA [362] also play important roles in Tregs-mediated immunotherapy.
Other treatments for PD
In addition, non-steroidal anti-inflammatory drugs (NSAIDs) [363], traditional Chinese medicine (TCM) [364], probiotics [365], vitamin D [366], electrical stimulation [367], stem cell therapy [368], all have proposed anti-inflammatory effects and have been used in the treatment of PD, with varying success.
NSAIDs
NSAIDs are a common analgesic and anti-inflammatory drug that can be absorbed from the stomach and intestinal mucosa and cross the BBB, thereby affecting the CNS [369]. NSAIDs affect PD neuropathology in different ways, producing beneficial, neutral and even harmful effects on neurons. On the one hand, NSAIDs provide neuroprotective effects on the progression of PD neuropathology by inhibiting the expression levels of COX-2 [370] and LRRK2 [371] and their associated inflammatory responses, enhancing endocannabinoid signaling [372] and restoring the activity of serotonergic neurons [373]. On the other hand, long-term use of NSAIDs may adversely affect PD neuropathology by inhibiting the neuroprotective effects of COX-2 and prostacyclin (PGI2) and enhancing the pro-inflammatory Leukotrienes (LTs) pathway. Therefore, a comprehensive understanding of the pharmacological effects of NSAIDs is essential for the treatment of PD [363].
Traditional Chinese medicine
TCM is a complete system of ancient Chinese medical theory and practice with a history of thousands of years. In recent years, TCM has attracted more and more attention in the treatment of PD because of its unique theoretical basis and clinical effect [364]. For example, gastrodin, the main bioactive component of Gastrodiae Rhizoma, has the effect of alleviating neuroinflammation associated with PD both in vivo and in vitro. Li et al. found that gastrodin protected DA neurons by inhibiting the expression of IL-1β and TNF-α in the SN of rotenone-induced PD rats [374]. In addition, Huang et al. found that Berberine alleviated NLRP3-associated neuroinflammation by enhancing autophagy activity in MPTP-induced mice and MPP+ treated BV2 cells in vivo and in vitro [375].
Probiotics
Gastrointestinal dysfunction is one of the most common non-motor symptoms in PD patients, with a prevalence of more than 80% [376]. Studies found that probiotics changed the composition of the PD-associated microbiota, thereby improved the gastrointestinal function of patients [377, 378]. However, the mechanism by which probiotics treat PD remains unclear. An in vitro study showed that probiotics reduced the expression of pro-inflammatory cytokines and oxidative stress in peripheral blood mononuclear cells (PBMC) of patients with PD [379].
Vitamin D
Vitamin D is a fat-soluble steroid vitamin that exists in nature in two main forms, vitamin D2 (ergocalciferol) and vitamin D3 (cholecalciferol) [380]. In recent years, the role of vitamin D in neurodegenerative diseases, particularly in PD, has received attention. In MPTP-induced PD mouse models, vitamin D treatment reduces DA neurodegeneration by upregulating the expression of anti-inflammatory cytokines (IL-10, IL-4, and TGF-β) and the M2 anti-inflammatory phenotype of microglia [381]. In addition, vitamin D can also reduce the cytotoxicity caused by α-syn aggregation by inhibiting ROS production [382]. In clinical studies, increasing vitamin D consumption has been shown to alleviate symptoms in PD patients. A randomized, double-blind trial found that the balance of younger PD patients (ages 52–66) was improved after taking high-dose (10,000 IU/day) of vitamin D for 16 weeks [383].
Electrical stimulation
Deep brain stimulation (DBS) is being widely used as a clinical intervention in the treatment of neuropsychiatric disorders, including PD. The primary target region for DBS electrodes is the subthalamic nucleus (STN), which plays an important role in motor function [384]. In 6-OHDA-induced PD rat models, STN-DBS inhibited the secretion of pro-inflammatory factors and promoted the expression of anti-inflammatory factors, and inhibited the activation of microglia and astrocyte, which played an anti-inflammatory role in PD [385, 386].
Stem cell therapy
Stem cells are a class of cells that have the potential to self-renew and differentiate into different cell types. According to their source, differentiation potential and characteristics, stem cells can be divided into many types, such as embryonic stem cells (ESCs), iPSCs, mesenchymal stem cells and neural stem cells [387]. Stem cell therapy is a promising treatment for neurodegenerative diseases, including PD, because of its angiogenesis, immunomodulatory, neuroprotective and anti-inflammatory functions [388, 389]. For example, a study found that human ESCs (hESCs)-derived MBNs projected long distance in the brain and restored their motor function of rat PD models [390]. Another study from non-human primates found that human iPSCs-derived DA neurons improved the spontaneous motor capacity of MPTP-induced monkey PD models (Macaca fascicularis) and showed ample neurite formation [391]. However, stem cell-based therapies have shown different results in PD, so further study is still needed in future.
Conclusions
In order to protect the host from foreign invasions, the immune system has evolved a series of intricate response mechanisms. CD4+ T cells are an integral part of adaptive immunity, in which different CD4+ T cell subsets play specific roles. PD is the second most common neurodegenerative disease, and neuroinflammation is an important risk factor for it. In this review, we describe the differentiation regulation of different CD4+ T cell subsets and their functions and mechanisms in PD, as well as summarize immunotherapies targeting CD4+ T cells, with a view to providing new strategies for the diagnosis and treatment of PD.
The hallmark of PD pathology is the loss of DA neurons, so the current treatment of PD is mainly through the supplementation of reduced dopamine, such as levodopa and dopamine receptor agonists. In general, levodopa and dopamine receptor agonist are symptomatic treatments only, do not modify disease course and sufficiently address all the symptoms of PD, especially non-motor symptoms. As a potential alternative, immunotherapy targeting CD4+ T cells may become a potential treatment for PD. Although there are many immunotherapies targeting CD4+ T cells and their cytokines, progress in clinical research has been slow. Therefore, accelerating the research on CD4+ T cells in PD will provide new theoretical guidance for us to develop more effective targeted drugs.
Data availability
Not applicable.
References
De Miranda BR, Goldman SM, Miller GW, Greenamyre JT, Dorsey ER (2022) Preventing Parkinson’s disease: an environmental agenda. J Parkinsons Dis 12(1):45–68. https://doi.org/10.3233/JPD-212922
Poewe W, Seppi K, Tanner CM, Halliday GM, Brundin P, Volkmann J et al (2017) Parkinson disease. Nat Rev Dis Primers 3:17013. https://doi.org/10.1038/nrdp.2017.13
Chaudhuri KR, Azulay JP, Odin P, Lindvall S, Domingos J, Alobaidi A et al (2024) Economic Burden of Parkinson’s Disease: a multinational, Real-World, cost-of-illness study. Drugs Real World Outcomes. https://doi.org/10.1007/s40801-023-00410-1
Albarmawi H, Zhou S, Shulman LM, Gandhi AB, Johnson A, Myers DE et al (2022) The economic burden of Parkinson disease among Medicare beneficiaries. J Manag Care Spec Pharm 28(4):405–414. https://doi.org/10.18553/jmcp.2022.28.4.405
Zhao N, Yang Y, Zhang L, Zhang Q, Balbuena L, Ungvari GS et al (2021) Quality of life in Parkinson’s disease: a systematic review and meta-analysis of comparative studies. CNS Neurosci Ther 27(3):270–279. https://doi.org/10.1111/cns.13549
Ye H, Robak LA, Yu M, Cykowski M, Shulman JM (2023) Genetics and Pathogenesis of Parkinson’s syndrome. Annu Rev Pathol 18:95–121. https://doi.org/10.1146/annurev-pathmechdis-031521-034145
Krzyzanowski B, Searles Nielsen S, Turner JR, Racette BA (2023) Fine particulate matter and Parkinson Disease Risk among Medicare beneficiaries. Neurology 101(21):e2058–e67. https://doi.org/10.1212/WNL.0000000000207871
Cryan JF, O’Riordan KJ, Sandhu K, Peterson V, Dinan TG (2020) The gut microbiome in neurological disorders. Lancet Neurol 19(2):179–194. https://doi.org/10.1016/S1474-4422(19)30356-4
Ascherio A, Schwarzschild MA (2019) Lifestyle and Parkinson’s disease progression. Mov Disord 34(1):7–8. https://doi.org/10.1002/mds.27566
He Y, Peng K, Li R, Zhang Z, Pan L, Zhang T et al (2022) Changes of T lymphocyte subpopulations and their roles in predicting the risk of Parkinson’s disease. J Neurol 269(10):5368–5381. https://doi.org/10.1007/s00415-022-11190-z
Bartl M, Xylaki M, Bahr M, Weber S, Trenkwalder C, Mollenhauer B (2022) Evidence for immune system alterations in peripheral biological fluids in Parkinson’s disease. Neurobiol Dis 170:105744. https://doi.org/10.1016/j.nbd.2022.105744
Tansey MG, Wallings RL, Houser MC, Herrick MK, Keating CE, Joers V (2022) Inflammation and immune dysfunction in Parkinson disease. Nat Rev Immunol 22(11):657–673. https://doi.org/10.1038/s41577-022-00684-6
Singh K, Sethi P, Datta S, Chaudhary JS, Kumar S, Jain D et al (2024) Advances in gene therapy approaches targeting neuro-inflammation in neurodegenerative diseases. Ageing Res Rev 98:102321. https://doi.org/10.1016/j.arr.2024.102321
Solleiro-Villavicencio H, Rivas-Arancibia S (2018) Effect of chronic oxidative stress on neuroinflammatory response mediated by CD4(+)T cells in neurodegenerative diseases. Front Cell Neurosci 12:114. https://doi.org/10.3389/fncel.2018.00114
Giri PM, Banerjee A, Ghosal A, Layek B (2024) Neuroinflammation in neurodegenerative disorders: current knowledge and therapeutic implications. Int J Mol Sci 25(7). https://doi.org/10.3390/ijms25073995
Wang P, Yao L, Luo M, Zhou W, Jin X, Xu Z et al (2021) Single-cell transcriptome and TCR profiling reveal activated and expanded T cell populations in Parkinson’s disease. Cell Discov 7(1):52. https://doi.org/10.1038/s41421-021-00280-3
Chen X, Feng W, Ou R, Liu J, Yang J, Fu J et al (2021) Evidence for Peripheral Immune activation in Parkinson’s Disease. Front Aging Neurosci 13:617370. https://doi.org/10.3389/fnagi.2021.617370
Brochard V, Combadiere B, Prigent A, Laouar Y, Perrin A, Beray-Berthat V et al (2009) Infiltration of CD4 + lymphocytes into the brain contributes to neurodegeneration in a mouse model of Parkinson disease. J Clin Invest 119(1):182–192. https://doi.org/10.1172/JCI36470
Williams GP, Schonhoff AM, Jurkuvenaite A, Gallups NJ, Standaert DG, Harms AS (2021) CD4 T cells mediate brain inflammation and neurodegeneration in a mouse model of Parkinson’s disease. Brain 144(7):2047–2059. https://doi.org/10.1093/brain/awab103
Kumar BV, Connors TJ, Farber DL, Human T (2018) Cell Development, localization, and function throughout life. Immunity 48(2):202–213. https://doi.org/10.1016/j.immuni.2018.01.007
Zhu X, Zhu J (2020) CD4 T Helper Cell subsets and Related Human Immunological disorders. Int J Mol Sci 21(21). https://doi.org/10.3390/ijms21218011
Bhattacharyya T, Karnezis AN, Murphy SP, Hoang T, Freeman BC, Phillips B et al (1995) Cloning and subcellular localization of human mitochondrial hsp70. J Biol Chem 270(4):1705–1710. https://doi.org/10.1074/jbc.270.4.1705
Caza T, Landas S (2015) Functional and phenotypic plasticity of CD4(+) T cell subsets. Biomed Res Int 2015:521957doi. https://doi.org/10.1155/2015/521957
Luckheeram RV, Zhou R, Verma AD, Xia B (2012) CD4(+)T cells: differentiation and functions. Clin Dev Immunol 2012:925135. https://doi.org/10.1155/2012/925135
Mosmann TR, Coffman RL (1989) TH1 and TH2 cells: different patterns of lymphokine secretion lead to different functional properties. Annu Rev Immunol 7:145–173. https://doi.org/10.1146/annurev.iy.07.040189.001045
Trinchieri G, Pflanz S, Kastelein RA (2003) The IL-12 family of heterodimeric cytokines: new players in the regulation of T cell responses. Immunity 19(5):641–644. https://doi.org/10.1016/s1074-7613(03)00296-6
Trinchieri G, Sher A (2007) Cooperation of toll-like receptor signals in innate immune defence. Nat Rev Immunol 7(3):179–190. https://doi.org/10.1038/nri2038
Zhu J, Jankovic D, Oler AJ, Wei G, Sharma S, Hu G et al (2012) The transcription factor T-bet is induced by multiple pathways and prevents an endogenous Th2 cell program during Th1 cell responses. Immunity 37(4):660–673. https://doi.org/10.1016/j.immuni.2012.09.007
Kanno Y, Vahedi G, Hirahara K, Singleton K, O’Shea JJ (2012) Transcriptional and epigenetic control of T helper cell specification: molecular mechanisms underlying commitment and plasticity. Annu Rev Immunol 30:707–731. https://doi.org/10.1146/annurev-immunol-020711-075058
Okamura H, Kashiwamura S, Tsutsui H, Yoshimoto T, Nakanishi K (1998) Regulation of interferon-gamma production by IL-12 and IL-18. Curr Opin Immunol 10(3):259–264. https://doi.org/10.1016/s0952-7915(98)80163-5
Gutcher I, Becher B (2007) APC-derived cytokines and T cell polarization in autoimmune inflammation. J Clin Invest 117(5):1119–1127. https://doi.org/10.1172/JCI31720
Holscher C (2004) The power of combinatorial immunology: IL-12 and IL-12-related dimeric cytokines in infectious diseases. Med Microbiol Immunol 193(1):1–17. https://doi.org/10.1007/s00430-003-0186-x
Szabo SJ, Kim ST, Costa GL, Zhang X, Fathman CG, Glimcher LH (2000) A novel transcription factor, T-bet, directs Th1 lineage commitment. Cell 100(6):655–669. https://doi.org/10.1016/s0092-8674(00)80702-3
Djuretic IM, Levanon D, Negreanu V, Groner Y, Rao A, Ansel KM (2007) Transcription factors T-bet and Runx3 cooperate to activate Ifng and silence Il4 in T helper type 1 cells. Nat Immunol 8(2):145–153. https://doi.org/10.1038/ni1424
Kohu K, Ohmori H, Wong WF, Onda D, Wakoh T, Kon S et al (2009) The Runx3 transcription factor augments Th1 and down-modulates Th2 phenotypes by interacting with and attenuating GATA3. J Immunol 183(12):7817–7824. https://doi.org/10.4049/jimmunol.0802527
Kaplan MH, Schindler U, Smiley ST, Grusby MJ (1996) Stat6 is required for mediating responses to IL-4 and for development of Th2 cells. Immunity 4(3):313–319. https://doi.org/10.1016/s1074-7613(00)80439-2
Zhu J, Guo L, Watson CJ, Hu-Li J, Paul WE (2001) Stat6 is necessary and sufficient for IL-4’s role in Th2 differentiation and cell expansion. J Immunol 166(12):7276–7281. https://doi.org/10.4049/jimmunol.166.12.7276
Yagi R, Zhu J, Paul WE (2011) An updated view on transcription factor GATA3-mediated regulation of Th1 and Th2 cell differentiation. Int Immunol 23(7):415–420. https://doi.org/10.1093/intimm/dxr029
Paul WE, Zhu J (2010) How are T(H)2-type immune responses initiated and amplified? Nat Rev Immunol 10(4):225–235. https://doi.org/10.1038/nri2735
Wei G, Abraham BJ, Yagi R, Jothi R, Cui K, Sharma S et al (2011) Genome-wide analyses of transcription factor GATA3-mediated gene regulation in distinct T cell types. Immunity 35(2):299–311. https://doi.org/10.1016/j.immuni.2011.08.007
Wohlfert EA, Grainger JR, Bouladoux N, Konkel JE, Oldenhove G, Ribeiro CH et al (2011) GATA3 controls Foxp3(+) regulatory T cell fate during inflammation in mice. J Clin Invest 121(11):4503–4515. https://doi.org/10.1172/JCI57456
Fang D, Cui K, Hu G, Gurram RK, Zhong C, Oler AJ et al (2018) Bcl11b, a novel GATA3-interacting protein, suppresses Th1 while limiting Th2 cell differentiation. J Exp Med 215(5):1449–1462. https://doi.org/10.1084/jem.20171127
Zhu J, Min B, Hu-Li J, Watson CJ, Grinberg A, Wang Q et al (2004) Conditional deletion of Gata3 shows its essential function in T(H)1-T(H)2 responses. Nat Immunol 5(11):1157–1165. https://doi.org/10.1038/ni1128
Usui T, Nishikomori R, Kitani A, Strober W (2003) GATA-3 suppresses Th1 development by downregulation of Stat4 and not through effects on IL-12Rbeta2 chain or T-bet. Immunity 18(3):415–428. https://doi.org/10.1016/s1074-7613(03)00057-8
Yagi R, Junttila IS, Wei G, Urban JF Jr., Zhao K, Paul WE et al (2010) The transcription factor GATA3 actively represses RUNX3 protein-regulated production of interferon-gamma. Immunity 32(4):507–517. https://doi.org/10.1016/j.immuni.2010.04.004
Schmitt E, Germann T, Goedert S, Hoehn P, Huels C, Koelsch S et al (1994) IL-9 production of naive CD4 + T cells depends on IL-2, is synergistically enhanced by a combination of TGF-beta and IL-4, and is inhibited by IFN-gamma. J Immunol 153(9):3989–3996
Deng Y, Wang Z, Chang C, Lu L, Lau CS, Lu Q (2017) Th9 cells and IL-9 in autoimmune disorders: Pathogenesis and therapeutic potentials. Hum Immunol 78(2):120–128. https://doi.org/10.1016/j.humimm.2016.12.010
Kara EE, Comerford I, Bastow CR, Fenix KA, Litchfield W, Handel TM et al (2013) Distinct chemokine receptor axes regulate Th9 cell trafficking to allergic and autoimmune inflammatory sites. J Immunol 191(3):1110–1117. https://doi.org/10.4049/jimmunol.1203089
Vegran F, Apetoh L, Ghiringhelli F (2015) Th9 cells: a novel CD4 T-cell subset in the immune war against cancer. Cancer Res 75(3):475–479. https://doi.org/10.1158/0008-5472.CAN-14-2748
Lu Y, Hong S, Li H, Park J, Hong B, Wang L et al (2012) Th9 cells promote antitumor immune responses in vivo. J Clin Invest 122(11):4160–4171. https://doi.org/10.1172/JCI65459
Kaplan MH (2013) Th9 cells: differentiation and disease. Immunol Rev 252(1):104–115. https://doi.org/10.1111/imr.12028
Anuradha R, George PJ, Hanna LE, Chandrasekaran V, Kumaran P, Nutman TB et al (2013) IL-4-, TGF-beta-, and IL-1-dependent expansion of parasite antigen-specific Th9 cells is associated with clinical pathology in human lymphatic filariasis. J Immunol 191(5):2466–2473. https://doi.org/10.4049/jimmunol.1300911
Fung MM, Chu YL, Fink JL, Wallace A, McGuire KL (2005) IL-2- and STAT5-regulated cytokine gene expression in cells expressing the tax protein of HTLV-1. Oncogene 24(29):4624–4633. https://doi.org/10.1038/sj.onc.1208507
Anuradha R, Munisankar S, Bhootra Y, Jagannathan J, Dolla C, Kumaran P et al (2016) IL-10- and TGFbeta-mediated Th9 responses in a human helminth infection. PLoS Negl Trop Dis 10(1):e0004317. https://doi.org/10.1371/journal.pntd.0004317
Ma CS, Tangye SG, Deenick EK (2010) Human Th9 cells: inflammatory cytokines modulate IL-9 production through the induction of IL-21. Immunol Cell Biol 88(6):621–623. https://doi.org/10.1038/icb.2010.73
Angkasekwinai P, Chang SH, Thapa M, Watarai H, Dong C (2010) Regulation of IL-9 expression by IL-25 signaling. Nat Immunol 11(3):250–256. https://doi.org/10.1038/ni.1846
Blom L, Poulsen BC, Jensen BM, Hansen A, Poulsen LK (2011) IL-33 induces IL-9 production in human CD4 + T cells and basophils. PLoS ONE 6(7):e21695. https://doi.org/10.1371/journal.pone.0021695
Jiang Y, Chen J, Bi E, Zhao Y, Qin T, Wang Y et al (2019) TNF-alpha enhances Th9 cell differentiation and antitumor immunity via TNFR2-dependent pathways. J Immunother Cancer 7(1):28. https://doi.org/10.1186/s40425-018-0494-8
Murugaiyan G, Beynon V, Pires Da Cunha A, Joller N, Weiner HL (2012) IFN-gamma limits Th9-mediated autoimmune inflammation through dendritic cell modulation of IL-27. J Immunol 189(11):5277–5283. https://doi.org/10.4049/jimmunol.1200808
Goswami R, Jabeen R, Yagi R, Pham D, Zhu J, Goenka S et al (2012) STAT6-dependent regulation of Th9 development. J Immunol 188(3):968–975. https://doi.org/10.4049/jimmunol.1102840
Perumal NB, Kaplan MH (2011) Regulating Il9 transcription in T helper cells. Trends Immunol 32(4):146–150. https://doi.org/10.1016/j.it.2011.01.006
Dardalhon V, Awasthi A, Kwon H, Galileos G, Gao W, Sobel RA et al (2008) IL-4 inhibits TGF-beta-induced Foxp3 + T cells and, together with TGF-beta, generates IL-9 + IL-10 + Foxp3(-) effector T cells. Nat Immunol 9(12):1347–1355. https://doi.org/10.1038/ni.1677
Staudt V, Bothur E, Klein M, Lingnau K, Reuter S, Grebe N et al (2010) Interferon-regulatory factor 4 is essential for the developmental program of T helper 9 cells. Immunity 33(2):192–202. https://doi.org/10.1016/j.immuni.2010.07.014
Elyaman W, Bassil R, Bradshaw EM, Orent W, Lahoud Y, Zhu B et al (2012) Notch receptors and Smad3 signaling cooperate in the induction of interleukin-9-producing T cells. Immunity 36(4):623–634. https://doi.org/10.1016/j.immuni.2012.01.020
Jabeen R, Goswami R, Awe O, Kulkarni A, Nguyen ET, Attenasio A et al (2013) Th9 cell development requires a BATF-regulated transcriptional network. J Clin Invest 123(11):4641–4653. https://doi.org/10.1172/JCI69489
Goswami R, Kaplan MH (2012) Gcn5 is required for PU.1-dependent IL-9 induction in Th9 cells. J Immunol 189(6):3026–3033. https://doi.org/10.4049/jimmunol.1201496
Chang HC, Zhang S, Thieu VT, Slee RB, Bruns HA, Laribee RN et al (2005) PU.1 expression delineates heterogeneity in primary Th2 cells. Immunity 22(6):693–703. https://doi.org/10.1016/j.immuni.2005.03.016
Park H, Li Z, Yang XO, Chang SH, Nurieva R, Wang YH et al (2005) A distinct lineage of CD4 T cells regulates tissue inflammation by producing interleukin 17. Nat Immunol 6(11):1133–1141. https://doi.org/10.1038/ni1261
Zhu J, Paul WE (2008) CD4 T cells: fates, functions, and faults. Blood 112(5):1557–1569. https://doi.org/10.1182/blood-2008-05-078154
Weaver CT, Harrington LE, Mangan PR, Gavrieli M, Murphy KM (2006) Th17: an effector CD4 T cell lineage with regulatory T cell ties. Immunity 24(6):677–688. https://doi.org/10.1016/j.immuni.2006.06.002
Shi Y, Wei B, Li L, Wang B, Sun M (2022) Th17 cells and inflammation in neurological disorders: possible mechanisms of action. Front Immunol 13:932152. https://doi.org/10.3389/fimmu.2022.932152
Gaffen SL, Jain R, Garg AV, Cua DJ (2014) The IL-23-IL-17 immune axis: from mechanisms to therapeutic testing. Nat Rev Immunol 14(9):585–600. https://doi.org/10.1038/nri3707
Bettelli E, Carrier Y, Gao W, Korn T, Strom TB, Oukka M et al (2006) Reciprocal developmental pathways for the generation of pathogenic effector TH17 and regulatory T cells. Nature 441(7090):235–238. https://doi.org/10.1038/nature04753
Mangan PR, Harrington LE, O’Quinn DB, Helms WS, Bullard DC, Elson CO et al (2006) Transforming growth factor-beta induces development of the T(H)17 lineage. Nature 441(7090):231–234. https://doi.org/10.1038/nature04754
Veldhoen M, Hocking RJ, Atkins CJ, Locksley RM, Stockinger B (2006) TGFbeta in the context of an inflammatory cytokine milieu supports de novo differentiation of IL-17-producing T cells. Immunity 24(2):179–189. https://doi.org/10.1016/j.immuni.2006.01.001
Korn T, Bettelli E, Gao W, Awasthi A, Jager A, Strom TB et al (2007) IL-21 initiates an alternative pathway to induce proinflammatory T(H)17 cells. Nature 448(7152):484–487. https://doi.org/10.1038/nature05970
Acosta-Rodriguez EV, Napolitani G, Lanzavecchia A, Sallusto F (2007) Interleukins 1beta and 6 but not transforming growth factor-beta are essential for the differentiation of interleukin 17-producing human T helper cells. Nat Immunol 8(9):942–949. https://doi.org/10.1038/ni1496
Ivanov II, McKenzie BS, Zhou L, Tadokoro CE, Lepelley A, Lafaille JJ et al (2006) The orphan nuclear receptor RORgammat directs the differentiation program of proinflammatory IL-17 + T helper cells. Cell 126(6):1121–1133. https://doi.org/10.1016/j.cell.2006.07.035
Tian Y, Wu Y, Ni B (2015) Signaling pathways and epigenetic regulations in the control of RORgammat expression in T Helper 17 cells. Int Rev Immunol 34(4):305–317. https://doi.org/10.3109/08830185.2014.911858
Yang XO, Pappu BP, Nurieva R, Akimzhanov A, Kang HS, Chung Y et al (2008) T helper 17 lineage differentiation is programmed by orphan nuclear receptors ROR alpha and ROR gamma. Immunity 28(1):29–39. https://doi.org/10.1016/j.immuni.2007.11.016
Josefowicz SZ, Lu LF, Rudensky AY (2012) Regulatory T cells: mechanisms of differentiation and function. Annu Rev Immunol 30:531–564. https://doi.org/10.1146/annurev.immunol.25.022106.141623
Taylor PA, Noelle RJ, Blazar BR (2001) CD4(+)CD25(+) immune regulatory cells are required for induction of tolerance to alloantigen via costimulatory blockade. J Exp Med 193(11):1311–1318. https://doi.org/10.1084/jem.193.11.1311
Gunnlaugsdottir B, Maggadottir SM, Skaftadottir I, Ludviksson BR (2013) The ex vivo induction of human CD103(+) CD25hi Foxp3(+) CD4(+) and CD8(+) Tregs is IL-2 and TGF-beta1 dependent. Scand J Immunol 77(2):125–134. https://doi.org/10.1111/sji.12009
Blinova VG, Vasilyev VI, Rodionova EB, Zhdanov DD (2023) The Role of Regulatory T Cells in the Onset and Progression of Primary Sjogren’s Syndrome. Cells 12(10). https://doi.org/10.3390/cells12101359
Wuest TY, Willette-Brown J, Durum SK, Hurwitz AA (2008) The influence of IL-2 family cytokines on activation and function of naturally occurring regulatory T cells. J Leukoc Biol 84(4):973–980. https://doi.org/10.1189/jlb.1107778
MaruYama T, Kobayashi S, Nakatsukasa H, Moritoki Y, Taguchi D, Sunagawa Y et al (2021) The Curcumin Analog GO-Y030 controls the Generation and Stability of Regulatory T Cells. Front Immunol 12:687669. https://doi.org/10.3389/fimmu.2021.687669
Fulford TS, Grumont R, Wirasinha RC, Ellis D, Barugahare A, Turner SJ et al (2021) c-Rel employs multiple mechanisms to promote the thymic development and peripheral function of regulatory T cells in mice. Eur J Immunol 51(8):2006–2026. https://doi.org/10.1002/eji.202048900
Kitagawa Y, Ohkura N, Kidani Y, Vandenbon A, Hirota K, Kawakami R et al (2017) Guidance of regulatory T cell development by Satb1-dependent super-enhancer establishment. Nat Immunol 18(2):173–183. https://doi.org/10.1038/ni.3646
Lozano T, Villanueva L, Durantez M, Gorraiz M, Ruiz M, Belsue V et al (2015) Inhibition of FOXP3/NFAT Interaction enhances T cell function after TCR stimulation. J Immunol 195(7):3180–3189. https://doi.org/10.4049/jimmunol.1402997
Sekiya T, Kashiwagi I, Yoshida R, Fukaya T, Morita R, Kimura A et al (2013) Nr4a receptors are essential for thymic regulatory T cell development and immune homeostasis. Nat Immunol 14(3):230–237. https://doi.org/10.1038/ni.2520
Heninger AK, Theil A, Wilhelm C, Petzold C, Huebel N, Kretschmer K et al (2012) IL-7 abrogates suppressive activity of human CD4 + CD25 + FOXP3 + regulatory T cells and allows expansion of alloreactive and autoreactive T cells. J Immunol 189(12):5649–5658. https://doi.org/10.4049/jimmunol.1201286
Apert C, Romagnoli P, van Meerwijk JPM (2018) IL-2 and IL-15 dependent thymic development of Foxp3-expressing regulatory T lymphocytes. Protein Cell 9(4):322–332. https://doi.org/10.1007/s13238-017-0425-3
Ono M, Yaguchi H, Ohkura N, Kitabayashi I, Nagamura Y, Nomura T et al (2007) Foxp3 controls regulatory T-cell function by interacting with AML1/Runx1. Nature 446(7136):685–689. https://doi.org/10.1038/nature05673
Chi JN, Yang JY, Hsueh CH, Tsai CY, Chuang HC, Tan TH (2022) MAP4K3/GLK inhibits Treg differentiation by direct phosphorylating IKKbeta and inducing IKKbeta-mediated FoxO1 nuclear export and Foxp3 downregulation. Theranostics 12(13):5744–5760. https://doi.org/10.7150/thno.72148
Morina L, Jones ME, Oguz C, Kaplan MJ, Gangaplara A, Fitzhugh CD et al (2023) Co-expression of Foxp3 and Helios facilitates the identification of human T regulatory cells in health and disease. Front Immunol 14:1114780. https://doi.org/10.3389/fimmu.2023.1114780
Breitfeld D, Ohl L, Kremmer E, Ellwart J, Sallusto F, Lipp M et al (2000) Follicular B helper T cells express CXC chemokine receptor 5, localize to B cell follicles, and support immunoglobulin production. J Exp Med 192(11):1545–1552. https://doi.org/10.1084/jem.192.11.1545
Schaerli P, Willimann K, Lang AB, Lipp M, Loetscher P, Moser B (2000) CXC chemokine receptor 5 expression defines follicular homing T cells with B cell helper function. J Exp Med 192(11):1553–1562. https://doi.org/10.1084/jem.192.11.1553
Crotty S (2014) T follicular helper cell differentiation, function, and roles in disease. Immunity 41(4):529–542. https://doi.org/10.1016/j.immuni.2014.10.004
Baumjohann D, Preite S, Reboldi A, Ronchi F, Ansel KM, Lanzavecchia A et al (2013) Persistent antigen and germinal center B cells sustain T follicular helper cell responses and phenotype. Immunity 38(3):596–605. https://doi.org/10.1016/j.immuni.2012.11.020
Tangye SG, Ma CS, Brink R, Deenick EK (2013) The good, the bad and the ugly - TFH cells in human health and disease. Nat Rev Immunol 13(6):412–426. https://doi.org/10.1038/nri3447
Varricchi G, Harker J, Borriello F, Marone G, Durham SR, Shamji MH (2016) T follicular helper (tfh) cells in normal immune responses and in allergic disorders. Allergy 71(8):1086–1094. https://doi.org/10.1111/all.12878
Qi J, Liu C, Bai Z, Li X, Yao G (2023) T follicular helper cells and T follicular regulatory cells in autoimmune diseases. Front Immunol 14:1178792. https://doi.org/10.3389/fimmu.2023.1178792
Walker LSK (2022) The link between circulating follicular helper T cells and autoimmunity. Nat Rev Immunol 22(9):567–575. https://doi.org/10.1038/s41577-022-00693-5
Dong L, He Y, Cao Y, Wang Y, Jia A, Wang Y et al (2021) Functional differentiation and regulation of follicular T helper cells in inflammation and autoimmunity. Immunology 163(1):19–32. https://doi.org/10.1111/imm.13282
Crotty ST, Follicular Helper (2019) Cell Biology: a decade of Discovery and diseases. Immunity 50(5):1132–1148. https://doi.org/10.1016/j.immuni.2019.04.011
Vinuesa CG, Linterman MA, Yu D, MacLennan IC (2016) Follicular helper T cells. Annu Rev Immunol 34:335–368. https://doi.org/10.1146/annurev-immunol-041015-055605
Choi YS, Eto D, Yang JA, Lao C, Crotty S (2013) Cutting edge: STAT1 is required for IL-6-mediated Bcl6 induction for early follicular helper cell differentiation. J Immunol 190(7):3049–3053. https://doi.org/10.4049/jimmunol.1203032
Eto D, Lao C, DiToro D, Barnett B, Escobar TC, Kageyama R et al (2011) IL-21 and IL-6 are critical for different aspects of B cell immunity and redundantly induce optimal follicular helper CD4 T cell (tfh) differentiation. PLoS ONE 6(3):e17739. https://doi.org/10.1371/journal.pone.0017739
Powell MD, Read KA, Sreekumar BK, Jones DM, Oestreich KJ (2019) IL-12 signaling drives the differentiation and function of a T(H)1-derived T(FH1)-like cell population. Sci Rep 9(1):13991. https://doi.org/10.1038/s41598-019-50614-1
Nurieva RI, Chung Y, Hwang D, Yang XO, Kang HS, Ma L et al (2008) Generation of T follicular helper cells is mediated by interleukin-21 but independent of T helper 1, 2, or 17 cell lineages. Immunity 29(1):138–149. https://doi.org/10.1016/j.immuni.2008.05.009
Moukambi F, Rabezanahary H, Fortier Y, Rodrigues V, Clain J, Benmadid-Laktout G et al (2019) Mucosal T follicular helper cells in SIV-infected rhesus macaques: contributing role of IL-27. Mucosal Immunol 12(4):1038–1054. https://doi.org/10.1038/s41385-019-0174-0
DiToro D, Winstead CJ, Pham D, Witte S, Andargachew R, Singer JR et al (2018) Differential IL-2 expression defines developmental fates of follicular versus nonfollicular helper T cells. Science 361(6407). https://doi.org/10.1126/science.aao2933
Cai G, Nie X, Zhang W, Wu B, Lin J, Wang H et al (2012) A regulatory role for IL-10 receptor signaling in development and B cell help of T follicular helper cells in mice. J Immunol 189(3):1294–1302. https://doi.org/10.4049/jimmunol.1102948
Sage PT, Schildberg FA, Sobel RA, Kuchroo VK, Freeman GJ, Sharpe AH (2018) Dendritic cell PD-L1 limits autoimmunity and follicular T cell differentiation and function. J Immunol 200(8):2592–2602. https://doi.org/10.4049/jimmunol.1701231
Nurieva RI, Chung Y, Martinez GJ, Yang XO, Tanaka S, Matskevitch TD et al (2009) Bcl6 mediates the development of T follicular helper cells. Science 325(5943):1001–1005. https://doi.org/10.1126/science.1176676
Liu X, Yan X, Zhong B, Nurieva RI, Wang A, Wang X et al (2012) Bcl6 expression specifies the T follicular helper cell program in vivo. J Exp Med 209(10):1841–1852. https://doi.org/10.1084/jem.20120219
Ma CS, Avery DT, Chan A, Batten M, Bustamante J, Boisson-Dupuis S et al (2012) Functional STAT3 deficiency compromises the generation of human T follicular helper cells. Blood 119(17):3997–4008. https://doi.org/10.1182/blood-2011-11-392985
Weinstein JS, Laidlaw BJ, Lu Y, Wang JK, Schulz VP, Li N et al (2018) STAT4 and T-bet control follicular helper T cell development in viral infections. J Exp Med 215(1):337–355. https://doi.org/10.1084/jem.20170457
Bollig N, Brustle A, Kellner K, Ackermann W, Abass E, Raifer H et al (2012) Transcription factor IRF4 determines germinal center formation through follicular T-helper cell differentiation. Proc Natl Acad Sci U S A 109(22):8664–8669. https://doi.org/10.1073/pnas.1205834109
Betz BC, Jordan-Williams KL, Wang C, Kang SG, Liao J, Logan MR et al (2010) Batf coordinates multiple aspects of B and T cell function required for normal antibody responses. J Exp Med 207(5):933–942. https://doi.org/10.1084/jem.20091548
Xu Y, Li Y, Wang C, Han T, Liu H, Sun L et al (2023) The reciprocal interactions between microglia and T cells in Parkinson’s disease: a double-edged sword. J Neuroinflammation 20(1):33. https://doi.org/10.1186/s12974-023-02723-y
Mosley RL, Hutter-Saunders JA, Stone DK, Gendelman HE (2012) Inflammation and adaptive immunity in Parkinson’s disease. Cold Spring Harb Perspect Med 2(1):a009381. https://doi.org/10.1101/cshperspect.a009381
Al-Bachari S, Naish JH, Parker GJM, Emsley HCA, Parkes LM (2020) Blood-brain barrier leakage is increased in Parkinson’s Disease. Front Physiol 11:593026. https://doi.org/10.3389/fphys.2020.593026
Chandra G, Rangasamy SB, Roy A, Kordower JH, Pahan K (2016) Neutralization of RANTES and Eotaxin prevents the loss of dopaminergic neurons in a mouse model of Parkinson Disease. J Biol Chem 291(29):15267–15281. https://doi.org/10.1074/jbc.M116.714824
Qin XY, Zhang SP, Cao C, Loh YP, Cheng Y (2016) Aberrations in peripheral inflammatory cytokine levels in Parkinson Disease: a systematic review and Meta-analysis. JAMA Neurol 73(11):1316–1324. https://doi.org/10.1001/jamaneurol.2016.2742
Arai H, Furuya T, Mizuno Y, Mochizuki H (2006) Inflammation and infection in Parkinson’s disease. Histol Histopathol 21(6):673–678. https://doi.org/10.14670/HH-21.673
Garfias S, Tamaya Dominguez B, Toledo Rojas A, Arroyo M, Rodriguez U, Boll C et al (2022) Peripheral blood lymphocyte phenotypes in Alzheimer and Parkinson’s diseases. Neurologia (Engl Ed) 37(2):110–121. https://doi.org/10.1016/j.nrleng.2018.10.022
Saunders JA, Estes KA, Kosloski LM, Allen HE, Dempsey KM, Torres-Russotto DR et al (2012) CD4 + regulatory and effector/memory T cell subsets profile motor dysfunction in Parkinson’s disease. J Neuroimmune Pharmacol 7(4):927–938. https://doi.org/10.1007/s11481-012-9402-z
Magistrelli L, Storelli E, Rasini E, Contaldi E, Comi C, Cosentino M et al (2020) Relationship between circulating CD4 + T lymphocytes and cognitive impairment in patients with Parkinson’s disease. Brain Behav Immun 89:668–674. https://doi.org/10.1016/j.bbi.2020.07.005
Su R, Zhou T (2021) Alpha-Synuclein Induced Immune cells activation and Associated Therapy in Parkinson’s Disease. Front Aging Neurosci 13:769506. https://doi.org/10.3389/fnagi.2021.769506
Gonzalez H, Contreras F, Pacheco R (2015) Regulation of the neurodegenerative process Associated to Parkinson’s disease by CD4 + T-cells. J Neuroimmune Pharmacol 10(4):561–575. https://doi.org/10.1007/s11481-015-9618-9
Tahmasebinia F, Pourgholaminejad A (2017) The role of Th17 cells in auto-inflammatory neurological disorders. Prog Neuropsychopharmacol Biol Psychiatry 79(Pt B):408–416. https://doi.org/10.1016/j.pnpbp.2017.07.023
De Francesco E, Terzaghi M, Storelli E, Magistrelli L, Comi C, Legnaro M et al (2021) CD4 + T-cell transcription factors in idiopathic REM sleep behavior disorder and Parkinson’s Disease. Mov Disord 36(1):225–229. https://doi.org/10.1002/mds.28137
Contaldi E, Magistrelli L, Milner AV, Cosentino M, Marino F, Comi C (2021) Expression of transcription factors in CD4 + T cells as potential biomarkers of Motor complications in Parkinson’s Disease. J Parkinsons Dis 11(2):507–514. https://doi.org/10.3233/JPD-202417
Liu SY, Qiao HW, Song TB, Liu XL, Yao YX, Zhao CS et al (2022) Brain microglia activation and peripheral adaptive immunity in Parkinson’s disease: a multimodal PET study. J Neuroinflammation 19(1):209. https://doi.org/10.1186/s12974-022-02574-z
Kustrimovic N, Comi C, Magistrelli L, Rasini E, Legnaro M, Bombelli R et al (2018) Parkinson’s disease patients have a complex phenotypic and functional Th1 bias: cross-sectional studies of CD4 + Th1/Th2/T17 and Treg in drug-naive and drug-treated patients. J Neuroinflammation 15(1):205. https://doi.org/10.1186/s12974-018-1248-8
Baba Y, Kuroiwa A, Uitti RJ, Wszolek ZK, Yamada T (2005) Alterations of T-lymphocyte populations in Parkinson disease. Parkinsonism Relat Disord 11(8):493–498. https://doi.org/10.1016/j.parkreldis.2005.07.005
Yang Q, Zhuang J, Cai P, Li L, Wang R, Chen Z (2021) JKAP relates to disease risk, severity, and Th1 and Th17 differentiation in Parkinson’s disease. Ann Clin Transl Neurol 8(9):1786–1795. https://doi.org/10.1002/acn3.51420
Chen Y, Qi B, Xu W, Ma B, Li L, Chen Q et al (2015) Clinical correlation of peripheral CD4+–cell sub–sets, their imbalance and Parkinson’s disease. Mol Med Rep 12(4):6105–6111. https://doi.org/10.3892/mmr.2015.4136
Mamula D, Khosousi S, He Y, Lazarevic V, Svenningsson P (2022) Impaired migratory phenotype of CD4(+) T cells in Parkinson’s disease. NPJ Parkinsons Dis 8(1):171. https://doi.org/10.1038/s41531-022-00438-0
Barcia C, Ros CM, Annese V, Gomez A, Ros-Bernal F, Aguado-Yera D et al (2011) IFN-gamma signaling, with the synergistic contribution of TNF-alpha, mediates cell specific microglial and astroglial activation in experimental models of Parkinson’s disease. Cell Death Dis 2(4):e142. https://doi.org/10.1038/cddis.2011.17
Mount MP, Lira A, Grimes D, Smith PD, Faucher S, Slack R et al (2007) Involvement of interferon-gamma in microglial-mediated loss of dopaminergic neurons. J Neurosci 27(12):3328–3337. https://doi.org/10.1523/JNEUROSCI.5321-06.2007
Pennock ND, White JT, Cross EW, Cheney EE, Tamburini BA, Kedl RM (2013) T cell responses: naive to memory and everything in between. Adv Physiol Educ 37(4):273–283. https://doi.org/10.1152/advan.00066.2013
MacMahon Copas AN, McComish SF, Fletcher JM, Caldwell MA (2021) The pathogenesis of Parkinson’s Disease: a complex interplay between astrocytes, Microglia, and T lymphocytes? Front Neurol 12:666737. https://doi.org/10.3389/fneur.2021.666737
Bai XB, Xu S, Zhou LJ, Meng XQ, Li YL, Chen YL et al (2023) Oral pathogens exacerbate Parkinson’s disease by promoting Th1 cell infiltration in mice. Microbiome 11(1):254. https://doi.org/10.1186/s40168-023-01685-w
Reynolds AD, Stone DK, Hutter JA, Benner EJ, Mosley RL, Gendelman HE (2010) Regulatory T cells attenuate Th17 cell-mediated nigrostriatal dopaminergic neurodegeneration in a model of Parkinson’s disease. J Immunol 184(5):2261–2271. https://doi.org/10.4049/jimmunol.0901852
Benveniste EN, Merrill JE (1986) Stimulation of oligodendroglial proliferation and maturation by interleukin-2. Nature 321(6070):610–613. https://doi.org/10.1038/321610a0
Saneto RP, Altman A, Knobler RL, Johnson HM, de Vellis J (1986) Interleukin 2 mediates the inhibition of oligodendrocyte progenitor cell proliferation in vitro. Proc Natl Acad Sci U S A 83(23):9221–9225. https://doi.org/10.1073/pnas.83.23.9221
Wenzel TJ, Haskey N, Kwong E, Greuel BK, Gates EJ, Gibson DL et al (2022) Dietary fats modulate neuroinflammation in mucin 2 knock out mice model of spontaneous colitis. Biochim Biophys Acta Mol Basis Dis 1868(3):166336doi. https://doi.org/10.1016/j.bbadis.2021.166336
Zalcman SS (2002) Interleukin-2-induced increases in climbing behavior: inhibition by dopamine D-1 and D-2 receptor antagonists. Brain Res 944(1–2):157–164. https://doi.org/10.1016/s0006-8993(02)02740-3
Huang Z, Meola D, Petitto JM (2011) Loss of CNS IL-2 gene expression modifies brain T lymphocyte trafficking: response of normal versus autoreactive Treg-deficient T cells. Neurosci Lett 499(3):213–218. https://doi.org/10.1016/j.neulet.2011.05.230
Blum-Degen D, Muller T, Kuhn W, Gerlach M, Przuntek H, Riederer P (1995) Interleukin-1 beta and interleukin-6 are elevated in the cerebrospinal fluid of Alzheimer’s and de novo Parkinson’s disease patients. Neurosci Lett 202(1–2):17–20. https://doi.org/10.1016/0304-3940(95)12192-7
Wandinger KP, Hagenah JM, Kluter H, Rothermundt M, Peters M, Vieregge P (1999) Effects of amantadine treatment on in vitro production of interleukin-2 in de-novo patients with idiopathic Parkinson’s disease. J Neuroimmunol 98(2):214–220. https://doi.org/10.1016/s0165-5728(99)00093-4
Williams-Gray CH, Wijeyekoon R, Yarnall AJ, Lawson RA, Breen DP, Evans JR et al (2016) Serum immune markers and disease progression in an incident Parkinson’s disease cohort (ICICLE-PD). Mov Disord 31(7):995–1003. https://doi.org/10.1002/mds.26563
Kim R, Kim HJ, Kim A, Jang M, Kim A, Kim Y et al (2018) Peripheral blood inflammatory markers in early Parkinson’s disease. J Clin Neurosci 58:30–33. https://doi.org/10.1016/j.jocn.2018.10.079
Miliukhina IV, Usenko TS, Senkevich KA, Nikolaev MA, Timofeeva AA, Agapova EA et al (2020) Plasma cytokines Profile in patients with Parkinson’s Disease Associated with mutations in GBA Gene. Bull Exp Biol Med 168(4):423–426. https://doi.org/10.1007/s10517-020-04723-x
Moradi S, Zamani A, Mazdeh M, Ramezani M, Komaki A, Talebi-Ghane E et al (2023) An inclusive study on cytokine gene expression in Parkinson’s disease: Advanced analysis using bayesian regression model. Hum Immunol 84(2):123–129. https://doi.org/10.1016/j.humimm.2022.11.001
Schroder JB, Pawlowski M, Meyer Zu Horste G, Gross CC, Wiendl H, Meuth SG et al (2018) Immune Cell activation in the cerebrospinal fluid of patients with Parkinson’s Disease. Front Neurol 9:1081. https://doi.org/10.3389/fneur.2018.01081
Martinez-Horta S, Bejr-Kasem H, Horta-Barba A, Pascual-Sedano B, Santos-Garcia D, de Deus-Fonticoba T et al (2021) Identifying comorbidities and lifestyle factors contributing to the cognitive profile of early Parkinson’s disease. BMC Neurol 21(1):477. https://doi.org/10.1186/s12883-021-02485-1
Ho YJ, Ho SC, Pawlak CR, Yeh KY (2011) Effects of D-cycloserine on MPTP-induced behavioral and neurological changes: potential for treatment of Parkinson’s disease dementia. Behav Brain Res 219(2):280–290. https://doi.org/10.1016/j.bbr.2011.01.028
Goes ATR, Jesse CR, Antunes MS, Lobo Ladd FV, Lobo Ladd AAB, Luchese C et al (2018) Protective role of chrysin on 6-hydroxydopamine-induced neurodegeneration a mouse model of Parkinson’s disease: involvement of neuroinflammation and neurotrophins. Chem Biol Interact 279:111–120. https://doi.org/10.1016/j.cbi.2017.10.019
Antunes MS, Cattelan Souza L, Ladd FVL, Ladd A, Moreira AL, Bortolotto VC et al (2020) Hesperidin ameliorates anxiety-depressive-like Behavior in 6-OHDA model of Parkinson’s disease by regulating Striatal Cytokine and neurotrophic factors levels and dopaminergic innervation loss in the striatum of mice. Mol Neurobiol 57(7):3027–3041. https://doi.org/10.1007/s12035-020-01940-3
Zaichick S, Caraveo G, Harnessing (2023) IGF-1 and IL-2 as biomarkers for calcineurin activity to tailor optimal FK506 dosage in alpha-synucleinopathies. Front Mol Biosci 10:1292555. https://doi.org/10.3389/fmolb.2023.1292555
Park KM, Bowers WJ (2010) Tumor necrosis factor-alpha mediated signaling in neuronal homeostasis and dysfunction. Cell Signal 22(7):977–983. https://doi.org/10.1016/j.cellsig.2010.01.010
Grell M, Wajant H, Zimmermann G, Scheurich P (1998) The type 1 receptor (CD120a) is the high-affinity receptor for soluble tumor necrosis factor. Proc Natl Acad Sci U S A 95(2):570–575. https://doi.org/10.1073/pnas.95.2.570
Grell M (1995) Tumor necrosis factor (TNF) receptors in cellular signaling of soluble and membrane-expressed TNF. J Inflamm 47(1–2):8–17
Shateri S, Khatami SH, Haghbin Toutounchi A, Rajaei S, Mahdavi M, Mahmoodi Baram S et al (2023) Plasma cytokines profile in patients with Alzheimer’s and Parkinson’s Disease: a comparative study in terms of inflammation. Int J Neurosci 1–10. https://doi.org/10.1080/00207454.2023.2292951
Tang L, Chen C, Xia B, Wu W, Wei R, Zhu G et al (2020) Effect of Wenshen-Yanggan decoction on Movement Disorder and Substantia Nigra Dopaminergic Neurons in mice with chronic Parkinson’s Disease. Evid Based Complement Alternat Med 2020:9838295. https://doi.org/10.1155/2020/9838295
Iwaoka K, Otsuka C, Maeda T, Yamahara K, Kato K, Takahashi K et al (2020) Impaired metabolism of kynurenine and its metabolites in CSF of parkinson’s disease. Neurosci Lett 714:134576. https://doi.org/10.1016/j.neulet.2019.134576
Boka G, Anglade P, Wallach D, Javoy-Agid F, Agid Y, Hirsch EC (1994) Immunocytochemical analysis of tumor necrosis factor and its receptors in Parkinson’s disease. Neurosci Lett 172(1–2):151–154. https://doi.org/10.1016/0304-3940(94)90684-x
Mogi M, Harada M, Riederer P, Narabayashi H, Fujita K, Nagatsu T (1994) Tumor necrosis factor-alpha (TNF-alpha) increases both in the brain and in the cerebrospinal fluid from parkinsonian patients. Neurosci Lett 165(1–2):208–210. https://doi.org/10.1016/0304-3940(94)90746-3
Bialecka M, Klodowska-Duda G, Kurzawski M, Slawek J, Gorzkowska A, Opala G et al (2008) Interleukin-10 (IL10) and tumor necrosis factor alpha (TNF) gene polymorphisms in Parkinson’s disease patients. Parkinsonism Relat Disord 14(8):636–640. https://doi.org/10.1016/j.parkreldis.2008.02.001
Wang L, Yi H, Liang X, Xu F, Li T, Yang X et al (2023) Plasma TNF-alpha and phosphorylated alpha-syn are associated with fatigue in patients with Parkinson’s disease. J Neuroimmunol 385:578222. https://doi.org/10.1016/j.jneuroim.2023.578222
Kouchaki E, Kakhaki RD, Tamtaji OR, Dadgostar E, Behnam M, Nikoueinejad H et al (2018) Increased serum levels of TNF-alpha and decreased serum levels of IL-27 in patients with Parkinson disease and their correlation with disease severity. Clin Neurol Neurosurg 166:76–79. https://doi.org/10.1016/j.clineuro.2018.01.022
Xiromerisiou G, Marogianni C, Lampropoulos IC, Dardiotis E, Speletas M, Ntavaroukas P et al (2022) Peripheral Inflammatory Markers TNF-alpha and CCL2 Revisited: Association with Parkinson’s Disease Severity. Int J Mol Sci 24(1). https://doi.org/10.3390/ijms24010264
Carvey PM, Chen EY, Lipton JW, Tong CW, Chang QA, Ling ZD (2005) Intra-parenchymal injection of tumor necrosis factor-alpha and interleukin 1-beta produces dopamine neuron loss in the rat. J Neural Transm (Vienna) 112(5):601–612. https://doi.org/10.1007/s00702-004-0222-z
Zhao C, Ling Z, Newman MB, Bhatia A, Carvey PM (2007) TNF-alpha knockout and minocycline treatment attenuates blood-brain barrier leakage in MPTP-treated mice. Neurobiol Dis 26(1):36–46. https://doi.org/10.1016/j.nbd.2006.11.012
Chertoff M, Di Paolo N, Schoeneberg A, Depino A, Ferrari C, Wurst W et al (2011) Neuroprotective and neurodegenerative effects of the chronic expression of tumor necrosis factor alpha in the nigrostriatal dopaminergic circuit of adult mice. Exp Neurol 227(2):237–251. https://doi.org/10.1016/j.expneurol.2010.11.010
Harms AS, Barnum CJ, Ruhn KA, Varghese S, Trevino I, Blesch A et al (2011) Delayed dominant-negative TNF gene therapy halts progressive loss of nigral dopaminergic neurons in a rat model of Parkinson’s disease. Mol Ther 19(1):46–52. https://doi.org/10.1038/mt.2010.217
Sriram K, Miller DB, O’Callaghan JP (2006) Minocycline attenuates microglial activation but fails to mitigate striatal dopaminergic neurotoxicity: role of tumor necrosis factor-alpha. J Neurochem 96(3):706–718. https://doi.org/10.1111/j.1471-4159.2005.03566.x
Sriram K, Matheson JM, Benkovic SA, Miller DB, Luster MI, O’Callaghan JP (2002) Mice deficient in TNF receptors are protected against dopaminergic neurotoxicity: implications for Parkinson’s disease. FASEB J 16(11):1474–1476. https://doi.org/10.1096/fj.02-0216fje
Takeuchi H, Jin S, Wang J, Zhang G, Kawanokuchi J, Kuno R et al (2006) Tumor necrosis factor-alpha induces neurotoxicity via glutamate release from hemichannels of activated microglia in an autocrine manner. J Biol Chem 281(30):21362–21368. https://doi.org/10.1074/jbc.M600504200
Guadagno J, Xu X, Karajgikar M, Brown A, Cregan SP (2013) Microglia-derived TNFalpha induces apoptosis in neural precursor cells via transcriptional activation of the Bcl-2 family member Puma. Cell Death Dis 4(3):e538. https://doi.org/10.1038/cddis.2013.59
Doll DN, Rellick SL, Barr TL, Ren X, Simpkins JW (2015) Rapid mitochondrial dysfunction mediates TNF-alpha-induced neurotoxicity. J Neurochem 132(4):443–451. https://doi.org/10.1111/jnc.13008
Wang MX, Cheng XY, Jin M, Cao YL, Yang YP, Wang JD et al (2015) TNF compromises lysosome acidification and reduces alpha-synuclein degradation via autophagy in dopaminergic cells. Exp Neurol 271:112–121. https://doi.org/10.1016/j.expneurol.2015.05.008
Bae EJ, Choi M, Kim JT, Kim DK, Jung MK, Kim C et al (2022) TNF-alpha promotes alpha-synuclein propagation through stimulation of senescence-associated lysosomal exocytosis. Exp Mol Med 54(6):788–800. https://doi.org/10.1038/s12276-022-00789-x
Sriram K, O’Callaghan JP (2007) Divergent roles for tumor necrosis factor-alpha in the brain. J Neuroimmune Pharmacol 2(2):140–153. https://doi.org/10.1007/s11481-007-9070-6
Kann O, Almouhanna F, Chausse B (2022) Interferon gamma: a master cytokine in microglia-mediated neural network dysfunction and neurodegeneration. Trends Neurosci 45(12):913–927. https://doi.org/10.1016/j.tins.2022.10.007
Hobson BD, Stanley AT, De Los Santos MB, Culbertson B, Mosharov EV, Sims PA et al (2023) Conserved and cell type-specific transcriptional responses to IFN-gamma in the ventral midbrain. Brain Behav Immun 111:277–291. https://doi.org/10.1016/j.bbi.2023.04.008
Zhang J, He H, Qiao Y, Zhou T, He H, Yi S et al (2020) Priming of microglia with IFN-gamma impairs adult hippocampal neurogenesis and leads to depression-like behaviors and cognitive defects. Glia 68(12):2674–2692. https://doi.org/10.1002/glia.23878
Pan W, Banks WA, Kastin AJ (1997) Permeability of the blood-brain and blood-spinal cord barriers to interferons. J Neuroimmunol 76(1–2):105–111. https://doi.org/10.1016/s0165-5728(97)00034-9
Hashioka S, Klegeris A, Schwab C, McGeer PL (2009) Interferon-gamma-dependent cytotoxic activation of human astrocytes and astrocytoma cells. Neurobiol Aging 30(12):1924–1935. https://doi.org/10.1016/j.neurobiolaging.2008.02.019
Lin CH, Chen CC, Chiang HL, Liou JM, Chang CM, Lu TP et al (2019) Altered gut microbiota and inflammatory cytokine responses in patients with Parkinson’s disease. J Neuroinflammation 16(1):129. https://doi.org/10.1186/s12974-019-1528-y
Rocha NP, Assis F, Scalzo PL, Vieira ELM, Barbosa IG, de Souza MS et al (2018) Reduced activated T lymphocytes (CD4 + CD25+) and plasma levels of cytokines in Parkinson’s Disease. Mol Neurobiol 55(2):1488–1497. https://doi.org/10.1007/s12035-017-0404-y
Diaz K, Kohut ML, Russell DW, Stegemoller EL (2022) Peripheral inflammatory cytokines and motor symptoms in persons with Parkinson’s disease. Brain Behav Immun Health 21:100442. https://doi.org/10.1016/j.bbih.2022.100442
Wang N, Li R, Feng B, Cheng Y, Guo Y, Qian H (2022) Chicoric Acid Prevents Neuroinflammation and Neurodegeneration in a Mouse Parkinson’s Disease Model: Immune Response and Transcriptome Profile of the Spleen and Colon. Int J Mol Sci 23(4). https://doi.org/10.3390/ijms23042031
Chen CM, Yen CY, Chen WL, Lin CH, Wu YR, Chang KH et al (2021) Pathomechanism Characterization and Potential Therapeutics Identification for Parkinson’s Disease Targeting Neuroinflammation. Int J Mol Sci 22(3). https://doi.org/10.3390/ijms22031062
Rodriguez-Cruz A, Romo-Mancillas A, Mendiola-Precoma J, Escobar-Cabrera JE, Garcia-Alcocer G, Berumen LC (2020) Effect of valerenic acid on neuroinflammation in a MPTP-induced mouse model of Parkinson’s disease. IBRO Rep 8:28–35. https://doi.org/10.1016/j.ibror.2019.12.002
Chakrabarty P, Ceballos-Diaz C, Lin WL, Beccard A, Jansen-West K, McFarland NR et al (2011) Interferon-gamma induces progressive nigrostriatal degeneration and basal ganglia calcification. Nat Neurosci 14(6):694–696. https://doi.org/10.1038/nn.2829
Xue X, Duan R, Zheng G, Chen H, Zhang W, Shi L (2022) Translocator protein (18 kDa) regulates the microglial phenotype in Parkinson’s disease through P47. Bioengineered 13(4):11061–11071. https://doi.org/10.1080/21655979.2022.2068754
Thevenet J, Pescini Gobert R, van Hooft R, Wiessner C, Sagot YJ (2011) Regulation of LRRK2 expression points to a functional role in human monocyte maturation. PLoS ONE 6(6):e21519. https://doi.org/10.1371/journal.pone.0021519
Kuss M, Adamopoulou E, Kahle PJ (2014) Interferon-gamma induces leucine-rich repeat kinase LRRK2 via extracellular signal-regulated kinase ERK5 in macrophages. J Neurochem 129(6):980–987. https://doi.org/10.1111/jnc.12668
Panagiotakopoulou V, Ivanyuk D, De Cicco S, Haq W, Arsic A, Yu C et al (2020) Interferon-gamma signaling synergizes with LRRK2 in neurons and microglia derived from human induced pluripotent stem cells. Nat Commun 11(1):5163. https://doi.org/10.1038/s41467-020-18755-4
Rathnayake D, Chang T, Udagama P (2019) Selected serum cytokines and nitric oxide as potential multi-marker biosignature panels for Parkinson disease of varying durations: a case-control study. BMC Neurol 19(1):56. https://doi.org/10.1186/s12883-019-1286-6
Shameli A, Xiao W, Zheng Y, Shyu S, Sumodi J, Meyerson HJ et al (2016) A critical role for alpha-synuclein in development and function of T lymphocytes. Immunobiology 221(2):333–340. https://doi.org/10.1016/j.imbio.2015.10.002
Derecki NC, Cardani AN, Yang CH, Quinnies KM, Crihfield A, Lynch KR et al (2010) Regulation of learning and memory by meningeal immunity: a key role for IL-4. J Exp Med 207(5):1067–1080. https://doi.org/10.1084/jem.20091419
Kipnis J, Derecki NC, Yang C, Scrable H (2008) Immunity and cognition: what do age-related dementia, HIV-dementia and ‘chemo-brain’ have in common? Trends Immunol 29(10):455–463. https://doi.org/10.1016/j.it.2008.07.007
Brombacher TM, Nono JK, De Gouveia KS, Makena N, Darby M, Womersley J et al (2017) IL-13-Mediated regulation of learning and memory. J Immunol 198(7):2681–2688. https://doi.org/10.4049/jimmunol.1601546
Chen F, Wang Y, Chen X, Yang N, Li L (2023) Targeting interleukin 4 and interleukin 13: a novel therapeutic approach in bullous pemphigoid. Ann Med 55(1):1156–1170. https://doi.org/10.1080/07853890.2023.2188487
Chomarat P, Banchereau J (1998) Interleukin-4 and interleukin-13: their similarities and discrepancies. Int Rev Immunol 17(1–4):1–52. https://doi.org/10.3109/08830189809084486
Junttila IS (2018) Tuning the cytokine responses: an update on Interleukin (IL)-4 and IL-13 receptor complexes. Front Immunol 9:888. https://doi.org/10.3389/fimmu.2018.00888
Yang MS, Park EJ, Sohn S, Kwon HJ, Shin WH, Pyo HK et al (2002) Interleukin-13 and – 4 induce death of activated microglia. Glia 38(4):273–280. https://doi.org/10.1002/glia.10057
Kolosowska N, Keuters MH, Wojciechowski S, Keksa-Goldsteine V, Laine M, Malm T et al (2019) Peripheral Administration of IL-13 induces anti-inflammatory Microglial/Macrophage responses and provides neuroprotection in ischemic stroke. Neurotherapeutics 16(4):1304–1319. https://doi.org/10.1007/s13311-019-00761-0
Chen D, Li J, Huang Y, Wei P, Miao W, Yang Y et al (2022) Interleukin 13 promotes long-term recovery after ischemic stroke by inhibiting the activation of STAT3. J Neuroinflammation 19(1):112. https://doi.org/10.1186/s12974-022-02471-5
Yang L, Zhou R, Tong Y, Chen P, Shen Y, Miao S et al (2020) Neuroprotection by dihydrotestosterone in LPS-induced neuroinflammation. Neurobiol Dis 140:104814. https://doi.org/10.1016/j.nbd.2020.104814
Cobourne-Duval MK, Taka E, Mendonca P, Soliman KFA (2018) Thymoquinone increases the expression of neuroprotective proteins while decreasing the expression of pro-inflammatory cytokines and the gene expression NFkappaB pathway signaling targets in LPS/IFNgamma -activated BV-2 microglia cells. J Neuroimmunol 320:87–97. https://doi.org/10.1016/j.jneuroim.2018.04.018
Tripathi P, Singh A, Bala L, Patel DK, Singh MP (2018) Ibuprofen protects from Cypermethrin-Induced changes in the Striatal dendritic length and spine density. Mol Neurobiol 55(3):2333–2339. https://doi.org/10.1007/s12035-017-0491-9
Morrison BE, Marcondes MC, Nomura DK, Sanchez-Alavez M, Sanchez-Gonzalez A, Saar I et al (2012) Cutting edge: IL-13Ralpha1 expression in dopaminergic neurons contributes to their oxidative stress-mediated loss following chronic peripheral treatment with lipopolysaccharide. J Immunol 189(12):5498–5502. https://doi.org/10.4049/jimmunol.1102150
Mori S, Sugama S, Nguyen W, Michel T, Sanna MG, Sanchez-Alavez M et al (2017) Lack of interleukin-13 receptor alpha1 delays the loss of dopaminergic neurons during chronic stress. J Neuroinflammation 14(1):88. https://doi.org/10.1186/s12974-017-0862-1
Aguirre CA, Concetta Morale M, Peng Q, Sanchez-Alavez M, Cintron-Colon R, Feng K et al (2020) Two single nucleotide polymorphisms in IL13 and IL13RA1 from individuals with idiopathic Parkinson’s disease increase cellular susceptibility to oxidative stress. Brain Behav Immun 88:920–924. https://doi.org/10.1016/j.bbi.2020.04.007
Yan Z, Yang W, Wei H, Dean MN, Standaert DG, Cutter GR et al (2021) Dysregulation of the adaptive Immune System in patients with early-stage Parkinson Disease. Neurol Neuroimmunol Neuroinflamm 8(5). https://doi.org/10.1212/NXI.0000000000001036
Brodacki B, Staszewski J, Toczylowska B, Kozlowska E, Drela N, Chalimoniuk M et al (2008) Serum interleukin (IL-2, IL-10, IL-6, IL-4), TNFalpha, and INFgamma concentrations are elevated in patients with atypical and idiopathic parkinsonism. Neurosci Lett 441(2):158–162. https://doi.org/10.1016/j.neulet.2008.06.040
Li T, Yang Z, Li S, Cheng C, Shen B, Le W (2018) Alterations of NURR1 and cytokines in the peripheral blood mononuclear cells: combined biomarkers for Parkinson’s Disease. Front Aging Neurosci 10:392. https://doi.org/10.3389/fnagi.2018.00392
Alvarez-Luquin DD, Arce-Sillas A, Leyva-Hernandez J, Sevilla-Reyes E, Boll MC, Montes-Moratilla E et al (2019) Regulatory impairment in untreated Parkinson’s disease is not restricted to Tregs: other regulatory populations are also involved. J Neuroinflammation 16(1):212. https://doi.org/10.1186/s12974-019-1606-1
Moradi Vastegani S, Khoshnam SE, Mansouri E, Ghafouri S, Bakhtiari N, Farbood Y et al (2023) Anti-inflammatory, anti-apoptotic, and neuroprotective potentials of anethole in Parkinson’s disease-like motor and non-motor symptoms induced by rotenone in rats. Metab Brain Dis 38(6):2159–2174. https://doi.org/10.1007/s11011-023-01230-6
Zaidi AA, Khan MA, Shahreyar ZA, Ahmed H (2020) Lauric acid: its role in behavioral modulation, neuro-inflammatory and oxidative stress markers in haloperidol induced Parkinson’s disease. Pak J Pharm Sci 33(2Supplementary):755–763
Huhner L, Rilka J, Gilsbach R, Zhou X, Machado V, Spittau B (2017) Interleukin-4 protects dopaminergic neurons in vitro but is dispensable for MPTP-Induced Neurodegeneration in vivo. Front Mol Neurosci 10:62. https://doi.org/10.3389/fnmol.2017.00062
Spittau B (2017) Interleukin 4-induced neuroprotection and regulation of microglia activation as a therapeutic approach in the MPTP model of Parkinson’s disease. Neural Regen Res 12(9):1433–1434. https://doi.org/10.4103/1673-5374.215250
Bok E, Cho EJ, Chung ES, Shin WH, Jin BK (2018) Interleukin-4 contributes to degeneration of dopamine neurons in the Lipopolysaccharide-treated Substantia Nigra in vivo. Exp Neurobiol 27(4):309–319. https://doi.org/10.5607/en.2018.27.4.309
Yeung SS, Ho YS, Chang RC (2021) The role of meningeal populations of type II innate lymphoid cells in modulating neuroinflammation in neurodegenerative diseases. Exp Mol Med 53(9):1251–1267. https://doi.org/10.1038/s12276-021-00660-5
Farne HA, Wilson A, Milan S, Banchoff E, Yang F, Powell CV (2022) Anti-IL-5 therapies for asthma. Cochrane Database Syst Rev 7(7):CD010834. https://doi.org/10.1002/14651858.CD010834.pub4
Gevaert P, Han JK, Smith SG, Sousa AR, Howarth PH, Yancey SW et al (2022) The roles of eosinophils and interleukin-5 in the pathophysiology of chronic rhinosinusitis with nasal polyps. Int Forum Allergy Rhinol 12(11):1413–1423. https://doi.org/10.1002/alr.22994
Harish A, Schwartz SA (2020) Targeted Anti-IL-5 therapies and future therapeutics for Hypereosinophilic Syndrome and Rare Eosinophilic conditions. Clin Rev Allergy Immunol 59(2):231–247. https://doi.org/10.1007/s12016-019-08775-4
Di Lazzaro G, Picca A, Boldrini S, Bove F, Marzetti E, Petracca M et al (2024) Differential profiles of serum cytokines in Parkinson’s disease according to disease duration. Neurobiol Dis 190:106371. https://doi.org/10.1016/j.nbd.2023.106371
Hasan Kadhum Al-Huchaimi S, Hameed Neamah Al-Kefaei G, Ahmed Alameedy B (2022) Effects of Toxoplasma gondii on levels of Interleukin-5 in Parkinson’s patients. Arch Razi Inst 77(1):213–220. https://doi.org/10.22092/ARI.2021.356478.1850
Walker DG, Lue LF, Serrano G, Adler CH, Caviness JN, Sue LI et al (2015) Altered expression patterns of inflammation-Associated and Trophic molecules in Substantia Nigra and Striatum Brain samples from Parkinson’s Disease, Incidental Lewy Body Disease and Normal Control cases. Front Neurosci 9:507. https://doi.org/10.3389/fnins.2015.00507
Ringheim GE (1995) Mitogenic effects of interleukin-5 on microglia. Neurosci Lett 201(2):131–134. https://doi.org/10.1016/0304-3940(95)12153-6
Liva SM, de Vellis J (2001) IL-5 induces proliferation and activation of microglia via an unknown receptor. Neurochem Res 26(6):629–637. https://doi.org/10.1023/a:1010983119125
Chen J, Guan L, Tang L, Liu S, Zhou Y, Chen C et al (2019) T Helper 9 cells: a New Player in Immune-Related diseases. DNA Cell Biol 38(10):1040–1047. https://doi.org/10.1089/dna.2019.4729
Beriou G, Bradshaw EM, Lozano E, Costantino CM, Hastings WD, Orban T et al (2010) TGF-beta induces IL-9 production from human Th17 cells. J Immunol 185(1):46–54. https://doi.org/10.4049/jimmunol.1000356
Chaban V, Clarke GJB, Skandsen T, Islam R, Einarsen CE, Vik A et al (2020) Systemic inflammation persists the First Year after mild traumatic brain Injury: results from the prospective Trondheim mild traumatic brain Injury Study. J Neurotrauma 37(19):2120–2130. https://doi.org/10.1089/neu.2019.6963
Saresella M, Calabrese E, Marventano I, Piancone F, Gatti A, Alberoni M et al (2011) Increased activity of Th-17 and Th-9 lymphocytes and a skewing of the post-thymic differentiation pathway are seen in Alzheimer’s disease. Brain Behav Immun 25(3):539–547. https://doi.org/10.1016/j.bbi.2010.12.004
de la Monte SM, Tong M, Hapel AJ (2023) Concordant and Discordant Cerebrospinal Fluid and Plasma Cytokine and Chemokine Responses in Mild Cognitive Impairment and Early-Stage Alzheimer’s Disease. Biomedicines 11(9). https://doi.org/10.3390/biomedicines11092394
Li H, Nourbakhsh B, Cullimore M, Zhang GX, Rostami A (2011) IL-9 is important for T-cell activation and differentiation in autoimmune inflammation of the central nervous system. Eur J Immunol 41(8):2197–2206. https://doi.org/10.1002/eji.201041125
Yoshimura S, Thome R, Konno S, Mari ER, Rasouli J, Hwang D et al (2020) IL-9 controls central nervous system autoimmunity by suppressing GM-CSF production. J Immunol 204(3):531–539. https://doi.org/10.4049/jimmunol.1801113
Donninelli G, Saraf-Sinik I, Mazziotti V, Capone A, Grasso MG, Battistini L et al (2020) Interleukin-9 regulates macrophage activation in the progressive multiple sclerosis brain. J Neuroinflammation 17(1):149. https://doi.org/10.1186/s12974-020-01770-z
Elyaman W, Bradshaw EM, Uyttenhove C, Dardalhon V, Awasthi A, Imitola J et al (2009) IL-9 induces differentiation of TH17 cells and enhances function of FoxP3 + natural regulatory T cells. Proc Natl Acad Sci U S A 106(31):12885–12890. https://doi.org/10.1073/pnas.0812530106
Picca A, Guerra F, Calvani R, Marini F, Biancolillo A, Landi G et al (2020) Mitochondrial Signatures in Circulating Extracellular Vesicles of Older Adults with Parkinson’s Disease: Results from the EXosomes in PArkiNson’s Disease (EXPAND) Study. J Clin Med 9(2). https://doi.org/10.3390/jcm9020504
Storelli E, Cassina N, Rasini E, Marino F, Cosentino M (2019) Do Th17 lymphocytes and IL-17 contribute to Parkinson’s Disease? A systematic review of available evidence. Front Neurol 10:13. https://doi.org/10.3389/fneur.2019.00013
Liu Z, Huang Y, Cao BB, Qiu YH, Peng YP (2017) Th17 cells induce dopaminergic neuronal death via LFA-1/ICAM-1 Interaction in a mouse model of Parkinson’s Disease. Mol Neurobiol 54(10):7762–7776. https://doi.org/10.1007/s12035-016-0249-9
Liu Z, Qiu AW, Huang Y, Yang Y, Chen JN, Gu TT et al (2019) IL-17A exacerbates neuroinflammation and neurodegeneration by activating microglia in rodent models of Parkinson’s disease. Brain Behav Immun 81:630–645. https://doi.org/10.1016/j.bbi.2019.07.026
Sommer A, Marxreiter F, Krach F, Fadler T, Grosch J, Maroni M et al (2018) Th17 lymphocytes induce neuronal cell death in a human iPSC-Based model of Parkinson’s Disease. Cell Stem Cell 23(1):123–31e6. https://doi.org/10.1016/j.stem.2018.06.015
Huangfu L, Li R, Huang Y, Wang S (2023) The IL-17 family in diseases: from bench to bedside. Signal Transduct Target Ther 8(1):402. https://doi.org/10.1038/s41392-023-01620-3
McGeachy MJ, Cua DJ, Gaffen SL (2019) The IL-17 family of cytokines in Health and Disease. Immunity 50(4):892–906. https://doi.org/10.1016/j.immuni.2019.03.021
Sun J, Zhang S, Zhang X, Zhang X, Dong H, Qian Y (2015) IL-17A is implicated in lipopolysaccharide-induced neuroinflammation and cognitive impairment in aged rats via microglial activation. J Neuroinflammation 12:165. https://doi.org/10.1186/s12974-015-0394-5
Liu S, Song X, Chrunyk BA, Shanker S, Hoth LR, Marr ES et al (2013) Crystal structures of interleukin 17A and its complex with IL-17 receptor A. Nat Commun 4:1888. https://doi.org/10.1038/ncomms2880
Yeremenko N (2021) Out of the shadow of interleukin-17A: the role of interleukin-17F and other interleukin-17 family cytokines in spondyloarthritis. Curr Opin Rheumatol 33(4):333–340. https://doi.org/10.1097/BOR.0000000000000805
Kebir H, Kreymborg K, Ifergan I, Dodelet-Devillers A, Cayrol R, Bernard M et al (2007) Human TH17 lymphocytes promote blood-brain barrier disruption and central nervous system inflammation. Nat Med 13(10):1173–1175. https://doi.org/10.1038/nm1651
Mohamed YT, Salama A, Rabie MA, Abd El Fattah MA (2023) Neuroprotective effect of secukinumab against rotenone induced Parkinson’s disease in rat model: involvement of IL-17, HMGB-1/TLR4 axis and BDNF/TrKB cascade. Int Immunopharmacol 114:109571. https://doi.org/10.1016/j.intimp.2022.109571
Gate D, Tapp E, Leventhal O, Shahid M, Nonninger TJ, Yang AC et al (2021) CD4(+) T cells contribute to neurodegeneration in Lewy body dementia. Science 374(6569):868–874. https://doi.org/10.1126/science.abf7266
Zhao X, Li L, Ma X, Li Y, Gao B, Luo W (2024) The role of immune and inflammatory-related indicators in cognitive dysfunction and disease severity in patients with parkinson’s disease. J Neural Transm (Vienna) 131(1):13–24. https://doi.org/10.1007/s00702-023-02704-8
Green HF, Khosousi S, Svenningsson P, Plasma (2019) IL-6 and IL-17A correlate with severity of motor and non-motor symptoms in Parkinson’s Disease. J Parkinsons Dis 9(4):705–709. https://doi.org/10.3233/JPD-191699
Korn T, Bettelli E, Oukka M, Kuchroo VK (2009) IL-17 and Th17 cells. Annu Rev Immunol 27:485–517. https://doi.org/10.1146/annurev.immunol.021908.132710
Kumar P, Monin L, Castillo P, Elsegeiny W, Horne W, Eddens T et al (2016) Intestinal Interleukin-17 receptor signaling mediates reciprocal control of the gut microbiota and autoimmune inflammation. Immunity 44(3):659–671. https://doi.org/10.1016/j.immuni.2016.02.007
Ivanov II, Atarashi K, Manel N, Brodie EL, Shima T, Karaoz U et al (2009) Induction of intestinal Th17 cells by segmented filamentous bacteria. Cell 139(3):485–498. https://doi.org/10.1016/j.cell.2009.09.033
Elsaesser H, Sauer K, Brooks DG (2009) IL-21 is required to control chronic viral infection. Science 324(5934):1569–1572. https://doi.org/10.1126/science.1174182
Yi JS, Du M, Zajac AJ (2009) A vital role for interleukin-21 in the control of a chronic viral infection. Science 324(5934):1572–1576. https://doi.org/10.1126/science.1175194
Schmitz I, Schneider C, Frohlich A, Frebel H, Christ D, Leonard WJ et al (2013) IL-21 restricts virus-driven Treg cell expansion in chronic LCMV infection. PLoS Pathog 9(5):e1003362. https://doi.org/10.1371/journal.ppat.1003362
Hu Z, Zuo C, Mao C, Shi C, Xu Y (2023) Peripheral immune markers and amyotrophic lateral sclerosis: a mendelian randomization study. Front Neurosci 17:1269354. https://doi.org/10.3389/fnins.2023.1269354
Agrawal S, Baulch JE, Madan S, Salah S, Cheeks SN, Krattli RP Jr. et al (2022) Impact of IL-21-associated peripheral and brain crosstalk on the Alzheimer’s disease neuropathology. Cell Mol Life Sci 79(6):331. https://doi.org/10.1007/s00018-022-04347-6
Mossner S, Kuchner M, Fazel Modares N, Knebel B, Al-Hasani H, Floss DM et al (2020) Synthetic interleukin 22 (IL-22) signaling reveals biological activity of homodimeric IL-10 receptor 2 and functional cross-talk with the IL-6 receptor gp130. J Biol Chem 295(35):12378–12397. https://doi.org/10.1074/jbc.RA120.013927
Sabat R, Ouyang W, Wolk K (2014) Therapeutic opportunities of the IL-22-IL-22R1 system. Nat Rev Drug Discov 13(1):21–38. https://doi.org/10.1038/nrd4176
Zindl CL, Lai JF, Lee YK, Maynard CL, Harbour SN, Ouyang W et al (2013) IL-22-producing neutrophils contribute to antimicrobial defense and restitution of colonic epithelial integrity during colitis. Proc Natl Acad Sci U S A 110(31):12768–12773. https://doi.org/10.1073/pnas.1300318110
Zheng Y, Danilenko DM, Valdez P, Kasman I, Eastham-Anderson J, Wu J et al (2007) Interleukin-22, a T(H)17 cytokine, mediates IL-23-induced dermal inflammation and acanthosis. Nature 445(7128):648–651. https://doi.org/10.1038/nature05505
Yoon CH, Lee D, Jeong HJ, Ryu JS, Kim MK (2018) Distribution of Interleukin-22-secreting Immune cells in Conjunctival Associated Lymphoid tissue. Korean J Ophthalmol 32(2):147–153. https://doi.org/10.3341/kjo.2017.0068
Perriard G, Mathias A, Enz L, Canales M, Schluep M, Gentner M et al (2015) Interleukin-22 is increased in multiple sclerosis patients and targets astrocytes. J Neuroinflammation 12:119. https://doi.org/10.1186/s12974-015-0335-3
Chen W, Wang J, Yang H, Sun Y, Chen B, Liu Y et al (2022) Interleukin 22 and its association with neurodegenerative disease activity. Front Pharmacol 13:958022. https://doi.org/10.3389/fphar.2022.958022
Liu X, Liu S, Tang Y, Pu Z, Xiao H, Gao J et al (2021) Intragastric Administration of Casein Leads to Nigrostriatal Disease progressed accompanied with persistent nigrostriatal-intestinal inflammation Activited and Intestinal Microbiota-Metabolic disorders Induced in MPTP Mouse Model of Parkinson’s Disease. Neurochem Res 46(6):1514–1539. https://doi.org/10.1007/s11064-021-03293-2
Huang Y, Liu Z, Wang XQ, Qiu YH, Peng YP (2014) A dysfunction of CD4 + T lymphocytes in peripheral immune system of Parkinson’s disease model mice. Zhongguo Ying Yong Sheng Li Xue Za Zhi 30(6):567–576
Zhang J, Ke KF, Liu Z, Qiu YH, Peng YP (2013) Th17 cell-mediated neuroinflammation is involved in neurodegeneration of abeta1-42-induced Alzheimer’s disease model rats. PLoS ONE 8(10):e75786. https://doi.org/10.1371/journal.pone.0075786
Ponath G, Park C, Pitt D (2018) The role of astrocytes in multiple sclerosis. Front Immunol 9:217doi. https://doi.org/10.3389/fimmu.2018.00217
Lee D, Jo H, Go C, Jang Y, Chu N, Bae S et al (2022) The roles of IL-22 and its receptor in the regulation of inflammatory responses in the brain. Int J Mol Sci 23(2). https://doi.org/10.3390/ijms23020757
Gao Z, Tan H, Song X, Zhuang T, Kong R, Wang Y et al (2024) Troxerutin dampened hypothalamic neuroinflammation via microglial IL-22/IL-22R1/IRF3 activation in dihydrotestosterone-induced polycystic ovary syndrome rats. Phytomedicine 124:155280. https://doi.org/10.1016/j.phymed.2023.155280
Li J, Zhao J, Chen L, Gao H, Zhang J, Wang D et al (2023) Alpha-synuclein induces Th17 differentiation and impairs the function and stability of Tregs by promoting RORC transcription in Parkinson’s disease. Brain Behav Immun 108:32–44. https://doi.org/10.1016/j.bbi.2022.10.023
Thome AD, Atassi F, Wang J, Faridar A, Zhao W, Thonhoff JR et al (2021) Ex vivo expansion of dysfunctional regulatory T lymphocytes restores suppressive function in Parkinson’s disease. NPJ Parkinsons Dis 7(1):41. https://doi.org/10.1038/s41531-021-00188-5
Reynolds AD, Banerjee R, Liu J, Gendelman HE, Mosley RL (2007) Neuroprotective activities of CD4 + CD25 + regulatory T cells in an animal model of Parkinson’s disease. J Leukoc Biol 82(5):1083–1094. https://doi.org/10.1189/jlb.0507296
Liu J, Gong N, Huang X, Reynolds AD, Mosley RL, Gendelman HE (2009) Neuromodulatory activities of CD4 + CD25 + regulatory T cells in a murine model of HIV-1-associated neurodegeneration. J Immunol 182(6):3855–3865. https://doi.org/10.4049/jimmunol.0803330
Reynolds AD, Stone DK, Mosley RL, Gendelman HE (2009) Nitrated alpha-synuclein-induced alterations in microglial immunity are regulated by CD4 + T cell subsets. J Immunol 182(7):4137–4149. https://doi.org/10.4049/jimmunol.0803982
Liesz A, Suri-Payer E, Veltkamp C, Doerr H, Sommer C, Rivest S et al (2009) Regulatory T cells are key cerebroprotective immunomodulators in acute experimental stroke. Nat Med 15(2):192–199. https://doi.org/10.1038/nm.1927
Rostami J, Fotaki G, Sirois J, Mzezewa R, Bergstrom J, Essand M et al (2020) Astrocytes have the capacity to act as antigen-presenting cells in the Parkinson’s disease brain. J Neuroinflammation 17(1):119. https://doi.org/10.1186/s12974-020-01776-7
Huang Y, Liu Z, Cao BB, Qiu YH, Peng YP (2017) Treg Cells Protect Dopaminergic Neurons against MPP + neurotoxicity via CD47-SIRPA Interaction. Cell Physiol Biochem 41(3):1240–1254. https://doi.org/10.1159/000464388
Huang Y, Liu Z, Cao BB, Qiu YH, Peng YP (2020) Treg Cells Attenuate Neuroinflammation and protect neurons in a mouse model of Parkinson’s Disease. J Neuroimmune Pharmacol 15(2):224–237. https://doi.org/10.1007/s11481-019-09888-5
Mollazadeh H, Cicero AFG, Blesso CN, Pirro M, Majeed M, Sahebkar A (2019) Immune modulation by curcumin: the role of interleukin-10. Crit Rev Food Sci Nutr 59(1):89–101. https://doi.org/10.1080/10408398.2017.1358139
Porro C, Cianciulli A, Panaro MA (2020) The Regulatory Role of IL-10 in neurodegenerative diseases. Biomolecules 10(7). https://doi.org/10.3390/biom10071017
Karpenko MN, Vasilishina AA, Gromova EA, Muruzheva ZM, Miliukhina IV, Bernadotte A (2018) Interleukin-1beta, interleukin-1 receptor antagonist, interleukin-6, interleukin-10, and tumor necrosis factor-alpha levels in CSF and serum in relation to the clinical diversity of Parkinson’s disease. Cell Immunol 327:77–82. https://doi.org/10.1016/j.cellimm.2018.02.011
Li D, Song X, Huang H, Huang H, Ye Z (2018) Association of Parkinson’s disease-related pain with plasma interleukin-1, interleukin-6, interleukin-10, and tumour necrosis factor-alpha. Neurosci Lett 683:181–184. https://doi.org/10.1016/j.neulet.2018.07.027
Haiyang WU, Ying W, Wei H, Huihui LI, Haisheng JI, Xiuxiu L (2023) Protective effect of Tongdu Tiaoshen acupuncture combined with xiaoxuming decoction on dopaminergic neurons in Parkinson’s disease model. J Tradit Chin Med 43(3):484–493. https://doi.org/10.19852/j.cnki.jtcm.20230214.005
Pan T, Xiao Q, Fan HJ, Xu L, Qin SC, Yang LX et al (2023) Wuzi Yanzong Pill relieves MPTP-induced motor dysfunction and neuron loss by inhibiting NLRP3 inflammasome-mediated neuroinflammation. Metab Brain Dis 38(7):2211–2222. https://doi.org/10.1007/s11011-023-01266-8
Johnston LC, Su X, Maguire-Zeiss K, Horovitz K, Ankoudinova I, Guschin D et al (2008) Human interleukin-10 gene transfer is protective in a rat model of Parkinson’s disease. Mol Ther 16(8):1392–1399. https://doi.org/10.1038/mt.2008.113
Schwenkgrub J, Joniec-Maciejak I, Sznejder-Pacholek A, Wawer A, Ciesielska A, Bankiewicz K et al (2013) Effect of human interleukin-10 on the expression of nitric oxide synthases in the MPTP-based model of Parkinson’s disease. Pharmacol Rep 65(1):44–49. https://doi.org/10.1016/s1734-1140(13)70962-9
Joniec-Maciejak I, Ciesielska A, Wawer A, Sznejder-Pacholek A, Schwenkgrub J, Cudna A et al (2014) The influence of AAV2-mediated gene transfer of human IL-10 on neurodegeneration and immune response in a murine model of Parkinson’s disease. Pharmacol Rep 66(4):660–669. https://doi.org/10.1016/j.pharep.2014.03.008
Zhu Y, Chen X, Liu Z, Peng YP, Qiu YH (2015) Interleukin-10 protection against Lipopolysaccharide-Induced neuro-inflammation and neurotoxicity in ventral mesencephalic cultures. Int J Mol Sci 17(1). https://doi.org/10.3390/ijms17010025
Zhu Y, Liu Z, Peng YP, Qiu YH (2017) Interleukin-10 inhibits neuroinflammation-mediated apoptosis of ventral mesencephalic neurons via JAK-STAT3 pathway. Int Immunopharmacol 50:353–360. https://doi.org/10.1016/j.intimp.2017.07.017
Gao Y, Tu D, Yang R, Chu CH, Hong JS, Gao HM, Through Reducing ROS, Production (2020) IL-10 suppresses Caspase-1-Dependent IL-1beta maturation, thereby preventing chronic neuroinflammation and neurodegeneration. Int J Mol Sci 21(2). https://doi.org/10.3390/ijms21020465
Yang S, Gao L, Lu F, Wang B, Gao F, Zhu G et al (2015) Transcription factor myocyte enhancer factor 2D regulates interleukin-10 production in microglia to protect neuronal cells from inflammation-induced death. J Neuroinflammation 12:33. https://doi.org/10.1186/s12974-015-0258-z
Cockey SG, McFarland KN, Koller EJ, Brooks MMT, De La Cruz G, Cruz E (2021) Il-10 signaling reduces survival in mouse models of synucleinopathy. NPJ Parkinsons Dis 7(1):30. https://doi.org/10.1038/s41531-021-00169-8
Collison LW, Workman CJ, Kuo TT, Boyd K, Wang Y, Vignali KM et al (2007) The inhibitory cytokine IL-35 contributes to regulatory T-cell function. Nature 450(7169):566–569. https://doi.org/10.1038/nature06306
Shen P, Roch T, Lampropoulou V, O’Connor RA, Stervbo U, Hilgenberg E et al (2014) IL-35-producing B cells are critical regulators of immunity during autoimmune and infectious diseases. Nature 507(7492):366–370. https://doi.org/10.1038/nature12979
Su LC, Liu XY, Huang AF, Xu WD (2018) Emerging role of IL-35 in inflammatory autoimmune diseases. Autoimmun Rev 17(7):665–673. https://doi.org/10.1016/j.autrev.2018.01.017
Duffy SS, Keating BA, Perera CJ, Lees JG, Tonkin RS, Makker PGS et al (2019) Regulatory T cells and their derived cytokine, Interleukin-35, reduce Pain in Experimental Autoimmune Encephalomyelitis. J Neurosci 39(12):2326–2346. https://doi.org/10.1523/JNEUROSCI.1815-18.2019
Fu J, Duan J, Mo J, Xiao H, Huang Y, Chen W et al (2020) Mild cognitive impairment patients have higher Regulatory T-Cell proportions compared with Alzheimer’s Disease-related dementia patients. Front Aging Neurosci 12:624304. https://doi.org/10.3389/fnagi.2020.624304
Lin B, Li Y, Jiang N, Huang S, Su W, Zhuo Y (2022) Interleukin-35 suppresses pyroptosis and protects against neuronal death in retinal ischaemia/reperfusion injury. Exp Eye Res 220:109109. https://doi.org/10.1016/j.exer.2022.109109
Luo F, Huang Y, Li Y, Zhao X, Xie Y, Zhang Q et al (2021) A narrative review of the relationship between TGF-beta signaling and gynecological malignant tumor. Ann Transl Med 9(20):1601. https://doi.org/10.21037/atm-21-4879
Roussa E, Wiehle M, Dunker N, Becker-Katins S, Oehlke O, Krieglstein K (2006) Transforming growth factor beta is required for differentiation of mouse mesencephalic progenitors into dopaminergic neurons in vitro and in vivo: ectopic induction in dorsal mesencephalon. Stem Cells 24(9):2120–2129. https://doi.org/10.1634/stemcells.2005-0514
Tesseur I, Nguyen A, Chang B, Li L, Woodling NS, Wyss-Coray T et al (2017) Deficiency in neuronal TGF-beta signaling leads to Nigrostriatal Degeneration and activation of TGF-beta signaling protects against MPTP Neurotoxicity in mice. J Neurosci 37(17):4584–4592. https://doi.org/10.1523/JNEUROSCI.2952-16.2017
Yi JJ, Barnes AP, Hand R, Polleux F, Ehlers MD (2010) TGF-beta signaling specifies axons during brain development. Cell 142(1):144–157. https://doi.org/10.1016/j.cell.2010.06.010
Roussa E, Farkas LM, Krieglstein K (2004) TGF-beta promotes survival on mesencephalic dopaminergic neurons in cooperation with shh and FGF-8. Neurobiol Dis 16(2):300–310. https://doi.org/10.1016/j.nbd.2004.03.006
Krieglstein K, Richter S, Farkas L, Schuster N, Dunker N, Oppenheim RW et al (2000) Reduction of endogenous transforming growth factors beta prevents ontogenetic neuron death. Nat Neurosci 3(11):1085–1090. https://doi.org/10.1038/80598
Brionne TC, Tesseur I, Masliah E, Wyss-Coray T (2003) Loss of TGF-beta 1 leads to increased neuronal cell death and microgliosis in mouse brain. Neuron 40(6):1133–1145. https://doi.org/10.1016/s0896-6273(03)00766-9
Zhou X, Zoller T, Krieglstein K, Spittau B (2015) TGFbeta1 inhibits IFNgamma-mediated microglia activation and protects mDA neurons from IFNgamma-driven neurotoxicity. J Neurochem 134(1):125–134. https://doi.org/10.1111/jnc.13111
Luo J (2022) TGF-beta as a key modulator of astrocyte reactivity: Disease Relevance and therapeutic implications. Biomedicines 10(5). https://doi.org/10.3390/biomedicines10051206
Sibuea S, Ho JK, Pouton CW, Haynes JM (2023) TGFbeta3, dibutyryl cAMP and a notch inhibitor modulate phenotype late in stem cell-derived dopaminergic neuron maturation. Front Cell Dev Biol 11:1111705. https://doi.org/10.3389/fcell.2023.1111705
Khedr EM, Gomaa AMS, Ahmed OG, Sayed HMM, Gamea A, Cognitive Impairment (2020) P300, and transforming growth factor beta1 in different forms of Dementia. J Alzheimers Dis 78(2):837–845. https://doi.org/10.3233/JAD-200885
Chen X, Hu Y, Cao Z, Liu Q, Cheng Y (2018) Cerebrospinal fluid inflammatory cytokine aberrations in Alzheimer’s Disease, Parkinson’s disease and amyotrophic lateral sclerosis: a systematic review and Meta-analysis. Front Immunol 9:2122. https://doi.org/10.3389/fimmu.2018.02122
Devi L, Raghavendran V, Prabhu BM, Avadhani NG, Anandatheerthavarada HK (2008) Mitochondrial import and accumulation of alpha-synuclein impair complex I in human dopaminergic neuronal cultures and Parkinson disease brain. J Biol Chem 283(14):9089–9100. https://doi.org/10.1074/jbc.M710012200
Diniz LP, Matias I, Araujo APB, Garcia MN, Barros-Aragao FGQ, Alves-Leon SV et al (2019) Alpha-synuclein oligomers enhance astrocyte-induced synapse formation through TGF-beta1 signaling in a Parkinson’s disease model. J Neurochem 150(2):138–157. https://doi.org/10.1111/jnc.14710
Liu Z, Chen HQ, Huang Y, Qiu YH, Peng YP (2016) Transforming growth factor-beta1 acts via TbetaR-I on microglia to protect against MPP(+)-induced dopaminergic neuronal loss. Brain Behav Immun 51:131–143. https://doi.org/10.1016/j.bbi.2015.08.006
Chen X, Liu Z, Cao BB, Qiu YH, Peng YP (2017) TGF-beta1 neuroprotection via inhibition of Microglial activation in a rat model of Parkinson’s Disease. J Neuroimmune Pharmacol 12(3):433–446. https://doi.org/10.1007/s11481-017-9732-y
Martinez-Canabal A, Wheeler AL, Sarkis D, Lerch JP, Lu WY, Buckwalter MS et al (2013) Chronic over-expression of TGFbeta1 alters hippocampal structure and causes learning deficits. Hippocampus 23(12):1198–1211. https://doi.org/10.1002/hipo.22159
Stayte S, Rentsch P, Troscher AR, Bamberger M, Li KM, Vissel B (2017) Activin A inhibits MPTP and LPS-Induced increases in inflammatory cell populations and loss of dopamine neurons in the mouse midbrain in vivo. PLoS ONE 12(1):e0167211. https://doi.org/10.1371/journal.pone.0167211
Jiang WW, Zhang ZZ, He PP, Jiang LP, Chen JZ, Zhang XT et al (2021) Emerging roles of growth differentiation factor-15 in brain disorders (review). Exp Ther Med 22(5):1270. https://doi.org/10.3892/etm.2021.10705
Goulding SR, Sullivan AM, O’Keeffe GW, Collins LM (2020) The potential of bone morphogenetic protein 2 as a neurotrophic factor for Parkinson’s disease. Neural Regen Res 15(8):1432–1436. https://doi.org/10.4103/1673-5374.274327
Zhao X, Jin T, Zheng C, Ma D, Zhang Y (2020) Imbalance of circulating Tfh/Tfr cells in patients with Parkinson’s Disease. Front Neurol 11:572205. https://doi.org/10.3389/fneur.2020.572205
Li R, Tropea TF, Baratta LR, Zuroff L, Diaz-Ortiz ME, Zhang B et al (2022) Abnormal B-Cell and tfh-cell profiles in patients with Parkinson Disease: a cross-sectional study. Neurol Neuroimmunol Neuroinflamm 9(2). https://doi.org/10.1212/NXI.0000000000001125
Tambasco N, Romoli M, Calabresi P (2018) Levodopa in Parkinson’s Disease: current status and future developments. Curr Neuropharmacol 16(8):1239–1252. https://doi.org/10.2174/1570159X15666170510143821
Dadsetan S, Balzano T, Forteza J, Agusti A, Cabrera-Pastor A, Taoro-Gonzalez L et al (2016) Infliximab reduces peripheral inflammation, neuroinflammation, and extracellular GABA in the cerebellum and improves learning and motor coordination in rats with hepatic encephalopathy. J Neuroinflammation 13(1):245. https://doi.org/10.1186/s12974-016-0710-8
Xu JJ, Guo S, Xue R, Xiao L, Kou JN, Liu YQ et al (2021) Adalimumab ameliorates memory impairments and neuroinflammation in chronic cerebral hypoperfusion rats. Aging 13(10):14001–14014. https://doi.org/10.18632/aging.203009
Dhillon S (2014) Certolizumab pegol: a review of its use in patients with axial spondyloarthritis or psoriatic arthritis. Drugs 74(9):999–1016. https://doi.org/10.1007/s40265-014-0239-z
Pavitrakar V, Mody R, Ravindran S (2022) Amelioration of cisplatin-induced renal inflammation by recombinant human golimumab in mice. Curr Pharm Biotechnol 23(7):970–977. https://doi.org/10.2174/1389201022666210810141139
Peter I, Dubinsky M, Bressman S, Park A, Lu C, Chen N et al (2018) Anti-tumor Necrosis factor therapy and incidence of Parkinson Disease among patients with inflammatory bowel disease. JAMA Neurol 75(8):939–946. https://doi.org/10.1001/jamaneurol.2018.0605
Zhou H (2005) Clinical pharmacokinetics of etanercept: a fully humanized soluble recombinant tumor necrosis factor receptor fusion protein. J Clin Pharmacol 45(5):490–497. https://doi.org/10.1177/0091270004273321
Zhao S, Mysler E, Moots RJ (2018) Etanercept for the treatment of rheumatoid arthritis. Immunotherapy 10(6):433–445. https://doi.org/10.2217/imt-2017-0155
Sanchez Carazo JL, Mahiques Santos L, Oliver Martinez V (2006) Safety of etanercept in psoriasis: a critical review. Drug Saf 29(8):675–685. https://doi.org/10.2165/00002018-200629080-00004
Puig L, Lopez-Ferrer A, Laiz A (2015) Etanercept in the treatment of psoriatic arthritis. Actas Dermosifiliogr 106(4):252–259. https://doi.org/10.1016/j.ad.2014.09.004
Senabre-Gallego JM, Santos-Ramirez C, Santos-Soler G, Salas-Heredia E, Sanchez-Barrioluengo M, Barber X et al (2013) Long-term safety and efficacy of etanercept in the treatment of ankylosing spondylitis. Patient Prefer Adherence 7:961–972. https://doi.org/10.2147/PPA.S33109
Shin SH, Kim EK, Lee KY, Kim HS (2019) TNF-alpha antagonist attenuates systemic lipopolysaccharide-induced brain white matter injury in neonatal rats. BMC Neurosci 20(1):45. https://doi.org/10.1186/s12868-019-0529-1
Cvetkovic RS, Keating G, Anakinra (2002) BioDrugs 16(4):303–311 discussion 13 – 4. https://doi.org/10.2165/00063030-200216040-00005
Larsen CM, Faulenbach M, Vaag A, Volund A, Ehses JA, Seifert B et al (2007) Interleukin-1-receptor antagonist in type 2 diabetes mellitus. N Engl J Med 356(15):1517–1526. https://doi.org/10.1056/NEJMoa065213
Nguyen T, Dima L, Willett KC (2023) Anakinra-An Interleukin-1 receptor antagonist for COVID-19. Am J Ther 30(2):e108–e16. https://doi.org/10.1097/MJT.0000000000001603
Parry-Jones AR, Stocking K, MacLeod MJ, Clarke B, Werring DJ, Muir KW et al (2023) Phase II randomised, placebo-controlled, clinical trial of interleukin-1 receptor antagonist in intracerebral haemorrhage: BLOcking the cytokine IL-1 in ICH (BLOC-ICH). Eur Stroke J 8(3):819–827. https://doi.org/10.1177/23969873231185208
Saag KG, Khanna PP, Keenan RT, Ohlman S, Osterling Koskinen L, Sparve E et al (2021) A randomized, phase II study evaluating the efficacy and safety of Anakinra in the treatment of gout flares. Arthritis Rheumatol 73(8):1533–1542. https://doi.org/10.1002/art.41699
Abbate A, Trankle CR, Buckley LF, Lipinski MJ, Appleton D, Kadariya D et al (2020) Interleukin-1 blockade inhibits the Acute Inflammatory response in patients with ST-Segment-Elevation myocardial infarction. J Am Heart Assoc 9(5):e014941. https://doi.org/10.1161/JAHA.119.014941
Koprich JB, Reske-Nielsen C, Mithal P, Isacson O (2008) Neuroinflammation mediated by IL-1beta increases susceptibility of dopamine neurons to degeneration in an animal model of Parkinson’s disease. J Neuroinflammation 5:8. https://doi.org/10.1186/1742-2094-5-8
Atzeni F, Carriero A, Boccassini L, D’Angelo S, Anti (2021) -IL-17 agents in the treatment of Axial Spondyloarthritis. Immunotargets Ther 10:141–153. https://doi.org/10.2147/ITT.S259126
Braun J, Baraliakos X, Kiltz U (2016) Secukinumab (AIN457) in the treatment of ankylosing spondylitis. Expert Opin Biol Ther 16(5):711–722. https://doi.org/10.1517/14712598.2016.1167183
Park TY, Jeon J, Lee N, Kim J, Song B, Kim JH et al (2023) Co-transplantation of autologous T(reg) cells in a cell therapy for Parkinson’s disease. Nature 619(7970):606–615. https://doi.org/10.1038/s41586-023-06300-4
Bhattacharya P, Budnick I, Singh M, Thiruppathi M, Alharshawi K, Elshabrawy H et al (2015) Dual role of GM-CSF as a pro-inflammatory and a Regulatory Cytokine: implications for Immune Therapy. J Interferon Cytokine Res 35(8):585–599. https://doi.org/10.1089/jir.2014.0149
Gendelman HE, Zhang Y, Santamaria P, Olson KE, Schutt CR, Bhatti D et al (2017) Evaluation of the safety and immunomodulatory effects of sargramostim in a randomized, double-blind phase 1 clinical Parkinson’s disease trial. NPJ Parkinsons Dis 3:10doi. https://doi.org/10.1038/s41531-017-0013-5
Olson KE, Bade AN, Schutt CR, Dong J, Shandler SJ, Boska MD et al (2016) Manganese-Enhanced Magnetic Resonance Imaging for Detection of Vasoactive Intestinal Peptide Receptor 2 agonist therapy in a model of Parkinson’s Disease. Neurotherapeutics 13(3):635–646. https://doi.org/10.1007/s13311-016-0449-z
Mosley RL, Lu Y, Olson KE, Machhi J, Yan W, Namminga KL et al (2019) A synthetic agonist to Vasoactive Intestinal Peptide Receptor-2 induces Regulatory T Cell neuroprotective activities in models of Parkinson’s Disease. Front Cell Neurosci 13:421. https://doi.org/10.3389/fncel.2019.00421
Chen CN, Hajji N, Yeh FC, Rahman S, Ali S, Wharton J et al (2023) Restoration of Foxp3(+) Regulatory T cells by HDAC-Dependent epigenetic modulation plays a pivotal role in resolving pulmonary arterial hypertension Pathology. Am J Respir Crit Care Med 208(8):879–895. https://doi.org/10.1164/rccm.202301-0181OC
Jang YS, Park SH, Kang SG, Lee JS, Ko HJ, Kim PH (2023) Combined Treatment with TGF-beta1, retinoic acid, and Lactoferrin robustly generate Inducible Tregs (iTregs) Against High Affinity ligand. Immune Netw 23(5):e37. https://doi.org/10.4110/in.2023.23.e37
Alrouji M, Al-Kuraishy HM, Al-Gareeb AI, Saad HM, Batiha GE (2023) A story of the potential effect of non-steroidal anti-inflammatory drugs (NSAIDs) in Parkinson’s disease: beneficial or detrimental effects. Inflammopharmacology 31(2):673–688. https://doi.org/10.1007/s10787-023-01192-2
Chen P, Zhang J, Wang C, Chai YH, Wu AG, Huang NY et al (2022) The pathogenesis and treatment mechanism of Parkinson’s disease from the perspective of traditional Chinese medicine. Phytomedicine 100:154044. https://doi.org/10.1016/j.phymed.2022.154044
Mirzaei H, Sedighi S, Kouchaki E, Barati E, Dadgostar E, Aschner M et al (2022) Probiotics and the treatment of Parkinson’s Disease: an update. Cell Mol Neurobiol 42(8):2449–2457. https://doi.org/10.1007/s10571-021-01128-w
Pignolo A, Mastrilli S, Davi C, Arnao V, Aridon P, Dos Santos Mendes FA et al (2022) Vitamin D and Parkinson’s Disease. Nutrients 14(6). https://doi.org/10.3390/nu14061220
Ni R, Yuan Y, Yang L, Meng Q, Zhu Y, Zhong Y et al (2022) Novel non-invasive transcranial electrical stimulation for Parkinson’s Disease. Front Aging Neurosci 14:880897. https://doi.org/10.3389/fnagi.2022.880897
Nasrolahi A, Shabani Z, Sadigh-Eteghad S, Salehi-Pourmehr H, Mahmoudi J (2024) Stem cell therapy for the treatment of Parkinson’s Disease: what Promise does it hold? Curr Stem Cell Res Ther 19(2):185–199. https://doi.org/10.2174/1574888X18666230222144116
Hassanzadeh Kiabi F, Gharooee Ahangar S, Beiranvand S (2024) Assessing blood-brain barrier function in the context of Pain Management. Cent Nerv Syst Agents Med Chem. https://doi.org/10.2174/0118715249283159240316091312
Ramazani E, Tayarani-Najaran Z, Fereidoni M (2019) Celecoxib, Indomethacin, and ibuprofen prevent 6-hydroxydopamine-induced PC12 cell death through the inhibition of NFkappaB and SAPK/JNK pathways. Iran J Basic Med Sci 22(5):477–484. https://doi.org/10.22038/IJBMS.2019.34011.8091
San Luciano M, Tanner CM, Meng C, Marras C, Goldman SM, Lang AE et al (2020) Nonsteroidal anti-inflammatory use and LRRK2 Parkinson’s Disease Penetrance. Mov Disord 35(10):1755–1764. https://doi.org/10.1002/mds.28189
Sabatucci A, Simonetti M, Tortolani D, Angelucci CB, Dainese E, Maccarrone M (2019) Role of steroids on the membrane binding ability of fatty acid Amide Hydrolase. Cannabis Cannabinoid Res 4(1):42–50. https://doi.org/10.1089/can.2018.0051
Miranda HF, Lemus I, Pinardi G (2003) Effect of the inhibition of serotonin biosynthesis on the antinociception induced by nonsteroidal anti-inflammatory drugs. Brain Res Bull 61(4):417–425. https://doi.org/10.1016/s0361-9230(03)00144-8
Li C, Chen X, Zhang N, Song Y, Mu Y (2012) Gastrodin inhibits neuroinflammation in rotenone-induced Parkinson’s disease model rats. Neural Regen Res 7(5):325–331. https://doi.org/10.3969/j.issn.1673-5374.2012.05.001
Huang S, Liu H, Lin Y, Liu M, Li Y, Mao H et al (2020) Berberine protects against NLRP3 inflammasome via ameliorating autophagic impairment in MPTP-Induced Parkinson’s Disease Model. Front Pharmacol 11:618787. https://doi.org/10.3389/fphar.2020.618787
Martinez-Martin P (2011) The importance of non-motor disturbances to quality of life in Parkinson’s disease. J Neurol Sci 310(1–2):12–16. https://doi.org/10.1016/j.jns.2011.05.006
Cassani E, Privitera G, Pezzoli G, Pusani C, Madio C, Iorio L et al (2011) Use of probiotics for the treatment of constipation in Parkinson’s disease patients. Minerva Gastroenterol Dietol 57(2):117–121
Georgescu D, Ancusa OE, Georgescu LA, Ionita I, Reisz D (2016) Nonmotor gastrointestinal disorders in older patients with Parkinson’s disease: is there hope? Clin Interv Aging 11:1601–1608. https://doi.org/10.2147/CIA.S106284
Magistrelli L, Amoruso A, Mogna L, Graziano T, Cantello R, Pane M et al (2019) Probiotics May have Beneficial effects in Parkinson’s Disease: in vitro evidence. Front Immunol 10:969. https://doi.org/10.3389/fimmu.2019.00969
Wang W, Li Y, Meng X (2023) Vitamin D and neurodegenerative diseases. Heliyon 9(1):e12877. https://doi.org/10.1016/j.heliyon.2023.e12877
Calvello R, Cianciulli A, Nicolardi G, De Nuccio F, Giannotti L, Salvatore R et al (2017) Vitamin D treatment attenuates Neuroinflammation and Dopaminergic Neurodegeneration in an animal model of Parkinson’s Disease, shifting M1 to M2 microglia responses. J Neuroimmune Pharmacol 12(2):327–339. https://doi.org/10.1007/s11481-016-9720-7
Zhang Y, Ji W, Zhang S, Gao N, Xu T, Wang X et al (2022) Vitamin D inhibits the early aggregation of alpha-synuclein and modulates exocytosis revealed by Electrochemical measurements. Angew Chem Int Ed Engl 61(1):e202111853. https://doi.org/10.1002/anie.202111853
Hiller AL, Murchison CF, Lobb BM, O’Connor S, O’Connor M, Quinn JF (2018) A randomized, controlled pilot study of the effects of vitamin D supplementation on balance in Parkinson’s disease: does age matter? PLoS ONE 13(9):e0203637. https://doi.org/10.1371/journal.pone.0203637
Ricci A, Rubino E, Serra GP, Wallen-Mackenzie A (2024) Concerning neuromodulation as treatment of neurological and neuropsychiatric disorder: insights gained from selective targeting of the subthalamic nucleus, para-subthalamic nucleus and zona incerta in rodents. Neuropharmacology 256:110003. https://doi.org/10.1016/j.neuropharm.2024.110003
Chen Y, Zhu G, Liu D, Zhang X, Liu Y, Yuan T et al (2020) Subthalamic nucleus deep brain stimulation suppresses neuroinflammation by Fractalkine pathway in Parkinson’s disease rat model. Brain Behav Immun 90:16–25. https://doi.org/10.1016/j.bbi.2020.07.035
Campos ACP, Kikuchi DS, Paschoa AFN, Kuroki MA, Fonoff ET, Hamani C et al (2020) Unraveling the role of astrocytes in Subthalamic Nucleus Deep Brain Stimulation in a Parkinson’s Disease Rat Model. Cell Mol Neurobiol 40(6):939–954. https://doi.org/10.1007/s10571-019-00784-3
Wang Y, Yuan T, Lyu T, Zhang L, Wang M, He Z et al (2025) Mechanism of inflammatory response and therapeutic effects of stem cells in ischemic stroke: current evidence and future perspectives. Neural Regen Res 20(1):67–81. https://doi.org/10.4103/1673-5374.393104
Gordon J, Lockard G, Monsour M, Alayli A, Choudhary H, Borlongan CV (2022) Sequestration of Inflammation in Parkinson’s Disease via Stem Cell Therapy. Int J Mol Sci 23(17). https://doi.org/10.3390/ijms231710138
Kim IK, Park JH, Kim B, Hwang KC, Song BW (2021) Recent advances in stem cell therapy for neurodegenerative disease: three dimensional tracing and its emerging use. World J Stem Cells 13(9):1215–1230. https://doi.org/10.4252/wjsc.v13.i9.1215
Grealish S, Diguet E, Kirkeby A, Mattsson B, Heuer A, Bramoulle Y et al (2014) Human ESC-derived dopamine neurons show similar preclinical efficacy and potency to fetal neurons when grafted in a rat model of Parkinson’s disease. Cell Stem Cell 15(5):653–665. https://doi.org/10.1016/j.stem.2014.09.017
Kikuchi T, Morizane A, Doi D, Magotani H, Onoe H, Hayashi T et al (2017) Human iPS cell-derived dopaminergic neurons function in a primate Parkinson’s disease model. Nature 548(7669):592–596. https://doi.org/10.1038/nature23664
Acknowledgements
Not applicable.
Funding
This study was supported by the National Natural Science Foundation of China (No. 82371271, U2002220), the innovation team of stress and disorder in nervous system in Yunnan Province (202305AS350011), and Yunling Scholar (No. 1097821401).
Author information
Authors and Affiliations
Contributions
Xiaowei Sun writes and edits, Jie Bai reviews and supported by Fundings and Rou Gu helps discussion.
Corresponding author
Ethics declarations
Ethics approval and consent to participate
Not applicable.
Consent for publication
Not applicable.
Conflict of interest
The authors report no competing interests.
Additional information
Publisher’s Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution-NonCommercial-NoDerivatives 4.0 International License, which permits any non-commercial use, sharing, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if you modified the licensed material. You do not have permission under this licence to share adapted material derived from this article or parts of it. The images or other third party material in this article are included in the article’s Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article’s Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by-nc-nd/4.0/.
About this article
Cite this article
Sun, X., Gu, R. & Bai, J. Differentiation and regulation of CD4+ T cell subsets in Parkinson’s disease. Cell. Mol. Life Sci. 81, 352 (2024). https://doi.org/10.1007/s00018-024-05402-0
Received:
Revised:
Accepted:
Published:
DOI: https://doi.org/10.1007/s00018-024-05402-0