Abstract
Diabetic kidney disease (DKD) is the predominant type of end-stage renal disease. Increasing evidence suggests thatglomerular mesangial cell (MC) inflammation is pivotal for cell proliferation and DKD progression. However, the exactmechanism of MC inflammation remains largely unknown. This study aims to elucidate the role of inflammatoryfactor high-mobility group box 1 (Hmgb1) in DKD. Inflammatory factors related to DKD progression are screened viaRNA sequencing (RNA-seq). In vivo and in vitro experiments, including db/db diabetic mice model, CCK-8 assay, EdUassay, flow cytometric analysis, Co-IP, FISH, qRT-PCR, western blot, single cell nuclear RNA sequencing (snRNA-seq),are performed to investigate the effects of Hmgb1 on the inflammatory behavior of MCs in DKD. Here, wedemonstrate that Hmgb1 is significantly upregulated in renal tissues of DKD mice and mesangial cells cultured withhigh glucose, and Hmgb1 cytopasmic accumulation promotes MC inflammation and proliferation. Mechanistically,Hmgb1 cytopasmic accumulation is two-way regulated by MC-specific cyto-lncRNA E130307A14Rik interaction andlactate-mediated acetylated and lactylated Hmgb1 nucleocytoplasmic translocation, and accelerates NFκB signalingpathway activation via directly binding to IκBα. Together, this work reveals the promoting role of Hmgb1 on MCinflammation and proliferation in DKD and helps expound the regulation of Hmgb1 cytopasmic accumulation in twoways. In particular, Hmgb1 may be a promising therapeutic target for DKD.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Background
Diabetic kidney disease (DKD) is the predominant cause of both end-stage renal disease and chronic kidney disease, which acts as a principal microvascular complication of diabetes [1, 2]. The main pathological features of DKD include interstitial fibrosis, atrophy of renal tubules, thickening of the glomerular basement membrane, and dilation of mesangial cells, all of which have a significant impact on the health of individuals [3]. In some sense, mesangial expansion is a crucial structural abnormality characterized by the abnormal growth of mesangial cell (MC) and excessive synthesis of matrix proteins. During the initial phase of DKD, the principal indication is the excessive growth of glomerular MCs, which gives rise to the extracellular matrix components production that block capillaries over time, thereby triggering glomerular sclerosis and kidney failure ultimately [4, 5]. But the reasons and effects of mesangial cell proliferation on kidney function are not clearly understood. Hence, it is crucial to comprehend the fundamental processes of mesangial cell growth in order to elucidate the disease-causing mechanisms of DKD.
As illustrated by growing studies at home and abroad, inflammatory response in the kidney conducts increasingly significant roles in the development and advancement of DKD, and that treatments targeting inflammation could potentially protect the kidneys in DKD [6]. As already exhibited by preclinical studies, multiple inflammatory signaling pathways, such as nuclear factor-kappa B (NF-κB), are activated in response to elevated glucose levels [7]. Since the complex cell heterogeneity in kidney, to identify cell specific targets might be the effective anti-inflammatory strategy in DKD. Our prior research indicated NF-κB activation participated in the generation of inflammatory substances by mesangial cells which reinforce mesangial cell growth [8,9,10]. This underscores the significance of the NF-κB pathway in mesangial cell inflammation. Nevertheless, the process of inflammation in mesangial cells continues to be mostly enigmatic.
The family of high mobility group (HMG), known for their ability to move quickly in polyacrylamide gel electrophoresis, consists of the nuclear proteins HMGA, HMGB, HMGN. Hmgb1, a highly abundant protein in mammalian cells and tissues, is the most common protein in the HMG family and the second most common protein in the nucleus [11]. In general, Hmgb1 is primarily found in the nucleus where it interacts with chromatin and affects transcription, DNA repairing, differentiation, and cell growth. In multifarious stressful conditions, it can shift back and forth from the nucleus to the cytoplasm, which not only serves as a cytokine that is secreted into the extracellular environment, but also acts as a DAMP molecule to induce inflammation [12,13,14]. Hmgb1 outside the cell can bind to different receptors on the cell surface, such as advanced glycation end-products (RAGE) and Toll-like receptors (TLR), which results in the activation of NF-κB nuclear transcription [15,16,17]. To sum up, these studies evidently demonstrate that extracellular Hmgb1 is closely related to NF-κB pathway. A recent report indicated that Hmgb1 was confined in the cytoplasm, enhancing the inflammatory reaction through NF-κB activation, which worsened the damage caused by cerebral ischemia reperfusion [18]. Nonetheless, the function and process of cytoplasmic Hmgb1 buildup in the inflammation of mesangial cells in DKD are still not understood.
As apparently displayed by our current research, the build-up of cytosolic Hmgb1 results in mesangial cell inflammation and proliferation by binding directly to IκBα and activating the NF-κB signaling. Apart from that, the movement of Hmgb1 from the nucleus to the cytoplasm induced by lactate, along with acetylation and lactylation, and the subsequent increase in the presence of Hmgb1 in the cytoplasm of mesangial cells under high glucose stress through the E130307A14Rik-Hmgb1 axis. These data collectively suggest that Hmgb1 cytoplasmic accumulation aggravates DKD progression.
Materials and methods
Cell culture
The mouse mesangial cell line was obtained from the American Type Culture Collection in the US. Cultured cells were incubated in DMEM supplemented with 10% fetal bovine serum from Gibco in California, USA. To create the standard state, 5.5 mmol/L glucose / 19.5 mmol/L mannitol (L-MC) was used, while the DKD condition was replicated with 25 mmol/L glucose (H-MC) as previously explained [19]. Subsequently, the cells were cultured with 5% CO2 at 37℃ in the incubator. Mycoplasma contamination was regularly screened by adopting the Mycoplasma PCR Detection Kit (Yeasen biotech, Shanghai, China).
Animal experiments
Blood sugar levels, urine protein levels, and creatinine levels were systematically and comprehensively assessed in db/db mice and db/m mice. As previously reported, the db/db mice at eight weeks old were deemed to be in the initial phases of DKD [20]. The Leprdb/+Leprdb mice (db/db, male, C57BL/BKS background) and the genetic controls (m+/+Leprdb) were obtained from Nanjing Biomedical Research Institute in Nanjing, China for conducting single-nucleus RNA sequencing (snRNA-seq), bulk RNA sequencing (RNA-seq), and in vivo knock down experiments. Experiments involving snRNA-seq and RNA-seq were conducted using 16-week-old male db/db mice (DKD group, n = 3) and age-matched control db/m mice (NC group, n = 3). Aside from that, male db/db mice aged 10 weeks were subjected to knockdown animal experiments where they received treatment with Lv-shRNA (LV-sh-E130307A14Rik group, n = 10) or control lentivirus (LV-sh-NC group, n = 10) through tail vein injection (1 × 107 TU/mL, 100 µL). Measurements of blood sugar, weight, creatinine, and microalbumin in urine were taken on a biweek basis. Four weeks later, all mice were sacrificed. All remaining kidneys were preserved under appropriate storage conditions for subsequent experiments.
Plasmids, siRNA, lentivirus and cell transfection
To create over-expression vectors, the cDNA sequences for Hmgb1, NF-κB-p65, and E130307A14Rik were cloned into the empty vector pcDNA3.1 from TSINGKE in Beijing, China. RiboBio inserted the complete mouse Hmgb1 cDNA sequence and its three truncated forms (A box, B box, and C tail) into the pcDNA3.1-3 × Flag vector. SiRNAs directed against Hmgb1 (si-H-1, si-H-2, and si-H-3) and E130307A14Rik (si-E-1, si-E-2, and si-E-3) as well as control substances were purchased from RiboBio in Guangzhou, China, and TSINGKE in Beijing, China. ShRNA sequences against E130307A14Rik and control hairpins were into pGLVH1/GFP vector (TSINGKE, Beijing, China) separately. The transfection was conducted by employing plasmid or siRNAs and Lipofectamine 2000 reagents in line with the manufacturers’ protocols. Acting as a direct Hmgb1 antagonist, glycyrrhizin (Selleck Chemical, TX, USA) inhibits the expression of Hmgb1. The Glycyrrhizin powder is dissolved in dimethyl sulfoxide, resulting in a final concentration of 10 µM in MCs [21].
Extraction of RNA followed by quantitative real-time polymerase chain reaction (qRT-PCR)
RNA extraction was performed with Trizol (Invitrogen, CA, USA) in accordance with the manufacturer’s instructions. The RNA was then reverse transcribed into cDNA by the PrimeScript RT kit (Takara, Otsu, Japan). Afterwards, the qRT-PCR analysis was performed with the SYBR Green Real-time PCR Master Mix Kit manufactured by Takara in Dalian, China. It’s particularly noteworthy that the analysis involved normalizing relative quantification data of lncRNAs and mRNAs to β-actin. Each experiment was conducted three times at least.
SnRNA-seq
Kidney tissue samples were obtained from db/db DKD mice (n = 3) and control mice (n = 3). Subsequently, single cell suspensions were prepared after perfusion collection, followed by capturing mRNA and performing reverse transcription on the 10×genomics platform. The constructed libraries underwent snRNA-seq using the Illumina sequencing platform from Omicsmart in Guangzhou, China. Normalized data function, RunTSNE function, and Find clustering function were employed to analyze the source data for integration, normalization, t-SNE dimensionality reduction, and cell clustering in order to identify differentially expressed genes at the single cell level.
RNA-seq
The Illumina HiSeq sequencing platform from TSINGKE in Beijing, China was adopted to look into examine the variation in mRNA expression levels in kidney samples from three db/db DKD mice and three control mice. Data analysis was conducted by TSINGKE (Beijing, China).
Western blot
Proteins were separated by SDS-polyacrylamide gel electrophoresis (8, 10, 12, 15% SDS-PAGE), transferred onto the polyvinylidene fluoride membrane (Millipore, Massachusetts, USA). The barrier was blocked with 5% skim milk for 2 h at room temperature, then incubated with the appropriate primary antibody at 4 °C for 12 to 16 h. Primary antibodies used in this study were Mcp-1, Tnf-α, Hmgb1, Lactyl-lysine, Acetyl-Lysine, IκBα, p-IκBα, NF-κB p65, p-p65, β-actin, and H3, all diluted to 1:1000 or 1:5000 from different suppliers like ABclonal, Abcam, PTM Bio, and Beyotime. This was followed by secondary antibodies at room temperature for 2 h and detection using enhanced chemiluminescence (ECL) system. The analysis of the partially quantified band data was carried out by Image J software.
Nucleocytoplasmic separation and expression detection
Nuclear and cytoplasmic protein components were extracted in accordance with the kit’s NE-PER Nuclear and Cytoplasmic Extractant (Thermo Scientific™) product brochure. Western blot was employed to detect protein expression levels. The β-actin protein served as a cytoplasmic reference, while the H3 protein functioned as a nuclear reference.
EdU test
Cells were added to 24-well plates following the guidelines of the EdU kit (RiboBio, Guangzhou, China). A concentration of 100 mM EdU was applied for 2 h. Afterwards, the cells underwent treatment with 4% paraformaldehyde for 30 min, followed by exposure to Triton X 100 for 10 min prior to staining with the required reagents. Subsequently, the fluorescent microscope (Leica, Wetzlar, Germany) was adopted to capture the treated cells at last.
Flow cytometric analysis
Cell suspensions were placed in 6-well plates at a density of 5.5 × 105 cells per well. Moreover, three compound wells were done for each group. Subsequently, the precipitates were soaked in 75% ethanol and stored at 4 °C for 6 h. Flow cytometry analysis was employed to identify alterations in cell cycle distribution.
RNA pull-down
Following the guidelines of the kit from Thermo Fisher Scientific in MA, USA, the biotin-labeled E130307A14Rik probe from GenePharma in Shanghai, China, was blended with magnetic beads for 2 h at 25 ℃. Subsequently, the magnetic beads were exposed to cell lysate overnight at 4 ℃. The complexes of RNA and protein were isolated by adopting biotin elution buffer. The proteins were recovered, purified (Beyotime Bitechnology, Shanghai, China), and western blot.
RNA immuno-precipitation (RIP)
The RIP kit (Millipore, Billerica, MA, USA) was used in this process. Microspheres were coated with antibodies by blending either anti-Hmgb1 or anti-IgG with magnetic beads for 4 h at 4 °C on a shaker. Afterwards, formaldehyde-treated cells were cross-linked with protein-RNA complexes. A fraction representing 10% of the lysate was used as a control, while the rest of the cell lysate was then exposed to the appropriate beads and incubated for 12–16 h at 4 °C. After immuno-precipitation, the unbound substances were removed and the bound RNA and proteins were purified, then analyzed separately using qRT-PCR and western blot techniques.
Co-immuno-precipitation (Co-IP)
Antibodies against Hmgb1 (ABclonal), IκBα (Abcam), Klac (PTM BIO), Ace (ABclonal), or IgG (CST) were attached to magnetic beads at 4 °C for 8 h. Cell lysis was conducted by adopting IP lysis from the Co-IP Kit (DIANA Biotechnology Co., Ltd, Wuhan, China). Subsequently, antibody-coated magnetic beads were mixed with cell lysates and left to incubate at 4 °C for 12 to 16 h. The proteins that adhered to specific antibodies were washed, then dissolved in lane marker buffer, and subsequently examined through western blotting.
Immunofluorescence (IF) staining
Cells were subjected to 4% paraformaldehyde for 30 min followed by exposure to 0.1% Triton X-100 for 10 min. Afterwards, cells were treated with 5% goat serum for 1 h. Subsequently, they were incubated overnight with a mixture of anti-Hmgb1 (1:50). A second FITC-labeled anti-rabbit antibody was performed. DAPI was adopted to dye the nucleus core. Finally, images were observed by fluorescence microscope or laser scanning confocal microscope, and analyzed with LASAFLite (Leica, Solms, Germany).
Bioinformatics analysis methods
Changes in biological processes were investigated in DKD by conducting Gene Ontology (GO) on genes expressed differently in DKD [22]. Subsequently, the GeneCards platform was utilized to identify molecules linked to inflammation [23]. The Hitpredict database (https://www.hitpredict.org/) was employed to predict binding proteins of Hmgb1 [24]. The RPIseq database was utilized to forecast the precise binding locations of lncRNAs with Hmgb1 [25]. DeepKla database (http://lin-group.cn/server/DeepKla/index.html) were adopted to predict lactylation sites of Hmgb1.
Statistical analysis
Statistical analysis of the results was conducted by employing GraphPad Prism 8.0.2 software from San Diego, California, USA. Quantitative data from the experiment were presented as the average value plus or minus the standard deviation. Group differences were evaluated by conducting either Student’s t-test or one-way ANOVA. A statistical significance was determined with a significance level below 0.05.
Results
Cytosolic Hmgb1 promotes inflammation and proliferation in mesangial cells
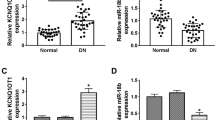
RNA-seq was conducted on renal tissue from mice with DKD and normal controls to identify inflammatory factors. The data revealed that 68 dysexpressed genes were found in DKD (P < 0.05, FPKM > 150, |log2FC| >1), consisting of 20 upregulated and 48 down-regulated genes (Fig. 1A). Based on GO analysis, the term ‘inflammatory response’ was found to be enriched with multiple genes including Hmgb1, Mep1b, Txnip, Nox4, Umod, Nlrc4, and Lipa (Fig. 1B). Moreover, combined the results of 290 inflammatory factors from Genecards database, 4 candidate genes were found. Among these, Hmgb1 was the only upregulated one among these (Fig. 1C). Therefore, we focused on Hmgb1 for further study. Subsequently, the levels of Hmgb1 were evaluated in H-MCs and renal tissues of DKD mice, which were conspicuously elevated (Fig. 1D-E). In comparison with L-MC, Hmgb1 cytoplasm protein levels increased and in contrast decreased levels of nuclear proteins in H-MC (Fig. 1F). What’s more, Hmgb1 was predominantly found in the nucleus of L-MC, but with exposure to high glucose, Hmgb1 was mostly located in the cytoplasm (Fig. 1G). Apart from that, the western blot findings indicated that the existence of Hmgb1 caused a significant increase in Mcp-1 and Tnf-α concentrations in L-MCs, On the contrary, lowering Hmgb1 in H-MCs resulted in lessened Mcp-1 and Tnf-α levels (Fig. 2A). Moreover, the EdU data showed that cell proliferation increased with Hmgb1 overexpression and decreased with its suppression (Fig. 2B). Flow cytometry analysis indicated that increased expression of Hmgb1 in L-MC led to a decrease in the population of cells in G1 phase and an increase in the population of cells in S phase, whereas decreased expression of Hmgb1 in H-MC resulted in more cells being arrested in G1 phase and fewer cells progressing to S phase (Fig. 2C). As a result, the data reveal that the build-up of Hmgb1 in the cytoplasm may control inflammation and cell growth in MCs.
Cytosolic Hmgb1 accumulates in mesangial cells under DKD condition. (A) Dysexpressed genes were examined in the renal tissue of db/db DKD mice (n = 3 for 16 weeks) and normal controls (n = 3 for 16 weeks) by RNA-seq (P < 0.05, FPKM > 150, |log2FC| >1). (B) GO term analysis of differentially expressed genes. (C) Venny shown that 4 DKD-associated inflammatory factors, including Hmgb1, Ttr, Ace and Nlrc4, Among them, Hmgb1 is upregulated and Ttr, Ace and Nlrc4 are downregulated. (D-E) qRT-PCR and western blot were used to detect the mRNA and protein expression levels of Hmgb1in L-MC and H-MC, in the renal tissue of db/db DKD mice (n = 3 for 16 weeks) and the normal group of mice (n = 3 for 16 weeks). (F-G) Western blot amd IF were performed to detect expression of Hmgb1 in the cytoplasm and nucleus in L-MC and H-MC, Scale bar, 3 μm. Data are presented as mean ± SD. *P < 0.05, **P < 0.01,***P < 0.001 and NS, no significance
Hmgb1 promotes inflammation and proliferation in mesangial cells. (A) The protein expression levels of Mcp-1 and Tnf-α were tested by western blot after transfecting Hmgb1 over-expression plasmid in L-MC or Hmgb1 siRNAs (si-H-1 and si-H-3) in H-MC. (B) EdU (scale bar, 20 μm) assays were performed to evaluate cell viability after transfecting Hmgb1 over-expression plasmid in L-MC or Hmgb1 siRNAs (si-H-1 and si-H-3) in H-MC, MCs was seeded at a density of 1 × 103/cm2 on confocal culture dishes. (C) Flow cytometry were performed to evaluate cell cycle after transfecting Hmgb1 over-expression plasmid in L-MC or Hmgb1 siRNAs (si-H-1 and si-H-3) in H-MC, Cell suspensions were placed in 6-well plates at a density of 5.5 × 105 cells per well. Data are presented as mean ± SD. *P < 0.05, **P < 0.01, ***P < 0.001 and NS, no significance
Hmgb1 activates the NF-κB pathway through interaction with IκBα
Using the Hitpredict database, we analyzed the potential binding proteins of Hmgb1 and identified NF-κB as a potential binding partner for Hmgb1 (Fig. 3A). And the Autodock software was further adopted to predict the relationship between Hmgb1 and NF-κB related molecules. IκBα which could potentially bind to Hmgb1 was found (Fig. 3B). Co-IP assay further confirmed their binding (Fig. 3C). Subsequently, western blot analysis displayed a conspicuous augment in the levels of p-IκBα and p-p65 in the overall protein owing to the over-expression of Hmgb1 in L-MC, along with higher p-p65 levels in the nucleus; on the other hand, reducing Hmgb1 protein level by using si-Hmgb1 or Glycyrrhetinic in H-MC (Fig.S2) led to a decrease in both, p-IκBα and p-p65 expressions (Fig. 3D). Altogether, as revealed by the above-mentioned results, upregulated Hmgb1 may initiated NF-κB activation through inducing IκBα phosphorylation in H-MC.
Hmgb1 activates NF-κB signal pathway via interacting with IκBα. (A) Prediction of proteins that may bind to Hmgb1 by Hitpredict database. (B) Autodock shows the binding pattern of Hmgb1 protein and IκBα protein: green indicated Hmgb1 and blue indicated IκBα. (C) Co-IP assay was applied in MCs protein lysates using separately anti-Hmgb1, anti-IκBα, or anti-IgG, and then, the levels of IκBα and Hmgb1 were detected by western blot. (D) The levels of NF-κB signaling pathway-related proteins (IκBα, p-IκBα, p65 and p-p65) were examined by western blot with Hmgb1 over-expression vector in L-MC group, Hmgb1 siRNA in H-MC or inhibitor (Glycyrrhizin, Gly) in H-MC. Results were displayed as mean ± SD. *P < 0.05, **P < 0.01, ***P < 0.001 and NS, no significance
Two ways to Hmgb1 cytopasmic accumulation: lactate-induced Hmgb1 lactylation and acetylation and direct interaction with MC-specific lncRNA E130307A14Rik
Glycolysis abnormalities in DKD mice give rise to glycolysis-derived lactate accumulation in the renal of DKD mice [26, 27]. As pointed out by relevant reports, lactate can directly induce Hmgb1 lactylation and acetylation, resulting in its translocation from the nucleus to the cytoplasm in macrophages [28]. Our study also explored the movement of Hmgb1 from the nucleus to the cytoplasm in mesangial cells. The qRT-PCR results revealed an increased expression of glycolysis-relevant genes (Hk1, Slc2a1, Pkm2 and Ldha) in H-MC (Fig. 4A). And compared to L-MC, lactate levels increased in H-MC (Fig. 4B). Lactate could reinforce the lactlation and acetylation Hmgb1 levels (Klac-Hmgb1 and Ace-Hmgb1) in L-MC (Fig. 4C). Thus, it suggests that lactate induced Hmgb1 lactylation and acetylation propels the nucleoplasmic translocation of Hmgb1 in mesangial cells under high glucose.
Two ways to Hmgb1 cytopasmic accumulation: lactate induced Hmgb1 lactylation and acetylation and direct interaction with MC specific lncRNA E130307A14Rik. (A) The mRNA expression levels of glycolysis genes (Hk1, Slc2a1, Pkm2 and Ldha) were measured by qRT-PCR in L-MC and H-MC. (B) Lactate levels in L-MC and H-MC were measured by Lactate Assay Kit. (C) L-MC were immunoprecipitated with anti-HMGB1 antibody after lactate stimulation followed by immunoblotting for Klac, Ace and Hmgb1. (D) Heatmap of 17 mesangial cell-specific lncRNAs by snRNA-seq. (E) 9 differentially expressed lncRNAs including 5 up-regulated (E130310I04Rik, Gm15261, Gm17276, E130307A14Rik and Gm28379) and 4 down-regulated (Gm16311, Gm14964, Gm15962 and Gm30524) in MCs were shown. (F) The qRT-PCR detected the expressiong of 4 candidate lncRNAs in MC, mesangial cell; TCMK-1, mice renal tubular epithelial cell; POD, mice podocyte and the expression of 4 candidate lncRNAs in L-MC and H-MC. (G) 4 candidate lncRNAs were predicted the precise interaction with Hmgb1 by RPIseq. (H) RIP assay was performed in cell lysates using anti-Hmgb1 or anti-IgG, followed by qRT-PCR validation of E130307A14Rik. (I) RNA pull-down was performed in cell lysates using the E130307A14Rik probe, followed by western blot validation of Hmgb1. (J) The structures of Hmgb1 and deletion mappings of Hmgb1 (FL-Hmgb1: full length of Hmgb1: 1-225, A box: 9–73 B box: 95–163 and C tail:186–215). (K) RIP-qPCR to identify the E130307A14Rik and binding domains in Hmgb1 by full length or truncated Hmgb1 proteins. (L) Prediction of Hmgb1 lactylation sites by DeepKla. (M) E130307A14Rik full-length and 4 truncated fragments were displayed with schematic diagram, and were predicted the precise interaction with Hmgb1 by RPIseq. (N) RNA pull down assay and western blot were used to detect Hmgb1 binds to the fragments of E130307A14Rik. (O) Western blot were performed to detect expression of Hmgb1 in L-MC and H-MC after overexpression or knockdown E130307A14Rik. Results were displayed as mean ± SD. *P < 0.05, **P < 0.01, ***P < 0.001 and NS, no significance
Current researches focus on Hmgb1 secretion and acting as a cytokine following with its nucleoplasmic translocation in diseases [29], but the mechanism of Hmgb1 cytopasmic accumulation in mesangial cells remains largely unknown. The function of proteins in DKD may be regulated by long non-coding RNAs (lncRNAs) on the basis of our previous research [30, 31], but it remains unclear about the specific role of mesangial cell-specific lncRNAs in DKD. By employing snRNA-seq, we found 17 mesangial cell-specific lncRNAs (Fig. 4D), and 9 DKD-relevant lncRNAs in mesangial cell cluster of DKD and NC mice, including 5 up-regulated lncRNAs and 4 down-regulated lncRNAs (Fig. 4E). Combined these results, 4 candidate lncRNAs (E130307A14Rik, Gm17276, E13010I04Rik and Gm14964) were obtained with the features of mesangial cell-specific and DKD-relevant. Candidate lncRNAs were detected through qRT-PCR in kidney intrinsic cells MC, POD, and TC under high glucose conditions. Among them, E130307A14Rik was specifically high expressed in H-MC (Fig. 4F). Moreover, RPIseq database showed the highest binding ability scores between Hmgb1 and E130307A14Rik (Fig. 4G), suggesting the potential role of E130307A14Rik in Hmgb1 of mesangial cell. Therefore, we focused on E130307A14Rik for further study. Subsequently, RIP and RNA pull down methods were employed to confirm the association between E130307A14Rik and Hmgb1 (Fig. 4H-I). Hmgb1 consists of three parts (A box, B box, and C tail), then Flag tagged complete Hmgb1 was produced along with three separate shortened sections that do not intersect in the inactive regions (Fig. 4J). RIP assays revealed that E130307A14Rik is bound to the A box of Hmgb1 (Fig. 4K). And through DeepKla databases analysis, we found that A box of Hmgb1 is susceptible to lactylation (Fig. 4L). Besides, the RNA pull down and western blot assays evidently displayed that E130307A14Rik fragments 1-1500 nt (#1 and #2) could bind specifically to Hmgb1 (Fig. 4M-N). As apparently demonstrated by, validation of western blot results demonstrated that upregulation of E130307A14Rik gave rise to elevated levels of Hmgb1 protein in L-MC, with a contrasting effect observed (Fig. 4O). Altogether, these experimental findings revealed that two ways of regulations promote Hmgb1 cytopasmic accumulation in mesangial cell via lactate induced Hmgb1 lactylation and acetylation and direct interaction with MC-specific E130307A14Rik.
E130307A14Rik-Hmgb1 axis mediates inflammation by NF-κB pathway
To demonstrate that E130307A14Rik can activate the NF-κB signal pathway by regulating Hmgb1, rescue experiments were performed to estimate the co-regulating effect of E130307A14Rik and Hmgb1 in NF-κB pathway. The western blot findings evidently demonstrated that upregulation of E130307A14Rik in L-MC cells resulted in higher levels of p-IκBα and p-p65 in the overall protein, along with increased p-p65 expression in the nucleus. This effect was reversed by inhibiting Hmgb1 expression. On the contrary, inhibiting the level of E130307A14Rik suppressed the expressions of p-IκBα and p-p65, but this effect was reversed when Hmgb1 expression was increased (Fig. 5A). To sum up, these results apparently revealed that E130307A14Rik could activate the NF-κB signal pathway through Hmgb1. Subsequently, to demonstrate the interaction between E130307A14Rik and Hmgb1 in MCs inflammation response. Rescue trials were performed accordingly. Western blot analysis illustrated that lowering Hmgb1 levels led to a decrease in the elevated levels of Mcp-1 and Tnf-α in L-MC cells originating from overexpressed E130307A14Rik. On the contrary, elevating Hmgb1 levels counteracted the effects of E130307A14Rik depletion on the inhibition of Mcp-1 and Tnf-α expression in H-MC cells (Fig. 5B). Overall, these data illustrated that E130307A14Rik-Hmgb1 axis aggravates inflammation response in MCs.
E130307A14Rik-Hmgb1 axis mediates inflammation by NF-κB pathway. (A) The rescue experiments were performed to detect the effect of E130307A14Rik on NF-κB signaling via regulating Hmgb1. The NF-κB signaling pathway (IκBα, p-IκBα, p65 and p-p65) was detected after regulation the levels of E130307A14Rik, Hmgb1 or both of them by western blot. (B) The protein expression levels of Mcp-1 and Tnf-α were tested after after regulation the level of E130307A14Rik, Hmgb1 or both of them by western blot. Results were displayed as mean ± SD. *P < 0.05, **P < 0.01, ***P < 0.001 and NS, no significance
Suppression of E130307A14Rik mitigates kidney damage in DKD mice through Hmgb1
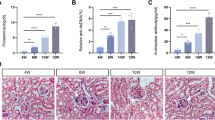
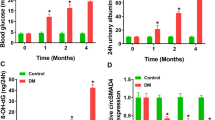
In vivo, we investigated how the E130307A14Rik-Hmgb1 axis impacts the kidney. LV-sh-E130307A14Rik and LV-sh-NC were administered to db/db DKD mice through the tail vein, with 10 mice in each group. The qRT-PCR findings indicated E130307A14Rik knockdown effectively downgraded the expression of E130307A14Rik in the kidneys compared to the LV-sh-NC group (Fig. 6A). Moreover, staining results for HE, PAS, and MASSON indicated potential improvement in pathological changes, the glomerular enlargement, tubulointerstitial fibrosis and mesangial matrix expansion resulted from diabetes were noticeably lessened (Fig. 6B). In comparison with db/m mice, Blood glucose, body weight, kidney weight to body weight ratio, urinary albumin, urinary creatinine, and UACR were increased in db/db mice (Fig. S4). Moreover, E130307A14Rik knockdown mice exhibited improvement in blood glucose, urinary albumin, urinary creatinine, and UACR compared to the controls (Fig. 6C). As obviously displayed by western blot results, in comparison with the controls, E130307A14Rik knockdown reduced the levels of Hmgb1, p-IκBα, p-p65 (Fig. 6D). Silencing E130307A14Rik decreased the levels of Mcp-1 and Tnf-α inflammatory factor proteins (Fig. 6E). As suggested by the above research finding, targeting the E130307A14Rik-Hmgb1 axis could be a potential strategy for treating kidney damage caused by diabetes through modulation of the NF-κB pathway.
E130307A14Rik knockdown alleviates renal injury in DKD mice by regulating Hmgb1. (A) E130307A14Rik expression levels in the renal tissue of LV-sh-E130307A14Rik group mice and LV-sh-NC group of mice (n = 10 for each mice group). (B) HE, PAS and MASSON staining revealed reduced damage in the kidney structure of E130307A14Rik knockdown mice (Scale bar = 100 μm). (C) Biochemical indicators of DKD were determined in E130307A14Rik knockdown mice and controls, including blood glucose, body weight, kidney weight to body weight ratio, urinary albumin, urinary creatinine, and UACR (n = 10 for each mice group). (D) The protein expression of Hmgb1 and key factors (IκBα, p-IκBα, p65 and p-p65) in the NF-κB signaling pathway in E130307A14Rik knockdown mice and the controls were detected by western blot. (E) Western blot were performed to assess the expression levels of Mcp-1 and Tnf-α in E130307A14Rik knockdown mice and controls. E130307A14Rik knockdown mice (n = 6 for 16 weeks) and controls (n = 6 for 16 weeks). Results were displayed as mean ± SD. *P < 0.05, **P < 0.01, ***P < 0.001 and NS, no significance
Discussion
Featured by heightened inflammatory pathways, release of cytokines and chemokines, and immune cell infiltration, kidney inflammation gives an impetus that the progression of DKD [32]. In recent times, molecules associated with inflammation in the kidneys have been linked to processes involved in DKD [33]. The specific function of inflammatory cytokines in diabetic kidney damage has not been confirmed yet. On that account, this research screened inflammatory factors in DKD mice via RNA-seq and revealed the role of Hmgb1 cytopasmic accumulation on mesangial cells inflammation and proliferation in DKD. Furthermore, our results demonstrated that lactate-mediated acetylated and lactylated Hmgb1 nucleocytoplasmic translocation and mesangial cells-specific cyto-lncRNA E130307A14Rik interaction participate in the Hmgb1 cytopasmic accumulation in mesangial cells, leading to accelerate NFκB signaling pathway activation via directly binding to IκBα (Fig. 7).
A persistent question in the study of Hmgb1 biology is the significance of cytosolic Hmgb1, as the transfer of Hmgb1 from the nucleus to the extracellular environment triggers in an augmented amount of Hmgb1 in the cytosol [11]. As suggested by studies indicate that cytosolic Hmgb1 triggers autophagy in mouse fibroblasts or human cancer cells under various environmental stressors such as starvation and oxidative damage, which gives rise to the release of DAMPs and subsequent inflammation [34, 35]. Furthermore, cytosolic Hmgb1 has been shown to interact with unbound nucleic acids, which results in the activation of the important cGAS/STING pathway, which plays a crucial role in inflammation [36, 37]. Our study indicates that cytoplasmic Hmgb1 might play a role in the inflammation of mesangial cells in DKD. As clearly revealed by the experimental results, Hmgb1 was upregulated in DKD in vivo and in vitro, accumulating abnormally in the cytoplasm of mesangial cells under high glucose conditions. Additionally, our findings indicated that cytosolic Hmgb1 accelerates the growth of mesangial cells and the production of the pro-inflammatory molecules, indicating the role of cytosolic Hmgb1 in the proliferation and inflammation of mesangial cells in DKD. Additionally, our findings from Co-IP and western blot analysis revealed that Hmgb1 has the ability to directly interact with IκBα. Moreover, Hmgb1 was found to enhance p-IκBα and p-p65. Conversely, the downregulation of Hmgb1 using siRNA or the inhibition of Hmgb1 with Gly resulted in decreased expression of p-IκBα and p-p65 in mesangial cells. As known, in resting cells, a dimer composed of NF-κB subunits p65 and p50 exists in an inactive state by binding to the IκB kinase complex (IκBα, IκBβ and IκBε) in the cytoplasm. When the cell is stimulated from the outside, the IκB kinase complex becomes active, leading to phosphorylation of IκB, which then quickly moves p65 into the nucleus and triggers the transcription of specific genes [38]. Collectively, as illustrated by these results, upregulated cytosolic Hmgb1 may initiated NF-κB activation through inducing IκBα phosphorylation in mesangial cells, which facilitates the mesangial cells proliferation and inflammation in DKD.
Post-translational modifications (PTMs) have a significant impact on the location and function of Hmgb1, as widely recognized in the scientific community [39]. Hmgb1 can transition from the nucleus to the cytoplasm through modifications of nuclear localization signals NLS1 and NLS2 via acetylation and deacetylation mechanisms [40]. Aside from acetylation, other alterations like lactylation may also control the movement of Hmgb1 [28]. Lactylation, a newly identified form of post-translational alteration, includes attaching lactyl groups to proteins by utilizing lactate produced from glycolysis [41]. Diabetic microvascular pathology, such as DKD, has been shown to have elevated glycolytic activity in a hyperglycemic condition [42]. It’s significant to note that our results highly accord with these studies, showing elevated levels of glycolysis indicators and lactate in mesangial cells when exposed to high glucose. Moreover, our research suggests that Klac-Hmgb1 and Ace-Hmgb1 are elevated in mesangial cells, suggesting that the localization of Hmgb1 in the cytosol of mesangial cells may be due to lactate-induced Hmgb1 lactylation and acetylation.
Traditionally, nuclear output is responsible for the cytoplasmic accumulation of Hmgb1. However, what causes it to reside in the cytoplasm are of concern to us. LncRNA is a type of functional RNA that is longer than 200 nucleotides and cannot be translated into proteins [43, 44]. It has been demonstrated that lncRNA plays a regulatory role of biological functions in the progression of numerous diseases, including DKD. Our previous research has shown that lnc-Rmrp promotes proliferation and fibrosis of the mesangial cell in DKD by miR-1a-3p [30], and the lnc-Rpph1 speeds up cell proliferation and inflammation of the mesangial cell by interacting with Gal-3 [31]. However, in view of the complexity of renal tissue cells, the search for mesangial cell-specific lncRNAs probably can answer the question of Hmgb1 cytoplasmic retention in mesangial cells. Consequently, snRNA-seq was utilized to delve deeper into the role of cytosolic Hmgb1 in mesangial cells in this study. This cutting-edge technology enables thorough sequencing analysis of genome, transcriptome, and epigenetics at the level of individual cells [45]. A new cyto-lncRNA E130307A14Rik specific to mesangial cells was discovered in this research using snRNA-seq. It was found to be overexpressed in the kidney tissues of mice with DKD and in mesangial cells exposed to high glucose. Furthermore, our experiments with RIP and RNA pull down showed a strong interaction between E130307A14Rik and Hmgb1, particularly with the function domain A box region of Hmgb1. Our findings from the DeepKla database indicate that the A box structural domain of Hmgb1 is vulnerable to lactylation. When considering the structure of Hmgb1 alongside our results, it implies that the A box of Hmgb1 plays a crucial role in the E130307A14Rik/Hmgb1 axis. This axis is accountable for triggering inflammation in mesangial cells and leading to renal injury via the NF-κB pathway, in both experimental models and living organisms. Therefore, we identified a new mechanism by which lactate induced Hmgb1 lactlation and acetylation and mesangial cell-specific cyto-lncRNA E130307A14Rik interaction regulated Hmgb1 cytopasmic accumulation in mesangial cell inflammation. In particular, these findings revealed that cytosolic Hmgb1-mediated NF-κB activation is a novel finding in clarifying the mechanism of DKD progression.
Conclusions
In brief, our research illustrates that the accumulation of Hmgb1 within the cytoplasm could potentially exacerbate inflammation and cellular proliferation in mesangial cells in diabetic kidney disease through its direct interaction with IκBα. More importantly, the experimental results revealed the regulation pattern of Hmgb1 cytopasmic accumulation in two ways from protein post-translational modifications level and single-cell lncRNA regulation level. These findings are advantageous for us to enrich and broaden our understanding of the mechanisms underlying DKD development.
Data availability
The data that support the findings of this study are available on request from the corresponding author, upon reasonable request.
References
Chan JCN, Lim LL, Wareham NJ, Shaw JE, Orchard TJ, Zhang P, Lau ESH, Eliasson B, Kong APS, Ezzati M et al (2021) The Lancet Commission on diabetes: using data to transform diabetes care and patient lives. Lancet 396(10267):2019–2082. https://doi.org/10.1016/S0140-6736(20)32374-6
Thomas MC, Brownlee M, Susztak K, Sharma K, Jandeleit-Dahm KA, Zoungas S, Rossing P, Groop PH, Cooper ME (2015) Diabetic kidney disease. Nat Rev Dis Primers 1:15018. https://doi.org/10.1038/nrdp.2015.18
Choi S, Hong SP, Bae JH, Suh SH, Bae H, Kang KP, Lee HJ, Koh GY (2023) Hyperactivation of YAP/TAZ drives alterations in mesangial cells through stabilization of N-Myc in diabetic nephropathy. J Am Soc Nephrol 34(5):809–828. https://doi.org/10.1681/ASN.0000000000000075
Hu S, Hang X, Wei Y, Wang H, Zhang L, Zhao L (2024) Crosstalk among podocytes, glomerular endothelial cells and mesangial cells in diabetic kidney disease: an updated review. Cell Commun Signal 22(1):136. https://doi.org/10.1186/s12964-024-01502-3
Thomas HY, Ford Versypt AN (2022) Pathophysiology of mesangial expansion in diabetic nephropathy: mesangial structure, glomerular biomechanics, and biochemical signaling and regulation. J Biol Eng 16(1):19. https://doi.org/10.1186/s13036-022-00299-4
Rohm TV, Meier DT, Olefsky JM, Donath MY (2022) Inflammation in obesity, diabetes, and related disorders. Immunity 55(1):31–55. https://doi.org/10.1016/j.immuni.2021.12.013
Hu X, Chen S, Ye S, Chen W, Zhou Y (2024) New insights into the role of immunity and inflammation in diabetic kidney disease in the omics era. Front Immunol 15:1342837. https://doi.org/10.3389/fimmu.2024.1342837
Sun Y, Peng R, Peng H, Liu H, Wen L, Wu T, Yi H, Li A, Zhang Z (2016) miR-451 suppresses the NF-kappaB-mediated proinflammatory molecules expression through inhibiting LMP7 in diabetic nephropathy. Mol Cell Endocrinol 433:75–86. https://doi.org/10.1016/j.mce.2016.06.004
Yi H, Peng R, Zhang LY, Sun Y, Peng HM, Liu HD, Yu LJ, Li AL, Zhang YJ, Jiang WH et al (2017) LincRNA-Gm4419 knockdown ameliorates NF-κB/NLRP3 inflammasome-mediated inflammation in diabetic nephropathy. Cell Death Dis 8(2):e2583. https://doi.org/10.1038/cddis.2016.451
Wu K, Peng R, Mu Q, Jiang Y, Chen J, Ming R, Zhao J, Zhang Z, Sun Y (2022) Rack1 regulates pro-inflammatory cytokines by NF-κB in diabetic nephropathy. Open Med (Wars) 17(1):978–990. https://doi.org/10.1515/med-2022-0487
Tang D, Kang R, Zeh HJ, Lotze MT (2023) The multifunctional protein HMGB1: 50 years of discovery. Nat Rev Immunol 23(12):824–841. https://doi.org/10.1038/s41577-023-00894-6
Wang H, Bloom O, Zhang M, Vishnubhakat JM, Ombrellino M, Che J, Frazier A, Yang H, Ivanova S, Borovikova L et al (1999) HMG-1 as a late mediator of endotoxin lethality in mice. Science 285(5425):248–251. https://doi.org/10.1126/science.285.5425.248
Mollnes TE (2008) High mobility group box-1 protein–one step closer to the clinic? Crit Care 12(4):168. https://doi.org/10.1186/cc6944
Chen R, Kang R, Tang D (2022) The mechanism of HMGB1 secretion and release. Exp Mol Med 54(2):91–102. https://doi.org/10.1038/s12276-022-00736-w
Chen Q, Guan X, Zuo X, Wang J, Yin W (2016) The role of high mobility group box 1 (HMGB1) in the pathogenesis of kidney diseases. Acta Pharm Sin B 6(3):183–188. https://doi.org/10.1016/j.apsb.2016.02.004
Hiramoto S, Tsubota M, Yamaguchi K, Okazaki K, Sakaegi A, Toriyama Y, Tanaka J, Sekiguchi F, Ishikura H, Wake H et al (2020) Cystitis-related bladder pain involves ATP-dependent HMGB1 release from macrophages and its downstream H2S/Cav3.2 signaling in mice. Cells 9(8):1748. https://doi.org/10.3390/cells9081748
Wang CM, Jiang M, Wang HJ (2013) Effect of NFκB inhibitor on highmobility group protein B1 expression in a COPD rat model. Mol Med Rep 7(2):499–502. https://doi.org/10.3892/mmr.2012.1181
Zhang W, Song J, Li W, Kong D, Liang Y, Zhao X, Du G (2020) Salvianolic acid D alleviates cerebral ischemia-reperfusion injury by suppressing the cytoplasmic translocation and release of HMGB1-triggered NF-κB activation to inhibit inflammatory response. Mediators Inflamm 2020:9049614. https://doi.org/10.1155/2020/9049614
Xu JL, Gan XX, Ni J, Shao DC, Shen Y, Miao NJ, Xu D, Zhou L, Zhang W, Lu LM (2018) SND p102 promotes extracellular matrix accumulation and cell proliferation in rat glomerular mesangial cells via the AT1R/ERK/Smad3 pathway. Acta Pharmacol Sin 39(9):1513–1521. https://doi.org/10.1038/aps.2017.184
Lin Z, Lv D, Liao X, Peng R, Liu H, Wu T, Wu K, Sun Y, Zhang Z (2023) CircUBXN7 promotes macrophage infiltration and renal fibrosis associated with the IGF2BP2-dependent SP1 mRNA stability in diabetic kidney disease. Front Immunol 14:1226962. https://doi.org/10.3389/fimmu.2023.1226962
Ohnishi M, Katsuki H, Fukutomi C, Takahashi M, Motomura M, Fukunaga M et al (2011 Oct-Nov) HMGB1 inhibitor glycyrrhizin attenuates intracerebral hemorrhage-induced injury in rats. Neuropharmacology 61(5–6):975–980. https://doi.org/10.1016/j.neuropharm.2011.06.026
Xie R, Li B, Jia L, Li Y (2022) Identification of core genes and pathways in melanoma metastasis via bioinformatics analysis. Int J Mol Sci 23(2):794. https://doi.org/10.3390/ijms23020794
Xu S, Li X, Zhang S, Qi C, Zhang Z, Ma R, Xiang L, Chen L, Zhu Y, Tang C et al (2023) Oxidative stress gene expression, DNA methylation, and gut microbiota interaction trigger Crohn’s disease: a multi-omics mendelian randomization study. BMC Med 21(1):179. https://doi.org/10.1186/s12916-023-02878-8
Li J, Liu C, Su H, Dong H, Wang Z, Wang Y et al (2024) Integrative analysis of LAG3 immune signature and identification of a LAG3-related genes prognostic signature in kidney renal clear cell carcinoma. Aging 16(3):2161–2180
Luo Y, Zhang Y, Pang S, Min J, Wang T, Wu D et al (2023) PCBP1 protects bladder cancer cells from mitochondria injury and ferroptosis by inducing LACTB mRNA degradation. Mol Carcinog 62(7):907–919
Kanasaki K (2023) The aberrant glycolysis in kidney proximal tubule: potential therapeutic target for DKD. Kidney Int 104(6):1056–1059
Song C, Wang S, Fu Z, Chi K, Geng X, Liu C, Cai G, Chen X, Wu D, Hong Q (2022) IGFBP5 promotes diabetic kidney disease progression by enhancing PFKFB3-mediated endothelial glycolysis. Cell Death Dis 13(4):340. https://doi.org/10.1038/s41419-022-04803-y
Yang K, Fan M, Wang X, Xu J, Wang Y, Tu F, Gill PS, Ha T, Liu L, Williams DL et al (2022) Lactate promotes macrophage HMGB1 lactylation, acetylation, and exosomal release in polymicrobial sepsis. Cell Death Differ 29(1):133–146. https://doi.org/10.1038/s41418-021-00841-9
Qiao X, Li W, Zheng Z, Liu C, Zhao L, He Y, Li H (2024) Inhibition of the HMGB1/RAGE axis protects against cisplatin-induced ototoxicity via suppression of inflammation and oxidative stress. Int J Biol Sci 20(2):784–800. https://doi.org/10.7150/ijbs.82003
Yang H, Wang J, Zhang Z, Peng R, Lv D, Liu H, Sun Y (2021) Sp1-Induced lncRNA Rmrp promotes mesangial cell proliferation and fibrosis in diabetic nephropathy by modulating the miR-1a-3p/JunD pathway. Front Endocrinol (Lausanne) 12:690784. https://doi.org/10.3389/fendo.2021.690784
Zhang P, Sun Y, Peng R, Chen W, Fu X, Zhang L, Peng H, Zhang Z (2019) Long non-coding RNA Rpph1 promotes inflammation and proliferation of mesangial cells in diabetic nephropathy via an interaction with Gal-3. Cell Death Dis 10(7):526. https://doi.org/10.1038/s41419-019-1765-0
Tang SCW, Yiu WH (2020) Innate immunity in diabetic kidney disease. Nat Rev Nephrol 16(4):206–222. https://doi.org/10.1038/s41581-019-0234-4
Navarro-González JF, Mora-Fernández C (2008) The role of inflammatory cytokines in diabetic nephropathy. J Am Soc Nephrol 19(3):433–442. https://doi.org/10.1681/ASN.2007091048
Wen Q, Liu J, Kang R, Zhou B, Tang D (2019) The release and activity of HMGB1 in ferroptosis. Biochem Biophys Res Commun 510(2):278–283. https://doi.org/10.1016/j.bbrc.2019.01.090
Wang Z, Zhou H, Zheng H, Zhou X, Shen G, Teng X, Liu X, Zhang J, Wei X, Hu Z et al (2021) Autophagy-based unconventional secretion of HMGB1 by keratinocytes plays a pivotal role in psoriatic skin inflammation. Autophagy 17(2):529–552. https://doi.org/10.1080/15548627.2020.1725381
Yanai H, Ban T, Wang Z, Choi MK, Kawamura T, Negishi H, Nakasato M, Lu Y, Hangai S, Koshiba R et al (2009) HMGB proteins function as universal sentinels for nucleic-acid-mediated innate immune responses. Nature 462(7269):99–103. https://doi.org/10.1038/nature08512
Andreeva L, Hiller B, Kostrewa D, Lässig C, de Oliveira Mann CC, Jan Drexler D, Maiser A, Gaidt M, Leonhardt H, Hornung V et al (2017) cGAS senses long and HMGB/TFAM-bound U-turn DNA by forming protein-DNA ladders. Nature 549(7672):394–398. https://doi.org/10.1038/nature23890
Capece D, Verzella D, Flati I, Arboretto P, Cornice J, Franzoso G (2022) NF-κB: blending metabolism, immunity, and inflammation. Trends Immunol 43(9):757–775. https://doi.org/10.1016/j.it.2022.07.004
Liu T, Li Q, Jin Q, Yang L, Mao H, Qu P, Guo J, Zhang B, Ma F, Wang Y et al (2023) Targeting HMGB1: a potential therapeutic strategy for chronic kidney disease. Int J Biol Sci 19(15):5020–5035. https://doi.org/10.7150/ijbs.87964
Tang Y, Zhao X, Antoine D, Xiao X, Wang H, Andersson U, Billiar TR, Tracey KJ (2016) Lu B.Regulation of posttranslational modifications of HMGB1 during immune responses. Antioxid Redox Signal 24(12):620–634. https://doi.org/10.1089/ars.2015.6409
Zhang D, Tang Z, Huang H, Zhou G, Cui C, Weng Y, Liu W, Kim S, Lee S, Perez-Neut M et al (2019) Metabolic regulation of gene expression by histone lactylation. Nature 574(7779):575–580. https://doi.org/10.1038/s41586-019-1678-1
Qi W, Keenan HA, Li Q, Ishikado A, Kannt A, Sadowski T, Yorek MA, Wu IH, Lockhart S, Coppey LJ et al (2017) Pyruvate kinase M2 activation may protect against the progression of diabetic glomerular pathology and mitochondrial dysfunction. Nat Med 23(6):753–762. https://doi.org/10.1038/nm.4328
Bridges MC, Daulagala AC, Kourtidis A (2021) LNCcation: lncRNA localization and function. J Cell Biol 220(2):e202009045. https://doi.org/10.1083/jcb.202009045
Yip CW, Sivaraman DM, Prabhu AV, Shin JW (2021) Functional annotation of lncRNA in high-throughput screening. Essays Biochem 65(4):761–773. https://doi.org/10.1042/EBC20200061
Oh JM, An M, Son DS, Choi J, Cho YB, Yoo CE, Park WY (2022) Comparison of cell type distribution between single-cell and single-nucleus RNA sequencing: enrichment of adherent cell types in single-nucleus RNA sequencing. Exp Mol Med 54(12):2128–2134. https://doi.org/10.1038/s12276-022-00892-z
Acknowledgements
None.
Funding
This study was supported by the National Natural Science Foundations of China (No. 82270876), CQMU Program for Youth Innovation in Future Medicine (W0173), Science and Technology Research Program of Chongqing Municipal Education Commission (KJQN202400439) and Key Discipline Clinical Laboratory Diagnostics Project of Guizhou Provincial Health Commission (QWjh[2021]160).
Author information
Authors and Affiliations
Contributions
KW, TW and HZ are the experimental designer and executor of the experimental research of this study, completes data analysis, writing the first draft of the paper; DL, ZL, RP, XL and HL participates in experimental design and analysis of experimental results; KW, YS and ZZ participates in experimental design, data analysis, and thesis writing. ZZ and YS conceived the project and supervised research. All authors read and approved the final manuscript.
Corresponding authors
Ethics declarations
Ethics approval and consent to participate
Approval for all animal testing was granted by the Institutional Animal Care and Use Committees at Chongqing Medical University (approval no.2022135, 27 May 2022). All animal experiments were performed in accordance with the rules of Basel Declaration.
Consent for publication
All the authors agree with the publication of the manuscript.
Competing interests
The authors declare that they have no competing interests.
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Electronic supplementary material
Below is the link to the electronic supplementary material.
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution-NonCommercial-NoDerivatives 4.0 International License, which permits any non-commercial use, sharing, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if you modified the licensed material. You do not have permission under this licence to share adapted material derived from this article or parts of it. The images or other third party material in this article are included in the article’s Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article’s Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by-nc-nd/4.0/.
About this article
Cite this article
Wu, K., Zha, H., Wu, T. et al. Cytosolic Hmgb1 accumulation in mesangial cells aggravates diabetic kidney disease progression via NFκB signaling pathway. Cell. Mol. Life Sci. 81, 408 (2024). https://doi.org/10.1007/s00018-024-05433-7
Received:
Revised:
Accepted:
Published:
DOI: https://doi.org/10.1007/s00018-024-05433-7