Abstract
Purpose
Calcaneal fractures (CFs) are rare but potentially debilitating injuries. Apart from the open, far lateral or sinus tarsi approach, operative treatment can be performed minimally invasive and percutaneously with intramedullary nailing. In this study, we sought to investigate the functional outcome of severe CFs treated with the C-Nail® implant.
Methods
Twenty-two CFs (9 × Sanders III and 8 × Sanders IV), operated between 2016 and 2019, were followed up with a mean duration of 36 (± 11) months. The AOFAS score, pre- and postoperative Böhler angles, wound healing disorders, and patient-reported outcome measures (PROMs) like pain levels and return to work/sport levels were assessed.
Results
The mean AOFAS score was 72.0 (± 9.8). Four patients sustained wound healing disorders, yet no implant-associated surgical revision was required. Fifty percent of patients were pain-free within 1 year. Within 1 year, about 50% of the patients could return to sports, and about 80% of the patients could return to work. PROMs and functional results align with those from other implants reported in the literature.
Conclusion
Intramedullary nailing of severe CFs with the C-Nail® implant can be considered a safe treatment alternative that yields acceptable results at mid-terms.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Calcaneal fractures (CFs) are rare injuries [1], mainly occurring in middle-aged men [2]. Historically, CFs were called “Lover’s fracture” or “Casanova fracture,” referring to a suitor who sustained this type of fracture after jumping from his inamorata’s balcony to avoid detection [3]. Nowadays, the most common etiology remains the direct axial force due to a fall from height [1]. Calcaneal fractures can have devastating consequences for the patient and cause long-term disability with a high socio-economic burden [4].
While there is an ongoing debate about whether CFs should be treated operatively or conservatively, some data suggest that operative treatment yields better results [5,6,7,8,9]. Open reduction and internal fixation with direct visualization of the fracture appears to be the “gold standard” [10]. The treatment aims to restore calcaneal width, height, shape, and alignment. The Böhler angle, defined by two lines tangent to the calcaneus anterior and superior aspect, ranges between 20 and 40° in healthy subjects [11]. The Böhler angle correlates with the severity of a CF, and its restoration is vital for the outcome [12].
Wound healing disorders are amongst the most common and feared complications after open surgery, with a prevalence of 1.3% for deep and up to 27% for superficial infections [13, 14]. Important risk factors are a high BMI, smoking, diabetes, and the severity of the fracture [15, 16]. Consequently, several techniques were developed to minimize the operative trauma and reduce the size of the wound to lower postoperative complications. Amongst these are minimally invasive approaches like the sinus tarsi approach, arthroscopically-assisted reduction and fixation, or percutaneous techniques like intramedullary nailing [17,18,19,20].
The first calcaneal intramedullary nail was implanted in 1882 by Dr. Gussenbauer, but the concept was abandoned until Goldzak et al. introduced an intramedullary nail for CFs in 2012 [21]. The goal was to find a treatment alternative with less soft tissue damage. In a prospective study, Simon et al. published results from 69 patients treated with the Calcanail® (FH Orthopedics, Heimsbrunn, France), yielding promising results [22]. Another implant, the C-Nail® (Medin, Nov. Město n. Moravě, Czech Republic), was introduced by Zwipp et al. in 2016 and showed good results in a multicenter study involving 106 patients yielding a mean AOFAS score of 89.5 6 months postoperatively [23]. Both Calcanail® and C-Nail® proved to be at least equally strong as the locking plate in a cadaveric biomechanical study [24]. Although Calcanail® and C-Nail® share similarities in their design, the implants achieve reduction and fixation through different mechanisms. While the Calcanail® is stabilized by two screws and relies on indirect reduction of the posterior facet, the C-Nail® requires direct visualization of the joint space through a sinus tarsi approach and several multi-directional screws [25]. There is still no clarity on whether the locking plate or intramedullary nailing is superior [26].
In 2019, Fourgeaux et al. and Herlyn et al. published functional outcomes of CFs treated with the Calcanail® implant. Fourgeaux et al. investigated 26 patients with a mean follow-up of 33 months. The fracture severity was balanced, with 46% having a Sanders II and 53% having a Sanders III/IV fracture. The mean AOFAS score was 79, and return to work was achieved after a mean duration of 6.5 months [27]. Herlyn et al. examined 20 patients prospectively with a mean follow-up of 11.3 months, achieving a mean AOFAS score of 71.6. The mean duration for return to work was 15.8 weeks; nine patients could not return to their previous sports activities. Results were matched with historical data of 20 feet treated with a locking plate through an extended lateral approach [28]. Finally, Steinhausen et al. performed a retrospective matched pair analysis of one hundred and one CFs treated with a locking plate or the C-Nail®. Sixty-two percent of patients receiving the C-Nail® had a Sanders IV fracture. The mean AOFAS score was 79.4 after 6 months without differences between the groups. However, there were significantly fewer complications, and patients were earlier able to perform full-weight bearing after receiving the C-Nail®. Finally, the authors suggest a more prolonged follow-up [29].
Most studies investigated the Calcanail® implant [22, 27, 28, 30,31,32], while fewer studies investigated functional outcomes of the C-Nail® implant with a follow-up of only 1 year or even less [23, 26, 29].
To our best knowledge, no data on return to work and return to sports levels is available for the C-Nail® implant, especially in severe (Sanders ≥ III) fractures with a longer follow-up. This study aimed to investigate the functional outcome at mid-terms after treatment of severe CFs using the C-Nail® implant in a cohort with mainly severe fractures.
Methods
Surgical technique
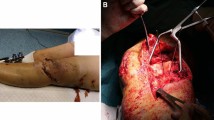
Patients were positioned laterally on the healthy side, and the fractured foot was placed on a soft pad. The posterior joint facet was reconstructed through a sinus tarsi approach, and osteosynthesis was performed with two cancellous screws. After restoration of the joint facet, the C-Nail® implant was introduced percutaneously below the insertion of the Achilles tendon in a posterior-anterior direction after probing with a K-wire. With the help of the three arms of the target instrument, the interlocking screws were placed through the nail, starting with the screw for the sustentaculum tali (Fig. 1a). Passive motion was started on day two postoperatively. On day five, partial weight-bearing was started. After 6 to 8 weeks, full weight-bearing was initiated.
C-Nail® target instrument and exemplary postoperative X-ray. a The sketch of the C-Nail® implant with the target instrument. Image with kind permission from Medin (Nov. Město n. Moravě, Czech Republic). b An exemplary postoperative X-ray. Here, two screws were placed through a sinus tarsi approach and four locking screws were placed through the nail. A drain was inserted at the sinus tarsi incision
Study design
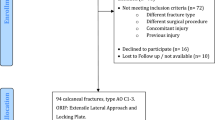
The C-Nail® implant was introduced in our department in 2016. Between 2016 and 2019, 43 CFs were treated using the C-Nail® implant. Three patients presented with bilateral CFs. After receiving IRB approval, all 40 patients were contacted and invited to a follow-up exam. One patient suffered from dementia and was thus not able to consent to participate; one patient refused participation. Seventeen patients were lost to follow-up. Finally, 22 CFs were examined (Fig. 2). The final population contained 20% women and 80% men.
Follow-up examination
Mean follow-up took part 36 months (± 11) post-surgery. Patients were asked to fill out the AOFAS score [33] and a self-constructed questionnaire for patient-reported outcome measures (PROMs), as shown in Table 1. Patients who had bilateral fractures were asked to undergo AOFAS scoring and PROMs individually for both feet.
Radiographic analysis
Preoperative Böhler angles were measured on preoperative lateral view X-rays. Postoperatively, patients received another lateral view X-ray of the fractured calcaneus to determine the postoperative Böhler angle (Fig. 1b). The change in the Böhler angle was used to assess the quality of the reduction.
Statistical analysis
Statistical analysis was performed using Prism 10 (GraphPad Software Inc., Boston, USA). Spearman’s correlations were calculated between the AOFAS score and the PROMs; correlation coefficients higher than r = 0.4 were interpreted as “moderate,” and coefficients higher than 0.7 were interpreted as “strong” [34].
Results
Twenty-two patients (5 female, 17 male) were included with a mean follow-up of 36 months (± 11). In seven patients (32%), the fracture was work-related. The mean age at injury was 51.2 years (± 10.2). Patient distribution according to the Sanders classification is shown in Fig. 3. Seventy-seven percent of the patients sustained a severe fracture (Type III/IV).
Studied population according to Sanders’s classification. Twenty-two calcaneal fractures were followed up. However, three CT scans were unretrievable. Most fractures (17/22 = 72%) presented a severe (Sanders III/IV) pattern. The letters (“A,” “B,” “AB,” “AC,” “BC”) inside the bars show the subgroup classification
The mean AOFAS score was 72.0 (± 9.8) at follow-up. The mean Böhler angle changed from 12.7° (± 9.5) preoperatively to 28.0° (± 6.3) postoperatively. Table 2 lists the recorded complications. While four (18.2%) wound-healing disorders occurred, no implant-associated surgical revision occurred.
Table 3 shows the number of patients being pain-free at certain times. Table 4 depicts the patients being able to perform full weight-bearing in relation to time. Tables 5 and 6 show the number of patients being able to return to sports and work at certain times, respectively.
There was a moderate positive correlation (r = 0.63, p = 0.003) between the time needed to return to full-weight bearing and the time required to return to work. Besides, there was a moderate negative correlation (r = − 0.55, p = 0.01) between the AOFAS score and the time needed to return to full-weight bearing. There was also a moderate negative correlation (r = − 0.62, p = 0.003) between the AOFAS score and the time needed to be pain free.
Discussion
This study examined 22 CFs treated with the C-Nail® implant for a mean follow-up of 36 (± 11) months. The mean AOFAS score was 72.0 (± 9.8). Fifty percent of patients were pain-free within 1 year. Also, within 1 year, 80% of patients could perform full weight-bearing and return to work. Finally, more than half of the patients could return to sports.
In our cohort, several complications occurred. Four patients sustained wound healing disorders, which is important since the minimally-invasive approach was developed to minimize soft tissue damage, wound healing disorders, and infections. Two patients required surgical revision: One patient presented with an open CF that required a single-stage debridement and lavage with implant retainment. The second patient was multi-morbid and needed a revision for a preexisting chronic decubitus at the heel. The two other wound-healing disorders did not require surgical revision. All wound healing disorders were thus classified as “non-implant associated” and did not occur at the site of the incisions. Finally, six patients reported local skin irritations like reddening or itching, which all eventually resolved. No other notable complications occurred. In the literature, equally low rates of wound healing disorders in minimally invasive calcaneal surgery range between 1.9 and 5.2% [23, 26,27,28, 31]. These low numbers support the use of minimally invasive approaches to minimize wound healing disorders and infections, especially as infection rates can be as high as 24.6% using the conventional far lateral approach [35]. Other reported complications for the Calcanail® and C-Nail® include regional pain syndromes or nerve entrapments and osteomyelitis [36]. None of these was recorded in our population.
The outcome after ankle and heel surgery can be objectified using the AOFAS score [33]. Our patients reported a mean score of 72.0 (± 9.8) at 36 months. Apart from Herlyn et al., who reported a mean score of 71.6 [28], scores in the literature are higher, ranging from 79 [27] to 92.6 [23]. Possible explanations for the lower AOFAS score in our population are the high rate of severe fractures, which usually present worse outcomes. While our cohort contained 77% Sanders III/IV fractures, the cohort studied by Zwipp et al. contained only 31% Sanders III/IV fractures [23]. Besides, some patients might have started to develop subtalar osteoarthritis after 36 months. However, this was not quantified as patients did not receive X-rays or further imaging routinely at follow-up.
Restoration of the Böhler angle is of paramount importance. In this study, the mean Böhler angle changed from 12.7° (± 9.5) preoperatively to 28.0° (± 6.3) postoperatively. This aligns with results published in the literature where preoperative angles range between − 3 and 14° and postoperative angles range between 20 and 33.3° [22, 23, 26,27,28, 31]. This shows that the procedure using the C-Nail® can restore the joint facet.
Functional outcome, apart from the AOFAS score, is heterogeneously reported in the literature. Fourgeaux et al. reported a mean duration of 6.5 months for the ability to return to work [27], while patients reported by Herlyn et al. only needed 15.8 weeks on average [28]. In our study, return to work levels is reported in time intervals, especially since patients could not remember the exact dates due to the long follow-up. Thus, a direct comparison is not possible. However, at 6 months, only 40.9% of patients returned to work; thus, the mean duration was possibly longer in our population. A possible explanation is the higher severity of fractures in our cohort. Concerning return to sports levels, overall available data is scarce. Herlyn et al. reported that 47% of patients could not return to pre-injury sports levels. In our cohort, only 27.3% could not return to sports activities. Obviously, due to different lengths of follow-up, those results are not comparable. However, Herlyn et al. had a follow-up of 11.3 months, and at this point in time, 54.4% of our patients were already able to return to sports. This contrasts with overall lower AOFAS scores reported by our patients.
Using other minimally invasive approaches, equally high functional levels are achievable. Bischofreiter et al. investigated the functional outcome of 49 patients that received minimally invasive stabilization of CFs using only screws in a technique described by Mattiassich et al. [19]. The studied population consisted of 35% Sanders III/IV fractures. The overall return to sport rate was almost 80% [37].
This study has several limitations: It was a retrospective, singe-center study and patients were operated by only one surgeon. Besides, there was no imaging at follow-up. Furthermore, out of 40 screened CFs, 17 were lost to follow-up, and only 22 were finally included in the analysis. However, this number is even slightly higher than in the study on the C-Nail® implant from Zeman et al. [26]. A major strength of the present study is that the mean follow-up is longer than in most comparable studies using the Calcanail® and C-Nail® [22, 23, 26,27,28,29,30,31].
Conclusion
Intramedullary nailing using the C-Nail® implant for severe CFs results in acceptable functional outcomes at mid-terms.
Data availability
The data that support the findings of this study are available from the corresponding author, PS, upon reasonable request.
References
Mitchell MJ, McKinley JC, Robinson CM. The epidemiology of calcaneal fractures. Foot. 2009;19:197–200.
Ribeiro EJC, Beletato RM, Prata SD, Rizzo MA. PO 18117 - Epidemiological study of calcaneal fractures. Sci J Foot Ankle. 2019;13:17S-17S.
García BEC, González EMG, Vinces KLB, Cajamarca JXL, Moreno APG, Campoverde MPC, et al. Calcaneal fracture, epidemiology, anatomy, mechanism of injury, classification, imaging presentation, clinical presentation, management and complications. EPRA Int J Multidiscip Res (IJMR). 2023;197–204.
Brauer CA, Manns BJ, Ko M, Donaldson C, Buckley R. An economic evaluation of operative compared with nonoperative management of displaced intra-articular calcaneal fractures. J Bone Jt Surg. 2005;87:2741–9.
Sanders R. Displaced intra-articular fractures of the calcaneus*. J Bone Jt Surg-Am. 2000;82:225–50.
Gougoulias N, Khanna A, McBride DJ, Maffulli N. Management of calcaneal fractures: systematic review of randomized trials. Br Méd Bull. 2009;92:153–67.
Kamath KR, Mallya S, Hegde A. A comparative study of operative and conservative treatment of intraarticular displaced calcaneal fractures. Sci Rep. 2021;11:3946.
Baliga S, Sutherland A, Bruce J. Surgical versus conservative interventions for displaced intra‐articular calcaneal fractures. Cochrane Database Syst Rev. 2010.
Fischer S, Meinert M, Neun O, Colcuc C, Gramlich Y, Hoffmann R, et al. Surgical experience as a decisive factor for the outcome of calcaneal fractures using locking compression plate: results of 3 years. Arch Orthop Trauma Surg. 2021;141:1691–9.
Guerado E, Bertrand ML, Cano JR. Management of calcaneal fractures: what have we learnt over the years? Injury. 2012;43:1640–50.
Keener BJ, Sizensky JA. The anatomy of the calcaneus and surrounding structures. Foot Ankle Clin. 2005;10:413–24.
Razik A, Harris M, Trompeter A. Calcaneal fractures: where are we now? Strat Trauma Limb Reconstr. 2018;13:1–11.
Al-Mudhaffar M, Prasad CVR, Mofidi A. Wound complications following operative fixation of calcaneal fractures. Injury. 2000;31:461–4.
Lim EVA, Leung JPF. Complications of intraarticular calcaneal fractures. Clin Orthop Relat Res. 2001;391:7–16.
Zhang W, Chen E, Xue D, Yin H, Pan Z. Risk factors for wound complications of closed calcaneal fractures after surgery: a systematic review and meta-analysis. Scand J Trauma, Resusc Emerg Med. 2015;23:18.
Su J, Cao X. Risk factors of wound infection after open reduction and internal fixation of calcaneal fractures. Medicine. 2017;96:e8411.
Rammelt S, Amlang M, Barthel S, Zwipp H. Minimally-invasive treatment of calcaneal fractures. Injury. 2004;35:55–63.
Gavlik J, Rammelt S, Zwipp H. Percutaneous, arthroscopically-assisted osteosynthesis of calcaneus fractures. Arch Orthop Trauma Surg. 2002;122:424–8.
Tornetta P. Percutaneous treatment of calcaneal fractures. Clin Orthop Relat Res. 2000;375:91–6.
Giannini S, Cadossi M, Mosca M, Tedesco G, Sambri A, Terrando S, et al. Minimally-invasive treatment of calcaneal fractures: a review of the literature and our experience. Injury. 2016;47:S138–46.
Goldzak M, Mittlmeier T, Simon P. Locked nailing for the treatment of displaced articular fractures of the calcaneus: description of a new procedure with calcanail®. Eur J Orthop Surg Traumatol. 2012;22:345–9.
Simon P, Goldzak M, Eschler A, Mittlmeier T. Reduction and internal fixation of displaced intra-articular calcaneal fractures with a locking nail: a prospective study of sixty nine cases. Int Orthop. 2015;39:2061–7.
Zwipp H, Paša L, ilka L, Amlang M, Rammelt S, Pompach M. Introduction of a new locking nail for treatment of intraarticular calcaneal fractures. J Orthop Trauma. 2016;30:e88–92.
Reinhardt S, Martin H, Ulmar B, Döbele S, Zwipp H, Rammelt S, et al. Interlocking nailing versus interlocking plating in intra-articular calcaneal fractures: a biomechanical study. Foot ankle Int. 2016;37:891–7.
Tarulli FR, Bernasconi A, Izzo A, Coviello A, Smeraglia F, Balato G, et al. Intramedullary nailing for calcaneal fractures: what are the available techniques? A review of the literature. Lo Scalpello - Otodi Educ. 2022;36:159–64.
Zeman J, Zeman P, Matejka T, Belatka J, Matejka J. Comparison of LCP and intramedullary nail osteosynthesis in calcaneal fractures. Acta Ortopédica Bras. 2019;27:288–93.
Fourgeaux A, Estens J, Fabre T, Laffenetre O, Hernandez JL y. Three-dimensional computed tomography analysis and functional results of calcaneal fractures treated by an intramedullary nail. Int Orthop. 2019;43:2839–47.
Herlyn A, Brakelmann A, Herlyn PK, Gradl G, Mittlmeier T. Calcaneal fracture fixation using a new interlocking nail reduces complications compared to standard locking plates – preliminary results after 1.6 years. Injury. 2019;50:63–8.
Steinhausen E, Martin W, Lefering R, Lundin S, Glombitza M, Mester B, et al. C-Nail versus plate osteosynthesis in displaced intra-articular calcaneal fractures—a comparative retrospective study. J Orthop Surg Res. 2021;16:203.
Falis M, Pyszel K. Treatment of displaced intra-articular calcaneal fractures by intramedullary nail. Preliminary report Ortop Traumatol Rehabil. 2016;18:141–7.
Fascione F, Mauro MD, Guelfi M, Malagelada F, Pantalone A, Salini V. Surgical treatment of displaced intraarticular calcaneal fractures by a minimally invasive technique using a locking nail: a preliminary study. Foot Ankle Surg. 2019;25:679–83.
Saß M, Rotter R, Mittlmeier T. Minimally invasive internal fixation of calcaneal fractures or subtalar joint arthrodesis using the Calcanail®. Oper Orthop Traumatol. 2019;31:149–64.
Schepers T, Heetveld MJ, Mulder PGH, Patka P. Clinical outcome scoring of intra-articular calcaneal fractures. J Foot Ankle Surg. 2008;47:213–8.
Schober P, Boer C, Schwarte LA. Correlation coefficients. Anesthesia. Analgesia. 2018;126:1763–8.
Backes M, Schepers T, Beerekamp MSH, Luitse JSK, Goslings JC, Schep NWL. Wound infections following open reduction and internal fixation of calcaneal fractures with an extended lateral approach. Int Orthop. 2014;38:767–73.
Bernasconi A, Iorio P, Ghani Y, Argyropoulos M, Patel S, Barg A, et al. Use of intramedullary locking nail for displaced intraarticular fractures of the calcaneus: what is the evidence? Arch Orthop Trauma Surg. 2022;142:1911–22.
Bischofreiter M, Litzlbauer W, Breulmann F, Kindermann H, Rodemund C, Mattiassich G. Return-to-sports after minimally invasive stabilization of intra-articular calcaneal fractures. Sportverletz Sportschaden. 2022;36:100–10.
Funding
Open Access funding enabled and organized by Projekt DEAL.
Author information
Authors and Affiliations
Contributions
PS: writing—original draft, data curation.
RE: investigation.
DB: formal analysis.
SF: writing—review and editing.
FW: validation.
YA: investigation.
CA: investigation.
MN: formal analysis.
PD: writing—review and editing.
EG: writing—review and editing.
RK: supervision, project administration, methodology, conceptualization.
Corresponding author
Ethics declarations
Ethics approval and consent to participate
All procedures were performed in accordance with the 1964 Helsinki Declaration and its later amendments. This study was approved by the Institutional Review Board of Rhénanie-Palatinat, Germany (Ethic Committee approval: 2019–14134). Informed consent was obtained from all subjects involved in the study.
Consent for publication
Written informed consent has been obtained from the patients to publish this paper.
Conflict of interest
The authors declare no competing interests.
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if changes were made. The images or other third party material in this article are included in the article's Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article's Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
Schippers, P., Engels, R., Benning, D. et al. Functional outcomes after intramedullary nailing (C-Nail®) of severe calcaneal fractures with mean follow-up of 36 months. Eur J Trauma Emerg Surg 50, 1111–1118 (2024). https://doi.org/10.1007/s00068-023-02433-3
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00068-023-02433-3