Abstract
Purpose
Assessing efficacy of electrical impedance tomography (EIT) in optimizing positive end-expiratory pressure (PEEP) for acute respiratory distress syndrome (ARDS) patients to enhance respiratory system mechanics and prevent ventilator-induced lung injury (VILI), compared to traditional methods.
Methods
We carried out a systematic review and meta-analysis, spanning literature from January 2012 to May 2023, sourced from Scopus, PubMed, MEDLINE (Ovid), Cochrane, and LILACS, evaluated EIT-guided PEEP strategies in ARDS versus conventional methods. Thirteen studies (3 randomized, 10 non-randomized) involving 623 ARDS patients were analyzed using random-effects models for primary outcomes (respiratory mechanics and mechanical power) and secondary outcomes (PaO2/FiO2 ratio, mortality, stays in intensive care unit (ICU), ventilator-free days).
Results
EIT-guided PEEP significantly improved lung compliance (n = 941 cases, mean difference (MD) = 4.33, 95% confidence interval (CI) [2.94, 5.71]), reduced mechanical power (n = 148, MD = − 1.99, 95% CI [− 3.51, − 0.47]), and lowered driving pressure (n = 903, MD = − 1.20, 95% CI [− 2.33, − 0.07]) compared to traditional methods. Sensitivity analysis showed consistent positive effect of EIT-guided PEEP on lung compliance in randomized clinical trials vs. non-randomized studies pooled (MD) = 2.43 (95% CI − 0.39 to 5.26), indicating a trend towards improvement. A reduction in mortality rate (259 patients, relative risk (RR) = 0.64, 95% CI [0.45, 0.91]) was associated with modest improvements in compliance and driving pressure in three studies.
Conclusions
EIT facilitates real-time, individualized PEEP adjustments, improving respiratory system mechanics. Integration of EIT as a guiding tool in mechanical ventilation holds potential benefits in preventing ventilator-induced lung injury. Larger-scale studies are essential to validate and optimize EIT’s clinical utility in ARDS management.
Similar content being viewed by others
Explore related subjects
Discover the latest articles, news and stories from top researchers in related subjects.Avoid common mistakes on your manuscript.
This meta-analysis highlights the electrical impedance tomography (EIT)’s potential in optimizing personalized positive end-expiratory pressure settings for patients with acute respiratory distress syndrome (ARDS), advancing pulmonary function and respiratory system mechanics. The study underscores the need for further integration of EIT into clinical practice to minimize ventilator-induced lung injury, bridging the gap between scientific understanding and practical application in ARDS care |
Introduction
Acute respiratory distress syndrome (ARDS) is a severe pulmonary condition characterized by respiratory failure and a significant mortality rate of 35–45% [1]. Mechanical ventilation is a critical intervention for ARDS patients; however, it may potentially exacerbate lung injury, giving rise to ventilator-induced lung injury (VILI) [2]. This underscores the need for personalized mechanical ventilation strategies to optimize patient outcomes [3]. A key strategy in supporting critically ill patients with ARDS is the application of positive end-expiratory pressure (PEEP), which helps to maintain alveolar recruitment [4,5,6] and improve oxygenation [7]. Nevertheless, the optimal level of PEEP remains the subject of ongoing debate and research [8, 9].
Traditionally, PEEP levels have been selected using conventional strategies, such as the ARDSNet PEEP/FiO2 table, which has become the standard approach for ARDS management [10]. Although various methods have been explored to personalize PEEP, including lung compliance, trans-pulmonary pressure, and inflection points on pressure–volume curves, these approaches do not fully account for the heterogeneous nature of lung disease in ARDS patients and consequently, may not be optimal for all ARDS patients [11]. Recently, electrical impedance tomography (EIT), a non-invasive imaging technique providing real-time regional lung information, has emerged as a promising tool to guide PEEP settings [12] for individualize intervention, potentially leading to improved respiratory mechanics, a crucial determinant of VILI, in patients with ARDS.
Despite the potential benefits of EIT-guided PEEP, its effectiveness compared to conventional methods of PEEP titration remains unclear [11]. To provide a more comprehensive understanding of these approaches and guide clinicians in delivering the best possible care for ARDS patients, we conducted a meta-analysis of randomized trials and observational studies comparing EIT-guided PEEP titration to conventional methods to guide PEEP titration aiming to enable improving respiratory system mechanics and thus the risk of VILI.
Materials and methods
Data sources
We conducted through searches of multiple databases (Scopus, PubMed, MEDLINE through Ovid, Cochrane Central Register of Controlled Trials, and LILACS) spanning from January 2012 to May 1, 2023. Our literature search combined terms (EIT OR “electrical impedance tomography”) AND (ARDS OR “acute respiratory distress syndrome” OR “acute respiratory failure” OR “acute lung injury”) AND (“mechanical ventilat*” OR peep OR “positive end-expiratory pressure” OR recruitment OR “tidal volume”) in titles, abstracts, and keywords. The focus was on human studies from 2012 onwards, with no language restrictions. Additionally, we scrutinized the reference lists of eligible studies to uncover potentially relevant ones.
Study selection
We included randomized controlled trials (RCTs) and non-randomized studies (NRS) involving adult ARDS patients on invasive mechanical ventilation, defined by the Berlin definition [13]. These studies compared EIT-guided PEEP selection with conventional PEEP titration methods and reported at least one primary or secondary outcome of interest. Conventional methods encompassed ARDSNet FiO2/PEEP table [13, 14], pressure–volume (PV) curve analysis, transpulmonary pressure adjustments, or other techniques. Exclusions comprised case reports, case series, conference abstracts, and review articles. Additionally, studies lacking control groups, those not specifically evaluating the impact of EIT-guided PEEP, or employed EIT solely for monitoring purposes were excluded.
Primary outcomes assessed respiratory system mechanics, including lung compliance, driving pressure (DP), plateau pressure, PEEP level, and mechanical power (MP). Secondary outcomes included PaO2/FiO2 ratio, 28-day all-cause mortality, in-hospital mortality, intensive care unit (ICU) lengths of stay, ventilator-free days, and EIT-based lung mechanics as reported by study authors. These EIT metrics included % of Silent Spaces, quantifying hypoventilated lung units, and %COV (coefficient of ventilation), indicating ventilation distribution along a gravitational axis [15,16,17].
Data abstraction and quality assessment
Two review authors (NS, CL) independently screened all titles and abstracts for eligibility. Subsequently, the full texts of the identified studies meeting initial screening criteria were assessed. The same two authors then independently determined eligibility for inclusion in the meta-analysis, with disagreements resolved through discussion or consultation with field experts (LB and HZ).
Data were extracted from included studies using a standardized form, with one author (NS) performing extraction and another author (CL) cross-checking the data. Information included patient characteristics (demographic and clinical), study population, intervention and control PEEP titration strategies, and outcomes (respiratory system mechanics measurements, PaO2/FiO2 ratio, mortality, lengths of stay, and ventilator-free days). We did not seek supplementary data beyond what was publicly available in the published articles.
Two authors (NS, CL) independently assessed the risk of bias (ROB) for each study. The Cochrane ROB-2 tool was used to for RCTs [18], while the Risk Of Bias In Non-randomized Studies-of Interventions (ROBINS-I) tool was applied to NRS [19]. ROB was categorized as low, of some concern, or high, with disagreements resolved through consensus.
Data synthesis
Random-effects models were employed to pool data in Review Manager Web [20]. We chose this model to account for potential variability across studies. This includes differences in study designs, patient populations, and interventions. Risk ratio (RR) for dichotomous outcomes and mean difference (MD) for continuous outcomes were reported, with 95% confidence intervals (CIs). Median and interquartile range data were converted to estimated mean and standard deviation where necessary [21]. A two-sided p value ≤ 0.05 indicated statistical significance.
Statistical heterogeneity was assessed using the Chi-square test (p value ≤ 0.1 considered significant) and I2 statistic (0–40% not important, 30–60% moderate heterogeneity, 50–90% substantial heterogeneity, 75–100% considerable heterogeneity) [22]. Potential publication bias was evaluated using Egger’s test and funnel plots in Stata when ≥ 10 studies were identified [23].
Sensitivity and subgroup analyses
Sensitivity analyses gauged the impact of RCT quality, high ROB, use of recruitment maneuvers before PEEP titration, studies with significant positive treatment effect, obese versus non-obese patients, ODCL method versus conventional method, EIT-guided PEEP versus ARDSNet PEEP/FiO2 table, and ODCL method versus ARDSNet PEEP/FiO2 table. Subgroup analyses were performed to investigate the sources of heterogeneity in the outcomes. These analyses were restricted to outcomes that were reported in a substantial number of studies, specifically those with a minimum of 10 studies contributing data. Aligning with our criteria of heterogeneity, we directed our subgroup analyses toward instances characterized by ‘substantial heterogeneity’ (I2 values ranging from 50 to 90%) and ‘considerable heterogeneity’ (I2 values between 75% and 100%). Subgroup analyses were conducted based on participant characteristics (age, body mass index, cause of ARDS, coronavirus disease 2019 (COVID-19), ARDS severity, duration of mechanical ventilation before data collection, duration of mechanical ventilation before inclusion) and interventions across studies (tidal volume, recruitment maneuver, incremental/decremental PEEP, conventional intervention, EIT intervention). Subgroup effects were assessed using the Chi-square test of heterogeneity (p value ≤ 0.1 indicating significance). Considerations included the number of trials and participants per subgroup, interaction plausibility, interaction importance, and potential confounding, guiding the decision to present or omit the subgroup analyses [22].
Results
Study identification
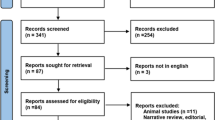
The search identified 421 records with 243 unique citations after removing duplicates. Of these, we excluded 218 records that did not meet eligibility criteria. We retrieved 25 full-text articles for closer review and excluded 12 studies that evaluated EIT monitoring [15, 24,25,26,27], included non-ARDS patients [28,29,30], had no control group [31, 32], or were letters with insufficient data [33, 34]. Consequently, we included 13 studies (n = 623 patients) in the analysis [35,36,37,38,39,40,41,42,43,44,45,46,47] (Fig. 1).
Study selection process diagram: Initially, 421 records were identified, which were then deduplicated to yield 243 unique citations. Subsequently, 218 records were excluded based on eligibility criteria. Following a comprehensive review of 25 full-text articles, an additional 12 studies were excluded based on specific criteria. This resulted in 13 studies that met the inclusion criteria and were included in the analysis
Characteristics of the included studies
Of the 13 included studies, 3 were RCTs, and 10 were non-randomized studies. Four studies specifically included patients with COVID-19-related ARDS. The average age of participants in the included studies ranged from 41 to 70 years. The average baseline PaO2/FiO2 ratio in 12 studies [35,36,37,38,39,40,41,42,43,44, 46, 47] was within the moderate ARDS range with only one study [45] reporting an average baseline PaO2/FiO2 ratio of 70 mmHg. One study [39] included patients on extracorporeal membrane oxygenation (ECMO). Although 2 studies reported average body mass index (BMI) within the normal range, 6 studies reported BMI within the overweight range and 5 studies within the obesity range. All participants in the included studies received sedation and neuromuscular blocking agents. Tidal volume administration varied across the studies. Ten studies [36,37,38, 41,42,43,44,45,46,47] utilized tidal volumes ranging from 6 to 8 ml/kg predicted body weight (PBW), while 2 studies [35, 40] used tidal volumes of 4–6 ml/kg PBW. Additionally, 1 study [39] utilized tidal volumes of 3–4 ml/kg PBW (Table 1).
In the control groups of the included trials, PEEP was titrated using PEEP/FiO2 tables in 7 studies [36,37,38, 41,42,43, 47], PV curves in 2 studies [40, 45], end-expiratory transpulmonary sliding table in 2 studies [42, 44], and physician-set PEEP or clinical PEEP in 3 studies [35, 39, 46].
In the intervention group, PEEP titration was guided by EIT. Eight studies [35,36,37, 39,40,41, 45, 46] used the intercept point of cumulated collapse and overdistension percentages curves by Costa et al. to guide PEEP titration [12], while the remaining 5 studies utilized various techniques including total percentage of collapse and distension [42, 44], global inhomogeneity (GI) index [38], regional compliance [43], and end-expiratory lung impedance (EELI) techniques [47]. Seven studies [35,36,37, 39, 43, 46, 47] performed a recruitment maneuver before PEEP titration, while the remaining six studies [38, 40,41,42, 44, 45] did not. The EIT belt was placed in the 4–5th intercostal space in 9 studies [35,36,37, 39,40,41, 44,45,46], in the 5–6th intercostal space in 1 study [47], and was not reported in 3 studies [38, 42, 43]. The position of the patient was reported in 9 studies [35,36,37,38,39,40,41,42, 44], with all patients in the supine position.
Risk of bias in included studies
The overall risk of bias was (supplemental Figures E1 and E2) judge to some concern. Notably, the main concern revolves around the potential bias due to confounding factors.
Primary outcomes
The pooled results of 12 studies indicated that compared to conventional methods, EIT-guided PEEP significantly increased lung compliance (n = 941 analyzed cases, MD = 4.33, 95% CI [2.94, 5.71], P < 0.00001, and I2 = 0%) (Fig. 2). EIT-guided (vs. conventional) PEEP titration significantly decreased mechanical power (n = 148 analyzed cases, MD = − 1.99, 95% CI [− 3.51, − 0.47], P = 0.01, and I2 = 0%) and DP (n = 903 analyzed cases, MD = − 1.20, 95% CI [− 2.33, − 0.07], P = 0.04, and I2 = 89%) (Figs. 3 and 4). However, there were no statistically significant differences between PEEP titration techniques regarding plateau pressure and PEEP level amidst significant heterogeneity (supplemental Figure E3 and E4).
Secondary outcomes
Three studies [40, 41, 45] (n = 259 patients) provided mortality data. The meta-analysis of all-cause hospital mortality, based on two studies (n = 142) with 62 deaths, revealed a pooled relative risk (RR) of 0.59 (95% CI [0.39, 0.89], P = 0.01, and I2 = 0%). Only 1 study [41] (n = 117) with 28 deaths reported all-cause mortality within 28 days, yielded a RR of 0.80 (95% CI [0.42, 1.52], P = 0.49). Post-hoc, pooling of the most protracted mortality (the combined overall effect estimates of both outcomes) including 259 patients and 90 deaths revealed a RR of 0.64, 95% CI [0.45, 0.91], P = 0.01, and I2 = 0% (supplemental Figure E5). Within these three studies, a trend towards higher lung compliance was noted, with one study demonstrating a significant improvement [45]. Concerning DP, two studies indicated a significant reduction [40, 45], while one study found no difference.
EIT-guided (vs. conventional) PEEP titration significantly reduced the % of silent spaces. (MD = − 5.23, 95% CI [− 8.72, − 1.74], P = 0.003, and I2 = 5%) (supplemental Figure E6). However, the effect of EIT-guided PEEP on PaO2/FiO2 ratio, lengths of ICU stay, and % COV was not significantly different from conventional methods, and heterogeneity was observed in the forest plot (supplemental Figures E7–E9). One study each reported ventilator-free days at day 28 [41] and duration of ventilation [40] with nonsignificant between group differences.
Sensitivity and subgroup analyses
Sensitivity analysis of RCTs (vs NRS) consistently demonstrated a positive effect of EIT-guided PEEP on lung compliance, with the pooled (MD) of 2.43 (95% CI − 0.39 to 5.26), indicating a trend towards improvement, but with some uncertainty in the estimate (Fig. 2). To further assess the robustness of these findings, additional analyses were conducted: excluding studies with high risk of bias affirmed the consistency of the treatment effect (MD = 4.01, 95% CI [2.45, 5.57], P < 0.00001, and I2 = 0%), enhancing confidence in the results (Fig. 5a); isolating the impact of EIT-guided PEEP from potential confounders by excluding studies with recruitment maneuver before PEEP trials still showed a positive trend (MD = 3.85, 95% CI [1.95, 5.75], P < 0.0001, and I2 = 0%), thereby reinforcing the direct impact of EIT-guided PEEP on lung compliance (Fig. 5b); and removing studies with significant positive treatment effects revealed that the overall positive trend was not driven solely by a few outlier studies, as the impact on lung compliance remained consistently positive and statistically significant (MD = 2.86, 95% CI [0.95, 4.78], P = 0.003, and I2 = 0%) (Fig. 5c). We performed a sensitivity analysis for obese patient subgroup to test the hypothesis that EIT-guided PEEP might be particularly advantageous for this specific subgroup due to their distinct respiratory challenges, such as lung atelectasis, nonhomogeneous ventilation, and an increased risk of VILI. However, our results demonstrated that EIT-guided PEEP improves respiratory system compliance in both obese (MD = 5.27, 95% CI [3.22, 7.33], P < 0.00001, and I2 = 0%) and non-obese patients (MD = 3.54, 95% CI [1.66, 5.41], P = 0.0002, and I2 = 0%), compare with conventional PEEP methods (Fig. 5d). We conducted a thorough examination comparing different PEEP titration strategies: ODCL method versus conventional method, EIT-guided PEEP versus ARDSNet PEEP/FiO2 table, and ODCL method versus ARDSNet PEEP/FiO2 table. In comparing ODCL method to conventional method, we observed MD in lung compliance of 4.62 (95% CI [3.10, 6.14], P < 0.00001, and I2 = 0%) (Fig. 5e). Similarly, when comparing EIT-guided PEEP to the ARDSNet PEEP/FiO2 table, MD was 3.17 (95% CI [0.76, 5.58], P = 0.01, and I2 = 0%) (Fig. 5f). Finally, the comparison between ODCL method and ARDSNet PEEP/FiO2 table resulted in MD of 3.58 (95% CI [0.23, 6.93], P = 0.04, and I2 = 0%) (Fig. 5g). These analyses, with their respective statistical metrics, highlighted consistent trends in lung compliance outcomes across different methods, demonstrating the robustness and consistency of our findings. Furthermore, we did sensitivity analysis for DP by excluding studies with high risk of bias and those using tidal volume less than 6. Excluding the high risk of bias study altered the MD to − 0.96 (95% CI [− 2.12, 0.19], P = 0.10, I2 = 89%) (supplemental Figure E10), and after removing studies using tidal volumes less than 6 changed the statistics to MD − 0.82 (95% CI [− 1.63, − 0.02], P = 0.04, I2 = 61%) (supplemental Figure E11).
Forest plots of sensitivity analysis for lung compliance: a Excluding studies with high risk of bias, b excluding studies with recruitment maneuver before PEEP, c excluding studies with significant positive treatment effect, d obese and non-obese patients, e ODCL method versus conventional method, f EIT-guided PEEP versus ARDSNet PEEP/FiO2 table, g ODCL method versus ARDSNet PEEP/FiO2 table. RM recruitment maneuver, BMI body mass index, ODCL intercept point of cumulated collapse and overdistension percentages curves, CI confidence interval, df degrees of freedom, I2 heterogeneity statistic, IV inverse variance method
For DP, there was a statistically significant subgroup effect observed in the severity of ARDS, incremental/decremental PEEP, and conventional intervention (supplemental Table E1). Regarding PEEP, there was a statistically significant subgroup effect observed in cause of ARDS, the severity of ARDS, recruitment maneuver before PEEP trial, and conventional and EIT interventions. For PaO2/FiO2 ratio, there was a statistically significant subgroup effect observed in recruitment maneuver before PEEP trial and EIT intervention. Notwithstanding, covariates were unevenly distributed across subgroups, indicating that the subgroup analysis might not produce valid results. However, the covariate distribution was not concerning for the comparison of EIT (vs. conventional)-guided PEEP in PaO2/FiO2 ratio classified in the presence and absence of a recruitment maneuver. Although EIT (vs conventional) PEEP titration had a significantly higher PaO2/FiO2 ratio, there was moderate between trial heterogeneity within the recruitment maneuver subgroup, resulting in uncertainty regarding the validity of the treatment effect estimate.
Publication bias
The Egger’s test yielded a non-significant p value of 0.26, suggesting the absence of publication bias. Inspection of the contour-enhanced funnel plot analysis, our findings suggest a mixed pattern of study results with regard to lung compliance. Some studies demonstrated significant positive treatment effects with higher compliance, while others showed non-significant effects with potentially varied compliance levels. The absence of significant publication bias, as indicated by the Egger’s regression test, lends support to the validity of our results (Supplemental Figure E12).
Discussion
In this meta-analysis, we noted a significant enhancement in lung compliance and a reduction in mechanical power when employing EIT-guided PEEP titration compared to conventional methods. These effects were observed in the absence of heterogeneity. Additionally, a noteworthy reduction in DP was identified, despite the presence of substantial heterogeneity.
In the pooled analysis, patients afflicted with ARDS, who received optimized PEEP adjustments guided by EIT, exhibited elevated lung compliance compared to those whose PEEP was titrated using conventional methods. This augmentation in compliance is noteworthy, as it signifies an enhanced recruitment of lung tissue and the potential mitigation of lung overdistension. This finding aligns with the underlying physiological rationale of real-time monitoring of EIT which enables personalized adjustments of PEEP based on the localized distribution of lung ventilation [48,49,50]. As such, the capacity of EIT to visualize ventilation distribution within distinct lung regions facilitates data-driven insights into PEEP titration and ventilator management. Specifically, EIT enables quantification of lung inhomogeneity, analysis of regional and global ventilation patterns, and identification of potentially recruitable lung areas [31, 51, 52].
Recent investigations have demonstrated the feasibility of employing EIT-guided PEEP titration in ARDS patients [25, 53]. To this end, Franchineau et al. have shown the feasibility and additional support provided by EIT-driven PEEP titration, even in severe ARDS patients undergoing ECMO. The strategies for EIT-guided PEEP titration involved various approaches, including the assessment of overdistension and collapse through regional compliance analysis, the trend of EELI identifying the point of significant EELI reduction as an indicator of lung volume loss, the determination of minimum GI index quantifying homogeneity of ventilation distribution across the lung, and regional compliance assessment. The main goal of utilizing these diverse approaches is to strike a harmonious balance between lung recruitment and the prevention of overdistension. According to a recent study by Jonkman et al. [35], EIT demonstrates notable advantages in guiding PEEP selection for ARDS patients. It furnishes essential information beyond the scope of targeting the highest compliance during PEEP trials. Therefore, EIT-guided PEEP may present greater precision and safety compared to the approach of optimizing for the best compliance.
Although there was a lack of difference in the level PEEP obtained with the EIT and conventional approaches observed in the inhomogeneous population, it is worth note that EIT-derived PEEP strategies have reduced MP [36] and DP [40], with lowered PEEP levels compared to conventional PEEP methods in the RCTs. The potential clinical significance of EIT-derived PEEP strategies, particularly in specific subgroups underlines the importance of considering not only the overall population but also subgroup analyses to elucidate the impact of EIT-derived strategies on PEEP and its implications for VILI-related variables. Our findings related to reduced MP, and to a lesser extent DP, provide support for the assertion that EIT-guided PEEP optimization holds promise for advancing lung-protective ventilation strategies. It is postulated that curtailing MP and DP might confer potential survival advantages in individuals grappling with ARDS [54,55,56,57,58,59].
Several additional findings from our study warrant commentary. First, the attenuation in the percentage of silent spaces favoring EIT-guided PEEP titration harmonizes with the overarching concept of curtailing lung collapse and areas prone to overdistension. This dynamic contributes to an ameliorated gas exchange capacity and a mitigated risk for VILI. However, it is noteworthy to acknowledge that our conclusions regarding silent spaces stem from a limited number of studies with a relatively small sample size, which inherently imposes constraints on the robustness of this finding. Second, we did not find effects between PEEP titration strategies on secondary endpoints, including PaO2/FiO2 ratio, ICU stay, and %COV. These findings suggest that while the optimization of PEEP guided by EIT may exert an effect on respiratory system mechanic parameters, its ramifications on other clinical indicators may be limited and were variably reported. Nevertheless, we did note a reduction in all-cause mortality rate may coincide with improvements in compliance and DP driving across three studies. Due to the limited sample size, limited inferences can be made regarding the impact of the alternative PEEP titration strategies on mortality. It is worth noting that recent studies suggest that lowering DP might provide patients potential survival benefits [1, 54, 59, 60].
Our meta-analysis distinguishes itself from the study conducted by Yu M et al. [61], through several key differences. Specifically, we opted to exclude four studies that were encompassed in the prior meta-analysis for specific reasons: (1) Weber [30]—this study was omitted because it concentrated on patients undergoing general anesthesia for otorhinolaryngeal surgery. This deviation from our study criteria, which focuses on adult ARDS patients on invasive mechanical ventilation as defined by the Berlin definition, led to its exclusion. (2) Karsten [29]—exclusion of this study was warranted as it involved patients with mild-to-moderate impairment of oxygenation. This variance in patient characteristics did not align with our targeted population of adult ARDS patients. (3) Jacopo Fumagalli [26]—we chose to exclude this study since it utilized EIT to assess the effects of PEEP titration strategies, rather than focusing on PEEP titration per our analysis criteria. (4) Becher [62]—given that this was a meeting abstract with insufficient data for inclusion in our paper, we opted not to incorporate it into our meta-analysis. These exclusions were made to ensure the alignment of our study criteria with the specific parameters outlined in the Berlin definition for adult ARDS patients on invasive mechanical ventilation.
Our study exhibits notable strengths. The inclusion of ARDS patients with diverse demographics and etiologies enhances the generalizability of our findings to heterogeneous patient cohorts. The sensitivity analysis reinforces the positive impact of EIT-guided PEEP titration on respiratory system mechanics, thereby emphasizing its potential as a promising area for future investigation. The absence of significant bias and publication bias further underscores the reliability and trustworthiness of our conclusions.
Our study is not without limitations. First, beyond the analyses related to lung compliance and mechanical power, heterogeneity persisted due to variations in participant characteristics (such as age, BMI, etiology of ARDS, baseline PaO2/FiO2 ratio, and duration of mechanical ventilation before inclusion) and interventions (including intervention methods, tidal volume, recruitment maneuver before PEEP trial, and incremental/decremental PEEP) among the included studies. This diversity restricts the extent of inferences that can be drawn from the collective results. The differences in conventional methods within the control group and the varied EIT-guided PEEP titration techniques employed in the intervention group contribute to this inter-study variation.
Second, our findings regarding the impact of EIT-guided PEEP on mechanical power are constrained by the small sample size. Third, variability in reporting outcomes limited our ability to pool data effectively. Lastly, we acknowledge that we did not assess the certainty of our findings through the grading of recommendations, assessment, development, and evaluations.
In conclusion, our systematic review and meta-analysis provide evidence endorsing the effectiveness of EIT-guided mechanical ventilation in ARDS. The real-time lung function assessment facilitated by EIT allows for personalized PEEP settings, resulting in enhanced lung compliance while concurrently reducing MP and DP. For future research, large-scale RCTs are warranted to validate these findings, with a particular focus on clinical outcomes such as mortality rate, the duration of mechanical ventilation, and overall ICU stay. Moreover, a critical need exists for standardizing EIT methodology for PEEP titration to ensure consistency in application and interpretation across studies.
Availability of data and materials
Availability of data and materials does not apply.
References
Bellani G, Laffey JG, Pham T, Fan E, Brochard L, Esteban A et al (2016) Epidemiology, patterns of care, and mortality for patients with acute respiratory distress syndrome in intensive care units in 50 countries. JAMA 315(8):788–800
Slutsky AS, Ranieri VM (2013) Ventilator-induced lung injury. N Engl J Med 369(22):2126–2136
Pelosi P, Ball L, Barbas CSV, Bellomo R, Burns KEA, Einav S et al (2021) Personalized mechanical ventilation in acute respiratory distress syndrome. Crit Care 25(1):250
Cipulli F, Vasques F, Duscio E, Romitti F, Quintel M, Gattinoni L (2018) Atelectrauma or volutrauma: the dilemma. J Thorac Dis 10(3):1258–1264
Gattinoni L, Caironi P, Cressoni M, Chiumello D, Ranieri VM, Quintel M et al (2006) Lung recruitment in patients with the acute respiratory distress syndrome. N Engl J Med 354(17):1775–1786
Caironi P, Cressoni M, Chiumello D, Ranieri M, Quintel M, Russo SG et al (2010) Lung opening and closing during ventilation of acute respiratory distress syndrome. Am J Respir Crit Care Med 181(6):578–586
Goligher EC, Kavanagh BP, Rubenfeld GD, Adhikari NK, Pinto R, Fan E et al (2014) Oxygenation response to positive end-expiratory pressure predicts mortality in acute respiratory distress syndrome. A secondary analysis of the LOVS and ExPress trials. Am J Respir Crit Care Med 190(1):70–76
Gattinoni L, Carlesso E, Cressoni M (2015) Selecting the ‘right’ positive end-expiratory pressure level. Curr Opin Crit Care 21(1):50–57
Sahetya SK, Goligher EC, Brower RG (2017) Fifty years of research in ARDS. Setting positive end-expiratory pressure in acute respiratory distress syndrome. Am J Respir Crit Care Med 195(11):1429–1438
Fan E, Del Sorbo L, Goligher EC, Hodgson CL, Munshi L, Walkey AJ et al (2017) An Official American Thoracic Society/European Society of Intensive Care Medicine/Society of critical care medicine clinical practice guideline: mechanical ventilation in adult patients with acute respiratory distress syndrome. Am J Respir Crit Care Med 195(9):1253–1263
Nieman GF, Satalin J, Andrews P, Aiash H, Habashi NM, Gatto LA (2017) Personalizing mechanical ventilation according to physiologic parameters to stabilize alveoli and minimize ventilator induced lung injury (VILI). Intensive Care Med Exp 5(1):8
Costa EL, Borges JB, Melo A, Suarez-Sipmann F, Toufen C Jr, Bohm SH et al (2009) Bedside estimation of recruitable alveolar collapse and hyperdistension by electrical impedance tomography. Intensive Care Med 35(6):1132–1137
Acute Respiratory Distress Syndrome N, Brower RG, Matthay MA, Morris A, Schoenfeld D, Thompson BT et al (2000) Ventilation with lower tidal volumes as compared with traditional tidal volumes for acute lung injury and the acute respiratory distress syndrome. N Engl J Med 342(18):1301–1308
Brower RG, Lanken PN, MacIntyre N, Matthay MA, Morris A, Ancukiewicz M et al (2004) Higher versus lower positive end-expiratory pressures in patients with the acute respiratory distress syndrome. N Engl J Med 351(4):327–336
Spadaro S, Mauri T, Böhm SH, Scaramuzzo G, Turrini C, Waldmann AD et al (2018) Variation of poorly ventilated lung units (silent spaces) measured by electrical impedance tomography to dynamically assess recruitment. Crit Care 22(1):1–9
Yoshida T, Piraino T, Lima CAS, Kavanagh BP, Amato MBP, Brochard L (2019) Regional ventilation displayed by electrical impedance tomography as an incentive to decrease positive end-expiratory pressure. Am J Respir Crit Care Med 200(7):933–937
Blankman P, Hasan D, Erik G, Gommers D (2014) Detection of ‘best’ positive end-expiratory pressure derived from electrical impedance tomography parameters during a decremental positive end-expiratory pressure trial. Critical care (London, England) 18(3):R95
Sterne JAC, Savovic J, Page MJ, Elbers RG, Blencowe NS, Boutron I et al (2019) RoB 2: a revised tool for assessing risk of bias in randomised trials. BMJ 366:l4898
Sterne JA, Hernan MA, Reeves BC, Savovic J, Berkman ND, Viswanathan M et al (2016) ROBINS-I: a tool for assessing risk of bias in non-randomised studies of interventions. BMJ 355:i4919
Review Manager Web (RevMan Web) [Computer program]. Version 6.0.0. The Cochrane Collaboration; 2023.
Wan X, Wang W, Liu J, Tong T (2014) Estimating the sample mean and standard deviation from the sample size, median, range and/or interquartile range. BMC Med Res Methodol 14:135
Deeks JJ HJ, Altman DG (editors). Chapter 10: Analysing data and undertaking meta-analyses. In: Higgins JPT, Thomas J, Chandler J, Cumpston M, Li T, Page MJ, Welch VA (editors). Cochrane Handbook for Systematic Reviews of Interventions version 6.3 (updated February 2022). Cochrane. 2022.
Stata [Computer program]. Version 18. College Station: StataCorp; 2023.
Long Y, Liu DW, He HW, Zhao ZQ (2015) Positive end-expiratory pressure titration after alveolar recruitment directed by electrical impedance tomography. Chin Med J 128(11):1421–1427
Franchineau G, Bréchot N, Lebreton G, Hekimian G, Nieszkowska A, Trouillet JL et al (2017) Bedside contribution of electrical impedance tomography to setting positive end-expiratory pressure for extracorporeal membrane oxygenation-treated patients with severe acute respiratory distress syndrome. Am J Respir Crit Care Med 196(4):447–457
Fumagalli J, Santiago RRS, Teggia Droghi M, Zhang C, Fintelmann FJ, Troschel FM et al (2019) Lung recruitment in obese patients with acute respiratory distress syndrome. Anesthesiology 130(5):791–803
Puel F, Crognier L, Soulé C, Vardon-Bounes F, Ruiz S, Seguin T et al (2020) Assessment of electrical impedance tomography to set optimal positive end-expiratory pressure for veno-venous ECMO-treated severe ARDS patients. J Crit Care 60:38–44
Bronco A, Grassi A, Meroni V, Giovannoni C, Rabboni F, Rezoagli E et al (2021) Clinical value of electrical impedance tomography (EIT) in the management of patients with acute respiratory failure: a single centre experience. Physiol Meas 42(7):074003
Karsten J, Voigt N, Gillmann HJ, Stueber T (2019) Determination of optimal positive end-expiratory pressure based on respiratory compliance and electrical impedance tomography: a pilot clinical comparative trial. Biomed Tech (Berl) 64(2):135–145
Weber J, Gutjahr J, Schmidt J, Lozano-Zahonero S, Borgmann S, Schumann S et al (2020) Effect of individualized PEEP titration guided by intratidal compliance profile analysis on regional ventilation assessed by electrical impedance tomography—a randomized controlled trial. BMC Anesthesiol 20(1):42
Zhao Z, Lee LC, Chang MY, Frerichs I, Chang HT, Gow CH et al (2020) The incidence and interpretation of large differences in EIT-based measures for PEEP titration in ARDS patients. J Clin Monit Comput 34(5):1005–1013
Perier F, Tuffet S, Maraffi T, Alcala G, Victor M, Haudebourg AF et al (2020) Electrical impedance tomography to titrate positive end-expiratory pressure in COVID-19 acute respiratory distress syndrome. Crit Care 24(1):1–9
Sella N, Zarantonello F, Andreatta G, Gagliardi V, Boscolo A, Navalesi P (2020) Positive end-expiratory pressure titration in COVID-19 acute respiratory failure: electrical impedance tomography vs. PEEP/FiO2 tables. CritCare (London, England). 24(1):540
van der Zee P, Somhorst P, Endeman H, Gommers D (2020) Electrical impedance tomography for positive end-expiratory pressure titration in COVID-19-related acute respiratory distress syndrome. Am J Respir Crit Care Med 202(2):280–284
Jonkman AH, Alcala GC, Pavlovsky B, Roca O, Spadaro S, Scaramuzzo G et al (2023) Lung RecruitmEnt assessed by EleCtRical Impedance Tomography (RECRUIT): a multicenter study of COVID-19 ARDS. Am J Respir Crit Care Med 208:25
Jimenez JV, Munroe E, Weirauch AJ, Fiorino K, Culter CA, Nelson K et al (2023) Electric impedance tomography-guided PEEP titration reduces mechanical power in ARDS: a randomized crossover pilot trial. Crit Care 27(1):1–7
Somhorst P, van der Zee P, Endeman H, Gommers D (2022) PEEP-FiO2 table versus EIT to titrate PEEP in mechanically ventilated patients with COVID-19-related ARDS. Crit Care 26(1):272
Liu X, Liu X, Meng J, Liu D, Huang Y, Sang L et al (2022) Electrical impedance tomography for titration of positive end-expiratory pressure in acute respiratory distress syndrome patients with chronic obstructive pulmonary disease. Crit Care 26(1):1–11
Di Pierro M, Giani M, Bronco A, Lembo FM, Rona R, Bellani G et al (2022) Bedside selection of positive end expiratory pressure by electrical impedance tomography in patients undergoing veno-venous extracorporeal membrane oxygenation support: a comparison between COVID-19 ARDS and ARDS from other etiologies. J Clin Med 11(6):1–10
Hsu HJ, Chang HT, Zhao Z, Wang PH, Zhang JH, Chen YS et al (2021) Positive end-expiratory pressure titration with electrical impedance tomography and pressure-volume curve: a randomized trial in moderate to severe ARDS. Physiol Meas 42(1):1–9
He H, Chi Y, Yang Y, Yuan S, Long Y, Zhao P et al (2021) Early individualized positive end-expiratory pressure guided by electrical impedance tomography in acute respiratory distress syndrome: a randomized controlled clinical trial. Crit Care 25(1):1–11
Gibot S, Conrad M, Courte G, Cravoisy A (2021) Positive end-expiratory pressure setting in COVID-19-related acute respiratory distress syndrome: comparison between electrical impedance tomography, PEEP/FiO2 tables, and transpulmonary pressure. Front Med 8:720920
Becher T, Buchholz V, Hassel D, Meinel T, Schädler D, Frerichs I et al (2021) Individualization of PEEP and tidal volume in ARDS patients with electrical impedance tomography: a pilot feasibility study. Ann Intensive Care 11(1):1–10
Scaramuzzo G, Spadaro S, Dalla Corte F, Waldmann AD, Böhm SH, Ragazzi R et al (2020) Personalized positive end-expiratory pressure in acute respiratory distress syndrome: comparison between optimal distribution of regional ventilation and positive transpulmonary pressure. Crit Care Med 48(8):1148–1156
Zhao Z, Chang MY, Chang MY, Gow CH, Zhang JH, Hsu YL et al (2019) Positive end-expiratory pressure titration with electrical impedance tomography and pressure–volume curve in severe acute respiratory distress syndrome. Ann Intensive Care 9(1):1–9
Heines SJH, Strauch U, van de Poll MCG, Roekaerts PMHJ, Bergmans DCJJ (2019) Clinical implementation of electric impedance tomography in the treatment of ARDS: a single centre experience. J Clin Monit Comput 33(2):291–300
Eronia N, Mauri T, Maffezzini E, Gatti S, Bronco A, Alban L et al (2017) Bedside selection of positive end-expiratory pressure by electrical impedance tomography in hypoxemic patients: a feasibility study. Ann Intensive Care 7(1):1–10
Frerichs I, Amato MB, van Kaam AH, Tingay DG, Zhao Z, Grychtol B et al (2017) Chest electrical impedance tomography examination, data analysis, terminology, clinical use and recommendations: consensus statement of the TRanslational EIT developmeNt stuDy group. Thorax 72(1):83–93
Bodenstein M, David M, Markstaller K (2009) Principles of electrical impedance tomography and its clinical application. Crit Care Med 37(2):713–724
Costa EL, Lima RG, Amato MB (2009) Electrical impedance tomography. Curr Opin Crit Care 15(1):18–24
Cornejo R, Iturrieta P, Olegário TMM, Kajiyama C, Arellano D, Guiñez D et al (2021) Estimation of changes in cyclic lung strain by electrical impedance tomography: proof-of-concept study. Acta Anaesthesiol Scand 65(2):228–235
Walsh BK, Smallwood CD (2016) Electrical impedance tomography during mechanical ventilation. Respir Care 61(10):1417–1424
Cinnella G, Grasso S, Raimondo P, D’Antini D, Mirabella L, Rauseo M et al (2015) Physiological effects of the open lung approach in patients with early, mild, diffuse acute respiratory distress syndrome: an electrical impedance tomography study. Anesthesiology 123(5):1113–1121
Amato MB, Meade MO, Slutsky AS, Brochard L, Costa EL, Schoenfeld DA et al (2015) Driving pressure and survival in the acute respiratory distress syndrome. N Engl J Med 372(8):747–755
Laffey JG, Bellani G, Pham T, Fan E, Madotto F, Bajwa EK et al (2016) Potentially modifiable factors contributing to outcome from acute respiratory distress syndrome: the LUNG SAFE study. Intensive Care Med 42(12):1865–1876
Zhang Z, Zheng B, Liu N, Ge H, Hong Y (2019) Mechanical power normalized to predicted body weight as a predictor of mortality in patients with acute respiratory distress syndrome. Intensive Care Med 45(6):856–864
Tonna JE, Peltan I, Brown SM, Herrick JS, Keenan HT, University of Utah Mechanical Power Study G (2020) Mechanical power and driving pressure as predictors of mortality among patients with ARDS. Intensive Care Med 46(10):1941–1943
Costa ELV, Slutsky AS, Brochard LJ, Brower R, Serpa-Neto A, Cavalcanti AB et al (2021) Ventilatory variables and mechanical power in patients with acute respiratory distress syndrome. Am J Respir Crit Care Med 204(3):303–311
Urner M, Juni P, Hansen B, Wettstein MS, Ferguson ND, Fan E (2020) Time-varying intensity of mechanical ventilation and mortality in patients with acute respiratory failure: a registry-based, prospective cohort study. Lancet Respir Med 8(9):905–913
Urner M, Juni P, Rojas-Saunero LP, Hansen B, Brochard LJ, Ferguson ND et al (2023) Limiting dynamic driving pressure in patients requiring mechanical ventilation. Crit Care Med 51(7):861–871
Yu M, Deng Y, Cha J, Jiang L, Wang M, Qiao S et al (2023) PEEP titration by EIT strategies for patients with ARDS: a systematic review and meta-analysis. Med Intens (Engl Ed) 47(7):383–390
Becher T BV, Schädler D, Frerichs I, Weiler N (2016) Electrical impedance tomography-based algorithm for personalized adjustment of mechanical ventilation in ards patients. In: ESICM LIVES; 2016 Oct 1–5; Milan, Italy: intensive care medicine experimental, vol 4(Suppl 1), p 30
Funding
This work was partially supported by the Canadian Institutes of Health Research to HZ (PJT190130).
Author information
Authors and Affiliations
Contributions
NS and HZ contributed to the conception or design of the work; NS and CL: acquisition, analysis, or interpretation of data for the work; NS, YX, CL, OR, LB, AS, KB, and HZ: drafting the work or reviewing it critically for important intellectual content. All authors have final approval of the version to be published and have agreed to be accountable for all aspects of the work in ensuring that questions related to the accuracy or integrity of any part of the work are appropriately investigated and resolved.
Corresponding authors
Ethics declarations
Conflicts of interest
All authors declare that they have no conflict of interest.
Ethics approval and consent to participate
Ethics approval and consent to participate does not apply.
Consent for publication
Consent for publication does not apply.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution-NonCommercial 4.0 International License, which permits any non-commercial use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if changes were made. The images or other third party material in this article are included in the article's Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article's Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by-nc/4.0/.
About this article
Cite this article
Songsangvorn, N., Xu, Y., Lu, C. et al. Electrical impedance tomography-guided positive end-expiratory pressure titration in ARDS: a systematic review and meta-analysis. Intensive Care Med 50, 617–631 (2024). https://doi.org/10.1007/s00134-024-07362-2
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00134-024-07362-2