Abstract
Purpose
Little is known about risk factors for sustaining a posterior cruciate ligament (PCL) rupture. Identifying risk factors is the first step in preventing a PCL rupture from occurring. The morphology of the knee in patients who ruptured their PCL may differ from that of control patients. The hypothesis was that the intercondylar notch dimensions, 3-D volumes of the intercondylar notch and, the 3-D volumes of both the ACL and the PCL were correlated to the presence of a PCL rupture.
Methods
The magnetic resonance imaging (MRI) scans of 30 patients with a proven PCL rupture were compared to 30 matched control patients with proven intact ACL and PCL. Control patients were selected from patients with knee trauma during sports but without cruciate ligament injury. Patients have been matched for age, height, weight, BMI, and sex. The volumes of the intercondylar notch and both the ACL and PCL were measured on 3D reconstructions. Second, the bicondylar width, the notch width, and the notch width index were measured of all subjects. The relationship between our measurements and the presence of a PCL rupture was analysed.
Results
The results show a significant difference in the volumes of the intercondylar notch and the ACL between patients with a ruptured PCL and control patients. Patients with a PCL rupture have smaller intercondylar notch volumes and smaller ACL volumes. There were no significant differences in the bicondylar width, notch width, and notch width index. In the control patients, a significant correlation between the volume of the PCL and the volume of the ACL was found (0.673, p < 0.001).
Conclusion
Patients with a PCL rupture have smaller intercondylar volumes and smaller ACL volumes when compared to control patients. Second, patients with smaller ACL volumes have smaller PCL volumes. This study shows, for the first time, that there are significant size and volume differences in the shape of the knee between patients with a PCL rupture and control patients.
Level of evidence
IV.
Similar content being viewed by others
Explore related subjects
Discover the latest articles, news and stories from top researchers in related subjects.Avoid common mistakes on your manuscript.
Introduction
Injuries to the posterior cruciate ligament (PCL) occur in approximately 1–4% of all sport-related traumatic knee injuries, depending on the type of sport [14, 17]. With the growing number of athletes and especially of competitive athletes [10], the absolute number of PCL injuries is growing and is likely to keep on growing in the next couple of years [3, 11].
In the short term, a PCL rupture, in most cases, causes pain and posterior laxity and reduces an individual’s ability to take part in sports. In the long term, deficiency of the PCL results in abnormal kinematics and increased contact pressures in the medial and patellofemoral compartments of the knee and may increase strain on the posterolateral knee structures, placing them at risk of subsequent injury [9, 25]. Long-term studies have found that degenerative changes after PCL injury occur primarily in the medial and patellofemoral compartments [2, 6, 8, 17, 20]. PCL injuries are still often overlooked during primary care [18, 23], resulting in delayed diagnosis and delayed treatment. Therefore, risk factors need to be identified. Recently, van Kuijk et al. found that the size and shape of the intercondylar notch and the tibial eminence are related to the risk of sustaining a PCL rupture [13]. This study is conducted on plain radiographs. The knee, however, is a 3-Dimensional, complex joint, best analysed on MRI. However, until this date, no studies using MRI have been conducted to investigate the morphological features of the PCL deficient knee. It might be possible that the shape of the intercondylar notch has a positive correlation with the soft tissue moving through it, such as the PCL.
Therefore, the purpose of this study was to investigate if the volumes of the cruciate ligaments, the sizes of the intercondylar notch, and the intercondylar notch dimension are related to the risk of sustaining a PCL rupture.
Material and methods
The institutional ethics review board of the Erasmus MC, Rotterdam, approved this study (MEC-2017-422).
Patient selection
Patients with a PCL rupture and control patients were selected from patients visiting our outpatient clinic of the Erasmus Medical Center, Rotterdam, The Netherlands, between January 2003 and May 2014. Patients and controls had to be practising pivoting sports competitively during the time of injury. Patients were only included if they had an isolated PCL rupture, confirmed by MRI or arthroscopy. Controls were selected from patients who had sustained a meniscal tear or a combined medial collateral ligament and meniscus injury and had an intact PCL and intact ACL confirmed by MRI or arthroscopy. Patients were excluded if they had radiographic evidence of knee osteoarthritis Kellgren and Lawrence score two or higher because secondary bone formation could change the notch shape and decrease or alter the volume. Patients were matched for age, height, weight, BMI, and sex.
The institutional ethics review board approved this study.
MRI protocol and segmentation
MR images were obtained using MRI scanners with a magnetic field strength of 1.0, 1.5, or 3.0 Tesla.
The MRI sequences used are sag PD, sag T2 FS, Cor PD FS, Coronal T2 TSE, axial T2 FS, axial PD. Patients' legs were positioned neutrally. To assess PCL injury, and the measurements in the knee described below, we used sagittal and coronal proton density-weighted turbo spin-echo (TSE) sequences (slice thickness 1 mm, repetition time (TR)/echo time (TE), 2700/27 ms), and the coronal T2-weighted TSE sequence with fat saturation (slice thickness 1 mm, TR/TE 5030/71 ms).
ACL and PCL volume measurements
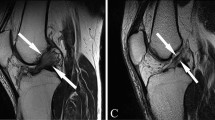
The volumes of the ACL in both groups, and the PCL in the controls, were obtained from sagittal T1-weighted series. Osirix software (open-source medical imaging software for MacOS X [Apple, Cupertino, CA]; OsiriX, Geneva, Switzerland) was used to manually outline the ACL and PCL. This method was tested and found to be reliable and accurate in previously conducted research[28]. The software calculated the volume as the sum of surface multiplied by the slice thickness (1 mm), the volumes were presented in two decimals. (see Fig. 1). Furthermore, the correlation between the size of the ACL and the PCL in control patients was analysed.
Femoral notch measurements
The boundaries of the intercondylar notch were measured according to Van Eck et al., who previously described the boundaries of the intercondylar notch [4]. The proximal border of the notch is defined as the image in which both femoral condyles were first clearly visible (Fig. 2A). The distal border of the notch is defined as the last image in which the condyles were continuous (Fig. 2B).
Additionally, the notch width index (NWI) was measured according to the method first described by Staeubli et al. [21] and later modified by Whitney et al. [26]. A reference line (RL) is defined as a tangent to the posterior subchondral aspect of both femoral condyles. All femoral widths are measured parallel to this reference line. In the coronal plane, the following measurements were applied: bicondylar width (BW) and notch width outlet (NW). The notch width index was calculated by dividing the NW by the BW (Fig. 3).
A T2 coronal plane was used in each patient to measure BW and NW. The slice chosen in every knee was the plane in which the ACL and PCL cross one another as close as possible to the midsubstance of the ACL [26]. This point was typically found on the first slice anterior to the appearance of the roof of the intercondylar notch.
Statistical analysis
The independent-sample t test was used to assess whether or not the volume of the intercondylar notch and the volumes of the ACL and PCL and the bicondylar width, the notch width, and the notch width index were significantly related to the presence of a PCL rupture. The results were not corrected for height, weight, BMI, age, and sex, since we matched our cases with our patients on those factors. A value of 0.05 was chosen as the level of significance.
The reliability of the measurements performed in this study was established using interclass correlation coefficients (ICCs). Twenty-eight MRI scans were randomly selected to be assessed a second time, two weeks after initial measurements. The observer did not know the values of previous measurements. A post hoc power analysis was performed, showing that the current study with 30 patients included in each group, had a power of 94.9%. The calculation showed that 28 patients in the control group and 28 patients with a PCL rupture were needed to reach a sufficient power. With 30 patients, the power was considered excellent.
The study population consisted of two groups of 30 patients matched for age, height, weight, BMI, and sex. There were six females (20%) in each group. The demographic data for each group are shown in Table 1.
Results
Measurements
Table 2 shows the means for the BW, NW, NWI, the volumes of the PCL and ACL, and the intercondylar sizes. A significant difference in the sizes of the intercondylar notch (p = 0.001) between patients with a PCL rupture and the control patients was found. Secondly, a significant difference between the volumes of the ACL (p = 0.039) in patients with a PCL rupture and patients with intact PCLs was found.
Patients with a PCL rupture had smaller intercondylar sizes (7.0 cm3 ± 2.2 compared to 8.6 cm3 ± 1.2) and smaller volumes of the ACL (1.1 cm3 ± 0.3 compared to 1.3 cm3 ± 0.3), when compared to patients with an intact PCL.
There were no significant differences in the bicondylar width, notch width, and notch width index.
The correlation between the size of the PCL and the ACL in the control patients was found to be a positive correlation of 0.7. Meaning patients with smaller volumes of the PCL are more likely to have smaller volumes of the ACL.
When looking at sex, the intercondylar sizes (p = 0.02) and the volumes of the ACL in males were significantly larger than in the controls (p = 0.01). For the females, only the intercondylar volumes were significantly different between patients and controls (p = 0.001) (Table 3).
The ICCs were considered excellent with values of 0.906 for BW (95% CI 0.807–0.955), 0.993 for NW (95% CI 0.984–0.997) and 0.952 for NWI (95% CI 0.899–0.977).
Discussion
The most important findings of this study are that patients with a PCL rupture had smaller intercondylar sizes and had smaller ACL volumes. To our knowledge, this is the first study to find anatomical risk factors for sustaining a PCL rupture. In a recent study on plain radiographs of the knee, van Kuijk et al. found that the shape of the intercondylar notch plays an important role in the PCL deficient knee [13]. With this current study, using MRI reconstructions of the intercondylar notch and the volumes of the PCL and ACL, it becomes clearer what specific anatomical features contribute to these findings on 2D plain radiographs.
Possibly, patients with smaller ACL volumes are also at greater risk for sustaining a PCL rupture. The absolute mean difference was 17 cubic millimetres, making it a statistically significant difference. Although the absolute difference is relatively small, raising the question if this would be clinically important, it is a difference of more than 10% in volume. Our opinion is, that more than 10% difference in size would be clinically relevant, and as stated, it was statistically different too. A positive correlation between the volumes of the PCL and the ACL was found, and although the sample size is small, it can be assumed that patients with smaller ACL volumes had smaller PCL volumes. Smaller PCLs can withhold less force and are more prone to rupture [15, 24]. Furthermore, the size of the PCL (and of the ACL) is correlated with the size of the intercondylar notch [16, 22]. It is well accepted that the volumes of the intercondylar notch, the PCL, and the ACL are all positively correlated. A question still unresolved is whether patients with smaller cruciate ligaments and smaller intercondylar notches rupture their ligament because of the relatively smaller force they can withhold, or because of chronic or acute damage because of notch impingement to the cruciate ligaments [1, 5, 19, 27]. However, notch impingement may play a lesser role in the risk for sustaining a PCL rupture, because of the anatomical position of the PCL posterior in the knee.
When comparing males to females, we find a similar result, with the note that we only have a small group of females, thus the statistical power of these results is low.
It is difficult to compare the results of this study to previously conducted research since this study is the first to have investigated the volumes of the intercondylar notch and the volumes of the PCL and ACL in correlation with a PCL rupture. Research is abundant into the intercondylar notch and the ACL deficient knee (see Supplemental File) [12, 24, 26, 28]. These studies found similar results in the ACL deficient knee as we have found in the PCL deficient knee. This current study, therefore, adds important new information, proving the importance of the volumes of the cruciate ligaments and the sizes of the intercondylar notch.
The risk factors in the current study are possibly modifiable (for example, during surgery with notch plasty), it is uncertain if changing the notch dimension, can reduce the risk for future PCL rupture, and notch plasty results are debated in the literature.
A limitation is the low number of patients included in the study. Ideally, more patient would have been included, to have more power, although the study has an adequate power. However, few patients have a sports-related isolated PCL rupture. Because the consequences of this type of injury are severe, we are confident that research into the PCL rupture is necessary.
Degenerative changes of the knee could result in osteophyte formation and narrowing of the intercondylar notch. These changes happen more often after PCL rupture. This could mean that the results found were based on post-traumatic degenerative changes. Therefore, patients with Kellgren and Lawrence grade 2 or more were excluded, reducing this possible bias as much as possible.
While prevention programs are implemented for preventing an ACL rupture during sports [7], it has not been investigated if these programs or comparable programs can help to reduce the incidence of PCL ruptures. However, for preventing a disease or injury in general, risk factors must first be identified, and that is, in our opinion, the clinical relevance of our study. We are convinced, this study is an important first step in identifying risk factors, and we hope that we have inspired researchers to further investigate the results found. This study shows, for the first time, that there are significant differences in the shape of the knee between patients with a PCL rupture and control patients.
Conclusion
This study shows that patients with a smaller intercondylar size and a smaller volume of the ACL are more prone to sustain PCL rupture. This is an important first step in identifying patients at risk for a PCL rupture. Identifying patients at risk is useful information if in the future, the risk of individuals for sustaining a PCL rupture might be reduced.
References
Bouras T, Fennema P, Burke S, Bosman H (2018) Stenotic intercondylar notch type is correlated with anterior cruciate ligament injury in female patients using magnetic resonance imaging. Knee Surg Sports Traumatol Arthrosc 26:1252–1257
Chahla J, Williams BT, LaPrade RF (2020) Posterior cruciate ligament. Arthroscopy 36:333–335
Chung KS (2021) An increasing trend of posterior cruciate ligament reconstruction in South Korea: epidemiologic analysis using Korean National Health Insurance System Database. Knee Surg Relat Res 33:44
van Eck CF, Martins CA, Vyas SM, Celentano U, van Dijk CN, Fu FH (2010) Femoral intercondylar notch shape and dimensions in ACL-injured patients. Knee Surg Sports Traumatol Arthrosc 18:1257–1262
Hassebrock JD, Gulbrandsen MT, Asprey WL, Makovicka JL, Chhabra A (2020) Knee ligament anatomy and biomechanics. Sports Med Arthrosc Rev 28:80–86
Hermans S, Corten K, Bellemans J (2009) Long-term results of isolated anterolateral bundle reconstructions of the posterior cruciate ligament: a 6- to 12-year follow-up study. Am J Sports Med 37:1499–1507
Huang YL, Jung J, Mulligan CMS, Oh J, Norcross MF (2020) A majority of anterior cruciate ligament injuries can be prevented by injury prevention programs: a systematic review of randomized controlled trials and cluster-randomized controlled trials with meta-analysis. Am J Sports Med 48:1505–1515
Jackson WF, van der Tempel WM, Salmon LJ, Williams HA, Pinczewski LA (2008) Endoscopically-assisted single-bundle posterior cruciate ligament reconstruction: results at minimum ten-year follow-up. J Bone Joint Surg Br 90:1328–1333
Kang KT, Koh YG, Jung M, Nam JH, Son J, Lee YH et al (2017) The effects of posterior cruciate ligament deficiency on posterolateral corner structures under gait- and squat-loading conditions: a computational knee model. Bone Joint Res 6:31–42
Kovacs RJ (2022) Participation in competitive athletics has increased dramatically in the past decade. Am College Cardiol 2016; https://www.acc.org/latest-in-cardiology/articles/2016/03/16/06/36/participation-in-competitive-athletics-has-increased-dramatically-in-the-past-decade. Accessed 31–05–2022, 2022.
Krutsch W, Zeman F, Zellner J, Pfeifer C, Nerlich M, Angele P (2016) Increase in ACL and PCL injuries after implementation of a new professional football league. Knee Surg Sports Traumatol Arthrosc 24:2271–2279
van Kuijk KSR, Eggerding V, Reijman M, van Meer BL, Bierma-Zeinstra SMA, van Arkel E et al (2021) Differences in Knee Shape between ACL injured and non-injured: a matched case-control study of 168 patients. J Clin Med 10:968
van Kuijk KSR, Reijman M, Bierma-Zeinstra SMA, Waarsing JH, Meuffels DE (2019) Posterior cruciate ligament injury is influenced by intercondylar shape and size of tibial eminence. Bone Joint J 101-B:1058–1062
Kumar A, Sinha S, Arora R, Gaba S, Khan R, Kumar M (2021) The 50 top-cited articles on the posterior cruciate ligament: a bibliometric analysis and review. Orthop J Sports Med 9:23259671211057852
Logterman SL, Wydra FB, Frank RM (2018) Posterior cruciate ligament: anatomy and biomechanics. Curr Rev Musculoskelet Med 11:510–514
Oshima T, Putnis S, Grasso S, Parker DA (2020) The space available for the anterior cruciate ligament in the intercondylar notch is less in patients with ACL injury. Knee Surg Sports Traumatol Arthrosc 28:2105–2115
Sanders TL, Pareek A, Barrett IJ, Kremers HM, Bryan AJ, Stuart MJ et al (2017) Incidence and long-term follow-up of isolated posterior cruciate ligament tears. Knee Surg Sports Traumatol Arthrosc 25:3017–3023
Schuttler KF, Ziring E, Ruchholtz S, Efe T (2017) Posterior cruciate ligament injuries. Unfallchirurg 120:55–68
Song GY, Ni QK, Zheng T, Feng H, Zhang ZJ, Zhang H (2021) Increased posterior tibial slope is associated with greater risk of graft roof impingement after anatomic anterior cruciate ligament reconstruction. Am J Sports Med 49:2396–2405
Song EK, Park HW, Ahn YS, Seon JK (2014) Transtibial versus tibial inlay techniques for posterior cruciate ligament reconstruction: long-term follow-up study. Am J Sports Med 42:2964–2971
Staeubli HU, Adam O, Becker W, Burgkart R (1999) Anterior cruciate ligament and intercondylar notch in the coronal oblique plane: anatomy complemented by magnetic resonance imaging in cruciate ligament-intact knees. Arthroscopy 15:349–359
Strada NA, Vutescu ES, Mojarrad M, Harrington R, Orman S, Evangelista P et al (2022) Can the posterior cruciate ligament (Pcl) predict anterior cruciate ligament (Acl) size for planning during Acl reconstruction? Orthop J Sports Med 10:2325967121S2325900376
Verhulst FV, MacDonald P (2020) Diagnosing PCL injuries: history, physical examination, imaging studies, arthroscopic evaluation. Sports Med Arthrosc Rev 28:2–7
van der Wal WA, Meijer DT, Hoogeslag RAG, LaPrade RF (2021) Meniscal tears, posterolateral and posteromedial corner injuries, increased coronal plane and increased sagittal plane tibial slope all influence ACL related knee kinematics and increase forces on the native and reconstructed anterior cruciate ligament: a systematic review of cadaveric studies. Arthroscopy. https://doi.org/10.1016/j.arthro.2021.11.044
Wang D, Graziano J, Williams RJ 3rd, Jones KJ (2018) Nonoperative treatment of PCL injuries: goals of rehabilitation and the natural history of conservative care. Curr Rev Musculoskelet Med 11:290–297
Whitney DC, Sturnick DR, Vacek PM, DeSarno MJ, Gardner-Morse M, Tourville TW et al (2014) Relationship between the risk of suffering a first-time noncontact ACL injury and geometry of the femoral notch and ACL: a prospective cohort study with a nested case-control analysis. Am J Sports Med 42:1796–1805
Winkler PW, Zsidai B, Wagala NN, Hughes JD, Horvath A, Senorski EH et al (2021) Evolving evidence in the treatment of primary and recurrent posterior cruciate ligament injuries, part 1: anatomy, biomechanics and diagnostics. Knee Surg Sports Traumatol Arthrosc 29:672–681
Wratten CJ, Tetsworth K, Hohmann E (2015) Three-dimensional femoral notch volume in anterior cruciate ligament-deficient versus anterior cruciate ligament-intact patients: a matched case-control study with inter-gender comparison. Arthroscopy 31:1117–1122
Funding
No funding was received.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors have no conflict of interest.
Ethical approval
The institutional ethics review board of the Erasmus MC, Rotterdam, approved this study (MEC-2017-422).
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if changes were made. The images or other third party material in this article are included in the article's Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article's Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
van Kuijk, K.S.R., Reijman, M., Bierma-Zeinstra, S.M.A. et al. Smaller intercondylar notch size and smaller ACL volume increase posterior cruciate ligament rupture risk. Knee Surg Sports Traumatol Arthrosc 31, 449–454 (2023). https://doi.org/10.1007/s00167-022-07049-5
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00167-022-07049-5