Abstract
Purpose
Tibial plateau fractures (TPFs) may lead to posttraumatic osteoarthritis and increase the risk for total knee arthroplasty (TKA). The aim of this systematic review was to analyse the conversion rate to TKA after TPF treatment.
Methods
A systematic search for studies reviewing the conversion rate to TKA after TPF treatment was conducted. The studies were screened and assessed by two independent observers. The conversion rate was analysed overall and for selected subgroups, including different follow-up times, treatment methods, and study sizes.
Results
A total of forty-two eligible studies including 52,577 patients were included in this systematic review. The overall conversion rate of treated TPF to TKA in all studies was 5.1%. Thirty-eight of the forty-two included studies indicated a conversion rate under 10%. Four studies reported a higher percentage, namely, 10.8%, 10.9%, 15.5%, and 21.9%. Risk factors for TKA following TPF treatment were female sex, age, and low surgeon and hospital volume. The conversion rate to TKA is particularly high in the first 5 years after fracture.
Conclusion
Based on the studies, it can be assumed that the conversion rate to TKA is approximately 5%. The risk for TKA is manageable in clinical practice.
Prospero registration number
CRD42023385311.
Level of evidence
IV.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Tibial plateau fractures (TPFs) are injuries of the proximal tibia that can be intraarticular or extraarticular. Treatment of these injuries can be nonoperative or operative. Surgical possibilities are a fixation procedure or primary total knee arthroplasty (TKA). The gold standard fixation method is open reduction and internal fixation (ORIF). Surgical treatment may lead to infection, knee stiffness, non-union, fixation failure, and posttraumatic osteoarthritis (PTOA) [43]. PTOA has been reported to occur relatively frequently in patients with TPF [27, 36]. The latter can lead to knee arthroplasty at an early or later stage. Compared to TKA due to primary osteoarthritis, knee arthroplasty with a previous TPF can present a major challenge due to stiffness, compromised bone quality, and bone stock as well as infection [6, 43].
In elderly patients, ORIF is a challenge due to poor bone quality, metaphyseal bone comminution, and a friable soft tissue envelope. One approach is to treat older patients with knee arthroplasty instead of a fixation procedure, which primarily poses different challenges [22, 52]. The risk of TKA after surgically treated TPF remains unclear.
The objective of this systematic review was to quantify the conversion rate to TKA after TPF treatment. It was hypothesised that the conversion rate is not as high as often assumed.
Methods
This systematic review was conducted according to Preferred Reporting Items for Systematic Reviews and Meta-Analyses (PRISMA) 2020 Guidelines [33].
Search strategy
The purpose of this review was to assess the risk of TKA following TPF treatment. A comprehensive systematic search using the PubMed, Medline, and Scopus databases was performed. The search terms were (“tibial plateau fracture”) OR (“proximal tibia fracture”) AND (“tka”) OR (“total knee arthroplasty”) OR (“total knee replacement”). The capitalised words represent Boolean operators. All articles published before December 2022, when the systematic search was conducted, were considered.
Inclusion criteria
Inclusion criteria comprised a mean follow-up of 1 year and a cohort of at least ten patients. The search was limited to the English and German languages. No study was excluded due to the year of publication. Systematic reviews, conference abstracts, review articles, and expert opinions were not included. Studies reporting on surgically treated TPFs as well as studies reporting on nonoperatively treated TPFs were considered.
Exclusion criteria
Literature reviewing TPFs treated with primary TKA was excluded. Studies analysing TPF treated with osteochondral allograft, alone or combined with a femoral osteotomy, were also not considered. Studies were not included if the full text was not available. Articles reporting pathological TPF were not examined in this systematic review. Different studies with the same number of patients and TKAs, same follow-up, same authors, and same hospital were considered only once.
Selection process and data collection
Two authors (Initials) independently reviewed the titles and abstracts of the retrieved articles. Next, duplicates were removed, and full texts were analysed by applying the inclusion and exclusion criteria. In case of disagreement on inclusion, a consensus was reached by discussion with a third author (AK). The references of the retrieved articles were manually screened. Afterwards, the studies were searched for the following data: number of patients with a TPF, follow-up time (mean, minimal, maximal), patients who have undergone TKA, and percent value (TKA/TPF). Missing information (e.g. percent value: TKA/TPF) was calculated manually with the specified data.
The total conversion rate of all studies was calculated as the sum of all patients and all TKAs. Furthermore, the conversion rate was determined for some selected subgroups. The results are presented graphically. The data evaluation was performed by two authors independently. A meta-analysis could not be performed due to the heterogeneity of the study data. Therefore, the content of the studies was analysed through a descriptive procedure.
To assess the trustworthiness, relevance, and results of the published papers, the Joanna Briggs Institute (JBI) critical appraisal checklist for case series [30] was used. Two authors applied the JBI tool independently for assessment of the selected articles. Any disagreement was resolved through discussion with a third author.
Results
Search results
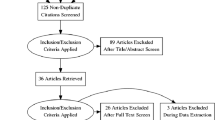
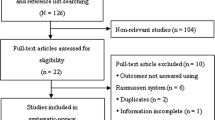
A total of 2087 articles were identified through a comprehensive search of the PubMed, Medline, and Scopus databases, resulting in twenty-five studies meeting the inclusion criteria. Through a manual search of the references in the retrieved papers, 17 articles were added. Finally, 42 studies were included in this systematic review (Fig. 1).
Study characteristics
In total, 52,577 patients were examined in the forty-two studies. The study with the largest number of participants reviewed 22,988 patients [49]. The key characteristics of the identified studies are summarised in Tables 1 and 2.
Thirty-five papers verified outcome after surgical treatment. Seven studies included surgically and non-surgically treated patients [3, 12, 20, 27, 28, 45, 49]. Four studies involved no TKA implantation during the follow-up time. Half of all studies reported a percentage between 2.5% and 7% (Fig. 2). Four publications had a percent value over 10%. The highest conversion rate was reported at 21.9% after a mean follow-up time of 6.8 years.
Boxplots showing the conversion rates [%] to total knee arthroplasty: overall, follow-up under 5 years, follow-up over 5 years, studies with more than 200 patients, studies with less than 200 patients (studies comparing treatment methods are not presented due to the small number of studies with nonoperative and operative treated patients)
The overall conversion rate of all patients and TKAs of the included studies was 5.1% (Table 3). Studies with a mean follow-up under 5 years reported that 4.2% of patients underwent TKA, compared to 5.9% in studies with a mean follow-up of more than 5 years. A lower conversion rate to TKA was determined in studies including surgically and non-surgically treated patients (4.6%). When considering only studies with surgically treated patients, the percentage was 6.3%.
Table 4 shows the results of the evaluation of the studies using the JBI tool.
Discussion
The most important finding of this systematic review was that the conversion rate to TKA is not as high as often assumed. Thirty-eight of the forty-two articles identified a conversion rate between 0 and 10%. Two studies specified that the percentage value was slightly higher at 10.8% and 10.9% [3, 23]. The highest conversion rates to TKA were 15.5% and 21.9% [9, 47]. The high percentage cannot be deduced from the available study results. Four articles reported no TKA during the follow-up time. This might be a result of the low number of patients in these studies or shorter follow-up.
The sum of all patients with TPF and all TKAs results in a conversion rate of 5.1%. Half of all included studies reported a percentage between 2.5 and 7%. The average risk was approximately 5% when considering only the five largest studies [12, 40, 45, 49, 51]. Based on the available publications, the risk for knee replacement can be expected to be approximately 5%.
Studies that included only surgically treated patients showed a higher conversion rate than studies including non-surgically treated patients. The reason for this might be that patients treated non-surgically had no or minimal displacement, which might influence the onset of PTOA.
ORIF is the gold standard for tibial plateau fracture [35]. Chan et al. [9] compared patients with external fixation to patients with internal fixation after TPF. The study reported no significant difference in outcome between these fixation methods. Some articles investigated the outcome of TPF with other treatment methods, such as the Allring fixator [2], Ilizarov fixator [37], or LISS (less invasive stabilisation system) plate [5]. Due to the small number of participants in the studies with different fixation methods, it was not possible to compare them directly with each other.
Three studies were designed as a matched cohort study. Risk for TKA was compared between patients with a previous TPF and patients without a previous TPF. The publication of Elsoe et al. [12] reported that 5.7% of patients with a previous TPF and 2% of patients without a TPF underwent TKA during the follow-up period. The risk for TKA was 3.5 times higher with a prior TPF. Wasserstein et al. [51] even described a 5.3-fold increased risk for TKA compared with a matched group from the general population. Tapper et al. [45] reported an increase in the risk of 3.2% in the surgically treated group of patients and 1.8% in the nonoperatively treated group compared with a reference group.
The risk for a TKA is particularly high in the first 5 years after the injury. Data from long-term studies show that comparatively fewer prostheses are fitted after 5 years [12, 51]. Scott et al. [40] and Ochen et al. [31] reported a time to TKA as 1.5 years and 1.9 years, respectively. The mean follow-up times in these studies were 7.1 years and 5 years. In relation to the follow-up time, a change to a TKA became necessary at an early stage. By comparing articles with a follow-up of less than 5 years and more than 5 years, we found slightly increased percentages for the 1st and 3rd quartiles and the median with a follow-up of more than 5 years. In summary, it can be assumed that the highest risk of converting to TKA is in the first 5 years after the fracture.
Some publications reported risk factors that led to the implantation of prostheses. The study by Wasserstein et al. [51] pointed out that bicondylar fractures are associated with increased risk of TKA. Eight publications included only bicondylar fractures. However, no increased conversion to TKA was found. In addition, Scott et al. [40] reported a higher conversion rate of unicondylar fractures compared to bicondylar fractures (not statistically significant).
Six publications pointed out a higher conversion rate among women [12, 19, 32, 40, 45, 51]. In the study by Su et al. [44], three patients underwent TKA, and all of them were women. Among other aspects, associations for higher conversion rates with the following were reported: tobacco [32], high BMI [19, 40], comorbidities [51], and a high rate of soft tissue injuries [19]. However, these correlations are not entirely clear. For example, according to Scott et al. [40], tobacco and diabetes are not significant risk factors. Wasserstein et al. [51] found no association between TKA and rural address, open fracture, associated tibial shaft fracture, hospital status, surgeon volume, or after-hours surgery. Brodke et al. [7] explicitly compared the conversion rate between hospitals and surgeons with high and low caseloads. It was detected that high-volume treatment of TPF reduced the risk of TKA. It can be assumed that low case numbers and female sex are risk factors for TKA after a TPF.
The included studies referred to controversial statements about age as a risk factor for TKA. The study by Kim et al. [25] compared the need for TKA between elderly and younger patients. No significant difference was found between these two age groups. Seven studies in this systematic review included only elderly patients [2, 4, 17, 21, 38, 41, 44]. No increased conversion to TKA was observed. However, the number of study participants and the follow-up time were significantly low. Three large studies [12, 45, 51] reported increased risk in elderly patients for TKA after TPF. Furthermore, these publications had a long follow-up time after the fracture. Additionally, the literature states that older age probably leads to poorer fracture healing [16, 29]. Therefore, it can be assumed that older age leads to more TKAs after TPF.
This systematic review has some limitations. Only five studies with more than a thousand patients were included. Most publications reviewed fewer than 100 study participants. In some studies, the mean follow-up time was short. Different treatment methods were used in the studies. Therefore, articles with different study sizes, follow-up, and treatment methods were compared with each other in terms of conversion to TKA, risk factors, and time to TKA.
Implications of this review: The risk of TKA following TPF is not as high as often assumed. Non-operative therapy and joint preservation surgery are good treatment methods, and the risk for TKA is manageable. Based on the publications, a conversion rate of approximately 5% can be concluded. The risk for TKA after TPF is manageable in clinical practice.
Conclusion
The conversion rate ranged from 0 to 21%. Based on the available data, risk for TKA can be assumed to be approximately 5%. Risk factors for TKA are female sex, elderly, and low surgeon and hospital volume. The risk for TKA increases in the first 5 years following TPF.
Abbreviations
- TPF:
-
Tibial plateau fracture
- TKA:
-
Total knee arthroplasty
- ORIF:
-
Open reduction and internal fixation
- PTOA:
-
Posttraumatic osteoarthritis
References
Ali AM, Burton M, Hashmi M, Saleh M (2003) Outcome of complex fractures of the tibial plateau treated with a beam-loading ring fixation system. J Bone Jt Surg Br 85:691–699
Ali AM, Burton M, Hashmi M, Saleh M (2003) Treatment of displaced bicondylar tibial plateau fractures (OTA-41C2&3) in patients older than 60 years of age. J Orthop Trauma 17:346–352
Assink N, Kraeima J, Meesters AML, El Moumni M, Bosma E, Nijveldt RJ et al (2022) 3D assessment of initial fracture displacement of tibial plateau fractures is predictive for risk on conversion to total knee arthroplasty at long-term follow-up. Eur J Trauma Emerg Surg. https://doi.org/10.1007/s00068-022-02139-y
Biyani A, Reddy NS, Chaudhury J, Simison AJ, Klenerman L (1995) The results of surgical management of displaced tibial plateau fractures in the elderly. Injury 26:291–297
Boldin C, Fankhauser F, Hofer HP, Szyszkowitz R (2006) Three-year results of proximal tibia fractures treated with the LISS. Clin Orthop Relat Res 445:222–229
Brockman BS, Maupin JJ, Thompson SF, Hollabaugh KM, Thakral R (2020) Complication rates in total knee arthroplasty performed for osteoarthritis and post-traumatic arthritis: a comparison study. J Arthroplasty 35:371–374
Brodke DJ, Morshed S (2021) Low surgeon and hospital volume increase risk of early conversion to total knee arthroplasty after tibial plateau fixation. J Am Acad Orthop Surg 29:25–34
Cavallero M, Rosales R, Caballero J, Virkus WW, Kempton LB, Gaski GE (2018) Locking plate fixation in a series of bicondylar tibial plateau fractures raises treatment costs without clinical benefit. J Orthop Trauma 32:333–337
Chan C, Keating J (2012) Comparison of outcomes of operatively treated bicondylar tibial plateau fractures by external fixation and internal fixation. Malays Orthop J 6:7–12
Citak C, Kayali C, Ozan F, Altay T, Karahan HG, Yamak K (2019) Lateral locked plating or dual plating: a comparison of two methods in simple bicondylar tibial plateau fractures. Clin Orthop Surg 11:151–158
Dall’oca C, Maluta T, Lavini F, Bondi M, Micheloni GM, Bartolozzi P (2012) Tibial plateau fractures: compared outcomes between ARIF and ORIF. Strateg Trauma Limb Reconstr 7:163–175
Elsoe R, Johansen MB, Larsen P (2019) Tibial plateau fractures are associated with a long-lasting increased risk of total knee arthroplasty a matched cohort study of 7950 tibial plateau fractures. Osteoarthr Cartil 27:805–809
Elsoe R, Larsen P, Petruskevicius J, Kold S (2018) Complex tibial fractures are associated with lower social classes and predict early exit from employment and worse patient-reported QOL: a prospective observational study of 46 complex tibial fractures treated with a ring fixator. Strateg Trauma Limb Reconstr 13:25–33
Elsoe R, Larsen P, Shekhrajka N, Ferreira L, Ostgaard SE, Rasmussen S (2016) The outcome after lateral tibial plateau fracture treated with percutaneus screw fixation show a tendency towards worse functional outcome compared with a reference population. Eur J Trauma Emerg Surg 42:177–184
Elsøe R, Larsen P, Rasmussen S, Hansen HA, Eriksen CB (2016) High degree of patient satisfaction after percutaneous treatment of lateral tibia plateau fractures. Dan Med J 63:A5174
Foulke BA, Kendal AR, Murray DW, Pandit H (2016) Fracture healing in the elderly: a review. Maturitas 92:49–55
Frattini M, Vaienti E, Soncini G, Pogliacomi F (2009) Tibial plateau fractures in elderly patients. Chir Organi Mov 93:109–114
Gonzalez LJ, Hildebrandt K, Carlock K, Konda SR, Egol KA (2020) Patient function continues to improve over the first five years following tibial plateau fracture managed by open reduction and internal fixation. Bone Jt J 102:632–637
Hansen L, Larsen P, Elsoe R (2022) Characteristics of patients requiring early total knee replacement after surgically treated lateral tibial plateau fractures: a comparative cohort study. Eur J Orthop Surg Traumatol 32:1097–1103
Honkonen SE (1994) Indications for surgical treatment of tibial condyle fractures. Clin Orthop Relat Res 302:199–205
Hsu CJ, Chang WN, Wong CY (2001) Surgical treatment of tibial plateau fracture in elderly patients. Arch Orthop Trauma Surg 121:67–70
Huang JF, Shen JJ, Chen JJ, Tong PJ (2016) Primary total knee arthroplasty for elderly complex tibial plateau fractures. Acta Orthop Traumatol Turc 50:702–705
Kalmet PHS, Van Horn YY, Sanduleanu S, Seelen HAM, Brink PRG, Poeze M (2019) Patient-reported quality of life and pain after permissive weight bearing in surgically treated trauma patients with tibial plateau fractures: a retrospective cohort study. Arch Orthop Trauma Surg 139:483–488
Keightley AJ, Nawaz SZ, Jacob JT, Unnithan A, Elliott DS, Khaleel A (2015) Ilizarov management of Schatzker IV to VI fractures of the tibial plateau: 105 fractures at a mean follow-up of 7.8 years. Bone Jt J 97-B:1693–1697
Kim JK, Hwang KT, Soh HS, Shon OJ, Park KC (2022) Comparison of tibial plateau fracture surgical outcomes between young and elderly patients: are outcomes really poorer in the elderly? Arch Orthop Trauma Surg 142:2419–2427
Krupp RJ, Malkani AL, Roberts CS, Seligson D, Crawford CH, Smith L (2009) Treatment of bicondylar tibia plateau fractures using locked plating versus external fixation. Orthopedics 32:559
Manidakis N, Dosani A, Dimitriou R, Stengel D, Matthews S, Giannoudis P (2010) Tibial plateau fractures: functional outcome and incidence of osteoarthritis in 125 cases. Int Orthop 34:565–570
Mehin R, O’Brien P, Broekhuyse H, Blachut P, Guy P (2012) Endstage arthritis following tibia plateau fractures: average 10-year follow-up. Can J Surg 55:87–94
Meinberg EG, Clark D, Miclau KR, Marcucio R, Miclau T (2019) Fracture repair in the elderly: clinical and experimental considerations. Injury 50(Suppl 1):S62–S65
Munn Z, Barker TH, Moola S, Tufanaru C, Stern C, McArthur A et al (2020) Methodological quality of case series studies: an introduction to the JBI critical appraisal tool. JBI Evid Synth 18:2127–2133
Ochen Y, Peek J, McTague MF, Weaver MJ, van der Velde D, Houwert RM et al (2020) Long-term outcomes after open reduction and internal fixation of bicondylar tibial plateau fractures. Injury 51:1097–1102
Oladeji LO, Dreger TK, Pratte EL, Baumann CA, Stannard JP, Volgas DA et al (2019) Total knee arthroplasty versus osteochondral allograft: prevalence and risk factors following tibial plateau fractures. J Knee Surg 32:380–386
Page MJ, Moher D, Bossuyt PM, Boutron I, Hoffmann TC, Mulrow CD et al (2021) PRISMA 2020 explanation and elaboration: updated guidance and exemplars for reporting systematic reviews. BMJ 372:n160
Pinter Z, Jha AJ, McGee A, Paul K, Lee S, Dombrowsky A et al (2020) Outcomes of knee replacement in patients with posttraumatic arthritis due to previous tibial plateau fracture. Eur J Orthop Surg Traumatol 30:323–328
Prat-Fabregat S, Camacho-Carrasco P (2016) Treatment strategy for tibial plateau fractures: an update. EFORT Open Rev 1:225–232
Rademakers MV, Kerkhoffs GM, Sierevelt IN, Raaymakers EL, Marti RK (2007) Operative treatment of 109 tibial plateau fractures: five- to 27-year follow-up results. J Orthop Trauma 21:5–10
Ramos T, Ekholm C, Eriksson BI, Karlsson J, Nistor L (2013) The Ilizarov external fixator–a useful alternative for the treatment of proximal tibial fractures. A prospective observational study of 30 consecutive patients. BMC Musculoskelet Disord 14:11
Roerdink WH, Oskam J, Vierhout PA (2001) Arthroscopically assisted osteosynthesis of tibial plateau fractures in patients older than 55 years. Arthroscopy 17:826–831
Row ER, Komatsu DE, Watson JT, Jones C, Kottmeier S (2018) Staged prone/supine fixation of high-energy multicolumnar tibial plateau fractures: a multicenter analysis. J Orthop Trauma 32:e117–e122
Scott BL, Lee CS, Strelzow JA (2020) Five-year risk of conversion to total knee arthroplasty after operatively treated periarticular knee fractures in patients over 40 years of age. J Arthroplasty 35:2084-2089.e2081
Shimizu T, Sawaguchi T, Sakagoshi D, Goshima K, Shigemoto K, Hatsuchi Y (2016) Geriatric tibial plateau fractures: clinical features and surgical outcomes. J Orthop Sci 21:68–73
Simpson D, Keating JF (2004) Outcome of tibial plateau fractures managed with calcium phosphate cement. Injury 35:913–918
Softness KA, Murray RS, Evans BG (2017) Total knee arthroplasty and fractures of the tibial plateau. World J Orthop 8:107–114
Su EP, Westrich GH, Rana AJ, Kapoor K, Helfet DL (2004) Operative treatment of tibial plateau fractures in patients older than 55 years. Clin Orthop Relat Res 421:240–248
Tapper VS, Pamilo KJ, Haapakoski JJ, Toom A, Paloneva J (2022) Risk of total knee replacement after proximal tibia fracture: a register-based study of 7,841 patients. Acta Orthop 93:179–184
Tarng YW, Lin KC (2019) A combined prone and supine approaches for complex three column tibial plateau fracture with posterolateral articular injury. Injury 50:1756–1763
Timmers TK, van der Ven DJ, de Vries LS, van Olden GD (2014) Functional outcome after tibial plateau fracture osteosynthesis: a mean follow-up of 6 years. Knee 21:1210–1215
van Dreumel RL, van Wunnik BP, Janssen L, Simons PC, Janzing HM (2015) Mid- to long-term functional outcome after open reduction and internal fixation of tibial plateau fractures. Injury 46:1608–1612
Vestergaard V, Becic Pedersen A, Borbjerg Hare K, MorvilleSchrøder H, Troelsen A (2020) Knee fracture increases TKA risk after initial fracture treatment and throughout life. Clin Orthop Relat Res 478:2036–2044
Warner SJ, Garner MR, Schottel PC, Fabricant PD, Thacher RR, Loftus ML et al (2018) The effect of soft tissue injuries on clinical outcomes after tibial plateau fracture fixation. J Orthop Trauma 32:141–147
Wasserstein D, Henry P, Paterson JM, Kreder HJ, Jenkinson R (2014) Risk of total knee arthroplasty after operatively treated tibial plateau fracture: a matched-population-based cohort study. J Bone Jt Surg Am 96:144–150
Wong MT, Bourget-Murray J, Johnston K, Desy NM (2020) Understanding the role of total knee arthroplasty for primary treatment of tibial plateau fracture: a systematic review of the literature. J Orthop Traumatol 21:7
Funding
Open access funding provided by Johannes Kepler University Linz. Supported by Johannes Kepler Open Access Publishing Fund. The authors received no specific funding for this work.
Author information
Authors and Affiliations
Contributions
All authors contributed to the conception of the systematic review. HDJ, KN, KA: study design, literature screening, data extraction. HDJ, KN, WPW: study assessment, data analysis, statistical analysis. HDJ, KN: drafting manuscript, tables, and figures. WPW, GT, KA: revision manuscript, tables, and figures. The final version was approved by all authors.
Corresponding author
Ethics declarations
Conflict of interest
We declare that there is no conflict of interest that could be perceived as prejudicing the impartiality of the research reported.
Ethical approval
Not applicable.
Informed consent
Not applicable.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if changes were made. The images or other third party material in this article are included in the article's Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article's Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
Haslhofer, D.J., Kraml, N., Winkler, P.W. et al. Risk for total knee arthroplasty after tibial plateau fractures: a systematic review. Knee Surg Sports Traumatol Arthrosc 31, 5145–5153 (2023). https://doi.org/10.1007/s00167-023-07585-8
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00167-023-07585-8