Abstract
Natural killer (NK) cells mediate potent anti-tumor responses, which makes them attractive targets for immunotherapy. The anti-tumor response of endogenous- or allogeneic NK cells can be enhanced through clinically available monoclonal antibodies that mediate antibody-dependent cellular cytotoxicity (ADCC). NK cell activation is regulated by interaction of inhibitory receptors with classical- and non-classical human leukocyte antigens (HLA) class I molecules. Inhibitory receptors of the killer immunoglobulin-like receptor (KIR) family interact with HLA-A, -B or –C epitopes, while NKG2A interacts with the non-classical HLA-E molecule. Both types of inhibitory interactions may influence the strength of the ADCC response. In the present review, we provide an overview of the effect of inhibitory KIRs and NKG2A on NK cell-mediated ADCC, which highlights the rationale for combination strategies with ADCC triggering antibodies and interference with the NK cell relevant inhibitory immune checkpoints, such as KIR and NKG2A.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Natural killer cells are potent mediators of antibody-dependent cellular cytotoxicity
Natural killer (NK) cells are innate immune cells that can mediate potent cytotoxic responses against cancer cells without the need for prior exposure to tumor-associated antigens. NK cells recognize a potential target cell by a broad array of membrane-associated receptors that interact with activating- or inhibitory ligands expressed by the target cell [1]. NK cell effector function is triggered when the net result of engagement via activating NK cell receptors is stronger than the inhibitory signals provided by the target cell [2]. NK cells can distinguish diseased cells from healthy cells through enhanced levels of activating ligands on virally infected or malignantly transformed cells. Healthy cells normally do not express high levels of these molecules as most activating NK cell ligands are molecules associated with cellular stress, malignant transformation or viral infection [1, 2]. The inhibitory receptors, on the other hand, set the threshold for NK cell activation. The most important group of inhibitory ligands are the Human Leukocyte Antigen (HLA) class I molecules expressed on virtually every healthy cell and which protect them from killing by NK cells [1, 2].
NK cells can mediate several effector functions and the most well-known is the killing of diseased cells through the release of granules containing perforin and granzymes or in a death receptor-dependent manner. In addition, they mediate helper functions through the release of cytokines like IFNγ that promote type 1 anti-tumor immunity [2]. NK cells are also potent mediators of antibody-dependent cellular cytotoxicity (ADCC). NK cell ADCC is mediated by the binding of the low affinity Fc-receptor, FcɣRIIIa or CD16, with antibodies bound to target cells [1]. FcɣRIIIa preferably interacts with antibodies of the IgG1 or IgG3 isotype in humans and the glycosylation- and fucosylation status of the antibody have been shown to impact the strength of the response [3]. Genetic variation of the FcɣRIIIa receptor can further influence the response and 234 single nucleotide polymorphisms (SNP) have been described in the FCGR3A gene, in coding and in non-coding regions [4]. The FcɣRIIIA-F158V polymorphism (rs396991) is the best characterized SNP in the FCGR3A gene with a functional effect. It is the result of a single nucleotide substitution from T to G at cDNA nucleotide position 559 leading to two different FcɣRIIIa allotypes: the high affinity variant with a valine (V) on amino acid position 158 and a lower affinity variant with a phenylalanine (F) at amino acid position 158 [5]. FcɣRIIIa signals via an intracellular CD3Ϛ domain and interaction with the Fc part of an antibody, bound to its target, provides a very strong activating signal to the NK cell. Engagement of only the FcɣRIIIa with an ADCC-inducing antibody is sufficient to trigger NK cell activation, which is in contrast to most other activating NK cell receptors for which signaling via at least two activating receptors is needed [6]. In a clinical trial with the ADCC-inducing antibody isatuximab, FcɣRIIIa 158 V correlated with a prolonged progression-free survival in relapsed or refractory multiple myeloma, which was mechanistically supported in in vitro assays showing enhanced NK cell-mediated ADCC [7]. This property and the option to enhance the NK cell response in a tumor-specific- or tumor-associated manner makes the use of ADCC-inducing antibodies a popular way to therapeutically boost the NK cell anti-tumor response.
Regulation of NK cell function by interaction of inhibitory NK cell receptors and HLA class I ligands
NK cells express a variety of receptors interacting with HLA class I ligands, among them activating- and inhibitory members of the family of killer immunoglobulin like receptors (KIRs) and NKG2A. Like their HLA ligands, the KIR genes are highly polymorphic. Therefore, many different protein variants and haplotypes exist, and KIR repertoires are further shaped by copynumber variation. Activating family members are named KIRxDSx as they possess a short (S) intracellular ITAM domain providing activating intracellular signaling. Depending on the presence of 2 or 3 extracellular immunoglobulin domains (D) they are named KIR2DSx or KIR3DSx [8]. Activating KIRs can interact with HLA class I, e.g., KIR2DS1 and KIR2DS2 with HLA-C and KIR2DS4 with HLA-C*05:01 [9], but the ligands for several of the other activating KIRs remain elusive. Inhibitory KIR (iKIR) family members express a long (L) intracellular domain leading to an inhibitory signaling cascade upon ligand interaction, which names them KIRxDLx and iKIRs typically recognize HLA class I molecules. The most frequently studied are KIR2DL1 interacting with HLA-C alleles possessing the C2 epitope characterized by a Lysine at aa position 80; KIR2DL2 or KIR2DL3 interacting with HLA-C alleles having the C1 epitope with a Asparagine at aa position 80 [10] and KIR3DL1 binding to HLA-B alleles with a Bw4 epitope or to HLA-A23, -A24 or –A32 [11].
iKIRs have a dual role regulating NK cell activation. The interaction between iKIRs and their HLA class I ligands results in an enhanced potential of the NK cell to respond to diseased cells upon engagement with an activating ligand, a process called “NK cell licensing” [12]. As a result, NK cells that do not express any inhibitory receptor for HLA class I are considered to be hyporesponsive unless they receive a very strong activating signal. Licensed NK cells more vigorously respond to a potential target cell [12, 13]. While iKIRs promote NK cell function through licensing, they also act as strong inhibitory immune checkpoints to control effector function of licensed NK cells. By doing so, iKIRs protect healthy cells from being killed by NK cells through the binding to their respective HLA class I ligands abundantly present on a healthy cell. In contrast to T cells, NK cells recognize HLA epitopes rather than individual HLA alleles, though they can sense to some extend alterations in the HLA peptidome [9]. This is also the reason why NK cells do not cause graft versus host pathology in an allogenic setting with HLA discrepancy which is in sharp contrast to T cells and a great benefit when exploiting NK cells for immunotherapy purposes [14].
The heterodimer CD94:NKG2A interacts with the non-classical HLA class I molecule, HLA-E. With only two frequently occurring protein variants, HLA-E is much less polymorphic than the classical class I molecules HLA-A, -B and –C [15]. While iKIRs are typically expressed on the highly mature NK cell subsets and exclusively on the cytotoxic CD56dim subset, NKG2A can also be found on less mature NK cells as well as on the cytokine producing CD56bright subset. NK cells can (co-)express one or a combination of inhibitory receptors, but, the percentage of NKG2A expressing NK cells in peripheral blood is usually much higher than the percentage of KIR expressing NK cells (20–80% for NKG2A vs. 0–15% for iKIRs) [16]. Like the iKIRs, NKG2A is involved in NK cell licensing and it sets the activation threshold for licensed NK cells and protects HLA-E expressing cells from killing by NK cells [15].
NKG2A and iKIRs as inhibitory immune checkpoint controllers for NK cell anti-tumor reactivity
In the quest to cure cancer, there is a booming interest in targeting inhibitory immune checkpoint molecules like PD1 and CTLA-4, which even resulted in the awarding of the Nobel Prize for medicine in 2018 to Allison and Honjo. In the past years, many other inhibitory immune checkpoint receptors have been identified, among them TIM-3, LAG-3, TIGIT and CD96. Under homeostatic conditions, these molecules mediate immune tolerance by providing negative feedback loops and controlling excessive immune cell activation. The downside of these receptors is that they also negatively impact anti-tumor immunity as their inhibitory ligands are frequently expressed on tumor cells or tumor-accessory cells, and the receptors themselves are often expressed on tumor infiltrating T cells (TILs), or on T cells in tumor draining lymph nodes and this expression has been associated with an exhausted functional T cell profile [17]. Immunotherapy with monoclonal antibodies blocking the interaction between the receptors and their ligands in the tumor itself or in the draining lymph node has been shown to enhance priming of anti-tumor CD4 and CD8 T cells and to release TILs from inhibition in animal models as well as in human [17]. The enormous potential of targeting these inhibitory receptors has been clearly exemplified in several of the clinical studies performed in humans with for example nivolumab, ipilimumab or pembrolizumab, that may provide clinical responses in some patients [18].
In contrast to the effect on T cells, the role of those prototypic immune checkpoint molecules in NK cells is much less clear and there is a lot of debate on, for example, the functional relevance of PD1 for NK cells [19]. Regarding its ligand PD-L1, one study indicates that PD-L1 targeting may be beneficial in PD-L1-negative tumors and that this is mediated through the direct binding of monoclonal antibodies to tumor-induced PD-L1 expression on the NK cells [20]. Besides PD-L1, NKG2A and the iKIRs are additional controllers of NK cell reactivity against self- and non-diseased cells and can therefore also be considered as critical inhibitory immune checkpoint receptors for NK cells. Hence, potentiating NK cell anti-tumor responses via the blockade of inhibitory interactions between KIRs or NKG2A and their HLA ligands is a highly interesting approach to boost the curative potential of NK-based therapies. Antibodies like lirilumab (anti-KIR) and monalizumab (anti-NKG2A) have been developed and tested for this purpose [21, 22]. While many tumors reduce or even completely lose HLA class I expression to escape from CD8 T cells, they frequently maintain or even enhance expression of HLA-E, presumably to protect them from killing by NKG2A-positive NK cells (thus the majority of NK cells) [23]. This makes NKG2A an especially interesting candidate to further target in clinical trials [22]. Currently, there are 16 trials registered at Clinicaltrials.gov that study the potential for monalizumab in cancer. In addition, lirilumab is being used in 13 clinical trials. Both monalizumab and lirilumab are utilized in combination with other therapeutic agents in the majority of these studies. Although these types of combination therapies have been well tolerated by patients, they do not yet result in optimal stimulation of NK cell anti-tumor efficacy and the exact combination resulting in optimal NK cell anti-tumor efficacy remains to be determined. While the stop of the INTERLINK-1 Phase 3 trial studying monalizumab with cetuximab (NCT04590963) was recently announced, other studies with different combination therapies, such as monalizumab with durvalumab, are ongoing (e.g., NCT05221840 and NCT02671435). It will be interesting to unravel the underlying reasons for the lack of improved survival and to understand how the treatment affected NK cells.
When NK cells are used in an allogeneic setting, interaction between iKIR and HLA can also be reduced through selection of so-called KIR-ligand mismatched donors [24]. The beneficial effect of a KIR-ligand mismatch became clear from animal- and human studies showing an NK mediated improved clinical outcome in leukemia patients upon haploidentical stem cell transplantation when KIR-ligand mismatched donors were selected [25]. Our group obtained comparable results in a mouse breast cancer model, providing evidence that the concept may also be relevant for solid tumors [26]. Furthermore, we and others demonstrated in in vitro models that KIR-ligand mismatched NK cells were more responsive to HLA class I expressing tumor cells, even in a setting where the NK cells were highly activated by IL-2 [27,28,29].
Triggering ADCC as a way to potentiate the NK cell anti-tumor response
The development of the hybridoma technology as well as more recent approaches to produce and optimize monoclonal antibodies for therapeutic purposes has revolutionized the cancer immunotherapy field. A plethora of clinical grade antibodies are currently available and many of them act in a multimodal way; for example, via deprivation of tumor growth factors, by triggering complement-dependent cytotoxicity (CDC), by promoting opsonization and subsequent degradation by macrophages, by potentiating the immune response through blockade of inhibitory receptors, and/or by triggering Fc receptor mediated ADCC [30]. Since monoclonal antibodies can be used in an off the shelf manner, they are attractive candidates to combine with other immunotherapeutic strategies that exploit the anti-tumor function of endogenous NK cells or allogeneic NK cells in a transplantation or adoptive transfer setting. Several monoclonal antibodies have been shown to induce ADCC mediated by NK cells and frequently studied examples are trastuzumab for Her2 expressing tumors, cetuximab (anti-EGFR), rituximab or obinutuzumab (anti-CD20) for B cell malignancies, daratumumab (anti-CD38) or elotuzumab (anti-CS1) in multiple myeloma (reviewed in [31]).
Influence of KIR and NKG2A on NK cell-mediated antibody-dependent cellular cytotoxicity
In the setting where tumor-specific ADCC triggering antibodies are used to promote NK cell activation, NK cells will receive a very strong activating signal which may override the inhibitory effects of KIR/NKG2A interaction with HLA class I. Several in vitro studies have explored the influence of KIR-ligand interaction and licensing status of the NK cell on the outcome of ADCC (Table 1 and Fig. 1). Most studies used rituximab (anti-CD20) to potentiate the NK cell response against B cell leukemias, in neuroblastoma ADCC can be triggered with anti-GD2, while in multiple myeloma daratumumab (anti-CD38) was used. All studies that addressed the role of licensing status of the NK cell demonstrated that both licensed- and non-licensed NK cells could mediate ADCC upon engagement of an antibody coated target cell [32,33,34]. Importantly, this showed that the hyporesponsive NK cell subsets, lacking expression of iKIRs, are also effective effector cells and can contribute to the overall anti-tumor response of bulk NK cells when an ADCC triggering antibody is present. Lisovsky et al.[32] separately examined the contribution of education to antibody-dependent NK cell activation and found that education through KIR3DL1 and KIR2DL1, but not KIR2DL3, increased antibody-mediated secretion of IFN-γ and CCL4, compared to uneducated counterparts.
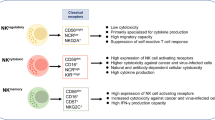
The effect of NK cell education status, KIR/HLA interaction, NKG2A/HLA-E interaction, and FCGR3A-p.158 genotypes on the efficacy of ADCC. Level of NK cell-mediated anti-tumor cytotoxicity increases from left to right. A Uneducated NK cells require stimulation by ADCC-inducing antibodies in order to target tumor cells. Moreover, maximal ADCC responses require NK cell education. B–C In educated NK cells, KIR-ligand matching provides a strong inhibitory signal, which can be overcome by adding ADCC-inducing antibodies. However, different levels of inhibition have been described for different KIR/HLA interactions. D Mismatched educated NK cells combined with ADCC-inducing antibodies have the highest level of cytotoxicity. E High levels of HLA-E can lower cytotoxic potential even though ADCC-inducing antibodies are present. Anti-NKG2A antibodies, such as monalizumab, could effectively block this interaction. F Additionally, the high affinity variant FCGR3A-p.158Val induces stronger ADCC, independent of educational status. Created with BioRender.com
All studies that addressed the potential inhibitory effect of KIR-ligand interaction on ADCC concluded that NK cells with KIRs that do not encounter their HLA ligands on the target cell mediate more potent responses than their matched counterparts [7, 28, 33, 35,36,37]. Kohrt et al. [37] observed that inhibition via KIR-ligand interaction was relevant when rituximab was used to trigger ADCC against CD20 expressing B cells but not when the Fc optimized variant obinutuzumab was used to trigger ADCC, illustrating that the exact nature of the antibody is important as well [37]. Of relevance, there are indications that not all KIR-ligand interactions mediate similar levels of ADCC inhibition. Makanga et al. [35] described that KIR2DL1/HLA-C C2 + and KIR3DL1/HLA-B Bw4 + signaling strongly mediated NK cell hypo-responsiveness to rituximab, whereas the effects through KIR2DL2/3 with HLA-C C1 + were less pronounced. This is consistent with findings by Sun et al. [7], where isatuximab-mediated ADCC was suppressed by KIR2DL1/HLA-C2 + interaction.
Non-classical HLA class I may also affect efficacy of ADCC. HLA-G interaction with KIR2DL4, which is present in all KIR haplotypes, inactivates NK cells and desensitizes breast cancer cells to trastuzumab treatment. In HLA-G-negative tumors, KIR2DL4 promotes ADCC through an IFN-γ-mediated feedback circuit until IFN-γ eventually upregulates PD-L1 on cancer cells [38]. Therefore, interfering with HLA-G/KIR2DL4 signaling combined with PD-L1/PD-1 targeting may potentiate trastuzumab treatment in those resistant cancers.
Albeit its frequent expression on NK cells, the role of NKG2A is relatively unexplored. Our group demonstrated that NK cells licensed via NKG2A mediated more potent anti-myeloma responses than unlicensed NK cells [28]. Furthermore, co-expression of NKG2A did not reduce the magnitude of the response against target cells expressing low- or intermediate levels of HLA-E when the NK cells were highly activated by IL-2 and in the presence of an ADCC triggering monoclonal antibody (moAb). High levels of HLA-E expression on target cells did however significantly reduce the NK cell response, indicating that the density of the inhibitory ligands is important as well [28].
NK cells, like many other immune effector cells, can be severely hampered in mediating their anti-tumor effects by an immunosuppressive tumor microenvironment (TME) including factors like hypoxia, prostaglandin E2, lactate and suppressive tumor-accessory cells [39, 40]. This emphasizes the need to develop combination strategies to facilitate anti-tumor immune effector functions. In vitro data, as well as several clinical studies encouragingly show that ADCC mediating moAb can promote NK function even under suppressive conditions (reviewed in [29]). Given the strong inhibitory effects of especially KIR-ligand interaction, interfering with these immune checkpoint molecules may be a way to further enhance the response. In a setting where endogenous NK cells are targeted, this can be done by using moAb with specificity for KIRs (e.g., lirilumab), as has been done in for example myeloma [41] or in tumors with high levels of HLA-E by using monalizumab [22]. In an allogeneic setting, selection of KIR-ligand mismatched donors may be an alternative strategy. Though, the additive effect of KIR-ligand mismatching in a transplant setting is still controversial and seems to be highly dependent on the exact transplantation setting. Furthermore, it may be interesting to further explore the synergistic effect of targeting KIR/NKG2A when chimeric antigen receptors (CARs) are used to redirect and enhance the NK cell anti-tumor response an alternative for ADCC triggering antibodies.
In either case, minimizing NK cell inhibition by interfering with KIR/NKG2A or any other relevant inhibitory immune checkpoint receptors, in combination with an approach to maximize NK cell activation via engagement of CD16 or a CAR may help to potentiate the NK cell anti-tumor effects which will be especially relevant for tumors with a highly suppressive TME.
References
Vivier E et al (2008) Functions of natural killer cells. Nat Immunol 9(5):503–510
Campbell KS, Hasegawa J (2013) Natural killer cell biology: an update and future directions. J Allergy Clin Immunol 132(3):536–544
Wang W et al (2015) NK cell-mediated antibody-dependent cellular cytotoxicity in cancer immunotherapy. Front Immunol 6:368
Mahaweni NM et al (2018) A comprehensive overview of FCGR3A gene variability by full-length gene sequencing including the identification of V158F polymorphism. Sci Rep 8(1):15983
Bowles JA, Weiner GJ (2005) CD16 polymorphisms and NK activation induced by monoclonal antibody-coated target cells. J Immunol Methods 304(1–2):88–99
Bryceson YT et al (2006) Synergy among receptors on resting NK cells for the activation of natural cytotoxicity and cytokine secretion. Blood 107(1):159–166
Sun H et al (2021) Individualized genetic makeup that controls natural killer cell function influences the efficacy of isatuximab immunotherapy in patients with multiple myeloma. J Immunother Cancer 9(7):556
Long EO, Colonna M, Lanier LL (1996) Inhibitory MHC class I receptors on NK and T cells: a standard nomenclature. Immunol Today 17(2):100
Pende D et al (2019) Killer Ig-like receptors (KIRs): their role in NK cell modulation and developments leading to their clinical exploitation. Front Immunol 10:1179
Colonna M et al (1993) HLA-C is the inhibitory ligand that determines dominant resistance to lysis by NK1- and NK2-specific natural killer cells. Proc Natl Acad Sci U S A 90(24):12000–12004
Stern M et al (2008) Human leukocyte antigens A23, A24, and A32 but not A25 are ligands for KIR3DL1. Blood 112(3):708–710
Kim S et al (2005) Licensing of natural killer cells by host major histocompatibility complex class I molecules. Nature 436(7051):709–713
Anfossi N et al (2006) Human NK cell education by inhibitory receptors for MHC class I. Immunity 25(2):331–342
Sutlu T, Alici E (2009) Natural killer cell-based immunotherapy in cancer: current insights and future prospects. J Intern Med 266(2):154–181
Braud VM et al (1998) HLA-E binds to natural killer cell receptors CD94/NKG2A, B and C. Nature 391(6669):795–799
Fauriat C et al (2008) Estimation of the size of the alloreactive NK cell repertoire: studies in individuals homozygous for the group A KIR haplotype. J Immunol 181(9):6010–6019
Wei SC, Duffy CR, Allison JP (2018) Fundamental mechanisms of immune checkpoint blockade therapy. Cancer Discov 8(9):1069–1086
Magee D et al (2020) Adverse event profile for immunotherapy agents compared with chemotherapy in solid organ tumors: a systematic review and meta-analysis of randomized clinical trials. Ann Oncol 31(1):50–60
Judge SJ et al (2020) Minimal PD-1 expression in mouse and human NK cells under diverse conditions. J Clin Investig 130(6):3051–3068
Dong W et al (2019) The mechanism of anti–pd-l1 antibody efficacy against pd-l1–negative tumors identifies nk cells expressing pd-l1 as a cytolytic effector. Cancer Discov 9(10):1422–1437
Alici E (2010) IPH-2101, a fully human anti-NK-cell inhibitory receptor mAb for the potential treatment of hematological cancers. Curr Opin Mol Ther 12(6):724–733
Andre P et al (2018) Anti-NKG2A mAb Is a Checkpoint Inhibitor that Promotes Anti-tumor Immunity by Unleashing Both T and NK Cells. Cell 175(7):1731-1743 e13
Wieten L et al (2014) Clinical and immunological significance of HLA-E in stem cell transplantation and cancer. Tissue Antigens 84(6):523–535
Ruggeri L et al (2002) Effectiveness of donor natural killer cell alloreactivity in mismatched hematopoietic transplants. Science 295(5562):2097–2100
Ruggeri L et al (2007) Donor natural killer cell allorecognition of missing self in haploidentical hematopoietic transplantation for acute myeloid leukemia: challenging its predictive value. Blood 110(1):433–440
Frings PW et al (2011) Elimination of the chemotherapy resistant subpopulation of 4T1 mouse breast cancer by haploidentical NK cells cures the vast majority of mice. Breast Cancer Res Treat 130(3):773–781
Ehlers FA et al (2021) ADCC-inducing antibody trastuzumab and selection of KIR-HLA ligand mismatched donors enhance the NK cell anti-breast cancer response. Cancers 13(13):3232
Mahaweni NM et al (2018) NKG2A expression is not per se detrimental for the anti-multiple myeloma activity of activated natural killer cells in an In vitro system mimicking the tumor microenvironment. Front Immunol 9(1415):6628
Mahaweni NM et al (2018) Tuning natural killer cell anti-multiple myeloma reactivity by targeting inhibitory signaling via KIR and NKG2A. Front Immunol 9:2848
Scott AM, Wolchok JD, Old LJ (2012) Antibody therapy of cancer. Nat Rev Cancer 12(4):278–287
Vacchelli E et al (2015) Trial watch: Tumor-targeting monoclonal antibodies for oncological indications. Oncoimmunology 4(1):556
Lisovsky I et al (2019) Differential contribution of education through KIR2DL1, KIR2DL3, and KIR3DL1 to antibody-dependent (AD) NK cell activation and ADCC. J Leukoc Biol 105(3):551–563
Nguyen R et al (2018) The role of interleukin-2, all-trans retinoic acid, and natural killer cells: surveillance mechanisms in anti-GD2 antibody therapy in neuroblastoma. Cancer Immunol Immunother 67(4):615–626
Tarek N et al (2012) Unlicensed NK cells target neuroblastoma following anti-GD2 antibody treatment. J Clin Invest 122(9):3260–3270
Makanga DR et al (2021) Low number of KIR ligands in lymphoma patients favors a good rituximab-dependent NK cell response. OncoImmunology 10(1):1936392
Forlenza CJ et al (2016) KIR3DL1 allelic polymorphism and HLA-B epitopes modulate response to anti-GD2 monoclonal antibody in patients with neuroblastoma. J Clin Oncol 34(21):2443–2451
Kohrt HE et al (2014) Anti-KIR antibody enhancement of anti-lymphoma activity of natural killer cells as monotherapy and in combination with anti-CD20 antibodies. Blood 123(5):678–686
Zheng G et al (2021) Interaction between HLA-G and NK cell receptor KIR2DL4 orchestrates HER2-positive breast cancer resistance to trastuzumab. Signal Transduct Target Ther 6(1):1–15
Melaiu O et al (2020) Influence of the tumor microenvironment on NK cell function in solid tumors. Front Immunol 10:3038
Vitale M et al (2014) Effect of tumor cells and tumor microenvironment on NK-cell function. Eur J Immunol 44(6):1582–1592
Nijhof IS et al (2015) Daratumumab-mediated lysis of primary multiple myeloma cells is enhanced in combination with the human anti-KIR antibody IPH2102 and lenalidomide. Haematologica 100(2):263–268
Borgerding A et al (2010) B-lymphoma cells escape rituximab-triggered elimination by NK cells through increased HLA class I expression. Exp Hematol 38(3):213–221
Chan WK et al (2012) Antibody-dependent cell-mediated cytotoxicity overcomes NK cell resistance in MLL-rearranged leukemia expressing inhibitory KIR ligands but not activating ligands. Clin Cancer Res 18(22):6296–6305
Erbe AK et al (2019) Follicular lymphoma patients with KIR2DL2 and KIR3DL1 and their ligands (HLA-C1 and HLA-Bw4) show improved outcome when receiving rituximab. J Immunother Cancer 7(1):70
Stein MN et al (2006) Antibody-dependent cell cytotoxicity to breast cancer targets despite inhibitory KIR signaling. Anticancer Res 26(3A):1759–1763
Wang W et al (2016) Human NK cells maintain licensing status and are subject to killer immunoglobulin-like receptor (KIR) and KIR-ligand inhibition following ex vivo expansion. Cancer Immunol Immunother 65(9):1047–1059
Author information
Authors and Affiliations
Contributions
N.A.B., F.A.I.E., and L.W. wrote the main manuscript text. All authors reviewed the manuscript.
Corresponding author
Ethics declarations
Conflict of interest
G.M.J.B. is Chief Executive Officer/Chief Medical Officer/Cofounder of CiMaas, BV, Maastricht, The Netherlands.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if changes were made. The images or other third party material in this article are included in the article's Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article's Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
Beelen, N.A., Ehlers, F.A.I., Bos, G.M.J. et al. Inhibitory receptors for HLA class I as immune checkpoints for natural killer cell-mediated antibody-dependent cellular cytotoxicity in cancer immunotherapy. Cancer Immunol Immunother 72, 797–804 (2023). https://doi.org/10.1007/s00262-022-03299-x
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00262-022-03299-x