Abstract
Joint hypermobility affects approximately 30% of the United Kingdom (UK) population, characterised by the ability to move joints beyond the physiological limits. Associated conditions include Ehlers-Danlos syndrome and hypermobility spectrum disorders, affecting individuals across physical, psychological and social levels detrimentally impacting their health and wellbeing. The scoping review aims to describe the known biopsychosocial impact of joint hypermobility conditions in adults over the last decade. Additional objectives include to (1) identify the types of studies that address these factors, (2) to understand how the impact of the condition is measured and managed and (3) what healthcare professionals (HCPs) are involved. The scoping review was conducted using the five-stage framework by Arksey and O’Malley. The search strategy related to two main keywords, “hypermobility” and, “biopsychosocial” across a number of electronic databases. A pilot search was conducted to determine the suitability of the databases and terms. Following the search, the data was extracted and charted, summarised and narratively reported. 32 studies met the inclusion criteria. The majority were conducted in either the UK or United States of America and case–control in design. The biopsychosocial impact was wide-ranging including, but not limited to, musculoskeletal system and dermatology, gastroenterology, mood and anxiety disorders, education and employments. This review is the first of its kind to summarise all reported symptoms and impact of joint hypermobility conditions in adults, highlighting a clear need to promote a multidisciplinary and holistic approach in raising awareness of these conditions and improving their management.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Joint hypermobility is primarily characterised by the ability to move a joint beyond what is considered to be within the normal range of motion [1], reported to affect around 30% of the United Kingdom (UK) population [2]. The two most common conditions linked to joint hypermobility, often viewed as indistinguishable from each other, are Ehlers-Danlos syndrome [(EDS), specifically hypermobile EDS (hEDS)], an inherited connective tissue disorder [1, 3], and hypermobility spectrum disorders (HSD) [3]. The prevalence of EDS and HSD varies, one study collecting data in Wales (UK) reported a prevalence of 0.2% [4], whilst another estimated it to be 3% in the UK general population [5].
Both EDS and HSD affect individuals across physical (biological), psychological and social levels [6] with the predominant physical manifestations being joint dislocations and musculoskeletal (MSK) pain [7, 8]. Fatigue, headaches, dizziness, and gastrointestinal symptoms are also frequently reported symptoms [7, 8]. Individuals have also been found to be more likely diagnosed with a psychiatric disorder such as depression or anxiety [9] and experience depressive symptoms and feelings of angst [8]. These varied physical and psychological manifestations consequently impact the social life of an individual with EDS/HSD contributing to social isolation, financial problems, and strained relationships [8].
This is just a small insight into some of the presenting complaints and the adverse consequence on an individual’s health, quality of life (QoL) and wellbeing. Due to the wide-ranging presentations, there is understandably a lack of awareness and understanding amongst healthcare professionals (HCPs). Diagnosing either EDS or HSD is quite challenging due to the varying symptoms across multiple levels. Frequently, individuals face a long diagnostic journey, some waiting as long as 10 years [8], whilst others are often misdiagnosed, both leading to a deterioration in their health [1, 7]. Considering this, the reported prevalence is believed to be much higher than recorded in current literature, due to misdiagnosis or underreporting [4]. Training HCPs across specialities (e.g., gastroenterologists) to recognise EDS and HSD presentations could reduce the adverse health and wellbeing consequences caused by a delayed diagnosis. For example, skin hyperextensibility is another known symptom of EDS and HSD, it has therefore been suggested that dermatologists could be trained to recognise, diagnose and/or refer for appropriate management [10].
The aim of this scoping review is to map the biopsychosocial impact reported in adults with EDS and/or HSD. The biopsychosocial approach [11] acknowledges the whole impact of the condition on an individual beyond just the physical manifestations, including the symptoms of a psychological and social nature and how each manifestation interlinks with one another. How the symptoms and QoL is measured and managed, as well as HCP involvement, will also be mapped. In doing so, this will increase understanding of the condition, knowing which HCPs should be trained to recognise the condition to aid early diagnosis and develop appropriate interventions to aid its effective management.
Methods
A protocol for the review has been written and submitted prior to commencing the review [12]. The review has been conducted and reported using the five-stage framework by Arksey and O’Malley [13]: (1) identifying the research question; (2) identifying relevant studies; (3) study selection; (4) charting the data; (5) collating, summarising and reporting the results. The optional sixth step for consulting with stakeholders to inform or validate the findings was not utilised for this scoping review. The search methodology also followed the recommendations of Gasparyan et al. [14] for a biomedical review.
Identifying the research question
The primary research question was developed following the PCC (population, concept, context) framework as recommended by the Joanna Briggs Institute [15]: “What evidence exists on the biopsychosocial impact of EDS and HSD in the adult population?”.
The objectives of the scoping review were to:
-
1.
Map the known evidence of the biopsychosocial impact of EDS/HSD in the adult population.
-
2.
Identify and report the types of studies used to identify the biopsychosocial impact.
-
3.
Identify and describe how the biopsychosocial impact is measured and managed.
-
4.
Identify and describe the HCP involvement.
Identifying relevant studies
The search terms used related to two main keywords, “hypermobility” and, “biopsychosocial” in combination with the Boolean terms, “AND” and, “OR”. Eight electronic databases were searched: MEDLINE, EMBASE, AMED, CINAHL, PsycINFO, Cochrane Library, PubMed, PEDro. A secondary search of clinical trials and study protocols was conducted in clinicaltrials.gov, EU clinical trials register and the ISRCTN registry. A final hand search of reference lists of the accepted articles was later conducted. The search strategies across the databases can be viewed in Table 1.
To determine the suitability of the search terms and electronic databases, a pilot search was conducted by two of the authors (NC and MJ). The pilot search was supported by an academic librarian. Adjustments to the search terms were made as appropriate, including removing and adding new terms.
Study selection
Eligibility criteria
The inclusion criteria for the review were:
-
Adult sample (over 18 years old) with a clinical diagnosis (i.e. by a clinician or using validated tools) of a joint hypermobility condition (e.g. EDS or HSD).
-
Study designs investigating the physical (biological), psychological and/or social impact (e.g. cross-sectional, qualitative, case studies).
-
Recent literature published between 2012 and 2022, to enhance relevance of the findings to current clinical practice.
Articles were excluded from the review if:
-
Inaccessible full-text articles.
-
Full-texts unavailable in the English language.
-
Systematic or literature reviews not meeting the eligibility criteria.
Selection process
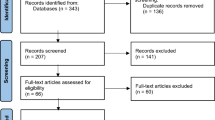
The search identified 1451 articles, of which 293 were exported following a title review. Duplicate articles were removed, leaving 182 articles for abstract review. Articles were excluded if they did not meet the inclusion criteria or abstracts were inaccessible once all attempts to retrieve abstracts were unsuccessful. Following a review of the abstracts, 118 of the articles were eligible for a full-text review, any exclusions had the reasons documented, as reviewed by two of the authors (NC and MJ). In addition, reference lists of the 32 accepted full-text articles were screened for articles that might have been missed during the database search, this resulted in 18 articles to screen and none eligible. Any uncertainties or disagreements were resolved through discussion with a third author (KS). Figure 1 represents the study selection process using a PRISMA-ScR flow diagram [16].
Charting the data
The data extraction tool was developed with headings that would accurately address the primary research question and objectives. A pilot data extraction was conducted by two of the authors (NC and MJ) during the pilot phase. The process was discussed and amendments to the tool were made as necessary to refine data collection. Queries arising during the data extraction process were discussed with the relevant senior authors (KS, LK and AR), appropriate to their area of expertise.
Data was extracted according to: (1) authors, year and country; (2) study design; (3) participant characteristics (sample size, gender, mean age and standard deviation, EDS/HSD diagnosis, recruitment date); (4) physical (biological) symptoms or conditions; (5) psychological symptoms or conditions; (6) social symptoms or conditions; (7) findings; (8) HCP involvement; (9) measurements; (10) management or treatment.
Collating, summarising and reporting the results
Data obtained within the extraction tool was collated, summarised and reported to narrate the biopsychosocial impact, symptoms and associated conditions adults with EDS/HSD. This has been presented in tabular format to supplement the narrative summary. The data was also collated, summarised and reported to acknowledge the HCP involvement, measurements and management/treatment. Verification of the data was conducted by three of the authors (NC, MJ and KS).
Results
Characteristics of included studies
Table 2 describes the characteristics of the 32 included studies. The majority of studies were conducted in either the UK or United States of America (USA) (n = 6, 19%), followed by France (n = 4, 13%) and were mostly case–control (n = 10, 31%) or cross-sectional (n = 8, 25%) in design. The sample size ranged from a total of 1 to 2404, with the majority (n = 31, 97%) having a predominantly female sample and a mean age range of 20–68.5 years (SD = 5.71–13.9).
All studies included samples with a clinical diagnosis of either EDS (inclusive of sub-types) or HSD [e.g., joint hypermobility syndrome (JHS)] as diagnosed by an appropriate clinician or validated tool. Diagnosis was mostly done by rheumatologists [17], geneticists [17], national experts in EDS [18] or primary care practitioners [19], with referrals to mental health professionals not uncommon though viewed as dismissive by individuals [20]. The Beighton Scoring System (n = 10, 31%) and Brighton Diagnostic criteria (n = 9, 28%) were most frequently used as the validated tool to support a diagnosis of joint hypermobility whilst a more recently revised diagnostic criteria for EDS was less frequently utilised (n = 3, 9%) [17, 21, 22].
Biopsychosocial impact
In this review, 31 (97%) of the included studies referred to physical manifestations whilst 29 (91%) studies referred to psychological manifestations. These manifestations were found to be either directly related to the EDS/HSD e.g., dysautonomia, or otherwise highly prevalent and clinically significant within this population e.g., anxiety and depression. Weak associations and less frequently reported symptoms and conditions have also been documented within this review for completeness. The social impact is referred to throughout the included studies (e.g., impact on QoL), more so in the qualitative studies where individuals had the opportunity to detail their lived experiences and diagnostic odyssey. The symptoms and conditions have been categorised by speciality sub-headings with Tables 3 and 4, and Fig. 2 providing more details.
MSK and dermatology
Limb hyperextension, joint flexibility, pain and dislocations are the most recognised symptoms of EDS and HSD, frequently reported throughout studies. One qualitative study [23] described how these MSK symptoms, like having a flexible body, can cause restrictions to daily living. Another [24] described how involvement from a specialist hypermobility physiotherapist improved their understanding of their own bodies via a two-way learning process which in turn motivated these individuals to engage in appropriate self-management of their condition. Within assessments of EDS/HSD, individuals are subject to dermatological evaluation [25], this is because skin hyperextensibility is as common as MSK symptoms [9, 26] with additional dermatological symptoms identified such as, thin skin [27,28,29] and abnormal scarring [9, 19]. A significant number of participants in one study [19] suggested that the MSK and skin symptoms began as early as childhood yet despite these widely recognised and long-standing symptoms, the condition is often underdiagnosed [25].
Pain and fatigue
Pain management specialists [21] can refer patients to be evaluated for a joint hypermobility condition due to the high prevalence of pain reported by this population. The pain experienced by these individuals affects the entire body including, but not limited to, back (94%) [30], knee (86%) [31], abdominal (61%) [32], foot (56%) [31], elbow (39%) [31] and neck (20%) [33]. The intensity of the pain ranges from, tiring and exhausting (93%) [19], chronic and constant (67%) [19] and severe to very severe (66%) [18]. Prevalence of fatigue is also reported to be as high as 77% [21] and can be measured using the Epworth Sleepiness Scale (ESS) [26, 34] or Fatigue Severity Scale (FSS) [25]. Fatigue and impaired sleep quality are considered to be a simultaneous experience to pain, as described by individuals with EDS/HSD, interfering with their ability to live a good QoL [23, 33]. Interestingly, some studies suggested that the presence of pain increases the likelihood of an individual with EDS/HDS also having a comorbid psychiatric disorder [9, 22].
Gastroenterology
Gastrointestinal symptoms are extremely common in this population, reported in over half of the included studies, therefore involvement from a gastroenterologist is not unusual. One retrospective study found that over 60% of their sample disclosed at least one gastrointestinal symptom at the time of their hEDS diagnosis [17]. Abdominal pain (50%) and nausea (50%) in this sample were the two most common gastrointestinal symptoms [17]. This was supported by another study, reporting higher prevalence found in an EDS sample, 79% and 71% respectively [35]. Furthermore, one study with a hEDS sample and accompanying gastrointestinal symptoms were significantly more likely to use medications for these symptoms (anti-secretory, antacids, laxatives) than the control group (p < 0.01) [32]. Though these symptoms are not considered serious, they can cause a detrimental impact to the individual’s QoL, as assessed by the Gastrointestinal Quality of Life Index (GIQLI) [35].
Autonomic nervous system (ANS) and cardiology
Dysautonomia is condition characterised by a malfunction of the ANS with associated symptoms such as dizziness, fainting and light headedness [31]. One study [21] found prevalence of dysautonomia at 70% amongst a hEDS/HSD sample, with those carrying this diagnosis significantly more likely to suffer with related symptoms, have an impaired QoL and exhibit exercise avoidance behaviours, subsequently leading to a more sedentary lifestyle. Individuals with dysautonomia and attempting to engage in physical therapy programmes are limited by the related symptoms, leading to a lack of significant improvement in their overall condition via such interventions [21]. This ANS malfunction is also responsible for postural tachycardia syndrome (PoTS), with prevalence in individuals with EDS/JHS ranging from 8% [31] to 64% [20]. Those with both JHS and PoTS were found to be at a significantly increased risk of gastrointestinal symptomology (p ≤ 0.05) [17], with higher reflux scores, regurgitation and dysphagia [36].
Rheumatology
Fibromyalgia, a chronic widespread pain (CWP) condition, has been identified in a small number of the included studies as a comorbid condition. Prevalence of the diagnosis ranges from as small as 5% [25] up to 41% [20] amongst benign JHS (BJHS) and EDS samples respectively. Interestingly, individuals with hEDS were significantly more likely to report this comorbid diagnosis if they likewise presented with gastrointestinal manifestations and chronic pain (p < 0.02) [17]. Complaints of tiring and exhausting pain were further found to be a predictive factor of a fibromyalgia diagnosis within one hEDS sample [19]. Individuals with joint hypermobility conditions have overlapping symptoms as those with fibromyalgia [31], therefore the increased likelihood of also having this CWP condition could be attributed to this reason.
Gynaecology and urology
Women are much more likely to be affected by this condition and as a result endure clinically significant urogynaecology-related symptoms like, pelvic organ prolapse (p < 0.01) [37, 38] as an example. These symptoms can have a detrimental impact on QoL, as measured by the Prolapse Quality of Life (P-QOL) [37, 38]. The impact of gynaecological issues is rarely acknowledged by the rheumatologists and primary care practitioners who predominantly make the diagnosis [38]. One study [37] found prolapse symptoms to be clinically significant across the general health perception, physical limitation, social limitation, personal relationships, emotions, sleep/energy and severity domains (p ≤ 0.05), as well as contributing to sexual and bowel dysfunctions. In addition to this, urinary incontinence was also cited as a clinically significant symptom within a BJHS sample (p < 0.01) with prevalence over 70% and a cause of significant embarrassment to women [38].
Neurology
Neurological assessments conducted by neurologists found manifestations in this population to include migraines and headaches, with severity of symptoms measured by the Migraine Disability Assessment (MIDAS) and HIT-6 [39]. Individuals with hEDS and migraines are significantly more likely to have an earlier onset of symptoms than those without hEDS (13 vs 17 years, p < 0.01), a higher number of days per month migraine episodes (15 vs 9 days, p = 0.01) and experience photophobia (p = 0.05) [39]. The migraine-related pain hEDS experience has been described as pulsating (76%) and constrictive (24%), with these individuals being significantly more likely to use migraine-related medication (e.g., NSAIDS, analgesics, triptans) (p ≤ 0.05) [39]. This is an example of the substantial impact of migraines on the QoL of hEDS individuals. However, it is still recommended that migraines are seen and managed as a separate condition rather than a sole manifestation of hEDS [39].
Respiratory
Respiratory symptoms have been inconsistently reported throughout the included studies and are quite varied, suggesting a weak association between EDS and/or HSD individuals. However, one study [34] recognises obstructive sleep apnoea (OSA) as highly prevalent yet under-recognised in HSD when compared to control groups (32% vs 6%, p < 0.01), hypopneas being the most common respiratory event within this HSD sample (64%) [34]. It may be that HSD individuals suffering from excessive daytime sleepiness and fatigue should also be assessed for OSA as a potential cause [34].
Mood and anxiety disorders
Almost half of included studies suggested EDS/HSD individuals were significantly more likely to experience mood and anxiety disorders than the general population (p < 0.01) [22]. The most frequently cited mood disorder being depression with prevalence ranging from 22% [30] to 69% [19], with anxiety having a higher prevalence at 75% [30]. The two disorders were most often measured in studies using the Hospital Anxiety and Depression Scale (HADS) [30, 40], whilst antidepressant and anxiolytic use was also noted within this sample [18]. Additional diagnoses of both mood and anxiety disorders included: major depression (ranging from 8% [41] to 37% [41]), bipolar disorder (less than 10% [20]), phobias [40] and post-traumatic stress disorder (PTSD) [9], though the latter were reported in less than 5%. Notably, one study found that HSD individuals experiencing muscle and body pain and gastrointestinal symptoms were at a significantly increased risk of experiencing depression (p < 0.01 and p < 0.03 respectively), with gastrointestinal symptoms alone being significant for anxiety (p < 0.01) [22].
Negative affect and cognition
Negative affect is the experience of negative emotions and psychological distress. This population described being fearful, specifically fear of movement [18, 26, 42]. One study utilised the Tampa Kinesiophobia Scale (TSK) to measure this, finding a statistically significant difference between individuals with EDS/HSD and without, including within the activity avoidance and somatic focus subscales (p < 0.01) [26]. Additionally, catastrophising (a cognitive distortion) was cited across two included studies. A sample of hEDS individuals with high levels of anxiety were found to score significantly higher in pain catastrophising (p < 0.01), as measured by the Pain Catastrophizing Scale (PCS) [18]. A qualitative study further offered an explanation to the above findings, describing how prior experiences of injuries have led to heightened levels of anxiety, resulting in participants catastrophising about future injuries [24]. The anxiety, fear of movement and pain catastrophising is a direct response to their unpredictable symptoms, resulting in individuals modifying or restricting their activities to avoid pain and potential injuries [26].
Eating disorders
Three case studies of young female women described EDS/JHS manifestations that contributed to the development of eating disturbances [28, 29]. Such disturbances included painful eating experiences [43] and selective eating behaviours due to temporomandibular pain and dislocations [28], as well as eating avoidance due to gastrointestinal problems like nausea and vomiting [28]. One female was diagnosed with the eating disorder anorexia nervosa (AN) and underwent an enhanced cognitive behavioural therapy programme to improve eating behaviours, body image and social functioning [29]. Notably, this study is the only that referenced a CBT programme to be utilised within this population, though specifically for an eating disorder. Additionally, their presenting symptoms which had primarily been attributed to AN could also be attributed to the EDS, specifically gastrointestinal symptoms which caused disordered eating [29].
Behavioural disorders
Three of the studies reported a comorbid diagnosis of attention deficit hyperactivity disorder (ADHD). One study found this behavioural disorder to be more frequent in EDS/HSD individuals than in the general population (5% vs 3%), though only significantly higher within those with HSD (p < 0.01) [22]. The other two studies reported a slightly higher prevalence of ADHD in EDS and hEDS samples, 7% [9] and 11% [17] respectively. The association between ADHD and EDS/HSD however, is weak and unclear and would warrant further exploration.
Psychosis, personality disorder and suicidal ideations
Including the psychiatric disorders already outlined, prevalence of others, though relatively low, have also been recognised such as, schizoaffective disorder (0.3% [22] and 1% [9]), schizotypal disorder (0.3% [22] and 1% [9]) and borderline personality disorder (4%) [9]. One study [41] examined suicidal behaviours in women with HSD finding that 31% of the sample had previously attempted suicide whilst 60% presented with a mild suicidal risk. Those with a history of suicidal attempt were also significantly more likely to have personality disturbances (p < 0.01), major depression (p < 0.03) and anxiety disorders (p < 0.04) [41].
Education and employment
The education of EDS/HSD individuals is significantly impacted, with individuals dropping out of education [20], being unable to enrol full-time [19] and when in school being subjected to bullying due to their physical appearance [28]. Similarly, these individuals also face difficulties in their professional lives, feeling unable to pursue their desired careers [20] or having to change their current role and handle less responsibilities [19]. These individuals additionally need to consider the accessibility of their workplace and their working environment to ensure it meets their needs and capabilities [44]. Changes to the individuals desired career path and working environment can contribute to reduced job satisfaction and feeling a lack of financial independence [44].
Hobbies and daily activities
Individuals with EDS/HSD are often forced to abandon their favourite hobbies or quit their athletic pursuits as a result of the many physical limitations that accompany the condition [20]. Though this is not applicable to all, some instead choose to persevere and make modifications appropriate to what they are capable of achieving and to pace themselves [24]. Whilst others simply lacked the energy, as well as the physical limitations, to participate in recreational activities and activities of daily living, such as doing housework [23]. They would often have to evaluate their energy levels and how they should distribute their energy throughout the day in order to complete simple daily household tasks (e.g., making food and going shopping) and fulfil their personal care needs (e.g., taking a shower) [22].
Social relationships
A qualitative study [6] examining the psychosocial influence in the daily life of individuals with EDS demonstrates the difficulties in maintaining social networks as a result of the debilitating symptoms that accompany the condition. They identified social isolation behaviours in some individuals due to not being able to participate in certain activities and the inability to make long-term plans. In order to be able to attend social events, these individuals must plan rest days in advance to conserve their energy, as previously discussed [22]. However, due to these behaviours and adjustments, these individuals often feel like they must justify themselves to friends and family who, like many HCPs, lack proper understanding and insight into the condition.
Miscellaneous associations and HCPs
Referrals for joint hypermobility assessments can also be made by cardiologists and orthopaedists [21]. Additional physical and psychological manifestations inconsistently cited across the 32 studies but noteworthy included: haematology [9, 22, 28], orthodontics [26, 29, 35] (e.g., dental crowding), ophthalmology [20, 22] (e.g., glaucoma), endocrinology [20], genetics [28], immunology [20], infectious disease [20], oncology [20], functional difficulties (e.g., DCD/dyspraxia) [31], learning difficulties (e.g., dyslexia [20, 22]), developmental disorders (e.g., Asperger disorder [9]) and substance use disorder (e.g., alcohol/substance use abuse [41]). Individuals with EDS/HSD also engage in complementary therapies such as acupuncture and massage [20].
Discussion
Of the 182 unique records identified, 32 studies met the inclusion criteria and informed the results discussed within this report. All included studies strongly evidenced the biopsychosocial impact of EDS and HSD on adults living with these conditions, supporting their presenting complaints to be diverse and fluctuating. Associations with some comorbidities and symptoms were found to be more significant than others, ranging in severity from person to person, all the while still demonstrating a detrimental impact to an individual’s QoL. In this review, the findings were separated into sub-specialities of physical (e.g., MSK and dermatology), psychological (e.g., negative affect and cognition) and social categories (e.g., social networks). Relationships between the sub-specialities were referenced throughout. Gastroenterology, mood disorders and anxiety disorders were evidently the most common physical and psychological manifestations of EDS/HSD with obvious implications to QoL cited across over half of the included studies.
Gastrointestinal symptoms are seemingly underdiagnosed across EDS/HSD populations despite its documented high prevalence [17, 35], though the underlying relationship is unclear [45]. These symptoms were also more likely if the individual had comorbid PoTS [9, 17], a condition knowingly linked to EDS/HSD. Similarly, having gastrointestinal symptoms increased the likelihood of individuals being diagnosed with a psychiatric disorder [22]. Eating disorders, like AN, are often diagnosed following the development of disordered eating behaviours as a result of gastrointestinal manifestations, such as nausea and bloating [29]. However, symptoms of EDS/HSD may resemble or even disguise themselves as an eating disorder and vice versa [29].
Amongst psychiatric disorders, anxiety and mood disorders (e.g., depression) were supported to be significantly more frequent in this population compared to the general population. One study argued that these disorders are a major feature of EDS and often these individuals are stigmatised by clinicians for having a mental health disorder without further investigation for the underlying cause and accompanying systemic issues they present with [9]. Pain tends to be the focus for EDS/HSD individuals as one of the predominant clinical symptoms of the condition [33], as well as the associated MSK symptoms. However, it has been found that an individual with pain was more likely to have a psychiatric disorder [9], whilst another study argued depression levels to be as equally common as pain amongst this population [33]. It is clearly not as simple as diagnosing and treating symptoms of EDS/HSD in isolation, but would rather benefit from a holistic approach given that one symptom has the potential to trigger or aggravate another [33].
The review further found, specifically within the five qualitative studies, that individuals with EDS/HSD face difficulties in achieving this diagnosis, frequently describing negative healthcare experiences. One qualitative study in particular provided valuable insight into the diagnostic odyssey of EDS specifically [20]. As a result of these cases being clinically complex and multisystemic, individuals endure overwhelming struggles within the healthcare system in an attempt to find a medically valid explanation for their symptoms. Most often, individuals are misdiagnosed and mistreated, this itself could exacerbate the already debilitating symptoms [24]. An early diagnosis is vital for the individual, to feel psychologically validated, to ensure access to appropriate treatment and to improve health and wellbeing [27].
Implications for practice
Based on the findings of the scoping review, EDS/HSD is evidently clinically complex and unexpectedly common, yet often goes undetected in daily practices [27, 46]. There is a clear need for a multidisciplinary collaboration to improve awareness, the diagnostic pathways and referral processes for this condition and its associated symptoms which could lead to an earlier diagnosis and better co-ordination of care.
There appears to be less focus within clinical practice for individuals with EDS/HSD that present with non-MSK and dermatological symptoms, such as gynaecological issues [37, 38], gastrointestinal manifestations [32, 35], excessive daytime sleepiness [34], and migraines [39]. This is largely attributed to a lack of training and education amongst HCPs and the clinical complexity of individual cases [20]. Development of a rigorous clinical assessment for EDS/HSD, recognising the multifactorial manifestations, would aid clinicians in making an earlier diagnosis and therefore enable better management of the condition, including referrals to appropriate HCPs as necessary. Such an assessment, for example, would better recognise that individuals with EDS/HSD presenting with both comorbid pain and gastrointestinal symptoms are at a higher risk of suffering from a mental health disorder [9, 22], offering the opportunity for earlier intervention.
Developing an effective assessment and treatment pathway for this condition will inevitably be complex given the diverse range of symptoms and conditions presented in this review. Some studies referenced specialist hypermobility clinics [31, 37, 38] and expert practitioners in EDS [18], though there are only a small number of specialist clinics in the UK [37], not everyone with this condition will have access. Improving the training and education for HCPs could improve the current long and often unnecessary diagnostic pathways these individuals are subjected to. Within this training, ensuring an empathetic patient–provider relationship is key as well as developing an ethical attitude and sensitivity in listening to strengthen the therapeutic relationship and develop a deeper understanding of this misunderstood condition [20, 21, 23].
Limitations
The review is limited to the adult population as specified by the eligibility criteria. However, it was clear across the included studies that some of these symptoms began before the age of 18 years. The majority of individuals in one study reported hypermobility, joint pain, dislocations and dermatological symptoms to have begun in childhood whilst the onset of depression, anxiety and fatigue mainly occurred after the age of 18 years [19]. The latter could however be attributed to a lack of awareness amongst HCPs of these symptoms being linked to HSD/EDS, especially in a younger population.
Conclusions
This scoping review covering the last decade is the first review of its kind to provide a comprehensive summary all the reported symptoms and impact of EDS and HSD in an adult population. Gastroenterology, mood disorders and anxiety disorders were the most frequently reported physical and psychological manifestations whilst the social impact causes a disruption within their social networks and professional life. The current assessment and management of individuals with EDS/HSD is fragmented, with HCPs lacking sufficient knowledge of the condition. The findings of the review should be used to inform future work that promotes a multidisciplinary approach in clinical practice, improves the awareness and education of HCPs across relevant specialities, and encourages continuity of care.
Data Availability
The data that support the findings of this review are available from the corresponding author upon reasonable request.
Abbreviations
- ADHD:
-
Attention deficit hyperactivity disorder
- AN:
-
Anorexia nervosa
- ANS:
-
Autonomic nervous system
- BJHS:
-
Benign joint hypermobility syndrome
- CWP:
-
Chronic widespread pain
- EDS:
-
Ehlers-Danlos syndrome
- ESS:
-
Epworth Sleepiness Scale
- GIQLI:
-
Gastrointestinal Quality of Life Index
- HADS:
-
Hospital anxiety and depression scale
- HCPs:
-
Healthcare professionals
- hEDS:
-
Hypermobile Ehlers-Danlos syndrome
- HSD:
-
Hypermobility spectrum disorders
- JHS:
-
Joint hypermobility syndrome
- MIDAS:
-
Migraine disability assessment
- MSK:
-
Musculoskeletal
- OSA:
-
Obstructive sleep apnoea
- PCC:
-
Population, concept, context
- PoTS:
-
Postural tachycardia syndrome
- P-QOL:
-
Prolapse quality of life
- PTSD:
-
Post-traumatic stress disorder
- QoL:
-
Quality of life
- SD:
-
Standard deviation
- TSK:
-
Tampa Kinesiophobia Scale
- UK:
-
United Kingdom
- USA:
-
United States of America
References
Aubry-Rozier B, Schwitzguebel A, Valerio F, Tanniger J, Paquier C, Berna C, Hugle T, Benaim C (2021) Are patients with hypermobile Ehlers-Danlos syndrome or hypermobility spectrum disorder so different? Rheumatol Int 41:1785–1794. https://doi.org/10.1007/s00296-021-04968-3
Hypermobility Syndromes Association (2022) Hypermobility syndromes association home. https://www.hypermobility.org. Accessed 12 March 2022
Yew KS, Kamps-Schmitt KA, Borge R (2021) Hypermobile Ehlers-Danlos syndrome and hypermobility spectrum disorders. Am Fam Physician 103:481–492
Demmler JC, Atkinson MD, Reinhold EJ, Choy E, Lyons RA, Brophy ST (2019) Diagnosed prevalence of Ehlers-Danlos syndrome and hypermobility spectrum disorder in Wales, UK: a national electronic cohort study and case–control comparison. BMJ Open 9:1–9. https://doi.org/10.1136/bmjopen-2019-031365
Kumar B, Lenert P (2017) Joint hypermobility syndrome: recognizing a commonly overlooked cause of chronic pain. Am J Med 130:640–647. https://doi.org/10.1016/j.amjmed.2017.02.013
Palomo-Toucedo IM, Leon-Larios F, Reina-Bueno M, del Carmen V-BM, Munuera-Martinez P, Dominguez-Maldonago G (2020) Psychosocial influence of Ehlers-Danlos syndrome in daily life of patients: a qualitative study. Int J Environ Res Public Health 17:1–14. https://doi.org/10.3390/ijerph17176425
Hope L, Juul-Kristensen B, Lovaas H, Lovvik C, Maeland S (2019) Subjective health complaints and illness perception amongst adults with joint hypermobility syndrome/Ehlers–Danlos syndrome-hypermobility type—a cross-sectional study. Disabil Rehabil 41:333–340. https://doi.org/10.1080/09638288.2017.1390695
Palmer S, Bridgeman K, Di Pierro I, Jones R, Phillips C, Wilson M (2019) The views of people with joint hypermobility syndrome on its impact, management and the use of patient-reported outcome measures. A thematic analysis of open-ended questionnaire responses. Musculoskelet Care 17:183–193. https://doi.org/10.1002/msc.1387
Hershenfeld SA, Wasim S, McNiven V, Parikh M, Majewski P, Faghfoury H, So J (2016) Psychiatric disorders in Ehlers-Danlos syndrome are frequent, diverse and strongly associated with pain. Rheumatol Int 36:341–348. https://doi.org/10.1007/s00296-015-3375-1
Castori M (2013) Joint hypermobility syndrome (a.k.a. Ehlers-Danlos Syndrome, hypermobility type): an updated critique. G Ital Dermatol Venereol 148:13–36
Engel GL (1981) The clinical application of the biopsychosocial model. J Med Philos 6(2):101–124
Clark NL, Johnson M, Rangan A, Swainston K, Kottam L (2022) Exploring the biopsychosocial impact of hypermobility spectrum disorders (HSD) and Ehlers-Danlos syndrome (EDS) in an adult population: a protocol for a scoping review. Research Square, Preprint Version 1. 21 Dec 2022. https://doi.org/10.21203/rs.3.rs-2179415/v1
Arksey H, O’Malley L (2005) Scoping studies: towards a methodological framework. Int J Soc Res Methodol 8:19–32. https://doi.org/10.1080/1364557032000119616
Gasparyan AY, Ayvazyan L, Blackmore H, Kitas GD (2011) Writing a narrative biomedical review: considerations for authors, peer reviewers, and editors. Rheumatol Int 31:1409–1417. https://doi.org/10.1007/s00296-011-1999-3
Peters MDJ, Godfrey CM, McInerney P, Soares CB, Khalil H, Parker D (2015) The Joanna Briggs Institute reviewers’ manual 2015: methodology for JBI scoping reviews. The Joanna Briggs Institute, Adelaide, pp 1–25
Tricco AC et al (2018) PRISMA extension for scoping reviews (PRISMA-ScR): checklist and explanation. Ann Int Med 169:467–473. https://doi.org/10.7326/M18-0850
Alomari M, Hitawala A, Chadalavada P, Covut F, Al Momani L, Khazaaleh S, Gosai F, Al Ashi S, Abushahin A, Schneider A (2020) Prevalence and predictors of gastrointestinal dysmotility in patients with hypermobile Ehlers-Danlos syndrome: a tertiary care center experience. Cureus 12:1–12. https://doi.org/10.7759/cureus.7881
Baeza-Velasco C, Bourdon C, Montalescot L, de Cazotte C, Pailhez G, Bulbena A, Hamonet C (2018) Low- and high-anxious hypermobile Ehlers-Danlos syndrome patients: comparison of psychosocial and health variables. Rheumatol Int 38:871–878. https://doi.org/10.1007/s00296-018-4003-7
Murray B, Yashar BM, Uhlmann WR, Clauw DJ, Petty EM (2013) Ehlers-Danlos syndrome, hypermobility type: a characterization of the patients’ lived experience. Am J Med Genet A 161A:2981–2988. https://doi.org/10.1002/ajmg.a.36293
Halverson CME, Clayton EW, Sierra AG, Francomano C (2021) Patients with Ehlers-Danlos syndrome on the diagnostic odyssey: rethinking complexity and difficulty as a hero’s journey. Am J Med Genet C 187C:416–424. https://doi.org/10.1002/ajmg.c.31935
Maya TR, Fettig V, Mehta L, Gelb BD, Kontorovich AR (2021) Dysautonomia in hypermobile Ehlers-Danlos syndrome and hypermobility spectrum disorders is associated with exercise intolerance and cardiac atrophy. Am J Med Genet A 185:3754–3761. https://doi.org/10.1002/ajmg.a.62446
Wasim S, Suddaby JS, Parikh M, Leylachian S, Ho B, Guerin A, So J (2019) Pain and gastrointestinal dysfunction are significant associations with psychiatric disorders in patients with Ehlers-Danlos syndrome and hypermobility spectrum disorders: a retrospective study. Rheumatol Int 39:1241–1248. https://doi.org/10.1007/s00296-019-04293-w
Saetre E, Eik H (2019) Flexible bodies—restricted lives: a qualitative exploratory study of embodiment in living with joint hypermobility syndrome/Ehlers-Danlos syndrome, hypermobility type. Musculoskelet Care 17:241–248. https://doi.org/10.1002/msc.1407
Terry RH, Palmer ST, Rimes KA, Clark CJ, Simmonds JV, Horwood JP (2015) Living with joint hypermobility syndrome: patient experiences of diagnosis, referral and self-care. Fam Pract 32:354–358. https://doi.org/10.1093/fampra/cmv026
Mullick G, Bhakuni DS, Shanmuganandan K, Garg MK, Vasdev V, Kartik S, Jain R (2013) Clinical profile of benign joint hypermobility syndrome from a tertiary care military hospital in India. Int J Rheum Dis 16:590–594. https://doi.org/10.1111/1756-185x.12024
Martinez KL, Mauss C, Andrews J, Saboda K, Huynh JM, Sanoja AJ, Jesudas R, Byers PH, Laukaitis CM (2021) Subtle differences in autonomic symptoms in people diagnosed with hypermobile Ehlers-Danlos syndrome and hypermobility spectrum disorders. Am J Med Genet A 85A:2012–2025. https://doi.org/10.1002/ajmg.a.62197
Folci M, Capsoni M (2016) Arthralgias, fatigue, paresthesias and visceral pain: can joint hypermobility solve the puzzle? A case report. BMC Musculoskelet Disord 17:1–6. https://doi.org/10.1186/s12891-016-0905-2
Baeza-Velasco C, Van den Bossche T, Grossin D, Hamonet C (2016) Difficulty eating and significant weight loss in joint hypermobility syndrome/Ehlers–Danlos syndrome, hypermobility type. Eat Weight Disord 21:175–183. https://doi.org/10.1007/s40519-015-0232-x
Lee M, Strand M (2017) Ehlers-Danlos syndrome in a young woman with anorexia nervosa and complex somatic symptoms. Int J Eat Disord 51:281–284. https://doi.org/10.1002/eat.22815
Berglund B, Pettersson C, Pigg M, Kristiansson P (2015) Self-reported quality of life, anxiety and depression in individuals with Ehlers-Danlos syndrome (EDS): a questionnaire study. BMC Musculoskelet Disord 16:1–5. https://doi.org/10.1186/s12891-015-0549-7
Clark CJ, Khattab AD, Carr ECJ (2014) Chronic widespread pain and neurophysiological symptoms in joint hypermobility syndrome (JHS). Int J Ther Rehabil 21:60–67. https://doi.org/10.12968/ijtr.2014.21.2.60
Inayet N, Hayat JO, Kaul A, Tome M, Child A, Poullis A (2018) Gastrointestinal symptoms in Marfan syndrome and hypermobile Ehlers-Danlos syndrome. Gastroenterol Res Pract 2018:1–8. https://doi.org/10.1155/2018/4854701
Albayrak I, Yilmaz H, Akkurt HE, Salli A, Karaca G (2015) Is pain the only symptom in patients with benign joint hypermobility syndrome? Clin Rheumatol 34:1613–1619. https://doi.org/10.1007/s10067-014-2610-6
Gaisl T, Giunta C, Bratton DJ, Sutherand K, Sclatzer C, Sievi N, Franzen D, Cistulli PA, Rohrbach M, Kohler M (2017) Obstructive sleep apnoea and quality of life in Ehlers-Danlos syndrome: a parallel cohort study. Thorax 72:729–735. https://doi.org/10.1136/thoraxjnl-2016-209560
Zeitoun JD, Lefevre JH, de Parades V, Sejourne C, Sobhani I, Coffin B, Hamonet C (2013) Functional digestive symptoms and quality of life in patients with Ehlers-Danlos syndromes: results of a national cohort study on 134 patients. PLoS ONE 8:1–8. https://doi.org/10.1371/journal.pone.0080321
Fikree A, Aziz Q, Sifrim D (2017) Mechanisms underlying reflux symptoms and dysphagia in patients with joint hypermobility syndrome, with and without postural tachycardia syndrome. Neurogastroenterol Motil 29:1–9. https://doi.org/10.1111/nmo.13029
Mastoroudes H, Giarenis I, Cardozo L, Srikrishna S, Vella M, Robinson D, Kazkaz H, Grahame R (2012) Prolapse and sexual function in women with benign joint hypermobility syndrome. BJOG Int J Obstet Gynaecol 120:187–192. https://doi.org/10.1111/1471-0528.12082
Mastoroudes H, Giarenis I, Cardozo L, Srikrishna S, Vella M, Robinson D, Kazkaz H, Grahame R (2013) Lower urinary tract symptoms in women with benign joint hypermobility syndrome: a case-control study. Int Urogynecol J 24:1553–1558. https://doi.org/10.1007/s00192-013-2065-3
Puledda F, Vigano A, Celletti C, Petolicchio B, Toscano M, Vicenzini E, Castori M, Laudani G, Valente D, Camerota F, Di Piero V (2015) A study of migraine characteristics in joint hypermobility syndrome a.k.a. Ehlers-Danlos syndrome, hypermobility type. Neurol Sci 36:1417–1424. https://doi.org/10.1007/s10072-015-2173-6
Bulbena-Cabre A, Rojo C, Pailhez G, Maso EB, Martin-Lopez LM, Bulbena A (2018) Joint hypermobility is also associated with anxiety disorders in the elderly population. Int J Geriatr Psychiatry 33:113–119. https://doi.org/10.1002/gps.4733
Baeza-Velasco C, Hamonet C, Montalescot L, Courtet P (2022) Suicidal behaviors in women with the hypermobile Ehlers-Danlos syndrome. Arch Suicide Res 26:1314–1326. https://doi.org/10.1080/13811118.2021.1885538
Liaghat B, Skou ST, Sondergaard J, Boyle E, Sograard K, Juul-Kristensesn B (2022) Clinical characteristics of 100 patients with hypermobility spectrum disorders and shoulder complaints with or without mechanical symptoms: a cross-sectional study. Archiv Phys Med Rehabil 103:1749–1757. https://doi.org/10.1016/j.apmr.2021.12.021
Berglund B, Bjorck E (2012) Women with Ehlers-Danlos syndrome experience low oral health-related quality of life. J Orofac Pain 26:307–314
De Baets S, Calders P, Verhoost L, Coussens M, Dewandele I, Malfait F, Vanderstraeten G, Van Hove G, Van de Velde D (2021) Patient perspectives on employment participation in the “hypermobile Ehlers-Danlos syndrome.” Disabil Rehabil 43:668–677. https://doi.org/10.1080/09638288.2019.1636316
Nee J, Kilaru S, Kelley J, Oza SS, Hirsch W, Ballou S, Lembo A, Wolf J (2019) Prevalence of functional GI diseases and pelvic floor symptoms in Marfan syndrome and Ehlers Danlos syndrome: a national cohort study. J Clin Gastroenterol 53:653–659. https://doi.org/10.1097/MCG.0000000000001173
Bisaralli R, Dutta PK, Marak AF, Naroem S (2017) Benign joint hypermobility syndrome: a case series. J Med Soc 31:59–62. https://doi.org/10.4103/0972-4958.198469
Acknowledgements
We would like to thank the Academic Librarian at South Tees Hospitals NHS Foundation Trust for their assistance in developing the search strategy.
Funding
Not applicable.
Author information
Authors and Affiliations
Contributions
Conceptualisation and design: NC, MJ, LK, KS; Acquisition, analysis and interpretation of the data: NC, MJ, LK, KS; Drafting the work or revising it critically for important intellectual content: NC, MJ, AR, LK, KS; Final approval of the version to be published: NC, MJ, AR, LK, KS; Agreement to be accountable for all the aspects of the work: NC, MJ, AR, LK, KS.
Corresponding author
Ethics declarations
Conflict of interest
The author declare that they have no conflict of interest.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if changes were made. The images or other third party material in this article are included in the article's Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article's Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
Clark, N.L., Johnson, M., Rangan, A. et al. The biopsychosocial impact of hypermobility spectrum disorders in adults: a scoping review. Rheumatol Int 43, 985–1014 (2023). https://doi.org/10.1007/s00296-023-05298-2
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00296-023-05298-2