Abstract
Purpose
Diabetic cardiomyopathy (DCM), a common complication of diabetes mellitus and is characterized by myocardial hypertrophy and myocardial fibrosis. Pyrroloquinoline quinone (PQQ), a natural nutrient, exerts strong protection against various myocardial diseases. Pyroptosis, a type of inflammation-related programmed cell death, is vital to the development of DCM. However, the protective effects of PQQ against DCM and the associated mechanisms are not clear. This study aimed to investigate whether PQQ protected against DCM and to determine the underlying molecular mechanism.
Methods
Diabetes was induced in mice by intraperitoneal injection of streptozotocin, after which the mice were administered PQQ orally (10, 20, or 40 mg/kg body weight/day) for 12 weeks. AC16 human myocardial cells were divided into the following groups and treated accordingly: control (5.5 mmol/L glucose), high glucose (35 mmol/L glucose), and HG + PQQ groups (1 and 10 nmol/L PQQ). Cells were treated for 24 h.
Results
PQQ reduced myocardial hypertrophy and the area of myocardial fibrosis, which was accompanied by an increase in antioxidant function and a decrease in inflammatory cytokine levels. Moreover, myocardial hypertrophy—(ANP and BNP), myocardial fibrosis—(collagen I and TGF-β1), and pyroptosis-related protein levels decreased in the PQQ treatment groups. Furthermore, PQQ abolished mitochondrial dysfunction and the activation of NF-κB/IκB, and decreased NLRP3 inflammation-mediated pyroptosis in AC16 cells under high-glucose conditions.
Conclusion
PQQ improved DCM in diabetic mice by inhibiting NF-κB/NLRP3 inflammasome-mediated cell pyroptosis. Long-term dietary supplementation with PQQ may be greatly beneficial for the treatment of DCM.
Graphical abstract
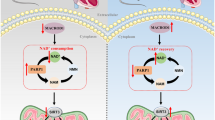
Diagram of the underlying mechanism of the effects of PQQ on DCM. PQQ inhibits ROS generation and NF-κB activation, which stimulates activation of the NLRP3 inflammasome and regulates the expression of caspase-1, IL-1β, and IL-18. The up-regulated inflammatory cytokines trigger myocardial hypertrophy and cardiac fibrosis and promote the pathological process of DCM.

Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Diabetic cardiomyopathy (DCM) is a major cardiovascular complication of diabetes mellitus and is the leading cause of mortality in diabetic patients [1]. Structural and functional abnormalities are the main features of DCM, which is characterized by myocardial hypertrophy, cardiac fibrosis, and cardiac dysfunction [2]. The pathogenesis of DCM includes mitochondrial dysfunction, inflammation, extracellular matrix deposition, and cell death [3]. The inflammatory response has been shown to play an important role in the pathophysiology of DCM [4, 5]. Bioactive substances in food have important protective effects against cardiac diseases via anti-inflammatory and anti-oxidative effects. The use of appropriate bioactive substances combined with clinical treatment may be an effective method for DCM management.
Pyrroloquinoline quinone (PQQ), a natural bioactive substance, is a water-soluble redox coenzyme that is considered to be a new B vitamin [6]. PQQ is distributed widely in multiple dietary sources and exhibits potential health benefits, such as anti-inflammatory [7], anti-oxidative [8], anti-diabetic [9], and cardioprotective effects [10]. Several studies have demonstrated that PQQ deficiency leads to immune dysfunction, growth impairment, and abnormal reproductive performance [11]. Mammals do not synthesize PQQ and, therefore, dietary supplementation with PQQ is essential for maintaining human health. Some studies have shown that PQQ protects the heart against oxidative stress injury [12], myocardial ischemia/reperfusion injury [13], hypertrophy [14], and heart failure [15]. However, the protective effect of PQQ against DCM and the associated mechanism are not clear.
Pyroptosis, which is characterized by the activation of the Nod-like receptor family pyrin domain-containing 3 (NLRP3) inflammasome, is a type of programmed cell death associated with inflammation [10]. Recent studies have demonstrated that pyroptosis is associated with DCM [16]. In the diabetic state, the NLRP3 inflammasome is assembled, leading to the cleavage of caspase-1. Cleaved caspase-1 is able to convert pro-interleukin-1β (pro-IL-1β) and pro-interleukin-18 (pro-IL-18) into mature IL-1β and IL-18, respectively [17, 18]. In addition, several studies have reported that NF-κB participates in the activation of the NLRP3 inflammasome, which triggers the transcription of NLRP3, IL-1β, and IL-18 [19, 20]. Luo et al.[21] found that silencing NLRP3 attenuates pyroptosis, cardiac fibrosis, cardiac inflammation, and cardiac dysfunction. In another study, the lncRNA-Kcnq1ot1/miR-214/NLRP3/caspase-1 signaling pathway was found to be a vital mechanism for the development of DCM [18]. Thus, targeting pyroptosis signaling molecules, such as NLRP3, caspase-1, IL-1β, and IL-18, has potential for the prevention and treatment of DCM.
In this study, we demonstrated for the first time that PQQ significantly alleviated myocardial damage, including myocardial fibrosis and myocardial hypertrophy, in diabetic mice. Further, PQQ was found to inhibit the activation of the NF-κB/pyroptosis signaling pathway in diabetic mice and high glucose-treated AC16 cells.
Materials and methods
Animals and establishment of the DCM model
PQQ, with a purity > 98%, was provided by Zhucheng HaoTian Pharm Co., Ltd. (Shandong, China). Male C57BL/6 mice (8 weeks old) were obtained from the Animal Experiment Center of Zhejiang Academy of Medicine Sciences (Hangzhou, China). All mice were housed at 22 ± 1 ℃ and 55 ± 5% humidity, with ad libitum access to food and water. The mice were randomly divided into the following five groups (n = 10 for each group): controls (Ctl), diabetic cardiomyopathy (DCM), diabetic mice treated with a low dose of PQQ (DCM + PQQL), diabetic mice treated with a medium dose of PQQ (DCM + PQQM), and diabetic mice treated with a high dose of PQQ (DCM + PQQH). Type 1 diabetes was induced by intraperitoneal injection (i.p.) of 50 mg/kg/day streptozotocin (STZ; Sigma, St. Louis, MO, USA) for 5 days. Five days after STZ injection, fasting blood glucose concentrations were measured using a contour glucose meter (Roche, Basel, Switzerland), and mice with glucose concentrations ≥ 16.7 mmol/L were used in the experiments. Subsequently, some diabetic mice were treated with PQQ orally (10, 20, or 40 mg/kg body weight/day). All mice were fed for 12 weeks and were then anesthetized with 3% pentobarbital sodium.
Cell culture and treatment
AC16 human myocardial cells were purchased from Otwo Biotech (HTX2571, Shenzhen, China) and were cultured in Dulbecco’s modified Eagle’s medium (DMEM; Gibco, Grand Island, NY, USA) with 10% fetal bovine serum (Biological Industries, Haemek, Israel) and 1% penicillin–streptomycin (TBD, Tianjin China), in an incubator at 37 °C and 5% CO2. The cells were then divided into the following groups and treated accordingly: control (5.5 mmol/L glucose), high glucose (HG, 35 mmol/L glucose), and HG + PQQ groups (1 and 10 nmol/L PQQ). Cells were treated for 24 h.
Cell viability assay
An MTT assay kit (Keygen Biotech, Jiangsu, China) was used to determine the protective effect of different concentrations of PQQ against HG-induced cell damage, according to the manufacturer’s instructions. After AC16 cells were passaged stably, they were seeded into 96-well plates at a density 1 × 104 cells/well. PQQ was added to the 96-well plate at increasing concentrations (1, 10, 100, 1000, 5000, 10,000, and 100,000 nmol/L). After 24 h, the cells were incubated with 50 μL of 1 × MTT for 4 h and then, 150 μL of DMSO was added to each well. Absorbance was measured at 490 nm.
Hematoxylin and eosin and Masson’s trichrome staining
Murine heart tissues were fixed with 4% paraformaldehyde and embedded in paraffin. They were then cut into 5 μm sections and stained using hematoxylin and eosin (H&E) and Masson’s trichrome protocols. The sections of the left ventricle were observed under an optical microscope (Olympus Corporation, Tokyo, Japan) at 400×, then the morphology of cardiomyocytes determined and collagen deposition in the interstitial and perivascular regions measured. The cardiomyocyte area and fibrotic area were determined using Image-Pro Plus imaging software (Media Cybernetics, Rockville, MD, USA).
RNA isolation and real-time RT-PCR
Total RNA was extracted from the left ventricle of mouse hearts using TRIzol (Tiangen Biotech, Beijing, China). A NanoDrop spectrophotometer (Wilmington, DE, USA) was used to determine RNA concentration. cDNA was synthesized using a reverse transcription kit (Life Technologies, Grand Island, NY, USA), and the cDNA was amplified and quantified using an ABI 7500 Fast real-time PCR system (Applied Biosystems, Foster City, CA, USA) with SYBR Green (Life Technologies, Grand Island, NY, USA). The reaction conditions were 95 ℃ for 5 min, followed by 40 cycles of 95 ℃ for 15 s, 60 ℃ for 30 s, and 72 ℃ for 45 s. mRNA expression levels were normalized to GAPDH levels. Relative mRNA expression levels were determined using the 2−△△Ct method. The primers sequences are listed in Table 1.
Western blotting analysis
Total protein was extracted using RIPA lysis buffer containing 1% protease inhibitor, and the concentration of the extracted protein was measured using a BCA kit. Equal amounts of protein were separated by 8–15% SDS-PAGE and transferred to nitrocellulose (NC) membranes. The NC membranes were blocked with 5% bovine serum albumin for 2 h at room temperature and then incubated with primary antibodies overnight at 4 ℃. The primary antibodies against different target proteins were listed as follows: NLRP3 (BA3677, Boster Biological Technology, Wuhan, China), caspase-1 (24232s, Cell Signaling Technology, Danvers, MA, U.S.A.), cleaved caspase-1 (4199s, Cell Signaling Technology, Danvers, MA, U.S.A.), IL-1β (12242s, Cell Signaling Technology, Danvers, MA, U.S.A.), IL-18 (54943s, Cell Signaling Technology, Danvers, MA, U.S.A.), NF-κB p65 (8242s, Cell Signaling Technology, Danvers, MA, U.S.A.), phospho-NF-κB p65 (3033s, Cell Signaling Technology, Danvers, MA, U.S.A.), IκBα (9242s, Cell Signaling Technology, Danvers, MA, U.S.A.), phospho-IκBα 9246s, Cell Signaling Technology, Danvers, MA, U.S.A.), collagen III (ab7778, Abcam, Cambridge, MA, U.S.A.), collagen I (14695-1-AP, Proteintech, Wuhan, China), TGF-β1 (ab9758, Abcam, Cambridge, MA, U.S.A.), β-actin (BK7018, Bioker, Hangzhou, China), and GAPDH (BK7021, Bioker, Hangzhou, China). NC membranes were then incubated with fluorescently labeled secondary antibodies (LI-COR Biosciences, Lincoln, NE, USA) for 1 h at room temperature in the dark. GAPDH and β-actin were used for normalization. The results were captured and analyzed using an Odyssey Imaging System (LI-COR Biosciences).
ELISA analysis
ELISAs were performed to determine the levels of IL-1β, IL-6, and TNF-α in heart tissue using commercially available kits (QuantiCyto, Shanghai, China) according to the manufacturer’s instructions. Total protein was extracted from heart tissues and the concentration of protein was determined using a BCA kit.
Assessment of oxidative stress
Heart tissue (0.3–0.4 g) was washed with cold saline to remove blood. A 10% tissue homogenate was prepared by completely grinding the heart tissue in nine volumes (w/v) of ice-cold saline using a grinding rod. The homogenate was then centrifuged at 3000×g for 15 min at 4 ℃ to separate the cell debris. All procedures were performed in accordance with the corresponding kit manufacturer’s protocol. Lactate dehydrogenase (LDH), creatine kinase MB (CK-MB), superoxide dismutase (SOD), glutathione peroxidase (GSH-px), and catalase (CAT) activity were measured using commercially available assay kits (Jiancheng, Nanjing, China). Malondialdehyde (MDA) concentrations were detected using a commercially available MDA assay kit (Jiancheng, Nanjing, China).
Detection of reactive oxygen species
AC16 cells were seeded into 6-well plates and treated with 35 mmol/L glucose and PQQ for 24 h. To measure intracellular reactive oxygen species (ROS) concentrations, the cells were incubated with 10 μmol/L 2ʹ,7ʹ-dichlorofluorescein diacetate (DCFH-DA; Abcam, Cambridge, MA, USA) for 45 min at 37 ℃. The cells were then washed three times with serum-free medium, and DCFH-DA fluorescence was observed using a fluorescence microscope (Olympus Corporation; magnification 400×). Fluorescence intensities were quantified using Image-Pro Plus (version 5.0; Media Cybernetics, Inc., Rockville, MD, USA).
Mitochondrial membrane potential detection
A JC-1 mitochondrial membrane potential assay kit (MedChemExpress, Shanghai, China) was used to detect changes in the mitochondrial membrane potential in AC16 cells treated with HG and PQQ. AC16 cells were cultured in six-well plates at a density of 5 × 105 cells/well, and incubated with 10 μL of JC-1 (200 μmol/L) for 20 min at 37 ℃. The images were captured using a fluorescence microscope (Olympus Corporation; magnification × 400).
Statistical analysis
Results are presented as mean ± standard deviation (SD) of at least three independent experiments. Multiple groups were analyzed using a one-way ANOVA. Differences were considered statistically significant if P < 0.05. Statistical analyses were performed using SPSS software (version 22.0; IBM, Armonk, NY, USA).
Results
Effects of PQQ on fasting blood glucose concentrations and heart weight in diabetic mice
Diabetic mice showed increased fasting blood glucose concentrations (22.19 ± 1.37 vs. 6.73 ± 0.17 mmol/L) and decreased body weight (23.16 ± 0.76 g vs. 26.88 ± 0.43 g) compared with mice in the control group. Treatment with 40 mg/kg/day PQQ significantly reduced the blood glucose concentrations of diabetic mice, but had no effect on body weight. The heart weight/body weight ratio significantly increased in the diabetic group, and this was ameliorated by treatment with 40 mg/kg/day PQQ (Table 2).
PQQ ameliorated diabetes-induced myocardial hypertrophy
The effects of PQQ on myocardial hypertrophy were determined in diabetic mice. Cardiomyocyte area was significantly increased in diabetic mice compared with control mice, and this was attenuated by PQQ treatment at 20 or 40 mg/kg/day (Fig. 1a, b). The levels of markers of myocardial hypertrophy, including atrial natriuretic peptide (ANP), brain natriuretic peptide (BNP), and myosin heavy chain beta (β-MHC), were increased in the DCM group. However, PQQ treatment ameliorated this increase in ANP, BNP, and β-MHC mRNA levels (Fig. 1c–e). Thus, PQQ had a protective effect against myocardial hypertrophy in DCM.
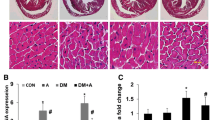
PQQ ameliorated diabetes-induced myocardial hypertrophy. a Representative H&E staining in the study groups. Chromatin and nucleic acids are stained blue and the cytoplasm and extracellular matrix are stained red; magnification, × 400; n = 5 per group. b Comparison of cardiomyocyte area in the mice from each group; n = 5. Relative mRNA expression levels of c ANP, d BNP, and e β-MHC were measured by real-time RT-PCR; n = 4 per group. Data are presented as mean ± SD, *P < 0.05, ***P < 0.001 vs. Ctl, #P < 0.05, ###P < 0.001 vs. DCM. DCM diabetic cardiomyopathy group, DCM + PQQL diabetic mice treated with 10 mg/kg BW/day PQQ, DCM + PQQM diabetic mice treated with 20 mg/kg BW/day PQQ, DCM + PQQH diabetic mice treated with 40 mg/kg BW/day PQQ
PQQ ameliorated diabetes-induced cardiac fibrosis
As shown in Fig. 2, collagen deposition in the myocardial interstitial and perivascular regions was significantly up-regulated in diabetic mice. However, treatment with 20 or 40 mg/kg/day PQQ decreased the area of fibrosis induced by diabetes. To further determine the effects of PQQ on cardiac fibrosis, we examined the levels of fibrosis-related mRNAs, including collagen I (Col I), collagen III (Col III), transforming growth factor-β1 (TGF-β1), and connective tissue growth factor (CTGF). As shown in Fig. 3a–d, the mRNA levels of Col I, Col III, TGF-β1, and CTGF were all increased in STZ-treated mice, but PQQ treatment recovered the levels of these mRNAs. Furthermore, PQQ treatment significantly inhibited the protein expression levels of COL I, COL III, and TGF-β1 in diabetic mice (Fig. 3e–g). These results demonstrated that PQQ had a protective effect against cardiac fibrosis in DCM.
PQQ ameliorated diabetes-induced cardiac fibrosis. a Representative Masson’s trichrome staining of interstitial fibrosis in the study groups; magnification, × 400; n = 5 per group. b Representative Masson’s trichrome staining of perivascular fibrosis in the study groups; magnification, × 400; n = 5. Collagen is stained blue and the myocardium is stained red. c Analysis of cardiac fibrosis area; n = 5 per group. Data are presented as mean ± SD, ***P < 0.001 vs. Ctl, ###P < 0.001 vs. DCM. DCM. DCM diabetic cardiomyopathy group, DCM + PQQL diabetic mice treated with 10 mg/kg BW/day PQQ, DCM + PQQM diabetic mice treated with 20 mg/kg BW/day PQQ, DCM + PQQH diabetic mice treated with 40 mg/kg BW/day PQQ
PQQ ameliorated cardiac fibrosis-related mRNA and protein levels. The relative mRNA expression levels of a Col I (n = 5), b Col III (n = 5), c TGF-β1 (n = 4), and d CTGF (n = 5) were measured by real-time RT-PCR. Protein expression levels of e COL I, f COL III, and g TGF-β1 were determined by western blotting analysis in the study groups, n = 4 per group. Data are presented as mean ± SD, *P < 0.05, **P < 0.01 vs. Ctl, #P < 0.05, ##P < 0.01 vs. DCM. DCM. DCM diabetic cardiomyopathy group, DCM + PQQL diabetic mice treated with 10 mg/kg BW/day PQQ, DCM + PQQM diabetic mice treated with 20 mg/kg BW/day PQQ, DCM + PQQH diabetic mice treated with 40 mg/kg BW/day PQQ
PQQ ameliorated diabetes-induced inflammation
To determine the protective role of PQQ against diabetes-induced inflammation, the IL-1β, IL-6, and TNF-α levels were assessed in heart tissue using ELISAs. The induction of diabetes increased the levels of IL-1β, IL-6, and TNF-α in the DCM model, and these effects were inhibited by PQQ (Fig. 4). The release of proinflammatory factors is associated with NLRP3 inflammasome activation. These results demonstrated that PQQ had anti-inflammatory actions in DCM.
PQQ ameliorated diabetes-induced inflammation. Levels of the inflammatory cytokines a IL-1β, b IL-6, and c TNF-α were measured by ELISA; n = 4 per group. Data are presented as mean ± SD, *P < 0.05, **P < 0.01 vs. Ctl, #P < 0.05, ##P < 0.01, ###P < 0.001 vs. DCM. DCM. DCM diabetic cardiomyopathy group, DCM + PQQL diabetic mice treated with 10 mg/kg BW/day PQQ, DCM + PQQM diabetic mice treated with 20 mg/kg BW/day PQQ, DCM + PQQH diabetic mice treated with 40 mg/kg BW/day PQQ
PQQ protected the heart from diabetes-induced oxidative stress
LDH and CK-MB are well-known indicators of myocardial damage. The LDH and CK-MB activities were higher in the diabetic group than the control group, but treatment with PQQ significantly ameliorated this increased activity (Fig. 5a, b). To determine whether PQQ ameliorated diabetes-induced oxidative stress, we measured the activities of MDA, SOD, GSH-px, and CAT in heart tissue. The SOD, GSH-px, and CAT activities were dramatically decreased and the MDA content was increased in the DCM group. However, these enzymatic activities were restored by PQQ treatment (Fig. 5c–f). These results showed that PQQ attenuated oxidative stress in DCM.
PQQ protected the heart from diabetes-induced oxidative stress. The activity or quantity of the myocardial damage-related indicators, a LDH and b CK-MB, and the oxidative stress-related indicators, c MDA, d SOD, e GSH-px, and f CAT were measured using commercial kits; n = 4 per group. Data are presented as mean ± SD, *P < 0.05, **P < 0.01, ***P < 0.001 vs. Ctl, #P < 0.05, ##P < 0.01, ###P < 0.001 vs. DCM. DCM. DCM diabetic cardiomyopathy group, DCM + PQQL diabetic mice treated with 10 mg/kg BW/day PQQ, DCM + PQQM diabetic mice treated with 20 mg/kg BW/day PQQ, DCM + PQQH diabetic mice treated with 40 mg/kg BW/day PQQ
Effects of PQQ on the pyroptosis signaling pathway in DCM
To determine the effect of PQQ on the pyroptosis signaling pathway in this DCM model, we measured changes in NLRP3, caspase-1, IL-1β, and IL-18 levels. The mRNA and protein expression levels of NLRP3 and caspase-1 were up-regulated in diabetic mice, but these levels were restored by PQQ treatment (Fig. 6a–d). Moreover, the protein levels of cleaved caspase-1, IL-1β, and IL-18 were markedly increased in the DCM model, and these changes were reversed by PQQ treatment (Fig. 6e–g).
PQQ ameliorated the diabetes-induced pyroptosis of cardiomyocytes. The relative mRNA expression levels of a NLRP3, and b caspase-1 were measured by real-time RT-PCR; n = 5. The protein levels of c NLRP3 (n = 4), d caspase-1 (n = 4), e activated-caspase-1 (n = 4), f IL-1β (n = 4), and g IL-18 (n = 3) were determined by western blotting analysis. Data are presented as mean ± SD, *P < 0.05, **P < 0.001 vs. Ctl, #P < 0.05, ##P < 0.01 vs. DCM. DCM. DCM diabetic cardiomyopathy group, DCM + PQQL diabetic mice treated with 10 mg/kg BW/day PQQ, DCM + PQQM diabetic mice treated with 20 mg/kg BW/day PQQ, DCM + PQQH diabetic mice treated with 40 mg/kg BW/day PQQ
The effects of PQQ on cell viability in response to HG
To determine the effect of different concentrations of PQQ on AC16 cells, we used an MTT assay kit to determine cell viability. AC16 cells were treated with increasing concentrations of PQQ (1, 10, 100, 1000, 5000, 10,000, and 100,000 nmol/L) for 24 h. At 100,000 nmol/L, PQQ caused significant cellular damage, whereas the other tested concentrations of PQQ had no obvious effect on AC16 cells under normal conditions (Fig. 7a). Therefore, AC16 cells were treated with 1–10,000 nmol/L PQQ under HG conditions. HG markedly inhibited cell viability compared with control cells, and PQQ protected AC16 cells from HG-induced damage (Fig. 7b).
The effects of PQQ on cell viability and pyroptosis signaling in AC16 cells under HG conditions. a & b AC16 cells were treated with different concentrations of PQQ (1, 10, 100, 1,000, 5,000, 10,000, and 10,0000 nmol/L) in basic DMEM (5.5 mmol/L glucose) or HG (35 mmol/L glucose) media for 24 h. Cell viability was measured by MTT assay, n = 6. The protein levels of c NLRP3, d cleaved-caspase-1, e caspase-1, f IL-1β, and g IL-18 were analyzed by western blotting, n = 4 per group. Mean ± SD, *P < 0.05, **P < 0.01, ***P < 0.001 vs. Ctl, #P < 0.05, ##P < 0.01, ###P < 0.001 vs. HG. HG high glucose; HG + 1 nmol/L PQQ, high glucose with 1 nmol/L PQQ; HG + 10 nmol/L PQQ, high glucose with 10 nmol/L PQQ
PQQ ameliorated pyroptosis signaling in AC16 cells under HG conditions
Based on the previous results, 1 nmol/L and 10 nmol/L were considered to be the minimum effective PQQ concentrations needed to protect against HG-induced damage. Thus, these concentrations were selected for subsequent experiments. As shown in Fig. 7c–g, the NLRP3, cleaved-caspase-1, caspase-1, IL-1β, and IL-18 protein levels were markedly increased in the HG group, but were decreased after treatment with 10 nmol/L PQQ. This indicated that 10 nmol/L PQQ may have a protective effect against the pyroptosis signaling pathway in AC16 cells under HG conditions.
PQQ ameliorated NF-κB activation in AC16 cells under HG conditions
The NF-κB signaling pathway triggers the activation of the NLRP3 inflammasome. As shown in Fig. 8a, b, the phosphorylation levels of NF-κB p65 and IκB were significantly elevated after HG stimulation. However, 10 nmol/L PQQ decreased the phosphorylation levels of NF-κB p65 and IκB.
PQQ ameliorated NF-κB activation and ROS generation in AC16 cells under HG conditions. a Protein levels of phosphorylated and total NF-κB p65 were determined by western blotting analysis, n = 4. b Protein levels of phosphorylated IκB and total IκB were determined by western blotting analysis, n = 4; c Intracellular ROS levels were determined using a DCFH-DA assay kit, n = 3. d Mitochondrial membrane potential was measured in AC16 cells using a JC-1 mitochondrial membrane potential assay kit, n = 3. Mean ± SD, *P < 0.05 vs. Ctl, #P < 0.05, ##P < 0.01 vs. HG. HG high glucose; HG + 1 nmol/L PQQ, high glucose with 1 nmol/L PQQ; HG + 10 nmol/L PQQ, high glucose with 10 nmol/L PQQ
PQQ ameliorated ROS generation in AC16 cells under HG conditions
To investigate the effects of PQQ on HG-induced ROS production, we measured the intracellular ROS levels and mitochondrial membrane potential. HG strongly stimulated ROS accumulation and repressed mitochondrial membrane potential in AC16 cells. However, PQQ ameliorated these effects on ROS production and of mitochondrial membrane potential (Fig. 8c, d).
Discussion
Multiple studies have shown that myocardial hypertrophy and myocardial fibrosis are common structural abnormalities in diabetic patients, leading to cardiac stiffness and cardiac dysfunction [22]. This study, for the first time, showed that dietary supplementation with PQQ had protective effects against myocardial hypertrophy and myocardial fibrosis in diabetic mice. We showed that PQQ significantly inhibited inflammation and increased antioxidant ability. Furthermore, the cardioprotective effects of PQQ were, in part, mediated by the NF-κB/NLPR3 inflammasome signaling pathway.
PQQ is the third most common redox coenzyme besides nicotinamide nucleotides and flavin nucleotides. It is widely present in vegetables and meat [23]. In humans, free PQQ is found in the heart, brain, liver, lungs, plasma, and breast milk [24], and it is necessary for maintaining the health of mammals. Dietary supplementation with PQQ has potential effects of improving the blood lipid profile, controlling blood glucose concentrations, and preventing cardiovascular diseases [25]. Devasani et al. reported that treatment with 10 or 20 mg/kg PQQ for 5 weeks improved glucose tolerance, insulin resistance, and plasma insulin concentrations, and attenuated serum concentrations of inflammatory cytokines (IL-1β, IL-6, and TNF-α) in rats fed a 10% fructose diet for 10 weeks [26]. Moreover, serum glucose concentrations have been reported to ameliorate the increase in antioxidant activity in diabetic mice receiving 20 mg/kg body weight/day PQQ (i.p.) [27]. Akagawa et al. showed that oral supplementation with PQQ (20 mg/kg day) remarkably alleviated impaired glucose tolerance in type 2 diabetic KK-Ay mice [6]. It has also been reported that 15 mg/kg PQQ (i.p.) mitigated myocardial infarct size and improved cardiac function after myocardial ischemia/reperfusion injury in rats [25]. In addition, in our previous study, oral PQQ administration (10, 20, 40 mg/kg day) for 4 weeks, was found to 40 mg/kg PQQ could significantly improve the oxidative injury of nerve cells and increase the learning and memory ability of aging rats [28]. However, the cardioprotective role of PQQ in diabetic mice has not previously been investigated.
The markers of myocardial hypertrophy, ANP, BNP, and β-MHC, were up-regulated in the heart tissue of diabetic mice. We found that oral administration of PQQ decreased myocardial hypertrophy-related mRNA levels and myocardial cell area. Other structural changes observed in DCM are myocardial interstitial fibrosis and perivascular fibrosis, which are characterized by increased COL I and COL III levels, resulting in impaired cardiac contractile function and diastolic function [29]. We found that PQQ treatment inhibited myocardial interstitial and perivascular collagen deposition in diabetic mice. Moreover, TGF-β1 is a classic pro-fibrotic factor, and activation of the TGF-β1/Smad2/3 signaling pathway promotes collagen production. Ma et al. showed that PQQ attenuates the protein expression of TGF-β1 in skeletal muscles after sciatic nerve transection [30]. We also found that 40 mg/kg PQQ significantly inhibited the expression of TGF-β1 mRNA and protein.
Emerging evidence suggests that diabetes-induced inflammation has a crucial role in the pathogenesis of DCM [31]. The expression and activation of pro-inflammatory cytokines, such as IL-1β, IL-6, IL-8, and TNF-α are involved in myocardial fibrosis, myocardial hypertrophy, oxidative stress-related injury, and cardiac dysfunction [32]. NF-κB participates in the expression of inflammatory factors as a transcription factor. The NLRP3 inflammasome is a newly identified marker of inflammation in DCM, and NF-κB is able to trigger NLRP3 inflammasome assembly [33]. Meanwhile, HG causes the migration of immune cells into the myocardium and increases macrophage pro-inflammatory M1 polarization, which lead to a marked increase in the levels of TNF-α, IL-1β, IL-6, and IL-18 [7]. Wilson et al. found that PQQ attenuates the levels of IL-6 and TNF-α, and reduces the activation of the MAPK signaling pathway in IL-1β-stimulated human synovial sarcoma SW982 cells [34]. Here, we found that PQQ exerted anti-inflammatory effects in DCM, and that PQQ decreased the activation of NF-κB and IκB.
In diabetes, mitochondrial dysfunction results in the over-production of ROS and oxidative stress-related injury, which can directly stimulate NF-κB activation. We found that PQQ increased SOD, GSH-px, and CAT activity; decreased LDH and CK-MB activity; and decreased MDA concentrations. These results indicated that PQQ may be a suitable antioxidant to protect against DCM. Mitochondria are the center of cell metabolism and, as such, are strongly linked to impaired metabolism associated with DCM. Diabetes can cause metabolic abnormalities in body. Hyperglycemia will lead to excessive electron leakage from the electron transport chain to form superoxide ions, causing the mitochondria to produce numerous ROS. ROS aggravates oxidative stress in cells and damages the mitochondrial and cytoplasmic environment. Furthermore, mitochondrial dysfunction will produce more ROS and activate a series of pro-inflammatory pathways that will eventually develop into DCM. Wang et al. [35] reported that swollen mitochondria and reduction in mitochondria count were observed in DCM hearts. Wu’s [15] study showed that early PQQ treatment prevented morphological changes in the heart mitochondria, reduced mitochondrial biogenesis dysfunction caused by pressure overload both in vivo and in vitro and helped maintain heart mitochondrial function. In the present study, we found that 10 nmol/L PQQ can effectively inhibit ROS generation, improve the decrease of mitochondrial membrane potential and maintain mitochondrial function in HG-treated AC16 cells. These results indicate that PQQ may improve DCM by ameliorating mitochondrial damage and reducing ROS production.
Previous studies have reported effects of PQQ on AC16 cells at different concentrations and on other cell types. Wen et al. found that PQQ had no effect on AC16 cells at concentrations from 1 to 200 μmol/L [10]. In our study, although PQQ had no statistically significant effect on cell viability at concentrations from 1 to 10,000 nmol/L, it had adverse effects on AC16 cells at 100,000 nmol/L. Wang et al. showed that PQQ had positive effects on HK-2 cells at 10–10,000 nmol/L, but markedly decreased cell viability after treatment for 48 h at 100,000 nmol/L, alone or in the presence of high glucose concentrations [27]. These results agree with those of our study. We chose 1 and 10 nmol/L to confirm the effect of PQQ on AC16 cells under HG conditions. PQQ was found to decrease pyroptosis-associated protein levels at 10 nmol/L under HG conditions.
Pyroptosis is a type of programmed cell death characterized by an inflammatory response and activation of the NLRP3 inflammasome. The NLRP3 inflammasome is a protein complex, including NLRP3, caspase-1, and ASC, that assembles in response to bacteria, pathogens, and diseases [17, 36]. Assembly of this inflammasome triggers activation of caspase-1 and the maturation of IL-1β and IL-18, leading to cell swelling, cell membrane rupture, and the release of cellular contents and inflammatory cytokines [37]. In diabetes, the activation of NF-κB stimulates the transcription of NLRP3 and activation of the NLRP3 inflammasome, resulting in the cleavage of caspase-1, which increases the production of mature IL-1β and IL-18 [38]. Recent evidence indicates that silencing the NLRP3 gene and inhibiting the activation of the NLRP3 inflammasome has protective effects against DCM development [39]. Long non-coding RNAs (lncRNAs) are important regulators of pyroptosis. Yang et al. reported that silencing lncRNA-Kcnq1ot1 decreased NLRP3 and caspase-1 expression levels to attenuate myocardial damage in DCM [18]. We found that PQQ treatment ameliorated the activation of the NLRP3 inflammasome signaling pathway, which is a potential mechanism for the cardioprotective role of PQQ.
In conclusion, the results of this study showed that PQQ reduced blood glucose concentrations and ameliorated myocardial hypertrophy and myocardial fibrosis in a model of diabetes. The NF-κB/NLRP3 inflammasome signaling pathway is a key target of PQQ treatment. These findings confirm the in vivo and in vitro benefits of PQQ, a natural nutrient, in the prevention and treatment of DCM. PQQ serves as an important oxidoreductase prosthetic group for redox reaction in vivo and assists quinolase to complete specific biological functions, thereby protecting cells from oxidative stress damage. Supplementing PQQ has a protective effect on many diseases, such as diabetes, osteoporosis and so on [8]. In Japan, Takaoki Kasahara et al. proposed to define PQQ as a new type of vitamin in 2003 [11]; in the United States, FDA included PQQ as a new food ingredient and obtained GRAS certification [40]; in the European Union, the European Food Safety Authority approved PQQ as a new food ingredient [41]. We clarify the role and mechanism of PQQ as a bioactive substance in alleviating the inflammatory death of cardiomyocytes and delaying the development of DCM, providing new ideas for the treatment of DCM. This research will contribute to the application of PQQ in the development of functional foods and new drugs.
Availability of data and material
The datasets used and/or analyzed during the current study are available from the corresponding author on reasonable request.
Abbreviations
- ANP:
-
Atrial natriuretic peptide
- BNP:
-
Brain natriuretic peptide
- CAT:
-
Catalase
- CK-MB:
-
Creatine kinase MB
- Col I:
-
Collagen I
- Col III:
-
Collagen III
- CTGF:
-
Connective tissue growth factor
- Ctl:
-
Controls
- DCM:
-
Diabetic cardiomyopathy
- DCM + PQQH:
-
Diabetic mice treated with a high dose of PQQ
- DCM + PQQL:
-
Diabetic mice treated with a low dose of PQQ
- DCM + PQQM:
-
Diabetic mice treated with a medium dose of PQQ
- GSH-px:
-
Glutathione peroxidase
- HG:
-
High glucose
- IKB:
-
Inhibitor of NF-κB
- LDH:
-
Lactate dehydrogenase
- MDA:
-
Malondialdehyde
- NF-κB:
-
Nuclear factor kappa-B
- NLRP3:
-
Nod-like receptor protein 3
- PQQ:
-
Pyrroloquinoline quinone
- ROS:
-
Reactive oxygen species
- SOD:
-
Superoxide dismutase
- STZ:
-
Streptozotocin
- TGF-β1:
-
Transforming growth factor-β1
- TNF-α :
-
Tumor necrosis factor-α
- β-MHC:
-
Myosin heavy chain beta
References
Evangelista I, Nuti R, Picchioni T, Dotta F, Palazzuoli A (2019) Molecular dysfunction and phenotypic derangement in diabetic cardiomyopathy. Int J Mol Sci 20(13):3264. https://doi.org/10.3390/ijms20133264
Dillmann WH (2019) Diabetic cardiomyopathy. Circ Res 124(8):1160–1162. https://doi.org/10.1161/CIRCRESAHA.118.314665
Jia G, Hill MA, Sowers JR (2018) Diabetic cardiomyopathy: an update of mechanisms contributing to this clinical entity. Circ Res 122(4):624–638. https://doi.org/10.1161/CIRCRESAHA.117.311586
Zhang Y, Zhang YY, Li TT, Wang J, Jiang Y, Zhao Y, Jin XX, Xue GL, Yang Y, Zhang XF, Sun YY, Zhang ZR, Gao X, Du ZM, Lu YJ, Yang BF, Pan ZW (2018) Ablation of interleukin-17 alleviated cardiac interstitial fibrosis and improved cardiac function via inhibiting long non-coding RNA-AK081284 in diabetic mice. J Mol Cell Cardiol 115:64. https://doi.org/10.1016/j.yjmcc.2018.01.001
Gu X, Shi Y, Chen X, Sun Z, Luo W, Hu X, Jin G, You S, Qian Y, Wu W, Liang G, Wu G, Chen Z, Chen X (2020) Isoliquiritigenin attenuates diabetic cardiomyopathy via inhibition of hyperglycemia-induced inflammatory response and oxidative stress. Phytomedicine 78:153319. https://doi.org/10.1016/j.phymed.2020.153319
Akagawa M, Nakano M, Ikemoto K (2016) Recent progress in studies on the health benefits of pyrroloquinoline quinone. Biosci Biotechnol Biochem 80(1):13–22. https://doi.org/10.1080/09168451.2015.1062715
Liu Z, Sun C, Tao R, Xu X, Xu L, Cheng H, Wang Y, Zhang D (2016) Pyrroloquinoline quinone decelerates rheumatoid arthritis progression by inhibiting inflammatory responses and joint destruction via modulating NF-kappaB and MAPK pathways. Inflammation 39(1):248–256. https://doi.org/10.1007/s10753-015-0245-7
Geng Q, Gao H, Yang R, Guo K, Miao D (2019) Pyrroloquinoline quinone prevents estrogen deficiency-induced osteoporosis by inhibiting oxidative stress and osteocyte senescence. Int J Biol Sci 15(1):58–68. https://doi.org/10.7150/ijbs.25783
Takada M, Sumi M, Maeda A, Watanabe F, Kamiya T, Ishii T, Nakano M, Akagawa M (2012) Pyrroloquinoline quinone, a novel protein tyrosine phosphatase 1B inhibitor, activates insulin signaling in C2C12 myotubes and improves impaired glucose tolerance in diabetic KK-A(y) mice. Biochem Biophys Res Commun 428(2):315–320. https://doi.org/10.1016/j.bbrc.2012.10.055
Wen J, Shen J, Zhou Y, Zhao X, Dai Z, Jin Y (2020) Pyrroloquinoline quinone attenuates isoproterenol hydrochlorideinduced cardiac hypertrophy in AC16 cells by inhibiting the NFkappaB signaling pathway. Int J Mol Med 45(3):873–885. https://doi.org/10.3892/ijmm.2020.4463
Kasahara T, Kato T (2003) A new redox-cofactor vitamin for mammals. Nature 422(6934):832–832. https://doi.org/10.1038/422832a
Xu F, Yu H, Liu J, Cheng L (2014) Pyrroloquinoline quinone inhibits oxygen/glucose deprivation-induced apoptosis by activating the PI3K/AKT pathway in cardiomyocytes. Mol Cell Biochem 386(1–2):107–115. https://doi.org/10.1007/s11010-013-1849-6
Tao R, Karliner JS, Simonis U, Zheng J, Zhang J, Honbo N, Alano CC (2007) Pyrroloquinoline quinone preserves mitochondrial function and prevents oxidative injury in adult rat cardiac myocytes. Biochem Biophys Res Commun 363(2):257–262. https://doi.org/10.1016/j.bbrc.2007.08.041
Nehra S, Bhardwaj V, Bansal A, Chattopadhyay P, Saraswat D (2017) Nanocurcumin-pyrroloquinoline formulation prevents hypertrophy-induced pathological damage by relieving mitochondrial stress in cardiomyocytes under hypoxic conditions. Exp Mol Med 49(12):e404. https://doi.org/10.1038/emm.2017.199
Xu X, Chen C, Lu WJ, Su YL, Shi JY, Liu YC, Wang L, Xiao CX, Wu X, Lu Q (2020) Pyrroloquinoline quinone can prevent chronic heart failure by regulating mitochondrial function. Cardiovasc Diagn Ther 10(3):453–469. https://doi.org/10.21037/cdt-20-129
Zeng C, Wang R, Hongmei T (2019) Role of pyroptosis in cardiovascular diseases and its therapeutic implications. Int J Biol Sci 15(7):1345–1357. https://doi.org/10.7150/ijbs.25783
Sharma BR, Kanneganti TD (2021) NLRP3 inflammasome in cancer and metabolic diseases. Nat Immunol 22(5):550–559. https://doi.org/10.1038/s41590-021-00886-5
Yang F, Qin Y, Lv J, Wang Y, Che H, Chen X, Jiang Y, Li A, Sun X, Yue E, Ren L, Li Y, Bai Y, Wang L (2018) Silencing long non-coding RNA Kcnq1ot1 alleviates pyroptosis and fibrosis in diabetic cardiomyopathy. Cell Death Dis 9(10):1000. https://doi.org/10.1038/s41419-018-1029-4
Ran X, Yan Z, Yang Y, Hu G, Liu J, Hou S, Guo W, Kan X, Fu S (2020) Dioscin improves pyroptosis in LPS-induced mice mastitis by activating AMPK/Nrf2 and inhibiting the NF-kappaB signaling pathway. Oxid Med Cell Longev 2020:8845521. https://doi.org/10.1155/2020/8845521
Tian L, Yan J, Li K, Zhang W, Lin B, Lai W, Bian L, Liu H, Xi Z, Liu X (2021) Ozone exposure promotes pyroptosis in rat lungs via the TLR2/4-NF-kappaB-NLRP3 signaling pathway. Toxicology 450:152668. https://doi.org/10.1016/j.tox.2020.152668
Luo B, Li B, Wang W, Liu X, Xia Y, Zhang C, Zhang M, Zhang Y, An F (2014) NLRP3 gene silencing ameliorates diabetic cardiomyopathy in a type 2 diabetes rat model. PLOS ONE 9(8):e104771. https://doi.org/10.1371/journal.pone.0104771
Marwick TH, Ritchie R, Shaw JE, Kaye D (2018) Implications of underlying mechanisms for the recognition and management of diabetic cardiomyopathy. J Am Coll Cardiol 71(3):339–351. https://doi.org/10.1016/j.jacc.2017.11.019
Kumazawa T, Sato K, Seno H, Ishii A, Suzuki O (1995) Levels of pyrroloquinoline quinone in various foods. Biochem J 307(2):331–333. https://doi.org/10.1042/bj3070331
Kumazawa T, Seno H, Urakami T, Matsumoto T, Suzuki O (1992) Trace levels of pyrroloquinoline quinone in human and rat samples detected by gas chromatography/mass spectrometry. Biochim Biophys Acta 1156(1):62–66. https://doi.org/10.1016/0304-4165(92)90096-d
Kumar N, Kar A (2015) Pyrroloquinoline quinone (PQQ) has potential to ameliorate streptozotocin-induced diabetes mellitus and oxidative stress in mice: a histopathological and biochemical study. Chem Biol Interact 240:278–290. https://doi.org/10.1016/j.cbi.2015.08.027
Devasani K, Kaul R, Majumdar A (2020) Supplementation of pyrroloquinoline quinone with atorvastatin augments mitochondrial biogenesis and attenuates low grade inflammation in obese rats. Eur J Pharmacol 881:173273. https://doi.org/10.1016/j.ejphar.2020.173273
Wang Z, Li Y, Wang Y, Zhao K, Chi Y, Wang B (2019) Pyrroloquinoline quinine protects HK-2cells against high glucose-induced oxidative stress and apoptosis through Sirt3 and PI3K/Akt/FoxO3a signaling pathway. Biochem Biophys Res Commun 508(2):398–404. https://doi.org/10.1016/j.bbrc.2018.11.140
Tang L, Li L, Hu W, Hu Z, Zhang L, Zhang L, Mei S, Chen J, Liu D, Liu Z, Wang Y (2017) The effect of pyrroloquinoline quinone on the learning and memory of aging rats and its mechanism. Chin J Food Hyg 29(4):407–411. https://doi.org/10.13590/j.cjfh.2017.04.004
Frangogiannis NG (2021) Cardiac fibrosis. Cardiovasc Res 117(6):1450–1488. https://doi.org/10.1093/cvr/cvaa324
Ma W, Zhang R, Huang Z, Zhang Q, Xie X, Yang X, Zhang Q, Liu H, Ding F, Zhu J, Sun H (2019) PQQ ameliorates skeletal muscle atrophy, mitophagy and fiber type transition induced by denervation via inhibition of the inflammatory signaling pathways. Ann Transl Med 7(18):440. https://doi.org/10.21037/atm.2019.08.101
Ghosh N, Katare R (2018) Molecular mechanism of diabetic cardiomyopathy and modulation of microRNA function by synthetic oligonucleotides. Cardiovasc Diabetol 17(1):43. https://doi.org/10.1186/s12933-018-0684-1
Jia G, DeMarco VG, Sowers JR (2016) Insulin resistance and hyperinsulinaemia in diabetic cardiomyopathy. Nat Rev Endocrinol 12(3):144–153. https://doi.org/10.1038/nrendo.2015.216
Pal PB, Sonowal H, Shukla K, Srivastava SK, Ramana KV (2017) Aldose reductase mediates NLRP3 inflammasome-initiated innate immune response in hyperglycemia-induced Thp1 monocytes and male mice. Endocrinology 158(10):3661–3675. https://doi.org/10.1210/en.2017-00294
Wilson AJ, Gill EK, Abudalo RA, Edgar KS, Watson CJ, Grieve DJ (2018) Reactive oxygen species signalling in the diabetic heart: emerging prospect for therapeutic targeting. Heart 104(4):293–299. https://doi.org/10.1136/heartjnl-2017-311448
Ma S, Jing F, Zhang R, Chen J, Han D, Li X, Bo Y, Li X, Fan M, Li C, Tian Z, Wang Y, Cao F (2017) SIRT1 activation by resveratrol alleviates cardiac dysfunction via mitochondrial regulation in diabetic cardiomyopathy mice. Oxid Med Cell Longev 2017:4602715. https://doi.org/10.1155/2017/4602715
Man SM, Karki R, Kanneganti TD (2017) Molecular mechanisms and functions of pyroptosis, inflammatory caspases and inflammasomes in infectious diseases. Immunol Rev 277(1):61–75. https://doi.org/10.1111/imr.12534
Liu P, Zhang Z, Li Y (2021) Relevance of the pyroptosis-related inflammasome pathway in the pathogenesis of diabetic kidney disease. Front Immunol 12:603416. https://doi.org/10.3389/fimmu.2021.603416
Luo B, Huang F, Liu Y, Liang Y, Wei Z, Ke H, Zeng Z, Huang W, He Y (2017) NLRP3 inflammasome as a molecular marker in diabetic cardiomyopathy. Front Physiol 8:519. https://doi.org/10.3389/fphys.2017.00519
Wen H, Ting JP, O’Neill LA (2012) A role for the NLRP3 inflammasome in metabolic diseases–did Warburg miss inflammation? Nat Immunol 13(4):352–357. https://doi.org/10.1038/ni.2228
Food and Drug Administration (2017) Generally recognized as safe (GRAS) notice of pyrroloquinoline quinone disodium salt as a food ingredient. https://www.fda.gov/media/110030/download
Turck D, Bresson JL, Burlingame B, Dean T, Fairweather-Tait S, Heinonen M, Hirsch-Ernst KI, Mangelsdorf I, Mcardle HJ, Naska AJEJ (2017) Safety of pyrroloquinoline quinone disodium salt as a novel food pursuant to regulation (EC) No 258/97. EFSA J 15(11):5058. https://doi.org/10.2903/j.efsa.2017.5058
Funding
This work was supported in part by the National Natural Science Foundation of China (82003445), the Nature Science Foundation of Zhejiang Province (LQ18H260003), and Key Subjects of Nutrition of Zhejiang Province (16-zc03).
Author information
Authors and Affiliations
Contributions
XFQ, YW, and YHZ designed the project and analyzed the data. XFQ wrote the manuscript. BZZ, WLH, MHL, LJZ, and ZL performed the western blotting, real-time PCR, ELISA, and oxidative stress assays. YHC, YFL, and ZQY performed the H&E and Masson’s trichrome staining. JGC and SM developed the mice model. All authors read and approved the final manuscript.
Corresponding authors
Ethics declarations
Conflict of interest
The authors have no conflicts of interest to declare that are relevant to the content of this article.
Ethical standards
This study was approved by the ethics committee of Zhejiang Academy of Medical Sciences, and all study protocols were approved by the Animal Care and Use Committee of Zhejiang Academy of Medical Sciences (2019–026). The ethical principles established by the National Institutes of Health Guide for the Care and Use of Laboratory Animals (NIH Publications No. 8523, revised 2011) were followed.
Consent for publication
All authors have approved the manuscript and agree with its submission to European Journal of Nutrition. We confirm that this manuscript has not been published in whole or in part.
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if changes were made. The images or other third party material in this article are included in the article's Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article's Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
Qu, Xf., Zhai, Bz., Hu, Wl. et al. Pyrroloquinoline quinone ameliorates diabetic cardiomyopathy by inhibiting the pyroptosis signaling pathway in C57BL/6 mice and AC16 cells. Eur J Nutr 61, 1823–1836 (2022). https://doi.org/10.1007/s00394-021-02768-w
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00394-021-02768-w