Abstract
Purpose
To demonstrate different topographic distributions of multiple-evanescent white dot syndrome (MEWDS) and secondary MEWDS disease and to describe possible associations.
Methods
Clinical evaluation and multimodal retinal imaging in 27 subjects with MEWDS (29 discrete episodes of MEWDS). Ophthalmic assessment included best-corrected visual acuity testing and multimodal retinal imaging with OCT, blue-light autofluorescence, fluorescein and indocyanine green angiography, fundus photography, and widefield pseudocolor and autofluorescence fundus imaging.
Results
The topographic distribution of MEWDS lesions was centered on or around the optic disc (n = 17, 59%), centered on the macula (n = 7, 24%), sectoral (n = 2, 7%), or was indeterminate (n = 3, 10%). The MEWDS episodes either occurred in the absence (‘primary MEWDS’; n = 14, 48%) or presence of concurrent chorioretinal pathology (‘secondary MEWDS’; n = 15, 52%). In patients with the latter, MEWDS lesions were often centered around a coexisting chorioretinal lesion. The majority of patients in both groups experienced resolution of their symptoms and retinal changes on multimodal imaging by 3 months.
Conclusions
Distinct distributions of MEWDS lesions were identified. MEWDS may occur in tandem with other chorioretinal pathology, which may impact the topography of MEWDS lesions.

Similar content being viewed by others
Explore related subjects
Discover the latest articles, news and stories from top researchers in related subjects.Avoid common mistakes on your manuscript.
Introduction
MEWDS was first described in 1984 as a unilateral, acute-onset, evanescent condition that presents with small clusters of discrete white dots most prominent in the perifoveal region and associated with a granular appearance of the fovea [1]. It was previously thought to be a primary choriocapillaritis [2], but more recent multimodal imaging studies suggest the retinal pigment epithelium (RPE)-photoreceptor complex to be the primary site of insult [3,4,5].
Classically, MEWDS is thought to occur in younger female patients, several of whom report a viral prodrome. However, an infectious or autoimmune etiology has yet to be elucidated and no associated systemic diseases have consistently been found [1, 6]. More recent reports have detailed a subset of cases with ‘MEWDS-like’ reactions, occurring contemporaneously with other ocular pathology which may result in exposure of retinal, RPE, and the Bruch membrane antigens to the immune system [7,8,9,10,11,12,13]. Various other descriptive terminology has been used for such ‘MEWDS-like’ reactions, including secondary MEWDS, epiMEWDS, and acute retinopathy [7, 8, 14]. While most affected patients experience complete visual recovery [6], others have protracted symptoms [15], which may be associated with the development of peripapillary atrophy, multifocal pigmentary changes, and/or acute zonal occult outer retinopathy (AZOOR) [16].
Here, we aim to further expand on these findings by illustrating different topographic distributions of MEWDS and/or MEWDS-like reactions that we have observed in our clinical practice in order to improve our understanding of its clinical manifestations.
Methods
Subjects for this retrospective cohort study were identified at the Oxford Eye Hospital, UK, over the period January 2016 to January 2023. Participants were identified from an audit of the departmental electronic medical record system (Medisoft, Leeds, UK), which was cross-referenced with records kept by 2 retinal specialists (PCI and SMS). All clinical examinations were performed as part of routine clinical care, and therefore this work did not require formal ethical review [17]. The study was conducted in adherence with the Declaration of Helsinki.
Patients were included if they met diagnostic criteria for MEWDS, which included multifocal gray-white chorioretinal spots with foveal granularity, hyperfluorescent dots in the early phase of fluorescein angiography (FFA), hypofluorescent dots in the late phase on indocyanine green angiography (ICGA), and ellipsoid zone disruptions on spectral domain optical coherence tomography (OCT) [18].
Clinical records were reviewed for demographic information (age, gender, and ocular co-pathology) and clinical presentation (visual acuity, main presenting complaint, and duration of symptoms). Multimodal retinal imaging was obtained, which included OCT and fundus autofluorescence (AF) imaging (both HRA + OCT, Heidelberg Engineering, Heidelberg, Germany), fundus photography (Topcon, Tokyo, Japan), ultra-widefield pseudo-color and AF fundus imaging (Optos, Dunfermline, UK), FFA, and ICGA (both, Heidelberg Engineering and/or Optos) [19].
To determine the topography of retinal lesions, a horizontal and vertical line (maximum width) was drawn through the area of the chorioretinal spots on ultra-widefield AF imaging; the intersection of these lines defined the center of the total area of MEWDS lesions (at or around the optic disc, macular, or sectoral). If ultra-widefield AF imaging was not available, multifield late-phase ICGA and/or ultra-widefield pseudo-color images were used. Three authors (AYO, JB, and PCI) discussed each case and determined the topographical distribution via consensus.
For statistical analysis, continuous data were described with the median and interquartile range (IQR). As the Shapiro–Wilk test demonstrated a non-normal distribution, the Mann–Whitney U test was used to compare nonparametric data (age at presentation) at a significance level of p < 0.05.
Results
Description of patient cohort
We analyzed 29 MEWDS events in 27 patients (17 female and 10 male) with a median age of 36 years (interquartile range [IQR] 25 to 51). All patients had unilateral disease, and 11 patients (39%) were high myopes (≥ − 6 diopters). Patient characteristics are summarized in Table 1.
Thirteen patients (13/27, 48%) had concurrent chorioretinal pathology, including chorioretinal scarring or atrophy (n = 3), lacquer cracks with (n = 3) or without (n = 2) myopic choroidal neovascular membrane, punctate inner choroiditis (PIC) (n = 2), angioid streaks (n = 1), previous central serous chorioretinopathy (CSC) with residual RPE changes (n = 1), and previous laser retinopexy (n = 1). Patients with concurrent chorioretinal pathology tended to be older at presentation than those without (median 44 [IQR 38–62] vs 26 [23–33] years, p < 0.001).
Recurrence of MEWDS was documented in 1 patient (#14; 3 distinct episodes within 2 years), which was associated with contemporaneous expansion of myopic lacquer cracks. Another two patients recalled a previous diagnosis of MEWDS at different centers (one 3 years ago and another 21 years before); however, no confirmatory records were available, and their symptoms reportedly resolved spontaneously without treatment. A fourth patient experienced photopsia and a temporal scotoma 2 years prior to presentation, which resolved over a 2-week period. This had been attributed to a posterior vitreous detachment (PVD) at the time, and there was no multimodal imaging from this episode to clarify whether this could have been MEWDS-related.
Topographical distribution of MEWDS lesions
Multimodal imaging revealed different topographical distributions of MEWDS lesions, which were best illustrated on ultra-widefield AF imaging (Fig. 1). The most common distribution was characterized by MEWDS lesions that were densest or most confluent around the optic disc (17 of 29 events, 59%). The variable area involving more eccentric lesions seemed to be centered on or around the optic disc. In a subset of eyes in this group, the macula was relatively spared. In 7 out of 29 events (24%), MEWDS lesions were centered on the macula, and 2 eyes (7%) presented with a sectoral distribution. The pattern could not be conclusively ascertained in the remainder (3/29, 10%) because high-quality widefield images were not available. Involvement or sparing of the fovea may be observed in any subtype, including foveal involvement in cases with sectoral lesions that otherwise spare the central retina (Fig. 1C) or relative fovea sparing in patients with MEWDS lesions centered on the macula (Fig. 1B).
Widefield fundus autofluorescence images illustrate three distinct topographical distributions of MEWDS lesions: lesions centered on the optic disc (A), centered on the macula (B), and lesions with a sectoral distribution (C). Notably, the patient in B had a concurrent chorioretinal pathology—macular punctate inner choroidopathy scars
Patients without identifiable concurrent chorioretinal pathology (14/27, 52%) had MEWDS lesions with a range of topographical distributions: centered on or around the optic disc (7/14, 50%), centered on the macula (3/14, 21%), and sectoral (1/14, 7%). For the remainder (3/14, 21%), the distribution could not be determined due to the absence of widefield imaging.
In patients with concurrent chorioretinal pathology (13/27, 48%), the topographical distribution of MEWDS lesions was frequently centered on the lesion that presumably triggered the MEWDS episode. For example, they were centered on the optic disc or its immediate surroundings in patients with juxtapapillary chorioretinal lesions or breaks in Bruch’s membrane and centered on the macula in the patient with macular chorioretinal lesions (Fig. 1B). In the patient with documented recurrence of MEWDS (#14), the first and third episodes were centered on the optic disc and were associated with expanding juxtapapillary lacquer cracks; the second was centered on the macula and occurred with an expanding lacquer crack within the macula (Fig. 2; second episode previously illustrated in detail in Ref. 13).
Patient (#14) with 3 documented episodes of MEWDS. The first episode showed dots centered on the disc and was associated with an expanding lacquer crack superior to the disc (A); the second was centered on the macula, with an expanding lacquer crack in the macula (B); the third was centered on the disc and was associated with an expanding lacquer crack inferotemporal to the disc (C).
However, topographic relationships between concurrent chorioretinal pathology and MEWDS lesions were not always well-defined. One patient (#11) with a macular chorioretinal scar had dots centered on the optic disc; however, an unusually marked distribution of peripapillary atrophy was observed at the same time. This was also the case for another patient (#15) with subfoveal RPE disturbances attributed to previous CSC, who had dots (MEWDS lesions) centered on the disc along with significant peripapillary atrophy and a possible juxtapapillary defect in Bruch’s membrane. Neither of these patients were myopic nor had glaucoma, and it was unclear whether the topographical distribution of MEWDS lesions was primarily associated with the peripapillary changes or macular pathology. In another patient (#3), PIC-related chorioretinal scars were present in the nasal and peripapillary regions, with MEWDS lesions centered on the macula.
Value of multimodal imaging
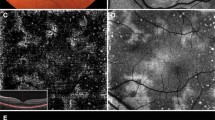
Widefield AF imaging was vital in visualizing the full extent of retinal lesions (Figs. 1, 2, and 3). Figure 3 illustrates that full topographic distribution was best captured on ultra-widefield AF imaging (A) but could not be ascertained on AF images limited to the posterior pole (B). Fluorescein angiography often did not add much information (C). The retinal changes in MEWDS were sometimes poorly visible on fundal examination (D), particularly in patients with myopic fundi. The combination of fundus AF and OCT (E) imaging was often invaluable in making the diagnosis. Moreover, potential underlying chorioretinal pathology was sometimes only visible on specific imaging modalities, such as the visualization of small breaks in Bruch’s membrane on late-phase ICGA images (F, G). In this example, late-phase ICGA images were also helpful for determining the nasal eccentricity of lesions and that hence, MEWDS lesions were approximately centered on the disc.
Multimodal imaging (patient #21) demonstrates the importance of different imaging modalities in diagnosing MEWDS, particularly in patients with high myopia. Widefield autofluorescence imaging (A) shows the lesions to be centered on the disc, which is not illustrated in 30° autofluorescence images (B). Fluorescein angiography (C) and widefield pseudo-color images (D) showed only faint lesions. Typical disruption of the ellipsoid band is shown on the macular OCT image (E). Late-phase indocyanine green angiography (30 − 40 min; F, G) shows hypocyanescent dots typical for MEWDS and highlights peripapillary breaks in Bruch’s membrane that are present concurrently. To determine the topography of retinal lesions, a horizontal and vertical line (maximum width) was drawn through the area of the chorioretinal spots on ultra-widefield AF imaging (A)
Patient #14, who had 3 distinct episodes of MEWDS, is another example illustrating the value of multimodal imaging when OCT images are difficult to interpret due to additional myopia-related pathology or mild disease (Fig. 2). The first episode featured only mild changes, which were not evident on pseudocolor images due to the appearance of her myopic fundus. The mild hyperautofluorescent dots and subtle photoreceptor layer disturbances were identified when reviewing her previous AF and OCT imaging after she presented with her second episode, due to the heightened index of suspicion.
Clinical course
Patients were followed up for a median of 8 months (IQR: 2–16 months). Follow-up data of at least 3 months’ duration were available from 18/27 (67%) patients. Of these, the majority (14/18, 78%) experienced resolution of their symptoms and retinal changes on multimodal imaging by 3 months. Four patients had symptoms persisting beyond 12 months: two had dots centered on the disc and two on the macula at their first presentation. At their final visit, there were a few persistent scattered white dots on AF, alongside persistent mild peripapillary ellipsoid zone loss and chorioretinal atrophy on OCT imaging. Of these 4 patients, 1 developed an acute zonal occult outer retinopathy (AZOOR)-like picture with thinning of the outer nuclear layer in the peripapillary region at 4 months.
Discussion
This study describes different topographical distributions of the fundus changes observed in MEWDS: centered on the macula, centered on the optic disc, or sectoral. Lack of multimodal retinal imaging, including widefield fundus autofluorescence and (very) late-phase ICG imaging, may explain why MEWDS fundus changes have previously been described as primarily affecting the perifoveal region. Widefield imaging is vital in visualizing the extent of retinal lesions, which may be poorly visible on fundal examination, particularly in myopic fundi [13].
Our series indicates that there may be an association between the topographical distribution of MEWDS lesions and coexisting chorioretinal pathology in some patients. The clinical significance of the topographical distributions in MEWDS and whether they carry any prognostic significance in respect of recurrence, recovery, development of AZOOR, or accelerated atrophy, remains to be elucidated. Based on our data, we cannot comment if different distribution patterns of MEWDS lesions may occur sequentially, as this would require prospective standardized recordings of high-quality wide-field autofluorescence images with short intervals. Of note, different patterns of distribution have also been described in other related conditions; for example, different patterns of spread in patients with AZOOR [20].
Almost half of our cohort had concurrent ocular co-pathologies involving the choroid and retina. This frequent co-occurrence mirrors recent studies, which described antecedent or concurrent ocular insults including choroidal neovascularization [10], angioid streaks [8], ocular trauma [9], and inflammatory conditions such as chorioretinitis [7]. A recent study that addressed the outcome of visual acuity in patients with MEWDS reported a similar coexistence of chorioretinal disease (31%; 21/68 patients) but excluded these patients from further analysis [6]. In our patient cohort, although the group with concurrent chorioretinal pathology was significantly older, both groups had similar retinal phenotypes without obvious difference in prognosis. Thus, we postulate that primary and secondary MEWDS are part of the same disease spectrum rather than a distinct entity.
It has been hypothesized that MEWDS develops from the complex interplay between genetic susceptibility and environmental triggers [21]. Environmental factors may include exposure to retinal antigens resulting from damage to the RPE-Bruch’s membrane interface, which may expose retinal antigens and trigger a local inflammatory response [7, 8], or potential associations with viral infections such as acute Epstein-Barr virus or herpes virus infections [22, 23]. However, the inherent problems with serum retinal autoantibody testing make it challenging to prove this theory [24, 25]. If such analysis becomes possible in the future, it might reveal specific ocular antigen(s), as seen in cancer- or melanoma-associated retinopathy, and may also help further our understanding of the similarities or differences in the pathogenesis of MEWDS and ‘secondary’ or ‘epi’-MEWDS.
We speculate that MEWDS may potentially be underdiagnosed, particularly in patients with atypical presentation and/or because comprehensive multimodal retinal imaging may not be performed if MEWDS is not suspected [26, 27]. Diagnostic difficulty may be further enhanced in patients with high myopia or due to confirmation bias in presence of concurrent chorioretinal pathology. For instance, photopsias in high myopes may also be attributed to nascent posterior vitreous detachment, and focusing on the concurrent chorioretinal pathology (such as a myopic CNV) may also distract from the diagnosis. As such, a higher index of suspicion in these patients may be helpful.
In conclusion, a heightened awareness of this retinal entity, its signs and symptoms, and a more rigorous use of multimodal imaging may help to improve the diagnosis of MEWDS as well as enhance our understanding of secondary MEWDS.
Strengths and limitations
Limitations include the retrospective nature of the study and all this entails, including the lack of standardized review intervals and imaging protocols. It is also not possible to comment on whether topographical distribution may change from one to another and if patterns may overlap. Despite the small number of patients included, which is due to the relative rarity of the condition, this study ranks among the larger cohorts of MEWDS cases reported. Multicenter studies with standardized high-quality imaging protocols and serial imaging in the acute phases may add to our findings and further enhance our understanding of this condition and its pathogenesis. This may also allow more robust associations between phenotypic expression and other parameters, such as outcomes or predictors of recurrence to be drawn.
References
Jampol LM, Sieving PA, Pugh D, Fishman GA, Gilbert H (1984) Multiple evanescent white dot syndrome. I. Clinical findings. Arch Ophthalmol 102(5):671–674
Gross NE, Yannuzzi LA, Freund KB, Spaide RF, Amato GP, Sigal R (2006) Multiple evanescent white dot syndrome. Arch Ophthalmol 124(4):493–500
Marsiglia M, Gallego-Pinazo R, Cunha de Souza E et al (2016) Expanded clinical spectrum of multiple evanescent white dot syndrome with multimodal imaging. Retina 36(1):64–74
Zicarelli F, Mantovani A, Preziosa C, Staurenghi G (2020) Multimodal imaging of multiple evanescent white dot syndrome: a new interpretation. Ocul Immunol Inflamm 28(5):814–820
Pichi F, Srvivastava SK, Chexal S et al (2016) En face optical coherence tomography and optical coherence tomography angiography of multiple evanescent white dot syndrome: new insights into pathogenesis. Retina 36(Suppl 1):S178–S188
Bosello F, Westcott M, Casalino G et al (2022) Multiple evanescent white dot syndrome: clinical course and factors influencing visual acuity recovery. Br J Ophthalmol 106(1):121–127
Cicinelli MV, Hassan OM, Gill MK, Goldstein D, Parodi MB, Jampol LM (2021) A multiple evanescent white dot syndrome-like reaction to concurrent retinal insults. Ophthalmol Retina 5(10):1017–1026
Gliem M, Birtel J, Müller PL et al (2019) Acute retinopathy in pseudoxanthoma elasticum. JAMA Ophthalmol 137(10):1165–1173
Landolfi M, Bhagat N, Langer P et al (2004) Penetrating trauma associated with findings of multiple evanescent white dot syndrome in the second eye: coincidence or an atypical case of sympathetic ophthalmia? Retina 24(4):637–645
Mathis T, Delaunay B, Cahuzac A, Vasseur V, Mauget-Faÿsse M, Kodjikian L (2018) Choroidal neovascularisation triggered multiple evanescent white dot syndrome (MEWDS) in predisposed eyes. Br J Ophthalmol 102(7):971–976
Bryan RG, Freund KB, Yannuzzi LA, Spaide RF, Huang SJ, Costa DL (2002) Multiple evanescent white dot syndrome in patients with multifocal choroiditis. Retina 22(3):317–322
Burke TR, Addison PKF, Pavesio CE (2022) Multifocal evanescent white dot syndrome-like phenotypes associated with inflammatory and myopic choroidal neovascularization. Ocul Immunol Inflamm 30(7–8):1707–1714
Ong AY, Birtel J, Charbel Issa P (2021) Multiple evanescent white dot syndrome (MEWDS) associated with progression of lacquer cracks in high myopia. Klin Monatsbl Augenheilkd 238(10):1098–1100
Essilfie J, Bacci T, Abdelhakim AH et al (2022) Are there two forms of multiple evanescent white dot syndrome? Retina 42(2):227–235
Hamed LM, Glaser JS, Gass JD, Schatz NJ (1989) Protracted enlargement of the blind spot in multiple evanescent white dot syndrome. Arch Ophthalmol 107(2):194–198
Fine HF, Spaide RF, Ryan EH, Matsumoto Y, Yannuzzi LA (2009) Acute zonal occult outer retinopathy in patients with multiple evanescent white dot syndrome. Arch Ophthalmol 127(1):66–70
Medical Research Council UKRI. Is my study research? Is my study research? http://www.hra-decisiontools.org.uk/research/. Accessed 15 Sep 2022
The Standardization of Uveitis Nomenclature (SUN) Working Group (2021) Classification criteria for multiple evanescent white dot syndrome. Am J Ophthalmol 228:198–204
Birtel J, Yusuf IH, Priglinger C, Rudolph G, Charbel Issa P (2021) Diagnosis of inherited retinal diseases. Klin Monatsbl Augenheilkd 238(3):249–259
Shifera AS, Pennesi ME, Yang P, Lin P (2017) Ultra-wide-field fundus autofluorescence findings in patients with acute zonal occult outer retinopathy. Retina 37(6):1104–1119
Jampol LM, Becker KG (2003) White spot syndromes of the retina: a hypothesis based on the common genetic hypothesis of autoimmune/inflammatory disease. Am J Ophthalmol 135(3):376–379
Yang CS, Hsieh MH, Su HI, Kuo YS (2019) Multiple evanescent white dot syndrome following acute Epstein-Barr virus infection. Ocul Immunol Inflamm 27(2):244–250
Haw YL, Yu TC, Yang CS (2020) A CARE-compliant article: a case report of possible association between recurrence of multiple evanescent white dot syndrome and the Herpesviridae family. Medicine (Baltimore) 99(15):e19794
Adamus G (2020) Current techniques to accurately measure anti-retinal autoantibodies. Expert Rev Ophthalmol 15(2):111–118
Chen JJ, McKeon A, Greenwood TM et al (2021) Clinical utility of antiretinal antibody testing. JAMA Ophthalmol 139(6):658–662
Shelsta HN, Rao RR, Bhatt HK, Jampol LM (2011) Atypical presentations of multiple evanescent white dot syndrome without white dots: a case series. Retina 31(5):973–976
Gal-Or O, Priel E, Rosenblatt I, Shulman S, Kramer M (2017) Multimodal imaging in an unusual cluster of multiple evanescent white dot syndrome. J Ophthalmol 2017:e7535320
Funding
This work was supported by the Dr. Werner Jackstädt Foundation, Wuppertal, Germany (Grant S0134-10.22 to J.B.), and the National Institute for Health Research (NIHR) Oxford Biomedical Research Centre (BRC). The funding organizations had no role in the design and conduct of the study; collection, management, analysis, and interpretation of the data; preparation, review, or approval of the manuscript; or decision to submit the manuscript for publication. The views expressed are those of the authors and not necessarily those of the NHS, the NIHR, or the Department of Health.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Competing interests
The authors declare no competing interests.
Additional information
Publisher's note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if changes were made. The images or other third party material in this article are included in the article's Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article's Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
Ong, A.Y., Birtel, J., Agorogiannis, E. et al. Topographic patterns of retinal lesions in multiple evanescent white dot syndrome. Graefes Arch Clin Exp Ophthalmol 261, 2257–2264 (2023). https://doi.org/10.1007/s00417-023-06032-1
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00417-023-06032-1