Abstract
Background
Acute kidney injury (AKI) is independently associated with increased morbidity and mortality across the life course, yet care for AKI remains mostly supportive. Raising awareness of this life-threatening clinical syndrome through education and advocacy efforts is the key to improving patient outcomes. Here, we describe the unique roles education and advocacy play in the care of children with AKI, discuss the importance of customizing educational outreach efforts to individual groups and contexts, and highlight the opportunities created through innovations and partnerships to optimize lifelong health outcomes.
Methods
During the 26th Acute Disease Quality Initiative (ADQI) consensus conference, a multidisciplinary group of experts discussed the evidence and used a modified Delphi process to achieve consensus on recommendations on AKI research, education, practice, and advocacy in children.
Results
The consensus statements developed in response to three critical questions about the role of education and advocacy in pediatric AKI care are presented here along with a summary of available evidence and recommendations for both clinical care and research.
Conclusions
These consensus statements emphasize that high-quality care for patients with AKI begins in the community with education and awareness campaigns to identify those at risk for AKI. Education is the key across all healthcare and non-healthcare settings to enhance early diagnosis and develop mitigation strategies, thereby improving outcomes for children with AKI. Strong advocacy efforts are essential for implementing these programs and building critical collaborations across all stakeholders and settings.
Similar content being viewed by others
Explore related subjects
Discover the latest articles, news and stories from top researchers in related subjects.Avoid common mistakes on your manuscript.
Introduction
Understanding of pediatric acute kidney injury (AKI) continues to advance, with increasing recognition of different phenotypes and underlying pathophysiology. Management of AKI remains mostly supportive, aimed at early identification and interventions to mitigate progression. Lack of AKI awareness among healthcare workers and insufficient knowledge in the public of risk factors, signs, symptoms, and complications of AKI impede early identification. Inappropriate resources in different clinical settings and limited governmental/institutional support challenge the ability to improve AKI care through education and/or quality improvement. The 26th Acute Disease Quality Initiative (ADQI) consensus conference was convened to improve clinical care and identify the research agenda in pediatric AKI. This article addresses the roles education and advocacy play in improving care and outcomes related to AKI in children. We ask and answer three key questions:
-
Question 1: What unique roles do education and advocacy play in advancing AKI care for children?
-
Question 2: How do we customize AKI education and advocacy efforts for diverse groups and settings?
-
Question 3: What innovations and partnerships will raise awareness, overcome barriers, and advocate for optimal lifelong outcomes in AKI?
Methods
The 26th ADQI consensus conference was held over 3 days in Napa, USA, in November 2021, and included an interdisciplinary group of clinicians and researchers from North and South America, Africa, Asia, and Europe. The first ADQI conference with a completely pediatric focus, this group included 47 multidisciplinary experts from pediatric nephrology, pediatric and adult critical care, pharmacy, epidemiology, health services research, pediatric nephrology nursing, nutrition, and patients, as previously described [1]. This meeting followed the established ADQI process [2]. A detailed description of the ADQI methodology is available at www.adqi.net. The broad objective of ADQI is to provide expert-based statements and a summary of current knowledge for use by clinicians and researchers according to ADQI’s professional judgment and to identify evidence gaps to establish research priorities.
The Education and Advocacy workgroup sought to develop consensus statements to enhance education efforts and to provide a framework for advocacy to improve outcomes of children with and at risk for AKI. The workgroup included clinicians and researchers, as well as an AKI survivor, and an expert in advocacy and social determinants of health. The consensus-building process employed an objective review of articles identified through a PubMed search. The results of this consensus conference are not based on a formal systematic review process; rather, a modified Delphi method was used to reach consensus, using evidence-based literature when possible, with the goal of addressing the key questions and articulating a research agenda to address knowledge gaps. A summary of the consensus conference has been previously published [1]. We describe our workgroup’s consensus findings, as well as detailed recommendations to be used as a framework for the advancement of pediatric AKI care through educational and advocacy approaches.
Results
A critical recommendation of the consensus panel was a need to improve pediatric AKI education and advocacy efforts:
Given the adverse immediate and lifelong outcomes for children with AKI, education and advocacy are essential, starting with the patient and family and expanding across health care teams, systems, and communities.
We thus sought to answer three questions developed during the ADQI consensus conference.
Question 1: What unique roles do education and advocacy play in advancing AKI care for children?
Consensus statements
1a. Given the significant short- and long-term risks to patients, and the high burden of AKI on healthcare systems, greater education about AKI is necessary for all members of the healthcare system.
1b. In the absence of easily recognizable signs and symptoms and the lack of specific treatment for AKI, education and advocacy are essential to improve understanding (awareness) and recognition of AKI.
Despite three decades of intensified research, AKI-related morbidity and mortality rates remain unacceptably high. AKI may lack clinical signs or symptoms and can occur in any patient. Therefore, a critical step in addressing the AKI epidemic is robust education aimed at improving awareness of the impact of AKI and recognition of risk factors. The first contact with the healthcare system for a patient with AKI is generally in the primary care setting, emergency room, or inpatient wards by non-nephrologists. The healthcare professional may be a medical student, resident, attending physician, advanced practice provider, nurse, community health care worker, or pharmacist. Each of these levels of direct patient care offers opportunities to improve AKI recognition and mitigate AKI risks [3].
AKI awareness remains variable across different healthcare settings, contributing to disparities in outcomes [4]. AKI often goes unrecognized in the community and outside the intensive care setting in the hospital [5]. Community-acquired AKI occurred in 1.5% of emergency room encounters and 37% of AKI was missed by the emergency or inpatient clinician in those admitted [6]. In a survey evaluating AKI education and knowledge among nursing staff in rural South Africa, only 37.8% reported confidence in managing a patient with AKI; 97% reported wanting additional training. Similarly, 61% of nurses across 11 districts reported never receiving training on AKI, and one-third of health care workers were unaware of dialysis availability at the National Referral Hospital in Malawi [7]. Given how frequently AKI goes unrecognized, developing AKI education specific to non-nephrologists is a critical step for improving AKI care [8].
Improving awareness and early identification of AKI must focus on improving clinical care. In Malawi, following a nurse-led educational intervention that included a comprehensive classroom and ward-based teaching on AKI, there was a significant improvement in the healthcare workers’ attitudes towards detecting or managing patients with suspected AKI with concomitant improvements in care processes (e.g., completion of fluid charts and recording of urine output) [9]. The use of checklists, standardized screening, and care protocols (“care bundles”) in both inpatient and outpatient settings enhance detection and identification of patients with or at risk for AKI [10]. Clinical assessment tools deployed in three low-resource countries predict KDIGO stage 3 AKI [11]. Educational interventions at teaching hospitals in the UK, designed to increase understanding of AKI, demonstrated increased physician awareness based on self-reported management of patients and comparison of AKI knowledge assessed on pre- and post-education questionnaires [12]. In another UK study, electronic alerts deployed at a teaching hospital not only raised awareness of AKI but improved outcomes, leading to less progression to higher stages of AKI, fewer emergency re-admissions, and a reduction in mortality [13]. A pediatric multi-center intervention to raise awareness of the impact of nephrotoxic medications on the development of AKI led to decreased AKI rates [14]. More studies are needed, particularly in the pediatric age group.
Improving education and awareness about kidney disease requires strong advocacy efforts to unify the different constituents who participate in AKI prevention, early recognition, and treatment (Fig. 1). These constituents include patients and family members, community members, physicians within and outside of nephrology, allied healthcare professionals, industry affiliates, government, and non-governmental organizations. Each has unique skills, vantage points, and priorities within the healthcare team that can be harnessed in mitigating pediatric AKI. Champions within each of these groups can highlight the relevance of AKI to their own constituents to advocate for and obtain the human and financial resources needed to grow and sustain these efforts.
Effective acute kidney injury (AKI) education programs center the child and family (yellow circle at center) and expand across health care teams, systems, and communities with champions embedded at every level (community (orange), healthcare systems (red), science and government (purple)), all supported by the pillar of advocacy
Research recommendations
-
1.
Future work should emphasize strong AKI-related advocacy efforts among all constituents.
-
2.
Future work should focus on the recognition and improvement of clinical care at the bedside through more accurate detection and identification of patients with or at risk for AKI.
-
3.
Future work should seek to bring knowledge of AKI and its risks to the general population.
Question 2: How do we customize AKI education and advocacy efforts for diverse groups and settings?
Consensus statement
2. Given the complexity of the healthcare system and multiple stakeholders involved, AKI education requires a comprehensive, multi-disciplinary approach with AKI champions embedded at every level, with appropriate consideration of local context.
AKI education may be accomplished through numerous methods, tailored for a variety of learners, at the micro (e.g., teaching individual learners, training program curriculum, teaching modules, alert systems for clinicians) and macro (e.g., healthcare system, community-wide educational programs, governmental policy) level. Recognizing the integral role that families provide in child health and development, and that most AKI develops in the community, AKI education programs should center on children and their families. Educating and empowering patients and families allow them to participate in AKI prevention at home, reducing the burden of undetected AKI in children. During illness, patients and families may not be aware of an AKI event or the associated long-term risks [15, 16]; patient and family education can yield healthy lifestyle modification and may improve follow-up, limiting repeat AKI events. Patients and families require diverse, adaptable, and multifaceted educational tools in a variety of primary languages, levels of health literacy, and cultural contexts. With increasing recognition of diminished health-related quality of life in AKI survivors [17, 18] and worse neurodevelopmental outcomes among pediatric AKI survivors [19,20,21,22], there is a need for evidence on how to provide appropriate psychosocial support to AKI survivors, tailored to the unique developmental needs of the child.
AKI affects the outcomes of many conditions and illnesses managed primarily by non-nephrologists (e.g., congenital heart disease undergoing surgical care, oncologic disease, and critical illness in neonates). Complex healthcare systems with highly specialized care teams can lead to overly routinized thinking that may limit recognition of off-target clinical concerns like AKI. Such siloed approaches could be overcome with focused education to enhance collaboration. Educational and advocacy efforts can be tailored to each discipline and for clinicians, bedside nurses, and other interdisciplinary team members (e.g., ICU dietitians and pharmacists) to optimize relevance for each. In lower income settings and rural areas, community health extension workers may be the first point of contact for patients, and much of the initial recognition and management of AKI is undertaken by them.
We recommend developing clear and consistent objectives for AKI education along with methods to evaluate their efficacy. These objectives should be developed with community engagement incorporating suggestions from the public, patients and caregivers, and community healthcare workers. For practitioners, AKI education must be a core competency [8, 23]. In the UK, the Academy of Royal Medical Colleges has codified the knowledge, skills, and behaviors required for safe and effective care of a patient with AKI [24]. This approach can be adapted for education of all healthcare professionals at all levels and should be integrated as part of continuing medical education. The Latin American Society of Nephrology and Hypertension created two online courses, one for nephrologists and one for primary care physicians, to improve AKI awareness [25]. Learning objectives for the two courses were specific to the needs of each target audience. There was a mean knowledge gain of 36% seen with pre- and post-course tests. Both groups expressed high rates of satisfaction with the activity and commitment to improve their clinical practice. With the implementation of educational programs will come the need to monitor knowledge gain, improvement in quality of care, and differences in patient outcomes.
While we recognize the importance of AKI education, there are limited data on how most effectively to structure such programs. Developing meaningful educational programs requires thoughtful preparation, innovative design, and a robust iterative review process. These are key principles in Education Design Research (EDR), a pragmatic and participatory approach for solving educational problems within the authentic, complex educational setting [26, 27]. For AKI education, given its broad and diverse spectrum of participants and stakeholders, local problem analysis is imperative. Identifying participants and examining barriers (e.g., time and competing priorities) to enhance awareness and knowledge is a necessary first step. This can be done with qualitative surveys, needs assessments, literature reviews, reviews of societal guidelines, and assessment of existing educational programs. Once this process is complete, design and implementation of educational systems can occur alongside continuous evaluation and iteration of each program. Online simulation modules for nursing students to recognize patient deterioration [28] and using virtual patients and concept mapping software to teach clinical reasoning skills to medical students are examples of EDR implementation [29]. EDR is also utilized outside of medical education programs highlighting the ability to apply these principles in diverse settings.
The nephrology community can learn from successful initiatives for other conditions (e.g., diabetes, HIV) where education has been shown to improve outcomes including clinical, financial, and patient quality of life. A multisector model with public/private partnership, community support, and use of local resources has shown success in achieving various Millennium Development Goals (MDGs) by increasing awareness and intervention [30]. Following the MDGs, the Sustainable Development Goals (SDGs) were established to provide a more holistic set of goals that promote healthy and sustainable societies; these have been applied to kidney health [31]. Multisector models with public/private partnerships that engage United Nations agencies, governments, businesses, and local community partners have been successful in achieving various MDGs by increasing awareness and intervention. The nephrology community must engage international partners working on global health targets to integrate AKI prevention in the programs. These efforts should be driven by the nephrology community through organizations like the International Pediatric Nephrology Association and the International Society of Nephrology through programs such as the AKI 0 by 25 program and engaging stakeholders at the policy level, including the World Health Organization.
Lessons from other health programs can inform the design of an AKI-focused curriculum [32]. Traditionally such programs were designed and taught by those from high-resource countries, with limited input from and consideration of diverse global perspectives and practices. Recently, the Synthesis and Translation of Research and Innovations from Polio Eradication (STRIPE) consortium described its collaborative process of developing content and curriculum for an international course, along with recommendations for future similar efforts [33]. The course designed by the STRIPE consortium has an online component (massive open online course (MOOC)) along with in-person courses taught by local experts that could reach students in a variety of public health contexts across the world.
While MOOCs are effective in reaching a global audience, their production can be resource intensive. With trainees increasingly using social media platforms for free open-access medical education [34], efforts are needed to develop online AKI educational resources that increase access to evidence-based information appropriate for pediatric populations. Nephrology-specific educational resources in the form of games, online journal clubs, and interactive learning are making education available globally 24 h a day [35, 36]. Such platforms can be harnessed to increase access to education outside of traditional classrooms, conferences, and local institutions.
Research recommendations
-
1.
Future work should begin with a thorough, in-depth problem analysis and evaluation of the educational problem which is key to successful implementation and future systematic change of education programs.
-
2.
Future work should include creating AKI education programs that are applicable to various settings and resources and adaptable to local needs and knowledge gaps.
Question 3: What innovations and partnerships will raise awareness, overcome barriers, and advocate for optimal lifelong outcomes in AKI?
Consensus statement
3. AKI awareness, prevention, and mitigation requires coordinated efforts to develop effective tools that will preempt and screen for AKI and provide guidance for care acutely and long-term. In partnership with industry, government, non-governmental organizations, and professional societies, these tools must leverage current and advancing technology to yield efficient and equitable care regardless of local resources.
While AKI-related education may increase awareness, timely recognition of AKI is dependent on the availability of diagnostic tools for AKI risk and recovery. Effectiveness of tools may depend on clinical context and available resources; increasing partnerships between industry, governmental, and non-governmental stakeholders will focus attention and resources to improve AKI diagnosis. A survey of global health information registries in 154 countries showed that while 57% of countries had transplant registries (range 15–100% by ISN region), 8% of countries had AKI registries and 4% had programs in place to detect AKI [37]. Partnerships to establish AKI registries with support from governmental and non-governmental stakeholders will facilitate data collection and inform local needs in addressing priority AKI populations. AKI advocates are needed to reach out to these entities through effective campaigns and persuade them to allocate resources to these efforts. Toolkits created and shared by content experts would support these local efforts [8].
In low-resource settings, inadequate training, shortage of healthcare workers, and lack of awareness by health care teams, governments, and the public are major barriers to recognizing AKI and understanding its significance as a health problem [38]. Government buy-in is crucial to ensure adequate resources to support the education of healthcare workers and the provision of diagnostic aids and basic therapies. Programs in low and lower middle-income countries can lose trained staff who leave to work in higher-resourced areas [39]. Appropriate support from the local government may encourage trained staff to remain in their own countries with the confidence that they may be able to develop successful programs.
Partnership with industry can be leveraged across multiple domains, whether it is the development and distribution of newer diagnostic tools, or harnessing information technology to educate, monitor or follow up patients with AKI. Limited diagnostic and treatment facilities in health centers are reported as a significant barrier in global AKI care [38]. Lack of laboratory infrastructure leads to substantial inequities in access to AKI diagnostics and further accentuates adverse healthcare outcomes from delayed diagnosis of AKI. Access to creatinine testing may be limited or unavailable in outpatient, rural, or low-income settings. Point of care creatinine can serve where central laboratory testing facilities may not be available [11]. Biomarkers of structural kidney injury could help identify children in need of additional monitoring in-hospital and also risk-stratify children who may benefit from additional clinical monitoring to assess kidney recovery [40]. Urine neutrophil gelatinase-associated lipocalin (NGAL) has been adapted to a urine dipstick test which correlates well with reference assays and has been used for diagnosis of pediatric AKI in Africa [41, 42]. Point-of-care tests that can be used in community settings to identify children based on creatinine or alternative indicators of AKI (e.g., saliva urea nitrogen, urine NGAL dipsticks) have potential to overcome barriers related to accessible, affordable, and equitable AKI diagnostics.
Increasing global interconnectedness raises opportunities to leverage technology to support equitable diagnosis of AKI. Technological approaches to facilitate AKI diagnosis and follow-up must be adapted based on the availability and integration of health information technology within health systems. Telemedicine can establish linkages across settings, both within and between countries, to ensure that patients in remote, rural, or low-income settings have access to specialized care and appropriate follow-up without necessarily requiring in-person referral [11]. This could improve clinical care, optimize follow-up, and expand education to health care workers in more remote settings.
In settings where advanced health information technology is limited, there is often relatively easier access to mobile health technology where apps could be used to integrate AKI risk assessment as part of the triage process for the sick child. A precision public health approach has been used to improve post-discharge outcomes in children following sepsis events in Uganda [43]. The program, called Smart discharges, uses risk prediction to identify at-risk children, counsel parents at discharge about potential complications and when to seek care, and connect high-risk children to community health centers and healthcare workers for follow-up. It can be used as a stand-alone mobile application or be integrated into existing electronic health platforms. Such a program can be adapted to include AKI risk factors and danger signs and represents an opportunity to leverage partnerships to improve AKI risk prediction, identification, and follow-up care in settings where formal systems are lacking.
In resource-sufficient settings that utilize electronic health records, clinical decision support systems could be adapted to prompt AKI assessment based on presenting signs and automated to detect AKI events and recommend additional monitoring and follow-up.
Research recommendations
-
1.
Future work should be focused on using iterative testing to refine diagnostic and therapeutic innovations.
-
2.
Future work should expand connections between healthcare, industry, government and other groups to bring AKI prevention, diagnosis, and care to all communities.
Conclusions
AKI is an increasingly important public health concern. These consensus statements emphasize that high-quality care for patients with AKI begins in the community with education and awareness campaigns to identify patients at risk for AKI (Fig. 2). Education is the key across all healthcare and non-healthcare settings to improve early diagnosis and implement mitigation strategies, thereby improving outcomes for children with AKI. More research is needed to design educational programs with clear and consistent objectives for AKI learning along with methods to address and evaluate the efficacy of implementation of these objectives. Education is essential but not sufficient; collaboration between health care teams, medical systems, and institutional organizations is necessary to develop AKI identification tools which leverage modern technology and are adaptable to any clinical venue, community, or resource environment. To realize these programs, strong advocacy efforts with clear messaging relevant to various stakeholders are needed to overcome financial, time, infrastructure, and human resource limitations. Developing strong communities of AKI champions may be the key to overcoming short- and long-term effects of this potentially devastating clinical syndrome and improving outcomes for children around the world.
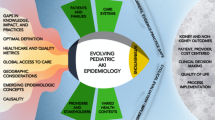
Education to improve acute kidney injury (AKI) awareness and recognition in children rests on the foundation of advocacy and must engage key stakeholders in developing multidisciplinary, context-appropriate, and customized approaches to improve AKI care globally and across all resource settings. NINJA, Nephrotoxic injury negated by just-in-time action program; NGAL, neutrophil gelatinase-associated lipocalin. Permission to use content, including icons, templates, and other original artwork, granted by BioRender
References
Goldstein SL, Akcan-Arikan A, Alobaidi R, Askenazi DJ, Bagshaw SM, Barhight M, Barreto E, Bayrakci B, Bignall ONR, Bjornstad E, Brophy PD, Chanchlani R, Charlton JR, Conroy AL, Deep A, Devarajan P, Dolan K, Fuhrman DY, Gist KM, Gorga SM, Greenberg JH, Hasson D, Ulrich EH, Iyengar A, Jetton JG, Krawczeski C, Meigs L, Menon S, Morgan J, Morgan CJ, Mottes T, Neumayr TM, Ricci Z, Selewski D, Soranno DE, Starr M, Stanski NL, Sutherland SM, Symons J, Tavares MS, Vega MW, Zappitelli M, Ronco C, Mehta RL, Kellum J, Ostermann M, Basu RK; Pediatric ADQI Collaborative (2022) Consensus-based recommendations on priority activities to address acute kidney injury in children: a modified Delphi consensus statement. JAMA Netw Open 5:e2229442
Kellum JA, Bellomo R, Ronco C (2008) Acute Dialysis Quality Initiative (ADQI): methodology. Int J Artif Organs 31:90–93
Kellum JA, Lameire N (2019) Advocacy for broader inclusion to combat the global threat of acute kidney injury. Nephrol Dial Transplant 34:1264–1265
Macedo E, Cerda J, Hingorani S, Hou J, Bagga A, Burdmann EA, Rocco VM, Mehta LR (2018) Recognition and management of acute kidney injury in children: the ISN 0by25 Global Snapshot study. PLoS One 13:e0196586
McGregor TL, Jones DP, Wang L, Danciu I, Bridges BC, Fleming GM, Shirey-Rice J, Chen L, Byrne DW, Van Driest SL (2016) Acute kidney injury incidence in noncritically ill hospitalized children, adolescents, and young adults: a retrospective observational study. Am J Kidney Dis 67:384–390
Bernardo EO, Cruz AT, Buffone GJ, Devaraj S, Loftis LL, Arikan AA (2018) Community-acquired acute kidney injury among children seen in the pediatric emergency department. Acad Emerg Med 25:758–768
Evans R, Rudd P, Hemmila U, Dobbie H, Dreyer G (2015) Deficiencies in education and experience in the management of acute kidney injury among Malawian healthcare workers. Malawi Med J 27:101–103
Liu KD, Goldstein SL, Vijayan A, Parikh CR, Kashani K, Okusa MD, Agarwal A, Cerda J, AKI!Now Initiative of the American Society of Nephrology (2020) AKI!Now Initiative: recommendations for awareness, recognition, and management of AKI. Clin J Am Soc Nephrol 15:1838–1847
Kirwan CJ, Wright K, Banda P, Chick A, Mtekateka M, Banda E, Kawale Z, Evans R, Dobbie H, Dreyer G (2016) A nurse-led intervention improves detection and management of AKI in Malawi. J Ren Care 42:196–204
Menon S, Tarrago R, Carlin K, Wu H, Yonekawa K (2021) Impact of integrated clinical decision support systems in the management of pediatric acute kidney injury: a pilot study. Pediatr Res 89:1164–1170
Macedo E, Hemmila U, Sharma SK, Claure-Del Granado R, Mzinganjira H, Burdmann EA, Cerda J, Feehally J, Finkelstein F, Garcia-Garcia G, Jha V, Lameire NH, Lee E, Levin NW, Lewington A, Lombardi R, Rocco MV, Aronoff-Spencer E, Tonelli M, Yeates K, Remuzzi G, Mehta RL, ISN 0by25 Trial Study Group (2021) Recognition and management of community-acquired acute kidney injury in low-resource settings in the ISN 0by25 trial: a multi-country feasibility study. PLoS Med 18:e1003408
Xu G, Baines R, Westacott R, Selby N, Carr S (2014) An educational approach to improve outcomes in acute kidney injury (AKI): report of a quality improvement project. BMJ Open 4:e004388
Atia J, Evison F, Gallier S, Hewins P, Ball S, Gavin J, Coleman J, Garrick M, Pankhurst T (2023) Does acute kidney injury alerting improve patient outcomes? BMC Nephrol 24:14–23
Goldstein SL, Dahale D, Kirkendall ES, Mottes T, Kaplan H, Muething S, Askenazi DJ, Henderson T, Dill L, Somers MJG, Kerr J, Gilarde J, Zaritsky J, Bica V, Brophy PD, Misurac J, Hackbarth R, Steinke J, Mooney J, Ogrin S, Chadha V, Warady B, Ogden R, Hoebing W, Symons J, Yonekawa K, Menon S, Abrams L, Sutherland S, Weng P, Zhang F, Walsh K (2020) A prospective multi-center quality improvement initiative (NINJA) indicates a reduction in nephrotoxic acute kidney injury in hospitalized children. Kidney Int 97:580–588
Diamantidis CJ, Burks E, Mohottige D, Riley J, Bowman C, Lunyera J, St Clair Russell J (2022) What do acute kidney injury survivors want to know about their condition: a qualitative study. Kidney Med 4:100423
Silver SA, Saragosa M, Adhikari NK, Bell CM, Harel Z, Harvey A, Kitchlu A, Neyra JA, Wald R, Jeffs L (2018) What insights do patients and caregivers have on acute kidney injury and posthospitalisation care? A single-centre qualitative study from Toronto, Canada. BMJ Open 8:e021418
Switzer GE, Puttarajappa CM, Kane-Gill SL, Fried LF, Abebe KZ, Kellum JA, Jhamb M, Bruce JG, Kuniyil V, Conway PT, Knight R, Murphy J, Palevsky PM (2022) Patient-reported experiences after acute kidney injury across multiple health-related quality-of-life domains. Kidney360 3:426–434
Mayer KP, Ortiz-Soriano VM, Kalantar A, Lambert J, Morris PE, Neyra JA (2022) Acute kidney injury contributes to worse physical and quality of life outcomes in survivors of critical illness. BMC Nephrol 23:137
Pande CK, Smith MB, Soranno DE, Gist KM, Fuhrman DY, Dolan K, Conroy AL, Akcan-Arikan A (2022) The neglected price of pediatric acute kidney injury: non-renal implications. Front Pediatr 10:893993
Myers SR, Glaser NS, Trainor JL, Nigrovic LE, Garro A, Tzimenatos L, Quayle KS, Kwok MY, Rewers A, Stoner MJ, Schunk JE, McManemy JK, Brown KM, DePiero AD, Olsen CS, Casper TC, Ghetti S, Kuppermann N, Pediatric emergency care applied research network (PECARN) DKA FLUID study group (2020) frequency and risk factors of acute kidney injury during diabetic ketoacidosis in children and association with neurocognitive outcomes. JAMA Netw Open 3:e2025481
Conroy AL, Opoka RO, Bangirana P, Idro R, Ssenkusu JM, Datta D, Hodges JS, Morgan C, John CC (2019) Acute kidney injury is associated with impaired cognition and chronic kidney disease in a prospective cohort of children with severe malaria. BMC Med 17:98
Pande CK, Noll L, Afonso N, Serrano F, Monteiro S, Guffey D, Puri K, Achuff BJ, Akcan-Arikan A, Shekerdemian L (2022) Neurodevelopmental outcomes in infants with cardiac surgery associated acute kidney injury. Ann Thorac Surg 114:2347–2354
National Institute for Health and Care Excellence (2019) Acute kidney injury: prevention, detection and management. London: (NICE guideline NG148). https://www.nice.org.uk/guidance/ng148. Accessed 6 Jan 2023
Lewington AJ, Cerda J, Mehta RL (2013) Raising awareness of acute kidney injury: a global perspective of a silent killer. Kidney Int 84:457–467
Lombardi R, Ferreiro A, Rosa-Diez G, Margolis A, Yu L, Younes-Ibrahim M, Burdmann EA, Oeyen F, Douthat W (2018) Raising awareness of acute kidney injury: a Latin American experience. Kidney Int Rep 3:1416–1423
van der Merwe B (2019) Design-based research for the development of a flexible learning environment. Health SA 24:1050
Collins A (1992) Toward a design science of education. Springer, Berlin, Heidelberg, pp 15–22
Koivisto JM, Haavisto E, Niemi H, Haho P, Nylund S, Multisilta J (2018) Design principles for simulation games for learning clinical reasoning: a design-based research approach. Nurse Educ Today 60:114–120
Hege I, Kononowicz AA, Adler M (2017) A clinical reasoning tool for virtual patients: design-based research study. JMIR Med Educ 3:e21
Pronyk PM, Muniz M, Nemser B, Somers MA, McClellan L, Palm CA, Huynh UK, Ben Amor Y, Begashaw B, McArthur JW, Niang A, Sachs SE, Singh P, Teklehaimanot A, Sachs JD, Millennium Villages Study Group (2012) The effect of an integrated multisector model for achieving the Millennium Development Goals and improving child survival in rural sub-Saharan Africa: a non-randomised controlled assessment. Lancet 379:2179–2188
Luyckx VA, Al-Aly Z, Bello AK, Bellorin-Font E, Carlini RG, Fabian J, Garcia-Garcia G, Iyengar A, Sekkarie M, van Biesen W, Ulasi I, Yeates K, Stanifer J (2021) Sustainable development goals relevant to kidney health: an update on progress. Nat Rev Nephrol 17:15–32
Schleiff M, Olateju A, Decker E, Neel AH, Oke R, Peters MA, Rao A, Alonge O (2020) A multi-pronged scoping review approach to understanding the evolving implementation of the Smallpox and Polio eradication programs: what can other Global Health initiatives learn? BMC Public Health 20:1698
Kalbarczyk A, Closser S, Rao A, Akinyemi O, Anwar HB, Mafuta E, Majumdar P, Alonge OO (2021) Translating implementation experiences and lessons learned from polio eradication into a global health course: insights from an International Consortium. Glob Health Sci Pract 9:682–689
Colbert GB, Topf J, Jhaveri KD, Oates T, Rheault MN, Shah S, Hiremath S, Sparks MA (2018) The social media revolution in nephrology education. Kidney Int Rep 3:519–529
Khashu S, Wanchoo N, Finuf KD, Lapman S, Gudsoorkar P, Jhaveri KD (2022) Utility of semi-private messaging application (WhatsApp(R)) for onconephrology education: a qualitative analysis of a ‘mastermind’ chat. Clin Kidney J 15:834–838
Stoneman S, Hiremath S (2020) Twitter-based journal clubs: bringing critical appraisal to the social table. Semin Nephrol 40:264–272
See EJ, Bello AK, Levin A, Lunney M, Osman MA, Ye F, Ashuntantang GE, Bellorin-Font E, Benghanem Gharbi M, Davison S, Ghnaimat M, Harden P, Htay H, Jha V, Kalantar-Zadeh K, Kerr PG, Klarenbach S, Kovesdy CP, Luyckx V, Neuen B, O’Donoghue D, Ossareh S, Perl J, Rashid HU, Rondeau E, Syed S, Sola L, Tchokhonelidze I, Tesar V, Tungsanga K, Kazancioglu RT, Wang AY, Yang CW, Zemchenkov A, Zhao MH, Jager KJ, Caskey F, Perkovic V, Jindal KK, Okpechi IG, Tonelli M, Feehally J, Harris DC, Johnson DW (2021) Availability, coverage, and scope of health information systems for kidney care across world countries and regions. Nephrol Dial Transplant 37:159–167
Lunyera J, Kilonzo K, Lewington A, Yeates K, Finkelstein FO (2016) Acute kidney injury in low-resource settings: barriers to diagnosis, awareness, and treatment and strategies to overcome these barriers. Am J Kidney Dis 67:834–840
McCulloch M, Luyckx VA, Cullis B, Davies SJ, Finkelstein FO, Yap HK, Feehally J, Smoyer WE (2021) Challenges of access to kidney care for children in low-resource settings. Nat Rev Nephrol 17:33–45
Ostermann M, Zarbock A, Goldstein S, Kashani K, Macedo E, Murugan R, Bell M, Forni L, Guzzi L, Joannidis M, Kane-Gill SL, Legrand M, Mehta R, Murray PT, Pickkers P, Plebani M, Prowle J, Ricci Z, Rimmele T, Rosner M, Shaw AD, Kellum JA, Ronco C (2020) Recommendations on acute kidney injury biomarkers from the acute disease quality initiative consensus conference: a consensus statement. JAMA Netw Open 3:e2019209
Batte A, Menon S, Ssenkusu JM, Kiguli S, Kalyesubula R, Lubega J, Berrens Z, Mutebi EI, Ogwang R, Opoka RO, John CC, Conroy AL (2022) Neutrophil gelatinase-associated lipocalin is elevated in children with acute kidney injury and sickle cell anemia, and predicts mortality. Kidney Int 102:885–893
Bjornstad EC, Muronya W, Kamija M, Smith Z, Munthali CK, Gibson K, Mottl AK, Charles A, Marshall SW, Golightly YM, Gower EW (2020) Validity of urine NGALds dipstick for acute kidney injury in a malawian trauma cohort. Kidney Int Rep 5:1791–1798
Wiens MO, Kissoon N, Kabakyenga J (2018) Smart hospital discharges to address a neglected epidemic in sepsis in low- and middle-income countries. JAMA Pediatr 172:213–214
Acknowledgements
The ADQI 26 workgroup: The following individuals contributed to the formulation and content of this work in accordance with their participation in the 26th Acute Disease Quality Initiative (ADQI XXVI).
Chairs:
Ayse Akcan Arikan, MD, Baylor College of Medicine, Department of Pediatrics, Divisions of Critical Care Medicine and Nephrology, Houston, TX, USA.
Rajit K. Basu, MD, MS, Northwestern University Feinberg School of Medicine, Ann & Robert Lurie Children’s Hospital of Chicago, Department of Pediatrics, Division of Critical Care Medicine, Chicago, IL, USA.
Stuart L. Goldstein, MD, Cincinnati Children’s Hospital Medical Center, Department of Pediatrics, Division of Nephrology & Hypertension, Cincinnati, OH, USA.
Rashid Alobaidi1, David J. Askenazi2, Sean M. Bagshaw1, Matthew Barhight3, Erin Barreto4, Benan Bayrakci5, O.N. Ray Bignall II6, Erica Bjornstad2, Patrick Brophy7, Jennifer Charlton8, Rahul Chanchlani9, Andrea L. Conroy10, Akash Deep11, Prasad Devarajan12, Kristin Dolan13, Dana Fuhrman14, Katja M. Gist12, Stephen M. Gorga15, Jason H. Greenberg16, Denise Hasson12, Emma Heydari1, Arpana Iyengar17, Jennifer Jetton18, Catherine Krawczeski6, Leslie Meigs19, Shina Menon20, Catherine Morgan1, Jolyn Morgan12, Theresa Mottes3, Tara Neumayr21, Zaccaria Ricci22, David T. Selewski23, Danielle Soranno10, Natalja Stanski12, Michelle Starr10, Scott M. Sutherland24, Jordan Symons20, Marcelo Tavares25, Molly Vega13, Michael Zappitelli26, Claudio Ronco27, Ravindra L. Mehta28, John Kellum29, and Marlies Ostermann30.
1Alberta Health Sciences University, Edmonton, Alberta, Canada
2University of Alabama at Birmingham, Children’s Hospital of Alabama, Birmingham, AL, USA
3Northwestern University Feinberg School of Medicine, Ann & Robert Lurie Children’s Hospital of Chicago, Chicago, IL, USA
4Hacettepe University, Ankara, Türkiye
5Mayo Clinic, Rochester, MN, USA
6Nationwide Children’s Hospital, Ohio State University, Columbus, OH, USA
7Golisano Children’s Hospital, Rochester University Medical Center, Rochester, NY, USA
8University of Virginia, Charlottesville, VA, USA
9McMaster University, McMaster Children’s Hospital, Hamilton, ON, Canada
10Riley Children’s Hospital, Indiana University School of Medicine, Indianapolis, IN, USA
11King’s College London, King’s College Hospital NHS Foundation Trust, London, UK
12Cincinnati Children’s Hospital Medical Center, Cincinnati, OH, USA
13Texas Children’s Hospital, Baylor College of Medicine, Houston, TX, USA
14Children’s Hospital of Pittsburgh, University of Pittsburgh Medical Center, Pittsburgh, PA, USA
15C.S. Mott Children’s Hospital, University of Michigan, Ann Arbor, MI, USA
16Yale University Medical Center, New Haven, CT, USA
17St. John’s National Academy of Health Sciences, Bangalore, India
18Stead Family Children’s Hospital, University of Iowa, Iowa City, IA, USA
19University of St. Thomas, Houston, TX USA
20Seattle Children’s Hospital, University of Washington, Seattle, WA, USA
21Washington University School of Medicine, St. Louis, MO, USA.
22University of Florence, Florence, Italy
23Medical University of South Carolina, Charleston, SC, USA
24Lucille Packard Children’s Hospital, Stanford University, Palo Alto, CA, USA
25Santa Casa dela Belo Horizonte, Belo Horizonte, Brazil
26Hospital for Sick Children, Toronto, Ontario, Canada
27San Bartolo Hospital, Universita di Padova, Vicenza, Italy
28University of California San Diego School of Medicine, La Jolla, CA, USA
29University of Pittsburgh Medical Center, Pittsburgh, PA, USA
30Guy’s and St. Thomas’ NHS Foundation Trust, London, UK
Funding
For full disclosure, we provide here an additional list of authors’ commitments and funding sources that are not directly related to this study:
Theresa Mottes is a consultant for Baxter, Medtronic.
Shina Menon is a consultant for Nuwellis, and Medtronic. She has grant funding for research that is not related to this project from the Gerber Foundation.
Jennifer Jetton—None.
Andrea Conroy has grant funding from the National Institute of Allergy and Infectious Diseases that is not related to this project.
Kristin Dolan—None.
Jordan Symons—None.
Author information
Authors and Affiliations
Consortia
Corresponding author
Ethics declarations
Conflict of interest
The authors declare no competing interests.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if changes were made. The images or other third party material in this article are included in the article's Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article's Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
Mottes, T., Menon, S., Conroy, A. et al. Pediatric AKI in the real world: changing outcomes through education and advocacy—a report from the 26th Acute Disease Quality Initiative (ADQI) consensus conference. Pediatr Nephrol 39, 1005–1014 (2024). https://doi.org/10.1007/s00467-023-06180-w
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00467-023-06180-w