Abstract
Objectives
This study was aimed at evaluating the clinical and radiological outcomes of novel dynamic navigation (DN)–aided endodontic microsurgery (EMS), with an analysis of potential prognostic factors.
Materials and methods
Forty-six teeth from 32 patients who received DN-aided EMS were included. Clinical and radiographic assessments were performed at least 1 year postoperatively. Two calibrated endodontists assessed radiological outcomes according to two-dimensional (2D) periapical radiography (PA) and three-dimensional (3D) cone-beam computed tomography (CBCT) imaging using Rud’s and Molven’s criteria and modified PENN 3D criteria, respectively. Fisher’s exact test was used for statistical analysis of the predisposing factors.
Results
Of the 32 patients with 46 treated teeth, 28 with 40 teeth were available for follow-up. Of the 28 patients, four (five teeth) refused to undergo CBCT and only underwent clinical and PA examinations, and the remaining 24 (35 teeth) underwent clinical, PA, and CBCT examinations. Combined clinical and radiographic data revealed a 95% (38/40) success rate in 2D healing evaluations and a 94.3% (33/35) success rate in 3D healing evaluations. No significant effect was found in sex, age, tooth type, arch type, preoperative lesion volume, preoperative maximum lesion size, presence/absence of crown and post, and the root canal filling state on the outcome of DN-aided EMS.
Conclusions
DN-aided EMS has a favorable prognosis and could be considered an effective and reliable treatment strategy. Further investigations with larger sample sizes are required to confirm these results.
Clinical relevance
DN-aided EMS could be considered an effective and reliable treatment strategy.
Similar content being viewed by others
Explore related subjects
Discover the latest articles, news and stories from top researchers in related subjects.Avoid common mistakes on your manuscript.
Introduction
As a predictable and reliable resort for treating persistent apical periodontitis, endodontic microsurgery (EMS) has achieved a high success rate of 94% based on evidence-based literature [1]. Resecting a 3-mm root end perpendicular to the long axis of the root could remove 98% of apical ramifications and is indicated for the principle of modern EMS [2]. The experience and perceptual skills of the operator are highly associated with the outcomes of freehand EMS. Operator-related risks, including excessive bone removal, incorrect root-end resection length and bevel, and injury to important anatomical structures, may occur, particularly in anatomically challenging scenarios. To address these problems and achieve predictable outcomes, guided EMS was introduced into the field of endodontics using novel computer-aided treatment methods. The guided methods include static navigation (SN) and dynamic navigation (DN). Several in vitro studies have shown high-accuracy results for SN and DN in guided osteotomy and root-end resection [3, 4]. Guided EMS replaces the carbide or diamond bur with a rotated trephine bur, which is conventionally used for the effective removal of implants and bone graft materials [5]. In guided EMS, the surgical path for osteotomy and root-end resection is designed and performed with sufficient consideration of the principles of modern surgery. SN-aided EMS is achieved using a three-dimensional (3D) printer for template fabrication with sleeves and a coordinated trephine bur. The DN-aided EMS provides real-time visualization and full guidance of the drill through various anatomic structures. The location, angulation, and depth of the surgical path can be optimally determined preoperatively. Compared with freehand EMS, guided EMS presents a more minimized atraumatic access and accurate root-end resection length and bevel.
Periapical radiography (PA) has traditionally been used to evaluate the radiological outcomes of EMS. The criteria established by Rud et al. (1972) and Molven et al. (1987) are used to assess the healing outcome of EMS [6, 7]. However, the overlap of hard and soft tissues with different radiodensities, existing background noise, and geometric distortion is a limitation of PA in detecting periapical lesions [8]. Cone-beam computed tomography (CBCT) acquires views by 3D projection that presents the target anatomical structure in the axial, coronal, and sagittal views. In the field of endodontics, CBCT has been used for endodontic diagnosis, morphological evaluation of the root canal, and preoperative planning in EMS [9]. CBCT can provide an accurate assessment of the location and size of periapical radiolucency and yield a more sensitive and specific result than PA [10, 11]. In 2017, Schloss et al. proposed a detailed evaluation grading of modified PENN 3D criteria for surgical outcome [12].
In the past decade, numerous studies have analyzed prognostic factors for EMS. Several studies have indicated that age [13, 14], sex [13,14,15], tooth location and type [15,16,17,18], lesion size [13, 14, 16], presence of crown and post [19], and root filling quality [13, 17] are potential prognostic factors for EMS. Modern EMS advocates a minimized operation for bone removal and precise root-end resection. Buniag et al. (2021) reported a retrospective study of targeted EMS with SN that yielded a 91.7% success rate [20]. However, the success rate and prognostic factors of DN-aided EMS with trephine have not yet been investigated. Therefore, this study was aimed at investigating the clinical and radiological outcomes of the novel DN-aided EMS. Radiological outcomes were evaluated using PA with Rud’s and Molven’s criteria and CBCT with modified PENN 3D criteria for at least 1 year of follow-up. Potential prognostic factors for the outcome of DN-aided EMS were also analyzed.
Materials and methods
Participant enrollment
This study was approved by the Ethics Committee of School and Hospital of Stomatology, Wuhan University (number 2020–06), and registered with the Chinese Clinical Trial Registry (ChiCTR2100042312). Patients who required EMS were enrolled after informed consent was obtained. All patients were informed of the benefits, risks, and required follow-up assessments. The patients were consecutively treated between November 2020 and January 2022. Follow-up assessments were performed at least 1 year postoperatively. The flow of participants throughout the study is shown in Fig. 1. The inclusion and exclusion criteria were as follows.
Inclusion criteria:
-
Diagnosis of symptomatic/asymptomatic apical periodontitis in previously root canal treated teeth
-
Patients aged 18–59 years
Exclusion criteria:
-
Severe systemic diseases (diabetes, osteoporosis, heart disease, etc.)
-
Pregnant and lactating women
-
Second or third molars
-
Teeth with severe periodontitis
-
Teeth with vertical/horizontal root fracture, perforated root canals, or root resorption
DN-aided EMS workflow
The DN-aided EMS was performed by an experienced endodontist with 8 years of EMS experience and had performed 20-sample guided osteotomy and root-end resection in vitro [21]. The procedures and principles of the EMS were followed the guidelines proposed by Kim and Kratchman [2]. Preoperative PA was performed using an X-ray machine (Planmeca Intra, Helsinki, Finland), exposing the sensors at 60 kVp, 7.0 mA, and exposure time adjusted for the location of the surgical teeth in the dental arch. Preoperative CBCT (Morita, J. Morita, MFG. CORP, Kyoto, Japan) imaging was performed with a thermoplastic device placed on the target tooth of the patient, which embeds nine or 10 radiopaque fiducial markers (Fig. 2a–d). CBCT scanning used the following parameters: tube voltage, 90 kVp; tube current, 7.0 mA; field of view, 80 × 80 mm; and voxel size, 0.16 mm. The DICOM dataset of CBCT was imported into DN software (DHC-ENDO1, DCARER Medical Technology, Suzhou, China) to establish navigation path planning. The drilling entry point, end point, and angle were virtually planned. Calibration and registration process was performed before the osteotomy. Calibration was conducted to match the handpiece-tracking array and the reference device (Fig. 2e). The reference device was fixed to the non-operative area of the dentition (Fig. 2f). Marker-based registration was then performed by completing the matching between the thermoplastic device with 6 radiopaque fiducial markers and the responding area in the 3D reconstruction of the patient’s dentition (Fig. 2f). Full mucoperiosteal flap elevation was used in all cases. Under DN guidance (Fig. 4m), a trephine bur with an outer diameter of 4 mm and a working length of 15.1 mm trephine (818–102, Changsha Tiantian Dental Equipment Co., LTD, Changsha, China) was used to perform the osteotomy and 3 mm of root-end resection. The remaining clinical procedures, including periapical curettage, methylene blue staining, root-end retrograde preparation, retrograde filling with iRoot BP Plus (Innovative Bioceramics, Vancouver, BC, Canada), and sutures, were performed using an endodontic microscope (OPMI PICO; Carl Zeiss, Göttingen, Germany).
Follow-up and outcome assessment
All patients were telephonically requested to attend the follow-up appointments at least 1-year postoperatively. The reason for this loss was recorded if the patient was unable to attend the follow-up. Clinical success was defined as the absence of any signs and/or symptoms, including pain or swelling, tenderness to percussion or palpation, mobility, sinus tract formation, or periodontal pocket. The parameters of PA and CBCT at follow-up were consistent with preoperative values. Paralleling technique was used to achieve the same angle between the sensor and the teeth before and after the EMS. The radiographic evaluations were performed as follows:
-
Two-dimensional (2D) radiographic healing assessment
The 2D radiographic outcomes of periapical films were defined by Rud et al. (1972) and Molven et al. (1987) [6, 7] and classified into four categories: complete healing, incomplete healing, uncertain healing, and unsatisfactory healing (Table 1). Complete healing and incomplete healing were dichotomized as successful radiographic evaluation. Uncertain healing and unsatisfactory healing were dichotomized as failures in the radiographic evaluation.
-
3D radiographic healing assessment
The 3D radiographic outcomes of CBCT imaging were defined using modified PENN 3D criteria [12] and classified into four categories: complete healing, limited healing, uncertain healing, and unsatisfactory healing (Table 1). Complete healing and limited healing were dichotomized as successful radiographic evaluation. Uncertain healing and unsatisfactory healing were dichotomized as failures in the radiographic evaluation.
Outcome designations
All radiographs were assessed independently by two examiners (Observer A, C.C. and Observer B, W.Z.) and the Cohen kappa value for agreement was calculated. Any disagreement regarding the 2D or 3D readings was resolved by discussion until a consensus was reached. Radiographic and clinical data were combined to determine the final outcomes, as follows:
-
Success, clinical success, and radiographic outcome success
-
Failure, clinical failure, and/or radiographic outcome failure
Evaluation factors
Evaluation factors possibly influencing prognosis were divided into patient- and tooth-related factors. Patient-related factors included age and sex. Tooth-related factors included tooth position, arch type, maximum lesion size, preoperative lesion volume, the presence/absence of crowns and posts, and root canal filling state, including the quality of lateral seal and length of root filling [22]. The preoperative volume of periapical radiolucency and preoperative maximum diameter in three orientations, including mesiodistal, apicocoronal, and buccolingual of the apical lesions, were determined using Mimics software (Materialize Mimics 21, Leuven, Belgium).
Statistical analysis
The kappa test was used to calculate the inter-observer and intra-observer reliability amongst the four healing categories. Regarding the intra-observer reliability, the second assessment was carried out by the same examiner 1 month after the initial assessment. For the statistical analysis, the dichotomous outcome of success or failure was used as the dependent variable. The Fisher exact test was used to confirm the presence of significant prognostic factors. All statistical analyses were conducted using SPSS Statistics version 27 (IBM Corp. Released 2020, Armonk, NY, USA). A value of P < 0.05 was considered statistically significant.
Results
In the 2D analysis, the intra-observer agreement results were substantial agreement (K = 0.73) for Observer A and substantial agreement (K = 0.74) for Observer B. In the 3D analysis, the intra-observer agreement results were perfect agreement (K = 0.95) for Observer A and perfect agreement (K = 0.89) for Observer B. Regarding the inter-observer reliability, the 2D and 3D analysis showed a substantial agreement (K = 0.79) and perfect agreement (K = 0.95), respectively.
After assessment and enrollment, a total of 46 treated teeth in 32 patients (14 men and 18 women) received DN-aided EMS and included in the study. Forty teeth from 28 patients were available for follow-up. The recall rate was 87.5% (28/32) for patients and 87% (40/46) for teeth. Four patients dropped out for the following reasons: two patients were pregnant, one relocated to another city and could not participate in the follow-up, and one could no longer be contacted.
Of the 28 patients, 13 were men and 15 were women with a mean age of 31.4 years. Of the 40 teeth, 32 were in the maxilla and 8 were in the mandible, including 29 anterior and 11 posterior teeth. The follow-up occurred between 12 and 20 months after surgery. The mean follow-up duration was 13 months. Four patients with five teeth who underwent clinical examination and PA refused CBCT. Finally, 28 patients with 40 teeth underwent clinical and PA examinations, and 24 with 35 teeth underwent clinical, PA, and CBCT examinations (Fig. 1).
At the follow-up appointment, two teeth of two patients exhibited signs of a sinus tract and unsatisfactory healing on radiological examination. No signs or symptoms were observed in the remaining teeth. The characteristics of the included DN-aided EMS cases with follow-up time are demonstrated in Table 2. The healing outcomes of PA and CBCT are summarized in Table 3. Combined clinical and radiographic data demonstrated that the success rates of DN-aided EMS were 95% (38/40) and 94.3% (33/35), as assessed using PA and CBCT, respectively. Representative anterior and posterior cases are shown in Figs. 3 and 4, respectively. The distribution and analysis of the cases per variable category are summarized in Table 4. No factor listed in Table 4 was associated with significant differences.
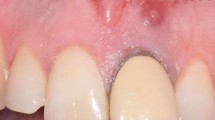
Typical anterior dynamic navigation (DN)–aided endodontic microsurgery case in tooth 13. a Preoperative photograph; the black arrow indicates the sinus tract. b Preoperative radiograph. c–e Preoperative coronal, sagittal, and axial cone-beam computed tomography (CBCT) sections and measurement. f–h Surgical path planning in DN software of coronal, axial, and sagittal view, respectively. i Three-dimensional view of surgical path planning in DN software. j Incision. k Flap elevation. l Diameter of osteotomy. m Methylene blue staining. n Retrograde preparation. o Retrograde filling. p Immediate postoperative radiograph. q One-year follow-up radiograph. r–t One-year follow-up CBCT of coronal, sagittal, and axial view
Typical posterior dynamic navigation (DN)–aided endodontic microsurgery case in tooth 46. a Preoperative photograph; the black arrow indicates the sinus tract. b Preoperative radiograph. c–e Preoperative sagittal, coronal, and axial cone-beam computed tomography (CBCT) sections and measurement. f–h Surgical path planning in DN software of coronal, axial, and sagittal view, respectively. i Three-dimensional view of surgical path planning in DN software. j Registration. k Incision. l Flap elevation. m Real-time views in the screen of DN system. n After guided osteotomies and root-end resections. o, p Retrograde preparation of mesial and distal root, respectively; black arrows indicate the root resection plane. q Retrograde filling. r Immediate postoperative radiograph. s One-year follow-up radiograph. t–v One-year follow-up CBCT of sagittal, coronal, and axial view
Discussion
This prospective study was aimed at evaluating the 1-year clinical and radiological outcomes and potential prognostic factors of novel navigation-guided EMS. The concept of guided endodontic surgery, including SN and DN technology, overcame the challenges of free-hand EMS up to an extent and allowed for a more appropriate length and bevel for root-end resection. Of all the published in vivo SN and DN endodontic surgery studies, except for one retrospective study, all were case report/series with favorable clinical and radiological outcomes (Table 5). To our knowledge, this is the first prospective study to investigate the prognosis of DN-aided EMS. As healing mainly happened within 1 year postoperatively, a 1-year follow-up is considered a feasible indicator of the final prognosis outcome [23]. In this study, a mean follow-up period of 13 months was deemed adequate for the analysis of the clinical and radiographic assessments. The success rates of DN-aided EMS 1 year postoperatively in PA and CBCT were both more than 94.3%, which is similar to the freehand EMS study [1].
Although histology is considered the gold standard for the evaluation of periapical healing, it is ethically forbidden to obtain tissue cores from patients at follow-up. Previous animal studies have shown that CBCT provides a similar result to histology in healing outcome [24, 25]. In addition, some studies reported 27–33% disagreement on the diagnosis between PA and CBCT in the follow-up images [8, 26, 27], as CBCT presents lesion changes in the cortical plate and trabecular bone more accurately. The present study also demonstrated differences in the outcomes between these two radiographic methods. In the present study, eight teeth taken for complete healing based on the 2D classification fell into the category of limited healing patterns in the PENN 3D criteria, and two teeth taken for incomplete healing based on the 2D classification fell into the category of uncertain healing in the PENN 3D criteria. CBCT demonstrated more radiographic defects in 3D views and resulted in a lower healing rate than PA [28]. These defects are not always associated with clinical failure but might indicate incomplete or defective healing in radiological outcomes [29]. A longer follow-up period is needed for a more reliable assessment of these controversial radiological outcomes.
At the 1-year follow-up, two patients exhibited both clinical and radiological failures. Failure occurred in tooth 11 in a 34-year-old woman and tooth 26 in a 24-year-old man (Table 2). After root-end resection and methylene blue staining, these two teeth were found to be suffered from apical dentin microfractures, one of which occurred in the palatal side of the resected root and the other occurred in the mesial side of the resected palatal root. Otterson et al. (2020) illustrated that, compared to freehand EMS, targeted EMS with trephine does not increase the risk of dentinal microcracks [30]. Some studies have illustrated that the development of dentinal microfractures in endodontically treated teeth is directly associated with shaping, cleaning, and filling procedures [31,32,33]. Moreover, Arias et al. (2021) reported that mastication and other functions of the patient are important factors in the presence of cracks [34]. Although the cracked dentine was eliminated by further resection of the root during surgery, microcracks may exist and can be further prolong. In addition, the factors of occlusal force and mastication performance of the patient still existed and might have led to the progressive development of microcracks, compromising healing. In the present study, four patients refused to undergo CBCT after receiving clinical and PA examinations. Of these four patients, two with two teeth were diagnosed with unsatisfactory healing by PA, as previously described. Therefore, we reasonably speculate that the actual CBCT success rate was lower than the current rate of 94.3%, which is a limitation of this study.
Previous freehand EMS studies have reported that tooth and arch types are important factors influencing success rates [15,16,17,18]. The low success rate of posterior and mandibular teeth may result from anatomical obstacles in visualization and access during osteotomy and root-end resection. In addition, altered sensation, associated with the injury of mental and inferior alveolar nerves, may happen after EMS procedures. The long-term or permanent altered sensation can have a serious impact on patient’s quality of life and even attribute to medicolegal consequences. A previous study reported a 14% incidence of altered sensation after mandibular premolar-molar surgery [35]. In the present study, six mandibular molar cases and one mandibular premolar case were included and no intraoperative complications occurred. Technically challenging cases, including the palatal root of the maxillary first molar, maxillary molar root adjacent to the maxillary sinus, the curve distal root of the mandibular first molar, maxillary and mandibular premolars, and root tip in approximation to the mental nerve, were included in this study (Table 2). However, some of these complexities may have precluded treatment with freehand EMS and are associated with the risk of complications, leading to a decrease in success rate. In our study, no significant differences were found between the arch types (maxilla versus mandible) and tooth types (anterior and posterior). The present study indicates that guided EMS is particularly beneficial in complex cases with thick cortical plates, limited access, and poor visualization.
The advantages of DN-aided EMS can be summarized as follows. First, for the clinician, the main advantage of the use of DN is the possibility of performing the surgical path optimally as designed and avoiding the incidence of iatrogenic errors. Second, excessive osteotomy may occur inadvertently in anatomically complex scenarios of free-hand EMS, particularly in posterior dental arch location. In our study, the diameter of surgical approach of minimal osteotomy with trephine was restricted to 4 mm in all cases. With the development of guided EMS, the conception of patient-centered orientation in minimally invasive operations may be further refined. Third, DN allows the modification of the original surgical path intraoperatively if needed, which is not possible in static guides. Finally, in DN-aided EMS with trephine bur, the cortical plate, cancellous bone, granulomatous tissue, and root tip could be removed simultaneously. Simplification of surgical procedures through DN-aided EMS improves clinical efficiency and may increase the clinical prevalence of EMS overall.
There are certain limitations associated with the DN-aided EMS method. Firstly, the cross-section of the root created by the surgical trephine is not flattened and appears as a curved shape, with the level and bevel of the curved edge determined by the surgical path and diameter of the trephine bur. This can lead to stress concentration on the root-end aspect, which may cause cemental tears over time and affect prognosis, as demonstrated by a finite element analysis investigation [36]. To address this issue, the curved edge is removed using a high-speed handpiece with a diamond or ET18D ultrasonic tip in the present cases. Additionally, the preoperative guided procedures of calibration and registration are complicated and time-consuming. However, this is offset by the reduction in intraoperative time during osteotomy and root-end resection. It is important to note that the DN requires a learning curve to develop a stable and consistent workflow and reduce operator-induced errors. In a previous study, it was recommended that operators practice on 20 or more in vitro samples to eliminate the influence of the learning curve [37]. In the present study, the operator practiced on 20 samples in vitro before operating on patients to achieve proficiency in DN [21]. Finally, the obscuration of the patient’s lips and cheeks, particularly in posterior areas, may prevent the use of trephine to facilitate access in the planned position and angle. Therefore, we proposed the conception of fully guided and half-guided navigation approaches in EMS. In the fully guided approach, DN guides the entire drilling process from the osteotomy to the root-end resection according to the planned position and angle. In contrast, in the half-guided approach, only 1–2-mm osteotomy deep into the bone is performed according to the programming position but not angle, which can assist the clinician in locating the position of the apex. The remaining drilling is then performed by the high-speed handpiece with a diamond.
The lack of a control group is a limitation of this single-cohort study. A further limitation is the relatively small sample size, as this was a single-center study. This may lead to a false-negative result when confirming the significant prognostic factors, and the results should be interpreted with caution. Despite these limitations, the present study provided preliminary and inductive conclusions of the outcome of DN-aided EMS. Further studies with larger sample sizes and randomized controlled trials should be conducted to draw more specific conclusions on the validity and effectiveness of this novel technique.
Conclusion
In conclusion, the success rate of DN-aided EMS 1 year postoperatively was 95% in 2D healing classifications and 94.3% in 3D healing classifications, which is similar to that of evidence-based freehand EMS studies. Sex, age, tooth type, arch type, preoperative lesion volume, preoperative maximum lesion size, presence/absence of crown, post, and root canal filling state did not affect the success rate of DN-aided EMS. The presented novel DN approach appears to be a predictable and clinically feasible method to assist EMS in guided osteotomy and root-end resection.
Data Availability
Data to perform these studies are available after a justified request to the authors.
References
Setzer FC, Shah SB, Kohli MR, Karabucak B, Kim S (2010) Outcome of endodontic surgery: a meta-analysis of the literature–part 1: comparison of traditional root-end surgery and endodontic microsurgery. J Endod 36:1757–1765
Kim S, Kratchman S (2006) Modern endodontic surgery concepts and practice: a review. J Endod 32:601–623
Dianat O, Nosrat A, Mostoufi B, Price JB, Gupta S, Martinho FC (2021) Accuracy and efficiency of guided root-end resection using a dynamic navigation system: a human cadaver study. Int Endod J 54:793–801
Perez C, Sayeh A, Etienne O, Gros CI, Mark A, Couvrechel C, Meyer F (2021) Microguided endodontics: accuracy evaluation for access through intraroot fibre-post. Aust Endod J 47:592–598
Solderer A, Al-Jazrawi A, Sahrmann P, Jung R, Attin T, Schmidlin PR (2019) Removal of failed dental implants revisited: questions and answers. Clin Exp Dent Res 5:712–724
Rud J, Andreasen JO, Jensen JE (1972) Radiographic criteria for the assessment of healing after endodontic surgery. Int J Oral Surg 1:195–214
Molven O, Halse A, Grung B (1987) Observer strategy and the radiographic classification of healing after endodontic surgery. Int J Oral Maxillofac Surg 16:432–439
Ramis-Alario A, Tarazona-Álvarez B, Peñarrocha-Diago M, Soto-Peñaloza D, Peñarrocha-Diago M, Peñarrocha-Oltra D (2021) Is periapical surgery follow-up with only two-dimensional radiographs reliable? A retrospective cohort type sensitivity study. Med Oral Patol Oral Cir Bucal 26:e711–e718
Setzer FC, Lee SM (2021) Radiology in Endodontics. Dent Clin North Am 65:475–486
Patel S, Dawood A, Mannocci F, Wilson R, Pitt Ford T (2009) Detection of periapical bone defects in human jaws using cone beam computed tomography and intraoral radiography. Int Endod J 42:507–515
Curtis DM, VanderWeele RA, Ray JJ, Wealleans JA (2018) Clinician-centered outcomes assessment of retreatment and endodontic microsurgery using cone-beam computed tomographic volumetric analysis. J Endod 44:1251–1256
Schloss T, Sonntag D, Kohli MR, Setzer FC (2017) A comparison of 2- and 3-dimensional healing assessment after endodontic surgery using cone-beam computed tomographic volumes or periapical radiographs. J Endod 43:1072–1079
Liao WC, Lee YL, Tsai YL, Lin HJ, Chang MC, Chang SF, Chang SH, Jeng JH (2019) Outcome assessment of apical surgery: a study of 234 teeth. J Formos Med Assoc 118:1055–1061
Kreisler M, Gockel R, Aubell-Falkenberg S, Kreisler T, Weihe C, Filippi A, Kühl S, Schütz S, d’Hoedt B, Clinical outcome in periradicular surgery (2013) effect of patient- and tooth-related factors–a multicenter study. Quintessence Int 44:53–60
Song M, Kim SG, Lee SJ, Kim B, Kim E (2013) Prognostic factors of clinical outcomes in endodontic microsurgery: a prospective study. J Endod 39:1491–1497
Pallarés-Serrano A, Glera-Suarez P, Tarazona-Alvarez B, Peñarrocha-Diago M, Peñarrocha-Diago M, Peñarrocha-Oltra D, Prognostic factors after endodontic microsurgery (2021) a retrospective study of 111 cases with 5 to 9 years of follow-up. J Endod 47:397–403
Huang S, Chen NN, Yu VSH, Lim HA, Lui JN (2020) Long-term success and survival of endodontic microsurgery. J Endod 46:149-157.e144
von Arx T, Jensen SS, Janner SFM, Hänni S, Bornstein MM (2019) A 10-year follow-up study of 119 teeth treated with apical surgery and root-end filling with mineral trioxide aggregate. J Endod 45:394–401
von Arx T, Jensen SS, Hänni S, Friedman S (2012) Five-year longitudinal assessment of the prognosis of apical microsurgery. J Endod 38:570–579
Buniag AG, Pratt AM, Ray JJ (2021) Targeted endodontic microsurgery: a retrospective outcomes assessment of 24 cases. J Endod 47:762–769
Chen C, Wang FS, Zhang R, Bian Z, Meng L (2022) An in vitro model study of computer-guided endodontic microsurgery. Chin J Stomatol 57:44–51
Kirkevang LL, Ørstavik D, Hörsted-Bindslev P, Wenzel A (2000) Periapical status and quality of root fillings and coronal restorations in a Danish population. Int Endod J 33:509–515
Halse A, Molven O, Grung B (1991) Follow-up after periapical surgery: the value of the one-year control. Endod Dent Traumatol 7:246–250
Chen I, Karabucak B, Wang C, Wang HG, Koyama E, Kohli MR, Nah HD, Kim S (2015) Healing after root-end microsurgery by using mineral trioxide aggregate and a new calcium silicate-based bioceramic material as root-end filling materials in dogs. J Endod 41:389–399
Paula-Silva FW, Santamaria M Jr, Leonardo MR, Consolaro A, da Silva LA (2009) Cone-beam computerized tomographic, radiographic, and histologic evaluation of periapical repair in dogs’ post-endodontic treatment. Oral Surg Oral Med Oral Pathol Oral Radiol Endod 108:796–805
Christiansen R, Kirkevang LL, Gotfredsen E, Wenzel A (2009) Periapical radiography and cone beam computed tomography for assessment of the periapical bone defect 1 week and 12 months after root-end resection. Dentomaxillofac Radiol 38:531–536
Kruse C, Spin-Neto R, Reibel J, Wenzel A, Kirkevang LL (2017) Diagnostic validity of periapical radiography and CBCT for assessing periapical lesions that persist after endodontic surgery. Dentomaxillofac Radiol 46:20170210
von Arx T, Janner SF, Hänni S, Bornstein MM (2016) Agreement between 2D and 3D radiographic outcome assessment one year after periapical surgery. Int Endod J 49:915–925
Azim AA, Albanyan H, Azim KA, Piasecki L (2021) The Buffalo study: outcome and associated predictors in endodontic microsurgery- a cohort study. Int Endod J 54:301–318
Otterson SW, Dutner JM, Phillips MB, Sidow SJ (2020) Surface integrity of root ends following apical resection with targeted trephine burs. G Ital Endod 34:60–66
Mohamed R, Majid S, Faiza A (2021) Root microcracks formation during root canal instrumentation using reciprocating and rotary files. J Contemp Dent Pract 22:259–263
Braun A, Hagelauer FJ, Wenzler J, Heimer M, Frankenberger R, Stein S (2018) Microcrack analysis of dental hard tissue after root canal irradiation with a 970-nm diode laser. Photomed Laser Surg 36:621–628
Vieira MLO, Dantas HV, de Sousa FB, Salazar-Silva JR, Silva E, Batista AUD, Lima TFR (2020) Morphologic changes of apical foramen and microcrack formation after foraminal enlargement: a scanning electron microscopic and micro-computed tomographic analysis. J Endod 46:1726–1732
Arias A, Lee YH, Peters CI, Gluskin AH, Peters OA (2014) Comparison of 2 canal preparation techniques in the induction of microcracks: a pilot study with cadaver mandibles. J Endod 40:982–985
Mainkar A, Zhu Q, Safavi K (2020) Incidence of altered sensation after mandibular premolar and molar periapical surgery. J Endod 46:29–33
Yoo YJ, Perinpanayagam H, Kim M, Zhu Q, Baek SH, Kwon HB, Kum KY (2022) Stress distribution on trephine-resected root-end in targeted endodontic microsurgery: a finite element analysis. J Endod 48:1517-1525.e1511
Golob Deeb J, Bencharit S, Carrico CK, Lukic M, Hawkins D, Rener-Sitar K, Deeb GR (2019) Exploring training dental implant placement using computer-guided implant navigation system for predoctoral students: a pilot study. Eur J Dent Educ 23:415–423
Lu YJ, Chiu LH, Tsai LY, Fang CY (2022) Dynamic navigation optimizes endodontic microsurgery in an anatomically challenging area. J Dent Sci 17:580–582
Fu W, Chen C, Bian Z, Meng L (2022) Endodontic microsurgery of posterior teeth with the assistance of dynamic navigation technology: a report of three cases. J Endod 48:943–950
Gambarini G, Galli M, Stefanelli LV (2019) Endodontic microsurgery using dynamic navigation system: a case report. J Endod 45:1397-1402.e1396
Chaves GS, Capeletti LR, Miguel JG, Loureiro MAZ, Silva E, Decurcio DA (2022) A novel simplified workflow for guided endodontic surgery in mandibular molars with a thick buccal bone plate: a case report. J Endod 48:930–935
Benjamin G, Ather A, Bueno MR, Estrela C (2021) Diogenes A. Preserving the neurovascular bundle in targeted endodontic microsurgery: a case series. J Endod 47:509–519
Kim U, Kim S, Kim E (2020) The application of “bone window technique” using piezoelectric saws and a CAD/CAM-guided surgical stent in endodontic microsurgery on a mandibular molar case. Restor Dent Endod 45:e27
Popowicz W, Palatyńska-Ulatowska A, Kohli MR (2019) Targeted endodontic microsurgery: computed tomography-based guided stent approach with platelet-rich fibrin graft: a report of 2 cases. J Endod 45:1535–1542
Giacomino CM, Ray JJ, Wealleans JA (2018) Targeted endodontic microsurgery: a novel approach to anatomically challenging scenarios using 3-dimensional-printed guides and trephine burs-a report of 3 cases. J Endod 44:671–677
Antal M, Nagy E, Braunitzer G, Fráter M, Piffkó J (2018) Accuracy and clinical safety of guided root end resection with a trephine: a case series. HEAD FACE MED 15:30
Ye S, Zhao S, Wang W, Jiang Q, Yang X (2018) A novel method for periapical microsurgery with the aid of 3D technology: a case report. BMC Oral Health 18:85
Ahn SY, Kim NH, Kim S, Karabucak B, Kim E (2018) Computer-aided design/computer-aided manufacturing-guided endodontic surgery: guided osteotomy and apex localization in a mandibular molar with a thick buccal bone plate. J Endod 44:665–670
Strbac GD, Schnappauf A, Giannis K, Moritz A, Ulm C (2017) Guided modern endodontic surgery: a novel approach for guided osteotomy and root resection. J Endod 43:496–501
Liu YF, Liao WQ, Jin GS, Yang QS, Peng W (2014) Additive manufacturing and digital design assisted precise apicoectomy: a case study. Rapid Prototyp J 20:33–40
Funding
This study was funded by grants (no. 81870761, 82071107) from the General Program of National Natural Scientific Foundation of China and grant (no. 2022020801010498) from Wuhan Special Project on Knowledge Innovation.
Author information
Authors and Affiliations
Contributions
Chen Chen: methodology, validation, resources, methodology, data curation, investigation, formal analysis, and writing original draft.
Rui Zhang: resources, methodology, validation, writing, review, and editing.
Wei Zhang: resources.
Zan Wang: data curation.
Li Qin: data curation.
Fangzhe Li: data curation.
Yun Chen: software support.
Zhuan Bian: conceptualization and resources.
Liuyan Meng: conceptualization, resources, writing, review, editing, supervision, project administration, and funding acquisition.
Corresponding author
Ethics declarations
Ethical approval
All procedures performed in studies involving human participants were in accordance with the ethical standards of the institutional research committee and with the 1964 Helsinki declaration and its later amendments or comparable ethical standards. This study was approved by the Ethics Committee of School and Hospital of Stomatology, Wuhan University (number 2020–06).
Research involving human participants and/or animals
This research involves human participants.
Informed consent
Informed consent was obtained from all individual participants included in the study.
Conflict of interest
The authors declare that they have no conflict of interest.
Additional information
Publisher's note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if changes were made. The images or other third party material in this article are included in the article's Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article's Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
Chen, C., Zhang, R., Zhang, W. et al. Clinical and radiological outcomes of dynamic navigation in endodontic microsurgery: a prospective study. Clin Oral Invest 27, 5317–5329 (2023). https://doi.org/10.1007/s00784-023-05152-6
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00784-023-05152-6