Abstract
Background
Previous studies suggest that dietary vitamin C is inversely associated with gastric cancer (GC), but most of them did not consider intake of fruit and vegetables. Thus, we aimed to evaluate this association within the Stomach cancer Pooling (StoP) Project, a consortium of epidemiological studies on GC.
Methods
Fourteen case–control studies were included in the analysis (5362 cases, 11,497 controls). We estimated odds ratios (ORs) and corresponding 95% confidence intervals (CIs) for the association between dietary intake of vitamin C and GC, adjusted for relevant confounders and for intake of fruit and vegetables. The dose–response relationship was evaluated using mixed-effects logistic models with second-order fractional polynomials.
Results
Individuals in the highest quartile of dietary vitamin C intake had reduced odds of GC compared with those in the lowest quartile (OR: 0.64; 95% CI: 0.58, 0.72). Additional adjustment for fruit and vegetables intake led to an OR of 0.85 (95% CI: 0.73, 0.98). A significant inverse association was observed for noncardia GC, as well as for both intestinal and diffuse types of the disease. The results of the dose–response analysis showed decreasing ORs of GC up to 150–200 mg/day of vitamin C (OR: 0.54; 95% CI: 0.41, 0.71), whereas ORs for higher intakes were close to 1.0.
Conclusions
The findings of our pooled study suggest that vitamin C is inversely associated with GC, with a potentially beneficial effect also for intakes above the currently recommended daily intake (90 mg for men and 75 mg for women).
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Gastric cancer (GC) is currently the fifth most common cancer type and the fourth leading cause of cancer death worldwide, with an estimated 1.1 million new cases and 770,000 deaths in 2020 [1]. Although incidence rates have been declining over recent decades [1, 2], an increase in incidence among adults younger than 50 years has been reported in several populations [3], and it has been suggested that the overall burden of GC will increase in the future, reaching around 1.8 million new cases and 1.3 million deaths per year by 2040 [4].
Among the factors which may influence GC risk, diet could play a relevant role [5, 6]. A recent umbrella review evaluating the effect of 147 unique diet-related exposures on GC risk did not find strong evidence for any of the investigated associations [7]. When considering evidence from prospective primary studies only, suggestive positive associations were reported for heavy alcohol consumption, salted fish consumption, and waist circumference, while a suggestive inverse association was observed for a healthy lifestyle score [7]. Additionally, intake of fruit and vegetables might influence GC risk, likely through their content in antioxidants including some vitamins [7]. Among them is vitamin C (ascorbic acid), which is a water-soluble vitamin that can be found in citrus and other fruits and vegetables. Vitamin C is an essential nutrient in humans and is involved in the regulation of a number of biological mechanisms, including iron metabolism, collagen and carnitine synthesis, catabolism of tyrosine and demethylation of proteins, DNA and RNA, and it also exerts both antioxidant and pro-oxidant activity at micromolar and millimolar concentrations, respectively [8]. Vitamin C might have antineoplastic effects in the stomach by reducing oxidative stress and subsequent cellular and DNA damage [9], inhibiting the formation of N-nitroso compounds and other carcinogens [10, 11], and potentially interfering with Helicobacter pylori infection, which is recognized as the main risk factor for GC [6, 12].
Pooled estimates from recent meta-analyses of observational studies seem to confirm an inverse association between dietary vitamin C and GC risk [13,14,15]. However, most of the studies included in these meta-analyses did not adjust for participants’ intake of fruit and vegetables [13,14,15], which could thus explain observed associations through the effect of other nutrients and antioxidants, considered either individually or jointly. Also, the current evidence on dietary vitamin C and GC was considered too limited by the World Cancer Research Fund to draw a conclusion in its 2018 report [11]. Together with the lack of adjustment for intake of fruit and vegetables in previous epidemiological studies [13,14,15], the number of those conducted so far reporting detailed results according to GC subsites and, especially, histological types, is limited [13, 14]. Furthermore, potential interactions between intake of vitamin C and risk factors for GC, such as tobacco smoking, alcohol drinking, and H. pylori infection, have not been thoroughly investigated [16].
We evaluated the association between dietary intake of vitamin C and GC accounting also for the potential confounding effect of fruit and vegetable consumption, as well as the occurrence of potential interactions between vitamin C and other factors, within the Stomach cancer Pooling (StoP) Project, an international consortium of epidemiological studies on GC [17].
Materials and methods
For the present analysis, version 3.2 of the StoP dataset was used, which includes 34 case–control or nested case–control studies totaling 13,121 GC cases and 31,420 controls. The StoP Project was established in 2012 as an international collaborative effort with the aim to elucidate determinants of risk and outcome of GC [17]. Data harmonization of core variables, such as those related to sociodemographic and some lifestyle factors, was carried out at the Coordinating Center in Milan, Italy after research teams shared the data from their previously conducted case–control or nested case–control studies.
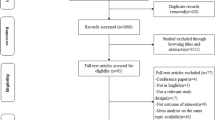
Fourteen studies participating in the StoP Project had available information on dietary intake of vitamin C and total energy intake and were thus included in this analysis (5362 cases, 11,497 controls [the flowchart describing the inclusion of study participants is reported in Supplementary Fig. 1]). Among them, seven were from Europe (two from Italy [18, 19], two from Spain [20, 21], and one each from Greece [22], Russia [23], and Portugal [24]), three from Asia (one each from China [25], Japan [26], and Iran [27]), and four from America (one from the USA [28] and three from Mexico [29,30,31]). Of the studies included in the analysis, eight were community-based [19, 20, 24, 25, 27,28,29,30] and six were clinic-based [18, 21,22,23, 26, 31] (Supplementary Table 1).
The participating studies were conducted in accordance with applicable laws, regulations and guidelines for the protection of human subjects. Furthermore, the StoP Project was approved by the University of Milan Review Board (reference 19/15, April 1, 2015).
Outcome and exposure assessment
In this analysis, cases were individuals with histologically confirmed GC. Information about histological type (intestinal, diffuse, other, the latter including mixed, undifferentiated, and unclassified type) and subsite (cardia, noncardia) of GC was available for ten [18,19,20,21, 23, 24, 27,28,29, 31] and eleven [18,19,20,21,22,23,24, 26,27,28,29] studies, respectively.
Within each study, participants’ intake of vitamin C (mg/day) was computed from food-frequency questionnaires (FFQs) using country-specific food composition tables. Subsequently, based on the study-specific distribution of intake among controls, dietary vitamin C was categorized into quartiles. Intake of vitamin C from supplements was excluded from the analysis since information on supplements was available only for four studies (Russia [23], China [25], Portugal [24], and Japan [26]) among those with available data on dietary vitamin C intake, with variable degree of detail on the specific type of supplement taken and with very limited data on the dose.
In each study, structured questionnaires were used to collect information on participants’ sociodemographic and lifestyle characteristics.
Statistical analysis
We estimated odds ratios (ORs) and corresponding 95% confidence intervals (CIs) for the association between dietary intake of vitamin C and GC using mixed-effects logistic models, with a random intercept for each study. Model 1 was adjusted for sex (male, female), age (≤ 40 years, 41–50 years, 51–60 years, 61–70 years, > 70 years), socioeconomic status (low, intermediate, or high, according to study-specific definitions based on education, income, or occupation), tobacco smoking status (never, former, current), alcohol drinking status (never, ever), and total energy intake (continuous). Model 2 was adjusted for the same set of covariates as model 1 and, additionally, for body mass index (BMI: underweight [< 18.5 kg/m2], normal weight [18.5–24.9 kg/m2], overweight [25–29.9 kg/m2], obese [≥ 30 kg/m2]) and intake of fruit and vegetables (low, intermediate, high, according to study-specific tertiles). Model 3 included the same covariates as model 2 and individuals in the highest and lowest 1% of vitamin C intake were excluded from the analysis. Model 4 was the same as model 2, except for total energy intake being modelled using a second-order fractional polynomial [32]. For all models, missing values of covariates were coded as a separate category for categorical variables, or replaced with the study-specific median values among controls together with dummy variables indicating replacements for continuous variables. Linear trends were assessed in similar models with intake of vitamin C in quartiles considered as a continuous variable. Additionally, for both the point estimate of the OR and the limit of its 95% CI closer to unity, we computed the E-value, which represents the minimum strength of association that an unmeasured confounder should have with both the exposure and the outcome to fully explain away the observed association between the exposure and the outcome, conditional on measured confounders [33].
Moreover, we stratified results according to the following: subsite (cardia, noncardia), histological type (intestinal, diffuse, other), type of study (clinic-based, community-based), sex (male, female), age (≤ 60 years, > 60 years), socioeconomic status (low, intermediate, high), BMI (underweight, normal weight, overweight, obese), smoking status (never, former, current), drinking status (never, ever), H. pylori seropositivity (negative, positive), and intake of fruit and vegetables (low, intermediate, high, according to study-specific tertiles). Data about H. pylori seropositivity were available for seven studies, and in four of them, it was assessed through enzyme-linked immunosorbent assay (ELISA) [23, 26, 29, 31], in one using multiplex serology [20], and in two with both ELISA and Western blot testing [24, 27]. Furthermore, we performed a sensitivity analysis by comparing all cases to seropositive controls, assuming that H. pylori infection be a necessary cause of GC, regardless of results of serological tests [17, 34]. Stratified analyses were adjusted for sex, age, socioeconomic status, tobacco smoking status, alcohol drinking status, BMI, intake of fruit and vegetables, and total energy intake. We tested for heterogeneity across strata using likelihood ratio tests comparing the models including the interaction terms between quartiles of vitamin C intake and the stratification variable with those excluding them.
Furthermore, we evaluated potential additive interactions between dietary vitamin C (higher vs. lower than the study-specific median intake among controls) and the following variables: age (≤ 60 years, > 60 years), sex (female, male), socioeconomic status (high, low/intermediate), tobacco smoking status (non-current, current), alcohol drinking status (never, ever), BMI (overweight/obese, normal weight), H. pylori seropositivity (negative, positive), intake of fruit and vegetables (high, intermediate/low), and intake of salt (low, intermediate/high). To this aim, we estimated the relative excess risk due to interaction (RERI) and the attributable proportion (AP) due to interaction and computed their 95% CI using the delta method [35, 36], after recoding variables of interest to use the stratum with the lowest OR of GC when both factors were considered jointly as the reference category [37].
Additionally, we assessed the dose–response relationship between dietary intake of vitamin C and GC with similar logistic mixed-effects models. We assessed its linearity by treating dietary vitamin C as a continuous variable in the model, and nonlinearity with first- and second-order fractional polynomials. We ran two different models adjusted for the same covariates as model 1 and model 2 described above for the main analysis, and in both cases we excluded from the analysis individuals in the lowest and in the highest 1% of intake of vitamin C. The model considered as the best fitting was the one with the lowest deviance [32].
All analyses were carried out using Stata software version 17 (StataCorp LLC. College Station. TX).
Results
Study participants’ characteristics are reported in Table 1 and Supplementary Table 2. More cases were male (61.88% vs. 54.64%), older than 60 years (63.37% vs. 57.87%), and had low socioeconomic status (57.29% vs. 45.66%) compared with controls. In addition, a higher proportion of cases than controls were obese (21.34% vs. 19.06%), current smokers (26.58% vs. 24.14%), and ever drinkers (64.85 vs. 63.29%). Similarly, H. pylori seropositivity (63.82% vs. 61.86%) was more common among cases than among controls when considering only participants from the seven studies with available information [20, 23, 24, 26, 27, 29, 31]. A larger proportion of controls reported high intake of fruit and vegetables compared with cases. Most cases were of noncardia (57.03%) and intestinal type GC (33.01%). Cases had a lower median intake of vitamin C and fewer of them were in the highest quartiles of intake compared with controls (Table 1).
Estimates of the association between dietary vitamin C and GC are reported in Table 2. The ORs were 0.78 (95% CI: 0.71, 0.86) in quartile 2, 0.69 (95% CI: 0.62, 0.76) in quartile 3 and 0.64 (95% CI: 0.58, 0.72) in quartile 4 of intake compared with quartile 1. However, when additionally adjusting for BMI and intake of fruit and vegetables, the observed association was attenuated and the OR for the highest versus lowest quartile of dietary vitamin C was 0.85 (95% CI: 0.73, 0.98). The E-value for the OR was 1.64, while it was 1.15 for the upper limit of its 95% CI (Supplementary Fig. 2). Exclusion of individuals in the highest and lowest 1% of intake or modelling total energy intake using fractional polynomials did not substantially modify results (Table 2).
A consistent inverse association across all considered quartiles of vitamin C was found for noncardia GC, while results were not significant for cardia GC (Table 3). As for histological types, individuals in quartile 4 of dietary vitamin C had reduced OR of both diffuse and intestinal types of GC compared with participants in quartile 1 (Table 3).
Findings of the stratified analyses are reported in Table 4. An inverse association between vitamin C and GC was observed for all considered quartiles of intake among clinic-based studies, but not among community-based ones. In addition, estimates showed non-significant associations across strata of both age and sex. Instead, considering the highest versus lowest quartiles of intake, an inverse association between vitamin C and GC, was observed among individuals reporting low (OR: 0.81; 95% CI: 0.66, 0.99) or high socioeconomic status (OR: 0.48; 95% CI: 0.29, 0.77), while a lack of association was observed among those with moderate socioeconomic status. Also, the association was significant among participants with normal weight and among overweight individuals. Quartile 4 of vitamin C intake was inversely associated with GC among never and former smokers and ever drinkers, while no association was found among other strata of tobacco smoking and alcohol drinking (Table 4). Additionally, vitamin C was found to be inversely associated with GC among individuals both with and without H. pylori seropositivity, with similar results when comparing all cases to seropositive controls. However, no significant heterogeneity across considered strata was detected.
Findings of the interaction analysis are reported in Supplementary Table 3. The only significant results were found for BMI, which showed a positive additive interaction with vitamin C. Indeed, participants with normal weight and with an intake of vitamin C lower than the median had the strongest association with GC among the considered joint strata (OR: 1.80; 95% CI: 1.56, 2.06), with 19% (95% CI: 8%, 31%) of GC cases among these doubly exposed individuals being attributable to interaction.
In line with the results of the overall analysis, the dose–response models showed attenuated estimates of ORs when adjusting for BMI and intake of fruit and vegetables (Fig. 1, Table 5), with ORs decreasing up to 150–200 mg/day of vitamin C (OR: 0.54; 95% CI: 0.41, 0.71). For higher intakes, instead, ORs tended to increase towards unity, which was included in the 95% CI for values of dietary vitamin C of 400 mg/day or higher.
Dose–response relationship between dietary intake of vitamin C and gastric cancer fitted by using one-stage logistic mixed-effects models with second-order fractional polynomial. Solid black line: ln(odds ratio, OR), dashed black line: 95% confidence interval, solid horizontal grey line: OR = 1. Model 1 (n = 15,888): adjusted for sex (male, female), age (≤ 40 years, 41–50 years, 51–60 years, 61–70 years, > 70 years, missing), socioeconomic status (low, intermediate, high, missing), tobacco smoking status (never, former, current, missing), alcohol drinking status (never, ever, missing), total energy intake (continuous). Model 2 (n = 15,200): adjusted for sex (male, female), age (≤ 40 years, 41–50 years, 51–60 years, 61–70 years, > 70 years, missing), socioeconomic status (low, intermediate, high, missing), tobacco smoking status (never, former, current, missing), alcohol drinking status (never, ever, missing), body mass index (underweight, normal weight, overweight, obese, missing), intake of fruit and vegetables (low, intermediate, high, missing), total energy intake (continuous). Reference value of dietary vitamin C: 6 mg/day
Discussion
Our pooled analysis of individual-level data suggests that dietary vitamin C is inversely associated with GC and, even though its strength was attenuated, this association persisted after adjustment for intake of fruit and vegetables. This relationship was limited to noncardia GC, with no significant association for cardia GC, while the results were similar for intestinal and diffuse types of GC. Although estimates showed occasional slight differences across strata of patients’ characteristics, no significant heterogeneity was found, suggesting that the association between vitamin C and GC does not substantially vary according to considered strata. However, the findings of the interaction analysis for BMI also suggest that individuals who would benefit the most from an increased intake of vitamin C are those with normal weight. This result could be either due to both a healthier diet among individuals who are neither overweight nor obese or to reverse causality, since GC might lead to weight loss itself [38, 39]. Lastly, the dose–response analysis indicates that dietary levels of vitamin C higher than the recommended intake, which is equal to 90 mg/day for men and 75 mg/day for women [40], and up to 150/200 mg/day could be beneficial for the reduction of GC risk.
Three recent meta-analyses reported an inverse association between dietary intake of vitamin C and GC, in line with our results [13,14,15]. In contrast with our findings, however, Li et al. found that this was consistent among both clinic- and community-based studies, while a non-significant result was observed for diffuse type GC [15]. In addition, some differences in their results compared with our findings might also be explained by differences in levels of intake of vitamin C between the study populations. A few additional studies have been published after those meta-analyses [41, 42], further confirming the inverse relationship between dietary vitamin C and GC. Moreover, Kim et al. reported that vitamin C was inversely associated with GC only among nonsmokers [41], in line with our results suggesting an association only among never and former smokers.
Our study was conducted using data from several case–control studies carried out in different geographic regions and which were harmonized centrally at the StoP coordinating center using a common methodology. In addition, we were able to adjust the analyses for a number of relevant covariates, including intake of fruit and vegetables that has been overlooked by most of previous epidemiological studies [13,14,15]. Also, the large sample size allowed us to investigate whether the relationship between dietary vitamin C and GC was consistent across strata of participants’ characteristics, which could help to identify individuals who would benefit the most from related nutritional interventions. With the same aim, we assessed the occurrence of additive interactions, which are commonly deemed more relevant at informing public health interventions compared with multiplicative interactions [35], between vitamin C and other selected risk or protective factors.
Among limitations, our analysis relied on previously conducted studies which were based on different methodologies, including the adoption of different FFQs used for exposure assessment together with country-specific databases, possibly contributing to heterogeneity between included studies and to some discrepancies with previous meta-analyses, as described above. In addition, studies contributing data to our analyses had a case–control design, which may suffer from selection bias, in particular among clinic-based studies [43, 44]. Furthermore, since dietary information was self-reported through questionnaires, exposure could be affected by recall bias, although it has been reported to be limited in case–control studies investigating micronutrients [45]. Similarly, information on relevant covariates, such as tobacco smoking, alcohol drinking, BMI, and others, might be affected by recall bias too. As for BMI, in particular, results of the interaction analysis might be biased also because individuals with GC might have undergone weight loss due to the disease itself before the actual diagnosis caused by tumor-related obstruction of the upper digestive tract, malabsorption, anorexia, and hypermetabolism [38, 39]. Thus, leading to apparent lower OR of GC among overweight or obese individuals. Moreover, evaluation of H. pylori serostatus has been reported to lead to misclassification of previous infection, differentially among cases and controls [46, 47], although this issue was partially addressed by the sensitivity analysis we carried out where we considered all cases as seropositive. Additionally, although the association between vitamin C and GC was still significant after adjustment for intake of fruit and vegetables, this finding warrants further investigation to rule out whether the observed relationship is due to a real effect of vitamin C or to other factors including nutrients that can be found in fruit and vegetables, and thus to various sources of bias, such as residual and unmeasured confounding. Indeed, since dietary vitamin C mostly derives from intake of fruit and vegetables, their intakes are typically related, hence making it difficult to separate the effect of vitamin C from that of other components present in fruit and vegetables, such as other antioxidants.
In conclusion, the results of the present analysis carried out by pooling data from fourteen epidemiological studies suggest that vitamin C is inversely associated with GC. However, further well-designed prospective studies, aimed at disentangling the complex relationships between intake of fruit and vegetables, vitamins and other antioxidants, and GC, are warranted to prove causality of the observed relationship between vitamin C and GC.
Data availability
Data described in the manuscript, code book, and analytic code will be made available upon request from the corresponding author pending approval of the participating study centers of the StoP Project.
Abbreviations
- AP:
-
Attributable proportion
- BMI:
-
Body mass index
- CI:
-
Confidence interval
- FFQ:
-
Food-frequency questionnaire
- GC:
-
Gastric cancer
- H. pylori :
-
Helicobacter pylori
- OR:
-
Odds ratio
- RERI:
-
Relative excess risk due to interaction
- StoP Project:
-
Stomach cancer Pooling Project
References
Sung H, Ferlay J, Siegel RL, Laversanne M, Soerjomataram I, Jemal A, Bray F. Global Cancer Statistics 2020: GLOBOCAN estimates of incidence and mortality worldwide for 36 cancers in 185 countries. CA Cancer J Clin. 2021;71:209–49.
Li M, Park JY, Sheikh M, et al. Population-based investigation of common and deviating patterns of gastric cancer and oesophageal cancer incidence across populations and time. Gut. 2022;72(5):846–54. https://doi.org/10.1136/GUTJNL-2022-328233.
Arnold M, Park JY, Camargo MC, Lunet N, Forman D, Soerjomataram I. Is gastric cancer becoming a rare disease? A global assessment of predicted incidence trends to 2035. Gut. 2020;69:823–9.
Morgan E, Arnold M, Camargo MC, et al. The current and future incidence and mortality of gastric cancer in 185 countries, 2020–40: a population-based modelling study. eClinicalMedicine 2022;47:101404.
Richa SN, Sageena G. Dietary factors associated with gastric cancer—a review. Transl Med Commun. 2022;7:1–11.
Tsugane S, Sasazuki S. Diet and the risk of gastric cancer: review of epidemiological evidence. Gastric Cancer. 2007;10:75–83.
Bouras E, Tsilidis KK, Triggi M, Siargkas A, Chourdakis M, Haidich AB. Diet and risk of gastric cancer: an umbrella review. Nutrients. 2022;14:1764.
Ngo B, Van Riper JM, Cantley LC. Yun J (2019) Targeting cancer vulnerabilities with high-dose vitamin C. Nat Rev Cancer. 2019;195(19):271–82.
Lü JM, Lin PH, Yao Q, Chen C. Chemical and molecular mechanisms of antioxidants: experimental approaches and model systems. J Cell Mol Med. 2010;14:840–60.
Mirvish SS. Effects of Vitamins C and E on N-Nitroso compound formation, carcinogenesis, and cancer. Cancer. 1986;58:1842–50.
World Cancer Research Fund/American Institute for Cancer Research. Diet, nutrition, physical activity and cancer: a global perspective. Continuous Update Project Expert Report 2018; 2018.
Cai X, Li X, Jin Y, Zhang M, Xu Y, Liang C, Weng Y, Yu W, Li X. Vitamins and Helicobacter pylori: an updated comprehensive meta-analysis and systematic review. Front Nutr. 2022;8:1308.
Kong P, Cai Q, Geng Q, Wang J, Lan Y, Zhan Y, Xu D. Vitamin intake reduce the risk of gastric cancer: meta-analysis and systematic review of randomized and observational studies. PLoS ONE. 2014;9: e116060.
Fang X, Wei J, He X, et al. Landscape of dietary factors associated with risk of gastric cancer: a systematic review and dose-response meta-analysis of prospective cohort studies. Eur J Cancer. 2015;51:2820–32.
Li P, Zhang H, Chen J, Shi Y, Cai J, Yang J, Wu Y. Association between dietary antioxidant vitamins intake/blood level and risk of gastric cancer. Int J Cancer. 2014;135:1444–53.
González CA, López-Carrillo L. Helicobacter pylori, nutrition and smoking interactions: their impact in gastric carcinogenesis. Scand J Gastroenterol. 2009;45:6–14.
Pelucchi C, Lunet N, Boccia S, et al. The stomach cancer pooling (StoP) project: study design and presentation. Eur J Cancer Prev. 2015;24:16–23.
Lucenteforte E, Scita V, Bosetti C, Bertuccio P, Negri E, La Vecchia C. Food groups and alcoholic beverages and the risk of stomach cancer: a case-control study in Italy. Nutr Cancer. 2008;60:577–84. https://doi.org/10.1080/01635580802054512.
Buiatti E, Palli D, Decarli A, et al. A case-control study of gastric cancer and diet in Italy. Int J Cancer. 1989;44:611–6.
Castaño-Vinyals G, Aragonés N, Pérez-Gómez B, et al. Population-based multicase-control study in common tumors in Spain (MCC-Spain): rationale and study design. Gac Sanit. 2015;29:308–15.
Santibañez M, Alguacil J, De La Hera MG, Navarrete-Muñoz EM, Llorca J, Aragonés N, Kauppinen T, Vioque J. Occupational exposures and risk of stomach cancer by histological type. Occup Environ Med. 2012;69:268–75.
Lagiou P, Samoli E, Lagiou A, Peterson J, Tzonou A, Dwyer J, Trichopoulos D. Flavonoids, vitamin C and adenocarcinoma of the stomach. Cancer Causes Control. 2004;15:67–72.
Zaridze D, Borisova E, Maximovitch D, Chkhikvadze V. Aspirin protects against gastric cancer: results of a case-control study from Moscow, Russia. J Cancer. 1999;82:473–6.
Lunet N, Valbuena C, Vieira AL, Lopes C, Lopes C, David L, Carneiro F, Barros H. Fruit and vegetable consumption and gastric cancer by location and histological type: case-control and meta-analysis. Eur J Cancer Prev. 2007;16:312–27.
Setiawan VW, Yu G-P, Lu Q-Y, et al. Allium vegetables and stomach cancer risk in China. Asian Pac J Cancer Prev. 2005;6:387–95.
Machida-Montani A, Sasazuki S, Inoue M, Natsukawa S, Shaura K, Koizumi Y, Kasuga Y, Hanaoka T, Tsugane S. Association of Helicobacter pylori infection and environmental factors in non-cardia gastric cancer in Japan. Gastric Cancer. 2004;71(7):46–53.
Pakseresht M, Forman D, Malekzadeh R, Yazdanbod A, West RM, Greenwood DC, Crabtree JE, Cade JE. Dietary habits and gastric cancer risk in north-west Iran. Cancer Causes Control. 2011;22:725–36.
Ward MH, Sinha R, Heineman EF, Rothman N, Markin R, Weisenburger DD, Correa P, Zahm SH. Risk of adenocarcinoma of the stomach and esophagus with meat cooking method and doneness preference. Int J Cancer. 1997;71:14–9.
Hernández-Ramírez RU, Galván-Portillo MV, Ward MH, Agudo A, González CA, Oñate-Ocaña LF, Herrera-Goepfert R, Palma-Coca O, López-Carrillo L. Dietary intake of polyphenols, nitrate and nitrite and gastric cancer risk in Mexico City. Int J Cancer. 2009;125:1424–30.
López-Carrillo L, Avila MH, Dubrow R. Chili pepper consumption and gastric cancer in Mexico: a case-control study. Am J Epidemiol. 1994;139:263–71.
López-Carrillo L, López-Cervantes M, Robles-Díaz G, Ramírez-Espitia A, Mohar-Betancourt A, Meneses-García A, López-Vidal Y, Blair A. Capsaicin consumption, Helicobacter pylori positivity and gastric cancer in Mexico. Int J Cancer. 2003;106:277–82.
Royston P, Ambler G, Sauerbrei W. The use of fractional polynomials to model continuous risk variables in epidemiology. Int J Epidemiol. 1999;28:964–74.
Van Der Weele TJ, Ding P. Sensitivity analysis in observational research: introducing the E-value. Ann Intern Med. 2017;167:268–74.
Peleteiro B, La Vecchia C, Lunet N. The role of Helicobacter pylori infection in the web of gastric cancer causation. Eur J Cancer Prev. 2012;21:118–25.
VanderWeele TJ, Knol MJ. A tutorial on interaction. Epidemiol Method. 2014;3:33–72.
Hosmer DW, Lemeshow S. Confidence interval estimation of interaction. Epidemiology. 1992;3:452–6.
Knol MJ, VanderWeele TJ, Groenwold RHH, Klungel OH, Rovers MM, Grobbee DE. Estimating measures of interaction on an additive scale for preventive exposures. Eur J Epidemiol. 2011;26:433–8.
Rosania R, Chiapponi C, Malfertheiner P, Venerito M. Nutrition in patients with gastric cancer: an update. Gastrointest Tumors. 2015;2:178–87.
Mansoor W, Roeland EJ, Chaudhry A, Liepa AM, Wei R, Knoderer H, Abada P, Chatterjee A, Klempner SJ. Early weight loss as a prognostic factor in patients with advanced gastric cancer: analyses from REGARD, RAINBOW, and RAINFALL phase III studies. Oncologist. 2021;26:e1538–47.
Institute of Medicine. Dietary reference intakes for vitamin C, vitamin E, selenium, and carotenoids. Washington, DC: National Academies Press; 2000. https://doi.org/10.17226/9810
Kim SA, Kwak JH, Eun CS, Han DS, Kim YS, Song KS, Choi BY, Kim HJ. Association of dietary antioxidant vitamin intake and gastric cancer risk according to smoking status and histological subtypes of gastric cancer: a case-control study in Korea. Nutr Cancer. 2022;75:652–61.
Hoang BV, Lee J, Choi IJ, Kim YW, Ryu KW, Kim J. Effect of dietary Vitamin C on gastric cancer risk in the Korean population. World J Gastroenterol. 2016;22:6257–67.
Sutton-Tyrrell K. Assessing bias in case-control studies. Proper selection of cases and controls. Stroke. 1991;22:938–42.
Kopec JA, Esdaile JM. Bias in case-control studies. A review. J Epidemiol Community Heal. 1990;44:179–86.
Friedenreich CM, Howe GR, Miller AB. Recall bias in the association of micronutrient intake and breast cancer. J Clin Epidemiol. 1993;46:1009–17.
Morais S, Costa A, Albuquerque G, et al. “True” Helicobacter pylori infection and non-cardia gastric cancer: a pooled analysis within the Stomach Cancer Pooling (StoP) Project. Helicobacter. 2022;8: e12883.
Biranjia-Hurdoyal SD, Seetulsingh-Goorah SP. Performances of four Helicobacter pylori serological detection kits using stool antigen test as gold standard. PLoS ONE. 2016;11: e0163834.
Acknowledgements
This study was funded by the Associazione Italiana per la Ricerca sul Cancro (Project number 21378, Investigator Grant). NL and SM are funded under the Unidade de Investigação em Epidemiologia—Instituto de Saúde Pública da Universidade do Porto (EPIUnit; UIDB/04750/2020) financed by national funds from the Foundation for Science and Technology—FCT (Portuguese Ministry of Science, Technology and Higher Education) and the Laboratório para a Investigação Integrativa e Translacional em Saúde Populacional (ITR; LA/P/0064/2020). SM also received funding under the scope of the project ‘NEON-PC—Neuro-oncological complications of prostate cancer: longitudinal study of cognitive decline’ (POCI-01-0145-FEDER-032358; Ref. PTDC/SAU-EPI/32358/2017) funded by FEDER through the Operational Program Competitiveness and Internationalization, and national funding from FCT, and the EPIUnit—Junior Research—Prog Financing (UIDP/04750/2020). The study was also supported by the Italian Ministry of Health through the project “Interaction of genomic and dietary aspects in gastric cancer risk: the global StoP project” (Grant number RF-2021-12373951). This research was supported in part by the Intramural Research Program of the US National Cancer Institute. The authors thank the European Cancer Prevention Organization for providing support for the project meetings.
Funding
Open access funding provided by Alma Mater Studiorum - Università di Bologna within the CRUI-CARE Agreement.
Author information
Authors and Affiliations
Contributions
Conceptualization: Michele Sassano, Paolo Boffetta; methodology: Michele Sassano, Paolo Boffetta; formal analysis: Michele Sassano; writing—original draft: Michele Sassano; project administration: Claudio Pelucchi, Carlo La Vecchia; supervision: Paolo Boffetta; data curation: all authors; writing—review and editing: all authors.
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Human rights statement and informed consent
All procedures followed were in accordance with the ethical standards of the responsible committee on human experimentation (institutional and national) and with the Helsinki Declaration of 1964 and later versions. The participating studies were conducted in accordance with applicable laws, regulations, and guidelines for the protection of human subjects, including obtainment of informed consent from participants where required by abovementioned laws, regulations and guidelines into force at the time when the individual studies were conducted.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if changes were made. The images or other third party material in this article are included in the article's Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article's Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
Sassano, M., Seyyedsalehi, M.S., Collatuzzo, G. et al. Dietary intake of vitamin C and gastric cancer: a pooled analysis within the Stomach cancer Pooling (StoP) Project. Gastric Cancer 27, 461–472 (2024). https://doi.org/10.1007/s10120-024-01476-8
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10120-024-01476-8