Abstract
Implementation science (IS) uses systematic methods to close gaps between research and practice by identifying and addressing barriers to implementation of evidence-based interventions (EBIs). To reach UNAIDS HIV targets, IS can support programs to reach vulnerable populations and achieve sustainability. We studied the application of IS methods in 36 study protocols that were part of the Adolescent HIV Prevention and Treatment Implementation Science Alliance (AHISA). Protocols focused on youth, caregivers, or healthcare workers in high HIV-burden African countries and evaluated medication, clinical and behavioral/social EBIs. All studies measured clinical outcomes and implementation science outcomes; most focused on early implementation outcomes of acceptability (81%), reach (47%), and feasibility (44%). Only 53% used an implementation science framework/theory. Most studies (72%) evaluated implementation strategies. Some developed and tested strategies, while others adapted an EBI/strategy. Harmonizing IS approaches allows cross study learning and optimization of delivery of EBIs and could support attainment of HIV goals.
Similar content being viewed by others
Explore related subjects
Discover the latest articles, news and stories from top researchers in related subjects.Avoid common mistakes on your manuscript.
Introduction
Adolescents and young adults (AYA) remain a key priority population for the achievement of global HIV targets. Research over the past decade has highlighted significantly poorer clinical outcomes across HIV testing, linkage to care, initiation of treatment and viral suppression among AYA compared to adult populations [1,2,3]. In addition, HIV incidence among AYA remains high, especially among adolescent girls and young women (AGYW), with an estimated 5000 new infections occurring among AGYW each week [4]. Although interventions for improving poor HIV outcomes among AYA exist, the majority have yet to be scaled up and implemented programmatically. To reach global HIV targets for AYA, it is critical to identify and address unique gaps in the translation and scale-up of evidence-based interventions (EBIs) among this key population. Critical gap areas for this population include adherence and retention, transitional care from pediatric to adult services, integration of mental health and sexual and reproductive health services into HIV services, and prevention of new infections [5].
Implementation science (IS) uses systematic methods to close the know-do gap that exists between research and clinical practice by identifying and addressing barriers to the implementation of EBIs. To accelerate progress towards UNAIDS 95-95-95 goals, global focus has shifted to IS to reach the most vulnerable populations, as well as sustain changes made to optimize HIV clinical outcomes [6, 7]. IS methods can address critical gaps, particularly for children and adolescents, in whom evidence is largely lacking and predominantly extrapolated from adult studies [8]. While this approach has enabled faster implementation of EBIs for this marginalized population, it may result in less effective implementation if there is inflexibility to adapt to the specific unique needs of the population which may result in lack of effectiveness [8]. By identifying the processes used in implementation, and measuring contextual factors influencing implementation, IS provides insight into the heterogeneity observed in implementation of EBIs across varied settings and helps identify how to optimize and adapt EBIs for maximum impact.
The emergent field of IS has wide variation in how measures are defined, applied and studied [9]. Frameworks provide a way to harmonize the use of IS measures and compare IS outcomes across a wide range of settings and populations. Using consistent approaches to measure and evaluate implementation processes and contextual influences on implementation of EBIs could be especially valuable for AYA, where rapid translation of research to clinical practice has the potential to significantly improve health for a future generation. In addition, IS data collection tools have largely been qualitative, with only a few quantitative tools validated in resource limited settings [10, 11]. Given the global distribution of the epidemic, understanding how IS concepts are applied in AYA HIV research, as well as how IS measures, outcomes and determinants are adapted for LMIC settings, is a key strategy to understanding how to end the HIV epidemic. Harmonizing IS measures across studies and settings, developing reliable and valid ways of assessing IS measures, and identifying when and how specific measures are selected, is critical to support innovations in the field of IS, and areas of focus for future AYA research. In this paper, we review ongoing AYA implementation research in the Adolescent HIV Prevention and Treatment Implementation Science Alliance (AHISA) network to identify IS measures, frameworks and outcomes used across the network and determine gaps in methodology and rigor.
Methods
Study Context
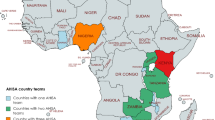
In 2017, to catalyze IS research within the field of adolescent HIV, the NIH convened the Adolescent HIV Prevention and Treatment Implementation Science Alliance (AHISA), a collaboration where researchers, program implementers, and policymakers could share experiences and exchange ideas to facilitate effective implementation of EBIs in the sub-Saharan context [12]. Principal and co-investigators of funded projects (study teams) were eligible to apply for AHISA membership if their research included evaluation of one or more domains within the HIV care continuum and focused on AYA in Africa. AHISA is currently composed of 26 study teams, conducting one or more research studies in 11 countries in Africa, including 5 countries with the highest prevalence of adolescent HIV globally (South Africa, Nigeria, Kenya, Uganda, Tanzania) [13].
Study Design & Data Collection
This review aimed to summarize ongoing studies conducted by AHISA members and characterize implementation and clinical outcomes measured, EBIs and implementation strategies tested, and identify gaps in the scientific agenda of IS for AYA across the HIV prevention and HIV care cascades. We presented the review’s aim and purpose to all AHISA member study teams during the 5th Annual AHISA Meeting (February 11–12, 2021). We requested study protocols and protocol manuscripts via email from the PI’s of all 26 study teams. Each AHISA study team provided between 1 and 3 study protocols for review.
Analysis
ATLAS.ti version 9 (Scientific Software Development GmbH) supported coding and analysis of submitted study documents. Codes were developed by the authors to extract information related to study context (study design, population, geographical setting), EBIs and clinical or efficacy/effectiveness outcomes assessed, implementation strategies tested, and implementation outcomes and/or determinants measured. We utilized Proctor’s Implementation Outcome Framework (IOM) [14] and the Reach, Effectiveness, Adoption, Implementation, and Maintenance (RE-AIM) framework [15] to define and classify outcomes (Table 1). IS outcomes were first identified if explicitly named in study documents. These outcomes were reviewed by manuscript co-authors for consistent interpretation between studies and re-categorized as needed to match definitions in Table 1. Additional IS outcomes described in study documents, but not explicitly named, were also categorized by co-authors using IOM and RE-AIM definitions in Table 1. All study populations that included any age bands between 10 and 24 years of age were grouped as AGYW if defined as female gender only, youth with HIV (YLH) if living with HIV, or youth if they included both populations living with and without HIV. Those that included adolescents (ages 10–19) only were classified as adolescents living with HIV (ALH). Where possible, we mapped implementation strategies to the Expert Recommendations for Implementing Change (ERIC) [16].
The coding team included four co-authors of this manuscript (KBS, SD, TC, IN), and two acknowledged researchers (SV, RS), who each participated in independent coding and code review. Each study document was independently coded by one author, and coded documents were reviewed by a second author. Disagreements were discussed and resolved through group discussion. Data were summarized using queries and code co-occurrence tables and re-presented in summary tables. Initially drafted summary tables were reviewed by three manuscript authors (IN, ADW, KBS) to ensure internal consistency in categorization across studies. Extracted and summarized data were returned to individual AHISA teams for review and verification of accuracy and completeness. In cases where the terminology between the study protocols and the review team’s conceptualization differed (e.g., defining an EBI versus strategy), the review team maintained its classification for internal consistency.
Ethics
This study did not involve human subject data and was exempt from IRB research oversight.
Results
This review focused on implementation outcomes, frameworks, and strategies applied to AYA HIV prevention and care among AHISA-affiliated studies. All 26 AHISA member study teams submitted one or more study protocols or protocol manuscripts, representing a total of 36 research studies. Studies represented ten countries; South Africa (10 studies [28%]), Kenya (6 [17%]), Zambia (3 [8%]), Tanzania (3 [8%]), Zimbabwe (3 [8%]), Nigeria (3 [8%]), and Uganda, Ghana, Botswana and Malawi (1 [3%] each). Four studies (11%) took place in multiple locations (Kenya and Canada, South Africa and Kenya, Malawi and South Africa, Kenya and Uganda). Fifteen studies (42%) focused on HIV prevention, 12 (33%) on HIV treatment, 3 (8%) on HIV testing, 3 (8%) studies on HIV treatment/testing/prevention, 2 studies on treatment/testing (6%), and 1 study (3%) on treatment/prevention. Of the 12 studies focused on HIV treatment, 4 were on transition to adult care, 2 on adherence alone, 3 on adherence and retention, 2 on mental health, and 1 on morbidity. Supplementary Table 1 summarizes strategies and outcomes across the HIV continuum of care.
Study Designs
Randomized designs were most common, with 12 (33%) cluster randomized clinical trials (RCTs), 9 (25%) individual RCTs, 4 (11%) stepped wedge RCTs, 1 (3%) 2 × 2 factorial design RCT, 1 (3%) that included both stepped wedge and individually randomized RCT designs, 1 (3%) described as cluster RCT with individual randomization within clusters. There were 6 (17%) cohort studies, 1 (3%) described as observational, and 1 (3%) exclusively qualitative research design. Overall, 8 (22%) were defined as pilot studies.
Aligned with the broad research emphasis of AHISA, studies focused on a range of AYA populations, with 13 including AGYW, 17 including youth, 12 including YLH, either alone or in combination with caregivers and health providers, and 1 each including antenatal mothers, HIV negative male youth and health care workers (Table 2). YLH-defined populations spanned a range of age groups; the most common (12 [33]%) age groups were 14–25 years, while 8 studies (22%) included only youth ≤ 19 years of age.
Evidence-Based Interventions
There was diversity in the types of EBIs delivered in the 25 studies. Broadly, these were classified into 14 (39%) studies delivering medications (PrEP and ART), 13 (36%) delivering behavioral or social interventions, 9 (25%) delivering clinical services beyond medication, 4 (11%) delivering health systems toolkits, and 2 (5%) providing economic support. A few studies used a combination of EBIs as their intervention. These studies combined EBIs across categories, including 3 studies that combined medication and clinical services and 1 study that combined behavioral or social interventions with economic support. Other studies evaluating combined EBIs integrated multiple EBIs from the same category (e.g., behavioral/social EBIs) into a single multicomponent EBI approach for the study.
These multicomponent EBI approaches are useful for strengthening the effect of a therapy on a single health outcome or to broaden the number of health outcomes targeted in the EBI package. For example, in the Sauti ya Vijana pilot [26, 27] and scale up study [28], a multicomponent behavioral/social EBI included components of trauma-informed cognitive behavioral therapy, interpersonal psychotherapy, and motivational interviewing, all unique mental health therapy EBIs focused on achieving specific mental health outcomes. In another multi-component approach, the Thetha Nami study [18] delivered a multicomponent clinical services and medication EBI, including universal test and treat, family planning, and pre-exposure prophylaxis, to reach a broader range of HIV and sexual and reproductive health outcomes.
Implementation Outcomes, Determinants, and Frameworks
Implementation outcomes were defined by Proctor’s IOF and RE-AIM. The definitions and example quotes for how each outcome was operationalized within study protocols are summarized in Table 1. All 36 studies measured at least one implementation outcome. The most commonly measured outcomes were acceptability (n = 29), implementation (n = 13), feasibility (n = 16), cost (n = 16), fidelity (n = 15), and reach (n = 17) (Table 3). Outcomes measured less commonly included appropriateness (n = 8), adoption (n = 9), sustainability (n = 6), maintenance (n = 5), and penetration [2] (Table 3). Earlier phase implementation outcomes (e.g., acceptability, feasibility, appropriateness, adoption) were more common across the studies than later phase outcomes (e.g. sustainability, maintenance) (Fig. 1). The operationalization of these outcomes was heterogeneous, and there were few occurrences in which a validated implementation outcome measure was utilized or utilized consistently across studies. Studies that focused on the same aspects of the HIV care continuum assessed IS outcomes at different timepoints, among different stakeholder groups and using different measurement tools. For example, the InTSHA and ATTACH studies both focused on transition to adult care and measured acceptability. However, the InTSHA study measured acceptability among those receiving the intervention using the Unified Theory of Acceptance and Use of Technology (UTAUT) [31, 32], while the ATTACH study measured acceptability among those delivering the intervention using the Acceptability of Intervention Measure [34].
Characterization of coverage in measurement of IS outcomes and strategies by EBI. AHISA study EBIs were classified into five representative categories. IS outcomes were listed by stage of implementation, ranging from early (acceptability, adoption, appropriateness, reach, feasibility), to mid (fidelity, implementation, penetration, cost), and late (maintenance, sustainability) stages. Presence or absence of specific implementation outcomes and strategies was assessed within each EBI category and organized into a heat map representing the overall evidence available for each implementation measure
All studies measured clinical outcomes or precursors to clinical outcomes alongside implementation outcomes, representing reliance on hybrid effectiveness-implementation trial designs. The clinical outcomes measured aligned closely with the EBIs being tested. Many studies included precursor outcomes that were proximal to clinical outcomes of interest. For example, the 3P study included PrEP interest and knowledge as precursors to PrEP uptake or adherence [35] and the ATTACH study measured transition readiness as a precursor to successful transition [25] (Table 3).
Less than half of studies (n = 16) assessed determinants of implementation of EBIs, and a few explored how specific strategies might overcome specific barriers. For example, the 3P study [35], the HIV prevention cascade study [20, 40], POWER PrEP [38] and Tu’Washindi [17] assessed barriers to PrEP at the individual, social, and cultural levels. The InTSHA study [23] focused on assessing how their social media implementation strategy overcame specific barriers and enhanced facilitators to transition care. While not specifically related to determinants, two studies described investigating mechanisms, mediators, and moderators (Project YES! [22] and SA IMARA [19] (Table 3)) of EBI implementation.
Only half (n = 19) of the studies specifically mentioned applying a framework, model, or theory to inform their studies. The most common were RE-AIM (n = 4) [15], the Consolidated Framework for Implementation Research (CFIR) (n = 3) [45], the FRAME (n = 2) [30] used to track adaptation, Proctor’s IOF (n = 4) [14], and the Exploration, Preparation, Implementation, Sustainment (EPIS) framework (n = 1), and PRECEDE (n = 1) [42]. Seven studies employed frameworks or theories that were not explicitly implementation science frameworks, including those focused on behavioral theories, like the HIV Prevention Cascade framework [36]. Of note, many studies utilized outcomes language from either RE-AIM or Proctor’s IOF without specifically mentioning these frameworks in their protocols (Table 3).
Implementation Strategies
Across AHISA, 26 studies incorporated one or more implementation strategies and 21 studies developed and tested a strategy. For example, the 3P study developed and tested a conditional financial incentive based on PrEP drug levels to motivate adherence [41], while the iCARE study developed and tested a combination demand creation and service provision implementation strategy that included personalized interactive SMS support and peer navigation [46]. Seven studies engaged in adapting an EBI; 3 only adapted an EBI while 4 adapted and tested an EBI. Adaptation was more common among the behavioral and social EBIs. For example, the MUHAS study did not test a strategy but did describe adapting the EBI to be delivered while observing COVID-19 prevention measures [47]. In contrast, the ATTACH study engaged in adapting an EBI disclosure toolkit, developing a transition toolkit, and testing the combined package with a strategy of tracking and training tools [25]. Testing strategies was most common among studies delivering medication EBIs (Fig. 1). When mapped to ERIC, implementation strategies were predominantly targeting change at the interpersonal level, including provider changes in training (e.g., use of training manuals, tracking sheets, and patient actors for simulation-based training), task shifting (e.g., to peers or lay counselors), and supervision. For studies delivering PrEP, the strategies tested occurred at different levels, including incentives (individual level), video and brochure education (individual level), interactive counseling (interpersonal level), and mobilization and community engagement (community level).
Discussion
This review of AHISA protocols and studies revealed a rich body of implementation science focusing on HIV prevention and HIV care interventions for AYA populations in high HIV-burden African countries. Most studies focused on early implementation outcomes of delivering medication, clinical, and behavioral/social EBIs and all used a hybrid trial approach that included measurement of clinical outcomes. The use of frameworks and assessment of determinants was reasonably common, but fewer studies utilized validated implementation outcome measures. Many studies delivered EBIs in parallel with an implementation strategy, with some experimentally testing strategies. Formal evaluation of mechanisms, moderators, and mediators of EBI implementation was uncommon.
Since the original formation of the AHISA in 2017, the use of frameworks, measurement of implementation outcomes, and testing of implementation strategies has expanded in NIH’s implementation science portfolio [12]. Facilitating this expansion, as part of the AHISA collaboration, study teams received intensive implementation science training to strengthen current research designs and inform future IS grants. Expanded training in IS among AHISA teams was reflected in the shared research protocols, with increasing use of IS frameworks in the most recently developed protocols. For example, the Sauti Ya Vijana scale protocol [28] included the CFIR framework to evaluate barriers and facilitators to implementation and the FRAME to evaluate intervention adaptations, expanding IS activities from those included in the earlier pilot [26, 27]. Additionally, almost all AHISA-related protocols dated 2020–2021 included a formal IS frameworks (CFIR, RE-AIM, FRAME, Proctor) [23, 28, 46, 48], whereas most protocols dated 2017–2019 did not. This extended use of IS frameworks among AHISA team research projects demonstrates progress towards achieving the AHISA goal of building implementation science capacity among adolescent HIV researchers in high HIV-burden African countries [12]. As implementation of HIV prevention and care interventions for AYA populations continues and moves from early- to mid- to late-implementation, we expect the AHISA portfolio to grow to include later stage implementation outcomes (e.g., sustainability and penetration) in addition to early implementation outcomes (e.g., acceptability and feasibility) that are common in the current portfolio. Similarly, we expect more studies to shift beyond identifying barriers to implementation and instead focus on testing implementation strategies. A series of similarly structured reviews of interventions addressing stigma [49], non-communicable diseases [50], and depression [51] in resource-limited settings observed few studies that measured later implementation outcomes, and had less specification and testing of implementation strategies, and suboptimal usage of implementation frameworks.
In this review, many studies included an implementation strategy, but often the strategy was not referred to using IS strategy terminology in the protocol. This represents an opportunity to strengthen future research in this area; operationalizing strategies using Proctor’s specification scheme [52] will contribute to the growing evidence linking specific IS strategies to particular outcomes. Additionally, many studies that utilized a strategy did not test the impact of the strategy on implementation outcomes experimentally (a traditional implementation study) but rather conducted hybrid effectiveness-implementation type I designs with clinical outcomes as the primary focus and inclusion of implementation outcomes [53]. As time progresses, we expect more research to employ hybrid type II (equal focus on clinical and implementation outcomes) and III designs (primary focus on implementation outcomes with inclusion of clinical outcomes), as well as purely implementation foci. Finally, most of the implementation strategies tested focused on interpersonal level changes, with the exception of studies focused on PrEP delivery, which included strategies at individual, interpersonal, and community levels. One gap that could be strategically addressed in future HIV prevention research would be testing implementation strategies at higher levels for non-PrEP EBIs. These could include systems-level and community-level strategies, which are well suited to achieve later implementation outcomes like sustainability and penetration. In a similar review of implementation science applied to PrEP delivery for pregnant and postpartum populations, the authors focused on earlier implementation outcomes. They noted fewer studies testing implementation strategies, and of those strategies being tested, fewer tested systems-level or higher level strategies [54].
Adaptation of EBIs was common in the AHISA-affiliated studies. Many interventions required adaptation to a different cadre of provider (often shifting to peers), a new population (e.g., AYA instead of adults) or context (shifting from in-person to mobile delivery), and often to settings with fewer resources than the ones where the EBI was originally developed and tested. Despite adaptation being common, only two studies (Sauti ya Vijana [28] and ATTACH [25]) utilized a published framework to structure the documentation of the adaptation process (the FRAME framework [30]). Most AHISA studies were affected by the COVID-19 pandemic during study implementation, which presented an opportunity to adapt intervention delivery rapidly and creatively to new platforms, such as mobile delivery of the ATTACH and MUHAS interventions [25, 47]. Given the dynamic nature of intervention implementation over time [55] and the need to be responsive to unanticipated circumstances, systematic evaluation of adaptations are critical to understand intervention optimization within given contexts as AYA research places greater focus on sustainability and scale-up.
Within implementation science, timely methodologic challenges include development and psychometric validation of implementation measures for contexts outside the US and Canada [10, 11, 56], as well as elucidating implementation strategy mechanisms and identifying moderators and mediators that activate or inhibit mechanisms [57]. Future implementation science projects in resource-limited settings have an opportunity to advance these scientific and pragmatic areas. Two studies in this review included mechanism, moderator, and mediator language. Similarly, few studies utilized validated implementation outcome measures like the acceptability, appropriateness, and feasibility measures by Weiner et al. [34]. This limited use may be warranted given the dearth of context-validated measures at this point in time. For example, one study that formally adapted and assessed validity of an implementation determinant measure of organizational readiness found that several new domains were required to reflect structural context [33], while a review and application of the CFIR to LMICs revealed the need to add a new domain and new constructs to improve compatibility for use in LMICs [37].
This review is limited in several ways. We only included studies affiliated with AHISA study teams. We did not undertake either a systematic review of all AYA HIV IS research nor a structured review of all NIH-funded studies in this area. The findings of this review are not generalizable to the broader arena of AYA HIV IS research. Some of the AHISA studies were designed when there was less discussion about the importance of harmonization, the application of implementation frameworks, the selection and operationalization of implementation outcomes, and the selection and testing of implementation strategies. As a result, much of the categorization of these items was completed by our team and may differ from how study teams might characterize their work. However, we provided study teams the opportunity to check all categorization in this manuscript to ensure accuracy. Additionally, it is a testament to the capacity-building impact of the AHISA program that protocols developed by teams after AHISA supported IS training incorporated many of these newer practices. Finally, due to less specification of implementation strategies within protocols, it was not possible to map strategies to an orienting list, such as the ERIC [16].
Conclusion
Current AHISA supported research delivers diverse EBIs and measures a range of clinical and implementation outcomes. Future studies that address lack of measurement harmonization across studies and focus on developing and validating implementation measures in heterogeneous contexts could improve development of an implementation-related foundation and improve cross-study comparisons. Additional opportunities for advancing the agenda of AYA HIV IS research include expanding the selection, specification, and testing of implementation strategies beyond the individual and interpersonal, documenting the motivation and results of adaptation of EBIs to new populations and contexts, especially resource-constrained settings, and expanding the scope of inquiry to include identification of mechanisms of action.
Data Availability
The majority of data is available through research article databases and clinicaltrials.gov. Non-publicly available protocols can be requested by contacting the lead author and PI of the AHISA-affiliated research project.
References
Idele P, Gillespie A, Porth T, Suzuki C, Mahy M, Kasedde S, et al. Epidemiology of HIV and AIDS among adolescents: current status, inequities, and data gaps. J Acquir Immune Defic Syndr. 1999;2014(66 Suppl 2):S144-153.
Han WM, Law MG, Egger M, Wools-Kaloustian K, Moore R, McGowan C, et al. Global estimates of viral suppression in children and adolescents and adults on antiretroviral therapy adjusted for missing viral load measurements: a multiregional, retrospective cohort study in 31 countries. Lancet HIV. 2021;8(12):e766–75.
Zanoni BC, Archary M, Buchan S, Katz IT, Haberer JE. Systematic review and meta-analysis of the adolescent HIV continuum of care in South Africa: the Cresting Wave. BMJ Glob Health. 2016;1(3): e000004.
Global HIV & AIDS statistics—fact sheet [Internet]. [cited 2022 Jun 28]. Available from: https://www.unaids.org/en/resources/fact-sheet.
Mark D, Armstrong A, Andrade C, Penazzato M, Hatane L, Taing L, et al. HIV treatment and care services for adolescents: a situational analysis of 218 facilities in 23 sub-Saharan African countries. J Int AIDS Soc. 2017;20(Suppl 3):21591.
Tun W, Go V, Yansaneh A. Implementation science: helping to accelerate progress toward achieving the 90-90-90 goal. AIDS Behav. 2019;23(Suppl 2):115–9.
Denison J, Pettifor A, Mofenson L, Kerrigan D. Developing an implementation science research agenda to improve the treatment and care outcomes among adolescents living with HIV in sub-Saharan Africa [Internet]. Population Council; 2016 [cited 2022 Jun 28]. Available from: https://knowledgecommons.popcouncil.org/departments_sbsr-hiv/195.
Mark D, Geng E, Vorkoper S, Essajee S, Bloch K, Willis N, et al. Making implementation science work for children and adolescents living with HIV. J Acquir Immune Defic Syndr. 1999;2018(78 Suppl 1):S58-62.
Villalobos Dintrans P, Bossert TJ, Sherry J, Kruk ME. A synthesis of implementation science frameworks and application to global health gaps. Glob Health Res Policy. 2019;4:25.
Lewis CC, Fischer S, Weiner BJ, Stanick C, Kim M, Martinez RG. Outcomes for implementation science: an enhanced systematic review of instruments using evidence-based rating criteria. Implement Sci. 2015;10(1):155.
SIRCTeam. Instrument repository [Internet]. SIRC [cited 2022 Jun 28]. Available from: https://societyforimplementationresearchcollaboration.org/measures-collection/.
Sturke R, Vorkoper S, Bekker LG, Ameyan W, Luo C, Allison S, et al. Fostering successful and sustainable collaborations to advance implementation science: the adolescent HIV prevention and treatment implementation science alliance. J Int AIDS Soc. 2020;23(Suppl 5): e25572.
Slogrove AL, Mahy M, Armstrong A, Davies MA. Living and dying to be counted: what we know about the epidemiology of the global adolescent HIV epidemic. J Int AIDS Soc. 2017;20(Suppl 3):21520.
Proctor E, Silmere H, Raghavan R, Hovmand P, Aarons G, Bunger A, et al. Outcomes for implementation research: conceptual distinctions, measurement challenges, and research agenda. Adm Policy Ment Health. 2011;38(2):65–76.
Glasgow RE, Vogt TM, Boles SM. Evaluating the public health impact of health promotion interventions: the RE-AIM framework. Am J Public Health. 1999;89(9):1322–7.
Waltz TJ, Powell BJ, Chinman MJ, Smith JL, Matthieu MM, Proctor EK, et al. Expert Recommendations for Implementing Change (ERIC): protocol for a mixed methods study. Implement Sci IS. 2014;9:39.
RTI International. Targeted interventions to address the multi-level effects of gender-based violence on PrEP uptake and adherence among adolescent girls and young women in Siaya County, Kenya [Internet]. clinicaltrials.gov; 2020 [cited 2022 Jun 27]. Report No.: NCT03938818. Available from: https://clinicaltrials.gov/ct2/show/NCT03938818.
Shahmanesh M. Isisekelo Sempilo: HIV prevention embedded in sexual health: a pilot trial to optimize peer (Thetha Nami) delivery of HIV prevention and care to adolescents and young adults in Rural KwaZulu-Natal. [Internet]. clinicaltrials.gov; 2022 [cited 2022 Jun 27]. Report No.: NCT04532307. Available from: https://clinicaltrials.gov/ct2/show/NCT04532307.
Donenberg G. Multilevel comprehensive HIV prevention package for South African adolescent girls and young women [Internet]. clinicaltrials.gov; 2021 [cited 2022 Jun 27]. Report No.: NCT04758390. Available from: https://clinicaltrials.gov/ct2/show/NCT04758390.
Thomas R, Skovdal M, Galizzi MM, Schaefer R, Moorhouse L, Nyamukapa C, et al. Improving risk perception and uptake of pre-exposure prophylaxis (PrEP) through interactive feedback-based counselling with and without community engagement in young women in Manicaland, East Zimbabwe: study protocol for a pilot randomized trial. Trials. 2019;20(1):668.
RTI International. Developing and testing a multi-level package of interventions for an integrated care delivery model of HIV prevention and treatment targeting adolescent girls in Zambia. clinicaltrials.gov; 2020 [cited 2022 Jun 27]. Report No.: NCT03995953. Available from: https://clinicaltrials.gov/ct2/show/NCT03995953.
Johns Hopkins Bloomberg School of Public Health. Transitioning adolescents to HIV self-management in Zambia (Known as: Project YES: Youth Engaging for Success) [Internet]. clinicaltrials.gov; 2019 [cited 2022 Jun 27]. Report No.: NCT04115813. Available from: https://clinicaltrials.gov/ct2/show/NCT04115813.
Zanoni B. InTSHA: interactive transition support for HIV-infected adolescents using social media [Internet]. clinicaltrials.gov; 2022 [cited 2022 Jun 27]. Report No.: NCT03624413. Available from: https://clinicaltrials.gov/ct2/show/NCT03624413.
Denison JA, Packer C, Nyambe N, Hershow RB, Caldas S, Miti S, et al. Family connections randomized controlled trial: assessing the feasibility and acceptability of an intervention with adolescents living with HIV and their caregivers in Ndola, Zambia. AIDS Care. 2022;34(4):459–68.
Njuguna IN, Beima-Sofie K, Mburu CW, Mugo C, Neary J, Itindi J, et al. Adolescent transition to adult care for HIV-infected adolescents in Kenya (ATTACH): study protocol for a hybrid effectiveness-implementation cluster randomised trial. BMJ Open. 2020;10(12): e039972.
Dow DE, Mmbaga BT, Gallis JA, Turner EL, Gandhi M, Cunningham CK, et al. A group-based mental health intervention for young people living with HIV in Tanzania: results of a pilot individually randomized group treatment trial. BMC Public Health. 2020;20(1):1358.
Dow DE, Mmbaga BT, Turner EL, Gallis JA, Tabb ZJ, Cunningham CK, et al. Building resilience: a mental health intervention for Tanzanian youth living with HIV. AIDS Care. 2018;30(sup4):12–20.
Duke University. SYV: a mental health intervention to improve HIV outcomes in Tanzanian youth [Internet]. clinicaltrials.gov; 2022 [cited 2022 Jun 27]. Report No.: NCT05374109. Available from: https://clinicaltrials.gov/ct2/show/NCT05374109.
Kamanda A, Embleton L, Ayuku D, Atwoli L, Gisore P, Ayaya S, et al. Harnessing the power of the grassroots to conduct public health research in sub-Saharan Africa: a case study from western Kenya in the adaptation of community-based participatory research (CBPR) approaches. BMC Public Health. 2013;13:91.
Wiltsey Stirman S, Baumann AA, Miller CJ. The FRAME: an expanded framework for reporting adaptations and modifications to evidence-based interventions. Implement Sci IS. 2019;14(1):58.
Holden RJ, Karsh BT. The technology acceptance model: its past and its future in health care. J Biomed Inform. 2010;43(1):159–72.
Holden RJ, Brown RL, Scanlon MC, Karsh BT. Modeling nurses’ acceptance of bar coded medication administration technology at a pediatric hospital. J Am Med Inform Assoc JAMIA. 2012;19(6):1050–8.
Means AR, Orlan E, Gwayi-Chore MC, Titus A, Kaliappan SP, Togbevi CI, et al. Structural readiness to implement community-wide mass drug administration programs for soil-transmitted helminth elimination: results from a three-country hybrid study. Implement Sci Commun. 2021;2(1):80.
Weiner BJ, Lewis CC, Stanick C, Powell BJ, Dorsey CN, Clary AS, et al. Psychometric assessment of three newly developed implementation outcome measures. Implement Sci IS. 2017;12(1):108.
Morton JF, Myers L, Gill K, Bekker LG, Stein G, Thomas KK, et al. Evaluation of a behavior-centered design strategy for creating demand for oral PrEP among young women in Cape Town, South Africa. Gates Open Res. 2020;4:29.
Moorhouse L, Schaefer R, Thomas R, Nyamukapa C, Skovdal M, Hallett TB, et al. Application of the HIV prevention cascade to identify, develop and evaluate interventions to improve use of prevention methods: examples from a study in east Zimbabwe. J Int AIDS Soc. 2019;22(Suppl 4): e25309.
Means AR, Kemp CG, Gwayi-Chore MC, Gimbel S, Soi C, Sherr K, et al. Evaluating and optimizing the consolidated framework for implementation research (CFIR) for use in low- and middle-income countries: a systematic review. Implement Sci IS. 2020;15(1):17.
Celum C. A cohort for evaluation of open-label PrEP delivery among Kenyan and South African women: the POWER cohort [Internet]. clinicaltrials.gov; 2021 [cited 2022 Jun 27]. Report No.: NCT03490058. Available from: https://clinicaltrials.gov/ct2/show/NCT03490058.
Scott JC, Van Pelt AE, Port AM, Njokweni L, Gur RC, Moore TM, et al. Development of a computerised neurocognitive battery for children and adolescents with HIV in Botswana: study design and protocol for the Ntemoga study. BMJ Open. 2020;10(8): e041099.
Thomas R, Skovdal M, Galizzi MM, Schaefer R, Moorhouse L, Nyamukapa C, et al. Improving risk perception and uptake of voluntary medical male circumcision with peer-education sessions and incentives, in Manicaland, East Zimbabwe: study protocol for a pilot randomised trial. Trials. 2020;21(1):108.
Celum CL, Gill K, Morton JF, Stein G, Myers L, Thomas KK, et al. Incentives conditioned on tenofovir levels to support PrEP adherence among young South African women: a randomized trial. J Int AIDS Soc. 2020;23(11): e25636.
Becan JE, Bartkowski JP, Knight DK, Wiley TRA, DiClemente R, Ducharme L, et al. A model for rigorously applying the Exploration, Preparation, Implementation, Sustainment (EPIS) framework in the design and measurement of a large scale collaborative multi-site study. Health Justice. 2018;6(1):9.
Larsen A, Wilson KS, Kinuthia J, John-Stewart G, Richardson BA, Pintye J, et al. Standardised patient encounters to improve quality of counselling for pre-exposure prophylaxis (PrEP) in adolescent girls and young women (AGYW) in Kenya: study protocol of a cluster randomised controlled trial. BMJ Open. 2020;10(6): e035689.
Wilson KS, Mugo C, Bukusi D, Inwani I, Wagner AD, Moraa H, et al. Simulated patient encounters to improve adolescent retention in HIV care in Kenya: study protocol of a stepped-wedge randomized controlled trial. Trials. 2017;18(1):619.
Damschroder LJ, Aron DC, Keith RE, Kirsh SR, Alexander JA, Lowery JC. Fostering implementation of health services research findings into practice: a consolidated framework for advancing implementation science. Implement Sci IS. 2009;4:50.
Taiwo B. Intensive combination approach to rollback the epidemic in Nigerian adolescents: UH3 phase [Internet]. clinicaltrials.gov; 2022 [cited 2022 Jun 27]. Report No.: NCT04950153. Available from: https://clinicaltrials.gov/ct2/show/NCT04950153.
Yamanis TJ. A pilot social network intervention to reduce HIV and IPV among adolescent girls [Internet]. [cited 2022 Jun 28]. Available from: https://reporter.nih.gov/search/TnqjPZ_l5E6lPOuq36tzew/project-details/9564984.
Iwelunmor J, Tucker JD, Obiezu-Umeh C, Gbaja-Biamila T, Oladele D, Nwaozuru U, et al. The 4 Youth by Youth (4YBY) pragmatic trial to enhance HIV self-testing uptake and sustainability: study protocol in Nigeria. Contemp Clin Trials. 2022;114: 106628.
Kemp CG, Jarrett BA, Kwon CS, Song L, Jetté N, Sapag JC, et al. Implementation science and stigma reduction interventions in low- and middle-income countries: a systematic review. BMC Med. 2019;17:6.
Kemp CG, Weiner BJ, Sherr KH, Kupfer LE, Cherutich PK, Wilson D, et al. Implementation science for integration of HIV and non-communicable disease services in sub-Saharan Africa: a systematic review. AIDS Lond Engl. 2018;32(Suppl 1):S93–105.
Wagenaar BH, Hammett WH, Jackson C, Atkins DL, Belus JM, Kemp CG. Implementation outcomes and strategies for depression interventions in low- and middle-income countries: a systematic review. Glob Ment Health Camb Engl. 2020;7: e7.
Proctor EK, Powell BJ, McMillen JC. Implementation strategies: recommendations for specifying and reporting. Implement Sci IS. 2013;8:139.
Curran GM, Bauer M, Mittman B, Pyne JM, Stetler C. Effectiveness-implementation hybrid designs: combining elements of clinical effectiveness and implementation research to enhance public health impact. Med Care. 2012;50(3):217–26.
Pintye J, Davey DLJ, Wagner AD, John-Stewart G, Baggaley R, Bekker LG, et al. Defining gaps in pre-exposure prophylaxis delivery for pregnant and post-partum women in high-burden settings using an implementation science framework. Lancet HIV. 2020;7(8):e582–92.
Chambers DA, Glasgow RE, Stange KC. The dynamic sustainability framework: addressing the paradox of sustainment amid ongoing change. Implement Sci. 2013;8(1):117.
Martinez RG, Lewis CC, Weiner BJ. Instrumentation issues in implementation science. Implement Sci. 2014;9(1):118.
Lewis CC, Klasnja P, Powell BJ, Lyon AR, Tuzzio L, Jones S, et al. From classification to causality: advancing understanding of mechanisms of change in implementation science. Front Public Health. 2018;6:136.
Ssewamala FM, Byansi W, Bahar OS, Nabunya P, Neilands TB, Mellins C, et al. Suubi+Adherence study protocol: a family economic empowerment intervention addressing HIV treatment adherence for perinatally infected adolescents. Contemp Clin Trials Commun. 2019;16:100463.
University of North Carolina, Chapel Hill. Developing and assessing a male engagement intervention in Option B+ in Malawi: a randomized controlled trial in Lilongwe. clinicaltrials.gov; 2021 [cited 2022 Jun 27]. Report No.: results/NCT03477279. Available from: https://clinicaltrials.gov/ct2/show/results/NCT03477279.
Rosenberg NE, Pettifor AE, Myers L, Phanga T, Marcus R, Bhushan NL, et al. Comparing four service delivery models for adolescent girls and young women through the “Girl Power” study: protocol for a multisite quasi-experimental cohort study. BMJ Open. 2017;7(12):e018480.
Gill K, Johnson L, Dietrich J, Myer L, Marcus R, Wallace M, Pidwell T, Mendel E, Fynn L, Jones K, Wiesner L, Slack C, Strode A, Spiegel H, Hosek S, Rooney J, Gray G, Bekker LG. Acceptability, safety, and patterns of use of oral tenofovir disoproxil fumarate and emtricitabine for HIV pre-exposure prophylaxis in South African adolescents: an open-label single-arm phase 2 trial. Lancet Child Adolesc Health. 2020;4(12):875–83. https://doi.org/10.1016/S2352-4642(20)30248-0.
Gill K, Happel AU, Pidwell T, Mendelsohn A, Duyver M, Johnson L, Meyer L, Slack C, Strode A, Mendel E, Fynn L, Wallace M, Spiegel H, Jaspan H, Passmore JA, Hosek S, Smit D, Rinehart A, Bekker LG. An open-label, randomized crossover study to evaluate the acceptability and preference for contraceptive options in female adolescents, 15 to 19 years of age in Cape Town, as a proxy for HIV prevention methods (UChoose). J Int AIDS Soc. 2020;23(10):e25626. https://doi.org/10.1002/jia2.25626.
Inwani I, Chhun N, Agot K, Cleland CM, Buttolph J, Thirumurthy H, Kurth AE, et al. High-yield HIV testing, facilitated linkage to care, and prevention for female youth in Kenya (GIRLS study): implementation science protocol for a priority population. JMIR Res Protoc. 2017;6(12):e179.
Pettifor A, Lippman SA, Kimaru L, Haber N, Mayakayaka Z, Selin A, Twine R, Gilmore H, Westreich D, Mdaka B, Wagner R, Gomez-Olive X, Tollman S, Kahn K. HIV self-testing among young women in rural South Africa: A randomized controlled trial comparing clinic-based HIV testing to the choice of either clinic testing or HIV self-testing with secondary distribution to peers and partners. EClinicalMedicine. 2020;21:100327. https://doi.org/10.1016/j.eclinm.2020.100327.
Nelson LE, Nyblade L, Torpey K, Logie CH, Qian HZ, Manu A, Gyamerah E, Boakye F, Appiah P, Turner D, Stockton M, Abubakari GM, Vlahov D. Multi-level intersectional stigma reduction intervention to increase HIV testing among men who have sex with men in Ghana: Protocol for a cluster randomized controlled trial. PLoS One. 2021;16(11):e0259324. https://doi.org/10.1371/journal.pone.0259324.
Sam-Agudu NA, Pharr JR, Bruno T, Cross CL, Cornelius LJ, Okonkwo P, Oyeledun B, Khamofu H, Olutola A, Erekaha S, Menson WNA, Ezeanolue EE. Adolescent Coordinated Transition (ACT) to improve health outcomes among young people living with HIV in Nigeria: study protocol for a randomized controlled trial. Trials. 2017;18(1):595. https://doi.org/10.1186/s13063-017-2347-z. Erratum in: Trials. 2018;19(1):104.
Subramanian S, Edwards P, Roberts ST, Musheke M, Mbizvo M. Integrated care delivery for HIV prevention and treatment in adolescent girls and young women in Zambia: protocol for a cluster-randomized controlled trial. JMIR Res Protoc. 2019;8(10):e15314. https://doi.org/10.2196/15314.
Rabin BA, Brownson RC, Haire-Joshu D, Kreuter MW, Weaver NL. A glossary for dissemination and implementation research in health. J Public Health Manag Pract. 2008;14(2):117–23. https://doi.org/10.1097/01.PHH.0000311888.
Dusenbury L, Brannigan R, Falco M, Hansen WB. A review of research on fidelity of implementation: implications for drug abuse prevention in school settings. Health Educ Res. 2003;18(2):237–56. https://doi.org/10.1093/her/18.2.237
Karsh BT. Beyond usability: designing effective technology implementation systems to promote patient safety. Qual Saf Health Care. 2004;13(5):388–94. https://doi.org/10.1136/qhc.13.5.388.
Lippman SA, Pettifor A, Rebombo D, Julien A, Wagner RG, Kang Dufour MS, Kabudula CW, Neilands TB, Twine R, Gottert A, Gómez-Olivé FX, Tollman SM, Sanne I, Peacock D, Kahn K. Evaluation of the Tsima community mobilization intervention to improve engagement in HIV testing and care in South Africa: study protocol for a cluster randomized trial. Implement Sci. 2017;12(1):9. https://doi.org/10.1186/s13012-016-0541-0.
Smith PJ, Oulo B, Wallace M, Gill K, Beijneveld JA, Bennie T, Myer L, Dietrich JJ, Johnson LF, Gray G, Bekker LG. Uptake and acceptability of medical male circumcision among young males in two culturally distinct settings in South Africa: a longitudinal, community-based study (the MACHO study). S Afr Med J. 2020;110(10):1050–5. https://doi.org/10.7196/SAMJ.2020.
Acknowledgements
The authorship team would like to thank AHISA membership teams for contributing their projects and reviewing project-specific data. We would also like to thank Rachel Sturke and Susan Vorkoper for their assistance with collecting and reviewing protocols. We would also like to thank Bill Kapogiannis, Nadia Sam Aguda, and Michael Mbizvo for early feedback on the study concept and data collection strategies.
Funding
This work was supported by the Adolescent HIV Prevention and Treatment Implementation Science Alliance (AHISA), a collaborative supported by the Center for Global Health Studies at the Fogarty International Center, the Office of the Global AIDS Coordinator, and other NIH Institutes and Centers. Support for ATLAS.ti software was provided through an ongoing AHISA small award (CRDF Global, G-202012-67159) to KBS and IN and K43TW011422-01A1 to IN. Additional support was provided by the UW Global Center for Integrated Health of Women, Adolescents and Children (Global WACh) and the University of Washington CFAR Behavioral Science Core (P30 AI027757). SMD’s efforts on this project were supported through NIH/NIAID Grant T32AI102623. ADW’s efforts on this project were supported through NIH/NIMH Grant K01MH121124. Projects reviewed in this manuscript are funded by the National Institutes of Health (NIH) or the Canadian Institute of Health Research (CIHR).
Author information
Authors and Affiliations
Contributions
KBS, IN and ADW developed the paper concept. KBS, IN, TC and SMD conducted protocol review and data abstraction. ADW, IN, and KBS wrote and revised the first drafts of the manuscript. All authors reviewed, meaningfully revised, and approved the final paper.
Corresponding author
Ethics declarations
Conflict of interest
The authors have no conflict of interest to declare.
Ethical Approval
This study did not involve human subject data and was exempt from IRB research oversight.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if changes were made. The images or other third party material in this article are included in the article's Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article's Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
Beima-Sofie, K., Njuguna, I., Concepcion, T. et al. Addressing the Know-Do Gap in Adolescent HIV: Framing and Measuring Implementation Determinants, Outcomes, and Strategies in the AHISA Network. AIDS Behav 27 (Suppl 1), 24–49 (2023). https://doi.org/10.1007/s10461-023-04021-3
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10461-023-04021-3