Abstract
Purpose
Breast cancer accounts for 30% of all female cancers in the US. Cytomegalovirus (CMV), a herpesvirus that establishes lifelong infection, may play a role in breast cancer. CMV is not oncogenic, yet viral DNA and proteins have been detected in breast tumors, indicating possible contribution to tumor development. CMV encodes cmvIL-10, a homolog of human cellular IL-10 (cIL-10) with potent immunosuppressive activities. We investigated the relationship between CMV infection, cytokines, and breast cancer.
Methods
We evaluated CMV serostatus and cytokine levels in plasma of women with benign breast disease (n = 38), in situ carcinoma (n = 41), invasive carcinoma, no lymph node involvement (Inv/LN−; n = 41), and invasive with lymph node involvement (Inv/LN+; n = 37).
Results
Fifty percent of the patient samples (n = 79) were CMV seropositive. There was no correlation between CMV status and diagnosis (p = 0.75). For CMV+ patients, there was a trend toward higher CMV IgG levels in invasive disease (p = 0.172). CmvIL-10 levels were higher in CMV+ in situ patients compared to the Inv/LN− and Inv/LN+ groups (p = 0.020). Similarly, cIL-10 levels were higher in CMV+ in situ patients compared to the Inv/LN− and Inv/LN+ groups (p = 0.043). The results were quite different in CMV− patients where cIL-10 levels were highest in Inv/LN− compared to benign, in situ, or Inv/LN+ (p = 0.019). African American patients were significantly associated with CMV+ status (p = 0.001) and had lower cmvIL-10 levels than Caucasian patients (p = 0.046).
Conclusion
No association was observed between CMV IgG and diagnosis, but CMV infection influences cytokine production and contributes to altered cytokine profiles in breast cancer.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Breast cancer is the second leading cause of cancer deaths for women in the United States. Although women with localized tumors have a 5-year survival rate near 100%, women with invasive tumors that spread to distant sites have a 5-year survival rate of only 30% [1, 2]. Identification of factors that promote in situ tumors to become invasive is necessary to improve treatment options and increase overall survival in breast cancer patients.
One factor linked to invasive breast cancer is human cytomegalovirus (CMV) [3,4,5]. CMV is a herpesvirus that establishes lifelong latent infection in 70% to 90% of the general population [6]. CMV periodically reactivates but typically causes clinical disease only in immunocompromised people. However, over a lifetime, CMV may reduce immune function [7,8,9], contribute to chronic conditions [10,11,12], and promote tumor progression [13,14,15,16].
CMV has been associated with tumor progression and metastatic spread [17]. For example, CMV antibody levels are higher in women with invasive breast cancer than in healthy women [18, 19]. Also, CMV DNA and proteins have been found in tumor biopsy samples and are associated with more invasive tumors [5, 20], higher tumor grade [21], and poor overall survival [22, 23]. Microbiome analysis of women with breast cancer revealed high levels of CMV [24]. CMV broadly influences host immune responses and may impact the ability of cancer cells to evade immune detection [25]. Of note, CMV encodes cmvIL-10, a viral cytokine and ortholog of human cellular interleukin-10 (cIL-10) with potent immune suppressive properties [26,27,28,29]. Immune suppression in the tumor microenvironment is a key factor in progression from localized to invasive tumors [30].
While cmvIL-10 is best known for immune suppression, this viral cytokine can also stimulate growth of tumor cells [31, 32]. CmvIL-10 that was produced by patient-derived glioma stem cells in culture was shown to enhance cell migration and invasion, thereby influencing the progression of malignant glioma [32]. Also, breast cancer cells exposed to cmvIL-10 in vitro exhibited enhanced cell proliferation, migration, and Matrigel invasion [33,34,35]. CmvIL-10 has the potential to impact any cell expressing the cIL-10 receptor, including tumor cells and the immune cells responding to the tumor.
To learn whether high levels of cmvIL-10 were associated with invasive breast cancer, we examined CMV serostatus and cytokine levels in a population of women with varying stages of breast disease. Previously collected plasma samples from patients with benign breast disease, in situ carcinoma, invasive carcinoma with no lymph node involvement (Inv/LN−), and invasive carcinoma with lymph node involvement (Inv/LN+) were evaluated by ELISA for CMV IgG, cmvIL-10, and human cIL-10, IL-6, and TNFα. We hypothesized that cmvIL-10 and cIL-10 levels would be highest in samples from patients with more invasive breast disease, indicating an immune suppressive environment that enabled tumor cells to escape ductal walls and invade surrounding tissue.
Methods
Patient samples
Samples for the study were from the CBCP biobank, a large tissue and blood repository of samples from women undergoing treatment for various types of breast disease. Plasma specimens were selected from retrospective collections of the CBCP. Based on disease status, they were grouped as benign (n = 38), in situ carcinoma (n = 41), invasive carcinoma with no lymph node involvement (n = 41) and invasive carcinoma with lymph node involvement (n = 37). Plasma was collected from most patients at the time of diagnosis (n = 105). In some patients with invasive carcinoma (Inv/LN− or Inv/LN+), plasma was collected following chemotherapy treatment (n = 52).
Enzyme linked immunosorbent assay (ELISA)
Plasma specimens were analyzed for CMV IgG via commercial assay (Trinity Biotech, Jamestown, NY) according to the manufacturer’s instructions. Briefly, the Immune Status Ratio (ISR) was determined using a ratio of optical density readings from the sample and a calibrator. Cytokine levels were analyzed using Human cIL-10, IL-6, and TNFα Duo Set ELISA kits according to the manufacturer’s instructions (R&D Systems, Minneapolis, MN). Measurement of cmvIL-10 was performed via ELISA using goat polyclonal antiserum as described previously [36]. For all cytokine ELISAs, protein concentrations (pg/ml) were determined by interpolation from a standard curve. Cytokine values measured in pg/ml were natural log transformed for statistical analyses.
Statistical analysis
Cytokine values were log transformed and analyzed using R statistical software. Statistical tests were applied to these data. The Wilcoxon rank sum test was used for testing the difference of numeric variables across two groups. The Chi-squared test and Fisher’s exact test were applied to evaluate the association of two categorical variables. One-way Analysis of Variance (ANOVA) and Kruskal–Wallis rank sum test (non-parametric test for ANOVA) were used to test numeric differences between multiple groups. When the normality assumption of ANOVA was not met, the Kruskal–Wallis rank sum test was used. Linear regression was performed to test the difference between disease diagnoses or evaluate the effect of sample collection time (at diagnosis vs after treatment).
Results
Study population
A total of 157 patient plasma samples were obtained from the CBCP biobank. The characteristics of the study population are shown in Table 1. The mean age of all patients included in this study at time of diagnosis was 51.0 years. The majority of patient samples were collected at time of diagnosis. For some patients with a diagnosis of invasive carcinoma (Inv/LN− or Inv/LN+), plasma samples were collected post treatment (Table 2).
To learn which patients harbored human CMV, plasma samples were tested for immunoglobulin G (IgG) specific for CMV. Patients were designated as CMV seropositive (CMV+) or seronegative (CMV−) based on the presence of CMV IgG. Fifty percent of the samples (n = 79) were CMV+ (Table 1). There was no significant difference in age at time of diagnosis between the CMV+ (52.2 ± 10.6) and CMV− (49.9 ± 9.8) groups. Likewise, there was no association between disease diagnosis and CMV status (p = 0.75). Race was significantly associated with CMV serostatus, and African American patients were predominantly CMV+ (20/22 participants) (p < 0.001).
CMV IgG levels
We next examined whether CMV IgG levels were associated with disease severity by evaluating the Immune Status Ratio (ISR). An ISR value over 1.1 is considered seropositive, but many patients have ISR values well above this level. Higher ISR values could indicate elevated levels of circulating IgG specific to CMV due to recent infection or virus reactivation. No significant differences in CMV + IgG levels were detected between the disease groups (Fig. 1, p = 0.172). However, a trend toward higher CMV + IgG levels in the Inv/LN− group was observed.
Cytokine levels
To learn whether cytokine levels were associated with disease severity, we measured three human cytokines in patient plasma samples: cIL-10, TNFα, and IL-6. There were no significant differences in human cIL-10 levels between disease groups in the overall study population (p = 0.252) (Fig. 2A). However, there were significant differences in cIL-10 levels among CMV+ patients (p = 0.043). CMV+ patients with a diagnosis of in situ carcinoma had higher cIL-10 levels than those with Inv/LN−, Inv/LN+, or Inv/LN− and LN + combined (p = 0.008, 0.031, and 0.005, respectively) (Table 3). Surprisingly, the results were quite different in the CMV− population. A difference was detected across the patient groups (p = 0.019); specifically, cIL-10 levels were significantly higher in patients with Inv/LN− compared to those with benign disease, in situ, or Inv/LN+ (p = 0.010, 0.011, and 0.012, respectively) (Table 3). In summary, the highest cIL-10 levels were observed in the in situ group for CMV+ patients, whereas cIL-10 levels were highest in the Inv/LN− group for CMV− patients (Fig. 2A).
Log cytokine levels in patients with breast disease. A Human cIL-10 levels for all patients in the study (n = 157), CMV+ patients only (n = 79), or CMV− patients (n = 78). B TNFα levels for all patients, CMV+, or CMV− patients. C IL-6 levels for all patients, CMV+, or CMV− patients. All statistical analyses were performed by one-way ANOVA (A, B) or Kruskal–Wallis one-way ANOVA (C)
A similar trend was observed for TNFα (Fig. 2B). There were no significant differences in TNFα levels between disease groups for the overall study population (p = 0.468). When stratified for CMV status, however, clear differences emerged. In the CMV+ group, although the difference did not achieve statistical significance, TNFα levels were higher in patients with benign and in situ disease compared to Inv/LN− and Inv/LN+ (p = 0.196) (Fig. 2B). Patients with in situ disease had higher TNFα levels than Inv/LN+ or Inv/LN− and Inv/LN+ combined (p = 0.073) (Table 3). For CMV− patients, TNFα levels were highest in the Inv/LN− group compared to those with benign disease, in situ, or Inv/LN+ (p = 0.055) (Table 3).
For IL-6, no significant differences among disease groups for the overall study population were noted (p = 0.409) (Fig. 2C). Among CMV+ patients, the highest levels of IL-6 were in the in situ group (p = 0.106), and the difference between IL-6 levels in in situ and Inv/LN+ was significant (p = 0.024) (Table 3). For the CMV− group, we observed the highest levels of IL-6 in the Inv/LN− patients (p = 0.115) approaching statistical significance (Table 3). Among these CMV− patients, the Inv/LN− patients had significantly higher IL-6 levels than in situ group (p = 0.030) (Table 3).
We next evaluated cmvIL-10 levels in CMV+ patients and found no significant difference in cmvIL-10 across all four disease groups (p = 0.108) (Fig. 3A). However, the in situ patients had significantly higher cmvIL-10 levels than the Inv/LN− (p = 0.014) (Fig. 3B) and the combined Inv/LN− and Inv/LN+ groups (p = 0.020) (Fig. 3C). The relative expression pattern for cmvIL-10 was reminiscent of that observed for cIL-10 levels in the CMV+ group (Fig. 2A). Notably, among CMV+ patients, the cmvIL-10 levels were significantly higher in Caucasian patients than in African American patients (p = 0.046) (Fig. 3D). There were no differences by race in either CMV+ or CMV− patients for the other cytokines evaluated (cIL-10, IL-6, or TNFα). Additionally, we evaluated whether sample collection time (at diagnosis vs after treatment) contributed to the differences in cytokine levels in either CMV+ or CMV− patients. We found there was no impact of sample collection time on differences in cytokine levels (Table 2).
Log cmvIL-10 levels in CMV+ patients with breast disease. A Comparison of cmvIL-10 levels among all groups. B Comparison between in situ and invasive without lymph node involvement (Inv/LN−). C Comparison between the in situ group and the Inv/LN− and Inv/LN+ groups combined. D Comparison of cmvIL-10 levels between CMV+ patients in all disease groups by race (CMV+/African American, n = 20, CMV+/Caucasian, n = 52). Statistical analysis performed via *one-way ANOVA and ΔWilcoxon rank sum test
The overall trend in this study was that cytokine profiles differed with respect to CMV serostatus (Fig. 4). In CMV+ patients, the highest cytokine levels were observed in the in situ group, with lower cytokine levels in the Inv/LN− group (Fig. 4A). CMV+ women with invasive carcinoma had the lowest levels of cmvIL-10 and cIL-10, which is the opposite of our initial prediction. In contrast, in CMV− women, the highest cytokine levels were in the Inv/LN− group, and levels in the in situ group were significantly lower (Fig. 4B). These results suggest that CMV infection impacts patterns of cytokine production in breast cancer.
Discussion
We set out to investigate the relationship between CMV infection and breast disease diagnosis. We evaluated CMV IgG and cytokine levels in patients with different types of breast disease, and we hypothesized that cytokine levels would be higher in patients with more invasive disease. Our hypothesis was partially correct. Cytokine levels were highest in patients with invasive disease, but this was only true for individuals who were negative for CMV (Fig. 4B). A striking difference was observed in CMV+ patients, where cytokine levels were lowest in patients with more invasive disease (Fig. 4A). Our results demonstrate that the relationship between breast disease stage and cytokine levels is complex and dependent on CMV status. These findings suggest that CMV infection strongly influences patterns of cytokine production in breast cancer.
We did not observe any association between CMV IgG status and breast disease diagnosis. CMV serostatus has not been positively associated with breast cancer except in a few specific cases. One study of Iranian women found CMV IgG was more prevalent in women with breast cancer (n = 49) compared to healthy controls (n = 49, 94% vs 69% seropositivity, p = 0.002) [37]. A study of Iraqi women reported that 100% of women with malignant breast cancer (n = 60) were positive for CMV IgG, and 8.3% of those women were positive for CMV IgM, suggesting a recent infection or reactivation [38]. However, in the Iraqi study, CMV was also widespread in women with benign breast disease (n = 20, 95% CMV+) and in healthy controls (n = 10, 90% CMV+), indicating a high level of CMV infection in the Iraqi population overall. In contrast, a study of breast cancer survivors in the United Kingdom reported no significant differences in seroprevalence between survivors (n = 38, 44.4% CMV+) and healthy women (n = 27, 44.7% CMV+) [39]. Likewise, there was no difference in CMV seropositivity between Australian women with breast cancer (n = 208, 59% CMV+) and healthy controls (n = 168, 57% CMV+) [18]. The patient samples analyzed in our study were all collected in the US from women ages 25 to 69, and overall CMV seroprevalence was 50.3%, which is more comparable to the UK and Australian studies than the Iranian and Iraqi studies. CMV seroprevalence in the population varies widely based on factors such as age, race, ethnicity, geography, socioeconomic status, education level, and healthcare disparities [40].
While CMV seropositivity is not strongly associated with breast cancer, there are significant differences in CMV IgG levels between breast cancer patients and healthy women [18, 19, 39]. The same Australian study reported higher mean CMV IgG levels in women with breast cancer compared to controls, and this was notable because there was no difference in IgG levels specific for another common herpesvirus, Epstein-Barr virus (EBV) [18]. A long-term Norwegian study found that elevated CMV IgG levels preceded development of breast cancer, yet there was no correlation with EBV IgG levels [19]. The UK study reported higher CMV IgG levels in breast cancer survivors compared to healthy controls, although the difference was not statistically significant [39]. Similarly, we saw a trend toward higher IgG levels in women with invasive carcinoma (Inv/LN−) compared to women with benign breast disease or in situ carcinoma (Fig. 1), but our sample size for each diagnosis was relatively small. Of note, we observed that CMV IgG levels were lowest in patients with the most invasive disease (Inv/LN+), suggesting that the relationship between CMV IgG levels and disease severity is not a linear correlation. Tumor progression is influenced by many factors, and our results suggest that these factors may include the presence of CMV, the status of the infection, and the level of immune response to the virus.
One focus of this study was to examine cmvIL-10 levels in breast cancer to evaluate any potential use as a biomarker for tumor progression or disease severity. Although we expected higher cmvIL-10 levels to correlate with immune suppression and therefore, more severe or invasive disease diagnosis, we found just the opposite. We observed the highest cmvIL-10 levels in individuals with in situ tumors (Fig. 3A). The level of cmvIL-10 was lower in patients with invasive tumors (Fig. 3B, C), which could indicate a change in CMV activation or replication when tumor cells break out of the encapsulated environment to invade the surrounding tissue. One possibility is that high cmvIL-10 levels in patients with an in situ diagnosis reflect a period of active virus replication, perhaps due to immune suppression or other stressors, creating a perfect storm of conditions that allow tumor cells to break through the ductal walls and invade surrounding breast tissue. Once this breakthrough event happens, an inflammatory immune response may be induced, and the tumor microenvironment would likely change dramatically. As the immune system rebounds and fights off virus infection, the immune cells may be unable to reverse the tumor invasion that has already occurred. This surge of immune activity could account for the lower levels of both cmvIL-10 and human cIL-10 observed in patients with invasive tumors. In glioblastoma multiforme (GBM) tumors, glioma cancer stem cells were found to be CMV+ and secrete cmvIL-10, influencing monocyte function, creating an immune suppressive environment, and promoting tumor progression [32].
Another possible explanation for our results is that lower levels of cmvIL-10 in invasive disease are due to the activity of neutralizing antibodies that eliminate cmvIL-10 from the bloodstream. Neutralizing antibodies to cmvIL-10 have been detected in both humans [36] and Rhesus macaques [41, 42], but any connection between cmvIL-10 neutralizing antibodies and tumor progression remains to be explored. There are many factors that contribute to tumor progression, and not all lesions do progress from in situ to invasive. Some in situ lesions remain localized for years without ever becoming invasive, and there is currently no reliable test to identify lesions with invasive potential [43]. Progress is being made toward identifying gene signatures that predict likelihood of invasion [44, 45], but more research is needed to understand the complex processes that govern tissue invasion.
We also found that cmvIL-10 levels were significantly lower among African American study participants compared to Caucasian participants (Fig. 4D). This finding is consistent with previous reports that CMV seroprevalence is higher in non-Caucasian populations [46, 47]; however, it is unclear whether the differences observed here may relate to differences in tumor status, CMV replication, immune function, or other factors. Notably, there was no difference in human cIL-10, TNFα, or IL-6 levels between African American and Caucasian study participants. A study of healthy adults in California reported higher levels of C-reactive protein (CRP) and IL-6 in African Americans compared to Caucasians, but no difference in cIL-10 or TNFα levels [48]. In this study, we also did not observe any correlation between cmvIL-10 levels and age, although a correlation with age was reported in a Taiwanese study of CMV+ patients with Aspergillus infection [49].
The patient plasma samples analyzed here represent single snapshots in time from individual patients with the same diagnosis. There were no serial samples from the same patient as disease progressed, so we did not have the opportunity to evaluate changes over time. However, even with our small sample size, we did see highly significant differences in cytokine levels between diagnosis groups with opposite profiles in CMV+ vs. CMV− patients. These results strongly suggest that either CMV has some influence in the progression of breast cancer, or conversely, that the progression of cancer has some influence over CMV reactivation and latency.
The majority of plasma samples in this study were drawn at the time of diagnosis. Among patients with invasive carcinoma with (Inv/LN+) or without lymph node involvement (Inv/LN−), some samples were collected after treatment with chemotherapeutic agents. Chemotherapy can suppress the immune system, making patients more susceptible to infections, including CMV reactivation. However, there is currently no evidence to suggest that chemotherapy directly triggers CMV reactivation. One report found no evidence of CMV reactivation following chemotherapy in a study of 93 patients with solid organ tumors in Turkey [50]. Our analysis found no significant impact of treatment on cytokine levels (Table 2), further supporting the notion that differences in cytokine levels are primarily due to CMV status and disease diagnosis.
It is also worth noting that this study relied on plasma from women with a diagnosis of breast disease, not a tissue biopsy sample from the site of the lesion. Direct analysis of tumor tissue, typically by immunohistochemistry staining or molecular techniques, can provide valuable information about gene expression patterns and protein localization and abundance, identifying potential disease markers or therapeutic targets within the tumor microenvironment. A logical future extension of this study would be to further stratify diagnoses by hormone receptor expression or other tumor markers. Regrettably, we did not have this information for all patient samples analyzed here. On the other hand, biopsy samples are typically processed by formalin fixation, paraffin embedded tissue, which may result in masking or modification of some antigens, formation of artifacts, and degradation of nucleic acids. By comparison, plasma samples reflect the state of the whole body, and it is remarkable to see such profound differences in systemic cytokine patterns between CMV+ and CMV− women with different diagnoses of breast disease. A particular strength of this study is that we stratified the data by diagnosis, making a distinction between invasive carcinoma with lymph node involvement (Inv/LN+) or without (Inv/LN−). Our analysis revealed stark differences between CMV+ and CMV− cytokine profiles not only between in situ and invasive disease, but between invasive with or without lymph node involvement (Fig. 2A, Table 3). Further analysis of CMV status and plasma cytokines may result in profiles that could be combined with other biomarkers such as circulating tumor DNA in liquid biopsies [51] to actively monitor tumor dynamics and response to treatment.
CMV establishes lifelong latent infection in the host. It is now widely understood that the viruses, bacteria, and fungi that make up the human microbiome play a significant role in human health and disease, and they can profoundly influence tumor development [52, 53]. In a murine breast cancer model, the microbiome profoundly impacted tumor development [54]. Tissue-resident intracellular bacteria enhanced survival of circulating tumor cells and strongly promoted metastatic spreading to the lungs [54]. The number of lung metastases were reduced when mice were administered antibiotics, confirming the role of the tumor microbiota in metastasis formation. In addition, commensal fungi have been observed to colonize pancreatic tumors, stimulating production of IL-33 and suppressing anti-tumor immune responses [55]. Our results clearly indicate a relationship between CMV status and systemic cytokine response in women with breast cancer, but these observations lead to more questions than they answer. In women with CMV, cytokine levels were higher in in situ and lower in invasive disease (LN−/LN+). But in women without CMV, cytokine levels were lower in situ and higher in invasive disease (LN−/LN+). We do not yet know whether this indicates that CMV infection may suppress anti-tumor responses, or if patients with CMV already have elevated cytokine levels due to virus infection, and those levels decrease in concert with tumor progression. While a profound difference in cytokine production was observed here between CMV+ and CMV− patients, more research is needed to fully understand the impact of CMV on breast cancer.
Data availability
No datasets were generated or analysed during the current study.
References
Cardoso F, Senkus E, Costa A, Papadopoulos E, Aapro M, Andre F, Harbeck N, Aguilar Lopez B, Barrios CH, Bergh J et al (2018) 4th ESO-ESMO international consensus guidelines for advanced breast cancer (ABC 4)dagger. Ann Oncol 29(8):1634–1657
Cardoso F, Spence D, Mertz S, Corneliussen-James D, Sabelko K, Gralow J, Cardoso MJ, Peccatori F, Paonessa D, Benares A et al (2018) Global analysis of advanced/metastatic breast cancer: decade report (2005–2015). The Breast 39:131–138
Harkins LE, Matlaf LA, Soroceanu L, Klemm K, Britt WJ, Wang W, Bland KI, Cobbs CS (2010) Detection of human cytomegalovirus in normal and neoplastic breast epithelium. Herpesviridae 1(1):8
Taher C, de Boniface J, Mohammad AA, Religa P, Hartman J, Yaiw KC, Frisell J, Rahbar A, Soderberg-Naucler C (2013) High prevalence of human cytomegalovirus proteins and nucleic acids in primary breast cancer and metastatic sentinel lymph nodes. PLoS ONE 8(2):e56795
Yang Z, Tang X, Hasing ME, Pang X, Ghosh S, McMullen TPW, Brindley DN, Hemmings DG (2022) Human cytomegalovirus seropositivity and viral DNA in breast tumors are associated with poor patient prognosis. Cancers (Basel) 14(5):1148
Mocarski ES, Shenk T, Pass RF (2006) Cytomegaloviruses. Lippincott-Raven Publishers, Philadelphia
Shen HC, Feng JY, Sun CY, Huang JR, Chen YM, Chen WC, Yang KY (2023) Analysis of the effect of cytomegalovirus infection in clinical outcomes and prolonged duration of SARS-CoV-2 shedding in intensive care unit patients with COVID-19 pneumonia. Ther Adv Respir Dis 17:17534666231209150
Unterberg M, Ehrentraut SF, Bracht T, Wolf A, Haberl H, von Busch A, Rump K, Ziehe D, Bazzi M, Thon P et al (2023) Human cytomegalovirus seropositivity is associated with reduced patient survival during sepsis. Crit Care 27(1):417
Ziehe D, Wolf A, Rahmel T, Nowak H, Haberl H, Bergmann L, Rump K, Dyck B, Palmowski L, Marko B et al (2024) Exploring the relationship between HCMV serostatus and outcomes in COVID-19 sepsis. Front Immunol 15:1386586
Jeremiah SS, Moin ASM, Butler AE (2024) Virus-induced diabetes mellitus: revisiting infection etiology in light of SARS-CoV-2. Metabolism 156:155917
Naceur I, Skhiri S, Ben Achour T, Said F, Smiti M, Ben Ghorbel I, Houman MH (2023) Particularities of infectious complications in systemic lupus erythematosus. Tunis Med 101(11):821–825
Ji Q, Lian W, Meng Y, Liu W, Zhuang M, Zheng N, Karlsson IK, Zhan Y (2024) Cytomegalovirus infection and Alzheimer’s disease: a meta-analysis. J Prev Alzheimers Dis 11(2):422–427
Soroceanu L, Matlaf L, Khan S, Akhavan A, Singer E, Bezrookove V, Decker S, Ghanny S, Hadaczek P, Bengtsson H et al (2015) Cytomegalovirus immediate-early proteins promote stemness properties in glioblastoma. Cancer Res 75(15):3065–3076
Utrera-Barillas D, Valdez-Salazar HA, Gomez-Rangel D, Alvarado-Cabrero I, Aguilera P, Gomez-Delgado A, Ruiz-Tachiquin ME (2013) Is human cytomegalovirus associated with breast cancer progression? Infect Agent Cancer 8(1):12
Soroceanu L, Matlaf L, Bezrookove V, Harkins L, Martinez R, Greene M, Soteropoulos P, Cobbs CS (2011) Human cytomegalovirus US28 found in glioblastoma promotes an invasive and angiogenic phenotype. Cancer Res 71(21):6643–6653
Michaelis M, Doerr HW, Cinatl J (2009) The story of human cytomegalovirus and cancer: increasing evidence and open questions. Neoplasia 11(1):1–9
Richardson AK, Walker LC, Cox B, Rollag H, Robinson BA, Morrin H, Pearson JF, Potter JD, Paterson M, Surcel HM et al (2020) Breast cancer and cytomegalovirus. Clin Transl Oncol 22(4):585–602
Richardson AK, Cox B, McCredie MR, Dite GS, Chang JH, Gertig DM, Southey MC, Giles GG, Hopper JL (2004) Cytomegalovirus, Epstein-Barr virus and risk of breast cancer before age 40 years: a case-control study. Br J Cancer 90(11):2149–2152
Cox B, Richardson A, Graham P, Gislefoss RE, Jellum E, Rollag H (2010) Breast cancer, cytomegalovirus and Epstein-Barr virus: a nested case-control study. Br J Cancer 102(11):1665–1669
Sepahvand P, Makvandi M, Samarbafzadeh A, Talaei-Zadeh A, Ranjbari N, Nisi N, Azaran A, Jalilian S, Pirmoradi R, Makvandi K et al (2019) Human cytomegalovirus DNA among women with breast cancer. Asian Pac J Cancer Prev 20(8):2275–2279
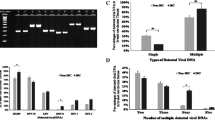
El-Shinawi M, Mohamed HT, Abdel-Fattah HH, Ibrahim SA, El-Halawany MS, Nouh MA, Schneider RJ, Mohamed MM (2016) Inflammatory and non-inflammatory breast cancer: a potential role for detection of multiple viral DNAs in disease progression. Ann Surg Oncol 23(2):494–502
Ahmed R, Yussif Y (2016) Immunohistochemical detection of human cytomegalovirus, Epstein-Barr virus and human papillomavirus in invasive breast carcinoma in Egyptian women: a tissue microarray study. J Solid Tumors 6(2):8–16
Touma J, Pantalone MR, Rahbar A, Liu Y, Vetvik K, Sauer T, Soderberg-Naucler C, Geisler J (2023) Human cytomegalovirus protein expression is correlated with shorter overall survival in breast cancer patients: a cohort study. Viruses 15(3):732
Banerjee S, Wei Z, Tian T, Bose D, Shih NNC, Feldman MD, Khoury T, De Michele A, Robertson ES (2021) Prognostic correlations with the microbiome of breast cancer subtypes. Cell Death Dis 12(9):831
Scalzo AA, Corbett AJ, Rawlinson WD, Scott GM, Degli-Esposti MA (2007) The interplay between host and viral factors in shaping the outcome of cytomegalovirus infection. Immunol Cell Biol 85(1):46–54
Spencer JV, Lockridge KM, Barry PA, Lin G, Tsang M, Penfold ME, Schall TJ (2002) Potent immunosuppressive activities of cytomegalovirus-encoded interleukin-10. J Virol 76(3):1285–1292
Slobedman B, Barry PA, Spencer JV, Avdic S, Abendroth A (2009) Virus-encoded homologs of cellular interleukin-10 and their control of host immune function. J Virol 83(19):9618–9629
Moore KW, de Waal MR, Coffman RL, O’Garra A (2001) Interleukin-10 and the interleukin-10 receptor. Annu Rev Immunol 19:683–765
Mosser DM, Zhang X (2008) Interleukin-10: new perspectives on an old cytokine. Immunol Rev 226:205–218
Gil Del Alcazar CR, Huh SJ, Ekram MB, Trinh A, Liu LL, Beca F, Zi X, Kwak M, Bergholtz H, Su Y et al (2017) Immune escape in breast cancer during in situ to invasive carcinoma transition. Cancer Discov 7(10):1098–1115
Spencer JV, Cadaoas J, Castillo PR, Saini V, Slobedman B (2008) Stimulation of B lymphocytes by cmvIL-10 but not LAcmvIL-10. Virology 374(1):164–169
Dziurzynski K, Wei J, Qiao W, Hatiboglu MA, Kong LY, Wu A, Wang Y, Cahill D, Levine N, Prabhu S et al (2011) Glioma-associated cytomegalovirus mediates subversion of the monocyte lineage to a tumor propagating phenotype. Clin Cancer Res 17(14):4642–4649
Valle Oseguera CA, Spencer JV (2014) cmvIL-10 stimulates the invasive potential of MDA-MB-231 breast cancer cells. PLoS ONE 9(2):e88708
Bishop R, Valle Oseguera CA, Spencer JV (2015) Human cytomegalovirus interleukin-10 promotes proliferation and migration of MCF-7 breast cancer cells. Cancer Cell Microenviron 2(1):e678
Valle Oseguera CA, Spencer JV (2017) Human cytomegalovirus interleukin-10 enhances matrigel invasion of MDA-MB-231 breast cancer cells. Cancer Cell Int 17:24
Young VP, Mariano MC, Tu CC, Allaire KM, Avdic S, Slobedman B, Spencer JV (2017) Modulation of the host environment by human cytomegalovirus with viral interleukin 10 in peripheral blood. J Infect Dis 215(6):874–882
Nakhaie M, Charostad J, Azaran A, Arabzadeh SAM, Motamedfar A, Iranparast S, Ahmadpour F, Talaeizadeh A, Makvandi M (2021) Molecular and serological prevalence of HCMV in Iranian patients with breast cancer. Asian Pac J Cancer Prev 22(7):2011–2016
AlNuaimi BN, Al-Assawi RH, Naji RZ (2018) Serodiagnosis of human cytomegalovirus in Iraqi breast cancer and fibroadenoma patients. Curr Res Microbiol Biotechnol 6(1):1466–1469
Arana Echarri A, Struszczak L, Beresford M, Campbell JP, Jones RH, Thompson D, Turner JE (2023) Immune cell status, cardiorespiratory fitness and body composition among breast cancer survivors and healthy women: a cross sectional study. Front Physiol 14:1107070
Fowler K, Mucha J, Neumann M, Lewandowski W, Kaczanowska M, Grys M, Schmidt E, Natenshon A, Talarico C, Buck PO et al (2022) A systematic literature review of the global seroprevalence of cytomegalovirus: possible implications for treatment, screening, and vaccine development. BMC Public Health 22(1):1659
Deere JD, Chang WLW, Villalobos A, Schmidt KA, Deshpande A, Castillo LD, Fike J, Walter MR, Barry PA, Hartigan-O’Connor DJ (2019) Neutralization of rhesus cytomegalovirus IL-10 reduces horizontal transmission and alters long-term immunity. Proc Natl Acad Sci USA 116(26):13036–13041
Logsdon NJ, Eberhardt MK, Allen CE, Barry PA, Walter MR (2011) Design and analysis of rhesus cytomegalovirus IL-10 mutants as a model for novel vaccines against human cytomegalovirus. PLoS ONE 6(11):e28127
Bergholtz H, Lien TG, Swanson DM, Frigessi A, Oslo Breast Cancer Research C, Daidone MG, Tost J, Warnberg F, Sorlie T (2020) Contrasting DCIS and invasive breast cancer by subtype suggests basal-like DCIS as distinct lesions. NPJ Breast Cancer 6:26
Xu H, Lien T, Bergholtz H, Fleischer T, Djerroudi L, Vincent-Salomon A, Sorlie T, Aittokallio T (2021) Multi-omics marker analysis enables early prediction of breast tumor progression. Front Genet 12:670749
Zheng ZY, Elsarraj H, Lei JT, Hong Y, Anurag M, Feng L, Kennedy H, Shen Y, Lo F, Zhao Z et al (2022) Elevated NRAS expression during DCIS is a potential driver for progression to basal-like properties and local invasiveness. Breast Cancer Res 24(1):68
Lantos PM, Permar SR, Hoffman K, Swamy GK (2015) The excess burden of cytomegalovirus in African American communities: a geospatial analysis. Open Forum Infect Dis 2(4):ofv180
Winter JR, Taylor GS, Thomas OG, Jackson C, Lewis JEA, Stagg HR (2020) Factors associated with cytomegalovirus serostatus in young people in England: a cross-sectional study. BMC Infect Dis 20(1):875
Paalani M, Lee JW, Haddad E, Tonstad S (2011) Determinants of inflammatory markers in a bi-ethnic population. Ethn Dis 21(2):142–149
Huang SF, Huang YC, Lee CT, Chou KT, Chen HP, Huang CC, Ji DD, Chan YJ, Yang YY (2022) Cytomegalovirus viral interleukin-10 in patients with Aspergillus infection and effects on clinical outcome. Mycoses 65(7):760–769
Demirel A, Nur Pilanci K, Inan N, Iris NE, Baygul A, Desmir G, Sonmez E (2021) Investigation of the effect of chemotherapy on cytomegalovirus reactivity in patients with solid organ tumors. Eur Res J 7(1):38–43
Mazzitelli C, Santini D, Corradini AG, Zamagni C, Trere D, Montanaro L, Taffurelli M (2023) Liquid biopsy in the management of breast cancer patients: where are we now and where are we going. Diagnostics (Basel) 13(7):1241
Papakonstantinou A, Nuciforo P, Borrell M, Zamora E, Pimentel I, Saura C, Oliveira M (2022) The conundrum of breast cancer and microbiome—a comprehensive review of the current evidence. Cancer Treat Rev 111:102470
Wang N, Sun T, Xu J (2021) Tumor-related microbiome in the breast microenvironment and breast cancer. J Cancer 12(16):4841–4848
Fu A, Yao B, Dong T, Chen Y, Yao J, Liu Y, Li H, Bai H, Liu X, Zhang Y et al (2022) Tumor-resident intracellular microbiota promotes metastatic colonization in breast cancer. Cell 185(8):1356-1372 e1326
Alam A, Levanduski E, Denz P, Villavicencio HS, Bhatta M, Alhorebi L, Zhang Y, Gomez EC, Morreale B, Senchanthisai S et al (2022) Fungal mycobiome drives IL-33 secretion and type 2 immunity in pancreatic cancer. Cancer Cell 40(2):153-167 e111
Shriver CD (2010) 21st century paradigm of tissue banking: the Clinical Breast Care Project. Mil Med 175(7 Suppl):49–53
Acknowledgements
We are grateful to the women who participated in the Clinical Breast Care Project.
Disclaimer
The contents of this publication are the sole responsibility of the author(s) and do not necessarily reflect the views, opinions, or policies of Uniformed Services University of the Health Sciences (USUHS), the Henry M. Jackson Foundation for the Advancement of Military Medicine, Inc., the Department of Defense (DoD) or the Departments of the Army, Navy, or Air Force. Mention of trade names, commercial products, or organizations does not imply endorsement by the U.S. government.
Funding
Open access funding provided by SCELC. Funding for this study was provided in part by the Uniformed Services University of the Health Sciences (USUHS) through the Henry M. Jackson Foundation for the Advancement of Military Medicine, Inc., #HU0001-19-20058/#5171 (CDS/HH) and #HU0001-21-20001/#5686. The funders had no role in the study design, data collection and analysis, decision to publish, or preparation of the manuscript.
Author information
Authors and Affiliations
Contributions
J.V.S. performed cytokine testing, wrote the main manuscript text, and helped prepare all figures and tables. J.L. performed statistical analysis and prepared data figures and tables. B.D. and S.S. identified patient samples for testing. All authors provided critical feedback and reviewed the manuscript.
Corresponding author
Ethics declarations
Conflict of interest
The authors declare no competing interests. H.H. is a co-founder and shareholder of miRoncol Diagnostics, Inc.
Ethical approval
The study was performed under a HIPAA-compliant, Institutional Review Board-approved protocol of the Clinical Breast Care Project (CBCP) [56].
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if changes were made. The images or other third party material in this article are included in the article's Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article's Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
Spencer, J.V., Liu, J., Deyarmin, B. et al. Cytokine levels in breast cancer are highly dependent on cytomegalovirus (CMV) status. Breast Cancer Res Treat (2024). https://doi.org/10.1007/s10549-024-07459-8
Received:
Accepted:
Published:
DOI: https://doi.org/10.1007/s10549-024-07459-8