Abstract
Background
The network theory of mental disorders asserts the pivotal role of feedback loops in psychopathology. We investigated intra-individual dynamics and potential feedback loops in psychological networks and their association with long-term outcomes.
Methods
At the beginning of the COVID-19 pandemic, data from a population-based cohort (N = 2029) were collected every three days for six months on well-being, worries, fatigue, sleep quality, social integration, and activity. Subgrouping—Group Iterative Multiple Model Estimation -was used to estimate networks of time-series data on the individual, subgroup, and group levels. Subgroup networks were compared and associations of subgroup membership with sociodemographic and health status variables at baseline and outcomes at follow-up were examined.
Results
Despite the large heterogeneity between individuals, a potential feedback loop involving sleep quality, fatigue and well-being was identified. Furthermore, two subgroups were identified, whereby the edges of the potential feedback loop were more present in Subgroup 1 than in Subgroup 2. Membership to Subgroup 1 was associated with lower education and fewer people aged over 60 in their household at baseline as well as poorer well-being, more worries, and more frequent and earlier COVID-19 diagnoses at follow-up.
Conclusions
The identified feedback loop might indeed represent a vicious cycle and thus contribute to the development of psychopathology. However, limitations such as the limited measurement density made it difficult to find temporal associations and call for a cautious interpretation of results.
Similar content being viewed by others
Explore related subjects
Discover the latest articles, news and stories from top researchers in related subjects.Avoid common mistakes on your manuscript.
Traditionally, mental disorders are hypothesized as latent diseases causing several symptoms such as sadness, worries, and sleep disturbances. This perspective is also reflected in diagnostic manuals like the ICD and the DSM, which facilitate communication, prognosis, and treatment planning. However, these categorical diagnoses are often criticized for oversimplifying mental health issues (Fried, 2022). Mental health problems are better understood as a spectrum of severity, ranging from severe symptoms to none. Furthermore, focusing solely on the diagnosis does not provide any information about the causes and the etiology of the disorder. This is especially important since different causes could lead to the same diagnosis and similar causes could lead to different diagnoses. This has led to more complex approaches that focus on the underlying biological and psychosocial mechanisms of mental disorders (e.g., Research Domain Criteria; RDoC; Insel, 2014) or cluster data-driven related symptoms into broader dimensions (e.g., Hierarchical Taxonomy of Psychopathology; HiTOP; Kotov et al., 2017).
However, these approaches were also criticized because they are predominantly oriented towards differences between persons, or rather towards differences between groups defined by diagnostic categories. Process-based approaches, such as the network approach, instead highlight the importance of studying processes within individuals. From the network perspective, mental disorders are conceptualized as networks of interacting elements instead of expressions of a latent disease (Borsboom, 2017; Schmittmann et al., 2013). In this view, elements of a network are causal agents rather than passive interchangeable indicators of a mental disorder. In other words, the nodes represent a web of interdependencies, with every component actively exerting influence on different timescales. This approach to psychopathology may be useful to capture all relevant symptoms, irrespective of diagnosis, circumventing issues with diagnostic boundaries and comorbidity (Hofmann et al., 2016). A large body of research on the network theory of psychopathology assumes that elements with high centrality, have particular importance in the development and maintenance of psychopathology and should thus be targeted in psychosocial interventions (Boschloo et al., 2016; Bryant et al., 2017; Marian & Sava, 2023). A highly central element is one with many and/or strong connections with other elements in the network. When activated, it is likely to spread activation throughout the network (Hofmann et al., 2016).
There has been a shift in academic discourse, wherein attention has moved away from examining isolated elements within a network and towards studying changes in topology (Bringmann et al., 2019), e.g., the dynamic interaction of network elements. The connections between these elements are not necessarily unidirectional. Instead, they can be reciprocal and/or self-sustaining, creating feedback loops in which, for instance, worrying may cause someone to sleep poorly, which in turn may cause them to feel more fatigue, which may diminish concentration, which again reinforces worrying. Feedback loops occur when symptoms activate and reinforce each other. When several nodes keep reinforcing each other over time, vicious cycles can arise, from which it may be difficult to escape (Borsboom & Cramer, 2013; Wichers, 2014). These self-perpetuating patterns might explain the development and maintenance of mental disorders. If an individual has difficulty escaping from the feedback loop, they may enter a downward spiral and over time develop a cluster of clinically relevant symptoms (e.g., Van den Bergh et al., 2020). While the network approach offers a new way of looking at these vicious cycles, the concept itself is well-established, for example in cognitive behavioral therapy and its manuals. For instance, one cognitive model of panic posits that panic attacks arise from a feedback loop where bodily sensations (e.g., increased heart rate) trigger catastrophic appraisals of the sensation (e.g., ‘I’m having a heart attack!’). This, in turn, increases heart rate and fear and could culminate in a panic attack (Clark, 1986). Furthermore, recent advancements formalized the network theory of panic disorder, postulating precise relationships among a set of symptoms and expresses these relationships through mathematical equations. This theory effectively explains core phenomena associated with panic disorder (Robinaugh et al., 2019).
Feedback loops are intra-individual processes that cannot be captured by inter-individual differences (Borsboom et al., 2021; Niu et al., 2023). The cross-sectional nature of many studies of network theory allows the effective description of differences between individuals but has limited ability to illuminate intra-individual changes, making it difficult to statistically model feedback loops (Contreras et al., 2019; Fried, 2020). To gain a deeper understanding of intra-individual changes, longitudinal studies are needed, which capture the temporal dynamics of symptom interactions. Time-series data analyzed with dynamic multilevel models enable person-by-person modeling of contemporaneous and time-lagged networks, depicting the idiographic topology and temporal dynamics of symptoms (Borsboom et al., 2021; Bos et al., 2017). Therefore, these techniques allow the modeling of feedback loops and thus a deeper understanding of an individual’s psychopathology.
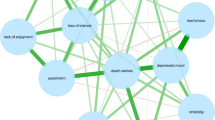
Recently, network analyses have extended to intensive longitudinal data (ILD), which permits the exploration of time-lagged associations (Fried et al., 2022; Martín-Brufau et al., 2020). Such dynamic network models have been applied to predict early change, treatment response, and dropout from psychological therapies (Fisher et al., 2021; Hamaker et al., 2018; Hehlmann et al., in press; Husen et al., 2016; Lutz et al., 2018). They have also been applied to examine potential feedback loops. For example, employing a dynamic multilevel model on time-series data from a convenience sample of 80 undergraduate students in the Netherlands, dynamic networks were identified that contained potentially vicious cycles between social isolation, worry, and anhedonia (Fried et al., 2022). Identifying reinforcing feedback loops is essential to understand heterogeneous health outcomes across different individuals. A nuanced expression of feedback loops can send people toward unique trajectories, i.e., different health outcomes. For example, interpreting physical sensations such as an increased heart rate as dangerous and a sign of a heart attack can lead to a panic attack, whereas interpreting them as harmless and a consequence of climbing stairs can lead to a relaxed state. Most studies have provided evidence that reinforcing feedback loops were more evident in individuals with either higher levels of psychopathology or at risk of psychopathology, compared with individuals in the general population (Bringmann et al., 2016; Klippel et al., 2018; Pe et al., 2015; Wigman et al., 2015). However, it is important to note that not all studies have confirmed this relationship, which emphasizes the need for further empirical investigation of the theoretically postulated role of feedback loops (Vos et al., 2017; Groen et al., 2019).
Feedback loops typically do not activate independently but are triggered externally, for example by critical life events such as the death of a loved one (Borsboom, 2017). While such critical life events can trigger the symptom networks of a few individuals and make them susceptible to psychopathological development, there are also events that affect large populations. The COVID-19 pandemic is a recent example that led to severe disruptions in everyday life all over the world. In addition to concerns about one's own health and that of friends and family, social gatherings have been severely restricted in many places for example through the closure of restaurants and cinemas, and the regulation of social contacts, leading to an increased psychosocial strain (Ammar et al., 2021). This heightened stress likely contributed to the rise in mental disorders during the pandemic (Lakhan et al., 2020). There is vast evidence that mental disorders are associated with physical illness, with each predisposing individuals to the other (Doherty & Gaughran, 2014; Isvoranu et al., 2021; Merikangas et al., 2015; von Hausswolff-Juhlin et al., 2009). This bidirectional relationship is critical during the COVID-19 pandemic, where restrictions to reduce infection can increase psychosocial stress and, consequently, physical illnesses. Beyond the psychosocial effects of the COVID-19 pandemic, the physical illness itself plays a crucial role and can worsen the physical health of individuals with mental illness, that already face physical health disparities (Melamed et al., 2020). Furthermore, physical illnesses can act as external events that trigger feedback loops in symptom networks, affecting psychological well-being (Borsboom, 2017). The reduced activity levels caused by the pandemic can also affect both mental and physical health (Violant-Holz et al., 2020). This underscores the importance of understanding the interplay of underlying processes to mitigate severe negative effects.
Therefore, the current study used a large population-based set of time-series data on various psychological variables (well-being, worries, fatigue, sleep quality, social integration, and activity) to investigate their intra-individual dynamics, potential feedback loops, and their association with related long-term mental and somatic health outcomes using an appropriate statistical method (i.e., Subgrouping—Group Iterative Multiple Model Estimation; S-GIMME Gates et al., 2017; Lane et al., 2019). The study had four main hypotheses: (1) Feedback loops can be identified in the participant data (2) Feedback loops differ between subgroups (smaller groups within our large sample who have similar patterns in their intra-individual dynamics), (3) Sociodemographic and health status variables differentiate between these subgroups, and (4) Subgroups differ in their long-term course of psychopathology and are also related to a distal somatic outcome measure (i.e., COVID-19 diagnosis).
Materials and Methods
Participants and Design
This study is an exploratory, anonymized re-analysis of two existing studies on COVID-19 infection rates (Balck et al., 2022; Klein et al., 2022). The ethics proposal of the original studies allows for anonymized data re-analysis. As the study is an exploratory re-analysis, no pre-registration is available. The cohort was recruited through local press, radio announcements, posters, flyers, an announcement on the city’s official homepage, and University internal e-mail distribution. From the interested individuals, a representative population-based sample was selected and supplemented by a risk group of individuals with a high number of professional contacts. This resulted in a sample of 3040 individuals.
After excluding 842 individuals with less than half of the assessments (i.e. 25 time points) and 169 individuals with no variance in their data (assessed by S-GIMME), the final sample included 2029 participants (59% female, 41% male) with a mean age of 48.1 years (SD = 14.68; range = 18–79). Of these, 850 (42%) individuals were classified as risk group due to their high number of professional contacts, including medical professionals (e.g. doctors and nurses), sales staff, teachers, students, and security and rescue workers. The sample’s demographic information can be found in supplemental material 1. Eight individuals were removed from further analyses because their S-GIMME models did not converge.
The study used a baseline assessment in April 2020, followed by app-based questionnaires completed every three days for six months, resulting in 50 measurement time points. Each participant had to fill out the questionnaires from the end of April/beginning of May 2020 to the end of September/beginning of October 2020. The participants took part in M = 32.95 measurement time points (SD = 6.92, Min = 25, Max = 51). Six participants completed the questionnaires twice at one or two time points, resulting in three participants with 51 measurement time points. In this study, the total number of time-series observations was N = 70,695. Given that the maximum possible number of observations would have been 101,050 (2021 participants with 50 measurement time-points), the rate of missing data was 30%, which corresponds to a compliance rate of 70%. Follow-up data were collected two years (April 2022) and 2.5 years (September 2022) after baseline, with 1068 individuals participating in the 2.5-years follow-up.
Instruments
Data collection was app-based, using an existing cell phone app (MillionFriends, Perfood GmbH) established by a start-up company that emerged from the University of Lübeck. The study questionnaires were integrated into the existing app.
Baseline Assessment
Demographic characteristics (i.e., risk group or not, age, gender, education, household size) and health status (i.e., history of depression, alcohol use, smoking) were collected at baseline using single-item questions via the app.
Time-series Data
At each measurement point, participants completed questions about well-being, worries, sleep quality, fatigue, and social integration in the app. Each variable is assessed with a single-item question on a visual analog scale ranging from 1 to 10. Lower values indicate a lower level of the variable, while higher values indicate a higher level. The cursor of the visual analog scale appeared at the first click. For example, sleep quality was assessed with the question ‘How good was your sleep in the last 72 h?’ on a scale from 1 (poor) to 10 (good) (for more information on assessment questions, see supplemental material S2). Furthermore, several activities (e.g., shopping for essentials, going to public spaces, a trip with friends) were assessed using binary responses (yes/no). To include activities as a variable in S-GIMME we summarized the activities on a scale from 1 to 10 (1 = no activities, 2 = one activity, 10 = all nine activities).
Follow-up Assessments
The follow-up assessments were assessed with the same app and repeated the questions from the time series data (well-being, worries, sleep quality, fatigue, social integration). In addition, a question about digital communication was added (Supplemental material 2). The 2.5-years follow-up was also in the same app and included further data on time and frequency of COVID-19 diagnoses.
Statistical Analyses
Data were analyzed using R version 4.1.2 (R Core Team, 2021), and SPSS version 26.0.0.1 (IBM, 2020). To test hypothesis 1, S-GIMME was conducted to estimate networks of time-series data on the individual, subgroup, and group levels using the gimme package (Gates et al., 2017; Lane et al., 2021). In keeping with conventions in network analysis, the elements of the networks will be described as nodes, while the associations between these nodes will be described as edges (Borsboom, 2017; Borsboom & Cramer, 2013). GIMME estimates dynamic directional networks that are generalizable as well as individual to each person and implements unified structural equation models to estimate vector autoregressive (VAR) models (Lane & Gates, 2017). S-GIMME improves upon the original GIMME by clustering individuals into subgroups using shared characteristics of individuals’ temporal processes before final idiographic modeling takes place. S-GIMME assumes stationarity. Therefore, we used the Kwiatkowski-Phillips-Schmidt-Shin (KPSS) test for the null hypothesis that a time series is level or trend stationary (Kwiatkowski et al., 1992). The test was conducted separately for each of the 2029 participants and 6 variables per participant using the R package tseries 0.10–52 (Trapletti et al., 2023). The KPSS test indicated that the majority of time series was level (74.70%) and trend (82.13%) stationary. Furthermore, to account for lags between signals, we have added omitted measurement times as missing values in the input time series. Even if long time periods are missing, one line of missingness is sufficient as a placeholder for the section of missing data. GIMME then uses full information maximum likelihood to handle the missing data and is therefore relatively robust to missing data (Beltz & Gates, 2017).
All variables entered into S-GIMME were z-standardized. We began the search for the group model with the autoregressive (AR) paths freed for estimation. The individual networks included contemporaneous associations and associations with a lag of one occasion. Contemporaneous associations show if one variable predicts another within the same measurement window, while lagged associations reveal if one variable predicts another over time. In this study, lagged associations indicate whether a variable is predicted by another variable assessed three days earlier. Contemporaneous and lagged parameters were assigned to the overall group if they were statistically significant for at least 75% of the time series. Subgroups (distinct clusters of individuals) were sought via the Walktrap algorithm, which allows community detection in networks based on random walks. These paths were estimated uniquely for each individual but had to improve the majority of the individuals’ models within the subgroup. Contemporaneous and lagged parameters were assigned to the subgroup if they were statistically significant for at least 50% of the time series. Individual dynamics were investigated by examining the network structures of ten randomly selected individuals. It is important to note that our study, with 25–50 measurement points, falls short of the recommended 60–400 measurement points (Hoekstra et al., 2023; Lane & Gates, 2017). Consequently, we anticipated detecting mostly strong effects, possibly missing smaller ones (Lane et al., 2019; Nestler & Humberg, 2021). Given that GIMME typically avoids false positives even with 50 measurement points, we expected the detected effects to be accurate and reliable, though potentially sparse (Lane et al., 2019; Nestler & Humberg, 2021). Furthermore, due to the long time intervals between observations, we expected to find more contemporaneous than lagged effects (Beltz & Gates, 2017; Wright et al., 2019).
To test hypothesis 2, subgroup networks were compared by analyzing all pathways that were present in more than 10% of individuals in the complete sample, using χ2-tests for the presence of edges. For edges that were present in 100% of individuals, two-tailed t-tests were conducted to compare subgroups in their edge strength.
Before testing hypothesis 3 and 4, nonparametric missing value imputation was performed for all baseline and follow-up variables with less than 30% missingness using missForest version 1.5 (Stekhoven & Bühlmann, 2012). The number of missing data was between 0 and 28% (M = 13%, SD = 13.27). Categorical variables were one-hot encoded, continuous variables were centered.
To test hypothesis 3, elastic net was used to select predictors for the subgroup membership from sociodemographic variables and health status (24 variables). An elastic net algorithm was chosen, because it handles psychological data well and protects against overfitting (Lutz et al., 2019; Pavlou et al., 2016). For elastic net regularization, the R package glmnet v4.1–6 (Friedman et al., 2010) was used. Elastic net regularization combines LASSO (least absolute shrinkage and selection operator) and ridge procedures. Both procedures shrink regression coefficients due to their predictive power, but only LASSO can shrink variable coefficients to zero. Furthermore, ridge regression, LASSO, and elastic net have two tuning parameters that determine the types of the penalties (α) and their strengths (λ). To choose the tuning parameters, we used k-fold cross-validation for Elastic-Net Regularized Generalized Linear Models to build sequences of α and λ for each model. Then, we selected the α and the λ with the lowest cross-validation prediction error. Subsequently, the resulting predictor variables were entered into a logistic regression model.
To test hypothesis 4, bivariate correlations were calculated for variable selection. All significant associations were further examined using a one-way multivariate analysis of variance (MANOVA) and post-hoc analyses of variance (ANOVAs). To better understand the differences between the subgroups regarding the time of onset of COVID-19, a survival analysis was performed using the Kaplan–Meier procedure (Kaplan & Meier, 1958), with January 2020 as the time origin for each individual representing the beginning of the COVID-19 pandemic in Germany.
Results
Hypothesis 1 Group Parameters and Intra-Individual Networks
The network in Fig. 1 represents the network for the complete sample. Except for the autoregressive effects, no group-level edges were found. The autoregressive effects show that, for each individual, each variable predicts its own value at the next time point, adjusted for the influence of other variables. After the autoregressive effects, the most common connection was a contemporaneous edge between fatigue and sleep quality, which was present in 422 (21%) individuals with an average regression weight of β = − 0.44. The average regression weight shows the direction and the strength of the relationship between fatigue and sleep quality, averaged across all individuals sharing this connection. This means that, on average, for those where fatigue is linked to sleep quality, higher fatigue at the same time is associated with poorer sleep quality. Since GIMME uses partial correlations, these relationships are adjusted for the influence of other variables. Almost as common were contemporaneous edges between sleep quality and well-being (19%, β = 0.55) and vice versa (19%, β = 0.48) as well as contemporaneous edges between fatigue and well-being (18%, β = − 0.43) and between sleep quality and fatigue (17%, β = − 0.36). As a sensitivity analysis, the group-level network was re-estimated for person-mean centered and detrended data to evaluate cluster stability and to account for non-stationarity. The networks remained stable for person-mean-centered and detrended data (Supplemental material 3).
Group-level network of the complete sample. Black edges are on the group level, and grey edges are on the individual level. Individual-level edges are shown only if they are present in more than 10% of the individuals. Solid lines represent contemporaneous effects; dashed lines represent lagged effects. The thickness of the edge represents the number of participants. The percentages indicate the number of individuals in which the edge occurs, and the numbers in parentheses below indicate the average beta weight of the edge
Figure 2 shows the networks of 10 randomly selected individuals. Initially, these intra-individual networks look somewhat heterogeneous, but a closer look reveals that 9 of the 10 individuals show at least one of the most frequently occurring paths at group level, i.e., the contemporaneous paths between sleep quality, fatigue, and well-being. In only one individual none of these paths is present (Fig. 2, Panel F). Three individuals (Fig. 2, Panel A, G, H) show two of these paths and two individuals (Fig. 2, Panel B, C) show three of these paths.
Hypothesis 2 Subgroups
S-GIMME identified two subgroups consisting of 695 and 1326 members, respectively. The network in Fig. 3, Panel A represents the network of Subgroup 1. The most common individual-level connections were the contemporaneous edges between fatigue and sleep quality (24%, β = − 0.47), between sleep quality and well-being (24%, β = 0.75), and between fatigue and well-being (24%, β = − 0.48). In Subgroup 2 the most common individual-level connection was a contemporaneous edge between fatigue and sleep quality (19%, β = − 0.44). Almost as common were contemporaneous edges between well-being and sleep quality (17%, β = 0.46) and vice versa (16%, β = 0.39; Fig. 3, Panel B). No subgroup-specific edges were found. Two-tailed t-tests revealed that the two subgroups differed significantly in the strength of the autoregressive effects of well-being (MSubgroup1 = 0.22, MSubgroup2 = 0.13, t = 6.48, p < 0.001), worries (MSubgroup1 = 0.42, MSubgroup2 = 0.16, t = 13.74, p < 0.001), fatigue (MSubgroup1 = 0.17, MSubgroup2 = 0.11, t = 3.41, p = 0.001) and social integration (MSubgroup1 = 0.32, MSubgroup2 = 0.18, t = 9.21, p < 0.001). The frequency of the edges presented in Fig. 4 differed significantly between the networks of the two subgroups. All the depicted edges are more frequent in Subgroup 1. For example, in Subgroup 1 the contemporaneous association of fatigue with well-being and worries is more common than in Subgroup 2. The significant differences between the two subgroups might imply a feedback loop consisting of fatigue, well-being, and sleep quality that was more frequent in Subgroup 1 whereas the network of subgroup 2 appears to be more loosely associated. Figure 2, Panels A–D show examples of four participants from the first subgroup with the feedback loop, whereas Panels E–J show examples of six participants from the second subgroup with the more loosely associated network.
Subgroup-level networks of Subgroup 1 (Panel A) and Subgroup 2 (Panel B) we well-being, wo worries, sq sleep quality, fa fatigue, si social integration, ac activity. Black edges are on the group level, and grey edges are on the individual level. Individual-level edges are shown only if they are present in more than 10% of the individuals. Solid lines represent contemporaneous effects; dashed lines represent lagged effects. The thickness of the edge represents the number of participants. The percentages indicate the number of individuals in which the edge occurs, and the numbers in parentheses below indicate the average beta weight of the edge
Differential frequency network of Subgroups 1 and 2 we well-being, wo worries, sq sleep quality, fa fatigue, si social integration, ac activity. The frequency of the presented edges differs significantly between the networks of the two subgroups (p ≤ 0.003, with Bonferroni correction). All presented edges are more frequent in Subgroup 1
Hypothesis 3 Baseline Differences Between Subgroups
The elastic net model selected three of the 24 baseline variables as predictors of subgroup membership, namely education (b = 0.08), cohousing count over 60 years (b = 0.09), and cohousing count under 18 years (b = − 0.02) (Differences between subgroups can be found in Supplemental Material S4). In the subsequent logistic regression model, education (b = 0.24, p = 0.017) and cohousing count over 60 years (b = 0.24, p = 0.008) were found to be significant predictors of subgroup membership (R2Nagelkerke = 0.01, see Table 1). These results indicate that individuals in Subgroup 1 with the feedback loop had lower education and fewer people aged over 60 in their household than individuals in Subgroup 2 with the more loosely associated network.
Hypothesis 4 Long-Term Effects of Subgroup Membership
Concerning follow-up variables, subgroup membership was significantly correlated with well-being (r = 0.04, p = 0.045), worries (r = − 0.05, p = 0.032), and sleep quality (r = 0.04, p = 0.046) at the 2-years follow-up and with the frequency of COVID-19 diagnoses (r = − 0.08, p < 0.014) at the 2.5-years follow-up (Supplemental material 5). MANOVA results showed statistically significant differences in well-being, worries, sleep quality, and frequency of COVID-19 diagnoses according to subgroup type (Pillai’s trace = 0.017, F(4, 1058) = 4.62, p = 0.001). Post-hoc ANOVAs revealed that the significant group effect in the MANOVA was due to significant differences in well-being (F(1, 2019) = 4.04, p = 0.045), worries (F(1, 2019) = 4.59, p = 0.032), sleep quality (F(1, 2019) = 4.00, p = 0.046), and frequency of COVID-19 diagnoses (F(1, 1061) = 6.06, p = 0.014). Individuals in Subgroup 1 with the feedback loop reported less well-being, more worries, worse sleep quality, and they were diagnosed more often with COVID-19 than individuals in Subgroup 2 with the more loosely associated network. According to the survival analysis, individuals in Subgroup 1 with the feedback loop received a COVID-19 diagnosis on average significantly earlier than individuals in Subgroup 2 with the more loosely associated network (30.41 months vs. 30.73 months; χ2(Tarone-Ware) = 6.80, p = 0.009).
Discussion
The purpose of this study was to assess potential feedback loops in intra-individual dynamics of selected psychological variables, to identify subgroups based on those feedback loops, and to examine baseline differences between subgroups as well as associations with long-term health outcomes. Results suggest that these dynamics were highly individual, with only autoregressive effects being present in at least 75% of the participants and therefore appearing at the group level. However, a closer look at the intra-individual dynamics shows that the dynamics that occurred more frequently at the group level were also, at least partially, reflected at the intra-individual level.
Concerning Hypothesis 1, the contemporaneous edges between sleep quality, fatigue, and well-being were present most frequently, indicating a potential feedback loop. This finding was robust for person-mean centered and detrended data. At the intra-individual level, it appears that the feedback loop was, partially, active in most individuals. Concerning Hypothesis 2, two subgroups were identified and edges within the potential feedback loop were present more commonly in Subgroup 1 than in Subgroup 2. Concerning Hypothesis 3, sociodemographic variables (education and cohousing count over 60 years) differentiated between the subgroups. The individuals in Subgroup 1 with the feedback loop had lower education and fewer people aged over 60 in their household than individuals in Subgroup 2 with the more loosely associated network. However, these variables accounted for only 1% of the total variance. Concerning Hypothesis 4, Subgroup 1 with the feedback loop reported less well-being, more worries, and worse sleep quality at the 2-years follow-up. Additionally, at the 2.5-years follow-up, participants in Subgroup 1 with the feedback loop reported more and earlier COVID-19 diagnoses. Taken together, these findings suggest that poor sleep quality, greater fatigue, and poorer well-being might indeed constitute a vicious cycle that is more pronounced in a subgroup of individuals and associated with adverse long-term mental and somatic health outcomes.
Furthermore, some interesting features were found in the subgroup networks. Firstly, it seems that individuals in Subgroup 1 with the feedback loop and stronger autoregressive effects may have difficulty escaping this feedback loop, making them more vulnerable to developing a mental disorder. Networks with more frequent associations are more vulnerable to oscillations, which can push them into a pathological state. In previous studies, denser networks were associated with the existence and persistence of depression (Cramer et al., 2016; Pe et al., 2015; van Borkulo et al., 2015). Our results align with previous research on early warning signs reflecting vulnerability for emotional disorders. Individuals who experience a higher autocorrelation have slower dynamics, which can be seen as predictive of a transition into depression (Leemput et al., 2014). In situations like the COVID-19 pandemic, identifying vulnerable individuals is crucial, as strongly connected networks tend to enter a depressed state when exposed to external stress (e.g., the COVID-19 pandemic), whereas networks with weaker connections tend to remain in or return to a non-depressed state (Cramer et al., 2016). Within such strongly connected networks, the removal of the stressor after the phase transition occurred did not cause the system to shift back to its original state (Cramer et al., 2016).
Secondly, there seems to be a strong association between sleep quality and well-being for individuals in Subgroup 1 with the feedback loop. However, this association is concerning, because data were collected during the COVID-19 lockdown, which significantly impacted sleep quality (Trabelsi et al., 2021). Impaired sleep quality is not only linked to diminished well-being, but also leads to adverse physical health outcomes, as sleep plays a crucial role in immune functions (Buxton & Marcelli, 2010). Furthermore, sleep disturbances are a frequent warning signal of psychological disorders (Bauer et al., 2006). This finding again suggests Subgroup 1’s vulnerability and it is tempting to suggest that the feedback loop identified in this study is associated with more frequent and earlier onset of COVID-19 diagnoses. However, the small average time difference of about eleven days between the two groups must be considered when interpreting the effect of subgroup membership on COVID-19 diagnoses.
Thirdly, sleep quality seemed to be closely linked not only to well-being but also to fatigue, which in turn affects well-being and worries. This association is also particularly strong in the vulnerable Subgroup 1 with the feedback loop. This would correspond to the idea that worrying does not protect from adverse health outcomes (Armstrong & Dregan, 2014; Fitzgerald et al., 2022; Hoffart et al., 2023; Pieper et al., 2010). Instead, worries often lead to health anxiety, negatively impacting well-being, social and occupational functioning, and health care utilization (Asmundson et al., 2010). Health anxiety became especially prominent during the COVID-19 pandemic (Tyrer, 2020). Symptoms like cough, dizziness, and difficulty breathing were frequently misinterpreted as COVID-19. This health-related fear is a common response during the pandemic, heightened by constant exposure to health threat messages on social media (Tyrer, 2020). For most people, anxiety was proportionate to the threat, helping them avoid crowded places during peak times of the pandemic. It was also normal to feel worried when visiting crowded places was unavoidable, such as at work or on public transportation. However, for some, COVID-19 anxiety quickly becomes disproportionate, significantly interfering with daily life. These individuals monitor their health obsessively, check their body obsessively, seek constant reassurance from others, browse compulsively health information, and frequently consult medical personnel. Even negative COVID-19 test results do not alleviate their fears due to doubts about test accuracy, creating a vicious cycle of increased anxiety, more symptoms, and further misinterpretation. Affected individuals may engage in excessive avoidance behaviors, such as isolating, frequent hand washing, checking body temperature, monitoring respiratory function, and repeatedly testing their sense of smell (Tyrer, 2020). These symptoms can persist even after the peak of the pandemic. It is tempting to transfer this pattern to subgroup 1, which experienced more worries, less well-being and worse sleep quality at the 2-years follow-up in April 2022, i.e., after the peaks of the pandemic. However, it is crucial to note that these differences were no longer evident at the 2.5-years follow-up.
It is possible that the presence of the feedback loop makes Subgroup 1 more vulnerable, but the reverse could also be true. Subgroup 1 with the feedback loop may have been heavily burdened even at the beginning of the COVID-19 pandemic, with the pandemic acting as the external stressor that activated the feedback loop in this group. One might assume that the risk group, those with frequent professional contact, would be more vulnerable to the feedback loop activation. However, this does not appear to be the decisive factor, as both subgroups have nearly identical numbers of risk individuals. Instead, it seems that individuals in Subgroup 1 with the feedback loop are more likely to have lower education levels, generally associated with a higher risk of developing common mental disorders (e.g., Araya et al., 2003) and psychiatric symptoms due to COVID-19 (e.g., Li et al., 2023). Furthermore, it is interesting that the more burdened Subgroup 1 with the feedback loop has fewer people aged over 60 in their household. This initially seems counterintuitive, as people aged over 60 are particularly affected by health risks related to COVID-19, potentially increasing family members' worries. One explanation could be that fewer people aged over 60 in the household might indicate fewer family members overall, which was found to be a protective factor during the pandemic (e.g., Li et al., 2023). Additionally, it may be more likely that younger household members lead to more worry, as they face more pandemic-related stressors such as job loss and school closure (Brunoni, et al., 2023; Xiong et al., 2020). Brunoni and colleagues (2023) found that people younger than 60 presented an increased risk, suggesting that having family members over 60, who are less affected by the pandemic, could serve as a protective factor. However, these are only initial ideas that need to be further investigated in future studies.
In clinical practice, identifying vulnerable individuals is crucial. Predictors, such as lower education and fewer people aged over 60 in their household can help identify these individuals before negative health outcomes arise. Screening the general population for these predictors during crises could enable preventive interventions. However, further research on predictors is necessary, as those identified in this study accounted for only 1% of the total variance. When symptoms are already present, group-level and/or subgroup-level feedback loops could assist clinicians in deciding where to focus their attention during the functional analysis when they are trying to identify perpetuating mechanisms that maintain a patient’s problems. Clinicians need to verify in each individual patient however which paths of the feedback loop (if any) are present for this patient. Therefore, knowledge of the group-level findings is an aid to but no substitute for individual functional analysis. Furthermore, the individual presence of the feedback loop must be investigated further in future studies, since S-GIMME can only demonstrate that individual paths, rather than the entire pattern of contemporaneous connections, occur more frequently.
However, network analysis has often been criticized for its uncertain clinical utility and methodological difficulties (Contreras et al., 2019; Hoekstra et al., 2023; Neal et al., 2022). The results are often unstable depending on the methods used by the researchers (Bastiaansen et al., 2020; Park et al., 2020), with no consensus on the best modeling approach (Schumacher et al., 2024). This leads to conflicting results that can confirm or contradict the theoretically postulated role of feedback loops in the development and maintenance of mental disorders (Vos et al., 2017). This issue is addressed in a new preprint from Siepe and Heck (2023), who used a relatively new approach called multiverse analysis (Steegen et al., 2016) to the test the robustness of GIMME. This method systematically evaluates the uncertainty linked to researcher choices by using a range of plausible model specifications. They found that GIMME results at the group level were generally robust, whereas subgroup-level estimations show some variations, and individual-level networks were sensitive to alternative modeling specifications. This observation aligns with other research that emphasizes both the need to consider an idiographic and a nomothetic perspective (Hofmann et al., 2020; Webb et al., 2023). Given the substantial inter-individual heterogeneity in our data, it is essential to consider individual processes alongside group-level results. In our data the findings at the group level can at least in part also be seen at the individual level. However, in line with the results from Siepe and Heck (2023), starting with group-level insights and then focusing on individual aspects in clinical discussions seems an appropriate approach.
Our study also has some limitations that must be considered when interpreting the results. The analyses of the current paper are secondary. Important associated limitations are that time-series data were assessed every three days for six months. The length of the measurement period is a strength of the study, but it resulted in a relatively small number of measurement time points (at least 25 and up to 50 time points) which is the main limitation of the study. The number of measurement time points required for an accurate estimation varies between 60 and 400 (Hoekstra et al., 2023; Lane & Gates, 2017). Therefore, it is possible that we only detected strong effects, and possibly missed some smaller ones (Lane et al., 2019; Nestler & Humberg, 2021). However, a balance between reliable results and tolerable participant burden must be found. The three-day interval between observations is a second limitation in the current study and may mean that important processes that occurred at a higher frequency were not captured. This could explain why we only found contemporaneous effects (Collins, 2006). Thirdly, we had to exclude a substantial amount of data due to issues with measurement commitment (n = 842) and data variability (n = 169). The 169 individuals with low variance in their data could be interpreted as a third subgroup that is resistant to change, as their values were very stable across repeated measurements. Despite these exclusions, our study retains a large sample size, which is an important strength. Furthermore, using a representative, population-based sample represents different types of psychopathology and allows generalization. The use of S-GIMME, which allows the analysis of intra-individual as well as group-level dynamics is innovative, and results are supported by the sensitivity analyses.
In conclusion, we identified a potential feedback loop between sleep quality, fatigue, and well-being which was more present in Subgroup 1 compared to Subgroup 2. Participants in Subgroup 1 showed denser networks and experienced less well-being, more worries, worse sleep quality and more COVID-19 diagnoses in the long-term. This vulnerability may be rooted in disproportionate health anxiety, which significantly impacted daily life (e.g., isolation). Our findings align with previous research highlighting feedback loops between psychological variables as critical indicators that could contribute to psychopathology (Fried et al., 2022; Hoffart et al., 2023).
These results underscore the importance of identifying vulnerable individuals and facilitating their access to treatment. While predictors such as lower education offer some insight, they alone are insufficient to explain variance and should be complemented with additional measures. The network approach may have high clinical relevance to expose individual vulnerability structures arising from dynamics in psychological variables that take place in daily life. In addition to identifying vulnerability structures, individual dynamics in psychological variables can also provide an indication of which person could benefit from which treatment (Uhl et al., 2024). Relevant processes at a group and/or subgroup-level could provide guidance for more detailed exploration at individual level. Integrating network analyses into existing feedback systems could serve as a basis for decisions on the patient-specific data needed to implement measurement-based psychological therapy and make personalized decisions regarding the timing and choice of interventions (Lutz et al., 2022). However, this is still more of a vision that requires further studies. Future research should prioritize addressing methodological challenges, such as network instability, while focusing on enhancing clinical utility.
Data Availability
All data are available online in a public repository (https://doi: 10.5061/dryad.h44j0zpn5).
Code Availability
Analytic code is available from the corresponding author (J.B.) on reasonable request.
References
Ammar, A., Trabelsi, K., Brach, M., Chtourou, H., Boukhris, O., Masmoudi, L., Bouaziz, B., Bentlage, E., How, D., Ahmed, M., Mueller, P., Mueller, N., Hammouda, O., Paineiras-Domingos, L., Braakman-jansen, A., Wrede, C., Bastoni, S., Pernambuco, C., Mataruna, L., & Hoekelmann, A. (2021). Effects of home confinement on mental health and lifestyle behaviours during the COVID-19 outbreak: Insight from the ECLB-COVID19 multicenter study. Biology of Sport, 38(1), 9–21. https://doi.org/10.5114/biolsport.2020.96857
Araya, R., Lewis, G., Rojas, G., & Fritsch, R. (2003). Education and income: Which is more important for mental health? Journal of Epidemiology & Community Health, 57(7), 501–505. https://doi.org/10.1136/jech.57.7.501
Armstrong, D., & Dregan, A. (2014). A population-based investigation into the self-reported reasons for sleep problems. PLoS ONE, 9(7), e101368. https://doi.org/10.1371/journal.pone.0101368
Asmundson, G. J. G., Abramowitz, J. S., Richter, A. A., & Whedon, M. (2010). Health anxiety: Current Perspectives and Future Directions. Current Psychiatry Reports, 12(4), 306–312. https://doi.org/10.1007/s11920-010-0123-9
Balck, A., Föh, B., Borsche, M., Rahmöller, J., Vollstedt, E.-J., Waldeck, F., Käding, N., Twesten, C., Mischnik, A., Gillessen-Kaesbach, G., Ehlers, M., Sina, C., Taube, S., Busch, H., Rupp, J., Katalinic, A., & Klein, C. (2022). Protocol of the Luebeck longitudinal investigation of SARS-CoV-2 infection (ELISA) study – a prospective population-based cohort study. BMC Public Health, 22(1), 1305. https://doi.org/10.1186/s12889-022-13666-z
Bastiaansen, J. A., Kunkels, Y. K., Blaauw, F. J., Boker, S. M., Ceulemans, E., Chen, M., Chow, S.-M., de Jonge, P., Emerencia, A. C., Epskamp, S., Fisher, A. J., Hamaker, E. L., Kuppens, P., Lutz, W., Meyer, M. J., Moulder, R., Oravecz, Z., Riese, H., Rubel, J., & Bringmann, L. F. (2020). Time to get personal? The impact of researchers choices on the selection of treatment targets using the experience sampling methodology. Journal of Psychosomatic Research, 137, 110211. https://doi.org/10.1016/j.jpsychores.2020.110211
Bauer, M., Grof, P., Rasgon, N., Bschor, T., Glenn, T., & Whybrow, P. C. (2006). Temporal relation between sleep and mood in patients with bipolar disorder. Bipolar Disorders, 8(2), 160–167. https://doi.org/10.1111/j.1399-5618.2006.00294.x
Beltz, A. M., & Gates, K. M. (2017). Network mapping with GIMME. Multivariate Behavioral Research, 52(6), 789–804. https://doi.org/10.1080/00273171.2017.1373014
Borsboom, D. (2017). A network theory of mental disorders. World Psychiatry, 16(1), 5–13. https://doi.org/10.1002/wps.20375
Borsboom, D., & Cramer, A. O. J. (2013). Network analysis: An integrative approach to the structure of psychopathology. Annual Review of Clinical Psychology, 9, 91–121. https://doi.org/10.1146/annurev-clinpsy-050212-185608
Borsboom, D., Deserno, M. K., Rhemtulla, M., Epskamp, S., Fried, E. I., McNally, R. J., Robinaugh, D. J., Perugini, M., Dalege, J., Costantini, G., Isvoranu, A.-M., Wysocki, A. C., van Borkulo, C. D., van Bork, R., & Waldorp, L. J. (2021). Network analysis of multivariate data in psychological science. Nature Reviews Methods Primers, 1(1), 58. https://doi.org/10.1038/s43586-021-00055-w
Bos, F. M., Snippe, E., de Vos, S., Hartmann, J. A., Simons, C. J. P., van der Krieke, L., de Jonge, P., & Wichers, M. (2017). Can we jump from cross-sectional to dynamic interpretations of networks implications for the network perspective in psychiatry. Psychotherapy and Psychosomatics, 86(3), 175–177. https://doi.org/10.1159/000453583
Boschloo, L., van Borkulo, C. D., Borsboom, D., & Schoevers, R. A. (2016). A prospective study on how symptoms in a network predict the onset of depression. Psychotherapy and Psychosomatics, 85(3), 183–184. https://doi.org/10.1159/000442001
Bringmann, L. F., Elmer, T., Epskamp, S., Krause, R. W., Schoch, D., Wichers, M., Wigman, J. T. W., & Snippe, E. (2019). What do centrality measures measure in psychological networks? Journal of Abnormal Psychology, 128(8), 892–903. https://doi.org/10.3929/ETHZ-B-000368126
Bringmann, L. F., Pe, M. L., Vissers, N., Ceulemans, E., Borsboom, D., Vanpaemel, W., Tuerlinckx, F., & Kuppens, P. (2016). Assessing temporal emotion dynamics using networks. Assessment, 23(4), 425–435. https://doi.org/10.1177/1073191116645909
Brunoni, A. R., Suen, P. J. C., Bacchi, P. S., Razza, L. B., Klein, I., Dos Santos, L. A., de Souza Santos, I., da Costa, L. V. L., Gallucci-Neto, J., Moreno, L. M., Pinto, B. S., de Cássia, S. F. L., de Sousa, J. P., Viana, M. C., Forte, P. M., de Altisent, O. C. M. C., Bittencourt, M. S., Pelosof, R., de Siqueira, L. L., & Benseñor, I. M. (2023). Prevalence and risk factors of psychiatric symptoms and diagnoses before and during the COVID-19 pandemic: findings from the ELSA-Brasil COVID-19 mental health cohort. Psychological medicine, 53(2), 446–457. https://doi.org/10.1017/S0033291721001719
Bryant, R. A., Creamer, M., O’Donnell, M., Forbes, D., McFarlane, A. C., Silove, D., & Hadzi-Pavlovic, D. (2017). Acute and chronic posttraumatic stress symptoms in the emergence of posttraumatic stress disorder: A network analysis. JAMA Psychiatry, 74(2), 135–142. https://doi.org/10.1001/jamapsychiatry.2016.3470
Buxton, O. M., & Marcelli, E. (2010). Short and long sleep are positively associated with obesity, diabetes, hypertension, and cardiovascular disease among adults in the United States. Social Science & Medicine, 71(5), 1027–1036. https://doi.org/10.1016/j.socscimed.2010.05.041
Clark, D. M. (1986). A cognitive approach to panic. Behaviour Research and Therapy, 24(4), 461–470. https://doi.org/10.1016/0005-7967(86)90011-2
Collins, L. M. (2006). Analysis of longitudinal data: The integration of theoretical model, temporal design, and statistical model. Annual Review of Psychology, 57(1), 505–528. https://doi.org/10.1146/annurev.psych.57.102904.190146
Contreras, A., Nieto, I., Valiente, C., Espinosa, R., & Vazquez, C. (2019). The study of psychopathology from the network analysis perspective: A systematic review. Psychotherapy and Psychosomatics, 88(2), 71–83. https://doi.org/10.1159/000497425
Cramer, A. O. J., van Borkulo, C. D., Giltay, E. J., van der Maas, H. L. J., Kendler, K. S., Scheffer, M., & Borsboom, D. (2016). Major depression as a complex dynamic system. PLOS ONE. https://doi.org/10.1371/journal.pone.0167490
de Vos, S., Wardenaar, K. J., Bos, E. H., Wit, E. C., Bouwmans, M. E. J., & de Jonge, P. (2017). An investigation of emotion dynamics in major depressive disorder patients and healthy persons using sparse longitudinal networks. PLOS ONE. https://doi.org/10.1371/journal.pone.0178586
Doherty, A. M., & Gaughran, F. (2014). The interface of physical and mental health. Social Psychiatry and Psychiatric Epidemiology, 49, 673–682. https://doi.org/10.1007/s00127-014-0847-7
Fisher, A., Soyster, P., & Ashlock, L. (2021). Machine learning algorithms for generating early warning signals in real time. Biological Psychiatry, 89(9), 58–59. https://doi.org/10.1016/j.biopsych.2021.02.162
Fitzgerald, H. E., Parsons, E. M., Indriolo, T., Taghian, N. R., Gold, A. K., Hoyt, D. L., Milligan, M. A., Zvolensky, M. J., & Otto, M. W. (2022). Worrying but not acting: The role of intolerance of uncertainty in explaining the discrepancy in COVID-19-related responses. Cognitive Therapy and Research, 46(6), 1150–1156. https://doi.org/10.1007/s10608-022-10321-0
Fried, E. I. (2020). Lack of theory building and testing impedes progress in the factor and network literature. Psychological Inquiry, 31(4), 271–288. https://doi.org/10.1080/1047840X.2020.1853461
Fried, E. I. (2022). Studying mental health problems as systems, not syndromes. Current Directions in Psychological Science, 31(6), 500–508. https://doi.org/10.1177/09637214221114089
Fried, E. I., Papanikolaou, F., & Epskamp, S. (2022). Mental health and social contact during the COVID-19 pandemic: An ecological momentary assessment study. Clinical Psychological Science, 10(2), 340–354. https://doi.org/10.1177/21677026211017839
Friedman, J., Hastie, T., & Tibshirani, R. (2010). Regularization paths for generalized linear models via coordinate descent. Journal of Statistical Software, 33(1), 1–22. https://doi.org/10.18637/jss.v033.i01
Gates, K. M., Lane, S. T., Varangis, E., Giovanello, K., & Guiskewicz, K. (2017). Unsupervised classification during time-series model building. Multivariate Behavioral Research, 52(2), 129–148. https://doi.org/10.1080/00273171.2016.1256187
Groen, R. N., Snippe, E., Bringmann, L. F., Simons, C. J. P., Hartmann, J. A., Bos, E. H., & Wichers, M. (2019). Capturing the risk of persisting depressive symptoms: A dynamic network investigation of patients’ daily symptom experiences. Psychiatry Research, 271, 640–648. https://doi.org/10.1016/j.psychres.2018.12.054
Hamaker, E. L., Asparouhov, T., Brose, A., Schmiedek, F., & Muthén, B. (2018). At the frontiers of modeling intensive longitudinal data: Dynamic structural equation models for the affective measurements from the COGITO study. Multivariate Behavioral Research, 53(6), 820–841. https://doi.org/10.1080/00273171.2018.1446819
Hehlmann, M. I., Moggia, D., Schwartz, B., Driver, C., Eberhardt, S., & Lutz, W. (in press). Outcome prediction in psychological therapy with continuous time dynamic modeling of affective states and emotion regulation. Journal of Consulting and Clinical Psychology.
Hoekstra, R. H. A., Epskamp, S., & Borsboom, D. (2023). Heterogeneity in individual network analysis: Reality or illusion? Multivariate Behavioral Research, 58(4), 762–786. https://doi.org/10.1080/00273171.2022.2128020
Hoffart, A., Burger, J., Johnson, S. U., & Ebrahimi, O. V. (2023). Daily dynamics and mechanisms of anxious symptomatology in the general population: A network study during the COVID-19 pandemic. Journal of Anxiety Disorders, 93, 102658. https://doi.org/10.1016/j.janxdis.2022.102658
Hofmann, S. G., Curtiss, J. E., & Hayes, S. C. (2020). Beyond linear mediation: Toward a dynamic network approach to study treatment processes. Clinical Psychology Review, 76, 101824. https://doi.org/10.1016/j.cpr.2020.101824
Hofmann, S. G., Curtiss, J., & McNally, R. J. (2016). A Complex network perspective on clinical science. Perspectives on Psychological Science, 11(5), 597–605. https://doi.org/10.1177/1745691616639283
Husen, K., Rafaeli, E., Rubel, J. A., Bar-Kalifa, E., & Lutz, W. (2016). Daily affect dynamics predict early response in CBT: Feasibility and predictive validity of EMA for outpatient psychotherapy. Journal of Affective Disorders, 206, 305–314. https://doi.org/10.1016/j.jad.2016.08.025
IBM. (2020). IBM SPSS statistics for windows (Version 26) [Computer software]. IBM Corp.
Insel, T. R. (2014). The NIMH research domain criteria (RDoC) project: Precision medicine for psychiatry. American Journal of Psychiatry, 171(4), 395–397. https://doi.org/10.1176/appi.ajp.2014.14020138
Isvoranu, A.-M., Abdin, E., Chong, S. A., Vaingankar, J., Borsboom, D., & Subramaniam, M. (2021). Extended network analysis: From psychopathology to chronic illness. BMC Psychiatry, 21, 119. https://doi.org/10.1186/s12888-021-03128-y
Kaplan, E. L., & Meier, P. (1958). Nonparametric estimation from incomplete observations. Journal of the American Statistical Association, 53(282), 457–481. https://doi.org/10.1080/01621459.1958.10501452
Klein, C., Borsche, M., Balck, A., Föh, B., Rahmöller, J., Peters, E., Knickmann, J., Lane, M., Vollstedt, E.-J., Elsner, S. A., Käding, N., Hauswaldt, S., Lange, T., Hundt, J. E., Lehrian, S., Giese, J., Mischnik, A., Niemann, S., Maurer, F., … & Katalinic, A. (2022). One-year surveillance of SARS-CoV-2 transmission of the ELISA cohort: A model for population-based monitoring of infection risk. Science Advances, 8(15). https://doi.org/10.1126/sciadv.abm5016
Klippel, A., Viechtbauer, W., Reininghaus, U., Wigman, J., van Borkulo, C., & MERGE, Myin-Germeys, I., & Wichers, M. (2018). The cascade of stress: A network approach to explore differential dynamics in populations varying in risk for psychosis. Schizophrenia Bulletin, 44(2), 328–337. https://doi.org/10.1093/schbul/sbx037
Kotov, R., Krueger, R. F., Watson, D., Achenbach, T. M., Althoff, R. R., Bagby, R. M., Brown, T. A., Carpenter, W. T., Caspi, A., Clark, L. A., Eaton, N. R., Forbes, M. K., Forbush, K. T., Goldberg, D., Hasin, D., Hyman, S. E., Ivanova, M. Y., Lynam, D. R., Markon, K., & Zimmerman, M. (2017). The hierarchical taxonomy of psychopathology (HiTOP): A dimensional alternative to traditional nosologies. Journal of Abnormal Psychology, 126(4), 454–477. https://doi.org/10.1037/abn0000258
Kwiatkowski, D., Phillips, P. C. B., Schmidt, P., & Shin, Y. (1992). Testing the null hypothesis of stationarity against the alternative of a unit root. Journal of Econometrics, 54(1–3), 159–178. https://doi.org/10.1016/0304-4076(92)90104-Y
Lakhan, R., Agrawal, A., & Sharma, M. (2020). Prevalence of depression, anxiety, and stress during COVID-19 pandemic. Journal of Neurosciences in Rural Practice, 11(4), 519–525. https://doi.org/10.1055/s-0040-1716442
Lane, S. T., Gates, K. M., Fisher, Z., Arizmendi, C., Molenaar, P. C. M., Hallquist, M., Pike, H. K., Henry, T. R., Duffy, K., Luo, L., Beltz, A. M., Wright, A. G. C., Park, J., & Castro-Alvarez, S. (2021). Gimme: Group iterative multiple model estimation. CRAN. https://doi.org/10.32614/CRAN.package.gimme
Lane, S. T., & Gates, K. M. (2017). Automated selection of robust individual-level structural equation models for time series data. Structural Equation Modeling: A Multidisciplinary Journal, 24(5), 768–782. https://doi.org/10.1080/10705511.2017.1309978
Lane, S. T., Gates, K. M., Pike, H. K., Beltz, A. M., & Wright, A. G. C. (2019). Uncovering general, shared, and unique temporal patterns in ambulatory assessment data. Psychological Methods, 24(1), 54–69. https://doi.org/10.1037/met0000192
Li, Z., He, J., Wang, Y., Bai, M., Zhang, Y., Chen, H., & Wang, J. (2023). A cross-sectional study on the mental health of patients with COVID-19 1 year after discharge in Huanggang, China. European archives of psychiatry and clinical neuroscience, 273(2), 301–310. https://doi.org/10.1007/s00406-022-01484-8
Lutz, W., Rubel, J. A., Schwartz, B., Schilling, V., & Deisenhofer, A.-K. (2019). Towards integrating personalized feedback research into clinical practice: Development of the trier treatment navigator (TTN). Behaviour Research and Therapy. https://doi.org/10.1016/j.brat.2019.103438
Lutz, W., Schwartz, B., & Delgadillo, J. (2022). Measurement-based and data-informed psychological therapy. Annual Review of Clinical Psychology, 18, 71–98. https://doi.org/10.1146/annurev-clinpsy-071720-014821
Lutz, W., Schwartz, B., Hofmann, S. G., Fisher, A. J., Husen, K., & Rubel, J. A. (2018). Using network analysis for the prediction of treatment dropout in patients with mood and anxiety disorders: A methodological proof-of-concept study. Scientific Reports. https://doi.org/10.1038/s41598-018-25953-0
Marian, Ş, & Sava, F. A. (2023). Identifying central negative thoughts using experience sampling and network analysis. Cognitive Therapy and Research, 47(5), 707–719. https://doi.org/10.1007/s10608-023-10400-w
Martín-Brufau, R., Suso-Ribera, C., & Corbalán, J. (2020). Emotion network analysis during COVID-19 quarantine—A longitudinal study. Frontiers in Psychology. https://doi.org/10.3389/fpsyg.2020.559572
Melamed, O. C., Hahn, M. K., Agarwal, S. M., Taylor, V. H., Mulsant, B. H., & Selby, P. (2020). Physical health among people with serious mental illness in the face of COVID-19: Concerns and mitigation strategies. General Hospital Psychiatry, 66, 30–33. https://doi.org/10.1016/j.genhosppsych.2020.06.013
Merikangas, K. R., Calkins, M. E., Burstein, M., He, J.-P., Chiavacci, R., Lateef, T., Ruparel, K., Gur, R. C., Lehner, T., Hakonarson, H., & Gur, R. E. (2015). Comorbidity of physical and mental disorders in the neurodevelopmental genomics cohort study. Pediatrics, 135(4), 927–938.
Neal, Z. P., Forbes, M. K., Neal, J. W., Brusco, M., Krueger, R., Markon, K. E., Steinley, D., Wasserman, S., & Wright, A. G. C. (2022). Critiques of network analysis of multivariate data in psychological science. Nature Reviews Methods Primers, 2, 90. https://doi.org/10.1038/s43586-022-00177-9
Nestler, S., & Humberg, S. (2021). GIMME’s ability to recover group-level path coefficients and individual-level path coefficients. Methodology. https://doi.org/10.5964/meth.2863
Niu, X., Taylor, M. M., Wicks, J. J., Fassett-Carman, A. N., Moser, A. D., Neilson, C., Peterson, E. C., Kaiser, R. H., & Snyder, H. R. (2023). Longitudinal relations between emotion regulation and internalizing therapy symptoms in emerging adults during the COVID-19 pandemic. Cognitive and Research, 47(3), 350–366. https://doi.org/10.1007/s10608-023-10366-9
Park, J. J., Chow, S.-M., Fisher, Z. F., & Molenaar, P. C. M. (2020). Affect and personality. European Journal of Psychological Assessment, 36(6), 1009–1023. https://doi.org/10.1027/1015-5759/a000612
Pavlou, M., Ambler, G., Seaman, S., De Iorio, M., & Omar, R. Z. (2016). Review and evaluation of penalised regression methods for risk prediction in low-dimensional data with few events. Statistics in Medicine, 35(7), 1159–1177. https://doi.org/10.1002/sim.6782
Pe, M. L., Kircanski, K., Thompson, R. J., Bringmann, L. F., Tuerlinckx, F., Mestdagh, M., Mata, J., Jaeggi, S. M., Buschkuehl, M., Jonides, J., Kuppens, P., & Gotlib, I. H. (2015). Emotion-network density in major depressive disorder. Clinical Psychological Science, 3(2), 292–300. https://doi.org/10.1177/2167702614540645
Pieper, S., Brosschot, J. F., van der Leeden, R., & Thayer, J. F. (2010). Prolonged cardiac effects of momentary assessed stressful events and worry episodes. Psychosomatic Medicine, 72(6), 570–577. https://doi.org/10.1097/PSY.0b013e3181dbc0e9
R Core Team. (2021). R: A language and environment for statistical computing [Computer software]. R Foundation for Statistical Comupting.
Robinaugh, D., Haslbeck, J., Waldorp, L., Kossakowski, J., Fried, E. I., Millner, A., McNally, R. J., Ryan, O., de Ron, J., van der Maas, H. L. J., van Nes, E. H., Scheffer, M., Kendler, K. S., & Borsboom, D. (2019). Advancing the network theory of mental disorders: A computational model of panic disorder. OpenScienceFramework. https://doi.org/10.31234/osf.io/km37w
Schmittmann, V. D., Cramer, A. O. J., Waldorp, L. J., Epskamp, S., Kievit, R. A., & Borsboom, D. (2013). Deconstructing the construct: A network perspective on psychological phenomena. New Ideas in Psychology, 31(1), 43–53. https://doi.org/10.1016/j.newideapsych.2011.02.007
Schumacher, L., Burger, J., Echterhoff, J., & Kriston, L. (2024). Methodological and Statistical Practices of Using Symptom Networks to Evaluate Mental Health Interventions: A Review and Reflections. Multivariate Behavioral Research. https://doi.org/10.1080/00273171.2024.2335401
Siepe, B., & Heck, D. W. (2023). Multiverse analysis for dynamic network models: Investigating the influence of plausible alternative modeling choices. OpenScienceFramework. https://doi.org/10.31219/osf.io/etm3u
Steegen, S., Tuerlinckx, F., Gelman, A., & Vanpaemel, W. (2016). Increasing transparency through a multiverse analysis. Perspectives on Psychological Science, 11(5), 702–712. https://doi.org/10.1177/1745691616658637
Stekhoven, D. J., & Bühlmann, P. (2012). MissForest—non-parametric missing value imputation for mixed-type data. Bioinformatics, 28(1), 112–118. https://doi.org/10.1093/bioinformatics/btr597
Trabelsi, K., Ammar, A., Masmoudi, L., Boukhris, O., Chtourou, H., Bouaziz, B., Brach, M., Bentlage, E., How, D., Ahmed, M., Mueller, P., Mueller, N., Hsouna, H., Romdhani, M., Hammouda, O., Paineiras-Domingos, L., Braakman-Jansen, A., Wrede, C., Bastoni, S., & Hoekelmann, A. (2021). Globally altered sleep patterns and physical activity levels by confinement in 5056 individuals ECLB COVID-19 international online survey. Biology of Sport, 38(4), 495–506. https://doi.org/10.5114/biolsport.2021.101605
Trapletti, A., Hornik, K., & LeBaron, B. (2023). tseries: Time series analysis and computational finance. R package version 0.10–53. Retrieved from https://CRAN.R-project.org/package=tseries
Tyrer, P. (2020). COVID-19 health anxiety. World Psychiatry, 19(3), 307–308. https://doi.org/10.1002/wps.20798
Uhl, J., Eberhardt, S., Schwartz, B., Rafaeli, E., & Lutz, W. (2024). Emotion dynamics of clients with test anxiety before and after an imagery-based treatment. Journal of Behavior Therapy and Experimental Psychiatry, 82, 101909. https://doi.org/10.1016/j.jbtep.2023.101909
van Borkulo, C., Boschloo, L., Borsboom, D., Penninx, B. W. J. H., Waldorp, L. J., & Schoevers, R. A. (2015). Association of symptom network structure with the course of depression. JAMA Psychiatry, 72(12), 1219–1226. https://doi.org/10.1001/jamapsychiatry.2015.2079
van de Leemput, I. A., Wichers, M., Cramer, A. O. J., Borsboom, D., Tuerlinckx, F., Kuppens, P., van Nes, E. H., Viechtbauer, W., Giltay, E. J., Aggen, S. H., Derom, C., Jacobs, N., Kendler, K. S., van der Maas, H. L. J., Neale, M. C., Peeters, F., Thiery, E., Zachar, P., & Scheffer, M. (2014). Critical slowing down as early warning for the onset and termination of depression. Proceedings of the National Academy of Sciences, 111(1), 87–92. https://doi.org/10.1073/pnas.1312114110
Van Den Bergh, N., Marchetti, I., & Koster, E. H. W. (2020). Bridges over troubled waters: Mapping the interplay between anxiety, depression and stress through network analysis of the DASS-21. Cognitive Therapy and Research, 45(1), 46–60. https://doi.org/10.1007/s10608-020-10153-w
Violant-Holz, V., Gallego-Jiménez, M. G., González-González, C. S., Muñoz-Violant, S., Rodríguez, M. J., Sansano-Nadal, O., & Guerra-Balic, M. (2020). Psychological health and physical activity levels during the COVID-19 pandemic: A systematic review. International Journal of Environmental Research and Public Health. https://doi.org/10.3390/ijerph17249419
Von Hausswolff-Juhlin, Y., Bjartveit, M., Lindström, E., & Jones, P. (2009). Schizophrenia and physical health problems. Acta Psychiatrica Scandinavica, 119, 15–21. https://doi.org/10.1111/j.1600-0447.2008.01309.x
Webb, C. A., Murray, L., Tierney, A. O., & Gates, K. M. (2023). Dynamic processes in behavioral activation therapy for anhedonic adolescents: Modeling common and patient-specific relations. Journal of Consulting and Clinical Psychology, No Pagination Specified-No Pagination Specified. https://doi.org/10.1037/ccp0000830
Wichers, M. (2014). The dynamic nature of depression: A new micro-level perspective of mental disorder that meets current challenges. Psychological Medicine, 44(7), 1349–1360. https://doi.org/10.1017/S0033291713001979
Wigman, J. T. W., van Os, J., Borsboom, D., Wardenaar, K. J., Epskamp, S., Klippel, A., & MERGE, Viechtbauer, W., Myin-Germeys, I., & Wichers, M. (2015). Exploring the underlying structure of mental disorders: Cross-diagnostic differences and similarities from a network perspective using both a top-down and a bottom-up approach. Psychological Medicine, 45(11), 2375–2387. https://doi.org/10.1017/S0033291715000331
Wright, A. G. C., Gates, K. M., Arizmendi, C., Lane, S. T., Woods, W. C., & Edershile, E. A. (2019). Focusing personality assessment on the person: Modeling general, shared, and person specific processes in personality and psychopathology. Psychological Assessment, 31(4), 502–515. https://doi.org/10.1037/pas0000617
Xiong, J., Lipsitz, O., Nasri, F., Lui, L. M., Gill, H., Phan, L., Chen-Li, D., Iacobucci, M., Ho, R., Majeed, A., & McIntyre, R. S. (2020). Impact of COVID-19 pandemic on mental health in the general population: A systematic review. Journal of Affective Disorders, 277, 55–64. https://doi.org/10.1016/j.jad.2020.08.001
Acknowledgements
We gratefully acknowledge the study participants of the ELISA study. We also thank all staff that facilitated the assessment of participants in the ELISA study.
Funding
Open Access funding enabled and organized by Projekt DEAL. The ELISA study was funded by the Federal Ministry of Education and Research (BMBF) within the Sub-project B-FAST of the joint project National Research Network of University Medicine on COVID-19 (BMBF—FKZ 01KX2021), by the State of Schleswig–Holstein, by the Tuberculosis Foundation SH, by intramural funds of the University of Lübeck, and crowdfunding from the citizens of Lübeck organized by the University of Lübeck.
Author information
Authors and Affiliations
Contributions
The ELISA study was designed by Christine Klein, Jan Rupp, and Alexander Katalinic with substantial input from Max Borsche, Alexander Balck, and Bandik Föh who also coordinated data collection. Jan Philipp Klein, Wolfgang Lutz, Nele Assmann, Jana Bommer, and Brian Schwartz conceived of the idea for the analyses presented here. Jana Bommer and Brian Schwartz conducted the statistical analyses and interpreted the results with substantial input from Jan Philipp Klein and Wolfgang Lutz. Jana Bommer wrote the manuscript with substantial input from Brian Schwartz, Jan Philipp Klein, and Wolfgang Lutz. All authors revised the manuscript critically and approved the final version.
Corresponding author
Ethics declarations
Conflict of interest
Jan Philipp Klein received funding for clinical trials (German Federal Ministry of Health, Servier), payments for presentations on internet interventions (GAIA, Oberberg, Servier, Stillachhaus), consulting fees from developers and distributors of internet interventions (all about me, Boehringer, Ethypharm, sympatient), payments for workshops and books (Beltz, Elsevier, Hogrefe and Springer) on psychotherapy for chronic depression and on psychiatric emergencies. He serves as vice chairman of the chapter “Digital Psychiatry” of the German psychiatric Association (DGPPN). The other authors declare that the research was conducted without any commercial or financial relationships construed as a potential conflict of interest.
Ethical Approval
The ELISA study was approved by the ethics committee of the University of Lübeck (Az. 20–150). All participants provided written informed consent before inclusion in the study.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if changes were made. The images or other third party material in this article are included in the article's Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article's Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
Bommer, J., Schwartz, B., Klein, C. et al. A Vicious Cycle? Group-Level Analysis of Intra-Individual Dynamics in Mental Health Variables. Cogn Ther Res (2024). https://doi.org/10.1007/s10608-024-10517-6
Accepted:
Published:
DOI: https://doi.org/10.1007/s10608-024-10517-6