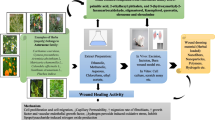
Abstract
Repairing the wound is a multistep process that includes the spatial and temporal synchronization of a different range of cell types to increase the speed of wound contraction, the proliferation of epithelial cells, and collagen formation. The need for proper management of acute wounds to be cured and not turned into chronic wounds is a significant clinical challenge. The traditional practice of medicinal plants in many regions of the world has been used in wound healing since ancient times. Recent scientific research introduced evidence of the efficacy of medicinal plants, their phyto-components, and the mechanisms underlying their wound-repairing activity. This review aims to briefly highlight the wound-curing effect of different plant extracts and purely natural substances in excision, incision, and burn experimental animal models with or without infection of mice, rats (diabetic and nondiabetic), and rabbits in the last 5 years. The in vivo studies represented reliable evidence of how powerful natural products are in healing wounds properly. They have good scavenging activity against Reactive oxygen species (ROS) and anti-inflammatory and antimicrobial effects that help in the process of wound healing. It is evident that incorporating bioactive natural products into wound dressings of bio- or synthetic polymers in nanofiber, hydrogel, film, scaffold, and sponge forms showed promising results in different phases of the wound-curing process of haemostasis, inflammation, growth, re-epithelialization, and remodelling.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
The human body includes different organs. One of them is the skin which occupies a large body area. It represents the outermost defensive covering of the body and an immunological barrier that regularly faces different external factors. It fortifies against mechanical pressure, microbial contagion, and septicity and maintains normal body temperature. It is responsible for the sensation of touch, heat, and cold (Richmond and Harris 2014; Kwiecien et al. 2019; Kumar P and Kothari 2021).
The antimicrobial protective role of different skin layers was evidenced through different previous studies. An external layer displays the composition of human skin outside the epidermis called microbiota, epidermis, dermis, adipose tissue, glands (sweat and sebaceous), and hair follicles (Kwiecien et al. 2019).
Epidermis is composed of keratinocytes, melanocytes, Langerhans’ cells, and Merkel cells. Keratinocytes are a significant type of cells that has a role in vitamin D formation and produce keratin and lipids to form a water barrier. Keratinocytes could act against chemical and biochemical toxins by creating pro-inflammatory cytokines, e.g., interleukins: IL-1α, IL-1β, IL-3, and IL-6, interferons-alpha and beta, transforming growth factors, tumour necrosis factors, and others (Blume-Peytavi et al. 2016). Melanocytes are responsible for skin pigmentation. The first line of protectors of the skin is represented by Langerhans cells. They transport antigens in the skin to the lymph node. The membranes of Merkel cells interact with free nerve endings in the skin, so they have a sensory function. The dermis layer includes the sweat glands, blood vessels, muscles, and sensory neurons (Yousef et al. 2017). Symbiotic microorganisms of bacteria and fungi are recognized as skin colonies with harmless and vital effects in protecting the skin. They are inside hair follicles, sweat and sebaceous glands to protect the skin against invasive and microbial pathogens. Among them, species of Staphylococcus, Malassezia, Demodex folliculorum, and Demodex brevis were the most important (Grice and Segre 2011; Ibrahim et al. 2020).
Wounds have happened due to the loss of histological composition of the skin tissue due to internal or external factors or sequential loss of function in any layer of the skin, which leads to tissue disturbance (Herman and Bordoni 2020). The existence of wounds permits the entrance of different microbial agents as bacteria and viruses or any foreign elements, into the body. Inflammation of skin wounds is happened because of local microbial infections. Also, a generalized systemic infection (septicemia) could be found, a life-threatening condition (Percival 2002). Consequently, more research should be done to find out simple and effective ways of taking care of skin wounds to heal properly. The main goals are to stop bleeding, get rid of microbial infection of wounds, and help wounds to heal effectively without any complications or deformities (Sarabahi et al. 2012; Jones 2015).
Once any damage has occurred to the skin tissue, multiple cellular and extracellular pathways act in a harmonized way, and their functions must be performed in the appropriate order at a suitable time to achieve repair, growth, and tissue regeneration (Richmond and Harris 2014).
Bleeding due to damaged blood vessels must be stopped, which is considered the initial reaction in the process of wound repair, besides platelet stimulation to compose a fibrin clot. Immediately after that, the disturbed tissues discharge growth factors and pro-inflammatory cytokines. Upon controlling the bleeding, many inflammatory cells such as monocytes, macrophages, and neutrophils are gathered at the wound site to provoke the inflammatory response (inflammatory phase). Moreover, the different self and exogenous antigens trigger the immune system to fight against them (Rodrigues et al. 2019; Alotaibi et al. 2021).
Angiogenesis is the following phase, which is parallel to the inflammation phase. The formation of a new blood vessel characterizes this phase. It is then followed by the growth and proliferative phases, which are predominate by fibroblast relocation and propagation, production of the matrix proteins, keratinocyte proliferation, differentiation, and restoration of hair follicles, etc. lastly, the wound healing process is finished with the remodelling of the extracellular matrix (ECM), besides the reordering of granulation tissue to scar tissue. Collagen synthesis and cross-linking afford stability to the healing tissue (Rodrigues et al. 2019). Figure 1 demonstrates the different phases of wound healing, while Table 1 summarizes herbal extracts studied using in vivo wound healing models. Structures of purely natural substances that were investigated using wound healing in vivo models showed in Fig. 2 and Table 2.
Botanical extracts have been extensively utilized in managing wounds in traditional medicine. Therefore, in vitro and in vivo studies have assessed different extracts for their wound-curing characteristics. Their phytochemical content is the purpose of their remedial features in wound repair. Other phytochemicals and plant-derived substances were investigated for their wound-healing activity as flavonols, flavanones, isoflavones, flavanols, flavonolignans, proanthocyanidins (Carvalho et al. 2021), β-glucans (Majtan and Jesenak 2018), bromelain (Fathi et al. 2020), curcumin (Akbik et al. 2014). It was disclosed that different botanicals and medicinal plants are widely used as a topical treatment for wound repairing, such as aloe vera, banana leaves (Sivamani et al. 2012), turmeric, Centella asiatica, Rosmarinus officinalis, Calendula officinalis (Artem Ataide et al. 2018).
Natural products such as plant extracts and other plant-derived products and their phytochemicals assist in managing inflammatory diseases, exert antimicrobial effects, and might aid skin tissue regeneration (Alherz et al. 2022; Attallah NG et al. 2022). They could remove oxidative stress and lower inflammation (Shah and Amini-Nik 2017). The wound-repairing ability of different plant extracts and their actives was confirmed in wound-curing animal models. Such plants improved collagen deposition, the proliferation of epithelial cells, and angiogenesis in diabetic and nondiabetic animal models (Binsuwaidan et al. 2022). Different types of plants are widely used in managing wounds and injuries from previous scientific research (Chingwaru et al. 2019).
The current review demonstrates and focuses on the latest findings in the last 5 years (2018–2022) regarding the in vivo studies of wound repairing effect of different plant extracts, the derived substances from plants, and pure natural substances as a new frontier in treating wounds.
Methods of collecting data
Data collected in the frame of this work were generated by common research engines such as ScienceDirect, Web of Science, PubMed, SciFinder-n, and Scopus, using the references “natural products”, “wound healing” and refining with keywords “animal models”, “burns”, “biological”, “plants” “wound dressings” and “inflammation”. A total of 2194 research items were examined out of which 190 fall into the scope of the review, thus, constituting the baseline of the current survey.
Botanicals and pure natural substances in the preclinical studies
The present review provided the research work, which included the preclinical studies (in vivo) of plant extracts and pure natural substances on wound healing in the last 5 years. The preclinical investigation by using animal models is important for acute and chronic wounds, in vitro studies could be used, but they do not assess the complexity of the wound healing process (Dunn et al. 2013; Zindle et al. 2021). Acute wounds occur through known sequential steps (Zindle et al. 2021). but chronic wounds exhibited impaired or delayed healing. The acute wound heals within 2–3 weeks, followed by the remodelling phase in normal healthy people. The normal healing sequence could be interrupted by other diseases such as diabetes, wound infection, foreign bodies, chronic inflammation, and ischemia. Microbial infection is the famous reason for wound-related morbidity (Said et al. 2009; Rajendran et al. 2018). This led to a physiological imbalance in the mechanism of healing. It might get stuck in one of the phases, and the wound then falls into the non-healing chronic type (FrykbergRobert 2015; Rajendran et al. 2018). It was reported that a wound is not healed in more than 6–8 weeks defined as a chronic/ non-healing wound (Rajendran et al. 2018). The universal goal of all studies about wound healing is to treat acute wounds perfectly in due time, so we avoid conversion into chronic ones and discover the appropriate therapy if the patient suffers from chronic wounds. Patients with chronic wounds suffer from pain, depression due to isolation from the community, and risk of amputation (Ivanková and Belovičová 2020).
Wound healing potentials of various plant extracts
Different studies of the wound-repairing effect of various plant extracts revealed the diversity of actives responsible for this activity. It was suggested that D-pinitol and caffeic acid, the major constituents of Boerhavia diffusa leaf methanol extract, contributed to the wound-healing effect (Juneja et al. 2020). In another study, the fraction contained a high level of polyphenolic compounds, separated from leaves methanol extract of Coccinia grandis showed a remarkable wound repair effect. This effect was due to (rutin), quercetin-3-O-neohesperidin, nicotiflorin, kaempferol-3-O-glucorhamnoside, and astragalin as well as seco-iridoids of oleuropein and ligstroside (Al-Madhagy et al. 2019). HPLC metabolic profiling of the methanol extract of Ephedra ciliata recognized quercetin as a major compound. The antioxidant and antimicrobial activities of quercetin were related to the wound-closure effect of the extract (Yaseen et al. 2020). Biological guided study of E. characias subsp. wulfenii extracts (methanol, n-hexane, and ethyl acetate) of the aerial parts were tested. It was explored that the methanol extract displayed significant wound-repairing activity in circular excision and linear incision wound models, as well as anti-inflammatory effects. This study explored whether quercetin derivatives (quercitrin, hyperoside, and guaijaverin) were responsible for the wound-repairing effect (Özbilgin et al. 2018). Regarding Jacaranda decurrens Cham., metabolic profiling was done to find out ten compounds in the extract of flavonoidal and triterpenoidal nature. It was concluded that these compounds improved the healing of wounds in this study (Serra et al. 2020). Hydroethanolic extract of leaves of Lafoensia pacari A. St.-Hil. was evaluated in accelerating the contraction of wounds. The plant contained punicalagin, ellagic acid, punicalin, kaempferol, quercetin-3-O-xylopyranoside, and quercitrin, which could be related to re-epithelialization, improved cell proliferation, and enhanced remodeling phase of the wounds (Pereira et al. 2018). The mats composed of polyurethane loaded with Nigella sativa oil were studied to assess the in vivo wound-repairing effect (Aras et al. 2021). The essential oil of Nigella sativa seeds contains thymoquinone, which was reported to have wound-healing activity (Haq et al. 2020). Different studies were performed to obtain an effective wound healing process e. g. loaded thymoquinone chitosan- lecithin micelles which keep thymoquinone at the site of wounds with controlled release of the drug (Negi et al. 2020). Hydro-ethanol extract from Vitis labrusca leaves was found to advance the healing of wounds due to the total phenolic and flavonoid content (Santos et al. 2021). Aqueous ethanol extract of Leaves of Curatella americana Linn. exerted remarkable wound healing properties due to its active constituents. Leaves contain compounds known as wound-healing agents, mainly quercetin, kaempferol, glucosides, catechin, and epicatechin (Fujishima et al. 2020). A homogenous polysaccharide was separated from the rhizomes of Curcuma zedoaria and tested in the process of healing wounds in diabetic rats. It was added with platelet-rich plasma exosomes and loaded to a hydrogel sponge of chitosan and silk. It was found that the previous combination was effective and safe to speed the curing of wounds in the case of diabetes (Xu et al. 2018). Methanol extract of Dodonaea viscosa leaves caused accelerated epithelization of excision wounds and increased tensile strength of incision wounds of rats. HPTLC chromatogram showed 10 constituents of flavonoids, tannins, and saponins, including rutin and kaempferol, with reported healing effects (Nayeem et al. 2021).
bio- and synthetic polymers of bioactive substances from natural products
Wound dressings can be created from a combination of bio- and synthetic polymers. Loading them with bioactive substances from natural products increased the good features of this combination. The combined bio- and synthetic polymers may have little or no anti-bacterial, anti-inflammatory, and antioxidant effects (Alven et al. 2020). Loading the bioactive natural product to either the combined polymers or to only one of them eliminates this problem. Bioactive materials such as curcumin (Lüer et al. 2012; Tejada et al. 2016), quercetin (Choudhary et al. 2020; Karuppannan et al. 2022), rutin (Zhou et al. 2021), bromelain (Kalalinia et al. 2021), thymoquinone, gentiopicroside (Almukainzi M. et al. 2022; Almukainzi May et al. 2022), hesperidin (Carvalho et al. 2021), and others were reported to enhance wound healing by adding them to bio- or synthetic polymers or both.
Different types of wound dressings have existed as traditional or passive, e.g., plasters and wool dressing which are not favorable nowadays because of the pain and possible re-skin damage. The interactive wound dressing of synthetic or bio-polymers could be represented as hydrogel, foams, sprays, films, and nanofibers, which introduced a moist environment for wound healing and facilitated water vapor transmission but with a limited anti-bacterial effect. Bioactive wound dressings could be represented by the previously mentioned types of interactive wound dressings, which may be composed of synthetic polymers of polyethylene glycol, polyvinyl pyrrolidone polyurethanes, poly-hydroxyethyl methacrylate, polyglycolic acid, polylactide, poly-ε-caprolactone, as well as biopolymers of pectin, chitosan, cellulose, dextran, and alginate, collagen, which are loaded with antibiotics or growth factors or vitamins, and/or bioactive natural products (Zahedi et al. 2010; Aderibigbe and Buyana 2018; Alven et al. 2020).
The merits of combining synthetic and bio-polymer with bioactive natural products in wound dressings for better wound healing were confirmed in many studies e.g., curcumin (Sharma et al. 2018), quercetin, and rutin (Zhou et al. 2021). Curcumin is the active substance of the roots of turmeric or Curcuma longa. It exerts strong antioxidant and anti-inflammatory, anti-bacterial effects but with low water solubility and oral bioavailability. Curcumin was loaded into bio- and synthetic polymers to overcome this problem (Alven et al. 2020). The combination between bio- and synthetic polymers could overcome the problem of poor mechanical support of bio-polymers (Aycan et al. 2019), besides overcoming the problem of lacking biocompatibility, biodegradability, and bad patient compliance of synthetic polymers (Mir et al. 2018). Effective wound dressing for skin burns represents a challenge to the healthcare system due to the probability of skin structure damage leading to an increased risk of infection. Quercetin and rutin are flavonoids with strong antioxidant, antimicrobial and anti-inflammatory effects but have limited water solubility. It was revealed that incorporating quercetin and rutin into polycaprolactone and chitosan oligosaccharides to form a new bioactive electrospun nanofiber membrane, exhibited superior efficacy among all nanofiber membranes for burn injuries (Zhou et al. 2021).
Regarding diabetic wounds, new scaffolds formed of polyethylene glycolylated graphene oxide collagen hybrid for nanoscale drug delivery of quercetin were tested. It was found that it provided a new scaffold with the advantages of being superior, stable, the controllable release of quercetin, biodegradable nanomaterial, and biocompatible, which permitted collagen formation and angiogenesis. Besides, the mesenchymal stem cells' proliferation and differentiation potential were promoted via adhesion to this scaffold. These new scaffolds could help in solving issues of deficient collagen hyperplasia and insufficient blood supply in the case of diabetic wounds (Chu et al. 2018).
Conclusions and future direction
The current review clarifies that nature introduces medicinal plants with remarkable wound-healing effects. Scientific evidence obtained in the last 5 years has allowed us to expand our knowledge about herbal medicines on wound healing and the underlying molecular mechanisms. Plants, with their natural actives, have the ability to cure wounds and to be utilized in skin wound care. Mainly due to their anti-inflammatory, antimicrobial, and antioxidant activities (Pazyar et al. 2014).
Recent literature has proved that different natural substances, such as flavonoids, saponins, phenolic compounds, and polysaccharides, can operate at various phases of the process through diverse mechanisms and are primarily responsible for the activity of herbal remedies active in wound healing. Polyphenolic compounds have been confirmed therapeutical agents in wound healing by regulating and modulating inflammatory responses. Numerous phytochemicals in medicinal plants have been revealed to be important regulators of homeostasis, re-epithelialization, and regeneration by encouraging fibroblast proliferation and/or collagen formation. Scientific research confirmed the powerful impact of medicinal plants and their phytochemicals in wound management through multiple connected mechanisms (Maver et al. 2015; Artem Ataide et al. 2018).
The development of novel wound care techniques that integrate herbal healing agents with modern products and procedures is in line with current trends in wound healing. Nanostructures and nanoformulations have recently shown promise in overcoming the limitations of conventional medications. They control the release of medicines, lower the dosages needed for healing, and enhance the solubility and effectiveness of water-insoluble herbal components in healing wounds. The optimal dressing for wound treatment is made of nanofibers due to their well-controlled porosity and resemblance to skin tissue. The incorporation of natural materials into nanofibrous architectures for wound dressing has been studied. A biocompatible formulation made of natural herbal extracts would give the consumer a “green” option, and almost fewer side effects once put on the skin.
Based on these findings, it is recommended that many therapeutic approaches be employed concurrently in managing wounds, especially chronic wound injuries, to speed up the healing process and prevent complications. Moreover, various problems need to be resolved to improve the efficacy and utilization of natural substances in wound healing. Multidisciplinary efforts are required to confirm the products’ safety, look at their adverse effects, and do double-blind controlled clinical trials. Good production standards and regulatory regulations are equally essential to increase practitioners’ use of phytotherapy and encourage its incorporation into national health systems.
Data availability
The authors confirm that the data supporting this study are available within the article.
References
Aburjai T, Al-Janabi R, Al-Mamoori F, Azzam H (2019) In vivo wound healing and antimicrobial activity of Alkanna strigose. Wound Med 25(1):100152
Aderibigbe BA, Buyana B (2018) Alginate in wound dressings. Pharmaceutics 10(2):42
Ahmed OM, Mohamed T, Moustafa H, Hamdy H, Ahmed RR, Aboud E (2018) Quercetin and low level laser therapy promote wound healing process in diabetic rats via structural reorganization and modulatory effects on inflammation and oxidative stress. Biomed Pharmacother 101:58–73
Ajmal G, Bonde GV, Mittal P, Khan G, Pandey VK, Bakade BV, Mishra B (2019a) Biomimetic PCL-gelatin based nanofibers loaded with ciprofloxacin hydrochloride and quercetin: a potential anti-bacterial and antioxidant dressing material for accelerated healing of a full thickness wound. Int J Pharm 567:118480
Ajmal G, Bonde GV, Thokala S, Mittal P, Khan G, Singh J, Pandey VK, Mishra B (2019b) Ciprofloxacin HCl and quercetin functionalized electrospun nanofiber membrane: fabrication and its evaluation in full thickness wound healing. Artif Cells Nanomed Biotechnol 47(1):228–240
Akbik D, Ghadiri M, Chrzanowski W, Rohanizadeh R (2014) Curcumin as a wound healing agent. Life Sci 116(1):1–7
Al-Madhagy SA, Mostafa NM, Youssef FS, Awad GE, Eldahshan OA, Singab ANB (2019) Metabolic profiling of a polyphenolic-rich fraction of Coccinia grandis leaves using LC-ESI-MS/MS and in vivo validation of its antimicrobial and wound healing activities. Food Funct 10(10):6267–6275
Algahtani MS, Ahmad MZ, Shaikh IA, Abdel-Wahab BA, Nourein IH, Ahmad J (2021) Thymoquinone loaded topical nanoemulgel for wound healing: formulation design and in-vivo evaluation. Molecules 26(13):3863
Alherz FA, Negm WA, Elekhnawy E, El-Masry TA, Haggag EM, Alqahtani MJ, Hussein IA (2022) Silver nanoparticles prepared using encephalartos laurentianus de wild leaf extract have inhibitory activity against candida albicans clinical isolates. J Fungi 8(10):1005
Ali A, Garg P, Goyal R, Kaur G, Li X, Negi P, Valis M, Kuca K, Kulshrestha S (2021) A novel herbal hydrogel formulation of moringa oleifera for wound healing. Plants 10(1):25
Ali A, Garg P, Goyal R, Khan A, Negi P, Li X, Kulshrestha S (2022) An efficient wound healing hydrogel based on a hydroalcoholic extract of Moringa oleifera seeds. S Afr J Bot 145:192–198
Almukainzi M, El-Masry TA, Negm WA, Elekhnawy E, Saleh A, Sayed AE, Ahmed HM, Abdelkader DH (2022a) Co-delivery of gentiopicroside and thymoquinone using electrospun m-PEG/PVP nanofibers: in-vitro and in vivo studies for antibacterial wound dressing in diabetic rats. Int J Pharm 625:122106
Almukainzi M, El-Masry TA, Negm WA, Elekhnawy E, Saleh A, Sayed AE, Khattab MA, Abdelkader DH (2022b) Gentiopicroside PLGA nanospheres: fabrication, in vitro characterization, antimicrobial action, and in vivo effect for enhancing wound healing in diabetic rats. Int J Nanomed 17:1203
Alotaibi B, Negm WA, Elekhnawy E, El-Masry TA, Elseady WS, Saleh A, Alotaibi KN, El-Sherbeni SA (2021) Antibacterial, immunomodulatory, and lung protective effects of boswellia dalzielii oleoresin ethanol extract in pulmonary diseases in vitro and in vivo studies. Antibiotics 10(12):1444
Aaa A, Attalah Oran S, Shakhanbeh JM (2022) In vitro and in vivo wound healing activities of Globularia arabica leaf methanolic extract in diabetic rats. J Cosmet Dermatol 2(10):4888–4900
Alsareii SA, Alzerwi NA, AlAsmari MY, Alamri AM, Mahnashi MH, Shaikh IA (2022) Topical application of premna integrifolia linn on skin wound injury in rats accelerates the wound healing process: evidence from in vitro and in vivo experimental models. Evid-Based Complement Altern Med. 2022:1–14
Alven S, Nqoro X, Aderibigbe BA (2020) Polymer-based materials loaded with curcumin for wound healing applications. Polymers 12(10):2286
Aras C, Tümay Özer E, Göktalay G, Saat G, Karaca E (2021) Evaluation of Nigella sativa oil loaded electrospun polyurethane nanofibrous mat as wound dressing. J Biomater Sci Polym Ed 32(13):1718–1735
Artem Ataide J, Caramori Cefali L, Machado Croisfelt F, Arruda Martins Shimojo A, Oliveira-Nascimento L, Gava MP (2018) Natural actives for wound healing: a review. Phytother Res 32(9):1664–1674
Attallah NG, Elekhnawy E, Negm WA, Hussein IA, Mokhtar FA, Al-Fakhrany OM (2022) In vivo and in vitro antimicrobial activity of biogenic silver nanoparticles against Staphylococcus aureus clinical isolates. Pharmaceuticals 15(2):194
Attallah NGM, Negm WA, Elekhnawy E, Elmongy EI, Altwaijry N, El-Haroun H, El-Masry TA, El-Sherbeni SA (2021) Elucidation of phytochemical content of cupressus macrocarpa leaves in vitro and in vivo anti-bacterial effect against methicillin-resistant staphylococcus aureus clinical isolates. Antibiotics (basel). 10(8):890
Aycan D, Selmi B, Kelel E, Yildirim T, Alemdar N (2019) Conductive polymeric film loaded with ibuprofen as a wound dressing material. Eur Polymer J 121:109308
Ayu CA, Weta IW, Aman IGM (2020) Moringa (Moringa oleifera) leaves extract gel improved wound healing by increasing fibroblasts, neovascularization and in male Wistar rats. IJAAM (indones J Anti-Aging Med). 4(1):28–32
Bagher Z, Ehterami A, Safdel MH, Khastar H, Semiari H, Asefnejad A, Davachi SM, Mirzaii M, Salehi M (2020) Wound healing with alginate/chitosan hydrogel containing hesperidin in rat model. J Drug Deliv Sci Technol 55:101379
Bihani T, Mhaske N (2020) Evaluation of in vivo wound healing activity of Plumeria obtusa L. (Champa) spray in rats. Wound Med. 28:100176
Binsuwaidan R, Elekhnawy E, Elseady WS, Keshk WA, Shoeib NA, Attallah NG, Mokhtar FA, Abd El Hadi SR, Ahmed E, Magdeldin S (2022) Anti-bacterial activity and wound healing potential of Cycas thouarsii R. Br n-butanol fraction in diabetic rats supported with phytochemical profiling. Biomed Pharmacother 155:113763
Blume-Peytavi U, Tan J, Tennstedt D (2016) Fragility of epidermis in newborns, children and adolescents (vol 30, pg 3, 2016). J Europ Acade Dermatol Venereol 30(9):1634–1634
Boakye YD, Agyare C, Ayande GP, Titiloye N, Asiamah EA, Danquah KO (2018) Assessment of wound-healing properties of medicinal plants: the case of Phyllanthus muellerianus. Front Pharmacol 9:945
Boudjelal A, Napoli E, Benkhaled A, Benazi L, Bey R, Gentile D, Ruberto G (2022) In vivo wound healing effect of Italian and Algerian Pistacia vera L. resins. Fitoterapia 159:105197
Carvalho MTB, Araújo-Filho HG, Barreto AS, Quintans-Júnior LJ, Quintans JSS, Barreto RSS (2021) Wound healing properties of flavonoids: A systematic review highlighting the mechanisms of action. Phytomedicine 90:153636
Chen L-Y, Cheng H-L, Kuan Y-H, Liang T-J, Chao Y-Y, Lin H-C (2021) Therapeutic potential of luteolin on impaired wound healing in streptozotocin-induced rats. Biomedicines 9(7):761
Chingwaru C, Bagar T, Maroyi A, Kapewangolo PT, Chingwaru W (2019) Wound healing potential of selected Southern African medicinal plants: a review. J Herb Med 17–18:100263
Choudhary A, Kant V, Jangir BL, Joshi VG (2020) Quercetin loaded chitosan tripolyphosphate nanoparticles accelerated cutaneous wound healing in Wistar rats. Eur J Pharmacol 880:173172
Chu J, Shi P, Yan W, Fu J, Yang Z, He C, Deng X, Liu H (2018) PEGylated graphene oxide-mediated quercetin-modified collagen hybrid scaffold for enhancement of MSCs differentiation potential and diabetic wound healing. Nanoscale 10(20):9547–9560
Du X, Wu L, Yan H, Jiang Z, Li S, Li W, Bai Y, Wang H, Cheng Z, Kong D et al (2021) Microchannelled alkylated chitosan sponge to treat noncompressible hemorrhages and facilitate wound healing. Nat Commun 12(1):4733
Dunn L, Prosser HC, Tan JT, Vanags LZ, Ng MK, Bursill CA (2013) Murine model of wound healing. JoVE (j Visual Exp) 75:e50265
El-ezz A, Abdel-Rahman LH, Al-Farhan BS, Mostafa DA, Ayad EG, Basha MT, Abdelaziz M, Abdalla EM (2022) Enhanced in vivo wound healing efficacy of a novel hydrogel loaded with copper (II) schiff base quinoline complex (CuSQ) solid lipid nanoparticles. Pharmaceuticals 15(8):978
Elloumi W, Mahmoudi A, Ortiz S, Boutefnouchet S, Chamkha M, Sayadi S (2022) Wound healing potential of quercetin-3-O-rhamnoside and myricetin-3-O-rhamnoside isolated from Pistacia lentiscus distilled leaves in rats model. Biomed Pharmacother 146:112574
Fathi AN, Sakhaie MH, Babaei S, Babaei S, Slimabad F, Babaei S (2020) Use of bromelain in cutaneous wound healing in streptozocin-induced diabetic rats: an experimental model. J Wound Care 29(9):488–495
Frykberg Robert G (2015) Challenges in the treatment of chronic wounds. Advan Wound Care. 4(9):560–582
Fu J, Huang J, Lin M, Xie T, You T (2020) Quercetin promotes diabetic wound healing via switching macrophages from M1 to M2 polarization. J Surg Res 246:213–223
Fujishima MAT, Sa DMC, Lima CMDS, Bittencourt JAH, Pereira WLA, Muribeca AdJB, Silva ECYY, de Silva MN, de Sousa FFO, Dos Santos CB (2020) Chemical profiling of Curatella americana Linn leaves by UPLC-HRMS and its wound healing activity in mice. PLoS ONE 15(1):0225514
Gebremeskel L, Bhoumik D, Sibhat GG, Tuem KB (2018) In vivo wound healing and anti-inflammatory activities of leaf latex of aloe megalacantha baker (Xanthorrhoeaceae). Evid-Based Complement Altern Med. 2018:1–7
Grice EA, Segre JA (2011) The Skin Microbiome. Nat Rev Microbiol 9(4):244–253
Haq A, Kumar S, Mao Y, Berthiaume F, Michniak-Kohn B (2020) Thymoquinone-loaded polymeric films and hydrogels for bacterial disinfection and wound healing. Biomedicines 8(10):386
Herman TF, Bordoni B. 2020. Wound classification.
Hernandez-Hernandez AB, Alarcon-Aguilar FJ, Garcia-Lorenzana M, Rodriguez-Monroy MA, Canales-Martinez MM (2021) Jatropha neopauciflora Pax latex exhibits wound-healing effect in normal and diabetic mice. J Evid-Based Integrat Med. 26:2515690X20986762
Hou Y, Xin M, Li Q, Wu X (2021) Glycyrrhizin micelle as a genistein nanocarrier: Synergistically promoting corneal epithelial wound healing through blockage of the HMGB1 signaling pathway in diabetic mice. Exp Eye Res 204:108454
Ibrahim AAE, Bagherani N, Smoller BR, Reyes-Baron C, Bagherani N (2020) Functions of the Skin. In: Smoller B, Bagherani N (eds) Atlas of Dermatology, Dermatopathology and Venereology. Springer International Publishing, Cham, pp 1–11
Ivanková V, Belovičová M 2020 Consequences of chronic wounds on patient’s lif. Укpaїнa Здopoв’я нaцiї. 2(3).
Jangde R, Srivastava S, Singh MR, Singh D (2018) In vitro and In vivo characterization of quercetin loaded multiphase hydrogel for wound healing application. Int J Biol Macromol 115:1211–1217
Jee J-P, Pangeni R, Jha SK, Byun Y, Park JW (2019) Preparation and in vivo evaluation of a topical hydrogel system incorporating highly skin-permeable growth factors, quercetin, and oxygen carriers for enhanced diabetic wound-healing therapy. Int J Nanomed 14:5449
Jones ML (2015) A short history of the development of wound care dressings. Brit J Healthcare Assist 9(10):482–485
Juneja K, Mishra R, Chauhan S, Gupta S, Roy P, Sircar D (2020) Metabolite profiling and wound-healing activity of Boerhavia diffusa leaf extracts using in vitro and in vivo models. J Tradit Complement Med 10(1):52–59
Kalalinia F, Aamiri N, Bayat S, Movaffagh J, Hahsemi M (2021) 671 burn wound healing effect of bromelain-loaded chitosan nanofibers. J Burn Care Res 42(1):S192–S192
Kant V, Jangir BL, Kumar V, Nigam A, Sharma V (2020a) Quercetin accelerated cutaneous wound healing in rats by modulation of different cytokines and growth factors. Growth Fact 38(2):105–119
Kant V, Kumar M, Jangir BL, Kumar V 2020b Temporal effects of different vehicles on wound healing potentials of quercetin: biochemical, molecular, and histopathological approaches. The International Journal of Lower Extremity Wounds:1534734620977582.
Karuppannan SK, Dowlath MJH, Ramalingam R, Musthafa SA, Ganesh MR, Chithra V, Ravindran B, Arunachalam KD (2022) Quercetin functionalized hybrid electrospun nanofibers for wound dressing application. Mater Sci Eng, B 285:115933
Kuma DN, Boye A, Kwakye-Nuako G, Boakye YD, Addo JK, Asiamah EA, Aboagye EA, Martey O, Essuman MA, Atsu Barku VY (2022) Wound healing properties and antimicrobial effects of parkia clappertoniana keay fruit husk extract in a rat excisional wound model. BioMed Res Intern. https://doi.org/10.1155/2022/9709365
Kumar P, Kothari V (2021) Wound healing research: current trends and future directions. Springer Singapore, Singapore
Kumar S, Kumar A, Kumar N, Singh P, Singh TU, Singh BR, Gupta PK, Thakur VK (2022) In vivo therapeutic efficacy of Curcuma longa extract loaded ethosomes on wound healing. Vet Res Commun 46(4):1033–1049
Kwiecien K, Zegar A, Jung J, Brzoza P, Kwitniewski M, Godlewska U, Grygier B, Kwiecinska P, Morytko A, Cichy J (2019) Architecture of antimicrobial skin defense. Cytokine Growth Factor Rev 49:70–84
Lambebo MK, Kifle ZD, Gurji TB, Yesuf JS (2021) Evaluation of wound healing activity of methanolic crude extract and solvent fractions of the leaves of vernonia auriculifera hiern (asteraceae) in mice. J Exp Pharmacol 13:677
Lee G, Ko Y-G, Bae KH, Kurisawa M, Kwon OK, Kwon OH (2022) Green tea catechin-grafted silk fibroin hydrogels with reactive oxygen species scavenging activity for wound healing applications. Biomat Res. 26(1):1–6
Lüer S, Troller R, Aebi C (2012) Anti-bacterial and antiinflammatory kinetics of curcumin as a potential antimucositis agent in cancer patients. Nutr Cancer 64(7):975–981
Majtan J, Jesenak M (2018) β-Glucans: multi-functional modulator of wound healing. Molecules 23(4):806
Msarabahi S, Tiwari V, Bhattacharya S (2012) Principles and practice of wound care. Thieme Med Sci Pub Private Ltd. 45(1):167–169
Maver T, Maver U, Stana Kleinschek K, Smrke DM, Kreft S (2015) A review of herbal medicines in wound healing. Int J Dermatol 54(7):740–751
Mir M, Ali MN, Barakullah A, Gulzar A, Arshad M, Fatima S, Asad M (2018) Synthetic polymeric biomaterials for wound healing: a review. Prog Biomater 7(1):1–21
Nayeem N, Asdaq SMB, Alamri AS, Alsanie WF, Alhomrani M, Mohzari Y, Alrashed AA, Alotaibi N, Alharbi MA, Aldhawyan NN (2021) Wound healing potential of Dodonaea viscosa extract formulation in experimental animals. J King Saud Univ-Sci 33(5):101476
Negi P, Sharma G, Verma C, Garg P, Rathore C, Kulshrestha S, Lal UR, Gupta B, Pathania D (2020) Novel thymoquinone loaded chitosan-lecithin micelles for effective wound healing: development, characterization, and preclinical evaluation. Carbohyd Polym 230:115659
Negm WA, El-Kadem AH, Elekhnawy E, Attallah NGM, Al-Hamoud GA, El-Masry TA, Zayed A (2022) Wound-healing potential of rhoifolin-rich fraction isolated from sanguisorba officinalis roots supported by enhancing re-epithelization, angiogenesis, anti-inflammatory, and antimicrobial effects. Pharmaceuticals (basel) 15(2):178
Nordin A, Kamal H, Yazid MD, Saim A, Idrus R (2019) Effect of Nigella sativa and its bioactive compound on type 2 epithelial to mesenchymal transition: a systematic review. BMC Complement Altern Med 19(1):290
Okur ME, Karadağ AE, Üstündağ Okur N, Özhan Y, Sipahi H, Ayla Ş, Daylan B, Demirci B, Demirci F (2020) In vivo wound healing and in vitro anti-inflammatory activity evaluation of Phlomis russeliana extract gel formulations. Molecules 25(11):2695
Özay Y, Güzel S, Erdoğdu İH, Pehlivanoğlu B, Aydın Türk B, Darcan S (2018) Evaluation of the wound healing properties of luteolin ointments on excision and incision wound models in diabetic and nondiabetic rats. Rec Nat Prod. 12(4):350–366
Özay Y, Güzel S, Yumrutaş Ö, Pehlivanoğlu B, Erdoğdu İH, Yildirim Z, Türk BA, Darcan S (2019) Wound healing effect of kaempferol in diabetic and nondiabetic rats. J Surg Res 233:284–296
Özbilgin S, Acıkara ÖB, Akkol EK, Süntar I, Keleş H, İşcan GS (2018) In vivo wound-healing activity of Euphorbia characias subsp. wulfenii: Isolation and quantification of quercetin glycosides as bioactive compounds. J Ethnopharmacol 224:400–408
Parveen A, Kulkarni N, Yalagatti M, Abbaraju V, Deshpande R (2018) In vivo efficacy of biocompatible silver nanoparticles cream for empirical wound healing. J Tissue Viability 27(4):257–261
Pazyar N, Yaghoobi R, Rafiee E, Mehrabian A, Feily A (2014) Skin wound healing and phytomedicine: a review. Skin Pharmacol Physiol 27(6):303–310
Percival NJ (2002) Classification of wounds and their management. Surg Infect (larchmt) 20(5):114–117
Pereira LOM, Vilegas W, Tangerina MMP, Arunachalam K, Balogun SO, Orlandi-Mattos PE, Colodel EM, Martins DTdO (2018) Lafoensia pacari A. St.-Hil.: wound healing activity and mechanism of action of standardized hydroethanolic leaves extract. J Ethnopharmacol 219:337–350
Rajendran NK, Kumar SSD, Houreld NN, Abrahamse H (2018) A review on nanoparticle based treatment for wound healing. J Drug Deliv Sci Technol 44:421–430
Rajoo A, Ramanathan S, Mansor SM, Sasidharan S (2021) Formulation and evaluation of wound healing activity of Elaeis guineensis Jacq leaves in a Staphylococcus aureus infected Sprague Dawley rat model. J Ethnopharmacol 266:113414
Rathod L, Bhowmick S, Patel P, Sawant K (2022) Calendula flower extract loaded collagen film exhibits superior wound healing potential: Preparation, evaluation, in-vitro & in-vivo wound healing study. J Drug Deliv Sci Technol 72:103363
Richmond JM, Harris JE (2014) Immunology and skin in health and disease. Cold Spring Harb Perspect Med 4(12):a015339
Rodrigues M, Kosaric N, Bonham CA, Gurtner GC (2019) Wound healing: a cellular perspective. Physiol Rev 99(1):665–706
Said HK, Roy NK, Gurjala AN, Mustoe TA (2009) Quantifying tissue level ischemia: Hypoxia response element-luciferase transfection in a rabbit ear model. Wound Rep Regenerat 17(4):473–479
Santos TS, Santos IDDd, Pereira-Filho RN, Gomes SVF, Lima-Verde IB, Marques MN, Cardoso JC, Severino P, Souto EB, Albuquerque-Júnior RLCd (2021) Histological evidence of wound healing improvement in rats treated with oral administration of hydroalcoholic extract of vitis labrusca. Curr Issues Mol Biol 43(1):335–352
Serra MB, Barroso WA, Rocha C, Furtado PGR, Borges ACR, Silva SN, Tangerina MMP, Nascimento JRd, Vilegas W, Alves AC et al (2020) Chemical characterization and wound healing property of jacaranda decurrens cham. (Bignoniaceae): an experimental study based on molecular mechanisms. Evid-Based Complement Altern Med. 2020:4749712
Shady NH, Soltane R, Maher SA, Saber EA, Elrehany MA, Mostafa YA, Sayed AM, Abdelmohsen UR (2022) Wound healing and antioxidant capabilities of zizyphus mauritiana fruits: in-vitro, in-vivo, and molecular modeling study. Plants 11(11):1392
Shah A, Amini-Nik S (2017) The role of phytochemicals in the inflammatory phase of wound healing. Int J Mol Sci 18(5):1068
Sharma M, Sahu K, Singh SP, Jain B (2018) Wound healing activity of curcumin conjugated to hyaluronic acid: in vitro and in vivo evaluation. Artif Cell Nanomed Biotechnol 46(5):1009–1017
Sivamani RK, Ma BR, Wehrli LN, Maverakis E (2012) Phytochemicals and naturally derived substances for wound healing. Adv Wound Care 1(5):213–217
Taddese SM, Gurji TB, Abdulwuhab M, Aragaw TJ (2021) Wound healing activities of hydromethanolic crude extract and solvent fractions of bersama abyssinica leaves in mice. Evid-Based Complement Altern Med. 2021:1–20
Tan WS, Arulselvan P, Ng S-F, Mat Taib CN, Sarian MN, Fakurazi S (2019) Improvement of diabetic wound healing by topical application of Vicenin-2 hydrocolloid film on Sprague Dawley rats. BMC Complement Altern Med 19(1):20
Taskan MM, Yuce HB, Karatas O, Gevrek F (2019) Topical quercetin gel application improved wound healing in Wistar rats. Annal Med Res 26(10):2397
Tejada S, Manayi A, Daglia M, Nabavi FS, Sureda A, Hajheydari Z, Gortzi O, Pazoki-Toroudi H, Nabavi MS (2016) Wound healing effects of curcumin: a short review. Curr Pharmaceut Biotechnol. 17(11):1002–1007
Tekleyes B, Huluka SA, Wondu K, Wondmkun YT (2021) Wound healing activity of 80% methanol leaf extract of zehneria scabra (lf) sond (cucurbitaceae) in mice. J Exp Pharmacol 13:537
Tessema Z, Molla Y (2021) Evaluation of the wound healing activity of the crude extract of root bark of Brucea antidysentrica, the leaves of Dodonaea angustifolia and Rhamnus prinoides in mice. Heliyon 7(1):e05901
Upadhyay G, Tiwari N, Maurya H, Upadhyay J, Joshi R, Ansari MN (2021) In vivo wound-healing and antioxidant activity of aqueous extract of Roylea elegans leaves against physically induced burn model in Wistar albino rats. Biotech 11(10):442
Wang L, Hu L, Peng Z, Cao H, Cao D, Long Y, Zou Z (2022) Luteolin is an effective component of platycodon grandiflorus in promoting wound healing in rats with cutaneous scald injury. Clin Cosmet Investig Dermatol 15:1715–1727
Wayal SR, Gurav SS (2021) Evaluation of wound healing potential of Bhallatakadi Ghrita–cow ghee based polyherbal formulation: in-vivo excision and incision wound model. J Complement Integrat Med 18(3):507–515
Xu N, Wang L, Guan J, Tang C, He N, Zhang W, Fu S (2018) Wound healing effects of a Curcuma zedoaria polysaccharide with platelet-rich plasma exosomes assembled on chitosan/silk hydrogel sponge in a diabetic rat model. Int J Biol Macromol 117:102–107
Yaseen HS, Asif M, Saadullah M, Asghar S, Shams MU, Bazmi RR, Saleem M, Yousaf HM, Yaseen M (2020) Methanolic extract of Ephedra ciliata promotes wound healing and arrests inflammatory cascade in vivo through downregulation of TNF-α. Inflammopharmacology 28(6):1691–1704
Yin G, Wang Z, Wang Z, Wang X (2018) Topical application of quercetin improves wound healing in pressure ulcer lesions. Exp Dermatol 27(7):779–786
Yousef H, Alhajj M, Sharma S. 2017. Anatomy, skin (integument), epidermis.
Yuan X, Han L, Fu P, Zeng H, Lv C, Chang W, Runyon RS, Ishii M, Han L, Liu K et al (2018) Cinnamaldehyde accelerates wound healing by promoting angiogenesis via up-regulation of PI3K and MAPK signaling pathways. Lab Invest 98(6):783–798
Zahedi P, Rezaeian I, Ranaei-Siadat SO, Jafari SH, Supaphol P (2010) A review on wound dressings with an emphasis on electrospun nanofibrous polymeric bandages. Polym Adv Technol 21(2):77–95
Zhou L, Cai L, Ruan H, Zhang L, Wang J, Jiang H, Wu Y, Feng S, Chen J (2021) Electrospun chitosan oligosaccharide/polycaprolactone nanofibers loaded with wound-healing compounds of Rutin and Quercetin as anti-bacterial dressings. Int J Biol Macromol 183:1145–1154
Zindle JK, Wolinsky E, Bogie KM (2021) A review of animal models from 2015 to 2020 for preclinical chronic wounds relevant to human health. J Tissue Viability 30(3):291–300
Funding
Open access funding provided by The Science, Technology & Innovation Funding Authority (STDF) in cooperation with The Egyptian Knowledge Bank (EKB). This review received no external funding.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflicts of interest
The authors declare no conflict of interest.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if changes were made. The images or other third party material in this article are included in the article's Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article's Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
El-Sherbeni, S.A., Negm, W.A. The wound healing effect of botanicals and pure natural substances used in in vivo models. Inflammopharmacol 31, 755–772 (2023). https://doi.org/10.1007/s10787-023-01157-5
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10787-023-01157-5