Abstract
Introduction
This study examined Vickers hardness as well as surface characteristics of different computer-aided design/computer-aided manufacturing (CAD/CAM) resin composites prior to and after storage in various media.
Materials and methods
CAD/CAM resin composite blocks (Grandio Blocs (GB), Lava Ultimate (LU), Brilliant Crios (BC), Cerasmart (GC), Shofu Block HC (SB), Tetric CAD (TC), Luxacam Composite (LC); incl. different translucency variants) were prepared, polished and surface free energy was determined. The specimens were divided into four groups: dry conditions for 24 h (25 °C), demineralized water (37 °C), Pepsi Cola (37 °C) and 75% ethanol (37 °C). After seven and 28 days of storage, Vickers hardness was determined. Surface roughness was measured after the entire storage period.
Results and discussion
Vickers hardness was in the range of about 150 HV for GB, around 115 HV for LU, and 80–100 HV for BC, GC, SB, TC and LC. Only minor differences (total: 50.2 (6.4)–56.2 (3.2) mN/m) in surface free energy could be detected. No relationship was observed between surface free energy and filler content. However, a correlation between filler content and Vickers hardness was evident. Artificial aging caused a decrease of Vickers hardness (up to −40 HV or 35%) depending on storage media, duration and material. The changes in surface texture after immersion in different media were below a value of ΔSa = 0.015 µm.
Conclusion
Artificial aging of CAD/CAM resin composites leads to a significant decrease of Vickers hardness for most materials, while only small changes in surface roughness were identified.
Graphical Abstract

Similar content being viewed by others
Explore related subjects
Discover the latest articles, news and stories from top researchers in related subjects.Avoid common mistakes on your manuscript.
1 Introduction
For the fabrication of tooth-colored, monolithic restorations, indirect resin-based composites (RBC) are an alternative to commonly used ceramics [1, 2]. In contrast to chair-side polymerizing direct resin-based composites, CAD/CAM (computer-aided design/computer-aided manufacturing) resin composites (synonym for indirect RBC) are industrially manufactured and milled after the digital design of the restoration [1]. Polymerization under high temperature and high pressures under industrial conditions produces higher polymerization rates than in direct composites (over 90%) [2]. This results in improved mechanical properties (flexural strength, hardness, density) [3] as well as reduced biofilm formation on the surface of the materials [4].
CAD/CAM resin composites consist of an organic resin matrix, inorganic fillers, and a bonding agent [1, 5]. The inorganic filler particles used in this process have a mostly amorphous character with a mass fraction of 62–83% [6]. Based on Ferracane’s classification, they are classified as “midfill hybrid composites” [7]. Additional sintering after the milling process as necessary for the most of ceramic materials is not required for CAD/CAM resin composites [2], which relevantly reduces laboratory time.
With regard to Vickers hardness (VH), Young’s modulus (E), and brittleness, in contrast to commonly used silicate ceramics (VH: 452.9–595.1; E = 61.0 GPa–67.2 GPa) CAD/CAM resin composites (VH: 62.2–102.3; E = 12.1 GPa–16.0 GPa) exhibit mechanical properties comparable to those of those of natural teeth (enamel: VH = 313.3 (22.7); E: 59.7 (13.0) GPa; dentin: VH: 62.3 (3.3); E: 16.5 (2.3) GPa) [8,9,10]. Especially in patients with parafunctions, these properties might help to reduce abrasion of the restoration as well as antagonists [11,12,13]. The fracture strength of crowns fabricated from different CAD/CAM resin composites has been reported to be similar to crowns fabricated from lithium disilicate ceramics and sufficient for molar bite force [14].
Since the application of CAD/CAM resin composites as dental materials for the fabrication of monolithic dental restorations is a rather novel approach, there is a lack of studies that investigate the clinical long-term behavior of corresponding restorations [15]. Previous results show a survival rate of 100% after one year for posterior onlays [16] and a clinical success rate of 95.0% after twelve months and 85.7% after 24 months for partial crowns [17]. A retrospective study over three years with CAD/CAM resin composite crowns reported a survival rate up to 96.4% [18]. As a result of nutrition, dental materials are exposed to different environments and must tolerate temperature fluctuations. The influence of such factors on the survival rate of restorations has been proven by various studies [19,20,21]. Especially for direct composites, a relevant influence of various media on the mechanical properties of the materials has been identified. For instance, both a decrease in Vickers hardness and an increase in surface roughness due to artificial aging by immersion in water or water-ethanol mixtures have been reported [22,23,24]. In particular, the chemical influence of ethanol by a degradation of the resin matrix and a disintegration of filler-silan-bonds have also been described [25,26,27].
These aging effects are reduced in materials with high filler/matrix proportions as well as those with a hydrophobic resin matrix [9, 22]. Although degradation of glass fillers due to storage in solvents has been proven [28], this effect seems to be subordinate [29]. By comparing several in vitro and in vivo studies, it was shown that storage in ethanol is associated with both a decrease in flexural strength and clinical performance in the form of chipping and/or fracture, or loss of anatomical form due to wear [27]. However, such correlations could not be identified for storage in water—although it is widely used as medium for simulating aging processes [22, 23].
Furthermore, a decrease in the fracture load of crowns made of CAD/CAM resin composites due to thermocycling [30] and a decrease in the flexural strength of CAD/CAM resin composites after storage in water (37 °C) for 30 days have been reported [31]. Acidic beverages such as Coca Cola also caused a reduction of Vickers hardness after 7 and 28 days of exposure, and CAD/CAM resin composites were more affected than ceramic materials. However, due to an underrepresentation of commercially available CAD/CAM resin composites, no correlation with physical properties could be drawn in this regard [32]. Furthermore, Ilie (2019) showed that accelerated aging has a higher impact on micromechanical properties such as Vickers hardness or indentation modulus than macroscale effects in terms of clinical performance such as chipping [33].
Microorganisms organized in oral biofilms are closely associated with the development of caries [34], gingivitis, periodontitis [35], and spreading infections [36]. Therefore, it is of clinical importance to minimize the formation of biofilm on the surface of dental restorations. High surface roughness promotes microbial adhesion [37, 38] by increasing the contact area between the organisms and the restoration surface [39] and reducing shear forces that result from salivary flow [40]. In the past, an Ra value (arithmetic mean height) of less than 0.2 µm has been established as a widely accepted threshold below which no significant further reduction in biofilm accumulation can be achieved by additional polishing [40, 41]. In this context, high surface roughness favors initial attachment of cells [42], while further growth and colonization of the biofilm occurs regardlessly of surface texture. With regard to RBCs, a relationship between roughness and biofilm formation is evident [43, 44]. Indirect composites generally showed less microbial attachment compared to direct composites under shear forces, but not under closed culture conditions [4].
For CAD/CAM resin composites, there are only few studies investigating the effects of artificial aging on mechanical properties, and the impact of different RBC formulations in materials of different manufacturers or the influence of translucency variants have largely been neglected [9, 33, 45]. Against this background, the present study investigates the surface characteristics of commercially available CAD/CAM resin composites by surveying vickers hardness, surface texture, surface free energy as well as potential correlations and their dependency on exposure to different aging media. The null hypotheses (H0) were as follows:
H0 (a) There is no difference between CAD/CAM resin composites with different translucencies in terms of Vickers hardness and surface energy.
H0 (b) There is no correlation between Vickers hardness or surface free energy and a previously investigated filler content of CAD/CAM resin composites [6].
H0 (c) There is no loss in Vickers hardness after aging in different storage media for the different CAD/CAM resin composites.
H0 (d) There is no difference in surface roughness after aging in different storage media for the different CAD/CAM resin composites.
2 Materials and methods
2.1 Materials
Different commercially available CAD/CAM resin composite blocks were used (Table 1). In order to compare the dependency of the individual performance of the materials on the grade of translucency, low/medium- (LT/MT) as well as high-translucency (HT) variants were analyzed where available.
2.2 Methods
2.2.1 Sample preparation
The CAD/CAM blocks were cut into rectangular slices (n = 104) with a thickness of 3 mm using the IsoMet®4000 Linear Precision saw (Buehler Ltd., Lake Bluff, IL, USA) under constant water irrigation (according to ISO 6872) [46]. All specimens were polished using a semi-automatic polishing unit “Pedemin-2/DAV-5” (Struers GmbH, Willich, Germany) and a standardized polishing regime employing silicon carbide papers with successively decreasing grain size (P220, P500, P1200, P2000, P4000) under water cooling and 300 rpm for 15 s, respectively. The samples were then cleaned in an ultrasonic bath (Bandelin electronic GmbH & Co. KG, Berlin, Germany) with demineralized water for ten minutes and randomized into four groups:
Group 1: Specimens were stored under dry conditions for 24 h at room temperature. Subsequently, Vickers hardness and surface roughness was determined.
Group 2: Specimens were stored in demineralized water at 37 °C.
Group 3: Specimens were stored in 75% ethanol/ demineralized water solution at 37 °C.
Group 4: Specimen were stored in Pepsi Cola at 37 °C.
In groups 2–4, Vickers hardness was measured after seven days and 28 days of storage and surface roughness after the entire storage period of 28 days.
2.2.2 Vickers hardness
Vickers hardness (VH) was determined with a microhardness tester (MHT-4, Anton Paar Group AG, Graz, Austria) in combination with research light microscope (Microphot-FXA, Nikon Corp., Tokio, Japan) under a 0.2 kg loading and 12 s dwell time (HV 0.2 according to DIN EN ISO 6507-1). For each material and time, fifteen indentations were analyzed (n = 15), where the distance between the center of two indentations was at least five times the indentation diagonal length. Diagonals were measured using a confocal laser scanning microscope (see “surface roughness”) and averaged. Vickers hardness was calculated according to DIN EN ISO 6507-1 using the formula [47]:
F = testing force in N; d = average diagonal length of indentation in mm.
2.2.3 Surface roughness
Confocal laser scanning microscopy (VK-X1000/X1050, KEYENCE, Osaka, Japan) with a ×50 magnification (CF IC EPI Plan 50x; NA = 0.8; WD = 0.54 mm), a red laser (λ = 661 nm), and a resolution of 1024 × 768 pixels was used for surface analysis. Measurements of surface and indentation diagonals were performed by “VK Viewer 1.1.2.174” software (Keyence Cooperation, Osaka, Japan). The surface data was subjected to a S-Filter of 0.8 µm and a L-Filter of 0.1 mm (filter-type: double Gaussian) and analyzed for arithmetical mean height (Sa) according to DIN EN ISO 25178-2 using the software “MultiFileAnalyzer” 2.1.3.89 (Keyence Cooperation, Osaka, Japan) [48].
2.2.4 Surface free energy
The surface free energy of all materials was measured using highly polished surfaces (Sa <0.02 µm). Contact angle measurements were performed by a DSA25S (Krüss, Hamburg, Germany) using purified water and diiodomethane. Eight measurements were performed for each test liquid, each with a drop volume of 0.2 µl and a time interval of 30 s between application and measurement at 23 °C under air atmosphere [49]. The application was software-controlled using the manufacturer’s own DO3252 “Liquid Needle” dosing unit. Analyses were performed with the software “ADVANCE 1.11” (Krüss, Hamburg, Germany) by averaging the contact angles on both sides (fitting method: ellipse) and surface free energy (total, dispersive and polar parts) was calculated according to Owens and Wendt [50].
2.2.5 Statistics
All data were analyzed for normal distribution according to Shapiro-Wilk. Differences in Vickers hardness and surface free energy between the materials and their manufacturer-specific translucency variants as well as the differences in Sa parameters were firstly checked for homogeneity of variances using the Levene test. In case of equality of variances, a one-way analysis of variance (ANOVA) and Bonferroni post-hoc tests were performed. Assuming inhomogeneous variances, statistical analysis was performed by Welch ANOVA followed by Dunnett-T3 post-hoc multiple comparisons. A possible correlation between Vickers hardness or surface free energy and the filler content of the CAD/CAM resin composites was investigated using a test for Pearson correlation and a quadratic regression with previously published data from our research group regarding the study of filler content of CAD/CAM resin composites [6]. Differences in mean values between the initial values for Vickers hardness depending on the storage medium and storage time were examined using a t test. A two-way ANOVA with Bonferroni post-hoc tests were used for statistical analysis of the influence of medium and time factors. Significance level was set to α = 0.05.
3 Results
After 24 h of dry storage, GB showed the highest (p < 0.001) Vickers hardness values with 148.8 (2.9)–152.2 (4.2) HV, followed by LU with 114.3 (2.6)–114.8 (3.4) HV, and LC with 102.4 (5.2) HV. The Vickers hardness of all other specimens (BC, GC, SB, TC) ranged between 79.0 (1.9) HV and 88.8 (2.1) HV (Table 2). No significant differences were identified between BC-LT and TC, BC-HT and GC, BC and SB as well as SB and TC (Fig. 1). With the exception of BC, no significant differences in Vickers hardness could be detected between the respective translucency variants within the samples of a single manufacturer (see Supplementary information, Table S3).
Storage in demineralized water, cola, and ethanol resulted in a strongly significant reduction (p < 0.001) of Vickers hardness for all samples except GB (Table 2). In contrast to all other specimens, the greatest decrease in Vickers hardness for GB was produced by storage in water. After exposure to ethanol, no changes in Vickers hardness for GB-HT (p = 0.398) and minor changes for GB-LT (p = 0.042) were measured.
Two-way ANOVA indicated that for BC, GC, SB, TC, and LC ethanol immersion caused the most prominent decline in Vickers hardness, which was significantly higher than for both demineralized water and cola (p < 0.001, respectively). For LU and GC, the duration of storage was also a significant factor for the observed decline in Vickers hardness (see supplementary information, Table S2).
Surface free energy of the specimens ranged between 50.2 (6.4) and 58.0 (0.6) mN/m. While the dispersive parts were between 28.3 (3.5) and 37.0 (1.8) mN/m, the polar parts were spread wider and ranged between 13.8 (1.1) and 24.2 (6.4) mN/m (Fig. 2). No differences could be identified between the translucency variants within materials from the same manufacturer (supplementary information, Table S1). The lowest polar fractions were identified for LU.
Surface free energy (with standard deviations) and its polar/dispersive parts (according to the Owens/Wendt approach [50])
A test for Pearson correlations showed a significant correlation between the filler content of the CAD/CAM resin composites and the observed Vickers hardness, but not for the surface free energy (Table 3). An additional quadratic regression resulted in a coefficient of determination of R² = 0.889. Based on the surface free energy results, it is qualitatively hypothesized, taking into account the study design, that no other correlation is present (see supplementary information, Fig. S1).
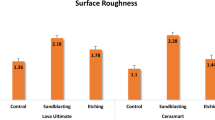
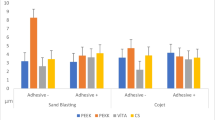
Regarding surface texture analysis, storage in the aging media caused a significant change in arithmetical mean height in almost all materials (Fig. 3). Highest values were observed after water storage for BC-LT and LU-HT with a change of ΔSa = 0.015 (0.003) µm, and ΔSa = 0.010 (0.002) µm, respectively. All other changes were smaller than ΔSa = 0.005 µm.
4 Discussion
The results of the current study are discussed in dependence on the four (a–d) null hypotheses.
H0 (a) There is no difference between the CAD/CAM resin composites with different translucencies in terms of Vickers hardness and surface energy.
This null hypothesis must be partially rejected. Initially, the various CAD/CAM resin composites showed partial differences in terms of Vickers hardness and three different ranges could be distinguished: (1) GB with 150 (5) HV, (2) LU with 115 (4) HV and (3) BC, GC, SB, TC as well as LC within a range of 79 (2) – 102 (6) HV. However, with the exception of BC, Vickers hardness did not differ between the translucency variants HT/LT (or MT) in materials from the same manufacturer. For BC, differences in HT and LT should be further investigated with an expanded sample number to assess whether a type I error can be excluded.
H0 (b) There is no correlation between Vickers hardness or surface free energy and filler content of CAD/CAM resin composites.
The null hypothesis was partially rejected, since a correlation with the filler content of the CAD/CAM resin composites could be demonstrated for Vickers hardness, but not for surface free energy. As already described by Alshabib et al. (2019), due to the high filler content of current CAD/CAM resin composites, pronounced changes in the mechanical properties can be expected when the filler content is varied [22].
H0 (c) There is no loss in Vickers hardness after aging in different storage media for the different CAD/CAM resin composites.
This null hypothesis could be rejected for all materials except GB. The changes in Vickers hardness of the CAD/CAM resin composites examined in this study were 10–20% reduction for LU and up to 35% reduction for BC, GC, SB, TC, and LC except for GB. This contrasts with the small reduction in Vickers hardness of up to 3% observed in Colombo et al. (2019) for zirconia-reinforced glass ceramic when placed in cola for 28 days. According to the p values, it can be assumed that exposure to demineralized water has a greater influence on the Vickers hardness of GB than cola or ethanol. To exclude a type I error, further studies with a larger number of samples are recommended here.
Changes in the mechanical properties of direct composites as induced by aging have been explained by chemical and physical degradation due to diffusion-related solvent sorption. These processes cause a softening of the resin matrix and reduction of polymeric chain interactions, which produces tensile stress that affects the matrix/filler interface [51] and leads to the formation of a porous subsurface layer [52]. Furthermore, hydrolysis affects the polymer network-structure by producing oligomers and monomers [23, 24]. In addition, it results in hydrolysis of the Si-O-Si bonds between filler particles and silanes, which finally weakens the filler-matrix-interface. Ferracane and Berge [29] reported that these aging effects are caused by the organic matrix and that degradation of the filler fraction plays a minor role [29]. Accordingly, degradation processes should be minimized in materials with high filler fractions [9], which supports little changes observed for GB in the current study. Moreover, the data of the current study underline that aging with cola has no additional effect than demineralized water. This observation might indicate that there is no other relevant effect producing additional stress that results from the exposure to acid (i.e. carbonic and phosphoric acid). Aging processes were highly relevant for ethanol as aging medium; this phenomenon could be attributed to the higher solubility of the organic matrix in ethanol and a simplified penetration by ethanol as a more organophilic molecule in contrast to water-based liquids. Consequences include potential degradation of the matrix and a weakening of the bonds between matrix and filler particles due to hydrolysis of the Si-O-Si bonds [22, 23].
H0 (d) There is no difference in surface roughness after aging in different storage media for the different CAD/CAM resin composites.
This null hypothesis must be rejected since for almost all CAD/CAM resin composites, changes in surface texture occurred after immersion in the various media. However, since changes in the mean value of Sa were in the range of the third decimal place, potential measurement errors must also be taken into consideration and the results have to be interpreted with caution. Nevertheless, it is evident that the observed maximum changes are in a scale of ΔSa = 0.015 µm and thus below the threshold value of an Ra or Sa value of 0.2 µm [40, 41], supporting the results of Schmohl et al. (2022) regarding the acid resistance of CAD/CAM resin composites [53]. Therefore, it is assumed that no clinical relevance can be derived regarding an impact on biofilm formation. Furthermore, it should be noted that other surface characteristics that might be the result of the fabrication and curing process may have a higher influence on biofilm formation than surface roughness and surface free energy [4, 54].
4.1 Limitations
Only changes in Vickers hardness due to storage in different media were considered in the current study. For a comprehensive evaluation of the mechanical properties, additional analyses of e.g. flexural strength and elastic modulus are recommended. No investigations were carried out on a common dental ceramic. In order to allow comparisons, further studies should consider this material as a reference in their study design. In addition, analyses of other in vitro or clinically relevant media (ethanol in lower concentration, chlorhexidine, saliva, etc.) and an investigation of an effect of the temperature could help to get a more detailed view. A potential leaching of the filler particles should be investigated, as has already been reported for direct composites after six months of storage [55]. In addition, further correlations with previous studies on filler content, distribution, and chemical composition should be considered.
5 Conclusion
H0(a): Commercially available CAD/CAM resin composites differ partially in Vickers hardness (79.0 (1.9)–152.2 (4.2) HV) and surface free energy (total: 50.2 (6.4)–56.2 (3.2) mN/m; dispersive: 28.3 (3.5)–37.0 (1.8) mN/m; polar: 13.8 (1.1)–24.2 (6.4) mN/m) regardless of their respective translucency variants, except for BC.
H0(b): For the correlation between Vickers hardness and filler content, both a Pearson and a quadratic correlation could be identified, whereas no correlation to surface free energy could be drawn.
H0(c): The Vickers hardness of the investigated materials were reduced by immersion in different media and can be divided into the following groups:
-
(1)
Highest Vickers hardness values of 150 (5) HV as well as no or only slight changes after immersion in various media were identified for Grandio Blocs (GB).
-
(2)
Lava Ultimate (LU) showed the second highest Vickers hardness, which was 115 (4) HV, decreasing 10–20% after storage in different media.
-
(3)
Brilliant Crios (BC), Cerasmart (GC), Shofu Block HC (SB), Tetric CAD (TC), and Luxacam Composite (LC) initially featured Vickers hardness values between 79 (2) and 102 (6) HV. Artificial aging produced a decline of up to −35% in Vickers hardness.
H0(d):Artificial aging produced only little changes in surface roughness (max. ΔSa = 0.015 (0.003) µm), a clinical relevance is to be doubted.
References
Mainjot AK, Dupont NM, Oudkerk JC, Dewael TY, Sadoun MJ. From artisanal to CAD-CAM blocks: state of the art of indirect composites. J Dent Res. 2016;95:487–95. https://doi.org/10.1177/0022034516634286
Lambert H, Durand J-C, Jacquot B, Fages M. Dental biomaterials for chairside CAD/CAM: State of the art. J Adv Prosthodont. 2017;9:486–95. https://doi.org/10.4047/jap.2017.9.6.486
Nguyen J-F, Migonney V, Ruse ND, Sadoun M. Resin composite blocks via high-pressure high-temperature polymerization. Dent Mater. 2012;28:529–34. https://doi.org/10.1016/j.dental.2011.12.003
Ionescu AC, Hahnel S, König A, Brambilla E. Resin composite blocks for dental CAD/CAM applications reduce biofilm formation in vitro. Dent Mater. 2020;36:603–16. https://doi.org/10.1016/j.dental.2020.03.016
Azeem RA, Sureshbabu NM. Clinical performance of direct versus indirect composite restorations in posterior teeth: A systematic review. J Conserv Dent. 2018;21:2–9. https://doi.org/10.4103/JCD.JCD_213_16
Koenig A, Schmidtke J, Schmohl L, Schneider-Feyrer S, Rosentritt M, Hoelzig H, et al. Characterisation of the Filler Fraction in CAD/CAM resin-based composites. Materials (Basel). 2021. https://doi.org/10.3390/ma14081986
Ferracane JL. Resin composite—state of the art. Dent Mater. 2011;27:29–38. https://doi.org/10.1016/j.dental.2010.10.020
Lawson NC, Bansal R, Burgess JO. Wear, strength, modulus and hardness of CAD/CAM restorative materials. Dent Mater. 2016;32:e275–83. https://doi.org/10.1016/j.dental.2016.08.222
Hampe R, Lümkemann N, Sener B, Stawarczyk B. The effect of artificial aging on Martens hardness and indentation modulus of different dental CAD/CAM restorative materials. J Mech Behav Biomed Mater. 2018;86:191–8. https://doi.org/10.1016/j.jmbbm.2018.06.028
Alamoush RA, Silikas N, Salim NA, Al-Nasrawi S, Satterthwaite JD. Effect of the composition of CAD/CAM composite blocks on mechanical properties. Biomed Res Int. 2018;2018:4893143 https://doi.org/10.1155/2018/4893143
Stawarczyk B, Özcan M, Trottmann A, Schmutz F, Roos M, Hämmerle C. Two-body wear rate of CAD/CAM resin blocks and their enamel antagonists. J Prosthet Dent. 2013;109:325–32. https://doi.org/10.1016/S0022-3913(13)60309-1
Lauvahutanon S, Takahashi H, Oki M, Arksornnukit M, Kanehira M, Finger WJ. In vitro evaluation of the wear resistance of composite resin blocks for CAD/CAM. Dent Mater J. 2015;34:495–502. https://doi.org/10.4012/dmj.2014-293
Hensel F, Koenig A, Doerfler H-M, Fuchs F, Rosentritt M, Hahnel S. CAD/CAM resin-based composites for use in long-term temporary fixed dental prostheses. Polym (Basel). 2021. https://doi.org/10.3390/polym13203469
Okada R, Asakura M, Ando A, Kumano H, Ban S, Kawai T, et al. Fracture strength testing of crowns made of CAD/CAM composite resins. J Prosthodont Res. 2018;62:287–92. https://doi.org/10.1016/j.jpor.2017.10.003
Miura S, Fujisawa M. Current status and perspective of CAD/CAM-produced resin composite crowns: a review of clinical effectiveness. Jpn Dent Sci Rev. 2020;56:184–9. https://doi.org/10.1016/j.jdsr.2020.10.002
Souza J, Fuentes MV, Baena E, Ceballos L. One-year clinical performance of lithium disilicate versus resin composite CAD/CAM onlays. Odontology. 2021;109:259–70. https://doi.org/10.1007/s10266-020-00539-3
Zimmermann M, Koller C, Reymus M, Mehl A, Hickel R. Clinical Evaluation of Indirect Particle-Filled Composite Resin CAD/CAM Partial Crowns after 24 Months. J Prosthodont. 2018;27:694–9. https://doi.org/10.1111/jopr.12582
Miura S, Kasahara S, Yamauchi S, Katsuda Y, Harada A, Aida J, et al. A possible risk of CAD/CAM-produced composite resin premolar crowns on a removable partial denture abutment tooth: a 3-year retrospective cohort study. J Prosthodont Res. 2019;63:78–84. https://doi.org/10.1016/j.jpor.2018.08.005
Larsen IB, Freund M, Munksgaard EC. Change in surface hardness of BisGMA/TEGDMA polymer due to enzymatic action. J Dent Res. 1992;71:1851–3. https://doi.org/10.1177/00220345920710111701
Gale MS, Darvell BW. Thermal cycling procedures for laboratory testing of dental restorations. J Dent. 1999;27:89–99. https://doi.org/10.1016/S0300-5712(98)00037-2
Sarrett DC. Clinical challenges and the relevance of materials testing for posterior composite restorations. Dent Mater. 2005;21:9–20. https://doi.org/10.1016/j.dental.2004.10.001
Alshabib A, Silikas N, Watts DC. Hardness and fracture toughness of resin-composite materials with and without fibers. Dent Mater. 2019;35:1194–203. https://doi.org/10.1016/j.dental.2019.05.017
Sunbul HA, Silikas N, Watts DC. Surface and bulk properties of dental resin- composites after solvent storage. Dent Mater. 2016;32:987–97. https://doi.org/10.1016/j.dental.2016.05.007
Hahnel S, Henrich A, Bürgers R, Handel G, Rosentritt M. Investigation of mechanical properties of modern dental composites after artificial aging for one year. Oper Dent. 2010;35:412–9. https://doi.org/10.2341/09-337-L
Pilliar RM, Vowles R, Williams DF. The effect of environmental aging on the fracture toughness of dental composites. J Dent Res. 1987;66:722–6. https://doi.org/10.1177/00220345870660030301
Al Badr RM, Abu Hassan H. Effect of immersion in different media on the mechanical properties of dental composite resins. Int J Appl Dent Sci. 2017;3:81–8
Heintze SD, Ilie N, Hickel R, Reis A, Loguercio A, Rousson V. Laboratory mechanical parameters of composite resins and their relation to fractures and wear in clinical trials-A systematic review. Dent Mater. 2017;33:e101–14. https://doi.org/10.1016/j.dental.2016.11.013
Söderholm KJ. Degradation of glass filler in experimental composites. J Dent Res. 1981;60:1867–75. https://doi.org/10.1177/00220345810600110701
Ferracane JL, Berge HX. Fracture toughness of experimental dental composites aged in ethanol. J Dent Res. 1995;74:1418–23. https://doi.org/10.1177/00220345950740071501
Attia A, Abdelaziz KM, Freitag S, Kern M. Fracture load of composite resin and feldspathic all-ceramic CAD/CAM crowns. J Prosthet Dent. 2006;95:117–23. https://doi.org/10.1016/j.prosdent.2005.11.014
Lucsanszky IJR, Ruse ND. Fracture toughness, flexural strength, and flexural modulus of new CAD/CAM resin composite blocks. J Prosthodont. 2020. https://doi.org/10.1111/jopr.13123
Colombo M, Poggio C, Lasagna A, Chiesa M, Scribante A. Vickers micro-hardness of new restorative CAD/CAM dental materials: evaluation and comparison after exposure to acidic drink. Materials. 2019. https://doi.org/10.3390/ma12081246
Ilie N. Altering of optical and mechanical properties in high-translucent CAD-CAM resin composites during aging. J Dent. 2019;85:64–72. https://doi.org/10.1016/j.jdent.2019.05.015
Selwitz RH, Ismail AI, Pitts NB. Dental caries. Lancet. 2007;369:51–9. https://doi.org/10.1016/S0140-6736(07)60031-2
Ramseier CA, Anerud A, Dulac M, Lulic M, Cullinan MP, Seymour GJ, et al. Natural history of periodontitis: Disease progression and tooth loss over 40 years. J Clin Periodontol. 2017;44:1182–91. https://doi.org/10.1111/jcpe.12782
Müller F. Oral hygiene reduces the mortality from aspiration pneumonia in frail elders. J Dent Res. 2015;94:14S–16S. https://doi.org/10.1177/0022034514552494
Pasmore M, Todd P, Pfiefer B, Rhodes M, Bowman CN. Effect of polymer surface properties on the reversibility of attachment of pseudomonas aeruginosa in the early stages of biofilm development. Biofouling. 2002;18:65–71. https://doi.org/10.1080/08927010290017743
von Fraunhofer JA, Loewy ZG. Factors involved in microbial colonization of oral prostheses. Gen Dent. 2009;57:136–43. quiz 144-5
Anselme K, Davidson P, Popa AM, Giazzon M, Liley M, Ploux L. The interaction of cells and bacteria with surfaces structured at the nanometre scale. Acta Biomater. 2010;6:3824–46. https://doi.org/10.1016/j.actbio.2010.04.001
Teughels W, van Assche N, Sliepen I, Quirynen M. Effect of material characteristics and/or surface topography on biofilm development. Clin Oral Implants Res. 2006;17:68–81. https://doi.org/10.1111/j.1600-0501.2006.01353.x
Bollen CML, Lambrechts P, Quirynen M. Comparison of surface roughness of oral hard materials to the threshold surface roughness for bacterial plaque retention: a review of the literature. Dent Mater. 1997;13:258–69. https://doi.org/10.1016/S0109-5641(97)80038-3
Dezelic T, Guggenheim B, Schmidlin PR. Multi-species biofilm formation on dental materials and an adhesive patch. Oral Health Prev Dent. 2009;7:47–53
Ikeda M, Matin K, Nikaido T, Foxton RM, Tagami J. Effect of surface characteristics on adherence of S. mutans biofilms to indirect resin composites. Dent Mater J. 2007;26:915–23. https://doi.org/10.4012/dmj.26.915
Contreras-Guerrero P, Ortiz-Magdaleno M, Urcuyo-Alvarado MS, Cepeda-Bravo JA, Leyva-Del Rio D, Pérez-López JE, et al. Effect of dental restorative materials surface roughness on the in vitro biofilm formation of Streptococcus mutans biofilm. Am J Dent. 2020;33:59–63.
Alamoush RA, Sung R, Satterthwaite JD, Silikas N. The effect of different storage media on the monomer elution and hardness of CAD/CAM composite blocks. Dent Mater. 2021;37:1202–13. https://doi.org/10.1016/j.dental.2021.04.009
ISO 6872:2015 + Amd.1:2018. Dentistry - Ceramic materials. Berlin: Beuth Verlag GmbH. https://doi.org/10.31030/2860803
ISO 6507-1:2018-01. Metallic materials - Vickers hardness test - Part 1: Test method. Berlin: Beuth Verlag GmbH. https://doi.org/10.31030/2778746
ISO 25178-2:2012. Geometrical product specifications (GPS) - Surface texture: Areal - Part 2: Terms, definitions and surface texture parameters. Berlin: Beuth Verlag GmbH. https://doi.org/10.31030/1754208
Huhtamäki T, Tian X, Korhonen JT, Ras RHA. Surface-wetting characterization using contact-angle measurements. Nat Protoc. 2018;13:1521–38. https://doi.org/10.1038/s41596-018-0003-z
Owens DK, Wendt RC. Estimation of the surface free energy of polymers. J Appl Polym Sci. 1969;13:1741–7. https://doi.org/10.1002/app.1969.070130815
Drummond JL. Degradation, fatigue, and failure of resin dental composite materials. J Dent Res. 2008;87:710–9. https://doi.org/10.1177/154405910808700802
Wu W, Toth EE, Moffa JF, Ellison JA. Subsurface damage layer of in vivo worn dental composite restorations. J Dent Res. 1984;63:675–80. https://doi.org/10.1177/00220345840630051401
Schmohl L, Roesner AJ, Fuchs F, Wagner M, Schmidt MB, Hahnel S, et al. Acid Resistance of CAD/CAM Resin Composites. Biomedicines. 2022. https://doi.org/10.3390/biomedicines10061383
Cazzaniga G, Ottobelli M, Ionescu AC, Paolone G, Gherlone E, Ferracane JL, et al. In vitro biofilm formation on resin-based composites after different finishing and polishing procedures. J Dent. 2017;67:43–52. https://doi.org/10.1016/j.jdent.2017.07.012
Drummond JL, Carlo F, de, Super BJ. Three-dimensional tomography of composite fracture surfaces. J Biomed Mater Res B Appl Biomater. 2005;74:669–75. https://doi.org/10.1002/jbm.b.30298
Funding
Open Access funding enabled and organized by Projekt DEAL.
Author information
Authors and Affiliations
Contributions
Conceptualization: JS, AK, FF; Methodology: FF, JS; Formal analysis and investigation: FF, JS; Writing—original draft preparation: FF, JS; Writing—review and editing: SH; AK, FF, JS; Vizualisation: FF; Resources: SH; Supervision: SH; AK, Administration: SH; AK, FF, JS. All authors contributed to the study conception as well as the design and read, edited and approved the final manuscript.
Corresponding author
Ethics declarations
Conflict of interest
The authors declare no competing interests.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
These authors contributed equally: Florian Fuchs, Julius Schmidtke
Supplementary information
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons license, and indicate if changes were made. The images or other third party material in this article are included in the article’s Creative Commons license, unless indicated otherwise in a credit line to the material. If material is not included in the article’s Creative Commons license and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this license, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
Fuchs, F., Schmidtke, J., Hahnel, S. et al. The influence of different storage media on Vickers hardness and surface roughness of CAD/CAM resin composites. J Mater Sci: Mater Med 34, 13 (2023). https://doi.org/10.1007/s10856-023-06713-7
Received:
Accepted:
Published:
DOI: https://doi.org/10.1007/s10856-023-06713-7