Abstract
Background
Cerebral ischemic injury leads to over-activation of microglia, which release pro-inflammatory factors that deteriorate neurological function during the acute phase of stroke. Thus, inhibiting microglial over-activation is crucial for reducing ischemic injury. Sirtuin 1 (Sirt1) has been shown to play a critical role in stroke, neurodegenerative diseases and aging. However, the effect of Sirt1 on the regulation of microglial activation following cerebral ischemic injury, as well as the underlying mechanism, remain unknown. Therefore, the purpose of the present study is to mainly investigate the effect of Sirt1 on oxygen-glucose deprivation/reoxygenation (OGD/R)-treated N9 microglia following treatment with the Sirt1 agonists resveratrol and SRT1720 and the Sirt1 antagonist sirtinol.
Methods
Cell viability, Apoptosis, activation and inflammatory responses of microglia, expressions and activity of Shh signaling pathway proteins were detected by Cell Counting Kit 8, Flow Cytometry, immunocytochemistry, ELISA, and Western blotting, respectively.
Results
The results demonstrated that treatment with resveratrol or SRT1720 could inhibit the activation of microglia and inflammation during OGD/R. Moreover, these treatments also led to the translocation of the GLI family zinc finger-1 (Gli-1) protein from the cytoplasm to the nucleus and upregulated the expression of Sonic hedgehog (Shh), Patched homolog-1 (Ptc-1), smoothened frizzled class receptor and Gli-1. By contrast, the inhibition of Sirt1 using sirtinol had the opposite effect.
Conclusion
These findings suggested that Sirt1 may regulate microglial activation and inflammation by targeting the Shh/Gli-1 signaling pathway following OGD/R injury.
Graphical abstract

Schematic representation of Sirt1 regulating the microglial activation and inflammation following oxygen-glucose deprivation/reoxygenation injury via mediation of Shh/Gli-1 signaling pathway.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Microglia are immune cells residing in the brain and spinal cord that can modulate local inflammatory and immune responses [1, 2]. Ischemic injury can activate microglia, which act as a double-edged sword with respect to stroke [3]. On the one hand, microglial activation promotes the release of pro-inflammatory cytokines, such as IFN-γ, IL-6, TNF-α and IL-1β, and aggravates ischemic injury. On the other hand, it also causes the release of anti-inflammatory cytokines, such as IL-10, and improves neurological function [1,2,3,4]. Therefore, regulating microglial activation is important in order to reduce injury and promote functional recovery after stroke.
Silent information regulator factor 2-related enzyme 1 (sirtuin 1/Sirt1), a nicotinamide adenine dinucleotide-dependent protein deacetylase, can modulate a wide range of biological processes, including oxidative stress, inflammation, aging, apoptosis and autophagy [5]. Previous studies have demonstrated that Sirt1 can exert protective effects against cerebral ischemia, Alzheimer’s disease, traumatic brain injury and Parkinson’s disease [6,7,8,9,10]. In addition, Sirt1 can regulate the activation of microglia [11,12,13]. However, the molecular mechanism underlying the effect of Sirt1 on the regulation of microglial activation has not been fully elucidated.
The Sonic hedgehog (Shh) signaling pathway has a key role in stem cell behavior, organ differentiation, embryonic development, axonal growth and regulation in the developing as well as the adult brain [14,15,16]. Following ischemic injury, neurodegeneration, infection or trauma in the brain or spinal cord, Shh signaling is activated and can improve neurological function by regulating inflammation, oxidative stress and apoptosis [15, 17,18,19,20,21,22]. For example, the BCL6/BCOR/SIRT1 complex has been reported to promote neurogenesis and suppress medulloblastoma formation by inhibiting Shh signaling [23]. Moreover, Sirt1 can regulate the viability of NIH3T3 cells and neurons following OGD/R injury in vitro via Shh signaling [13, 24]. However, whether Sirt1 can regulate microglial activation after stroke and whether this would involve the Shh signaling pathway remains not quite clear.
Therefore, in the present study, cultured microglia were exposed to OGD/R to mimic ischemia/reperfusion injury in vitro and were used to determine whether Sirt1 could regulate microglial activation and inflammation following OGD/R injury in vitro and whether these effects were mediated via Shh/GLI family zinc finger-1 (Gli-1) signaling. The effects of Sirt1 agonists and antagonists on microglial viability, activation and inflammation, as well as the nuclear translocation of Gli-1 and the expression of Shh signaling pathway components following OGD/R injury were also examined.
Materials and methods
Culture of N9 microglia
N9 microglia (kindly provided by the Department of Anesthesia, The Affiliated Children’s Hospital of Chongqing Medical University, Chongqing, China) were cultured in DMEM/F-12 (HyClone; Cytiva) supplemented with 10% FBS (PAN-Biotech), 100 U/ml streptomycin and 100 U/ml penicillin at 37 °C in a humidified atmosphere with 5% CO2. The cells were digested with 0.125% trypsin and subcultured at a 1:3 ratio when they reached 80% confluence.
OGD/R model
The OGD/R model was established in N9 microglia according to previously described methods [13].For oxygen-glucose deprivation, microglia were maintained in D-Hanks solution with a humidified anaerobic incubator (Thermo 3111; Thermo Fisher Scientific, Inc.) containing 94% N2, 1% O2 and 5% CO2 at 37 °C for 150 min. For reoxygenation, microglia were incubated in a humidified normoxic environment with complete medium for 24 h.
Drug treatment
To determine whether Sirt1 was associated with Shh signaling, microglia were divided into five groups as follows: (i) Normal (Nor) group, microglia (~ 100,000 cells/ml) cultured in complete medium without OGD/R; (ii) control (Ctrl) group, microglia (~ 100,000 cells/ml) cultured in complete medium containing 0.4% DMSO for 24 h, then subjected to OGD/R as aforementioned; (iii) resveratrol (Res) group, microglia (~ 100,000 cells/ml) cultured in complete medium containing the Sirt1 agonist resveratrol (20 µmol/l; 99% purity; MilliporeSigma) for 24 h, then subjected to OGD/R as aforementioned; (iv) SRT1720 (SRT) group, microglia (~ 100,000 cells/ml) cultured in complete medium containing the Sirt1 agonist SRT1720 hydrochloride (0.5 µmol/l; 99.92% purity; MedChemExpress) for 24 h, then subjected to OGD/R as aforementioned; and (v) sirtinol group, microglia (~ 100,000 cells/ml) cultured in complete medium containing the Sirt1 antagonist sirtinol (10 µmol/l; 98% purity; MedChemExpress) for 24 h, then subjected to OGD/R as aforementioned. All drugs were dissolved in DMSO (cat. no. D2650; MilliporeSigma) respectively and then diluted to the corresponding concentration with culture medium.
Cell counting Kit-8 (CCK-8) assay
Microglial viability was estimated using a CCK-8 assay (Dojindo Laboratories, Inc.). Briefly, N9 microglia were seeded in poly-L-lysine-coated 96-well plates (~ 5,000 cells/well) and received the aforementioned treatments. The cells were incubated for 4 h at 37 °C, and the CCK-8 solution was then added to each well (10 µl in 100 µl culture). Absorbance was measured at 450 nm using a microplate reader (Thermo Labsystems).
Flow cytometry
The N9 microglia were collected after treatment with each drug following OGD/R injury, washed three times in ice-cold PBS and resuspended in PBS at a concentration of 1 × 106 cells/ml; subsequently, 5 µl Annexin V fluorescein isothiocyanate and propidium iodide were added, followed by culture at room temperature in the dark for 15 min; next detected the apoptotic cells by flow cytometry (FACSCalibur™; BD Biosciences). Then the data were analyzed with CytExpert 2.0 software (Beckman Coulter) which the percentage of early apoptosis and late apoptosis were showed in the upper right quadrant and the lower right quadrant respectively. Finally, the percentage of apoptosis of microglia can be quantified as the sum of the percentage of early apoptosis and late apoptosis.
ELISA
The levels of the inflammatory cytokine TNF-α, IL-1β and IL-10 in cell supernatants were measured using ELISA kits (cat. nos. EMC102a, EMC001b and EMC005, respectively; Neobioscience Technology Co., Ltd.) according to the manufacturer’s instructions.
Immunocytochemistry
Microglia from each group were seeded on poly-L-lysine-coated coverslips (500 cells/coverslip), fixed with 4% formaldehyde solution at room temperature for 30 min, incubated with 1% Triton X-100 at 37 °C for 30 min, subsequently blocked with 5% goat or donkey serum (cat. no. SAP-9100; Beijing Zhongshan Golden Bridge; cat. no. D9663; MilliporeSigma) at 37 °C for 1 h. The cells were then incubated overnight at 4 °C with anti-ionized calcium-binding adaptor molecule 1 (Iba1; monoclonal; rabbit; 1:100 dilution; cat. no. ab178847; Abcam) or anti- Gli-1 (polyclonal; rabbit; 1:100; cat. no. ab273018; Abcam) antibody. While there were no primary antibodies in the negative controls. The cells were incubated with Cy3-conjugated goat anti-rabbit IgG (1:200; cat. no. SA00009-2; ProteinTech Group, Inc.) at 37 °C for 1 h the next day. The nuclei were counterstained with DAPI (cat. no. C1005; Beyotime Institute of Biotechnology) in the dark at 25 °C for 5 min. All images were captured using an A1 + R laser confocal microscope (Nikon Corporation).
Western blotting
Microglia were homogenized in RIPA lysis buffer (cat. no. P0013C; Beyotime Institute of Biotechnology) containing 1% phenylmethane sulfonyl fluoride (cat. no. ST506; Beyotime Institute of Biotechnology) and incubated on ice for 30 min. The protein concentration of each extract was measured using a BCA Protein Assay Reagent Kit (cat. no. P0010; Beyotime Institute of Biotechnology) following centrifugation (13,684 x g at 4 °C) for 10 min. A total of 40 µg protein per lane was loaded and separated via 10% SDS-PAGE, then transferred onto PVDF membranes (cat. no. 03010040001; MilliporeSigma). The membranes were blocked with 5% skimmed milk at room temperature for 2 h, then incubated overnight at 4 °C with the following primary antibodies: Monoclonal rabbit anti-Iba1 antibody (1:1000 dilution; cat. no. ab178847; Abcam); polyclonal rabbit antibodies against Shh, Patched homolog-1 (Ptc-1), smoothened frizzled class receptor (Smo), Gli-1, caspase-3, Bax (1:1000; cat. nos. ab19897, ab53715, ab235183, ab273018, ab13847, ab263897; all from Abcam), IL-10, TNF-α and IL-1β (1:1,000; cat. nos. bs-0698R, bs-0078R and bs-0812R; all from BIOSS); and monoclonal rabbit anti-GAPDH (loading control; 1:1000; cat. no. AF1186; Beyotime Institute of Biotechnology). The membranes were incubated with horseradish peroxidase-conjugated AffiniPure goat anti-rabbit antibody (1:2000; cat. no. ZB-2301; Beijing Zhongshan Golden Bridge) at 37 °C for 1 h the next day. Finally, the protein bands were visualized using enhanced chemiluminescence reagent (cat. no. P0018FS; Beyotime Institute of Biotechnology), and their intensities were analyzed using Quantity One v. 4.6.6 software (Bio-Rad Laboratories, Inc.).
Statistical analysis
The data are expressed as the mean ± standard deviation. Statistical analysis was carried out using one-way ANOVA analysis of variance followed by Tukey’s post-hoc test with SPSS 22.0 (IBM Corp.). P < 0.05 was considered as a statistically significant difference.
Results
Effects of Sirt1 on the viability and apoptosis of microglia following OGD/R injury in vitro
Firstly, we consulted the relevant literature to determine the dosages of these drugs [13, 24,25,26,27,28]. Then our team has studied dosages of resveratrol and SRT1720 following OGD/R injury in the pre experiment stage by CCK-8 assays and the results showed that the optimal drug concentrations of resveratrol and SRT1720 were 20 µmol/l and 0.5 µmol/l respectively (P < 0.05, Fig. S1A,B). However, in the previous articles published by our team [13, 24], it has been studied that the drug concentration of sirtinol following OGD/R injury was 10 µmol/l, so the present study is directly discussed on the previous research.
The effects of Sirt1 on microglial viability were examined using CCK-8 assays following OGD/R injury. Compared with the Nor group, the viability of microglia in the Ctrl, Res, SRT and sirtinol groups was significantly decreased (P < 0.05, Fig. 1 A). Res and SRT treatments had similar effects on the viability of microglia relative to the Ctrl group (Fig. 1 A). However, viability was significantly decreased in the sirtinol group compared with the Res and SRT groups (P < 0.05, Fig. 1 A).
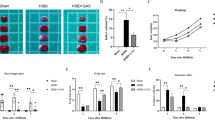
Effects of Sirt1 on the viability and apoptosis of microglia following OGD/R injury in vitro
A Effect of Sirt1 on the viability of microglia following OGD/R injury. Compared with the Ctrl group, Res and SRT treatment significantly increased while sirtinol significantly reduced the viability of microglia. B Effect of Sirt1 on the apoptosis of microglia following OGD/R injury, as determined using flow cytometry. C Effect of Sirt1 on the expression of apoptosis proteins in microglia following OGD/R injury, as determined using western blotting. *P < 0.05 vs. Nor; #P < 0.05 vs. Ctrl; ▲P < 0.05 vs. Res; $P < 0.05 vs. SRT; ANOVA. n = 3
Microglial apoptosis, as well as the protein expression levels of caspase-3 and Bax, were examined using flow cytometry and western blot analysis, respectively. The percentage of apoptotic microglia and the protein expression levels of caspase-3 and Bax were significantly increased in the Ctrl, Res, SRT and sirtinol groups compared with the Nor group (P < 0.05). However, these were significantly decreased in the Res and SRT groups compared with the Ctrl group (P < 0.05, Fig. 1B and C), and significantly increased in the sirtinol group compared with the Res and SRT groups following OGD/R injury (P < 0.05, Fig. 1B and C). These results demonstrated that Sirt1 could regulate the viability and apoptosis of microglia following OGD/R injury in vitro.
Effects of Sirt1 on activation of microglia and inflammation following OGD/R injury in vitro
Morphological changes and upregulation of Iba1 protein expression levels are characteristic of microglial activation [4]. Therefore, morphological changes and Iba1 protein expression levels were examined using immunofluorescence and western blotting. In the Nor group, almost all microglia exhibited small cell bodies, thin-branched processes and weak fluorescence. However, activated microglia, which were characterized by enlarged cell bodies, thick processes and stronger fluorescence intensity, were observed in the Ctrl and sirtinol groups following OGD/R injury. Moreover, Res and SRT reversed the signs of microglial activation compared with the Ctrl and sirtinol groups following OGD/R injury (P < 0.05, Fig. 2 A). In addition, the protein expression of Iba1 exhibited the same trend, as determined by fluorescence intensity (P < 0.05, Fig. 2B and C).
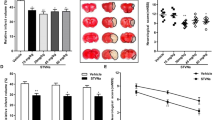
Effects of Sirt1 on microglial activation and inflammation following OGD/R injury in vitro(A) Immunofluorescence images showed the activation of microglia in each group following OGD/R injury. The anti-Iba1 antibody was replaced with PBS to serve as NC. Red, Iba1; blue, DAPI. Scale bar, 50 μm. (B and C) Effect of Sirt1 on the protein expression of Iba1, as evaluated using western blotting. (D-J) Effect of Sirt1 on the secretion of the inflammatory cytokines IL-10, TNF-α and IL-1β following OGD/R injury, as assessed using ELISA and western blotting. *P < 0.05 vs. Nor; #P < 0.05 vs. Ctrl; ▲P < 0.05 vs. Res; $P < 0.05 vs. SRT; ANOVA. n = 3
Activated microglia serve a dual role during ischemia, releasing pro-inflammatory cytokines (such as TNF-α and IL-1β) that can aggravate ischemic injury, whilst promoting the release of anti-inflammatory cytokines (such as IL-10) to reduce ischemic injury [2]. Therefore, ELISA and western blotting were used to examine the protein levels of TNF-α, IL-1β and IL-10 in culture supernatants and in cell lysates, respectively, following OGD/R. The protein levels of TNF-α, IL-1β and IL-10 were significantly increased in the culture supernatant and in the cell lysates 24 h after OGD/R injury in the Ctrl, Res and SRT and sirtinol groups compared with those in the Nor group (P < 0.05, Fig. 2D-J). In the Res and SRT groups, the protein levels of TNF-α and IL-1β were significantly reduced and those of IL-10 were significantly increased compared with the Ctrl group (P < 0.05, Fig. 2D-J). In the sirtinol group, the protein levels of TNF-α and IL-1β were significantly increased and those of IL-10 were significantly decreased compared with the Res and SRT groups (P < 0.05, Fig. 2D-J). These results suggested that Sirt1 could regulate activation of N9 microglia and inflammation following OGD/R injury in vitro.
Effects of Sirt1 on nuclear translocation of Gli-1 and expression of shh, Ptc-1, smo and Gli-1 in N9 microglia following OGD/R injury in vitro
Shh signaling plays an important role in embryogenesis, cell proliferation and differentiation, as well as tissue repair [16]. Therefore, the subsequent experiments were used to determine whether Sirt1 affected the nuclear translocation of Gli-1 and the expression levels of components of the Shh signaling pathway, such as Shh, Ptc-1, Smo and Gli-1.
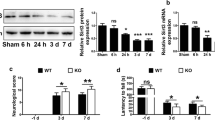
Immunofluorescence staining demonstrated that Gli-1 accumulated in the cytoplasm in the Nor group and was also mostly observed in the cytoplasm in the Ctrl group. In the Res and SRT groups, Gli-1 was translocated from the cytoplasm to the nucleus. However, in the sirtinol group, Gli-1 was mostly observed in the cytoplasm (Fig. 3 A). Moreover, western blot analysis indicated that the protein expression levels of Shh, Ptc-1, Smo and Gli-1 were significantly increased in the Res and SRT groups compared with the Ctrl group and were significantly decreased in the sirtinol group compared with the Res and SRT groups (P < 0.05, Fig. 3B-F). These results indicated that Sirt1 regulated the nuclear translocation of Gli-1 and the expression levels of components of the Shh signaling pathway in N9 microglia following OGD/R injury in vitro.
Effects of Sirt1 on the translocation of Gli-1 molecules and the expression of Shh, Ptc-1, Smo and Gli-1 in N9 microglia following OGD/R injury in vitro
(A) Effects of Sirt1 on the translocation of Gli-1 following OGD/R injury. Gli-1 accumulated in the cytoplasm in the Nor group, but it was partly transferred to the nucleus in the Ctrl and sirtinol groups and almost completely transferred to the nucleus in the Res and SRT groups. The anti-Gli-1 antibody was replaced with PBS to serve as NC. Red, Gli-1; blue, DAPI. Scale bar, 50 μm. (B-F) Effect of Sirt1 on Shh, Ptc-1, Smo and Gli-1 protein expression in microglia following OGD/R injury, as assessed using western blotting. *P < 0.05 vs. Nor; #P < 0.05 vs. Ctrl; ▲P < 0.05 vs. Res; $P < 0.05 vs. SRT; ANOVA. n = 3
Discussion
The present study demonstrated that stimulation with the Sirt1 agonists Res or SRT could suppress the microglial activation and apoptosis, reduce inflammation, trigger Gli-1 translocation from the cytoplasm to the nucleus and upregulate the protein expression levels of Shh, Ptc-1, Smo and Gli-1 following OGD/R in vitro. By contrast, inhibition of Sirt1 using sirtinol had the opposite effect. These findings suggest that, following OGD/R injury, Sirt1 regulates microglial activation and inflammation via the Shh/Gli-1 signaling pathway.
Activated microglia acquire either an ‘M1’ phenotype and release pro-inflammatory cytokines, or an ‘M2’ phenotype associated with the release of anti-inflammatory cytokines [2]. Butturini et al. [29] reported that hypoxia induced the phosphorylation and S-glutathionylation of STAT1, leading to aberrant M1 microglial activation. In an in vitro lipopolysaccharide-induced microglial activation model, sevoflurane reduced microglial activation by suppressing NF-κB and MAPK signaling [30]. Stromal cell-derived factor-1 can induce microglial activation through the PI3K and ERK signaling pathways [31]. Salidroside suppresses M1 microglial polarization and promotes spinal cord injury functional recovery through AMPK/mTOR-mediated autophagic flux stimulation [32]. Res can suppress M1 microglial polarization via peroxisome proliferator-activated receptor γ coactivator 1-α or Sirt1 [33]. Melatonin was also shown to inhibit microglial activation via the SIRT1/nuclear factor erythroid 2-related factor 2 pathway [34]. The present study demonstrated that stimulation with the Sirt1 agonists, Res or SRT, could inhibit activation of microglia by triggering the translocation of Gli-1 molecules and upregulating the expression of components of the Shh signaling pathway. Sirt1 inhibition using sirtinol had the opposite effect. Taken together, these findings suggest that microglial activation may be regulated through various signaling pathways and could be targeted using multiple drugs.
Lu et al. [27] reported that activated Sirt1 can inhibit microglial activation by inhibiting Wnt/β-catenin signaling. In a mouse model of type-2 diabetes, Sirt1 activation inhibited microglial activation by upregulating BDNF [35]. Moreover, Sirt1 can reduce microglia-dependent amyloid-β toxicity by inhibiting NF-κB signaling [36]. These findings suggested that Sirt1 may affect microglial activation through various signaling pathways. In addition, according to the literature, we know that resveratrol can activate microglia, promote the M2 polarization of microglia and reduce neuroinflammation [37, 38]. Duan et al. [39] reported that SRT2140, an Sirt1 agonist, could attenuate CUMS-induced depressive-like behaviors via shifting microglial polarization toward the M2 phenotype. SRT1720, an agonist of Sirt1, can improve cell viability, promote M2 microglia polarization, suppress inflammatory response and inhibit oxidative damage via modulation of ROS-mediated NLRP3 inflammasome signaling after subarachnoid hemorrhage [40]. At present, our team has not yet conducted research on the polarization of microglia, which will be the next research goal of our team to explore the pathway how to regulate the polarization of microglia by Sirt1 agonist or antagonist in vivo and in vivo respectively.
Shh, Ptc-1, Smo and Gli-1 are principle components of the canonical Shh signaling pathway, which is maintained in an ‘off’ state in the absence of Shh ligand for Ptc and inhibition of Smo [21]. When Shh binds to the Ptc-1 receptor, inhibition of Smo is relieved, thereby activating Gli transcription factors and allowing Gli proteins to translocate from the cytoplasm into the nucleus, further mediating the downstream effects of the Shh signaling pathway [41]. In the 1-methyl-4-phenyl-1,2,3,6-tetrahydropyridine (MPTP)-induced in vivo model of Parkinson’s disease, activated microglia were found to express Shh, and most neural cells, except oligodendrocytes, responded to microglia-derived Shh in MPTP-treated substantia nigra [42]. Moreover, activation of Shh signaling by purmorphamine inhibited activation of lipopolysaccharide-treated BV2 microglia through the PI3K/AKT pathway and protected dopaminergic neurons in a mouse model of Parkinson’s disease [43]. Lai et al. [44] reported that epigallocatechin gallate and minocycline increased the expression of Shh and that the anti-inflammatory effects of brain-derived neurotrophic factor were mediated by erythropoietin/Shh in microglia. These previous studies indicated that Shh/Gli-1 signaling may represent a potential therapeutic target for the regulation of microglial activation in central nervous system diseases. Furthermore, the findings of the present study were consistent with other researches which demonstrated that inhibition of microglial overactivation was closely associated with the Shh signaling pathway. Therefore, identifying drugs or targets activating Shh signaling pathway may exert neuroprotective effects by inhibiting microglial activation and reducing inflammation following OGD/R injury or cerebral ischemic injury.
However, there remain several questions to be further elucidated. For example, whether pretreatment with resveratrol, SRT1720 and sirtinol can affect the viability, apoptosis rate, activation and neuroinflammation of microglia, as well as the expression of Shh signaling-related molecules, prior to OGD/R injury in vitro and cerebral ischemic injury in vivo; whether Sirt1 can act through the Shh signaling pathway in microglia following cerebral ischemic injury in vivo and whether its effects are neuroprotective or neurorestorative; and whether Sirt1 can promote the polarization of microglia towards the ‘M1’ or ‘M2’ subtype. Is ‘M1’ microglia polarized into ‘M2’ subtype or is ‘M2’ microglia polarized into ‘M1’ subtype when administered following OGD/R injury in vitro or cerebral ischemic injury in vivo, and whether it is involved in the Shh signaling pathway. In the future, these issues will be further investigated by conducting animal experiments in vivo.
Conclusion
To sum up, the findings of the present study may provide insight into the mechanism underlying Sirt1-regulated activation of microglia and neurological inflammation in the acute phase of stroke (Fig. 3). In the future, it will be necessary to examine how Sirt1 regulates the Shh/Gli-1 signaling pathway and to confirm the results of the present study in vivo.
Data availability
The datasets used and/or analyzed during the present study may be obtained from the corresponding author on reasonable request.
References
Hickman S, Izzy S, Sen P et al (2018) Microglia in neurodegeneration. Nat Neurosci 21:1359–1369
Kim E, Cho S (2016) Microglia and monocyte-derived macrophages in stroke. Neurotherapeutics 13:702–718
Ma Y, Wang J, Wang Y et al (2017) The biphasic function of microglia in ischemic stroke. Prog Neurobiol 157:247–272
Xu H, Qin W, Hu X et al (2018) Lentivirus-mediated overexpression of OTULIN ameliorates microglia activation and neuroinflammation by depressing the activation of the NF-kappaB signaling pathway in cerebral ischemia/reperfusion rats. J Neuroinflamm 15:83
Meng X, Tan J, Li M et al (2017) Sirt1: role under the condition of ischemia/hypoxia. Cell Mol Neurobiol 37:17–28
Gomes BAQ, Silva JPB (2018) Neuroprotective mechanisms of resveratrol in Alzheimer’s disease: role of SIRT1. Oxid Med Cell Longev. https://doi.org/10.1155/2018/8152373
Li X, Feng Y, Wang XX et al (2020) The critical role of SIRT1 in Parkinson’s Disease: mechanism and therapeutic considerations. Aging Dis 11:1608–1622
Lu H, Wang B (2017) SIRT1 exerts neuroprotective effects by attenuating cerebral ischemia/reperfusion-induced injury via targeting p53/microRNA-22. Int J Mol Med 39:208–216
Yan J, Luo A, Gao J et al (2019) The role of SIRT1 in neuroinflammation and cognitive dysfunction in aged rats after anesthesia and surgery. Am J Transl Res 11:1555–1568
Zhang XS, Wu Q, Wu LY et al (2016) Sirtuin 1 activation protects against early brain injury after experimental subarachnoid hemorrhage in rats. Cell Death Dis 7:e2416
Cheng W, Yu P, Wang L et al (2015) Sonic hedgehog signaling mediates resveratrol to increase proliferation of neural stem cells after oxygen-glucose deprivation/reoxygenation injury in vitro. Cell Physiol Biochem 35:2019–2032
Li L, Sun Q, Li Y et al (2015) Overexpression of SIRT1 induced by resveratrol and inhibitor of miR-204 suppresses activation and proliferation of Microglia. J Mol Neurosci 56:858–867
Tang F, Guo S, Liao H et al (2017) Resveratrol enhances neurite outgrowth and synaptogenesis via sonic hedgehog signaling following oxygen-glucose deprivation/reoxygenation Injury. Cell Physiol Biochem 43:852–869
Arensdorf AM, Dillard ME, Menke JM et al (2017) Sonic hedgehog activates phospholipase A2 to enhance smoothened ciliary translocation. Cell Rep 19:2074–2087
Martinez JA, Kobayashi M, Krishnan A et al (2015) Intrinsic facilitation of adult peripheral nerve regeneration by the sonic hedgehog morphogen. Exp Neurol 271:493–505
Patel SS, Tomar S, Sharma D et al (2017) Targeting sonic hedgehog signaling in neurological disorders. Neurosci Biobehav Rev 74:76–97
Huang JG, Shen CB, Wu WB et al (2014) Primary cilia mediate sonic hedgehog signaling to regulate neuronal-like differentiation of bone mesenchymal stem cells for resveratrol induction in vitro. J Neurosci Res 92:587–596
Huang SS, Cheng H, Tang CM et al (2013) Anti-oxidative, anti-apoptotic, and pro-angiogenic effects mediate functional improvement by sonic hedgehog against focal cerebral ischemia in rats. Exp Neurol 247:680–688
Hung HC, Hsiao YH, Gean PW (2014) Learning induces sonic hedgehog signaling in the amygdala which promotes neurogenesis and long-term memory formation. Int J Neuropsychopharmacol 18:pyu071
Sanchez MA, Armstrong RC (2018) Postnatal sonic hedgehog (shh) responsive cells give rise to oligodendrocyte lineage cells during myelination and in adulthood contribute to remyelination. Exp Neurol 299:122–136
Yao PJ, Petralia RS, Mattson MP (2016) Sonic hedgehog signaling and hippocampal neuroplasticity. Trends Neurosci 39:840–850
Zhang J, Li Y, Zhang ZG et al (2009) Bone marrow stromal cells increase oligodendrogenesis after stroke. J Cereb Blood Flow Metab 29:1166–1174
Tiberi L, Bonnefont J, van den Ameele J et al (2014) A BCL6/BCOR/SIRT1 complex triggers neurogenesis and suppresses medulloblastoma by repressing Sonic hedgehog signaling. Cancer Cell 26:797–812
Guo S, Liao H, Liu J et al (2018) Resveratrol activated sonic hedgehog signaling to enhance viability of NIH3T3 cells in Vitro via Regulation of Sirt1. Cell Physiol Biochem 50:1346–1360
Sui D, Xie Q, Yi W et al (2016) Resveratrol protects against sepsis-associated encephalopathy and inhibits the NLRP3/IL-1β axis in Microglia. Mediators Inflamm. https://doi.org/10.1155/2016/1045657
Liu J, Jiao K, Zhou Q et al (2021) Resveratrol alleviates 27-hydroxycholesterol-induced senescence in nerve cells and affects zebrafish locomotor behavior via activation of SIRT1-mediated STAT3 signaling. Oxid Med Cell Longev. https://doi.org/10.1155/2021/6673343
Lu P, Han D, Zhu K et al (2019) Effects of Sirtuin 1 on microglia in spinal cord injury involvement of Wnt/β-catenin signaling pathway. NeuroReport 30:867–874
Zhang Y, Anoopkumar-Dukie S, Mallik SB et al (2021) SIRT1 and SIRT2 modulators reduce LPS-induced inflammation in HAPI microglial cells and protect SH-SY5Y neuronal cells in vitro. J Neural Transm (Vienna) 128:631–644
Butturini E, Boriero D, Carcereri de Prati A et al (2019) STAT1 drives M1 microglia activation and neuroinflammation under hypoxia. Arch Biochem Biophys 669:22–30
Yu X, Zhang F, Shi J (2019) Effect of sevoflurane treatment on microglia activation, NF-kB and MAPK activities. Immunobiology 224:638–644
Lu DY, Tang CH, Yeh WL et al (2009) SDF-1alpha up-regulates interleukin-6 through CXCR4, PI3K/Akt, ERK, and NF-kappaB-dependent pathway in microglia. Eur J Pharmacol 613:146–154
Wang C, Wang Q, Lou Y et al (2018) Salidroside attenuates neuroinflammation and improves functional recovery after spinal cord injury through microglia polarization regulation. J Cell Mol Med 22:1148–1166
Yang X, Xu S, Qian Y (2017) Resveratrol regulates microglia M1/M2 polarization via PGC-1α in conditions of neuroinflammatory injury. Brain Behav Immun. https://doi.org/10.1016/j.bbi.2017.03.003
Arioz BI, Tastan B, Tarakcioglu E et al (2019) Melatonin attenuates LPS-induced acute depressive-like behaviors and microglial NLRP3 inflammasome activation through the SIRT1/Nrf2 pathway. Front Immunol. https://doi.org/10.3389/fimmu.2019.01511
Lang X, Zhao N, He Q et al (2020) Treadmill exercise mitigates neuroinflammation and increases BDNF via activation of SIRT1 signaling in a mouse model of T2DM. Brain Res Bull 165:30–39
Chen J, Zhou Y, Mueller-Steiner S et al (2005) SIRT1 protects against microglia-dependent amyloid-beta toxicity through inhibiting NF-kappaB signaling. J Biol Chem 280:40364–40374
Yang X, Xu S, Qian Y et al (2017) Resveratrol regulates microglia M1/M2 polarization via PGC-1α in conditions of neuroinflammatory injury. Brain Behav Immun 64:162–172
Ma S, Fan L, Li J et al (2020) Resveratrol promoted the M2 polarization of microglia and reduced neuroinflammation after cerebral ischemia by inhibiting miR-155. Int J Neurosci 130(8):817–825
Duan C, Zhang J, Wan T et al (2020) SRT2104 attenuates chronic unpredictable mild stress-induced depressive-like behaviors and imbalance between microglial M1 and M2 phenotypes in the mice. Behav Brain Res 378:112296
Xia D, Yuan J, Jiang X et al (2021) SIRT1 promotes M2 microglia polarization via reducing ROS-Mediated NLRP3 Inflammasome signaling after subarachnoid hemorrhage. Front Immunol 12:770744
Arensdorf AM, Marada S, Ogden SK (2016) Smoothened regulation: a tale of two signals. Trends Pharmacol Sci 37:62–72
Lee JH, Chung YC, Bok E et al (2017) Injury-stimulated sonic hedgehog expression in microglia contributes to neuroinflammatory response in the MPTP model of Parkinson’s disease. Biochem Biophys Res Commun 482:980–986
Shao S, Wang GL, Raymond C et al (2017) Activation of sonic hedgehog signal by purmorphamine, in a mouse model of Parkinson’s disease, protects dopaminergic neurons and attenuates inflammatory response by mediating PI3K/AKt signaling pathway. Mol Med Rep 16:1269–1277
Lai SW, Chen JH, Lin H et al (2018) Regulatory Effects of neuroinflammatory responses through brain-derived neurotrophic factor signaling in Microglial cells. Mol Neurobiol 55:7487–7499
Acknowledgements
We are grateful to the equipment support provided by the laboratory of the First Affiliated Hospital of Chongqing Medical University, the relevant technical guidance offered by teachers and the help from colleagues.
Funding
The present study was supported by several grants named the National Nature Science Foundation of China (Grant No. 81671309 and 81971229), the Tibet Nature Science Foundation of Tibet (grant no. XZ2017ZR-ZY026) and the Postgraduate Research and Innovation Project of Chongqing (Grant No. CYS17148) respectively.
Author information
Authors and Affiliations
Contributions
HL largely conceived the study, performed the experiments and drafted the manuscript. QY provided the funding and revised the manuscript. JH, JL, YC, HZ, XL and JW performed part of the experiments, organized the figures, collected and analyzed the data. All the authors have read and approved the final manuscript.
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflicts of interest.
Ethical approval
This article does not contain any studies with human participants or animals performed by any of the authors.
Additional information
Publisher’s Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if changes were made. The images or other third party material in this article are included in the article's Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article's Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
Liao, H., Huang, J., Liu, J. et al. Sirt1 regulates microglial activation and inflammation following oxygen-glucose deprivation/reoxygenation injury by targeting the Shh/Gli-1 signaling pathway. Mol Biol Rep 50, 3317–3327 (2023). https://doi.org/10.1007/s11033-022-08167-6
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11033-022-08167-6