Summary
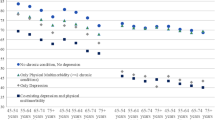
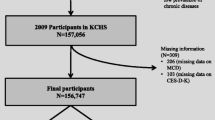
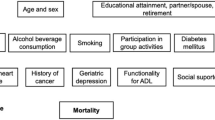
Given the rapid increase in the prevalence of chronic diseases in aging populations, this prospective study including 17 707 adults aged ≥45 years from China Health and Retirement Longitudinal Study was used to estimate the associations between chronic disease, multimorbidity, and depression among middle-aged and elderly adults in China, and explore the mediating factors. Depressive symptoms were assessed using the 10-item Centre for Epidemiological Studies Depression Scale (CES-D-10) questionnaire. Twelve chronic physical conditions, including hypertension, diabetes, dyslipidemia, cancer, chronic lung disease, liver disease, heart failure, stroke, kidney disease, arthritis or rheumatism, asthma, digestive disease were assessed. The prevalence rates for physical multimorbidity and depression (CES-D-10 ≥10) were 43.23% and 36.62%, respectively. Through multivariable logistic models and generalized estimating equation (GEE) models, we found all 12 chronic physical conditions, and multimorbidity were significantly associated with depression. Both mobility problems and chronic pain explained more than 30% of the association for all chronic conditions, with particularly high percentages for stroke (51.56%) and cancer (51.06%) in mobility problems and cancer (53.35%) in chronic pain. Limited activities of daily living (ADL) explained 34.60% of the stroke-cancer relationship, while sleep problems explained between 10.15% (stroke) and 14.89% (chronic lung disease) of the association. Individuals with chronic diseases or multimorbidity are significantly more likely to be depressed. Functional symptoms involving limitations of ADL and mobility difficulties mediated much of the association between chronic diseases and incident depression. These symptoms could be targeted for interventions to ameliorate the incidence of depression among individuals with chronic conditions.
Article PDF
Similar content being viewed by others
Avoid common mistakes on your manuscript.
References
Zeng Y. Towards Deeper Research and Better Policy for Healthy Aging —Using the Unique Data of Chinese Longitudinal Healthy Longevity Survey. China Economic J, 2012,5(2–3):131–149
Fang EF, Scheibye-Knudsen M, Jahn HJ, et al. A research agenda for aging in China in the 21st century. Age Res Rev, 2015,24(Pt B):197–205
Yang G, Wang Y, Zeng Y, et al. Rapid health transition in China, 1990–2010: findings from the Global Burden of Disease Study 2010. Lancet, 2013,381(9882):1987–2015
Yu J, Li J, Cuijpers P, et al. Prevalence and correlates of depressive symptoms in Chinese older adults: a population-based study. Int J Geriatr Psychiatry, 2012,27(3):305–312
Zhang B, Li J. Gender and marital status differences in depressive symptoms among elderly adults: the roles of family support and friend support. Aging Ment Health, 2011,15(7):844–854
Rudisch B, Nemeroff CB. Epidemiology of comorbid coronary artery disease and depression. Biol Psychiatry, 2003,54(3):227–240
Anderson RJ, Freedland KE, Clouse RE, et al. The prevalence of comorbid depression in adults with diabetes: a meta-analysis. Diabetes Care, 2001,24(6):1069–1078
Matcham F, Rayner L, Steer S, et al. The prevalence of depression in rheumatoid arthritis: a systematic review and meta-analysis. Rheumatology (Oxford), 2013,52(12):2136–2148
Moussavi S, Chatterji S, Verdes E, et al. Depression, chronic diseases, and decrements in health: results from the World Health Surveys. Lancet, 2007,370(9590):851–858
Abegunde DO, Mathers CD, Adam T, et al. The burden and costs of chronic diseases in low-income and middle-income countries. Lancet, 2007,370(9603):1929–1938
Bisschop MI, Kriegsman DM, Deeg DJ, et al. The longitudinal relation between chronic diseases and depression in older persons in the community: the Longitudinal Aging Study Amsterdam. J Clin Epidemiol, 2004,57(2):187–194
Olvera RL, Fisher-Hoch SP, Williamson DE, et al. Depression in Mexican Americans with diagnosed and undiagnosed diabetes. Psychol Med, 2016,46(3):637–646
Tong A, Wang X, Li F, et al. Risk of depressive symptoms associated with impaired glucose metabolism, newly diagnosed diabetes, and previously diagnosed diabetes: a meta-analysis of prospective cohort studies. Acta Diabetol, 2016,53(4):589–598
Nouwen A, Nefs G, Caramlau I, et al. Prevalence of depression in individuals with impaired glucose metabolism or undiagnosed diabetes: a systematic review and meta-analysis of the European Depression in Diabetes (EDID) Research Consortium. Diabetes Care, 2011,34(3):752–762
Xue J, Chen S, Bogner HR, et al. The prevalence of depressive symptoms among older patients with hypertension in rural China. Int J Geriatr Psychiatry, 2017,32(12):1411–1417
Kawada T. The prevalence of depression in rheumatoid arthritis: a systematic review and meta-analysis. Rheumatology (Oxford), 2014,53(3):578
Palmer S, Vecchio M, Craig JC, et al. Prevalence of depression in chronic kidney disease: systematic review and meta-analysis of observational studies. Kidney Int, 2013,84(1):179–191
Xiao T, Qiu H, Chen Y, et al. Prevalence of anxiety and depression symptoms and their associated factors in mild COPD patients from community settings, Shanghai, China: a cross-sectional study. BMC Psychiatry, 2018,18(1):89
Krebber AM, Buffart LM, Kleijn G, et al. Prevalence of depression in cancer patients: a meta-analysis of diagnostic interviews and self-report instruments. Psycho-oncology, 2014,23(2):121–130
Chen MH, Su TP, Chen YS, et al.. Higher risk of developing major depression and bipolar disorder in later life among adolescents with asthma: a nationwide prospective study. J Psychiatr Res, 2014,49:25–30
Fei K, Benn EK, Negron R, et al. Prevalence of Depression Among Stroke Survivors: Racial-Ethnic Differences. Stroke, 2016,47(2):512–515
Read JR, Sharpe L, Modini M, et al.. Multimorbidity and depression: A systematic review and meta-analysis. J Affect Disord, 2017,221:36–46
Lewinsohn PM, Hoberman HM, Teri L, et al. An integrative theory of depression. Theoretical issues in behavior therapy. Orlando, FL: Academic Press. 1985.
Paunio T, Korhonen T, Hublin C, et al.. Poor sleep predicts symptoms of depression and disability retirement due to depression. J Affect Disord, 2015,172:381–389
Zis P, Daskalaki A, Bountouni I, et al.. Depression and chronic pain in the elderly: links and management challenges. Clin Interv Aging, 2017,12:709–720
Zhao Y, Hu Y, Smith JP, et al. Cohort profile: the China Health and Retirement Longitudinal Study (CHARLS). Int J Epidemiol, 2014,43(1):61–68
Song A, Liang Y, Yan Z, et al. Highly prevalent and poorly controlled cardiovascular risk factors among Chinese elderly people living in the rural community. Eur J Prev Cardiol, 2014,21(10):1267–1274
National Cholesterol Education Program (NCEP) Expert Panel on Detection E, and Treatment of High Blood Cholesterol in Adults (Adult Treatment Panel III). Third Report of the National Cholesterol Education Program (NCEP) Expert Panel on Detection, Evaluation, and Treatment of High Blood Cholesterol in Adults (Adult Treatment Panel III) final report. Circulation, 2002,106(25):3143–3421.
Association AD. Diagnosis and classification of diabetes mellitus. Diabetes Care, 2014,37 Suppl 1:S81–90
Marengoni A, Rizzuto D, Wang HX, et al. Patterns of chronic multimorbidity in the elderly population. J Am Geriatr Soc, 2009,57(2):225–230
Kriegsman DM, Penninx BW, van Eijk JT, et al. Self-reports and general practitioner information on the presence of chronic diseases in community dwelling elderly. A study on the accuracy of patients’ self-reports and on determinants of inaccuracy. J Clin Epidemiol, 1996,49(12):1407–1417
Qin T, Liu W, Yin M, et al.. Body mass index moderates the relationship between C-reactive protein and depressive symptoms: evidence from the China Health and Retirement Longitudinal Study. Sci Rep, 2017,7:39 940
Chen HJ, Mui AC. Factorial validity of the Center for Epidemiologic Studies Depression Scale short form in older population in China. Int Psychogeriatr, 2014,26(1):49–57
Katz S, Ford AB, Moskowitz RW, et al.. Studies of illness in the aged. The index of ADL: a standardized measure of biological and psychosocial function. JAMA, 1963,185:914–919
Lawton MP, Brody EM. Assessment of older people: self-maintaining and instrumental activities of daily living. Gerontologist, 1969,9(3):179–186
Hylands-White N, Duarte RV, Raphael JH. An overview of treatment approaches for chronic pain management. Rheumatol Int, 2017,37(1):29–42
Yoshida K, Lin TC, Wei M, et al. The roles of post-diagnosis accumulation of morbidities and lifestyle changes on excess total and cause-specific mortality risk in rheumatoid arthritis. Arthritis Care Res (Hoboken), 2019. doi: https://doi.org/10.1002/acr.24120
Ni Y, Tein JY, Zhang M, et al.. Changes in depression among older adults in China: A latent transition analysis. J Affect Disord, 2017,209:3–9
Lichtman JH, Froelicher ES, Blumenthal JA, et al. Depression as a risk factor for poor prognosis among patients with acute coronary syndrome: systematic review and recommendations: a scientific statement from the American Heart Association. Circulation, 2014,129(12):1350–1369
Peters A, McEwen BS.. Stress habituation, body shape and cardiovascular mortality. Neurosci Biobehav Rev, 2015,56:139–150
Mahmood S, Hassan SZ, Tabraze M, et al. Prevalence and Predictors of Depression Amongst Hypertensive Individuals in Karachi, Pakistan. Cureus, 2017,9(6):e1397
Badescu SV, Tataru C, Kobylinska L, et al. The association between Diabetes mellitus and Depression. J Med Life, 2016,9(2):120–125
Pashaki MS, Mezel JA, Mokhtari Z, et al. The prevalence of comorbid depression in patients with diabetes: A meta-analysis of observational studies. Diabetes Metab Syndr, 2019,13(6):3113–3119
Kim SY, Chanyang M, Oh DJ, et al. Association between depression and rheumatoid arthritis: two longitudinal follow-up studies using a national sample cohort. Rheumatology (Oxford), 2020,59(8):1889–1897
Besirli A, Alptekin JO, Kaymak D, et al. The Relationship Between Anxiety, Depression, Suicidal Ideation and Quality of Life in Patients with Rheumatoid Arthritis. Psychiatr Q, 2020,91(1):53–64
Soosova MS, Macejova Z, Zamboriova M, et al. Anxiety and depression in Slovak patients with rheumatoid arthritis. J Ment Health, 2017,26(1):21–27
Read JR, Sharpe L, Modini M, et al.. Multimorbidity and depression: A systematic review and meta-analysis. J Affect Disord, 2017,221:36–46
Stubbs B, Vancampfort D, Veronese N, et al. Depression and physical health multimorbidity: primary data and country-wide meta-analysis of population data from 190 593 people across 43 low- and middle-income countries. Psychol Med, 2017,47(12):2107–2117
Katon W, Lin EH, Von Korff M, et al. Integrating depression and chronic disease care among patients with diabetes and/or coronary heart disease: the design of the TEAMcare study. Contemp Clin Trials, 2010,31(4):312–322
Beck AT. The evolution of the cognitive model of depression and its neurobiological correlates. Am J Psychiatry, 2008,165(8):969–977
Williamson GM. Extending the activity restriction model of depressed affect: evidence from a sample of breast cancer patients. Health Psychol, 2000,19(4):339–347
Hepgul N, Mondelli V, Pariante CM. Psychological and biological mechanisms of cytokine induced depression. Epidermol Psichiatr Soc, 2010,19(2):98–102
Gaskin DJ, Richard P. The economic costs of pain in the United States. J Pain, 2012,13(8):715–724
Gerrits MM, van Oppen P, van Marwijk HW, et al. Pain and the onset of depressive and anxiety disorders. Pain, 2014,155(1):53–59
van den Akker M, van Steenkiste B, Krutwagen E, et al. Disease or no disease? Disagreement on diagnoses between self-reports and medical records of adult patients. Eur J Gen Pract, 2015,21(1):45–51
Acknowledgments
We thank Benjamin Knight, MSc., from Liwen Bianji, Edanz Editing China (http://www.liwenbianji.cn/ac), for editing the English text of a draft of this manuscript.
Author information
Authors and Affiliations
Corresponding author
Additional information
This study was supported by the MOE (Ministry of Education in China) Liberal Arts and Social Sciences Youth Foundation (No. 16YJC630047).
Conflict of Interest Statement
The authors have declared no conflicts of interest for this article.
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License https://creativecommons.org/licenses/by/4.0/), which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if changes were made. The images or other third party material in this article are included in the article’s Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article’s Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
Jiang, Ch., Zhu, F. & Qin, Tt. Relationships between Chronic Diseases and Depression among Middle-aged and Elderly People in China: A Prospective Study from CHARLS. CURR MED SCI 40, 858–870 (2020). https://doi.org/10.1007/s11596-020-2270-5
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11596-020-2270-5