Abstract
Purpose of Review
The purpose of the review is to summarize the expression and function of CSF1R and its ligands in bone homeostasis and constraints on therapeutic targeting of this axis.
Recent Findings
Bone development and homeostasis depends upon interactions between mesenchymal cells and cells of the mononuclear phagocyte lineage (MPS), macrophages, and osteoclasts (OCL). The homeostatic interaction is mediated in part by the systemic and local production of growth factors, macrophage colony-stimulating factor (CSF1), and interleukin 34 (IL34) that interact with a receptor (CSF1R) expressed exclusively by MPS cells and their progenitors. Loss-of-function mutations in CSF1 or CSF1R lead to loss of OCL and macrophages and dysregulation of postnatal bone development. MPS cells continuously degrade CSF1R ligands via receptor-mediated endocytosis. As a consequence, any local or systemic increase or decrease in macrophage or OCL abundance is rapidly reversible.
Summary
In principle, both CSF1R agonists and antagonists have potential in bone regenerative medicine but their evaluation in disease models and therapeutic application needs to carefully consider the intrinsic feedback control of MPS biology.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
The essential requirement for macrophage colony-stimulating factor (CSF1) in bone development became evident with the identification of causal loss-of-function mutations in the Csf1 gene in mice and rats [1,2,3] that were associated with severe osteopetrosis. There are also isolated reports of CSF1 deficiency in human malignant osteopetrosis [4] although this is more commonly associated with mutations in genes expressed specifically in osteoclasts (OCL) and required for the process of bone resorption [5]. The bone developmental defect in CSF1 deficiency in mice is associated with the loss of bone-resorbing OCL [6]. Conversely, genetic studies of Paget’s disease, a disorder of excessive OCL function, revealed an association with the human CSF1 locus [7]. In mice, the osteopetrosis and OCL deficiency correct with age [8, 9]. CSF1 signals via a plasma membrane tyrosine kinase receptor encoded by the Csf1r gene. Homozygous mutation of Csf1r in mice and rats is also associated with osteopetrosis [10, 11•]. The rather more severe phenotype of the receptor mutation in mice and the age-dependent correction in CSF1-deficient models likely reflect the contribution of a second ligand, interleukin 34 (IL34), which binds to an overlapping site on the receptor and can complement CSF1 deficiency when expressed as a transgene [12]. By contrast, mutation of Csf1 in the toothless (tl/tl) rat is associated with unremitting osteopetrosis and OCL deficiency but a much less severe effect on postnatal somatic growth than in mice [3, 13]. The importance of species differences is discussed further below.
Osteoporosis is commonly attributed to an imbalance between the physiologically coupled processes of osteoclastic bone resorption and osteoblastic bone formation [14, 15, 16•]. Current therapies aimed at arresting bone loss, bisphosphonates and specific antibodies, are targeted against OCL [17, 18]. The appropriate balance between bone resorption and formation/calcification is clearly also crucial in acute osteolysis in chronic inflammation, infection, and malignancy [19] and conversely in bone regeneration in response to fracture. Given the phenotypic consequences of CSF1 and CSF1R mutations during development, these molecules would appear as obvious therapeutic targets for bone-related pathologies and regenerative medicine. To assess both the opportunities and the risks of such a strategy, it is necessary to have an understanding of the expression, regulation, and function of the CSF1R gene and both of its agonists in bone. This review provides an overview of current knowledge.
CSF1R Protein Expression is Restricted to Mononuclear Phagocytes
A key question when considering CSF1R as a therapeutic target, and in the interpretation of the biological activity of agonists, antagonists, and mutations, is the localization of expression. The transcription of the Csf1r gene in vivo has been tracked through the generation and analysis of Csf1r reporter transgenes in mice, rats, and chickens [20,21,22,23,24,25], and the molecular basis of transcriptional regulation has been reviewed elsewhere [26]. Csf1r mRNA is expressed by the earliest phagocytes generated in the yolk sac [27] and the Csf1r reporter transgenes are expressed by tissue macrophages throughout the developing embryo [25, 28]. The expression of Csf1r mRNA tracks with expression of other macrophage markers in transcriptome analysis of tissue macrophages [29] and reflects the progressive expansion of tissue macrophages during embryo development and further increases in the postnatal period [30]. In adult mice, Csf1r mRNA and protein are absent from pluripotent hematopoietic stem cells in the bone marrow [31, 32•, 33] and induced during differentiation/lineage commitment in myeloid progenitors. Csf1r mRNA is expressed by blood monocytes, granulocytes, tissue macrophages, dendritic cells, and OCL [33,34,35]. In granulocytes, Csf1r mRNA is co-expressed with several other macrophage-specific transcripts that are not translated into protein [34].
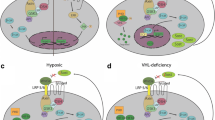
There have been multiple reports of expression of Csf1r mRNA or CSF1R protein outside of the myeloid lineages including developing neurons, intestinal and renal epithelial cells, and smooth muscle and mesangial cells [36, 37]. These reports are inconsistent with other evidence (reviewed in [38]). Expression outside the myeloid lineages is not supported by localization of any of the Csf1r reporter transgenes in any species, nor in situ localization of Csf1r mRNA [27, 39]. To address the issue finally, we generated a knock-in transgene that reports CSF1R protein expression [32•]. Visualization in bone marrow revealed expression in megakaryocytes, which had not previously been appreciated and may be relevant to thrombocytopenia observed in CSF1-treated animals and patients [38]. Figure 1 shows a schematic view of the MPS of bone, and images of the Csf1r-FusionRed transgene in mouse bone marrow, highlighting distinct MPS subpopulations associated with specific niches on the bone surface and within the marrow.
The mononuclear phagocyte populations of mouse bone. The schematic at left highlights the diversity of mononuclear phagocyte populations (osteoclasts, monocyte, macrophages (Mϕ), and committed progenitors (CMP, OMP)) found in mouse bone and the local and systemic sources of growth factors CSF1 and IL34. The images at right show the co-localization of the Csf1r-FusionRed transgene [32•] and the macrophage-restricted F4/80 antigen [45•]. The low power image confirms that the majority of bone marrow hematopoietic and mesenchymal (osteoblast, fibroblast, adipocyte, endothelial) cells lack expression of the FusionRed reporter [32•]. Osteoclasts (Panel A) express FusionRed but lack F4/80 [45•]. Mϕ populations associated with the bone surface (B), hematopoietic islands (C), and sinusoids (D) express both FusionRed and F4/80. F4/80 is relatively low on monocytes. Panels A and D contain multiple FusionRed-positive mononuclear cells; presumptive monocytes; and their progenitors. At bottom of Panel D, the large FusionRed-positive, F4/80-negative cell is a megakaryocyte
Outside of the marrow, expression of the CSF1R-FusionRed reporter was restricted to macrophages [32•]. There is no evidence of expression of CSF1R protein outside of the macrophage lineage in any organ at any time in development. All of the Csf1r reporters analyzed in multiple species highlight the abundance and regular distribution of resident macrophages in every tissue in the body, which is an important consideration when contemplating CSF1R as a therapeutic target.
In the specific case of bone, Wittrant et al. [40] claimed that Csf1r mRNA and protein were detectable in mouse calvarial osteoblasts and reported direct effects of CSF1 administration on osteoblast function. These workers excluded contamination of their cultures by monocyte-macrophages on the basis of flow cytometry analysis of macrophage surface markers on cells harvested by trypsinization. However, macrophage adhesion to plastic is not trypsin-sensitive and the authors did not show direct staining of their cultures. The expression of Csf1r mRNA in osteoblasts or any other mesenchymal population was excluded by Dai et al. [41] and it is not evident in published single-cell RNA sequencing (scRNA-seq) profiles of mouse bone marrow stromal cell populations [42, 43]. Chang et al. [44] resolved this conflict. They identified macrophages as a major persistent contaminant of standard mouse calvarial osteoblast cultures, detecting both Csf1r and Adgre1 (F4/80) mRNA and F4/80 protein in situ. These studies led to the characterization of a resident bone macrophage population, termed osteomacs, which express CD169 (Siglec 1), line the surface of bone (see Fig. 1), and contribute to bone homeostasis and repair independently of OCL [44, 45•].
One exception to the macrophage-restricted expression of CSF1R occurs in the placenta. Visvader and Verma [46] first demonstrated that placental trophoblasts utilize a distinct upstream promoter to drive expression of CSF1R in the human placenta. This promoter in humans lies some 25kb upstream of the macrophage transcription start site (TSS), within the 3′ end of the upstream PDGFRB locus. An alternative non-coding exon splices into an acceptor site upstream of the first coding exon. In mice, Csf1r mRNA was detected in the first trophoblast precursors in the ectoplacental cone [47] and was abundant in mature placenta [27] but the precise transcriptional regulation is not conserved. In mice, the major TSS in placenta lie within 500 bp of the macrophage TSS again encoding alternative 5′ UTR exons [24]. Interestingly, this distal promoter region contains the major TSS utilized selectively by OCL and may also have essential enhancer activity for some tissue macrophage populations [48]. Our ongoing studies of Csf1r transcriptional regulation raised a surprising conundrum. Germ-line deletion of a highly conserved enhancer (Fms intronic regulatory element, or FIRE) in the first intron of the mouse gene (Csf1r∆FIRE/∆FIRE ) led to the selective loss of several tissue macrophage populations and abolished expression of Csf1r mRNA and protein in bone marrow progenitors and blood monocytes but had no effect on OCL numbers or bone density [49]. CSF1R-deficient animals and human patients are clearly OCL-deficient and anti-CSF1R antibody also blocks OCL differentiation in osteoblast co-cultures in vitro [50]. Conditional deletion of Csf1r in Tnfrsf11a (Rank)–positive cells also ablates OCL development in mice [51•]. Lineage tracing studies suggested that erythro-myeloid progenitors (EMP) initially seed OCL in the embryo, and ongoing OCL maintenance is supported by fusion of HSC-derived monocytes. The latter cells may rescue OCL deficiencies associated with loss of Csf1r in EMP [51•].
Since resident macrophages and OCL are fragmented during disaggregation [52], the analysis of the Csf1r hypomorphic marrow may have excluded these populations. In common with other macrophage populations in the mutant mice, they probably utilize other enhancers to support Csf1r transcription [49]. In the case of OCL, there is also the unique Csf1r promoter. Transcription factors that might bind to the OCL-specific upstream element to promote Csf1r transcription have not been identified. One candidate is the master regulator NFATC1 [53]. The transcription factor PPARG is essential for osteoclastogenesis and in turn regulates Fos, which is also required [54]. A seminal study in this area indicated that committed OCL progenitors may be enriched for expression of Pparg [55]. Published Chip-Seq data on bone marrow–derived macrophages (BMDM) indicate that PPARG binds to FIRE and to multiple other distal elements in a ligand-independent manner and that binding is up-regulated by interleukin 4 [56]. Research in our group and others identified unique roles for the transcription factor MITF in osteoclastogenesis [57,58,59]. MITF interacts genetically and physically with the macrophage transcription factor PU.1 (Spi1) [58, 59]. We are currently exploring the removal of the OCL-specific promoter region from the mouse germ-line. The loss of CSF1R in bone marrow did not impact on expression of FLT3 in progenitor cells [49] and it is possible that FLT3L can compensate in OCL differentiation in mice independently of CSF1R expression. The reciprocal compensation has been described in mouse dendritic cell differentiation, where CSF1R can compensate for the lack of FLT3 [60]. Lean et al. [61] suggested that FLT3L is responsible for age-dependent recovery of OCL in CSF1-deficient mice, although this was prior to the discovery of IL34. Indeed, Nakamichi et al. [62] provided evidence for an IL34-dependent OCL progenitor population in the spleen of op/op mice. The effect of a compound Csf1/Il34 mutation in mice or rats has not yet been reported.
Expression and Function of CSF1 and IL34 in Bone
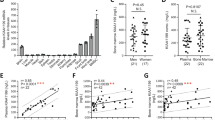
Csf1 mRNA is expressed widely in all species studied, predominantly in cells of mesenchymal lineages. Il34 mRNA in humans is most highly expressed in the brain, spleen, and epidermis (see BioGPS.org; Gtex.org), with transcription initiated from distinct promoters [63]. Figure 2 shows expression profiles of the two regulators in mouse from BioGPS. These profiles highlighted the expression of Csf1 by mast cells and the region-specific expression of Il34 in the brain. More importantly, these data highlighted the induction of Il34 mRNA during induced maturation and calcification in calvarial osteoblasts [44]. Expression of Il34 by differentiating mouse calvarial osteoblasts was confirmed by others [64]. The promoter-based analysis by the FANTOM5 consortium [63] showed that many distinct types of mesenchymal cells express Il34 from a third transcription start site. Few of these resources provide quantification and location of expression in bone in situ.
Expression of Csf1 and Il34 mRNA in mouse. Figure shows screenshots from BioGPS.org of the expression of Csf1 and Il34 mRNA in a wide range of mouse tissues and cells. Csf1 is expressed in embryonic fibroblasts (MEF), ES cells, stimulated mast cells, osteoblasts, and various mesenchymal cell lines. As expected, Il34 was detected primarily in the epidermis and brain, but was also induced during differentiation of primary osteoblasts
Ryan et al. [65] described the detection of a Csf1 promoter-lacZ transgene in osteoblasts and fibroblasts specifically enriched on trabecular surfaces in bone in proximity to OCL. The major secreted and circulating form of CSF1 is a chondroitin sulphate proteoglycan, a biology that is conserved in birds [66]. Nandi et al. [67] reported that transgenic expression of the proteoglycan isoform, rather than cell surface or glycoprotein isoforms, was required to reverse the OCL deficiency and osteopetrosis in op/op mice [67, 68]. In rat bone marrow, the 4.6kb Csf1 mRNA encoding the secreted CSF1 protein is abundant and readily detected by Northern blot [69]. Interestingly, the 1.4kb transcript encoding membrane CSF1 was induced following ovariectomy.
Conditional deletion of floxed Csf1 alleles in C57BL/6 mice as well as the selective restoration of CSF1 expression in op/op mice supported the idea that local CSF1 production is essential for normal bone development (reviewed in [70]). There is some evidence for an effect of mouse genetic background on the penetrance of CSF1 mutations, and it is notable that C57BL/6J female develop early-onset osteoporosis [71]. Harris et al. [72] reported a generic deletion of Csf1 in mesenchymal cells using Meox-cre was sufficient to drive marked reduction in OCL and tissue macrophages leading to osteopetrosis and impaired osteocyte differentiation and survival. Subsequent restricted deletion in osteocytes, using Dmp1-cre, produced little or no bone phenotype [73, 74] suggesting these cells are not a major source of growth factor. The existence of separate niches within marrow is suggested by deletion of Csf1 expression in osteolineage and vascular compartments. Whereas conditional deletion in osteolineage cells using Osx-cre reproduced bone developmental abnormalities, deletion in the vascular compartment with Cdh5-cre had a selective effect on marrow monocytes [74]. Selective expression of Csf1 and Il34 is evident in mouse bone single-cell RNA-seq data. In profiles of bone cells cultured from developing calvaria [75•], Csf1 mRNA was detected in all of the mesenchymal populations, whereas Il34 was more restricted to chondrocytes and immature osteoblasts. As reported previously, Csf1r+/Adgre1+ macrophages were abundant in these cultures and lacked expression of either ligand. Low level cross contamination of some osteoblasts with Csf1r mRNA in the scRNA-seq data likely reflects adhesion of macrophage remnants [52]. The scRNA-seq data support adipocyte-primed leptin receptor positive (LEPR+) mesenchymal cells and sinusoidal endothelial cells [42, 43, 74] as sources of both Csf1 and Il34 in mouse marrow. In overview, all the available data suggests that local CSF1/IL34 is important, and likely mediates interactions between osteoblasts and CSF1R-expressing macrophages, OCL and progenitors as summarized schematically in Fig. 1.
CSF1R Signals in Bone Development
The local production of CSF1 and the development of OCL each appear relatively late in mouse gestation [76]. In 17-day-old embryos, Csf1 transcripts were present in cells lining the outside of the midregion of the metatarsals. At 18 days, Csf1 transcripts were detected by in situ hybridization in newly mineralized cartilage. OCL precursors fuse and the mature OCL invades the mineralized cartilage of the rudiments to excavate the future bone marrow cavity. In these studies, CSF1 was considered a possible chemoattractant as well as a growth factor for OCL precursors. Given the late appearance in gestation, it is not surprising that skeletal development in Csf1- and Csf1r-deficient mice and rats appears relatively normal at birth; the major effects of the mutations appear in the postnatal period. In the case of CSF1 deficiency, transplacental transfer of the growth factor probably compensates for the loss in the embryo. Because of the relative infertility of the op/op and tl/tl females, homozygous mutant pups are derived from heterozygous matings and they are not entirely macrophage-deficient at birth [77]. However, CSF1R-deficient rat embryos are macrophage-deficient [78•] and in mouse the embryonic macrophage population can be depleted by anti-CSF1R administration to the mother [79]. So, professional phagocytes in the embryo are genuinely redundant. The phagocytic activities of the abundant macrophage population in the embryo are not restricted to bone; they are involved in apoptotic cell removal throughout the body [80]. Wood et al. [81] examined the basis for macrophage redundancy in the clearance of apoptotic cells from the interdigital spaces in the footpad of macrophage-deficient PU.1 knockout mice. In the absence of macrophages, phagocytosis was taken over by mesenchymal neighbors. These amateurs appeared somewhat less efficient at recognition engulfment and digestion of apoptotic debris than professionals, but the task was nevertheless completed in a relatively normal time frame and there was no accumulation of pyknotic nuclei.
Even the postnatal development of the skeleton is not completely compromised in animals that are macrophage- and OCL-deficient. Albeit with a much more extensive trabecular network and increased bone density, there is a bone marrow cavity with active hematopoiesis. Despite the absence of hematopoietic island macrophages in the fetal liver and bone marrow, which function in regulation of erythropoiesis and myelopoiesis (see Fig. 1) [82, 83], the mutant animals are not anemic and there is no accumulation of expelled red cell nuclei in the fetal liver. So, to some extent, amateurs must also fulfill some of the tasks normally undertaken by macrophages and OCL in bone development and hematopoiesis. In fact, it is not even certain that any of the impacts of the lack of macrophages and OCL reflect non-redundant functions within bone as opposed to indirect systemic effects. CSF1R signals intersect the regulation of somatic growth via the growth hormone-IGF1 axis and mutant animals are deficient in circulating IGF1 [78•, 84]
As mentioned above, there has been only one isolated report of recessive CSF1 mutation in human osteopetrosis. However, subtle variants in CSF1 protein sequence could potentially alter binding to CSF1R. Such variants determine the species specificity of CSF1:CSF1R interaction. Mouse CSF1 binds poorly to human CSF1R whereas human CSF1 is active in mouse. Pig CSF1 is equally active in mouse and human [85,86,87]. A comparative analysis of the conservation of CSF1:CSF1R contact residues based on the crystal structure of the complex identified multiple candidate substitutions that might contribute to the species specificity [87]. Large-scale exome and genomic sequencing of human genomes (https://gnomad.broadinstitute.org) has identified numerous point mutations within the 150 amino acid bioactive human CSF1 core. They include receptor contact residues and amino acids that are conserved across all mammalian species. Without testing the biological activity of these allelic variants, we cannot determine whether there is any loss of function. However, given the expression of IL34 in bone, it is also possible that loss-of-function mutations in CSF1 in humans do not actually manifest in an overt bone phenotype. By contrast, bi-allelic CSF1R mutations in human patients are associated with skeletal dysplasia and osteosclerosis [88•, 89•]. The syndrome has been called “brain abnormalities, neurodegeneration, and dysosteosclerosis” (BANDDOS, OMIM # 618476; reviewed in [90]). Individuals surviving infancy probably have at least one hypomorphic allele and may not be entirely CSF1R-deficient [38]. No evidence of severe growth retardation seen in rodents has been reported in BANDDOS patients and at least some of the individuals had normal circulating TRAP5b, indicating the functional presence of OCL [88•].
The analysis of the bone phenotype in Csf1r mutant mice is compromised by the strain-dependent pre-weaning lethality. Both ligand and receptor mutations were associated with expanded epiphyseal chondrocyte region, severely disturbed matrix structure, and disorganized collagen fibrils [41, 91]. The layered organization of osteoblasts on the bone-forming surface and the direction of their matrix deposition appeared disrupted, and there was a defect in mineralization. Although these phenotypes were attributed to the lack of OCL, they are also consistent with the regulation of osteoblast differentiation by osteomacs [44].
The effect of null Csf1r mutation (Csf1rko) has been analyzed in more detail in the rat [78•]. As shown in Fig. 3A, B, there is delay in subarticular ossification of short bones, secondary ossification center formation of long bones, and hip-joint formation. One phenotype that was not reported in mutant mice is a profound lack of mineralization in the cranial case and defective cranial suture closure (Fig. 3C) whereas the skull base is hyper-mineralized as it is in human bi-allelic mutations (leading in human to impacts on the cerebellum and the Dandy-Walker malformation). Flat bones are formed by intramembranous ossification, a process that unlike endochondral ossification involves condensation of mesenchymal stem cells (MSC) and their direct differentiation into osteoblasts [92]. Figure 3D highlights disorganization of the tibial diaphyseal region in juvenile Csf1rko rats. There is some evidence of conversion of the abnormal bone into “mature” cortical template but the more mature bone often contains empty osteocyte lacunae. The impact of the Csf1rko was associated with substantive loss of both OCL and osteomacs (Fig. 3E). Residual resident macrophages showed evidence of efferocytosis, but the marrow also showed evidence of accumulation of pyknotic nuclei.
Phenotypic analysis of skeletal development in Csf1r knockout rats. Homozygous knockout mutation of Csf1r in rats (Csf1rko) was generated by Pridans et al. [11•] and impacts on skeletal development were described in [78•]. This figure contains previously unpublished images highlighting aspects of the mutant phenotype and its reversal by bone marrow cell transfer. A–C show μCT images demonstrating the delay in ossification in the digits and formation of the hip-joint and defective cranial suture closure. D shows the tibial diaphyseal region in juvenile WT and Csf1rko rats and the presence of empty osteocyte lacunae. The Csf1rko was associated with substantive loss of both OCL pink stained for expression of tartrate-resistant acid phosphatase (TRAP) and osteomacs (brown stained for expression of IBA1 (E). The inset shows that the residual macrophages showed evidence of efferocytosis but extracellular pyknotic nuclei are also evident (arrowheads). F shows that IBA1+ macrophages are also depleted in skeletal muscle in the Csf1rko rat associated with the reduction in muscle fiber diameter and postnatal somatic growth retardation that is observed in these animals [79]. Transfer of WT bone marrow (BMT) at weaning without conditioning corrected all of these musculoskeletal phenotypes, as exemplified by restoration of muscle mass and fiber diameter (G)
IL34 is also expressed in bone, but thus far no biological function has been identified. No loss-of-function human IL34 mutation has been reported nor is there any evidence of association with IL34 alleles with bone phenotypes. Similarly, no skeletal phenotype or impact on somatic growth has been reported in the mouse IL34 knockout [93]. IL34 is more highly conserved across mammalian species than CSF1 [88•] and the gnomAD database (gnomad.broadinstitute.org) records numerous coding variants that impact highly conserved amino acids. Since, IL34 knockout mice are viable and fertile, it is possible that there are also bi-allelic mutations in humans with little overt phenotype. Baghdadi et al. [94] presented evidence that IL34 production by multiple myeloma cells contributes to tumor-associated osteolysis. In the rat, homozygous Csf1r mutation has a much more profound effect on somatic growth than Csf1 mutation, implying a role for Il34 [13], but both Csf1 and Csf1r mutants are entirely OCL-deficient. Unlike op/op mice, Csf1tl/tl rats show no evidence of age-dependent recovery of OCL [3], and indeed, there is no evidence of extramedullary hematopoiesis in the spleen.
Rescue of the Effect of CSF1R Mutation by Bone Marrow Cell Transfer
Consistent with the lack of irreversible consequences of the lack of embryonic macrophages, the severe phenotypes observed in Csf1r knockout mice and rats can be rescued by postnatal intraperitoneal transfer of wild-type bone marrow cells without any conditioning [78•, 95]. In the rats, this rescue can be achieved as late as weaning, providing a unique model to dissect the precise roles of CSF1R-dependent cells in skeletal morphogenesis [78•]. Surprisingly, rescue is achieved without restoring the blood monocyte population or CSF1-responsive progenitor cells in the bone marrow. Donor bone marrow cells proliferate and differentiate to form macrophages in the peritoneal cavity and appear to traffic directly to distal sites throughout the body, including the brain. Donor-derived macrophages appeared prior to OCL in all of the affected locations in bone indicating that they provide the pioneering cells in primary and secondary ossification center formation, in cranial ossification and suture closure (Batoon et al. Manuscript submitted). In the bone marrow, both hematopoietic island macrophages and OCL were restored from cells of donor origin, whereas the hematopoietic compartment was populated by recipient progenitor cells. These findings in mice and rats support the view that OCL can be generated entirely from bone marrow without input from embryonic erythro-myeloid progenitors. Phenotypic rescue was associated with restoration of somatic growth and circulating IGF1 levels [78•]. CSF1R-dependent macrophages are also abundant in skeletal muscle, cartilage, and tendon and their loss in the Csf1rko was associated with reduction in muscle fiber diameter in juveniles (Fig. 3F and [79]). Wild-type BM transfer also restored muscle macrophage populations and muscle fiber diameter (Fig. 3G). The precise interplay between systemic and local impacts of the BM transfer in bone requires further investigation.
CSF1R and Homeostasis
Tamoxifen-inducible Cre recombinase (ER2-cre) transgenic lines have been widely used in lineage trace models of macrophage and OCL ontogeny. One of the assumptions in studies of macrophage ontogeny is that tamoxifen is a neutral agonist that does not impact macrophage differentiation [96]. The toxicity of tamoxifen in OCL was reported many years ago [97]. In the process of developing a conditional deletion approach for OCL using OCL-specific promoters [98], we tested the effect of tamoxifen treatment at doses routinely used in inducible recombination on OCL in vivo. We found that initial ablation of OCL was followed by a rebound osteoclastogenesis and loss of trabecular bone (unpublished). The acute depletion of OCL by tamoxifen was confirmed recently, alongside a complex dose-dependence wherein low doses actually had the reverse effect [99•]. Current front-line treatments for osteoporosis, bisphosphonates [100] and antibodies against RANKL [101•], also deplete OCL. Cessation of treatment, especially with anti-RANKL, is associated with a rebound osteoporosis [102•].
CSF1 likely contributes to the rebound phenomenon. CSF1 (or IL34) binding to CSF1R is followed by receptor-mediated endocytosis and degradation of both ligand and receptor [103]. New receptors are constantly synthesized and trafficked to the cell surface so that in the steady state macrophages continuously internalize and degrade their ligand. Receptor-mediated endocytosis by macrophages in the liver and spleen controls the circulating CSF1 concentration [104]. As a consequence, CSF1 is elevated in the circulation in CSF1R-deficient animals and in response to anti-CSF1R antibody treatment [10, 78•, 105, 106]. When ligand is removed, CSF1R accumulates on the cell surface and the expression of CSF1R target genes declines rapidly [107, 108]. Interestingly, CSF1R is removed from the cell surface by ectodomain cleavage in response to various toll-like receptor agonists [109]. This could provide a mechanism for acute local or systemic increases in CSF1 in the absence of increased synthesis.
We and others have proposed that macrophages also control the local availability of their own growth factor within tissues as well as systemically [96, 110]. Consequently, when CSF1R-positive cells are depleted locally, there is an intrinsic drive to restore the homeostatic distribution. By the same token, an excess of CSF1R-positive cells in any tissue is unsustainable unless local or systemic CSF1 availability is increased. One clear example of increased ligand availability is the effect of female hormones on Csf1 transcription [69, 111]. In the specific case of bone, the question is, how local is local? There are multiple CSF1R-positive cells in marrow: monocytes and their progenitors, osteomacs, hematopoietic island macrophages, and OCL (Fig. 1; [112]). These populations could potentially compete with each other for available growth factor.
CSF1R-Directed Therapy: More or Less or Both?
The relationship between systemic and local CSF1, the potential role of IL34, the diversity of target cells in bone, species specificity, and the intrinsic homeostatic mechanisms each need to be considered in the development of optimal treatment regimes for CSF1R-direct therapies. Administration of recombinant CSF1 was sufficient to reverse/correct many of the bone developmental phenotypes in op/op mice and tl/tl rats as well as liver and splenic macrophage populations [77, 113,114,115]. The treatment was less effective at restoring resident macrophage populations in other locations, somatic growth, and female fertility [77, 115]. The dose-dependence of rescue by exogenous CSF1 was not analyzed. By adulthood, the dose applied may not have been sufficient to saturate clearance by the liver and spleen. CSF1 administered systemically is probably also selectively accessible to the bone marrow, which shares with the liver a sinusoidal endothelial lining permitting blood cell egress [116].
The first report of CSF1 administration to mice documented an expansion of the CSF1-responsive marrow cell population as well as a monocytosis [85]. The potential of recombinant CSF1 as a therapeutic agent was constrained by the short half-life; the bioactive dimeric recombinant protein is well below the clearance threshold so that in early clinical trials continuous infusion was required. This issue was addressed by the generation and characterization of a CSF1-Fc fusion protein [117] which has been tested in a range of preclinical studies. Daily treatment for 4 days produced a monocytosis and increased liver and spleen mass that peaked around 7–10 days and was rapidly reversed [86, 117, 118]. CSF1-Fc treatment also caused an expansion of mature OCL populations on trabecular bone surfaces and the epiphyseal plate. In the short time frame of these studies, there was no change in bone density or trabecular architecture. However, Lloyd et al. [119, 120] found that prolonged high-dose daily administration of CSF1 to mice increased serum bone turnover markers but nevertheless produced an anabolic effect attributed to the coupled activation of osteoblasts. The same phenomenon was observed in chickens treated with an equivalent avian CSF1-Fc protein [21]. The interpretation of CSF1 response based upon OCL-osteoblast coupling neglects the expansion and stimulation of osteomacs, which likely act directly to promote osteoblast function [44]. The anabolic effects of CSF1 have been harnessed to promote intramembranous ossification in models of bone repair [45•, 121•]. CSF1-Fc dosing can be titrated to increase osteomacs without impacting osteoclast number [121•]. While CSF1-Fc did not reverse the age-dependent osteopenic phenotype observed in female C57BL/6J mice, it promoted a pro-anabolic response post-fracture in both healthy and osteoporotic bones [121•]. The effect was influenced by age and gender [121•], reinforcing the importance of considering these variables when investigating CSF1/CSF1R-directed therapies.
There have been few reports of the effect of IL34 administration. IL34 can replace CSF1 for the generation of OCL from mouse bone marrow progenitors or human monocytes in vitro [64]. Daily IP injections of a relatively low dose of recombinant IL34 increased myeloid cell populations in the marrow and reduce trabecular volume, but the effect on OCL numbers was not reported. IL34 has an affinity for other potential receptors (PTPRZ, CD138) through binding to proteoglycans [122] which may influence the in vivo pharmacology.
Several studies have targeted CSF1/CSF1R signaling to reduce OCL number or function to mitigate bone loss. CSF1R kinase inhibitors and anti-CSF1R antibodies have been evaluated for therapeutic intervention in diseases where macrophages contribute to pathology, e.g., neurodegenerative disease, cancer, inflammation, and fibrosis [123•, 124]. Relatively few studies have focused on bone. PLX3397, which inhibits CSF1R and related kinases, was reported to reduce LPS-induced osteolysis, but the effects were small and OCL were largely retained [125, 126]. Similarly, He et al. [127] found that PLX3397 inhibited CSF1-dependent excess osteoclastogenesis in a mouse neurofibromatosis model in response to ovariectomy. The dose was high (80 mg/kg) but the effects were small and OCL were only marginally altered. Prolonged treatment with another widely applied CSF1R kinase inhibitor, GW2580, inhibited OCL function in vitro and was effective in various inflammatory models [128, 129] but OCL depletion was not observed in vivo. Gleevec (Imatinib), which is in clinical use for treatment of chronic myelogenous leukemia, is also an inhibitor of CSF1R kinase activity, albeit less specific, and effects on OCL may contribute to dysregulated calcium/phosphate homeostasis in patients [130, 131]. In overview, OCL and peripheral macrophage populations are relatively resistant to CSF1R kinase inhibitors. This is partly because macrophage/OCL survival requires lower threshold signal than proliferation, so a drug must provide almost complete and sustained inhibition of CSF1R kinase activity to be effective. It is also likely a consequence of intrinsic homeostasis, where any loss of CSF1R-positive cells drives the local CSF1 concentration higher and promotes compensatory proliferation.
Blocking antibodies are potentially more effective because they can saturate surface receptors and have more favorable half-life/pharmacokinetics. Both anti-CSF1R and anti-CSF1 antibodies have been found to ablate OCL and/or inhibit OCL activity with consequent reduction in bone loss in mice [50, 71, 132,133,134]. The effects seem to be specific to excess OCL activity. For example, whereas prolonged anti-CSF1R depletion of OCL prevented spontaneous bone loss in female C57BL/6J mice, it did not alter bone density in males [71]. Neonatal treatment of mice with anti-CSF1 was sufficient to phenocopy effects of the op/op mutation on bone [135]. Cenci et al. [111] described increased OCL numbers in an Egr1 mutant mouse line, attributed to increased local production of CSF1. A neutralizing antibody to CSF1 restored rates of bone resorption to normal in mutant animals and also completely prevented ovariectomy-induced bone loss in control animals. Anti-CSF1 or anti-CSF1R antibodies have also been evaluated in patients with the focus on inflammatory disease and on depleting tumor-associated macrophages [123•]. Administration of the humanized anti-CSF1R antibody AMG820 in cancer patients produced sustained elevation of circulating CSF1 and ablation of dermal macrophages. There was no effect on circulating TRAP5b, considered a marker of OCL activity [106, 136]. Similarly, a detailed Phase 1 trial of a neutralizing anti-CSF1 antibody in a large cohort of volunteers demonstrated no effect on TRAP5b in peripheral blood, despite a clear dose-dependent decrease in circulating blood monocyte populations [137•]. However, they did observe a reduction in detectable CTX-1, an alternative marker of active resorption. The recipients of anti-CSF1 treatment exhibited periorbital swelling in the eye. In parallel non-human primate studies, this was associated with accumulation of basophilic materials (mainly hyaluronic acid glycosaminoglycans). They reported similar accumulation in multiple other organs. Periorbital swelling is also observed in patients treated with anti-CSF1R [123•] but the mechanism remains unknown. The relative lack of effect of anti-CSF1 contrasts with the ability of anti-RANKL (Denosumab) to produce a 40–50% decline in TRAP5b at least in individuals with elevated TRAP5b associated with osteoporosis [138, 139]. Prolonged anti-RANKL treatment did produce a decline in OCL-specific transcripts in subsequent bone marrow biopsies [140]. One consequence of prolonged OCL depletion was a decrease in circulating dipeptidyl peptidase 4 and an increase in glucagon-like peptide 1, which the authors speculate provides a link between bone and energy metabolism.
There are caveats in comparing effects of anti-CSF1R in animal models and humans. In the presence of anti-CSF1R, CSF1 rises locally and systemically to produce a new steady state where ligand may compete for binding to the receptor. The relative affinity of antibody and ligand for the receptor determines this set point and in turn whether macrophage and OCL populations can be depleted. There is some evidence for differences between rodents and humans. In humans, the circulating CSF1 concentration was very low (<50pg/ml); with a maximal dose of AMG820, it increased 105-fold, to 1000ng/ml [106]. Circulating CSF1 appears higher (around 5ng/ml) in rodents and increased only 20–50-fold in anti-CSF1R-treated mice [105] or in Csf1rko rats [78•]. These findings suggest the human CSF1R has a higher affinity for ligand, and consequently, it may be more difficult to achieve sustainable blockade with anti-CSF1R antibodies. A second important difference between mouse and human lies in the regulation of CSF1 expression. Whereas mouse macrophages are dependent on exogenous ligand, in all other species (including rats and humans) CSF1 is expressed constitutively by macrophages themselves [70]. Autocrine CSF1/CSF1R signaling in OCL in humans may be less accessible to inhibition by antibodies.
Conclusions
Anti-CSF1R or anti-CSF1 treatment is reasonably well-tolerated, albeit with significant side effects including periorbital edema noted above [123, 137•]. There may be applications in acute bone loss associated with infection, bone metastasis, or glucocorticoid treatment. Paradoxically, CSF1 treatment may produce similar outcomes. In both cases, the effects are likely to be rapidly reversible because of the intrinsic homeostasis. Indeed, promising clinical trials of anti-CSF1R in chronic graft versus host disease have been based on a repeated intermittent treatment [123•]. In overview, while there is no doubt that CSF1/CSF1R signals control OCL and macrophage function in bone during development, the therapeutic applications of this knowledge remain unclear.
References
Papers of particular interest, published recently, have been highlighted as: • Of importance
Wiktor-Jedrzejczak W, Bartocci A, Ferrante AW Jr, Ahmed-Ansari A, Sell KW, Pollard JW, Stanley ER. Total absence of colony-stimulating factor 1 in the macrophage-deficient osteopetrotic (op/op) mouse. Proc Natl Acad Sci U S A. 1990;87(12):4828–32. https://doi.org/10.1073/pnas.87.12.4828.
Yoshida H, Hayashi S, Kunisada T, Ogawa M, Nishikawa S, Okamura H, et al. The murine mutation osteopetrosis is in the coding region of the macrophage colony stimulating factor gene. Nature. 1990;345(6274):442–4. https://doi.org/10.1038/345442a0.
Van Wesenbeeck L, Odgren PR, MacKay CA, D’Angelo M, Safadi FF, Popoff SN, et al. The osteopetrotic mutation toothless (tl) is a loss-of-function frameshift mutation in the rat Csf1 gene: evidence of a crucial role for CSF-1 in osteoclastogenesis and endochondral ossification. Proc Natl Acad Sci U S A. 2002;99(22):14303–8. https://doi.org/10.1073/pnas.202332999.
Lajeunesse D, Busque L, Menard P, Brunette MG, Bonny Y. Demonstration of an osteoblast defect in two cases of human malignant osteopetrosis. Correction of the phenotype after bone marrow transplant. J Clin Invest. 1996;98(8):1835–42. https://doi.org/10.1172/JCI118984.
Sobacchi C, Schulz A, Coxon FP, Villa A, Helfrich MH. Osteopetrosis: genetics, treatment and new insights into osteoclast function. Nat Rev Endocrinol. 2013;9(9):522–36. https://doi.org/10.1038/nrendo.2013.137.
Cecchini MG, Hofstetter W, Halasy J, Wetterwald A, Felix R. Role of CSF-1 in bone and bone marrow development. Mol Reprod Dev. 1997;46(1):75–83. https://doi.org/10.1002/(SICI)1098-2795(199701)46:1<75::AID-MRD12>3.0.CO;2-2.
Albagha OM, Visconti MR, Alonso N, Langston AL, Cundy T, Dargie R, et al. Genome-wide association study identifies variants at CSF1, OPTN and TNFRSF11A as genetic risk factors for Paget’s disease of bone. Nat Genet. 2010;42(6):520–4. https://doi.org/10.1038/ng.562.
Begg SK, Bertoncello I. The hematopoietic deficiencies in osteopetrotic (op/op) mice are not permanent, but progressively correct with age. Exp Hematol. 1993;21(4):493–5.
Nilsson SK, Lieschke GJ, Garcia-Wijnen CC, Williams B, Tzelepis D, Hodgson G, Grail D, Dunn AR, Bertoncello I. Granulocyte-macrophage colony-stimulating factor is not responsible for the correction of hematopoietic deficiencies in the maturing op/op mouse. Blood. 1995;86(1):66–72.
Dai XM, Ryan GR, Hapel AJ, Dominguez MG, Russell RG, Kapp S, Sylvestre V, Stanley ER. Targeted disruption of the mouse colony-stimulating factor 1 receptor gene results in osteopetrosis, mononuclear phagocyte deficiency, increased primitive progenitor cell frequencies, and reproductive defects. Blood. 2002;99(1):111–20.
• Pridans C, Raper A, David GM, Alves J, Sauter KA, Lefevre L, et al. Pleiotropic impacts of macrophage and microglial deficiency on development in rats with targeted mutation of the Csf1r locus. JImmunol. 2018;201(9):2683-99. The first description of the Csf1r null mutation in rats, highlighting differences to more widely studied mouse models.
Wei S, Nandi S, Chitu V, Yeung YG, Yu W, Huang M, Williams LT, Lin H, Stanley ER. Functional overlap but differential expression of CSF-1 and IL-34 in their CSF-1 receptor-mediated regulation of myeloid cells. J Leukoc Biol. 2010;88(3):495–505. https://doi.org/10.1189/jlb.1209822.
Hume DA, Caruso M, Keshvari S, Patkar OL, Sehgal A, Bush SJ, Summers KM, Pridans C, Irvine KM. The mononuclear phagocyte system of the rat. J Immunol. 2021;206(10):2251–63. https://doi.org/10.4049/jimmunol.2100136.
Fischer V, Haffner-Luntzer M. Interaction between bone and immune cells: implications for postmenopausal osteoporosis. Semin Cell Dev Biol. 2022;123:14–21. https://doi.org/10.1016/j.semcdb.2021.05.014.
Sims NA, Martin TJ. Coupling signals between the osteoclast and osteoblast: how are messages transmitted between these temporary visitors to the bone surface? Front Endocrinol (Lausanne). 2015;6:41. 10.3389/fendo.2015.00041.
• Sims NA, Martin TJ. Osteoclasts provide coupling signals to osteoblast lineage cells through multiple mechanisms. Annu Rev Physiol. 2020;82:507-29. https://doi.org/10.1146/annurev-physiol-021119-034425. Recent comprehensive review of osteoclast-osteoblast coupling mechanisms.
Reid IR, Billington EO. Drug therapy for osteoporosis in older adults. Lancet. 2022;399(10329):1080–92. https://doi.org/10.1016/S0140-6736(21)02646-5.
Takahata M, Shimizu T, Yamada S, Yamamoto T, Hasegawa T, Fujita R, Kobayashi H, Endo T, Koike Y, Amizuka N, Todoh M, Okumura JI, Kajino T, Iwasaki N. Bone biopsy findings in patients receiving long-term bisphosphonate therapy for glucocorticoid-induced osteoporosis. J Bone Miner Metab. 2022;40:613–22. https://doi.org/10.1007/s00774-022-01323-9.
Mbalaviele G, Novack DV, Schett G, Teitelbaum SL. Inflammatory osteolysis: a conspiracy against bone. J Clin Invest. 2017;127(6):2030–9. https://doi.org/10.1172/JCI93356.
Balic A, Garcia-Morales C, Vervelde L, Gilhooley H, Sherman A, Garceau V, Gutowska MW, Burt DW, Kaiser P, Hume DA, Sang HM. Visualisation of chicken macrophages using transgenic reporter genes: insights into the development of the avian macrophage lineage. Development. 2014;141(16):3255–65. https://doi.org/10.1242/dev.105593.
Garceau V, Balic A, Garcia-Morales C, Sauter KA, McGrew MJ, Smith J, et al. The development and maintenance of the mononuclear phagocyte system of the chick is controlled by signals from the macrophage colony-stimulating factor receptor. BMC Biol. 2015;13:12. https://doi.org/10.1186/s12915-015-0121-9.
Irvine KM, Caruso M, Cestari MF, Davis GM, Keshvari S, Sehgal A, Pridans C, Hume DA. Analysis of the impact of CSF-1 administration in adult rats using a novel Csf1r-mApple reporter gene. J Leukoc Biol. 2020;107(2):221–35. https://doi.org/10.1002/JLB.MA0519-149R.
Hawley CA, Rojo R, Raper A, Sauter KA, Lisowski ZM, Grabert K, Bain CC, Davis GM, Louwe PA, Ostrowski MC, Hume DA, Pridans C, Jenkins SJ. Csf1r-mApple transgene expression and ligand binding in vivo reveal dynamics of CSF1R expression within the mononuclear phagocyte system. J Immunol. 2018;200(6):2209–23. https://doi.org/10.4049/jimmunol.1701488.
Sasmono RT, Oceandy D, Pollard JW, Tong W, Pavli P, Wainwright BJ, Ostrowski MC, Himes SR, Hume DA. A macrophage colony-stimulating factor receptor-green fluorescent protein transgene is expressed throughout the mononuclear phagocyte system of the mouse. Blood. 2003;101(3):1155–63. https://doi.org/10.1182/blood-2002-02-0569.
Sauter KA, Pridans C, Sehgal A, Bain CC, Scott C, Moffat L, Rojo R, Stutchfield BM, Davies CL, Donaldson DS, Renault K, McColl BW, Mowat AM, Serrels A, Frame MC, Mabbott NA, Hume DA. The MacBlue binary transgene (csf1r-gal4VP16/UAS-ECFP) provides a novel marker for visualisation of subsets of monocytes, macrophages and dendritic cells and responsiveness to CSF1 administration. PLoS ONE. 2014;9(8):e105429. https://doi.org/10.1371/journal.pone.0105429.
Rojo R, Pridans C, Langlais D, Hume DA. Transcriptional mechanisms that control expression of the macrophage colony-stimulating factor receptor locus. Clin Sci (Lond). 2017;131(16):2161–82. https://doi.org/10.1042/CS20170238.
Lichanska AM, Browne CM, Henkel GW, Murphy KM, Ostrowski MC, McKercher SR, et al. Differentiation of the mononuclear phagocyte system during mouse embryogenesis: the role of transcription factor PU.1. Blood. 1999;94(1):127–38.
Rae F, Woods K, Sasmono T, Campanale N, Taylor D, Ovchinnikov DA, Grimmond SM, Hume DA, Ricardo SD, Little MH. Characterisation and trophic functions of murine embryonic macrophages based upon the use of a Csf1r-EGFP transgene reporter. Dev Biol. 2007;308(1):232–46. https://doi.org/10.1016/j.ydbio.2007.05.027.
Summers KM, Bush SJ, Hume DA. Network analysis of transcriptomic diversity amongst resident tissue macrophages and dendritic cells in the mouse mononuclear phagocyte system. PLoS Biol. 2020;18(10):e3000859. https://doi.org/10.1371/journal.pbio.3000859.
Summers KM, Hume DA. Identification of the macrophage-specific promoter signature in FANTOM5 mouse embryo developmental time course data. J Leukoc Biol. 2017;102(4):1081–92. https://doi.org/10.1189/jlb.1A0417-150RR.
Nestorowa S, Hamey FK, Pijuan Sala B, Diamanti E, Shepherd M, Laurenti E, Wilson NK, Kent DG, Göttgens B. A single-cell resolution map of mouse hematopoietic stem and progenitor cell differentiation. Blood. 2016;128(8):e20–31. https://doi.org/10.1182/blood-2016-05-716480.
• Grabert K, Sehgal A, Irvine KM, Wollscheid-Lengeling E, Ozdemir DD, Stables J, et al. A transgenic line that reports CSF1R protein expression provides a definitive marker for the mouse mononuclear phagocyte system. J Immunol. 2020;205(11):3154-66. https://doi.org/10.4049/jimmunol.2000835. Analysis of a knock-in transgenic line demonstrates conclusively that CSF1R is not expressed outside of the mononuclear phagocyte lineage, a key to interpreting effects of therapeutic interventions.
Tagoh H, Himes R, Clarke D, Leenen PJ, Riggs AD, Hume D, et al. Transcription factor complex formation and chromatin fine structure alterations at the murine c-fms (CSF-1 receptor) locus during maturation of myeloid precursor cells. Genes Dev. 2002;16(13):1721–37. https://doi.org/10.1101/gad.222002.
Sasmono RT, Ehrnsperger A, Cronau SL, Ravasi T, Kandane R, Hickey MJ, Cook AD, Himes SR, Hamilton JA, Hume DA. Mouse neutrophilic granulocytes express mRNA encoding the macrophage colony-stimulating factor receptor (CSF-1R) as well as many other macrophage-specific transcripts and can transdifferentiate into macrophages in vitro in response to CSF-1. J Leukoc Biol. 2007;82(1):111–23. https://doi.org/10.1189/jlb.1206713.
Summers KM, Bush SJ, Wu C, Hume DA. Generation and network analysis of an RNA-seq transcriptional atlas for the rat. NAR Genom Bioinform. 2022;4(1):lqac017. https://doi.org/10.1093/nargab/lqac017.
Chitu V, Biundo F, Stanley ER. Colony stimulating factors in the nervous system. Semin Immunol. 2021;54:101511. https://doi.org/10.1016/j.smim.2021.101511.
Chitu V, Stanley ER. Regulation of embryonic and postnatal development by the CSF-1 receptor. Curr Top Dev Biol. 2017;123:229–75. https://doi.org/10.1016/bs.ctdb.2016.10.004.
Hume DA, Caruso M, Ferrari-Cestari M, Summers KM, Pridans C, Irvine KM. Phenotypic impacts of CSF1R deficiencies in humans and model organisms. J Leukoc Biol. 2020;107(2):205–19. https://doi.org/10.1002/JLB.MR0519-143R.
Sehgal A, Donaldson DS, Pridans C, Sauter KA, Hume DA, Mabbott NA. The role of CSF1R-dependent macrophages in control of the intestinal stem-cell niche. Nat Commun. 2018;9(1):1272. https://doi.org/10.1038/s41467-018-03638-6.
Wittrant Y, Gorin Y, Mohan S, Wagner B, Abboud-Werner SL. Colony-stimulating factor-1 (CSF-1) directly inhibits receptor activator of nuclear factor-{kappa}B ligand (RANKL) expression by osteoblasts. Endocrinology. 2009;150(11):4977–88. https://doi.org/10.1210/en.2009-0248.
Dai XM, Zong XH, Akhter MP, Stanley ER. Osteoclast deficiency results in disorganized matrix, reduced mineralization, and abnormal osteoblast behavior in developing bone. J Bone Miner Res. 2004;19(9):1441–51. https://doi.org/10.1359/JBMR.040514.
Baryawno N, Przybylski D, Kowalczyk MS, Kfoury Y, Severe N, Gustafsson K, Kokkaliaris KD, Mercier F, Tabaka M, Hofree M, Dionne D, Papazian A, Lee D, Ashenberg O, Subramanian A, Vaishnav ED, Rozenblatt-Rosen O, Regev A, Scadden DT. A cellular taxonomy of the bone marrow stroma in homeostasis and leukemia. Cell. 2019;177(7):1915–32 e16. https://doi.org/10.1016/j.cell.2019.04.040.
Tikhonova AN, Dolgalev I, Hu H, Sivaraj KK, Hoxha E, Cuesta-Dominguez A, et al. The bone marrow microenvironment at single-cell resolution. Nature. 2019;569(7755):222–8. https://doi.org/10.1038/s41586-019-1104-8.
Chang MK, Raggatt LJ, Alexander KA, Kuliwaba JS, Fazzalari NL, Schroder K, Maylin ER, Ripoll VM, Hume DA, Pettit AR. Osteal tissue macrophages are intercalated throughout human and mouse bone lining tissues and regulate osteoblast function in vitro and in vivo. J Immunol. 2008;181(2):1232–44. https://doi.org/10.4049/jimmunol.181.2.1232.
• Batoon L, Millard SM, Wullschleger ME, Preda C, Wu AC, Kaur S, et al. CD169(+) macrophages are critical for osteoblast maintenance and promote intramembranous and endochondral ossification during bone repair. Biomaterials. 2019;196:51-66. https://doi.org/10.1016/j.biomaterials.2017.10.033. Key paper defining the functional importance of osteomacs, independent of osteoclasts, in regulation of osteoblast function.
Visvader J, Verma IM. Differential transcription of exon 1 of the human c-fms gene in placental trophoblasts and monocytes. Mol Cell Biol. 1989;9(3):1336–41. https://doi.org/10.1128/mcb.9.3.1336-1341.1989.
Passey RJ, Williams E, Lichanska AM, Wells C, Hu S, Geczy CL, et al. A null mutation in the inflammation-associated S100 protein S100A8 causes early resorption of the mouse embryo. J Immunol. 1999;163(4):2209–16.
Ovchinnikov DA, DeBats CE, Sester DP, Sweet MJ, Hume DA. A conserved distal segment of the mouse CSF-1 receptor promoter is required for maximal expression of a reporter gene in macrophages and osteoclasts of transgenic mice. J Leukoc Biol. 2010;87(5):815–22. https://doi.org/10.1189/jlb.0809557.
Rojo R, Raper A, Ozdemir DD, Lefevre L, Grabert K, Wollscheid-Lengeling E, Bradford B, Caruso M, Gazova I, Sánchez A, Lisowski ZM, Alves J, Molina-Gonzalez I, Davtyan H, Lodge RJ, Glover JD, Wallace R, Munro DAD, David E, et al. Deletion of a Csf1r enhancer selectively impacts CSF1R expression and development of tissue macrophage populations. Nat Commun. 2019;10(1):3215. https://doi.org/10.1038/s41467-019-11053-8.
Nara Y, Kitaura H, Ogawa S, Shen WR, Qi J, Ohori F, et al. Anti-c-fms antibody prevents osteoclast formation and bone resorption in co-culture of osteoblasts and osteoclast precursors in vitro and in ovariectomized mice. Int J Mol Sci. 2020;21(17). https://doi.org/10.3390/ijms21176120.
• Jacome-Galarza CE, Percin GI, Muller JT, Mass E, Lazarov T, Eitler J, et al. Developmental origin, functional maintenance and genetic rescue of osteoclasts. Nature. 2019;568(7753):541-5. https://doi.org/10.1038/s41586-019-1105-7. Definitive study of the development and homeostatic maintenance of osteoclasts in the mouse, pointing to potential therapies for osteoclast deficiency.
Millard SM, Heng O, Opperman KS, Sehgal A, Irvine KM, Kaur S, Sandrock CJ, Wu AC, Magor GW, Batoon L, Perkins AC, Noll JE, Zannettino ACW, Sester DP, Levesque JP, Hume DA, Raggatt LJ, Summers KM, Pettit AR. Fragmentation of tissue-resident macrophages during isolation confounds analysis of single-cell preparations from mouse hematopoietic tissues. Cell Rep. 2021;37(8):110058. https://doi.org/10.1016/j.celrep.2021.110058.
Kurotaki D, Yoshida H, Tamura T. Epigenetic and transcriptional regulation of osteoclast differentiation. Bone. 2020;138:115471. https://doi.org/10.1016/j.bone.2020.115471.
Wan Y, Chong LW, Evans RM. PPAR-gamma regulates osteoclastogenesis in mice. Nat Med. 2007;13(12):1496–503. https://doi.org/10.1038/nm1672.
Wei W, Zeve D, Wang X, Du Y, Tang W, Dechow PC, et al. Osteoclast progenitors reside in the peroxisome proliferator-activated receptor gamma-expressing bone marrow cell population. Mol Cell Biol. 2011;31(23):4692–705. https://doi.org/10.1128/MCB.05979-11.
Daniel B, Nagy G, Czimmerer Z, Horvath A, Hammers DW, Cuaranta-Monroy I, Poliska S, Tzerpos P, Kolostyak Z, Hays TT, Patsalos A, Houtman R, Sauer S, Francois-Deleuze J, Rastinejad F, Balint BL, Sweeney HL, Nagy L. The nuclear receptor PPARgamma controls progressive macrophage polarization as a ligand-insensitive epigenomic ratchet of transcriptional memory. Immunity. 2018;49(4):615–26 e6. https://doi.org/10.1016/j.immuni.2018.09.005.
Hershey CL, Fisher DE. Mitf and Tfe3: members of a b-HLH-ZIP transcription factor family essential for osteoclast development and function. Bone. 2004;34(4):689–96. https://doi.org/10.1016/j.bone.2003.08.014.
Luchin A, Purdom G, Murphy K, Clark MY, Angel N, Cassady AI, Hume DA, Ostrowski MC. The microphthalmia transcription factor regulates expression of the tartrate-resistant acid phosphatase gene during terminal differentiation of osteoclasts. J Bone Miner Res. 2000;15(3):451–60. https://doi.org/10.1359/jbmr.2000.15.3.451.
Luchin A, Suchting S, Merson T, Rosol TJ, Hume DA, Cassady AI, Ostrowski MC. Genetic and physical interactions between microphthalmia transcription factor and PU.1 are necessary for osteoclast gene expression and differentiation. J Biol Chem. 2001;276(39):36703–10. https://doi.org/10.1074/jbc.M106418200.
Durai V, Bagadia P, Briseno CG, Theisen DJ, Iwata A, Davidson JT, et al. Altered compensatory cytokine signaling underlies the discrepancy between Flt3(-/-) and Flt3l(-/-) mice. J Exp Med. 2018;215(5):1417–35. https://doi.org/10.1084/jem.20171784.
Lean JM, Fuller K, Chambers TJ. FLT3 ligand can substitute for macrophage colony-stimulating factor in support of osteoclast differentiation and function. Blood. 2001;98(9):2707–13. https://doi.org/10.1182/blood.v98.9.2707.
Nakamichi Y, Mizoguchi T, Arai A, Kobayashi Y, Sato M, Penninger JM, Yasuda H, Kato S, DeLuca HF, Suda T, Udagawa N, Takahashi N. Spleen serves as a reservoir of osteoclast precursors through vitamin D-induced IL-34 expression in osteopetrotic op/op mice. Proc Natl Acad Sci U S A. 2012;109(25):10006–11. https://doi.org/10.1073/pnas.1207361109.
The FANTOM Consortium, Forrest AR, Kawaji H, Rehli M, et al. A promoter-level mammalian expression atlas. Nature. 2014;507(7493):462-470. https://doi.org/10.1038/nature13182.
Chen Z, Buki K, Vaaraniemi J, Gu G, Vaananen HK. The critical role of IL-34 in osteoclastogenesis. PLoS ONE. 2011;6(4):e18689. https://doi.org/10.1371/journal.pone.0018689.
Ryan GR, Dai XM, Dominguez MG, Tong W, Chuan F, Chisholm O, Russell RG, Pollard JW, Stanley ER. Rescue of the colony-stimulating factor 1 (CSF-1)-nullizygous mouse (Csf1(op)/Csf1(op)) phenotype with a CSF-1 transgene and identification of sites of local CSF-1 synthesis. Blood. 2001;98(1):74–84. https://doi.org/10.1182/blood.v98.1.74.
Garceau V, Smith J, Paton IR, Davey M, Fares MA, Sester DP, Burt DW, Hume DA. Pivotal advance: avian colony-stimulating factor 1 (CSF-1), interleukin-34 (IL-34), and CSF-1 receptor genes and gene products. J Leukoc Biol. 2010;87(5):753–64. https://doi.org/10.1189/jlb.0909624.
Nandi S, Akhter MP, Seifert MF, Dai XM, Stanley ER. Developmental and functional significance of the CSF-1 proteoglycan chondroitin sulfate chain. Blood. 2006;107(2):786–95. https://doi.org/10.1182/blood-2005-05-1822.
Dai XM, Zong XH, Sylvestre V, Stanley ER. Incomplete restoration of colony-stimulating factor 1 (CSF-1) function in CSF-1-deficient Csf1op/Csf1op mice by transgenic expression of cell surface CSF-1. Blood. 2004;103(3):1114–23. https://doi.org/10.1182/blood-2003-08-2739.
Lea CK, Sarma U, Flanagan AM. Macrophage colony stimulating-factor transcripts are differentially regulated in rat bone-marrow by gender hormones. Endocrinology. 1999;140(1):273–9. https://doi.org/10.1210/endo.140.1.6451.
Sehgal A, Irvine KM, Hume DA. Functions of macrophage colony-stimulating factor (CSF1) in development, homeostasis, and tissue repair. Semin Immunol. 2021;54:101509. https://doi.org/10.1016/j.smim.2021.101509.
Sauter KA, Pridans C, Sehgal A, Tsai YT, Bradford BM, Raza S, Moffat L, Gow DJ, Beard PM, Mabbott NA, Smith LB, Hume DA. Pleiotropic effects of extended blockade of CSF1R signaling in adult mice. J Leukoc Biol. 2014;96(2):265–74. https://doi.org/10.1189/jlb.2A0114-006R.
Harris SE, MacDougall M, Horn D, Woodruff K, Zimmer SN, Rebel VI, Fajardo R, Feng JQ, Gluhak-Heinrich J, Harris MA, Abboud Werner S. Meox2Cre-mediated disruption of CSF-1 leads to osteopetrosis and osteocyte defects. Bone. 2012;50(1):42–53. https://doi.org/10.1016/j.bone.2011.09.038.
Werner SL, Sharma R, Woodruff K, Horn D, Harris SE, Gorin Y, Lee DY, Hua R, Gu S, Fajardo RJ, Habib SL, Jiang JX. CSF-1 in osteocytes inhibits Nox4-mediated oxidative stress and promotes normal bone homeostasis. JBMR Plus. 2020;4(7):e10080. https://doi.org/10.1002/jbm4.10080.
Emoto T, Lu J, Sivasubramaniyam T, Maan H, Khan AB, Abow AA, Schroer SA, Hyduk SJ, Althagafi MG, McKee TD, Fu F, Shabro S, Ulndreaj A, Chiu F, Paneda E, Pacheco S, Wang T, Li A, Jiang JX, et al. Colony stimulating factor-1 producing endothelial cells and mesenchymal stromal cells maintain monocytes within a perivascular bone marrow niche. Immunity. 2022;55:862–878.e8. https://doi.org/10.1016/j.immuni.2022.04.005.
• Ayturk UM, Scollan JP, Goz Ayturk D, Suh ES, Vesprey A, Jacobsen CM, et al. Single-cell RNA sequencing of calvarial and long-bone endocortical cells. J Bone Miner Res. 2020;35(10):1981-91. https://doi.org/10.1002/jbmr.4052. Single-cell RNA-seq analysis of bone marrow stroma reveals the main cellular sources of CSF1 and IL34 and confirms lack of expression of the receptor in mesenchymal cells.
Hofstetter W, Wetterwald A, Cecchini MG, Mueller C, Felix R. Detection of transcripts and binding sites for colony-stimulating factor-1 during bone development. Bone. 1995;17(2):145–51. https://doi.org/10.1016/s8756-3282(95)00163-8.
Cecchini MG, Dominguez MG, Mocci S, Wetterwald A, Felix R, Fleisch H, Chisholm O, Hofstetter W, Pollard JW, Stanley ER. Role of colony stimulating factor-1 in the establishment and regulation of tissue macrophages during postnatal development of the mouse. Development. 1994;120(6):1357–72. https://doi.org/10.1242/dev.120.6.1357.
• Keshvari S, Caruso M, Teakle N, Batoon L, Sehgal A, Patkar OL, et al. CSF1R-dependent macrophages control postnatal somatic growth and organ maturation. PLoS Genet. 2021;17(6):e1009605. https://doi.org/10.1371/journal.pgen.1009605. Key study showing that the effects of CSF1R mutation in rats on musculoskeletal development can be reversed by transfer of wild-type bone marrow cells without conditioning.
Hoeffel G, Chen J, Lavin Y, Low D, Almeida FF, See P, Beaudin AE, Lum J, Low I, Forsberg EC, Poidinger M, Zolezzi F, Larbi A, Ng LG, Chan JKY, Greter M, Becher B, Samokhvalov IM, Merad M, Ginhoux F. C-Myb(+) erythro-myeloid progenitor-derived fetal monocytes give rise to adult tissue-resident macrophages. Immunity. 2015;42(4):665–78. https://doi.org/10.1016/j.immuni.2015.03.011.
Henson PM, Hume DA. Apoptotic cell removal in development and tissue homeostasis. Trends Immunol. 2006;27(5):244–50. https://doi.org/10.1016/j.it.2006.03.005.
Wood W, Turmaine M, Weber R, Camp V, Maki RA, McKercher SR, et al. Mesenchymal cells engulf and clear apoptotic footplate cells in macrophageless PU.1 null mouse embryos. Development. 2000;127(24):5245–52. https://doi.org/10.1242/dev.127.24.5245.
Levesque JP, Summers KM, Bisht K, Millard SM, Winkler IG, Pettit AR. Macrophages form erythropoietic niches and regulate iron homeostasis to adapt erythropoiesis in response to infections and inflammation. Exp Hematol. 2021;103:1–14. https://doi.org/10.1016/j.exphem.2021.08.011.
Levesque JP, Summers KM, Millard SM, Bisht K, Winkler IG, Pettit AR. Role of macrophages and phagocytes in orchestrating normal and pathologic hematopoietic niches. Exp Hematol. 2021;100:12–31 e1. https://doi.org/10.1016/j.exphem.2021.07.001.
Gow DJ, Sester DP, Hume DA. CSF-1, IGF-1, and the control of postnatal growth and development. J Leukoc Biol. 2010;88(3):475–81. https://doi.org/10.1189/jlb.0310158.
Hume DA, Pavli P, Donahue RE, Fidler IJ. The effect of human recombinant macrophage colony-stimulating factor (CSF-1) on the murine mononuclear phagocyte system in vivo. J Immunol. 1988;141(10):3405–9.
Keshvari S, Genz B, Teakle N, Caruso M, Cestari MF, Patkar OL, Tse BWC, Sokolowski KA, Ebersbach H, Jascur J, MacDonald KPA, Miller G, Ramm GA, Pettit AR, Clouston AD, Powell EE, Hume DA, Irvine KM. Therapeutic potential of macrophage colony-stimulating factor (CSF1) in chronic liver disease. Dis Model Mech. 2022;15. https://doi.org/10.1242/dmm.049387.
Gow DJ, Garceau V, Kapetanovic R, Sester DP, Fici GJ, Shelly JA, Wilson TL, Hume DA. Cloning and expression of porcine colony stimulating factor-1 (CSF-1) and colony stimulating factor-1 receptor (CSF-1R) and analysis of the species specificity of stimulation by CSF-1 and Interleukin 34. Cytokine. 2012;60(3):793–805. https://doi.org/10.1016/j.cyto.2012.08.008.
• Guo L, Bertola DR, Takanohashi A, Saito A, Segawa Y, Yokota T, et al. Bi-allelic CSF1R mutations cause skeletal dysplasia of dysosteosclerosis-Pyle disease spectrum and degenerative encephalopathy with brain malformation. Am J Hum Genet. 2019;104(5):925-35. https://doi.org/10.1016/j.ajhg.2019.03.004. First identification of homozygous recessive CSF1R mutations in humans and their effect on bone.
• Oosterhof N, Chang IJ, Karimiani EG, Kuil LE, Jensen DM, Daza R, et al. Homozygous mutations in CSF1R cause a pediatric-onset leukoencephalopathy and can result in congenital absence of microglia. Am J Hum Genet. 2019;104(5):936-47. https://doi.org/10.1016/j.ajhg.2019.03.010. First identification of homozygous recessive CSF1R mutations in humans and their effect on bone.
Guo L, Ikegawa S. From HDLS to BANDDOS: fast-expanding phenotypic spectrum of disorders caused by mutations in CSF1R. J Hum Genet. 2021;66(12):1139–44. https://doi.org/10.1038/s10038-021-00942-w.
Sakagami N, Amizuka N, Li M, Takeuchi K, Hoshino M, Nakamura M, Nozawa-Inoue K, Udagawa N, Maeda T. Reduced osteoblastic population and defective mineralization in osteopetrotic (op/op) mice. Micron. 2005;36(7-8):688–95. https://doi.org/10.1016/j.micron.2005.06.008.
Blair HC, Larrouture QC, Li Y, Lin H, Beer-Stoltz D, Liu L, Tuan RS, Robinson LJ, Schlesinger PH, Nelson DJ. Osteoblast differentiation and bone matrix formation in vivo and in vitro. Tissue Eng Part B Rev. 2017;23(3):268–80. https://doi.org/10.1089/ten.TEB.2016.0454.
Wang Y, Szretter KJ, Vermi W, Gilfillan S, Rossini C, Cella M, Barrow AD, Diamond MS, Colonna M. IL-34 is a tissue-restricted ligand of CSF1R required for the development of Langerhans cells and microglia. Nat Immunol. 2012;13(8):753–60. https://doi.org/10.1038/ni.2360.
Baghdadi M, Ishikawa K, Nakanishi S, Murata T, Umeyama Y, Kobayashi T, Kameda Y, Endo H, Wada H, Bogen B, Yamamoto S, Yamaguchi K, Kasahara I, Iwasaki H, Takahata M, Ibata M, Takahashi S, Goto H, Teshima T, Seino KI. A role for IL-34 in osteolytic disease of multiple myeloma. Blood Adv. 2019;3(4):541–51. https://doi.org/10.1182/bloodadvances.2018020008.
Bennett FC, Bennett ML, Yaqoob F, Mulinyawe SB, Grant GA, Hayden Gephart M, Plowey ED, Barres BA. A combination of ontogeny and CNS environment establishes microglial identity. Neuron. 2018;98(6):1170–83 e8. https://doi.org/10.1016/j.neuron.2018.05.014.
Hume DA, Irvine KM, Pridans C. The mononuclear phagocyte system: the relationship between monocytes and macrophages. Trends Immunol. 2019;40(2):98–112. https://doi.org/10.1016/j.it.2018.11.007.
Arnett TR, Lindsay R, Kilb JM, Moonga BS, Spowage M, Dempster DW. Selective toxic effects of tamoxifen on osteoclasts: comparison with the effects of oestrogen. J Endocrinol. 1996;149(3):503–8. https://doi.org/10.1677/joe.0.1490503.
Chiu WS, McManus JF, Notini AJ, Cassady AI, Zajac JD, Davey RA. Transgenic mice that express Cre recombinase in osteoclasts. Genesis. 2004;39(3):178–85. https://doi.org/10.1002/gene.20041.
• Xie Z, McGrath C, Sankaran J, Styner M, Little-Letsinger S, Dudakovic A, et al. Low-dose tamoxifen induces significant bone formation in mice. JBMR Plus. 2021;5(3):e10450. https://doi.org/10.1002/jbm4.10450. Interesting study of the complex effects of tamoxifen on bone turnover and OCL function in mice.
Hughes DE, Wright KR, Uy HL, Sasaki A, Yoneda T, Roodman GD, et al. Bisphosphonates promote apoptosis in murine osteoclasts in vitro and in vivo. J Bone Miner Res. 1995;10(10):1478–87. https://doi.org/10.1002/jbmr.5650101008.
• McDonald MM, Khoo WH, Ng PY, Xiao Y, Zamerli J, Thatcher P, et al. Osteoclasts recycle via osteomorphs during RANKL-stimulated bone resorption. Cell. 184(5):1330-1347.e13. https://doi.org/10.1016/j.cell.2021.02.002. Identification of a novel mechanism of osteoclast turnover via fission to produce osteomorphs.
• Anastasilakis AD, Makras P, Yavropoulou MP, Tabacco G, Naciu AM, Palermo A. Denosumab discontinuation and the rebound phenomenon: a narrative review. J Clin Med. 2021;10(1). https://doi.org/10.3390/jcm10010152. Description of the phenomenon of rebound osteoporosis following discontinuation of anti-RANKL therapy.
Stanley ER, Chitu V. CSF-1 receptor signaling in myeloid cells. Cold Spring Harb Perspect Biol. 2014;6(6). https://doi.org/10.1101/cshperspect.a021857.
Bartocci A, Mastrogiannis DS, Migliorati G, Stockert RJ, Wolkoff AW, Stanley ER. Macrophages specifically regulate the concentration of their own growth factor in the circulation. Proc Natl Acad Sci U S A. 1987;84(17):6179–83. https://doi.org/10.1073/pnas.84.17.6179.
MacDonald KP, Palmer JS, Cronau S, Seppanen E, Olver S, Raffelt NC, et al. An antibody against the colony-stimulating factor 1 receptor depletes the resident subset of monocytes and tissue- and tumor-associated macrophages but does not inhibit inflammation. Blood. 2010;116(19):3955–63. https://doi.org/10.1182/blood-2010-02-266296.
Papadopoulos KP, Gluck L, Martin LP, Olszanski AJ, Tolcher AW, Ngarmchamnanrith G, Rasmussen E, Amore BM, Nagorsen D, Hill JS, Stephenson J Jr. First-in-human study of AMG 820, a monoclonal anti-colony-stimulating factor 1 receptor antibody, in patients with advanced solid tumors. Clin Cancer Res. 2017;23(19):5703–10. https://doi.org/10.1158/1078-0432.CCR-16-3261.
Stacey KJ, Fowles LF, Colman MS, Ostrowski MC, Hume DA. Regulation of urokinase-type plasminogen activator gene transcription by macrophage colony-stimulating factor. Mol Cell Biol. 1995;15(6):3430–41. https://doi.org/10.1128/MCB.15.6.3430.
Amano H, Hofstetter W, Cecchini MG, Fleisch H, Felix R. Downregulation of colony-stimulating factor-1 (CSF-1) binding by CSF-1 in isolated osteoclasts. Calcif Tissue Int. 1995;57(5):367–70. https://doi.org/10.1007/BF00302072.
Sester DP, Beasley SJ, Sweet MJ, Fowles LF, Cronau SL, Stacey KJ, et al. Bacterial/CpG DNA down-modulates colony stimulating factor-1 receptor surface expression on murine bone marrow-derived macrophages with concomitant growth arrest and factor-independent survival. J Immunol. 1999;163(12):6541–50.
Guilliams M, Thierry GR, Bonnardel J, Bajenoff M. Establishment and maintenance of the macrophage niche. Immunity. 2020;52(3):434–51. https://doi.org/10.1016/j.immuni.2020.02.015.
Cenci S, Weitzmann MN, Gentile MA, Aisa MC, Pacifici R. M-CSF neutralization and egr-1 deficiency prevent ovariectomy-induced bone loss. J Clin Invest. 2000;105(9):1279–87. https://doi.org/10.1172/JCI8672.
Kaur S, Raggatt LJ, Batoon L, Hume DA, Levesque JP, Pettit AR. Role of bone marrow macrophages in controlling homeostasis and repair in bone and bone marrow niches. Semin Cell Dev Biol. 2017;61:12–21. https://doi.org/10.1016/j.semcdb.2016.08.009.
Symons AL, MacKay CA, Leong K, Hume DA, Waters MJ, Marks SC Jr. Decreased growth hormone receptor expression in long bones from toothless (osteopetrotic) rats and restoration by treatment with colony-stimulating factor-1. Growth Factors. 1996;13(1-2):1–10. https://doi.org/10.3109/08977199609034562.
Felix R, Cecchini MG, Fleisch H. Macrophage colony stimulating factor restores in vivo bone resorption in the op/op osteopetrotic mouse. Endocrinology. 1990;127(5):2592–4. https://doi.org/10.1210/endo-127-5-2592.
Wiktor-Jedrzejczak W, Urbanowska E, Aukerman SL, Pollard JW, Stanley ER, Ralph P, Ansari AA, Sell KW, Szperl M. Correction by CSF-1 of defects in the osteopetrotic op/op mouse suggests local, developmental, and humoral requirements for this growth factor. Exp Hematol. 1991;19(10):1049–54.
Heil J, Olsavszky V, Busch K, Klapproth K, de la Torre C, Sticht C, Sandorski K, Hoffmann J, Schönhaber H, Zierow J, Winkler M, Schmid CD, Staniczek T, Daniels DE, Frayne J, Metzgeroth G, Nowak D, Schneider S, Neumaier M, et al. Bone marrow sinusoidal endothelium controls terminal erythroid differentiation and reticulocyte maturation. Nat Commun. 2021;12(1):6963. https://doi.org/10.1038/s41467-021-27161-3.
Gow DJ, Sauter KA, Pridans C, Moffat L, Sehgal A, Stutchfield BM, Raza S, Beard PM, Tsai YT, Bainbridge G, Boner PL, Fici G, Garcia-Tapia D, Martin RA, Oliphant T, Shelly JA, Tiwari R, Wilson TL, Smith LB, et al. Characterisation of a novel Fc conjugate of macrophage colony-stimulating factor. Mol Ther. 2014;22(9):1580–92. https://doi.org/10.1038/mt.2014.112.
Stutchfield BM, Antoine DJ, Mackinnon AC, Gow DJ, Bain CC, Hawley CA, Hughes MJ, Francis B, Wojtacha D, Man TY, Dear JW, Devey LR, Mowat AM, Pollard JW, Park BK, Jenkins SJ, Simpson KJ, Hume DA, Wigmore SJ, Forbes SJ. CSF1 restores innate immunity after liver injury in mice and serum levels indicate outcomes of patients with acute liver failure. Gastroenterology. 2015;149(7):1896–909 e14. https://doi.org/10.1053/j.gastro.2015.08.053.
Lloyd SA, Simske SJ, Bogren LK, Olesiak SE, Bateman TA, Ferguson VL. Effects of combined insulin-like growth factor 1 and macrophage colony-stimulating factor on the skeletal properties of mice. In Vivo. 2011;25(3):297–305.
Lloyd SA, Yuan YY, Simske SJ, Riffle SE, Ferguson VL, Bateman TA. Administration of high-dose macrophage colony-stimulating factor increases bone turnover and trabecular volume fraction. J Bone Miner Metab. 2009;27(5):546–54. https://doi.org/10.1007/s00774-009-0071-9.
• Batoon L, Millard SM, Raggatt LJ, Sandrock C, Pickering E, Williams K, et al. Treatment with a long-acting chimeric CSF1 molecule enhances fracture healing of healthy and osteoporotic bones. Biomaterials. 2021;275:120936. https://doi.org/10.1016/j.biomaterials.2021.120936. Key demonstration that CSF1 treatment can promote bone repair and calcification.
Lelios I, Cansever D, Utz SG, Mildenberger W, Stifter SA, Greter M. Emerging roles of IL-34 in health and disease. J Exp Med. 2020;217(3). https://doi.org/10.1084/jem.20190290.
• Ordentlich P. Clinical evaluation of colony-stimulating factor 1 receptor inhibitors. Semin Immunol. 2021;54:101514. https://doi.org/10.1016/j.smim.2021.101514. Comprehensive review of anti-CSF1R therapeutic options and efficacy.
Han J, Chitu V, Stanley ER, Wszolek ZK, Karrenbauer VD, Harris RA. Inhibition of colony stimulating factor-1 receptor (CSF-1R) as a potential therapeutic strategy for neurodegenerative diseases: opportunities and challenges. Cell Mol Life Sci. 2022;79(4):219. https://doi.org/10.1007/s00018-022-04225-1.
Mun SH, Park PSU, Park-Min KH. The M-CSF receptor in osteoclasts and beyond. Exp Mol Med. 2020;52(8):1239–54. https://doi.org/10.1038/s12276-020-0484-z.
Wang XF, Wang YJ, Li TY, Guo JX, Lv F, Li CL, Ge XT. Colony-stimulating factor 1 receptor inhibition prevents against lipopolysaccharide -induced osteoporosis by inhibiting osteoclast formation. Biomed Pharmacother. 2019;115:108916. https://doi.org/10.1016/j.biopha.2019.108916.
He Y, Rhodes SD, Chen S, Wu X, Yuan J, Yang X, Jiang L, Li X, Takahashi N, Xu M, Mohammad KS, Guise TA, Yang FC. c-Fms signaling mediates neurofibromatosis type-1 osteoclast gain-in-functions. PLoS One. 2012;7(11):e46900. https://doi.org/10.1371/journal.pone.0046900.
Conway JG, McDonald B, Parham J, Keith B, Rusnak DW, Shaw E, Jansen M, Lin P, Payne A, Crosby RM, Johnson JH, Frick L, Lin MHJ, Depee S, Tadepalli S, Votta B, James I, Fuller K, Chambers TJ, et al. Inhibition of colony-stimulating-factor-1 signaling in vivo with the orally bioavailable cFMS kinase inhibitor GW2580. Proc Natl Acad Sci U S A. 2005;102(44):16078–83. https://doi.org/10.1073/pnas.0502000102.
Conway JG, Pink H, Bergquist ML, Han B, Depee S, Tadepalli S, Lin P, Crumrine RC, Binz J, Clark RL, Selph JL, Stimpson SA, Hutchins JT, Chamberlain SD, Brodie TA. Effects of the cFMS kinase inhibitor 5-(3-methoxy-4-((4-methoxybenzyl)oxy)benzyl)pyrimidine-2,4-diamine (GW2580) in normal and arthritic rats. J Pharmacol Exp Ther. 2008;326(1):41–50. https://doi.org/10.1124/jpet.107.129429.
El Hajj DI, Gallet M, Mentaverri R, Sevenet N, Brazier M, Kamel S. Imatinib mesylate (Gleevec) enhances mature osteoclast apoptosis and suppresses osteoclast bone resorbing activity. Eur J Pharmacol. 2006;551(1-3):27–33. https://doi.org/10.1016/j.ejphar.2006.09.007.
Vandyke K, Fitter S, Dewar AL, Hughes TP, Zannettino AC. Dysregulation of bone remodeling by imatinib mesylate. Blood. 2010;115(4):766–74. https://doi.org/10.1182/blood-2009-08-237404.
Kitaura H, Zhou P, Kim HJ, Novack DV, Ross FP, Teitelbaum SL. M-CSF mediates TNF-induced inflammatory osteolysis. J Clin Invest. 2005;115(12):3418–27. https://doi.org/10.1172/JCI26132.
Martinez-Martinez A, Munoz-Islas E, Ramirez-Rosas MB, Acosta-Gonzalez RI, Torres-Rodriguez HF, Jimenez-Andrade JM. Blockade of the colony-stimulating factor-1 receptor reverses bone loss in osteoporosis mouse models. Pharmacol Rep. 2020;72(6):1614–26. https://doi.org/10.1007/s43440-020-00091-5.
Lin W, Xu D, Austin CD, Caplazi P, Senger K, Sun Y, Jeet S, Young J, Delarosa D, Suto E, Huang Z, Zhang J, Yan D, Corzo C, Barck K, Rajan S, Looney C, Gandham V, Lesch J, et al. Function of CSF1 and IL34 in macrophage homeostasis, inflammation, and cancer. Front Immunol. 2019;10:2019. https://doi.org/10.3389/fimmu.2019.02019.
Wei S, Lightwood D, Ladyman H, Cross S, Neale H, Griffiths M, Adams R, Marshall D, Lawson A, McKnight AJ, Stanley ER. Modulation of CSF-1-regulated post-natal development with anti-CSF-1 antibody. Immunobiology. 2005;210(2-4):109–19. https://doi.org/10.1016/j.imbio.2005.05.005.
Razak AR, Cleary JM, Moreno V, Boyer M, Calvo Aller E, Edenfield W, et al. Safety and efficacy of AMG 820, an anti-colony-stimulating factor 1 receptor antibody, in combination with pembrolizumab in adults with advanced solid tumors. J Immunother Cancer. 2020;8(2). https://doi.org/10.1136/jitc-2020-001006.
• Pognan F, Couttet P, Demin I, Jaitner B, Pang Y, Roubenoff R, et al. Colony-stimulating factor-1 antibody lacnotuzumab in a phase 1 healthy volunteer study and mechanistic investigation of safety outcomes. J Pharmacol Exp Ther. 2019;369(3):428-42. https://doi.org/10.1124/jpet.118.254128. Important trial of anti-CSF1 treatment in non-human primates and healthy volunteers.
Bone HG, Bolognese MA, Yuen CK, Kendler DL, Miller PD, Yang YC, Grazette L, San Martin J, Gallagher JC. Effects of denosumab treatment and discontinuation on bone mineral density and bone turnover markers in postmenopausal women with low bone mass. J Clin Endocrinol Metab. 2011;96(4):972–80. https://doi.org/10.1210/jc.2010-1502.
Bone HG, Bolognese MA, Yuen CK, Kendler DL, Wang H, Liu Y, San Martin J. Effects of denosumab on bone mineral density and bone turnover in postmenopausal women. J Clin Endocrinol Metab. 2008;93(6):2149–57. https://doi.org/10.1210/jc.2007-2814.
Weivoda MM, Chew CK, Monroe DG, Farr JN, Atkinson EJ, Geske JR, Eckhardt B, Thicke B, Ruan M, Tweed AJ, McCready LK, Rizza RA, Matveyenko A, Kassem M, Andersen TL, Vella A, Drake MT, Clarke BL, Oursler MJ, Khosla S. Identification of osteoclast-osteoblast coupling factors in humans reveals links between bone and energy metabolism. Nat Commun. 2020;11(1):87. https://doi.org/10.1038/s41467-019-14003-6.
Acknowledgements
We acknowledge the core support from the Mater Foundation for research in our laboratory.
Funding
Open Access funding enabled and organized by CAUL and its Member Institutions. DAH is supported by an NHMRC Investigator Grant (GNT2009750).
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of Interest
The authors have no existing conflicts of interest.
Human and Animal Rights and Informed Consent
This article does not contain any studies with human or animal subjects performed by any of the authors.
Additional information
Publisher’s Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
This article is part of the Topical Collection on Osteoimmunology
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if changes were made. The images or other third party material in this article are included in the article's Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article's Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
Hume, D.A., Batoon, L., Sehgal, A. et al. CSF1R as a Therapeutic Target in Bone Diseases: Obvious but Not so Simple. Curr Osteoporos Rep 20, 516–531 (2022). https://doi.org/10.1007/s11914-022-00757-4
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11914-022-00757-4