Abstract
Purpose of Review
Interstitial lung disease (ILD) is a common manifestation of systemic sclerosis (SSc). We explore the importance of early detection, monitoring, and management of SSc-ILD.
Recent Findings
All patients with SSc are at risk of ILD and should be screened for ILD at diagnosis using a high-resolution computed tomography (HRCT) scan. Some patients with SSc-ILD develop a progressive phenotype characterized by worsening fibrosis on HRCT, decline in lung function, and early mortality. To evaluate progression and inform treatment decisions, regular monitoring is important and should include pulmonary function testing, evaluation of symptoms and quality of life, and, where indicated, repeat HRCT. Multidisciplinary discussion enables comprehensive evaluation of the available information and its implications for management. The first-line treatment for SSc-ILD is usually immunosuppression. The antifibrotic drug nintedanib has been approved for slowing lung function decline in patients with SSc-ILD.
Summary
Optimal management of patients with SSc-ILD requires a multidisciplinary and patient-centered approach.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Systemic sclerosis (SSc) is a rare multifaceted autoimmune disease characterized by progressive fibrosis of the skin and internal organs, immune dysregulation, and vasculopathy [1]. Interstitial lung disease (ILD) is a common manifestation of SSc and contributes significantly to the overall morbidity and mortality of patients with SSc. The pathogenesis of SSc-ILD involves multiple components including interstitial inflammation and fibrosis [2]. In some patients, SSc-ILD is progressive, with poor outcomes including premature death [3]. In this article, we explore the importance of early detection, monitoring, and management of ILD in patients with SSc.
Detection of SSc-ILD
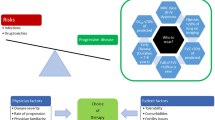
SSc-ILD is classified as pulmonary fibrosis seen on high-resolution computed tomography (HRCT) or chest radiography, with a basilar predominance, or the occurrence of “Velcro” crackles on chest auscultation, not due to another cause such as congestive heart failure [1]. The estimated prevalence of ILD in patients with SSc varies widely depending on the population studied and the methodology used. In a Canadian registry, 64% of 289 patients with SSc who had HRCT scans were diagnosed with ILD, compared with 22% of 1168 patients who had a chest X-ray [4]. In a Norwegian population-based cohort of 650 patients with SSc, ILD was evident on HRCT in half the patients [3]. Risk factors for the development of ILD in patients with SSc include male sex, diffuse cutaneous SSc (dcSSc), African-American race, and the presence of certain autoantibodies such as anti-topoisomerase I (ATA), anti-Th/To, and anti-U3 RNP [5, 6]. The risk of developing ILD is greatest in the first few years after diagnosis of SSc [7] (Fig. 1). However, it is important to be aware that patients with SSc with no established risk factors are still at risk of developing ILD. A recent analysis of data from 826 patients with SSc-ILD in the EUSTAR database found that only 21% of patients had a disease duration < 3 years, 50% had dcSSc, and 53% were ATA-positive [8••]. This highlights the importance of not assuming that only patients with early dcSSc are at risk of SSc-ILD.
Early development of lung function impairment in patients with SSc in the EUSTAR database (adapted with permission from [7])
While a chronic dry cough and dyspnea are common symptoms in patients with SSc-ILD, many patients remain asymptomatic [9]. Furthermore, patients with SSc with evidence of ILD on HRCT may have normal pulmonary function tests (PFTs) [10, 11]. In a retrospective analysis of 188 patients with SSc-ILD on HRCT, 31% of patients had FVC ≥ 80% predicted [11]. Thus relying on symptoms, or impaired lung function to drive screening for SSc-ILD would result in missed diagnoses. In Delphi consensus exercises, expert groups in the USA and in Europe agreed that all patients diagnosed with SSc should undergo a HRCT scan of the chest at baseline to screen for ILD [12, 13••].
HRCT scans from a patient without interstitial lung abnormalities and a patient with early fibrotic lung disease are shown in Figs. 2a and b. In addition to identifying the presence of ILD, HRCT enables evaluation of the extent and pattern of fibrosis. This is important, as a greater extent of fibrotic ILD on HRCT is associated with poorer outcomes [3, 14, 15], as are specific imaging features, such as traction bronchiectasis and honeycombing [16]. Establishing an imaging pattern in connective tissue disease-related ILDs is difficult and subject to high inter-observer variability [17, 18]. The most common imaging pattern observed on HRCT in patients with SSc-ILD is non-specific interstitial pneumonia (NSIP), characterized by bilateral ground-glass opacities, reticulation and traction bronchiectasis that is most prominent in the lower lobes (Fig. 2c); however, some patients with SSc-ILD show a usual interstitial pneumonia (UIP) pattern (Fig. 2d) [19]. In addition, a number of patients do not fulfill the definition for any specific pattern. It is important to note that the imaging classification paradigm is continuously evolving, and it is more important to recognize the presence of new or evolving ILD than the specific fibrotic pattern. Table 1 reviews the standard and non-standard lexicons used in the setting of fibrosis in thoracic radiology. Although some terms are more specific to fibrotic ILD than others, given the heterogeneity in experience and reporting standards among radiologists, identification of any of these words should prompt the referring clinician to question the presence of ILD.
Examples of imaging patterns seen in patients with SSc. a Axial HRCT image from the normal lung bases of a 55-year-old woman undergoing staging for pancreatic cancer. The only visible structures are bronchovascular bundles and pleural reflections; there are no interstitial lung abnormalities. b Early fibrotic ILD in a 47-year-old woman with SSc. There are many crossing lines (reticulations), indicating early fibrotic lung disease. It is difficult to apply a specific pattern at this early stage. c An NSIP pattern in a 52-year-old woman with SSc. The pattern is characterized by ground-glass opacities, traction bronchiectasis, and subpleural sparing. d A UIP pattern of fibrotic ILD in a 59-year-old man with SSc. There are extensive reticulations and honeycombing throughout the basilar and peripheral lungs
Progression and Monitoring of SSc-ILD
SSc-ILD has a variable natural history [20]. Some patients have relatively stable disease for a prolonged period, while others develop a progressive phenotype characterized by worsening fibrosis on HRCT, progressive decline in lung function, worsening dyspnea, and an increase in mortality [3]. Risk factors for the progression of SSc-ILD include advanced age, low baseline FVC and/or DLco, a greater extent of ILD on HRCT, the presence of ATA, and the absence of anti-centromere antibodies [6, 14, 15, 21, 22].
Patients with SSc-ILD should undergo regular PFTs to evaluate lung function and monitor disease severity and rapidity of progression (Fig. 3) [13••]. In an analysis of 535 patients with SSc-ILD in the EUSTAR database, over a mean follow-up of 5 years, 63% had stable or improved FVC (defined as a decline in FVC < 5% predicted or an increase in FVC) while 23% had a decline in FVC of > 10% predicted (Fig. 4) [8••]. It is important to note that recent stability in FVC does not indicate that FVC will remain stable over the following year [8••]. Among patients with SSc-ILD in the EUSTAR database who had stable FVC (defined as a decline or improvement of < 5% predicted) over a 12-month period, approximately 30% had a decline in FVC of ≥ 5% predicted over the following 12 months [8••].
Proposed algorithm for the detection, monitoring, and management of patients with SSc-ILD (reproduced with permission from [13••])
Change in FVC over a mean follow-up of 5 years in patients with SSc-ILD in the EUSTAR database [8••]
As well as PFTs, monitoring of patients with SSc-ILD should include evaluation of symptoms, quality of life, exercise-induced oxygen desaturation, and repeat HRCT where indicated (e.g., if there has been a worsening of PFTs or symptoms) (Fig. 3) [13••]. Protocols for monitoring patients with SSc-ILD vary, but most experts agree that PFTs and respiratory symptoms should be assessed at least every 6–12 months and screening for pulmonary hypertension, a common comorbidity of SSc-ILD [23], should be performed annually via echocardiogram. Rheumatologists are advised to refer patients with SSc-ILD to an expert ILD center, or to establish a relationship with such a center. These centers can monitor disease progression closely and adopt a multidisciplinary approach to ensure re-evaluation of a patient’s therapeutic regimen.
While there is no well-established definition for progression of SSc-ILD, experts have proposed that a decline in FVC of ≥ 10% of the predicted value, or a decline in FVC of 5–9% of the predicted value accompanied by a decline in DLco of ≥ 15% of the predicted value, may represent clinically meaningful progression [24]. When interpreting the results of PFTs, it is important to consider whether other factors may be contributing to an observed decline, e.g., a worsening of pulmonary hypertension or a concomitant respiratory infection. The same applies to an observed worsening in dyspnea, cough, or quality of life: a thorough investigation is needed to ascertain whether such a worsening is due to progression of ILD rather than to the onset or worsening of other manifestations of SSc or comorbidities. “Small” deteriorations in PFTs should not be ignored as these may accumulate over time and are associated with an increased risk of mortality [3, 22, 25]. Among 228 patients with SSc-ILD in a Norwegian cohort, after patients were stratified by change in FVC over a mean follow-up of 6.2 years, the 10-year survival rate was 59% in patients with a decline in FVC of ≥ 5% predicted compared to 78% in patients with a decline or an increase < 5% predicted [3].
Furthermore, an increase in the extent of fibrotic abnormalities on HRCT indicates disease progression. A seminal study at a UK center found that extensive ILD, defined as > 30% extent of fibrosis on HRCT (based on a mean score of five sections, each estimated to the nearest 5%) or an extent of fibrosis on HRCT of 10–30% with an FVC < 70% predicted, was strongly predictive of mortality (hazard ratio 3.46) [14]. While most studies have focused on analyses of thresholds, any increase in the extent of fibrotic abnormalities on HRCT has prognostic implications [3, 26]. Automated post-processing software is available to quantify the extent of fibrotic changes on CT [27] but is rarely used in a routine clinical environment. Data are mixed on the prognostic value of specific imaging patterns in patients with SSc-ILD, with some studies showing no prognostic value of a UIP pattern compared with NSIP [28] and others showing worse outcomes in patients with a UIP pattern on HRCT [29].
Multidisciplinary discussion involving, at minimum, a rheumatologist, pulmonologist, and radiologist enables a comprehensive evaluation of the information obtained during monitoring and its implications for the care of the patient. Multidisciplinary discussion may take place virtually or at face-to-face meetings. Input from all parties is valuable: the rheumatologist can provide the most complete picture of the patient’s overall health status, the pulmonologist can guide the interpretation of PFTs, and the radiologist can advise on changes observed on HRCT that may have prognostic relevance.
Management of SSc-ILD
There is no established algorithm for when patients with SSc-ILD should receive pharmacological therapy or which treatments they should receive. However, there is an increasing recognition of the importance of early treatment of SSc-ILD to improve patient outcomes, given that lung function lost to fibrosis cannot be recovered and there is a strong association between decline in lung function and mortality. The information gathered through monitoring should be discussed from the perspective of whether a change or escalation of therapy is required. Decisions about treatment should be based on assessment of the patient’s overall health status, ascertainment of ILD severity and progression, risk factors for ILD progression, and consideration of the patient’s preferences [13••, 30].
In most patients, the first-line treatment for SSc-ILD is immunosuppression, and many patients with SSc-ILD will in any case be taking an immunomodulatory therapy to manage other manifestations of their SSc, such as skin fibrosis [31]. The most commonly used immunosuppressant therapy in patients with SSc-ILD is mycophenolate, which is better tolerated than cyclophosphamide and non-inferior to cyclophosphamide in its effects on lung function [32]. In Scleroderma Lung Study I (SLS I), performed in 158 patients with SSc-ILD, the mean decline in FVC % predicted after 1 year was 1.0% in patients treated with oral cyclophosphamide compared with 2.6% in the placebo group [33]. Later, in SLS II, conducted in 142 patients, mean improvements in FVC % predicted were similar between patients treated with mycophenolate for 2 years and patients treated with oral cyclophosphamide for 1 year followed by placebo for 1 year (2.2% and 2.9%, respectively) [32]. Mycophenolate is associated with a risk of gastrointestinal intolerance and infections but can be administered for prolonged periods. The side effects of cyclophosphamide limit its long-term use [34].
Tocilizumab, an interleukin-6 (IL-6) receptor antagonist, was investigated as a treatment for SSc in two placebo-controlled trials in patients with early inflammatory dcSSc: the phase II faSScinate trial [35] and the phase III focuSSced trial [36]. The primary endpoint, change in modified Rodnan skin score (mRSS), was not met in either of these trials, but secondary endpoints suggested a beneficial effect of tocilizumab on FVC. In the focuSSced trial, among 210 patients with SSc, the mean change from baseline in FVC % predicted at week 48 was − 0.4% in the tocilizumab group compared with − 4.6% in the placebo group [36]. In the subgroup of 136 patients with SSc-ILD at baseline (defined as ground-glass opacification and/or fibrosis with a basal predominance on HRCT), the mean change from baseline in FVC % predicted at week 48 was − 0.1% in patients treated with tocilizumab compared with − 6.3% in the placebo group [37••]. Based on these findings, tocilizumab has been approved by the US Food and Drug Administration for slowing the decline in lung function in patients with SSc-ILD. Adverse events associated with tocilizumab include infections, liver enzyme elevations, and injection site reactions [38].
Open-label and observational studies suggest that rituximab, a monoclonal anti-CD20 antibody that depletes B-cells, may have a beneficial effect on lung function in patient with SSc-ILD [39], but evidence from randomized, double-blind, controlled trials is lacking. The results of the RECITAL (NCT01862926) and EvER-ILD (NCT02990286) trials will illuminate the potential role of rituximab in patients with SSc-ILD.
Nintedanib is an antifibrotic therapy that inhibits processes fundamental to the progression of lung fibrosis [40]. Nintedanib has been approved by the FDA and other regulatory bodies for reducing the rate of decline in FVC in patients with SSc-ILD, as well as for the treatment of idiopathic pulmonary fibrosis and other progressive fibrosing ILDs. The SENSCIS trial enrolled 576 patients with SSc-ILD and an extent of fibrotic ILD on HRCT (based on assessment of the whole lung) of ≥ 10%. The inclusion criteria did not require evidence of recent or ongoing progression of SSc-ILD. The rate of decline in FVC over 52 weeks was − 52.4 mL/year in the nintedanib group and − 93.3 mL/year in the placebo group, corresponding to a relative reduction of 44%. The rate of decline in FVC % predicted over 52 weeks was − 1.4%/year in the nintedanib group and − 2.6%/year in the placebo group. The side effects of nintedanib were mainly gastrointestinal and manageable for most patients through symptom management and dose adjustment [41••, 42]. Importantly, nintedanib was effective at reducing the rate of decline in FVC both when used as monotherapy and when used as add-on to a stable dose of mycophenolate [43], and had a consistent effect across subgroups of patients with SSc-ILD, including those with limited versus diffuse cutaneous SSc and ATA-negative versus ATA-positive patients [41••, 44].
Autologous hemopoietic stem cell transplantation (HSCT) is a therapeutic option for select patients with severe progressive SSc-ILD and has been recommended in treatment guidelines [45, 46]. HSCT is associated with marked improvements in disease progression and event-free survival, but also with significant short-term mortality and it should only be performed at expert centers after careful consideration of the risk:benefit for the individual patient.
Lung transplantation is available to a minority of patients with SSc-ILD who have not responded to treatment and do not have contraindications. In a retrospective study of outcomes in 90 patients with SSc at 14 European centers, survival rates 1, 3, and 5 years after transplant were 81%, 68%, and 61% [47]. Potential candidates for lung transplant should be referred to an expert center for evaluation as soon as possible.
Optimal management of patients with SSc-ILD requires a multifaceted approach, including management of symptoms, extra-pulmonary manifestations of SSc and comorbidities, and the appropriate use of non-pharmacological therapies such as pulmonary rehabilitation [48]. Supplemental oxygen should be considered for patients with severe hypoxemia [49]. Patient education and support should be regarded as an integral part of patient care [50]. Patient groups, such as those run by the Scleroderma Foundation (www.scleroderma.org), provide valuable support to communities of patients and their caregivers.
Conclusions
ILD is a common manifestation of SSc that may become fibrosing and progressive, resulting in loss of lung function and premature death. All patients diagnosed with SSc should be screened for ILD at baseline using an HRCT scan. Regular monitoring of patients with SSc-ILD is important to evaluate progression and inform treatment decisions. The mainstay of therapy for SSc-ILD is immunosuppression. The antifibrotic drug nintedanib has demonstrated efficacy in reducing the rate of decline in FVC when used as monotherapy and as add-on to mycophenolate. A multidisciplinary approach to the assessment, monitoring, and management of SSc-ILD provides the best care for patients.
Change history
25 August 2022
A Correction to this paper has been published: https://doi.org/10.1007/s11926-022-01085-3
References
Papers of particular interest, published recently, have been highlighted as: •• Of major importance
van den Hoogen F, Khanna D, Fransen J, Johnson SR, Baron M, Tyndall A, et al. 2013 classification criteria for systemic sclerosis: an American College of Rheumatology/European League Against Rheumatism collaborative initiative. Arthritis Rheum. 2013;65:2737–47.
Nihtyanova SI, Denton CP. Pathogenesis of systemic sclerosis associated interstitial lung disease. J Scleroderma Relat Disord. 2020;5:6–16.
Hoffmann-Vold AM, Fretheim H, Halse AK, Seip M, Bitter H, Wallenius M, et al. Tracking impact of interstitial lung disease in systemic sclerosis in a complete nationwide cohort. Am J Respir Crit Care Med. 2019;200:1258–66.
Steele R, Hudson M, Lo E, Baron M, Canadian Scleroderma Research Group. Clinical decision rule to predict the presence of interstitial lung disease in systemic sclerosis. Arthritis Care Res (Hoboken). 2012;64:519–24.
Steen VD. Autoantibodies in systemic sclerosis. Semin Arthritis Rheum. 2005;35:35–42.
Nihtyanova SI, Schreiber BE, Ong VH, Rosenberg D, Moinzadeh P, Coghlan JG, et al. Prediction of pulmonary complications and long-term survival in systemic sclerosis. Arthritis Rheumatol. 2014;66:1625–35.
Jaeger VK, Wirz EG, Allanore Y, Rossbach P, Riemekasten G, Hachulla E, et al. Incidences and risk factors of organ manifestations in the early course of systemic sclerosis: a longitudinal EUSTAR study. PLoS One. 2016;11:e0163894.
•• Hoffmann-Vold AM, Allanore Y, Alves M, Brunborg C, Airó P, Ananieva LP, et al. Progressive interstitial lung disease in patients with systemic sclerosis-associated interstitial lung disease in the EUSTAR database. Ann Rheum Dis 2021;80:219–227. This analysis of the EUSTAR database showed that patients with SSc who have no established risk factors for ILD are still at risk of developing progressive ILD.
Hu S, Hou Y, Wang Q, Li M, Xu D, Zeng X. Prognostic profile of systemic sclerosis: analysis of the clinical EUSTAR cohort in China. Arthritis Res Ther. 2018;20:235.
Suliman YA, Dobrota R, Huscher D, Nguyen-Kim TDL, Maurer B, Jordan S, et al. Brief report: pulmonary function tests: high rate of false-negative results in the early detection and screening of scleroderma-related interstitial lung disease. Arthritis Rheumatol. 2015;67:3256–61.
Showalter K, Hoffmann A, Rouleau G, Aaby D, Lee J, Richardson C, et al. Performance of forced vital capacity and lung diffusion cutpoints for associated radiographic interstitial lung disease in systemic sclerosis. J Rheumatol. 2018;45:1572–6.
Rahaghi FF, Strek ME, Southern BD, Saggar R, Hsu VM, Mayes MD, et al. Expert consensus on the screening, treatment, and management of patients with systemic sclerosis-associated interstitial lung disease (SSc-ILD), and the potential future role of anti-fibrotic drugs in a treatment paradigm for SSc-ILD: a Delphi consensus study. Poster presented at the American Thoracic Society International Conference, Dallas, TX, USA; May 17–22, 2019. Available at: https://www.usscicomms.com/respiratory/ats2019/rahaghi
•• Hoffmann-Vold AM, Maher TM, Philpot EE, Ashrafzadeh A, Barake R, Barsotti S, et al. The identification and management of interstitial lung disease in systemic sclerosis: evidence-based European consensus statements. Lancet Rheumatol 2020;2:E71–83. This article summarizes the findings of a Delphi consensus panel, including a suggested algorithm for the detection, monitoring, and management of SSc-ILD.
Goh NS, Desai SR, Veeraraghavan S, Hansell DM, Copley SJ, Maher TM, et al. Interstitial lung disease in systemic sclerosis: a simple staging system. Am J Respir Crit Care Med. 2008;177:1248–54.
Moore OA, Goh N, Corte T, Rouse H, Hennessy O, Thakkar V, et al. Extent of disease on high-resolution computed tomography lung is a predictor of decline and mortality in systemic sclerosis-related interstitial lung disease. Rheumatology. 2013;52:155–60.
Walsh SL, Sverzellati N, Devaraj A, Keir GJ, Wells AU, Hansell DM. Connective tissue disease related fibrotic lung disease: high resolution computed tomographic and pulmonary function indices as prognostic determinants. Thorax. 2014;69:216–22.
Walsh SL, Calandriello L, Sverzellati N, Wells AU, Hansell DM, UIP observer consort. Interobserver agreement for the ATS/ERS/JRS/ALAT criteria for a UIP pattern on CT. Thorax. 2016;71:45–51.
Widell J, Lidén M. Interobserver variability in high-resolution CT of the lungs. Eur J Radiol Open. 2020;7:100228.
Desai SR, Veeraraghavan S, Hansell DM, Nikolakopolou A, Goh NSL, Nicholson AG, et al. CT features of lung disease in patients with systemic sclerosis: comparison with idiopathic pulmonary fibrosis and nonspecific interstitial pneumonia. Radiology. 2004;232:560–7.
Vonk MC, Walker UA, Volkmann ER, Kreuter M, Johnson SR, Allanore Y. Natural variability in the disease course of SSc-ILD: implications for treatment. Eur Respir Rev. 2021;30:200340.
Winstone TA, Assayag D, Wilcox PG, Dunne JV, Hague CJ, Leipsic J, et al. Predictors of mortality and progression in scleroderma-associated interstitial lung disease: a systematic review. Chest. 2014;146:422–36.
Goh NS, Hoyles RK, Denton CP, Hansell DM, Renzoni EA, Maher TM, et al. Short-term pulmonary function trends are predictive of mortality in interstitial lung disease associated with systemic sclerosis. Arthritis Rheumatol. 2017;69:1670–8.
Young A, Vummidi D, Visovatti S, Homer K, Wilhalme H, White ES, et al. Prevalence, treatment, and outcomes of coexistent pulmonary hypertension and interstitial lung disease in systemic sclerosis. Arthritis Rheumatol. 2019;71:1339–49.
Khanna D, Mittoo S, Aggarwal R, Proudman SM, Dalbeth N, Matteson EL, et al. Connective tissue disease-associated interstitial lung diseases (CTD-ILD) – report from OMERACT CTD-ILD Working Group. J Rheumatol. 2015;42:2168–71.
Volkmann ER, Tashkin DP, Sim M, Li N, Goldmuntz E, Keyes-Elstein L, et al. Short-term progression of interstitial lung disease in systemic sclerosis predicts long-term survival in two independent clinical trial cohorts. Ann Rheum Dis. 2019;78:122–30.
Jhajj A, Gill HP, Hague CJ, Murphy D, Elicker B, Soon J, et al. Pulmonary physiology is poorly associated with radiological extent of disease in systemic sclerosis-associated interstitial lung disease. Eur Respir J. 2019;53:1802182.
Ley-Zaporozhan J, Giannakis A, Norajitra T, Weinheimer O, Kehler L, Dinkel J, et al. Fully automated segmentation of pulmonary fibrosis using different software tools. Respiration 2021:1–8.
Takei R, Arita M, Kumagai S, Ito Y, Tokioka F, Koyama T, et al. Radiographic fibrosis score predicts survival in systemic sclerosis-associated interstitial lung disease. Respirology. 2018;23:385–91.
Mango RL, Matteson EL, Crowson CS, Ryu JH, Makol A. Assessing mortality models in systemic sclerosis-related interstitial lung disease. Lung. 2018;196:409–16.
Roofeh D, Lescoat A, Khanna D. Treatment for systemic sclerosis-associated interstitial lung disease. Curr Opin Rheumatol. 2021;33:240–8.
Li Q, Wallace L, Patnaik P, Alves M, Gahlemann M, Kohlbrenner V, et al. Disease frequency, patient characteristics, comorbidity outcomes and immunosuppressive therapy in systemic sclerosis and systemic sclerosis-associated interstitial lung disease: a US cohort study. Rheumatology (Oxford). 2021;60:1915–25.
Tashkin DP, Roth MD, Clements PJ, Furst DE, Khanna D, Kleerup EC, et al. Mycophenolate mofetil versus oral cyclophosphamide in scleroderma-related interstitial lung disease (SLSII): a randomised controlled, double-blind, parallel group trial. Lancet Respir Med. 2016;4:708–19.
Tashkin DP, Elashoff R, Clements PJ, Goldin J, Roth MD, Furst DE, et al. Cyclophosphamide versus placebo in scleroderma lung disease. N Engl J Med. 2006;354:2655–66.
Barnes H, Holland AE, Westall GP, Goh NS, Glaspole IN. Cyclophosphamide for connective tissue disease-associated interstitial lung disease. Cochrane Database Syst Rev. 2018;1:CD010908.
Khanna D, Denton CP, Jahreis A, et al. Safety and efficacy of subcutaneous tocilizumab in adults with systemic sclerosis (faSScinate): a phase 2, randomised, controlled trial. Lancet. 2016;387:2630–40.
Khanna D, Lin CJF, Furst DE, Goldin J, Kim G, Kuwana M, et al. Tocilizumab in systemic sclerosis: a randomised, double-blind, placebo-controlled, phase 3 trial. Lancet Respir Med. 2020;8:963–74.
•• Roofeh D, Lin CJF, Goldin J, Kim GH, Furst DE, Denton CP, et al. Tocilizumab prevents progression of early systemic sclerosis-associated interstitial lung disease. Arthritis Rheumatol 2021;73:1301–1310. The results of a post hoc analysis of the subgroup of patients with SSc-ILD in the focuSSced trial showed that lung function was preserved over 48 weeks in patients who received tocilizumab versus placebo.
Genentech, Inc. ACTEMRA® (tocilizumab) injection prescribing information. 2021. Available at: https://www.gene.com/download/pdf/actemra_prescribing.pdf
Goswami RP, Ray A, Chatterjee M, Mukherjee A, Sircar G, Ghosh P. Rituximab in the treatment of systemic sclerosis-related interstitial lung disease: a systematic review and meta-analysis. Rheumatology (Oxford) 2020;keaa550.
Wollin L, Distler JHW, Denton CP, Gahlemann M. Rationale for the evaluation of nintedanib as a treatment for systemic sclerosis–associated interstitial lung disease. J Scleroderma Relat Dis. 2019;4:212–8.
•• Distler O, Highland KB, Gahlemann M, Azuma A, Fischer A, Mayes MD, et al. Nintedanib for systemic sclerosis-associated interstitial lung disease. N Engl J Med 2019;380:2518–2528. The results of the SENSCIS trial showed that the rate of decline in FVC over 52 weeks in patients with SSc-ILD was lower in those who received nintedanib versus placebo.
Seibold JR, Maher TM, Highland KB, Assassi S, Azuma A, Hummers LK, et al. Safety and tolerability of nintedanib in patients with systemic sclerosis-associated interstitial lung disease: data from the SENSCIS trial. Ann Rheum Dis. 2020;79:1478–84.
Highland KB, Distler O, Kuwana M, Allanore Y, Assassi S, Azuma A, et al. Efficacy and safety of nintedanib in patients with systemic sclerosis-associated interstitial lung disease treated with mycophenolate: subgroup analysis of the SENSCIS trial. Lancet Respir Med. 2021;9:96–106.
Kuwana M, Allanore Y, Denton CP, Distler JHW, Steen V, Khanna D, et al. Nintedanib in patients with systemic sclerosis-associated interstitial lung disease: subgroup analyses by autoantibody status and modified Rodnan skin thickness score. Arthritis Rheumatol. 2022;74:518–26.
Kowal-Bielecka O, Fransen J, Avouac J, Becker M, Kulak A, Allanore Y, et al. Update of EULAR recommendations for the treatment of systemic sclerosis. Ann Rheum Dis. 2017;76:1327–39.
Sullivan KM, Majhail NS, Bredeson C, Carpenter PA, Chatterjee S, Crofford LJ, et al. Systemic sclerosis as an indication for autologous hematopoietic cell transplantation: position statement from the American Society for Blood and Marrow Transplantation. Biol Blood Marrow Transplant. 2018;24:1961–4.
Pradère P, Tudorache I, Magnusson J, Savale L, Brugiere O, Douvry B, et al. Lung transplantation for scleroderma lung disease: an international, multicenter, observational cohort study. J Heart Lung Transplant. 2018;37:903–11.
Wijsenbeek MS, Holland AE, Swigris JJ, Renzoni EA. Comprehensive supportive care for patients with fibrosing interstitial lung disease. Am J Respir Crit Care Med. 2019;200:152–9.
Jacobs SS, Krishnan JA, Lederer DJ, Ghazipura M, Hossain T, Tan AM, et al. Home oxygen therapy for adults with chronic lung disease. An official American Thoracic Society clinical practice guideline. Am J Respir Crit Care Med. 2020;202:e121–41.
Hoffmann-Vold AM, Allanore Y, Bendstrup E, Bruni C, Distler O, Maher TM, et al. The need for a holistic approach for SSc-ILD - achievements and ambiguity in a devastating disease. Respir Res. 2020;21:197.
Hansell DM, Bankier AA, MacMahon H, McLoud TC, Müller NL, Remy J. Fleischner Society: glossary of terms for thoracic imaging. Radiology. 2008;246:697–722.
Acknowledgements
The authors meet criteria for authorship as recommended by the International Committee of Medical Journal Editors (ICMJE). The authors did not receive payment for development of this article. Writing support was provided by Elizabeth Ng and Wendy Morris of Fleishman-Hillard, London, UK, which was contracted and funded by Boehringer Ingelheim Pharmaceuticals, Inc. Boehringer Ingelheim was given the opportunity to review the article for medical and scientific accuracy as well as intellectual property considerations. The authors wish to thank Dr. Nishant Gupta for reviewing their manuscript.
Funding
Boehringer Ingelheim Pharmaceuticals, Inc has supported the page processing and open-access charges for this article.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of Interest
SAK and SAS have nothing to disclose. JWN reports speaker fees from Boehringer Ingelheim.
Human and Animal Rights and Informed Consent
All reported studies/experiments with human or animal subjects performed by the authors have been previously published and complied with all applicable ethical standards (including the Helsinki declaration and its amendments, institutional/national research committee standards, and international/national/institutional guidelines).
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
The original online version of this article was revised due to a retrospective Open Access order.
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if changes were made. The images or other third party material in this article are included in the article’s Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article’s Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
Khanna, S.A., Nance, J.W. & Suliman, S.A. Detection and Monitoring of Interstitial Lung Disease in Patients with Systemic Sclerosis. Curr Rheumatol Rep 24, 166–173 (2022). https://doi.org/10.1007/s11926-022-01067-5
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11926-022-01067-5