Abstract
Intercostal artery pseudoaneurysm (IAP) represents an extremely rare vascular abnormality developing after an insult to the vascular wall with blood collection within the vascular wall layers and subsequent dilatation. Treatment options, apart from observation, include embolization, endovascular stenting, and surgical correction. We describe the case of a 73-year-old male patient with colonic adenocarcinoma pulmonary metastasis. Repetitive wedge resections and a right lower lobectomy were performed to remove multiple metastatic lesions. At follow-up assessment, the patient reported localized thoracotomy site pain progressing with time and unresponsive to oral analgesics. Chest computed tomography (CT) revealed a pseudoaneurysm of 4-cm diameter of the right 5th intercostal artery. The patient underwent embolization of the lumen and was discharged from the hospital after 24 h. Successive CT re-assessment checks were unremarkable.
Similar content being viewed by others
Explore related subjects
Discover the latest articles, news and stories from top researchers in related subjects.Avoid common mistakes on your manuscript.
Introduction
Pseudoaneurysms of the intercostal arteries (IAP) are extremely rare vascular entities. These develop due to vascular wall insults secondarily to trauma or percutaneous interventions where blood collects within the vascular wall layers [1]. Distinctively different, true aneurysms are full-thickness dilated arteries mostly associated with genetic diseases such as neurofibromatosis type 1. As the intercostal arteries originate from the posterior intercostal arteries stemming out from the aorta (anterior intercostal arteries originate from the internal thoracic arteries), rupture with arterial bleeding is a catastrophic risk. Limited available information exists on their management. In this paper, we present an IAP case developing after repetitive thoracotomies, strongly resembling metastasis and treated by thrombin embolization. Successive follow-up checks were unremarkable.
Case report
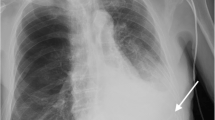
A 73-year-old male patient developed bilateral pulmonary metastases a year after a sigmoidectomy for adenocarcinoma. The right-sided lesions were managed once by video-assisted thoracoscopic surgery (VATS) and twice by posterolateral thoracotomy incisions (5th intercostal space) for repetitive wedge resections, including a lower lobectomy for a centrally located metastasis. These surgical procedures were uneventful. After three postoperative months, he complained of increasing localized thoracotomy site pain of grades 4–5 at visual analogue scale (VAS), non-responding to oral analgesics. The chest X-ray at 3 months showed an abnormal round opacity of the right middle zone. Differential diagnosis included mainly metastasis and infection which necessitated further imaging investigations. Contrast chest computed tomography (CT) identified a 4-cm diameter pseudoaneurysm of the right 5th intercostal artery at the lateral thoracotomy level (Fig. 1). Management options for this lesion included observation with rescanning, surgical aneurysmectomy, or radiologic embolization. After discussion with the patient and considering the bleeding risk and disabling pain, we selected the least invasive treatment option of embolization. The interventional radiologist successfully injected in the lumen 3.5 ml of thrombin under CT guidance obliterating the IAP (Fig. 2). The patient remained 24 h in hospital for observation. Repetitive CT scans prior to discharge and at 6 months were unremarkable.
Discussion
This extremely rare finding is commonly the result of iatrogenic vascular injury, i.e., sternotomy, thoracoscopy, thoracentesis, percutaneous lung biopsy, and even after transaortic transcatheter aortic valve implantation (TAVI) [1, 2]. It is even observed after liver biopsy, biliary procedures, or nephrectomy [1]. Furthermore, non-procedure–related IAPs may present as acute back pain [3]. Symptoms are largely nonspecific, including acute or chronic pain of increasing intensity, dyspnea, or presence of a pulsatile thoracic mass [4]. The non-specific symptomatology may cause confusion to an undiscerning physician leading to misdiagnosis of chronic pain and mistreatment with long-term analgesics. Abnormal chest X-rays may resemble metastasis, leading to a diagnostic contrast CT study. A rupture may lead to life-threatening hemothorax requiring immediate hemorrhage control interventions. Hemomediastinum is rare and was observed only in one patient [3]. The Adamkiewicz artery is the largest anterior radiculomedullary artery which originates from the posterior branch of the intercostal artery. It enters the spinal canal and supplies several segments of the spinal cord. Damage or thrombosis of the vessel may cause infarction of the spinal cord. Therefore, it is crucial to identify the Adamkiewicz artery prior to any intervention to prevent serious potential neurologic complications [5]. The main treatment options for IAPs, as described in case reports, include stent insertion, observation, aneurysmectomy [6], and embolization. Thrombin is a common embolic material for intravascular application. It stimulates thrombus formation by activating fibrinogen with minimal side effects. Alternatively, endovascular coil embolization could be considered an option.
Conclusions
We conclude that IAPs are rare but potentially life-threatening and commonly misdiagnosed and mistreated. A suspicion should exist in postoperative thoracic patients with persisting thoracotomy pain and abnormal imaging, particularly in CT contrast scans. Percutaneous thrombin embolization should be the preferred treatment over surgery.
References
Liu C, Ran R, Li X, Liu G, Wang C, Li J. Massive hemothorax caused by intercostal artery pseudoaneurysm: a case report. J Cardiothorac Surg. 2021;16:156.
Lenders G, Van Schil P, Rodrigus I, Bosmans J. Intercostal artery pseudoaneurysm: a rare complication of transaortic transcatheter aortic valve implantation. Interact Cardiovasc Thorac Surg. 2012;15:550–2.
Junck E, Utarnachitt R. Ruptured intercostal artery pseudoaneurysm: a rare cause of acute back pain. BMJ Case Rep. 2015;2015:bcr2015209788.
Callaway MP, Wilde P, Angelini G. Treatment of a false aneurysm of an intercostal artery using a covered intracoronary stent-graft and a radial artery puncture. Br J Radiol. 2000;73:1317–9.
Agarwal A, Weerakkody Y, Marshall M, Singh T. Intercostal artery pseudoaneurysm with spontaneous resolution in the setting of an artery of Adamkiewicz. J Neurointerv Surg. 2017;9:e31.
Aoki T, Okada A, Tsuchida M, Hayashi J. Ruptured intercostal artery pseudoaneurysm after blunt thoracic trauma. Thorac Cardiovasc Surg. 2003;51:346–7.
Funding
None.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Ethics approval
Not applicable.
Informed consent statement
Informed consent was obtained to publish this report.
Conflict of interest
None declared.
Statement of human and animal rights
Not applicable.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if changes were made. The images or other third party material in this article are included in the article's Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article's Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
Kostopanagiotou, K., Wojtyś, M.E., Kiełbowski, K. et al. Post-thoracotomy intercostal artery pseudoaneurysm manifesting as a chest wall metastasis. Indian J Thorac Cardiovasc Surg 39, 384–386 (2023). https://doi.org/10.1007/s12055-023-01485-9
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12055-023-01485-9