Abstract
The objective of this study is to gain insight into the inherent structure of anxiety and depressive symptoms by combining the strengths of latent factor analysis and network analysis. The sample comprised 743 children and adolescents aged 4–18 years (M = 11.64, SD = 3.66, 61% males) who sought routine care outpatient psychotherapy. Parents or primary caregivers rated anxiety and depressive symptoms of their children on a DSM-5-/ICD-10-based symptom checklist. First, we analyzed the factor structure of the internalizing symptoms using exploratory factor analysis (EFA). Next, we conducted a network analysis and identified central and bridge symptoms that may explain comorbidity between anxiety disorders and depression. We then employed exploratory graph analysis (EGA) as an alternative tool within the framework of network psychometrics to estimate the number of dimensions (i.e., communities within a network). Finally, we tested a model based on these results using confirmatory factor analysis. The results demonstrate a complex interplay between anxiety and depressive symptom domains. Four factors/communities were identified by EFA and EGA, but the item-community allocation differed, and the interpretation of factors/communities was unclear. A clear distinction between these domains could not be supported. However, associations within a domain were stronger than associations between the two domains. We identified pain, suicidal, irritable, and afraid of adults as bridge items between the symptom domains. In conclusion, our findings further advance the general understanding of the frequently reported co-occurrence of anxiety and depressive symptoms and diagnoses in clinical practice. Identifying bridge symptoms may inform intervention practices by targeting specific symptoms that contribute to the maintenance of anxious and depressive behaviors.
Similar content being viewed by others
Explore related subjects
Discover the latest articles, news and stories from top researchers in related subjects.Avoid common mistakes on your manuscript.
Anxiety and depression are common mental disorders in children and adolescents, with worldwide prevalence estimates of 6.5% (95% CI: 4.7–9.1) for anxiety disorders and 2.6% (95% CI: 1.7–3.9) for depressive disorders (Polanczyk et al., 2015). Symptoms of anxiety and depression often overlap in children (Melton et al., 2016). This frequent co-occurrence is associated with greater symptom severity, more complicated treatment, and a more difficult diagnostic assessment, highlighting the need to better understand the associations between the two domains (Melton et al., 2016). In consideration of the clinical significance of comorbid anxiety symptoms in patients with depression, the DSM-5 (American Psychiatric Association [APA], 2013) added the specifier ‘with anxious distress’ to the diagnosis of major depressive disorder (MDD). This specifier should be considered if at least two out of five anxiety symptoms (e.g., difficulties concentrating because of worry, feeling tense, feeling restless) are present for the majority of the depressive episode. A previous study demonstrated that approximately 75% of patients with MDD met the DSM-5 criteria for this specifier (Zimmerman et al., 2019). Compared to patients with MDD who did not meet criteria for the specifier, these patients demonstrated poorer functioning and coping, even after controlling for the presence of any anxiety disorder, thus underlining the additional clinical utility of the ‘with anxious distress’ specifier (Zimmerman et al., 2019). Similarly, in the ICD-11 (World Health Organization [WHO], 2019), the diagnosis ‘mixed anxiety and depression’ can be given if symptoms of both disorders are present with similar intensity, but do not fulfill the diagnostic criteria for either disorder when considered separately.
Several explanations have been provided in the attempt to understand the comorbidity between anxiety and depression (cf. Cummings et al., 2014). One assumption is that comorbidity is an artifact of an imperfect diagnostic classification system, by which comorbidity results from overlapping symptom criteria (Cummings et al., 2014). However, in a meta-analysis of general population studies, Angold et al. (1999) found that eliminating overlapping symptoms did not eliminate comorbidity. Moreover, symptoms such as fatigue or concentration difficulties are indeed features of both anxiety and depression and thus cannot simply be excluded from diagnostic criteria (Angold et al., 1999). Alternative explanations for the comorbidity between anxiety and depression are that anxiety may lead to depression or vice versa (Cummings et al., 2014), or that the combined presentation of anxiety and depressive symptoms may constitute a distinct diagnosis (Angold et al., 1999). Additionally, shared and unique risk factors are suggested to contribute to depression-anxiety comorbidity (cf. Klein & Riso, 1993). These risk factors include a combination of environmental/social (e.g., school, peers, family-related), biological (e.g., a sensitive behavioral inhibition system and a hypoactive behavioral activation system), and behavioral (e.g., avoidance) factors (Cummings et al., 2014). Other demographic, socioeconomic, and lifestyle related factors might also influence later depression or anxiety (Almeida et al., 2012). This variety of explanatory approaches emphasizes the need to better understand and conceptualize the comorbidity between anxiety disorders and depressive disorders.
In addition to illuminating the comorbidity between anxiety and depression, some research efforts have focused on understanding the heterogeneity within anxiety or depression, which complicates matters further. As pointed out by De Jonge et al. (2015, p. 312), “There is no single theory that captures the majority of the variance of depression in the population, nor a single treatment that is helpful for all depressed individuals”. Besides, current treatments for depression are also generally effective for most other internalizing disorders, suggesting that the diagnostic entity of ‘depression’, as it is currently defined in the DSM-5, is not ideal in terms of its clinical utility (De Jonge et al., 2015). Addressing the growing dissatisfaction with the conceptualization of ‘depression’, Harald and Gordon (2012) performed a meta-review of depressive subtyping models and proposed five categories of subtypes: (1) symptom-based subtypes, (2) aetiologically based subtypes, (3) time of onset-based subtypes, (4) gender-based depression, and (5) treatment resistant depression. Symptom-based subtypes include melancholia, psychotic depression, atypical depression and anxious depression (Harald & Gordon, 2012), and it is at best questionable whether all of these subtypes benefit equally from the same kind of treatment (De Jonge et al., 2015). The same line of thought may be applied to the nine different DSM-5 anxiety disorders, since these disorders differ strongly in etiology, core symptoms, and required treatment (cf. APA, 2013).
Latent factor analysis of anxiety and depressive symptoms
What we know for a fact is that there is a large number of symptoms that have been associated with one or more diagnostic categories. But what exactly does this association between symptoms and diagnosis look like? Traditionally, symptoms of mental disorders have been modeled using latent factor analysis (LFA), such as exploratory factor analysis (EFA) or confirmatory factor analysis (CFA). LFA assumes that the positive manifold between a set of symptoms is due to a common underlying latent factor. While the EFA approach allows all items to load freely on different factors, CFA typically only allows items to load on one factor and constrains all cross-loadings to zero. One reason for the popularity of LFA is most likely that it simplifies the complex associations of psychological symptoms. The fundamental assumption of LFA is appealing, since it implies that similar to medical conditions, there is a clearly identifiable cause, resulting in a set of symptoms. According to this approach, correctly identifying this cause would simplify the appropriate diagnostics and treatment (Kotov et al., 2017).
Many studies have applied LFA to disentangle anxiety and depressive symptoms. In a systematic review, Cosco et al. (2012) summarized the findings for the latent structure of the Hospital Anxiety and Depression Scale, which was specifically designed to reliably differentiate between anxiety and depression in adolescents over the age of 15 years and adults. Although this scale assumes two separate factors for anxiety and depression, the authors found mixed factor-analytic findings, reflecting various one-, two-, three-, and four-factor solutions. Accordingly, these results cast doubt on whether anxiety and depression can be viewed as two separate latent constructs (Cosco et al., 2012).
Another prominent example of conceptualizing anxiety and depressive symptoms through LFA is the empirical work of the Hierarchical Taxonomy of Psychopathology (HiTOP) research group. In this approach, disorders such as MDD, generalized anxiety disorder (GAD) and post-traumatic stress disorder (PTSD) are modeled as latent factors belonging to the higher-order distress dimension, whereas other anxiety disorders such as social phobia or specific phobia, modeled as first-order factors, belong to the second-order fear dimension. The distress and fear dimensions, in turn, are subsumed under the internalizing spectrum (Kotov et al., 2017). Yet, despite these valuable advances in conceptualizing the multidimensionality of psychopathology, ambiguity regarding LFA remains in at least two aspects (Borsboom & Cramer, 2013). First, LFA assumes the positive associations between a set of symptoms to be due to a common underlying latent factor. Simply put, it is assumed that the latent factor causes the co-occurrence of symptoms (e.g., depressed mood causes symptoms such as insomnia and concentration problems). However, this assumption can be challenged from both a theoretical and a statistical perspective: From a theoretical standpoint, the assumption of an underlying condition contrasts with current diagnostic classification standards, which (with very few exceptions, such as for PTSD) do not make explicit etiological assumptions. From a statistical standpoint, this assumption implies that after statistically controlling for the latent factor, all inter-item correlations should be zero and all item-total correlations should only differ by their measurement error, both of which are generally not the case. Second, and related to the statistical issue, LFA has been criticized for ignoring the complex interplay among individual symptoms (Borsboom & Cramer, 2013). For instance, one might hypothesize that depressed mood causes concentration problems and sleep problems, and that concentration and sleep problems may then both generate additional symptoms and maintain or worsen the depressed mood, resulting in a self-sustaining state.
Network analysis of anxiety and depressive symptoms
Network analysis (NA) has advanced as an alternative viewpoint to conceptualize mental disorders and aims to address the aforementioned areas of ambiguity. In a psychological network, nodes (e.g., symptoms) are connected via edges (e.g., positive or negative associations). NA attempts to understand mental disorders by focusing on the relationships among the symptoms without modeling latent factors (Borsboom & Cramer, 2013). For example, being tired might lead to rumination in the evening. In turn, this might decrease the ability to concentrate, and the conglomerate of these symptoms and their interrelations is currently called depression. This example illustrates the theorem behind network models, which assume that symptoms directly and causally influence one another’s emergence (Borsboom & Cramer, 2013; van Bork et al., 2017). In this regard, symptoms are understood as “active agents in networks of interacting components rather than passive indicators of latent variables” (van Bork et al., 2017, p. 767).
Network theory has several implications for our conception of diagnosis and treatment (Borsboom, 2017). For example, identifying central (i.e., important) symptoms that activate a range of other symptoms of clusters in a mental disorder network could provide targets for therapeutic interventions (Borsboom, 2017). Since each individual most probably exhibits their own very specific network configuration, this perspective fits well with our understanding of individualized treatment approaches (Borsboom, 2017). Notably, the assumptions of network theory are in line with the principles of cognitive-behavioral interventions in the diagnosis and treatment of mental disorders (Borsboom, 2017). For example, cognitive-behavioral therapy aims to change dysfunctional cognitions patients frequently fall back on (e.g., rumination) in order to change their behavior (e.g., withdrawal). The distinction between more central variables (which are directly connected to a number of other variables/symptoms) and more peripheral variables (which are located on the border of a causal system and may be interpreted as an outcome of the other symptoms and their interactions) is a unique feature of network models and cannot be made using traditional psychometric models (Borsboom, 2008). In addition, NA offers a novel perspective on comorbidity, insofar as symptoms that are common to two disorders (e.g., sleep problems or concentration difficulties in depression and GAD) might simultaneously activate the network of these two disorders (Borsboom, 2017; Cramer et al., 2010). Instead of considering comorbidity as an artifact of the diagnostic system due to overlapping criteria (see above), network theory suggests that “comorbidity is an intrinsic feature of mental disorders” (Borsboom, 2017, p. 7) and that “comorbidity should be seen as part of the flesh and bones of psychopathology” (Borsboom, 2017, p. 8).
In addition to comorbidity, NA may be able to explain several other important psychological concepts, such as resilience, vulnerability, the vulnerability-stress model, and the observation that symptoms often persist long after the trigger has been removed, which further supports the utility of this approach. NA explains resilience and vulnerability in terms of tightly vs. loosely connected networks (Cramer et al., 2016). In tightly connected networks, the activation of a symptom through an external event very quickly activates an array of other symptoms. In this case, a person is very vulnerable to external stressors. In loosely connected networks, the activation might not spread when a symptom is activated through an external event, making the person more resilient. These considerations are in line with the vulnerability-stress model, which states that the emergence of symptoms depends on the individual vulnerability as well as the occurrence of environmental stressors. Network theory can also account for the observation that symptoms persist even after the trigger has been removed. This is particularly pronounced in PTSD, where the symptoms remain long after the traumatic experience, but it also holds true for other mental disorders. The external trigger activates the network, but after activation, the network remains in a stable active state and maintains itself. Accordingly, Borsboom (2017) describes suffering from a mental disorder as being trapped in the stable state of a self-sustaining network.
Previous studies have applied NA to symptoms of mental disorders across all age groups in clinical and community samples (reviewed by Contreras et al., 2019). Overall, it has been suggested that clinical networks are characterized by more densely connected nodes than ‘healthy’ networks (Borsboom, 2017). As such, network topologies from the general population may not be generalizable to clinical samples. For example, Funkhouser et al. (2020) found that the network structure and symptom centrality of internalizing symptoms demonstrated only weak to moderate generalizability across community and clinical samples.
Several studies have specifically examined anxiety and depressive symptoms in a single network in clinical samples, yielding transdiagnostic insights (Beard et al., 2016; Fisher et al., 2017; Groen et al., 2020; Heeren et al., 2018; Kaiser et al., 2021; Langer et al., 2019). Two of these studies focused on intra-individual networks (i.e., based on time series data) in adults diagnosed with anxiety and/or depression (Fisher et al., 2017; Groen et al., 2020). It was suggested that anger (Fisher et al., 2017) or worrying (Groen et al., 2020) may be symptoms that are associated with a large number of depressive and anxiety symptoms, thus potentially connecting these two symptom domains. The remaining studies analyzed samples of adults diagnosed with anxiety and/or depression, or adults from a large psychiatric sample (Beard et al., 2016), based on cross-sectional (Heeren et al., 2018; Langer et al., 2019) or longitudinal data (Beard et al., 2016; Kaiser et al., 2021). It seems striking that all of these studies report a complex interplay between anxiety and depressive symptoms with multiple cross-connections.
While NA may provide a valuable alternative to LFA to conceptualize mental disorders, most of the aforementioned NA studies have important methodological shortcomings, such as a lack of network reliability and accuracy measures, very small sample sizes, or no measures of bridge centrality (i.e., which symptoms may act as ‘middlemen’ between two disorders), highlighting the need for further research.
Overall, three general findings emerge from the literature, that is, (a) comorbidity between anxiety and depression is associated with greater symptom severity, more complicated treatment, and a more difficult diagnostic assessment compared to the sole presence of symptoms of one of these disorders, emphasizing the necessity to better understand the associations between these two domains (Cummings et al., 2014; Melton et al., 2016); (b) both LFA and NA allow us to conceptualize the co-occurrence of anxiety and depression symptoms; however, there is still a need for further research on how the strengths of these statistical methods can be profitably combined; (c) to the best of our knowledge, no NA study has examined parent-rated symptoms of anxiety and depression in clinically referred children and adolescents to date. Given that childhood and adolescence constitute a vulnerable period for the development of internalizing disorders (Essau et al., 2014), it is crucial to refine knowledge about the associations between anxiety and depressive symptoms while growing up.
Objective
The objective of the present study was to apply both LFA and NA in order to gain insights into the inherent structure of parent-rated anxiety and depressive symptoms in children and adolescents aged 4–18 years (N = 743) referred to routine clinical care, thus integrating the methodological strengths of both approaches. While LFA is able to reduce complexity and to provide particularly parsimonious interpretations of complex multivariate data, NA offers a more nuanced and detailed insight into the associations between different items or symptoms.
We decided to use parent ratings as we aimed to consider a broad age span in our analyses, incorporating young children, who might have difficulties with understanding questionnaires and/or expressing their moods and feelings. This also allowed us to include a larger sample (compared to using self-report forms, which were only available for adolescents aged 11 years and older). Of note, parents are considered as important informants in the diagnostics of mental disorders in children and adolescents, as highlighted in current literature supporting the integration of multiple informants into the diagnostic process (e.g., Achenbach, 2020; De Los Reyes et al., 2013, 2015; Dirks et al., 2012).
Based on previous results and following our understanding that comorbidity between anxiety and depression may be explained by shared relationships with intermediary symptoms, we hypothesized that overlapping symptoms in the DSM-5 classification of anxiety disorders and depression, such as irritability, worried, tired and sleep problems, would serve as bridge symptoms, potentially linking other symptoms of depression and anxiety.
Methods
Participants and procedures
The participants of the present study were 743 children and adolescents aged 4–18 years (M = 11.64, SD = 3.66, 61% males) who sought routine care outpatient psychotherapy at the School for Child and Adolescent Cognitive Behavior Therapy (AKiP) at the University Hospital of Cologne. During an initial screening process, the current state of symptomatology (i.e., before beginning cognitive behavioral therapy) of the children and adolescents was assessed using several questionnaires. In this context, the families also received the German Symptom Checklist for Screening Mental Disorders in Children and Adolescents (FBB-SCRREN; Döpfner & Görtz-Dorten 2017), which was to be completed by the mother or father (or another legal caregiver), or by both parents together and was the basis for our analyses. Inclusion criteria for the study were that the children and adolescents had to be between 4 and 18 years old. Since the data were collected under routine care conditions to provide outpatient psychotherapy, the families did not receive any reward for completing the questionnaires.
Measures
The German FBB-SCREEN is a standardized proxy-rating questionnaire that is part of the German Diagnostic System for Mental Disorders in Children and Adolescents based on the ICD-10 and DSM-5 (DISYPS-III; Döpfner & Görtz-Dorten, 2017). The FBB-SCREEN is a screening questionnaire to assess the child’s or adolescent’s symptomatology in a proxy rating form (i.e., by parents, teachers) as part of a multimodal behavioral and psychological diagnostic process (cf. Döpfner & Petermann, 2012). In the present study, the FBB-SCREEN was completed by either the mother, the father, or a legal caregiver, or by both parents together.
The FBB-SCREEN questionnaire comprises 49 items assessing common emotional and behavioral symptoms in children and adolescents. Each item is rated on a 4-point Likert scale ranging from 0 (age-typical/not at all) to 3 (very much), with higher scores reflecting greater symptom severity. The items can be aggregated to seven syndrome scales and three broadband scales (Externalizing Symptoms, Internalizing Symptoms, Contact Behavior) by averaging the associated item scores. In the present study, twelve items assessing anxiety core symptoms and nine items assessing depression core symptoms were included, resulting in a total of 21 items assessing internalizing symptoms. The FBB-SCREEN scale scores have demonstrated sound psychometric properties in terms of the basic factorial configuration and reliability (i.e., internal consistency, item-total correlations) in a large representative national sample (Döpfner & Görtz-Dorten, 2017) and additionally for the domain of externalizing symptoms in a clinical, representative, and special-needs school sample (Thöne et al., 2022).
Analytic plan
Exploratory factor analysis
As a starting point, we explored the underlying data structure and conducted parallel analysis for ordinal data (Horn, 1965; Spearman correlations; principal component analysis factor extraction) using the R package EFA.dimensions (O’Connor, 2000). Following this, we assessed EFA solutions comprising two, three, and four correlated factors using the weighted least squares means and variance adjusted (WLSMV) estimator and oblique GEOMIN rotation in Mplus. Factor loadings ≥ 0.30 were considered substantial (Kline, 2014). For all latent factor analyses, missing data were handled using pairwise present analysis (Muthén & Muthén, 2017).
Network analysis
Network estimation
A psychometric network of anxiety and depressive symptoms was estimated using the R package bootnet (Epskamp et al., 2018). We constructed a Gaussian graphical model (GGM), in which nodes represent observed variables and edges can be interpreted as partial correlation coefficients between two variables, after controlling for all other variables in the network. To estimate our network, we used the Gaussian graphical model ModSelect algorithm (i.e., ggmModSelect) in view of our large sample size, and Spearman correlations in view of the ordinal data structure (Epskamp et al., 2018). In brief, this algorithm searches for an optimal GGM by minimizing the extended Bayesian information criterion of 100 non-regularized (i.e., without penalties for model complexity) GGM models ranging from sparse to dense. This algorithm continues to refit all models, thereby subsequently adding and removing edges until the extended Bayesian information criterion (tuning parameter = 0.5) can no longer be improved. The tuning parameter controls the level of sparsity, i.e., the number of edges removed. A tuning parameter of 0.5 is rather conservative, likely leading to the removal of spurious edges as well as potentially some true edges (Epskamp & Fried, 2018). The layout of the resulting network is based on the Fruchterman–Reingold algorithm, which places related nodes close to each other. Furthermore, a simulation study on the performance of network estimation by varying sample size was run using the netSimulator function (2,500 iterations; Spearman correlations; ggmModSelect network) from the bootnet package (Epskamp et al., 2018). The resulting plots provide insights into the sensitivity, specificity, and correlations between the ‘true’ and the estimated edges (Epskamp et al., 2018). Missing data were handled using pairwise deletion.
Node centrality
The importance of individual nodes was assessed using common node centrality indices (Epskamp et al., 2018). The node strength is the sum of the absolute values of the weights of the edges connected to a node and is a measure of overall connectedness. Betweenness expresses the number of times a node lies on the shortest path between any other two nodes and is used to infer which nodes might frequently act as ‘middlemen’ in network transactions. Closeness centrality indicates how close, in terms of edge distance, a node is on average to all other nodes.
Network accuracy and stability
After network estimation, we applied several bootstrapping procedures to assess the accuracy of the parameter estimates (Epskamp et al., 2018). The accuracy of the edge weights was evaluated by nonparametric bootstrapping (2,500 iterations) with 95% bootstrapped confidence intervals (CIs). Moreover, centrality stability was assessed using case-dropping subset bootstrap (2,500 iterations), thus correlating the original centrality indices with those obtained from smaller subsets of data. The correlation stability coefficients (CS coefficients) quantify the maximum proportion of cases that can be dropped to retain a correlation of at least 0.70 with the original centrality indices. The CS coefficients should not be below 0.25, and preferably above 0.5 (Epskamp et al., 2018). Furthermore, bootstrapped difference tests were calculated to test whether two edge weights significantly differed from each other with regard to their strength, closeness, and betweenness. It should be noted that multiple testing correction when carrying out bootstrapped difference tests in NA has not yet been developed (Epskamp et al., 2018).
Bridge strength
Nodes likely to explain the comorbidity between anxiety and depressive symptoms were identified using bridge indices from the R package networktools (Jones et al., 2017). A major advantage of these bridge indices compared to the traditional centrality measures is that network communities (e.g., mental disorders) can be specified a priori, thus taking the DSM-5-based nomenclature into account (Jones et al., 2019). We calculated bridge strength, which indicates a node’s total connectivity with other communities. Since bridge strength indices have been shown to be equivalent to the sum of network cross-loadings, which in turn are roughly equivalent to EFA loadings (Christensen & Golino, 2021), it is possible to interpret network loadings in terms of effect sizes. This approach seeks to facilitate a more standardized comparison across samples. Christensen and Golino (2021) proposed the following rules of thumb: An effect size of 0.15 indicates a small effect, an effect size of 0.25 indicates a moderate effect, and an effect size of 0.35 indicates a large effect.
Exploratory graph analysis
Next, we employed EGA (Golino & Epskamp, 2017), which has been proposed within the framework of network psychometrics to estimate the number of dimensions (i.e., communities) within a network. Compared to more traditional techniques, which estimate the number of dimensions underlying multivariate data (e.g., parallel analysis), the EGA approach not only estimates the number of dimensions but also identifies and visualizes via a network plot which items belong to each dimension. In the present study, we tested EGA as an alternative approach to EFA and parallel analysis using the R package EGAnet to further understand the dimensionality of the anxiety and depressive symptoms (Golino & Epskamp, 2017). EGA estimates a GGM with Least Absolute Shrinkage and Selection Operator (LASSO) regularization and a tuning parameter minimizing the extended Bayesian information criterion (EBIC). A walktrap algorithm is then employed, which identifies communities in networks. The reliability of the community structure was subsequently verified using 1,000 bootstrapped replications (Golino & Epskamp, 2017).
Confirmatory factor analysis
In a final step, we evaluated the resulting network communities from our EGA on a confirmatory level. Based on the item-community structure suggested by the EGA, we modeled the analogous CFA item-factor configuration using a first-order correlated-factors model. In line with the typical definition of CFA, items were only allowed to load on their respective factor, while cross-loadings were constrained to zero. CFA was conducted using WLSMV (delta parameterization) for ordinal data in Mplus version 8.4 (Muthén & Muthén, 2017). To gain further insight into the factorial structure across different sex and age groups, we additionally performed the CFA on the model derived from the EGA analysis in four subsamples (males; females; children < 11 years; adolescents ≥ 11 years).
In accordance with recommendations (Browne & Cudeck, 1992; Hu & Bentler, 1999), model goodness of fit was assessed using chi-square statistics, the comparative fit index (CFI ≥ 0.95 indicates good fit), the Tucker-Lewis index (TLI ≥ 0.95 indicates good fit), the root mean square error of approximation (RMSEA ≤ 0.08 indicates acceptable fit; RMSEA ≤ 0.05 indicates good fit), and the standardized root mean square residual (SRMR ≤ 0.08 indicates acceptable fit; SRMR ≤ 0.05 indicates good fit). The amount of missing data per item for the full sample varied from 1.6 to 2.1%. Covariance coverage for the full sample was greater than 99% for each item of the FBB-SCREEN.
Results
Sample characteristics
Table 1 summarizes item characteristics including the mean (SD), skewness and kurtosis for each FBB-SCREEN anxiety and depression item. In the present sample, internal consistencies and item-total correlations of the Anxiety Symptoms scale (twelve items; Cronbach’s alpha = 0.72; rit = 0.16 − 0.48) and the Depressive Symptoms scale (nine items; Cronbach’s alpha = 0.78; rit = 0.38 − 0.61) were generally satisfactory to good. Only item A10 Separation anxiety demonstrated a low item-total correlation (rit = 0.16), although excluding this item did not substantially change the Cronbach’s alpha of the respective scale. Additionally, the item characteristics of all 49 items of the FBB-SCREEN are summarized in Table S1 in the online supplement.
Exploratory factor analysis of anxiety and depressive symptoms
The Horn parallel analysis for ordinal data revealed that a maximum of four factors should be extracted. Our EFA solution with two correlated factors revealed several substantial cross-loadings and negative factor loadings, resulting in a factorial configuration that was not clearly interpretable (Table S2). A similar pattern was observed for the EFA yielding three factors (Table S2). Our EFA solution with four correlated factors yielded the most reasonable results (Table 2), with anxiety items loading on three different factors (F1, F2, F3) and depression items loading on two different factors (F3, F4). This solution accounted for 34% of the total variance. However, it became apparent that the four factors were not straightforward to interpret. It might be speculated that F2 reflects some kind of Social anxiety and F4 Depressive mood, although it appears that each factor comprises several semantically different items. The interpretation was further complicated by eight substantial (> 0.30) cross-loadings involving four anxiety items (A11, A12, A14, A16) and two depression items (D25, D26). Factor correlations were low to moderate: Factor 2 – Factor 4 (0.05), Factor 1 – Factor 3 (0.16), Factor 1 – Factor 2 (0.18), Factor 1 – Factor 4 (0.21), Factor 3 – Factor 4 (0.30) to Factor 2 – Factor 3 (0.41). The results of the EFA demonstrate that some items could not be clearly assigned to either an anxiety- or a depression-related factor.
Network analysis of anxiety and depressive symptoms
Network estimation
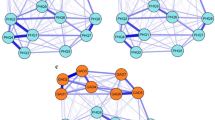
Figure 1 depicts the partial Spearman correlation network. Out of 210 edges, 50 edges (24%) were significantly different from zero (p < .05), resulting in a network density of 0.24. Edge weights ranged from − 0.13 to 0.38 (M = 0.04), and two estimated edges showed small negative partial correlations (-0.13; − 0.12). The strongest edge (0.38) was estimated between A13 Afraid of peers and A14 Afraid of adults. Results from the simulation study for our estimated network demonstrated very high specificity and correlation accuracy, and lower sensitivity (Figure S1). These findings indicate that there is a high probability of observing an edge between two nodes where one edge truly exists. Since the choice of appropriate network estimation methods is still under debate (Isvoranu & Epskamp, 2021), we additionally report network estimates for two other partial correlation networks with lower tuning parameters (λ = 0.1, λ = 0.25) as well as a regularized partial correlation network using the EBICglasso estimation approach (λ = 0.5; Figure S2). Although these networks differ in terms of their network density, they nevertheless demonstrate similar network configurations and associations between the items, suggesting that we can confidently interpret our network.
Node centrality
The strength, closeness, and betweenness centrality z-scores are presented in Fig. 2. Regarding the anxiety symptoms, item A14 Afraid of adults had the highest strength, and regarding the depressive symptoms, items D25 Tired and D28 Suicidal had the highest strength. These nodes followed a similar pattern on the closeness and betweenness measures.
Network accuracy and stability
The estimated network demonstrated adequate accuracy and stability for most parameters. In terms of network stability, the centrality indices strength and closeness showed CS coefficients above the minimum cut-off of 0.25 but below the preferred cut-off of 0.50 (0.36 and 0.44, respectively), whereas the CS coefficient for betweenness was below the minimum cut-off (0.13; Fig. 2). Hence, the rank ordering of the items regarding betweenness should not be interpreted, as it lacks stability, and the rank ordering of the items regarding strength and closeness should be interpreted with caution. Item D25 Tired, which had the highest strength and closeness, had a significantly higher strength than 12 of the 20 remaining items, and a significantly stronger closeness than 11 of the 20 remaining items (Figure S3 and Figure S4; see also Figure S5). In terms of the estimated accuracy of our partial correlations, results of non-parametric bootstrapping suggest that the absolute strength of approximately the ten strongest edges can be interpreted with confidence, as bootstrapped and sample partial correlations are well aligned (Figure S6). This finding is in accordance with the results of our simulation study, which demonstrated high correlation stability for these edges. For all other edges, bootstrapped and sample partial correlations diverged substantially (Figure S6). Similar results emerged for the stability, i.e., the order of the edge weights, which can be interpreted confidently for approximately the five edges with the highest weights, for which the CIs rarely overlap with those of other edges. For all other edges, the CIs substantially overlap with those of other edges (Figure S6). This finding is also depicted in Figure S7, which shows that the five highest edge weights are significantly higher (i.e., no overlapping CIs) than most other edge weights.
Bridge strength
We identified four items in the top 80th percentile of bridge strength, as suggested by Jones et al. (2019). Figure 3 outlines the bridge strength results. The item with the highest bridge strength was D29 Pain, followed by D28 Suicidal, D23 Irritable, and A14 Afraid of adults. The network loadings of the items are summarized in Table S3. According to Christensen and Golino (2021), the network loadings of the bridge symptoms indicate small effects. Case-dropping subset bootstrap (2,500 iterations) yielded a CS coefficient of 0.28, indicating that these results should be interpreted with caution.
Exploratory graph analysis
The EGA using the walktrap algorithm revealed four communities of items (Figure S8). The reliability of this structure was verified using 1,000 bootstrapped replications, which showed that four communities were revealed in 60% of all cases (three communities: 37%; five communities: 3%). We identified two communities (visualized in pink and purple) that comprised depressive symptoms and two communities (visualized in turquoise and green) that mainly comprised anxiety symptoms, although two depression items (D28 Suicidal; D29 Pain) were related to the green anxiety community. Notably, the parallel analysis from our EFA analysis also revealed a four-factor solution.
Confirmatory factor analysis of the anxiety and depression EGA communities
Based on the results of the EGA analysis, we constructed a latent factor model with four correlated factors, modeling the same item-community configuration as suggested by the walktrap algorithm (Figure S8). While model estimation terminated normally, we found that the latent variable covariance matrix was not positive definite, due to problems with a linear dependency associated with Factor 4. Goodness-of-fit indices indicated poor model fit (CFI: 0.88, TLI: 0.86; RMSEA: 0.069; SRMR: 0.075). Overall, substantial factor loadings emerged on all factors (Factor 1: |lambda| = 0.40 to 0.73, M = 0.63; Factor 2: |lambda| = 0.53 to 0.75, M = 0.68; Factor 3: |lambda| = 0.29 to 0.64, M = 0.52; and Factor 4: |lambda| = 0.60 to 0.71, M = 0.65). In addition, there were significant (p < .001), moderate to strong positive factor correlations: Factor 2 – Factor 3 (0.46), Factor 1 – Factor 3 (0.50), Factor 1 – Factor 4 (0.51), Factor 3 – Factor 4 (0.65), Factor 1 – Factor 2 (0.85) to Factor 2 – Factor 4 (0.86; see Table S4). In addition, we assessed this item-factor configuration based on the EGA walktrap algorithm results in four different subsamples using CFA (males; females; children < 11 years; adolescents ≥ 11 years; Tables S5-S8). Similar to our CFA in the full sample, goodness-of-fit indices indicated poor model fit in all four subsamples (Tables S5-S8). Moreover, the same difficulties with a latent covariance matrix that was not positive definite also occurred in the subsample of children < 11 years associated with Factor 2 and in the subsample of males associated with Factor 4, respectively. Besides, we found only weak positive correlations between the symptom scale Anxiety and age (r = .19, p < .001, n = 740) and sex (rpbis = 0.20, p < .001, n = 740) and weak positive correlations between the symptom scale Depression and age (r = .36, p < .001, n = 734) and sex (rpbis = 0.16, p < .001, n = 734). These findings indicate that the influence of age and sex on the symptom structure in our sample may only be small.
Discussion
The present study aimed to conceptualize the associations between symptoms of anxiety and depression in children and adolescents who sought routine care outpatient psychotherapy by combining and comparing the results of LFA and NA. In general, the results of both EFA and EGA (performed in the context of NA) most likely support a structure comprising four factors or communities, respectively, though the item-factor/item-community configuration derived from the two approaches differed in some aspects. A factor structure obtained from the EGA results could not be confirmed using CFA; however, this might be due to methodological restrictions (see below). Beyond the grouping of symptoms, NA offered a deeper insight into the associations between anxiety and depressive symptoms, highlighting a complex interplay between the symptoms of the two domains.
Exploratory factor analysis highlights a substantial overlap between anxiety and depressive symptoms
Both the a-priori defined anxiety and depression scale demonstrated satisfactory internal consistency, and the item-total correlations were satisfactory to good for most of the items. However, the EFA solution comprising two correlated factors of anxiety and depressive symptoms did not yield adequate model fit, and we observed several significant cross-loadings and negative factor loadings. A four-factor solution, as suggested by the parallel analysis, yielded an adequate model fit. One of the extracted factors (F4) captured mainly depressive symptoms while two other factors (F1 and F2) mainly comprised anxiety symptoms. Notably, factor F2 only included two items and was thus very weak. The anxiety symptoms assigned to factor F1 varied in content, and like factor F3, which captured both anxiety and depressive symptoms, this factor was difficult to interpret. Moreover, regarding the two-factor model, we observed several significant cross-loadings, which further complicated a straightforward interpretation of this solution. It should be noted that if a positive manifold of a set of items exists, extracting a latent factor is a mathematical necessity, which confirms the notion of a common factor but neither leads to new insights nor explores alternative explanations for the item-item correlations (van Bork et al., 2017). Our findings indicate that symptoms of anxiety and depression as conceptualized in the DSM-5 cannot be clearly assigned to separate dimensions, but that substantial overlap exists. These results are in line with previous research pointing out the difficulty to clearly differentiate between anxiety and depressive symptomatology (Cosco et al., 2012), which frequently leads to comorbid diagnoses (Angold et al., 1999; Melton et al., 2016). These findings are in accordance with previous research on shared and unique risk factors, which may contribute to the development of both anxiety and depression (Cummings et al., 2014).
Network analysis offers a nuanced yet complex perspective on the associations between anxiety and depressive symptoms
Network estimation revealed a complex interplay between anxiety and depressive symptoms, demonstrating multiple associations between the items associated with these two domains. These associations might potentially provide an explanation for why the two-factor model revealed by the EFA did not yield an adequate model fit. An examination of the centrality indices revealed that strength and closeness centrality indices could be interpreted with some caution. Items D25 Tired, D28 Suicidal, and A14 Afraid of adults showed the highest strengths, suggesting that these items show more and/or stronger associations with other symptoms than do other items. It is worth noting that in particular, item D25 Tired was associated with a large number of other symptoms from both dimensions, potentially highlighting its transdiagnostic impact on several other psychological symptoms. Interestingly, we found that the five strongest edges, which were significantly stronger than all other edges, only represented associations within the anxiety domain or within the depression domain. In other words, none of these edges represented an association between a depression and an anxiety item. This finding is consistent with the results of previous network studies (Beard et al., 2016; Langer et al., 2019) and suggests that the idea of domain-specific underlying factors cannot be fully disregarded (Cosco et al., 2012; Kotov et al., 2017).
Using bridge strength analysis, we identified four items (D29 Pain, D28 Suicidal, D23 Irritable, A14 Afraid of adults) that may link the depression and anxiety domains, with small effect sizes according to the classification by Christensen and Golino (2021). These findings were somewhat surprising, as with the exception of D23 Irritable, we did not hypothesize that these specific symptoms would act as bridges between anxiety and depression. Regarding item D29 Pain, it is conceivable that some children express both depressed mood and anxiety through somatic symptoms, which might offer an explanation for the bridge function of this item. Vegetative symptoms are, in fact, criteria for depression and nearly all anxiety disorders in the ICD-11 (WHO, 2019) as well as the DSM-5 (APA, 2013). Moreover, Means-Christensen et al. (2008) showed that depression and anxiety are frequently associated with pain, such as muscle pain, headaches or stomach pains in primary care patients. Accordingly, in clinical practice, if a child or adolescent diagnosed with either an anxiety or depressive disorder demonstrates one of these bridge symptoms, therapists should thoroughly explore the presence of comorbid depressive or anxiety symptoms, respectively, as the presence of a bridge symptom might hint at the activation of the particular other community in the network. The identification of irritable as a bridge item is an interesting finding, since irritability has been suggested as a transdiagnostic symptom of both externalizing and internalizing disorders (Beauchaine & Tackett, 2020). From a developmental perspective, irritability in early childhood predicts the development of both internalizing and externalizing disorders as well as greater functional impairment and outpatient treatment use in later childhood (Beauchaine & Tackett, 2020; Dougherty et al., 2015). The identification of item D28 Suicidal as a bridge item may be attributable to the potential association of both anxiety and depressive symptoms with severe psychological strain, and consequently also with suicidal tendencies. Due to the cross-sectional nature of the data considered in the present study, we were unfortunately unable to establish a temporal sequence of the emergence of the symptoms. However, as suicidal behavior is regarded as a consequence rather than a cause of the complex interplay between psychological, social, and biological factors (O’Connor & Nock, 2014), it is likely that other anxiety and depressive symptoms precede suicidal tendencies. As such, the term ‘bridge item’ might me misleading, as it indicates that this item might be responsible for the jump from one symptom complex to the next. This remains to be clarified in future studies using longitudinal data. Contrary to our expectations and previous results (Groen et al., 2020), the symptoms tired and worried did not emerge as bridge items. A possible statistical explanation for this finding might be that floor effects for these items resulted in an attenuation of the variance estimates (about 50% of the parents rated both items with zero). Another, more content-related explanation might be that the symptoms tired and worried constitute internal mental states which can be neither clearly observed nor unambiguously scored from a parent’s perspective. This suggests that even if tired or worried were ‘true’ bridge items, parents may overlook them, and older children or adolescents may be better informants for their own mental states. Accordingly, this finding may point to the particular importance of including self-report measures when diagnosing internalizing disorders (Hope et al., 1999), as long as self-report is feasible based on the child’s age. By contrast, the symptoms afraid of adults, pain, suicidal, and irritable may constitute more noticeable behaviors, which could be identified by parents if they are ‘truly’ bridge items.
Taken together, the results of the NA offer a very nuanced and detailed view on the associations between a number of anxiety and depressive symptoms, highlighting multiple interrelations within and also between the two domains and pointing at the special importance of the items afraid of adults, pain, suicidal, and irritable, which serve as middlemen between the two domains. Since both a detailed consideration of the associations between symptoms and a reduction of complexity by assigning symptoms to underlying factors/communities may be of practical interest and relevance, we tried to further explore the dimensionality of the internalizing symptoms.
Exploratory graph analysis reveals four communities of anxiety and depressive symptoms
Within the scope of examining the dimensionality of anxiety and depressive symptoms, we employed EGA as an alternative approach to EFA and parallel analysis. While LFA provides information about the factor structure underlying a set of items, EGA not only estimates the number of dimensions, but also identifies and visualizes via a network plot which items belong to each dimension (Golino & Epskamp, 2017). This is an important advantage over more traditional techniques such as EFA, where assigning items to factors is typically done manually and may lead to different solutions when performed by different researchers. In EGA, items are still allowed to be connected with items from other communities. These connections are similar to cross-loadings in latent factor analysis, but in CFA, cross-loadings are typically constrained to zero due to the assumption that symptoms can be clearly assigned to a latent factor. Given the partly overlapping symptom criteria for anxiety and depressive disorders, the connections between symptoms across domains tolerated by the EGA might represent an advantage of this approach over the CFA approach when analyzing the structure of internalizing symptoms.
The results of our EGA identified, in 60% of cases, four communities (three communities: 37%, five communities: 3%). Although it is interesting that both the EGA and the parallel analysis yielded four communities/factors, the results from these two approaches differed from each other. The solution suggested by the EGA draws a clearer distinction between anxiety and depression compared to that derived from the EFA. Only two depression items (D29 Pain, D28 Suicidal) were assigned to a community consisting of anxiety items. This corresponds to our identification of these two items as bridge items and to the finding that they loaded on F1 in the EFA, which was composed of items from both domains. However, similar to our EFA results, it was difficult to unambiguously interpret the meaning of the communities.
In a final step, we tested the community structure suggested by the EGA using a CFA, thereby constraining all cross-loadings to zero. Thereby, we tested the factorial structure both in our total sample and in subsamples separated by age and sex. We found poor model fit in all samples. Among other aspects, this might be due to constraining the item cross-loadings to zero, which may not be a realistic proposition and has led to a growing dissatisfaction with this procedure (Marsh et al., 2014). By comparison, EGA, and NA in general, may provide more nuanced insights into the multidimensionality of psychological constructs, which is in line with previously observed cross-loadings between internalizing symptoms (Cosco et al., 2012).
Strengths and limitations
A major strength of our study is that we combined the advantages of LFA and NA to obtain a comprehensive view on the structure underlying internalizing symptoms and the interplay between a range of anxiety and depressive symptoms. Moreover, we considered anxiety and depressive symptoms together in joint analyses using current state-of-the-art analytical techniques (including simulation studies, analyses of network accuracy and stability estimates, bootstrapping procedures, analysis of bridge centrality).
One major limitation is that we included only parent ratings in our analyses, because correlations between multiple informants, particularly between self-ratings and other informants (e.g., parents, teachers), have often been shown to be low to moderate in children and adolescents with anxiety disorders (De Los Reyes et al., 2015; Miller et al., 2014) or depression (De Los Reyes et al., 2015; Lewis et al., 2014), and likewise with externalizing disorders (De Los Reyes et al., 2015; Thöne et al., 2021, 2022). There is a growing recognition that such discrepancies between different informants might reflect how the children’s or adolescents’ behavior varies meaningfully across contexts, such as at home or at school (De Los Reyes et al., 2013; Dirks et al., 2012; Thöne et al., 2021, 2022). Moreover, children and adolescents may be more reliable informants about their own covert internal states than their parents or teachers. Thus, further research assessing measurement invariance across informants is needed to learn more about the robustness and generalizability of the conceptualization of anxiety and depression symptoms.
Besides, in line with this and as data were collected under routine conditions, we could not provide more detailed information on the sociodemographic characteristics of the mothers, fathers, or other primary caregivers. As the ratings of these informants might differ, future studies could examine whether findings on the structure underlying internalizing symptoms vary by caregiver perspective.
Another limitation of the present study is that due to the cross-sectional design, we are unable to draw any conclusions regarding the causality of associations between anxiety and depressive symptoms. Ideally, future studies should also analyze longitudinal data in order to uncover causal relationships or to track the developmental trajectory of internalizing disorders. As one of the major strengths of NA is the identification of central symptoms, i.e., symptoms that might be particularly important in therapeutic terms, associated with a large number of other symptoms, it would be especially relevant to evaluate how these symptoms change over time. For example, having identified a symptom such as irritable as therapeutically important, clinical research could be advanced by systematically evaluating network-based interventions (i.e., a priori identifying central and bridge symptoms in the individual patient and specifically targeting these) compared to routine therapy. Such study designs would provide important contributions for individualized treatment. In the long term, early interventions for these symptoms might stop the spread of activation to other symptoms, thus alleviating further psychological burden.
Conclusion
The combination of LFA and NA offered a comprehensive view on the structure underlying internalizing symptoms and the associations between symptoms within and across the anxiety and depression domains. There are multiple complex associations between internalizing symptoms. However, associations within the anxiety domain or the depression domain are generally stronger than associations across domains. Moreover, despite the multiple associations revealed by the NA, it was possible to identify domain-specific, underlying factors/communities. The results of our EFA and EGA indicate that anxiety and depressive symptoms can most likely be assigned to four factors/communities. However, for both EFA and EGA, communities could not be interpreted unambiguously and both solutions yielded an inadequate model fit. The consideration of the items afraid of adults, pain, irritable and potentially suicidal is of special clinical relevance, as these items were identified as middlemen between the anxiety and depression communities. The present findings provide a deeper understanding of the interrelations between internalizing symptoms in childhood and adolescence and their underlying structure. As the use of cross-sectional data constitutes an important shortcoming, future studies should include longitudinal data to illuminate the causal associations between the individual symptoms.
Availability of data and material (data transparency)
Available upon reasonable request.
Code availability (software application or custom cCde)
Available upon reasonable request.
References
Achenbach, T. M. (2020). Bottom-Up and top-down paradigms for psychopathology: a half-century odyssey. Annual Review of Clinical Psychology, 16, 1–24. https://doi.org/10.1146/annurev-clinpsy-071119-115831
Almeida, O. P., Draper, B., Pirkis, J., Snowdon, J., Lautenschlager, N. T., Byrne, G., Sim, M., Stocks, N., Kerse, N., Flicker, L., & Pfaff, J. J. (2012). Anxiety, depression, and comorbid anxiety and depression: risk factors and outcome over two years. International Psychogeriatrics, 24(10), 1622–1632. https://doi.org/10.1017/S104161021200107X
American Psychiatric Association (2013). Diagnostic and Statistical Manual of Mental Disorders (5th ed.). American Psychiatric Association. https://doi.org/10.1176/appi.books.9780890425596
Angold, A., Costello, E. J., & Erkanli, A. (1999).Comorbidity. Journal of child psychology and psychiatry, and allied disciplines, 40(1),57–87.
Beard, C., Millner, A. J., Forgeard, M. J. C., Fried, E. I., Hsu, K. J., Treadway, M. T., Leonard, C. V., Kertz, S. J., & Björgvinsson, T. (2016). Network analysis of depression and anxiety symptom relationships in a psychiatric sample. Psychological Medicine, 46(16), 3359–3369. https://doi.org/10.1017/S0033291716002300
Beauchaine, T. P., & Tackett, J. L. (2020). Irritability as a transdiagnostic vulnerability trait:current issues and future directions. Behavior Therapy, 51(2), 350–364. https://doi.org/10.1016/j.beth.2019.10.009
Borsboom, D. (2008). Psychometric perspectives on diagnostic systems. Journal of Clinical Psychology, 64(9), 1089–1108. https://doi.org/10.1002/jclp.20503
Borsboom, D. (2017). A network theory of mental disorders. World Psychiatry, 16(1), 5–13. https://doi.org/10.1002/wps.20375
Borsboom, D., & Cramer, A. O. J. (2013). Network analysis: an integrative approach to the structure of psychopathology. Annual Review of Clinical Psychology, 9, 91–121. https://doi.org/10.1146/annurev-clinpsy-050212-185608
Browne, M. W., & Cudeck, R. (1992). Alternative Ways of assessing Model Fit. Sociol Methods Res, 21(2), 230–258.
Christensen, A. P., & Golino, H. (2021). On the equivalency of factor and network loadings. Behavior Research Methods, 53(4), 1563–1580. https://doi.org/10.3758/s13428-020-01500-6
Contreras, A., Nieto, I., Valiente, C., Espinosa, R., & Vazquez, C. (2019). The study of psychopathology from the network analysis perspective: a systematic review. Psychotherapy and Psychosomatics, 88(2), 71–83. https://doi.org/10.1159/000497425
Cosco, T. D., Doyle, F., Ward, M., & McGee, H. (2012). Latent structure of the hospital anxiety and Depression Scale: a 10-year systematic review. Journal of Psychosomatic Research, 72(3), 180–184.
Cramer, A. O. J., Van Borkulo, C. D., Giltay, E. J., Van Der Maas, H. L. J., Kendler, K. S., Scheffer, M., & Borsboom, D. (2016). Major depression as a complex dynamic system. Plos One, 11(12), 1–20. https://doi.org/10.1371/journal.pone.0167490
Cramer, A. O. J., Waldorp, L. J., Van Der Maas, H. L. J., & Borsboom, D. (2010). Comorbidity: a network perspective. Behavioral and Brain Sciences, 33(2–3), 137–150. https://doi.org/10.1017/S0140525X09991567
Cummings, C. M., Caporino, N. E., & Kendall, P. C. (2014). Comorbidity of anxiety and depression in children and adolescents: 20 years after. Psychlogical Bulletin, 140(3), 816–845. https://doi.org/10.1037/a0034733.Comorbidity
De Jonge, P., Wardenaar, K. J., & Wichers, M. (2015). What kind of thing is depression? Epidemiology and Psychiatric Sciences, 24(4), 312–314. https://doi.org/10.1017/S2045796015000207
De Los Reyes, A., Augenstein, T. M., Wang, M., Thomas, S. A., Drabick, D. A. G., Burgers, D. E., & Rabinowitz, J. (2015). The validity of the Multi-Informant Approach to assessing child and adolescent Mental Health. Psychological Bulletin, 141(4), 858–900. https://doi.org/10.1037/a0038498
De Los Reyes, A., Thomas, S. A., Goodman, K. L., & Kundey, S. M. A. (2013). Principles underlying the use of multiple Informants’ reports. Annu Rev Clin Psychol, 9, 123–149. https://doi.org/10.1146/annurev-clinpsy-050212-185617
Dirks, M. A., De Los Reyes, A., Briggs-Gowan, M., Cella, D., & Wakschlag, L. S. (2012). Annual research review: embracing not erasing contextual variability in children’s behavior - theory and utility in the selection and use of methods and informants in developmental psychopathology. Journal Of Child Psychology And Psychiatry, 53(5), 558–574. https://doi.org/10.1111/j.1469-7610.2012.02537.x
Döpfner, M., & Görtz-Dorten, A. (2017). Diagnostik-System für psychische Störungen nach ICD-10 und DSM-5 für Kinder und Jugendliche – III [Diagnostic System of Mental Disorders in children and adolescents based on the ICD-10 and DSM-5] (DISYPS–III). Hogrefe.
Döpfner, M., & Petermann, F. (2012). Diagnostik psychischer Störungen im Kindes-und Jugendalter. Leitfaden Kinder- und Jugendpsychotherapie (2 vol.). Vol). Hogrefe Verlag.
Dougherty, L. R., Smith, V. C., Bufferd, S. J., Kessel, E., Carlson, G. A., & Klein, D. N. (2015). Preschool irritability predicts child psychopathology, functional impairment, and service use at age nine. Journal of Child Psychology and Psychiatry and Allied Disciplines, 56(9), 999–1007. https://doi.org/10.1111/jcpp.12403
Epskamp, S., Borsboom, D., & Fried, E. I. (2018). Estimating psychological networks and their accuracy: a tutorial paper. Behavior Research Methods, 50(1), 195–212. https://doi.org/10.3758/s13428-017-0862-1
Epskamp, S., & Fried, E. I. (2018). A tutorial on regularized partial correlation networks. Psychological Methods, 23(4), 617–634. https://doi.org/10.1037/met0000167
Essau, C. A., Lewinsohn, P. M., Olaya, B., & Seeley, J. R. (2014). Anxiety Disorders in adolescents and psychosocial outcomes at Age 30. Journal of Affective Disorders, 163, 125–132. https://doi.org/10.1016/j.jad.2013.12.033
Fisher, A. J., Reeves, J. W., Lawyer, G., Medaglia, J. D., & Rubel, J. A. (2017). Exploring the Idiographic Dynamics of Mood and anxiety via Network Analysis. Journal of Abnormal Psychology, 126(8), 1044–1056. https://doi.org/10.1037/abn0000311
Funkhouser, C. J., Correa, K. A., Gorka, S. M., Nelson, B. D., Phan, L., K., & Shankman, S. A. (2020). The replicability and generalizability of internalizing Symptom Networks across five samples. Journal of Abnormal Psychology, 129(2), 191–2013.
Golino, H. F., & Epskamp, S. (2017). Exploratory graph analysis: a new approach for estimating the number of dimensions in psychological research. Plos One, 12(6), 1–26. https://doi.org/10.1371/journal.pone.0174035
Groen, R. N., Ryan, O., Wigman, J. T. W., Riese, H., Penninx, B. W. J. H., Giltay, E. J., Wichers, M., & Hartman, C. A. (2020). Comorbidity between depression and anxiety: assessing the role of bridge mental states in dynamic psychological networks. BMC Medicine, 18(1), https://doi.org/10.1186/s12916-020-01738-z
Harald, B., & Gordon, P. (2012). Meta-review of depressive subtyping models. Journal of Affective Disorders, 139(2), 126–140. https://doi.org/10.1016/j.jad.2011.07.015
Heeren, A., Jones, P. J., & McNally, R. J. (2018). Mapping network connectivity among symptoms of social anxiety and comorbid depression in people with social anxiety disorder. Journal of Affective Disorders, 228(October 2016), 75–82. https://doi.org/10.1016/j.jad.2017.12.003
Hope, T. L., Adams, C., Reynolds, L., Powers, D., Perez, R. A., Kelley, M., & Lou (1999). Parent vs. self-report: contributions toward diagnosis of adolescent psychopathology. Journal of Psychopathology and Behavioral Assessment, 21(4), 349–363. https://doi.org/10.1023/A:1022124900328
Horn, J. L. (1965). A rationale and test for the number of factors in factor analysis. Psychometrika, 30(2), 179–185. https://doi.org/10.1007/BF02289447
Hu, L., & Bentler, P. M. (1999). Cutoff criteria for fit indexes in covariance structure analysis: conventional criteria versus new alternatives. Struct Equ Modeling, 6(1), 1–55.
Isvoranu, A. M., & Epskamp, S. (2021). Which Estimation Method to Choose in Network Psychometrics? Deriving Guidelines for Applied Researchers. Preprint.
Jones, P. J., Heeren, A., & McNally, R. J. (2017). Commentary: a network theory of mental disorders. Frontiers in Psychology, 16, 5–13. https://doi.org/10.1002/wps.20375
Jones, P. J., Ma, R., & McNally, R. J. (2019). Bridge centrality: A Network Approach to understanding Comorbidity. Multivariate Behavioral Research, 0(0), 1–15. https://doi.org/10.1080/00273171.2019.1614898
Kaiser, T., Herzog, P., Voderholzer, U., & Brakemeier, E. L. (2021). Unraveling the comorbidity of depression and anxiety in a large inpatient sample: network analysis to examine bridge symptoms. Depression and Anxiety, 38(3), 307–317. https://doi.org/10.1002/da.23136
Klein, D. N., & Riso, L. P. (1993). Psychiatric disorders: problems of boundaries and comorbidity. In C. G. Costello (Ed.), Basic issues in psychopathology. Guilford Press.
Kline, P. (2014). An Easy Guide to factor analysis. An Easy Guide to factor analysis. Routledge. https://doi.org/10.4324/9781315788135
Kotov, R., Waszczuk, M. A., Krueger, R. F., Forbes, M. K., Watson, D., Clark, L. A., Achenbach, T. M., Althoff, R. R., Ivanova, M. Y., Bagby, M., Brown, R., Carpenter, T. A., Caspi, W. T., Moffitt, A., Eaton, T. E., Forbush, N. R., Goldberg, K. T., Hasin, D., Hyman, D., & Zimmerman, S. E., M (2017). The hierarchical taxonomy of psychopathology (HiTOP): a dimensional alternative to traditional nosologies. Journal Of Abnormal Psychology, 126(4), 454–477. https://doi.org/10.1037/abn0000258
Langer, J. K., Tonge, N. A., Piccirillo, M., Rodebaugh, T. L., Thompson, R. J., & Gotlib, I. H. (2019). Symptoms of social anxiety disorder and major depressive disorder: a network perspective. Journal of Affective Disorders, 243, 531–538. https://doi.org/10.1016/j.jad.2018.09.078
Lewis, A. J., Bertino, M. D., Bailey, C. M., Skewes, J., Lubman, D. I., & Toumbourou, J. W. (2014). Depression and suicidal behavior in adolescents: a multi-informant and multi-methods approach to diagnostic classification. Frontiers in Psychology, 5(JUL), 1–9. https://doi.org/10.3389/fpsyg.2014.00766
Marsh, H. W., Morin, A. J., Parker, P. D., & Kaur, G. (2014). Exploratory structural equation modeling: an integration of the best features of exploratory and confirmatory factor analysis. Annu Rev Clin Psychol, 10(November), 85–110. https://doi.org/10.1146/annurev-clinpsy-032813-153700
Means-Christensen, A. J., Roy-Byrne, P. P., Sherbourne, C. D., Craske, M. G., & Stein, M. B. (2008). Relationships among pain, anxiety, and depression in primary care. Depression and Anxiety, 25(7), 593–600. https://doi.org/10.1002/da.20342
Melton, T. H., Croarkin, P. E., Strawn, J. R., & McClintock, S. M. (2016). Comorbid anxiety and depressive symptoms in children and adolescents: a systematic review and analysis. Journal of Psychiatric Practice, 22(2), 84–98. https://doi.org/10.1097/PRA.0000000000000132
Miller, L. D., Martinez, Y. J., Shumka, E., & Baker, H. (2014). Multiple informant agreement of child, parent, and teacher ratings of child anxiety within community samples. Canadian Journal of Psychiatry, 59(1), 34–39. https://doi.org/10.1177/070674371405900107
Muthén, L. K., & Muthén, B. O. (2017). Mplus user’s guide (8th ed.). Muthén & Muthén.
O’Connor, B. P. (2000). SPSS and SAS programs for determining the number of components using parallel analysis and Velicer’s MAP test. Behavior Research Methods Instruments and Computers, 32(3), 396–399.
O’Connor, R. C., & Nock, M. K. (2014). The psychology of suicidal Behaviour. The Lancet Psychiatry, 1(1), 73–85. https://doi.org/10.1016/S2215-0366(14)70222-6
Polanczyk, G. V., Salum, G. A., Sugaya, L. S., Caye, A., & Rohde, L. A. (2015). Annual research review: a meta-analysis of the worldwide prevalence of mental disorders in children and adolescents. Journal of Child Psychology and Psychiatry and Allied Disciplines, 56(3), 345–365. https://doi.org/10.1111/jcpp.12381
Thöne, A. K., Junghänel, M., Görtz-Dorten, A., Breuer, D., del Giudice, T., Hanisch, C., Hennemann, T., & Döpfner, M. (2022). Empirically based dimensions of externalizing symptoms in children and adolescents: a multitrait-multisource approach. Journal of Psychopathology and Behavioral Assessment, 44(3), 844–861. https://doi.org/10.1007/s10862-022-09983-7
Thöne, A. K., Junghänel, M., Görtz-Dorten, A., Dose, C., Hautmann, C., Jendreizik, L. T., Treier, A. K., Vetter, P., von Wirth, E., Banaschewski, T., Becker, K., Brandeis, D., Dürrwächter, U., Geissler, J., Hebebrand, J., Hohmann, S., Holtmann, M., Huss, M., Jans, T., & Döpfner, M. (2021). Disentangling symptoms of externalizing disorders in children using multiple measures and informants. Psychological Assessment, 33(11), 1065. https://doi.org/10.1037/pas0001053
van Bork, R., Epskamp, S., Rhemtulla, M., Borsboom, D., & van der Maas, H. L. J. (2017). What is the p-factor of psychopathology? Some risks of general factor modeling. Theory and Psychology, 27(6), 759–773. https://doi.org/10.1177/0959354317737185
World Health Organization. (2019). International Statistical classification of Diseases and related health problems ICD-11 (11th ed.). World Health Organization.
Zimmerman, M., Martin, J., McGonigal, P., Harris, L., Kerr, S., Balling, C., Kiefer, R., Stanton, K., & Dalrymple, K. (2019). Validity of the DSM-5 anxious distress specifier for major depressive disorder. Depression and Anxiety, 36(1), 31–38. https://doi.org/10.1002/da.22837
Acknowledgements
We would like to gratefully thank all the participating patients and their families.
Funding
Open Access funding enabled and organized by Projekt DEAL. Not applicable.
Author information
Authors and Affiliations
Contributions
All authors made substantial contributions to the conception or design of the work. Material preparation and data analyses were performed by MJ and AT and reviewed by CD and MD. The first draft of the manuscript was written by MJ and AT, and all authors commented on previous versions of the manuscript. All authors critically revised the manuscript for important intellectual content and approved the final manuscript. All authors agree to be accountable for all aspects of the work in ensuring that questions related to the accuracy or integrity of any part of the work are appropriately investigated and resolved.
Corresponding author
Ethics declarations
Conflicts of interest/competing interests
AGD and MD are supervisors and lecturers at the School for Child and Adolescent Behavior Therapy (AKiP) and authors of the Diagnostic System for Mental Disorders in Children and Adolescents (DISYPS-III), which was used in the present study. They have received income as heads of AKiP at the University of Cologne and royalties from the publisher of the DISYPS-III. All remaining authors declare no conflicts of interest.
Ethics approval
All procedures performed in this study were in accordance with the ethical standards of the institutional and/or national research committee and with the 1964 Helsinki declaration and its later amendments or comparable ethical standards. All studies, including the present study, conducted with data collected in the process of routine therapy at the School for Child and Adolescent Behavior Therapy (AKiP), were approved by the ethics committee of the University of Cologne (15-401).
Consent to participate
All parents declared their consent for the use of data (e.g., questionnaire data) gathered on their child during the time of treatment at the School for Child and Adolescent Behavior Therapy (AKiP) for research purposes. Adolescents/Young adults of legal age provided this consent themselves.
Additional information
Publisher’s Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Michaela Junghänel and Ann-Kathrin Thöne share the first authorship and they equally contributed to the manuscript.
Electronic supplementary material
Below is the link to the electronic supplementary material.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if changes were made. The images or other third party material in this article are included in the article's Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article's Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
Junghänel, M., Thöne, AK., Dose, C. et al. Conceptualizing anxiety and depression in children and adolescents: a latent factor and network analysis. Curr Psychol 43, 1248–1263 (2024). https://doi.org/10.1007/s12144-023-04321-w
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12144-023-04321-w