Summary
Background
We evaluated the frequency of incidental papillary thyroid microcarcinomas (mPTC) in thyroidectomies performed for benign diseases, to better characterize this nosologic entity and to assess the best treatment.
Methods
Between 2009 and 2017, a total of 1777 patients underwent surgery for benign thyroid disease. Patients with preoperative undetermined or positive for malignancy cytology were excluded, as well as incidental thyroid cancer larger than 1 cm.
Results
Total thyroidectomy was performed in 1649 patients (92.7%) and hemithyroidectomy in 128 (7.2%). Papillary thyroid cancer, sized between 2–10 mm, was found in 89 patients (5%), which were all by definition microcarcinomas (mPTC). In 11 patients mPTCs were multifocal and in 7 bilateral. Just 6 patients received hemithyroidectomy and later underwent radical surgery without complications. No tumor-related morbidity or mortality was observed. The χ2 test showed a statistically significant association between mPTC and non-toxic multinodular goiter.
Discussion
In the literature, the rates of incidental mPTC vary, due to various factors such as histopathological examination and sampling numbers. Regarding surgical treatment, some authors support a “conservative” approach for the positive prognosis, but considering that it can be associated with mortality, lymph node recurrence and metastasis, its treatment is still controversial.
Conclusions
Our experience confirms that total thyroidectomy in multinodular goiter is a safe procedure, which ensures endocrine control and oncologic complete tumor resection, in case of mPTC. In uninodular goiter, we recommend hemithyroidectomy; if mPTC is discovered, we suggest radical surgery especially in patients older than 50 years and with familial disposition for thyroid cancer and peripheral tumors larger than 5 mm and aggressive variants.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Incidental thyroid cancer (ITC) is a malignant tumor occasionally discovered through pathological examination after thyroidectomy for benign thyroid disease [1]. Usually they are papillary thyroid microcarcinomas (mPTC), which were defined in 1988 by the World Health Organization as a papillary tumor with a diameter up to 10 mm (“minute” <5 mm and “tiny” between 5 and 10 mm), low aggressiveness and very low risk of distant metastases [2]. A review of the available data in the literature report the incidence of ITC to be between 7 and 21.6% in surgical specimens [1, 3, 4].
Despite the excellent prognosis, cases of mPTC with lymph node metastases are described: this occurred in adult patients with apparently benign cervical cysts and no palpable disease in the thyroid gland; moreover, recurrences in the residual parenchyma or distant metastasis are reported [1, 5,6,7,8]. For this reason, the detection and clinical management of occult thyroid carcinomas remain a controversial topic. In the present study, we retrospectively review the data of patients who underwent surgery for benign thyroid diseases in our university hospital with the aim to estimate the frequency of incidental thyroid cancer, to characterize the lesions, and to discuss the most suitable approach.
Patients and methods
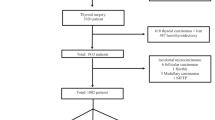
Between January 2009 and December 2017, at the University Hospital of Naples Federico II, 2487 patients were surgically treated for thyroid diseases. Of these, we excluded 631 patients, who presented nodules bigger than 1 cm or had undetermined or positive malignancy preoperative cytology (Thy 3–5 according to the British Thyroid Association Thyroid FNAC Reporting Guidelines) [9]. In all, 1777 patients (1374 women [77.3%] and 403 men [22.7%]) underwent thyroidectomy for benign diseases: a total thyroidectomy was performed in 1649 subjects (92.7%) and a hemithyroidectomy in 128 (7.2%). The indications for surgery were multinodular non-toxic goiter in 1469 patients (82.66%), multinodular toxic goiter in 177 (9.96%), uninodular non-toxic goiter in 104 (5.85%), and uninodular toxic goiter (Plummer’s disease) in 27 patients (1.51%).
Thyroid nodules, studied by ultrasound, showed no suspicious sign of malignancy.
In the multinodular toxic or non-toxic goiter a total thyroidectomy was performed, whereas in uninodular toxic and non-toxic goiter a hemithyroidectomy was the treatment of choice.
Histopathological examination included the following: sections of fresh samples about 1 cm thick, which were fixed in formalin 4% for 24 h, embedded in paraffin and then further sectioned up to 4–5 µm.
The χ2 test was used to evaluate the association between the incidence of mPTC in total thyroidectomy and hemithyroidectomy and in toxic and non-toxic goiter.
The study has been performed in accordance with the Declaration of Helsinki and “good clinical practice” guidelines. All patients signed a consent form for the surgical procedure and for the storage and scientific use of their data.
Results
Histopathological examination identified 89 patients of ITC (5%; 89/1777); all were papillary thyroid carcinomas (PTCs), with a diameter less than or equal to 10 mm, therefore considered microPTC (mPTC). This group included 18 males (20.2%) and 71 females (79.8%). The median age was 46.7 years old (range 19–75 years old, standard deviation [SD] 13.53). In all, 28 patients (31.4%) were 40 years old or younger. All preoperative cytologies, if performed, were negative for malignant cells. Surgical procedures were total thyroidectomy in 83 patients (93.2%) and hemithyroidectomy in 6 (6.8%). Preoperative diagnosis was multinodular non-toxic goiter in the 83 cases of total thyroidectomy; in the 6 hemithyroidectomies the diagnosis was uninodular non-toxic goiter.
The percentage of mPTC in total thyroidectomy was 5.03% (83/1649), while in patients undergoing total thyroidectomy for multinodular non-toxic goiter it was 5.6% (83/1469). In partial thyroidectomy, the percentage of mPTC was 4.6% (6/128) while it was 5.7% in patients undergoing hemithyroidectomy for uninodular non-toxic goiter (6/104). Thus, the incidence of mPTC in patients with non-toxic thyroid disease was 5.6% (89/1573). No ITCs have been observed in multinodular and uninodular toxic goiter.
The mPTCs had a diameter between 2 and 10 mm, all cases meeting the Porto Proposal criteria [10]. There were no capsular or vascular invasion or lymph node metastasis. In 11 patients (12.3%) multifocal mPTCs were present, 7 (7.8%) of which were bilateral. Other pathological pictures associated with goiter/mPTC were the following: Hurthle cell adenoma in 2 patients (2.2%), lymphocytic thyroiditis in 21 (23.5%) and regressive, nonspecific phenomena in 19 (21.4%) (Tables 1 and 2).
The most frequent variant of mPTC was the classical form, which was found in 61 patients (68.5%), followed by the follicular variant in 25 patients (28%) and diffuse sclerosing, mixed and oncocitic Warthin-like variant each found in1 case (1.1%) (Fig. 1).
The 6 patients who received a hemithyroidectomy, underwent a completion thyroidectomy, without complication and without sign of tumor at the histopathological examination.
There was no difference between the incidence of mPTC in total thyroidectomy and hemithyroidectomy (P = 0.7, χ2 test) or the incidence in women and men (P = 0.5).
We also performed a χ2 test to compare the incidence of mPTC in non-toxic and toxic goiter and the association was statistically significant (P = 0.0009).
Follow-up comprised clinical examination, blood and instrumental tests for a minimum of 1.5 years and a maximum of 10 years and we have not observed any morbidity or mortality linked to the mPTCs.
Discussion
In our experience, in the 5% (n = 89) of the patients who underwent surgery for benign thyroid disease the final histology revealed a mPTC. In our data, the values were slightly lower than the average reported in the literature (Table 3; [1, 3, 4, 6, 11,12,13,14,15,16]). Our data must be evaluated in light of the fact that our inclusion criteria were very strict and selective, for example, we excluded TIR3 patients. An accurate diagnostic procedure allowed us to preoperatively diagnose a large number of mPTCs that were therefore excluded from our study.
Considering only our patients with non-toxic thyroid disease, the incidence of mPTC is 5.6% and this is closer to the values found in the literature: Tezelman et al. have found a frequency of 7.2%, [13], while Bradly et al. reported an incidence of 10% in multinodual goiter [12].
A crucial point, in our opinion, is the preparation of surgical specimens analyzed by the pathologist. This may partially explain the disparity of published data. More than 50% of carcinomas had a size between 1 and 5 mm and therefore, the use of thin sections represents a critical factor for early detection of occult carcinoma. In the literature, the histopathologic aspect has not been widely discussed and we have found a considerable heterogeneity in the description of the techniques used. Another factor that can bias the overall incidence is the sampling number. The studies that report a higher incidence of PTC have analyzed fewer patients [6, 11, 14, 15]. The authors that, instead, have considered a more numerous cohort reported incidences closer to ours [13, 16].
At the histopathological examination, we did not detect follicular cancer or poor differentiated cancers. All the 89 cases were papillary microcarcinomas, mostly showing a less aggressive variant (classical and follicular); only one case had a more aggressive subtype, the diffuse sclerosing variant, in line with the results reported in the literature [1, 3, 13,14,15,16,17,18,19,20].
In our study the female/male ratio was 3.9:1 (no difference in the incidences of mPTC by χ2 test), similar to the results of other recent studies. This finding may be explained by the higher number of diagnostic tests performed on women because of the greater prevalence of thyroid benign disease in females [15, 18].
As epidemiologic data, we highlight the association between the incidence of mPTC and non-toxic multinodular goiter. A few authors have analyzed this association, with different results [3, 15]. Miccoli et al. found a significant difference in the incidence between non-toxic and toxic disease, with a higher number of ITC in euthyroid patients [1]. Cerci et al. compared the incidence of ITC in toxic and non-toxic multinodular goiter, testing the idea that hyperthyroidism can be a protective factor, and found a similar incidence of cancer in the two groups [11].
The surgical approach in mPTC is still controversial. Regarding the mPTC diagnosed preoperatively, the 2015 American Thyroid Association guidelines suggest active surveillance instead of immediate surgery for low-risk mPTC [21] and many authors have followed this strategy [22, 23].
In 2016, Fukuoka et al. suggested active surveillance based on ultrasound criteria, such as calcification pattern and vascularization: lesions with stronger calcification and poorer vascularity showed a lower tendency to progress [22]. Considering risks and benefits of the surgical procedures, in carefully selected patients, a protocol based on active surveillance with periodic checks and ultrasound examinations can be proposed to low-risk patients [23].
Even the treatment options for ITC-mPTC are variable and different.
Some authors, followers of the so-called “Porto Proposal Criteria” introduced in 2003 by Rosai et al. [10], continue to support a “conservative” surgical approach on the basis of specific characteristics of mPTC: excellent prognosis, low aggressiveness and high responsiveness to metabolic radioiodine therapy.
Despite the overall excellent prognosis, in the literature mPTC is associated with a 1.0% disease-related mortality rate, a 5.0% lymph node recurrence rate, and a 2.5% distant metastasis rate [5]. Therefore, other authors, even taking into account the possibility of multifocality and the risks associated with a second surgery, support total thyroidectomy as the most acceptable procedure [6, 12, 24, 25]. Moreover, total thyroidectomy allows easier follow-up, in particular with regard to scintigraphic scan and thyroglobulin measurement [6].
The American and European guidelines suggest a conservative approach in patients with unifocal mPTC (classic or follicular variant) without extrathyroid infiltration and evidence of lymph node metastases: a completion thyroidectomy can be avoided in patients treated with lobectomy for benign disease [9, 21].
In our university hospital, the surgical approach for multinodular goiter is total thyroidectomy. It can be the procedure of choice because it is safe procedure and allows to achieve endocrine control and complete tumor resection if ITC is discovered, especially considering that the risks for major complications, (e.g., permanent hypoparathyroidism or recurrent laryngeal injury) are greater in reoperation than in primary operation for benign disease [6, 13]. In case of uninodular goiter partial thyroidectomy can be performed: the statistical analysis of our data confirm that the incidence of ITC in hemythyroidectomy is not significantly increased to justify total thyroidectomy in these patients. However, considering the above, in our opinion it is safer to perform a completion thyroidectomy if a mPTC is diagnosed during the histopathological examination, especially in the following: patients older than 50 years and with familial disposition for thyroid cancer; peripheral tumors larger than 5 mm and with aggressive variants.
As the majority of cases with incidental mPTC are low aggressive variants, we believe total thyroidectomy without prophylactic central neck dissection is appropriate, as also suggested by the American guidelines for small, noninvasive and clinically node-negative PTC [21]. Thus, if total thyroidectomy was the first therapeutic step, we just perform an endocrine and oncologic follow-up. If, however, at first a partial thyroidectomy was performed, we suggest a completion thyroidectomy without central neck dissection.
After surgery, radioiodine ablation is not recommended in patients with unifocal, low risk carcinoma or in the presence of multifocal tumor when the sum of all the foci is less than 1 cm, and thyroid hormone therapy should be administered in replacement doses [21].
We suggest that after surgery, patients should be followed with periodic ultrasound examination of the neck and measurement of serum thyroglobulin.
Take home message
-
A review of the literature and analysis of our data showed that mPTC is an important nosologic entity and its management is still controversial.
-
In our opinion, in case of multinodular non-toxic goiter, performing total thyroidectomy achieves the best results regarding the endocrine disease, and also the oncologic radicality if a mPTC is discovered.
-
In case of uninodular goiter, it is appropriate to perform a hemithyroidectomy and if a mPTC is found, we recommend a completion thyroidectomy, especially in determined cases.
-
The association between ITC-mPTC and non-toxic disease must be further investigated with other studies.
Abbreviations
- ITC:
-
incidental thyroid cancer
- mPTC:
-
papillary thyroid microcarcinoma
- PTC:
-
papillary thyroid carcinoma
References
Miccoli P, Minuto MN, Galleri D, et al. Incidental thyroid carcinoma in a large series of consecutive patients operated on for benign thyroid disease. ANZ J Surg. 2006;76(3):123–6. Mar.
Williams ED, Sobin LH. Who histological classification of thyroid tumors: a commentary on the second edition. Cancer. 1989;63(5):908–11.
Gelmini R, Franzoni C, Pavesi E, et al. Incidental thyroid carcinoma (itc): a retrospective study in a series of 737 patients treated for benign disease. Ann Ital Chir. 2010;81(6):421–7.
Antonelli W. Occult thyroid microcarcinomas in benign thyroid disease. Prev Res. 2016;5(4):130–3. https://doi.org/10.11138/Per/2016.5.4.130.
Chow SM, Law SC, Chan JK, et al. Papillary microcarcinoma of the thyroid-prognostic significance of lymph node metastasis. Cancer. 2003;98:31–40.
Sakorofas GH, Stafyla V, Kolettis T, et al. Microscopic papillary thyroid cancer as an incidental finding in patients treated surgically for presumably benign thyroid disease. J Postgrad Med. 2007;53(1):23–6.
Gelao L, Criscitiello C, Esposito A, et al. Dendritic cell-based vaccines: clinical applications in breast cancer. Immunotherapy. 2014;6(3):349–60. https://doi.org/10.2217/Imt.13.169.
Santangelo M, De Rosa P, Spiezia S, et al. Healing of surgical incision in kidney transplantation: a single transplant center’s experience. Transplant Proc. 2006;38(4):1044–6.
British Thyroid Association, Royal College of Physicians. British thyroid association guidelines for the management of thyroid cancer. 2nd ed. 2007. http://www.british-thyroidassociation.org/guidelines/.
Rosai J, Livoisi VA, Sobrinho-Simoes M, et al. Renaming papillary micro-carcinoma of the thyroid gland: the Porto Proposal. Int J Surg Pathol. 2003;11:249–51.
Cerci C, Cerci SS, Eroglu E, et al. Thyroid cancer in toxic and non-toxic multinodular goiter. Postgrad Med. 2007;53(3):157–60.
Bradly DP, Reddy V, Prinz RA, et al. incidental papillary carcinoma in patients treated surgically for benign thyroid disease. Surgery. 2009;146(6):1099–104.
Tezelman S, Borucu I, Senvuerek Giles Y, et al. The change in surgical practice from subtotal to near-total or total thyroidectomy in the treatment of patients with benign multinodular goiter. World J Surg. 2009;33(3):400–5.
Pezzolla A, Lattarulo S, Milella M, et al. Incidental carcinoma in thyroid pathology: our experience and review of the literature. Ann Ital Chir. 2010;81(3):165–9.
Askitis D, Efremidou EI, Karanikas M, et al. Incidental thyroid carcinoma diagnosed after total thyroidectomy for benign thyroid diseases: incidence and association with thyroid disease type and laboratory Markers. Int J Endocrinol. 2013; https://doi.org/10.1155/2013/451959.
Maturo A, Tromba L, De Anna L, et al. Incidental thyroid carcinomas. A Retrospective study. G Chir. 2017;38(2):94–101.
Piscitelli P, Piscitelli P, Santoriello A, Buonaguro FM, CROM, Human Health Foundation Study Group, et al. Incidence of breast cancer in italy:mastectomies and quadrantectomies performed between 2000 And 2005. J Exp Clin Cancer Res. 2009;19(28):86. https://doi.org/10.1186/1756-9966-28-86.
Criscitiello C, Giuliano M, Curigliano G, et al. surgery of the primary tumor in de novo metastatic breast cancer: to do or not to do? Eur J Surg Oncol. 2015;41(10):1288–92. https://doi.org/10.1016/J.Ejso.2015.07.013.
Kuo EJ, Goffredo P, Sosa JA, et al. Aggressive variants of papillary thyroid microcarcinoma are associated with extrathyroidal spread and lymph-node metastases: a population-level analysis. Thyroid. 2013;23(10):1305–11. https://doi.org/10.1089/Thy.2012.0563.
De Rosa P, Santangelo M, Scala A, et al. Difficult vascular conditions in kidney transplantation. Transplant Proc. 2006;38(4):1040–3.
Haugen BR, Alexander EK, Bible KC, et al. American Thyroid Association management guidelines for adult patients with thyroid nodules and differentiated thyroid cancer: the american thyroid association guidelines task force on thyroid nodules and differentiated thyroid cancer. Thyroid. 2015;26(1):1–133. https://doi.org/10.1089/Thy.2015.0020.
Fukuoka O, Sugitani I, Ebina A, Toda K, Kawabata K, et al. Natural history of asymptomatic papillary thyroid microcarcinoma: time-dependent changes in calcification and vascularity during active surveillance. World J Surg. 2016;40(3):529–37. https://doi.org/10.1007/S00268-015-3349-1.
Leboulleux S, Tuttle RM, et al. Papillary thyroid microcarcinoma: time to shift from surgeryto active surveillance? Lancet Diabetes Endocrinol. 2016;4(11):30180–2. https://doi.org/10.1016/S2213-8587.
Santangelo M, Clemente M, Spiezia S, et al. Wound complications after kidney transplantation in nondiabetic patients. Transplant Proc. 2009;41(4):1221–3. https://doi.org/10.1016/J.Transproceed.2009.03.098.
Santangelo M, Zuccaro M, De Rosa P, et al. Older kidneys donor transplantation: five years experience without biopsy and using clinical laboratory and macroscopic anatomy evaluation. Transplant Proc. 2007;39(6):1835–7.
Author information
Authors and Affiliations
Contributions
All authors contributed significantly to the present research and reviewed the entire manuscript. G. Peluso contributed to execution of the study, to the analysis and interpretation of the data and to the drafting and editing of the manuscript. S. Masone reviewed and approved the final manuscript and performed some of the surgical operations. C. Criscitiello participated in the editing and review of the manuscript. S. Campanile, C. Dodaro and A. Calogero contributed to the review of the literature. P. Incollingo contributed to the editing of the manuscript and the English language. G. Minieri and M. Menkulazi edited the tables and the image. A. Scotti, V. Tammaro, A. Jamshidi, L. Pelosio, M. Caggiano and N. Carlomagno performed some of the surgical operations. M.L. Santangelo contributed to the design and the execution of the study, performed some of the surgical operations, reviewed and approved the final manuscript.
Corresponding author
Ethics declarations
Conflict of interest
G. Peluso, S. Masone, S. Campanile, C. Criscitiello, C. Dodaro, A. Calogero, P. Incollingo, G. Minieri, M. Menkulazi, A. Scotti, V. Tammaro, A. Jamshidi, L. Pelosio, M. Caggiano, N. Carlomagno, and M.L. Santangelo declare that they have no competing interests.
Ethical standards
The study has been performed in accordance with the Declaration of Helsinki and “good clinical practice” guidelines. Written informed consent was obtained from the patients for utilization of their data. All data generated or analyzed during this study are included in this published article and are available from the corresponding author.
Additional information
Publisher’s Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if changes were made. The images or other third party material in this article are included in the article’s Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article’s Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
Peluso, G., Masone, S., Campanile, S. et al. Incidental thyroid papillary microcarcinoma on 1777 surgically treated patients for benign thyroid disease. memo 13, 126–133 (2020). https://doi.org/10.1007/s12254-019-00567-y
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12254-019-00567-y