Abstract
Background/purpose
Many studies suggest that insulin resistance in obese patients bridges mental illness. Our objective was to identify the association between levels of depression and anxiety with insulin resistance, and its relationship with obesity and abdominal obesity
Methods
A cross-sectional analytical study was carried out in Honduras. Sociodemographic variables, anthropometric parameters, HOMA index, and level of severity of anxiety and depression were collected, and a descriptive, bivariate, and multivariate were performed.
Results
In a sample of 381 adult patients, the bivariate analysis showed a statistic association of insulin resistance with all remaining variables. However, multivariate analysis showed a significative association of anxiety with BMI, depression, waist circumference, and insulinemia, while depression was associated with HOMA, anxiety, insulinemia, glycemia, and waist circumference.
Conclusions
Our results provide important evidence of a direct and growing association between HOMA-IR and the severity of depression, and indirectly with anxiety. Secondarily, also with anthropometric factors (BMI and WC), traditionally associated with cardiovascular risk. This finding has important implications both for the early diagnosis of these mental pathologies, taking into account HOMA-IR values, and for preventive interventions focused on maintaining blood insulin levels.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
In the past few years, there has been an interest in studying the possible association between biochemical insulin resistance (IR), developed in the context of abdominal obesity, and the clinical manifestations of psychiatric diseases such as anxiety and depression. There is scientific evidence showing insulin resistance as the main pathophysiological substrate of these mental disorders [1, 2]. In the connection among all these factors, it is worth wondering which disorder is the source and support of the others.
In general, nearly 13% of the world’s adult population is obese [3]. In case of the capital city of Honduras, Tegucigalpa, the prevalence values of obesity in women and men aged between 20 and 64 years are 27% and 18%, respectively [4]. On the other hand, in this same population, the prevalence of the depressive syndrome reaches 26.4%, whereas that of anxiety is 5.7%. Curiously, it has been observed that excess weight and morbid abdominal circumference are frequently concomitant with these affective disorders in a large part of this population [5, 6].
Obesity is associated with an excessive accumulation of abdominal fat and to insulin resistance [7]. The metabolic changes linked to obesity seem to exert a negative repercussion on the psychological sphere [8]. Consequently, in a number of studies, it has been observed that obesity is a predictor of long-term depression [9] or also the coexistence of abdominal obesity with anxiety and depression [10]. In addition, it seems that factors such as the accumulation of perivisceral fat and the distribution of body fat are related with higher anxiety and depression scores in both genders [11]. Even so, there is controversy regarding this issue, since some studies have suggested a weak or null association between metabolic syndrome and anxiety or depression [12].
Many studies suggest that the absence or reduction of sensitivity to insulin in obese patients establishes a connection with mental ailments. Therefore, a number of studies illustrate this bidirectional relationship showing that the depression and anxiety symptoms are positively correlated with the fasting plasma insulin concentrations, and inversely correlated with sensitivity to insulin [13]. Additionally, this alteration produces adaptive metabolic changes positively correlated with the clinical manifestations of depression [14].
At the brain level, a number of experimental studies have confirmed the neuroprotective function of insulin, ensuring synaptic plasticity. However, the insulin receptor dysfunction leads to an increase in dopamine degradation, which can be the basis for the depressive symptoms [2]. Furthermore, mechanisms have been proposed in which inadequate insulin signaling modifies the neurogenesis of the hippocampus, synaptic plasticity, the response of the hypothalamic-pituitary-adrenal (HPA) axis, and the reward system, which would favor the onset of depressive states [15].
Factors associated with geography, such as the number of sunlight hours, the urban organization [16] or even psychosocial factors inherent to each culture [17] might exert a direct or indirect influence on the relationship between biological factors (biochemical or anthropometric) and this type of mental health problems. Given the above, and due to the still limited availability of information related to different environments, this study was designed with the objective of identifying the association of depression and anxiety with IR, and of determining how the degree of these pathologies influences such association. In addition, it intends to elucidate the relationship between this association and obesity. All of the above will allow proposing a new approach on treatment lines that may assist in the therapeutic management of these patients.
Material and methods
Design
A cross-sectional study was carried out.
Study population
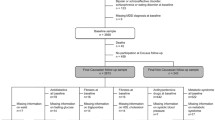
Adult patients presenting anxiety and/or depression symptoms and signs, who attended the Dr. Mario Mendoza Acute Psychiatric Hospital between February 2018 and August 2020, referred from Primary Health Care centers across the entire country were included.
The exclusion criteria were (i) pregnancy; (ii) complicated chronic disease; (iii) use in the last 6 months of antidepressants, anxiolytics, anticolinergics, antihistamines, antiarrhythmics, antihypertensives, digitalis drugs, beta-blockers, thiazide diuretics, antibiotics, non-steroidal anti-inflammatory drugs (NSAIDs), anticonvulsants, glucocorticosteroids/anabolics, or oral contraceptives; (iv) smoking habit and/or alcoholism; and (v) drug use or abstinence (cocaine and amphetamines).
Data collection
The data collection was carried out in a two-step procedure: (i) in the medical consultation the specific variables of the study (anthropometric variables, anxiety and depression) were taken together with the identification data of the patient and analytical tests for biochemical variables were requested. (ii) Subsequently, through the hospital’s electronic registry, the results of biochemical variables and sociodemographic data of the patients were obtained.
Anthropometric measures
The body mass index (BMI) was calculated, in kg/m2.Abdominal obesity was determined with an anatomical tape by measuring the waist circumference (WC) and categorized as follow: (i) in men: 94–101 cm, increased cardiovascular risk (ICR); ≥ 102cm, high cardiovascular risk (HCR); (ii) in women: 80–87 cm, ICR; ≥ 88 cm, HCR.
Determination of biochemical insulin resistance
The HOMA index was measured to determine insulin resistance considering the following equation:
HOMA = \( \frac{f\mathrm{asting}\ \mathrm{glycaemia}\ \left(\frac{\mathrm{mg}}{\mathrm{dl}}\right)\ \mathrm{x}\ \mathrm{insulinemia}\left(\frac{\upmu \mathrm{Ui}}{\mathrm{ml}}\right)\ }{405} \)
Indicating insulin resistance with HOMA index values ≥ 3.2 [18].
Determination of the depression and anxiety severity levels
The Hamilton scales for anxiety and depression were used. The Hamilton scale for depression is a 17-item questionnaire. Its total score varies from 0 to 52. The following cutoff points are suggested: not depressed: 0–7 mild/minor depression: 8–13 moderate depression: 14–18 severe depression: 19–22 very severe depression: >23 [19]. The Hamilton anxiety rating scale-HARS has 14 items with a total score ranged from 0 to 56 points and classified as follows: 0–5 points: no anxiety, 6–14 points: mild anxiety, >15 points: moderate/severe anxiety [20].
Data analysis
The IBM SPSS Statistics v25 program was used. A descriptive analysis of the qualitative variables through of absolute and percentage frequencies, and quantitative variables by means of central tendency, dispersion, and position measures was performed. It was assessed if IR (as a dichotomous variable) was statistically associated with the outcome variables (anxiety and depression), as well as with other independent variables (sociodemographic and clinical). For qualitative variables, the inference was performed through Pearson’s Chi-square test or Fisher’s exact test and the effect size was measured through odds ratios (OR). For the quantitative variables, the comparison of means test was performed, and the effect size was measured with Cohen’s d. A correlation matrix between quantitative variables was also constructed. Finally, multivariate regression models were constructed to avoid confusion biases resulting from the non-randomization of the sample. In these models, adjusted ORs of each variable and the significance of the models themselves were obtained. In all the aforementioned analyses, significance was established with p-values below 0.05.
The calculation of the sample size for the comparison of proportions or means requires previous information that we lack because this is the first study carried out in our area with this objective. Therefore, it is an exploratory analysis; however, the Gpower software was used to calculate the post hoc power (1-beta) of the analyses by introducing the sample size obtained, a significance of 0.05 and the observed effect size, accepting only results higher than 0.8 which is the standard value commonly defines an analysis with sufficient statistical power.
Ethical criteria
Before the study was initiated, its protocol was approved by the Medical Ethics Committee (CR-061) of the Dr. Mario Mendoza Acute Psychiatric Hospital in Tegucigalpa. Once informed about the study dynamics and objective, the participants voluntarily signed an informed consent before their inclusion. The study was conducted according to the recommendations set forth in the Declaration of Helsinki for biomedical research studies in human beings. No invasive tests or samplings were required besides those derived from the routine care practice, and the information was duly coded to anonymize the clinical data prior to their tabulation and analysis.
Results
A sample consisting of 381 adult patients aged between 24 and 59 years was obtained, with a mean/standard deviation of 43±11.2 years, and with majority of females (74%).
According to the HOMA index, an IR rate of 81.1% was observed in 309 patients, who were distributed into the following degrees: 6 (1.9%), mild; 140 (45.3%), moderate; 137 (44.3%), high; and 26 (8.4%), severe.
Table 1 assesses the statistical association between IR and other qualitative variables. A statistical association was observed with all the variables (gender, BMI, waist circumference, and the “anxiety” and “depression” outcome variables). ORs of the ordinal categories presented a growing trend in each case, reflecting an increasingly higher risk at each step up in the levels.
Table 2 shows a statistical association analysis similar, but with numerical variables, observing such type of association in all the variables, except for age. Nevertheless, Cohen’s d, which considers an important effect with values above 0.8, was obtained only for the insulinemia values and the scores obtained in the Hamilton scales.
The correlation matrix (Table 3) showed that most of the variables were significantly correlated, but with irrelevant correlation coefficients. The best correlation coefficients were obtained for the HOMA-insulinemia, BMI-weight, and Hamilton’s anxiety-depression score pairs. These two scores obtained correlations coefficients similar to HOMA, whose value reached 0.5, indicating a moderate correlation.
Finally, for each outcome (depression and anxiety), two types of multivariate models were conducted: logistic (upper part of Table 4) and linear (lower part of Table 4).
The models for anxiety showed that the scores obtained in the depression scale and in insulinemia were significant. Furthermore, the logistic regression model also showed statistical significance for BMI and waist circumference. Similarly, in the models for depression, insulinemia, HOMA, and the scores of anxiety scale were significant; additionally, each model showed the statistical association with other variables. Some variables were not significant, but were kept as part of the model because, when they were removed, the quality of the model was reduced.
The quality of the logistic regression models has been expressed through the Akaike information criterion (AIC), and the quality of the linear models is shown through their statistical significance and both presented p< 0.001.
Discussion
Depression and anxiety are highly prevalent health problems in the world population, and seem to have a metabolic substrate related to IR [21,22,23,24].
We found an association of depression and anxiety with biochemical IR (HOMA) as qualitative (Table 1), as quantitative (Table 2) bivariate analyses. Furthermore, higher ORs for anxiety and depression were observed for IR group and these risks increased according to the severity of the pathologies. A correlation between these three variables was also observed. However, the multivariate models have shown an association between the HOMA-depression binomial on the one hand (adjusted OR=6.67) and the anxiety-depression binomial variables. The HOMA-anxiety association observed in the bivariate analysis has not been confirmed in the multivariate models, evidencing a confusion bias. Nevertheless, all analysis performed showed the statistical association between the HOMA and depression values, either considered as continuous or as categorical variables, also showing clinical relevant effect size. These results would imply that there is a hormone-related component, insulinemia, acting as a risk factor for depression and, indirectly, for anxiety due to the association between them [25]. Previous studies have confirmed a positive relationship between IR and depression, although not with anxiety [14].
Obesity is one of the most important risk factors for health, and one of its main complications is insulin resistance [26]. This association, as is the case in other studies [27–28], has been verified in our results. Due to their relationship with obesity and cardiovascular diseases [29], BMI and abdominal waist circumference were evaluated finding statistical significance in the logistic regression models for both parameters; BMI, for the anxiety model, and WC, for both anxiety and for depression models. However, they were not significant in the linear models. This could be due to that the changes in the numerical values from the anxiety and depression tests associated with these independent variables were small, although sufficient for changing the subjects from healthy to illness categories. It means that the changes observed were numerically small, but clinically relevant. Thus, as previously described [5, 30], obesity, through BMI and WC, is associated with depression and anxiety, either due to endocrine-based physiological mechanisms or through psychosocial factors such as self-perception of body image or self-esteem, widely associated with obese individuals. A previous study showed that abdominal obesity was associated to major depressive disorder, but not with generalized anxiety, although it included adults younger than 22 years only [31].
Regarding gender, women in our study present almost twice the risk (OR=1.92) for IR. However, it is described that healthy women present higher sensitivity to insulin than men [32, 33]. This discrepancy can be related to the age distribution among women, since half of them were over 45 years old and 25% were between 52 and 59 years old. Therefore, they were close or already going through menopause, and there could be a loss of sensitivity to insulin and an increased abdominal adiposity related with estrogen deficit [34].
Nevertheless, in the multivariate models, the gender factor did not attain statistical significance either for depression or anxiety, with only a statistical trend being observed in the linear regression model for depression indicating that female gender is a risk factor for depression (Table 4). Statistical significance was probably not reached due to the sample size. However, when the gender variable was removed the model fit (adjusted R2=0.63) worsened, thus confirming the influence of this variable. In fact, it has been described that depression is linked to gender, being more prevalent in women [35, 36] and showed a greater association between depression and IR in women than in men [24].
Regarding age, in the bivariate analysis little association was observed, finding the best statistical significance between age and depression, although with a negligible correlation coefficient. In the multivariate analysis, only the linear regression model for depression presents certain statistical trend of the effect of age, not attaining significance. In this sense, a number of studies corroborate higher prevalence of depression with age [31], although association between IR and depression in adolescents has also been reported [37, 38].
Even so, the effect of age or gender on the association between IR and depression/anxiety might also be explained by other factors such as poverty, violence, and gender and ethnic inequalities [35], an aspect not addressed in this research.
Our results have important clinical implications, since the biological factors studied can be adopted for the early diagnoses of these pathologies and they are also associated with cardiovascular diseases, which are the leading cause of death worldwide [39].
Both the cardiovascular problems and the risk factors associated with the depression and anxiety disorders are very frequent reasons for consultation appointments in primary care, reason why the correct counseling from primary care to maintain a healthy anthropometry and a good insulin sensitivity could significantly reduce the morbi-mortality of the general population at the physical, psychological and emotional levels.
Strengths and limitations
Cross-sectional studies present the limitations inherent to observational studies; however, they are cost-effective and useful to identify prevalence values and risk factors associated with health problems.
The main limitation is the non-randomization during the recruitment of patients, but this has been solved by multivariate analysis, preventing confusion bias derived from a single bivariate analysis, as is the case in previous studies [5]. Furthermore, previous studies have reported the statistical association between IR-HOMA and depression, but many of them did not report the effect size [21, 24], while others that did, obtained lower odd ratios [23].
Finally, the sample size might have been insufficient to attain significance in some variables; however, the study has enough statistical power to meet the objectives set forth. Thus, these limitations do not affect the internal validity of the study to meet the objectives set forth for the Honduran population.
Conclusion
These results provide important evidence of a direct and increasing association between HOMA-IR and the severity of depression and, indirectly, with anxiety. Therefore, insulin resistance is an important risk factor for the onset of these mental ailments. Secondarily, evidence is also shown of the association between anthropometric factors (BMI and WC), traditionally associated with cardiovascular risk, and the presence of these mental health problems.
This finding has important implications both for the early diagnosis of these mental pathologies, considering the HOMA-IR values, and for preventive interventions focused on maintaining the levels of blood insulin.
References
Hiles SA, Révész D, Lamers F, Giltay E, Penninx BWJH. Bidirectional prospective associations of metabolic syndrome components with depression, anxiety, and antidepressant use. Depress Anxiety. 2016;33(8):754–64. https://doi.org/10.1002/da.22512.
Kleinridders A, Cai W, Cappellucci L, Ghazarian A, Collins WR, Vienberg SG, Pothos EN, Kahn CR. Insulin resistance in brain alters dopamine turnover and causes behavioral disorders. PNAS. 2015;112:3463–8. https://doi.org/10.1073/pnas.1500877112.
WHO. La OMS revela las principales causas de muerte y discapacidad en el mundo: 2000-2019. n.d.. WHO. Retrieved April 19, 2021, from https://www.who.int/es/news/item/09-12-2020-who-reveals-leading-causes-of-death-and-disability-worldwide-2000-2019
OPS/OMS Honduras - OPS/OMS Honduras. n.d.. OPS, 2020. Retrieved March 23, 2021, from https://www.paho.org/hon/index.php?option=com_content&view=article&id=1359:gobierno-y-ops-oms-promueven-estilos-de-vida-saludable-en-fuerza-laboral&Itemid=0
Bocicor AE, Buicu G, Varga A, Tatar R, Daniela S, Tilea I, Gabos-Grecu I. Association between increased waist circumference and depression and anxiety trend. Acta Med Marisiensis. 2015;61:87–90. https://doi.org/10.1515/amma-2015-0028.
Gomes AP, Soares ALG, Menezes AMB, Assunção MC, Wehrmeister FC, Howe LD, Gonçalves H. Adiposity, depression and anxiety: interrelationship and possible mediators. Rev Saude Publica. 2019;53:103. https://doi.org/10.11606/S1518-8787.2019053001119.
Ros Pérez M, Medina-Gómez G. Obesity, adipogenesis and insulin resistance. Endocrinol. Nutr. (English Edition). 2011;58(7):360–9. https://doi.org/10.1016/j.endoen.2011.05.004.
Hryhorczuk C, Sharma S, Fulton SE. Metabolic disturbances connecting obesity and depression. Front Neurosci. 2013;7:177. https://doi.org/10.3389/fnins.2013.00177.
Luppino FS, de Wit LM, Bouvy PF, Stijnen T, Cuijpers P, Penninx BW, Zitman FG. Overweight, obesity, and depression: a systematic review and meta-analysis of longitudinal studies. Arch Gen Psychiatry. 2010;67(3):220–9. https://doi.org/10.1001/archgenpsychiatry.2010.2.
Jagielski AC, Brown A, Hosseini-Araghi M, Thomas GN, Taheri S. The association between adiposity, mental well-being, and quality of life in extreme obesity. PLoS ONE. 2014;9(3):e92859. https://doi.org/10.1371/journal.pone.0092859.
Rajan TM, Menon V. Psychiatric disorders and obesity: a review of association studies. J Postgrad Med. 2017;63(3):182–90. https://doi.org/10.4103/jpgm.JPGM_712_16.
Akbari H, Sarrafzadegan N, Aria H, Garaei AG, Zakeri H. Anxiety but not depression is associated with metabolic syndrome: the Isfahan Healthy Heart Program. J Res Med Sci. 2017;22:90. https://doi.org/10.4103/jrms.JRMS_288_16.
Shomaker LB, Goodman E. An 8-year prospective study of depressive symptoms and change in insulin from adolescence to young adulthood. Psychosom Med. 2015;77(8):938–45. https://doi.org/10.1097/PSY.0000000000000230.
Shomaker LB, Tanofsky-Kraff M, Young-Hyman D, Han JC, Yanoff LB, Brady SM, Yanovski SZ, Yanovski JA. Psychological symptoms and insulin sensitivity in adolescents. Pediatr Diabetes. 2010;11(6):417–23. https://doi.org/10.1111/j.1399-5448.2009.00606.x.
Lyra E, Silva NM, Lam MP, Soares CN, Munoz DP, Milev R, De Felice FG. Insulin resistance as a shared pathogenic mechanism between depression and type 2 diabetes. Front Psychiatry. 2019;10:57. https://doi.org/10.3389/fpsyt.2019.00057.
Evans GW. The built environment and mental health. J Urban Health. 2003 Dec;80(4):536–55. https://doi.org/10.1093/jurban/jtg063.
Arroyo-Johnson C, Mincey KD. Obesity epidemiology worldwide. Gastroenterol Clin N Am. 2016;45(4):571–9. https://doi.org/10.1016/j.gtc.2016.07.012.
Hernández J, Tuero A, Vargas D. Usefulness of HOMA-IR index with an only insulinemia determination to diagnose an insulin resistance [Utilidad del índice HOMA-IR con una sola determinación de insulinemia para diagnosticar resistencia insulínica]. Rev Cuba Endocrinol. 2011;22(2):69–77.
Ramos-Brieva JA, Cordero A. Validation of the Spanish version of the Hamilton Scale for Depression [Validación de la versión castellana de la Escala de Hamilton para la Depresión]. Actas Luso Esp Neurol Psiquiatr Cienc Afines. 1986;14:324–34.
Lobo A, Chamorro L, Luque A, Dal-Ré R, Badia X, Baró E, Grupo de Validación en Español de Escalas Psicométricas (GVEEP). Validación de las versiones en español de la Montgomery-Asberg Depression Rating Scale y la Hamilton Anxiety Rating Scale para la evaluación de la depresión y de la ansiedad [Validation of the Spanish versions of the Montgomery-Asberg depression and Hamilton anxiety rating scales]. Med Clin. 2002;118(13):493–9. https://doi.org/10.1016/s0025-7753(02)72429-9.
Austin AW, Gordon JL, Lavoie KL, Arsenault A, Dasgupta K, Bacon SL. Differential association of insulin resistance with cognitive and somatic symptoms of depression. Diabet Med. 2014;31(8):994–1000. https://doi.org/10.1111/dme.1246.
Jaremka LM, Pacanowski CR. Social anxiety symptoms moderate the link between obesity and metabolic function. Psychoneuroendocrinology. 2019;110:104425. https://doi.org/10.1016/j.psyneuen.2019.104425.
Lee JH, Park SK, Ryoo JH, Oh CM, Mansur RB, Alfonsi JE, Cha DS, Lee Y, McIntyre RS, Jung JY. The association between insulin resistance and depression in the Korean general population. J Affect Disord. 2017;208:553–9. https://doi.org/10.1016/j.jad.2016.10.027.
Webb M, Davies M, Ashra N, Bodicoat D, Brady E, Webb D, Moulton C, Ismail K, Khunti K. The association between depressive symptoms and insulin resistance, inflammation and adiposity in men and women. PLoS ONE. 2017;12(11):e0187448. https://doi.org/10.1371/journal.pone.0187448.
Kalin NH. The critical relationship between anxiety and depression. Am J Psychiatry. 2020;177(5):365–7. https://doi.org/10.1176/appi.ajp.2020.20030305.
Barazzoni R, Gortan Cappellari G, Ragni M, Nisoli E. Insulin resistance in obesity: an overview of fundamental alterations. Eat Weight Disord. 2018;23(2):149–57. https://doi.org/10.1007/s40519-018-0481-6.
Mirrakhimov AE, Lunegova OS, Kerimkulova AS, Moldokeeva CB, Nabiev MP, Mirrakhimov EM. Cut off values for abdominal obesity as a criterion of metabolic syndrome in an ethnic Kyrgyz population (Central Asian region). Cardiovasc Diabetol. 2012;11:16. https://doi.org/10.1186/1475-2840-11-16.
Velásquez-Rodríguez CM, Velásquez-Villa M, Gómez-Ocampo L, Bermúdez-Cardona J. Abdominal obesity and low physical activity are associated with insulin resistance in overweight adolescents: a cross-sectional study. BMC Pediatr. 2014;14:258. https://doi.org/10.1186/1471-2431-14-258.
Cercato C, Fonseca FA. Cardiovascular risk and obesity. Diabetol Metab Syndr. 2019;11:74. https://doi.org/10.1186/s13098-019-0468-0.
Ahlberg AC, Ljung T, Rosmond R, McEwen B, Holm G, Akesson HO, Björntorp P. Depression and anxiety symptoms in relation to anthropometry and metabolism in men. Psychiatry Res. 2002;112(2):101–10. https://doi.org/10.1016/s0165-1781(02)00192-0.
Gómez-Restrepo C, Bohórquez A, Pinto Masis D, Gil Laverde JF, Rondón Sepúlveda M, Díaz-Granados N. Prevalencia de depresión y factores asociados con ella en la población colombiana [The prevalence of and factors associated with depression in Colombia]. Rev Panam Salud Publica. Spanish 2004;16(6):378-386. https://doi.org/10.1590/s1020-49892004001200003.
Geer EB, Shen W. Gender differences in insulin resistance, body composition, and energy balance. Gend Med. 2009;6(Suppl 1):60–75. https://doi.org/10.1016/j.genm.2009.02.002.
Tramunt B, Smati S, Grandgeorge N, Lenfant F, Arnal JF, Montagner A, Gourdy P. Sex differences in metabolic regulation and diabetes susceptibility. Diabetologia. 2020;63(3):453–61. https://doi.org/10.1007/s00125-019-05040-3.
Mauvais-Jarvis F, Clegg DJ, Hevener AL. The role of estrogens in control of energy balance and glucose homeostasis. Endocr Rev. 2013 Jun;34(3):309–38. https://doi.org/10.1210/er.2012-1055.
Matud MP, Guerrero K, Matías RG. Relevance of sociodemographic variables in gender differences in depression [Relevancia de las variables sociodemográficas en las diferencias de género en depresión]. Int J Clin Health Psychol. 2006;6(1):7–21.
Salk RH, Hyde JS, Abramson LY. Gender differences in depression in representative national samples: meta-analyses of diagnoses and symptoms. Psychol Bull. 2017;143(8):783–822. https://doi.org/10.1037/bul0000102.
Singh MK, Leslie SM, Packer MM, Zaiko YV, Phillips OR, Weisman EF, Wall DM, Jo B, Rasgon N. Brain and behavioral correlates of insulin resistance in youth with depression and obesity. Horm Behav. 2019;108:73–83. https://doi.org/10.1016/j.yhbeh.2018.03.009.
Perry BI, Khandaker GM, Marwaha S, Thompson A, Zammit S, Singh SP, Upthegrove R. Insulin resistance and obesity, and their association with depression in relatively young people: findings from a large UK birth cohort. Psychol Med. 2020;50(4):556–65. https://doi.org/10.1017/S0033291719000308.
GBD 2013 Mortality and Causes of Death Collaborators. Global, regional, and national age-sex specific all-cause and cause-specific mortality for 240 causes of death, 1990-2013: a systematic analysis for the Global Burden of Disease Study 2013. Lancet. 2015;385(9963):117-71. https://doi.org/10.1016/S0140-6736(14)61682-2.
Acknowledgments
Juan Pablo: conception and design, acquisition of data, clinical interpretation of data, writing. Rubén: design, analysis of data and statistical interpretation, and final approval of the version to be published. Mercedes: conception and design, clinical interpretation of data, writing and final approval of the version to be published.
Funding
Open Access funding provided thanks to the CRUE-CSIC agreement with Springer Nature.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Ethics approval and consent to participate
This was a research involving human participants. All participants were informed about objectives and dynamic of the study and all of them affirmed that they understood this information and signed the informed consent to participate in the study. The study protocol was previously reviewed and accepted by a competent ethics committee as indicated in the methods section.
Conflict of interest
The authors declare no competing interests.
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if changes were made. The images or other third party material in this article are included in the article's Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article's Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
Díaz-Carías, J.P., Morilla Romero de la Osa, R. & Cano-Rodríguez, M. Relationship between insulin-biochemical resistance levels and the degree of depression and anxiety in patients from Honduras. Int J Diabetes Dev Ctries 43, 750–757 (2023). https://doi.org/10.1007/s13410-022-01113-z
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s13410-022-01113-z