Abstract
Rucaparib is an oral small-molecule poly(ADP-ribose) polymerase inhibitor indicated for patients with recurrent ovarian cancer in the maintenance and treatment settings and for patients with metastatic castration-resistant prostate cancer associated with a deleterious BRCA1 or BRCA2 mutation. Rucaparib has a manageable safety profile; the most common adverse events reported were fatigue and nausea in both indications. Accumulation in plasma exposure occurred after repeated administration of the approved 600-mg twice-daily dosage. Steady state was achieved after continuous twice-daily dosing for a week. Rucaparib has moderate oral bioavailability and can be dosed with or without food. Although a high-fat meal weakly increased maximum concentration and area under the curve, the effect was not clinically significant. A mass balance analysis indicated almost a complete dose recovery of rucaparib over 12 days, with metabolism, renal, and hepatic excretion as the elimination routes. A population pharmacokinetic analysis of rucaparib revealed no effect of age, sex, race, or body weight. No starting dose adjustments were necessary for patients with mild-to-moderate hepatic or renal impairment; the effect of severe organ impairment on rucaparib exposure has not been evaluated. In patients, rucaparib moderately inhibited cytochrome P450 (CYP) 1A2 and weakly inhibited CYP3As, CYP2C9, and CYP2C19. Rucaparib weakly increased systemic exposures of oral contraceptives and oral rosuvastatin and marginally increased the exposure of oral digoxin (a P-glycoprotein substrate). In vitro studies suggested that rucaparib inhibits transporters MATE1, MATE2-K, OCT1, and OCT2. No clinically meaningful drug interactions with rucaparib as a perpetrator were observed. An exposure–response analysis revealed dose-dependent changes in selected clinical efficacy and safety endpoints. Overall, this article provides a comprehensive review of the clinical pharmacokinetics, pharmacodynamics, drug–drug interactions, effects of intrinsic and extrinsic factors, and exposure–response relationships of rucaparib.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Rucaparib has an absolute oral bioavailability of 36%. Steady state is reached following a 1-week treatment. Rucaparib can be dosed with or without food. |
Rucaparib is eliminated through both metabolism and excretion. |
Body weight, body mass index, age, race, sex, cytochrome P450 phenotypes, mild-to-moderate renal or hepatic impairment, and concomitant proton pump inhibitors have no clinically significant effects on the pharmacokinetics of rucaparib. |
Rucaparib has a manageable clinical drug–drug interaction profile as a perpetrator of cytochrome P450 enzymes and transporters. |
An exposure–response analysis suggests dose-dependent efficacy and safety and supports the rucaparib starting dose of 600 mg twice daily. |
1 Introduction
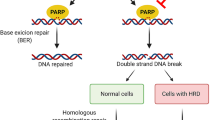
The 17-member poly(ADP-ribose) polymerase (PARP) superfamily of nuclear enzymes plays a critical role in the repair of DNA damage via the base excision repair/single-strand break repair pathway [1,2,3]. Poly(ADP-ribose) polymerase inhibition results in unrepaired single-strand breaks progressing to double-strand breaks, which normal cells mend by homologous recombination (HR) mediated via BRCA1 and BRCA2 (BRCA) [4,5,6,7]. However, as tumor cells harboring a BRCA mutation or other HR deficiency (HRD) are not capable of error-free repair of double-strand breaks, PARP inhibition in this setting leads to synthetic lethality [8,9,10,11,12,13,14,15,16,17,18,19,20].
Rucaparib, formerly known as AG-014699 and PF-01367338, is a potent, orally available, small-molecule inhibitor of PARP1, PARP2, and PARP3 [15, 21,22,23]. It is approved in Europe as monotherapy for recurrent ovarian cancer in the treatment setting based on the results from the Study 10 (NCT01482715) and ARIEL2 (NCT01891344) trials, and approved in the USA and Europe in the maintenance setting based on the results from the ARIEL3 (NCT01968213) trial [21, 24]. Rucaparib is also approved in the USA for the treatment of patients with metastatic castration-resistant prostate cancer (mCRPC) associated with a deleterious BRCA mutation based on the results from the TRITON2 (NCT02952534) study [21].
This review discusses the pharmacokinetic (PK) and pharmacodynamic properties, drug–drug interactions (DDIs), special populations, and exposure–response relationships based on published studies from the rucaparib research and development program, both preclinical and clinical, in order to provide guidance on its use in patients with cancer. In the past decade, a number of PARP inhibitors have been successfully developed, with similarities and differences in clinical pharmacology, safety, and efficacy systemically assessed [25,26,27,28]. However, rucaparib clinical pharmacology data from previous publications are incomplete. Thus, this systematic review’s objective is to summarize the available data to best define the clinical pharmacology profile of rucaparib.
2 Discovery and Mode of Action
Rucaparib was identified through a systematic process based on in vitro structure–activity relationships and in vivo evaluation of radio- and chemopotentiation [22]. Rucaparib was tested along with 42 structurally diverse, potent PARP inhibitors with inhibitory constants for PARP1 that range from 1.4 to 5.1 nmol/L [22]. Of the panel of candidate PARP inhibitors tested, rucaparib, a benzimidazole with a partition coefficient of 2.4, enhanced temozolomide antitumor activity the most without body weight loss in mice bearing SW620 xenografts [22]. The chemical structure and physicochemical properties of rucaparib are shown in Fig. 1. Rucaparib is synthesized as the camsylate salt, a white to pale yellow powder that is formulated into a tablet for oral use [21].
Chemical structure of rucaparib camsylate [21]
Rucaparib works by promoting synthetic lethality, where the disruption of two DNA repair pathways results in the accumulation of DNA damage and cell death [29]. Poly(ADP-ribose) polymerases are recruited to the sites of single-strand breaks where they cleave nicotinamide adenine dinucleotide to catalyze the formation of poly(ADP-ribose) [PAR] polymers on target nuclear proteins. These PAR polymers act as a signal to recruit additional proteins and initiate the repair of damaged DNA. Crystallographic analysis revealed that rucaparib mimics the nicotinamide moiety of nicotinamide adenine dinucleotide and binds to the PARP active site. In cell-free in vitro assays, rucaparib had high binding affinity for PARP1 (inhibitory constant 1.4 nmol/L) and PARP2 (inhibitory constant 0.17 nmol/L) [22]. The rucaparib concentration required to inhibit PARP1, PARP2, and PARP3 function by 50% (IC50) is 0.8, 0.5, and 28 nM, respectively.
Cytotoxicity, DNA damage, and HR repair after 24-h exposure to rucaparib was examined in nine human ovarian, breast, and pancreatic cancer cell lines (BRCA wild type, mutant BRCA1, mutant BRCA2, epigenetically silenced BRCA1, heterozygous for BRCA2) and in normal and HRD-positive (deficient XRCC3) Chinese hamster ovary cell lines [15]. At rucaparib concentrations up to 10 µM, greater cytotoxicity was observed in the cell lines with a BRCA mutation or HRD than in BRCA wild-type cells or those that were heterozygous for a BRCA2 mutation [15]. Rucaparib induced DNA double-strand breaks in all nine cell lines studied; however, HR repair was only observed in cells with functional BRCA [15]. In a separate in vitro study, the proliferation of 26 of 39 representative human ovarian cancer cell lines bearing a wide range of HR deficiencies other than a BRCA mutation was inhibited by 50% at rucaparib at concentrations ≤13 µM [30]. Cell lines with a low expression of genes involved in HR were particularly sensitive to rucaparib [30]. Rucaparib also potentiated the effects of DNA-damaging chemotherapy in ovarian cancer cells that were both sensitive and resistant to rucaparib monotherapy [30]. In UWB1.289 cells (BRCA1 mutant) exposed to rucaparib, concentration-dependent increases in PAR inhibition and DNA damage culminated in G2/M cell-cycle arrest, apoptosis, and decreased cell viability [29]. In vivo, rucaparib decreased tumor growth in mouse xenograft models of human cancer with deficiencies in BRCA, as well as those with other defects leading to HRD [15, 31]. Mouse plasma and tumor concentrations of rucaparib increased with rucaparib dose and were inversely correlated with PAR levels and directly correlated with greater tumor growth inhibition [29].
3 Clinical Experience of Rucaparib
Results from four key clinical trials have established rucaparib as a generally well-tolerated monotherapy with antitumor activity in patients with recurrent high-grade ovarian carcinoma in the treatment [32,33,34] and maintenance settings [35]. Study 10 was a phase I/II trial establishing the recommended starting dose of rucaparib in patients with solid tumors and evaluating the safety, efficacy, and PK of rucaparib in patients with BRCA-mutated ovarian cancer [33]. ARIEL2 was a phase II trial conducted to assess the safety and efficacy of rucaparib in patients with high-grade ovarian cancer [32, 36]. In an integrated efficacy analysis of Study 10 and ARIEL2 in patients with relapsed ovarian cancer associated with a germline and/or somatic BRCA mutation who were treated with two or more chemotherapies, the investigator-assessed objective response rate (ORR) was 53.8% (95% confidence interval [CI] 43.8–63.5), and the investigator-assessed progression-free survival (PFS) was 10.0 months (range, 0.0–22.1; 95% CI 7.3–12.5) [37]. The European Commission’s conditional marketing authorization was based on an efficacy analysis of a subset of patients from Study 10 and ARIEL2 with platinum-sensitive disease. The investigator-assessed confirmed ORR was 64.6% (95% CI 53.0–75.0), and median PFS was 10.9 months (95% CI 8.4–12.8) [24].
The use of rucaparib as an alternative treatment option to standard-of-care chemotherapy for patients with relapsed BRCA-mutated ovarian carcinoma is supported based on the results from the phase III ARIEL4 study (NCT02855944) [34]. ARIEL4, a randomized open-label study, evaluated the efficacy and safety of rucaparib as a treatment for patients with BRCA-mutated relapsed ovarian carcinoma who had received two or more prior chemotherapies. Rucaparib significantly improved median PFS compared with chemotherapy in the intent-to-treat population (7.4 vs 5.7 months, hazard ratio 0.67, 95% CI 0.52–0.86, p = 0.0017) [34].
ARIEL3, a randomized, double-blind, placebo-controlled, phase III study, evaluated rucaparib as a maintenance treatment in patients with recurrent ovarian cancer [35]. In this study, median PFS was longer with rucaparib than placebo in patients with a BRCA-mutant carcinoma (16.6 vs 5.4 months, hazard ratio 0.23, 95% CI 0.16–0.34, p < 0.0001) and those with an HRD carcinoma (defined as a BRCA mutant or BRCA wild-type/high genomic loss of heterozygosity ≥ 16%; 13.6 vs 5.4 months, hazard ratio 0.32, 95% CI 0.24–0.42, p < 0.0001), and in the intent-to-treat population (10.8 vs 5.4 months, hazard ratio 0.36; 95% CI 0.30–0.45, p < 0.0001) [35]. Based on these data, rucaparib was approved in the USA and European Union for the maintenance treatment of adult patients with recurrent ovarian cancer who are in a complete or partial response to platinum-based chemotherapy [21, 24].
Rucaparib is also approved in the USA for the treatment of patients with a deleterious BRCA mutation-associated mCRPC who have been treated with androgen receptor-directed therapy and taxane-based chemotherapy [21]. The approval was based on the results from TRITON2, an open-label phase II study that evaluated rucaparib in patients with mCRPC associated with a deleterious alteration in DNA damage repair genes [38]. Among patients with a BRCA mutation, the confirmed ORR was 43.5% (95% CI 31.0–56.7) for the independent radiology review-evaluable population and 50.8% (95% CI 38.1–63.4) for the investigator-evaluable population [38]. Rucaparib is currently under investigation as a single agent and in combination with cytotoxic, antiangiogenic, or immunotherapeutic agents for patients with solid tumors and those harboring a BRCA mutation or characterized as having HRD [39, 40].
4 Pharmacokinetics of Rucaparib
The PK profile of rucaparib monotherapy has been characterized in patients with advanced solid tumors, including those with advanced ovarian and prostate cancer. No studies of rucaparib in healthy volunteers have been performed because PARP inhibitors are clastogenic [22, 41]. Intensive PK data for rucaparib were obtained from 238 patients after administration of single or multiple doses in the following: a first-in-human phase I study [42], absolute oral bioavailability study [43] (A4991014; NCT01009190), ascending dose and food-effect phase I–II studies (Study 10) [44], mass balance study (NCT02986100) [45], hepatic impairment study (NCT03521037) [46], drug interaction studies (NCT02740712, NCT03954366) [47, 48], and a phase I dose-escalation study in Japanese patients (RUCA-J; NCT03499444) [49]. Additionally, sparse PK data were collected from >1027 patients in Study 10 [44], ARIEL2 Part 1 [32], ARIEL3, TRITON2, and the phase III TRITON3 study (NCT02975934) of rucaparib in the mCRPC setting.
In these studies, plasma rucaparib concentrations were determined using validated liquid chromatography with tandem mass spectrometry methods [50]. A noncompartmental analysis was used to estimate standard plasma PK parameters for rucaparib based on intensive PK data. Rucaparib population PK analyses were first performed using combined data from 453 patients who participated in the phase I Study A4991014, Study 10, and ARIEL2 [51]. Rucaparib PK was well described by a two-compartment model with sequential zero-order and first-order absorption and first-order elimination [51]. The model was then validated externally with sparse PK data from ARIEL3 and subsequently with sparse PK data from TRITON2 and TRITON3.
4.1 Single-Dose Pharmacokinetics
An early study in patients with advanced solid tumors showed that rucaparib given as an intravenous infusion followed by oral temozolomide, had linear PK at escalating dose levels (intravenous infusion of 1–18 mg/m2) [42]. Inter-subject variability in the area under the concentration–time curve (AUC) normalized for the actual dose was approximately 54% (percent coefficient of variation [CV%]), similar to that following oral administration [44], suggesting that a large part of PK variability is in disposition kinetics. Dose by body surface area did not decrease inter-subject PK variability; thus, fixed-dose levels were used in later clinical studies [42].
Rucaparib was tested in subsequent clinical studies as a monotherapy. Single-dose PK values of oral rucaparib were obtained from Study 10 Part 1, in which 55 patients with advanced solid tumors received doses from 40 to 840 mg [44]. Median time to maximum plasma concentration (Cmax), Tmax, was 1.5–6 h (Fig. 2) [44]. Once Cmax was reached, mean plasma rucaparib concentrations declined slowly in an apparent biexponential manner. PK parameters are summarized in Table 1.
Mean (standard deviation [SD]) plasma rucaparib concentration–time profiles following once-daily [QD] (a, b) and twice-daily [BID] (c, d) oral administration of rucaparib in patients with advanced solid tumors. Error bars represent SD. Reprinted from Kristeleit et al. [33]
4.2 Multiple-Dose Pharmacokinetics
Plasma rucaparib PK following continuous administration of rucaparib at 40–500 mg once daily (QD) and 240–840 mg twice daily (BID) was determined in 55 patients with an advanced solid tumor who participated in Study 10 Part 1 (Table 1, Fig. 2) [44]. Steady-state plasma rucaparib PK was achieved after continuous dosing for a week [44]. A decision to switch dosing frequency from QD to BID was made to further increase rucaparib exposure while avoiding possible saturable oral absorption as suggested by available data at that time (limited solubility, relatively moderate oral bioavailability, and precipitation in the presence of a chloride ion, Sect. 4.4.1). Importantly, the tablet burden was high given the low tablet strength (40, 60, and 120 mg), with a yet greater tablet burden if higher dose levels were to be pursued with a QD dosing schedule. Rucaparib steady-state PK at the recommended dose level of 600 mg BID using the commercial tablet formulation was determined in 18 evaluable patients in Study 10 Part 3 [44]. Arithmetic mean (CV%) for steady-state Cmax (Cmax,ss) and AUC from time 0 to tau were 1940 ng/mL (54%) and 15,800 ng·h/mL (58%), respectively. The steady-state accumulation ratio for AUC ranged from 1.60 to 2.33 following QD dosing and from 1.47 to 5.44 following BID dosing [44].
4.3 Dose Proportionality
Rucaparib PK exposure increased with ascending dose levels (40–500 mg QD and 240–840 mg BID) in Study 10 Part 1 (Fig. 2) [44]. Dose proportionality for steady-state PK parameters after log transformation for QD and BID was assessed using the power model [52] and the following equation:
where Y is a measure of rucaparib PK exposure (i.e., Cmax, AUC from 0 to 24 h [AUC0–24h]). A slope of 1 indicates dose proportionality. For the QD regimen, the slopes of Cmax and AUC0–24h were 0.92 (90% CI 0.69–1.15, R2 = 0.795) and 0.98 (90% CI 0.72–1.25, R2 = 0.775), respectively. For the BID regimen, the corresponding values were 1.03 (90% CI 0.42–1.63, R2 = 0.261) and 1.04 (90% CI 0.42–1.67, R2 = 0.253), respectively [44].
4.4 Absorption, Distribution, Metabolism, and Elimination
4.4.1 Absorption
Absolute bioavailability of oral rucaparib was evaluated in an open-label, multicenter, dose-escalating, phase I study of fasted patients with advanced solid tumors (A4991014; NCT01009190) [43]. Each patient received an intravenous bolus dose and an oral dose of rucaparib. Rucaparib showed a dose-independent mean oral bioavailability of 36% (range 30–45%) across the tested oral dose range of 12–120 mg based on the ratio of dose-normalized AUC [21, 43]. Oral bioavailability has not been tested at doses > 120 mg.
The effect of a high-fat meal on the rate and extent of rucaparib absorption was assessed at the 40 mg (n = 3), 300 mg (n = 6), and 600 mg (n = 26) dose levels in Study 10 Parts 1 and 3 [44]. In Part 1, mean rucaparib plasma concentration profiles and PK parameters following single administration of rucaparib 40 mg and 300 mg were similar between fed and fasted conditions. In Part 3 (600 mg dose level), patients received rucaparib with and without a meal in a crossover design with a 7-day washout in between. Rucaparib Cmax increased by 20% (90% CI 99–146), AUC0–24h increased by 38% (90% CI 117–162), and median time to Cmax was delayed by 2.5 h (4.0–7.8 h) after a high-fat meal versus the fasted state [21, 44]. Given the limited food effect on rucaparib PK, no meal restrictions were applied in later clinical trials. Collective clinical safety and efficacy data later confirmed that the food effect is not clinically significant and that rucaparib can be given with or without food [21, 32, 33, 35, 53]. The reason for the apparent difference in the food effect at low doses (40 and 300 mg) and a high dose (600 mg) remains undetermined, but a dose-dependent food effect is not surprising given that rucaparib has relatively high permeability and low solubility (possibly a Biopharmaceutical Classification System Class II drug).
Rucaparib has lower solubility at lower pH and in the presence of chloride ions. The effect of a concomitant proton pump inhibitor on rucaparib absorption was tested in a population PK model, but no apparent effect was observed (see Sect. 5.1 for more information). As the main gastrointestinal site of rucaparib absorption has not been determined, any effect of gastrointestinal complications, such as bowel resection and intestinal obstruction, on systemic exposure to rucaparib also remains unknown.
Relative oral bioavailability among different oral formulations was compared in the population PK analysis. Capsules, low-strength tablets, and high-strength tablets (commercial formulation) showed comparable steady-state exposures. This was expected based on the rapid in vitro dissolution rates of the tested immediate-release formulations of rucaparib. Accordingly, efficacy and safety data were pooled across trials regardless of which oral formulation was used for the new drug application [51].
4.4.2 Distribution
Plasma protein-binding affinity of rucaparib is moderate in human plasma and concentration independent at clinical dose levels. In vitro dialysis chamber methodology showed that rucaparib was 70% protein-bound in plasma at therapeutic concentrations [21, 54].
In vitro, the mean red blood cell-to-plasma concentration ratio for rucaparib was 1.83 and concentration independent in human blood [21, 54]. In vivo, the blood-to-plasma AUC ratio of total 14C-radioactivity was approximately 0.781 in patients after a single oral dose of [14C]-rucaparib 600 mg [45]. The results in both studies indicated relatively low rucaparib distribution in red blood cells, but the clinical AUC ratio of 0.781 is lower than the ratio from the in vitro data. This is likely due to the formation of metabolites that have a lower uptake by red blood cells than rucaparib.
Rucaparib had a steady-state volume of distribution of 113–262 L following a single intravenous dose of rucaparib 12–40 mg in patients with advanced solid tumors participating in the phase I A4991014 study [43]. These values were considerably greater than the plasma volume, suggesting tissue distribution/binding. In the pooled population PK analysis, mean estimates for the volume of the central compartment and peripheral compartment were 17 and 166 L, respectively [51]. There was no apparent compartment volume-dose trend in the population PK analysis at therapeutic dose levels.
Quantitative whole-body autoradiography of [14C]-rucaparib camsylate in rats suggested rucaparib binding in pigmented tissues. This may explain the photosensitivity observed in clinical trials of rucaparib. Patients receiving rucaparib are advised not to spend time in sunlight and to protect themselves from the sun when outside [21, 24].
Clinical data are limited on the distribution and attendant effects in the central nervous system for rucaparib (and other PARP inhibitors). In vivo PK studies in male CD-1 mice confirmed the limited brain penetration of all PARP inhibitors evaluated (rucaparib, niraparib, olaparib, talazoparib, and veliparib) [55]. This is consistent with in vitro data showing that PARP inhibitors are substrates of P-glycoprotein (P-gp) and/or breast cancer resistance protein (BCRP). Interestingly, rucaparib (and niraparib) showed antitumor efficacy in an intracranial BRCA1-mutant, triple-negative, breast cancer MDA-MB-436 xenograft mouse model following oral administration [55]. Moreover, clinical activity was observed in a rucaparib-treated patient with germline BRCA2-mutant triple-negative breast cancer and central nervous system involvement. The patient experienced complete resolution of neurological symptoms after one cycle of rucaparib and progressed after 9 months (overall survival was 25 months) [55]. It is possible that brain tumors disrupted the blood–brain barrier, allowing the intracranial exposure of rucaparib to reach therapeutic concentrations. Taken together, rucaparib could be effective in treating brain metastases with BRCA mutations, but additional studies are needed.
4.4.3 Metabolism and Excretion
The carboxylic acid M324, an inactive oxidative metabolite of rucaparib, has been observed in humans [56]. Preliminary metabolite profiling in plasma samples collected from three patients in Study 10 treated with rucaparib 600 mg BID suggested that M324 is a major metabolite of rucaparib [44]. In vitro studies indicated that rucaparib had a low metabolic turnover rate. The turnover rate calculated as a percentage of M324:rucaparib was well below 10% after a 2-h incubation with human liver microsomes [54]. M324 formation was mediated mainly by CYP1A2 and CYP3A, which were estimated to be responsible for 27% and 64% of the hepatic CYP-mediated metabolism of rucaparib to M324, respectively, whereas the other five CYPs showed no or negligible activity [54]. The contributions of non-CYP elimination pathways were not measured in this assay and must be accounted for when estimating total metabolic clearance and/or potential effect of a co-administered drug on the metabolism of rucaparib to M324.
Rucaparib clearance was 13.9–18.4 L/h following a single intravenous dose of rucaparib 12–40 mg in 35 patients with advanced solid tumors participating in the phase I A4991014 study [43]. In Study 10 Part 1, the apparent rucaparib clearance at steady state was comparable after the administration of 50–500 mg QD (26.7–47.5 L/h) and the administration of 240–840 mg BID (26.2–58.6 L/h) [44]. At the approved rucaparib 600-mg BID dosage, apparent rucaparib clearance at steady state ranged from 15.3 to 79.2 L/h [21].
A single-dose mass balance study was performed to characterize the disposition and metabolic identification of orally administered [14C]-rucaparib 600 mg (≈ 140 μCi) in six patients with advanced solid tumors [45]. The mean elimination half-life was 25.9 and 30.4 h based on rucaparib concentration and total radioactivity in plasma, respectively [45]. Mean post-dose recovery of total radioactivity was 89.3% (urine 17.4%; feces 71.9%) over 12 days [45], inferring almost complete excretion. The mean (CV%) urinary clearance of total 14C-rucaparib was 11.4 L/h (29%). Metabolite profiling conducted in plasma, urine, and feces in the mass balance study showed that rucaparib was metabolized via oxidation, N-demethylation, N-methylation, and glucuronidation to seven identifiable metabolites (Fig. 3) [45]. Unchanged rucaparib and M324 were the major drug-related components in all matrices, with the other metabolites detected in trace amounts. Unchanged rucaparib and M324 comprised 64.0% and 18.6% of total radioactivity in plasma, respectively, 44.9% and 50.0% of total radioactivity recovered urine, and 94.9% and 5.1% of total radioactivity recovered in feces [45]. The high fecal recovery of unchanged rucaparib could be attributed to hepatic excretion and/or incomplete oral absorption.
Potential phase I and phase II metabolic pathways of rucaparib following a single oral dose of [14C]-rucaparib 600 mg. Numbered arrows denote the following: 1, N-demethylation; 2, oxidation; 3, glucuronidation; and 4, N methylation. The dashed-line box indicates that the position of the glucuronide on M324 cannot be concluded. F feces, P plasma, U urine. Reprinted from Liao et al. [45], with permission from Springer
In a dedicated hepatic impairment study, patients with normal hepatic function (n = 8) or moderate hepatic impairment (n = 8) received a single oral dose of 600 mg of rucaparib. The mean percentage (CV%) 24-h urinary recovery of rucaparib was 3.7% (43%) for the normal group and 3.3% (69%) for the impairment group, corresponding to a mean (CV%) renal clearance of 3.21 L/h (19%) and 2.77 mL/min (59%), respectively [46].
Population PK of rucaparib 600 mg BID indicated no apparent difference in rucaparib PK among patients with different phenotypes of CYP1A2 (normal, n = 28; hyperinducer, n = 133) and CYP2D6 (poor metabolizer, n = 9; normal metabolizer, n = 75; intermediate metabolizer, n = 69; ultra-rapid metabolizer, n = 4) [51]. The medians and distributions of exposures between former smokers (n = 95) and those who never smoked (n = 246) overlapped following administration of rucaparib 600 mg BID. The sample size of current smokers (n = 16) was too small to conduct meaningful comparisons. In the population PK model, baseline creatinine clearance (CLCR) was a significant covariate on rucaparib clearance, with an approximately 27% variation in rucaparib clearance from the differences in CLCR (10th to 90th percentiles) [51].
5 Intrinsic Factors Affecting Rucaparib Pharmacokinetics
Covariates of clinical interest were assessed for potential influence on rucaparib in the population PK analysis and in dedicated clinical trials.
5.1 Demographics
As evaluated in the population PK analysis of rucaparib 600 mg BID, body weight, body mass index, age, and race showed no statistically significant effect on rucaparib PK [57]. The lack of a body weight effect on rucaparib exposure justifies the use of fixed-dose administration rather than dosing based on body weight or body surface area [51, 57]. Age initially showed an effect on rucaparib clearance in the population PK model; however, the effect was insignificant when baseline CLCR was included in the model as a covariate, likely owing to a correlation between CLCR and age [57].
A population PK analysis suggested that Asian patients had comparable exposures to White patients, while exposures in Black patients appeared to be high relative to other patients. However, these results are considered preliminary because individuals who were non-White comprised < 10% of the population (21 Asian patients; eight Black patients). PK data collected from the phase I dose-escalation study in Japanese patients (RUCA-J) suggested a dose-proportional increase in steady-state exposures and overlapping PK profiles with Western patients. The difference in steady-state AUC from time 0 to tau (CV%) of rucaparib 600 mg BID is not considered clinically significant between Japanese patients (28,100 ng·h/mL [40.8%]) [49] and Western patients (16,900 ng·h/mL [54%]) [44] based on a manageable safety profile in Japanese patients; thus, Japanese patients were treated at the same starting dose (600 mg BID) in subsequent clinical studies.
Rucaparib PK in different settings was compared in the population PK analyses. Rucaparib exposures in patients with ovarian cancer who received rucaparib in a maintenance setting (ARIEL3, n = 359) were about 20% lower than those in a treatment setting (Study 10, ARIEL2, n = 412). Part of the difference in rucaparib exposures was explained by baseline covariates (e.g., CLCR, albumin level), but none of these covariates were considered clinically significant [57]. Patients with mCRPC in TRITON2 (n = 199 patients) [58] and TRITON3 (n = 19 patients) showed comparable PK as compared to patients with ovarian cancer, suggesting the lack of a sex-based PK difference between patients with ovarian and prostate cancer.
5.2 Special Populations
5.2.1 Renal Impairment
PK profiles of rucaparib 600 mg BID were estimated using the population PK model for mild-to-moderate renal impairment. The model-predicted steady-state AUC (AUCss) was approximately 15% and 32% higher for patients with mild (n = 148; baseline CLCR 60–89 mL/min) and moderate (n = 72; CLCR 30–59 mL/min) renal impairment, respectively, than that for patients with normal renal function (n = 143; CLCR ≥90 mL/min). Such mild increases in exposure were not considered clinically significant when comparing safety data. Therefore, no dose adjustment is recommended for patients with mild or moderate renal impairment [21].
The PK characteristics of rucaparib in patients with severe renal impairment (CLCR < 30 mL/min) or patients undergoing dialysis are limited. Harold et al. [59] described a case report of a patient on three-times-a-week hemodialysis who started rucaparib monotherapy at one third of the recommended dose (200 mg BID) for the treatment of BRCA-associated breast and recurrent ovarian cancer. Trough concentrations of rucaparib in the blood samples of the patient were below the concentrations reported in ARIEL2; yet, a clinically significant disease response was attained [59]. On the basis of the limited PK sampling, the plasma concentration drop following hemodialysis was approximately 11% (7 h and 20 min in between) as compared with a 17% drop on a non-dialysis control day (7 h in between) [59]. The apparent minimal effect of hemodialysis on rucaparib PK could be due to the widespread distribution of rucaparib in tissues coupled with a slow intercompartmental clearance; rucaparib eliminated from plasma during dialysis may be largely replenished from tissues after dialysis.
5.2.2 Hepatic Impairment
Population PK of rucaparib 600 mg BID indicated no apparent difference in rucaparib behavior in the setting of mild hepatic impairment [21, 51]. The model-predicted AUCss was comparable between patients with normal hepatic function (n = 337) and mild hepatic impairment (total bilirubin between 1.0 and 1.5 × upper limit of normal and any aspartate aminotransferase, n = 34) per National Cancer Institute Organ Dysfunction Working Group criteria [51, 60].
A dedicated PK study (NCT03521037) was conducted to compare the PK in patients with moderate hepatic impairment (total bilirubin > 1.5 × upper limit of normal and ≤ 3 × the upper limit of normal, n = 8) versus patients with normal hepatic function (n = 8) [46]. On the basis of the Cmax and time to Cmax results, moderate hepatic impairment had no apparent effect on the oral bioavailability of rucaparib and formation kinetics of M324 [46]. Patients with moderate hepatic impairment showed slightly higher AUC from time 0 extrapolated to infinity of rucaparib and AUC from time zero to last quantifiable measurement of M324 than patients with normal hepatic function, with geometric mean ratios (90% CI) of 1.446 (0.668–3.131) and 1.483 (0.766–2.868), respectively [46]. It was observed that the higher AUC values coincided with slower renal clearance of rucaparib and M324 in patients with moderate hepatic impairment despite the similar baseline CLCR between the two groups; thus, the observed PK differences between hepatic function groups might be in part due to different renal clearance of rucaparib and M324 [46]. Similar trends of AUC changes were observed when patients were classified using the Child–Pugh criteria for hepatic function [46]. The effect of moderate hepatic impairment on rucaparib AUC was similar in magnitude to the effects of a high-fat meal and moderate renal impairment and was thus not considered clinically significant [44, 46, 51]. Hence, no dose adjustment is recommended for patients with mild-to-moderate hepatic impairment [21, 46]. Nevertheless, caution should be used for patients with moderate hepatic impairment as the safety of rucaparib has not been well characterized in this population.
6 Drug–Drug Interactions
The potential for DDIs associated with rucaparib and concomitant medications have been investigated by the use of dedicated in vitro testing and clinical studies in patients with an advanced solid tumor [47, 48, 54, 61].
6.1 Rucaparib as a Victim
Results from in vitro assays were indicative of low DDI potential for rucaparib as a victim. Rucaparib showed moderate permeability across Caco-2 cell monolayers. In transfected cells expressing drug transporters, rucaparib was a substrate for P-gp and BCRP, but not a substrate for hepatic (organic anion-transporting polypeptide [OATP] 1B1, OATP1B3) or renal uptake transporters (organic anion transporter [OAT] 1, OAT3, or organic cation transporter [OCT]) 2 [54]. Rucaparib oral PK was dose proportional across rucaparib dosages (40 mg QD to 840 mg BID), and the oral bioavailability of rucaparib was independent of rucaparib doses with a mean value of 36% [43, 44]. Thus, the oral bioavailability of rucaparib in patients who received rucaparib 600 mg had a negligible impact from P-gp and BCRP [54].
Clinically significant DDIs with concomitant treatment of CYP perpetrators are not expected. In the population PK analysis, patients with different CYP1A2 and CYP2D6 phenotypes showed comparable rucaparib PK. While a significant contribution of CYP3A to rucaparib metabolism cannot be excluded based on in vitro CYP phenotyping and human absorption, distribution, metabolism, and elimination data [45, 54], the low rucaparib turnover rate justifies no restrictions on the concomitant use of CYP perpetrators in patients receiving rucaparib [54].
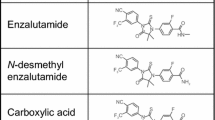
Rucaparib has shown promising activity when combined with the androgen receptor inhibitor enzalutamide in patients with mCRPC associated with HR repair gene alterations [38]. Given that enzalutamide is also a strong CYP3A4 inducer, attention was required to characterize rucaparib PK to support the use of enzalutamide in combination with rucaparib. In the phase Ib RAMP study (NCT04179396), the combination of rucaparib 600 mg BID and enzalutamide 160 mg QD was administered in patients with mCRPC [61]. The combined treatment had no significant effect on the PK concentrations of rucaparib and its metabolite M324 [61]. Trough PK values of enzalutamide and its metabolite N-desmethyl enzalutamide in the combined treatment remained similar to those observed in the previous studies of enzalutamide 160 mg QD alone [61, 62]. On the basis of these results, the phase III trial CASPAR (NCT04455750) has been initiated to further study the combination of rucaparib and enzalutamide [63].
Additionally, rucaparib concentrations from 0.5 to 50 μM showed moderate human plasma protein binding with the average of 70%, indicating that concomitant administrations of highly protein-bound medications, such as enzalutamide, are unlikely to result in fluctuations in plasma concentrations of unbound rucaparib [54]. When the concomitant treatment of a proton pump inhibitor was evaluated as a time-varying covariate in the population PK analysis, dose-normalized, steady-state minimum plasma concentration of rucaparib was comparable in patients who received rucaparib with or without a proton pump inhibitor [51].
The European Medicines Agency (EMA) and US Food and Drug Administration guidelines recommend that active metabolites contributing to ≥ 50% of overall activity should be investigated in vitro for their DDI potential as victims of CYP and transporter modulators [64, 65]. In enzymatic assays, the IC50 values of M324 against PARP1, PARP2, and PARP3 were ≥ 34-fold higher than that of rucaparib [24]. Similarly, M324 showed ≥ 77-fold higher IC50 values in cytotoxicity assays than rucaparib against selected BRCA-mutant cell lines. Given the limited in vitro activity, no DDI assessment for M324 as a substrate of enzymes and transporters was conducted.
6.2 Rucaparib as a Perpetrator
In vitro, rucaparib reversibly inhibited CYP1A2, CYP2C9, CYP2C19, CYP2D6, and CYP3As. No time-dependent inhibition of any CYP enzymes was observed [54]. Rucaparib inhibited UGT1A1 but not UGT2B7 [54]. In cultured human hepatocytes, rucaparib showed a concentration-dependent induction of CYP1A2 messenger RNA (and a down-regulation of CYP3A4 messenger RNA (0.05–13 μM) and decreased CYP2B6 messenger RNA at ≥2.08 μM [54]. Rucaparib inhibited P-gp and BCRP and slightly inhibited OATP1B1, OATP1B3, OAT1, and OAT3 [54].
In an open-label, sequential, DDI phase I study (NCT02740712), the effects of rucaparib on the PK of probe substrates for CYP isoenzymes and P-gp were assessed in 17 patients with advanced solid tumors [47]. Patients received CYP probe substrates as a modified Cooperstown 5 + 1 cocktail (CYP1A2, caffeine; CYP2C9, S-warfarin; CYP2C19, omeprazole; and CYP3A, midazolam) [66] and the P-gp probe digoxin (delivered separately 1 day after the cocktail) both before rucaparib administration and at rucaparib steady state following rucaparib 600 mg BID for 1 week. Rucaparib moderately inhibited CYP1A2; weakly inhibited CYP2C9, CYP2C19, and CYP3A; and marginally increased digoxin exposure (Table 2, Fig. 4) [47].
Effect of rucaparib on the PK of probe drugs. AUC0–72h area under the concentration–time curve from time 0 to 72 h, AUC0–96h AUC from time 0 to 96 h, AUC0–inf AUC extrapolated from time 0 to infinity, AUC0–last AUC from time 0 up to the last timepoint with a quantifiable concentration, BCRP breast cancer resistance protein, CI confidence interval, Cmax maximum plasma concentration, CYP cytochrome P450, GMR geometric mean ratio, P-gp P-glycoprotein.
In an open-label phase I study (NCT03954366), the effects of rucaparib on the PK of BCRP substrate rosuvastatin and oral contraceptives ethinylestradiol and levonorgestrel were evaluated in patients with solid tumors [48]. Rucaparib 600 mg BID for 2 weeks weakly increased the plasma exposures of rosuvastatin and the oral contraceptives (Table 2, Fig. 4) [48]. However, the limited effects of rucaparib on the probe drug exposures are not considered clinically significant, and dose adjustments of rosuvastatin and oral contraceptives are not needed when co-administered with rucaparib.
Given that rucaparib inhibited renal transporters OCT1, OCT2, MATE1, and MATE2-K (IC50, 4.3, 31, 0.63, and 0.19 μM, respectively) in vitro, caution is advised when rucaparib is co-administered with sensitive substrates of MATEs, OCT1, and OCT2, such as metformin [54]. As renal excretion of creatinine is partially mediated by OCT2, MATE1, and MATE2-K [67], inhibition of these transporters by rucaparib and other PARP inhibitors [68, 69] causes reversible creatinine elevation without decreasing renal function. As a result, serum creatinine-based calculation of glomerular filtration rate is no longer a reliable surrogate of renal function for PARP inhibitors [70].
6.3 Metabolite as a Perpetrator
Following a single oral dose of [14C]-rucaparib 600 mg, the plasma AUC0–24h ratio of M324 to rucaparib is 30.4% and the AUC ratio of [14C]-M324 to total radioactivity is 18.6% [45]. On the basis of the EMA criteria [64, 65], M324 is regarded as a major metabolite of rucaparib [45]. The assessment of DDI risk of M324 as a perpetrator using in vitro inhibition studies on human CYP isoforms and transporters demonstrated that M324 inhibited CYP2C8, CYP2C19, and the other CYPs, for example., CYP1A2, CYP2B6, CYP2C9, CYP2D6, and CYP3A4/5 (IC50, 47.5, 51.0, and >80 µM, respectively), and inhibited OAT3, OATP1B1, P-gp, BCRP, MATE1, and MATE2-K (IC50, 5.67, 15.6, 10.9, 3.98, 251, and 70.7 µM, respectively). M324 did not inhibit OAT1 or OCT2 at concentrations up to 500 µM. In human plasma, M324 at concentrations up to 60 μM exhibited a concentration-independent protein binding with the mean free fraction of 8.88%. In the RUCA-J study in Japanese patients, the clinical Cmax for M324 at steady state was 411 ng/mL. According to EMA and US Food and Drug Administration DDI guidelines [64, 71], DDIs analyzed using static models suggested no DDI risk for M324 as a perpetrator of major human CYPs and transporters (except BCRP). According to EMA guidance [64], the design of the aforementioned DDI study (NCT03954366) is considered sufficient for evaluating the effect of both the parent drug (rucaparib) and metabolite (M324) on the PK of oral rosuvastatin (BCRP substrate). Overall, the in vitro and clinical studies did not reveal any additional clinically significant DDI signals.
7 Exposure–Response Analysis
Exploratory exposure–response analyses were conducted in support of regulatory filings to the US Food and Drug Administration and EMA. Given some patients had dose modifications/interruptions, model-estimated individual Cmax,ss and AUCss at the nominal dose levels were corrected by actual dose levels up to the event of interest. Linear logistic regression was used for binary endpoints, linear regression was used for continuous endpoints, and Cox regression was used for time-to-event endpoints.
7.1 Exposure–Efficacy Relationships
In support of the original new drug application supporting ovarian cancer treatment, exposure–efficacy relationships were explored for selected efficacy endpoints in patients with ovarian cancer with a deleterious BRCA mutation who received two or more lines of platinum-based chemotherapies in Study 10 and ARIEL2 (n = 117, 300–840 mg BID) [57]. A significant correlation was detected between AUCss and independent radiology review-assessed ORR in platinum-sensitive patients with a progression-free interval of ≥ 6 months following the last platinum-containing regimen (n = 75, p = 0.017) [57]. No apparent correlation was observed for other efficacy endpoints. The results of this exposure–efficacy analysis suggested that better efficacy could be achieved by maximizing rucaparib exposure [57].
In the exposure–efficacy analyses of patients with mCRPC in TRITON2, no clinically meaningful relationships between rucaparib steady-state exposure and response were detected, possibly owing to the narrow range of PK exposures [58]. However, additional covariate analyses suggested that higher AUCss correlated with greater maximal tumor shrinkage in TRITON2 patients with measurable disease [58].
7.2 Exposure–Safety Relationships
Data from Study 10 and ARIEL2 were also pooled to test for associations of dose-normalized Cmax,ss with clinical biochemical adverse events and adverse events with a severity grade of 3 or higher in patients with ovarian cancer [32, 44, 57]. Overall, PK data were available for 375 patients who received at least one dose of rucaparib in these studies. The starting doses ranged from 40 mg QD to 840 mg BID [57]. After accounting for covariates, Cmax was significantly correlated with grade ≥ 2 serum creatinine increase (p < 0.001), grade ≥ 3 alanine aminotransferase (increase (p ≤ 0.033), grade ≥ 3 aspartate aminotransferase increase (p = 0.027), grade ≥ 3 platelet decrease (p = 0.04), grade ≥ 3 fatigue/asthenia (p = 0.029), and maximal hemoglobin decrease from baseline (p = 0.001) [57]. However, such adverse effects can be managed by dose modification and, thus, no adjustment of starting dose is necessary [57].
Similar to the exposure–efficacy analysis above, correlations between dose normalized Cmax,ss and selected safety endpoints were assessed in ARIEL3 (n = 359) and TRITON2 (n = 199) [58]. In ARIEL3, statistically significant correlations were observed for grade ≥ 2 creatinine increase (p < 0.001), grade ≥ 3 ALT increase (p = 0.003), grade ≥ 3 hemoglobin decrease (p < 0.001), and grade ≥ 3 cholesterol increase (p < 0.001). In TRITON2, statistically significant correlations with dose-corrected Cmax,ss were observed for grade ≥ 2 creatinine elevation (p = 0.004) [58] and grade ≥ 3 hemoglobin (p = 0.033).
The effect of rucaparib on cardiac repolarization was studied in 54 patients with ovarian cancer who received doses from 40 mg QD to 840 mg BID. Changes of QT corrected according to Fridericia’s formula from baseline were fitted to time-matched plasma rucaparib concentration data using linear mixed-effects models. At the predicted median Cmax,ss following rucaparib 600 mg BID, the projected QT corrected according to Fridericia’s formula increase from baseline was 11.5 ms (90% CI 8.8–14.2). As the risk for clinically significant QT corrected according to Fridericia’s formula increase from baseline (i.e., > 20 ms [72, 73]) is low, no specific electrocardiogram monitoring is indicated clinically.
8 Summary and Future Perspectives
The clinical pharmacology of rucaparib has been well characterized. Rucaparib has a moderate oral bioavailability and can be administered with or without food. The elimination of rucaparib is accomplished through multiple pathways, including metabolism and excretion. No active metabolite was identified.
The DDI risk of rucaparib is minimal and manageable. Rucaparib is not a strong perpetrator of CYP enzymes or efflux transporters, and DDIs that affect rucaparib PK are not clinically significant. Although no medicines are prohibited for the combination or coadministration with rucaparib, the EMA summary of product characteristics and US prescribing information note that coadministration of rucaparib and CYP substrates may increase the systemic exposure of these drugs and recommend dose adjustment of CYP substrates if clinically indicated.
Demographics, CYP polymorphism, and mild-to-moderate organ dysfunction showed no clinically meaningful effect on rucaparib PK. Nevertheless, close monitoring is needed when rucaparib is administered in special populations (e.g., patients with renal and hepatic impairment). A quantitative exposure–efficacy analysis highlighted the importance of maintaining rucaparib treatment intensity for optimal efficacy, and the exposure–safety analysis allowed a better understanding and effective management of adverse effects and DDIs.
Although numerous nonclinical and clinical studies have been conducted to characterize the absorption, distribution, metabolism, excretion, and DDIs, as well as effects of various intrinsic and extrinsic factors on rucaparib PK, clinical pharmacology characterization is a continuous process, and such data should be interpreted in the context of clinical safety and efficacy in specific patient populations. As with other PARP inhibitors, gaps remain even with the current understanding of rucaparib clinical pharmacology. For example, the intestinal absorption sites of rucaparib have not been determined. Future research of intrinsic and extrinsic factors affecting rucaparib PK variability and more comprehensive characterization of exposure–response relationships would be valuable. These studies could examine the effects of penetration and transporter-mediated efflux on rucaparib distribution in target tumors, not only from patient to patient but also among different tumors within a single patient. Additionally, in vivo analyses may be warranted for potential DDI risks, such as OCT1 and MATE1/2-K inhibition, because these have only been evaluated in vitro. Despite these limitations, the extensive assessments currently available allow a robust understanding of rucaparib clinical pharmacology. In conclusion, clinical pharmacology assessments of rucaparib supported selecting 600 mg BID with or without food as the starting dose for patients with cancer.
References
Schreiber V, Dantzer F, Ame JC, de Murcia G. Poly(ADP-ribose): novel functions for an old molecule. Nat Rev Mol Cell Biol. 2006;7:517–28.
Rouleau M, Patel A, Hendzel MJ, Kaufmann SH, Poirier GG. PARP inhibition: PARP1 and beyond. Nat Rev Cancer. 2010;10:293–301.
Scott CL, Swisher EM, Kaufmann SH. Poly (ADP-ribose) polymerase inhibitors: recent advances and future development. J Clin Oncol. 2015;33:1397–406.
Moynahan ME, Chiu JW, Koller BH, Jasin M. Brca1 controls homology-directed DNA repair. Mol Cell. 1999;4:511–8.
Moynahan ME, Pierce AJ, Jasin M. BRCA2 is required for homology-directed repair of chromosomal breaks. Mol Cell. 2001;7:263–72.
Venkitaraman AR. Cancer susceptibility and the functions of BRCA1 and BRCA2. Cell. 2002;108:171–82.
Walsh CS. Two decades beyond BRCA1/2: homologous recombination, hereditary cancer risk and a target for ovarian cancer therapy. Gynecol Oncol. 2015;137:343–50.
Bryant HE, Schultz N, Thomas HD, Parker KM, Flower D, Lopez E, et al. Specific killing of BRCA2-deficient tumours with inhibitors of poly(ADP-ribose) polymerase. Nature. 2005;434:913–7.
Farmer H, McCabe N, Lord CJ, Tutt ANJ, Johnson DA, Richardson TB, et al. Targeting the DNA repair defect in BRCA mutant cells as a therapeutic strategy. Nature. 2005;434:917–21.
McCabe N, Turner NC, Lord CJ, Kluzek K, Białkowska A, Swift S, et al. Deficiency in the repair of DNA damage by homologous recombination and sensitivity to poly(ADP-ribose) polymerase inhibition. Cancer Res. 2006;66:8109–15.
Ashworth A. A synthetic lethal therapeutic approach: poly(ADP) ribose polymerase inhibitors for the treatment of cancers deficient in DNA double-strand break repair. J Clin Oncol. 2008;26:3785–90.
Mendes-Pereira AM, Martin SA, Brough R, McCarthy A, Taylor JR, Kim J-S, et al. Synthetic lethal targeting of PTEN mutant cells with PARP inhibitors. EMBO Mol Med. 2009;1:315–22.
Williamson CT, Muzik H, Turhan AG, Zamò A, O’Connor MJ, Bebb DG, et al. ATM-deficiency sensitizes mantle cell lymphoma cells to poly(ADP-ribose) polymerase-1 inhibitors. Mol Cancer Ther. 2010;9:347–57.
McEllin B, Camacho CV, Mukherjee B, Hahm B, Tomimatsu N, Bachoo RM, et al. PTEN loss compromises homologous recombination repair in astrocytes: implications for GBM therapy with temozolomide or PARP inhibitors. Cancer Res. 2010;70:545–64.
Drew Y, Mulligan EA, Vong WT, Thomas HD, Kahn S, Kyle S, et al. Therapeutic potential of poly(ADP-ribose) polymerase inhibitor AG014699 in human cancers with mutated or methylated BRCA1 or BRCA2. J Natl Cancer Inst. 2011;103:334–46.
Nijman SMB. Synthetic lethality: general principles, utility and detection using genetic screens in human cells. FEBS Lett. 2011;585:1–6.
Helleday T. The underlying mechanism for the PARP and BRCA synthetic lethality: clearing up the misunderstandings. Mol Oncol. 2011;5:387–93.
Reinbolt RE, Hays JL. The role of PARP inhibitors in the treatment of gynecologic malignancies. Front Oncol. 2013;3:237.
De Lorenzo SB, Patel AG, Hurley RM, Kaufmann SH. The elephant and the blind men: making sense of PARP inhibitors in homologous recombination deficient tumor cells. Front Oncol. 2013;3:228.
Ceccaldi R, Liu JC, Amunugama R, Hajdu I, Primack B, Petalcorin MI, et al. Homologous-recombination-deficient tumours are dependent on Poltheta-mediated repair. Nature. 2015;518:258–62.
Rubraca (rucaparib) tablets [prescribing information]. Boulder (CO): Clovis Oncology, Inc.; 2022.
Thomas HD, Calabrese CR, Batey MA, Canan S, Hostomsky Z, Kyle S, et al. Preclinical selection of a novel poly(ADP-ribose) polymerase inhibitor for clinical trial. Mol Cancer Ther. 2007;6:945–56.
Wahlberg E, Karlberg T, Kouznetsova E, Markova N, Macchiarulo A, Thorsell AG, et al. Family-wide chemical profiling and structural analysis of PARP and tankyrase inhibitors. Nat Biotechnol. 2012;30:283–8.
Rubraca (rucaparib) tablets [summary of product characteristics]. Swords, Ireland: Clovis Oncology Ireland Ltd.; 2019.
Mittica G, Ghisoni E, Giannone G, Genta S, Aglietta M, Sapino A, et al. PARP inhibitors in ovarian cancer. Recent Pat Anticancer Drug Discov. 2018;13:392–410.
Valabrega G, Scotto G, Tuninetti V, Pani A, Scaglione F. Differences in PARP inhibitors for the treatment of ovarian cancer: mechanisms of action, pharmacology, safety, and efficacy. Int J Mol Sci. 2021;22:4203.
Wang H, Wu M, Liu H, Zhou H, Zhao Y, Geng Y, et al. Comparison of the efficacy and safety of PARP inhibitors as a monotherapy for platinum-sensitive recurrent ovarian cancer: a network meta-analysis. Front Oncol. 2021;11: 785102.
Xu Y, Ding L, Tian Y, Bi M, Han N, Wang L. Comparative efficacy and safety of PARP inhibitors as maintenance therapy in platinum sensitive recurrent ovarian cancer: a network meta-analysis. Front Oncol. 2020;10: 573801.
Robillard L, Nguyen M, Harding TC, Simmons AD. In vitro and in vivo assessment of the mechanism of action of the PARP inhibitor rucaparib. Cancer Res. 2017;77(Suppl. 13):abstract 2475.
e, Kolarova T, Qi JW, Manivong K, Chalukya M, et al. Therapeutic potential of the poly(ADP-ribose) polymerase inhibitor rucaparib for the treatment of sporadic human ovarian cancer. Mol Cancer Ther. 2013;12:1002–15.
Nesic K, Kondrashova O, Hurley RM, McGehee CD, Vandenberg CJ, Ho GY, et al. Acquired RAD51C promoter methylation loss causes PARP inhibitor resistance in high-grade serous ovarian carcinoma. Cancer Res. 2021;81:4709–22.
Swisher EM, Lin KK, Oza AM, Scott CL, Giordano H, Sun J, et al. Rucaparib in relapsed, platinum-sensitive high-grade ovarian carcinoma (ARIEL2 Part 1): an international, multicentre, open-label, phase 2 trial. Lancet Oncol. 2017;18:75–87.
Kristeleit R, Shapiro GI, Burris HA, Oza AM, LoRusso P, Patel MR, et al. A phase I-II study of the oral PARP inhibitor rucaparib in patients with germline BRCA1/2-mutated ovarian carcinoma or other solid tumors. Clin Cancer Res. 2017;23:4095–106.
Kristeleit R, Lisyanskaya A, Fedenko A, Dvorkin M, de Melo AC, Shparyk Y, et al. Rucaparib versus standard-of-care chemotherapy in patients with relapsed ovarian cancer and a deleterious BRCA1 or BRCA2 mutation (ARIEL4): an international, open-label, randomised, phase 3 trial. Lancet Oncol. 2022;23:465–78.
Coleman RL, Oza AM, Lorusso D, Aghajanian C, Oaknin A, Dean A, et al. Rucaparib maintenance treatment for recurrent ovarian carcinoma after response to platinum therapy (ARIEL3): a randomised, double-blind, placebo-controlled, phase 3 trial. Lancet. 2017;390:1949–61.
Konecny GE, Ozo AM, Tinker AV, Coleman RL, O’Malley DM, Maloney L, et al. Rucaparib in patients with relapsed, primary platinum-sensitive high-grade ovarian carcinoma with germline or somatic BRCA mutations: integrated summary of efficacy and safety from the phase II study ARIEL2. Gynecol Oncol. 2017;145(Suppl. 1):2.
Oza AM, Tinker AV, Oaknin A, Shapira-Frommer R, McNeish IA, Swisher EM, et al. Antitumor activity and safety of the PARP inhibitor rucaparib in patients with high-grade ovarian carcinoma and a germline or somatic BRCA1 or BRCA2 mutation: integrated analysis of data from Study 10 and ARIEL2. Gynecol Oncol. 2017;147:267–75.
Abida W, Patnaik A, Campbell D, Shapiro J, Bryce AH, McDermott R, et al. Rucaparib in men with metastatic castration-resistant prostate cancer harboring a BRCA1 or BRCA2 gene alteration. J Clin Oncol. 2020;38:3763–72.
ClinicalTrials.gov. A study to evaluate rucaparib in patients with solid tumors and with deleterious mutations in HRR genes (LODESTAR). https://clinicaltrials.gov/ct2/show/NCT04171700. Accessed 25 Aug 2021.
ClinicalTrials.gov. A study to evaluate rucaparib in combination with other anticancer agents in patients with a solid tumor (SEASTAR). https://clinicaltrials.gov/ct2/show/NCT03992131. Accessed 25 Aug 2021.
Jenner ZB, Sood AK, Coleman RL. Evaluation of rucaparib and companion diagnostics in the PARP inhibitor landscape for recurrent ovarian cancer therapy. Future Oncol. 2016;12:1439–56.
Plummer R, Jones C, Middleton M, Wilson R, Evans J, Olsen A, et al. Phase I study of the poly(ADP-ribose) polymerase inhibitor, AG014699, in combination with temozolomide in patients with advanced solid tumors. Clin Cancer Res. 2008;14:7917–23.
Wilson RH, Evans TJ, Middleton MR, Molife LR, Spicer J, Dieras V, et al. A phase I study of intravenous and oral rucaparib in combination with chemotherapy in patients with advanced solid tumours. Br J Cancer. 2017;116:884–92.
Shapiro GI, Kristeleit RS, Burris HA, LoRusso P, Patel MR, Drew Y, et al. Pharmacokinetic study of rucaparib in patients with advanced solid tumors. Clin Pharmacol Drug Dev. 2019;8:107–18.
Liao M, Watkins S, Nash E, Isaacson J, Etter J, Beltman J, et al. Evaluation of absorption, distribution, metabolism, and excretion of [14C]-rucaparib, a poly(ADP-ribose) polymerase inhibitor, in patients with advanced solid tumors. Invest New Drugs. 2019;38:765–75.
Grechko N, Skarbova V, Tomaszewska-Kiecana M, Ramlau R, Centkowski P, Drew Y, et al. Pharmacokinetics and safety of rucaparib in patients with advanced solid tumors and hepatic impairment. Cancer Chemother Pharmacol. 2021;88:259–70.
Xiao JJ, Nowak D, Ramlau R, Tomaszewska-Kiecana M, Wysocki PJ, Isaacson J, et al. Evaluation of drug-drug interactions of rucaparib and CYP1A2, CYP2C9, CYP2C19, CYP3A, and P-gp substrates in patients with an advanced solid tumor. Clin Transl Sci. 2019;12:58–65.
Liao M, Jeziorski KG, Tomaszewska-Kiecana M, Láng I, Jasiówka M, Skarbová V, et al. A phase 1, open-label, drug-drug interaction study of rucaparib with rosuvastatin and oral contraceptives in patients with advanced solid tumors. Cancer Chemother Pharmacol. 2021;88:887–97.
Tamura K, Matsumoto K, Yonemori K, Hasegawa K, Habeck J, Jones E, et al. Evaluation of rucaparib in Japanese patients with a previously treated advanced solid tumor. Cancer Res. 2021;81(Suppl. 13):abstract CT124.
Sparidans RW, Durmus S, Schinkel AH, Schellens JH, Beijnen JH. Liquid chromatography-tandem mass spectrometric assay for the PARP inhibitor rucaparib in plasma. J Pharm Biomed Anal. 2014;88:626–9.
Green M, Ma SC, Goble S, Giordano H, Maloney L, Simmons AD, et al. Population pharmacokinetics of rucaparib in patients with advanced ovarian cancer or other solid tumors. Cancer Chemother Pharmacol. 2022;89:671–82.
Smith BP, Vandenhende FR, DeSante KA, Farid NA, Welch PA, Callaghan JT, et al. Confidence interval criteria for assessment of dose proportionality. Pharm Res. 2000;17:1278–83.
Abida W, Campbell D, Patnaik A, Shapiro JD, Sautois B, Vogelzang NJ, et al. Non-BRCA DNA damage repair gene alterations and response to the PARP inhibitor rucaparib in metastatic castration-resistant prostate cancer: analysis from the phase 2 TRITON2 study. Clin Cancer Res. 2020;26:2487–96.
Liao M, Jaw-Tsai S, Beltman J, Simmons AD, Harding TC, Xiao JJ. Evaluation of in vitro absorption, distribution, metabolism and excretion and assessment of drug-drug interaction of rucaparib, an orally potent poly(ADP-ribose) polymerase inhibitor. Xenobiotica. 2020;50:1032–42.
Nguyen M, Robillard L, Harding TC, Xiao JJ, Simmons AD, Kristeleit H, et al. Intracranial evaluation of the in vivo pharmacokinetics, brain distribution, and efficacy of rucaparib in BRCA-mutant, triple-megative breast cancer. Cancer Res. 2019;79(Suppl. 13):3888.
Center for Drug Evaluation and Research. Multi-discipline review/summary, clinical, non-clinical for NDA 209115. US Department of Health and Human Services; Food and Drug Administration; Center for Drug Evaluation and Research. 2017. https://www.accessdata.fda.gov/drugsatfda_docs/nda/2016/209115Orig1s000MultiDisciplineR.pdf. Accessed 2 Aug 2019.
Konecny GE, Oza AM, Tinker AV, Oaknin A, Shapira-Frommer R, Ray-Coquard I, et al. Population exposure-efficacy and exposure-safety analyses for rucaparib in patients with recurrent ovarian carcinoma from Study 10 and ARIEL2. Gynecol Oncol. 2021;161:688–775.
Chowdhury S, Patnaik A, Campbell D, Shapiro J, Bryce AH, McDermott R, et al. Rucaparib population pharmacokinetics (PPK) and exposure-response (ER) analyses in patients (pts) with metastatic castration-resistant prostate cancer (mCRPC) in TRITON2. Ann Oncol. 2020;31(Suppl. 4):S533–4.
Harold JA, Free SC, Bradley WH. Pharmacokinetics and clinical response to single agent rucaparib in a dialysis dependent patient with BRCA associated breast and recurrent ovarian cancer. Gynecol Oncol Rep. 2018;26:91–3.
National Cancer Institute (NCI). Cancer Therapy Evaluation Program (CTEP) Protocol Template for Organ Dysfunction Studies. National Cancer Institute (NCI). 2018. https://ctep.cancer.gov/protocolDevelopment/templates_applications.htm. Accessed 20 Jun 2018.
Rao A, Morris D, Assikis VJ, Jha GG, Ryan CJ, Ablaza A-J, et al. Rucaparib plus enzalutamide in patients (pts) with metastatic castration-resistant prostate cancer (mCRPC): pharmacokinetics (PK) and safety data from the phase Ib RAMP study. J Clin Oncol. 2021;39(Suppl. 6):79.
Center for Drug Evaluation and Research. Clinical pharmacology and biopharmaceutics review(s). U.S. Department of Health and Human Services; Food and Drug Administration; Center for Drug Evaluation and Research. 2012. https://www.accessdata.fda.gov/drugsatfda_docs/nda/2012/203415Orig1s000ClinPharmR.pdf. Accessed 9 Apr 2020.
A clinical study evaluating the benefit of adding rucaparib to enzalutamide for men with metastatic prostate cancer that has become resistant to testosterone-deprivation therapy (CASPAR). ClinicalTrials.gov identifier: NCT04455750. https://clinicaltrials.gov/ct2/show/NCT04455750. Accessed 5 Apr 2021.
European Medicines Agency. Guideline on the investigation of drug interactions. 2012. https://www.ema.europa.eu/en/documents/scientific-guideline/guideline-investigation-drug-interactions_en.pdf. Accessed 8 Aug 2019.
US Department of Health and Human Services Food and Drug Administration. Guidance for industry. Drug interaction studies: study design, data analysis, implications for dosing, and labeling recommendations. 2012. https://www.xenotech.com/wp-content/uploads/2020/07/2012-FDA-DDI-Guidance.pdf. Accessed 4 Aug 2019.
Chainuvati S, Nafziger AN, Leeder JS, Gaedigk A, Kearns GL, Sellers E, et al. Combined phenotypic assessment of cytochrome p450 1A2, 2C9, 2C19, 2D6, and 3A, N-acetyltransferase-2, and xanthine oxidase activities with the “Cooperstown 5+1 cocktail.” Clin Pharmacol Ther. 2003;74:437–47.
Mathialagan S, Rodrigues AD, Feng B. Evaluation of renal transporter inhibition using creatinine as a substrate in vitro to assess the clinical risk of elevated serum creatinine. J Pharm Sci. 2017;106:2535–41.
Coleman RL, Ledermann JA. Maintenance treatment for recurrent ovarian carcinoma: evidence supporting the efficacy and safety of PARP inhibitors. Eur Oncol Haematol. 2019;15:29–40.
LaFargue CJ, Dal Molin GZ, Sood AK, Coleman RL. Exploring and comparing adverse events between PARP inhibitors. Lancet Oncol. 2019;20:e15-28.
Zibetti Dal Molin G, Westin SN, Msaouel P, Gomes LM, Dickens A, Coleman RL. Discrepancy in calculated and measured glomerular filtration rates in patients treated with PARP inhibitors. Int J Gynecol Cancer. 2020;30:89–93.
US Food and Drug Administration (FDA). Clinical drug interaction studies: cytochrome P450 enzyme- and transporter-mediated drug interactions guidance for industry. 2020. https://www.fda.gov/regulatory-information/search-fda-guidance-documents/clinical-drug-interaction-studies-cytochrome-p450-enzyme-and-transporter-mediated-drug-interactions. Accessed 13 Oct 2020.
Sarapa N, Britto MR. Challenges of characterizing proarrhythmic risk due to QTc prolongation induced by nonadjuvant anticancer agents. Expert Opin Drug Saf. 2008;7:305–18.
US Department of Health and Human Services Food and Drug Administration. Guidance for industry: E14 clinical evaluation of QT/QTc interval prolongation and proarrhythmic potential for non-antiarrhythmic drugs. 2005. https://www.fda.gov/downloads/Drugs/GuidanceComplianceRegulatoryInformation/Guidances/UCM073153.pdf. Accessed 16 Jul 2021.
Acknowledgements
Editorial assistance with the preparation of the manuscript was funded by Clovis Oncology Inc., the developers of rucaparib, and provided by Malcolm Darkes, Shelly Lim, Nathan Yardley, and Stephen Bublitz of Ashfield MedComms, an Inizio company.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Funding
This work was funded by Clovis Oncology, Inc.
Conflicts of interest//competing interests
Mingxiang Liao, Jeri Beltman, Heidi Giordano, Thomas C. Harding, Lara Maloney, Andrew D. Simmons, and Jim J. Xiao are or were employees of Clovis Oncology Inc. and may own stock or have stock options in that company.
Ethics approval
Not applicable.
Consent to participate
Not applicable.
Consent for publication
Not applicable.
Availability of data and material
Not applicable.
Code availability
Not applicable.
Authors’ Contributions
All authors were fully responsible for all content and editorial decisions.
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution-NonCommercial 4.0 International License, which permits any non-commercial use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if changes were made. The images or other third party material in this article are included in the article's Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article's Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by-nc/4.0/.
About this article
Cite this article
Liao, M., Beltman, J., Giordano, H. et al. Clinical Pharmacokinetics and Pharmacodynamics of Rucaparib. Clin Pharmacokinet 61, 1477–1493 (2022). https://doi.org/10.1007/s40262-022-01157-8
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s40262-022-01157-8