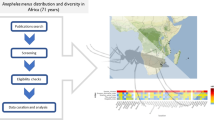
Abstract
Purpose of Review
The invasive Asian mosquito vector—Anopheles stephensi Liston, 1901—is poised to greatly complicate malaria eradication efforts across Africa. This species has been reported in an increasing number of African nations and has the potential to introduce malaria into most of Africa’s largest cities. Climate change is a dominant force changing population dynamics across the continent and driving human populations to migrate to urban centers.
Recent Findings
This work presents all high-quality surveillance data documenting An. stephensi to date, including an overlooked report of the species collected in Egypt in 1966. Finally, we provide detailed images of adult and larval morphology and bionomics descriptions.
Summary
Based on our current knowledge of Anopheles stephensi, we explore how climate change may impact its distribution and malaria rates in the coming decades. We also identify key knowledge gaps related to this species invasion including the most up-to-date information on the taxonomy, morphological characters, and bionomics of An. stephensi. Tools that are publicly available via VectorMap are also presented along with guidance on strengthening surveillance programs targeting An. stephensi using these tools.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
The incursion of Anopheles stephensi Liston, 1901, into Africa is undermining decades of work to reduce malaria infections across the continent. Here, we present our current knowledge of this species spread and summarize tools currently available to track and predict its impact. Climate change may exacerbate the challenge to limit the expansion of An. stephensi, but there are lessons from the past that may be useful to guide our response.
The type locality of An. stephensi is Ellichpur, India, and its native range extends from the Indo-China region into the Middle East including Saudi Arabia and Oman [1]. It is widely reported that the first introduction of An. stephensi into continental Africa was in Djibouti in 2012, following surveillance of unprecedented malaria outbreaks in Djibouti City [2•]. However, this is erroneous, and our detailed literature search recovered documentation of An. stephensi larvae and adults collected from Ras Ghareb, Egypt along the coast of the Gulf of Suez in 1966 [3•]. There do not appear to be any other reports of this species found in Africa until it was detected in Djibouti. Since 2012, An. stephensi has been detected throughout Northeast Africa and as far South as Nigeria and Kenya [4•, 5•, 6•, 7•]. How exactly An. stephensi spread to Africa is still a mystery. Recent studies have shown that mosquito species are traveling great distances using high-altitude wind migration [8]. This may be a mechanism for An. stephensi to cross the Red Sea and spread across the continent [9]. However, other evidence suggests that given the distribution pattern so far, it is possible that marine cargo ships may be helping to spread this species [10]. A map of the current country-level distribution of An. stephensi in Africa is provided in Fig. 1, and a list of references confirming these detections for the first time is provided in Table 1.
Confirmed country-level distribution of Anopheles stephensi in Africa. Countries in red have confirmed the presence of An. stephensi on at least one occasion. Base map sourced from Global Administrative Areas (GADM) version 4.0: https://gadm.org/download_country.html. Accessed August 8, 2023
Anopheles stephensi has been implicated in severe malaria outbreaks in Djibouti where, until 2011, malaria was considered all but eradicated [2•, 13]. One study estimated that malaria rates in neighboring Ethiopia could increase by at least 50% if effective control measures for An. stephensi are not implemented [14]. As primarily an urban malaria vector, An. stephensi is wreaking havoc on populations not typically exposed to malaria or Africa’s native malaria vector species. This invader is also a competent vector of both Plasmodium falciparum and P. vivax malaria parasites, as well as O’nyong-nyong virus, making it a formidable threat to human health [15, 16]. While climate change is not implicated as a cause of this invasive species introduction, it is highly likely to increase malaria rates across the continent as humans migrate from rural areas and concentrate in urban centers. Some predictions claim that up to 60% of the estimated 2.3 billion Africans will be urban dwellers by 2050 [17]. Indeed, several preliminary predictions of this species’ potential distribution and impact on malaria transmission identify virtually every low-altitude urban area at risk for the highest levels of malaria burden increases [14, 18•].
While mitigating the impact of An. stephensi in Africa is a daunting challenge, there are lessons from history that can offer guidance. Although the invasion of Africa by An. stephensi is a major event, it is not the first time a major malaria vector has invaded a continent outside its native range. The invasion of the African vector species An. arabiensis into Brazil—first detected in 1930—ended with the successful eradication of populations despite their establishment for over 10 years [19]. Here, we explore strategies that were implemented nearly 100 years ago that still contribute to the successful mitigation or eradication of An. stephensi in Africa.
Climate Change and Malaria in Africa
It should be noted that although the combined countries of Africa contribute less greenhouse gas emissions annually than larger, single countries such as the USA or China, they are far more vulnerable to the most severe consequences of climate change [20]. Already, the continent is feeling the impact of an overall decline in rainfall over the past 50 years, linked to climate change [21]. This decline in moisture availability has resulted in a “push” on populations from rural areas into urban zones as traditional subsistence agriculture becomes less dependable, while increasing urbanization also “pulls” populations into these areas in search of better economic opportunities [22]. This “push–pull” towards urban zones from rural areas is predicted to continue for the rest of the century [23]. In fact, urban land cover in Sub-Saharan Africa is predicted to expand by more than twelve times current levels by 2050 [17].
Rising average temperatures will have a direct impact on the entire life cycle of both mosquito vectors and malaria parasites. Temperature fluctuations have shown to either increase or decrease parasite development, with optimal to maximum suitability ranges all supporting development [24•]. Air temperature is therefore a useful predictor of malaria prevalence [25]. Studies show that certain regions, such as West and Central Africa, will see malaria rates drop, while others in Southern Africa may experience increased infection rates [26]. A study of global incidence of bird malaria also found a strong correlation between rising temperatures and Plasmodium infection rates among birds [27]. They suggested that temperature anomalies had more impact on infection rates than migratory routes, suggesting that climate change impacts risk of infection. Impacts of bird malaria are observed earlier than those in humans, as there are typically no interventions to mitigate malaria infection in wild bird populations [28].
A recent study demonstrated that temperature, rather than precipitation, may be a better indicator of when peak activity of An. stephensi may occur throughout the year [29] and in both An. stephensi and An. gambiae s.l., there is a close association of temperature to the environmental suitability of malaria transmission [30]. Duration and productivity of parasite development are highly correlated to temperature as well [11]. Monitoring changes in temperature and precipitation and relating that data to vector surveillance results will be key to fully understanding the impacts of climate change to malaria transmission.
Know the Vector, Know the Threat
To predict how climate change may impact An. stephensi spread across Africa, we must understand its taxonomic status and corresponding biology. The current taxonomic status of An. stephensi is unresolved, and there are three known egg phenotypes: the type form, mysorensis Sweet & Rao, and an intermediate form [31•]. In the Indian subcontinent, the type form is regarded as highly anthropophilic in urban areas, whereas the mysorensis form is primarily zoophilic and confined mostly to rural areas [32]. To date, egg morphology from An. stephensi material collected in Africa, including both urban and rural collections of An. stephensi, have yet to be reported. It is not known if the mysorensis form is present in Africa or if it will play a significant role in malaria transmission [33]. DNA analysis of the samples used to support the first report of An. stephensi in Djibouti corresponded to the type form [2•], and later network analysis using mtDNA COI barcodes for samples collected in Djibouti and Ethiopia again confirmed these populations as the “type form” of An. stephensi, with data analysis supporting at least two points of origin—one from India-Pakistan and one from the Arabian Peninsula. Phylogenetic analysis further revealed that An. stephensi specimens collected in Ethiopia and Djibouti were two distinct populations originating from different locations in Pakistan [31•].
Larval habitats of An. stephensi are highly unusual as compared to nearly all other Anopheles species in that they can include a range of artificial containers, such as domestic water storage or rainwater drainage systems [34], like those preferred by other problematic domesticated mosquitoes, (e.g., Aedes aegypti (Linnaeus, 1762)). Larvae of the An. stephensi ‘mysorensis’ form are also commonly found in earthenware containers in rural areas [35]. This similarity to the dengue fever vector Ae. aegypti offers an opportunity to modify existing vector surveillance and control efforts to target An. stephensi. Larvae have also been found to be highly saline-tolerant; however, it is not known if this observation is the type or mysorensis form, or some unidentified form [36]. Larvae of An. stephensi have demonstrated great ability to adapt to local environmental conditions as it spreads further into Africa [7•]. Therefore, characterizing the habitats of breeding sites will be an essential element of effective surveillance. In Table 2, we provide a comprehensive list of habitats where An. stephensi larvae have been collected in Africa based on published reports.
Female An. stephensi appear to be primarily endophilic and endophagic; however, exophilic/exophagic behavior has been observed during the warmer times of the year [38]. While considered highly anthropophilic, An. stephensi will also readily feed on domestic livestock [39]. A recent survey of An. stephensi in Chennai, India, found the highest densities of Plasmodium-infected adults associated with cattle sheds and other thatched roof structures, rather than human dwellings [37]. This suggests that An. stephensi may be feeding on humans inside their homes but exiting these structures to rest outside, which would render indoor residual spraying efforts or indoor pyrethroid spray catches ineffective to control, or capture, host-seeking An. stephensi. It is important to note that routinely employed CDC light traps are not as effective for capturing adult An. stephensi as outdoor aspiration, resting boxes and animal baited traps [39].
Knowledge Gaps
Our team developed VectorMap (vectormap.si.edu)—a free, open-access data platform that preserves curated surveillance data to track the distribution of arthropod vectors, model their potential distribution in space and time, and analyze bionomic data, such as seasonality, host preferences, and feeding patterns [40, 41]. Users from around the world can submit their data directly to VectorMap using a web-based portal. A key feature of VectorMap is the detail at which each observation is documented, including information about the collection and identification methods, pathogen screening results, and voucher status [42]. These data can characterize our cumulative observations about vector distributions and highlight key knowledge gaps. VectorMap currently contains only 123 unique observation records for An. stephensi in Africa, representing 942 specimens collected from Djibouti, Egypt, Ethiopia, Kenya, Somalia, and the Sudan. A map displaying these records by stage (immatures or adults) is presented in Fig. 2. Each of these records were captured from published literature, but do not represent the complete distribution as we know it today. Recent reports of An. stephensi from Ghana, and Eritrea were reported during a 2023 World Health Organization regional meeting but have yet to publish surveillance data in peer-reviewed journals [12•]. Other distribution reports, such as Nigeria, have not reported locality information in sufficient detail to allow accurate mapping [6•]. The volume of publicly available, high-quality surveillance data targeting An. stephensi in Africa must be improved to track this species range and predict where it may be moving next more accurately. Even with our limited knowledge, there appears to be significant gaps in surveillance coverage already, particularly in central Africa. More concerning, not a single study of An. stephensi in Africa has thus far preserved morphological voucher specimens in a publicly accessible repository or institution. Perhaps this is due to how mosquito surveillance has changed in recent years. Modern surveillance is focused more on collection and testing adults for pathogens, rather than surveying the immature habitats. Reliance on adult surveillance for An. stephensi is not effective, as (1) the species are not overly attracted to light and (2) this species is establishing in urban, light pollution-heavy environments. For these reasons, An. stephensi can be hiding in plain sight and often missed in routine surveillance efforts. WRBU has preserved genetic voucher material from the initial detection of An. stephensi in Djibouti along with morphological vouchers from across its native range as part of the National mosquito collection. However, more genetic material and morphological vouchers representing all life stages collected throughout Africa are urgently needed.
Map of Anopheles stephensi surveillance results from VectorMap. Data were obtained from records published in the following institutions and accessed through the VectorMap data portal (http://www.vectormap.si.edu) on 21 July 2023 [2•, 3•, 4•, 5•, 6•, 7•, 37]. Base map sourced from Global Administrative Areas (GADM) version 4.0: https://gadm.org/download_country.html. Accessed August 8, 2023
Population levels of mosquito vector species are highly dependent on environmental variables such as temperature, precipitation, and vegetation [43, 44]. These variables can be used to model the distribution and seasonality of mosquito vector populations [45]. Geographic Information Systems (GIS) techniques are widely being implemented to make correlations between mosquito surveillance data and environmental observations [46]. GIS offers the capability to make more accurate predictions of where and when mosquito larvae are present within a given landscape.
With high-quality data, it is even possible to make predictions of how species ranges may be impacted in the coming decades due to expected impacts from climate change [47]. Standardization of accurate and precise field collection data and regular preservation of voucher specimens documenting An. stephensi observations will provide a foundation for the development of models and data-driven mitigation strategies. By linking vector surveillance data to environmental data and even human malaria incidence, we can gain a clearer understanding of where and when risk of infection is the highest and when implementation of control strategies will be the most effective.
Climate change is predicted to continue impacting the distribution of vector species in Africa over the course of this century [48]. A recent study modeling the potential shifts in distributions of Aedes albopictus (Skuse, 1895) and Ae. aegypti predicted some areas that currently support these species will become too hot and dry to support these populations while other areas that currently do not support these species may become more favorable by the end of the century [49]. Several studies have also predicted similar scenarios for malaria in Africa [26, 50]. For example, projected future climatic conditions are expected to cause increased suitability for malaria transmission in the East African highlands and further South into Sub-Saharan Africa where previously malaria transmission was rare [28]. It is imperative to establish robust surveillance systems that capture longitudinal datasets and routinely close gaps in surveillance coverage overtime. These data should iteratively update models on the projected distribution of An. stephensi as well as malaria risk, as new data is made available.
Morphological identification of both the larval and adult life stages will be essential to An. stephensi surveillance efforts in Africa. Given the difficulty associated with collecting adult An. stephensi specimens in urban environments, and the desire to screen these samples for Plasmodium infection, targeted larval collections may be the most effective way to confirm or rule out the presence of An. stephensi. However, without expert knowledge of diagnostic morphology and the capability to examine specimens at high magnification, this will be a major challenge to execute across Africa. Africa’s most notorious native malaria vectors, members of the An. gambiae complex, look very similar to An. stephensi larvae, as are all members of the subgenus Cellia. This means An. stephensi cannot be readily distinguished from native species unless examined by a well-trained taxonomist. Support to develop training programs for local para-taxonomists across the continent is urgently needed so that more individuals are capable of confirming the presence of An. stephensi in its immature stages.
Identification keys are available for the adult and larval stages of An. stephensi [51,52,53,54]. However, these keys will need to be updated regularly as we learn the complete distribution of An. stephensi in Africa. As most mosquito control workers will be unfamiliar with this invasive species, we have provided diagnostic morphological characters for adult and larval stages in Figs. 3 and 4, respectively [1]. Field-ready identification tools covering both morphological and molecular approaches will also be essential. Morphological keys available on mobile devices covering all life stages, including images of immatures and eggs would support training of para-taxonomists to reliably identify specimens captured during surveillance and separate specimens for Plasmodium screening. Widespread use of field-based molecular screening tools would allow local confirmation of vector species and Plasmodium infection without the need for costly shipments to far flung laboratories.
Diagnostic characters of Anopheles stephensi adult female. Adult: A Habitus, adult female. B Head, adult female lateral view: (1) Palp segment 5 entirely pale; (2) maxillary palpus with pale bands; (3) erect head scales broad, white on vertex and dark brown laterally and posteriorly. C Thorax, adult female dorsal view; scutum with obvious pale scales in addition to setae; scutal fossa with scattered pale scales. D Wing, adult female lateral view: (1) Vein 1A with 3 dark spots; wing with pale spots present on nearly all veins. E Abdomen, adult female dorsal view: II–VII-Te without dark scale tufts. F Abdomen, adult female lateral view: V–VIII-S usually with pale scales [1]
Diagnostic characters of Anopheles stephensi larvae. Larva: A Habitus. B Head, dorsal view: Seta 1-A small, unbranched; setae. C Head, dorsal view: setae 2,3-C smooth, not aciculate; distance between seta 2-C > distance between setae 2-C and 3-C on one side. D Head, dorsal view: setae 5–7-C long and branched. E Thorax, lateral view: setae 1,2-P inserted on dark, sclerotized tubercles. F Thorax, dorsal view: (1) setae 9,10-P and 9,10-M not all unbranched. (2) setae 9-M plumose, branched from base; (3) setae 10–12-M unbranched. G Thorax, dorsal view: setae 9,10-T branched [1]
A growing global concern is rising insecticide resistance (IR) among Anopheles species, particularly to pyrethroids, which are commonly used on insecticide-treated bed nets (ITNs) and for indoor residual spraying (IRS) [55]. Any surveillance system should therefore incorporate IR screening as well to identify where resistance may be developing. Resistance data should also be shared broadly so that local mosquito control workers have knowledge of what insecticide classes may be failing and which ones may still be effective. VectorMap also hosts, IRMap, a map service dedicated to preserving and sharing insecticide resistance surveillance results. A key feature of IRMap is to integrate molecular confirmations (e.g., kdr mutations) and traditional testing methods (CDC bottle assay) within a single, standardized data schema. This allows for multiple data streams to combine within the database for a more comprehensive view of resistance rates. Climate change is not considered a driver of IR in mosquitoes, rather an over reliance on chemical control of insects in general is to blame [56]. This also supports the non-chemical alternative of point-source reduction targeting larval habitats.
Finally, a streamlined data collection system and pipelines for open data sharing will greatly improve our knowledge and ensure that high-quality surveillance data detailing vector occurrence, pathogen detection, human disease incidence, and IR detections are all standardized and made freely available. Raw data should be made available for independent analyses, and the system should present data visualizations such as dynamic dashboards that provide real-time information to local decision makers and health planners [57].
Lessons from History
With such a daunting task before us, perhaps there are some lessons from history that can guide our response. Almost 100 years ago, another malaria vector colonized a new continent and quickly caused malaria cases to rise. In March 1930, R.C. Shannon reported some unusual larvae from a streambed at Natal, Brazil, and identified them as the major Afrotropical vector Anopheles gambiae. Molecular analyses of preserved voucher specimens from these collections later confirmed these were its sister taxa—Anopheles arabiensis Patton, 1905 [58]. Nearly 10 years from the initial discovery of this invasive species in Brazil, one of the most ambitious and successful eradication campaigns was undertaken. Initially however, experts struggled to convince public authorities of the importance of this introduction and only after significant rises in malaria cases and deaths were proper resources allocated to the issue [19]. Fred Soper and D. B. Wilson described the issue this way:
“That it was done only after the regional disaster of 1938 was due entirely to the fact that local health officers did not have the necessary authority to overcome the power of vested interests.”
Even before widespread support for this issue was granted, the Brazilian Malaria Service (BMS) worked to characterize the bionomics of this invader in as much detail as possible. The BMS made observations across Northeast Brazil characterizing larvae habitat, adult feeding behavior, duration and viability of eggs, and seasonal variation [19, 59]. Once it became clear that An. arabiensis was quickly spreading across Brazil and that malaria case rates were rising at an alarming rate, the Brazilian Government, with support from the Rockefeller Foundation, formed the Antimalaria Service, among their goals was the total eradication of An. arabiensis. Eradication of an entire species from a continent was a monumental challenge; however, they drew inspiration from the successful eradication of Ae. aegypti from Havana, Cuba, by targeted elimination of breeding sites as led by CPT William C. Gorgas (US Army) [60]. The foundation of both eradication campaigns was the parceling of land into individual control “zones.” Each of these zones was assigned an inspector who was individually responsible for implementing source reduction and applying larvicide [19]. Soper and Wilson stressed the importance of communication and accountability that resonates today:
“… it was always the inspector who actually carried out the anti-[arabiensis] measures and since he often worked alone and far from headquarters, it was essential to establish individual responsibility for work done and individual responsibility for checking such work.”
It should be noted that in addition to point-source reduction of breeding sites, the program also included support for public education on reducing malaria transmission risk, the dispersal of anti-malaria drugs, and a program requiring the de-insectization of buildings, as well as planes and other vehicles, to reduce further introductions [19]. By 1940, no trace of An. arabiensis could be found in Brazil and the program was suspended.
There are a few key takeaways from this historic campaign that could be applied to dealing with An. stephensi in Africa: (1) It will require carefully documented scientific evidence to convince authorities to provide additional support. (2) A strong understanding of the invasive species biology is essential to developing a successful control strategy. (3) Empowering local inspectors to take individual responsibility for their communities decentralizes decision making and makes control efforts more efficient, and with these coordinated efforts.
There are also a few key differences between the introduction of An. arabiensis and An. stephensi. Firstly, surveillance was conducted by taxonomists. Larvae of An. arabiensis were morphologically distinct from local Brazilian mosquito species as they belonged to a different subgenus, thus were readily identified during routine sampling. In Africa, we do not have this advantage. Anopheles stephensi belong to the same subgenus (Cellia) as the most common local malaria vectors so introductions will be much more challenging to detect. Adults are not readily collected in routine surveillance and, larval surveys are infrequently used by vector control teams. Secondly, government and philanthropist organizations agreed to make eradication the goal in Brazil and provided appropriate support. To date, there is no official goal by governments or NGOs operating in Africa to eradicate this invasive species or moves to provide the necessary support to do so.
Conclusions
The impact of climate change on vector-borne disease trends in Africa over the remainder of the century will be difficult to predict. One clear trend is the “push” and “pull” on rural populations to migrate to urban areas, creating megacity metropolises [22]. At the same time, An. stephensi is stealthily spreading and establishing in urban areas and is predicted to find suitable habitat across the entire continent [18•]. Since its demonstrated role in malaria outbreaks in Djibouti, there has been a steady drumbeat from the scientific community that increased surveillance for this species is necessary [2•, 61, 62]. A growing number of experts are also calling for immediate increased support for the control of this species to start slowing its spread [63]. Compounding this problem is the fact that mosquito control workers in Africa are grossly understaffed and in desperate need of additional support with as few as 8% of national malaria programs reporting the capacity to conduct routine surveillance [64]. An undertrained, ill-equipped vector control workforce that is mostly unfamiliar with this species, and already stretched thin is a recipe for disaster. It is imperative that new tools be made widely available in Africa to improve species detection, and better understand the risk it poses to the continental goal of malaria eradication through additional efforts to assess Plasmodium infection and IR prevalence.
History provides examples of how invasive mosquito species can be eradicated. When An. arabiensis invaded Brazil in the 1930s, it took nearly 10 years to convince authorities and funding agencies to allocate more resources to the problem and to officially make eradication a goal. However, by empowering local communities with knowledge, tools, and funding support, eradication became an attainable goal. Prioritizing larval control also provides a non-chemical, cost effective measure to reduce vector populations [65]. It is also important to note that the eradication of An. arabiensis was only possible after significant effort to convince government officials and funding organizations to support the goal of eradication [66].
Critically, most of our current knowledge about this vector comes from observations made across its native range [67]. Therefore, more observations of this species across Africa are needed to fully understand how its presence is impacting malaria transmission. While implementing control, we must also be mindful of rising IR among vector species and screen samples for such control measure failures to adjust insecticide use. Non-chemical interventions, public health education and a free flow of data are also needed. The invasion of An. stephensi is a stark reminder of the many arthropod vector threats impacting human and animal health in Africa. Even without this emerging issue, climate change will bring many more challenges before the end of the century.
Data availability
All data presented here is publicly available.
Change history
08 December 2023
A Correction to this paper has been published: https://doi.org/10.1007/s40475-023-00312-w
References
Papers of particular interest, published recently, have been highlighted as: • Of importance
Wilkerson RC, Linton Y-M, Strickman D. Mosquitoes of the world (Vols 1 & 2). Johns Hopkins University Press; 2021.
• Faulde MK, Rueda LM, Khaireh BA. First record of the Asian malaria vector Anopheles stephensi and its possible role in the resurgence of malaria in Djibouti, Horn of Africa. Acta Trop. 2014;139:39–43 This publication reports the initial discovery of Anopheles stephensi collected from Djibouti.
• Gad AM. Anopheles stephensi Liston in Egypt, UAR. Mosq News. 1967;27(2):171. This publication reports the initial discovery of Anopheles stephensi collected from Egypt in 1966; this appears to be the first report of this species in Africa.
• Ahmed A, Khogali R, Elnour MA, Nakao R, Salim B. Emergence of the invasive malaria vector Anopheles stephensi in Khartoum State, Central Sudan. Parasit Vectors. 2021;14(1):1–5. This publication reports the initial discovery of Anopheles stephensi collected from the Sudan.
• Ali S, Samake JN, Spear J, Carter TE. Morphological identification and genetic characterization of Anopheles stephensi in Somaliland. Parasit Vectors. 2022;15(1):247. (This publication reports the initial discovery of Anopheles stephensi collected from Somalia.)
• Nigerian Institute of Medical Research. 2022. NIMR discovers new malaria vector in northern Nigeria. https://nimr.gov.ng/nimr/wp-content/uploads/2022/07/NIMR-discovers-new-malaria-vector-in-northern-Nigeria-Healthwise_-healthwise.punchng.com_.pdf. Date: July 26, 2022. Accessed July 2023. This publication reports the initial discovery of Anopheles stephensi collected from Nigeria; this is not a peer-reviewed study.
• Ochomo EO, Milanoi S, Abong’o B, Onyango B, Muchoki M, Omoke D, Olanga E, Njoroge L, Juma E, Otieno JD, Matoke D. Molecular surveillance leads to the first detection of Anopheles stephensi in Kenya., 31 May 2023, PREPRINT (Version 2) available at Research Square: https://doi.org/10.21203/rs.3.rs-2498485/v2. Accessed August 2023. This publication reports the initial discovery of Anopheles stephensi collected from Kenya.
Huestis DL, Dao A, Diallo M, Sanogo ZL, Samake D, Yaro AS, Ousman Y, Linton Y-M, Krishna A, Veru L, Krajacich BJ. Windborne long-distance migration of malaria mosquitoes in the Sahel. Nature. 2019;574(7778):404–8.
Lehmann T, Bamou R, Chapman JW, Reynolds DR, Armbruster PA, Dao A, Yaro AS, Burkot TR, Linton Y-M. Urban malaria may be spreading via the wind—here’s why that’s important. Proc Natl Acad Sci. 2023;120(18):e2301666120
Ahn J, Sinka M, Irish S, Zohdy S. Modeling marine cargo traffic to identify countries in Africa with greatest risk of invasion by Anopheles stephensi. Sci Rep. 2023;13(1):876.
Blanford JI, Blanford S, Crane RG, Mann ME, Paaijmans KP, Schreiber KV, Thomas MB. Implications of temperature variation for malaria parasite development across Africa. Sci Rep. 2013;3(1):1300.
• World Health Organization. Partners convening: a regional response to the invasion of Anopheles stephensi in Africa: Meeting Report, 8–10 March 2023. https://apps.who.int/iris/handle/10665/369368. This publication reports the initial discovery of Anopheles stephensi collected from Eritrea Ghana; this is not a peer-reviewed study.
de Santi VP, Khaireh BA, Chiniard T, Pradines B, Taudon N, Larréché S, Mohamed AB, de Laval F, Berger F, Gala F, Mokrane M. Role of Anopheles stephensi mosquitoes in malaria outbreak, Djibouti, 2019. Emerg Infect Dis. 2021;27(6):1697.
Hamlet A, Dengela D, Tongren JE, Tadesse FG, Bousema T, Sinka M, Seyoum A, Irish SR, Armistead JS, Churcher T. The potential impact of Anopheles stephensi establishment on the transmission of Plasmodium falciparum in Ethiopia and prospective control measures. BMC Med. 2022;20(1):135.
Howes RE, Battle KE, Mendis KN, Smith DL, Cibulskis RE, Baird JK, Hay SI. Global epidemiology of Plasmodium vivax. Am J Trop Med Hyg. 2016;95(6 Suppl):15.
Mutsaers M, Engdahl CS, Wilkman L, Ahlm C, Evander M, Lwande OW. Vector competence of Anopheles stephensi for O’nyong-nyong virus: a risk for global virus spread. Parasit Vectors. 2023;16(1):1–8.
Angel S, Parent J, Civco DL, Blei A, Potere D. The dimensions of global urban expansion: Estimates and projections for all countries, 2000–2050. Prog Plan. 2011;75(2):53–107.
• Sinka ME, Pironon S, Massey NC, Longbottom J, Hemingway J, Moyes CL, Willis KJ. A new malaria vector in Africa: predicting the expansion range of Anopheles stephensi and identifying the urban populations at risk. Proc Natl Acad Sci. 2020;117(40):24900–8. This publication presents the most recent predicted habitat suitability for Anopheles stephensi in Africa.
Soper FL, Wilson DB. Anopheles gambiae in Brazil, 1930 to 1940. Rockefeller Foundation; 1943.
Henderson JV, Storeygard A, Deichmann U. Has climate change driven urbanization in Africa? J Dev Econ. 2017;1(124):60–82. https://doi.org/10.1016/j.jdeveco.2016.09.001
Henderson JV, Storeygard A, Deichmann U. Has climate change driven urbanization in Africa? J Dev Econ. 2017;1(124):60–82.
Marchiori L, Maystadt JF, Schumacher I. The impact of weather anomalies on migration in subSaharan Africa. J Environ Econ Manag. 2012;63(3):355–74. https://doi.org/10.1016/j.jeem.2012.02.001
Marchiori L, Maystadt JF, Schumacher I. The impact of weather anomalies on migration in sub-Saharan Africa. J Environ Econ Manag. 2012;63(3):355–74.
• Mafwele BJ, Lee JW. Relationships between transmission of malaria in Africa and climate factors. Sci Rep. 2022;12(1):14392. This publication details how temperature will impact malaria transmission and climate change in Africa.
Weiss DJ, Bhatt S, Mappin B, Van Boeckel TP, Smith DL, Hay SI, Gething PW. Air temperature suitability for Plasmodium falciparum malaria transmission in Africa 2000–2012: a high-resolution spatiotemporal prediction. Malar J. 2014;13(1):1–11.
Diouf I, Adeola AM, Abiodun GJ, Lennard C, Shirinde JM, Yaka P, Ndione JA, Gbobaniyi EO. Impact of future climate change on malaria in West Africa. Theoret Appl Climatol. 2022;1:1–3.
Garamszegi LZ. Climate change increases the risk of malaria in birds. Glob Change Biol. 2011;17(5):1751–9.
Caminade C, McIntyre KM, Jones AE. Impact of recent and future climate change on vector-borne diseases. Ann N Y Acad Sci. 2019;1436(1):157–73.
Miazgowicz KL, Mordecai EA, Ryan SJ, Hall RJ, Owen J, Adanlawo T, Balaji K, Murdock CC. Mosquito species and age influence thermal performance of traits relevant to malaria transmission. biorxiv. 2019;14:769604.
Villena OC, Ryan SJ, Murdock CC, Johnson LR. Temperature impacts the environmental suitability for malaria transmission by Anopheles gambiae and Anopheles stephensi. Ecology. 2022;103(8):e3685.
• Carter TE, Yared S, Getachew D, Spear J, Choi SH, Samake JN, Mumba P, Dengela D, Yohannes G, Chibsa S, Murphy M. Genetic diversity of Anopheles stephensi in Ethiopia provides insight into patterns of spread. Parasit Vectors. 2021;14(1):602. This publication reports the initial discovery of Anopheles stephensi collected from Ethiopia.
Rao BA, Sweet WC, Subba Rao AM. Ova measurements of A. stephensi type and A. stephensi var. mysorensis. J Malaria Inst India. 1938;1:261–6.
Subbarao SK, Vasantha K, Adak T, Sharma VP, Curtis CF. Egg-float ridge number in Anopheles stephensi: ecological variation and genetic analysis. Med Vet Entomol. 1987;1(3):265–71.
Vatandoost H, Oshaghi MA, Abaie MR, Shahi M, Yaaghoobi F, Baghaii M, Hanafi-Bojd AA, Zamani G, Townson H. Bionomics of Anopheles stephensi Liston in the malarious area of Hormozgan province, southern Iran, 2002. Acta Trop. 2006;97(2):196–203.
Chakraborty S, Ray S, Tandon N. Seasonal prevalence of Anopheles stephensi larvae and existence of two forms of the species in an urban garden in Calcutta City. Indian J Malariol. 1998;35(1):8–14.
Manouchehri AV, Javadian E, Eshighy N, Motabar M. Ecology of Anopheles stephensi Liston in southern Iran. Trop Geogr Med. 1976;28(3):228–32.
Thomas S, Ravishankaran S, Justin NA, Asokan A, Mathai MT, Valecha N, Montgomery J, Thomas MB, Eapen A. Resting and feeding preferences of Anopheles stephensi in an urban setting, perennial for malaria. Malar J. 2017;16(1):1–7.
Sinka ME, Bangs MJ, Manguin S, Chareonviriyaphap T, Patil AP, Temperley WH, Gething PW, Elyazar IR, Kabaria CW, Harbach RE, Hay SI. The dominant Anopheles vectors of human malaria in the Asia-Pacific region: occurrence data, distribution maps and bionomic précis. Parasit Vectors. 2011;4(1):1–46.
Balkew M, Mumba P, Yohannes G, Abiy E, Getachew D, Yared S, Worku A, Gebresilassie A, Tadesse FG, Gadisa E, Esayas E. An update on the distribution, bionomics, and insecticide susceptibility of Anopheles stephensi in Ethiopia, 2018–2020. Malar J. 2021;20(1):1–3.
Foley DH, Wilkerson RC, Birney I, Harrison S, Christensen J, Rueda LM. MosquitoMap and the Mal-area calculator: new web tools to relate mosquito species distribution with vector borne disease. Int J Health Geogr. 2010;9(1):1–8.
Foley DH, Maloney FA Jr, Harrison FJ, Wilkerson RC, Rueda LM. Online spatial database of US Army public health command region-west mosquito surveillance records: 1947–2009. US Army Med Dep J. 2011;1:29–36.
Foley DH, Wilkerson RC, Rueda LM. Importance of the “what”,“when”, and “where” of mosquito collection events. J Med Entomol. 2009;46(4):717–22.
Molyneux DH. Common themes in changing vector-borne disease scenarios. Trans R Soc Trop Med Hyg. 2003;97(2):129–32.
Crombie MK, Gillies RR, Arvidson RE, Brookmeyer P, Weil GJ, Sultan M, Harb M. An application of remotely derived climatological fields for risk assessment of vector-borne diseases: a spatial study of filariasis prevalence in the Nile Delta, Egypt. Photogramm Eng Remote Sens. 1999;65(ANL/ER/JA-37529). https://www.osti.gov/biblio/943107
El-Zeiny A, El-Hefni A, Sowilem M. Geospatial techniques for environmental modeling of mosquito breeding habitats at Suez Canal Zone, Egypt. Egypt J Remote Sens Space Sci. 2017;20(2):283–93.
Attaway DF, Jacobsen KH, Falconer A, Manca G, Waters NM. Risk analysis for dengue suitability in Africa using the ArcGIS predictive analysis tools (PA tools). Acta Trop. 2016;1(158):248–57.
Campbell LP, Luther C, Moo-Llanes D, Ramsey JM, Danis-Lozano R, Peterson AT. Climate change influences on global distributions of dengue and chikungunya virus vectors. Phil Trans R Soc B: Biol Sci. 2015;370(1665):20140135.
Li C, Managi S. Global malaria infection risk from climate change. Environ Res. 2022;1(214):114028.
Laporta GZ, Potter AM, Oliveira JF, Bourke BP, Pecor DB, Linton YM. Global distribution of Aedes aegypti and Aedes albopictus in a climate change scenario of regional rivalry. Insects. 2023;14(1):49.
Ototo EN, Ogutu JO, Githeko A, Said MY, Kamau L, Namanya D, Simiyu S, Mutimba S. Forecasting the potential effects of climate change on malaria in the Lake Victoria Basin using regionalized climate projections. Acta Parasitol. 2022;67(4):1535–63.
Gunathilaka N, Fernando T, Hapugoda M, Abeyewickreme W, Wickremasinghe R. Revised morphological identification key to the larval anopheline (Diptera: Culicidae) of Sri Lanka. Asian Pac J Trop Biomed. 2014;1(4):S222–7.
Coetzee M. Key to the females of Afrotropical Anopheles mosquitoes (Diptera: Culicidae). Malar J. 2020;19(1):1–20.
Walter Reed Biosystematics Unit Identification Keys: Afrotropical Region: Adult-Anopheles: http://wrbu.si.edu/keys/AF_AN_A/Anopheles_Afro_AFRICOM_A.html. Accessed August 2023.
Walter Reed Biosystematics Unit Identification Keys: Afrotropical Region: Larva-Anopheles: https://wrbu.si.edu/keys/AF_AN_L/Anopheles_Afro_AFRICOM_L.html. Accessed August 2023.
Mnzava AP, Knox TB, Temu EA, Trett A, Fornadel C, Hemingway J, Renshaw M. Implementation of the global plan for insecticide resistance management in malaria vectors: progress, challenges and the way forward. Malar J. 2015;14:1–9.
Coetzee M, Koekemoer LL. Molecular systematics and insecticide resistance in the major African malaria vector Anopheles funestus. Annu Rev Entomol. 2013;7(58):393–412.
Gupta SK, Singh H, Joshi MC, Sharma A. Digital dashboards with paradata can improve data quality where disease surveillance relies on real-time data collection. Digital Health. 2023;9:20552076231164096.
Parmakelis A, Russello MA, Caccone A, Marcondes CB, Costa J, Forattini OP, Sallum MAM, Wilkerson RC, Powell JR. Historical analysis of a near disaster: Anopheles gambiae in Brazil. Am J Trop Med Hyg. 2008;78(1):176.
Causey OR, Deane LM, Deane MP. Ecology of Anopheles gambiae in Brazil. Am J Trop Med. 1943;1(23):73.
Faerstein E, Winkelstein W Jr. William Gorgas: Yellow fever meets its nemesis. Epidemiology. 2011;22(6):872.
Seyfarth M, Khaireh BA, Abdi AA, Bouh SM, Faulde MK. Five years following first detection of Anopheles stephensi (Diptera: Culicidae) in Djibouti, Horn of Africa: populations established —malaria emerging. Parasitol Res. 2019;118(3):725–32.
World Health Organization. Vector alert: anopheles stephensi invasion and spread in Africa and Sri Lanka. World Health Organization. 2022. https://apps.who.int/iris/handle/10665/365710
Samarasekera U. A missed opportunity? Anopheles stephensi in Africa. Lancet. 2022;400(10367):1914–5.
Russell TL, Farlow R, Min M, Espino E, Mnzava A, Burkot TR. Capacity of National Malaria Control Programmes to implement vector surveillance: a global analysis. Malar J. 2020;19(1):1–9.
Killeen GF, Fillinger U, Knols BG. Advantages of larval control for African malaria vectors: low mobility and behavioural responsiveness of immature mosquito stages allow high effective coverage. Malar J. 2002;1:1–7.
Lopes G, Cueto M. ‘Eradication was a dirty word’: Anti-gambiae campaign, between cooperation and rivalry (1938–1940). Glob Public Health. 2023;18(1):2200559.
Mnzava A, Monroe AC, Okumu F. Anopheles stephensi in Africa requires a more integrated response. Malar J. 2022;21(1):1–6.
Funding
This work was financially supported by the Armed Forces Health Surveillance Division-Global Emerging Infections Surveillance Branch (AFHSD-GEIS) under the award P0050_23_WR. The activities undertaken at the Walter Reed Biosystematics Unit (WRBU) were performed under a Memorandum of Understanding between the Walter Reed Army Institute of Research (WRAIR) and the Smithsonian Institution, with institutional support provided by both organizations.
Author information
Authors and Affiliations
Contributions
D.B.P. and Y.M.L. wrote the main manuscript text and prepared figures 2 and 3. A.M.P. prepared tables 1-2 and figures 1 and 4. All authors reviewed the manuscript.
Corresponding author
Ethics declarations
Disclaimer
Material has been reviewed by the Walter Reed Army Institute of Research. There is no objection to its presentation and/or publication. The opinions or assertions contained herein are the private views of the author, and are not to be construed as official, or as reflecting true views of the Department of the Army or the Department of Defense.
Competing of Interest
The authors declare no competing interests.
Human and Animal Rights and Informed Consent
This article does not contain any studies with human or animal subjects performed by any of the authors.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
The original online version of this article was revised: Any reference to the distribution of Anopheles stephensi in Zanzibar is erroneous.
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if changes were made. The images or other third party material in this article are included in the article's Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article's Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
Pecor, D.B., Potter, A.M. & Linton, YM. Implications of Climate Change and Anopheles stephensi Liston in Africa: Knowledge Gaps and Lessons from History. Curr Trop Med Rep 10, 320–330 (2023). https://doi.org/10.1007/s40475-023-00296-7
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s40475-023-00296-7