Abstract
Young people who self-harm require support and resources to address their self-harm. However, they are often reluctant to seek help for their self-harm. Despite efforts to increase help-seeking, the rates of self-harm in this population continue to increase. A better understanding of the factors that influence help-seeking for self-harm in young people is necessary. This systematic review aimed to synthesize the existing literature on the known facilitators and barriers to help-seeking for self-harm in young people. Across the 33 studies included in this review, the age range of young people was 11 to 30 years. Facilitators and barriers to help-seeking for self-harm were extracted and mapped onto a systems thinking framework. The synthesis indicated that there were 17 known facilitators and twice as many barriers across the help-seeking system hierarchy. Most of these facilitators and barriers were related to lower levels of the system (i.e., service delivery and the social environment, and young people who self-harm). There was limited consideration of broader systemic factors that influence help-seeking for self-harm and the interactions between these facilitators and barriers in influencing help-seeking. Future research should consider the use of systems thinking frameworks and methods in understanding and addressing this complex problem.
Similar content being viewed by others
Explore related subjects
Discover the latest articles, news and stories from top researchers in related subjects.Avoid common mistakes on your manuscript.
Introduction
A global health concern is self-harm, a behavior that is highly prevalent in young people. Compared to young people who do not self-harm, those who self-harm are more likely to experience adverse outcomes, including non-fatal outcomes such as financial hardship and poor mental health, and fatal outcomes such as suicide (Borschmann et al., 2017; Daukantaitė et al., 2021; Hawton et al., 2015). Despite the high prevalence of self-harm in young people and the serious consequences of self-harm, only a small proportion of young people seek help for their self-harm (e.g., Morey et al., 2008; Ystgaard et al., 2009), emphasizing a need to better understand the factors that influence help-seeking for self-harm in this population. The current study addresses this need, by taking a systems thinking perspective in the synthesis of the existing literature on the facilitators and barriers to help-seeking for self-harm in young people.
It has been estimated that each year, more than 700,000 people worldwide die by suicide (World Health Organization, 2021). For every death by suicide, many more people engage in self-harm, with or without suicidal intent. There is evidence indicating complex differences between people who self-harm with suicidal intent and those who self-harm without suicidal intent. For example, Mars et al. (2014) reported that people who self-harm with suicidal intent tend to experience higher levels of depressive and anxiety symptoms compared to those who self-harm without suicidal intent. Cleare et al. (2021), more recently, reported that people who self-harm with suicidal intent experience greater suicidal ideation, feelings of defeat and internal entrapment, and perceived burdensomeness, compared to those who self-harm without suicidal intent. The added complexity is that suicidal intent is temporally dynamic, such that suicidal intent fluctuates from time to time (Bryan, 2020). Despite these complexities, the overarching issue of self-harm warrants attention because self-harm remains an important risk factor for suicide (Carroll et al., 2014). There is evidence indicating that one in 25 people who present to the hospital for self-harm, irrespective of suicidal intent, die by suicide within five years of their presentation to the hospital (Carroll et al., 2014). Thus, the current study adopts a broad definition of self-harm; that is, any non-fatal act of injuring oneself deliberately, irrespective of the degree of suicidal intent (Knipe et al., 2022). Self-harm is viewed as a coping mechanism for managing emotional distress (Royal College of Psychiatrists, 2010).
Self-harm is prevalent in many populations, including people experiencing homelessness (e.g., Barrett et al., 2018), people from low- and middle-income countries (e.g., Knipe et al., 2019), and older people (e.g., Morgan et al., 2018). Self-harm is also highly prevalent in adolescents or young people (e.g., Gillies et al., 2018). In self-harm and suicide research, the period of adolescence is often defined by the chronological age of the young person (as opposed to their physical or cognitive development status) but there is little consensus on the chronological age definition (Hawton et al., 2012; see also Sawyer et al., 2018). The age range used to define adolescents or young people in self-harm and suicide research is broad, with a lower age limit of 10 years (e.g., Beckman et al., 2018) to an upper limit of 30 years (e.g., Cleary et al., 2017). Thus, the current study adopts a broad definition of adolescence, considering studies that described their sample as young people (e.g., youth, adolescents, teens, teenagers). Self-harm in young people has elicited increased attention worldwide because the prevalence of self-harm is higher in young people than in the general community (e.g., Australian Institute of Health & Welfare, 2024; McManus et al., 2019) and self-harm tends to first occur and peak in adolescence (e.g., Nock et al., 2013). It has been estimated that 20% of young people engage in self-harm and the average age of the first self-harm incident is 13 years (Gillies et al., 2018; Lucena et al., 2022; Nock et al., 2013). The prevalence of self-harm has continued to increase over the last few decades (Griffin et al., 2018; McManus et al., 2019; Sara et al., 2022). The study by Griffin et al. (2018) indicated a 22% increase in hospital emergency department presentations for self-harm between the 10-year period of 2007 and 2016, with more pronounced increases in females and young people aged 10 to 14 years. The study by Sara et al. (2022) also indicated an increase in the prevalence of self-harm in young people since COVID-19, with more pronounced increases in young people from socio-economically advantaged and urban areas. Importantly, self-harm in adolescence increases the likelihood of adverse experiences later in life (Borschmann et al., 2017; Daukantaitė et al., 2021; Hawton et al., 2015). For example, the population-based cohort study by Borschmann et al. (2017) indicated that people who self-harm in their adolescence (at 15 years of age) were more likely to encounter social disadvantages (e.g., financial hardship) and poorer mental health (e.g., substance dependence) that persisted into adulthood (at 35 years) when compared to people who did not self-harm in their adolescence. Self-harm in adolescence also increases the risk of fatal outcomes such as suicide (Hawton et al., 2015).
The lasting impacts of self-harm in adolescence on personal and social functioning and quality of life underscores the need to address self-harm in this population. Young people who self-harm would benefit from support and resources to not only manage and/or reduce their self-harm but also identify and confront the causes of this behavior (e.g., underlying emotional distress). A necessary step in accessing the support and resources required is that the young person seek help for their self-harm and this involves the disclosure of their self-harm. However, young people who self-harm are often reluctant to disclose their self-harm, keeping it a secret (Chandler, 2018). Help-seeking is described as “any action or activity carried by a [young person] who perceives [themselves] as needing personal, psychological, affective assistance of health or social services with the purposes of meeting this need in a positive way” (Barker, 2007). Help can be sought from formal, professional sources (e.g., psychologists, counselors) or informal sources (e.g., family, friends). There is evidence indicating that young people prefer seeking help from informal sources over formal sources (Rickwood & Braithwaite, 1994; Rickwood et al., 2007). It has been estimated that around 30% of young people sought help from informal sources following their self-harm (Ystgaard et al., 2009) while less than 20% of young people sought help from formal sources (Morey et al., 2008; Ystgaard et al., 2009). Irrespective of the type of help-seeking sources, the low rates of help-seeking for self-harm in young people are a concern as it suggests that young people who self-harm are not receiving the support and resources they need. These unmet needs will likely contribute to the rising prevalence of self-harm in this population.
Several reviews have been conducted to synthesize the factors that influence help-seeking, with a few of these reviews focused only on the facilitators and barriers to help-seeking for self-harm in young people (Michelmore & Hindley, 2012; Rowe et al., 2014) and other reviews on help-seeking for mental health problems in young people more generally (Aguirre Velasco et al., 2020; Barrow & Thomas, 2022; Gulliver et al., 2010; Radez et al., 2021). Across these reviews, there were facilitators and barriers common to both help-seeking for self-harm and mental health problems more generally. These common facilitators include assurance of confidentiality, being treated with respect and with no judgment, and previous positive experiences while common barriers include stigma, negative responses from others, and poor mental health literacy (Aguirre Velasco et al., 2020; Barrow & Thomas, 2022; Gulliver et al., 2010; Michelmore & Hindley, 2012; Radez et al., 2021; Rowe et al., 2014). However, across these reviews, it was apparent that some barriers relate to only help-seeking for self-harm and not mental health problems. Some notable barriers include the fear of being perceived as “attention-seeking”, or the fear that others would prevent them from future self-harm (i.e., fear around interventions) (Rowe et al., 2014). Thus, it would be necessary to refrain from assuming that the facilitators and barriers to help-seeking for mental health problems would also apply to help-seeking for self-harm. The latest review that focused only on help-seeking for self-harm in young people was published by Rowe et al. (2014), and this review synthesized the known facilitators and barriers across 11 studies, reporting that there are many barriers to help-seeking for self-harm in young people and comparatively, only a few facilitators. Given that nearly a decade has passed since the publication by Rowe et al. (2014), an updated review of the literature is needed. In addition to an updated review, it is proposed that a systems thinking perspective be taken to this review, to generate new insights and contribute to the knowledge base of help-seeking for self-harm in young people.
The discipline of systems thinking has had a long history in understanding and responding to complex problems (Leveson, 2004; Rasmussen, 1997). Proponents of systems thinking argue that, when attempting to understand and respond to complex problems, breaking the system (e.g., “help-seeking for self-harm” system) down into individual components and analyzing the components is limited (Leveson, 2004; Rasmussen, 1997). Instead, they argue that the system needs to be represented as a single unit of analysis, allowing the study of how its components interact to influence behavior (e.g., help-seeking for self-harm) (Leveson, 2004; Rasmussen, 1997). In complex systems, such as healthcare (Kannampallil et al., 2011; Raben et al., 2018), the interactions among components are non-linear and difficult to predict, leading to the potential for unintended consequences. For example, a decision to re-direct funding from face-to-face mental health services to online services, with the intent to increase help-seeking, can impact the accessibility and quality of face-to-face services. This, in turn, can have adverse impacts on young people who prefer and benefit from face-to-face services.
A well-established systems thinking framework is Rasmussen’s Risk Management Framework (Rasmussen, 1997), which was developed initially to understand accident causation but has since been applied more broadly to understand system performance. Rasmussen’s Risk Management Framework posits that systems comprise several hierarchical levels (e.g., government, regulators, local government, service delivery, individuals, and infrastructure) (Rasmussen, 1997). Stakeholders at each of these levels share the responsibility for the system’s performance and safety. This is because the decisions and actions of all system stakeholders, from those proximal in space and time to the behavior (e.g., a young person who self-harm, their friends and family), to those more distal in space and time (e.g., government, policymakers), contribute to the emergent behavior of the system. Rasmussen’s Risk Management Framework has been used to understand, holistically, the network of factors that influence behavior by representing where the factors reside across the system hierarchy (Rasmussen, 1997; Svedung & Rasmussen, 2002). The use of this systems thinking framework can support the identification of leverage points in the system, where interventions can result in effective behavioral change across the system (Meadows, 1999).
A handful of studies have applied systems thinking frameworks and methods to public health domains (e.g., Austin et al., 2002; Koorts et al., 2022), including in mental health (e.g., Lane et al., 2020; Occhipinti et al., 2021; Vacher et al., 2023). Of most relevance across these studies, is the study conducted by Lane et al. (2020). Lane et al. applied Rasmussen’s Risk Management Framework to understand barriers to treatment access for people with eating disorders. In their study, they extracted the known barriers to treatment access for people with eating disorders from the existing literature and mapped these barriers across the “eating disorder treatment” system hierarchy. In doing so, Lane et al. reported that many of the known barriers related to lower levels of the system hierarchy—individuals and social processes (e.g., belief in eating disorder seriousness, stigma and shame, attitudes towards professional help). Comparatively, there were fewer known barriers related to higher levels of the system hierarchy (e.g., government policy and budgeting, service delivery). Their study informed the current understanding of treatment access for people with eating disorders, by highlighting the gaps in knowledge and the importance of studying system-level barriers to improve treatment access. In addition to the insights generated from the use of Rasmussen’s Risk Management Framework in the study by Lane et al., important insights have also been generated from the use of other systems thinking frameworks and methods. For example, the study by Occhipinti et al. (2021), which applied system dynamics modeling to develop a simulation model of mental health system behavior. Using system dynamics modeling, they simulated the effects of different programs and initiatives in the mental health care system on suicidal behavior in a few regional Australian populations. Their study informed the optimal mix of programs and initiatives that can be implemented within the mental health system to reduce deaths by suicide (by up to 16% over 10 years) across the region. The point here is that systems thinking frameworks and methods (e.g., Rasmussen’s Risk Management Framework, system dynamics modeling) can generate new, important insights that can enhance the current knowledge base and inform policy decision-making. These insights would not have been observed if reductionistic approaches were used to address complex problems.
Current Study
Self-harm is highly prevalent in young people, representing a major health concern in this population. Young people who self-harm would benefit from support and resources to address their self-harm., but only a small proportion of young people seek help for their self-harm. Reviews have been conducted previously to understand the factors that influence help-seeking for self-harm in this population, with the last review published in 2014. An updated systematic review of the factors that influence help-seeking for self-harm in young people is, therefore, timely. In particular, a systematic review that adopts a new perspective on this topic, to generate new insights and further contribute to the knowledge base. The current study was designed to address this gap. More specifically, the current study aimed to synthesize the existing literature on the facilitators and barriers to help-seeking for self-harm in young people, and analyze and map these facilitators and barriers across the help-seeking system hierarchy using a systems thinking framework.
Method
Protocol
This systematic review was prospectively registered in the International Prospective Register of Systematic Reviews (PROSPERO; registration number CRD42023384541) (Booth et al., 2011). This review was conducted in line with the Preferred Reporting Items for Systematic Review and Meta-analyses (PRISMA) guidelines (Page et al., 2021). Ethics approval was not required for this systematic review as no human recruitment or participant was involved.
Electronic Search
The literature search for the systematic review was carried out between the period of 9 December 2022 and 5 January 2023 (inclusive), on four databases: PubMed, Medline, PsycINFO, and Scopus. Covidence (Veritas Health Innovation, n.d.), a web-based collaborative software platform, was used to facilitate the literature searching and screening process.
The aim and scope of the systematic review determined the Boolean search terms relating to “self-harm”, “youth”, and “help-seeking”. All of the terms were searched by title, abstract, and keywords, to ensure that the initial search results contained only relevant records and that they were manageable in further rounds of screening. The final search strategy was consistent across all four databases and was as follows: ((“self harm” OR “self-harm”) OR (suicide*) OR (suicide* AND (attempt OR ideation OR behavio*)) OR (“self injur*” OR “self-injur*) OR (“non-suicidal” OR “nonsuicidal” AND ((“self harm” OR “self-harm”) OR (“self injur*” OR “self-injur*”))) OR “deliberate” AND ((“self harm” OR “self-harm”) OR (“self injur*” OR “self-injur*”)))) AND (young OR youth OR adolescen* OR teen OR children) AND (((seek* OR sought) AND (help OR service OR support OR treat*)) OR disclos*).
Although this systematic review provides an updated review to the one published by Rowe et al. (2014), no restrictions on publication dates were applied to the search. A reason for this is that this systematic review represents the first in the field of self-harm research to apply a systems thinking perspective in the analysis of factors that influence help-seeking for self-harm, and as such, restrictions on publication dates will result in an incomplete understanding of these factors across the help-seeking system hierarchy.
Eligibility Criteria
A set of inclusion and exclusion criteria was applied during the screening process to identify records relevant to this review.
Inclusion Criteria
Records were included in the review if they met all of the following criteria:
-
(i)
The primary study sample involved young people with a history of self-harm. The definition of self-harm has been a point of controversy among researchers regarding the inclusion of suicidal intent in its definition (Butler & Malone, 2013; Zareian & Klonsky, 2019). Given the review is focused on help-seeking and not on the aetiology of self-harm, a broad definition of self-harm was adopted in this review, and studies where self-harm was described as an act of self-injury, irrespective of suicidal intent, were included. The adoption of this broad definition also ensures that relevant records were not excluded.
-
(ii)
The definition of “young people” was not restricted by age. Given there is little consensus on the age definition for adolescence (Sawyer, 2018), studies in which the sample was described to consist of young people (e.g., youth, adolescents, teens, teenagers) were included.
-
(iii)
The outcome of interest in the study was help-seeking for self-harm, from either formal or informal sources.
-
(iv)
The record was published in English language and the full-text version of the record was available.
Exclusion Criteria
Records were excluded from the review if they did not meet the inclusion criteria or any of the following criteria:
-
(i)
The outcome of interest in the study was help-seeking for mental health problems more generally.
-
(ii)
The study was not peer-reviewed (e.g., pre-prints, conference articles, student theses).
-
(iii)
The record was a review article (e.g., narrative review, systematic review), a commentary, or a personal retrospective article.
The second author conducted the initial search, removed record duplicates, and reviewed the retrieved records against the eligibility criteria, first by title and abstract, and then by the full-text version. Discussions were held between the first and second authors if there were insufficient details reported in the title, abstract, or full-text version of the record. A consensus decision was then made to include or exclude the record from this review. The screening process resulted in the final set of records, of which all were articles, in the systematic review.
Quality Assessment
The quality of the articles included in the systematic review was assessed using the Mixed Methods Appraisal Tool (Hong et al., 2018). The Mixed Methods Appraisal Tool allowed for the quality assessment of studies with diverse designs (e.g., qualitative, quantitative descriptive, and mixed-methods studies) (Pace et al., 2012; Pluye et al., 2009). The Mixed Methods Appraisal Tool checklist includes two screening questions relating to the research question of the study and the data collected to address the research question, and five questions relating to the methodological quality of the study. Each question required a response of “Yes” (scored as “1”), “No” or “Can’t tell” (both scored as “0”). For articles with qualitative and quantitative study designs, the score on each of the five questions relating to the methodological quality was summed and the total score reflected the quality of the study. For articles with a mixed-methods study design, the score on each of the questions relating to methodological quality (total of 15 questions) was summed, divided by 15, and then multiplied by five. A total score of zero indicates the lowest quality and five indicates the highest quality. The two screening questions were not scored.
The second author conducted the quality assessment of the studies in the included articles and the first author conducted an independent quality assessment for 25% of these articles (randomly allocated) as an inter-rater reliability check for this assessment. The inter-rater reliability score (Cohen’s Kappa) was 0.90, indicating almost perfect agreement (Landis & Koch, 1977). Discussions were held between the first and second authors to resolve the disagreements.
Data Extraction and Presentation
Relevant information was extracted from each article. Publication information extracted included the author names and publication year. Study characteristics extracted included the geographical context of the study, sample size, participant demographics (age, gender or sex), study design, and definition of self-harm used in the study.
Factors that influence help-seeking for self-harm were also extracted, where they were reported by the author(s) of the included articles to have influenced help-seeking for self-harm. The factors were coded and reported in this systematic review as facilitators of help-seeking, barriers to help-seeking, and other factors associated with help-seeking. For this review, facilitators were defined as factors that promote or enable help-seeking for self-harm (e.g., assurance with trust, privacy, and confidentiality). Barriers were defined as factors that prevent or obstruct help-seeking for self-harm (e.g., fear of worrying others or being burdensome). Other factors were defined as factors that describe the demographics of young people (e.g., gender identity) or characteristics of their help-seeking (e.g., before or after their self-harm) and were reported to differ in their likelihood of help-seeking for self-harm.
The facilitators and barriers to help-seeking for self-harm were mapped onto a “help-seeking system” hierarchy (underpinned by Rasmussen’s Risk Management Framework; Rasmussen, 1997), of which there were six levels.
-
1.
Government: Federal and state government agencies and policymakers.
-
2.
Regulatory bodies and associations: Organizations that facilitate the regulation of the domain (e.g., Australian Health Practitioner Regulation Agency), lobby groups, and mental health advocacy bodies.
-
3.
Local area government and organization management: Service management and local organizations (e.g., schools, hospitals, institutions).
-
4.
Service delivery and social environment: Health professionals and the social support networks (e.g., friends, family, carers) of young people who self-harm.
-
5.
Individuals and processes: Young people who self-harm.
-
6.
Equipment, infrastructure, and surroundings: The equipment, infrastructure, and surroundings of the local environment with which young people interact when seeking help.
For example, if a study identified that having a previous positive experience encouraged young people to seek help for self-harm, the facilitator “Previous positive experience” was placed at the Individuals and processes level of the system hierarchy, as this facilitator relates to young people’s perceptions of their last help-seeking attempt. If a study identified that the lack of support or advocacy prevented them from seeking help for self-harm, the barrier “Lack of support/advocacy” was placed at the Service delivery and social environment level of the system hierarchy, as this barrier relates to the inaction by others around young people. In addition to the extraction of factors that influence help-seeking for self-harm, relationships between the factors (causal or correlational) were extracted, where they were reported by the author(s) of the included articles. For example, if a study identified that long wait times for a mental health support service led to young people feeling ignored or abandoned, and these feelings prevented future help-seeking for self-harm, the relationship between “Long wait times” and “Feeling ignored or abandoned” was documented.
The first and second authors extracted the data from the articles included in this systematic review and the fourth author conducted an independent data extraction for 25% of these articles (randomly allocated) as an inter-rater reliability check for this data extraction. The inter-rater reliability score (Cohen’s Kappa) was 0.75, indicating substantial agreement (Landis & Koch, 1977). Discussions were held between the first, second, and fourth authors to resolve the disagreements.
Results
Full-Text Selection
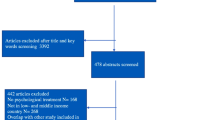
The search across the four databases (PubMed, Medline, PsycINFO, Scopus) retrieved a total of 4953 records. Of these records, 2803 duplicate records were identified and removed from the systematic review. Following the removal of these duplicate records, the title and abstract of the remaining 2132 records were screened based on the eligibility criteria. This resulted in a total of 1918 records excluded. The full-text version of the remaining 214 records was assessed for their eligibility and this resulted in a further 181 records being excluded. The screening process resulted in the inclusion of 33 records, all of which were articles, in this systematic review (Fig. 1).
Quality Assessment
The articles included in the systematic review were assessed for their study methodological quality using the Mixed Methods Appraisal Tool (Hong et al., 2018). The quality scores for articles that adopted a qualitative study design (n = 13) ranged from four to five, quantitative study design (n = 13) ranged from two to four, and mixed-methods study design (n = 7) ranged from two to four. The quality score for each of the articles included in the systematic review is presented in Fig. 2 (refer to Supplementary Material for raw scores of each item in the Mixed Methods Appraisal Tool checklist).
Quality assessment of the articles included in the systematic review. Note. Quality assessment was conducted using the Mixed Methods Appraisal Tool (Hong et al., 2018). The three panels in this figure reflect the study design (i.e., qualitative, quantitative, mixed-methods) adopted in the respective articles. The Y-axis indicates the article citation and the X-axis indicates the quality score (Color figure online)
Publication Information
The articles included in this systematic review were published between the years 2003 and 2023, with 2017 and 2021 having the highest number of publications (n = 4 in each year).
Study Characteristics
Study characteristics regarding the geographical context of the study, sample size, and participant demographics (age, gender or sex) from each of the articles included in this systematic review can be found in Table 1.
The largest proportion of studies were conducted in the United Kingdom (UK; n = 11, 35.48%). This was followed by Australia (n = 6, 18.18%) and the United States of America (USA; n = 5, 15.15%). The sample sizes reported across the studies varied extensively, from seven participants (McAndrew & Warne, 2014) to 11406 participants (Fadum et al., 2013). The age distribution of participants across the studies was not consistently reported, with some studies reporting detailed information (mean, standard deviation, range) and others reporting minimal information (range only). The youngest age for young people (lower limit) across the studies was 11 years (Lustig et al., 2021; Mojtabai & Olfson, 2008) and the oldest age (upper limit) was 30 years (Cleary, 2017). The gender or sex distribution of participants across the studies was also not consistently reported. Some studies reported gender distribution while others reported sex distribution. Further, some studies reported detailed information on the gender or sex distribution while others reported minimal information (e.g., the number or proportion of participants for only one gender or sex, even if their study included participants of other genders or sex).
Study characteristics regarding the study design and the self-harm definition adopted in the study from each of the articles included in this review can also be found in Table 1. There was an equal number of articles that adopted a qualitative (n = 13, 39.39%) or quantitative study design (n = 13, 39.39%), and the remaining articles adopted a mixed-methods study design (n = 7, 21.21%). The definition of self-harm differed across the articles included in this review. In many articles, self-harm was defined as a deliberate act of injuring oneself, but definitions differed in whether there was suicidal intent behind this behavior. A handful of articles included in this review focused on suicide attempts, which could be considered as self-harm with suicidal intent (i.e., where the intended outcome is fatal). Some of the articles focused on suicidality, defined “the risk of suicide, usually indicated by suicidal ideation or intent, especially as evident in the presence of a well-elaborated suicidal plan” (American Psychological Association, 2018), which can also include self-harm behaviors (Keefner & Stenvig, 2021).
Factors that Influence Help-Seeking for Self-Harm
The factors that influence help-seeking for self-harm extracted from the articles can be found in Table 2, and the descriptions for these factors can be found in Table 3.
The known facilitators of help-seeking for self-harm and where they reside across the help-seeking system hierarchy can be found in Fig. 3. A total of 17 distinct facilitators for self-harm in young people were extracted from the articles. Across the system, there was one facilitator relating to the regulatory bodies and associations, eight facilitators relating to the service delivery and environment, seven relating to the individual and processes, and one relating to equipment, infrastructure, and surroundings. There were no facilitators relating to the government, or local area government and organisation management. The facilitators that were most frequently reported across the studies included non-judgment or acceptance of self-harm by others (n = 7), communication by others (n = 5), online service delivery (n = 4), and assurance of trust, privacy, and confidentiality from others (n = 3).
The known barriers to help-seeking for self-harm and where they reside across the system can be found in Fig. 4. A total of 34 distinct barriers to help-seeking for self-harm in young people were extracted from the studies. Across the system, there were two barriers relating to regulatory bodies and associations, two relating to the local area government and organizational management, four relating to service delivery and environment, and 26 relating to the individual and processes. There were no barriers relating to the government, or equipment, infrastructure, and surroundings. The barriers that were most frequently reported across the studies included young people feeling ashamed or embarrassed of their self-harm (n = 12), their perception that they can manage their self-harm on their own (n = 11), their fear of worrying others or being a burden (n = 8), their fear of being judged or stigmatized (n = 8), and trust, privacy, and confidentiality concerns (n = 7).
The relationships between the factors reported in the articles were also extracted and are illustrated in Fig. 5. The relationships extracted were only identified once or twice across the studies, and most of these relationships were between a facilitator and an other factor, or between a barrier and an other factor. Gender identity was most frequently identified as having a relationship with a barrier. For example, gender identity was associated with young people being discriminated against or victimized (Burke et al., 2021), feeling ignored or abandoned (Fortune et al., 2008b), and their fear of worrying others or being burdensome (Fortune et al., 2008b). Only a handful of relationships were found between facilitators or barriers. One example was that long wait times for a support service were associated with young people feeling ignored or abandoned (Byrne et al., 2021).
Relationships between the known facilitators, barriers, and other factors, across the help-seeking system. Note. The green-colored boxes indicate the known facilitators, the red-colored boxes indicate the known barriers, and the white-colored boxes indicate other factors extracted from the studies. The number in parenthesis indicates the number of studies from which the factor was extracted. Relationships are indicated by the lines linking the factors, and the number of studies from which the relationships were extracted are indicated on the lines. The green-colored lines indicate relationships between known facilitators, the red-colored lines indicate relationships between known barriers, the yellow-colored lines indicate relationships between a known faciliator and an other factor, the purple-colored lines indicate relationships between a known barrier and an other factor, and the blue-colored lines indicate relationships between other factors (Color figure online)
Discussion
Self-harm in young people represents a major health concern, with these young people being at risk of adverse social and health outcomes later in their lives. Young people who self-harm are likely to benefit from support and resources to address their self-harm but they often do not seek help. There is a need to understand the factors that influence help-seeking for self-harm in young people, yet the most recent review on this topic was published in 2014 (Rowe et al., 2014). This current study was conducted to provide an updated review of the factors that influence help-seeking for self-harm in young people. More specifically, this systematic review (i) synthesized the existing literature on the known facilitators and barriers to help-seeking for self-harm in young people, and (ii) used a nuanced approach, a systems thinking framework (Rasmussen’s Risk Management Framework; Rasmussen, 1997) to analyze these factors across the help-seeking system hierarchy. This review is the first in the field to have taken a systems thinking perspective to understand the factors that influence help-seeking for self-harm in young people.
Facilitators and Barriers to Help-Seeking for Self-Harm
In recent years, researchers have proposed the use of systems thinking frameworks and methods to study mental health, with some having implemented these frameworks and methods to better understand areas of mental health (e.g., Lane et al., 2020) or to inform priority-setting (e.g., Occhipinti et al., 2021). The use of a systems thinking framework, Rasmussen’s Risk Management Framework (Rasmussen, 1997), in this systematic review, provided insights into the key focus areas in research on help-seeking for self-harm in young people and demonstrated knowledge gaps in the existing literature. Five key findings emerged from this systems thinking-based analysis.
The first finding was that the majority of the known facilitators and barriers to help-seeking for self-harm were related to lower levels of the system hierarchy. More specifically, these factors were related to the decisions and actions of the professionals who provide care (e.g., counselors, psychologists) and social support networks (e.g., friends, family) (Service delivery and social environment level) and those of the young people who self-harm (Individuals and processes level). Comparatively, there were fewer known facilitators and barriers related to higher levels of the system, which include the Local area government and organization management, Regulatory bodies and associations, and the Government levels. This disproportionate representation of factors in the system is a common observation across different domains of research, as evident in studies that have used systems thinking frameworks and methods. For example, studies have sought to identify what is known regarding barriers to treatment access for individuals with eating disorders (Lane et al., 2020), the factors that enable child sexual abuse in sport (Dodd et al., 2023), the factors that contribute to cycling incidents (Salmon et al., 2022), and the factors influencing risk at rail level crossings (Read et al., 2021), have all concluded that more is known regarding the lower level factors.
The disproportionate focus on the health professionals who provide care, social support networks, and young people identified in this systematic review is likely to reflect a knowledge gap, resulting from the paucity of research on how decisions and actions of those in the higher levels of the system hierarchy, especially the Government level, influence help-seeking for self-harm in young people. This knowledge gap suggests that research to date has overlooked key systems thinking tenets; namely, that outcomes (e.g., help-seeking or a lack of help-seeking) are created by the interactions between stakeholders at all system levels and are the responsibility of all system stakeholders (Rasmussen, 1997). This first finding, therefore, suggests that more expansive research is required to better understand help-seeking for self-harm, with a sound starting point being to investigate the impact of policy initiatives and changes to these initiatives on help-seeking for self-harm. An example policy initiative in Australia is the Better Access initiative that provides rebates to eligible individuals so they can access up to 10 individual and up to 10 group allied mental health services (Australian Government Department of Health & Aged Care, 2022). One of the eligibility requirements to use Better Access is that the individuals must have a mental health diagnosis. However, there is some evidence suggesting that this requirement is a barrier to help-seeking (Pirkis et al., 2022). Future research investigating how factors relating to the higher levels of the help-seeking for self-harm system influence help-seeking for self-harm in young people is recommended, as it is highly likely that these factors would have impacts on help-seeking for self-harm in young people.
The second finding was that there were 17 distinct facilitators of help-seeking for self-harm in young people. Among these known facilitators, many were related to the actions and decisions of professionals who provide care and the social support networks of young people who self-harm (Service delivery and social environment level). More specifically, these facilitators included non-judgment and acceptance of self-harm by others, communication by others, and assurance of trust, privacy, and confidentiality from others. Non-judgment or acceptance of self-harm by others was the most frequently reported facilitator across the studies. This finding is important because it suggests that a potential avenue to encourage help-seeking behaviour is through the interactions of young people who self-harm with professionals who provide care and their social networks. These professional and social support structures play a critical role in reflecting positive values and beliefs that can facilitate help-seeking behaviors (Lauriks et al., 2014; Schenk et al., 2018). Additionally, future research is needed to better understand the drivers of these facilitators; that is, factors that promote these facilitators of help-seeking for self-harm.
The third finding was that there were 34 distinct barriers to help-seeking for self-harm in young people. Among these known barriers, many were related to the young people who self-harm themselves (Individuals and processes level). More specifically, these barriers included disbelief in the seriousness of self-harm, previous negative experiences, their personal feelings (e.g., feeling ashamed or embarrassed about their self-harm) and personal fears (e.g., fear of being judged or stigmatized for their self-harm). The most frequently reported barriers included young people’s personal feelings of shame and embarrassment, their belief that they can self-manage their self-harm, and their fear of worrying others or being burdensome. Notably, many barriers related to young people’s personal feelings and personal fears about how others may respond to their self-harm. These feelings and fears may not be validated—others may not respond to their self-harm the way they had expected—but they remain significant barriers to help-seeking for self-harm in this population. These barriers are exceptionally difficult to address, as they can be deeply entrenched in a young person’s values and long-held beliefs, or how they think of and perceive their self-harm. However, one could argue that while these barriers are related to the young people who self-harm themselves, these are driven by societal beliefs and norms (e.g., the societal stigma associated with self-harm may result in a young person to self-stigmatize their own self-harm). This means that a possible leverage point to break down the barriers to help-seeking is through addressing societal attitudes and treatment towards one another.
The fourth finding, which was alluded to earlier in the discussion of our second and third findings, was that there were twice as many barriers to help-seeking for self-harm than there were facilitators. Our systems thinking-based analysis of the facilitators and barriers to help-seeking for self-harm indicated that more is known about the barriers to help-seeking for self-harm compared to facilitators. It may be the case that there are simply more barriers than there are facilitators, or that the research focus has been on barriers. The latter would suggest that the field does not have an in-depth understanding of the facilitators of help-seeking for self-harm. Future research could explore the use of methods such as appreciative inquiry (Bushe, 2011) to better understand the facilitators of help-seeking for self-harm and how these factors may be integrated into practice to enhance help-seeking. An additional benefit could be gained by integrating such methods with systems thinking frameworks and methods (e.g., Rasmussen’s Risk Management Framework), encouraging the consideration of all levels of the help-seeking for self-harm system hierarchy and how the decisions and actions of actors who reside in each level influence the young person’s help-seeking behaviors.
The fifth and final finding was that there is a lack of research that considers the relationships between the known facilitators or barriers to help-seeking for self-harm in young people. This is perhaps most concerning, as understanding the interactions that drive behavior is a central tenet of systems thinking. Further, it is arguably not possible to optimize behavior without understanding such interactions. Only a few studies have identified relationships, and of the relationships identified, the most frequently reported relationships were associated with the gender identity of the young person, a demographic factor, rather than another facilitator or a barrier. For example, gender identity was associated with the fear of being judged or stigmatized, resulting in a barrier to help-seeking for self-harm (Fortune et al., 2008b) or with trust, privacy, and confidentiality concerns (Fortune et al., 2008a). One of the characteristics of a complex system (Cilliers, 1998), and a principle underlying systems thinking (Rasmussen, 1997), is that behavioral outcomes (e.g., help-seeking for self-harm) result from interactions between decisions and actions across the entire system. Thus, the lack of research that considers relationships between the facilitators or barriers suggests that researchers have typically taken a reductionist view of this complex issue, by analyzing these facilitators or barriers in isolation. If help-seeking for self-harm in young people is viewed as a complex problem, then it is critical that the interactions between facilitators and barriers that influence young people’s help-seeking behaviors are well-understood.
A Note on the Quality of the Articles
In discussing the key findings from this systematic review, it is worth noting the outcomes of the quality assessment of the articles included in the review. Articles were assessed for their methodological quality using the Mixed Methods Appraisal Tool (Hong et al., 2018) but were not excluded based on low methodological quality. Overall, the articles included in this review demonstrated reasonable levels of methodological quality. However, interestingly, articles that adopted a qualitative study design scored higher than those that adopted a quantitative or mixed-methods study design. This does not necessarily suggest that qualitative study designs are superior methodologically compared to quantitative study designs or mixed-methods study designs, primarily because they were assessed on different criteria. Common methodological issues observed in the quantitative study design or quantitative components of the mixed-methods study design included insufficient, or the lack of, information reported around the representativeness of the sample and risk of nonresponse bias (see Supplementary Material). These methodological issues have also been noted in other systematic reviews (e.g., Thomason & Moghaddam, 2021; Zhuang et al., 2023).
Limitations
A limitation of this systematic review relates to the types of records included in the review; namely, only articles published in peer-reviewed journals were included. This means that findings from studies reported in other publication types; namely, gray literature such as conference proceedings, government reports, and student theses were not considered in this synthesis and analysis of this review. The inclusion of gray literature may pose methodological challenges in the review (e.g., lack of scientific rigor, additional time and resources in literature searching) but the benefits of including gray literature (e.g., reduced publication bias) could outweigh these challenges (Paez, 2017).
A second limitation relates to the broad definition of self-harm adopted in this review. The current, fifth edition Diagnostic and Statistical Manual of Mental Disorders (DSM-5) recognizes non-suicidal self-injury (i.e., self-harm without suicidal intent) as clinically distinct from suicidal self-harm (i.e., self-harm with suicidal intent) (American Psychiatric Association, 2013) but the diagnostic criteria for non-suicidal self-injury require further study and it remains controversial as to whether the definition of self-harm should include suicidal intent. Studies have demonstrated differences between self-harm with and without suicidal intent in their genetic etiology (Campos et al., 2020) and psychological risk profiles (Cleare et al., 2021; Mars et al., 2014). However, people who self-harm, engage in self-harm with and without suicidal intent (e.g., Wilkinson et al., 2011) and their suicidal intent can fluctuate temporally (e.g., Bryan, 2020). In light of the ongoing controversy and the inconsistent findings, this review adopted a broad definition of self-harm, including articles that focus on help-seeking for self-harm, irrespective of the suicidal intent behind the self-harm. By adopting this broad definition, it is assumed that the facilitators and barriers to help-seeking are similar across help-seeking for self-harm with suicidal intent and those without suicidal intent, when they may differ. Future research should consider whether the facilitators or barriers for help-seeking might differ when seeking help for self-harm with and without suicidal intent.
A third limitation relates to the variability in the age definition of young people across the articles included in this systematic review. The period of adolescence is not well defined, with some defining this period as ages between 10 to 19 years, and others 15 to 24 years or more inclusively, 10 to 24 years (Sawyer et al., 2018). Thus, this review included articles that described their study sample as young people, youth, adolescents, teens, or teenagers. How adolescence is conceptualized and defined has implications on our understanding of help-seeking behaviors, such that the developmental transition from being a child to being an adolescent can influence the way help is sought and/or the types of help-seeking sources they prefer. This is particularly important because many current health systems are limited in their ability to provide the comprehensive care young people require (Sawyer et al., 2018), which may consequently affect help-seeking behaviors.
The fourth limitation relates to the lack of consideration of gender or sex differences in this systematic review. This review did not consider gender or sex differences in the facilitators and barriers to help-seeking for self-harm; however, it was apparent that gender identity was associated with several factors (e.g., barrier: being discriminated against or victimized). Therefore, it would be important for these gender or sex differences in help-seeking behaviors to be accounted for when developing interventions or strategies to improve help-seeking in young people. It is worth noting that across the articles included in this systematic review, there was inconsistent reporting on gender or sex distribution of the study sample. Some studies reported gender distribution while others reported sex distribution, and some studies reported detailed information on gender or sex distribution while others reported minimal information. This inconsistent reporting of gender or sex distribution makes it difficult to assess whether there are gender or sex differences in the facilitators and barriers to help-seeking for self-harm. Future research should ensure that all relevant study sample characteristics are collected and reported.
The final limitation relates to the research field more broadly, and that is the conceptualization of help-seeking behaviors. Studies typically focus on assessing help-seeking behaviors at a single point in time and this focus means that only a fraction of one’s help-seeking process is considered. However, the help-seeking process is often prolonged, non-linear, and dynamic. In the context of young people who self-harm, a young person might “move in and out” of help-seeking for their self-harm, depending on their experiences of insecurity and unfamiliarity with mental health support, structural obstacles, and the process of finding and seeking help (e.g., Lost in Space model; Westberg et al., 2020). Future research should account for the dynamic nature of help-seeking for self-harm in young people, as not doing so will undermine the effectiveness of strategies implemented to improve help-seeking in this population.
Conclusion
Self-harm in adolescence has lasting impacts on their personal and social functioning and quality of life. Young people who self-harm would benefit from support and resources, but the rates of help-seeking in this population remain low. Thus, it is necessary to understand the facilitators and barriers to help-seeking for self-harm in young people, from a novel, systems thinking perspective. This systematic review synthesized the existing literature on the known facilitators and barriers to help-seeking for self-harm in young people from a systems thinking perspective. The systems thinking-based analysis revealed five key findings. First, there is a biased representation of research focus on the lower levels of the help-seeking for self-harm system. Second, many of the known facilitators related to the service delivery and social environment while, third, many of the known barriers related to young people who self-harm and their cognitions and feelings. Fourth, there were twice as many known barriers than there were known facilitators. Fifth and finally, there is a lack of research that considers the relationships between the known facilitators or barriers to help-seeking for self-harm in young people. In addition to contributing to the knowledge base on help-seeking for self-harm in young people, the review also identified key gaps in the knowledge base. Namely, a lack of research on how higher levels of the system influence help-seeking for self-harm in young people and how facilitators and barriers interact to influence help-seeking for self-harm in this population. This systematic review demonstrates the benefits of using systems thinking frameworks and methods in understanding the facilitators and barriers to help-seeking for self-harm in young people.
Data Availability
Not applicable.
References
Aguirre Velasco, A., Cruz, I. S. S., Bilings, J., Jimenez, M., & Rowe, S. L. (2020). What are the barriers, facilitators and interventions targeting help-seeking behaviours for common mental health problems in adolescents? A systematic review. BMC Psychiatry, 20(1), 293. https://doi.org/10.1186/s12888-020-02659-0
American Psychiatric Association. (2013). Diagnostic and statistical manual of mental disorders (DSM-5). American Psychiatric Association.
American Psychological Association (2018). Suicidality. https://dictionary.apa.org/suicidality
Austin, E., Blakley, B., Salmon, P. M., Braithwaite, J., & Clay-Williams, R. (2022). Identifying constraints on everyday clinical practice: Applying work domain analysis to Emergency Department Care. Human Factors, 64(1), 74–98. https://doi.org/10.1177/0018720821995668
Australian Government Department of Health and Aged Care. (2022). Improving Better Access for all Australians. https://www.health.gov.au/ministers/the-hon-mark-butler-mp/media/improving-better-access-for-all-australians
Australian Institute of Health and Welfare. (2024). Suicide and self-harm monitoring system. https://www.aihw.gov.au/suicide-self-harm-monitoring
Barker, G. (2007). Adolescents, social support and help-seeking behaviour: An international literature review and programme consultation with recommendations for action (WHO Discussion papers on Adolescence). https://www.who.int/publications/i/item/9789241595711
Barrett, P., Griffin, E., Corcoran, P., O’Mahony, M. T., & Arensman, E. (2018). Self-harm among the homeless population in Ireland: A national registry-based study of incidence and associated factors. Journal of Affective Disorders, 229, 523–531. https://doi.org/10.1016/j.jad.2017.12.040
Barrow, E., & Thomas, G. (2022). Exploring perceived barriers and facilitators to mental health help-seeking in adolescents: A systematic literature review. Educational Psychology in Practice, 38(2), 173–193. https://doi.org/10.1080/02667363.2022.2051441
Beckman, K., Mittendofer-Rutz, E., Waern, M., Larsson, H., Runeson, B., & Dahlin, M. (2018). Method of self-harm in adolescents and young adults and risk of subsequent suicide. The Journal of Child Psychology and Psychiatry, 59(9), 948–956. https://doi.org/10.1111/jcpp.12883
Bellairs-Walsh, I., Perry, Y., Krysinka, K., Byrne, S. J., Boland, A., Michail, M., Lamblin, M., Gibson, K. L., Lin, A., Li, T. Y., Hetrick, S., & Robinson, J. (2020). Best practice when working with suicidal behaviour and self-harm in primary care: A qualitative exploration of young people’s perspectives. British Medical Journal Open, 10(10), e038855. https://doi.org/10.1136/bmjopen-2020-038855
Berger, E., Hasking, P., & Martin, G. (2013). ‘Listen to them’: Adolescents’ views on helping young people who self-injure. Journal of Adolescence, 36(5), 935–945. https://doi.org/10.1016/j.adolescence.2013.07.011
Booth, A., Clarke, M., Ghersi, D., Moher, D., Petticrew, M., & Stewart, L. (2011). An international registry of systematic-review protocols. The Lancet, 377(9760), 108–109. https://doi.org/10.1016/S0140-6736(10)60903-8
Borschmann, R., Becker, D., Coffey, C., Spry, E., Moreno-Betancur, M., Moran, P., & Patton, G. C. (2017). 20-year outcomes in adolescents who self-harm: A population-based cohort study. The Lancet Child & Adolescent Health, 1(3), 195–202. https://doi.org/10.1016/S2352-4642(17)30007-X
Bryan, C. J. (2020). The temporal dynamics of the wish to live and the wish to die among suicidal individuals. In A. C. Page & W. G. J. Stritzke (Eds.), Alternatives to suicide (pp. 71–88). Academic Press. https://doi.org/10.1016/B978-0-12-814297-4.00004-2
Burke, T. A., Bettis, A. H., Barnicle, S. C., Wang, S. B., & Fox, K. R. (2021). Disclosure of self-injurious thoughts and behaviors across sexual and gender identities. Pediatrics. https://doi.org/10.1542/peds.2021-050255
Bushe, G. R. (2011). Appreciative inquiry: Theory and critique. In D. Boje, B. Burnes, & J. Hassard (Eds.), The Routledge companion to organizational change (pp. 87–103). Routledge. https://doi.org/10.4324/9780203810279.ch6
Butler, A. M., & Malone, K. (2013). Attempted suicide v. non-suicidal self-injury: Behaviour, syndrome or diagnosis? British Journal of Psychiatry, 202(5), 324–325. https://doi.org/10.1192/bjp.bp.112.113506
Byrne, S. J., Bellairs-Walsh, I., Rice, S. M., Bendall, S., Lamblin, M., Boubis, E., McGregor, B., O’Keefe, M., & Robinson, J. (2021). A qualitative account of young people’s experiences seeking care from emergency departments for self-harm. International Journal of Environmental Research and Public Health. https://doi.org/10.3390/ijerph18062892
Campos, A. I., Verweij, K. J. H., Statham, D. J., Madden, P. A. F., Maciejewski, D. F., Davis, K. A. S., John, A., Hotopf, M., Heath, A. C., Martin, N. G., & Renteria, M. E. (2020). Genetic aetiology of self-harm ideation and behaviour. Scientific Reports, 10(1), 9713. https://doi.org/10.1038/s41598-020-66737-9
Carroll, R., Metcalfe, C., & Gunnell, D. (2014). Hospital presenting self-harm and risk of fatal and non-fatal repetition: Systematic review and meta-analysis. PLoS ONE, 9(2), e89944. https://doi.org/10.1371/journal.pone.0089944
Chandler, A. (2018). Seeking secrecy: A qualitative study of younger adolescents’ accounts of self-harm. Young, 26(4), 313–331. https://doi.org/10.1177/1103308817717367
Chen, R., Wang, Y., Liu, L., Lu, L., Wilson, A., Gong, S., Zhu, Y., Sheng, C., Zeng, Y., Li, Y., & Ou, J. (2020). A qualitative study of how self-harm starts and continues among Chinese adolescents. Bjpsych Open, 7(1), e20. https://doi.org/10.1192/bjo.2020.144
Cilliers, P. (1998). Complexity and postmodernism: Understanding complex systems. London: Routledge.
Cleare, S., Wetherall, K., Eschle, S., Forrester, R., Drummond, J., & O’Connor, R. C. (2021). Using the integrated motivational-volitional (IMV) model of suicidal behaviour to differentiate those with and without suicidal intent in hospital treated self-harm. Preventive Medicine, 153(Pt 1), 106592. https://doi.org/10.1016/j.ypmed.2021.106592
Cleary, A. (2017). Help-seeking patterns and attitudes to treatment amongst men who attempted suicide. Journal of Mental Health, 26(3), 220–224. https://doi.org/10.3109/09638237.2016.1149800
Daukantaitė, D., Lundh, L.-G., Wångby-Lundh, M., Claréus, B., Bjärehed, J., Zhou, Y., & Liljedahl, S. I. (2021). What happens to young adults who have engaged in self-injurious behavior as adolescents? A 10-year follow-up. European Child & Adolescent Psychiatry, 30, 475–492. https://doi.org/10.1007/s00787-020-01533-4
Dodd, K., Solomon, C., Naughton, M., Salmon, P. M., & McLean, S. (2023). What enables child sexual abuse in sport? A systematic review. Trauma Violence Abuse. https://doi.org/10.1177/15248380231190666
Evans, E., Hawton, K., & Rodham, K. (2005). In what ways are adolescents who engage in self-harm or experience thoughts of self-harm different in terms of help-seeking, communication and coping strategies? Journal of Adolescence, 28(4), 573–587. https://doi.org/10.1016/j.adolescence.2004.11.001
Fadum, E. A., Stanley, B., Rossow, I., Mork, E., Tormoen, A. J., & Mehlum, L. (2013). Use of health services following self-harm in urban versus suburban and rural areas: A national cross-sectional study. BMJ Open. https://doi.org/10.1136/bmjopen-2013-002570
Farr, J., Surtees, A. D. R., Richardson, H., & Michail, M. (2021). Exploring the processes involved in seeking help from a general practitioner for young people who have been at risk of suicide. International Journal of Environmental Research and Public Health. https://doi.org/10.3390/ijerph18042120
Fortune, S., Sinclair, J., & Hawton, K. (2008). Adolescents’ views on preventing self-harm. A large community study. Social Psychiatry and Psychiatric Epidemiology, 43(2), 96–104. https://doi.org/10.1007/s00127-007-0273-1
Fortune, S., Sinclair, J., & Hawton, K. (2008b). Help-seeking before and after episodes of self-harm: A descriptive study in school pupils in England. BMC Public Health, 8, 369. https://doi.org/10.1186/1471-2458-8-369
Fox, K. R., Bettis, A. H., Burke, T. A., Hart, E. A., & Wang, S. B. (2022). Exploring adolescent experiences with disclosing self-injurious thoughts and behaviors across settings. Research on Child and Adolescent Psychopathology, 50(5), 669–681. https://doi.org/10.1007/s10802-021-00878-x
Freedenthal, S., & Stiffman, A. R. (2007). “They might think I was crazy”: Young American Indians’ reasons for not seeking help when suicidal. Journal of Adolescent Research, 22(1), 58–77. https://doi.org/10.1177/0743558406295969
Frost, M., Casey, L. M., & O’Gorman, J. G. (2017). Self-injury in young people and the help-negation effect. Psychiatry Research, 250, 291–296. https://doi.org/10.1016/j.psychres.2016.12.022
Frost, M., Casey, L., & Rando, N. (2016). Self-injury, help-seeking, and the internet: Informing online service provision for young people. Crisis, 37(1), 68–76. https://doi.org/10.1027/0227-5910/a000346
Gillies, D., Christou, M. A., Dixon, A. C., Featherston, O. J., Rapti, I., Garcia-Anguita, A., Villasis-Keever, M., Reebye, P., Christou, E., Al Kabir, N., & Christou, P. A. (2018). Prevalence and characteristics of self-harm in adolescents: Meta-analyses of community-based studies 1990–2015. Journal of the American Academy of Child and Adolescent Psychiatry, 57(10), 733–741. https://doi.org/10.1016/j.jaac.2018.06.018
Griffin, E., McMahon, E., McNicholas, F., Corcoran, P., Perry, I. J., & Arensman, E. (2018). Increasing rates of self-harm among children, adolescents and young adults: A 10-year national registry study 2007–2016. Social Psychiatry and Psychiatric Epidemiology, 53(7), 663–671. https://doi.org/10.1007/s00127-018-1522-1
Gulliver, A., Griffiths, K. M., & Christensen, H. (2010). Perceived barriers and facilitators to mental health help-seeking in young people: A systematic review. BMC Psychiatry, 10, 113. https://doi.org/10.1186/1471-244X-10-113
Hassett, A., & Isbister, C. (2017). Young men’s experiences of accessing and receiving help from child and adolescent mental health services following self-harm. SAGE Open. https://doi.org/10.1177/2158244017745112
Hawton, K., Bergen, H., Cooper, J., Turnbull, P., Waters, K., Ness, J., & Kapur, N. (2015). Suicide following self-harm: Findings from the Multicentre Study of Self-Harm in England, 2000–2012. Journal of Affective Disorders, 175, 147–151. https://doi.org/10.1016/j.jad.2014.12.062
Hawton, K., Saunders, K. E. A., & O’Connor, R. C. (2012). Self-harm and suicide in adolescents. The Lancet, 379(9834), 2373–2382. https://doi.org/10.1016/S0140-6736(12)60322-5
Hong, Q., Pluye, P., Fabruegues, S., Barlett, G., Boardman, F., Cargo, M., Dagenais, P., Gagnon, M. P., Griffiths, F., Nicolau, B., O’Cathain, A., Rousseau, M. C., & Vedel, I. (2018). Mixed Methods Appraisal Tool (MMAT). McGill University Department of Family Medicine.
Kannampallil, T. G., Schauer, G. F., Cohen, T., & Patel, V. L. (2011). Considering complexity in healthcare systems. Journal of Biomedical Informatics, 44(6), 943–947. https://doi.org/10.1016/j.jbi.2011.06.006
Keefner, T. P., & Stenvig, T. (2021). Suicidality: An evolutionary concept analysis. Issues in Mental Health Nursing, 42(3), 227–238. https://doi.org/10.1080/01612840.2020.1793243
Kelada, L., Hasking, P., & Melvin, G. (2016). The relationship between nonsuicidal self-injury and family functioning: Adolescent and parent perspectives. Journal of Marital and Family Therapy, 42(3), 536–549. https://doi.org/10.1111/jmft.12150
Klineberg, E., Kelly, M. J., Stansfeld, S. A., & Bhui, K. S. (2013). How do adolescents talk about self-harm: A qualitative study of disclosure in an ethnically diverse urban population in England. BMC Public Health, 13, 572. https://doi.org/10.1186/1471-2458-13-572
Knipe, D., Metcalfe, C., Hawton, K., Pearson, M., Dawson, A., Jayamanne, S., Konradsen, F., Eddleston, M., & Gunnell, D. (2019). Risk of suicide and repeat self-harm after hospital attendance for non-fatal self-harm in Sri Lanka: A cohort study. The Lancet Psychiatry, 6(8), 659–666. https://doi.org/10.1016/S2215-0366(19)30214-7
Knipe, D., Padmanathan, P., Newton-howes, G., Chan, L. F., & Kapur, N. (2022). Suicide and self-harm. The Lancet, 399(10338), 1903–1916. https://doi.org/10.1016/S0140-6736(22)00173-8
Koorts, H., Salmon, P. M., Swain, C. T. V., Cassar, S., Strickland, D., & Salmon, J. (2022). A systems thinking approach to understanding youth active recreation. International Journal of Behavioral Nutrition and Physical Activity, 19(1), 53. https://doi.org/10.1186/s12966-022-01292-2
Landis, J. R., & Koch, G. G. (1977). The measurement of observer agreement for categorical data. Biometrics, 33(1), 159–174. https://doi.org/10.2307/2529310
Lane, B. R., Read, G. J. M., Cook, L., & Salmon, P. M. (2020). A systems thinking perspective on the barriers to treatment access for people with eating disorders. International Journal of Eating Disorders, 53(2), 174–179. https://doi.org/10.1002/eat.23214
Laskite, A., & Laskene, S. (2011). Adolescents’ intentional self-mutilation. Russian Education & Society, 53(9), 83–88. https://doi.org/10.2753/res1060-9393530907
Lauriks, S., de Wit, M. A., Buster, M. C., Fassaert, T. J., van Wifferen, R., & Klazinga, N. S. (2014). The use of the Dutch Self-Sufficiency Matrix (SSM-D) to inform allocation decisions to public mental health care for homeless people. Community Mental Health Journal, 50(7), 870–878. https://doi.org/10.1007/s10597-014-9707-x
Leveson, N. (2004). A new accident model for engineering safer systems. Safety Science, 42(4), 237–270. https://doi.org/10.1016/s0925-7535(03)00047-x
Levi-Belz, Y., Gavish-Marom, T., Barzilay, S., Apter, A., Carli, V., Hoven, C., Sarchiapone, M., & Wasserman, D. (2019). Psychosocial factors correlated with undisclosed suicide attempts to significant others: Findings from the Adolescence SEYLE Study. Suicide and Life Threatening Behaviors, 49(3), 759–773. https://doi.org/10.1111/sltb.12475
Lucena, N. L., Rossi, T. A., Azevedo, L. M. G., & Pereira, M. (2022). Self-injury prevalence in adolescents: A global systematic review and meta-analysis. Children and Youth Services Review. https://doi.org/10.1016/j.childyouth.2022.106634
Lustig, S., Koenig, J., Resch, F., & Kaess, M. (2021). Help-seeking duration in adolescents with suicidal behavior and non-suicidal self-injury. Journal of Psychiatric Research, 140, 60–67. https://doi.org/10.1016/j.jpsychires.2021.05.037
Mars, B., Heron, J., Crane, C., Hawton, K., Kidger, J., Lewis, G., Macleod, J., Tilling, K., & Gunnell, D. (2014). Differences in risk factors for self-harm with and without suicidal intent: Findings from the ALSPAC cohort. Journal of Affective Disorders, 168, 407–414. https://doi.org/10.1016/j.jad.2014.07.009
McAndrew, S., & Warne, T. (2014). Hearing the voices of young people who self-harm: Implications for service providers. International Journal of Mental Health Nursing, 23(6), 570–579. https://doi.org/10.1111/inm.12093
McDermott, E. (2015). Asking for help online: Lesbian, gay, bisexual and trans youth, self-harm and articulating the ‘failed’ self. Health (london, England), 19(6), 561–577. https://doi.org/10.1177/1363459314557967
McDermott, E., Hughes, E., & Rawlings, V. (2018). Norms and normalisation: Understanding lesbian, gay, bisexual, transgender and queer youth, suicidality and help-seeking. Culture, Health, and Sexuality, 20(2), 156–172. https://doi.org/10.1080/13691058.2017.1335435
McManus, S., Gunnell, D., Cooper, C., Bebbington, P. E., Howard, L. M., Brugha, T., Jenkins, R., Hassiotis, A., Weich, S., & Appleby, L. (2019). Prevalence of non-suicidal self-harm and service contact in England, 2000–14: Repeated cross-sectional surveys of the general population. Lancet Psychiatry, 6(7), 573–581. https://doi.org/10.1016/s2215-0366(19)30188-9
Meadows, D. (1999). Leverage points: Places to intervene in a system. The Sustainability Institute, Hartland
Michelmore, L., & Hindley, P. (2012). Help-seeking for suicidal thoughts and self-harm in young people: A systematic review. Suicide and Life-Threatening Behavior, 42(5), 507–524. https://doi.org/10.1111/j.1943-278X.2012.00108.x
Mojtabai, R., & Olfson, M. (2008). Parental detection of youth’s self-harm behavior. Suicide and Life-Threatening Behaviors, 38(1), 60–73. https://doi.org/10.1521/suli.2008.38.1.60
Morey, C., Corcoran, P., Arensman, E., & Perry, I. J. (2008). The prevalence of self-reported deliberate self harm in Irish adolescents. BMC Public Health, 8, 79. https://doi.org/10.1186/1471-2458-8-79
Morgan, C., Webb, R. T., Carr, M. J., Kontopantelis, E., Chew-Graham, C. A., & Kapur, N. (2018). Self-harm in a primary care cohort of older people: Incidence, clinical management, and risk of suicide and other causes of death. The Lancet Psychiatry, 5(11), 905–912. https://doi.org/10.1016/S2215-0366(18)30348-1
Nada-Raja, S., Morrison, D., & Skegg, K. (2003). A population-based study of help-seeking for self-harm in young adults. Australian and New Zealand Journal of Psychiatry, 37(5), 600–605. https://doi.org/10.1046/j.1440-1614.2003.01252.x
Nixon, M. K., Cloutier, P., & Jansson, S. M. (2008). Nonsuicidal self-harm in youth: A population-based survey. Canadian Medical Association Journal, 178(3), 306–312. https://doi.org/10.1503/cmaj.061693
Nock, M. K., Greif Green, J., Hwang, I., McLaughlin, K. A., Sampson, N. A., Zaslavsky, A. M., & Kessler, R. C. (2013). Prevalence, correlates, and treatment of lifetime suicidal behavior among adolescents: Results from the National Comorbidity Survey Replication Adolescent Supplement. JAMA Psychiatry, 70(3), 300–310. https://doi.org/10.1001/2013.jamapsychiatry.55
Occhipinti, J.-A., Skinner, A., Carter, S., Heath, J., Lawson, K., McGill, K., McClure, R., & Hickie, I. B. (2021). Federal and state cooperation necessary but not sufficient for effective regional mental health systems: Insights from systems modelling and simulation. Scientific Reports, 11(1), 11209. https://doi.org/10.1038/s41598-021-90762-x
Owens, C., Hansford, L., Sharkey, S., & Ford, T. (2016). Needs and fears of young people presenting at accident and emergency department following an act of self-harm: Secondary analysis of qualitative data. British Journal of Psychiatry, 208(3), 286–291. https://doi.org/10.1192/bjp.bp.113.141242
Pace, R., Pluye, P., Bartlett, G., Macaulay, A. C., Salsberg, J., Jagosh, J., & Seller, R. (2012). Testing the reliability and efficiency of the pilot Mixed Methods Appraisal Tool (MMAT) for systematic mixed studies review. International Journal of Nursing Studies, 49(1), 47–53. https://doi.org/10.1016/j.ijnurstu.2011.07.002
Paez, A. (2017). Gray literature: An important resource in systematic reviews. Journal of Evidence-Based Medicine, 10(3), 233–240. https://doi.org/10.1111/jebm.12266
Page, M. J., McKenzie, J. E., Bossuyt, P. M., Boutron, I., Hoffman, T. C., Mulrow, C. D., Shamseer, L., Tetzlaff, J. M., Akl, E. A., Brennan, S. E., Chou, R., Glanville, J., Grimshaw, J. M., Hrobjartsson, A., Lalu, M. M., Li, T., Loder, E. W., Mayo-Wilson, E., McDonald, S., & Moher, D. (2021). The PRISMA 2020 statement: An updated guideline for reporting systematic review. BMJ, 372, n71. https://doi.org/10.1136/bmj.n71
Pirkis, J., Currier, D., Harris, M., Mihalopoulos, C., Arya, V., Banfield, M., Bassilios, B., Buchanan, B., Butterworth, P., Brophy, L., Burgess, P., Chatterton, M. L., Chilver, M., Eagar, K., Faller, J., Fossey, E., Fatanou, M., Gunn, J., Kruger, A., Williamson, M. (2022). Evaluation of Better Access. https://www.health.gov.au/sites/default/files/2022-12/main-report-evaluation-of-the-better-access-initiative.pdf
Pluye, P., Gagnon, M. P., Griffiths, F., & Johnson-Lafleur, J. (2009). A scoring system for appraising mixed methods research, and concomitantly appraising qualitative, quantitative and mixed methods primary studies in Mixed Studies Reviews. International Journal of Nursing Studies, 46(4), 529–546. https://doi.org/10.1016/j.ijnurstu.2009.01.009
Raben, D. C., Viskum, B., Mikkelsen, K. L., Hounsgaard, J., Bogh, S. B., & Hollnagel, E. (2018). Application of a non-linear model to understand healthcare processes: Using the functional resonance analysis method on a case study of the early detection of sepsis. Reliability Engineering & System Safety, 177, 1–11. https://doi.org/10.1016/j.ress.2018.04.023
Radez, J., Reardon, T., Creswell, C., Lawrence, P. J., Evdoka-Burton, G., & Waite, P. (2021). Why do children and adolescents (not) seek and access professional help for their mental health problem? A systematic review of quantitative and qualitative studies. European Child & Adolescent Psychiatry, 30(2), 183–211. https://doi.org/10.1007/s00787-019-01469-4
Rasmussen, J. (1997). Risk management in a dynamic society: A modelling problem. Safety Science, 27(2–3), 183–213. https://doi.org/10.1016/S0925-7535(97)00052-0
Read, G. J. M., Cox, J. A., Hulme, A., Naweed, A., & Salmon, P. M. (2021). What factors influence risk at rail level crossings? A systematic review and synthesis of findings using systems thinking. Safety Science. https://doi.org/10.1016/j.ssci.2021.105207
Rickwood, D. J., & Braithwaite, V. A. (1994). Social-psychological factors affecting help-seeking for emotional problems. Social Science & Medicine, 39(4), 563–572. https://doi.org/10.1016/0277-9536(94)90099-X
Rickwood, D. J., Deane, F. P., & Wilson, C. J. (2007). When and how do young people seek professional help for mental health problems? Medical Journal of Australia, 187(S7), S35-39. https://doi.org/10.5694/j.1326-5377.2007.tb01334.x
Rosenrot, S. A., & Lewis, S. P. (2020). Barriers and responses to the disclosure of non-suicidal self-injury: A thematic analysis. Counselling Psychology Quarterly, 33(2), 121–141. https://doi.org/10.1080/09515070.2018.1489220
Rowe, S. L., French, R. S., Henderson, C., Ougrin, D., Slade, M., & Moran, P. (2014). Help-seeking behaviour and adolescent self-harm: A systematic review. Australian and New Zealand Journal of Psychiatry, 48(12), 1083–1095. https://doi.org/10.1177/0004867414555718
Royal College of Psychiatrists. (2010). Self-harm, suicide and risk: Helping people who self-harm (Council Report CR158). http://www.rcpsych.ac.uk/publications/collegereports/cr/cr158.aspx
Salmon, P. M., Naughton, M., Hulme, A., & McLean, S. (2022). Bicycle crash contributory factors: A systematic review. Safety Science. https://doi.org/10.1016/j.ssci.2021.1055116
Sara, G., Wu, J., Uesi, J., Jong, N., Perkes, I., Knight, K., O’Leary, F., Trudgett, C., & Bowden, M. (2022). Growth in emergency department self-harm or suicidal ideation presentations in young people: Comparing trends before and since the COVID-19 first wave in New South Wales, Australia. Australian & New Zealand Journal of Psychiatry, 57(1), 58–68. https://doi.org/10.1177/00048674221082518
Sawyer, S. M., Azzopardi, P. S., Wickremarathne, D., & Patton, G. C. (2018). The age of adolescence. The Lancet Child & Adolescent Health, 2(3), 223–228. https://doi.org/10.1016/S2352-4642(18)30022-1
Schenk, L., Sentse, M., Lenkens, M., Engbersen, G., van de Mheen, D., Nagelhout, G. E., & Severiens, S. (2018). At-risk youths’ self-sufficiency: The role of social capital and help-seeking orientation. Children and Youth Services Review, 91, 263–270. https://doi.org/10.1016/j.childyouth.2018.06.015
Sen, B. (2004). Adolescent propensity for depressed mood and help-seeking: Race and gender differences. The Journal of Mental Health Policy and Economics, 7(3), 133–145.
Svedung, I., & Rasmussen, J. (2002). Graphic representation of accident scenarios: Mapping system structure and the causation of accidents. Safety Science, 40(5), 397–417. https://doi.org/10.1016/S0925-7535(00)00036-9
Thomason, S., & Moghaddam, N. (2021). Compassion-focused therapies for self-esteem: A systematic review and meta-analysis. Psychology and Psychotherapy: Theory, Research and Practice, 94, 737–759. https://doi.org/10.1111/papt.12319
Vacher, C., Skinner, A., Occhipinti, J.-A., Rosenberg, S., Ho, N., Song, Y. J. C., & Hickie, I. B. (2023). Improving access to mental health care: A system dynamics model of direct access to specialist care and accelerated specialist service capacity growth. Medical Journal of Australia, 218(7), 309–314. https://doi.org/10.5694/mja2.51903
Veritas Health Innovation. (n.d.). Covidence systematic review software. In www.covidence.org.
Vivier, T., Moro, M. R., Baubet, T., Pionnie-Dax, N., Grandclerc, S., Spiers, S., & Lachal, J. (2023). Gender in the suicidal experience: A qualitative study among adolescents. Archives of Suicide Research, 27(2), 505–521. https://doi.org/10.1080/13811118.2021.2021337
Wadman, R., Vostanis, P., Sayal, K., Majumder, P., Harroe, C., Clarke, D., Armstrong, M., & Townsend, E. (2018). An interpretative phenomenological analysis of young people’s self-harm in the context of interpersonal stressors and supports: Parents, peers, and clinical services. Social Science & Medicine, 212, 120–128. https://doi.org/10.1016/j.socscimed.2018.07.021
Westberg, K. H., Nygren, J. M., Nyholm, M., Carlsson, I. M., & Svedberg, P. (2020). Lost in space - an exploration of help-seeking among young people with mental health problems: A constructivist grounded theory study. Archives of Public Health, 78, 93. https://doi.org/10.1186/s13690-020-00471-6
Wilkinson, P., Kelvin, R., Roberts, C., Dubicka, B., & Goodyer, I. (2011). Clinical and psychosocial predictors of suicide attempts and nonsuicidal self-injury in the adolescent depression antidepressants and psychotherapy trial. American Journal of Psychiatry, 168(5), 495–501. https://doi.org/10.1176/APPI.AJP.2010.10050718
World Health Organization. (2021). Suicide worldwide in 2019. https://www.who.int/publications/i/item/9789240026643
Ystgaard, M., Arensman, E., Hawton, K., Madge, N., van Heeringen, K., Hewitt, A., de Wilde, E. J., De Leo, D., & Fekete, S. (2009). Deliberate self-harm in adolescents: Comparison between those who receive help following self-harm and those who do not. Journal of Adolescence, 32(4), 875–891. https://doi.org/10.1016/j.adolescence.2008.10.010
Zaki, L. F., Gross, M., & Pachankis, J. E. (2017). Help-seeking for nonsuicidal self-injury in sexual minority adolescent and young adult females. Journal of Gay & Lesbian Mental Health, 21(2), 171–187. https://doi.org/10.1080/19359705.2016.1273156
Zareian, B., & Klonsky, E. D. (2019). Nonsuicidal and suicidal self-injury. In J. J. Wasburn (Ed.), Nonsuicidal self-injury: Advances in research and practice. Routledge. https://doi.org/10.4324/9781315164182
Zhuang, S., Tan, D. W., Reddrop, S., Dean, L., Maybery, M., & Magiati, I. (2023). Psychosocial factors associated with camouflaging in autistic people and its relationship with mental health and well-being: A mixed methods systematic review. Clinical Psychology Review, 105, 102335. https://doi.org/10.1016/j.cpr.2023.102335
Acknowledgements
The authors gratefully acknowledge the Editor of Adolescent Research Review and the anonymous reviewers for their expertise and valuable feedback.
Funding
Open Access funding enabled and organized by CAUL and its Member Institutions. The project is funded by the University of the Sunshine Coast Internal Funding Scheme (LAUNCH).
Author information
Authors and Affiliations
Contributions
JAC led the conceptualization of this study, designed, coordinated, and participated in the data extraction and interpretation, and drafted the manuscript; LM participated in the literature search, coordinated and participated in the data extraction and interpretation, and reviewed and edited the manuscript; DFH was involved in the conceptualization of this study, coordinated and participated in the data extraction and interpretation, and reviewed and edited the manuscript; GJMR was involved in the conceptualization of this study, participated in the data extraction and interpretation, and reviewed and edited the manuscript; PMS was involved in the conceptualization of this study, and reviewed and edited the manuscript. All authors read and approved the manuscript.
Corresponding author
Ethics declarations
Conflict of interest
The authors report no conflicts of interest.
Generative AI and AI-Assisted Technologies in the Writing Process
The authors declare that generative AI and AI-assisted technologies were not used in the preparation of this work.
Preregistration
The systematic review was prospectively registered in the International Prospective Register of Systematic Reviews (PROSPERO; Registration Number: CRD42023384541).
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if changes were made. The images or other third party material in this article are included in the article's Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article's Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
Cox, J.A., Mills, L., Hermens, D.F. et al. A Systematic Review of the Facilitators and Barriers to Help-Seeking for Self-Harm in Young People: A Systems Thinking Perspective. Adolescent Res Rev 9, 411–434 (2024). https://doi.org/10.1007/s40894-024-00241-3
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s40894-024-00241-3