Abstract
Introduction
Many inflammatory conditions, such as asthma, show circadian symptoms that are worse at night. Delayed-release prednisone was developed for bedtime administration to optimize inhibition of nocturnally elevated pro-inflammatory cytokines. A proof-of-concept study was undertaken to examine the impact of delayed-release prednisone on nocturnal awakenings in patients with asthma requiring treatment with oral steroids.
Methods
In this single-center, open-label study, patients receiving long-term treatment with conventional prednisone administered at 08:00 h were switched to 4 weeks of treatment with the same dose of delayed-release prednisone given at 22:00 h. The primary efficacy endpoint was the change in number of nocturnal awakenings during the final 2 weeks of each treatment phase.
Results
Seven patients received treatment with delayed-release prednisone. Mean nocturnal awakenings because of asthma decreased from 10.0 ± 5.45 with conventional prednisone to 2.1 ± 4.41 with delayed-release prednisone, a mean reduction of −7.9 ± 6.07 (82.7% reduction). Delayed-release prednisone was generally well tolerated, and there were no unexpected safety findings.
Conclusions
Although the size of the efficacy population was too small to detect any statistically significant changes in nocturnal asthma control, this proof-of-concept study suggests that nighttime administration of delayed-release prednisone provides better asthma symptom control compared with morning administration of conventional prednisone.
Funding
Horizon Pharma, Inc (formerly Nitec Pharma GmbH).
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
More than 60 years after their first clinical use, corticosteroids still form the mainstay of treatment for inflammatory conditions [1, 2]. With awareness of potential safety and tolerability issues arising from systemic exposure, topical corticosteroid preparations were developed, including inhaled formulations for use in inflammatory respiratory conditions (e.g., asthma). In other inflammatory conditions (e.g., rheumatoid arthritis or polymyalgia rheumatica), the chronic systemic nature or inaccessible location of the affected site precludes routine topical treatment and, therefore, administration of corticosteroids remains predominantly via the oral route. The need to improve the benefit:risk ratio for these patients continues to drive the development of this important class of treatment.
A common feature of many inflammatory conditions, including asthma, is the circadian pattern of symptoms [3, 4]. Recognition of this characteristic in rheumatoid arthritis prompted development of an oral formulation of prednisone that can be taken at bedtime, but releases the active ingredient approximately 4 h later, at the appropriate time to inhibit the nocturnal peak of pro-inflammatory cytokines that are associated with morning symptoms [5, 6]. In patients with rheumatoid arthritis, delayed-release prednisone reduces morning stiffness significantly more than the same dose of conventional prednisone (3–10 mg/day) taken in the morning, with benefit sustained over 12 months of treatment [7, 8]. Although in Europe, it is predominantly used to treat rheumatoid arthritis, in the USA and other countries the common nature of many inflammatory conditions is recognized in the approved indication of delayed-release prednisone as an anti-inflammatory or immunosuppressive agent for a range of conditions, including allergic and respiratory conditions.
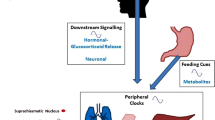
The circadian nature of asthma symptoms is widely recognized by clinicians and patients alike. The involvement of clock genes located centrally and in the lung has been reported [4]. In the UK, 37% of patients with asthma reported frequent nighttime symptoms and in a large Europe-wide survey of patients with asthma, 54.5% reported one or more nights during the previous week with waking because of asthma [9, 10]. Nocturnal symptoms are usually indicative of poor asthma control [11]. Although adjustment of inhaled therapy may be sufficient for most patients, frequent nocturnal asthma symptoms are characteristic of severe persistent asthma that is difficult to treat [11, 12]. Patients with these symptoms usually require long-term treatment with oral corticosteroids in addition to inhaled therapy. In the USA, an estimated 4% of patients with asthma receive treatment with oral corticosteroids for at least 6 months, predominantly at doses up to 10 mg per day [13].
As in rheumatoid arthritis, there might be room to improve the optimal or preferred delivery of glucocorticoids and possibly improve the therapeutic ratio in patients with severe persistent nocturnal asthma who require longer term therapy. Delayed-release prednisone (also known as modified-release prednisone) once released in the gastrointestinal track behaves exactly like conventional (immediate-release prednisone) [5]. When taken orally at bedtime, prednisone peaks in the plasma approximately 6 h later [5]. This corresponds to the time when the hypothalamic–pituitary–adrenal (HPA) axis is most active, and is the preferred time to deliver glucocorticoid therapy from both an efficacy (i.e., most heightened inflammatory period) and a safety perspective (least likely to dampen the HPA axis long term) [3, 5, 6]. As we report here, the Modified-Release Prednisone for Treatment of Nocturnal Asthma (MONA) study was an exploratory proof-of-concept study to evaluate the impact on nocturnal symptoms of a switch from conventionally administered immediate-release prednisone to delayed-release prednisone in patients with severe asthma.
Methods
Patients
Patients included in the study were aged at least 18 years with a diagnosis of severe persistent asthma based on the American Thoracic Society (ATS) criteria [14], following monitoring for at least 18 months. All patients required continued treatment with oral corticosteroids for at least 12 months, in addition to standard therapy (high doses of inhaled steroids plus long-acting beta-2 agonist), and all patients had frequent nocturnal symptoms (at least three nocturnal awakenings because of asthma during the final screening week). Patients with hospital admission for asthma and/or lower airway infection in the 4 weeks before study entry were excluded from the study.
Study Design
This was a single-center, open-label, Phase IIa, sequential, single-treatment proof-of-concept study performed between July 2008 and May 2010. Eligible patients received treatment with conventional prednisone during a 4-week period (Weeks 0–4; treatment period 1) before switching to the same dose of delayed-release prednisone for 4 weeks (Weeks 4–8; treatment period 2). Conventional prednisone was administered at 08:00 h ± 30 min and delayed-release prednisone was administered at 22:00 h ± 30 min.
Assessments
Scheduled visits occurred at Week 0 and every 2 weeks to week 8. The primary efficacy endpoint was the change in the mean number of nocturnal awakenings during the final 2 weeks of each treatment phase. Secondary endpoints included changes in respiratory function measured by morning and evening peak expiratory flow (PEF), forced expiratory volume in 1 s (FEV1), and forced vital capacity (FVC) at the end of each treatment period. The impact of asthma on patients was determined at the end of each treatment period, using the Asthma Control Questionnaire (ACQ) and Asthma Quality of Life Questionnaire (AQLQ) [15, 16]. For the ACQ (which assesses asthma control over the previous week), a decrease in score corresponds to an improvement in asthma control [16]. For the AQLQ (which assesses the impact of asthma on health-related quality of life during the previous 2 weeks), an increase in score corresponds to an improvement in quality of life [15].
Safety
Safety and tolerability data were collected for all patients. Safety assessments included physical examination, vital signs, and laboratory and/or biological data. All adverse events (AEs) were recorded with information on their severity, relation to study medication, duration, and whether they were considered serious.
Statistical Analysis
All analyses were descriptive. The study was not designed or powered to detect statistical differences in endpoints. The study aimed to recruit a minimum of five and a maximum of 20 patients. The safety population comprised all patients dispensed any study medication. The efficacy population comprised all patients who completed both treatment periods.
Compliance with Ethics Guidelines
The study was conducted in accordance with the International Conference on Harmonization Guidelines for Good Clinical Practice and the Declaration of Helsinki. The protocol was approved by the local ethics committee/institutional review board, and all patients provided informed written consent prior to study-related procedures.
Results
Study Population
Of 15 patients screened, a total of 12 patients were eligible to enter treatment period 1, receiving conventional prednisone; these patients constituted the safety population. During this period, five patients were withdrawn; the remaining patients entered the delayed-release prednisone treatment period (treatment period 2) and completed the study (efficacy population; Fig. 1). Patient demographics are shown in Table 1. Previous medical history in the study population included surgical procedures in 11 patients [mostly cesarean section or appendicectomy (58%)], history of infection (58%), gastrointestinal pregnancy or perinatal conditions, reproductive or breast disorders, respiratory disorders, vascular disorders, and phlebitis, which occurred in two (16.7%) patients each. Prednisone doses for the patients completing the study ranged from 5 mg to 45 mg/day with a median dose of 20 mg/day both before and after switch to delayed-release prednisone, indicating parity in the doses between both study arms.
Efficacy
Following the switch to delayed-release prednisone, the number of nocturnal awakenings because of asthma decreased from a mean (SD) of 10.0 ± 5.45 to 2.1 ± 4.41, a mean reduction of −7.9 ± 6.07 and mean relative reduction of −82.7% (Table 2). The number of nocturnal awakenings was reduced in six out of the seven patients (Fig. 2). Improvements were also seen in other measures of lung function (Table 3).
General asthma control, as assessed by the ACQ, improved from a mean (SD) of 18.7 ± 3.30 in the final week of conventional prednisone treatment to a mean (SD) of 11.4 ± 3.46 in the final week of therapy with delayed-release prednisone. Asthma-related quality of life scores (as measured by the AQLQ) improved from a mean (SD) of 130.9 ± 19.69 in the final 2 weeks of conventional prednisone treatment to a mean (SD) of 162.2 ± 25.97 in the final 2 weeks of delayed-release prednisone treatment. Improvements in these patient-reported outcomes were seen in six out of the seven patients (Fig. 3).
Safety and Tolerability
Most AEs reported during the study were of mild-to-moderate intensity and most were respiratory disorders. During the first treatment period (conventional prednisone), seven patients (58.3%) experienced at least one AE, with one considered serious (asthma exacerbation and arterial thrombosis). The most common AEs were reported in the Infections and Infestations category (33%). None of the AEs are considered related to study treatment. During the second treatment period (delayed-release prednisone), six patients (85.7%) experienced at least one AE, none serious. The most common AEs reported were in the Respiratory, Thoracic and Mediastinal Disorders category (42.9%). In two patients, the AEs (tremor and insomnia in one patient, and insomnia in one patient) were considered related to study treatment. There were no deaths or life-threatening AEs associated with study treatments. No clinically relevant changes in hematological or biochemical parameters, or vital signs were observed during the study.
Discussion
Results from this small proof-of-concept study suggest that patients requiring oral corticosteroid treatments for severe nocturnal asthma benefit from a switch to delayed-release prednisone.
Nocturnal asthma is a variable exacerbation of the underlying asthma condition associated with increases in symptoms, need for medication, and worsening of lung function. These changes are related to sleep and/or circadian events [17]. Studies in patients with nocturnal asthma have demonstrated circadian changes in circulating eosinophils numbers that correlated with peak-flow variation [18, 19]. Fluctuating eosinophil inflammation was also observed in bronchoalveolar lavage fluid and in transbronchial biopsies of patients with asthma, with greater magnitude of increase in those with nocturnal symptoms [20, 21]. These data suggest that circadian activation of inflammatory cells has a pathogenic role in the development of nighttime airflow limitation. Therefore, as with other inflammatory conditions with circadian symptoms, an anti-inflammatory drug targeting this nocturnal peak in airway inflammation could show benefits over the same treatment used at other times of the day. This concept was explored more than 20 years ago, although nocturnal corticosteroid administration was not investigated [22]. The impact on nocturnal asthma symptoms of inhaled steroid administration time is unclear [23]. In our proof-of-concept study, delayed-release prednisone given at 22:00 h was superior to conventional prednisone given at 08:00 h. The improvement in asthma control and nocturnal symptoms observed with delayed-release prednisone might result from the delivery of anti-inflammatory therapy at the most appropriate time to inhibit pathophysiological processes that result in symptoms.
Delayed-release prednisone was generally well tolerated, and there were no deaths or life-threatening AEs. There were no unexpected safety findings. These results are consistent with those with rheumatoid arthritis [7, 8, 24].
Although the size of the efficacy population was too small to detect any statistically significant changes, this proof-of-concept study suggests that delayed-release prednisone provides better asthma symptom control compared with standard morning administration of conventional prednisone. The limitations of an small, open-label, nonrandomized study such as this are well known and further study of delayed-release prednisone in patients with severe asthma is warranted to investigate whether switching to this treatment from the more conventional formulation improves outcomes and potentially allows a reduction in corticosteroid dose, as has been noted in the treatment of rheumatoid arthritis [25].
Conclusion
This proof-of-concept study suggests that nighttime administration of delayed-release prednisone provides better asthma symptom control compared with morning administration of conventional immediate-release prednisone. Timed delivery of prednisone during the peak inflammatory period (early morning sleeping hours) may be the most efficacious time to administer exogenous glucocorticoids to patients with nocturnal asthma.
References
Buttgereit F. A fresh look at glucocorticoids. How to use an old ally more effectively. Bull NYU Hosp Joint Dis. 2012;70(Suppl. 1):S26–9.
Buttgereit F, Gibofsky A. Delayed-release prednisone—a new approach to an old therapy. Expert Opin Pharmacother. 2013;14:1097–106.
Cutolo M, Straub RH, Buttgereit F. Circadian rhythms of nocturnal hormones in rheumatoid arthritis: translation from bench to bedside. Ann Rheum Dis. 2009;67:905–8.
Durrington HJ, Farrow SN, Loudon AS, Ray DW. The circadian clock and asthma. Thorax. 2014;69:90–2.
Derendorf H, Ruebsamen K, Clarke L, Schaeffler A, Kirwan JR. Pharmacokinetics of modified-release prednisone tablets in healthy subjects and patients with rheumatoid arthritis. J Clin Pharmacol. 2013;53:326–33.
Kirwan JR, Clarke L, Hunt LP, et al. Effect of novel therapeutic glucocorticoids on circadian rhythms of hormones and cytokines in rheumatoid arthritis. Ann NY Acad Sci. 2010;1193:127–33.
Buttgereit F, Doering G, Schaeffler A, et al. Efficacy of modified-release versus standard prednisone to reduce duration of morning stiffness of the joints in rheumatoid arthritis (CAPRA-1): a double-blind, randomised controlled trial. Lancet. 2008;371:205–14.
Buttgereit F, Doering G, Schaeffler A, et al. Targeting pathophysiological rhythms: prednisone chronotherapy shows sustained efficacy in rheumatoid arthritis. Ann Rheum Dis. 2010;69:1275–80.
Fletcher M, Hiles D. Continuing discrepancy between patient perception of asthma control and real-world symptoms: a quantitative online survey of 1,083 adults with asthma from the UK. Prim Care Respir J. 2013;22:431–8.
Price D, Fletcher M, van der Molen T. Asthma control and management in 8,000 European patients: the REcognise Asthma and LInk to Symptoms and Experience (REALISE) survey. Prim Care Respir Med. 2014;24:14009.
Bateman ED, Hurd SS, Barnes PJ, et al. Global strategy for asthma management and prevention: GINA executive summary. Eur Respir J. 2008;31:143–78.
Chanez P, Wenzel SE, Anderson GP, et al. Severe asthma in adults: what are the important questions? J Allergy Clin Immunol. 2007;119:1337–8.
Lüttgen MA, Rummel A, Batra A, Mitar I. Oral glucocorticoid treatment of severe/uncontrolled asthma—current practice in the US. Am J Respir Crit Care Med. 2010;181:A6660.
Anon. Proceedings of the ATS workshop on refractory asthma: current understanding, recommendations, and unanswered questions. American Thoracic Society. Am J Respir Crit Care Med. 2000;162:2341–51.
Juniper EF, Guyatt GH, Cox FM, Ferrie PJ, King DR. Development and validation of the Mini Asthma Quality of Life Questionnaire. Eur Respir J. 1999;14:32–8.
Juniper EF, O’Bryne PM, Guyatt GH, Ferrie PJ, King DR. Development and validation of a questionnaire to measure asthma control. Eur Respir J. 2014;14:902–7.
Martin RJ, Banks-Schlegel S. Chronobiology of asthma. Am J Respir Crit Care Med. 1998;158:1002–7.
Bates ME, Clayton M, Calhoun W, et al. Relationship of plasma epinephrine and circulating eosinophils to nocturnal asthma. Am J Respir Crit Care Med. 1994;149:667–72.
Calhoun WJ, Bates ME, Schrader L, Sedgwick JB, Busse WW. Characteristics of peripheral blood eosinophils in patients with nocturnal asthma. Am Rev Respir Dis. 1992;145:577–81.
Jarjour NN, Busse WW. Cytokines in bronchoalveolar lavage fluid of patients with nocturnal asthma. Am J Respir Crit Care Med. 1995;152:1474–7.
Kraft M, Djukanovic R, Wilson S, Holgate ST, Martin RJ. Alveolar tissue inflammation in asthma. Am J Respir Crit Care Med. 1996;154:1505–10.
Beam WR, Weiner DE, Martin RJ. Timing of prednisone and alternations of airways inflammation in nocturnal asthma. Am Rev Respir Dis. 1992;146:1524–30.
Pincus DJ, Szefler SJ, Ackerson LM, Martin RJ. Chronotherapy of asthma with inhaled steroids: the effect of dosage timing on drug efficacy. J Allergy Clin Immunol. 1995;95:1172–8.
Buttgereit F, Mehta D, Kirwan J, et al. Low-dose prednisone chronotherapy for rheumatoid arthritis: a randomised clinical trial (CAPRA-2). Ann Rheum Dis. 2013;72:204–10.
Cutolo M, Iaccarino L, Doria A, et al. Efficacy of the switch to modified-release prednisone in rheumatoid arthritis patients treated with standard glucocorticoids. 2013;31:498–505.
Acknowledgments
Sponsorship for this study was funded by Horizon Pharma, Inc (formerly Nitec Pharma GmbH) Mannheim, Germany and Deerfield, Illinois, USA. Sponsorship and article processing charges for this study were funded by Horizon Pharma USA, Inc. The study was designed by M. Aubier, C. Knauer, and S. Witte; M. Aubier, C. Taillé, and L. Alavoine recruited patients to the study. Data were gathered and analyzed by Horizon Pharma, Inc (Mannheim, Germany). M. Aubier had full access to all the data in the study and takes responsibility for the integrity of the data and the accuracy of the analyses. All authors contributed to the interpretation of the data and were involved in the decision to publish. All named authors meet the International Committee of Medical Journal Editors (ICMJE) criteria for authorship for this manuscript, take responsibility for the integrity of the work as a whole, and have given final approval for the version to be published. The authors thank the patients and investigators who took part in this study. The authors take full responsibility for the content of the paper. Medical writing support, editorial assistance, and collation and incorporation of comments from all authors were provided by Dr. Diane Storey of Direct Publishing Solutions Ltd. and funded by Horizon Pharma, Inc.
Disclosures
M. Aubier, C. Taillé, and L. Alavoine report no conflict of interest. S. Witte was previously an employee of Horizon Pharma GmbH, Mannheim, Germany. C. Knauer, J. Kent, and J. Ball are presently employees of Horizon Pharma, Inc and report having stock options.
Compliance with ethics guidelines
All procedures followed were in accordance with the ethical standards of the responsible committee on human experimentation (institutional and national) and with the Helsinki Declaration of 1964, as revised in 2013. Informed consent was obtained from all patients for being included in the study.
Open Access
This article is distributed under the terms of the Creative Commons Attribution-NonCommercial 4.0 International License (http://creativecommons.org/licenses/by-nc/4.0/), which permits any noncommercial use, distribution, and reproduction in any medium, provided you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons license, and indicate if changes were made.
Author information
Authors and Affiliations
Corresponding author
Electronic supplementary material
Below is the link to the electronic supplementary material.
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution-NonCommercial 4.0 International License, which permits any non-commercial use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if changes were made. The images or other third party material in this article are included in the article's Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article's Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by-nc/4.0/.
About this article
Cite this article
Alavoine, L., Taillé, C., Ball, J. et al. Nocturnal Asthma: Proof-of-Concept Open-Label Study with Delayed-Release Prednisone. Pulm Ther 1, 43–52 (2015). https://doi.org/10.1007/s41030-015-0001-z
Received:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s41030-015-0001-z