Abstract
Background
Observational studies have shown that matrix metalloproteinases (MMPs) are associated with sepsis. However, it is unknown whether this association represents a causal relationship.
Methods
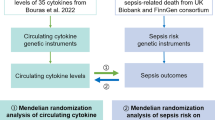
Mendelian randomization (MR) analysis was conducted to assess the potential causal role of circulating MMPs in sepsis. Single nucleotide polymorphisms (SNPs) associated with circulating MMPs levels were used as instrumental variables (IVs). In a sepsis genome-wide association study comprising 1573 cases and 454,775 European ancestry controls, we examined these IVs' effects using a two-sample MR study. Causal estimates were calculated using inverse variance weighting (IVW), the weighted median method, and MR-Egger analysis.
Results
Genetically predict that MMP-1 (OR = 1.011, 95% CI 0.772–1.325, p = 0.936), MMP-3 (OR = 1.036, 95% CI 0.862–1.244, p = 0.707), MMP-7 (OR = 1.206, 95% CI 0.960–1.515, p = 0.108), MMP-8 (OR = 1.041, 95% CI 0.949–1.144, p = 0.395), MMP-9 (OR = 1.101, 95% CI 0.831–1.458, p = 0.503), MMP-10 (OR = 1.028, 95% CI 0.840–1.260, p = 0.789) was not associated with the risk of sepsis.
Conclusions
The MR study does not provide evidence that circulating levels of MMPs (1, 3, 7, 8, 9, 10) were the causes of sepsis.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
1 Introduction
Sepsis is a condition where the host's dysregulated response to infection leading to life-threatening organ dysfunction [1]. Sepsis is a significant global health concern, with approximately 50 million cases occurring each year, and is the first cause of death among critically ill patients [2]. Matrix metalloproteinases (MMPs) are enzymes that require zinc to function and are involved in degrading and reactivating the extracellular matrix. The biological processes facilitated by MMPs include cell proliferation, differentiation, adhesion, angiogenesis, apoptosis, and inflammation [3, 4].
Studies on MMPs in sepsis have been extensively published [5]. Sepsis patients have higher circulating levels of MMP-1 and a decreased survival rate [6]. It is found that humans and mice deficient in both MMP-8 and tumor necrosis factor receptor 1 were more likely to survive in sepsis, and plasma MMP-8 was positively correlated with sequential organ failure assessment scores and interleukin-6(IL-6) [7]. Some observational studies have shown that MMP-9 is upregulated during septic shock, thereby causing thrombocytopenia [8] and reduced MMP-9/tissue inhibitor of metalloproteinase-1(TIMP-1) ratio may lead to multi-organ dysfunction [9]. The results of these studies confirm the importance of MMPs in sepsis, considering them as promising biomarkers for diagnosis.
Furthermore, such correlative evidence indicates that MMPs are associated with the risk of developing sepsis, but the causality cannot be established from observational studies. In light of the lack of randomized clinical trials (RCTs), to objectively test whether MMPs play a role in the development of sepsis, Mendelian randomization (MR) methods are employed to test causality. In MR, the effect of exposure (MMPs) on sepsis risk is examined using a genetic instrumental variable [10]. Because the instrumental variable is randomly distributed at conception, it is not subject to confounding effects. A common genetic variant associated with MMPs in genome-wide association studies (GWASs) serves as an instrumental variable for measuring MMPs. We explored the causal risk of developing sepsis from a genetic perspective to providing a basis for further prevention and diagnosis.
2 Methods
2.1 Study Design
Two-sample MR was conducted using GWAS data. The MR approach was based on the following three assumptions [11] (Fig. 1): Assumption 1, the genetic variant selected as instrumental variable is associated with MMPs; Assumption 2, the genetic variant is not associated with any unmeasured confounders; Assumption 3, the genetic variant is associated with sepsis only through MMPs, not through other pathways.
2.2 Data Sources
Association data for MMPs is compiled from the GWAS Catalog (https://www.ebi.ac.uk/gwas/). Recently, a large-scale proteogenomic study of 5368 Europeans indicated genetic variants related to 1989 serum proteins and common diseases were associated with 4035 independent associations between 2091 serum proteins, 36% of which had never been reported before [12]. The GWAS data for MMP-8 (n = 5365) and MMP-9 (n = 5357) were selected as a source of exposure data. Furthermore, in the recent large-scale mapping of protein quantitative trait loci, circulating levels of MMPs were measured among 90 candidate biomarkers related to cardiovascular risk, including MMP-1 (n = 16,889), MMP-3 (n = 20,791), MMP-7 (n = 18,245), and MMP-10 (n = 16,933) [13]. Detailed links to the corresponding data sources are provided (Supplementary Table S1).
Likewise, the genetic susceptibility to sepsis was obtained from the GWAS Catalog (https://www.ebi.ac.uk/gwas/) A GLMM-based GWA tool, fastGWA-GLMM, was applied to the UKB data of 456,348 individuals, 11,842,647 variants, and 2989 binary traits and identified 259 rare variants associated with 75 traits, illustrating the use of imputed genotype data in a large cohort to identify rare variants for binary complex traits [14]. Sepsis cases were collected from the UK Biobank, which included 1573 sepsis cases, defined as explicit sepsis [2], and 454,775 control subjects. Data from sepsis are selected from the final summary data, and links to sources are provided (Supplementary Table S1). Since all data were derived from previously published GWASs, the study did not require ethical approval.
2.3 Genetic Variants
As for the exposure data, genetic variants with genome-wide association thresholds (p < 5.0 × 10–6) were selected as instrumental variables (IVs) and applied a clumping algorithm (r2 threshold = 0.001; kb = 10 mB) to eliminate linkage disequilibrium. Additionally, strongly correlated IVs were selected based on F-statistics > 10 (F-value calculation formula below) to satisfy the correlation assumption of MR analysis: variants are strongly correlated with exposure [15].
Beta is the effect size of the single-nucleotide polymorphisms (SNPs) of exposure; SE is the standard error of the SNP of exposure)
It was found that 7 SNPs were associated with MMP-1, 7 SNPs were associated with MMP-3, 4 SNPs were associated with MMP-7, 7 SNPs were associated with MMP-8, 3 SNPs were associated with MMP-9, and 6 SNPs were associated with MMP-10. The effect size was measured in the MMPs change of circulating concentration for each additional effect allele, as shown in Supplementary Table S2-7. No linkage disequilibrium was found between SNPs.
2.4 Statistical Analysis
Mendelian analysis was primarily performed using inverse variance weighting (IVW), which provides a combined causal estimate from each SNP. IVW is considered conventional MR since it is equivalent to a two-stage least squares or allele score analysis using individual-level data [16]. However, horizontal polymorphism and null IV can lead to biased IVW estimates, so two complementary methods were applied. The Weighted Median method will provide reliable effect estimates with less than half of the IVs invalid. Mendelian randomization-Egger (MR-Egger) analysis was used to evaluate the pleiotropy effects [11]. Similarly, sensitivity analyses were conducted to determine reliable results [17]. The results of MMPs and sepsis were first tested for heterogeneity and horizontal multiplicity, followed by a leave-one-out analysis computed the meta-effect of remaining SNPs through iterative culling of each SNP. Leave-one-out analysis demonstrated the robustness of the causal relationship between exposure and outcome.
The statistical analysis was performed using R software (version 4.2.1) and the "TwoSampleMR" package in Rstudio (version 0.5.6), and the overall estimates of IVW, MR-Egger, and Weighted median methods were performed using the "forestploter" package (version 0.2.6). A Bonferroni-corrected significance threshold of p = 0.05/6, but we prespecified a Bonferroni-corrected significance threshold of p = 0.008 to adjust for multiple testing with a view to six exposures. Associations with p values between 0.05 and 0.008 were considered suggestive evidence of a possible association.
3 Results
In the primary analysis, IVW was used to provide estimates of the causal relationship between MMPs and sepsis, indicating that MMP-1 (OR = 1.011, 95% CI 0.772–1.325, p = 0.936), MMP-3 (OR = 1.036, 95% CI 0.862–1.244, p = 0.707), MMP-7 (OR = 1.206, 95% CI 0.960–1.515, p = 0.108), MMP-8 (OR = 1.041, 95% CI 0.949–1.144, p = 0.395), MMP-9 (OR = 1.101, 95% CI 0.831–1.458, p = 0.503), MMP-10 (OR = 1.028, 95% CI 0.840–1.260, p = 0.789) were not significantly associated with the risk of sepsis.
MR-Egger's and the weighted median method's overall estimates were consistent with the IVW analysis (Table 1). Moreover, the sensitivity analysis revealed no horizontal pleiotropy or heterogeneity (Supplementary Table S8). After systematically eliminating SNP through the leave-one-out analysis, the outcomes show minimal alteration, demonstrating that no single variant influenced the association between MMPs (1, 3, 7, 8, 9, 10) and sepsis (Fig. 2).
4 Discussion
Genetic variants are used to assess whether a risk factor has a causal impact on an outcome in MR study. As far as we are aware, this is the first MR study to evaluate the effects of MMPs on the occurrence of sepsis. Consequently, the study found no causal relationship between MMPs (1, 3, 7, 8, 9, 10) and sepsis in Europeans. In other words, altered levels of circulating MMPs are unrelated to the development of sepsis.
MMPs could degrade all components of the extracellular matrix, thus facilitating cell migration within tissues and increasing the availability of growth factors bound to the matrix. Previous observational studies identified that elevated plasma levels of MMP-1, MMP-3, MMP-8, MMP-9, and MMP-10 were linked with the severity of sepsis and mortality in sepsis patients [18,19,20,21,22,23]. A prospective study noted that MMP-8 had an area under the ROC curve of 0.87 (95% CI 0.82–0.92) for the diagnosis of sepsis. MMP-9 had an area under the receiver operating characteristic (ROC) curve of 0.73 (95% CI 0.65–0.80) for detection of a non-septic state, and sepsis is associated with a higher plasma level of MMP-8 and MMP-9 [24]. Animal studies of sepsis discovered that reducing or inhibiting MMP-9 and MMP-8 was associated with improved survival and outcomes. MMP8 has therefore been considered a promising biomarker for treating sepsis [7, 25]. Therefore, MMPs have been widely recognized and studied as potential contributors to sepsis during the past decade. However, our results do not prove a causal relationship between MMPs and sepsis risk.
In addition, MMPs and sepsis have shown contradictory findings in published observational studies. Some studies showed that the circulating MMPs and TIMPs levels were not related to the risk of sepsis [24, 26] Furthermore, lipopolysaccharide administration causes the release of MMP-9 [27], and MMP-9 improves survival in patients with sepsis by mobilizing the bone marrow-derived endothelial progenitor cells that appear to assist in the neovascularization and endothelial repair of ischemic tissues [28, 29]. These studies support our findings that MMPs did not promote the occurrence of sepsis.
Several limitations have been identified in our study. First, we examined only a linear association between circulating MMPs (1, 3, 7, 8, 9, 10) and sepsis risk in the current MR study and did not find any evidence of a U-shaped relationship. Second, our study only examined the role of circulating MMPs and did not consider the role of intracellular MMPs in sepsis. Third, all the associated data for MMPs and sepsis were drawn from Europeans, so it is essential to exercise caution when applying these findings to Asian populations.
5 Conclusion
We did not find evidence of a causal relationship between circulating MMPs and sepsis to bolster the results of most previous observational studies. Previous studies have suggested that sepsis and MMPs may be connected, but confounding factors or reverse causality may also be at play. Sepsis and circulating MMPs require further research.
Data Availability Statement
The original contributions presented in the study are included in the article/Supplementary Material. If you have any more questions, please feel free to contact the corresponding author for further information.
References
Evans L, Rhodes A, Alhazzani W, Antonelli M, Coopersmith CM, French C, et al. Surviving sepsis campaign: international guidelines for management of sepsis and septic shock 2021. Intensive Care Med. 2021;47(11):1181–247. https://doi.org/10.1007/s00134-021-06506-y.
Rudd KE, Johnson SC, Agesa KM, Shackelford KA, Tsoi D, Kievlan DR, et al. Global, regional, and national sepsis incidence and mortality, 1990–2017: analysis for the global burden of disease study. Lancet. 2020;395(10219):200–11. https://doi.org/10.1016/s0140-6736(19)32989-7.
Vanlaere I, Libert C. Matrix metalloproteinases as drug targets in infections caused by gram-negative bacteria and in septic shock. Clin Microbiol Rev. 2009;22(2):224–39. https://doi.org/10.1128/cmr.00047-08. (Table of Contents).
Rodríguez D, Morrison CJ, Overall CM. Matrix metalloproteinases: what do they not do? New substrates and biological roles identified by murine models and proteomics. Biochim Biophys Acta. 2010;1803(1):39–54. https://doi.org/10.1016/j.bbamcr.2009.09.015.
Huang M, Cai S, Su J. The pathogenesis of sepsis and potential therapeutic targets. Int J Mol Sci. 2019. https://doi.org/10.3390/ijms20215376.
Vandenbroucke RE, Dejager L, Libert C. The first MMP in sepsis. EMBO Mol Med. 2011;3(7):367–9. https://doi.org/10.1002/emmm.201100146.
Steeland S, Van Ryckeghem S, Vandewalle J, Ballegeer M, Van Wonterghem E, Eggermont M, et al. Simultaneous inhibition of tumor necrosis factor receptor 1 and matrix metalloproteinase 8 completely protects against acute inflammation and sepsis. Crit Care Med. 2018;46(1):e67–75. https://doi.org/10.1097/CCM.0000000000002813.
Larkin CM, Hante NK, Breen EP, Tomaszewski KA, Eisele S, Radomski MW, et al. Role of matrix metalloproteinases 2 and 9, toll-like receptor 4 and platelet-leukocyte aggregate formation in sepsis-associated thrombocytopenia. PLoS ONE. 2018;13(5):e0196478. https://doi.org/10.1371/journal.pone.0196478.
Lorente L, Martin MM, Sole-Violan J, Blanquer J, Paramo JA. Matrix metalloproteinases and their inhibitors as biomarkers of severity in sepsis. Crit Care. 2010;14(1):402. https://doi.org/10.1186/cc8211.
Didelez V, Sheehan N. Mendelian randomization as an instrumental variable approach to causal inference. Stat Methods Med Res. 2007;16(4):309–30. https://doi.org/10.1177/0962280206077743.
Bowden J, Davey Smith G, Burgess S. Mendelian randomization with invalid instruments: effect estimation and bias detection through Egger regression. Int J Epidemiol. 2015;44(2):512–25. https://doi.org/10.1093/ije/dyv080.
Gudjonsson A, Gudmundsdottir V, Axelsson GT, Gudmundsson EF, Jonsson BG, Launer LJ, et al. A genome-wide association study of serum proteins reveals shared loci with common diseases. Nat Commun. 2022;13(1):480. https://doi.org/10.1038/s41467-021-27850-z.
Folkersen L, Gustafsson S, Wang Q, Hansen DH, Hedman ÅK, Schork A, et al. Genomic and drug target evaluation of 90 cardiovascular proteins in 30,931 individuals. Nat Metab. 2020;2(10):1135–48. https://doi.org/10.1038/s42255-020-00287-2.
Jiang L, Zheng Z, Fang H, Yang J. A generalized linear mixed model association tool for biobank-scale data. Nat Genet. 2021;53(11):1616–21. https://doi.org/10.1038/s41588-021-00954-4.
Hemani G, Zheng J, Elsworth B, Wade KH, Haberland V, Baird D, et al. The MR-Base platform supports systematic causal inference across the human phenome. Elife. 2018. https://doi.org/10.7554/eLife.34408.
Burgess S, Butterworth A, Thompson SG. Mendelian randomization analysis with multiple genetic variants using summarized data. Genet Epidemiol. 2013;37(7):658–65. https://doi.org/10.1002/gepi.21758.
Yavorska OO, Burgess S. MendelianRandomization: an R package for performing Mendelian randomization analyses using summarized data. Int J Epidemiol. 2017;46(6):1734–9. https://doi.org/10.1093/ije/dyx034.
Ricarte-Bratti JP, Brizuela NY, Jaime-Albarran N, Montrull HL. IL-6, MMP 3 and prognosis in previously healthy sepsis patients. Rev Fac Cien Med Univ Nac Cordoba. 2017;74(2):99–106.
Tressel SL, Kaneider NC, Kasuda S, Foley C, Koukos G, Austin K, et al. A matrix metalloprotease-PAR1 system regulates vascular integrity, systemic inflammation and death in sepsis. EMBO Mol Med. 2011;3(7):370–84. https://doi.org/10.1002/emmm.201100145.
Gäddnäs FP, Sutinen MM, Koskela M, Tervahartiala T, Sorsa T, Salo TA, et al. Matrix-metalloproteinase-2, -8 and -9 in serum and skin blister fluid in patients with severe sepsis. Crit Care. 2010;14(2):R49. https://doi.org/10.1186/cc8938.
Lorente L, Martín MM, Solé-Violán J, Blanquer J, Páramo JA. Matrix metalloproteinases and their inhibitors as biomarkers of severity in sepsis. Crit Care. 2010;14(1):402. https://doi.org/10.1186/cc8211.
Mühl D, Nagy B, Woth G, Falusi B, Bogár L, Weber G, et al. Dynamic changes of matrix metalloproteinases and their tissue inhibitors in severe sepsis. J Crit Care. 2011;26(6):550–5. https://doi.org/10.1016/j.jcrc.2011.02.011.
Yazdan-Ashoori P, Liaw P, Toltl L, Webb B, Kilmer G, Carter DE, et al. Elevated plasma matrix metalloproteinases and their tissue inhibitors in patients with severe sepsis. J Crit Care. 2011;26(6):556–65. https://doi.org/10.1016/j.jcrc.2011.01.008.
Martin G, Asensi V, Montes AH, Collazos J, Alvarez V, Carton JA, et al. Role of plasma matrix-metalloproteases (MMPs) and their polymorphisms (SNPs) in sepsis development and outcome in ICU patients. Sci Rep. 2014;4:5002. https://doi.org/10.1038/srep05002.
Lauhio A, Hästbacka J, Pettilä V, Tervahartiala T, Karlsson S, Varpula T, et al. Serum MMP-8, -9 and TIMP-1 in sepsis: high serum levels of MMP-8 and TIMP-1 are associated with fatal outcome in a multicentre, prospective cohort study. Hypothetical impact of tetracyclines. Pharmacol Res. 2011;64(6):590–4. https://doi.org/10.1016/j.phrs.2011.06.019.
Yassen KA, Galley HF, Webster NR. Matrix metalloproteinase-9 concentrations in critically ill patients. Anaesthesia. 2001;56(8):729–32. https://doi.org/10.1046/j.1365-2044.2001.02083.x.
Albert J, Radomski A, Soop A, Sollevi A, Frostell C, Radomski MW. Differential release of matrix metalloproteinase-9 and nitric oxide following infusion of endotoxin to human volunteers. Acta Anaesthesiol Scand. 2003;47(4):407–10. https://doi.org/10.1034/j.1399-6576.2003.00059.x.
Hristov M, Erl W, Weber PC. Endothelial progenitor cells: mobilization, differentiation, and homing. Arterioscler Thromb Vasc Biol. 2003;23(7):1185–9. https://doi.org/10.1161/01.Atv.0000073832.49290.B5.
Rafat N, Hanusch C, Brinkkoetter PT, Schulte J, Brade J, Zijlstra JG, et al. Increased circulating endothelial progenitor cells in septic patients: correlation with survival. Crit Care Med. 2007;35(7):1677–84. https://doi.org/10.1097/01.Ccm.0000269034.86817.59.
Acknowledgements
The authors are grateful to Dr Folkersen, Dr Salminen, Dr Jiang, et al. for making summary-level association statistics of MMPs and sepsis possible and accessible. We also want to acknowledge all participants and investigators in these studies.
Funding
This study was supported by funds from the National key research and development plan (2018YFC2001904), the National Science Foundation of China (Grant Nos. 81701958 and 81960357), Guizhou Provincial Science and Technology Projects (Qian Ke He Jichu[2020]1Y330, Qian Ke He Jichu-ZK[2022]Yiban 370).
Author information
Authors and Affiliations
Contributions
CZY contributed to the conceptualization and methodology of the study. HYB and DHH played a part in the data analysis and visualization of results. QFZ and CL contributed to the validation of results and data curation. CZY and XL participated in drafting and reviewing the main manuscript. All authors reviewed and approved the manuscript.
Corresponding author
Ethics declarations
Conflict of Interest
The authors have no competing interests to declare relevant to this article's content.
Consent for Publication
All individuals have individual rights that are not to be infringed. Individual participants in studies have, for example, the right to decide what happens to the (identifiable) personal data gathered, to what they have said during a study or an interview, as well as to any photograph that was taken. This is especially true concerning images of vulnerable people (e.g. minors, patients, refugees, etc.) or the use of images in sensitive contexts. In many instances authors will need to secure written consent before including images.
Ethics Approval
Two-sample MR was conducted using GWAS data. The study did not require ethical approval since all data were derived from summary statistics from previously published GWASs.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if changes were made. The images or other third party material in this article are included in the article's Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article's Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
Yang, C., Long, C., Zhang, Q. et al. Mendelian Randomization Study of the Relationship Between Serum Matrix Metalloproteinases and the Occurrence of Sepsis. Intensive Care Res 3, 215–220 (2023). https://doi.org/10.1007/s44231-023-00047-2
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s44231-023-00047-2