Abstract
Ultrasound (US), computed tomography (CT), and magnetic resonance imaging (MRI) have high diagnostic accuracy in the diagnosis of acute appendicitis. Nowadays imaging is part of the diagnostic algorithm of appendicitis and the advantages are demonstrated by the reduced negative appendectomies rates. US is the preferred first line imaging in acute appendicitis. The US diagnosis of complicated and uncomplicated appendicitis is well characterized by different signs but the paradigm of US to take in mind is that the non-visualization of the appendix cannot exclude acute appendicitis. In US, when the appendix is not visualized, or US is inconclusive, second-line imaging examination should be performed. The aims of this pictorial are 1. to illustrate the US signs of complicated and uncomplicated AA; 2. to describe the conditions in which other imaging modalities should be performed to reach a definitive diagnosis.
Similar content being viewed by others
Explore related subjects
Discover the latest articles, news and stories from top researchers in related subjects.Avoid common mistakes on your manuscript.
Introduction
The Acute Appendicitis (AA) diagnosis is assessed by combining clinical scores, laboratory data and imaging results [1, 2]. Clinical scores such as Adult Appendicitis Score, Appendicitis Inflammatory Response and RIPASA score identify patients with intermediate risk who need an imaging test to reach a diagnosis and are superior Modified Alvarado Score [3, 4]. Imaging significantly reduces the rate of negative appendicectomies in case of suspected AA. Ultrasonography (US), computed tomography (CT) and magnetic resonance imaging (MRI) are highly accurate for the diagnosis of AA [1, 2], but according to the WSES Jerusalem guidelines (2020), US examination should be the first-line imaging [5]. The combination of US findings with clinical and laboratory parameters improve diagnostic accuracy, but when clinical suspicious persist after an US examination with negative or inconclusive results, a second-line imaging examination should be performed: a US re-evaluation, a CT or a MRI. CT and MRI should be preferred in children and pregnant women, whereas CT is usually warranted in adults and non-cooperative patients [1, 6]. The decision, regarding which diagnostic test is the best, depends on local expertise, imager availability, patient sex and age, and clinical conditions [1, 7]. Appendiceal lumen obstruction has always been considered the trigger of acute appendicitis, or lymphoid hyperplasia in young patients. The appendix obstructed keeps secerning mucus that determines appendiceal dilatation and increase of endoluminal pressure that can lead to vascular parietal damage and consequent ischemia and perforation with periappendiceal infection [8, 9]. Recently microbiota has been suggested to play an important role in the development of appendicitis because of the increased incidence of Crohn’s disease, ulcerative colitis, and Clostridium difficile infection after appendectomy [9, 10]. Appendix is now considered important for intestinal homeostasis and appendicitis may act as a trigger event in the development of bowel inflammatory diseases [11].
The treatment of appendicitis is strictly correlated to the transmural extension of the disease and it is defined as complicated or uncomplicated. Non-operative management is performed in selected patients with uncomplicated forms of AA for these reasons a distinction between complicated and uncomplicated forms of is fundamental. Imaging guides the treatment and a recently proposed classification [12] describes five imaging pattern: normal appendix (type 0), non-visualized appendix (type X), uncomplicated AA (type 1), complicated AA without perforation (type 2), and complicated AA with perforation (type 3). Instead, the CT staging of appendicitis define four grades: I normal, II mild appendicitis, III appendicitis with localized peritonitis, IV perforated appendicitis [13]. The classification between complicated and uncomplicated appendicitis varies among scientific society and imaging modalities but the presence of an appendicolith is considered as an independent prognostic risk factor for treatment failure in NOM of uncomplicated AA [1, 14, 15]. The role of imaging in the scenarios of operative or non-operative management requires accurate distinction between complicated appendicitis with high risk of perforation and uncomplicated appendicitis [12].
US signs of uncomplicated and complicated AA
Ultrasound is highly accurate in the diagnosis of appendicitis although its accuracy is less than CT, it may be influenced by different factors and the expertise of the operator, intrabdominal fat and appendix position are the principal factors [16,17,18,19]. The diagnostic criteria of acute appendicitis are the same among different imaging modalities (US, CT, MRI), they are divided in primary and secondary findings. The primary signs are related to appendix alterations, meanwhile secondary signs are related to periappendiceal inflammation [5, 6, 20, 21]. During US, appendix can be imaged with both high resolution, high frequency linear array 7.5–10 MHz and curvilinear array 3.5–7.0 MHz. The first is usually preferred also per the excellent detailed information, although the curvilinear probe is usually the first utilized to avoid any satisfaction errors (other diseases mimicking appendicitis) [22], to better localize the cecum and the terminal ileum, and in obese patients.
Primary signs
During US, the appendix appears as a blind-ended peristaltic tubular structure. The diameter of normal appendix, when visualized, is less than 6 mm, the length is extremely variable [23, 24]. An appendiceal diameter > 6 mm on axial axis (serosa to serosa) under probe compression is considered a positive sign but it should not be considered alone but always in association with other signs because the appendix could be dilated by endoluminal material and not obstructed; the appendix is non-compressible although in case of perforation it may become compressible [25,26,27,28,29,30]. One clinical signs that should be considered is the positive McBurney Sign that is the pain evocated during the compression with the probe of the non-compressible appendix [28]. A parietal thickness > 3 mm (mucosa to serosa) is considered a pathological sign. Another sign related to wall appearance is the parietal stratification and its loss, with non-visualization of the mucosal surface and increased thickness of an hyperechogenic submucosa. With the progress of the inflammation, the hyperechogenic submucosa tends to present focal interruption due to the transmural progression of the disease indicting the presence of complicated appendicitis. In advanced complicate stages, the parietal wall can appear thinned and interrupted. The loss of normally echogenic submucosal layer is a uniquely helpful discriminator of complicated versus uncomplicated appendicitis [31]. Increased Doppler flow can be detected within the inflamed appendiceal wall, this sign is specific but has low sensitivity [9, 32]. The appendix might contain colonic material including gas or fluid. Endoluminal gas was considered an exclusion criterion of AA indicating appendix patency, although it is characteristic of gangrenous appendicitis [33]. Appendicolith has been considered as a characteristic sign of appendicitis, but its significance has been strongly remodulated because it is present in 4% of asymptomatic patients and in less of 50% of patients with AA. In symptomatic patients with appendicolith and other inflammatory changes of the appendix should be considered for an early appendicectomy even in absence of other complicated signs of appendicitis [34,35,36] (Figs. 1, 2).
Acute uncomplicated appendicitis (curvilinear probe in overweight patient). A 41-year-old female with right-sided abdominal pain. a Longitudinal scan of appendix. The appendix is recognized as a blind ended tubular structure (white arrow). Psoas muscle (*). b Axial view of the appendix. The wall is thickened with stratified appearance (target sign) with hyperechoic submucosa. The periappendiceal fat is hyperechoic and inhomogeneous simulating a mass effect around the appendix (*). c Axial view power Doppler evaluation. The vascular signal is increased within the appendiceal wall and into periappendiceal fat (arrow)
Acute uncomplicated appendicitis (linear probe). A 21-year-old female with leukocytosis and McBurney’s point tenderness. a Axial view. The appendix presents thickened and stratified wall. The submucosa is hyperechogenic (target sign). Periappendiceal fat is hyperechoic (fat stranding *). A small amount of free fluid is detectable (arrow). b At color Doppler evaluation, vascular signal is increased in the appendiceal wall
Secondary signs
Secondary signs are related to periappendiceal inflammation. Hyperechogenicity of periappendiceal fat, reactive lymph nodes, free fluid, abscess and thickening of peritoneum can be detected. Inflamed fat appears as echogenic thick zone around the appendix and sometimes it can present mass effect on adjacent structures [9, 12, 21, 28].
Free fluid can be assessed in the right lower quadrant, around the appendix but also between bowel loops. The terminal ileum can appear hypoperistaltic (sentinel loop) [37].
Uncomplicated and complicated appendicitis.
Differentiation between a complicated and uncomplicated AA is crucial for the correct management. The presence of an appendicolith is an independent prognostic risk factor for treatment failure in NOM of uncomplicated AA, in these cases, an early surgical approach is recommended [1, 35]. Focal interruption of submucosa layer indicates transmural progression of the inflammation progress and is consider a sign of complicated appendicitis such as interruption of the parietal wall (complicated without perforation) [31]. The presence of abscess or periappendiceal phlegmon indicated a complicate appendicitis with perforation. The role of the US in staging appendicitis is not accurately stated, although US can represent a definitive diagnostic modality in selected case. First, when appendix is completely visualized during US, intraluminal appendicolith can be detected and patients can be stratified. Moreover, the US can accurately identify wall discontinuity and focal defects that imply transmural extension of inflammatory process and perforation in complicated AA. Peri-appendicular abscesses and fluid collections are easily detected during US too, although in severe complicated forms, with larger fluid collection in the right lower quadrant, the cecal appendix may not be clearly recognizable anymore and a second line imaging technique is required. In spite of the high accuracy of CT and US in selected patients, no safe differentiation between uncomplicated and complicated forms can be made upon imaging alone. Hence, a combination of clinical scores, laboratory value (white blood cell count and C-reactive Protein), US, and CT findings are usually preferred to reach a correct diagnosis [13, 38] (Figs. 3, 4).
Complicated appendicitis with focal submucosal focal lesion. A 16-year-old male with right groin bulging and tenderness. B-mode ultrasound examination of complicated appendicitis (a, b). The increased diameter of the appendix (a, b) is associated with thickening of the periappendiceal fat stranding (b) (**), and focal wall discontinuity at the appendiceal tip (b). An intraluminal appendicolith is also detected (hyperechogenic linear spot at the appendiceal orifice) (white arrow)
Acute complicated appendicitis (linear probe). A 53-year-old male with RLQ pain and vomiting. US examination with linear probe. Longitudinal scan (a), the appendix appears markedly distended with linear hyperechoic endoluminal material representing an appendicolith. The periappendiceal fat is inhomogeneous, hyperechoic and pockets of fluid are detectable close to the appendix. Axial scan (b), the appendix shows thickened wall and multiple focal submucosa interruption
Acute appendicitis: when ultrasound is not enough
Despite the high accuracy of US, there are still some scenarios in which other imaging methods (CT or MRI) should be performed [1, 16]: (1) when the appendix is not clearly or completely visualized during US, (2) when the inflammatory changes involve the appendix and the other structures in the right lower quadrant, (3) when ultrasound detects “chaos in right lower quadrant”.
Scenario 1
During US, the appendix is not visualized or not completely visualized
One paradigm of US diagnosis of AA is that the lack of visualization of the appendix does not exclude AA. In case of inconclusive US, a second line imaging is required. In many of these cases, the appendix may be retrocecal or pelvic, being difficult to be displayed in US [28, 29]. Normal appendix in adults asymptomatic patients can be visualized during US in 50–71% of population and it is negatively influenced by intrabdominal fat [39,40,41], oppositively during CT and MRI, normal appendix is visualized in almost 80% of the population and are positively influenced by the presence of intrabdominal fat [41, 42]. It is important to underline this concept, because in case of clinical and laboratory suspicions of appendicitis, not only the non-visualization of the appendix cannot exclude appendicitis, moreover the appendix, also if normal, should be assessed completely in its length because inflammation can be distant from the orifice and can be limited to the tip (tip appendicitis) [9, 43] (Figs. 5, 6, 7).
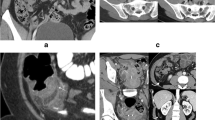
Appendix not visualized. A 55-year-old female with lower abdominal and right groin tenderness. During US, the appendix was not visualized. Because of clinical symptoms and high level of WBC, neutrophils and CRP a contrast-enhanced CT (a coronal, b axial) is performed. CT shows an enlarged (8 mm) retrocecal subhepatic appendicitis with globular periappendiceal fat stranding. In the lumen of the appendicitis there is a coprolite (arrow)
Appendix not clearly recognized. A 66-year-old male with epigastric abdominal pain and fever. a US examination with curvilinear probe. Positive Murphy’s US sign. Mass effect of hyperechogenic fat in the RLQ. An anechoic structure not better characterizable is appreciated within the inflamed fat, deep exploration and probe compression is not possible for severe pain and abdominal resistance. Second line imaging is required to characterize the inflammatory process in the RLQ. b–d Contrast-enhanced CT (b coronal, c, d axial) shows retrocecal appendicitis extending into the pelvis with globular periappendiceal fat stranding and focal thickening of the cecum at appendix orifice
Appendix is not completely visualized. A 52-year-old male with two weeks of diffuse abdominal pain. a, b US examination with curvilinear probe. Free fluid is detected in the RLQ, the terminal ileum is mildly dilated and fluid filled, the appendix is not visualized. c–e Contrast-enhanced CT (c, d coronal, e axial). CT contrast-enhanced (c, d coronal, e axial) shows retrocecal pelvic appendicitis (arrow) with periappendiceal fat stranding and b free fluid surrounding appendix (*). The appendix (arrow) is dilated with hyperemic wall. An appendicolith is recognizable within the lumen. Appendiceal wall is interrupted with abscess formation (e) (red arrow). The ileum is dilated, and fluid filled for peritonitis (sentinel bowel loop). Complicated appendicitis with perforation and abscess
Scenario 2
Too many inflammatory changes in the RLQ
Many non-surgical conditions may determine inflammatory changes in the right lower quadrant that do not originate in the appendix, but instead may be in the cecum or in the ileum or secondary to pelvic inflammatory disease such as cecal diverticulitis, epiploic appendicitis, omental infarction, infectious colitis, inflammatory bowel diseases, malignancies etc. These processes lead to secondary thickening and inflammation of the appendix (reactive appendicitis) and clinically present acute RLQ pain. A careful and accurate differential diagnosis should be made between surgical and non-surgical conditions and the appendix should be confidently individuated as the epicenter of the inflammation. US can be inaccurate and it requires high level of confidence and expertise. Therefore, when there are too many inflammatory changes in the RLQ that involve all the structures, secondary imaging is necessary to make a definitive diagnosis, and prevent erroneous management. Appendiceal involvement in Crohn’s disease may be observed and is commonly seen in combination with involvement of the terminal ileum and cecum [44]; thickening of the appendix and terminal ileum should alert radiologists to rule out the presence of Crohn’s disease [5], on the other hand, Crohn’s may manifest with firstly granulomatous appendiceal involvement [45, 46]. A misdiagnosis and surgical treatment of secondarily appendix inflammation in these patients may evolve in long-term post-surgical complications. Generally during US, the inflammatory changes are diffuse and the epicenter is not clearly identified in the appendix, radiologists should perform second line imaging to achieve a confident diagnosis to determine the cause and to stratify patients for surgical or - non-surgical management [47, 48] (Figs. 8, 9, 10).
Crohn disease. A 27-year-old female presented with 4 days of fever and diarrhea. a, b US examination with linear probe. Walls of the cecum (a) and the terminal ileum (b) are thickened with stratified appearance and thickened hyperechogenic submucosa layer. The appendix is enlarged (> 6 mm). c, d Contrast-enhanced CT (c coronal, d axial). Diffuse thickening and mural hyperenhancement of the ascending colon, cecum and terminal ileum. The appendix is visualized in a retrocecal position with thickened wall as a secondary involvement (reactive appendicitis) (arrow). A suspected diagnosis of bowel inflammatory disease is formulated, non-operative management is carried out and sequent Crohn’s disease is confirmed at the colonoscopy
Cecal diverticulum. A 51-year-old female with one-week history of RLQ pain. a, b US examination with linear probe. During US (a longitudinal), the fat around the cecum (*) is edematous and hyperechogenic and the cecum shows circumferential wall thickening. In the axial view axial (b) there is an out pouching from the lateral cecum wall that shows hyperechoic internal foci and shadowing. The appendix is not visualized. c–e Contrast-enhanced CT. At CT-enhanced fat stranding surrounds the cecum and a cecal diverticulum, with mixed endoluminal content. Other non-inflamed cecal diverticula are detected. The appendix is retrocecal with medial course and appears normal for caliber and walls
Appendiceal cancer. A 68-year-old male with acute RLQ pain. a US examination with linear probe. During US an irregular thickening of the cecum, with a mass-like appearance is detected. The margins are spiculated and there is pericecal fat stranding with a small amount of free fluid. During US, hepatic lesions are detected (b). c–e Contrast-enhanced CT. CT coronal (c) and axial (d, e) images show multiple metastatic liver lesion (c) with eccentric thickening of the cecum with stranding and spiculation on the adjacent fat. The presence also of liver metastasis and pathological thickening of the cecum suggest a malignant lesion of the cecum with metastatic liver disease
Scenario 3
The “chaos” in right lower quadrant
Severe inflammatory changes in the right lower quadrant may determine difficulties in the recognition during US of anatomical structures. Fluid collections and involvement of adjacent organs behind the appendix cannot be localized accurately during US. In these cases, second line imaging is required to determine the cause, the extension and structure involvement in the inflammatory process. Although ultrasound may be diagnostic in assessing the presence of an inflammatory process in the RLQ, it cannot be sufficient in determining the cause and the extension. Second line imaging such as CT or MRI, in stable and selected patients, are necessary to define the cause and involvement of RLQ and pelvic structures (Fig. 11).
The chaos in right lower quadrant. A 52-year-old female with acute onset pelvic pain. a US examination with curvilinear probe. During US (a) severe inflammatory changes are detected in the right lower quadrant extending into the pelvis. Fluid collection is appreciated around the cecum, the ileocecal valve, the appendix (that is not clearly visualized) and the salpinges. Positive Murphy’s US sign. b, c Contrast-enhanced CT (b coronal, c axial). At contrast enhanced CT severe inflammatory changes are detected around the cecum, ileocecal valve, appendix and right salpinx; the appendix is not clearly visualized. At histology severe inflammatory is detected and the origins of inflammatory cannot be identified: cecum, terminal ileum, appendix and right salpinx are equally involved, and the origin of the inflammatory process is not assessed
Conclusion
A multidisciplinary approach involving clinical assessment, scoring systems, and appropriate imaging is essential for accurate diagnosis and optimal patient care in suspected acute appendicitis. Each component of this approach contributes to overall diagnostic accuracy and helps healthcare professionals for the correct management. Nowadays, appendicitis management can be operative or non-operative, this approach is also sustained by the emerging immune and homeostatic role of the appendix. Discriminating between complicated and non-complicated appendicitis is necessary, but imaging alone cannot be accurate and imaging findings need to be always correlated to laboratory test and clinical picture. The US should be the first imaging modality to approach patients with suspected appendicitis, but the non-visualization or non-complete visualization of the appendix do not exclude appendicitis. Furthermore, there are different scenarios that require a second line imaging: when the appendix is non visualized, when there are too many inflammatory changes or parietal thickening of cecum and ileum, and when the inflammatory process is extremely severe determining the chaos in the RLQ.
References
Di Saverio S, Podda M, De Simone B, Ceresoli M, Augustin G, Gori A, Boermeester M, Sartelli M, Coccolini F, Tarasconi A et al (2020) Diagnosis and treatment of acute appendicitis: 2020 update of the WSES Jerusalem guidelines. World J Emerg Surg 15(1):27
Eng KA, Abadeh A, Ligocki C, Lee YK, Moineddin R, Adams-Webber T, Schuh S, Doria AS (2018) Acute Appendicitis: A Meta-Analysis of the Diagnostic Accuracy of US, CT, and MRI as Second-Line Imaging Tests after an Initial US. Radiology 288(3):717–727
Chisthi MM, Surendran A, Narayanan JT (2020) RIPASA and air scoring systems are superior to alvarado scoring in acute appendicitis: Diagnostic accuracy study. Ann Med Surg (Lond) 59:138–142
Scott AJ, Mason SE, Arunakirinathan M, Reissis Y, Kinross JM, Smith JJ (2015) Risk stratification by the Appendicitis Inflammatory Response score to guide decision-making in patients with suspected appendicitis. Br J Surg 102(5):563–572
Dirks K, Calabrese E, Dietrich CF, Gilja OH, Hausken T, Higginson A, Hollerweger A, Maconi G, Maaser C, Nuernberg D et al (2019) EFSUMB Position Paper: Recommendations for Gastrointestinal Ultrasound (GIUS) in Acute Appendicitis and Diverticulitis. Ultraschall Med 40(2):163–175
Mostbeck G, Adam EJ, Nielsen MB, Claudon M, Clevert D, Nicolau C, Nyhsen C, Owens CM (2016) How to diagnose acute appendicitis: ultrasound first. Insights Imaging 7(2):255–263
Aspelund G, Fingeret A, Gross E, Kessler D, Keung C, Thirumoorthi A, Oh PS, Behr G, Chen S, Lampl B et al (2014) Ultrasonography/MRI versus CT for diagnosing appendicitis. Pediatrics 133(4):586–593
Bhangu A, Soreide K, Di Saverio S, Assarsson JH, Drake FT (2015) Acute appendicitis: modern understanding of pathogenesis, diagnosis, and management. Lancet 386(10000):1278–1287
Borruel Nacenta S, Ibanez Sanz L, Sanz Lucas R, Depetris MA, Martinez Chamorro E (2023) Update on acute appendicitis: Typical and untypical findings. Radiologia (Engl Ed) 65(Suppl 1):S81–S91
Clanton J, Subichin M, Drolshagen K, Daley T, Firstenberg MS (2013) Fulminant Clostridium difficile infection: An association with prior appendectomy? World J Gastrointest Surg 5(8):233–238
Zhang L, Hu C, Zhang Z, Liu R, Liu G, Xue D, Wang Z, Wu C, Wu X, She J et al (2023) Association between prior appendectomy and the risk and course of Crohn’s disease: A systematic review and meta-analysis. Clin Res Hepatol Gastroenterol 47(3):102090
Hoffmann JC, Trimborn CP, Hoffmann M, Schroder R, Forster S, Dirks K, Tannapfel A, Anthuber M, Hollerweger A (2021) Classification of acute appendicitis (CAA): treatment directed new classification based on imaging (ultrasound, computed tomography) and pathology. Int J Colorectal Dis 36(11):2347–2360
Kim HC, Yang DM, Lee CM, Jin W, Nam DH, Song JY, Kim JY (2011) Acute appendicitis: relationships between CT-determined severities and serum white blood cell counts and C-reactive protein levels. Br J Radiol 84(1008):1115–1120
Kus CC, Ilgin C, Yegen C, Demirbas BT, Tuney D (2022) The role of CT in decision for acute appendicitis treatment. Diagn Interv Radiol 28(6):540–546
Gorter RR, Eker HH, Gorter-Stam MA, Abis GS, Acharya A, Ankersmit M, Antoniou SA, Arolfo S, Babic B, Boni L et al: Diagnosis and management of acute appendicitis. EAES consensus development conference 2015. Surg Endosc 2016, 30(11):4668–4690.
Terasawa T, Blackmore CC, Bent S, Kohlwes RJ (2004) Systematic review: computed tomography and ultrasonography to detect acute appendicitis in adults and adolescents. Ann Intern Med 141(7):537–546
Karul M, Berliner C, Keller S, Tsui TY, Yamamura J (2014) Imaging of appendicitis in adults. Rofo 186(6):551–558
Tyler PD, Carey J, Stashko E, Levenson RB, Shapiro NI, Rosen CL (2019) The Potential Role of Ultrasound in the Work-up of Appendicitis in the Emergency Department. J Emerg Med 56(2):191–196
Harel S, Mallon M, Langston J, Blutstein R, Kassutto Z, Gaughan J (2022) Factors Contributing to Nonvisualization of the Appendix on Ultrasound in Children With Suspected Appendicitis. Pediatr Emerg Care 38(2):e678–e682
Reddan T, Corness J, Mengersen K, Harden F (2016) Ultrasound of paediatric appendicitis and its secondary sonographic signs: providing a more meaningful finding. J Med Radiat Sci 63(1):59–66
Monsonis B, Mandoul C, Millet I, Taourel P (2020) Imaging of appendicitis: Tips and tricks. Eur J Radiol 130:109165
Rogers LF (2000) Keep looking: satisfaction of search. AJR Am J Roentgenol 175(2):287
Group L: Low-dose CT for the diagnosis of appendicitis in adolescents and young adults (LOCAT): A pragmatic, multicentre, randomised controlled non-inferiority trial. . Lancet Gastroenterol Hepatol 2017:793–804.799.
Kessler N, Cyteval C, Gallix B, Lesnik A, Blayac PM, Pujol J, Bruel JM, Taourel P (2004) Appendicitis: evaluation of sensitivity, specificity, and predictive values of US, Doppler US, and laboratory findings. Radiology 230(2):472–478
Chicaiza HP, Malia L, Mulvey CH, Smith SR (2018) Revisiting the Appendiceal Diameter via Ultrasound for the Diagnosis of Acute Appendicitis. Pediatr Emerg Care 34(11):757–760
Jeffrey RB, Jain KA, Nghiem HV (1994) Sonographic diagnosis of acute appendicitis: interpretive pitfalls. AJR Am J Roentgenol 162(1):55–59
Trout AT, Towbin AJ, Fierke SR, Zhang B, Larson DB (2015) Appendiceal diameter as a predictor of appendicitis in children: improved diagnosis with three diagnostic categories derived from a logistic predictive model. Eur Radiol 25(8):2231–2238
Kadasne R, Sabih DE, Puri G, Sabih Q (2021) Sonographic diagnosis of appendicitis: A pictorial essay and a new diagnostic maneuver. J Clin Ultrasound 49(8):847–859
Tamburrini S, Brunetti A, Brown M, Sirlin CB, Casola G (2005) CT appearance of the normal appendix in adults. Eur Radiol 15(10):2096–2103
Yaqoob J, Idris M, Alam MS, Kashif N (2014) Can outer-to-outer diameter be used alone in diagnosing appendicitis on 128-slice MDCT? World J Radiol 6(12):913–918
Xu Y, Jeffrey RB, Chang ST, DiMaio MA, Olcott EW (2017) Sonographic Differentiation of Complicated From Uncomplicated Appendicitis: Implications for Antibiotics-First Therapy. J Ultrasound Med 36(2):269–277
Gaitini D, Beck-Razi N, Mor-Yosef D, Fischer D, Ben Itzhak O, Krausz MM, Engel A (2008) Diagnosing acute appendicitis in adults: accuracy of color Doppler sonography and MDCT compared with surgery and clinical follow-up. AJR Am J Roentgenol 190(5):1300–1306
Ip C, Wang EH, Croft M, Lim W (2021) Appendiceal Intraluminal Gas: A CT Marker for Gangrenous Appendicitis. Radiol Res Pract 2021:7191348
Ranieri DM, Enzerra MD, Pickhardt PJ (2021) Prevalence of Appendicoliths Detected at CT in Adults With Suspected Appendicitis. AJR Am J Roentgenol 216(3):677–682
Taib AG, Kler A, Prayle M, Kanakalingam D, Fani M, Asaad P: Appendicolith appendicitis: should we be operating sooner? A retrospective cohort study. Ann R Coll Surg Engl 2023.
Mallinen J, Vaarala S, Makinen M, Lietzen E, Gronroos J, Ohtonen P, Rautio T, Salminen P (2019) Appendicolith appendicitis is clinically complicated acute appendicitis-is it histopathologically different from uncomplicated acute appendicitis. Int J Colorectal Dis 34(8):1393–1400
Ali N, Leshchinskiy S, Johnson M, D’Agostino R (2018) The sentinel loop sign. Abdom Radiol (NY) 43(11):3192–3194
Foley WD (2018) CT Features for Complicated versus Uncomplicated Appendicitis: What Is the Evidence? Radiology 287(1):116–118
Yabunaka K, Katsuda T, Sanada S, Fukutomi T: Sonographic appearance of the normal appendix in adults. J Ultrasound Med 2007, 26(1):37–43; quiz 45–36.
Hamid MA, Afroz R, Ahmed UN, Bawani A, Khan D, Shahab R, Salim A (2020) The importance of visualization of appendix on abdominal ultrasound for the diagnosis of appendicitis in children: A quality assessment review. World J Emerg Med 11(3):140–144
Kim DW, Suh CH, Yoon HM, Kim JR, Jung AY, Lee JS, Cho YA (2018) Visibility of Normal Appendix on CT, MRI, and Sonography: A Systematic Review and Meta-Analysis. AJR Am J Roentgenol 211(3):W140–W150
Benjaminov O, Atri M, Hamilton P, Rappaport D (2002) Frequency of visualization and thickness of normal appendix at nonenhanced helical CT. Radiology 225(2):400–406
Mazeh H, Epelboym I, Reinherz J, Greenstein AJ, Divino CM (2009) Tip appendicitis: clinical implications and management. Am J Surg 197(2):211–215
Ripolles T, Martinez MJ, Morote V, Errando J (2006) Appendiceal involvement in Crohn’s disease: gray-scale sonography and color Doppler flow features. AJR Am J Roentgenol 186(4):1071–1078
Otsuka R, Shinoto K, Okazaki Y, Sato K, Hirano A, Isozaki T, Tamachi T, Hirai T, Yonemoto S, Matsubara H (2019) Crohn’s Disease Presenting as Granulomatous Appendicitis. Case Rep Gastroenterol 13(3):398–402
Mostyka M, Fulmer CG, Hissong EM, Yantiss RK (2021) Crohn Disease Infrequently Affects the Appendix and Rarely Causes Granulomatous Appendicitis. Am J Surg Pathol 45(12):1703–1706
Tamburrini S, Setola FR, Belfiore MP, Saturnino PP, Della Casa MG, Sarti G, Abete R, Marano I (2019) Ultrasound diagnosis of typhlitis. J Ultrasound 22(1):103–106
Tamburrini S, Consoli L, Garrone M, Sfuncia G, Lugara M, Coppola MG, Piccirillo M, Toto R, Stella SM, Sofia S et al (2022) The “Black Pattern”, a Simplified Ultrasound Approach to Non-Traumatic Abdominal Emergencies. Tomography 8(2):798–814
Funding
None to report.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no known competing financial interests or personal relationships that could have appeared to influence the work reported in this paper.
Informed consent
Written informed consent was obtained from the patient for publication of this case report and accompanying images.
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if changes were made. The images or other third party material in this article are included in the article's Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article's Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
Comune, R., Tamburrini, S., Durante, A. et al. Ultrasonography (US) examination of acute appendicitis (AA): diagnosis of complicated and uncomplicated forms and when US is not enough. J Med Imaging Intervent Radiol 11, 14 (2024). https://doi.org/10.1007/s44326-024-00002-5
Received:
Accepted:
Published:
DOI: https://doi.org/10.1007/s44326-024-00002-5