Abstract
Presynaptic increase in striatal dopamine is the primary dopaminergic abnormality in schizophrenia, but the underlying mechanisms are not understood. Here, we hypothesized that increased expression of endogenous GDNF could induce dopaminergic abnormalities that resemble those seen in schizophrenia. To test the impact of GDNF elevation, without inducing adverse effects caused by ectopic overexpression, we developed a novel in vivo approach to conditionally increase endogenous GDNF expression. We found that a 2–3-fold increase in endogenous GDNF in the brain was sufficient to induce molecular, cellular, and functional changes in dopamine signalling in the striatum and prefrontal cortex, including increased striatal presynaptic dopamine levels and reduction of dopamine in prefrontal cortex. Mechanistically, we identified adenosine A2a receptor (A2AR), a G-protein coupled receptor that modulates dopaminergic signalling, as a possible mediator of GDNF-driven dopaminergic abnormalities. We further showed that pharmacological inhibition of A2AR with istradefylline partially normalised striatal GDNF and striatal and cortical dopamine levels in mice. Lastly, we found that GDNF levels are increased in the cerebrospinal fluid of first episode psychosis patients, and in post-mortem striatum of schizophrenia patients. Our results reveal a possible contributor for increased striatal dopamine signalling in a subgroup of schizophrenia patients and suggest that GDNF—A2AR crosstalk may regulate dopamine function in a therapeutically targetable manner.
Similar content being viewed by others
Introduction
Schizophrenia is a debilitating neuropsychiatric disease affecting 1% of the global population. The clinical features of schizophrenia include positive, negative, and cognitive symptoms, and at least some of these clinical manifestations are thought to reflect neurochemical disturbances, such as abnormalities in dopamine, glutamate, serotonin, adenosine, and gamma-aminobutyric acid signalling [1,2,3,4,5]. Among the various abnormalities observed in individuals with schizophrenia, dysfunctional dopamine signalling is a commonly reported pathology [6]. Recent studies suggest that in patients with disturbed dopamine signalling, increased presynaptic dopamine synthesis capacity and release in the nigrostriatal dopamine pathway are the primary dopaminergic abnormalities [7,8,9,10]. In addition, striatal hyperdopaminergia is associated with reduced dopamine function in the prefrontal cortex (PFC) [11,12,13]. However, there are currently no animal models showing that increased presynaptic function in the striatum can drive other schizophrenia-like phenotypes, including the cortical hypodopaminergia. As a result, we have limited understanding of the underlying mechanisms driving these abnormalities, and of possible treatment strategies.
Glial cell line-neurotrophic factor (GDNF) is a secreted protein expressed predominantly in striatal interneurons [14]. GDNF is a potent neurotrophic factor for midbrain dopamine neurons in culture [15] and promotes dopamine synthesis and dopaminergic neuron fibre outgrowth if applied ectopically into the brain in animal models and humans [16,17,18,19,20]. Furthermore, amphetamine, a drug that increases synaptic dopamine levels and is associated with increased susceptibility to developing schizophrenia [21,22,23,24,25,26,27,28], increases endogenous GDNF expression in the nigrostriatal tract [21, 24], and a two-fold increase in endogenous GDNF levels is sufficient to increase striatal dopamine synthesis and release in mice [29]. Despite these multiple lines of suggestive evidence, functional analysis linking GDNF signalling to schizophrenia is currently lacking.
We and others have shown that ectopic gene overexpression in highly structured tissues, including the brain, can induce side-effects and artefacts, yielding results that are difficult to interpret [29,30,31,32,33,34,35,36,37,38,39,40]. These findings have suggested that retaining the physiological gene expression pattern and levels is particularly important for studying the function of morphogens such as GDNF. We recently showed that Gdnf 3'UTR contains negative regulation elements and that the replacement of Gdnf 3'UTR with a 3'UTR less responsive to negative regulation enhances GDNF expression by about 2–3-fold at the post-transcriptional level, limited to cells that normally express GDNF [29].
Here, we generate a novel mouse model allowing us to conditionally upregulate endogenous GDNF. We find that increased levels of GDNF are sufficient to induce altered dopamine signalling, including striatal hyperdopaminergia and cortical hypodopaminergia, as well as behavioural deficits and gene expression alterations similar to individuals with schizophrenia. We then identify A2AR as a possible therapeutic target and show that administration of specific A2AR antagonist istradefylline partially normalises striatal and cortical dopamine levels in mice. Lastly, we find that GDNF levels are increased in the cerebrospinal fluid (CSF) of first episode psychosis (FEP) patients and in post-mortem striata of schizophrenia patients. Thus, our work demonstrates that 2–3-fold elevation in endogenous GDNF expression increases striatal presynaptic dopaminergic signalling and induces hypodopaminergia in prefrontal cortex in mice and suggests that elevated GDNF could contribute to the disease in a subgroup of patients with elevated GDNF levels. Our data also suggests A2AR as a potential drug target in a subgroup of schizophrenia patients with elevated GDNF.
Results
Generation of Gdnf conditional hypermorph allele
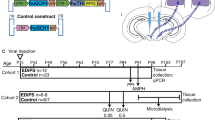
GDNF is a neurotrophic factor expressed in striatal interneurons that stimulate dopamine signalling in the nigrostriatal dopamine pathway [14,15,16, 20, 29]. At the same time, increased dopamine synthesis capacity and release in dorsal striatum have been associated with psychosis in schizophrenia patients [8]. We asked whether elevated endogenous GDNF expression in mice is sufficient to induce striatal hyperdopaminergia and other schizophrenia-associated changes in the brain. To avoid ectopic GDNF overexpression related developmental defects [29, 41,42,43,44,45], we generated a novel conditional hypermorph allele enabling an increase in the endogenous, spatially unaltered expression of GDNF in a temporally controlled manner using the Cre-Lox system (Gdnf conditional hypermorphic mice, Gdnf cHyper). To that end, we inserted a FLEx cassette [46] containing the bovine growth hormone polyadenylation sequence (bGHpA; a 3'UTR sequence previously shown to lead to increased expression from the cognate mRNA [47]) in an inverted orientation immediately downstream of the stop codon of the mouse Gdnf gene (Fig. 1A and Supplementary Fig. S1A, B). Based on our previous work on Gdnf 3'UTR [29], we hypothesised that by affecting only post-transcriptional regulation, Cre-mediated recombination would result in increased Gdnf expression without changing Gdnf’s expression pattern (Fig. 1B).
A Schematic of the Gdnf cHyper allele (top panel) and the resulting mRNA carrying a short 3'UTR (bottom panel) devoid of negative regulation elements in the 3'UTR. pA, polyadenylation signal. B Schematic of the conditional gene upregulation strategy to elevate endogenous gene expression in natively expressing cells. When using the conditional hypermorph allele, Cre-mediated recombination would result in an elevated gene expression specifically in cells that normally express the gene. C Striatal Gdnf mRNA levels in adult Gdnf cHyper;Nestin-Cre mice, measured with qPCR. Box plots show median, upper, and lower quartiles, as well as maximum and minimum values. N = 7–17 mice per group. One-way ANOVA, Tukey’s multiple comparisons test. ***p < 0.001. D Total tissue dopamine levels in the striatum, measured with HPLC. Box plots show median, upper, and lower quartiles, as well as maximum and minimum values. N = 4–10 mice per group. One-way ANOVA, Tukey’s multiple comparisons test. *p < 0.05. E Total tissue dopamine levels in the substantia nigra, measured with HPLC. Box plots show median, upper, and lower quartiles, as well as maximum and minimum values. N = 5–10 mice per group. One-way ANOVA, Tukey’s multiple comparisons test. *p < 0.05. F Gdnf mRNA expression pattern in dorsal striatum, detected using RNAscope probes. Arrows indicate cells with high Gdnf signal. Scale bar 50 µm (d, left panels) or 10 µm (d, right panels, higher magnification). G Stimulated dopamine release in striatal slices across four consecutive stimulations, measured with fast-scan cyclic voltammetry. Mean ± SEM. n = 10–20 striatal slices (from N = 4–8 mice) per group. Two-way repeated measures ANOVA, Tukey’s multiple comparisons test. *p < 0.05; **p < 0.01 between cHyper/cHyper +Cre and wt/wt +Cre. H Similar to (G) but showing dopamine re-uptake. Mean ± SEM. n = 10–20 striatal slices (from N = 4–8 mice) per group. Two-way repeated measures ANOVA, Tukey’s multiple comparisons test. #p < 0.05 between wt/cHyper +Cre and wt/wt +Cre.
To verify endogenous GDNF overexpression in Gdnf cHyper mice, we first analysed the kidneys, where Gdnf expression pattern and the outcome of Gdnf gene level alterations are well characterised. Mice lacking GDNF have no kidneys [41,42,43], whereas constitutive endogenous GDNF overexpression causes a reduction in kidney size and other histological alterations [29, 44, 45]. In line with these studies, crossing Gdnf cHyper mice to a Pgk1-Cre line, where Cre expression results in ubiquitous recombination [48], resulted in increased Gdnf mRNA and GDNF protein expression and reduced kidney size (Supplementary Fig. S1C–E). Similarly, crossing Gdnf cHyper mice to a tamoxifen-inducible Esr1-Cre line [49] increased Gdnf mRNA expression in embryonic kidneys after tamoxifen administration to pregnant females, while retaining the developmental stage-appropriate expression pattern of Gdnf (Supplementary Fig. S1F, G). These results demonstrate that, as hypothesised, the Gdnf cHyper allele enables temporally controlled increase of endogenous Gdnf without altering its expression pattern.
Increased endogenous GDNF levels increase striatal dopamine function
Next, we addressed how CNS-specific overexpression of GDNF affects striatal dopamine function. We crossed Gdnf cHyper mice to a Nestin-Cre line, where Cre is expressed specifically in the CNS during mid-gestation (E11.5 onwards) [50]. In the nigrostriatal system, GDNF is mostly produced by a sparse and regularly spaced population of striatal parvalbumin interneurons [14] that regulate striatal output [51]. We found that Gdnf mRNA and GDNF protein levels were increased in an allele dose-dependent manner in the striatum of 2-month-old Gdnf cHyper;Nestin-Cre mice (Fig. 1C and Supplementary Fig. S1H), whereas Gdnf’s expression pattern remained normal (Fig. 1F). We then found that Nestin-Cre-driven elevation of endogenous GDNF significantly increased the levels of total tissue dopamine in the striatum and substantia nigra (SN) (Fig. 1D, E). In addition, fast-scan cyclic voltammetry (FSCV) experiments, measuring the kinetics of phasic dopamine release and re-uptake in acute brain slices, demonstrated increased dopamine release and re-uptake in the striatum (Fig. 1G, H). The tissue levels of dopamine metabolites 3,4-dihydroxyphenylacetic acid (DOPAC) and homovanillic acid (HVA) in the striatum and SN were not altered (Supplementary Fig. S1I, J), and the total number of dopaminergic neurons in the SN was normal (Supplementary Fig. S1K). Altogether, these results demonstrated that developmental upregulation of endogenous GDNF in Gdnf cHyper;Nestin-Cre mice at mid-gestation results in increased striatal presynaptic dopamine function.
Increased endogenous GDNF levels reduce dopamine signalling in the PFC
Studies on schizophrenia patients suggest that increased striatal dopamine signalling associates with reduced dopamine signalling in the PFC [7, 12, 52,53,54]. Therefore, we asked if increased dopaminergic signalling in the striatum is associated with a cortical hypodopaminergia in Gdnf cHyper;Nestin-Cre mice. We found a marked reduction in PFC dopamine levels in both Gdnf wt/cHyper;Nestin-Cre and Gdnf cHyper/cHyper;Nestin-Cre mice compared with controls (Fig. 2A), while the levels of DOPAC and HVA remained unchanged (Supplementary Fig. S2A, B). We next analysed dopamine signalling in the ventral tegmental area (VTA) using FSCV recordings in the VTA subregion that gives rise to the mesocortical dopamine fibres innervating the PFC [55]. We found a substantial decrease in somatodendritic dopamine release and reuptake (Fig. 2B, C), suggesting that dopaminergic signalling is reduced in the mesocortical pathway. Further analysis at the cellular level revealed a reduced number of dopamine transporter-positive (DAT+) dopaminergic synaptic boutons in the medial PFC and in the association cortex in Gdnf cHyper/cHyper;Nestin-Cre mice compared with controls (Fig. 2D, E, Supplementary Fig. S2C, D), in line with reduced PFC dopaminergic innervation observed in post-mortem samples from individuals with schizophrenia [52]. At the same time, the number of dopamine neurons in the VTA was unchanged (Supplementary Fig. S2E), and the levels of dopamine, and dopamine metabolites DOPAC and HVA in ventral striatum showed a small, non-significant increase in Gdnf cHyper/cHyper;Nestin-Cre mice compared with controls (Supplementary Fig. S2F–H). These results align with findings from humans, suggesting enhanced dopamine synthesis and release in dorsal but not in ventral striatum [8, 10, 56]. Altogether, these results demonstrate that an increase in presynaptic nigrostriatal dopamine signalling via an increase in endogenous GDNF levels is associated with a PFC hypodopaminergic state in Gdnf cHyper/cHyper;Nestin-Cre mice.
A Total dopamine levels in the PFC, measured with HPLC. Box plots show median, upper, and lower quartiles, as well as maximum and minimum values. N = 5–10 mice per group. One-way ANOVA, Tukey’s multiple comparisons test. *p < 0.05. B Stimulated dopamine release in slices from ventral tegmental area (VTA) across four consecutive stimulations, measured with fast-scan cyclic voltammetry. Mean ± SEM. n = 2–6 striatal slices per group, one slice per animal. Two-way repeated measures ANOVA, Tukey’s multiple comparisons test. #p < 0.05; ##p < 0.01 between Gdnf wt/wt;Nestin-Cre and Gdnf wt/cHyper;Nestin-Cre mice. C Similar to (B) but showing dopamine re-uptake. Mean ± SEM. n = 2–6 striatal slices per group, one slice per animal. Two-way repeated measures ANOVA, Tukey’s multiple comparisons test. #p < 0.05 between Gdnf wt/wt;Nestin-Cre and Gdnf wt/cHyper;Nestin-Cre mice. D Quantification of the number of dopamine transporter (DAT)-positive synaptic boutons in the prelimbic area in the PFC. Box plots show median, upper, and lower quartiles, as well as maximum and minimum values. N = 4–6 mice per group (average values from n = 2–3 slices per animal). One-way ANOVA, Tukey’s multiple comparisons test. *p < 0.05. E Representative images of immunohistochemistry for DAT showing dopamine synapses in the prelimbic area in the PFC. Scale bar 50 µm.
Mid-gestational increase in endogenous GDNF results in schizophrenia-like behavioural abnormalities
To investigate the behavioural outcome of aberrant dopamine signalling in Gdnf cHyper/cHyper;Nestin-Cre mice, we used a panel of behavioural tests. We first used the prepulse inhibition (PPI) test, which reflects the ability to successfully integrate and inhibit sensory information. PPI refers to a reduction in startle response in response to an intense stimulus if preceded by a lower intensity stimulus [57]. Individuals with schizophrenia and other schizotypal disorders, as well as animal models with schizophrenia-like features have diminished responses to PPI [58,59,60,61,62], which is believed to predominantly reflect impaired striatal and cortical dopamine transmission [60, 61, 63]. We found that the extent of PPI was significantly reduced in Gdnf cHyper/cHyper;Nestin-Cre mice compared with controls (Fig. 3A), whereas the startle response was not changed (Fig. 3B), suggesting that altered dopamine signalling was accompanied by a deficit in sensorimotor gating.
A Pre-pulse inhibition test showing the percentage of inhibition across four different intensities of pre-pulse stimulus. Mean ± SEM. N = 6–7 mice per group. Two-way ANOVA. ***p < 0.001 genotype effect. B Startle response (arbitrary units) in response to a 120 dB stimulus. Mean ± SEM. N = 6–7 mice per group. Welch’s t-test. n.s, not significant. C Average home cage activity, measured as distance travelled, in individually housed Gdnf wt/wt;Nestin-Cre and Gdnf cHyper/cHyper;Nestin-Cre mice over 4 days. Shaded area denotes dark period (lights off), corresponding to the active period in mice. Gdnf cHyper/cHyper;Nestin-Cre mice lack the initial activity peak observed in wild-type littermate controls. Mean ± SEM. N = 13–19 mice per group. Two-way repeated measures ANOVA, Time × Genotype interaction p < 0.0001. Sidak’s multiple comparisons test. **p < 0.01; ***p < 0.001. D Daily water intake in individually housed Gdnf wt/wt;Nestin-Cre and Gdnf cHyper/cHyper;Nestin-Cre mice. Mean ± SEM. N = 7–8 mice per group. Two-way repeated measures ANOVA, Genotype effect p = 0.0371. Sidak’s multiple comparisons test. *p < 0.05. E Average water intake in individually housed Gdnf wt/wt;Nestin-Cre and Gdnf cHyper/cHyper;Nestin-Cre mice over 4 days. Mean ± SEM. N = 7–8 mice per group. Welch’s t-test. *p < 0.05. F Number of visits to water bottle compartments during the dark period in individually tracked mice in the IntelliCage setting. Note that unlike Gdnf wt/wt;Nestin-Cre mice, Gdnf cHyper/cHyper;Nestin-Cre mice do not exhibit reduced activity towards the end of the active (dark) period. Mean ± SEM. N = 9–14 mice per group. Two-way repeated measures ANOVA, Genotype effect p < 0.0001. Sidak’s multiple comparisons test. *p < 0.05; **p < 0.01; ***p < 0.001. G Total number of visits to water bottle compartments in individually tracked mice in the IntelliCage group-housed setting over 4 days. Mean ± SEM. N = 9–14 mice per group. Welch’s t-test. ***p < 0.001.
Next, we used home-cage monitoring to analyse the pattern of daily activity. Apathy and/or avolition, an inability to initiate and perform routine daily tasks is a core negative symptom of schizophrenia [64,65,66] and often manifests as prolonged periods of inactivity [67,68,69]. While not all aspects of avolition can be evaluated in mice, general activity in a familiar environment (a home cage) is relatively easy to assess using the InfraMot system. We found that wild-type animals displayed a well-described activity peak at the onset of the dark period, corresponding to the start of the active period (subjective day) in mice (Fig. 3C). By contrast, Gdnf cHyper/cHyper;Nestin-Cre mice lacked this initial activity peak and remained less active throughout the day (Fig. 3C). This phenotype was not caused by a general deficit in movement, as evident from normal exploration behaviour in novel environment observed in the open field test (Supplementary Fig. S3A), suggesting that Gdnf cHyper/cHyper;Nestin-Cre mice exhibit a phenotype resembling apathy or avolition.
Next, based on the observation that 6–20% of individuals with schizophrenia display polydipsia (excessive drinking) [70,71,72], we measured daily water intake in Gdnf cHyper/cHyper;Nestin-Cre mice in individually housed male mice and female mice grouped housed in the IntelliCage setting, where the activity of each mouse is tracked with a subcutaneous transponder [73]. We found that compared with controls, Gdnf cHyper/cHyper;Nestin-Cre mice showed increased water intake in the home cage (Fig. 3D, E) and increased number of visits to water bottle containing corners in IntelliCage (Fig. 3F, G), suggesting a polydipsia-like phenotype. There were no differences between genotypes in tests measuring anxiety (Supplementary Fig. S3B), compulsory behaviour (Supplementary Fig. S3C), learning and memory (Supplementary Fig. S3D, F), motor impulsivity (Supplementary Fig. S3E) or problem solving (Supplementary Fig. S3G).
Together, our results suggest that striatal hyperdopaminergia and PFC hypodopaminergia in Gdnf cHyper/cHyper;Nestin-Cre mice are associated with specific deficits in sensorimotor gating, daily activity and drinking behaviour, but not with general locomotor activity, anxiety, compulsive behaviour or cognitive function.
Increase in endogenous GDNF at mid-gestation induces gene expression changes in the PFC
To gain a comprehensive understanding of gene expression changes in the PFC, we performed RNAseq analysis of PFC from Gdnf cHyper;Nestin-Cre mice at 2 months of age. We identified 311 differentially expressed (DE) genes in Gdnf wt/cHyper;Nestin-Cre mice and 214 genes in Gdnf cHyper/cHyper;Nestin-Cre mice compared to controls (Supplementary Fig. S4A, B). We found that 58 of the 214 DE genes had previously been associated with schizophrenia in either genome-wide association studies (GWAS) or in transcriptomic analyses from patients (Supplementary Table S1), suggesting that GDNF overexpression recapitulates a subset of the molecular abnormalities underlying schizophrenia. The identified genes included Drd2 and Adora2a, as well as several other genes with established strong association with schizophrenia, including activity regulated cytoskeleton associated protein (Arc), BTG2 anti-proliferation factor 2 (Btg2), and inverted formin, FH2 and WH2 domain containing (Inf2) (Fig. 4A and Supplementary Fig. S4C) [74,75,76,77,78,79,80,81,82,83,84,85,86,87]. Gene Ontology (GO) analysis revealed myelination and dopamine signalling as the most enriched GO terms in the PFC among DE genes in both heterozygous and homozygous mice (Fig. 4B and Supplementary Fig. S4D), in line with gene expression studies on individuals with schizophrenia [7, 58, 75, 88,89,90,91]. Similarly, unbiased clustering of enriched GO categories highlighted changes in biological processes related to dopamine system function, myelination, and neuronal development (Fig. 4C and Supplementary Fig. S5). Given that dysregulation of genes belonging to these GO categories is commonly observed in patient studies, our results suggest that the biological processes affected in schizophrenia are also perturbed in Gdnf cHyper;Nestin-Cre mice.
A An MA plot showing DE genes (green dots) in the PFC of Gdnf cHyper/cHyper;Nestin-Cre compared to Gdnf wt/wt;Nestin-Cre mice. Selected schizophrenia-related DE genes are highlighted in red. B Top enriched non-redundant GO biological process categories of DE genes in the PFC of Gdnf cHyper/cHyper;Nestin-Cre compared to Gdnf wt/wt;Nestin-Cre mice. C Scatter plot of clusters of top 150 enriched GO biological process categories in Gdnf cHyper/cHyper;Nestin-Cre mice.
Striatal elevation of endogenous GDNF in adults induces cortical hypodopaminergia
Symptoms of schizophrenia typically start in adolescence or adulthood. Furthermore, amphetamine and its derivatives increase nigrostriatal GDNF expression in experimental animals and trigger psychosis in some individuals [21,22,23,24,25,26,27]. Thus, we next explored if some of the dopamine system abnormalities found in Gdnf cHyper;Nestin-Cre mice could be induced by an adult-onset increase of endogenous GDNF expression specifically in the striatum. To that end, we injected AAV-Cre bilaterally into the striata of adult Gdnf cHyper mice (Fig. 5A). Two months after striatal AAV-Cre injection, Gdnf expression in the striatum was increased in Gdnf wt/cHyper and Gdnf cHyper/cHyper mice compared with controls (Fig. 5B). FSCV analysis in the striatum of Gdnf wt/cHyper mice showed an increase in dopamine release in response to a burst stimulus compared with wild-type littermates (Fig. 5C), and the levels of dopamine and dopamine metabolites in the PFC were significantly reduced, by ~40% (Fig. 5D and Supplementary Fig. S6F, G). There were no significant differences in the total levels of striatal dopamine or dopamine metabolites (Supplementary Fig. S6A–C), or evoked dopamine release and reuptake (Supplementary Fig. S6D, E). Thus, two-fold adult onset increase in endogenous GDNF expression in the striatum is sufficient to trigger schizophrenia-like hypodopaminergia in the PFC, likely via increased activity of striatal dopamine signalling.
A Schematic of adult-onset upregulation of endogenous GDNF using AAV-Cre. B Striatal Gdnf mRNA levels measured with qPCR. Box plots show median, upper, and lower quartiles, as well as maximum and minimum values. N = 7–8 mice per group. One-way ANOVA, Tukey’s multiple comparisons test. *p < 0.05; ***p < 0.001. C Striatal dopamine release in response to burst stimulus, relative to single stimulus, measured by fast-scan cyclic voltammetry. Box plots show median, upper and lower quartiles, and maximum and minimum values. n = 10–11 striatal slices (from N = 6 mice) per group. Unpaired t-test. *p < 0.05. D Total tissue dopamine levels in the PFC, measured with HPLC. Box plots show median, upper, and lower quartiles, as well as maximum and minimum values. N = 6–8 mice per group. One-way ANOVA, Tukey’s multiple comparisons test. *p < 0.05. E Top enriched non-redundant GO biological process categories of DE genes in the PFC of Gdnf wt/cHyper mice compared to Gdnf wt/wt mice. F Similar to (D) but showing top enriched categories between Gdnf cHyper/cHyper and Gdnf wt/wt mice. G Venn diagram indicating overlapping DE genes in the PFC between Gdnf cHyper;Nestin-Cre and Gdnf cHyper + AAV-Cre mice. Genes differentially expressed in either heterozygous or homozygous mice compared to wild-type controls are shown. H Venn diagrams indicating overlapping DE genes in the PFC between post-mortem human PFC RNAseq datasets originating from the Harvard Brain Bank and Charing Cross Hospital, and Gdnf cHyper;Nestin-Cre mice. I Similar to (G) but showing the overlap between human datasets and Gdnf cHyper + AAV-Cre mice.
To gain insight into molecular response in the PFC, we then analysed PFC gene expression with RNAseq 2 months after adult-onset increase in striatal GDNF. We found 338 DE genes in the PFC of either Gdnf wt/cHyper or Gdnf cHyper/cHyper mice compared with controls, and identified GO terms related to synaptic transmission and immune response as the predominant affected functional categories, similar to findings from human studies [75, 92, 93] (Fig. 5E, F and Supplementary Fig. S6H–K). Notably, we found that 72 genes were differentially expressed in both adult onset and mid-gestation GDNF elevation models (Fig. 5G), indicating the existence of molecular convergence between the two models.
Next, we compared our PFC RNAseq datasets to two previously published studies describing transcriptional changes in the post-mortem PFC samples from individuals with schizophrenia and matched controls [75, 94]. Of the genes differentially expressed in either Gdnf wt/cHyper;Nestin-Cre or Gdnf cHyper/cHyper;Nestin-Cre mice, 45 genes (~10%) overlapped with DE genes in either of these two studies, including Adora2a, Arc, Btg2 and Inf2 (Fig. 5H). Similarly, 38 genes (11%) differentially expressed in the PFC after AAV-Cre-induced adult-onset elevation of striatal GDNF were also identified in at least one of the human studies (Fig. 5I). Therefore, gene expression changes in the PFC of both models share similarities with the findings from human patients.
A2AR antagonism alleviates dopamine system changes in Gdnf cHyper/cHyper;Nestin-Cre mice
To further elucidate the changes caused by increased endogenous GDNF levels that may contribute to phenotypes related to schizophrenia, we performed RNAseq in the striatum and substantia nigra (SN) of Gdnf cHyper;Nestin-Cre mice at 2–3 months of age and Gdnf cHyper mice 2 months after striatal AAV-Cre delivery (Supplementary Fig. S7A, C–J). Due to GDNF’s importance in regulating the midbrain dopamine system, we compared the effects of developmental and adult-onset GDNF upregulation on dopamine system-related gene expression across different brain areas. Between all analysed regions and models, we identified a total of 57 DE dopamine system-related genes (Fig. 6A and Supplementary Fig. S7B). Of these, 15 were differentially expressed after both developmental and adult-onset GDNF elevation, including Adora2a, Drd1, Tyrosine hydroxylase (Th), and Nuclear receptor subfamily 4 group A member 2 (Nr4a2, also known as Nurr1) (Fig. 6A, red arrows, and Supplementary Fig. S7K, L), illustrating a pronounced effect of a 2–3-fold increase in endogenous GDNF on the dopamine system.
A Chord diagram depicting dopamine system-related genes differentially expressed in the prefrontal cortex (PFC), striatum (STR), or substantia nigra (SN) of Gdnf cHyper;Nestin-Cre mice. DE genes overlapping with those differentially expressed in Gdnf cHyper + AAV-Cre mice are shown with red arrows. Genes downregulated in Gdnf cHyper mice compared with wild-type controls are indicated with a blue bar and genes upregulated in Gdnf cHyper mice are indicated with a pink bar next to the name of the gene. WT, Gdnf wt/wt;Nestin-Cre; HET, Gdnf wt/cHyper;Nestin-Cre; HOM, Gdnf cHyper/cHyper;Nestin-Cre. B Experiment schematic of A2AR inhibition using istradefylline. BSL, baseline; VEH, vehicle. See Methods for details. C Average daily voluntary consumption of istradefylline-containing solution in the beginning (d1-d3), middle (d4-d7) and end (d8-d10) of the 10-day treatment period. Mean ± SEM. N = 5–7 mice per group. Two-way ANOVA Genotype × Period interaction. ***p < 0.001. D Striatal dopamine levels normalised to wild-type controls in Gdnf wt/wt;Nestin-Cre and Gdnf cHyper/cHyper;Nestin-Cre before and after istradefylline treatment, measured with HPLC. Mean ± SEM. N = 5–13 mice per group. One-way ANOVA, Tukey’s multiple comparisons test. *p < 0.05; ***p < 0.001; n.s, not significant. E Similar to (D) but showing normalised dopamine levels in the prefrontal cortex. Mean ± SEM. N = 5–13 mice per group. One-way ANOVA, Tukey’s multiple comparisons test. **p < 0.01; n.s, not significant. F Striatal Gdnf mRNA levels in Gdnf wt/wt;Nestin-Cre and Gdnf cHyper/cHyper;Nestin-Cre mice after istradefylline treatment. Mean ± SEM. N = 5–13 mice per group. One-way ANOVA, Tukey’s multiple comparisons test. **p < 0.01.
Adora2a, encoding for Adenosine A2A receptor (A2AR) is a G-protein coupled receptor that regulates the balance of adenosine/dopamine signalling through its interactions with D2R [95,96,97]. Adenosine decreases dopamine signalling through D2R, while A2AR antagonists, such as caffeine are believed to enhance dopamine signalling through D2R [96, 98, 99]. Our RNAseq analysis revealed a downregulation of striatal and PFC Adora2a expression in Gdnf cHyper;Nestin-Cre mice (Figs. 4A, 6A and Supplementary Fig. S7K). This caught our attention, because Adora2a is required for GDNF-stimulated dopamine release in vitro [100]; reduced striatal Adora2a expression has been identified in a subgroup of schizophrenia patients [83]; and some schizophrenia patients voluntarily self-administer excessive amounts of coffee that contains caffeine, a non-selective antagonist for adenosine receptors, as the active ingredient [101, 102]. Finally, a selective A2AR antagonist istradefylline [103] has been shown to be effective in an animal model of obsessive-compulsive disorder triggered by a D2R agonist [104]. Therefore, we hypothesized that A2AR inhibition could alleviate some of the endogenous GDNF-induced schizophrenia-like features.
To address this hypothesis, we tested how istradefylline regulates the dopamine system of Gdnf cHyper/cHyper;Nestin-Cre mice. First, we analysed voluntary intake of istradefylline-containing solution over a period of 10 days (Fig. 6B). Since Gdnf cHyper/cHyper;Nestin-Cre mice have higher water intake at baseline (Fig. 3D, G), we measured daily consumption of istradefylline-containing solution and adjusted the concentration of istradefylline for each animal to achieve a consistent dose of 4 mg/kg/day (Supplementary Fig. S8A, B). We found that while Gdnf cHyper/cHyper;Nestin-Cre mice consumed less istradefylline-containing solution over the first 3 days, they started to self-administer significantly more istradefylline than the control mice towards the end of the 10-day treatment period (Fig. 6C and Supplementary Fig. S8C), consistent with the increased caffeine consumption observed in some individuals with schizophrenia. Next, we analysed the effect of istradefylline on dopamine levels in the striatum and PFC and found that by the end of the treatment period, tissue dopamine levels in these regions were partially normalised (Fig. 6D, E). Reversal of dopamine levels prompted us to investigate the effect of istradefylline on GDNF expression. In cell lines, adenosine signalling increases GDNF expression via multiple cAMP response elements in its promoter [105,106,107,108] and, conversely, A2AR inhibition downregulates GDNF expression [109]. qPCR analysis revealed that istradefylline downregulated striatal GDNF expression in Gdnf cHyper/cHyper;Nestin-Cre mice (Fig. 6F), suggesting that partial renormalisation of striatal GDNF levels could be triggering the partial normalisation of striatal and, consequently, PFC dopamine levels. Collectively, these results show that selective inhibition of A2AR alleviates dopamine system abnormalities both in the PFC and striatum of Gdnf cHyper/cHyper;Nestin-Cre mice.
GDNF levels are increased in the CSF of first-episode psychosis patients
To investigate the possible link between GDNF and schizophrenia in humans, we evaluated GDNF levels in the cerebrospinal fluid (CSF) from first episode psychosis (FEP) patients. CSF was collected from 70 FEP patients, who were either fully naive to antipsychotic drugs as per interview and available medical records or had been prescribed an antipsychotic drug for less than 2 months. For comparison, we used CSF from healthy controls (HCs). We found that FEP patients naive to antipsychotic drugs (see Table 1 and Supplementary Table S2 for demographics and clinical characteristics) displayed significantly higher CSF GDNF levels than HCs (Fig. 7A), suggesting that elevated GDNF levels in unmedicated FEP patients are associated with schizophrenia. We also observed an increase in FEP patients with prior history of antipsychotic drugs compared with HCs, but this did not reach statistical significance due to high variance among the patients (Fig. 7A). As a group, FEP patients displayed higher CSF GDNF levels than HCs (Supplementary Fig. S9A), demonstrating that, overall, higher GDNF levels are associated with schizophrenia. We then assessed the relative importance of other potential confounders and found that the single most important factor influencing CSF GDNF levels was indeed case status (Supplementary Fig. S9B). The distribution of GDNF levels was significantly different between healthy controls and FEP subjects, with controls centring more around the mean (Supplementary Fig. S9C).
A Comparison of GDNF in cerebrospinal fluid obtained from 44 healthy controls (HCs) and 69 first-episode psychosis (FEP) subjects, including 29 medication-naive individuals (Non-med.) and 40 individuals with prior exposure to antipsychotics (Med.). NPX, Normalized Protein eXpression (see Methods for details). Mean ± SEM. One-way ANOVA, Tukey’s multiple comparisons test. *p < 0.05. B Correlation between cerebrospinal fluid GDNF levels and the Clinical Global Impression score in 70 FEP subjects. Pearson product-moment correlation.
To study how GDNF levels associate with the severity of illness in FEP patients, we used the Clinical Global Impression (CGI) for severity of illness (CGI-S) scores. This analysis indicated that CSF GDNF levels correlated with a more severe clinical profile (Fig. 7B, Table 2). No significant differences were observed between FEP patients and HCs regarding age, sex distribution, body mass index, and nicotine usage (Table 1). There were no differences in GDNF levels in the serum of FEP patients compared with controls (Supplementary Fig. S9D).
Subsequently, to evaluate how changes in CSF GDNF levels could reflect GDNF expression in the striatum where GDNF is highly expressed, we utilised raw data from a previously published transcriptomics study analysing striatal gene expression in post-mortem samples from healthy controls and patients with schizophrenia, bipolar disorder, or major depressive disorder [110]. In line with our findings, the results showed a highly significant increase in striatal GDNF mRNA levels in post-mortem striatum in individuals with schizophrenia compared to controls (Supplementary Fig. S9E, F). Together, these results show an overall average higher GDNF expression in schizophrenia patients and suggest that elevated GDNF may contribute to the disease, particularly in patients with highest elevation of GDNF levels.
Discussion
Schizophrenia is a heterogeneous disorder, as indicated by the large number of genetic associations, a wide spectrum of symptoms, and comorbidities with other neuropsychiatric disorders. Recent GWAS analyses suggest that thousands of common genetic variants with small effect sizes contribute to the risk of schizophrenia, and that loci with large effect sizes are very rare [111]. Importantly, by far the most GWAS hits associate with the non-coding genome [112, 113], suggesting that gene regulation, including expression levels play an important role in determining susceptibility to schizophrenia.
GDNF is a neurotrophic factor known for its role in promoting dopamine synthesis and dopamine neuron survival in the midbrain dopamine system [15,16,17,18]. Ectopic GDNF overexpression promotes dopamine synthesis in vitro and in vivo [35, 37, 114], and mice with 2–3-fold constitutively elevated endogenous GDNF expression exhibit increased striatal dopamine levels [29]. Although striatal hyperdopaminergia is observed in some schizophrenic and prodromal individuals [8], and the genomic region containing the GDNF gene has been associated with schizophrenia by several independent studies [115,116,117], there have been no studies attempting to investigate the possible contribution of GDNF to dopaminergic abnormalities in schizophrenia.
Here, we report that both mid-gestation- and adult-onset elevation of endogenous GDNF is sufficient to increase presynaptic dopamine function in the striatum and reduce dopamine signalling in the PFC in mice. In FEP patients, GDNF levels are increased in the CSF, and GDNF levels positively correlate with clinical severity scores. It is important to note that the 2–3-fold increase in endogenous GDNF expression achieved in Gdnf cHyper mice is considerably higher than the ~20% average increase in GDNF levels in the CSF that we observed in schizophrenia patients. However, in some patients the increase in GDNF is more prominent. Therefore, analysis on how GDNF levels in the CSF relate to various parameters, such as dopamine metabolism, A2AR levels and ligand binding, coffee intake, avolition and polydipsia is an important future perspective.
In mice, we found that increased levels of endogenous GDNF were associated with reduced presynaptic dopamine signalling in the PFC, regardless of whether GDNF was increased during mid-gestation or in the adult. However, the timing of endogenous GDNF upregulation impacted distinct pathways. For example, the predominant affected pathways in the PFC after developmental GDNF elevation included myelination and intracellular signalling, whereas adult-onset increase in endogenous GDNF caused changes in the expression of synaptic genes and immune response (Figs. 4B, C, 5E, F and Supplementary Fig. S4D). Together, these observations suggest that both mid-gestation and adult-onset elevation in endogenous GDNF result in striatal hyperdopaminergia and cortical hypodopaminergia. However, the effect of endogenous GDNF levels on other biological processes is critically dependent on the timing of GDNF expression.
RNAseq analysis identified adenosine 2A receptor as one of the genes differentially expressed in multiple brain regions in Gdnf cHyper;Nestin-Cre mice. We therefore used istradefylline, a selective first-in-class A2AR antagonist to test if reducing A2AR activity in Gdnf cHyper/cHyper;Nestin-Cre mice could improve dopaminergic system abnormalities. We found that Gdnf cHyper/cHyper;Nestin-Cre mice voluntarily consumed more istradefylline, resembling the increased caffeine intake observed in some individuals with schizophrenia. Ten days of istradefylline administration reduced striatal GDNF expression and partially reversed the developmentally induced striatal hyperdopaminergia and cortical hypodopaminergia in Gdnf cHyper/cHyper;Nestin-Cre mice. This suggests that selective A2AR antagonism may alleviate some of the symptoms of schizophrenia, with a potential specific relevance for a subgroup of patients with high striatal GDNF levels.
Why would selective A2AR antagonism be advantageous in schizophrenia? In mice, GDNF-producing striatal interneurons express both A2AR and A1R receptors [118, 119], which have antagonistic functions (Fig. 8). A2AR activation triggers cAMP production which has been shown to activate Gdnf transcription in various cell types via cAMP response elements (CRE) in Gdnf promoter [106,107,108, 120]. Given that A2AR antagonism acutely reduces GDNF-induced dopamine release in synaptosomes and striatal slices [100], A2AR signalling could promote GDNF-triggered dopamine release. Thus, A2AR antagonism may alleviate schizophrenia symptoms by two complementary mechanisms: acutely via inhibition of enhanced GDNF-driven striatal dopamine release and chronically via downregulation of striatal GDNF expression (Fig. 8).
Left: Dopaminergic system abnormalities in Gdnf cHyper mice and in individuals with schizophrenia are induced by elevated endogenous GDNF expression in striatal interneurons (blue). In these interneurons, GDNF expression is at least partly regulated by the interplay between A2AR-induced and A1R-mediated inhibition of cAMP signalling that promotes GDNF expression through cAMP response elements (CRE) in Gdnf promoter (inset). Activation of GDNF receptor RET in SN dopamine neurons (green) enhances dopamine release in the dorsal striatum, leading to reduced mesocortical dopamine innervation and dopamine signalling (yellow) in the prefrontal cortex via a yet unknown mechanism. Right: Chronic administration of istradefylline, a specific A2AR antagonist, leads to inhibition of A2AR in GDNF-expressing interneurons, resulting in reduced intracellular cAMP signalling and reduced Gdnf expression (inset). Consequently, striatal GDNF signalling is dampened, leading to reduced dopamine release by SN dopamine neurons and normalization of dopamine signalling in both nigrostriatal and mesocortical dopamine pathways. In addition, A2AR antagonism has an acute effect on GDNF-stimulated dopamine release via a currently unknown mechanism. Figure created with BioRender.com.
One-size-fits-all therapeutic approaches for schizophrenia do not exist. Many patients are refractory to current medication and so have no effective medication, underpinning a need for identifying additional risk factors for a better prediction of treatment response in patient subgroups [121]. In that regard, first episode psychosis patients with high levels of GDNF in the CSF may be of special interest for future research on A2AR and RET inhibition therapy. In dopamine neurons, GDNF mainly signals via RET receptor [122, 123], suggesting that RET inhibitors such as Selpercatinib [124] and Pralsetinib [125], currently used in cancer therapy, may carry potential to treat a subgroup of patients with schizophrenia.
It remains to be determined how GDNF levels in the CSF and the brain relate to GDNF levels in the serum, and how changes in GDNF reflect disease status and treatment response. Several studies have shown that treatment with antipsychotics impacts serum GDNF levels [126,127,128,129,130]. While the results are somewhat controversial, some of these reports suggest that antipsychotics increase serum GDNF levels, although it is unknown if GDNF levels are also increased in the brain. Our results suggest that GDNF levels in the serum and CSF may not be directly correlated; thus, the impact of antipsychotics on striatal GDNF expression awaits further investigation. However, in cultured cells, GDNF expression is impacted by signalling through D2 and 5-HT2A receptors that are targeted by second-generation antipsychotics [131,132,133]. Therefore, it is possible that inhibiting these receptors by antipsychotics directly increases GDNF expression in the brain. However, even if this is the case, any possible downstream changes in dopamine levels would not lead to increased dopamine signalling through D2 receptors, because the latter are blocked by the drug. In that context, increased levels of GDNF could potentially be beneficial in other processes such as adult neurogenesis or neuronal plasticity [134] to support neuronal function in disease. This would be in line with the observation that some atypical antipsychotics increase neurogenesis in adult hippocampus [135], although the underlying mechanisms are unknown. Taken together, the regulation of GDNF levels by antipsychotics and its impact on dopamine signalling and neuronal function in schizophrenia remain important directions for future research.
Lastly, we devised a novel approach to study the effect of an increase in GDNF expression limited to GDNF naturally transcribing cells. Many regulatory genes have a tightly controlled spatiotemporal expression pattern, which is critical to their proper function. Importantly, human studies have shown that as little as a 1.5–2-fold increase in endogenous gene expression levels or biological activity is sufficient to cause neurological disease [136,137,138,139,140]. In addition, while neurotrophic factors, including GDNF, are generally considered to be beneficial in the context of neurological disease, our study demonstrates that the outcomes of neurotrophic factor signalling can be context-dependent and that too high neurotrophic signalling can also drive disease. Therefore, to better understand gene function and therapeutic potential and to create better disease models, it would be advantageous to maintain gene expression from the natural cellular source and at close to physiological expression levels, rather than overexpress with transgenic or viral delivery methods [29, 141] (Supplementary Fig. S10). The levels of more than half of all protein-coding genes are predicted to be negatively regulated through the 3'UTR [142, 143], suggesting that the conditional hypermorph strategy described here is likely to be applicable to other genes. While each approach to study gene function has its limitations, we believe that an ability to conditionally increase gene expression at the post-transcriptional level as implemented in our research, may provide important new opportunities for both basic and translational research.
Materials and methods
Detailed description of Materials and Methods can be found in Supplementary Methods.
Experimental model and subject details
Human samples
Ethical approval was given by Stockholm Regional Ethics Committee (Dnr 2010/879-31/1). Demographics and clinical characteristics of the study participants are provided in Table 1. Informed consent was obtained from all included subjects.
Animals
Animal experiments were conducted according to the 3R principles of the European Union Directive 2010/63/EU and following local laws and regulations. Protocols were authorised by the national Animal Experiment Board of Finland.
Method details
CSF collection and GDNF detection
CSF sampling was performed between 7:45AM and 10:00AM. Samples were centrifuged at 1438 g for 10 min at 4 °C. Supernatant was divided into aliquots and stored at −80 °C. The panel ‘Inflammation’ from Olink Bioscience (Uppsala, Sweden) was used to assess protein levels in the CSF.
Generation of Gdnf cHyper knock-in allele
The targeting construct for the Gdnf cHyper allele (Supplementary Fig. S1A) contained a 4021 bp 5' homologous arm, a 610 bp cassette containing the bovine growth hormone polyadenylation signal (bGHpA) in an inverted orientation flanked by the FLEx system [46] starting immediately after the stop codon, a 2615 bp Pgk1-puΔtk-bGHpA sequence flanked by Frt sites, and a 2927 bp 3' homologous arm. G4 embryonic stem cells were electroporated with 30 μg of linearized targeting construct. After puromycin selection, colonies were screened by long-range PCR for both 5' and 3' homologous arms and correct PCR products were verified by sequencing. Correctly targeted ES cells were injected into C57BL/N6Crl mouse blastocysts to generate chimeric mice. Germline transmission was achieved by breeding male chimeras with C57BL/N6Crl females. The Pgk1-puΔtk-bGHpA sequence was removed using the CAG-Flp mouse line at F2.
Quantification and statistical analyses
Sample size
Sample size was determined based on preliminary experiments and prior experience with the used assays. No statistical methods were used to predetermine sample size.
Rules for stopping data collection
Rules for stopping data collection were not defined.
Data inclusion/exclusion criteria and handling of outliers
Data was excluded based on insufficient quality (assessed immediately after acquisition and before analysis).
Research subjects or units of investigation
In human studies, research subjects correspond to individual patients or controls. In animal experiments, research subjects correspond to individual animals, except for FSCV experiments, where the experimental units are brain slices.
Randomization
Because the genotype of the animal determined the experimental group, randomization to treatment was not possible. To reduce possible bias, only litters including animals from different genotypes were included. In behavioural tests, animals were tested in a random order. Treatments were administered in a random order.
Blinding
Experiments were performed by investigators blinded to experimental groups.
Statistical analysis
Values are presented as mean ± standard error of the mean. Statistical comparison between two groups was performed using unpaired Student’s t-test or Welch’s t-test, where appropriate. Multiple comparisons were performed with one-way or two-way analysis of variance (ANOVA), followed by Tukey’s or Sidak’s post hoc test. Statistical significance was set at P < 0.05.
Data availability
The GEO accession number for RNA sequencing data is GSE162974.
Change history
08 June 2022
Supplementary Methods and Supplementary Tables link are switched.
References
Jauhar S, Johnstone M, McKenna PJ. Schizophrenia. Lancet. 2022;399:473–86.
Uno Y, Coyle JT. Glutamate hypothesis in schizophrenia. Psychiatry Clin Neurosci. 2019;73:204–15.
Hrovatin K, Kunej T, Dolzan V. Genetic variability of serotonin pathway associated with schizophrenia onset, progression, and treatment. Am J Med Genet B Neuropsychiatr Genet. 2020;183:113–27.
Pasquini S, Contri C, Merighi S, Gessi S, Borea PA, Varani K, et al. Adenosine Receptors in Neuropsychiatric Disorders: Fine Regulators of Neurotransmission and Potential Therapeutic Targets. Int J Mol Sci. 2022;23. https://www.mdpi.com/about/announcements/784.
Schmidt MJ, Mirnics K. Neurodevelopment, GABA system dysfunction, and schizophrenia. Neuropsychopharmacology. 2015;40:190–206.
McCutcheon RA, Abi-Dargham A, Howes OD. Schizophrenia, Dopamine and the Striatum: From Biology to Symptoms. Trends Neurosci. 2019;42:205–20.
Howes OD, Kapur S. The dopamine hypothesis of schizophrenia: version III-the final common pathway. Schizophr Bull. 2009;35:549–62.
Howes OD, Kambeitz J, Kim E, Stahl D, Slifstein M, Abi-Dargham A, et al. The nature of dopamine dysfunction in schizophrenia and what this means for treatment. Arch Gen Psychiatry. 2012;69:776–86.
Howes OD, Hird EJ, Adams RA, Corlett PR, McGuire P. Aberrant Salience, Information Processing, and Dopaminergic Signaling in People at Clinical High Risk for Psychosis. Biol Psychiatry. 2020;88:304–14.
McCutcheon R, Beck K, Jauhar S, Howes OD. Defining the Locus of Dopaminergic Dysfunction in Schizophrenia: A Meta-analysis and Test of the Mesolimbic Hypothesis. Schizophr Bull. 2018;44:1301–11.
Fusar-Poli P, Howes OD, Allen P, Broome M, Valli I, Asselin MC, et al. Abnormal frontostriatal interactions in people with prodromal signs of psychosis: a multimodal imaging study. Arch Gen Psychiatry. 2010;67:683–91.
Slifstein M, van de Giessen E, Van Snellenberg J, Thompson JL, Narendran R, Gil R, et al. Deficits in prefrontal cortical and extrastriatal dopamine release in schizophrenia: a positron emission tomographic functional magnetic resonance imaging study. JAMA Psychiatry. 2015;72:316–24.
Rao N, Northoff G, Tagore A, Rusjan P, Kenk M, Wilson A, et al. Impaired Prefrontal Cortical Dopamine Release in Schizophrenia During a Cognitive Task: A [11C]FLB 457 Positron Emission Tomography Study. Schizophr Bull. 2019;45:670–9.
Hidalgo-Figueroa M, Bonilla S, Gutierrez F, Pascual A, Lopez-Barneo J. GDNF is predominantly expressed in the PV+ neostriatal interneuronal ensemble in normal mouse and after injury of the nigrostriatal pathway. J Neurosci. 2012;32:864–72.
Lin LF, Doherty DH, Lile JD, Bektesh S, Collins F. GDNF: a glial cell line-derived neurotrophic factor for midbrain dopaminergic neurons. Science. 1993;260:1130–2.
Tomac A, Lindqvist E, Lin LF, Ogren SO, Young D, Hoffer BJ, et al. Protection and repair of the nigrostriatal dopaminergic system by GDNF in vivo. Nature. 1995;373:335–9.
Gash DM, Zhang Z, Ovadia A, Cass WA, Yi A, Simmerman L, et al. Functional recovery in parkinsonian monkeys treated with GDNF. Nature. 1996;380:252–5.
Kordower JH, Emborg ME, Bloch J, Ma SY, Chu Y, Leventhal L, et al. Neurodegeneration prevented by lentiviral vector delivery of GDNF in primate models of Parkinson’s disease. Science. 2000;290:767–73.
Ibanez CF, Andressoo JO. Biology of GDNF and its receptors - Relevance for disorders of the central nervous system. Neurobiol Dis. 2017;97:80–9.
Love S, Plaha P, Patel NK, Hotton GR, Brooks DJ, Gill SS. Glial cell line-derived neurotrophic factor induces neuronal sprouting in human brain. Nat Med. 2005;11:703–4.
Morrow BA, Roth RH, Redmond DE, Elsworth JD. Impact of methamphetamine on dopamine neurons in primates is dependent on age: implications for development of Parkinson’s disease. Neuroscience. 2011;189:277–85.
Callaghan RC, Cunningham JK, Allebeck P, Arenovich T, Sajeev G, Remington G, et al. Methamphetamine use and schizophrenia: a population-based cohort study in California. Am J Psychiatry. 2012;169:389–96.
Li H, Lu Q, Xiao E, Li Q, He Z, Mei X. Methamphetamine enhances the development of schizophrenia in first-degree relatives of patients with schizophrenia. Can J Psychiatry. 2014;59:107–13.
Valian N, Ahmadiani A, Dargahi L. Escalating Methamphetamine Regimen Induces Compensatory Mechanisms, Mitochondrial Biogenesis, and GDNF Expression, in Substantia Nigra. J Cell Biochem. 2017;118:1369–78.
Wearne TA, Cornish JL. A Comparison of Methamphetamine-Induced Psychosis and Schizophrenia: A Review of Positive, Negative, and Cognitive Symptomatology. Front Psychiatry. 2018;9:491.
Laruelle M, Abi-Dargham A, van Dyck CH, Gil R, D’Souza CD, Erdos J, et al. Single photon emission computerized tomography imaging of amphetamine-induced dopamine release in drug-free schizophrenic subjects. Proc Natl Acad Sci USA. 1996;93:9235–40.
Breier A, Su TP, Saunders R, Carson RE, Kolachana BS, de Bartolomeis A, et al. Schizophrenia is associated with elevated amphetamine-induced synaptic dopamine concentrations: evidence from a novel positron emission tomography method. Proc Natl Acad Sci USA. 1997;94:2569–74.
Abi-Dargham A, Gil R, Krystal J, Baldwin RM, Seibyl JP, Bowers M, et al. Increased striatal dopamine transmission in schizophrenia: confirmation in a second cohort. Am J Psychiatry. 1998;155:761–7.
Kumar A, Kopra J, Varendi K, Porokuokka LL, Panhelainen A, Kuure S, et al. GDNF Overexpression from the Native Locus Reveals its Role in the Nigrostriatal Dopaminergic System Function. PLoS Genet. 2015;11:e1005710.
Beck KD, Irwin I, Valverde J, Brennan TJ, Langston JW, Hefti F. GDNF induces a dystonia-like state in neonatal rats and stimulates dopamine and serotonin synthesis. Neuron. 1996;16:665–73.
Cunha C, Angelucci A, D’Antoni A, Dobrossy MD, Dunnett SB, Berardi N, et al. Brain-derived neurotrophic factor (BDNF) overexpression in the forebrain results in learning and memory impairments. Neurobiol Dis. 2009;33:358–68.
Alcantara S, Pozas E, Ibanez CF, Soriano E. BDNF-modulated spatial organization of Cajal-Retzius and GABAergic neurons in the marginal zone plays a role in the development of cortical organization. Cereb Cortex. 2006;16:487–99.
Emerich DF, Plone M, Francis J, Frydel BR, Winn SR, Lindner MD. Alleviation of behavioral deficits in aged rodents following implantation of encapsulated GDNF-producing fibroblasts. Brain Res. 1996;736:99–110.
Georgievska B, Kirik D, Bjorklund A. Overexpression of glial cell line-derived neurotrophic factor using a lentiviral vector induces time- and dose-dependent downregulation of tyrosine hydroxylase in the intact nigrostriatal dopamine system. J Neurosci. 2004;24:6437–45.
Hebert MA, Van Horne CG, Hoffer BJ, Gerhardt GA. Functional effects of GDNF in normal rat striatum: presynaptic studies using in vivo electrochemistry and microdialysis. J Pharm Exp Ther. 1996;279:1181–90.
Hebert MA, Gerhardt GA. Behavioral and neurochemical effects of intranigral administration of glial cell line-derived neurotrophic factor on aged Fischer 344 rats. J Pharm Exp Ther. 1997;282:760–8.
Hudson J, Granholm AC, Gerhardt GA, Henry MA, Hoffman A, Biddle P, et al. Glial cell line-derived neurotrophic factor augments midbrain dopaminergic circuits in vivo. Brain Res Bull. 1995;36:425–32.
Manfredsson FP, Tumer N, Erdos B, Landa T, Broxson CS, Sullivan LF, et al. Nigrostriatal rAAV-mediated GDNF overexpression induces robust weight loss in a rat model of age-related obesity. Mol Ther. 2009;17:980–91.
Nutt JG, Burchiel KJ, Comella CL, Jankovic J, Lang AE, Laws ER Jr, et al. Randomized, double-blind trial of glial cell line-derived neurotrophic factor (GDNF) in PD. Neurology. 2003;60:69–73.
Rosenblad C, Georgievska B, Kirik D. Long-term striatal overexpression of GDNF selectively downregulates tyrosine hydroxylase in the intact nigrostriatal dopamine system. Eur J Neurosci. 2003;17:260–70.
Moore MW, Klein RD, Farinas I, Sauer H, Armanini M, Phillips H, et al. Renal and neuronal abnormalities in mice lacking GDNF. Nature. 1996;382:76–9.
Pichel JG, Shen L, Sheng HZ, Granholm AC, Drago J, Grinberg A, et al. Defects in enteric innervation and kidney development in mice lacking GDNF. Nature. 1996;382:73–6.
Sanchez MP, Silos-Santiago I, Frisen J, He B, Lira SA, Barbacid M. Renal agenesis and the absence of enteric neurons in mice lacking GDNF. Nature. 1996;382:70–3.
Li H, Jakobson M, Ola R, Gui Y, Kumar A, Sipila P, et al. Development of the urogenital system is regulated via the 3’UTR of GDNF. Sci Rep. 2019;9:5302.
Li H, Kurtzeborn K, Kupari J, Gui Y, Siefker E, Lu B, et al. Postnatal prolongation of mammalian nephrogenesis by excess fetal GDNF. Development. 2021;148. https://doi.org/10.1242/dev.197475.
Schnutgen F, Doerflinger N, Calleja C, Wendling O, Chambon P, Ghyselinck NB. A directional strategy for monitoring Cre-mediated recombination at the cellular level in the mouse. Nat Biotechnol. 2003;21:562–5.
Kakoki M, Tsai YS, Kim HS, Hatada S, Ciavatta DJ, Takahashi N, et al. Altering the expression in mice of genes by modifying their 3’ regions. Dev Cell. 2004;6:597–606.
Lallemand Y, Luria V, Haffner-Krausz R, Lonai P. Maternally expressed PGK-Cre transgene as a tool for early and uniform activation of the Cre site-specific recombinase. Transgenic Res. 1998;7:105–12.
Hayashi S, McMahon AP. Efficient recombination in diverse tissues by a tamoxifen-inducible form of Cre: a tool for temporally regulated gene activation/inactivation in the mouse. Dev Biol. 2002;244:305–18.
Tronche F, Kellendonk C, Kretz O, Gass P, Anlag K, Orban PC, et al. Disruption of the glucocorticoid receptor gene in the nervous system results in reduced anxiety. Nat Genet. 1999;23:99–103.
Berke JD. Functional properties of striatal fast-spiking interneurons. Front Syst Neurosci. 2011;5:45.
Akil M, Pierri JN, Whitehead RE, Edgar CL, Mohila C, Sampson AR, et al. Lamina-specific alterations in the dopamine innervation of the prefrontal cortex in schizophrenic subjects. Am J Psychiatry. 1999;156:1580–9.
Weinberger DR, Berman KF, Daniel DG. Mesoprefrontal cortical dopaminergic activity and prefrontal hypofunction in schizophrenia. Clin Neuropharmacol. 1992;15:568A–9A.
Davis KL, Kahn RS, Ko G, Davidson M. Dopamine in schizophrenia: a review and reconceptualization. Am J Psychiatry. 1991;148:1474–86.
Lammel S, Hetzel A, Hackel O, Jones I, Liss B, Roeper J. Unique properties of mesoprefrontal neurons within a dual mesocorticolimbic dopamine system. Neuron. 2008;57:760–73.
McCollum LA, McCullumsmith RE, Roberts RC. Tyrosine hydroxylase localization in the nucleus accumbens in schizophrenia. Brain Struct Funct. 2016;221:4451–8.
Hoffman HS, Searle JL. Acoustic and temporal factors in the evocation of startle. J Acoust Soc Am. 1968;43:269–82.
Kellendonk C, Simpson EH, Polan HJ, Malleret G, Vronskaya S, Winiger V, et al. Transient and selective overexpression of dopamine D2 receptors in the striatum causes persistent abnormalities in prefrontal cortex functioning. Neuron. 2006;49:603–15.
Li YC, Kellendonk C, Simpson EH, Kandel ER, Gao WJ. D2 receptor overexpression in the striatum leads to a deficit in inhibitory transmission and dopamine sensitivity in mouse prefrontal cortex. Proc Natl Acad Sci USA. 2011;108:12107–12.
Koch M, Bubser M. Deficient sensorimotor gating after 6-hydroxydopamine lesion of the rat medial prefrontal cortex is reversed by haloperidol. Eur J Neurosci. 1994;6:1837–45.
Swerdlow NR, Shoemaker JM, Kuczenski R, Bongiovanni MJ, Neary AC, Tochen LS, et al. Forebrain D1 function and sensorimotor gating in rats: effects of D1 blockade, frontal lesions and dopamine denervation. Neurosci Lett. 2006;402:40–5.
Bolkan SS, Carvalho Poyraz F, Kellendonk C. Using human brain imaging studies as a guide toward animal models of schizophrenia. Neuroscience. 2016;321:77–98.
Siuta MA, Robertson SD, Kocalis H, Saunders C, Gresch PJ, Khatri V, et al. Dysregulation of the norepinephrine transporter sustains cortical hypodopaminergia and schizophrenia-like behaviors in neuronal rictor null mice. PLoS Biol. 2010;8:e1000393.
Fervaha G, Foussias G, Takeuchi H, Agid O, Remington G. Measuring motivation in people with schizophrenia. Schizophr Res. 2015;169:423–6.
Strauss GP, Cohen AS. A Transdiagnostic Review of Negative Symptom Phenomenology and Etiology. Schizophr Bull. 2017;43:712–9.
Sauve G, Brodeur MB, Shah JL, Lepage M. The Prevalence of Negative Symptoms Across the Stages of the Psychosis Continuum. Harv Rev Psychiatry. 2019;27:15–32.
Strauss GP, Bartolomeo LA, Harvey PD. Avolition as the core negative symptom in schizophrenia: relevance to pharmacological treatment development. NPJ Schizophr. 2021;7:16.
Strassnig MT, Harvey PD, Miller ML, Depp CA, Granholm E. Real world sedentary behavior and activity levels in patients with schizophrenia and controls: An ecological momentary assessment study. Ment Health Phys Act. 2021;20. https://doi.org/10.1016/j.mhpa.2020.100364.
Granholm E, Holden JL, Mikhael T, Link PC, Swendsen J, Depp C, et al. What Do People With Schizophrenia Do All Day? Ecological Momentary Assessment of Real-World Functioning in Schizophrenia. Schizophr Bull. 2020;46:242–51.
Chen LC, Bai YM, Chang MH. Polydipsia, hyponatremia and rhabdomyolysis in schizophrenia: A case report. World J Psychiatry. 2014;4:150–2.
Evenson RC, Jos CJ, Mallya AR. Prevalence of polydipsia among public psychiatric patients. Psychol Rep. 1987;60:803–7.
Verghese C, de Leon J, Josiassen RC. Problems and progress in the diagnosis and treatment of polydipsia and hyponatremia. Schizophr Bull. 1996;22:455–64.
Endo T, Maekawa F, Voikar V, Haijima A, Uemura Y, Zhang Y, et al. Automated test of behavioral flexibility in mice using a behavioral sequencing task in IntelliCage. Behav Brain Res. 2011;221:172–81.
Allen NC, Bagade S, McQueen MB, Ioannidis JP, Kavvoura FK, Khoury MJ, et al. Systematic meta-analyses and field synopsis of genetic association studies in schizophrenia: the SzGene database. Nat Genet. 2008;40:827–34.
Maycox PR, Kelly F, Taylor A, Bates S, Reid J, Logendra R, et al. Analysis of gene expression in two large schizophrenia cohorts identifies multiple changes associated with nerve terminal function. Mol Psychiatry. 2009;14:1083–94.
Jagannathan K, Calhoun VD, Gelernter J, Stevens MC, Liu J, Bolognani F, et al. Genetic associations of brain structural networks in schizophrenia: a preliminary study. Biol Psychiatry. 2010;68:657–66.
Zhan L, Kerr JR, Lafuente MJ, Maclean A, Chibalina MV, Liu B, et al. Altered expression and coregulation of dopamine signalling genes in schizophrenia and bipolar disorder. Neuropathol Appl Neurobiol. 2011;37:206–19.
Lewis CM, Levinson DF, Wise LH, DeLisi LE, Straub RE, Hovatta I, et al. Genome scan meta-analysis of schizophrenia and bipolar disorder, part II: Schizophrenia. Am J Hum Genet. 2003;73:34–48.
Sun J, Kuo PH, Riley BP, Kendler KS, Zhao Z. Candidate genes for schizophrenia: a survey of association studies and gene ranking. Am J Med Genet B Neuropsychiatr Genet. 2008;147B:1173–81.
Ng MY, Levinson DF, Faraone SV, Suarez BK, DeLisi LE, Arinami T, et al. Meta-analysis of 32 genome-wide linkage studies of schizophrenia. Mol Psychiatry. 2009;14:774–85.
Deng X, Takaki H, Wang L, Kuroki T, Nakahara T, Hashimoto K, et al. Positive association of phencyclidine-responsive genes, PDE4A and PLAT, with schizophrenia. Am J Med Genet B Neuropsychiatr Genet. 2011;156B:850–8.
Vercammen A, Weickert CS, Skilleter AJ, Lenroot R, Schofield PR, Weickert TW. Common polymorphisms in dopamine-related genes combine to produce a ‘schizophrenia-like’ prefrontal hypoactivity. Transl Psychiatry. 2014;4:e356.
Villar-Menendez I, Diaz-Sanchez S, Blanch M, Albasanz JL, Pereira-Veiga T, Monje A, et al. Reduced striatal adenosine A2A receptor levels define a molecular subgroup in schizophrenia. J Psychiatr Res. 2014;51:49–59.
Schizophrenia Working Group of the Psychiatric Genomics C. Biological insights from 108 schizophrenia-associated genetic loci. Nature. 2014;511:421–7.
Huentelman MJ, Muppana L, Corneveaux JJ, Dinu V, Pruzin JJ, Reiman R, et al. Association of SNPs in EGR3 and ARC with Schizophrenia Supports a Biological Pathway for Schizophrenia Risk. PLoS One. 2015;10:e0135076.
Manago F, Mereu M, Mastwal S, Mastrogiacomo R, Scheggia D, Emanuele M, et al. Genetic Disruption of Arc/Arg3.1 in Mice Causes Alterations in Dopamine and Neurobehavioral Phenotypes Related to Schizophrenia. Cell Rep. 2016;16:2116–28.
Pergola G, Di Carlo P, D’Ambrosio E, Gelao B, Fazio L, Papalino M, et al. DRD2 co-expression network and a related polygenic index predict imaging, behavioral and clinical phenotypes linked to schizophrenia. Transl Psychiatry. 2017;7:e1006.
Tkachev D, Mimmack ML, Ryan MM, Wayland M, Freeman T, Jones PB, et al. Oligodendrocyte dysfunction in schizophrenia and bipolar disorder. Lancet. 2003;362:798–805.
Hakak Y, Walker JR, Li C, Wong WH, Davis KL, Buxbaum JD, et al. Genome-wide expression analysis reveals dysregulation of myelination-related genes in chronic schizophrenia. Proc Natl Acad Sci USA. 2001;98:4746–51.
McCullumsmith RE, Gupta D, Beneyto M, Kreger E, Haroutunian V, Davis KL, et al. Expression of transcripts for myelination-related genes in the anterior cingulate cortex in schizophrenia. Schizophr Res. 2007;90:15–27.
Mitkus SN, Hyde TM, Vakkalanka R, Kolachana B, Weinberger DR, Kleinman JE, et al. Expression of oligodendrocyte-associated genes in dorsolateral prefrontal cortex of patients with schizophrenia. Schizophr Res. 2008;98:129–38.
Mirnics K, Middleton FA, Marquez A, Lewis DA, Levitt P. Molecular characterization of schizophrenia viewed by microarray analysis of gene expression in prefrontal cortex. Neuron. 2000;28:53–67.
Mistry M, Gillis J, Pavlidis P. Meta-analysis of gene coexpression networks in the post-mortem prefrontal cortex of patients with schizophrenia and unaffected controls. BMC Neurosci. 2013;14:105.
Glatt SJ, Everall IP, Kremen WS, Corbeil J, Sasik R, Khanlou N, et al. Comparative gene expression analysis of blood and brain provides concurrent validation of SELENBP1 up-regulation in schizophrenia. Proc Natl Acad Sci USA. 2005;102:15533–8.
Fuxe K, Marcellino D, Borroto-Escuela DO, Guescini M, Fernandez-Duenas V, Tanganelli S, et al. Adenosine-dopamine interactions in the pathophysiology and treatment of CNS disorders. CNS Neurosci Ther. 2010;16:e18–42.
Bonaventura J, Navarro G, Casado-Anguera V, Azdad K, Rea W, Moreno E, et al. Allosteric interactions between agonists and antagonists within the adenosine A2A receptor-dopamine D2 receptor heterotetramer. Proc Natl Acad Sci USA. 2015;112:E3609–18.
Ferre S, Bonaventura J, Tomasi D, Navarro G, Moreno E, Cortes A, et al. Allosteric mechanisms within the adenosine A2A-dopamine D2 receptor heterotetramer. Neuropharmacology. 2016;104:154–60.
Ballesteros-Yanez I, Castillo CA, Merighi S, Gessi S. The Role of Adenosine Receptors in Psychostimulant Addiction. Front Pharm. 2017;8:985.
Berger AA, Winnick A, Welschmeyer A, Kaneb A, Berardino K, Cornett EM, et al. Istradefylline to Treat Patients with Parkinson’s Disease Experiencing “Off” Episodes: A Comprehensive Review. Neurol Int. 2020;12:109–29.
Gomes CA, Vaz SH, Ribeiro JA, Sebastiao AM. Glial cell line-derived neurotrophic factor (GDNF) enhances dopamine release from striatal nerve endings in an adenosine A2A receptor-dependent manner. Brain Res. 2006;1113:129–36.
Hughes JR, McHugh P, Holtzman S. Caffeine and schizophrenia. Psychiatr Serv. 1998;49:1415–7.
McLellan TM, Caldwell JA, Lieberman HR. A review of caffeine’s effects on cognitive, physical and occupational performance. Neurosci Biobehav Rev. 2016;71:294–312.
Kanda T, Jackson MJ, Smith LA, Pearce RK, Nakamura J, Kase H, et al. Adenosine A2A antagonist: a novel antiparkinsonian agent that does not provoke dyskinesia in parkinsonian monkeys. Ann Neurol. 1998;43:507–13.
Asaoka N, Nishitani N, Kinoshita H, Nagai Y, Hatakama H, Nagayasu K, et al. An Adenosine A2A Receptor Antagonist Improves Multiple Symptoms of Repeated Quinpirole-Induced Psychosis. eNeuro. 2019;6. https://doi.org/10.1523/ENEURO.0366-18.2019.
Yamagata K, Hakata K, Maeda A, Mochizuki C, Matsufuji H, Chino M, et al. Adenosine induces expression of glial cell line-derived neurotrophic factor (GDNF) in primary rat astrocytes. Neurosci Res. 2007;59:467–74.
Grimm L, Holinski-Feder E, Teodoridis J, Scheffer B, Schindelhauer D, Meitinger T, et al. Analysis of the human GDNF gene reveals an inducible promoter, three exons, a triplet repeat within the 3’-UTR and alternative splice products. Hum Mol Genet. 1998;7:1873–86.
Verity AN, Wyatt TL, Lee W, Hajos B, Baecker PA, Eglen RM, et al. Differential regulation of glial cell line-derived neurotrophic factor (GDNF) expression in human neuroblastoma and glioblastoma cell lines. J Neurosci Res. 1999;55:187–97.
Lamberti D, Vicini E. Promoter analysis of the gene encoding GDNF in murine Sertoli cells. Mol Cell Endocrinol. 2014;394:105–14.
Ke RH, Xiong J, Liu Y. Adenosine A2a receptor induces GDNF expression by the Stat3 signal in vitro. Neuroreport. 2012;23:958–62.
Lanz TA, Reinhart V, Sheehan MJ, Rizzo SJS, Bove SE, James LC, et al. Postmortem transcriptional profiling reveals widespread increase in inflammation in schizophrenia: a comparison of prefrontal cortex, striatum, and hippocampus among matched tetrads of controls with subjects diagnosed with schizophrenia, bipolar or major depressive disorder. Transl Psychiatry. 2019;9:151.
Smeland OB, Frei O, Dale AM, Andreassen OA. The polygenic architecture of schizophrenia—rethinking pathogenesis and nosology. Nat Rev Neurol. 2020;16:366–79.
Baresic A, Nash AJ, Dahoun T, Howes O, Lenhard B. Understanding the genetics of neuropsychiatric disorders: the potential role of genomic regulatory blocks. Mol Psychiatry. 2020;25:6–18.
Roussos P, Mitchell AC, Voloudakis G, Fullard JF, Pothula VM, Tsang J, et al. A role for noncoding variation in schizophrenia. Cell Rep. 2014;9:1417–29.
Pothos EN, Davila V, Sulzer D. Presynaptic recording of quanta from midbrain dopamine neurons and modulation of the quantal size. J Neurosci. 1998;18:4106–18.
Cooper-Casey K, Mesen-Fainardi A, Galke-Rollins B, Llach M, Laprade B, Rodriguez C, et al. Suggestive linkage of schizophrenia to 5p13 in Costa Rica. Mol Psychiatry. 2005;10:651–6.
Bespalova IN, Angelo GW, Durner M, Smith CJ, Siever LJ, Buxbaum JD, et al. Fine mapping of the 5p13 locus linked to schizophrenia and schizotypal personality disorder in a Puerto Rican family. Psychiatr Genet. 2005;15:205–10.
Suarez BK, Duan J, Sanders AR, Hinrichs AL, Jin CH, Hou C, et al. Genomewide linkage scan of 409 European-ancestry and African American families with schizophrenia: suggestive evidence of linkage at 8p23.3-p21.2 and 11p13.1-q14.1 in the combined sample. Am J Hum Genet. 2006;78:315–33.
Saunders A, Macosko EZ, Wysoker A, Goldman M, Krienen FM, de Rivera H, et al. Molecular Diversity and Specializations among the Cells of the Adult Mouse Brain. Cell. 2018;174:1015–30 e16.
Krienen FM, Goldman M, Zhang Q, CHDR R, Florio M, Machold R, et al. Innovations present in the primate interneuron repertoire. Nature. 2020;586:262–9.
Parekh PA, Garcia TX, Hofmann MC. Regulation of GDNF expression in Sertoli cells. Reproduction. 2019;157:R95–R107.
Tognin S, van Hell HH, Merritt K, Winter-van Rossum I, Bossong MG, Kempton MJ, et al. Towards Precision Medicine in Psychosis: Benefits and Challenges of Multimodal Multicenter Studies-PSYSCAN: Translating Neuroimaging Findings From Research into Clinical Practice. Schizophr Bull. 2020;46:432–41.
Taraviras S, Marcos-Gutierrez CV, Durbec P, Jani H, Grigoriou M, Sukumaran M, et al. Signalling by the RET receptor tyrosine kinase and its role in the development of the mammalian enteric nervous system. Development. 1999;126:2785–97.
Drinkut A, Tillack K, Meka DP, Schulz JB, Kugler S, Kramer ER. Ret is essential to mediate GDNF’s neuroprotective and neuroregenerative effect in a Parkinson disease mouse model. Cell Death Dis. 2016;7:e2359.
Andreev-Drakhlin A, Cabanillas M, Amini B, Subbiah V. Systemic and CNS Activity of Selective RET Inhibition With Selpercatinib (LOXO-292) in a Patient With RET-Mutant Medullary Thyroid Cancer With Extensive CNS Metastases. JCO Precis Oncol. 2020;4. https://doi.org/10.1200/PO.20.00096.
Locantore P, Novizio R, Corsello A, Paragliola RM, Pontecorvi A, Corsello SM. Discovery, preclinical development, and clinical application of pralsetinib in the treatment of thyroid cancer. Expert Opin Drug Discov. 2021;17:101–7.
Xiao W, Ye F, Ma L, Tang X, Li J, Dong H, et al. Atypical antipsychotic treatment increases glial cell line-derived neurotrophic factor serum levels in drug-free schizophrenic patients along with improvement of psychotic symptoms and therapeutic effects. Psychiatry Res. 2016;246:617–22.
Skibinska M, Kapelski P, Pawlak J, Rajewska-Rager A, Dmitrzak-Weglarz M, Szczepankiewicz A, et al. Glial Cell Line-Derived Neurotrophic Factor (GDNF) serum level in women with schizophrenia and depression, correlation with clinical and metabolic parameters. Psychiatry Res. 2017;256:396–402.
Ye F, Zhan Q, Xiao W, Sha W, Zhang X. Altered serum levels of glial cell line-derived neurotrophic factor in male chronic schizophrenia patients with tardive dyskinesia. Int J Methods Psychiatr Res. 2018;27:e1727.
Niitsu T, Shirayama Y, Matsuzawa D, Shimizu E, Hashimoto K, Iyo M. Association between serum levels of glial cell-line derived neurotrophic factor and attention deficits in schizophrenia. Neurosci Lett. 2014;575:37–41.
Tunca Z, Kivircik Akdede B, Ozerdem A, Alkin T, Polat S, Ceylan D, et al. Diverse glial cell line-derived neurotrophic factor (GDNF) support between mania and schizophrenia: a comparative study in four major psychiatric disorders. Eur Psychiatry. 2015;30:198–204.
Hisaoka K, Nishida A, Takebayashi M, Koda T, Yamawaki S, Nakata Y. Serotonin increases glial cell line-derived neurotrophic factor release in rat C6 glioblastoma cells. Brain Res. 2004;1002:167–70.
Ahmadiantehrani S, Ron D. Dopamine D2 receptor activation leads to an up-regulation of glial cell line-derived neurotrophic factor via Gbetagamma-Erk1/2-dependent induction of Zif268. J Neurochem. 2013;125:193–204.
Ohta K, Fujinami A, Kuno S, Sakakimoto A, Matsui H, Kawahara Y, et al. Cabergoline stimulates synthesis and secretion of nerve growth factor, brain-derived neurotrophic factor and glial cell line-derived neurotrophic factor by mouse astrocytes in primary culture. Pharmacology. 2004;71:162–8.
Bonafina A, Trinchero MF, Rios AS, Bekinschtein P, Schinder AF, Paratcha G, et al. GDNF and GFRalpha1 Are Required for Proper Integration of Adult-Born Hippocampal Neurons. Cell Rep. 2019;29:4308–19 e4.
Chikama K, Yamada H, Tsukamoto T, Kajitani K, Nakabeppu Y, Uchimura N. Chronic atypical antipsychotics, but not haloperidol, increase neurogenesis in the hippocampus of adult mouse. Brain Res. 2017;1676:77–82.
Ross OA, Braithwaite AT, Skipper LM, Kachergus J, Hulihan MM, Middleton FA, et al. Genomic investigation of alpha-synuclein multiplication and parkinsonism. Ann Neurol. 2008;63:743–50.
Glessner JT, Wang K, Cai G, Korvatska O, Kim CE, Wood S, et al. Autism genome-wide copy number variation reveals ubiquitin and neuronal genes. Nature. 2009;459:569–73.
Elia J, Glessner JT, Wang K, Takahashi N, Shtir CJ, Hadley D, et al. Genome-wide copy number variation study associates metabotropic glutamate receptor gene networks with attention deficit hyperactivity disorder. Nat Genet. 2011;44:78–84.
Gennarino VA, Singh RK, White JJ, De Maio A, Han K, Kim JY, et al. Pumilio1 haploinsufficiency leads to SCA1-like neurodegeneration by increasing wild-type Ataxin1 levels. Cell. 2015;160:1087–98.
Liao HM, Chao YL, Huang AL, Cheng MC, Chen YJ, Lee KF, et al. Identification and characterization of three inherited genomic copy number variations associated with familial schizophrenia. Schizophr Res. 2012;139:229–36.
Doyle A, McGarry MP, Lee NA, Lee JJ. The construction of transgenic and gene knockout/knockin mouse models of human disease. Transgenic Res. 2012;21:327–49.
Friedman RC, Farh KK, Burge CB, Bartel DP. Most mammalian mRNAs are conserved targets of microRNAs. Genome Res. 2009;19:92–105.
Khabar KS. The AU-rich transcriptome: more than interferons and cytokines, and its role in disease. J Interferon Cytokine Res. 2005;25:1–10.
Acknowledgements
The authors thank S. Wiss, J. Lahtinen, K. Hovirinta, N. Messner, M. Niiranen, H. Niittymäki and J. Palmu for technical assistance, M. Hanzel for language editing, and Kert Mätlik, S. Ollila and members of the Andressoo lab for discussions on the manuscript. Genetically modified mice were generated at the Turku Center for Disease Modeling. Mouse Behavioral Phenotyping Facility is supported by Helsinki Institute of Life Science and Biocenter Finland. KM was supported by the doctoral program Brain and Mind and Alfred Kordelin Foundation. DRG was supported by the Finnish Parkinson Foundation, Fulbright Finland, the doctoral program Brain and Mind and the Biomedicum Helsinki Foundation. GT was supported by the Finnish Parkinson Foundation. AP was supported by Jane and Aatos Erkko Foundation. JJK was supported by the Finnish Cultural Foundation and Emil Aaltonen Foundation. JJ was supported by the Swedish Research Council, the Swedish Foundation for Strategic Research, the Swedish Brain Foundation, and the Swedish Government Initiative for Strategic Research Areas (MultiPark & StemTherapy). JOA was supported by the Academy of Finland (grant no. 297727), Sigrid Juselius Foundation, Center of Innovative Medicine (CIMED), Alzheimerfonden, Hjärnfonden, Swedish Research Council (grant no. 2019-01578), Faculty of Medicine at the University of Helsinki, Helsinki Institute of Life Science, and by European Research Council (ERC) under the European Union’s Horizon 2020 research and innovation programme (grant no. 724922). SC was supported by the Swedish Research Council (Grant No. 523-2014-3467). This work was also supported by grants from the Swedish Medical Research Council (SE: 2021-02251_VR, GE: 2019:01452, FP: 2017-03054), the Swedish Brain Foundation, Torsten Söderbergs Stiftelse, Stockholm County Council (ALF; SC, CMS, and SE), Center for Psychiatry Research and the Karolinska Institutet.
Funding
Open Access funding provided by University of Helsinki including Helsinki University Central Hospital.
Author information
Authors and Affiliations
Contributions
KM planned and designed experiments, analysed and interpreted the data, prepared figures, and wrote the manuscript. KM, SO, DRG, ARM-R, FE, GT, LC, LLP, AP, TPP and JJK performed experiments and analysed the data. AD, KM, EB and NS analysed RNA sequencing results. FE, FP, GE, SC, CMS and SE collected and analysed human data. FZ and PS designed the cloning strategy and generated the Gdnf cHyper mouse line. JJ produced the AAV. J-OA, SC, CMS and SE provided funding. J-OA conceptualized the conditional hypermorph approach, designed the Gdnf cHyper allele, supervised the project and contributed to writing the manuscript. All authors have read and approved the manuscript.
Corresponding authors
Ethics declarations
Competing interests
CMS is a scientific advisor to Outermost Therapeutics Inc. The rest of the authors declare that they have no competing interests.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary information
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons license, and indicate if changes were made. The images or other third party material in this article are included in the article’s Creative Commons license, unless indicated otherwise in a credit line to the material. If material is not included in the article’s Creative Commons license and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this license, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
Mätlik, K., Garton, D.R., Montaño-Rodríguez, A.R. et al. Elevated endogenous GDNF induces altered dopamine signalling in mice and correlates with clinical severity in schizophrenia. Mol Psychiatry 27, 3247–3261 (2022). https://doi.org/10.1038/s41380-022-01554-2
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/s41380-022-01554-2
- Springer Nature Limited
This article is cited by
-
Analysis of post-market adverse events of istradefylline: a real-world study base on FAERS database
Scientific Reports (2024)
-
Biomarkers in the cerebrospinal fluid of patients with psychotic disorders compared to healthy controls: a systematic review and meta-analysis
Molecular Psychiatry (2023)
-
Finding an Optimal Level of GDNF Overexpression: Insights from Dopamine Cycling
Cellular and Molecular Neurobiology (2023)