Abstract
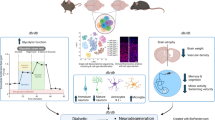
Analyzing changes in gene expression within specific brain regions of individuals with Type 2 Diabetes (T2DM) who do not exhibit significant cognitive deficits can yield valuable insights into the mechanisms underlying the progression towards a more severe phenotype. In this study, transcriptomic analysis of the cortex and hippocampus of mice with long-term T2DM revealed alterations in the expression of 28 genes in the cerebral cortex and 15 genes in the hippocampus. Among these genes, six displayed consistent changes in both the cortex and hippocampus: Interferon regulatory factor 7 (Irf7), Hypoxia-inducible factor 3 alpha (Hif-3α), period circadian clock 2 (Per2), xanthine dehydrogenase (Xdh), and Transforming growth factor β-stimulated clone 22/TSC22 (Tsc22d3) were upregulated, while Claudin-5 (Cldn5) was downregulated. Confirmation of these changes was achieved through RT-qPCR. At the protein level, CLDN5 and IRF7 exhibited similar alterations, with CLDN5 being downregulated and IRF7 being upregulated. In addition, the hippocampus and cortex of the T2DM mice showed decreased levels of IκBα, implying the involvement of NF-κB pathways as well. Taken together, these results suggest that the weakening of the blood-brain barrier and an abnormal inflammatory response via the Interferon 1 and NF-κB pathways underlie cognitive impairment in individuals with long-standing T2DM
Similar content being viewed by others
Background
Several clinical studies have revealed that a significant number of patients with long-term Type 2 Diabetes Mellitus (T2DM) may experience mood disorders along with mild cognitive deficits, particularly in verbal memory, information processing speed, attention, and task implementation [1, 2]. In accordance with these observations, in a recent publication we demonstrated that wild-type (WT) mice subjected to the high-fat diet (HFD) and streptozotocin (STZ) experimental regimen develop classical signs of metabolic syndrome (i.e., weight gain, hyperglycemia, and impaired responses to the glucose and insulin tolerance tests), subtle deficits in spatial learning and working memory and impairments in spatial memory [3]. In light of these findings and acknowledging that the prolonged impact of T2DM may contribute to more profound cognitive deficits and potentially trigger the onset of neurodegeneration [1, 2, 4, 5], we now inquire: What molecular mechanisms undergo changes in the brains of individuals with long-standing type 2 diabetes before or at the onset of the first signs of cognitive deficits? To address this question, we examined the gene expression patterns in the hippocampus and cerebral cortex of late adult/old mice with long-standing T2DM-like disorder and minor cognitive deficits, compared to non-T2DM mice.
Methods
All the animal procedures were approved by the ethics committees of the CBM and the local authorities (PROEX 204/19), and were performed in accordance with the guidelines of the European Union (2010/63/UE). C57BL/6 J WT mice were bred at the CBM animal facility and kept in ventilated racks at 22 ± 2 °C and 55 ± 10% humidity with a 12 h/12 h light cycle and free access to food and water at all times. At 7-9 months of age, animals were subjected to HFD (60% kcal from fat) for 14 weeks, at which time an intraperitoneal injection of STZ (40 mg/kg) per day was performed for 5 days [6, 7]. Although STZ is a compound commonly used as an experimental model of type 1 diabetes, its use at multiple low doses and in combination with HFD allows it to mimic the final stages of T2DM [8]. After the STZ treatment, HFD was continued for another 6 weeks, when the mice were 12–14 months-old. This type of experimental approach is significantly different from previous investigations in mice, where either a single dose of STZ was employed on 2 month-old mice or where both HFD and STZ were administered, albeit in mice aged 2 months or even as young as 1 month [7, 8]. It is worth noting that mice are considered adults until they reach 10–14 months of age (source: https://www.jax.org/news-and-insights/jax-blog/2017/november/when-are-mice-considered-old). Consequently, toward the end of our experimental period, our mice would likely begin to display signs of aging. This phenomenon allows for a more accurate emulation of the potential effects seen in individuals with long-term, untreated Type 2 diabetes.
Behavioral tests, immunoblotting, RNA-sequencing and data analysis, transcript enrichment analysis, and statistical analysis were performed at the end of the experiment. The corresponding procedures have been described in a previous publication [3] and are also summarized in the figure legends and supplementary information. Gene expresion changes consistent between cortex and hippocampus were validated by RT-qPCR following the protocol described in [9] (see supplementary information for details).
Results
In our previous study [3], we demonstrated that adult mice subjected to a 5-month T2DM paradigm (as described above in the Methods) exhibited deficits in spatial memory. In support of the previous finding, in Supplementary Fig. 1 we show that this paradigm leads to deficits in the nest-building test (Supplementary Fig. 1A), which measures general health and stress levels [10] and in the exploratory behavior in the open and closed arms in the elevated plus maze (Supplementary Fig. 1B). Although we did not observe significant differences in the elevated plus maze test, it is noteworthy that 5 out of the 8 mice tested spent more time in the open arm than in the closed arm, which is generally considered indicative of a low anxiety state [11].This would not be surprising when considering that reduced anxiety may precede depression, and that some individuals with chronic T2DM develop depression [1, 2]. Additionally, we confirm that the cognitive changes accompanying T2DM have a biochemical correlate in the brain, evidenced by elevated levels of mTORC1 phosphorylated at Serine 2448 (Supplementary Fig. 1C). While phosphorylation of mTOR at Serine 2448 plays a central role in regulating cell growth, protein synthesis, and metabolism in response to insulin and other growth factors, it also triggers the phosphorylation of serine residues on insulin receptor substrate (IRS) proteins, ultimately resulting in a reduction in insulin signaling (insulin resistance) [12,13,14]. These findings, in conjunction with those from our most recent publication, lead us to the conclusion that, even in a genetically typical background (C57BL/6), chronic measures leading to peripheral insulin resistance give rise to both biochemical and functional impairments within the mouse brain.
To gain mechanistic insights on how T2DM might be leading to brain function changes, we carried out a transcriptomic analysis of cortical and hippocampal samples from the control and the T2DM mice used for the behavioral and biochemical studies. Total RNA from the cortex and hippocampus of 3 control and 3 T2DM mice was extracted and after poly(A)+ selection RNA sequencing was carried out using the Illumina methodology as described previously [3]. Typically, three biological replicates per group are considered sufficient to yield reliable results and facilitate effective statistical analyses. Figure 1A shows that T2DM resulted in significant changes in the expression of 28 genes in the cerebral cortex (6 downregulated and 22 upregulated) and 15 in the hippocampus (7 upregulated and 8 downregulated). 6 of these genes were common for both structures: Hif-3α, IrfF7, Per2, Xdh, Tsc22d3 are upregulated, and Cldn5 is downregulated (marked in Fig. 1A, see also Supplementary Tables 1 and 2). An overrepresentation analysis (ORA) using the ClusterProfiler R package (see Materials and Methods) was conducted to determine whether known biological functions or processes are over-represented in these differentially expressed genes (DEGs). The gene ontology (GO) plot in Fig. 1B offers insights into the pathways that could be most influenced by the up and downregulation of these genes: inflammation and immunity (e.g., Irf7, Irf9, Ifit1, GM19439, Ly6C), cellular rhythmicity (e.g., Ciart, Per2, Dbp, Tef), metabolism (AMPK, Tsc22d3, AdipoR2, Mt2, Fkbp5, AsgR1, Cyp26b), maintenance of the blood-brain barrier/vascular integrity (e.g., Cldn5, Cav1, MMP14, Sdc4), oxidative metabolism/response to hypoxia (e.g., Gpt2, Xdh, Hif-3α, Tsc22d3, Mt2), regulation of gene expression (Xlr4a), cell-cell interaction/morphogenesis (Xlr4a, Hspg2, Sdc4, Zic4, Bmp6, Sned1, Col1a), and neurotransmission/synaptic plasticity (e.g., Xlr4a, CamK1, Slc6a13). The functional association of these DEGs is also shown in a dot plot visualization representing the log10(pvalue) for each enriched pathway (Supplementary Fig. 2).
A Gene Expression Differences in the Cerebral Cortex and Hippocampus of Control and Chronic Type 2 Diabetes Mellitus (T2DM) Mice. Hierarchical cluster analysis with q-value < 0.05 of Differential Gene Expression (DEGs) of the Cortex (left panel) and Hippocampus (right panel) of Type 2 Diabetes Mellitus (T2DM) and control (CTL) WT mice. Each row represents a single gene and each column represents a condition sample. Each subcolumn represents an individual sample (3 mice per condition). Gene intensities are log2 transformed and displayed as colors ranging from blue to garnet representing the changing process from downregulation to upregulation as shown in the key. Common differentially expressed genes are marked in boxes. B Predicted Functional Connections Between Misregulated Genes in the Cortex and Hippocampus of Chronic Type 2 Diabetes Mellitus (T2DM) Mice. GOChord plot showcases the connection between chosen pathways and the genes linked to Type 2 Diabetes Mellitus (T2DM). Genes are depicted in a spectrum of blue-to-garnet colors, representing their log2-Fold-Change values. This visualization offers insight into the relationships between pathways and genes, enhancing our understanding of their potential roles in T2DM.
We then proceeded to validate the changes of the 6 common genes in cortex and hippocampus at the mRNA and protein level. RT-qPCR of cortex and hippocampal RNA from 5 T2DM and control mice confirmed these gene expression changes for all except for Per2, which was significant in RNA from the cerebral cortex but not from hippocampus (Fig. 2A). Furthermore, given that there is not always a correlation between mRNA and protein levels (i.e., translation efficiency, protein degradation, protein stability, feedback loops and compensatory mechanisms), we next analyzed the protein levels of 4 of the transcripts for which we had appropiate antibodies: CLDN5, IRF7, PER2, and HIF-3α. Figure 2B shows that T2DM induces protein-level changes in both CLDN5 and IRF7 in the hippocampus, mirroring the alterations observed at the mRNA level. Furthermore, Fig. 2C shows that T2DM significantly decreases CLDN5 at the protein level in the cerebral cortex -also consistent with the transcriptomic findings-, while IRF7 is higher than in non-T2DM but it does not reach statistical significance. In any event, and consistent with the increase in IRF7, we observed a significant reduction of IκBα in the hippocampus and, though not significant, a clear decrease compared to controls was also noted in the cerebral cortex of T2DM (Fig. 2D). IκBα senses an inflammatory environment by undergoing phosphorylation followed by degradation, releasing NF-κB from its cytoplasmic location to translocate into the nucleus to initiate the transcription of genes involved in various processes of the immune and inflammatory response [15]. Therefore, the activation of NF-κB in the brain appears to be another inflammatory consequence in our T2DM mice. Western blot analysis of HIF-3α and PER2 did not reveal significant differences between control and T2DM mice in either brain structure (see Supplementary Fig. 3).
A RT-qPCR analysis of RNA levels of Hif-3α, Irf7, Per2, Xdh, Tsc22d3 and Cldn5 in the hippocampus and cortex of mice with T2DM. Upper row: Hippocampal RNA levels of CTL (n = 5) and T2DM (n = 5), one-tailed unpaired t-test: Hif-3α, *P = 0,0399; Irf7, **P = 0,0012; Per2, not significant; Xdh, *P = 0,0471; Tsc22d3; *P = 0,0484; Cldn5, *P = 0,0480. Lower row: Cortex RNA levels of CTL (n = 5) and T2DM (n = 5), one-tailed unpaired t-test: Hif-3α, *P = 0,0216; Irf7, **P = 0,0018; Per2, *P = 0,0108; Xdh, *P = 0,0170; Tsc22d3, *P = 0,0183; Cldn5, *P = 0,0208. B Immunoblotting of hippocampal extracts from T2DM and control mice with antibodies against CLDN5 (left, CTL n = 13, T2DM n = 15, unpaired t test, ****P < 0.0001, data normalized to the CTL group) and IRF7 (right, CTL n = 7, T2DM n = 11, unpaired t test, *P = 0.0385, data normalized to the CTL group). Note that all samples from T2DM mice exhibited reduced CLDN5 levels whereas not all -same- samples had high levels of IRF7. C Immunoblotting of cortex extracts from T2DM and control mice with antibodies against CLDN5 (left, CTL n = 11, T2DM n = 17 unpaired t test, *P = 0.032, data normalized to the CTL group) and IRF7 (right, CTL n = 13 T2DM n = 17, unpaired t test, not significant, data normalized to the CTL group). Note that all samples from T2DM mice exhibited reduced CLDN5 levels whereas not all -same- samples had high levels of IRF7. D Immunoblotting of hippocampal and cortical extracts from T2DM and control mice with an antibody against IkBα (hippocampus left panelf, CTL n = 10, T2DM n = 10, unpaired t test, *P = 0.0111, data normalized to the CTL group) and (cortex right panel, CTL n = 13, T2DM n = 16, unpaired t test, not significant (P = 0.069), data normalized to the CTL group). Note that like for IRF7 the changes in the cortex of mice with T2DM are clear compared to the control mice but without reaching significance.
Discussion
Our computational data analysis reveals that the alterations induced by T2DM in the cortex and hippocampus of mice align with the anticipated changes commonly observed in how this disease affects other organs in the body. In fact, the genes miss-regulated in these two structures are associated to alterations in vascular integrity/permeability, inflammation, metabolism, cellular stress, response to hypoxia, which typically occur in the course of diabetes [16, 17]. However, the observation that in addition to mRNA significant changes occur at the protein level for CLDN5 and IRF7 give to these two molecules a central role in the initiation of functional changes attributed to T2DM.
How could the loss of CLDN5 by T2DM then affect brain function? CLDN5 is a protein that plays a crucial role in the formation and maintenance of tight junctions between endothelial cells in various tissues, including the BBB and blood vessels [18, 19]. Since tight junctions are important for controlling the diffusion of molecules between cells and regulating the permeability of tissues [20, 21] it appears reasonable to claim that the reduced levels of CLDN5 would result in vascular endothelial dysfunction. This in turn would lead to increased vascular permeability, allowing molecules and cells to cross the blood vessel walls more easily triggering, among other consequences, the inflammatory response. Consistent with an scenario of high inflammatory activity, we observed reduced levels of IκBα in our T2DM mice, suggesting that the NF-κB -mediated inflammatory pathway is also activated [15]. Furthermore, the induction of an abnormal inflammatory environment in the brain of individuals with chronic T2DM is supported by the increased levels at the mRNA and protein level of IRF7. IRF7 belongs to the group of transcription factors that play important roles in the regulation of both innate and adaptive immune responses to pathogens, damaged cells, or irritants [22]. Activation of IRF7 is responsible for the expression of Type I Interferons (INFs), which play both positive and negative roles. On the positive side, INFs play a critical role in the body’s defense against viruses by stimulating the immune system, inhibiting viral replication, and activating immune cells to eliminate infected cells. While IRF7 is not reported to directly cause cell damage, overactivation of IRF7 could contribute to cell damage and tissue injury through the production of excessive amounts of interferons and other inflammatory molecules by a process known as “interferonopathies”. In line with this notion, our T2DM mice exhibited increased mRNA levels of Irf9 (Interferon regulatory factor 9) and Ifit1 (Interferon-induced protein with tetratricopeptide repeats 1) (refer to Fig. 1A). In fact, while Irf9 also participates in the regulation of Interferon1 activation [23], Ifit1 is a member of the IFIT member of the interferon-stimulated genes [24].
At this point, we believe it is worth clarifying that while the inflammatory response predicted by both the increase in IRF7 and the decrease in IκBα may result from the diffusion of circulating cells and small molecules into the brain, it is also plausible that the inflammatory response could be a consequence of microorganisms that have escaped their natural niches and now invade the brain. Supporting this scenario is the fact that upregulation of Irf7, Irf9, and Ifit1 is part of the molecular machinery activated in defense against viral infections [22,23,24]. Additionally, it is well-established that diabetes can induce dysbiosis and disrupt the cellular barriers that ordinarily confine pathogens within their native niches [25]. More work is needed to identify the determinant of the increased inflammatory activity in the T2DM setting.
In conclusion, our data is in line with the notion that vascular alterations are among the initial effects of T2DM on the brain, achieved through the downregulation of the tight junction protein CLDN5. Further work is required to determine whether CLDN5 decreases as a consequence of the effect of hyperglycemia, for example through affecting the expression of particular microRNAs [26] or through the activation of inflammatory mechanisms [27]. The fact that all T2DM mice have low levels of CLDN5 in cortex and hippocampus but not all have elevated levels of IRF7 (see Fig. 2B, C) would be more consistent with the first possibility. In any case, in addition to the mechanistic interpretation, our work opens the possibility of targeting INFs and NF-kβ pathways to prevent the onset and progression of cognitive defects in individuals with T2DM.
Data availability
All data supporting the findings of this study are available from the corresponding authors upon request. The Illumina paired end reads (FASTQ) generated for this study are available at The European Nucleotide Archive (ENA; http://www.ebi.ac.uk/ena/). The RNA raw sequencing data from mouse cortex in control conditions were previously submitted with the study accession number PRJEB61249 and used in another study. Mouse hippocampus RNA raw sequencing data in control and High fat diet/Steprotozotocin conditions have been deposited under the study accession number PRJEB61724 (https://www.ebi.ac.uk/ena/browser/view/PRJEB61724). The dataset pertaining to the High-fat diet/Streptozotocin conditions in the mouse cortex was also submitted under this same study.
References
Biessels GJ, Despa F. Cognitive decline and dementia in diabetes mellitus: mechanisms and clinical implications. Nat Rev Endocrinol. 2018;14:591–604.
Brands AMA, Van den Berg E, Manschot SM, Biessels GJ, Kappelle LJ, De Haan EHF, et al. A detailed profile of cognitive dysfunction and its relation to psychological distress in patients with type 2 diabetes mellitus. J Int Neuropsychol Soc. 2007;13:288–97.
Carús-Cadavieco M, Berenguer López I, Montoro Canelo A, Serrano-Lope MA, González-de la Fuente S, Aguado B, et al. Cognitive decline in diabetic mice predisposed to Alzheimer’s disease is greater than in wild type. Life Sci Alliance. 2023;6:e202201789.
Wahlin A, Nilsson E, Fastbom J. Cognitive performance in very old diabetic persons: the impact of semantic structure, preclinical dementia, and impending death. Neuropsychology. 2002;16:208–16.
Antal B, McMahon LP, Sultan SF, Lithen A, Wexler DJ, Dickerson B, et al. Type 2 diabetes mellitus accelerates brain aging and cognitive decline: complementary findings from UK Biobank and meta-analyses. eLife. 2022;11:e73138.
Furman BL. Streptozotocin-induced diabetic models in mice and rats. Curr Protoc Pharm. 2015;70:5.47.1–5.47.20.
Johnson MS, Ryals JM, Wright DE. Diabetes-induced chemogenic hypoalgesia is paralleled by attenuated stimulus-induced fos expression in the spinal cord of diabetic mice. J Pain. 2007;8:637–49.
Johnson MS, Ryals JM, Wright DE. Early loss of peptidergic intraepidermal nerve fibers in an STZ-induced mouse model of insensate diabetic neuropathy. Pain. 2008;140:35–47.
Palomer E, Martín-Flores N, Jolly S, Pascual-Vargas P, Benvegnù S, Podpolny M, et al. Epigenetic repression of Wnt receptors in AD: a role for Sirtuin2-induced H4K16ac deacetylation of Frizzled1 and Frizzled7 promoters. Mol Psychiatry. 2022;27:3024–33.
Neely CLC, Pedemonte KA, Boggs KN, Flinn JM. Nest building behavior as an early indicator of behavioral deficits in mice. J Vis Exp. 2019:e60139.
Rodgers RJ. Animal models of “anxiety”: where next? Behav Pharm. 1997;8:477–96.
Figueiredo VC, Markworth JF, Cameron-Smith D. Considerations on mTOR regulation at serine 2448: implications for muscle metabolism studies. Cell Mol Life Sci CMLS. 2017;74:2537–45.
Boucher J, Kleinridders A, Kahn CR. Insulin receptor signaling in normal and insulin-resistant states. Cold Spring Harb Perspect Biol. 2014;6:a009191.
Ardestani A, Lupse B, Kido Y, Leibowitz G, Maedler K. mTORC1 signaling: a double-edged sword in diabetic β cells. Cell Metab. 2018;27:314–31.
Liu T, Zhang L, Joo D, Sun SC. NF-κB signaling in inflammation. Signal Transduct Target Ther. 2017;2:17023.
Rhea EM, Leclerc M, Yassine HN, Capuano AW, Tong H, Petyuk VA, et al. State of the science on brain insulin resistance and cognitive decline due to Alzheimer’s disease. Aging Dis. 2023.
Willette AA, Xu G, Johnson SC, Birdsill AC, Jonaitis EM, Sager MA, et al. Insulin resistance, brain atrophy, and cognitive performance in late middle-aged adults. Diabetes Care. 2013;36:443–9.
Chiba H, Ichikawa-Tomikawa N, Imura T, Sugimoto K. The region-selective regulation of endothelial claudin-5 expression and signaling in brain health and disorders. J Cell Physiol. 2021;236:7134–43.
Greene C, Hanley N, Campbell M. Claudin-5: gatekeeper of neurological function. Fluids Barriers CNS. 2019;16:3.
Xu L, Nirwane A, Yao Y. Basement membrane and blood-brain barrier. Stroke Vasc Neurol. 2019;4:78–82.
Lochhead JJ, Yang J, Ronaldson PT, Davis TP. Structure, function, and regulation of the blood-brain barrier tight junction in central nervous system disorders. Front Physiol. 2020;11:914.
Qing F, Liu Z. Interferon regulatory factor 7 in inflammation, cancer and infection. Front Immunol. 2023;14:1190841.
Suprunenko T, Hofer MJ. The emerging role of interferon regulatory factor 9 in the antiviral host response and beyond. Cytokine Growth Factor Rev. 2016;29:35–43.
Diamond MS, Farzan M. The broad-spectrum antiviral functions of IFIT and IFITM proteins. Nat Rev Immunol. 2013;13:46–57.
Lau WL, Tran T, Rhee CM, Kalantar-Zadeh K, Vaziri ND. Diabetes and the gut microbiome. Semin Nephrol. 2021;41:104–13.
Kujawa M, O’Meara M, Li H, Xu L, Meda Venkata SP, Nguyen H, et al. MicroRNA-466 and microRNA-200 increase endothelial permeability in hyperglycemia by targeting Claudin-5. Mol Ther Nucleic Acids. 2022;29:259–71.
Haruwaka K, Ikegami A, Tachibana Y, Ohno N, Konishi H, Hashimoto A, et al. Dual microglia effects on blood brain barrier permeability induced by systemic inflammation. Nat Commun. 2019;10:5816.
Acknowledgements
The next-generation sequencing (NGS) data analysis has been performed by the Genomics and NGS Core Facility at the Centro de Biología Molecular Severo Ochoa (CBM, CSIC-UAM).
Funding
This work was partially supported by grants PID2019-104389RB-I00 and PID2022-138334OB-I00 funded by MCIN/AEI/ 10.13039/501100011033, “ERDF/FEDER A way of making Europe” and by the European Union NextGenerationEU/PRTR CSIC’s Interdisciplinary Thematic Platform PTI + NEURO-AGING, to CGD and by European Union JPND “EpiAD” Grant to CGD. This work was partially supported by grants PID2022-137384OA-I00 and RYC2021-031713-I funded by MCIU/AEI to EP.
Author information
Authors and Affiliations
Contributions
CGD and EP designed the overall approach, coordinated the study and drafted the manuscript. MCC and IBL did all biological studies. MSL participated in the T2DM induction and in the behavioral tests. SGdF carried out the gene expression and pathway analysis. BA supervised all systems biology studies. FXG gave experimental and conceptual supervision and helped prepare the manuscript. All authors read and approved the final manuscript.
Corresponding authors
Ethics declarations
Competing interests
The authors declare no competing interests.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary information
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution-NonCommercial-NoDerivatives 4.0 International License, which permits any non-commercial use, sharing, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if you modified the licensed material. You do not have permission under this licence to share adapted material derived from this article or parts of it. The images or other third party material in this article are included in the article’s Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article’s Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by-nc-nd/4.0/.
About this article
Cite this article
Carús-Cadavieco, M., González de la Fuente, S., Berenguer López, I. et al. Loss of Cldn5 -and increase in Irf7-in the hippocampus and cerebral cortex of diabetic mice at the early symptomatic stage. Nutr. Diabetes 14, 64 (2024). https://doi.org/10.1038/s41387-024-00325-y
Received:
Revised:
Accepted:
Published:
DOI: https://doi.org/10.1038/s41387-024-00325-y
- Springer Nature Limited