Abstract
Neurotrophin signaling modulates the differentiation and function of mature blood cells. The expression of neurotrophin receptors and ligands by hematopoietic and stromal cells of the bone marrow indicates that neurotrophins have the potential to regulate hematopoietic cell fate decisions. This study investigates the role of neurotrophins and Tropomyosin receptor kinases (Trk) in the development of megakaryocytes (MKs) and their progeny cells, platelets. Results indicate that primary human MKs and MK cells lines, DAMI, Meg-01 and MO7e express TrkA, the primary receptor for Nerve Growth Factor (NGF) signaling. Activation of TrkA by NGF enhances the expansion of human MK progenitors (MKPs) and, to some extent, MKs. Whereas, inhibition of TrkA receptor by K252a leads to a 50% reduction in the number of both MKPs and MKs and is associated with a 3-fold increase in the production of platelets. In order to further confirm the role of TrkA signaling in platelet production, TrkA deficient DAMI cells were generated using CRISPR-Cas9 technology. Comparative analysis of wild-type and TrkA-deficient Dami cells revealed that loss of TrkA signaling induced apoptosis of MKs and increased platelet production. Overall, these findings support a novel role for TrkA signaling in platelet production and highlight its potential as therapeutic target for Thrombocytopenia.
Similar content being viewed by others
Introduction
Platelets, the smallest cellular component of circulating blood, are critically involved in hemostasis, thrombosis, and inflammation1,2,3,4. Diverse pathological conditions impact platelet production and/or clearance leading to aberrant platelet counts, which pose health risks due to severe hemorrhage, thrombus formation, or impaired immune response2,5,6,7,8. Current therapies for managing these abnormalities are neither time- nor cost-effective, and other conditions, such as infection and alloimmunization, limit their efficacy6,9,10,11. Cell-based approaches aiming at ex vivo platelet production are promising but necessitate further research for optimization12,13. In order to develop efficacious therapies, it is crucial to gain a better understanding of the molecular mechanisms underlying platelet production (thrombopoiesis).
Thrombopoiesis is a multistage process requiring megakaryocyte (MK) maturation and fragmentation in the bone marrow (BM), triggered by an array of growth factors and cytokines14,15,16,17,18. Neurotrophins are among the growth factors expressed in the bone marrow and act by binding tropomyosin receptor kinases (Trks) and/or the low affinity receptor p75NTR19. Of those, nerve growth factor (NGF) binds more specifically to TrkA, brain-derived neurotrophic factor (BDNF) and neurotrophin-4/5 (NT-4/5) to TrkB, and neurotrophin-3 (NT3) to TrkC20. Ligand binding to Trks is followed by receptor dimerization, phosphorylation of the intracellular domain via intrinsic kinase activity, and recruitment of different adaptor and effector proteins, which transmit the trophic message to downstream signaling molecules19. The receptor-mediated neurotrophic message is then converted to diverse cellular outcomes with the activation of PI3K (Phosphatidylinositol-3 kinase), phospholipase C gamma (PLC-γ), and MAPK pathways19.
Neurotrophins are essential factors for survival, proliferation, and differentiation of both neuronal and non-neuronal cells21,22,23,24. Previous studies have shown that neurotrophins and their receptors are expressed by both mature and immature cells of the hematopoietic system25,26,27,28,29. Although the role of neurotrophins, more specifically NGF/TrkA, in mature blood cells has been widely explored30,31,32,33,34,35,36,37,38,39,40,41, their functions in hematopoietic stem and progenitor cells are poorly understood. Several megakaryocytic cell lines (Meg-01, K562) are known to express TrkA42. When given in combination with sodium butyrate, an inducer of megakaryocytic differentiation, NGF promotes the commitment of K562 cells to the megakaryocytic lineage43. Treatment of erythroleukemic and megakaryocytic cell lines (HEL, Meg-J, CMK, and M07e) with a Trk receptor inhibitor, K252a, induces polyploidization and increases MK differentiation markers44,45,46,47. Despite the limited reports indicating a role for the neurotrophin pathway in MK development, actions of neurotrophins in subsequent platelet formation has not been elucidated. In this study, we aimed to investigate the undefined role of neurotrophin signaling in MK differentiation and platelet production. We utilized both primary cell culture and a cell line model to examine the megakaryopoietic and thrombopoietic aspects of neurotrophins, specifically NGF/TrkA signaling. Besides ligand or inhibitor-mediated modulation of TrkA, we also established TrkA-knockout DAMI cells via CRISPR-Cas9 system (clustered regularly interspaced short palindromic repeats-CRISPR associated protein 9 nuclease) to further confirm the involvement of TrkA in platelet production. Data from this study indicate that neurotrophin signaling has a bimodal role in megakaryopoiesis and thrombopoiesis. Signaling through TrkA supports megakaryopoiesis by inducing MK progenitor expansion and MK survival but subsequently suppresses MK maturation and fragmentation into platelets.
Materials and Methods
Reagents and antibodies
Recombinant human thrombopoietin (rhTPO), interleukin I-beta (rhIL-1β), interleukin 6 (rhIL-6), stem cell factor (rhSCF), nerve growth factor beta (rhNGF-β), and granulocyte-macrophage colony stimulating factor (rhGM-CSF) were purchased from R&D systems (Minneapolis, MN, USA). K252a was purchased from Calbiochem (San Diego, CA, USA). The following fluorochrome-conjugated anti-human antibodies were used for flow cytometry analysis: FITC-labelled human lineage cocktail 4 (CD2, CD3, CD4, CD7, CD8, CD10, CD11b, CD14, CD19, CD20, CD56, CD235a), Sca-1-FITC, CD34-PE Cy7, CD41-APC, TrkA-PE (all from BD Pharmingen, San Diego, CA, USA), CD61-AF 647 were obtained from Biolegend (San Diego, CA, USA). The nuclear dyes, 7-Aminoactinomycin D (7-AAD) and propidium iodine (PI), were also from BD Pharmingen.
Cell lines and culture
Unless otherwise stated, all cell lines used in this study were cultured in media containing 10% fetal bovine serum (FBS), 2 mM glutamine, and 1% penicillin-streptomycin-gentamicin (PSG), and maintained at 37 °C in a 5% CO2 humidified atmosphere. Specifically, Meg-01, M07e, and Dami cells were obtained from Dr. Richard Phipps (University of Rochester Medical Center, Rochester, NY, USA) and cultured in RPMI 1640 (Roswell Park Memorial Institute Medium). 10 ng/ml rhGM-CSF was used to induce proliferation of M07e cells. Human embryonic kidney (HEK 293 T) cells were obtained from Invitrogen/Life Technologies (Grand Island, NY, USA), and cultured in Dulbecco’s Modified Eagle Medium (DMEM).
Ex vivo differentiation of primary human megakaryocytes
CD34+ cells derived from BM or umbilical cord blood were purchased from Allcells (Emeryville, CA, USA), and differentiated as previously described48. For inducing MK progenitor (MKP) cell differentiation and expansion, CD34+ cells were cultured for 7 days in Iscove’s modified Dulbecco media (IMDM, Invitrogen/Life Technologies) containing 20% BIT 9500 (Stem Cell Technologies, Tukwila, WA, USA), 0.8% low density lipoprotein (LDL, L-8292, Sigma-Aldrich Corp., St. Louis, MO, USA), 100 ng/mL rhTPO, 10 ng/mL rhIL-1β, 10 ng/mL rhIL-6, and 50 ng/mL rhSCF. At day 7, cells were plated in fresh media without rhSCF, and either used for experiments or further cultured for 7 days to differentiate into MKs.
Immunoblotting assay
Protein lysates were prepared as previously described49. Protein content was quantified by Bradford assay, and samples were separated in 7.5% sodium dodecyl sulfate-polyacrylamide gel electrophoresis (SDS-PAGE). Proteins were electrophoretically transferred onto Hybond ECL nitrocellulose membrane (GE Healthcare Bio-Sciences Corporation, Piscataway, NJ, USA), and incubated with primary antibodies raised against human TrkA (sc-118, 1:1000), TrkB (sc-20542, sc-12, 1:1000), TrkC (sc-14025, sc-117, 1:1000), p75NTR (sc-8317, 1:1000), phospho-Trk (Tyr680/Tyr681, sc-7996-R, 1:1000), Erk1 (sc-94, 1:1000), phospho-Erk (sc-7383, 1:1000), α-tubulin (sc-8035, 1:1000; all from Santa Cruz Biotechnologies Inc., Santa Cruz, CA, USA), Akt (9272, 1:2000), and phospho-Akt (4060, 1:2000, all from Cell Signaling Technology, Danvers, MA, USA). Species-specific infrared secondary antibodies (Li-Cor Biosciences, Lincoln, NE) were used to detect bound antibodies, followed by visualization using Li-Cor Odyssey Infrared Imaging System. Densitometry was performed using Image Studio Lite software (Li-Cor Biosciences).
Reverse transcriptase polymerase chain reaction (RT-PCR)
Total RNA was extracted from cells using Trizol reagent according to the manufacturer’s instructions (Ambion/Life Technologies, Carlsbad, CA, USA). 1 µg RNA was DNAse I-treated (Invitrogen/Life Technologies, Carlsbad, CA, USA) and subjected to cDNA synthesis by iScript cDNA synthesis kit (Biorad, Hercules, California, USA). Primer pairs listed in Table 1 were used to amplify the cDNA of human TrkA, TrkB, TrkC, p75NTR, NGF, and GAPDH. Trk, tropomyosin receptor kinase; p75NTR, p75 neurotrophin receptor; GAPDH, glyceraldehyde 3-phosphate dehydrogenase; sgTrkA, single guide RNA for TrkA; ssODN, single-stranded oligodeoxynucleotide.
Flow cytometric analysis of megakaryocytes, megakaryocyte progenitors, and culture-derived platelets
Dami cells were plated at 1 × 105 cells in 1 ml media per well in a 24-well plate and incubated for 72 h under the specified treatment conditions (200 ng/ml rhNGF-β; 200 nM K252a). At the indicated time points, cells were homogenously mixed and 50 µl of cell suspension was stained first with anti-human CD61-AF 647 antibody for 20 min followed by staining with 7-AAD for 10 min at room temperature (RT). Absolute counts of MKs and platelet-like particles (PLPs) in 10 µl volume were quantified using a Accuri C6 flow cytometer (BD Biosciences, CA, USA) as previously described48. Data were analyzed using FlowJo software (TreeStar, Ashland, OR, USA). CD61+ 7-AAD− Dami cells are designated as intact MKs. PLPs are distinguished as CD61+ 7-AAD− cells falling into the gate based on forward and side scatter of human whole blood platelets50. To normalize well-to-well variation, PLP counts were calculated as PLP per MK.
For detection of ex vivo differentiated MKPs and MKs, cells were seeded at 1 × 105 cells/ml media (IMDM, 10% BIT 9500, rhIL-6, rhIL-1β, 100 ng/ml rhTPO, 0.8% LDL) into a 24-well plate. At the indicated time points, cells were homogenously mixed, 350 µl of cell suspension was transferred from each well into two separate tubes, and stained for culture-derived MKPs/MKs and platelets. After staining, cells were washed with PBS and resuspended in 50 µl volume. Using Accuri C6, absolute cell count in 10 µl was determined. Following compensation, unstained cells and fluorescence minus one controls were used to properly gate each cell type. Using FITC-labelled human lineage cocktail and anti-human Sca-1 antibodies, Lin- Sca-1− cells were selected. Among those, CD34+ CD41+ cells were gated as MKPs and CD34−CD41+ cells were identified as MKs. Culture-derived platelets were detected by CD61+ PI- staining in the size gate of human platelets and platelet per MK counts were used for evaluation.
Cell cycle analysis
Cell cycle analysis was performed using a FITC-BrdU Flow Kit (BD Biosciences, CA, USA). Briefly, serum starvation (1 h) was performed for synchronization of cells at G0/G1 phase. Cells were subsequently split at 2.05 × 105 in 0.5 ml media (RPMI with 10% FBS and 1% PSG) in a 48-well plate and cultured 24 h. Cells were pulsed with 5 µl BrdU (1 mM) for 30 min prior to the end of 24 h incubation, then processed according to the manufacturer’s protocol. After flow cytometric acquisition, cell fractions at S, G0/G1, and G2/M phases were determined based on the intensities of anti-BrdU-FITC and total nuclear dye, 7-AAD.
Apoptosis assay
Annexin V-PE 7-AAD Apoptosis Kit from BD Biosciences was used to determine Annexin V+ early and late apoptotic cells. Briefly, 1 × 105 cells were immunostained with both Annexin V-PE and cell impermeable nuclear dye, 7-AAD following the manufacturer’s instructions. Sample analysis was performed in Accuri C6 flow cytometer by acquiring 10,000 events/sample. Annexin V+ 7-AAD− cells were considered early apoptotic cells while double positive cells were considered late apoptotic cells. Annexin V− 7-AAD + cells were considered dead.
Generation of TrkA deficient cells by CRISPR
These were generated by employing CRISPR technology51. Briefly, oligos for TrkA guide RNA (sgTrkA forward and reverse, Table 1) were designed to contain 20 nucleotides (NG_007493: 50324-50344 nucleotides) with a 5′-GGG protospacer adjacent motif (PAM) located in exon 1 of TrkA and 5′ flanking sequence complementary to a BbsI precut vector. Oligos were purchased from Integrated DNA Technologies (Coralville, IA, USA), annealed, and cloned into the pSpCas9 (BB)-2A-GFP plasmid (Addgene, #48138) as described by Ran et al.51. This system allows for the coexpression of sgTrkA and Cas9 from a single construct and use of Enhanced Green Fluorescent Protein (EGFP) as a reporter. Dami cells were nucleofected with the CRISPR construct along with the repair template (TrkA ssODN Primer 1 and 2 in Table 1) using Nucleofection Kit C and the X-05 program settings in Amaxa Nucleofector I device (Lonza/Amaxa Biosystems, Cologne, Germany), according to the manufacturer’s instructions. Nucleofected cells were then seeded into a 12-well plate containing 1.5 ml complete media and cultured for 24 h prior to sorting.
For fluorescence-activated cell sorting (FACS), GFP-positive Dami cells were sorted using a 130 µm nozzle at BD FACSAria™ Cell Sorting System. Sorted cells were cultured for 24 h and seeded in a 96-well plate by serial limiting dilution. Single cell colonies were grown, expanded, and pre-screened for the presence of expected nucleotide change by Restriction Fragment Length Polymorphism Analysis of PCR-Amplified Fragments (PCR-RFLP). For this purpose, the region flanking the mutation site in TrkA DNA sequence was PCR-amplified using TrkA-RFLP forward and reverse primers (Table 1). Resultant 201 nucleotide base pair PCR product was subjected to XmaI digestion. Uncleaved band following XmaI digestion indicated successful deletion of the guanine nucleotide. Clones preselected by PCR-RFLP were further sequenced for validation.
Statistical analysis
Statistical analysis was performed using Graphpad Prism Software (La Jolla, CA, USA). Student’s t test was used to compare means of two groups. Data from multiple groups were analyzed by one-way analysis of variance (ANOVA) or two-way ANOVA, where appropriate, and followed by Bonferroni test for multiple comparisons. Results were represented as mean ± standard error of means (SEM). P values equal or lower than 0.05 were considered statistically significant.
Results
Neurotrophin receptors are expressed both in primary human megakaryocytes and megakaryocytic cell lines
First, we characterized the expression of neurotrophin receptors in primary human MKs and several MK cell lines. Primary human MKs were obtained by ex vivo differentiation of umbilical cord blood-derived CD34+ cells with a two-stage culture method. Human megakaryocytic cell lines Meg-01, M07e, and Dami, represent different stages of MK differentiation. Although TrkA expression of human CD34+ cells and Meg-01 cells has been previously reported25,28,42, we performed a comprehensive expression analysis for the neurotrophin receptors TrkA, TrkB, TrkC, and p75NTR in primary MKs and MK cell lines. HEK293T cells were used as a positive control since a previous report from our group and the current study revealed endogenous expression of all neurotrophin receptor subtypes in HEK293Ts52. Immunoblot (Fig. 1a) and non-quantitative RT-PCR (Fig. 1b) analysis demonstrated that TrkA is the common isoform expressed by both MK cell lines and primary MKs, whereas TrkC was only expressed in the MK cell lines. Primary MKs showed a protein smear for p75NTR, however we were unable to detect any RNA for it by RT PCR. Furthermore, TrkB expression was not detected in primary MKs (Fig. 1a). Since TrkA is the only neurotrophin receptor subtype expressed in both normal human MKs and human MK cell lines, we focused on the NGF-TrkA signaling axis for the remainder of this study.
Neurotrophin receptors are expressed both in human primary MKPs, MKs and MK cell lines. (a) Human umbilical cord blood-derived CD34+ cells were differentiated in a suspension culture containing IMDM, 20% BIT 9500, 8% Low Density Lipoprotein, 100 ng/mL rhTPO, 10 ng/mL rhIL-1β, 10 ng/mL rhIL-6, for 7 days with 50 ng/mL rhSCF, and another 7 days without rhSCF. At day 14, the final MK-rich (73%) cell suspension was used to prepare total RNA and protein lysates. Protein lysates were also made from Dami, meg-01 and MO7e cell lines. HEK293T cells were used as a positive control due to endogenous expression of all neurotrophin receptor types. At least 30 µg protein from each cell type was resolved via SDS-PAGE and subjected to immunoblotting assays for the indicated proteins. The blot shown is representative of three experiments. (b) Non-quantitative, reverse transcriptase PCR was used to detect the expression of neurotrophin receptors in ex vivo differentiated human MKs and MK cell lines. Glyceraldehyde 3-phosphate dehydrogenase (GAPDH) mRNA was amplified to normalize the neurotrophin receptor expression level. The results shown are representative of three independent experiments. (c) Human bone-marrow derived CD34+ cells were differentiated ex vivo for 7 days in the presence of IMDM, 20% BIT 9500, 8% Low Density Lipoprotein, 100 ng/mL rhTPO, 10 ng/mL IL-1β, 10 ng/mL rhIL-6, and 50 ng/mL rhSCF. The Day 7 culture containing 38% MKPs (Lin-CD34+CD41+) and 23.7% MKs (Lin-CD34−CD41+) was analyzed for TrkA surface expression by flow cytometry. Graphs of fluorescence minus one control for TrkA staining are shown as staining controls for TrkA antibody. The data shows the presence of TrkA expression in both MKPs (20.1%) and MKs (20.8%). All treatments were done in triplicates in each experiment and data are representative of two independent experiments.
To further explore the distribution of TrkA in immature MKPs and MKs, human BM-derived CD34+ cells were differentiated in MKP expansion media. After a 7-day culture, cells were subsequently analyzed for TrkA expression via flow cytometry, where MKP (38%) and MK (23.7%) cells were initially delineated by CD34 and CD41 expression (Fig. 1c). We ultimately observed that 20.8% of MKs and 20.1% of MKPs have surface expression of TrkA.
NGF/TrkA signaling supports MKP expansion but blocks platelet production
Since TrkA was found to be expressed on MKPs and MKs, we next examined whether NGF-induced TrkA signaling has a functional role in expansion and differentiation of MK lineage cells. For this purpose, a mixture of culture-derived MKPs and MKs was generated from human BM-derived CD34+ cells and seeded in a multi-well plate containing serum-free medium supplemented with TPO, IL-6, IL-1β, and hLDL. Cells were cultured for 72 h in the presence of NGF or K252a. Absolute counts of MKPs and MKs were assessed by flow cytometry. As demonstrated in Fig. 2a, NGF treatment significantly enhanced the expansion of MKPs (p < 0.01) compared to control, however had no effect on MK counts (Fig. 2b). In contrast, treatment with K252a, alone or in combination with NGF, significantly reduced the number of both MKPs (p < 0.001, Fig. 2a) and MKs (p < 0.0001, Fig. 2b).
NGF/TrkA signaling supports the expansion of MKPs but blocks platelet production. Human MKPs and MKs differentiated from BM-derived CD34+ cells were plated in a medium containing 100 ng/mL rhTPO, 10 ng/mL rhIL-1β, 10 ng/mL rhIL-6 and treated with both NGF (200 ng/ml) and K252a (200 nM), alone and in combination. The control cultures were treated with phosphate-buffered saline (PBS). Following 72 h incubation, 350 µl cell suspension was stained with antibodies against MK lineage-specific markers, and each sample was analyzed for MKP, MK, and platelet-like particle counts by flow cytometry. The addition of NGF to the cytokine cocktail led to further expansion of MKPs (a) and a slight increase in MK (b) counts, but did not induce a significant change in CD41 surface expression among neither CD34+ (c) nor CD34- (d) cells comprising MKPs and MKs, respectively In contrast, K252a treatment caused a decline in both MKP (a) and MK (b) counts while decreasing their CD41 expression (c,d). Panels (c and d) also show histogram plot from one representative experiment. (f) NGF did not alter platelet per MK yield whereas K252a augmented platelet production. All treatments were done in triplicates in each experiment and data are representative of two independent experiments. Results presented are the mean ± SEM and analyzed by one-way ANOVA, **p < 0.01, ***p < 0.001, ****p < 0.0001. n.s. denotes statistically not significant.
The increase in MKP numbers following NGF stimulation might be a result of commitment of early progenitors to MK lineage, or increased clonal expansion of lineage committed cells. In order to assess this possibility, we analyzed the surface expression of CD41 among CD34+ cell population (Fig. 2c), which is a lineage-specific marker upregulated during MK differentiation. While, NGF treatment alone did not significantly increase the median fluorescence intensity (MFI) of CD41 in MKPs (Fig. 2c), MKPs generated in presence of K252a alone (p < 0.05) or NGF and K252a combination (p < 0.05) showed significantly decreased levels of CD41 expression compared to control or DMSO In addition, CD41 MFI among CD34− cells (Fig. 2d) encompassing MKs was not altered by NGF however it was significantly reduced by K252a treatment (K252a vs DMSO, p < 0.01; NGF + K252a vs DMSO, p < 0.001). Altogether, these results suggest that inhibition of TrkA signaling by K252a supports clonal expansion of MKPs but does not promote MK lineage commitment. K252a-mediated reduction in CD41 MFI among CD34+ and CD34− cells indicates that TrkA-mediated signaling is important for preservation of MK lineage markers.
Lastly, we examined whether TrkA signaling impacts platelet production from ex vivo differentiated MKs. We therefore quantified the culture-derived platelet content in the aforementioned treatment conditions. We did not observe any change in the number of platelets with NGF at 72 h (Fig. 2e). However, K252a either alone (p < 0.0001), or in combination with NGF (p < 0.0001), resulted in a 3-fold increase in platelet generation. It should be noted that the indolocarbazole K252a inhibits tyrosine kinase activity or TrkA regardless of its binding to NGF53. Collectively, these results strongly suggest that inhibition of TrkA signaling promotes thrombopoiesis.
Dami cells serve as a model to study TrkA signaling
As our work with primary MK cultures indicated that TrkA signaling differentially modulates megakaryopoiesis and subsequent thrombopoiesis (Fig. 2), we were prompted to further investigate the regulatory role of TrkA-mediated signaling in these two processes. We performed subsequent mechanistic studies in Dami cells, which express TrkA (Fig. 1) and serve as a useful in vitro model to study MK differentiation and platelet production54,55.
We first assessed the functionality of TrkA receptors in Dami cells by performing short-term NGF exposure. Dami cells were subjected to serum withdrawal for 1 h, then exposed to NGF (200 ng/ml) for 5 min in serum free conditions. Whole cell lysates were generated and subsequently probed with total and phosphoprotein-specific antibodies against TrkA and Akt. 5 min NGF exposure induced the tyrosine phosphorylation of TrkA at Tyr680/Tyr681 (Tyr674/Tyr675 on human TrkA isoform) (Fig. 3a). Moreover, phosphorylation of TrkA was associated with the activation of PI3K/Akt, which is a common downstream mediator of TrkA signaling (Fig. 3b)19. As expected, Akt phosphorylation was abrogated by 1 h pretreatment with LY294002 (50 µM), a PI3K inhibitor (Supplementary Fig. 2d). In contrast, 15 min pretreatment with K252a (200 nM) blocked the phosphorylation of TrkA (Fig. 3a) and Akt (Fig. 3b) both, suggesting that the inhibition of TrkA activity by K252a also results in attenuation of downstream signaling events.
Dami cells serve as a model to study TrkA signaling. Dami cells were subjected to 1 h serum starvation and pre-treated with 200 nM of K252a, a Trk inhibitor, for 15 min prior to the end of 1 h incubation. Then cells were incubated with 200 ng/ml rhNGF for 5 min. Total cell extracts were obtained and analyzed by immunoblotting using the indicated antibodies. Representative immunoblotting images show the NGF-induced phosphorylation of (a) TrkA (Tyr680/Tyr681, 140 kD) and simultaneous phosphorylation of downstream (b) Akt (Ser473, 60 kD). 15 min pre-treatment of Dami cells with 200 nM K252a, a Trk inhibitor, blocks the phosphorylation of both (a) TrkA and downstream (b) Akt proteins. Densitometric analysis for TrkA and Akt levels were expressed as the ratio of phosphorylated form to total protein normalized by α-tubulin. The bar graphs show the data as the mean fold change ± SEM of immunoblot images from three independent experiments. Data were analyzed by one-way ANOVA (a,b). *p < 0.05, ***p < 0.001, ****p < 0.0001. (c) Dami cells were seeded at a density of 1 × 105 cells/ml in RPMI 1640, containing 5% FBS, 1% PSG, and then treated with 200 ng/ml rhNGF and 200 nM K252a, both alone or in combination. DMSO served as a vehicle control for K252a. The treatments were terminated at 48 h and 50 µl cell suspension was stained with anti-human CD61-AF647 antibody and nuclear dye, 7-AAD. Counts of intact Dami cells (7-AAD−CD61+) and platelet-like particles (7-AAD−CD61+) in 10 µl volume were determined by flow cytometry. Platelet-like particle counts were normalized by the number of MKs measured in each sample volume. Measures of total MK counts revealed a slight increase with NGF (statistically not significant.) and a significant decrease in the presence of K252a. (d) Inversely correlated with decreased MK counts in K252a-containing culture, platelet-like particle counts showed a statistically significant increase following exposure to K252a for 48 h. Data in (c,d) were analyzed by one-way ANOVA; (*p < 0.05, ****p < 0.0001).
Next, we investigated the effect of NGF or K252a treatment on Dami cells in order to validate that Dami cells recapitulate the response observed in primary human MKs (Fig. 2b). Dami cells were seeded in a multi-well plate containing RPMI with 5% FBS and cultured for 48 h with the respective treatments. Flow cytometric analysis showed that similar to our observations in primary MK culture, NGF did not affect Dami cell counts, whereas K252a caused approximately 3-fold decrease in cell count (p < 0.0001) at 48 h (Fig. 3c). In addition, K252a induced a significant increase (~2–4 fold) in platelet-like particle counts compared to DMSO control at 48 h (p < 0.0001, Fig. 3d). Based on these findings, we concluded that Dami cells have functional TrkA receptors which can be modulated through inhibitions of TrkA phosphorylation by K252a and that these cells recapitulate the response we observed in primary MKs after activation or inhibition of TrkA signaling.
Inhibition of TrkA signaling by K252a promotes platelet production by inducing cell cycle arrest and apoptosis in Dami cells
During thrombopoiesis, MKs undergo endomitosis, followed by proplatelet/platelet production and subsequent apoptosis. Since, inhibition of TrkA signaling by K252a leads to increased PLP production, we sought to analyze cell proliferation and survival in Dami cells under those treatment conditions. Through flow cytometric analysis of BrdU incorporation and total DNA staining, we determined that K252a treatment arrests the cell cycle at G0/G1 and G2/M phases (Fig. 4a), which leads to a 50% reduction in the percentage of actively proliferating cells (p < 0.0001, Fig. 4b). Furthermore, K252a treatment elevated the frequency of total Annexin V+ cells, which is indicative of early and late apoptotic cells (p < 0.05 for DMSO vs K252a, Fig. 4c). Collectively, these data suggest that TrkA inhibition by K252A indeed drives MK cells towards decreased cell proliferation, cell survival, leading to higher levels of platelet production.
Inhibition of TrkA signaling by K252a causes cell cycle arrest and increased apoptosis in Dami cells. (a,b) Cell cycle analysis was performed by seeding 2.5 × 105 cells in a 48-well plate after 1 h serum starvation and pulsing them with BrdU for 30 min prior to the end of 24 h incubation. After staining with anti-BrdU-FITC and total DNA dye, 7-AAD, cells were analyzed by flow cytometry. BrdU-FITC+ 7-AAD+ cells represent the actively proliferating cells. NGF does not cause a significant change in cell proliferation, however, K252a treatment alone or in combination with NGF leads to cell cycle arrest at G0/G1 and G2/M phases and generates a 50% reduction in cell proliferation. (c) Slow growth rate with K252a was also due to increased apoptosis-mediated cell death. Results presented are the mean ± SEM of at least three independent experiments. Data in (b,c) were analyzed by one-way ANOVA (*p < 0.05, **p < 0.01, ****p < 0.0001). (d) Fold change in MK counts (e) Fold change in PLP count (f) percetage of Annexin V+ cells and (g) TrkA phosphorylation, upon treatment with Etoposide and Bryostatin.
It is well known that platelet production is associated with apoptosis56. In order to investigate if, other known inducers of apoptosis, also affect TrkA phosphorylation and cause a similar effect on MK counts as well as PLP production, Dami cells were treated with two drugs, Etoposide (1 μM) and Bryostatin (10 nM) for 72 hours as described before57,58. Results showed, that Etoposide and Bryostatin both significantly reduce MK counts and increase PLP production (to levels similar to those obtained by K252a treatment, Fig. 4d,e, p < 0.0001 as compared DMSO), without any effect on TrkA phosphorylation (Fig. 4g). However, it is noteworthy that these drugs caused significantly more apoptosis than K252a (Fig. 4f), and that there is no correlation between percentage of apoptosis induced by these drugs (Annexin V+ cells) and PLP counts (Supplementary Fig. 4d). These results support a previously well-known notion that increased apoptosis can induce an increase in PLP production. However, the same cannot be said about K252a mediated increase in PLP production, because, K252a causes similar increase in PLP production, via modulating TrkA phsphorylation and at a much less extent of cellular apoptosis.
Genetic knock-out of TrkA expression by CRISPR induces decrease in cell proliferation and survival of Dami cells and increases platelet production, similar to K252a treatment
K252a is a robust inhibitor of tyrosine kinases (including PKC, PKA, PKG, MLCK, CaMK, Trks), however it is highly selective for Trk receptor subtypes in a concentration range of 10–200 nM59,60,61,62. Since the highest concentration of this range (i.e. 200 nM) was used in our experiments, we created a TrkA knockout Dami cell line (TrkA−/−) using CRISPR/Cas9 gene knockout system (Fig. 5a) to validate that K252a-mediated changes in MK cell proliferation, and platelet production were due to the inhibition of TrkA signaling51. While wild-type Dami cells have homogenous surface expression of TrkA (91.5%, Fig. 5b), our knockout strategy caused complete loss of TrkA as shown by flow cytometry analysis of TrkA surface expression (Fig. 5b) and loss of TrkA-mediated Akt phosphorylation (Fig. 5c).
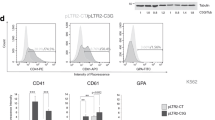
TrkA deficient Dami cells exhibit decreased growth rate and cell survival as well as increased platelet production. (a) For CRISPR/Cas9-mediated targeting of TrkA DNA, TrkA guide RNA (sgTrkA) was designed as complementary to a 20 nucleotide sequence (underlined; NG_007493: 50324-50344) with a 5′- GGG protospacer adjacent motif (PAM) (in square) located in the first exon of TrkA DNA. sgTrkA sequence was then inserted into an SpCas9(BB)-2A-GFP expression plasmid and nucleofected into Dami cells along with a 100 bp repair template (listed in Methods). In cells transfected with the expression plasmid and the repair template, Cas9 will be directed to the target sequence by sgTrkA due complementary base pairing and recognizes the 5′-GGG PAM sequence. Cas9 then introduces a double strand cut three nucleotides upstream of the GGG motif, which will trigger the DNA repair response. Repair by utilization of the template sequence leads to a single nucleotide (gray) deletion in the region which results in a frame-shift (DGA > MGP) in the TrkA mRNA and impairs the expression of TrkA protein. (b) Loss of TrkA expression was validated through flow cytometry by immunostaining wild-type (WT) and TrkA knockout (TrkA−/−) cells for TrkA surface expression. (c) Loss of NGF-mediated phosphorylation of Akt also confirmed the absence of functional TrkA signaling in TrkA−/− cells. (d) TrkA knockout cells showed a decreased growth rate compared to their WT counterparts. (e,f) Cell cycle analysis demonstrated a reduction in S phase cells coupled with an increase in G0/G1 and sub-G0 cell percentage. (g) Loss of TrkA expression also led to increased apoptotic death after a 24 h incubation. (h) TrkA−/− cells exhibited increased baseline production of platelet like particles. Results were plotted as mean with SEM from three independent experiments. Data in (d,e and h) were analyzed by two-way ANOVA; Student’s t test was used to evaluate the data in (g). (n.s. (not significant), *p < 0.05, **p < 0.01, ****p < 0.0001).
After establishing TrkA−/− cells, we performed a functional analysis to assess the growth, survival and baseline platelet production of these cells compared to WT Dami cells. Equal number of WT and TrkA−/− Dami cells were plated in RPMI medium containing 5% FBS and cultured for 72 h. As shown in Fig. 5d, TrkA−/− cell culture displayed a slower growth rate relative to WT Dami cells (p < 0.001 at 48 h) as seen with K252a treated WT Dami cells (Fig. 4a,b). Cell cycle analysis (Fig. 5e,f) revealed that the loss of TrkA led to the increased percentage of sub-G0 (p < 0.01, dead cells) and G0/G1(p < 0.05) cells while S phase cells (36.7% vs 53% in TrkA−/− and WT, respectively, p < 0.0001) was significantly decreased We also assessed the percentage of apoptotic cells and observed a 2-fold higher Annexin V+ cell in TrkA−/− cells compared to WT cell culture (p < 0.0001, Fig. 5g). These findings suggest that TrkA is important for cell cycle initiation and survival for MKs. These data also corroborate with that shown in Fig. 3c, indicating that NGF-induced TrkA signaling is necessary but not sufficient to increase Dami cell proliferation.
Loss of TrkA-mediated signaling also impacts platelet production. TrkA−/− cells exhibited a higher baseline level of PLP production, (approximately 5–7 fold increase) relative to WT Dami cells at the selected time points (p < 0.0001, Fig. 5h). Based on the decreased cell growth, survival, and increased platelet production observed in TrkA−/− cells, we concluded that loss of TrkA generates a phenotype similar to the one in K252a-treated WT Dami cells (Figs 3 and 4). Overall, these data indicate that TrkA signaling is necessary for MK cell proliferation and survival, while blocking platelet production.
TrkA signaling is necessary for platelet production as well as MK proliferation
In order to further confirm that the effects of K252a are indeed through inhibition of TrkA signaling, the TrkA−/− cells were treated with K252a for up to 72 hours and cell counts, cell survival as well as PLP counts were measured. While, DMSO (vehicle) treatment decreased cell growth (p < 0.0001, Fig. 6a), this effect was not due to increased apoptosis (Fig. 6b). Beyond DMSO’s effects, K252a significantly decreased cell growth (DMSO vs K252a, p < 0.001 at 48 h, p < 0.0001 at 72 h, Fig. 6a) and this was associated with significant increase in Annexin V+ apoptotic cells (p < 0.0001, Fig. 6b). These results as well as the data shown in Fig. 5, clearly indicate that TrkA signaling is essential for MK cell proliferation/survival and the absence of this receptor renders the TrkA−/− cells, especially susceptible to toxic effects of DMSO as well as K252a (even more so than WT Dami cells). Interestingly, while DMSO led to a significant increase in platelet-like particle counts (p < 0.01, Fig. 6c), via some unknown, not-apoptosis related effect; in the absence of TrkA receptor, K252a failed to stimulate platelet production. These findings confirm that K252a modulates thrombopoiesis through inhibitions of TrkA signaling.
K252a modulates thrombopoiesis through TrkA inhibition. TrkA−/− Dami cells were treated with 200 nM K252a, or vehicle (DMSO) for 72 h. Cell suspension from each condition was analyzed by flow cytometry at indicated time points for MK content and intact platelet-like particles. Additionally, following 24 h incubation, 1 × 105 cells were removed from each well and stained with Annexin V-PE and 7-AAD for apoptotic cell analysis. The data show that K252a is still able to cause a decrease in (a) cell growth rate and increase in (b) apoptotic cell percentage in TrkA knockout cells, implying that K252a does not only target TrkA but affects additional intrinsic factors. However, (c) K252a is no longer to increase the platelet production in TrkA knockout cells. Results were plotted as mean with SEM of at least three independent experiments. Data in (a,c) were analyzed by two-way ANOVA; one-way ANOVA was used to evaluate the data in (b). (**p < 0.01, ***p < 0.001, ****p < 0.0001).
Discussion
In this study, we investigated a novel regulatory role of TrkA signaling in megakaryopoiesis and thrombopoiesis. TrkA has previously been detected in CD34+ umbilical cord blood cells28 and our findings show that its expression is preserved throughout the MK lineage, in megakaryocytic cells lines as well as MKs differentiated from human primary CD34+ hematopoietic stem cells (henceforth termed as primary MKPs/MKs). In primary MKPs, treatment with NGF, a ligand for TrkA receptor, promoted expansion of the progenitor cells whereas exposure to K252a, a Trk inhibitor, reduced the numbers of both primary MKPs and MKs accompanied by a decrease in CD41 expression indicating that NGF-induced signaling drives the clonal expansion of the committed MKPs and is necessary for retainment of MK lineage markers16. Interestingly, NGF-mediated signals that are pro-mitogenic in progenitor cells, are not sufficient to induce MK expansion indicating that NGF asserts differential effects on mitotic MKPs versus endomitotic MK cells. Further pharmacologic inhibition of TrkA signaling via K252a decreased MKP proliferation and increased platelet production despite the presence of NGF. These findings demonstrate that TrkA signaling stimulates MKP proliferation and MK survival where as its inhibition induces platelet production by MK cells.
This role of TrkA signaling in megakaryocytic cells was further established via the use of CRISPR/CAS9 mediated knock out of TrkA in Dami cells. This cell line was found to recapitulate the effects of K252a on primary MKPs/MKs. Owing to the technical difficulty in conducting knock out experiments in primary cells, Dami cells were deemed to be a suitable substitute for performing these experiments. As expected, TrkA−/− Dami cells exhibited reduced proliferative capacity and increased production of platelet-like-particles, substantiating the function of TrkA signaling in this phenomenon. We also observed a positive correlation between the increase in platelet production and the percentage of apoptotic cells in TrkA-null Dami cells. Further, treatment of K252a to TrkA−/− cells, failed to increase PLP production, clearly indicating that K252a mediates its effects through inhibition of TrkA signaling. The link between localized activation of caspases and inhibition of proapoptotic proteins in platelet-forming MKs has been reported by multiple groups63,64,65,66,67. Besides, overexpression of anti-apoptotic proteins was shown to impair platelet production68.
In addition, we found that NGF induces activation of PI3K/Akt signaling pathway in a TrkA dependent manner in Dami cells. PI3K/Akt is known to mediate NGF-induced cell survival in neuronal cells and cardiomyocytes69,70. Upon NGF-mediated activation, Akt translocates to the nucleus and phosphorylates the proapoptotic transcription factor, Forkhead Box O3 (FOXO3)70. This leads to binding of 14-3-3 to FOXO3 and its sequestration in the cytoplasm70. Akt also promotes cell survival by inactivating Bad and preventing caspase 9 activation70. The same PI3K/Akt/FOXO3 signaling has been shown to mediate MK survival64. Therefore, Pi3K/Akt pathway might mediate decreased cell survival in K252a-treated or TrkA knockout cells which in turn drives increased platelet production.
Overall, we have shown that through activation of TrkA, NGF acts as a proliferation and/or pro-survival factor and supports early megakaryopoiesis but inhibits later platelet production from mature MKs. These findings might have several clinical implications for the treatment of hematologic disorders. Previous studies have reported that altered TrkA expression in myeloid and lymphoid leukemia provide either a proliferation or a survival advantage to CD34+ hematopoietic cells71,72. Therefore, TrkA was proposed as a therapeutic target for these malignancies52,73. In myeloproliferative disorders such as polycythemia vera or essential thrombocythemia, HSCs and early hematopoietic progenitors excessively proliferate due to increased cytokine sensitivity74, ultimately giving rise to increased MK and platelet production75. Besides altered TrkA signaling in myeloid malignancies, normal TrkA signaling can contribute to a myeloproliferative phenotype in the context of cytokine-hypersensitive HSCs and early hematopoietic progenitors. Hence, targeting TrkA, regardless of its normal or abnormal activity, might help to control excess proliferation of cells in myeloproliferative disorders.
In non-hematopoietic cancers, protection of MKPs against chemotherapy-induced cytotoxicity via the administration of hematopoietic cytokines (Stem Cell Factor [SCF], Interleukin 11 [IL-11] and thrombopoietin receptor agonists) has been previously proposed76,77,78. Given NGF’s role in MKP expansion and MK survival, NGF could be evaluated as a protective agent against chemotherapy-induced progenitor cell death in cancers with no TrkA involvement.
Lastly, patients receiving chemotherapy or undergoing myeloablative treatment for bone marrow transplantation experience thrombocytopenia due to the loss of hematopoietic stem and progenitor cells76. Recovery of complete blood cell counts takes approximately 20 days, which renders patients susceptible to infections and bleeding79. Platelet transfusion is the first line of treatment for severe thrombocytopenia in those patients76,80,81. However, limitations of platelet transfusion therapy include donor dependency, short platelet shelf-life, alloimmunization and infection risks11,82,83,84,85. The alternative approach to eliminate donor dependency and alloimmunization risk is the infusion of ex vivo differentiated MKPs or platelets generated from the patient’s own cells86,87,88. Current studies are investigating the best source of stem cells, timeline and order of cytokine addition to the culture in order to govern stem cell differentiation to MKs88,89. NGF/TrkA signaling can support these culture systems at an early stage where MKP enrichment is desired. Withdrawal of NGF or pulsing MKs with K252a analogs after MKs are generated might improve the platelet yield by promoting thrombopoiesis. Besides K252a, new TrkA antagonists, such as ALE0540, RN624, REN1820 are under development and are expected to provide TrkA-specific targeting90,91,92. Given the clinical potential of our findings, further in-depth investigation of the NGF-TrkA axis in thrombopoiesis using in vivo models is warranted. In addition, human platelets also possess TrkA expression on their cell surface (data not shown) and store NGF in their dense granules93. Hence investigations into the effects of NGF/TrkA signaling on platelet function might prove beneficial to prevent thrombotic events as well as to improve platelet storage by suppressing platelet activation.
References
Semple, J. W., Italiano, J. E. & Freedman, J. Platelets and the immune continuum. Nat Rev Immunol 11, 264–274 (2011).
Smyth, S. S. et al. Platelet functions beyond hemostasis. J Thromb Haemost 7, 1759–1766, https://doi.org/10.1111/j.1538-7836.2009.03586.x (2009).
Morrell, C. N., Aggrey, A. A., Chapman, L. M. & Modjeski, K. L. Emerging roles for platelets as immune and inflammatory cells. Blood 123, 2759–2767, https://doi.org/10.1182/blood-2013-11-462432 (2014).
McFadyen, J. D. & Kaplan, Z. S. Platelets are not just for clots. Transfus Med Rev 29, 110–119, https://doi.org/10.1016/j.tmrv.2014.11.006 (2015).
Smock, K. J. & Perkins, S. L. Thrombocytopenia: an update. Int J Lab Hematol 36, 269–278, https://doi.org/10.1111/ijlh.12214 (2014).
Schafer, A. I. Thrombocytosis. New England Journal of Medicine 350, 1211–1219, https://doi.org/10.1056/NEJMra035363 (2004).
Vannucchi, A. M. & Barbui, T. Thrombocytosis and thrombosis. Hematology Am Soc Hematol Educ Program, 363–370, https://doi.org/10.1182/asheducation-2007.1.363 (2007).
Skoda, R. C. Thrombocytosis. Hematology Am Soc Hematol Educ Program, 159–167, https://doi.org/10.1182/asheducation-2009.1.159 (2009).
Izak, M. & Bussel, J. B. Management of thrombocytopenia. F1000Prime Reports 6, 45, https://doi.org/10.12703/P6-45 (2014).
Bleeker, J. S. & Hogan, W. J. Thrombocytosis: Diagnostic Evaluation, Thrombotic Risk Stratification, and Risk-Based Management Strategies. Thrombosis 2011, 16, https://doi.org/10.1155/2011/536062 (2011).
Hod, E. & Schwartz, J. Platelet transfusion refractoriness. British Journal of Haematology 142, 348–360, https://doi.org/10.1111/j.1365-2141.2008.07189.x (2008).
Nurhayati, R. W., Ojima, Y. & Taya, M. Recent developments in ex vivo platelet production. Cytotechnology 68, 2211–2221, https://doi.org/10.1007/s10616-016-9963-4 (2016).
Balduini, A., Di Buduo, C. A. & Kaplan, D. L. Translational approaches to functional platelet production ex vivo. Thromb Haemost 115, 250–256, https://doi.org/10.1160/th15-07-0570 (2016).
Yu, M. & Cantor, A. B. Megakaryopoiesis and thrombopoiesis: an update on cytokines and lineage surface markers. Methods Mol Biol 788, 291–303, https://doi.org/10.1007/978-1-61779-307-3_20 (2012).
Italiano, J. E. Jr. Unraveling mechanisms that control platelet production. Semin Thromb Hemost 39, 15–24, https://doi.org/10.1055/s-0032-1331157 (2013).
Deutsch, V. R. & Tomer, A. Advances in megakaryocytopoiesis and thrombopoiesis: from bench to bedside. Br J Haematol 161, 778–793, https://doi.org/10.1111/bjh.12328 (2013).
Zheng, C. et al. TPO-independent megakaryocytopoiesis. Crit Rev Oncol Hematol 65, 212–222, https://doi.org/10.1016/j.critrevonc.2007.11.003 (2008).
Machlus, K. R. & Italiano, J. E. The incredible journey: From megakaryocyte development to platelet formation. The Journal of Cell Biology 201, 785–796, https://doi.org/10.1083/jcb.201304054 (2013).
Reichardt, L. F. Neurotrophin-regulated signalling pathways. Philos Trans R Soc Lond B Biol Sci 361, 1545–1564, https://doi.org/10.1098/rstb.2006.1894 (2006).
Huang, E. J. & Reichardt, L. F. Trk receptors: roles in neuronal signal transduction. Annu Rev Biochem 72, 609–642, https://doi.org/10.1146/annurev.biochem.72.121801.161629 (2003).
Shibayama, E. & Koizumi, H. Cellular localization of the Trk neurotrophin receptor family in human non-neuronal tissues. Am J Pathol 148, 1807–1818 (1996).
Sariola, H. The neurotrophic factors in non-neuronal tissues. Cell Mol Life Sci 58, 1061–1066 (2001).
Caporali, A. & Emanueli, C. Cardiovascular Actions of Neurotrophins. Physiological Reviews 89, 279–308, https://doi.org/10.1152/physrev.00007.2008 (2009).
Skaper, S. D. The neurotrophin family of neurotrophic factors: an overview. Methods Mol Biol 846, 1–12, https://doi.org/10.1007/978-1-61779-536-7_1 (2012).
Chevalier, S. et al. Expression and functionality of the trkA proto-oncogene product/NGF receptor in undifferentiated hematopoietic cells. Blood 83, 1479–1485 (1994).
Matsuda, H., Coughlin, M. D., Bienenstock, J. & Denburg, J. A. Nerve growth factor promotes human hemopoietic colony growth and differentiation. Proc Natl Acad Sci USA 85, 6508–6512 (1988).
Labouyrie, E. et al. Expression of Neurotrophins and their Receptors in Human Bone Marrow. The American Journal of Pathology 154, 405–415 (1999).
Bracci-Laudiero, L. et al. CD34-positive cells in human umbilical cord blood express nerve growth factor and its specific receptor TrkA. J Neuroimmunol 136, 130–139 (2003).
Aloe, L., Simone, M. D. & Properzi, F. Nerve growth factor: a neurotrophin with activity on cells of the immune system. Microsc Res Tech 45, 285–291, doi:10.1002/(sici)1097-0029(19990515/01)45:4/5<285::aid-jemt12>3.0.co;2-3 (1999).
Hillis, J., O’Dwyer, M. & Gorman, A. M. Neurotrophins and B-cell malignancies. Cell Mol Life Sci 73, 41–56, https://doi.org/10.1007/s00018-015-2046-4 (2016).
Datta-Mitra, A., Kundu-Raychaudhuri, S., Mitra, A. & Raychaudhuri, S. P. Cross talk between neuroregulatory molecule and monocyte: nerve growth factor activates the inflammasome. PLoS One 10, e0121626, https://doi.org/10.1371/journal.pone.0121626 (2015).
Kritas, S. K. et al. Nerve growth factor interactions with mast cells. Int J Immunopathol Pharmacol 27, 15–19 (2014).
Samah, B., Porcheray, F. & Gras, G. Neurotrophins modulate monocyte chemotaxis without affecting macrophage function. Clin Exp Immunol 151, 476–486, https://doi.org/10.1111/j.1365-2249.2007.03578.x (2008).
Huang, X. Q. & Zhu, B. D. Effect of nerve growth factor on erythropoiesis in mice and its underlying mechanism. Zhongguo Shi Yan Xue Ye Xue Za Zhi 16, 1365–1371 (2008).
Gibbs, B. F., Zillikens, D. & Grabbe, J. Nerve growth factor influences IgE-mediated human basophil activation: functional properties and intracellular mechanisms compared with IL-3. Int Immunopharmacol 5, 735–747, https://doi.org/10.1016/j.intimp.2004.12.004 (2005).
Sato, Y., Tsuboi, Y., Kurosawa, H., Sugita, K. & Eguchi, M. Anti-apoptotic effect of nerve growth factor is lost in congenital insensitivity to pain with anhidrosis (CIPA) B lymphocytes. J Clin Immunol 24, 302–308, https://doi.org/10.1023/B:JOCI.0000025452.79585.a1 (2004).
Coppola, V. et al. Ablation of TrkA function in the immune system causes B cell abnormalities. Development 131, 5185–5195, https://doi.org/10.1242/dev.01383 (2004).
Vega, J. A., Garcia-Suarez, O., Hannestad, J., Perez-Perez, M. & Germana, A. Neurotrophins and the immune system. J Anat 203, 1–19 (2003).
Kobayashi, H., Gleich, G. J., Butterfield, J. H. & Kita, H. Human eosinophils produce neurotrophins and secrete nerve growth factor on immunologic stimuli. Blood 99, 2214–2220 (2002).
la Sala, A., Corinti, S., Federici, M., Saragovi, H. U. & Girolomoni, G. Ligand activation of nerve growth factor receptor TrkA protects monocytes from apoptosis. J Leukoc Biol 68, 104–110 (2000).
Otten, U. & Gadient, R. A. Neurotrophins and cytokines–intermediaries between the immune and nervous systems. Int J Dev Neurosci 13, 147–151 (1995).
Koch, A. et al. Inhibition of Abl tyrosine kinase enhances nerve growth factor-mediated signaling in Bcr-Abl transformed cells via the alteration of signaling complex and the receptor turnover. Oncogene 27, 4678–4689, https://doi.org/10.1038/onc.2008.107 (2008).
Xie, P., Chan, F. S., Ip, N. Y. & Leung, M. Nerve growth factor potentiated the sodium butyrate- and PMA-induced megakaryocytic differentiation of K562 leukemia cells. Leuk Res 24, 751–759 (2000).
Yokoe, H. et al. Induction of polyploidization in the human erythroleukemia cell line (HEL) by protein kinase inhibitor (K252a) and the phorbol-ester TPA. Leuk Lymphoma 25, 333–343, https://doi.org/10.3109/10428199709114173 (1997).
Iwabe, K. et al. K-252a-induced polyploidization and differentiation of a human megakaryocytic cell line, Meg-J: transient elevation and subsequent suppression of cyclin B1 and cdc2 expression in the process of polyploidization. British Journal of Haematology 102, 812–819, https://doi.org/10.1046/j.1365-2141.1998.00819.x (1998).
Quentmeier, H., Zaborski, M. & Drexler, H. G. Effects of thrombopoietin, interleukin-3 and the kinase inhibitor K-252a on growth and polyploidization of the megakaryocytic cell line M-07e. Leukemia 12, 1603–1611 (1998).
Wen, Q. et al. Integrative screening approach identifies regulators of polyploidization and targets for acute megakaryocytic leukemia. Cell 150, 575–589, https://doi.org/10.1016/j.cell.2012.06.032 (2012).
Sahler, J., Bernard, J. J., Spinelli, S. L., Blumberg, N. & Phipps, R. P. The Feverfew plant-derived compound, parthenolide enhances platelet production and attenuates platelet activation through NF-κB inhibition. Thrombosis research 127, 426–434, https://doi.org/10.1016/j.thromres.2010.12.013 (2011).
Kiebala, M., Polesskaya, O., Yao, Z., Perry, S. W. & Maggirwar, S. B. Nuclear factor-kappa B family member RelB inhibits human immunodeficiency virus-1 Tat-induced tumor necrosis factor-alpha production. PLoS One 5, e11875, https://doi.org/10.1371/journal.pone.0011875 (2010).
O’Brien, J. J. et al. 15-deoxy-Δ12,14-PGJ2 enhances platelet production from megakaryocytes. Blood, https://doi.org/10.1182/blood-2008-05-158535 (2008).
Ran, F. A. et al. Genome engineering using the CRISPR-Cas9 system. Nat. Protocols 8, 2281–2308, https://doi.org/10.1038/nprot.2013.143 (2013).
Sniderhan, L. F. et al. Neurotrophin signaling through tropomyosin receptor kinases contributes to survival and proliferation of non-Hodgkin lymphoma. Exp Hematol 37, 1295–1309, https://doi.org/10.1016/j.exphem.2009.08.005 (2009).
Angeles, T. S., Yang, S. X., Steffler, C. & Dionne, C. A. Kinetics of trkA tyrosine kinase activity and inhibition by K-252a. Arch Biochem Biophys 349, 267–274, https://doi.org/10.1006/abbi.1997.0490 (1998).
Greenberg, S. M., Rosenthal, D. S., Greeley, T. A., Tantravahi, R. & Handin, R. I. Characterization of a new megakaryocytic cell line: the Dami cell. Blood 72, 1968–1977 (1988).
Lev, P. R. et al. Production of functional platelet-like particles by the megakaryoblastic DAMI cell line provides a model for platelet biogenesis. Platelets 22, 28–38, https://doi.org/10.3109/09537104.2010.515271 (2011).
Josefsson, E. C. et al. Platelet production proceeds independently of the intrinsic and extrinsic apoptosis pathways. Nat Commun 5, 3455, https://doi.org/10.1038/ncomms4455 (2014).
Karpinich, N. O., Tafani, M., Rothman, R. J., Russo, M. A. & Farber, J. L. The course of etoposide-induced apoptosis from damage to DNA and p53 activation to mitochondrial release of cytochrome c. J Biol Chem 277, 16547–16552, https://doi.org/10.1074/jbc.M110629200 (2002).
Mohammad, R. M. et al. Bryostatin 1 induces apoptosis and augments inhibitory effects of vincristine in human diffuse large cell lymphoma. Leuk Res 19, 667–673 (1995).
Tapley, P., Lamballe, F. & Barbacid, M. K252a is a selective inhibitor of the tyrosine protein kinase activity of the trk family of oncogenes and neurotrophin receptors. Oncogene 7, 371–381 (1992).
Knusel, B. & Hefti, F. K-252 compounds: modulators of neurotrophin signal transduction. J Neurochem 59, 1987–1996 (1992).
Raychaudhuri, S. P., Sanyal, M., Weltman, H. & Kundu-Raychaudhuri, S. K252a, a high-affinity nerve growth factor receptor blocker, improves psoriasis: an in vivo study using the severe combined immunodeficient mouse-human skin model. J Invest Dermatol 122, 812–819, https://doi.org/10.1111/j.0022-202X.2003.12602.x (2004).
Berg, M. M., Sternberg, D. W., Parada, L. F. & Chao, M. V. K-252a inhibits nerve growth factor-induced trk proto-oncogene tyrosine phosphorylation and kinase activity. Journal of Biological Chemistry 267, 13–16 (1992).
Testa, U. Platelet formation: a link between apoptosis and differentiation. Blood 100, 1111–1112, https://doi.org/10.1182/blood-2002-06-1853 (2002).
Perdomo, J., Yan, F. & Chong, B. H. A megakaryocyte with no platelets: anti-platelet antibodies, apoptosis, and platelet production. Platelets 24, 98–106, https://doi.org/10.3109/09537104.2012.669508 (2013).
De Botton, S. et al. Platelet formation is the consequence of caspase activation within megakaryocytes. Blood 100, 1310–1317, https://doi.org/10.1182/blood-2002-03-0686 (2002).
Abd-Elrahman, I. et al. Differential regulation of the apoptotic machinery during megakaryocyte differentiation and platelet production by inhibitor of apoptosis protein Livin. Cell Death Dis 4, e937, https://doi.org/10.1038/cddis.2013.454 (2013).
Gordge, M. P. Megakaryocyte apoptosis: sorting out the signals. Br J Pharmacol 145, 271–273, https://doi.org/10.1038/sj.bjp.0706202 (2005).
Kaluzhny, Y. et al. BclxL overexpression in megakaryocytes leads to impaired platelet fragmentation. Blood 100, 1670–1678, https://doi.org/10.1182/blood-2001-12-0263 (2002).
Caporali, A. et al. Identification of the prosurvival activity of nerve growth factor on cardiac myocytes. Cell Death Differ 15, 299–311, https://doi.org/10.1038/sj.cdd.4402263 (2007).
Nguyen, T. L. X., Kim, C. K., Cho, J.-H., Lee, K.-H. & Ahn, J.-Y. Neuroprotection signaling pathway of nerve growth factor and brain-derived neurotrophic factor against staurosporine induced apoptosis in hippocampal H19-7 cells. Exp Mol Med 42, 583–595, https://doi.org/10.3858/emm.2010.42.8.060 (2010).
Mulloy, J. C. et al. AML1-ETO fusion protein up-regulates TRKA mRNA expression in human CD34+ cells, allowing nerve growth factor-induced expansion. Proc Natl Acad Sci USA 102, 4016–4021, https://doi.org/10.1073/pnas.0404701102 (2005).
Kim, M. S. et al. c-Src activation through a TrkA and c-Src interaction is essential for cell proliferation and hematological malignancies. Biochem Biophys Res Commun 441, 431–437, https://doi.org/10.1016/j.bbrc.2013.10.082 (2013).
Renne, C., Minner, S., Kuppers, R., Hansmann, M. L. & Brauninger, A. Autocrine NGFbeta/TRKA signalling is an important survival factor for Hodgkin lymphoma derived cell lines. Leuk Res 32, 163–167, https://doi.org/10.1016/j.leukres.2007.05.019 (2008).
Kawasaki, H., Nakano, T., Kohdera, U. & Kobayashi, Y. Hypersensitivity of megakaryocyte progenitors to thrombopoietin in essential thrombocythemia. American Journal of Hematology 68, 194–197, https://doi.org/10.1002/ajh.1178 (2001).
Bain, B. J. The Relationship between the Myelodysplastic Syndromes and the Myeloproliferative Disorders. Leukemia & Lymphoma 34, 443–449, https://doi.org/10.3109/10428199909058471 (1999).
Kuter, D. J. In Oncology Vol. 29 282 (2015).
Zeuner, A. et al. Chemotherapy-induced thrombocytopenia derives from the selective death of megakaryocyte progenitors and can be rescued by stem cell factor. Cancer Res 67, 4767–4773, https://doi.org/10.1158/0008-5472.can-06-4303 (2007).
Bhatia, M., Davenport, V. & Cairo, M. S. The role of interleukin-11 to prevent chemotherapy-induced thrombocytopenia in patients with solid tumors, lymphoma, acute myeloid leukemia and bone marrow failure syndromes. Leuk Lymphoma 48, 9–15, https://doi.org/10.1080/10428190600909115 (2007).
Slayton, W. B. et al. Developmental differences in megakaryocyte maturation are determined by the microenvironment. Stem Cells 23, 1400–1408, https://doi.org/10.1634/stemcells.2004-0373 (2005).
Hillyer, C. Platelet transfusion for patients with cancer: Clinical practice guidelines of the American society of clinical oncology C. A. Schiffer, K. C. Anderson, C. L. Bennett, et al. J Clin Oncol 19:1519–1538, 2001. Transfusion Medicine Reviews 16, 183–184, https://doi.org/10.1053/s0887-7963(02)80051-7 (2002).
Prica, A., Sholzberg, M. & Buckstein, R. Safety and efficacy of thrombopoietin-receptor agonists in myelodysplastic syndromes: a systematic review and meta-analysis of randomized controlled trials. British Journal of Haematology 167, 626–638, https://doi.org/10.1111/bjh.13088 (2014).
Katus, M. C., Szczepiorkowski, Z. M., Dumont, L. J. & Dunbar, N. M. Safety of platelet transfusion: past, present and future. Vox Sang 107, 103–113, https://doi.org/10.1111/vox.12146 (2014).
Mathai, J. Problem of bacterial contamination in platelet concentrates. Transfus Apher Sci 41, 139–144, https://doi.org/10.1016/j.transci.2009.07.012 (2009).
Holbro, A., Infanti, L., Sigle, J. & Buser, A. Platelet transfusion: basic aspects. Swiss Med Wkly 143, w13885, https://doi.org/10.4414/smw.2013.13885 (2013).
Chandrashekar, S. & Kantharaj, A. Legal and ethical issues in safe blood transfusion. Indian J Anaesth 58, 558–564, https://doi.org/10.4103/0019-5049.144654 (2014).
Smith, B. W. & Murphy, G. J. Stem cells, megakaryocytes, and platelets. Curr Opin Hematol 21, 430–437, https://doi.org/10.1097/moh.0000000000000064 (2014).
Xi, J. et al. Infusion of megakaryocytic progenitor products generated from cord blood hematopoietic stem/progenitor cells: results of the phase 1 study. PLoS One 8, e54941, https://doi.org/10.1371/journal.pone.0054941 (2013).
Panuganti, S., Papoutsakis, E. T. & Miller, W. M. Bone marrow niche-inspired, multiphase expansion of megakaryocytic progenitors with high polyploidization potential. Cytotherapy 12, 767–782, https://doi.org/10.3109/14653241003786148 (2010).
Masuda, S., Li, M. & Belmonte, J. C. I. In vitro generation of platelets through direct conversion: first report in My Knowledge (iMK). Cell Research 23, 176–178, https://doi.org/10.1038/cr.2012.142 (2013).
Dawbarn, D. et al. NGF receptor TrkAd5: therapeutic agent and drug design target. Biochem Soc Trans 34, 587–590, https://doi.org/10.1042/bst0340587 (2006).
Watson, J. J. et al. TrkAd5: A novel therapeutic agent for treatment of inflammatory pain and asthma. J Pharmacol Exp Ther 316, 1122–1129, https://doi.org/10.1124/jpet.105.095844 (2006).
Hefti, F. F. et al. Novel class of pain drugs based on antagonism of NGF. Trends Pharmacol Sci 27, 85–91, https://doi.org/10.1016/j.tips.2005.12.001 (2006).
Hochstrasser, T., Ehrlich, D., Sperner-Unterweger, B. & Humpel, C. Antidepressants and anti-inflammatory drugs differentially reduce the release of NGF and BDNF from rat platelets. Pharmacopsychiatry 46, 29–34, https://doi.org/10.1055/s-0032-1314843 (2013).
Acknowledgements
We thank Dr. Craig Morrel, Dr. Edith Lord, Dr. Janet Sparks, and Dr. Gail Johnson for their insight and advice for the development of this research study; Dr. Richard Phipps for providing the cell lines and technical support; Drs. Elaine Smolock, Joseph Jackson and Ryan Connor for their assistance in the manuscript preparation. This work was supported by grants from the National Institute of Health (NIH R01 HL128155; R01 NS054578; R01 NS066801) to Dr. Maggirwar, (NIH RO1 DK098251) to Dr. Palis, Pilot funding from Center for AIDS Research, University of Rochester (NIH 5 P30 AI078498-08) to Dr. Singh, and scholarship for graduate studies from Ministry of National Education of Turkey (MEB) to Dr. Kizilyer.
Author information
Authors and Affiliations
Contributions
A.K. performed experiments, interpreted data and wrote the manuscript. M.V.S. and J.P. interpreted data and wrote the manuscript. V.B.S. and S.S. performed experiments. S.B.M. planned and generated the study design, interpreted data and wrote the manuscript.
Corresponding author
Ethics declarations
Competing Interests
The authors declare no competing interests.
Additional information
Publisher’s note: Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary information
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons license, and indicate if changes were made. The images or other third party material in this article are included in the article’s Creative Commons license, unless indicated otherwise in a credit line to the material. If material is not included in the article’s Creative Commons license and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this license, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
Kizilyer, A., Singh, M.V., Singh, V.B. et al. Inhibition of Tropomyosin Receptor Kinase A Signaling Negatively Regulates Megakaryopoiesis and induces Thrombopoiesis. Sci Rep 9, 2781 (2019). https://doi.org/10.1038/s41598-019-39385-x
Received:
Accepted:
Published:
DOI: https://doi.org/10.1038/s41598-019-39385-x
- Springer Nature Limited