Abstract
Acinetobacter baumannii infection has become a major cause of healthcare-associated infection and a critical pathogen in the WHO antimicrobial resistance research and development priority list. Catheter-related septicemia is one of the major clinical manifestations of A. baumannii infection associated with high morbidity and mortality. In this study, we used a clinical A. baumannii strain (LAC-4) that is hypervirulent to immunocompetent C57BL/6 and BALB/c mice and established a mouse model of intraperitoneal (i.p.) A. baumannii infection. Our study showed that i.p. LAC-4 infection of C57BL/6 and BALB/c mice induces a lethal or sublethal infection with high bacterial burdens in peritoneal cavity, blood and tissues and the infected mice either succumbed to the infection within 24 hours or completely recovered from the infection. The infection induces acute peritoneal recruitment of neutrophils and other innate immune cells, and the local and systemic production of proinflammatory cytokines and chemokines (IL-1β, IL-5, IL-6, TNF-α, RANTES, MIP-1β, MCP-1, KC and IL-10). Mechanistic studies suggest an important role of macrophages in the host innate defense in this model in that in vitro stimulation of peritoneal macrophages with killed LAC-4 induced a similar pattern of cytokine/chemokine responses to those in the infected mice, and depletion of peritoneal macrophages rendered the mice significantly more susceptible to the infection. Thus, this mouse infection model will provide an alternative and useful tool for future pathogenesis studies of A. baumannii-associated septicemia and identification and characterization of important virulence factors, as well as serve as a surrogate model for rapid evaluation of novel therapeutics and vaccines for this emerging infectious agent.
Similar content being viewed by others
Introduction
Acinetobacter baumannii is a major cause of hospital-acquired infections worldwide1,2,3,4. In addition, A. baumannii infections are increasingly difficult to treat due to its rapid development of resistance to multiple antibiotics5,6. Indeed, A. baumannii has recently been listed as a critical priority pathogen (Priority 1) for R&D of new antibiotics by the WHO7.
Catheter-related bacteremia and sepsis is one of the major manifestations and most severe forms of A. baumannii infection in hospital setting and the overall mortality of can be as high as 70%1,8. The mouse model of intraperitoneal (i.p.) A. baumannii infection has been commonly used for studying the infection pathogenesis and for evaluating novel therapeutics and vaccine efficacy9,10,11,12,13,14,15. However, to establish an effective infection and bacteremia in mice, most A. baumannii isolates will be required either to be admixed with porcine mucin prior to inoculation, or immunocompromised hosts such as neutropenic or diabetic mice must be used4,12,16. Despite the common use of mouse models of i.p. A. baumannii infection by the Acinetobacter research community, only a few studies have systemically characterized this model, particularly the host response to the infection15,17. Those studies showed that the infection induces production of interleukin (IL)-17 and IL-23 and neutrophils play an important role in host resistance to the infection, which is independent of the IL-17/IL-23 pathway15.
We have previously identified a clinical isolate of A. baumannii (LAC-4) that is much more virulent in mice when it was inoculated intranasally (i.n.)18 or intravenously (i.v.)19 as compared to most other clinical isolates and ATCC type strains of A. baumannii20,21, with significantly higher bacterial burdens in the lungs and enhanced extrapulmonary dissemination to the spleen18. Genomic analysis of the LAC-4 isolate reveals that it harbors unusually high copies of five insertion sequences and possesses a rare capsule biosynthesis locus contained within a genomic island of approximately 33 kb in length22. In this study, we evaluated the potential of this clinical isolate for its utility in a mouse model of intraperitoneal infection and characterized the innate host cellular and proinflammatory cytokine responses to the infection.
Results
Intraperitoneal infection of LAC-4 in C57BL/6 and BALB/c mice
To determine if this strain is also hypervirulent in mice when inoculated intraperitoneally, we first compared survival rates of C57BL/6 and BALB/c mice after i.p. inoculation with varying doses of ATCC 17961 and LAC-4. All C57BL/6 and BALB/c mice succumbed to infection within 24 h after i.p. inoculation with 107 or 106 colony forming units (CFU) of LAC-4, and 80% of the either mouse strain succumbed to 105 CFU of LAC-4 infection (Fig. 1, lower panel). In contrast, no mice died after i.p. inoculation with up to 6.4 × 107 CFU ATCC 17961, but 80% of C57BL/6 and 60% of BALB/c mice succumbed to 5 × 108 CFU of ATCC 17961 inoculation (Fig. 1, upper panel). Thus, LAC-4 is at least ~100 times more virulent than ATCC 17961 in both C57BL/6 and BALB/c mice when inoculated intraperitoneally, which is similar to the virulence difference between the two isolates when inoculated intranasally or intravenously18,19.
Surviving rates of C57BL/6 and BALB/c mice following i.p. inoculation with A. baumannii ATCC17961 (top panel) and LAC-4 (bottom panel). Groups of 5 C57BL/6 or BALB/c mice were i.p. inoculated with various numbers of ATCC17961 or LAC-4 as indicated and their clinical outcome monitored daily for 7 days. The number of surviving mice/total number of mice infected were 11/15 and 12/15 for C57BL/6 and BALB/c mice infected with ATCC17961, respectively, and 1/15 for C57BL/6 and BALB/c mice infected with LAC-4.
Kinetics of in vivo bacterial growth after i.p. LAC-4 inoculation
To further characterize the host response to i.p. LAC-4 infection, groups of C57BL/6 mice were inoculated i.p. with either a lethal (107 CFU) or a sublethal dose (5 × 104 CFU) of LAC-4 and the kinetics of bacterial growth in the peritoneal cavity, lungs, spleen, kidneys and blood were determined. As shown in Fig. 2, regardless of the initial inoculum dose, LAC-4 cells were detected in blood and all tissues examined at 4 hours post inoculation (h p.i.). In mice inoculated with the lethal dose of LAC-4, the bacterial burdens in the peritoneal cavity and blood at 4 h p.i. were about 50-fold higher than the inoculum, and the bacterial burdens in the lung, spleen and kidney reached 107 CFU per organ (Fig. 2A), indicating rapid local replication and systemic dissemination of LAC-4 after i.p. inoculation. All the mice succumbed to the infection before 24 h p.i. In mice inoculated with the sublethal dose of LAC-4, the bacterial burdens in the peritoneal cavity, blood, spleen and kidneys had decreased significantly at 24 h p.i. and were generally below the detection limit by 48 h p.i., with the exception in the lung where small numbers of bacteria were consistently cultured throughout the study period (168 h p.i.) (Fig. 2B).
Bacterial burdens in the peritoneal cavity, blood, lungs, spleen, and kidneys of C57BL/6 mice following i.p. LAC-4 inoculation. Groups of C57BL/6 mice (n = 5) were i.p. inoculated with 1 × 107 (A) or 5 × 104 (B) CFU of A. baumannii LAC-4. Bacterial burdens in the peritoneal lavage fluid, blood and respective organs at various times post-inoculation were determined by quantitative bacteriology. Data from individual mouse are presented as scatter plot and the horizontal bar represents the mean. The results represent one of at least two experiments with similar results. The detection limits for bacterial burdens were indicated as black dotted lines (A,B).
Inflammatory cell responses in the peritoneal cavity after i.p. LAC-4 infection
To characterize the host innate immune responses to i.p. LAC-4 infection, total number of peritoneal lavage cells and their subpopulations from mice i.p. inoculated with a lethal (107 CFU) or sublethal (5 × 104 CFU) dose of LAC-4 were examined. As anticipated, macrophages and lymphocytes were the predominant types of peritoneal cells at 0 h, followed by mast cells and eosinophils. Neutrophils were almost absent at this time point (Figs 3 and S1). At 4 h p.i., the total number of peritoneal cells was not significantly changed in lethally infected mice, but the number and percentage of peritoneal neutrophils and, to a lesser extent, eosinophils were significantly increased (P < 0.05). Accordingly, the total number and particularly the percentage of peritoneal macrophages and lymphocytes were significantly decreased (Figs 3 and S1).
Peritoneal inflammatory cell responses in mice with a lethal or sublethal intraperitoneal infection of A. baumannii LAC-4. Groups of C57BL/6 mice (n = 5) were inoculated i.p. with a lethal (1 × 107 CFU, 4 h only) or sublethal (5 × 104 CFU) dose of LAC-4 and killed at 0, 4, 24, 48, 72 and 168 hours post-inoculation. The peritoneal cavity was lavaged, and the total cell counts were determined with a hemacytometer and differential cell counts were determined on cytospin slides (Cytospin 3, Shandon, Pittsburgh, PA) stained with Hema-3 (Fisher Scientific, Kalamazoo, MI). Data from individual mouse are presented as scatter plot and the horizontal bar represents the mean. The results are representative of at least two independent experiments with similar results. *p < 0.05 vs. 0 h group (One-way ANOVA with Dunnet’s multiple comparisons test).
Similar to the lethally infected mice, the sublethally infected mice showed no significant change in the total number of peritoneal cells at 4 h p.i. (Figs 3 and S1), despite the presence of nearly 107 CFU LAC-4 in the peritoneal lavage fluid at this time point (Fig. 2B). The total number of peritoneal cells in the sublethally infected mice was significantly increased at 24 h p.i., peaked at 48 h p.i. and remained significantly above baseline at day 7 (Figs 3 and S1). In addition, both the proportion and total number of peritoneal neutrophils were increased at 4 h p.i., peaked between 24 and 48 h p.i., and remained higher than baseline level by day 7 (Figs 3 and S1). Although the percentage of peritoneal macrophages was significantly reduced at 4 and 24 h p.i. as a result of increased neutrophil recruitment, the total number of macrophages was not significantly affected at those time points and was significantly increased thereafter (P < 0.05). Both the total number and percentage of peritoneal lymphocytes were significantly decreased at 4, 24 and 48 h p.i., began to recover at 72 h p.i. and returned to the baseline level at 168 h p.i. Although some statistically significant changes in the total numbers of eosinophils and mast cells were observed at some time points after the infection, their total numbers and associated changes were overall minor (Figs 3 and S1).
We also analyzed the phenotype changes of peritoneal cells in the sublethally infected mice over the course of the infection (0 to 168 h p.i.). A representative result from three independent experiments is shown in Fig. 4. The percentage of CD11b+ peritoneal cells was significantly increased between 4 and 96 h p.i. whereas the percentage of CD11c+ cells significantly decreased from 24 h p.i. and thereafter, and did not return to the baseline level at 168 h p.i., the end of our study (Fig. 4A). Consistent with the cytology data, the percentages of F4/80+ and Gr-1+ cells were significantly decreased or increased respectively; these changes peaked at 24 h p.i. (Fig. 4A). In addition, there was significant reduction in the percentage of F4/80+ cells at 168 h p.i. (Fig. 4A).
Activation of F4/80+ peritoneal macrophages following intraperitoneal inoculation with A. baumannii LAC-4. Groups of C57BL/6 mice were i.p. inoculated with 3.3 × 104 CFU of freshly cultured LAC-4. Mice were euthanized at the indicated times and the peritoneal cavity was lavaged. The expression of CD11b+, CD11c+, F4/80+, Gr-1+, CD19+ and CD3+ cells (A,C) as well as the expression of CD40, CD80, CD86 and MHC-II by F4/80+ macrophages (B) and TCRβ and TCRγδ by CD3+ lymphocytes (C), measured as mean fluorescence intensity (MFI), was determined by FACS analysis. Data are compiled from two independent experiments (n = 3 for each experiment) with similar results, and are presented as mean ± SD of % positive cells. *p < 0.05; **p < 0.01; ***p < 0.001 vs 0 h (One-way ANOVA with Dunnet’s multiple comparisons test).
Analysis of the activation markers on F4/80+ peritoneal macrophages showed a significant increase in the percentage of CD80+ macrophages and decrease in the percentages of CD86+ or MHC-II expressing macrophages while the percentage of CD40+ macrophages generally showed no substantial changes over the course of the infection (Fig. 4B). As anticipated, the majority of the peritoneal lymphocytes are CD19+ B cells with small percentage of CD3+ T cells (Fig. 4C). The percentage of CD19+ lymphocytes decreased significantly at 24 h p.i. but returned almost to the baseline level by 48 h. On the other hand, there were no significant changes in the percentages of CD3+ cells until day 7 when its percentage increased significantly (Fig. 4C). Within CD3+ cells, overall there were no significant changes in the proportions of αβTCR+ or γδTCR+ cells, except that the percentage of γδTCR+ cells were significantly, but with large variations, increased at 24 h p.i. (Fig. 4C).
Intraperitoneal LAC-4 infection induces potent local and systemic proinflammatory cytokine and chemokine responses
To further characterize the inflammatory and innate immune responses to i.p. LAC-4 infection and their potential implication in the infection pathogenesis, local (peritoneal lavage fluid) and systemic (serum) levels of a panel of 21 proinflammatory cytokines and chemokines were determined at various time points after infection; several of these have previously been implicated in the immunopathogenesis of A. baumannii infection in mouse models of i.p., i.v., and i.n. infections and in human cell culture studies4,15,18,21,23. Compared to 0 h, lethally infected mice showed significant increases in the levels of 14 out of the 21 chemokines/cytokines measured in the peritoneal lavage fluid at 4 h p.i. (Fig. 5) whereas the sublethal infection induced a transient elevation in the level of IL-1α, IL-1β, IL-6, KC, MCP-1, MIP-1β and TNF-α in the peritoneal lavage fluid; these levels peaked at 4 h p.i. and generally returned to the baseline level by 48 h p.i. (Fig. 5).
Cytokine and chemokine levels in the peritoneal lavage fluid and sera of C57BL/6 mice following lethal or sublethal i.p. LAC-4 infection. Groups of C57BL/6 mice (n = 5) were i.p. inoculated with 1 × 107 (lethal) or 5 × 104 (sublethal) CFU of LAC-4, and sacrificed at the indicated hours post-inoculation. Cytokine and chemokine levels were determined in the sera and peritoneal lavage fluid using 21-plex Milliplex mouse cytokine/chemokine kits on a Luminex 100IS system. The detection limit for all cytokines and chemokines is <10 pg/ml (dot lines). All values are mean ± SD. *p < 0.05; **p < 0.01; ***p < 0.001 vs 0 h (One-way ANOVA with Dunnet’s multiple comparisons test). The levels of IL-2, IL-3, IL12p70, IL-13, and VEGF were below <10 pg/ml in all samples assayed and they were not plotted in the graph for clarity purpose.
Similarly, i.p. inoculation of mice with a lethal dose (107 CFU) of LAC-4 induced significant elevation of serum levels of GM-CSF, IL-10, IL-12p40, IL-1β, IL-5, IL-6, KC, MCP-1, MIP-1β, RANTES, and TNF-α at 4 h p.i. (Fig. 5). Mice receiving a sublethal dose (5 × 104 CFU) of LAC-4 i.p. inoculation showed significant increases in the serum levels of IL-6, IL-10, IL-12p40, KC, MCP-1, MIP-1β, RANTES and TNF-α only at 4 h and almost all those elevated cytokines/chemokines returned to the baseline levels by 48 h (Fig. 5). There were no significant changes in the serum levels of IFN-γ, IL-4 or IL-9, or any of the other analytes tested (IL-2, IL-3, IL-12p70, IL-13, and VEGF) at any time point, regardless of the inoculation doses used. These results suggest that the sublethal i.p. infection with LAC-4 is a relatively acute and severe one but the host is able to control the infection and clear the infection rapidly and efficiently under normal circumstance.
In vitro cytokine/chemokine responses by peritoneal macrophages to killed LAC-4
Macrophages are one of the predominant residential innate immune cells in the peritoneal cavity. Previous studies by us and others have shown that macrophages play important roles in the early host defense against A. baumannii and other Gram-negative bacterial pathogens15,19,24,25. To further understand the interaction between LAC-4 and peritoneal macrophages, we examined the chemokine and cytokine responses to in vitro formalin-fixed LAC-4 (ffLAC-4) stimulation by cultured peritoneal macrophages (Fig. 6). In corroboration with the in vivo serum and peritoneal lavage fluid data from the infected mice (Fig. 5), the levels of IL-6, IL-10, KC, MIP-1β, RANTES, and TNF-α were significantly increased in the culture supernatant of peritoneal macrophages at both 24 and 48 h whereas the GM-CSF level increased at 24 h only and the levels of IL-1α, IL-1β, and MCP-1 increased at 48 h only. Levels of IL-2, IL-3, IL-4, IL-5, IL-9, IL-12p40, IL-12p70, IL-13, IL-17, IFN-γ and VEGF remained unchanged at both time points (data not shown).
Proinflammatory cytokine and chemokine responses by formalin-fixed LAC-4 (ffLAC-4)-stimulated peritoneal macrophages. Peritoneal lavage cells were harvested from 8–10 wk-old, female C57BL/6 mice (n = 5) and 5 × 105 cells were incubated with ffLAC-4 (MOI = 100) or culture media alone. Medium (DMEM) was supplemented with 10% FBS, 5.5 µM 2-Mercaptoethanol, 25 mg/ml 4-(2-hydroxyethyl)-1-piperazineethanesulfonic acid (HEPES) and non-essential amino acids (MEM-NEAA). Cell culture supernatants were collected at 24 and 48 h. The concentrations of indicated cytokines/chemokines were measured using a 21-plex Milliplex mouse cytokine/chemokine kit on a Luminex 100IS system. The detection limit for all cytokines and chemokines is <10 pg/ml. Data are presented as scatter plot of duplicate culture wells, and the horizontal bar represents the mean. *P < 0.05, **P < 0.01, ***P < 0.001 vs media group (Two-way ANOVA with Sidak’s multiple comparisons test).
Role of peritoneal macrophages in resistance to i.p. LAC-4 infection in mice
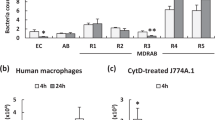
Results of the above experiments and from previous studies by other laboratories suggest that macrophages may play an important role in host defense against i.p. LAC-4 infection15,19,24,25. To obtain direct evidence of the contribution of macrophages in host defense against i.p. LAC-4 infection, groups of C57BL/6 mice were i.p. treated with clodronate-liposomes to deplete peritoneal macrophages (depleted mice) or PBS-liposomes as treatment control (control mice). Twenty-four hours later, the mice were i.p. inoculated with 4.8 × 104 CFU LAC-4, and bacterial burdens in the peritoneal lavage fluid, blood, lung, and spleen were determined 4 and 24 h p.i. Compared to control mice, the bacterial burdens in the depleted mice at 4 h p.i. were generally comparable (peritoneal lavage fluid) or slightly higher (blood and other tissues) (Fig. 7). At 24 h p.i., significantly higher numbers of bacteria were recovered in all examined tissues of depleted mice (P < 0.001 for peritoneal lavage fluid and P < 0.01 for blood, spleen and lung, respectively) (Fig. 7). In addition, the bacterial burdens were generally reduced in the tissues and blood at 24 h p.i. as compared to 4 h p.i., with the exception of the lungs where the bacterial burdens were higher.
In vivo macrophage depletion enhances the host susceptibility to i.p. A. baumannii LAC-4 infection. Groups of C57BL/6 mice were i.p. treated with either clodronate-liposomes (clodronate) to deplete peritoneal macrophages or PBS-liposomes (PBS) as sham-depletion controls. Twenty-four hours later, all mice were i.p. inoculated with 4.8 × 104 CFU freshly cultured A. baumannii LAC-4. Five mice from each group were euthanized at 4 and 24 h post-inoculation. The bacterial burdens in the peritoneal lavage fluid, blood, spleen, and lung were determined by quantitative bacteriology. Data from individual mouse are presented as scatter plot and the horizontal bar represents the mean (n = 5). **P < 0.01 and ***P < 0.001 (Two-way ANOVA with Sidak’s multiple comparisons test).
Discussion
Septicemia is one of the major clinical manifestations of A. baumannii infection3,4. The mouse model of i.p. A. baumannii infection has been commonly used for infection pathogenesis studies and for anti-A. baumannii therapeutics and vaccines evaluation. However, there are surprisingly few studies on the characterization of this model15,17,21,26. In this study, we described a mouse model of i.p. A. baumannii infection using a hypervirulent strain and commonly used mouse strains, and characterized the innate cellular and proinflammatory cytokine responses to the infection. Our results shared several similarities with other published studies in which the innate immune responses to i.p. infection with a clinical A. baumannii strain have been examined in some details15,17,26. The infected mice either succumb to the infection very rapidly or completely recover from the infection within 1–2 days. These results suggest that the i.p. A. baumannii infection in mice appears to fit a “single-hit” infection model27. Similar to most A. baumannii clinical and type strains studied, the minimal dose of LAC-4 needed to cause a lethal i.p. infection (106 CFU) is substantially lower than that of i.n. inoculation (~108 CFU)12.
The reason for the observed hypervirulence of LAC-4 in mice remains unknown. The ability of rapid systemic dissemination by LAC-4 was originally postulated as a potential contributing factor for its high virulence in i.n. inoculation12. However, the systemic dissemination is irrelevant in i.v. infection19 and only play a limited role in i.p infection in this study, suggesting that other unidentified mechanisms may contribute to the hypervirulence of this strain.
To the best of our knowledge, LAC-4 is one of only a few reported clinical and type A. baumannii strains/isolates that are hypervirulent to commonly used immunocompetent mice (such as C57BL/6 and BALB/c mice) and which cause 100% mortality within 48 hours of inoculation15,18,19,20,21,23,28,29. Previous studies by others have generally used porcine mucin or immunocompromised mice (such as neutropenic or diabetic mice)21,23,30,31,32,33 to enhance bacterial virulence or host susceptibility, in order to ensure a successful infection. Alternatively, a large inoculation dose (up to 1010 CFU) is required to induce an infection in conventional mice34. The ability to use a low challenge inoculum and conventional mouse strains (such as BALB/c and C57BL/6) in the experimental model described here has several advantages over other models. These include the likely mimicry of human natural infection and a better model reproducibility. In addition, the presence of an intact immune system would allow for the study of the interaction between bacterial infection and host immune system, and for evaluation of immune-based anti-A baumannii therapeutics. Moreover, LAC-4 is a multidrug resistant strain and its genome is fully sequenced and annotated18,22,35. However, it should be noted that LAC-4 displays a genomic profile distinct from most of the other outbreak isolates reported to date, as well as from ATCC 17978, ATCC 19606 and AYE strains22; this may limit the utilization of this model to certain type of studies.
Results of the kinetics and tissue bacterial burden study suggest that LAC-4 possesses unique capabilities of rapid local replication and systemic dissemination to blood and other tissues. The presence of higher bacterial burdens than the initial inoculum at the site of inoculation (peritoneal cavity) and blood at 4 h p.i. is noteworthy because various A. baumannii strains/isolates reported to date generally do not replicate in immunocompetent mice16,19,20,21,23,36,37. The immediate, net increase in the local LAC-4 burden suggests that this strain is capable of evading the host innate immunity since the doubling time of this strain in in vitro culture is similar to other A. baumannii strains19. Our previous studies in the mouse model of i.n. infection also suggests that the host innate immunity appears to be less effective in controlling LAC-4 proliferation as compared to some ATCC strains or clinical isolates18.
Similar to i.n. A. baumannii infection in mice, i.p. LAC-4 infection induced a rapid recruitment of neutrophils and associated reduction in the percentages of peritoneal macrophages and lymphocytes (Fig. 3). We and others have shown that neutrophils and macrophages play important roles in host innate resistance to different routes of A. baumannii infection23,31,38. It has also been demonstrated that neutrophils, but not NK1.1+ cells, play a crucial role in host defense against i.p. A. baumannii infection15. However, the role of macrophages remains unknown. In this study, we found that the tissue and blood bacterial burdens in macrophage-depleted mice were significantly higher than macrophage-intact mice following i.p. LAC-4 challenge (Fig. 7), suggesting that macrophages also play an important role in host defense against i.p. A. baumannii infection19,24. In this regard, our preliminary FACS analysis of the subpopulation and activation of peritoneal cells (Fig. 4) indicates a substantial reduction in the surface expression of CD86 co-stimulation molecule and MHC-II by F4/80+ peritoneal macrophages at 24 h.p.i. This suggests that the LAC-4 is able to suppress the macrophage activation and its function, which may in turn contribute to the subsequent clinical outcome of the infected mice. On the other hand, the infection showed minimal effects on the composition of B or T lymphocytes with the exception that the proposition of γδT cells were significantly increased at 24 h.p.i. Since it is well recognized that the peritoneal macrophages are heterogeneous populations with distinct development and function and mount dynamic responses to infection39, further detailed profiling and characterization of this population of cells in response to A. baumannii will be needed.
As reported in other A. baumannii infection studies in mice and in human cell cultures, i.p. LAC-4 infection induced significant increases in the local and systemic levels of many different cytokines/chemokines (Fig. 5). It has been suggested that the cytokine/chemokine response observed in the infected mice reflects more the high bacterial burdens than it does the host innate immunity23,30,32,33,40. On the other hand, elevated levels (such as TNF-α) are generally not directly related to mortality either40.
We previously profiled the local (lung) and systemic (serum) cytokine/chemokine responses to i.n. LAC-4 infection in mice18. It appears that the cytokine/chemokine response to i.n. and i.p. infection with LAC-4 share a similar profile, in that the serum levels of TNF-α, RANTES, MIP-1β, MCP-1, KC, IL-12p40, IL-6, IL-1β, GM-CSF and anti-inflammatory cytokine IL-10 were significantly increased whereas the IL-17 level was significantly increased only in i.n., but not i.p., infected mice, perhaps reflecting the fact the double negative resident lung T cells are a major IL-17 producing source41. It is interesting to note that the cytokine/chemokine responses at the site of inoculation also shared many similarities, despite the distinctive anatomic location (peritoneal cavity for i.p. vs lung for i.n.); both routes of LAC-4 inoculation induced significantly increases in the level of IL-1α, IL-1β, IL-6, MIP-1β, MCP-1, and KC and, to a lesser magnitude, TNF-α and RANTES in the peritoneal or lung lavage fluid, respectively (Fig. 5). On the other hand, GM-CSF and IL-17 were increased only in the lung lavage fluid following i.n. LAC-4 infection18, likely reflecting the anatomical differences in the type of resident cytokine-producing cells and the regulatory pathway of these cytokines.
As anticipated, both quantitative and qualitative differences were observed in the cytokine/chemokine responses to different doses of i.p. LAC-4 inoculation (Fig. 5). There was a dose-related difference in the level of RANTES and IL-10 in the peritoneal lavage fluid, whereas increases in IFN-γ, IL-17, IL-4, IL-5 and IL-9 were only observed in the mice challenged with the high dose of LAC-4. On the other hand, the cytokine/chemokine changes in the serum were more dose-related. Those results suggest that the local and systemic cytokine/chemokine responses to A. baumannii in mice are largely related to the challenge strain and dose used and less influenced by the challenge route. Further studies and detailed analysis of the cytokine and chemokine responses will be needed to better understand their role in the infection pathogenesis and host defense.
As in i.p. LAC-4 infected mice, in vitro stimulation of peritoneal macrophages with ffLAC-4 induced high levels of TNF-α, RANTES, MIP-1β, MCP-1, KC, GM-CSF, IL-10, IL-6, IL-1α and IL-1β production in the culture supernatant (Fig. 6), suggesting that macrophages participate in the early inflammatory responses and host defense against i.p. LAC-4 infection and contribute to the initiation of a cascade of proinflammatory cytokine/chemokine production and innate immune cell recruitment.
In conclusion, our study has demonstrated that i.p. LAC-4 infection of immunocompetent C57BL/6 and BALB/c mice induces a lethal or sublethal infection, depending on the inoculation dose, with high bacterial burdens in peritoneal cavity, blood and tissues. The infection induces acute peritoneal recruitment of neutrophils and other innate immune cells, as well as the local and systemic production of proinflammatory cytokines and chemokines. This mouse infection model will provide an alternative and useful tool for future pathogenesis studies of A. baumannii-associated septicemia and identification and characterization of important virulence factors, and can serve as a surrogate model for rapid evaluation of novel therapeutics and vaccines for this emerging infectious agent.
Methods
Mice
Eight- to 12-wk-old specific-pathogen-free female C57BL/6 and BALB/c mice were purchased from Charles River Laboratories (St. Constant, Quebec). The mice were maintained and used in accordance with the recommendations of the Canadian Council on Animal Care Guide to the Care and Use of Experimental Animals. All experimental procedures were approved by the institutional animal care committee (Institute for Biological Sciences, National Research Council Canada).
A. baumannii
A. baumannii ATCC 17961 (American Tissue Type Culture, Manassas, VA) and LAC-4 were used in the study. LAC-4 is a multidrug resistant clinical isolate originally from an endemic outbreak in a hospital at the Los Angeles County42 and has been demonstrated to be a hypervirulent isolate in mice by i.n. or i.v. inoculation18,19.
Intraperitoneal A. baumannii inoculation and sample collections
For i.p. inoculation in mice, freshly cultured inocula were prepared for each experiment from frozen stocks of A. baumannii as previously described23. Mice were inoculated with indicated numbers of A. baumannii in 100 µl saline using a 1.0 ml tuberculin syringe with a 30 G needle. Actual inocula in each experiment were determined by plating 10-fold serial dilutions on brain-heart infusion (BHI) agar plates. The clinical appearance of the mice was monitored and scored as described previously23. Groups of three to five infected mice were sacrificed at pre-determined time points post inoculation. The peritoneal cavity was lavaged with 10 ml of phosphate buffered saline (PBS) supplemented with 3 mM Ethylenediaminetetraacetic acid (EDTA) and 1% fetal bovine sera (FBS). Blood samples were collected for bacterial culture or serum separation. The lungs, spleens, and kidneys were aseptically removed and used for quantitative bacteriology.
Quantitative bacteriology
The lungs, spleen and kidneys were homogenized in sterile saline using aerosol-proof homogenizers. Aliquots (100 µl) of 10-fold serial dilutions of the tissue homogenates, whole blood, and peritoneal lavage fluid were cultured on BHI agar plates to quantify the number of viable A. baumannii in the respective samples23.
Quantification and FACS analysis of peritoneal lavage cells
The total number of peritoneal lavage cells was determined with a hemacytometer and differential cell counts were determined on cytospin slides (Cytospin 3, Shandon, Pittsburgh, PA) stained with Hema-3 (Fisher Scientific, Kalamazoo, MI)18. The lavage fluid was centrifuged at 2,450 × g for 7 min, and the supernatant collected, filter-sterilized and stored at −20 °C.
The percentage and activation of some peritoneal cell populations were also determined by FACS analysis as described previously24 and in Supplementary Methods. Briefly, the cells were washed in PBS containing 1% BSA, and incubated with unlabeled anti-CD16/CD32 (clone 2.4G2) monoclonal antibodies (BD Biosciences, San Jose, CA) for 15 min to block non-specific Fc receptor binding. Aliquots containing ~106 cells were stained with antibody cocktails containing appropriate fluorochrome-conjugated mAb for 30 min at 4 °C. The anti-F4/80 mAb was used as a marker for macrophages and the activation of F4/80+ macrophages was further analyzed using anti-CD80 (clone 16–10A1), anti-CD86 (clone GL1), anti-CD40 (clone 3/23), and anti-MHCII (AF6-120.1) antibodies. After staining, the cells were washed twice with the above PBS/BSA solution, fixed with 200 μl of 1% paraformaldehyde (Polysciences Inc., Warrington, PA), and stored in the dark at 4 °C until ready for analysis. The data were acquired using a FACS Canto flow cytometer (BD Biosciences) and analyzed using FlowJo software (Tree Star, Inc., Ashland, OR).
Production of cytokines and chemokines by A. baumannii-stimulated peritoneal macrophages
In some experiments, the peritoneal lavage cells from uninfected mice were harvested. One ml aliquots of the cells (5 × 105 cells/ml) were seeded into 24-well tissue culture plates (Becton Dickinson, Mississauga ON), and stimulated with 5 × 107 formalin-fixed LAC-4 cells (ffLAC-4) or media only as controls43. Culture supernatants were harvested at 24 or 48 h after the addition of ffLAC-4, centrifuged, and stored at −20 °C until assay.
Cytokine and chemokine assays
Levels of cytokines and chemokines in the sera, peritoneal lavage fluid, and cell culture supernatant were measured using 21-plex Milliplex MAP mouse cytokine/chemokine kits (Millipore, Ltd. Billerica, MA) on a Luminex 100IS system (Luminex, Austin, TX), as specified by the manufacturer. Samples were assayed in duplicate, and cytokine/chemokine concentrations were calculated against the standards using Beadview software (ver 1.03, Upstate)23.
In vivo macrophage depletion
Peritoneal macrophages were depleted by i.p. administration of liposomes encapsulated dichloromethylene diphosphonate (clodronate, or CL2MDP). Liposomes containing clodronate (clodronate-liposomes) and liposomes encapsulating PBS (PBS-liposomes) were purchased from Liposoma BV (Amsterdam, Netherland). Groups of five C57BL/6 mice were i.p. injected with 100 µl of clodronate-liposomes or PBS-liposomes at 24 and 4 h prior to infection. Mice were then inoculated i.p. with 5 × 104 CFU LAC-4 as described above. Infected mice were sacrificed at 4 and 24 h p.i., and the blood, peritoneal lavage fluid, lungs, and spleens were aseptically collected, and used for quantitative bacteriology23.
Statistical analysis
Data are presented as means ±SD for each group, unless otherwise specified. Differences in quantitative measurements were assessed by Student’s t test, one-way or two-way analysis of variance (ANOVA) followed by Bonferroni’s post-hoc multiple comparison tests, when appropriate. Differences were considered significant when P < 0.05.
Data Availability
The datasets generated during and/or analysed during the current study are available from the corresponding author on reasonable request.
References
Kuo, L. C. et al. Multidrug-resistant Acinetobacter baumannii bacteraemia: clinical features, antimicrobial therapy and outcome. Clin. Microbiol. Infect. 13, 196–198 (2007).
Joly-Guillou, M. L. Clinical impact and pathogenicity of Acinetobacter. Clin. Microbiol. Infect. 11, 868–873 (2005).
Peleg, A. Y., Seifert, H. & Paterson, D. L. Acinetobacter baumannii: emergence of a successful pathogen. Clini. Microbiol. Rev. 21, 538–582 (2008).
McConnell, M. J., Actis, L. & Pachon, J. Acinetobacter baumannii: human infections, factors contributing to pathogenesis and animal models. FEMS Microbiol. Rev. 37, 130–155 (2013).
Fournier, P. & Richet, H. The epidemiology and control of Acinetobacter baumannii in health care facilities. Clin. Infect. Dis. 42, 692–699 (2006).
Tipton, K. A., Chin, C. Y., Farokhyfar, M., Weiss, D. S. & Rather, P. N. Role of capsule in resistance to disinfectants, host antimicrobials, and desiccation in Acinetobacter baumannii. Antimicrob. Agents Chemother. 62, e01188–18 (2018).
https://www.who.int/medicines/publications/global-priority-list-antibiotic-resistant-bacteria/en/.
Ballouz, T. et al. Risk Factors, Clinical Presentation, and Outcome of Acinetobacter baumannii Bacteremia. Front. Cell Infect. Microbiol. 7, 156, https://doi.org/10.3389/fcimb.2017.00156 (2017).
Dinc, G. et al. Antimicrobial efficacy of doripenem and its combinations with sulbactam, amikacin, colistin, tigecycline in experimental sepsis of carbapenem-resistant Acinetobacter baumannii. New Microbiol. 38, 67–73 (2015).
Ostorhazi, E. et al. Intramuscularly administered peptide A3-APO is effective against carbapenem-resistant Acinetobacter baumannii in mouse models of systemic infections. Biopolymers 96, 126–129 (2011).
Lopez-Rojas, R. et al. Efficacy of cecropin A-melittin peptides on a sepsis model of infection by pan-resistant Acinetobacter baumannii. Eur. J. Clin. Microbiol. Infect. Dis. 30, 1391–1398 (2011).
Harris, G., KuoLee, R., Xu, H. H. & Chen, W. Mouse models of Acinetobacter baumannii infection. Curr.Protocols Microbiol. 46, 6G 3 1-6G 3 23 (2017).
McConnell, M. J., Rumbo, C., Bou, G. & Pachon, J. Outer membrane vesicles as an acellular vaccine against Acinetobacter baumannii. Vaccine 29, 5705–5710 (2011).
Lopez-Rojas, R. et al. Impaired virulence and in vivo fitness of colistin-resistant Acinetobacter baumannii. J. Infect. Dis. 203, 545–548 (2011).
Breslow, J. M. et al. Innate immune responses to systemic Acinetobacter baumannii infection in mice: neutrophils, but not interleukin-17, mediate host resistance. Infect. Immun. 79, 3317–3327 (2011).
Luo, G. et al. Diabetic murine models for Acinetobacter baumannii infection. J. Antimicrob. Chemother. 67, 1439–1445 (2012).
Murray, G. L. et al. Global gene expression profile of Acinetobacter baumannii during bacteremia. J. Infect. Dis. 215, S52–S57 (2017).
Harris, G. et al. A mouse model of Acinetobacter baumannii-associated pneumonia using a clinically isolated hypervirulent strain. Antimicrob. Agents Chemother. 57, 3601–3613 (2013).
Bruhn, K. W. et al. Host fate is rapidly determined by innate effector-microbial interactions during Acinetobacter baumannii bacteremia. J. Infect. Dis. 211, 1296–1305 (2015).
Jacobs, A. C. et al. AB5075, a highly virulent isolate of Acinetobacter baumannii, as a model strain for the evaluation of pathogenesis and antimicrobial treatments. MBio 5, e01076–01014 (2014).
Ketter, P. M. et al. Severe Acinetobacter baumannii sepsis is associated with elevation of pentraxin 3. Infect. Immun. 82, 3910–3918 (2014).
Ou, H. Y. et al. Complete genome sequence of hypervirulent and outbreak-associated Acinetobacter baumannii strain LAC-4: epidemiology, resistance genetic determinants and potential virulence factors. Sci. Rep 5, 8643, https://doi.org/10.1038/srep08643 (2015).
van Faassen, H. et al. Neutrophils play an important role in host resistance to respiratory infection with Acinetobacter baumannii in mice. Infect. Immun. 75, 5597–5608 (2007).
Qiu, H. et al. Role of macrophages in early host resistance to respiratory Acinetobacter baumannii infection. PLoS One 7, e40019, https://doi.org/10.1371/journal.pone.0040019 (2012).
Garcia-Patino, M. G., Garcia-Contreras, R. & Licona-Limon, P. The immune response against Acinetobacter baumannii, an emerging pathogen in nosocomial infections. Front. Immunol. 8, 441, https://doi.org/10.3389/fimmu.2017.00441 (2017).
Breslow, J. M. et al. Morphine, but not trauma, sensitizes to systemic Acinetobacter baumannii infection. J. Neuroimmune Pharmacol. 6, 551–565 (2011).
Noecker, C. et al. Simple mathematical models do not accurately predict early SIV dynamics. Viruses 7, 1189–1217 (2015).
Joly-Guillou, M. L. & Wolff, M. In Acinetobacter Biology and Pathogenesis. (eds E. Bergogne-Berezin, H. Friedman, & M. Bendinelli) 167–174 (Springer 2008).
McConnell, M. J. et al. Vaccination with outer membrane complexes elicits rapid protective immunity to multidrug-resistant Acinetobacter baumannii. Infect. Immun. 79, 518–526 (2011).
Eveillard, M. et al. The virulence variability of different Acinetobacter baumannii strains in experimental pneumonia. J. Infect. 60, 154–161 (2010).
Joly-Guillou, M. L., Wolff, M., Pocidalo, J. J., Walker, F. & Carbon, C. Use of a new mouse model of Acinetobacter baumannii pneumonia to evaluate the postantibiotic effect of imipenem. Antimicrob. Agents Chemother. 41, 345–351 (1997).
Qiu, H., KuoLee, R., Harris, G. & Chen, W. High susceptibility to respiratory Acinetobacter baumannii infection in A/J mice is associated with a delay in early pulmonary recruitment of neutrophils. Microbes Infect. 11, 946–955 (2009).
Qiu, H., KuoLee, R., Harris, G. & Chen, W. Role of NADPH phagocyte oxidase in host defense against acute respiratory Acinetobacter baumannii infection in mice. Infect. Immun. 77, 1015–1021 (2009).
Cirioni, O. et al. Colistin enhances therapeutic efficacy of daptomycin or teicoplanin in a murine model of multiresistant Acinetobacter baumannii sepsis. Diagn. Microbiol. Infect. Dis. 86, 392–398 (2016).
Valentine, S. C. et al. Phenotypic and molecular characterization of Acinetobacter baumannii clinical isolates from nosocomial outbreaks in Los Angeles County, California. J. Clin. Microbiol. 46, 2499–2507 (2008).
Bentancor, L. V., O’Malley, J. M., Bozkurt-Guzel, C., Pier, G. B. & Maira-Litran, T. Poly-N-acetyl-beta-(1-6)-glucosamine is a target for protective immunity against Acinetobacter baumannii infections. Infect. Immun. 80, 651–656 (2012).
Bentancor, L. V. et al. Evaluation of the trimeric autotransporter Ata as a vaccine candidate against Acinetobacter baumannii infections. Infect. Immun. 80, 3381–3388 (2012).
Asplund, M. B., Coelho, C., Cordero, R. J. & Martinez, L. R. Alcohol impairs J774.16 macrophage-like cell antimicrobial functions in Acinetobacter baumannii infection. Virulence 4, 467–472 (2013).
Cassado Ados, A., D’Imperio Lima, M. R. & Bortoluci, K. R. Revisiting mouse peritoneal macrophages: heterogeneity, development, and function. Front. Immunol. 6, 225, https://doi.org/10.3389/fimmu.2015.00225 (2015).
Russo, T. A. et al. Rat pneumonia and soft-tissue infection models for the study of Acinetobacter baumannii biology. Infect. Immun. 76, 3577–3586 (2008).
Cowley, S. C., Meierovics, A. I., Frelinger, J. A., Iwakura, Y. & Elkins, K. L. Lung CD4-CD8- double-negative T cells are prominent producers of IL-17A and IFN-gamma during primary respiratory murine infection with Francisella tularensis live vaccine strain. J. Immunol. 184, 5791–5801 (2010).
Chang, H. C. et al. Species-level identification of isolates of the Acinetobacter calcoaceticus-Acinetobacter baumannii complex by sequence analysis of the 16S-23S rRNA gene spacer region. J. Clin. Microbiol. 43, 1632–1639 (2005).
Choi, C., Lee, J., Lee, Y., Park, T. & Lee, J. Acinetobacter baumannii invades epithelial cells and outer membrane protein A mediates interactions with epithelial cells. BMC Microbiol. 8, 216 (2008).
Acknowledgements
This work was partially funded by the intramural program (A-base) of National Research Council Canada.
Author information
Authors and Affiliations
Contributions
H.X. and W.C. conceived all the study. G.H. and R.K.L. performed the experiments and analyzed the data. H.X. and W.C. wrote the manuscript. All authors edited and approved the manuscript.
Corresponding author
Ethics declarations
Competing Interests
The authors declare no competing interests.
Additional information
Publisher’s note: Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary information
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons license, and indicate if changes were made. The images or other third party material in this article are included in the article’s Creative Commons license, unless indicated otherwise in a credit line to the material. If material is not included in the article’s Creative Commons license and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this license, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
Harris, G., KuoLee, R., Xu, H.H. et al. Acute intraperitoneal infection with a hypervirulent Acinetobacter baumannii isolate in mice. Sci Rep 9, 6538 (2019). https://doi.org/10.1038/s41598-019-43000-4
Received:
Accepted:
Published:
DOI: https://doi.org/10.1038/s41598-019-43000-4
- Springer Nature Limited
This article is cited by
-
The aryl hydrocarbon receptor and FOS mediate cytotoxicity induced by Acinetobacter baumannii
Nature Communications (2024)