Abstract
The dysfunction of tight-junction integrity caused by necrotic enteritis (NE) is associated with decreased nutrient absorption and gut injury in broiler chickens. Although probiotic Enterococcus faecium (E. faecium) has been reported to possess immune-regulatory characteristics and can prevent diarrhea in pigs, very little information exists in relation to the specific regulatory impact of E. faecium NCIMB 11181 on NE-induced intestinal barrier injury of broiler chickens. This study was conducted to investigate the protective effects of probiotic E. faecium NCIMB 11181 on NE-induced intestinal barrier injury in broiler chickens. The study also aimed to elucidate the mechanisms that underpin these protective effects. One hundred and eighty Arbor Acres (AA) broiler chicks (one day old) were randomly assigned using a 2 × 2 factorial arrangement into two groups fed different levels of dietary E. faecium NCIMB 11181 (0 or 2 × 108 CFU/kg of diet) and two disease-challenge groups (control or NE challenged). The results showed that NE induced body weight loss, intestinal lesions, and histopathological inflammation, as well as intestinal-cell apoptosis. These symptoms were alleviated following the administration of probiotic E. faecium NCIMB 11181. Pretreatment with probiotic E. faecium NCIMB 11181 significantly upregulated the expression of the Claudin-1 gene encoding a tight-junction protein. Claudin-1 and HSP70 protein expression were also increased in the jejunum regardless of NE infection. Furthermore, NE-infected birds fed with E. faecium displayed notable increases in MyD88, NF-κB, iNOS, PI3K, GLP-2, IL-1β, IL-4, and HSP70 mRNA expression. E. faecium NCIMB 11181 administration also significantly improved the animals’ intestinal microbial composition regardless of NE treatment. These findings indicated that addition of E. faecium NCIMB 11181 to poultry feed is effective in mitigating NE-induced gut injury, possibly by strengthening intestinal mucosal barrier function, as well as modulating gut microflora and intestinal mucosal immune responses.
Similar content being viewed by others
Introduction
Necrotic enteritis (NE) is caused by Clostridium perfringens (C. perfringens) types A and C. C. perfringens is a spore-forming, anaerobic, gram-positive, rod-shaped bacterium that produces a range of necrotizing toxins including α-toxin and NetB toxin1. NE infection in broiler chickens disrupts the composition of their intestinal microbial community2,3,4, damages gut morphology, causes intestinal inflammation, and impairs gut barrier function5,6; these chickens also exhibit increased gut permeability7,8 and depressed growth6. Thus, strategies to alleviate the detrimental effects of NE infection on intestinal mucosal barrier integrity are of great significance for the health of broiler chickens.
Evidence has indicated that the administration of probiotic bacteria improves intestinal function by maintaining paracellular permeability, enhancing the physical mucous layer, stimulating the immune system, and modulating the composition and activity of resident microbiota9. The regulatory effects of probiotics on human, pig, and chicken intestinal homeostasis have been extensively studied10,11, and interactions between probiotic bacteria, commensal bacteria, and the epithelial barrier are thought to be important in this regard. Enterococcus faecium (E. faecium) is one of the most important lactic acid-producing bacterial species belonging to the autochthonous microbiota of human and animal gastrointestinal tracts. The Enterococcus genus is also found in the microbiota of multifarious food sources12,13, with some species being commonly used as probiotics in food preservatives or feed additives because they produce antimicrobial substances such as organic acids and bacteriocins14,15. These species also exert positive effects on disease incidence, do not carry virulence-factor genes, and are sensitive to specific antibiotics12,13,16. In animals, E. faecium probiotics are mainly used to treat or prevent diarrhea, to facilitate immune stimulation, or to improve growth. For example, feed supplementation with probiotic E. faecium has been shown to protect pigs from the pathogenic bacteria E. coli17,18,19. E. faecium also protected against viruses, chlamydia, and parasitic infections in swine and mice20,21,22. Specifically, these protective effects reduced the pathogenic bacterial load in internal organs, impeded virulence-gene expression by resident pathogens, and/or modulated inflammatory responses, thereby reducing the number of piglets suffering from diarrhea and improving their growth performance17,18,19,23,24. Furthermore, studies have shown that the addition of E. faecium to sow feed possibly modified the composition of the pigs’ intestinal bacterial community by increasing the prevalence of beneficial bacteria and reducing pathogenic bacterial load25. In vitro studies have demonstrated that E. faecium can affect trans-epithelial electrical resistance and epithelial permeability while also modulating tight-junction (TJ) protein expression and distribution26,27,28. In addition, results from experiments in poultry have revealed that dietary E. faecium probiotics modulated intestinal microflora composition29,30, restrained the spread of pathogens, stimulated intestinal mucosal immune responses, and enhanced the birds’ resistance to intestinal pathogen infections including those caused by Salmonella, E. coli, Campylobacter, and C. perfringens31,32,33,34.
Probiotic E. faecium strain 11181 is currently authorized by the European Food Safety Authority (EFSA) Panel as a feed supplement for fattening and improving the growth performance of animals16,35. This strain has been shown to effectively increase daily weight gain and improve feed conversion in weaning piglets36. Pajarillo et al.35 also reported that administration of E. faecium NCIMB 11181 to pigs enhanced gut health by promoting the growth of beneficial bacteria and inhibiting the proliferation of gut pathogens. In addition, our previous study also found that adding E. faecium NCIMB 11181 at 5 × 107 CFU/kg to the diet of broiler chickens improved growth performance, while a dietary inclusion of 1–2 × 108 CFU/kg stimulated the systemic immune response of broiler chickens37. However, the effects of probiotics on intestinal barrier function are strain-dependent and not ubiquitous. Moreover, very little information exists regarding the regulatory impact of probiotic E. faecium NCIMB 11181 strains on NE-induced intestinal barrier injury and the associated mechanisms that underpin these reactions. Therefore, the objectives of this study were (1) to test whether oral supplementation with E. faecium NCIMB 11181 protected gut barrier function against NE infection and (2) to characterize the changes of intestinal microbiome as well as the Toll-like receptor (TLR)/NF-κB signal pathway-mediated mucosal immune response.
Results
Growth performance
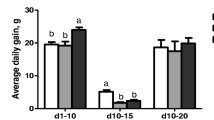
The evaluation of body weight (BW) and body-weight gain (BWG) in broiler chickens in the NE-challenge group is illustrated in Fig. 1. Compared with the unchallenged birds, NE-challenged birds exhibited significant reductions in BW (P < 0.01) and BWG during the specific challenge periods as well as the entire testing period (P < 0.05). A strong interaction between dietary E. faecium and NE infection was observed in relation to BW at day (d) 21 and d 26, and BWG at d 13–21 and d 22–26 (P < 0.05). NE-challenged birds fed diets supplemented with E. faecium showed a significant improvement in BW and BWG compared with NE-challenged birds fed only the basal diet (P < 0.05).
Effect of dietary E. faecium 11181 on growth performance of broiler chickens challenged with NE. (A) Body weight at d 21, 26, and 35 (3, 7, and 15 days post-infection [DPI]). (B) Body-weight gain during d 13–21, d 22–26, d 27–35, and d 1–35 (challenge-3 DPI, 3–7 DPI, 7–17 DPI, and the entire testing period). Individual data points are presented as box plots, showing the median (horizontal lines), the lower and upper quartiles (lower and upper borders of the boxes), and minimum and maximum values (lower and upper whiskers). The different lowercase letters on the bars indicate significant differences (P < 0.05). NC = Non-NE-infected + no E. faecium treatment, NT = non-NE-infected + E. faecium treatment, PC = NE-infected + no E. faecium treatment, PT = NE-infected + E. faecium treatment.
Liver bacterial translocation
A significant cooperative effect (P < 0.05) was found between E. faecium addition and NE infection in terms of C. perfringens invasion of the liver at 7 and 17 day post-infection (DPI, d 26 and 35) (Fig. 2). Challenged birds fed diets supplemented with E. faecium NCIMB 11181 showed lower C. perfringens numbers in the liver at d 26 compared with the NE-infected birds fed a basal diet. In addition, feeding E. faecium significantly reduced the number of C. perfringens cells in the liver compared with the unsupplemented group regardless of challenge (P < 0.05).
Effect of dietary E. faecium 11181 on bacterial translocation to the liver of broiler chickens challenged with NE. Each dot (n = 6) represents an individual sample under different treatments. The lowercase letters on the dots indicate significant differences (P < 0.05). NC = Non-NE-infected + no E. faecium treatment, NT = non-NE-infected + E. faecium treatment, PC = NE-infected + no E. faecium treatment, PT = NE-infected + E. faecium treatment.
Gut lesion scores and histopathological observations
As shown in Fig. 3, although gut lesion scores were not influenced by E. faecium supplementation, NE infection caused a significant increase (P < 0.05) in gut lesion scores in uninfected birds at 7 DPI (d 26). In addition, there was a notable interactive effect (P < 0.05) between E. faecium supplementation and NE challenge in relation to the jejunum lesion scores at 3 DPI (d 21); NE-infected birds receiving E. faecium-supplemented diets exhibited a significant score decrease at 3 DPI (P < 0.05). Figure 4A–D shows the histopathological observations at 7 DPI, which revealed that the lesions in the NC (birds without NE infection and feed without E. faecium, Fig. 4A) and NT (birds without NE infection, but feed supplemented with E. faecium, Fig. 4B) groups were only found in the mucosal layer. The intestinal glands were arranged closely without significant reduction. We observed inflammatory-cell infiltration in the lamina propria, which included plasmocytes and the lymphocytes (black arrows). In the PC group (birds infected with NE, but feed without E. faecium, Fig. 4C), the lesion was serious and invaded the submucosal and muscle layer. The mucosa was not visible and more necrotic cell clusters were observed with shrunken nucleoli or karyorrhexis and karyolysis (red arrow). In addition, a large amount of inflammatory-cell infiltration was observed including heterophils, granulocytes, and lymphocytes (black arrows). Furthermore, connective tissue hyperplasia and inflammatory-cell infiltration appeared in the submucosal and muscle layer (yellow arrow). The lesion injury in the PT group (birds infected with NE, and feed supplemented with E. faecium, Fig. 4D) was only in the mucosal layer and did not invade the submucosal and muscle layer. The intestinal glands in the mucosa were loosely arranged and fewer in number (red arrow), and inflammatory-cell infiltration in connective tissue was observed mainly in lymphocytes (black arrow). Histopathological analysis (Fig. 4E) revealed that the NE challenge resulted in an increase in the pathological grade of the jejunum, while NE-induced morphological/structural damage of the intestine and inflammation were attenuated by supplementation with E. faecium NCIMB 11181.
Effect of dietary E. faecium 11181 on lesion scores in the jejunum of broiler chickens challenged with NE. Values are means (n = 6) with the standard error of the mean (SEM) represented by vertical bars. The lowercase letters on the bars indicate significant differences (P < 0.05). NC = Non-NE-infected + no E. faecium treatment, NT = non-NE-infected + E. faecium treatment, PC = NE-infected + no E. faecium treatment, PT = NE-infected + E. faecium treatment.
Effect of dietary E. faecium 11181 on histopathological changes and pathological grade of the jejunum of broiler chickens challenged with NE at d 26 (7 DPI). Histopathological changes in the (A) the NC group, (B) the NT group, (C) the PC group, and (D) the PT group. (E) Histopathological grade of the jejunum at d 26 (7 DPI). Values are means (n = 6) with SEM represented by vertical bars. Magnification = 400×. The black arrow shows inflammatory-cell infiltration, the red arrow shows the necrotic cell clusters with shrunken nucleoli or karyorrhexis and karyolysis, and the yellow arrow shows the connective tissue hyperplasia and inflammatory-cell infiltration in the submucosal and muscle layer.
Intestinal-cell proliferation and apoptosis
The proliferation (brownish, PCNA-positive cells) and apoptosis (brownish, TUNEL-positive cells) of the epithelial cells at d 26 in the jejunum are shown in Figs 5 and 6, respectively. Although NE infection had no significant effect on cell proliferation and apoptosis in the jejunum compared with non-infected birds, E. faecium administration resulted in an obvious increase (P < 0.05) in the number of PCNA-positive cells (cell proliferation marker) and an obvious reduction (P < 0.05) in the number of TUNEL-positive cells (cell apoptosis marker) in the jejunal villus compared with that of untreated birds.
Effect of dietary E. faecium 11181 on the percentage of PCNA-positive cells in the jejunum of broiler chickens challenged with NE at d 26 (7 DPI). PCNA protein expression was assessed in jejunum tissue by immunohistochemistry using the anti-PCNA antibody in (A) the NC group, (B) the NT group, (C) the PC group, and (D) the PT group. The red arrow points out a PCNA-positive cell in the jejunal crypt and the yellow arrow points out a PCNA-positive cell in the jejunal villus. (E) Integral optical density (IOD) of PCNA expression. Values are means (n = 6) with SEM represented by vertical bars. Magnification = 400×.
Effect of dietary E. faecium 11181 on the percentage of TUNEL-positive cells in the jejunum of broiler chickens challenged with NE at d 26 (7 DPI). A TUNEL assay in jejunum sections after 7 days of NE infection in broiler chickens from (A) the NC group, (B) the NT group, (C) the PC group, and (D) the PT group. The blue color represents the live cells in the jejunal villus, and the brown color represents the apoptotic cells. The red arrow points out a typical apoptotic cell in the jejunal crypt and the yellow arrow points out a typical apoptotic cell in the jejunal villus. (E) Integral optical density (IOD) of TUNEL expression. Values are means (n = 6) with the SEM represented by vertical bars. Magnification = 400×.
Cecal microbiome
To characterize the phylogenetic composition of bacterial communities in the cecum, we first performed 16S rRNA gene sequencing analysis and compared the α-diversity and β-diversity of microbiota in the cecum of the different treatment groups. Our results revealed that the α-diversity of the cecal microbiota on d 26 (Table 1 and Fig. 7) was not (P > 0.05) influenced by NE infection or probiotic treatment. However, a principal component analysis (PCA) revealed (Fig. 8) a clear difference in microbial community composition among the different groups, indicating significant variability in their microbial profiles. Furthermore, we assessed the taxonomic profiles of the numerically abundant bacteria by analyzing the 16S rRNA gene sequences of the cecum (Fig. 9A and Supplemented Fig. 1). NE infection without E. faecium treatment resulted in a relative reduction in the proportion of the genus Lactobacillus compared with the non-infected and untreated group, while the group fed E. faecium but without NE infection showed the highest relative abundance (P < 0.05) of Lactobacillus and Butyricicoccus in the cecum compared to the negative control. Compared with the NE-infected group without probiotic treatment, the infected birds fed E. faecium did not differ in their relative abundance of the genera Butyricicoccus but Lactobacillus in the cecum (Fig. 9B).
Effect of dietary E. faecium 11181 on the cecal microbiota α-diversity indices (in cecal feces) of broiler chickens challenged with NE at d 26 (n = 6). (A) Chao diversity index. (B) Shannon diversity index. (C) Simpson diversity index. (D) PD whole tree diversity index. NC = Non-NE-infected + no E. faecium treatment, NT = non-NE-infected + E. faecium treatment, PC = NE-infected + no E. faecium treatment, PT = NE-infected + E. faecium treatment.
Effects of dietary E. faecium 11181 on cecal microbiota β-diversity (community similarity) of broilers challenged with NE at d 26 (n = 6). Principal component analysis (PCA) plot of samples in different treatment groups using the abundance information at the genus level. NC = Non-NE-infected + no E. faeciumtreatment, NT = non-NE-infected + E. faecium treatment, PC = NE-infected + no E. faecium treatment, PT = NE-infected + E. faecium treatment.
Effect of dietary E. faecium 11181 on the taxonomic composition of cecal microbiota in broiler chickens challenged with NE at d 26 (n = 6). (A) Relative abundance of the top 15 microorganisms at the genus level. (B) Different abundances at genus levels. NC = Non-NE-infected + no E. faecium treatment, NT = non-NE-infected + E. faecium treatment, PC = NE-infected + no E. faecium treatment, PT = NE-infected + E. faecium treatment.
Jejunal TLR signaling pathway immune-related cytokines- and growth factor-associated gene expression
As shown in Tables 2, 3, NE infection significantly upregulated the mRNA levels of the immune-related molecules TLR-2, IL-1β, IL-4, IL-10, IFN-γ, and iNOS and the growth factors TGF-β3 and IGF-2. Conversely, the NE challenge significantly downregulated mRNA expression of the TLR-signal-pathway negative regulator A20 in the jejunum compared with the expression levels in the non-infected groups. Compared with non-supplemented groups, inclusion of E. faecium to the diet remarkably increased gene expression levels of TLR2, MyD88, NF-κB, IL-4, iNOS, TGF-β3, PI3K, IGF-2, GLP-2, and EGFR; however, the ratio of IFN-γ to IL-4 decreased, and HSP70 protein level was increased as well. In addition, there was a significant interactive effect of NE infection and E. faecium treatment on MyD88, NF-κB, IL-1β, IL-4, iNOS, PI3K, GLP-2, HSP70 and HSP90 mRNA expression (P < 0.05); specifically, NE-infected birds fed with E. faecium displayed a notable increase in the mRNA levels of these genes.
Jejunal tight-junction gene and protein expression
Reverse transcription (RT)-PCR analysis (Table 3) revealed that NE infection sharply downregulated (P < 0.05) the expression levels of claudin-3 (CLDN-3) and zona occludens-1 (ZO-1) genes and upregulated (P < 0.05) the myosin light chain kinase (MLCK)-gene mRNA expression in the jejunum compared with the expression in non-infected birds. Compared with the non-supplemented groups, probiotic administration notably upregulated (P < 0.05) claudin-1 (CLDN-1) mRNA levels. In addition, a significant cooperative relationship was observed for CLDN-3 and occludin (OCLN) gene expression levels between E. faecium supplementation and NE infection. NE-induced increases in CLDN-3 and OCLN mRNA levels were alleviated by E. faecium supplementation. Western Blot (WB) results (Fig. 10) indicated that NE infection resulted in a significant increase in the relative levels of MLCK protein and a reduction in ZO-1 protein levels in the jejunum mucosa compared with the non-challenged groups but no significant difference was observed in the abundance of CLDN-1, CLDN-3, and OCLN protein between the infected and non-infected groups. However, birds fed E. faecium showed a significant upregulation in CLDN-1 protein levels. A cooperative effect between E. faecium supplementation and NE infection was noted for CLDN-3 protein expression (P < 0.05). The highest CLDN-3 protein levels were observed in the probiotic-treated, non-infected birds (P < 0.05), whereas no clear difference was observed in CLDN-3 protein levels among the other three treatment groups.
Effect of dietary E. faecium 11181 on tight-junction protein levels in the jejunum of broiler chickens challenged with NE at d 26. (A) MLCK and HSP70 (B) Claudin-1, Claudin-3, Occludin and ZO-1. Each result represents the mean value ± SEM (n = 6). The lowercase letters on the bars indicate significant differences (P < 0.05). NC = Non-NE-infected + no E. faecium treatment, NT = non-NE-infected + E. faecium treatment, PC = NE-infected + no E. faecium treatment, PT = NE-infected + E. faecium treatment.
Discussion
The subclinical form of C. perfringens associated-NE can adversely affect growth performance in poultry1,6. Poor growth performance is considered to be primarily caused by coccidia-induced leakage of proteins, including plasma, into the lumen of the small intestine; this condition provides nutrient substrates that facilitate the rapid replication of C. perfringens and concomitant damage to the digestive ability of the small intestine1. In accordance with previous studies pertaining to growth performance38,39, we observed that NE exerted a significant negative influence on BWG of broiler chickens. Conversely, E. faecium NCIMB 11181 addition to animal feed is effective in improving growth performance following NE infection. The positive effect of dietary E. faecium supplementation in relation to growth performance was also confirmed in other birds29,37,40 and pigs23,41.
Intestinal lesion scores, histopathological grades, bacterial translocation, and intestinal-cell proliferation and apoptosis indices are important indicators of intestinal health, recovery, and function. In this study, NE infection resulted in a significant increase in gut lesion scores, intestinal-cell apoptosis, bacterial load in the liver, and intestinal histopathological grades. These results, which are consistent with previous studies, indicated that NE can damage gut barrier structure, enhance gut permeability, and induce intestinal inflammation in broiler chickens6,38,39. Nevertheless, we showed that NE-induced gut injury and intestinal-cell apoptosis was attenuated and the NE-induced increase of C. perfringens in the liver was partially suppressed by E. faecium NCIMB 11181 supplementation. Similar effects of probiotics were also reported in previous studies on birds38,42. Thus, our findings suggest that pretreatment with probiotic E. faecium can protect intestinal epithelial barrier integrity from NE infection by reducing intestinal inflammation and inhibiting apoptosis of intestinal epithelial cells.
The intestinal barrier is regulated by tight-junction proteins (TJPs) that consist of several unique proteins including the junction adhesion molecule, the transmembrane protein occludin, members of the claudin family, and linker proteins such as the zonula occludin protein family43. This mechanical barrier plays an important role in the absorption of nutrients, electrolytes, and water, as well as the maintenance of intestinal-barrier integrity and function and the protection of the gut from enteric pathogen invasion44,45. Intestinal TJ barrier disruption not only increases membrane permeability to luminal antigens and bacterial translocation (leading to endogenous infection, sustained inflammation and tissue damage) but also reduces the absorption of nutrients7,45,46,47. In this study, NE infection significantly downregulated CLDN-3 and ZO-1 mRNA levels and ZO-1 protein content but upregulated MLCK mRNA expression and protein levels in the jejunum compared with the non-infected birds. Several studies in birds and humans have demonstrated that enterotoxin produced by C. perfringens disrupted the intestinal TJP complex, altered gut-barrier function, and led to intestinal epithelial cell apoptosis and death7,8. Additionally, the intestinal MLCK pathway is involved in both the degradation or distribution of TJs and intestinal permeability8,48. Thus, the occurrence of these phenomena suggests that NE infection disrupts multiple intestinal TJPs and compromises the structural integrity of the gut barrier, thereby leading to bacterial translocation into the liver due to the increased gut permeability. Pretreatment with E. faecium notably upregulated CLDN-1 mRNA levels and protein content in the jejunum mucosa of birds, regardless of NE infection. Furthermore, non-infected birds fed E. faecium showed higher CLDN-3 protein levels compared with the NE-infected birds. CLDN-1 is a member of the multiple-spanning, transmembrane, claudin protein family, which comprises of more than 20 members and has been shown to play an important role in barrier formation and paracellular selectivity in various tissues45. Thus, our results suggest that E. faecium addition protected intestinal barrier function against intestinal pathogens possibly via the upregulation of CLDN-1 protein levels. Enhanced tight junctions following E. faecium supplementation resulted in reduced gut permeability and reduced pathogen invasion. In accordance with our findings, several other studies have shown that probiotic E. faecium reinforced epithelial barrier function in pigs and mice with intestinal inflammation19,49,50 and prevented Enterotoxigenic E. coli (ETEC)-induced reductions in CLDN-1 mRNA and protein levels in pig cell models26,27,28.
TLR-mediated signaling pathways are involved in regulating intestinal epithelial barrier integrity51. Pro-inflammatory cytokines such as TNF-α, IFN-γ, and IL-1β have been reported to increase intestinal permeability and tissue damage via the dysregulation of TJPs52,53, while various regulatory peptides including anti-inflammatory cytokines (TGF-β, IL-4 and IL-10), growth factors (EGF, GLP-2 and IGF-2), negative regulators (A20, Tollip and PI3K) of the TLR signaling pathway, and HSPs have been demonstrated to protect intestinal barrier function by regulating tight junction expression and facilitating the repair of damaged gut tissue54,55,56,57. In order to elucidate the mechanism by which dietary probiotic E. faecium NCIMB 11181 supplementation affects intestinal barrier function and health, we further evaluated the changes in the intestinal mucosal toll-like receptors (TLR) and their downstream targets in NE-infected broiler chickens. We found that the NE challenge not only increased the mRNA expression of pro-inflammatory cytokines like TLR-2, IL-1β, IL-4, IFN-γ, and iNOS but also that of the anti-inflammatory cytokine IL-10 in the gut of the infected chickens; these results are similar to previous reports in broilers58,59. Moreover, our results revealed that NE infection upregulated the mRNA levels of the growth factors TGF-β3 and IGF-2 while reducing the levels of TLR-signaling-pathway negative regulator A20 in the jejunum compared with the non-infected groups. These results showed that NE infection differentially modulated intestinal immune-related gene expression, resulting in the activation of intestinal immune-inflammatory responses. Compared with non-supplemented groups, inclusion of E. faecium in the diet remarkably increased the gene expression levels of TLR-2, MyD88, NF-κB, iNOS, TGF-β3, PI3K, IGF-2, GLP-2, and EGFR. In accordance with our results, previous studies have demonstrated that E. faecium affected the expression of intestinal immune-related genes, growth factors, and HSPs in vivo40,60,61 and in vitro26,27,49,62. In addition, NE-infected birds fed with E. faecium displayed a notable increase in the relative gene expression of MyD88, NF-κB, IL-1β, IL-4, iNOS, PI3K, GLP-2, HSP70, and HSP90. Furthermore, our study also found that E. faecium NCIMB 11181 administration upregulated HSP70 protein expression in the jejunum irrespective of NE infection. Thus, our findings indicated that E. faecium administration not only supported effective intestinal innate immune-defense responses against pathogen infection by modulation of the TLR signaling pathway but also regulated intestinal immune balance and prevented excessive inflammation by differentially modulating pro-inflammatory and anti-inflammatory cytokines, growth factors, heat shock proteins, and TLR-signaling negative regulators when confronted with an NE challenge. Enhanced intestinal barrier function in NE-infected birds following E. faecium pretreatment might be attributable to the associated increase in the expression of TLR-2, IL-4, iNOS, GLP-2, HSP70, HSP90, and PI3K production in the intestinal tract. Improved intestinal barrier function in NE-infected birds given E. faecium pretreatment resulted in reduced bacterial translocation to the liver and less systemic inflammation. Taken together, these findings suggest that pretreatment with probiotic E. faecium NCIMB 11181 can effectively prevent intestinal inflammation triggered by NE infection, promote wound healing, and enhance intestinal epithelial barrier function. These results are consistent with previous in vivo studies in pigs and poultry19,31,32 and in vitro studies of E. faecium in enterobacterial disease26,27,28,62.
To further investigate the mechanism underlying E. faecium mitigating NE-induced gut injury, cecal microbiota structure was analyzed by Illumina MiSeq sequencing. In accordance with previous studies in chickens41,63, we observed no significant difference in α-diversity following 16S rRNA gene pyrosequencing of the cecal microbiota in NE-challenged birds with or without E. faecium supplementation, suggesting that neither probiotic treatment nor NE infection (alone or in combination) vastly modified the diversity of the intestinal microbiota. This finding could be due to inhibition of the proliferation of minor components of the microbiota by C. perfringens infection63 and inhibition of C. perfringens itself by E. faecium14,15,34,64. However, principal component analysis (PCA) showed that β-diversity of the cecal microbiota was, in fact, altered by E. faecium addition and NE challenge (both alone and together), indicating that these treatments significantly disturbed intestinal bacterial community profiles.
We also observed an increase in the relative abundance of the genera Lactobacillus and Butyricicoccus in the cecum of unchallenged-birds receiving E. faecium, suggesting that the inclusion of E. faecium in the diet of birds promoted the growth of potentially beneficial bacteria. This is in agreement with previous results29,41,65. Lactobacillus are responsible for higher levels of anti-inflammatory and systemic responses, and for out-competing and exclusively displacing pathogenic bacteria on the mucosal surfaces of the host66,67. Butyricicoccus spp. can degrade resistant starch or fiber to produce short-chain fatty acids (SCFA), especially butyric acid68. Recent evidence suggested that microbiota-derived butyrate was essential for the regulation of the immune response and the maintenance of intestinal epithelium integrity69,70. In addition, Butyricicoccus has been shown to play an important role in preventing NE infection in broilers2,71. Therefore, the evidence supports that pretreatment with E. faecium effectively prevents disturbances to the cecal microbiome induced by C. perfringens infection by enhancing the proliferation of beneficial bacteria and hindering the growth of potential pathogens. This results in a stable gut ecosystem with greater species richness, a phenomenon that possibly accounts for the significant improvement in growth performance and gut health of broilers. Beneficial intestinal microbiota shapes and promotes gut immunity homeostasis72. Furthermore, we speculate that E. faecium NCIMB 11181 improves gut barrier integrity by modulating the intestinal microbiome. Further fecal-metabolome analyses are required to explore the impact of probiotic E. faecium NCIMB 11181 on fecal metabolite profiles. These analyses would allow us to establish possible causal links between probiotic metabolites and gut function.
Conclusion
Pretreating poultry feed with probiotic E. faecium NCIMB 11181 confers a significant protective effect against NE-induced gut injury in broiler chickens, possibly by enhancing the expression of intestinal TJP CLDN-1 and HSP70, differentially modulating cytokine expression, and upregulating intestinal gene expression of the TLR negative-regulator PI3K and the growth factor GLP-2, and modulating the intestinal microflora structure. Further work is required to fully validate these specific mechanisms.
Materials and Methods
Animal ethics statement
All study procedures were approved by the Animal Care and Use Committee of China Agricultural University and were in accordance with the Guidelines for Experimental Animals established by the Ministry of Science and Technology (Beijing, China). All efforts were made to minimize the suffering of the animals.
Experimental design, birds, and diets
A 2 × 2 factorial arrangement was employed in a completely randomized design to investigate the effects of two levels of E. faecium supplementation (0 or 2 × 108 CFU/kg of feed, the dosage of E. faecium was based on the recommendation of its producer and our previous study) and two levels of NE (NE-challenged or unchallenged) on broiler chickens. One-day-old, male AA broiler chicks (n = 180) with similar body weights were obtained from a commercial hatchery (Beijing Arbor Acres Poultry Breeding Company). All the birds were weighed and randomly assigned to one of the four experimental groups. Each group had three replicate pens with 15 birds per pen. The treatment groups were as follows: (i) negative control group (birds without NE infection and feed without E. faecium, NC), (ii) E. faecium-treated group (birds without NE infection, but feed supplemented with E. faecium, NT), (iii) NE-infected control group (birds infected with NE, but feed without E. faecium, PC), and (iv) the probiotic-treated and NE-infected group (birds infected with NE, and feed supplemented with E. faecium, PT). Subclinical NE was induced in broiler birds as previously described38. The NE-challenged birds were restricted to isolated compartments of the pen to avoid cross-infection. An antibiotic-free, commercial, basic diet was prepared according to the National Research Council (NRC, 1994) requirements for starter (d 1–21) and grower (d 22–42) periods. The composition of the basal feed and associated nutrient levels are presented in Table 4. The probiotic-treated feed included 200 mg E. faecium per kg of feed (NCIMB11181, viable count ≥1 × 109 CFU/g, obtained from Probiotics International Ltd. Co., UK). The purchased E. faecium microcapsules are obtained by a sequence of liquid fermentation, filtration, micro-encapsulation, and quick freezing. To ensure the homogeneity of the additives, approximately 5 kg of the basal feed was thoroughly mixed with the additive in a plastic bucket. To ensure that the probiotic dosages were performed correctly, samples of the E. faecium-treated feed were taken, serial dilutions were made, cultures were grown in sodium azide-crystal violet-esculin agar (CM 1507, Beijing Land Bridge Technology Co., LTD) at 37°C for 24 h under an anaerobic environment, and the number of E. faecium bacteria was counted using the spread-plate counting method. The chicks were reared on net-floor cages in a closed and ventilated enclosure. Each pen had a floor space of 11,200 (160 × 70) cm2 and was equipped with a separate feeding trough and nipple drinkers. In accordance with the AA Broiler Management Guide, all the birds received continuous light for the first 24 h and were then maintained under a 23-h light/1-h dark cycle for the remainder of the study. The temperature in the pen was maintained at 33–34 °C for the first three days and then gradually decreased by 2 °C per week until a final temperature of 22–24 °C was achieved. The relative humidity was kept at 60–70% in the first week and at 50–60% thereafter. All the birds were allowed ad libitum access to feed and water throughout the study.
Growth performance
All broilers were individually weighed, and body weight (BW) and average body weight gain (ABWG) were measured at different experimental periods (at d 13–21, d 22–26, d 27–35, and d 21–26). The death rate was calculated during two periods: d 1–12 and d 13–35.
Intestinal NE lesion scoring and sample collection
On 3, 7 and 14 d post-C. perfringens infection (at 21, 26 and 35 days of age), two bird was randomly selected from each replicate pen, weighed, and euthanized by cervical dislocation. The jejunum was collected and scored for NE gut lesions on a scale of 0 (none) to 4 (high) by three independent observers who were blinded to the experimental design, as previously described73. On 7 DPI, 1-cm-long samples of the jejunum (between Meckel’s diverticulum and the proximal end of the jejunum), were snap-frozen in liquid nitrogen and stored at −80 °C for subsequent mRNA and protein analysis. In addition, ~2-cm-long samples of the jejunum were washed with PBS and then fixed in 4% paraformaldehyde solution for subsequent histopathological observation and immune-histochemical examination. Approximately 3 g of the digesta from the cecum were collected in sterile tubes and immediately frozen at -80 °C for microbial DNA analysis. Liver tissue was aseptically collected and frozen immediately at -40 °C for bacterial translocation (BT) analysis.
Histological and histopathological examination
The fixed jejunum-tissue samples were dehydrated in a tissue processor (Leica Microsystems K. K., Tokyo, Japan) and embedded in paraffin wax as previously described38. The embedded tissue was cut into 5-μm sections using a microtome (Leica Microsystems K. K.) and mounted on polylysine-coated glass slides (Boster Corporation, China). Hematoxylin-Eosin (HE) staining was performed using a routine protocol for histological and histopathological analyses. Histopathological examinations were conducted by light microscopy and findings were imaged and analyzed using a pathological image analysis system (Leica Qwin, Jiangsu, China) with a digital camera (DP72; Olympus). The pathological grade of the jejunum was evaluated by summing the evaluated scores of three factors:
(i) Inflammation (score 0–3): 0 = no inflammatory-cell infiltration; 1 = slight inflammatory-cell infiltration; 2 = moderate inflammatory-cell infiltration; 3 = severe inflammatory-cell infiltration. (ii) Extent of lesions (score 0–3): 0 = No lesion; 1 = Lesion in the mucosal layer; 2 = Lesion in the mucosal layer and submucosa; 3 = Transparent cell wall. (iii) Crypt Damage (score 0–4): 0 = No lesion in crypt; 1 = 1/3 crypt lesion; 2 = 2/3 crypt lesion; 3 = only the epithelial surface was intact; 4 = Crypt and epithelium not visible.
Proliferating cell nuclear antigen (PCNA) immunohistochemistry analysis
The immunostaining of jejunum-tissue sections was performed following the same procedure as described in previous studies74. Briefly, the tissue sections were deparaffinized twice with xylene for 10 min and rehydrated in a graded concentration series of ethanol. A microwave oven (MYA-2270M, Haier, Qindao, China) was used for heat-induced antigen retrieval in citrate buffer solution (pH 6.0) for 20 min (5 min at high power [700 W] and 15 min at low power [116 W]). After cooling the tissue to room temperature for 2–3 h, 3% H2O2 was used to block endogenous peroxidases. To facilitate blocking of non-specific antibody binding, the tissue sections were incubated with 5% (V/V) bovine serum albumin (BSA) in PBST (PBS, pH = 7.4, 0.1%V/V Tween 20) at 37 °C for 30 min. The tissue sections were then incubated with the mouse anti-PCNA primary antibody (1:500 dilution) (GB11010, Wuhan Servicebio technology Co. Ltd., China) overnight at 4 °C and subsequently incubated at 37 °C for 50 min with the appropriate horseradish peroxidase (HRP)-conjugated secondary antibody (Wuhan Servicebio Technology Co. Ltd., China). All the sections were also immunostained with the chromogenic marker diaminobenzidine (DAB, G1211, Wuhan Servicebio Technology Co. Ltd., China) and counterstained with hematoxylin. Finally, the sections were washed, dried, dehydrated, cleared, and mounted with a coverslip. Serial sections were examined under a light microscope (BH-2; Olympus, Japan) with a digital camera (DP72; Olympus), and fields of view showing different regions of the jejunum tissue were selected and captured in each section. Proliferating cells (brown-yellow, PCNA-positive) were measured in high-power fields selected at random (400 × magnification, 50 × 50 μm) with a computerized image-analysis system (MultiScanBase v. 14.02, Computer Scanning System, Warsaw, Poland). Accumulated integral optical density (IOD) for positive staining in each image was analyzed using the Image-Pro Plus 6.0 software (Media Cybernetics, Inc., MD, USA).
Terminal deoxynucleotidyl transferase dUTP nick end labeling (TUNEL) assay
The TUNEL assay was carried out according to the manufacturer’s instructions for the Apoptosis Detection Kit (11684817910, Roche, USA). Briefly, the paraffin sections of jejunum tissue were dewaxed with 100% xylene and rehydrated in a graded series of ethanol. Next, the activity of endogenous peroxidases was quenched in 3% H2O2 with distilled water at 37 °C for 10 min, and the sections were incubated with proteinase K (diluted 1:200 in Tris-buffered saline [TBS]) at 37 °C for 5–10 min in a humid chamber. A labeling mixture including digoxin-dUTP in terminal deoxynucleotidyl transferase (TdT) enzyme buffer was added to the sections and incubated at 37 °C for 2 h. After three continuous washes with TBS for 2 min, the sections were incubated with anti-digoxin-biotin conjugate diluted at 1:100 in blocking reagent for 30 min at 37 °C. The tissue sections were subsequently incubated for 1 h at 37 °C with streptavidin-biotin complex (SABC) diluted at 1:100 in TBS. Labeling was visualized with DAB and the sections were counterstained with hematoxylin. The negative control was performed in an identical manner, except that the TdT enzyme buffer was omitted from the incubation. The IOD of TUNEL-positive cells in the jejunum was assessed by a digital microscope and camera system (Nikon DS-Ri1, Japan). For each section, five fields (400 × magnification, 50 × 50 μm) from each area of the image were analyzed using Image-Pro Plus 6.0 (USA) image analysis software. By selecting ‘color-chosen target’ in the options bar of the morphologic analysis system, all TUNEL-positive cells in the field were marked in color. Finally, the ‘calculating’ option was selected in the options bar to automatically calculate the number of cells and the IOD values.
Intestinal permeability analysis via bacterial-translocation measurements
The number of C. perfringens cells in the liver was analyzed using the plate-pouring method as previously described38. Bacterial translocation was expressed in colony forming units (log10 CFU/gram of tissue).
DNA extraction and pyrosequencing
Total genomic DNA from cecal samples was extracted using the QIAamp Fast Stool Mini Kit (Qiagen, Hilden, Germany) according to the manufacturer’s instructions. DNA integrity was assessed by agarose gel electrophoresis, and then the genomic DNA was used as a template for PCR amplification. The bacterial 16S rRNA V3–V4 gene region was amplified using the KAPA HiFi Hotstart ReadyMix PCR kit (Kapa Biosystems, USA) and primers F341 and R806 (F341: ACTCCTACGGGRSGCAGCAG, R806: GGACTACVVGGGTATCTAATC). PCR amplification was carried out in a 25-µL reaction system and the amplification conditions were as follows: initial pre-denaturation at 98°C for 3 min; 30 cycles of denaturation at 95°C for 100 s, renaturation at 50°C for 60 s, and elongation at 72°C for 2 min; and a final elongation step at 72°C for 10 min. The amplification product was assessed by agarose gel electrophoresis (5 µl PCR product, 1.5% agarose gel) at 100 V for 60 min to facilitate size verification. The associated product was subsequently purified using an AxyPrepTM DNA Gel Extraction kit (AXYGEN, USA). Finally, 16S rRNA gene sequencing was performed using the Illumina HiSeq PE250 sequencing platform (Illumina, Santa Clara, CA) at the Realbio Technology Co., Ltd. (Shanghai, China) according to the manufacturer’s instructions.
The raw sequence data obtained from the Illumina HiSeq platform were quality-filtered and demultiplexed using the Quantitative Insights into Microbial Ecology (QIIME) version 1.8.0-dev. First, the sequences were trimmed to eliminate all low-quality sequence reads; sequence reads (of 400–440 nt) with an average quality score of at least 25 were retained by SOAPaligner (v 2.21). USEARCH version 7.1 software was used for the trimmed sequence read clusters and cutoffs (based on 97% similar identity) for operational taxonomic units (OUT), and chimeric sequences were identified and removed using UCHIME. α-diversity measures, including the number and evenness of species, the observed OTUs/reads, Good’s coverage, Shannon index, Simpson index and Chao 1 were investigated by MOTHUR v.1.35.0, and the significance of these estimates was determined using a Mann-Whitney U test. In addition, jack-knifed β-diversity was calculated from unweighted and weighted UniFrac distances, and a principal component analysis (PCA) was performed in QIIME. A Kruskal-Wallis test was used to determine the significance of the differences between groups. In addition, MetaStat was used to identify the bacterial taxa differentially represented between groups at genus or higher taxonomy levels.
Real-time polymerase chain reaction (PCR)
Total RNA was isolated from snap-frozen jejunum tissue samples using the RNAiso Plus Kit (TaKaRa, Dalian, China) according to the manufacturer’s instructions. The quality and quantity of the total RNA were measured with a spectrophotometer (NanoDrop-2000, Thermo Fisher Scientific, Waltham, MA) using the 260:280 nm absorbance ratio. First-strand cDNA was synthesized using a PrimeScriptTM RT reagent Kit with gDNA Eraser (Perfect Real Time; Takara Biotechnology Co. Ltd., Dalian, China) according to the manufacturer’s instructions. The cDNA was used to perform quantitative real-time PCR (Applied Biosystems 7500 Fast Real-Time PCR System, USA) for target-gene expression according to the standard protocol38. Primer sequences (Table 5) for chicken TLR signal pathway-related genes (TLR2, MyD88, NF-κB, IL-1β, IL-4, IL-8, IL-10, IFN-γ, TNF-α, iNOS, Tollip, A20, PI3K), MLCK, tight-junction protein genes (CLDN-1, CLDN-3, OCLN, ZO-1), growth-factor genes (TGF-β2, TGF-β3, IGF-2, GLP-2, EGFR), heat-shock-protein genes (HSP60, HSP70 and HSP90), and the household gene GAPDH were designed and synthesized by Sango Biotech Co., Ltd (Shanghai, China). The result were showed as 2−△△CT.
Western blot
Frozen jejunal mucosa was homogenized and lysed in ice-cold lysis buffer containing 50 mmol/L Tris-HCl (pH 7.4), 150 mmol/L NaCl, 1% Nonidet P (NP)−40, 0.1% sodium dodecyl sulfate (SDS), 1.0 mmol/L phenylmethylsulfonyl fluoride (PMSF), 1.0 mmol/L sodium orthovanadate (Na3VO4), 1.0 mmol/L sodium fluoride (NaF), and a protease and phosphatase inhibitor cocktail (P1045, Beyotime Biotechnology, Co., Ltd., Beijing). The resultant cell lysate was centrifuged at 12,000 × g for 15 min at 4 °C to remove cellular debris. Protein concentrations were determined using a Pierce™ bicinchoninic acid (BCA) protein assay kit (CW0014, CWBIO Ltd., Beijing). Equal amounts of protein (30 μg) were separated on 8%, 10%, or 12% SDS-polyacrylamide gels (Tris-glycine-SDS-polyacrylamide gel electrophoresis), and transferred to a methanol-presoaked polyvinylidene difluoride (PVDF) membrane (IPVH000101, Millipore, USA). The membranes were inoculated with 5% skimmed-milk solution in TBS containing 0.05% Tween-20 (TBST blocking solution) at 37 °C for 1 h and were then incubated with primary antibodies overnight at 4 °C. The primary antibodies were anti-MLCK (M7905, Sigma-Aldrich, USA), anti-ZO-1 (61–7300, Invitrogen Corporation, Camarillo, USA), polyclonal rabbit anti-chicken CLDN-1, CLDN-3, and OCLN (antibodies against recombinant chicken CLDN-1, CLDN-3, and OCLN proteins were prepared in our laboratory and patents are currently being authorized). The blots were stripped and incubated with anti-β-actin antibody (A1978, Sigma-Aldrich, USA) to demonstrate equal loading. After incubation at room temperature for 3 h with HRP-conjugated goat anti-rabbit IgG (A0208) or goat anti-mouse IgG antibodies (A0216, Beyotime Biotechnology, Co., Ltd., Beijing), the chemiluminescence signal was detected using the ECL-Plus chemiluminescent kit (Hua Xing Bo Chuang Biotechnology Center, Beijing) and a luminescence imager (Tanon 5200, Tanon Science & Technology Co., Ltd., Shanghai). Quantification of band density was conducted using Image J software.
Statistical analysis
For the normally distributed data (growth performance, gut lesion scores, liver C. perfringens, intestinal histopathological scores, intestinal PCNA-positive and TUNEL-positive cell numbers, relative mRNA expression, protein expression), the main effect and interaction effects were analyzed using the general linear model (GLM) procedure in SPSS 22.0 (SPSS Inc, Chicago, Illinois, USA). The results were expressed as treatment means with their pooled SEM. The one-way ANOVA and multiple comparisons were performed when interactive effects differed significantly. α-diversity and β-diversity were analyzed using the Mann-Whitney U test. The relative abundance of microorganisms obtained from 16S rRNA sequencing was analyzed using the Kruskal-Wallis test to compare the difference between two groups or all four treatments. P < 0.05 was considered significant.
References
Van Immerseel, F. et al. Clostridium perfringens in poultry: an emerging threat for animal and public health. Avian pathology: journal of the W.V.P.A 33, 537–549, https://doi.org/10.1080/03079450400013162 (2004).
Antonissen, G. et al. Microbial shifts associated with necrotic enteritis. Avian pathology: journal of the W.V.P.A 45, 308–312, https://doi.org/10.1080/03079457.2016.1152625 (2016).
Fasina, Y. O., Newman, M. M., Stough, J. M. & Liles, M. R. Effect of Clostridium perfringens infection and antibiotic administration on microbiota in the small intestine of broiler chickens. Poultry science 95, 247–260, https://doi.org/10.3382/ps/pev329 (2016).
Xu, S. et al. Bacillus licheniformis normalize the ileum microbiota of chickens infected with necrotic enteritis. Scientific reports 8, 1744, https://doi.org/10.1038/s41598-018-20059-z (2018).
Zahoor, I., Ghayas, A. & Basheer, A. Genetics and genomics of susceptibility and immune response to necrotic enteritis in chicken: a review. Molecular biology reports 45, 31–37, https://doi.org/10.1007/s11033-017-4138-8 (2018).
Timbermont, L., Haesebrouck, F., Ducatelle, R. & Van Immerseel, F. Necrotic enteritis in broilers: an updated review on the pathogenesis. Avian pathology: journal of the W.V.P.A 40, 341–347, https://doi.org/10.1080/03079457.2011.590967 (2011).
Awad, W. A., Hess, C. & Hess, M. Enteric Pathogens and Their Toxin-Induced Disruption of the Intestinal Barrier through Alteration of Tight Junctions in Chickens. Toxins 9, https://doi.org/10.3390/toxins9020060 (2017).
Lu, R. Y., Yang, W. X. & Hu, Y. J. The role of epithelial tight junctions involved in pathogen infections. Molecular biology reports 41, 6591–6610, https://doi.org/10.1007/s11033-014-3543-5 (2014).
Boirivant, M. & Strober, W. The mechanism of action of probiotics. Current opinion in gastroenterology 23, 679–692, https://doi.org/10.1097/MOG.0b013e3282f0cffc (2007).
Cisek, A. A. & Binek, M. Chicken intestinal microbiota function with a special emphasis on the role of probiotic bacteria. Polish journal of veterinary sciences 17, 385–394 (2014).
van Baarlen, P., Wells, J. M. & Kleerebezem, M. Regulation of intestinal homeostasis and immunity with probiotic lactobacilli. Trends in immunology 34, 208–215, https://doi.org/10.1016/j.it.2013.01.005 (2013).
Barbosa, J., Borges, S. & Teixeira, P. Selection of potential probiotic Enterococcus faecium isolated from Portuguese fermented food. International journal of food microbiology 191, 144–148, https://doi.org/10.1016/j.ijfoodmicro.2014.09.009 (2014).
Karimaei, S. et al. Antibacterial potential and genetic profile of Enterococcus faecium strains isolated from human normal flora. Microbial pathogenesis 96, 67–71, https://doi.org/10.1016/j.micpath.2016.05.004 (2016).
Franz, C. M., van Belkum, M. J., Holzapfel, W. H., Abriouel, H. & Galvez, A. Diversity of enterococcal bacteriocins and their grouping in a new classification scheme. FEMS microbiology reviews 31, 293–310, https://doi.org/10.1111/j.1574-6976.2007.00064.x (2007).
Klose, V., Bayer, K., Bruckbeck, R., Schatzmayr, G. & Loibner, A. P. In vitro antagonistic activities of animal intestinal strains against swine-associated pathogens. Veterinary microbiology 144, 515–521, https://doi.org/10.1016/j.vetmic.2010.02.025 (2010).
EFSA. Guidance on the safety assessment of Enterococcus faecium in animal nutrition The EFSA Journal 10, 2682 (2010).
Bednorz, C. et al. Feeding the Probiotic Enterococcus faecium Strain NCIMB 10415 to Piglets Specifically Reduces the Number of Escherichia coli Pathotypes That Adhere to the Gut Mucosa. Appl Environ Microb 79, 7896–7904, https://doi.org/10.1128/Aem.03138-13 (2013).
Taras, D., Vahjen, W., Macha, M. & Simon, O. Performance, diarrhea incidence, and occurrence of Escherichia coli virulence genes during long-term administration of a probiotic Enterococcus faecium strain to sows and piglets. Journal of animal science 84, 608–617 (2006).
Lodemann, U. et al. Effects of Ex Vivo Infection with ETEC on Jejunal Barrier Properties and Cytokine Expression in Probiotic-Supplemented Pigs. Digestive diseases and sciences 62, 922–933, https://doi.org/10.1007/s10620-016-4413-x (2017).
Pollmann, M., Nordhoff, M., Pospischil, A., Tedin, K. & Wieler, L. H. Effects of a probiotic strain of Enterococcus faecium on the rate of natural chlamydia infection in swine. Infection and immunity 73, 4346–4353, https://doi.org/10.1128/IAI.73.7.4346-4353.2005 (2005).
Benyacoub, J. et al. Enterococcus faecium SF68 enhances the immune response to Giardia intestinalis in mice. The Journal of nutrition 135, 1171–1176, https://doi.org/10.1093/jn/135.5.1171 (2005).
Kreuzer, S. et al. Feeding of the probiotic bacterium Enterococcus faecium NCIMB 10415 differentially affects shedding of enteric viruses in pigs. Veterinary research 43, 58, https://doi.org/10.1186/1297-9716-43-58 (2012).
Zeyner, A. & Boldt, E. Effects of a probiotic Enterococcus faecium strain supplemented from birth to weaning on diarrhoea patterns and performance of piglets. Journal of animal physiology and animal nutrition 90, 25–31, https://doi.org/10.1111/j.1439-0396.2005.00615.x (2006).
Scharek, L. et al. Influence of a probiotic Enterococcus faecium strain on development of the immune system of sows and piglets. Veterinary immunology and immunopathology 105, 151–161, https://doi.org/10.1016/j.vetimm.2004.12.022 (2005).
Starke, I. C., Pieper, R., Neumann, K., Zentek, J. & Vahjen, W. Individual responses of mother sows to a probiotic Enterococcus faecium strain lead to different microbiota composition in their offspring. Beneficial microbes 4, 345–356, https://doi.org/10.3920/BM2013.0021 (2013).
Klingspor, S. et al. Enterococcus faecium NCIMB 10415 modulates epithelial integrity, heat shock protein, and proinflammatory cytokine response in intestinal cells. Mediators of inflammation 2015, 304149, https://doi.org/10.1155/2015/304149 (2015).
Kern, M. et al. Altered Cytokine Expression and Barrier Properties after In Vitro Infection of Porcine Epithelial Cells with Enterotoxigenic Escherichia coli and Probiotic Enterococcus faecium. Mediators of inflammation 2017, 2748192, https://doi.org/10.1155/2017/2748192 (2017).
Tian, Z. et al. Enterococcus faecium HDRsEf1 Protects the Intestinal Epithelium and Attenuates ETEC-Induced IL-8 Secretion in Enterocytes. Mediators of inflammation 2016, 7474306, https://doi.org/10.1155/2016/7474306 (2016).
Samli, H. E., Senkoylu, N., Koc, F., Kanter, M. & Agma, A. Effects of Enterococcus faecium and dried whey on broiler performance, gut histomorphology and intestinal microbiota. Archives of animal nutrition 61, 42–49, https://doi.org/10.1080/17450390601106655 (2007).
Luo, J. et al. Proteome changes in the intestinal mucosa of broiler (Gallus gallus) activated by probiotic Enterococcus faecium. J Proteomics 91, 226–241, https://doi.org/10.1016/j.jprot.2013.07.017 (2013).
Karaffova, V. et al. Interaction of TGF-beta4 and IL-17 with IgA secretion in the intestine of chickens fed with E. faecium AL41 and challenged with S. Enteritidis. Research in veterinary science 100, 75–79, https://doi.org/10.1016/j.rvsc.2015.04.005 (2015).
Karaffova, V. et al. TLR4 and TLR21 expression, MIF, IFN-beta, MD-2, CD14 activation, and sIgA production in chickens administered with EFAL41 strain challenged with Campylobacter jejuni. Folia Microbiol 62, 89–97, https://doi.org/10.1007/s12223-016-0475-6 (2017).
Caly, D. L., D’Inca, R., Auclair, E. & Drider, D. Alternatives to Antibiotics to Prevent Necrotic Enteritis in Broiler Chickens: A Microbiologist’s Perspective. Frontiers in microbiology 6, 1336, https://doi.org/10.3389/fmicb.2015.01336 (2015).
Cao, G. T. et al. Effects of a probiotic, Enterococcus faecium, on growth performance, intestinal morphology, immune response, and cecal microflora in broiler chickens challenged with Escherichia coli K88. Poultry science 92, 2949–2955, https://doi.org/10.3382/ps.2013-03366 (2013).
Pajarillo, E. A. B. et al. Effects of probiotic Enterococcus faecium NCIMB 11181 administration on swine fecal microbiota diversity and composition using barcoded pyrosequencing. Anim Feed Sci Tech 201, 80–88 (2015).
Vrotniakien˙e, V., Jatkauskas,J. Effects of probiotics dietary supplementation on diarrhea incidence,fecal shedding of Escherichia coli and growth performance in post-weaned piglets. Vet.Med.Zoot. 63 (2013).
Wu, Y., Zhen, W., Geng, Y., Wang, Z. & Guo, Y. Effects of dietary Enterococcus faecium NCIMB 11181 supplementation on growth performance and cellular and humoral immune responses in broiler chickens. Poultry science, https://doi.org/10.3382/ps/pey368 (2018).
Wu, Y. et al. Effects of Bacillus coagulans supplementation on the growth performance and gut health of broiler chickens with Clostridium perfringens-induced necrotic enteritis. J Anim Sci Biotechnol 9, 9, https://doi.org/10.1186/s40104-017-0220-2 (2018).
Song, B. C. et al. Effect of microencapsulated sodium butyrate dietary supplementation on growth performance and intestinal barrier function of broiler chickens infected with necrotic enteritis. Anim Feed Sci Tech 232, 6–15, https://doi.org/10.1016/j.anifeedsci.2017.07.009 (2017).
Huang, L., Luo, L., Zhang, Y., Wang, Z. & Xia, Z. Effects of the Dietary Probiotic, Enterococcus faecium NCIMB11181, on the Intestinal Barrier and System Immune Status in Escherichia coli O78-Challenged Broiler Chickens. Probiotics and antimicrobial proteins, https://doi.org/10.1007/s12602-018-9434-7 (2018).
Wang, Y. B. et al. Intestinal microbiota and oral administration of Enterococcus faecium associated with the growth performance of new-born piglets. Beneficial microbes 7, 529–538, https://doi.org/10.3920/BM2015.0099 (2016).
Nagpal, R. & Yadav, H. Bacterial Translocation from the Gut to the Distant Organs: An Overview. Annals of nutrition & metabolism 71(Suppl 1), 11–16, https://doi.org/10.1159/000479918 (2017).
Peterson, L. W. & Artis, D. Intestinal epithelial cells: regulators of barrier function and immune homeostasis. Nature reviews. Immunology 14, 141–153, https://doi.org/10.1038/nri3608 (2014).
Schneeberger, E. E. & Lynch, R. D. The tight junction: a multifunctional complex. American journal of physiology. Cell physiology 286, C1213–1228, https://doi.org/10.1152/ajpcell.00558.2003 (2004).
Suzuki, T. Regulation of intestinal epithelial permeability by tight junctions. Cell Mol Life Sci 70, 631–659, https://doi.org/10.1007/s00018-012-1070-x (2013).
Berkes, J., Viswanathan, V. K., Savkovic, S. D. & Hecht, G. Intestinal epithelial responses to enteric pathogens: effects on the tight junction barrier, ion transport, and inflammation. Gut 52, 439–451 (2003).
Turner, J. R. Intestinal mucosal barrier function in health and disease. Nature reviews. Immunology 9, 799–809, https://doi.org/10.1038/nri2653 (2009).
Chelakkot, C., Ghim, J. & Ryu, S. H. Mechanisms regulating intestinal barrier integrity and its pathological implications. Experimental & molecular medicine 50, 103, https://doi.org/10.1038/s12276-018-0126-x (2018).
Lodemann, U., Dillenseger, A., Aschenbach, J. R. & Martens, H. Effects of age and controlled oral dosing of Enterococcus faecium on epithelial properties in the piglet small intestine. Beneficial microbes 4, 335–344, https://doi.org/10.3920/BM2013.0004 (2013).
Yan, T. et al. Enterococcus faecium HDRsEf1 elevates the intestinal barrier defense against enterotoxigenic Escherichia coli and regulates occludin expression via activation of TLR-2 and PI3K signalling pathways. Letters in applied microbiology 67, 520–527, https://doi.org/10.1111/lam.13067 (2018).
Nighot, M. et al. Lipopolysaccharide-Induced Increase in Intestinal Epithelial Tight Permeability Is Mediated by Toll-Like Receptor 4/Myeloid Differentiation Primary Response 88 (MyD88) Activation of Myosin Light Chain Kinase Expression. The American journal of pathology 187, 2698–2710, https://doi.org/10.1016/j.ajpath.2017.08.005 (2017).
Edelblum, K. L. & Turner, J. R. The tight junction in inflammatory disease: communication breakdown. Current opinion in pharmacology 9, 715–720, https://doi.org/10.1016/j.coph.2009.06.022 (2009).
Capaldo, C. T. & Nusrat, A. Cytokine regulation of tight junctions. Biochimica et biophysica acta 1788, 864–871, https://doi.org/10.1016/j.bbamem.2008.08.027 (2009).
Lee, S. H. Intestinal permeability regulation by tight junction: implication on inflammatory bowel diseases. Intestinal research 13, 11–18, https://doi.org/10.5217/ir.2015.13.1.11 (2015).
van Eden, W. Diet and the anti-inflammatory effect of heat shock proteins. Endocrine, metabolic & immune disorders drug targets 15, 31–36 (2015).
Kondo, T., Kawai, T. & Akira, S. Dissecting negative regulation of Toll-like receptor signaling. Trends in immunology 33, 449–458, https://doi.org/10.1016/j.it.2012.05.002 (2012).
Catrysse, L., Vereecke, L., Beyaert, R. & van Loo, G. A20 in inflammation and autoimmunity. Trends in immunology 35, 22–31, https://doi.org/10.1016/j.it.2013.10.005 (2014).
Oh, S. T. & Lillehoj, H. S. The role of host genetic factors and host immunity in necrotic enteritis. Avian pathology: journal of the W.V.P.A 45, 313–316, https://doi.org/10.1080/03079457.2016.1154503 (2016).
Park, S. S. et al. Immunopathology and cytokine responses in broiler chickens coinfected with Eimeria maxima and Clostridium perfringens with the use of an animal model of necrotic enteritis. Avian Dis 52, 14–22, https://doi.org/10.1637/7997-041707-Reg (2008).
Lodemann, U., Hubener, K., Jansen, N. & Martens, H. Effects of Enterococcus faecium NCIMB 10415 as probiotic supplement on intestinal transport and barrier function of piglets. Archives of animal nutrition 60, 35–48, https://doi.org/10.1080/17450390500468099 (2006).
Tarasova, E. et al. The influence of probiotic Enterococcus faecium strain L5 on the microbiota and cytokines expression in rats with dysbiosis induced by antibiotics. Beneficial microbes 1, 265–270, https://doi.org/10.3920/BM2010.0008 (2010).
Loss, H., Aschenbach, J. R., Ebner, F., Tedin, K. & Lodemann, U. Effects of a pathogenic ETEC strain and a probiotic Enterococcus faecium strain on the inflammasome response in porcine dendritic cells. Veterinary immunology and immunopathology 203, 78–87, https://doi.org/10.1016/j.vetimm.2018.08.004 (2018).
Lin, Y. et al. Disruption in the cecal microbiota of chickens challenged with Clostridium perfringens and other factors was alleviated by Bacillus licheniformis supplementation. PloS one 12, e0182426, https://doi.org/10.1371/journal.pone.0182426 (2017).
Shin, M. S., Han, S. K., Ji, A. R., Kim, K. S. & Lee, W. K. Isolation and characterization of bacteriocin-producing bacteria from the gastrointestinal tract of broiler chickens for probiotic use. Journal of applied microbiology 105, 2203–2212, https://doi.org/10.1111/j.1365-2672.2008.03935.x (2008).
Beirao, B. C. B. et al. Effect of an Enterococcus faecium probiotic on specific IgA following live Salmonella Enteritidis vaccination of layer chickens. Avian pathology: journal of the W.V.P.A 47, 325–333, https://doi.org/10.1080/03079457.2018.1450487 (2018).
Peng, Q. et al. Effects of dietary Lactobacillus plantarum B1 on growth performance, intestinal microbiota, and short chain fatty acid profiles in broiler chickens. Poultry science 95, 893–900, https://doi.org/10.3382/ps/pev435 (2016).
Tsai, Y. T., Cheng, P. C. & Pan, T. M. The immunomodulatory effects of lactic acid bacteria for improving immune functions and benefits. Applied microbiology and biotechnology 96, 853–862, https://doi.org/10.1007/s00253-012-4407-3 (2012).
Moens, F. & De Vuyst, L. Inulin-type fructan degradation capacity of Clostridium cluster IV and XIVa butyrate-producing colon bacteria and their associated metabolic outcomes. Beneficial microbes 8, 473–490, https://doi.org/10.3920/BM2016.0142 (2017).
Singh, N. et al. Activation of Gpr109a, receptor for niacin and the commensal metabolite butyrate, suppresses colonic inflammation and carcinogenesis. Immunity 40, 128–139, https://doi.org/10.1016/j.immuni.2013.12.007 (2014).
Kelly, C. J. et al. Crosstalk between Microbiota-Derived Short-Chain Fatty Acids and Intestinal Epithelial HIF Augments Tissue Barrier Function. Cell host & microbe 17, 662–671, https://doi.org/10.1016/j.chom.2015.03.005 (2015).
Eeckhaut, V. et al. The Probiotic Butyricicoccus pullicaecorum Reduces Feed Conversion and Protects from Potentially Harmful Intestinal Microorganisms and Necrotic Enteritis in Broilers. Frontiers in microbiology 7, 1416, https://doi.org/10.3389/fmicb.2016.01416 (2016).
Round, J. L. & Mazmanian, S. K. The gut microbiota shapes intestinal immune responses during health and disease. Nature reviews. Immunology 9, 313–323, https://doi.org/10.1038/nri2515 (2009).
Gholamiandehkordi, A. R. et al. Quantification of gut lesions in a subclinical necrotic enteritis model. Avian pathology: journal of the W.V.P.A 36, 375–382, https://doi.org/10.1080/03079450701589118 (2007).
He, X. et al. Chronic Heat Stress Damages Small Intestinal Epithelium Cells Associated with the Adenosine 5’-Monophosphate-Activated Protein Kinase Pathway in Broilers. Journal of agricultural and food chemistry 66, 7301–7309, https://doi.org/10.1021/acs.jafc.8b02145 (2018).
Acknowledgements
This research was funded by the National Key Research and Development Plan (No. 2107YFD0500506) and the National Special Fund for Agro-scientific Research in the Public Interest (20140304-07). Funders had no role in the study design, analysis, or writing of this article.
Author information
Authors and Affiliations
Contributions
Zhong Wang and Yuanyuan Wu designed the research; Yuanyuan Wu, Wenrui Zhen,-and Yanqiang Geng performed the research and analyzed the data; Yuanyuan Wu wrote the manuscript; Zhong Wang and Yuming Guo participated in the revision of the manuscript. All authors contributed to data interpretation and approved the final version of the manuscript.
Corresponding author
Ethics declarations
Competing Interests
The authors declare no competing interests.
Additional information
Publisher’s note: Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary information
41598_2019_46578_MOESM1_ESM.pdf
Supplementary Figure 1. Effect of dietary E. faecium 11181 supplementation on taxonomic composition of cecum microbiota relative abundance in broiler chickens challenged with NE (n=6)
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons license, and indicate if changes were made. The images or other third party material in this article are included in the article’s Creative Commons license, unless indicated otherwise in a credit line to the material. If material is not included in the article’s Creative Commons license and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this license, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
Wu, Y., Zhen, W., Geng, Y. et al. Pretreatment with probiotic Enterococcus faecium NCIMB 11181 ameliorates necrotic enteritis-induced intestinal barrier injury in broiler chickens. Sci Rep 9, 10256 (2019). https://doi.org/10.1038/s41598-019-46578-x
Received:
Accepted:
Published:
DOI: https://doi.org/10.1038/s41598-019-46578-x
- Springer Nature Limited
This article is cited by
-
Effects of Tibetan Sheep–Derived Compound Probiotics on Growth Performance, Immune Function, Intestinal Tissue Morphology, and Intestinal Microbiota in Mice
Probiotics and Antimicrobial Proteins (2024)
-
Dietary supplemental coated essential oils and organic acids mixture improves growth performance and gut health along with reduces Salmonella load of broiler chickens infected with Salmonella Enteritidis
Journal of Animal Science and Biotechnology (2023)
-
Effects of Bacillus methylotrophicus SY200 Supplementation on Growth Performance, Antioxidant Status, Intestinal Morphology, and Immune Function in Broiler Chickens
Probiotics and Antimicrobial Proteins (2023)
-
Bacillus amyloliquefaciens BLCC1-0238 Alone or in Combination with Mannan-Oligosaccharides Alleviates Subclinical Necrotic Enteritis in Broilers
Probiotics and Antimicrobial Proteins (2022)
-
Effects of Treatment with Lactobacilli on Necrotic Enteritis in Broiler Chickens
Probiotics and Antimicrobial Proteins (2022)