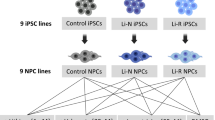
Abstract
Lithium is an effective, well-established treatment for bipolar disorder (BD). However, the mechanisms of its action, and reasons for variations in clinical response, are unclear. We used neural precursor cells (NPCs) and lymphoblastoid cell lines (LCLs), from BD patients characterized for clinical response to lithium (using the “Alda scale” and “NIMH Retrospective Life chart method”), to interrogate cellular phenotypes related to both disease and clinical lithium response. NPCs from two biologically related BD patients who differed in their clinical response to lithium were compared with healthy controls. RNA-Seq and analysis, mitochondrial membrane potential (MMP), cell viability, and cell proliferation parameters were assessed, with and without in vitro lithium. These parameters were also examined in LCLs from 25 BD patients (16 lithium responders and 9 non-responders), and 12 controls. MMP was lower in both NPCs and LCLs from BD; but it was reversed with in vitro lithium only in LCLs, and this was unrelated to clinical lithium response. The higher cell proliferation observed in BD was unaffected by in vitro lithium. Cell death was greater in BD. However, LCLs from clinical lithium responders could be rescued by addition of in vitro lithium. In vitro lithium also enhanced BCL2 and GSK3B expression in these cells. Our findings indicate cellular phenotypes related to the disease (MMP, cell proliferation) in both NPCs and LCLs; and those related to clinical lithium response (cell viability, BCL2/GSK3B expression) in LCLs.
Similar content being viewed by others
Introduction
Bipolar disorder (BD) is a highly heritable psychiatric illness, having a lifetime prevalence of 1–3%1. Although considered to have neurodevelopmental origins, the symptoms usually manifest in adulthood2. Lithium and valproate have been the mainstay of treatment for BD3, but their mechanisms of action and pharmacogenomics are poorly understood. Response to lithium varies considerably among patients, with 40–50% patients showing inadequate clinical response. Family members often share a similar pattern of lithium response, suggesting a genetic basis4. In our experience, lithium non-responders tend to be more severely ill5. However, it remains unclear whether non-response is the cause or effect of clinical severity. Currently, identification of patients who are likely to show a favorable response to lithium relies upon clinical criteria that lack specificity and sensitivity. Lithium remains a well-established drug for treatment of BD, and reliably predicting lithium response using molecular markers would be useful in initiating effective treatment earlier.
Several studies have used lymphoblastoid cell lines (LCLs) to study lithium response in vitro6. However, only a few studies have accounted for clinical response to lithium7,8,9,10,11,12,13,14,15,16. The identification of molecular markers for clinical response to lithium in lymphocytes/LCLs has huge potential for clinical translation. However, cells of neuronal lineage are more appropriate for studying the biological determinants of BD, and mechanisms of lithium action.
Human induced pluripotent stem cell (IPSC) models allow for the derivation of specific brain cell types, thus recapitulating the disease in a physiological context. Recent studies on iPSC-derived NPCs and neurons2 have found abnormalities in neural patterning, post-mitotic calcium signaling, and neuronal excitability in BD. Only a limited number of studies have examined IPSC derived neurons from BD patients who have been clinically characterized for lithium response. Increased neuronal excitability in IPSC-derived hippocampal neurons from BD patients has been shown to be selectively reduced by lithium in neurons from those patients who are clinical lithium responders17,18. Another recent study has identified an altered set-point regulation of CRMP2 (a downstream target of GSK-3B) phosphorylation to be a hallmark of IPSC derived neurons from lithium responsive BD patients19.
In this study, we have used a combination of cellular models (LCLs and IPSC-derived NPCs) to explore cellular parameters that clearly differentiate BD and healthy controls. In addition, we aimed to examine if these parameters could be reversed through addition of in vitro lithium, and if so, whether this reversal is associated with clinical lithium response.
We have used iPSC-derived neural precursor cells (NPCs) of BD patients from a family with multiple affected members who differed in their clinical response to lithium, and compared these to healthy population controls. Identified phenotypes were further studied in larger samples of LCLs from BD patients characterized for lithium response. Reversal of these phenotypes was attempted with in vitro lithium and valproate; the latter being the drug of choice for clinical lithium non-responders in our sample.
A hypothesis-free approach using RNA-Seq analysis did not reveal genome-wide gene expression differences in NPCs with or without in vitro lithium. A hypothesis-based approach based on existing literature (Supplementary Table 1) found cellular phenotypes related to disease [mitochondrial membrane potential (MMP) and cell proliferation] in NPCs and LCLs; and those related to lithium treatment response (cell viability and BCL2/GSK3B expression) in LCLs.
Materials and Methods
Clinical recruitment
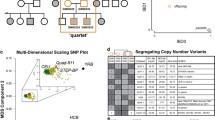
All BD patients had been recruited as part of a previous study which had systematically characterized 210 patients for clinical lithium response5. Family A (Fig. 1) had two BD patients clearly discordant for clinical lithium response (B1 – non-responder and B2 – responder), and had been recruited as part of a family-based cohort study of psychiatric illness in the Indian population, the Accelerator program for Discovery in Brain disorders using Stem cells (ADBS)20. All patients were assessed for clinical lithium response using the Alda Scale and NIMH Retrospective Life chart method4,21. A subset of 25 BD patients who exhibited extreme phenotypes for clinical lithium response [Lithium responders with Alda score ≥7 (N = 16) and lithium non-responders with Alda score ≤3 (N = 9)] were included in the current study (clinical details in Supplementary Table 2). All DSM-IV psychiatric diagnoses were corroborated by two trained psychiatrists using the Mini International Neuropsychiatric Interview22. Healthy controls (N = 12) who had neither Axis-I psychiatric illness nor family history of psychiatric illness in the previous two generations were also recruited. The NIMHANS ethics committee approved the study protocols and written informed consent was obtained from all participants. All research methods were carried out in accordance with the relevant guidelines and regulations.
LCL generation and characterization
Lymphoblastoid cell lines were generated using Epstein Barr Virus from peripheral blood mononuclear cells as previously described23. The cells were grown in RPMI-1640 (Himedia) medium containing 15% heat-inactivated fetal bovine serum (Gibco), 1% Penicillin-Streptomycin (Gibco) and 1% Glutamax (Gibco), as a suspension culture, in 5% CO2 incubator at 37 °C. Immunophenotyping of LCLs24 by flow cytometry (BD FACSVerse, BD Biosciences, USA) confirmed that the cells were positive for B cell marker CD19, and negative for both the T cell marker CD3 and the Natural Killer cell marker CD56 (Supplementary Figure 1A).
Differentiation of NPCs from human IPSCs
IPSCs of two patients with BD (lines B1 and B2 from family A), and one unrelated healthy control (C1) were obtained from the ADBS20. These IPSCs had been generated from LCLs as previously described25,26. Whole exome sequencing from this family has been previously published27 and rare damaging variants in B1 and B2 have been identified (Supplementary Table 3). A fibroblast-derived control IPSC (C2) was also used for the experiments. All NPC samples except C1, were from males.
NPCs were generated as previously described28. A well-characterized high-quality IPSC culture was enzymatically dissociated using StemPro Accutase (Gibco) and cultured in suspension until day 7 in Embryoid body (EB) medium [Knockout DMEM (Gibco), 20% KOSR (Gibco), 0.1 mM Non-Essential Amino Acids (Gibco), 2 mM Glutamax, 1% Penicillin-Streptomycin (Gibco), and 0.1 mM Betamercaptoethanol (Gibco)]. EB medium was replaced with Neural Induction Medium [DMEM/F12 (Gibco), N2 supplement (Gibco), 8 ng/ml bFGF (Gibco), 1x Glutamax (Gibco), 1x Penicillin-Streptomycin (Gibco), 1x Non-essential Amino Acids (Gibco) and 2 µg/ml Heparin (Sigma)] from day 7 to 14. Subsequently, EBs were plated on Matrigel (Corning) coated dishes and allowed to form neural rosettes. The neural rosettes were then passaged by manual selection and tertiary rosettes were mechanically dissociated through pipetting and plated as an NPC monolayer. The medium was then replaced with Neural Expansion Medium [DMEM/F12 (Gibco), N2 supplement (Gibco), B27 supplement without Vitamin A (Gibco), 8 ng/ml bFGF (Gibco), 1x Glutamax (Gibco), 1x Penicillin-Streptomycin (Gibco), 1x Non-essential Amino Acids (Gibco) and 2 µg/ml Heparin (Sigma)]. Quantitative immunolabelling revealed comparable NPC differentiation from IPSC lines (Nestin: C1–99.2 ± 0.4%, C2–99.3 ± 0.4%, B1–99.1 ± 0.6%, B2–99 ± 0.5%; Pax6: C1–95.2 ± 1.4%, C2, 94.2 ± 2% B1–94.8 ± 2.2%, B2–96.3 ± 1.8%; Fig. 2A).
Experiments using NPCs. (A) Representative immunocytochemistry of NPCs showing Nestin+ cells in all the four cell lines used for experiments. (B) Comparison of high MMP population percentage (MTDR) in the three groups at baseline and after in-vitro treatment with lithium (1 mM) or valproate (0.7 mM) for 7 days by flow cytometry (N = 5). (C) Representative immunocytochemistry of NPCs showing Nestin+ cells with mitochondria localized using TOMM22, and selection of regions of interest for calculation of mitochondrial area fraction. (D) Comparison of mitochondrial area (N = 3). (E) Comparison of dead cell population percentage in the three groups at baseline and after in-vitro treatment by flow cytometry (N = 5). (F) Representative immunocytochemistry of NPCs showing EdU+ cells indicating cells in S phase of cell cycle. (G) Comparison of EdU+ cells in the three groups at baseline and after in-vitro treatment (N = 3). All data are shown as mean ± s.e.m.; Experiments were performed in at least 3 independent experiments (N) for each cell line; For group comparisons, initially appropriate ANOVA test was applied and if significant, independent multiple comparison test were performed. Significance level: *p ≤ 0.05, **p ≤ 0.01, ***p ≤ 0.001, ****p ≤ 0.0001. Abbreviations: NPCs, neural precursor cells, MTDR, mitotracker deep red; MMP, mitochondrial membrane potential, EdU, 5-ethynyl-2′-deoxyuridine.
Gross chromosomal integrity as checked through karyotyping was normal. Mycoplasma contamination was checked regularly with an enzyme-based mycoplasma detection kit (Lonza) as per manufacturer’s instructions.
Drug treatment in NPCs
Cells were seeded at a density of 100 000 cells/cm2 on a tissue culture treated surface additionally coated with Matrigel. Approximately 12 hours post-seeding; the drugs were added to the media [Lithium Chloride (Sigma) at a working concentration of 1 mM or Sodium Valproate (Sigma) at a working concentration of 0.7 mM] or kept untreated. Cellular assays and RNA extraction were performed on day 7. Experiments were performed in biological triplicates.
Drug treatment in LCLs
Four million LCLs were seeded in each of the three T25 flasks having RPMI-1640 complete media as described before 1) 1 mM Lithium Chloride, or 2) 0.7 mM Sodium Valproate, or kept untreated. Post 7 days of treatment, LCLs were processed for cellular assays. Cells were also used for DNA and RNA extraction. Experiments were performed in biological triplicates.
Immunocytochemical analyses of NPCs
Cells were fixed in 4% paraformaldehyde (Sigma) for 20 min, permeabilized in 0.1% Triton X-100 (Invitrogen) at room temperature for 10 min and blocked in 3% donkey serum for 40 min. They were then incubated in primary antibodies for 60 min (Supplementary Table 5) followed by secondary antibodies for 30 min (Alexa Fluor dyes, Invitrogen; Supplementary Table 5). The nuclei were counterstained with DAPI (4′,6-diamidino-2-phenylindole, Life technologies) for 5 min and coverslips were mounted on slides with Vectashield (Vector labs). Fluorescent imaging was performed on fields of view containing uniform DAPI staining using a Fluoview 3000 (Olympus) microscope. Images were processed with ImageJ64 (v 1.47) software and immunolabelled cells counted manually by a blinded observer. At least 10 representative images were taken for each experiment, which was done in biological triplicates.
Whole transcriptome sequencing (RNA-Seq) and analysis
RNA-Seq was performed on the Illumina® Hi-Seq platform as per manufacturer’s protocol. There were two biological replicates available per sample. FastQC (v0.11.5; http://www.bioinformatics.babraham.ac.uk/projects/fastqc) was used for the quality of raw reads. It examines per base and per sequence quality scores, per base and per sequence GC content, per base N content and sequence length distribution. Cutadapt (v2.4) was used to remove adapter contamination in raw reads. The filtered reads were aligned to the human reference genome hg19 (GRCh37) using HISAT (v2.1). SAM to BAM conversion and sorting were done with Samtools 1.3 (https://sourceforge.net/projects/samtools/files/samtools/1.3/). The relative abundance of transcripts, measured as FPKM (Fragments Per Kilobase of transcript per Million mapped reads), was estimated using Cuffdiff (v2.02). Differentially expressed genes in response to lithium treatment were determined from the FPKM values obtained for each gene by calculating the fold change. Genes which showed >2-fold difference with FDR adjusted P-value < 0.05 were considered differentially expressed.
Mitochondrial membrane potential (MMP) and cell death assay
Live staining with Mitotracker Deep Red (MTDR, Invitrogen, at a working concentration of 100 nM) and a vital dye, Propidium Iodide (Invitrogen) at 15 µg/ml in NPCs, Sytox Green (Invitrogen) at 30 nM in LCLs followed by flow cytometry (BD FACSVerse™) was done to assess MMP and cell death respectively. Verapamil (Sigma) was also included at a working concentration of 5 µM to prevent potential dye leak. Experiments were performed in biological triplicates. FlowJo software was used for the analysis. Gates were applied on scatter plot using FSC vs SSC parameters to remove debris. Finally, quadrant gates were applied using MTDR vs Sytox green signal to analyze the cell population of interest. The change in the percentage of the cell population of interest (gated in Q1 and Q3) was examined to study cell viability and MMP (Supplementary Figure 1B).
Pharmacological agents were included as a positive depolarization control. Treatment of cells with Carbonyl cyanide m-chlorophenyl hydrazone (CCCP) (Sigma), a respiratory uncoupler/protonophore, at 50 µM29,30, or 2% paraformaldehyde (Sigma)31,32 for 30 minutes resulted in significant reduction of MMP (Supplementary Figure 1C). This validates the use of MTDR to investigate MMP, as has been reported in previous studies33,34,35,36.
Mitochondrial area in NPCs
Immunocytochemistry and analysis were performed as described earlier. Individual regions of interest were first chosen based on Nestin staining and mitochondrial immunolabelling with anti-TOMM22 was assessed in binary images.
Mitochondrial DNA content in LCLs
Total genomic DNA was extracted from LCLs and relative mitochondrial DNA (mtDNA) copy number was estimated by SYBR Green assay in a q-PCR system (Thermofisher). Cytochrome B (Cyt B) and NADH dehydrogenase 1 (ND1) genes were used to represent the mtDNA, and pyruvate kinase (PK) gene was used to represent the nuclear DNA. The primers selected for this experiment were based on an earlier study for mtDNA copy number by Gu et al.24. Relative mtDNA copy numbers of the genes Cyt B and ND1, normalized to the single-copy nuclear gene PK and relative to the calibrator is given by 2−ΔΔCt.
Cell proliferation/cycle assays
NPC proliferation assay was performed using the Click-it EdU Alexa Fluor 488 imaging kit (Invitrogen) in biological triplicates. EdU was added at a concentration of 10 µM in media incubated for an hour at 37 °C. Subsequently, cells were fixed and immunocytochemistry performed using the EdU detection cocktail and DAPI. The ratio of EDU positive to DAPI positive nuclei gave the percentage of cells in the proliferative phase.
Cell cycle assays were performed in LCLs fixed in 70% ethanol and subsequently incubated with Propidium Iodide dye (Invitrogen) at 15 ug/ml and RNase A (Invitrogen) at 40 ug/ml at 37 °C for 30 min. Flow cytometry was performed as described earlier. FlowJo software was used for the analysis. Appropriate gates were applied on scatter plot using parameters required to remove debris and clumps from analysis while including only singlet cells. A histogram plot was generated for the gated singlet cells. The histogram plot was analyzed to estimate the percentage of cells in different phases of cell-cycle (Supplementary Figure 1D, E).
Gene expression studies in LCLs
To estimate relative gene expression, total RNA was isolated using Trizol (Ambion) and converted to cDNA using SuperScript VILO cDNA Synthesis Kit (Thermofisher). Pooled RNA from untreated control samples was aliquoted and cDNA was synthesized to prepare calibrator. The calibrator sample was used to calculate the relative quantification (RQ). The use of calibrator also normalizes inter plate assay variation for multiple runs.
The TaqMan gene expression assays were used for relative quantification of the target genes. Housekeeping gene GAPDH was used for BCL2 and GSK3B expression, whereas HPRT was used for NR1D1 expression. The q-PCR was duplexed by simultaneous amplification and quantification of both, target gene and housekeeping gene in a single q-PCR reaction. The test sample cDNA along with No Template Control (NTC), calibrator, and Reverse Transcriptase (RT) negative sample were run in triplicates using the Real-time q-PCR system (AB7500; Thermofisher) to achieve the threshold cycle (Ct) value. The calculation used to estimate relative gene expression or RQ value is as follows:
The relative gene expression or RQ value, normalized to an endogenous gene and relative to a calibrator, is given by 2−ΔΔCt.
Statistical analysis
Deviance from normal distribution was checked using Shapiro-Wilk test. For normal distributions, one-way analysis of variance (ANOVA) and Student t-test were used for comparisons between controls and cases or between therapeutic response groups. For variables that were not normally distributed, Kruskal-Wallis & Mann-Whitney tests were used for comparison between groups. For in vitro treatment experiments also, we applied paired ANOVA and paired Student t-test in normally distributed data. For variables that did not follow normal distribution, the respective non-parametric test was applied, i.e. Friedman test (alternative to paired ANOVA) and Wilcoxon test.
While performing multiple tests, p-values were corrected using the appropriate correction method (viz. Dunn’s, Sidak’s, Tukey’s, and Holm-Sidak’s). All tests were two-tailed and the results with p values ≤ 0.05 were considered statistically significant. Results are presented in means with standard error of means (S.E.M). All statistical analyses were performed using GraphPad Prism version 7.00 for Windows, GraphPad Software, La Jolla California, USA (www.graphpad.com).
Results
RNA-Seq analysis of NPCs with and without in vitro lithium treatment
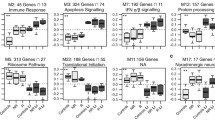
B1 (Lithium non-responder), B2 (Lithium responder), and control (C1 and C2) NPCs were treated in vitro with lithium (1 mM) for 7 days, followed by RNA-Seq analysis (Supplementary dataset) to investigate molecular markers of drug response. For a false discovery rate of 0.05, no genes were detected to be differentially expressed across the NPCs, before and after in vitro lithium. Other comparisons were underpowered due to the genetic variability between the studied NPCs.
Mitochondrial membrane potential (MMP) and cell viability assays in NPCs
After exploring for deficits in MMP and cell viability in the NPCs, reversal was attempted with 7 days of in vitro lithium (1 mM), and valproate (0.7 mM); followed by flow cytometry analyses. The concentrations were based on the physiological dose range and available literature on cellular changes with in vitro drug treatment7,37,38.
At baseline, the percentage of cells with high MMP was significantly lower in BD NPCs compared to control NPCs (Fig. 2B); however, there were no significant differences between B1 and B2. In vitro drug treatment also showed no differences. Mitochondrial area fraction measured by TOMM22 immunolabeling was similar across all groups (Fig. 2C,D).
BD NPCs had a significantly higher percentage of dead cells compared to controls at baseline (Fig. 2E). However, there were no significant differences between B1 and B2, or after in vitro drug treatment on this parameter either.
Cell proliferation assay in NPCs
Our experiments showed more EdU labelled cells (S phase) in BD NPCs compared to control NPCs (Fig. 2F,G). Similar to previous assays, there were no significant differences between B1 and B2, or after in vitro drug treatment.
Experimental validation of NPC results in larger sample size of LCLs
Our experiments on NPCs suggested a clear cellular phenotype in BD NPCs that however, did not reverse with in vitro drug treatment, or correlate with clinical lithium response. Hence, we decided to investigate these results in a peripheral model system, to assess its clinical utility. We used LCLs (an accepted cellular model for BD), from healthy controls and patients from the extremes of the clinical lithium response spectrum.
As in the NPCs, the percentage of cells with high MMP was significantly lower in BD LCLs compared to control LCLs (Fig. 3A). But this did not differ significantly between responders and non-responders. Mitochondrial DNA copy numbers in LCLs were also similar across groups (Fig. 3B,C). Interestingly, unlike in NPCs, in vitro lithium and valproate reversed the MMP deficit in LCLs derived from both responders and non-responders.
Experiments using LCLs. (A) Comparison of high MMP population percentage in the three groups at baseline and after in-vitro treatment with lithium (1 mM) or valproate (0.7 mM) for 7 days. (B) Comparison of relative quantification values of mitochondrial DNA- Cyt B, and (C) ND1, from qPCR normalized to PK (single copy nuclear DNA) at baseline and after treatment with lithium. (D) Comparison of G2/M population percentage in the three groups at baseline and after in-vitro treatment. (E) Comparison of dead cell population percentage in the three groups at baseline and after in-vitro treatment. (F) Relative gene expression of GSK3B across groups - comparison for RQ expression values of GSK3B gene from qPCR normalized to GAPDH (endogenous control). (G) Relative gene expression of BCL2 across groups - comparison for RQ expression values of BCL2 gene from qPCR normalized to GAPDH (endogenous control). All data are shown as mean ± s.e.m.; Experiments were performed in 3 independent experiments for each cell line; N, number of subject LCLs in each group. For group comparisons, initially appropriate ANOVA test was applied and if significant, independent multiple comparison test were performed. Significance level: *p ≤ 0.05, **p ≤ 0.01, ***p ≤ 0.001, ****p ≤ 0.0001. Abbreviations: LCLs, lymphoblastoid cell lines, MTDR, mitotracker deep red; MMP, mitochondrial membrane potential, PI, propidium iodide.
Similar to NPCs, BD LCLs also had greater numbers of proliferative cells (G2/M) in both responders and non-responders (Fig. 3D). The addition of valproate, but not lithium reversed this abnormality.
The dead cell percentage was significantly higher in BD LCLs, and this could be rescued by in vitro lithium in clinical responders (Fig. 3E). Valproate could reverse this abnormality in both responders and non-responders.
Gene expression analysis related to cell viability
We performed LCL gene expression analysis of BCL2, GSK3B and NR1D1. These have been found involved in the mechanism of lithium action/risk for bipolar disorder and cell viability (Supplementary Table 4). The BCL2 gene encodes for an integral outer mitochondrial membrane protein that regulates cell death by controlling mitochondrial membrane permeability39. GSK3B is involved in multiple signaling pathways controlling cellular metabolism, differentiation, death, and survival40. The NR1D1 gene, also known as Rev-ErbAα, encodes a transcription factor that is a member of the nuclear receptor subfamily 1; deletion of this gene affects the survival of neurons during postnatal development41. We found that in vitro lithium enhanced the expression of BCL2 and GSK3B specifically in LCLs from clinical lithium responders (Fig. 3F,G), and not in other groups. NR1D1 expression was similar across groups and remained unchanged after in vitro drug treatment.
Discussion
In BD, genetic factors may underlie risk of occurrence of disease, as well as response to treatment. Therefore, to delineate those mechanisms that could have a bearing on response to lithium, we chose two BD patients from the same family (i.e. shared genetic background) who were discordant in their response to lithium (Fig. 1) and characterized the cellular phenotypes related to disease and lithium treatment. In addition, we also examined cellular phenotypes in LCLs from a set of unrelated patients, and controls.
Mitochondrial dysfunction is one of the most consistently replicated findings across existing literature on BD18,42. We also found that the proportion of cells with high MMP is lower in cells derived from BD patients (Figs. 2B, 3A). Independent in vitro exposure to either lithium or valproate increased this proportion in patient-derived LCLs (Fig. 3A) but not NPCs (Fig. 2B). Former studies have shown that lithium treatment increased mitochondrial complex activity in leukocytes43 while valproate treatment enhanced NDUFV2 gene expression44.
The percentage of proliferating cells were higher in patient-derived cultures [NPCs (Fig. 2G) and LCLs (Fig. 3D)]. Increased cell proliferation in both NPCs and LCLs in BD patients suggests that this is a disease-related marker. Our findings corroborate with previous literature45,46,47,48 on dysregulation of genes associated with the G1 or G2 checkpoints of the cell cycle in BD. Exposure to in vitro lithium did not alter this phenotype, either in LCLs or in NPCs; irrespective of clinical response to lithium. A similar dissonance between clinical response to lithium, and in vitro lithium, has been reported by previous researchers49,50 in patient-derived T-lymphocytes. Collectively, these findings demonstrate that, although this cell proliferation phenotype strongly correlates with disease, it is not a reliable marker of clinical response to lithium.
Unlike in NPCs, in vitro lithium treatment of LCLs from BD helps to maintain cell viability as demonstrated by a decrease in the percentage of dead cells (“Responders-Lithium,” Fig. 3E). We also found an increase in BCL2 and GSK3B expression concomitant with in vitro lithium exposure in these LCLs (Fig. 3G). Previous studies have also shown that lymphocytes derived from BD patients have increased expression of the pro-apoptotic BAX protein, and are more prone to apoptosis50. GSK3B, a direct target of lithium, has also been shown to modulate cell survival40,51,52. In vitro lithium exposure (at 1 mM) for eight days has also been previously demonstrated to increase GSK3B mRNA53. Shorter durations of lithium exposure have not induced changes in GSK3B expression in earlier studies8,53.
Lithium has been used for the treatment of BD since 194954. Several molecular pathways and cellular processes have been implicated in its actions55, including its effect on cell viability56,57. Our finding that the addition of in vitro lithium is able to reduce the percentage of dead cells, in LCLs from clinical responders alone, suggests that the improvement of impaired cell viability with in vitro lithium could be used as a proxy marker for clinical lithium response.
As BD is usually an adolescent/adult onset disorder, it would have been ideal to also examine cortical neurons derived from NPCs. The absence of any effect of in-vitro lithium on the NPC based experiments, and lack of significant genome-wide result in the RNA-Seq analysis in our study, along with negative results in PSC derived embryoid bodies from another study58, indicate that we may need to use a more differentiated cell type to understand the effects of lithium in BD. Positive results using RNA-Seq have been reported earlier with the same duration and concentration of in-vitro lithium exposure in LCLs15,16.
The findings of this study, although novel and encouraging, have to be considered in the background of certain limitations. We have used a modest number of cell lines. The patients and controls were not matched for age or sex. The study was conducted in patients who had already been ill and on treatment since many years; they were not medication-naïve. Prospective studies, with greater number of cell lines, from medication-naïve patients and age and sex-matched controls exploring further differentiated cell types would provide more conclusive evidence.
To summarize, our findings indicate that there are cellular phenotypes related to disease (MMP, cell proliferation) in NPCs and LCLs from BD; and that the clinical effectiveness of lithium correlates well with improved cell viability in LCLs following addition of lithium in vitro. Confirmation of this finding through prospective studies in treatment-naïve patients who can be followed up after initiation of lithium treatment, would have immense clinical potential. Predicting treatment response to lithium is valuable in initiating appropriate treatment earlier on and improving clinical outcomes.
References
Grande, I., Berk, M., Birmaher, B. & Vieta, E. Bipolar disorder. Lancet (London, England) 387, 1561–1572 (2016).
Hoffmann, A., Sportelli, V., Ziller, M. & Spengler, D. From the Psychiatrist’s Couch to Induced Pluripotent Stem Cells: Bipolar Disease in a Dish. Int. J. Mol. Sci. 19 (2018).
López-Muñoz, F., Shen, W. W., D’Ocon, P., Romero, A. & Álamo, C. A History of the Pharmacological Treatment of Bipolar Disorder. Int. J. Mol. Sci. 19 (2018).
Grof, P. et al. Is response to prophylactic lithium a familial trait? J. Clin. Psychiatry 63, 942–7 (2002).
Kapur, V. et al. Clinical factors associated with lithium treatment response in bipolar disorder patients from India. Asian J. Psychiatr. 0, (2018).
Viswanath, B. et al. Cellular models to study bipolar disorder: A systematic review. J. Affect. Disord. 184, 36–50 (2015).
Cruceanu, C., Alda, M., Grof, P., Rouleau, G. A. & Turecki, G. Synapsin II is involved in the molecular pathway of lithium treatment in bipolar disorder. PLoS One 7, 1–8 (2012).
McCarthy, M. J. et al. Functional genetic variation in the Rev-Erbα pathway and lithium response in the treatment of bipolar disorder. Genes. Brain. Behav. 10, 852–861 (2011).
McEachin, R. C. et al. A genetic network model of cellular responses to lithium treatment and cocaine abuse in bipolar disorder. BMC Syst. Biol. 4, 158 (2010).
Shamir, A. et al. Inositol monophosphatase in immortalized lymphoblastoid cell lines indicates susceptibility to bipolar disorder and response to lithium therapy [2]. Molecular Psychiatry 3, 481–482 (1998).
Squassina, A. et al. The PDLIM5 gene and lithium prophylaxis: An association and gene expression analysis in Sardinian patients with bipolar disorder. Pharmacol. Res. 57, 369–373 (2008).
Squassina, A. et al. Insulin-like growth factor 1 (IGF-1) expression is up-regulated in lymphoblastoid cell lines of lithium responsive bipolar disorder patients. Pharmacol. Res. 73, 1–7 (2013).
Sun, X. et al. Identification of lithium-regulated genes in cultured lymphoblasts of lithium responsive subjects with bipolar disorder. Neuropsychopharmacology 29, 799–804 (2004).
Tseng, M. et al. BDNF protein levels are decreased in transformed lymphoblasts from lithium-responsive patients with bipolar disorder. J. Psychiatry Neurosci. 33, 449–53 (2008).
Pisanu, C. et al. Convergent analysis of genome-wide genotyping and transcriptomic data suggests association of zinc finger genes with lithium response in bipolar disorder. Am. J. Med. Genet. Part B Neuropsychiatr. Genet. 177, 658–664 (2018).
Breen, M. S. et al. Lithium-responsive genes and gene networks in bipolar disorder patient-derived lymphoblastoid cell lines. Pharmacogenomics J. 16, 446–453 (2016).
Stern, S. et al. Mechanisms Underlying the Hyperexcitability of CA3 and Dentate Gyrus Hippocampal Neurons Derived From Patients With Bipolar Disorder. Biol. Psychiatry, https://doi.org/10.1016/j.biopsych.2019.09.018 (2019).
Mertens, J. et al. Differential responses to lithium in hyperexcitable neurons from patients with bipolar disorder. Nature 527, 95–9 (2015).
Tobe, B. T. D. et al. Probing the lithium-response pathway in hiPSCs implicates the phosphoregulatory set-point for a cytoskeletal modulator in bipolar pathogenesis. Proc. Natl. Acad. Sci. USA 114, E4462–E4471 (2017).
Viswanath, B. et al. Discovery biology of neuropsychiatric syndromes (DBNS): a center for integrating clinical medicine and basic science. BMC Psychiatry 18, 106 (2018).
Roy-Byrne, P., Post, R. M., Uhde, T. W., Porcu, T. & Davis, D. The longitudinal course of recurrent affective illness: life chart data from research patients at the NIMH. Acta Psychiatr. Scand. Suppl. 317, 1–34 (1985).
Sheehan, D. V. et al. The Mini-International Neuropsychiatric Interview (M.I.N.I.): the development and validation of a structured diagnostic psychiatric interview for DSM-IV and ICD-10. J. Clin. Psychiatry 59 (Suppl 20), 22–33;quiz 34–57 (1998).
Ashok, A. et al. Does retinoic acid reverse cell cycle dysregulation in Alzheimer’s disease lymphocytes? Asian J. Psychiatr. 39, 174–177.
Hussain, T., Kotnis, A., Sarin, R. & Mulherkar, R. Establishment & characterization of lymphoblastoid cell lines from patients with multiple primary neoplasms in the upper aero-digestive tract & healthy individuals. Indian J. Med. Res. 135, 820–829 (2012).
Najar, A. H. et al. Derivation of iPSC lines from two patients with familial Alzheimer’s disease from India. Stem Cell Res. 34, 101370 (2019).
Iyer, S., Bhatia, P., Rao, M. & Mukherjee, O. Developing two reference control samples for the Indian population. Stem Cell Res. 30, 38–42 (2018).
Ganesh, S. et al. Exome sequencing in families with severe mental illness identifies novel and rare variants in genes implicated in Mendelian neuropsychiatric syndromes. Psychiatry Clin. Neurosci. 73, pcn.12788 (2018).
Mukherjee, O., Acharya, S. & Rao, M. Making NSC and Neurons from Patient-Derived Tissue Samples. in. Methods in molecular biology (Clifton, N.J.) 1919, 9–24 (2019).
Cottet-Rousselle, C., Ronot, X., Leverve, X. & Mayol, J.-F. Cytometric assessment of mitochondria using fluorescent probes. Cytom. Part A 79A, 405–425 (2011).
Perry, S. W., Norman, J. P., Barbieri, J., Brown, E. B. & Gelbard, H. A. Mitochondrial membrane potential probes and the proton gradient: a practical usage guide. Biotechniques 50, 98–115 (2011).
Chang, H.-Y. et al. Flow Cytometric Detection of Mitochondrial Membrane Potential. BIO-PROTOCOL 3 (2013).
Zerin, T., Kim, J.-S., Gil, H.-W., Song, H.-Y. & Hong, S.-Y. Effects of formaldehyde on mitochondrial dysfunction and apoptosis in SK-N-SH neuroblastoma cells. Cell Biol. Toxicol. 31, 261–272 (2015).
Jang, K.-J. et al. Mitochondrial function provides instructive signals for activation-induced B-cell fates. Nat. Commun. 6, 6750 (2015).
Mot, A. I., Liddell, J. R., White, A. R. & Crouch, P. J. Circumventing the Crabtree Effect: A method to induce lactate consumption and increase oxidative phosphorylation in cell culture. Int. J. Biochem. Cell Biol. 79, 128–138 (2016).
Nagy, S. T. et al. Effects of high ambient temperature on fish sperm plasma membrane integrity and mitochondrial activity — A flow cytometric study. Acta Biol. Hung. 67, 125–132 (2016).
Peña, F. J., Ball, B. A. & Squires, E. L. A New Method for Evaluating Stallion Sperm Viability and Mitochondrial Membrane Potential in Fixed Semen Samples. Cytom. Part B Clin. Cytom. 94, 302–311 (2018).
Hampton, P. J., Jans, R., Flockhart, R. J., Parker, G. & Reynolds, N. J. Lithium regulates keratinocyte proliferation via glycogen synthase kinase 3 and NFAT2 (nuclear factor of activated T cells 2). J. Cell. Physiol. 227, 1529–1537 (2012).
Hunsberger, J. G. et al. Novel integrative genomic tool for interrogating lithium response in bipolar disorder. Transl. Psychiatry 5, e504 (2015).
Lindsay, J., Esposti, M. D. & Gilmore, A. P. Bcl-2 proteins and mitochondria—Specificity in membrane targeting for death ☆. BBA - Mol. Cell Res. 1813, 532–539 (2011).
Maurer, U., Preiss, F., Brauns-Schubert, P., Schlicher, L. & Charvet, C. GSK-3 - at the crossroads of cell death and survival. J. Cell Sci. 127, 1369–78 (2014).
Chomez, P. et al. Increased cell death and delayed development in the cerebellum of mice lacking the rev-erbA(alpha) orphan receptor. Development 127, 1489–98 (2000).
Cataldo, A. M. et al. Abnormalities in mitochondrial structure in cells from patients with bipolar disorder. Am. J. Pathol. 177, 575–585 (2010).
de Sousa, R. T. et al. Lithium increases leukocyte mitochondrial complex I activity in bipolar disorder during depressive episodes. Psychopharmacology (Berl). 232, 245–250 (2015).
Washizuka, S., Iwamoto, K., Kakiuchi, C., Bundo, M. & Kato, T. Expression of mitochondrial complex I subunit gene NDUFV2 in the lymphoblastoid cells derived from patients with bipolar disorder and schizophrenia. Neurosci. Res. 63, 199–204 (2009).
Kim, K. H. et al. Transcriptomic Analysis of Induced Pluripotent Stem Cells Derived from Patients with Bipolar Disorder from an Old Order Amish Pedigree. PLoS One 10, e0142693 (2015).
Benes, F. M. et al. Regulation of the GABA cell phenotype in hippocampus of schizophrenics and bipolars. Proc. Natl. Acad. Sci. 104, 10164–10169 (2007).
Benes, F. M., Lim, B. & Subburaju, S. Site-specific regulation of cell cycle and DNA repair in post-mitotic GABA cells in schizophrenic versus bipolars. Proc. Natl. Acad. Sci. USA 106, 11731–6 (2009).
Marianthi, L., Olga, P., Aristotelis, C., Nikolaos, V. & Fragiskos, K. Gene Expression Analysis of Fibroblasts from Patients with Bipolar Disorder. J. Neuropsychopharmacol. Ment. Heal. 1, 1–9 (2015).
Squassina, A. et al. Leukocyte telomere length positively correlates with duration of lithium treatment in bipolar disorder patients. Eur. Neuropsychopharmacol. 26, 1241–1247 (2016).
Pietruczuk, K., Lisowska, K. A., Grabowski, K., Landowski, J. & Witkowski, J. M. Proliferation and apoptosis of T lymphocytes in patients with bipolar disorder. Sci. Rep. 8, 3327 (2018).
Jacobs, K. M. et al. GSK-3: A Bifunctional Role in Cell Death Pathways. Int. J. Cell Biol. 2012, 1–11 (2012).
Yoshino, Y. & Ishioka, C. Inhibition of glycogen synthase kinase-3 beta induces apoptosis and mitotic catastrophe by disrupting centrosome regulation in cancer cells. Sci. Rep. 5, 13249 (2015).
Geoffroy, P. A. et al. Lithium response in bipolar disorders and core clock genes expression. World J. Biol. Psychiatry 1–14 https://doi.org/10.1080/15622975.2017.1282174 (2017).
CADE, J. F. J. Lithium salts in the treatment of psychotic excitement. Med. J. Aust. 2, 349–52 (1949).
Jope, R. S. Anti-bipolar therapy: mechanism of action of lithium. Mol. Psychiatry 4, 117–28 (1999).
Chen, R.-W. & Chuang, D.-M. Long Term Lithium Treatment Suppresses p53 and Bax Expression but Increases Bcl-2 Expression. J. Biol. Chem. 274, 6039–6042 (1999).
Rowe, M. K. & Chuang, D.-M. Lithium neuroprotection: molecular mechanisms and clinical implications. Expert Rev. Mol. Med. 6, 1–18 (2004).
Mayshar, Y., Yanuka, O. & Benvenisty, N. Teratogen screening using transcriptome profiling of differentiating human embryonic stem cells. J. Cell. Mol. Med. 15, 1393–1401 (2011).
Acknowledgements
The authors would like to thank Dr. Preeti Joshi, (Retd.) Professor of Biophysics, NIMHANS; Dr. Y C Janardhan Reddy, Professor of Psychiatry, NIMHANS and Dr. Mitradas M. Panicker (Retd.) Faculty of Neurobiology, NCBS, for providing critical inputs during various parts of the project. We are grateful towards Dr Manjunath, Assistant Professor of Neurovirology, NIMHANS and Phillippo, PhD Scholar, NIMHANS for their constructive criticism and valuable suggestions related to FACS experiments and also allowing us to access the Flowcytometry facility. We sincerely thank Dr. Ravi Muddashetty and Dr. Dasaradhi Palakodety for providing computational facilities for transcriptome analysis. We would also like to thank Ms. Varalakshmi R. and Mr. Suneela Kumar B. for the technical support. We would like to thank the clinicians and staff at the NIMHANS; as well as the participants and their families for their co-operation. This work was supported by a grant from the Department of Biotechnology (COE), India funded grants- “Targeted generation and interrogation of cellular models and networks in neuro-psychiatric disorders using candidate genes” (BT/01/CEIB/11/VI/11/2012) and “Accelerating program for discovery in brain disorders using stem cells” (BT/PR17316/MED/31/326/2015) (ADBS); the Department of Science and Technology, India funded grants- “Imaging-genomics approach to identify molecular markers of Lithium response in Bipolar disorder” through the DST-INSPIRE Faculty Fellowship awarded to Dr. Biju Viswanath (Project number 00671, Code: IFA-12-LSBM-44) and SCIENCE& ENGINEERING RESEARCH BOARD (SERB) project “Dissecting the biology of lithium response in human induced pluripotent stem cell derived neurons from patients with bipolar affective disorder” (FILE NO. ECR/2016/002076). SI, RKN, ASC, RS and SKS is funded by the DBT -ADBS. PP is initially funded by DBT -COE and currently being funded by DBT-ADBS. RN is funded by the grant- Consortium on Vulnerability to Externalizing Disorders and Addictions (c-VEDA), jointly funded by Indian Council for Medical Research (ICMR) and the Newton Grant from the Medical Research Council (MRC), United Kingdom. The results of this work have been partially presented as poster in conferences- at XXVth World Congress of Psychiatry Genetics, Orlando, 2017; XXVIth World Congress of Psychiatry Genetics, Glasgow, Scotland, 2018.
Author information
Authors and Affiliations
Consortia
Contributions
P.P. – LCL experiments, wrote first draft, read and approved final manuscript. R.N. – LCL experiments, read and approved final manuscript. R.K.N. - performed clinical assessments, read and approved final manuscript. S.I. – NPC experiments, read and approved final manuscript. A.C. – RNA-Seq and analysis, read and approved final manuscript. S.A. - RNA-Seq and analysis, read and approved final manuscript. S.S. – NPC experiments, read and approved final manuscript. R.S. – NPC experiments, read and approved final manuscript. S.J. – Supervision of clinical assessments, read and approved final manuscript. M.P. - supervised cellular experiments, read and approved final manuscript. B.V. - wrote first draft, prepared figures, supervised clinical assessments and cellular experiments, read and approved final manuscript.
Corresponding author
Ethics declarations
Competing interests
The authors declare no competing interests.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary information
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons license, and indicate if changes were made. The images or other third party material in this article are included in the article’s Creative Commons license, unless indicated otherwise in a credit line to the material. If material is not included in the article’s Creative Commons license and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this license, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
Paul, P., Iyer, S., Nadella, R.K. et al. Lithium response in bipolar disorder correlates with improved cell viability of patient derived cell lines. Sci Rep 10, 7428 (2020). https://doi.org/10.1038/s41598-020-64202-1
Received:
Accepted:
Published:
DOI: https://doi.org/10.1038/s41598-020-64202-1
- Springer Nature Limited
This article is cited by
-
Focal adhesion is associated with lithium response in bipolar disorder: evidence from a network-based multi-omics analysis
Molecular Psychiatry (2024)
-
The Crosstalk Between Pathological Tau Phosphorylation and Mitochondrial Dysfunction as a Key to Understanding and Treating Alzheimer’s Disease
Molecular Neurobiology (2020)