Abstract
The ability of cancer cells to undergo partial-epithelial mesenchymal transition (p-EMT), rather than complete EMT, poses a higher metastatic risk. Although Fusobacterium nucleatum mainly inhabits in oral cavity, attention has been focused on the F. nucleatum involvement in colorectal cancer development. Here we examined the p-EMT regulation by F. nucleatum in oral squamous cell carcinoma (OSCC) cells. We cultured OSCC cells with epithelial, p-EMT or EMT phenotype with live or heat-inactivated F. nucleatum. Expression of the genes involved in epithelial differentiation, p-EMT and EMT were examined in OSCC cells after co-culture with F. nucleatum by qPCR. Cell growth and invasion of OSCC cells were also examined. Both live and heat-inactivated F. nucleatum upregulated the expression of p-EMT-related genes in OSCC cells with epithelial phenotype, but not with p-EMT or EMT phenotype. Moreover, F. nucleatum promoted invasion of OSCC cells with epithelial phenotype. Co-culture with other strains of bacteria other than Porphyromonas gingivalis did not alter p-EMT-related genes in OSCC cells with epithelial phenotype. F. nucleatum infection may convert epithelial to p-EMT phenotype via altering gene expression in OSCC. Oral hygiene managements against F. nucleatum infection may contribute to reduce the risk for an increase in metastatic ability of OSCC.
Similar content being viewed by others
Introduction
Head and neck cancer is the seventh most common cancer overall (the fifth most common in men and the 12th most common in women), accounting for an estimated 888,000 new cases in 20181. Oral cancer, predominantly oral squamous cell carcinoma (OSCC), is a significant health problem and is considered the leading cause of death from oral diseases in many countries. According to GLOBOCAN (The global burden of cancer), it is estimated 354,864 new cases and 177,384 deaths of oral cancer in 20181. Traditional risk factors of OSCC include alcohol consumption, tobacco and tobacco-derivate chewing and oral virus infections (HPV). Other factors include infections by poor oral hygiene, exposure to ionizing radiation, and environmental pollutants2,3. Thus, various causes of cancer are known to be closely involved in lifestyle choices such as smoking, drinking and diet. Inflammation caused by infections has been suggested to be one of the most important cause of cancers4. As more than 700 bacterial species exist in an oral cavity, bacterial infection may cause oral cancer. However, it remains unclear the role of bacteria in oral carcinogenesis even though a lot of bacteria inhabit in the oral cavity.
Fusobacterium nucleatum is an obligate Gram-negative anaerobic bacilli, which mainly inhabits in oral cavity5. It is associated with periodontal disease and pregnancy complications such as neonatal sepsis, still-birth and pre-term birth6,7. Moreover, it has been reported the association between F. nucleatum and colorectal8,9, esophageal10 and breast cancer11. Although there are many reports on the detection of Fusobacterium in OSCC tissues12,13,14, the detailed mechanism of Fusobacterium in OSCC cells remains unclear. The fact that F. nucleatum is abundant in the oral cavity of OSCC patients seems to be important in tumorigenesis and progression of oral cancer.
Epithelial mesenchymal transition (EMT) is a process by which epithelial cells lose their cell polarity and cell–cell adhesion, and gain mesenchymal properties. It can be seen during development, wound healing, inflammation, and cancer development. EMT contributes to cancer progression by imparting the mesenchymal phenotypes associated with the cells of highly aggressive tumors15. EMT is not binary process and cells move through between full epithelial and mesenchymal states, which is called the intermediate state of EMT, partial EMT (p-EMT)16. Cancer cells with p-EMT state act like cancer cells with mesenchymal state, but they do not completely lose their epithelial features17. We previously showed that p-EMT genes such as SERPINE1, ITGA5, TGFBI, P4HA2, CDH13, and LAMC2 are potent poor prognostic markers in head and neck squamous cell carcinoma (HNSCC) patients by bioinformatic analysis18. Thus, understanding the state of p-EMT is crucial in finding a target cancer potential including cancer development and malignancy.
It recently has been reported that F. nucleatum is associated with EMT in cancer development. F. nucleatum decrease the levels of epithelial marker including E-cadherin and increase the levels of EMT-associated transcription factors including Snail and Slug in colorectal cancer progression19. Moreover, ZEB1 level is upregulated by F. nucleatum exposure in oral cancer cells20. However, the contribution of F. nucleatum to the regulation of p-EMT in OSCC remains unclear.
Methods
Cell culture
In this study, we used OSCC cell lines, HCS2, HOC313, HOC621, HOC719PE and HOC719NE. HSC2 cells were provided by the Japanese Collection of Research Bioresources Cell Bank. HOC313, HOC621, HOC719PE and HOC719NE cells were provided from Prof. Kamata (Hiroshima University). We previously found that HOC719NE and HOC313 have EMT features including loss of E-cadherin expression21,22. They were maintained in Dulbecco’s Modified Eagle Medium (Nacalai tesque, Inc., Kyoto, Japan) supplemented with 10% heat-inactivated FBS (Invitrogen) under conditions of 5% CO2 in air at 37˚C.
Bacterial culture
Fusobacterium nucleatum (JCM8532, ATCC10953, JCM11024, and ATCC23726) and Porphyromonas gingivalis (ATCC33277) were cultured by brain heart infusion (BHI, Becton Dickinson, Sparks, MD, USA) supplemented with 5 µg/mL hemin and 0.5 µg/mL menadione anaerobically at 37 °C. Streptococcus mutans (UA159) was cultured by BHI anaerobically at 37 °C. Pseudomonas aeruginosa (PAO1) and Escherichia coli (ATCC23511) were grown using lennox L broth (LB, Thermo Fisher Scientific, MA, USA) with shaking at 37 °C. All bacteria were cultured to the absorbance at OD590 = 1.0 and used for following experiments.
For F. nucleatum inactivation, the bacterial cells were heat-inactivated at 100 °C for 15 min. Killing was confirmed by absence of growth on sheep blood agar plate (Becton Dickinson, Sparks, MD, USA). Other bacteria, P. gingivalis, S. mutans, P. aeruginosa, and E. coli were also heat-inactivated at 100 °C for 15 min.
To analyze the presence of bacteria, F. nucleatum were stained with CytoTell UltraGreen (AAT Bioquest, CA, USA) in accordance with the manufacturer’s instructions. Briefly, the bacterial cells were treated with CytoTell UltraGreen for 15 min at 37 °C, and then treated to HOC621 cells at the concentration of 100 MOI for 3 h. The cells were fixed with 4% formalin for 30 min and then permeabilized with 0.1% Triton X-100 in PBS for 2 min on ice, followed by Hoechst 33,342 for 30 min. The samples were mounted and observed by a Nikon A1 laser fluorescence confocal microscopy (A1 R HD25, Nikon, Tokyo). Images were acquired with the NIS-Elements software (Nikon, Tokyo, Japan).
Colony-forming unit (CFU) determination
To quantify the viability of bacteria within host cells, colony-forming units were quantified as follows. OSCC cells were cultured on a 48-well plate, followed by treatment with F. nucleatum for 3 h, and then treated with antibiotics (200 μg/mL metronidazole and 300 μg/mL gentamicin) for 60 min to kill the F. nucleatum on the cell surface. The cells were lysed by adding 200 μL of H2O and the extract was spread on a sheep blood agar using a spiral plater (EDDY-Jet, IUL Instruments, Königswinter, Germany). Agar plates inoculated were incubated for 5 days in an anaerobic jar at 37 °C, and then, formed colonies were counted according to the manufacturer’s instructions.
Cell proliferation assay
Cells were suspended 5,000 cells/well in 96-well plate. After 24, 48, and 72 h, proliferating cells were determined by using cell-counting kit 8 (CCK-8) solution (Dojindo Molecular Technique, Inc.). 10 µl of CCK-8 solution was added in each well and incubated for 1 h in CO2 incubator at 37 °C. The signal of proliferating cells was measured absorbance at 450 nm using microplate reader model 680 (BIORAD).
qPCR
Total RNA was isolated from the cells by using the RNeasy Mini Kit (Qiagen) according to the manufacturer’s instructions. RNA concentration and purity were determined by standard spectrophotometric methods using a NanoDrop ND-2000 (NanoDrop Technologies). cDNA was synthesized from 1 µg total RNA using the PrimeScript II reverse transcriptase (Takara Bio Inc.). Expression of p-EMT, EMT and epithelial differentiation-relatedgenes were measured using TB Green Premix Ex Taq II (Takara Bio Inc.) with a LightCycler 96 system (Roche). The primers used in this study are shown in Supplementary Table S1. Relative mRNA expression of each transcript was normalized to the endogenous control GAPDH mRNA and were calculated using the comparative cycle threshold method.
Heatmap was generated by R package pheatmap. Expression values were centered and scaled in the row direction, each gene.
In vitro invasion assay
For in vitro invasion assay, we used a 24-well cell culture insert with 8 μm pores (3097, Falcon, Becton Dickinson). The membrane of cell culture insert was coated with 20 μg of matrigel (Becton Dickinson) for reconstituting basement membrane substance. 0.5 ml of serum-free medium were added in the lower compartment. 1.5 × 105 cells were resuspended in 100 μl of serum-free medium and placed in the upper compartment of the cell culture insert for 12–24 h. After incubation, the cells that penetrated the membrane into the lower side of the filter through the pores were fixed with formalin and then were stained by hematoxylin. The invasion ability of the cells was determined by counting the penetrating cells onto the lower side. We assayed 3 times. The penetrating cells in randomly selected 3 fields were counted for each assay under a microscope at × 100 magnification.
Statistical analysis
For cell proliferation and qRT-PCR analyses, the t-test was used to compare results between two groups. A P-value of < 0.05 was considered significant.
Results
It recently has been shown that F. nucleatum plays a role in EMT induction of cancer cells. Moreover, the ability of cancer cells to undergo p-EMT poses a higher metastatic risk rather than complete EMT. We previously classified the OSCC cell lines as “epithelial”, “p-EMT”, and “EMT” phenotype by gene expression profiles (Fig. 1A). In this study, four subspecies of F. nucleatum (JCM8532, ATCC10953, JCM11024, and ATCC23726) and five OSCC cell lines (EMT phenotype, HOC313 and HOC719NE; p-EMT phenotype, HOC719-PE; epithelial phenotype, HOC621 and HSC2) were used (Fig. 1B). In our preliminary experiments, the effects of F. nucleatum at MOI = 10 and 100 on cell proliferation and gene expression was similar. Therefore, we used F. nucleatum at MOI = 10 in the following experiments. We cultured OSCC cells with live or heat-inactivated F. nucleatum for 4 days. As shown in Fig. 2A, we confirmed that bacterial cells after heating for 15 min at 100 °C did not grow on blood agar.
Strategies of this study. (A) The list of OSCC cell lines that showing their properties; epithelial phenotype, p-EMT phenotype, and EMT phenotype. The properties were defined by gene expression18. (B) Study flow of Fusobacterium nucleatum treatment to OSCC cells for analyses including the cell proliferation, in vitro invasion assay and gene expression. Four subspecies of F. nucleatum and 5 OSCC cell lines were used. After OSCC was co-cultured with F. nucleatum for 96 h and then washed by PBS five times. After washing, cells were used for the analyses.
Preparation of heat-inactivated F. nucleatum and attachment of F. nucleatum on the surface of OSCC cells. (A) Pictures of F. nucleatum colonies. The heat-inactivated F. nucleatum bacterial cells were prepared by heating for 15 min at 100 °C. Bacterial cells show no colony forming on sheep blood agar after heat inactivation. (B) Attachment of F. nucleatum on the surface of OSCC cells. Green fluorescent-labeled live or heat-inactivated F. nucleatum (JCM8532 and ATCC10953) were co-culture with OSCC cells for 3 h. After washing by PBS, attached cells on the surface of OSCC cells were checked by immunofluorescence microscopy. Images show that heat-inactivated or live bacterial cells attach on the surface of OSCC cells. Moreover, invaded bacterial cells into OSCC cells were examined by culture on blood agar after treatment with antibiotics. Table shows the number of invaded F. nucleatum (CFU/ml) in OSCC cells (HOC621, HSC2, HOC719-PE, and HOC719-NE).
We first examined the attachment between OSCC cells and bacterial cells. HOC621 cells were co-cultured with green fluorescent-labeled live or heat-inactivated F. nucleatum (JCM8532 and ATCC10953) for 3 h, and then the cells were washed three times by PBS. After co-culture, live or heat-inactivated F. nucleatum was observed on the surface of HOC621 cells (Fig. 2B). We also examined the invasive potential of F. nucleatum (JCM8532, ATCC10953, JCM11024, and ATCC23726) into OSCC cells. After treatment with antibiotics, intracellular live bacterial cells were cultured on blood agar. Bacterial culture revealed that some bacterial cells invaded into OSCC cells (Fig. 2B).
Then, we compared the effects of live or heat-inactivated F. nucleatum on cell morphology, proliferation, and gene expression in HOC313 cells (EMT phenotype) and HOC621 cells (epithelial phenotype). After 48 and 72 h, co-culture with live or heat-inactivated F. nucleatum did not change the morphology of OSCC cells (Fig. 3A). Co-culture with live F. nucleatum, except heat-inactivated F. nucleatum (ATCC10953), did not affect cell proliferation in both HOC313 and HOC621 cells (Fig. 3B). We also examined the cell proliferation of HOC621 cells after co-culture with other subspecies of F. nucleatum (JCM11024 and ATCC23726). Among them, co-culture with live or heat-inactivated F. nucleatum, except heat-inactivated F. nucleatum (ATCC23726), did not affect cell proliferation in HOC621 cells (Supplementary Fig. S1). Thus, co-culture with most F. nucleatum subspecies did not affect cell morphology and cell proliferation of OSCC cells.
Cell morphology and proliferation in OSCC cells after co-culture with F. nucleatum. (A) Morphological images of OSCC cells after co-culture with F. nucleatum for 48 and 72 h. HOC313 and HOC621 were co-cultured with live or heat-inactivated F. nucleatum (JCM8532 and ATCC10953, MOI = 10). (B) Cell proliferation of HOC313 and HOC621 cells after co-culture with live or heat-inactivated F. nucleatum (JCM8532 and ATCC10953, MOI = 10). The graphs show the results as mean ± S.D. of three independent experiments. (*) represents P-value of < 0.05 compared to control (no treatment).
Although F. nucleatum is associated with EMT in cancer development19, the involvement of p-EMT in F. nucleatum infection remains unclear. Therefore, we examined the involvement of F. nucleatum in the regulation of p-EMT of OSCC. Expression of epithelial differentiation-related genes, p-EMT-related genes, and EMT-related genes was examined by qPCR in HOC313 and HOC621 cells with live F. nucleatum (JCM11024 and ATCC23726). In HOC621 cells, but not HOC 313 cells, p-EMT-related and EMT-related genes were remarkably upregulated by co-culture with live F. nucleatum (Fig. 4A,B). Moreover, we confirmed similar tendency in other subspecies of F. nucleatum (JCM11024, and ATCC23726) in HOC621 cells (Supplementary Fig. S2). The upregulated levels of p-EMT-related genes depended on the bacterial subspecies, indicating that pathogenicity may vary depending on the bacterial subspecies. These findings suggest that live F. nucleatum may upregulate p-EMT genes in OSCC cells with epithelial phenotype.
Co-culture with live F. nucleatum upregulates p-EMT-related genes in epithelial phenotype, HOC621 cells, but not in EMT phenotype, HOC313 cells. After co-culture with live F. nucleatum (JCM8532 and ATCC10953, MOI = 10), expression of epithelial differentiation-related, p-EMT-related, and EMT-related genes was determined by qPCR in EMT phenotype, HOC313 (A) and epithelial phenotype, HOC621 cells (B). The graphs show the results as mean ± S.D. of three independent experiments. (*) represents P-value of < 0.05 compared to control (no treatment).
Next, we examined whether the phenotype brought about by live F. nucleatum were also caused by heat-inactivated F. nucleatum. The heat-inactivated F. nucleatum (JCM8532 and ATCC10953) did not alter the expression of p-EMT-related genes in HOC313 cells (Fig. 5A). Interestingly, heat-inactivated F. nucleatum as well as live F. nucleatum upregulated p-EMT-related genes in HOC621 cells (Fig. 5B and Supplementary Fig. S2). Thus, both live and heat-inactivated F. nucleatum upregulated p-EMT-related genes in OSCC cells with epithelial phenotype, but not with EMT phenotype. To confirm these findings, we examined the gene expression in other OSCC cells with epithelial and EMT phenotype after co-culture with live or heat-inactivated F. nucleatum (Fig. 6). Alteration of p-EMT-related genes in epithelial phenotype, HSC2 cells (Supplementary Fig. S3) was remarkable after co-culture with live or heat-inactivated F. nucleatum, compared with EMT phenotype, HOC719-NE cells (Supplementary Fig. S4). We also examined the effect of live or heat-inactivated F. nucleatum in p-EMT phenotype, HOC719-PE cells. As expected, both live and heat-inactivated F. nucleatum did not alter the expression of p-EMT-related genes in HOC719-PE cells (Fig. 6 and Supplementary Fig. S5).
Co-culture with heat-inactivated F. nucleatum upregulates p-EMT-related genes in eEpithelial phenotype, HOC621 cells. After co-culture with heat-inactivated F. nucleatum (JCM8532 and ATCC10953, MOI = 10), expression of epithelial differentiation-related, p-EMT-related, and EMT-related genes was determined by qPCR in HOC313 (A) and HOC621 cells (B). The graphs show the results as mean ± S.D. of three independent experiments. (*) represents P-value of < 0.05 compared to control (no treatment).
Heatmap of gene expression by co-culture with live or heat-inactivated F. nucleatum in OSCC cells. Heatmap shows live or heat-inactivated F. nucleatum (JCM8532, ATCC10953, JCM11024, and ATCC23726) in OSCC with epithelial (HOC621 and HSC2), p-EMT (HOC719-PE), and EMT phenotype (HOC313 and HOC719-NE). Gene expression data is shown in Fig. 4 (HOC313 and HOC621), Fig. 5 (HOC313 and HOC621), Supplementary Fig. S2 (HOC621), Supplementary Fig. S3 (HOC719-NE), Supplementary Fig. S4 (HSC2), and Supplementary Fig. S5 (HOC-719-PE).
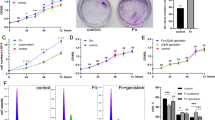
It has been shown that p-EMT program in cancer cells enhances the invasive properties. Therefore, we examined the invasion ability of HOC621 cells after treatment with 4 subspecies of F. nucleatum (JCM8532, ATCC10953, JCM11024, and ATCC23726) by in vitro invasion assay. Most live or heat-inactivated F. nucleatum subspecies statistically promoted the invasion ability (Fig. 7A,B). Enhanced invasion ability by F. nucleatum was also observed in HSC2 cells (Supplementary Fig. S6). These findings indicate that F. nucleatum may enhance the invasion ability via upregulation of p-EMT-related genes in OSCC cells with epithelial phenotype.
Invasive ability is promoted by co-culture with live or heat-inactivated F. nucleatum in epithelial phenotype, HOC621 cells. After co-culture with 4 subspecies of live or heat-inactivated F. nucleatum (MOI = 10), invasion ability was determined by in vitro invasion assay in epithelial phenotype, HOC621 cells. (A) Pictures showed the invaded OSCC cells after co-cultured with 4 subspecies of live or heat-inactivated F. nucleatum. (B) Graph shows the number of invaded OSCC cells after co-cultured with 4 subspecies of live or heat-inactivated F. nucleatum. Three independent experiments were used to calculate the mean ± S.D. (*) represents P-value of < 0.05 compared to control (no treatment).
To know whether upregulation of p-EMT-related genes in OSCC cells with epithelial phenotype is specific event by F. nucleatum, we examined the gene expression in HOC621 cells after treatment with other strains, such as P. gingivalis (ATCC33277), S. mutans (UA159), P. aeruginosa (PAO1), and E. coli (ATCC23511). These bacteria did not change the morphology of HOC621 cells (Supplementary Fig. S7A). E. coli and S. mutans did not affect cell proliferation, but P. gingivalis and P. aeruginosa suppressed cell proliferation (Supplementary Fig. S7B). Most bacterial cells, except P. gingivalis, did not affect the expression of p-EMT-related genes (Fig. 8A and Supplementary Fig. S8).
Remarkable upregulation of p-EMT-related genes by F. nucleatum in epithelial phenotype, HOC621 cells. (A) Heatmap shows the expression levels of epithelial differentiation-related, p-EMT-related, and EMT-related genes after co-culture with heat-inactivated F. nucleatum, P. gingivalis, S. mutans, P. aeruginosa, and E. coli in epithelial phenotype, HOC621 cells. Gene expression data is shown in Supplementary Fig. S8. (B) Schematic model showing that F. nucleatum promotes invasion of OSCC cells via conversion from epithelial to p-EMT phenotype.
Discussion
Bacteria, fungi, viruses, and archaea naturally colonize in the oral cavity. The oral microbiota refers to a highly varied and complicated ecosystem of these organisms. Over 700 bacterial species are endemic to the oral cavity, and oral commensal bacteria play a critical role in the maintenance of a normal oral physiological environment and the development of systemic diseases23,24. It recently has been shown that oral commensal bacteria may be involved in the pathogenesis of OSCC25,26. The proportion of anaerobes within the biofilms on the surfaces of OSCC tissues is higher than that in the healthy control, indicating that OSCC surfaces provide an important reservoir for anaerobic bacteria27. There are many reports showing that Fusobacterium were detected in OSCC tissues28,29. Moreover, Fusobacterium was enriched in OSCC biopsy compared to fibroepithelial polyp as a control13. Thus, distribution of bacteria including Fusobacterium in OSCC tissues may be distinct from that in healthy oral mucosal tissues. As shown in Fig. 2B, Fusobacterium can invade into OSCC cells. Previous report also shows that F. nucleatum adheres to and invades into human gingival epithelial cells (HGECs) and OSCC cells30. Interestingly, the spontaneous mutant of F. nucleatum isolated as defective in autoagglutination was unable to invade into HGECs and OSCC cells, suggesting the requirement for bacterial components to their invasion30. Moreover, glucose inhibition assay shows that lectin-like interactions are involved in the attachment of F. nucleatum to OSCC cells30. In the present study, both live and heat-inactivated F. nucleatum enhanced the invasion ability of OSCC cells via upregulation of p-EMT genes. Although some bacterial cells directly invaded into OSCC cells, most bacterial cells attached on the surface of the cells (Fig. 2B). Notably, heat-inactivated F. nucleatum as well as live F. nucleatum upregulated p-EMT-related genes and enhanced the invasive ability. These findings suggest that heat-resistant bacterial cell components may be involved in promoting invasion ability via upregulation of p-EMT genes. However, further experiments will be required for clarifying this mechanism.
In recent years, attention has been focused on the involvement of F. nucleatum in colorectal cancer8,9,31. In colon tissue of patients with colorectal cancer, increased amount of F. nucleatum was significantly detected, compared with healthy people32,33. Moreover, F. nucleatum colonies in primary colorectal cancer tissues were detected in metastatic liver tissues34. Thus, cumulative clinical evidence indicates that the enrichment of F. nucleatum may correlate with colorectal cancer metastasis32,34,35,36,37. Interestingly, the outer membrane proteins of F. nucleatum, Fusobacterium adhesion A (FadA) and Fibroblast activation protein 2 (Fap2) have been focused as a pathogen of colorectal cancer. FadA is required for bacterial attachment and invasion of gingival epithelial cells and endothelial cells30. FadA-mediated interaction with E-cadherin is involved in attachment and invasion into colorectal cancer cells8. Fap2 also plays a critical function in the development of colorectal cancer. Fap2 is involved in the inactivation of immune cells including T cells and NK cells via an immunoreceptor, TIGIT in colorectal cancer31. Moreover, Fusobacteria use a hematogenous route to reach colon adenocarcinomas via interaction between Fap2 and Gal-GalNAc9. We will examine the involvement of outer membrane proteins of F. nucleatum, FadA and Fap2 in the promotion of invasion via upregulation of p-EMT genes in OSCC cell with epithelial phenotype.
Recently, it has been shown that exposure of primary epithelial cell cultures to heat-inactivated F. nucleatum induces downregulation of E-cadherin and upregulation of N-cadherin, vimentin, Snail, matrix metalloproteinase-2 and toll-like receptor 4 (TLR-4) and promotes migration38. Another study shows that heat-inactivated F. nucleatum upregulates TLR-4 in oral keratinocyte39. TLR-4 is known to be responsible for recognition of LPS and activation of this pathway results in increased production of inflammatory cytokines40. Indeed, we showed that heat-inactivated F. nucleatum promoted invasion via upregulation of p-EMT genes in OSCC cells with epithelial phenotype. These findings suggest that F. nucleatum LPS may be involved in p-EMT and/or EMT induction via TLR signaling. Interestingly, previous studies show that LPS promotes EMT via activation of TLR4/JNK signaling41,42. Importantly, the effect of F. nucleatum on upregulation of the genes involved in invasion, survival, and EMT is comparable or greater than other periodontal bacteria, P. gingivalis, Treponema denticola, and Tannerella forsythia. In the present study, S. mutans, P. aeruginosa, and E. coli did not affect the expression of p-EMT-related genes. Interestingly, P. gingivalis, which is also known as periodontal pathogen, upregulated p-EMT genes in HOC621 cells (Fig. 8A). Cumulative evidences suggest that F. nucleatum and/or P. gingivalis among periodontal bacteria may have greater effects of promoting invasion, survival, and p-EMT/EMT during OSCC progression.
It is recognized that the ability of cancer cells to undergo p-EMT, rather than complete EMT, poses a higher metastatic risk16. Recent single cell transcriptome analysis in HNSCC identifies several genes involved in p-EMT program43. Among these p-EMT-related genes, we identified the prognosis-related genes, such as SERPINE1, TGFBI, ITGA5, CDH13, P4HA2, and LAMC218. Thus, p-EMT program is correlated with poor prognosis of HNSCC. Importantly, the enrichment of F. nucleatum is frequently observed in OSCC tissues compared to healthy oral mucosal tissues. Conversion from epithelial to p-EMT phenotype via alteration of gene expression by F. nucleatum infection may lead to increase a metastatic ability of OSCC (Fig. 8B). As F. nucleatum is well known oral commensal bacterium involved in periodontal diseases, oral hygiene managements for reducing the amount of F. nucleatum may contribute to reduce the risk for an increase in metastatic ability of OSCC.
References
Bray, F. et al. Global cancer statistics 2018: GLOBOCAN estimates of incidence and mortality worldwide for 36 cancers in 185 countries. CA Cancer J. Clin. 68, 394–424. https://doi.org/10.3322/caac.21492 (2018).
Anand, P. et al. Cancer is a preventable disease that requires major lifestyle changes. Pharm. Res. 25, 2097–2116. https://doi.org/10.1007/s11095-008-9661-9 (2008).
Irimie, A. I. et al. Current Insights into Oral Cancer Epigenetics. Int J Mol Sci 19, doi:https://doi.org/10.3390/ijms19030670 (2018).
Kuper, H., Adami, H. O. & Trichopoulos, D. Infections as a major preventable cause of human cancer. J. Intern. Med. 248, 171–183. https://doi.org/10.1046/j.1365-2796.2000.00742.x (2000).
Long, S. P., C.; Fischer, M. Principles and Practice of Pediatric Infectious Diseases, 5th Edition. 1015–1017 (Elsevier Inc, 2018).
Han, Y. W. et al. Fusobacterium nucleatum induces premature and term stillbirths in pregnant mice: Implication of oral bacteria in preterm birth. Infect. Immun. 72, 2272–2279. https://doi.org/10.1128/iai.72.4.2272-2279.2004 (2004).
Wang, X. et al. Comparative microbial analysis of paired amniotic fluid and cord blood from pregnancies complicated by preterm birth and early-onset neonatal sepsis. PLoS ONE 8, e56131. https://doi.org/10.1371/journal.pone.0056131 (2013).
Rubinstein, M. R. et al. Fusobacterium nucleatum promotes colorectal carcinogenesis by modulating E-cadherin/beta-catenin signaling via its FadA adhesin. Cell Host Microbe 14, 195–206. https://doi.org/10.1016/j.chom.2013.07.012 (2013).
Abed, J. et al. Fap2 mediates fusobacterium nucleatum colorectal adenocarcinoma enrichment by binding to tumor-expressed Gal-GalNAc. Cell Host Microbe 20, 215–225. https://doi.org/10.1016/j.chom.2016.07.006 (2016).
Yamamura, K. et al. Human microbiome fusobacterium nucleatum in esophageal cancer tissue is associated with prognosis. Clin. Cancer Res. 22, 5574–5581. https://doi.org/10.1158/1078-0432.Ccr-16-1786 (2016).
Parhi, L. et al. Breast cancer colonization by Fusobacterium nucleatum accelerates tumor growth and metastatic progression. Nat Commun 11, 3259. https://doi.org/10.1038/s41467-020-16967-2 (2020).
Al-Hebshi, N. N. et al. Inflammatory bacteriome featuring Fusobacterium nucleatum and Pseudomonas aeruginosa identified in association with oral squamous cell carcinoma. Sci. Rep. 7, 1834. https://doi.org/10.1038/s41598-017-02079-3 (2017).
Perera, M. et al. Inflammatory bacteriome and oral squamous cell carcinoma. J Dent Res 97, 725–732. https://doi.org/10.1177/0022034518767118 (2018).
Zhao, H. et al. Variations in oral microbiota associated with oral cancer. Sci Rep 7, 11773. https://doi.org/10.1038/s41598-017-11779-9 (2017).
Derynck, R. & Weinberg, R. A. EMT and cancer: More than meets the eye. Dev Cell 49, 313–316. https://doi.org/10.1016/j.devcel.2019.04.026 (2019).
Saitoh, M. Involvement of partial EMT in cancer progression. J. Biochem. 164, 257–264. https://doi.org/10.1093/jb/mvy047 (2018).
Pastushenko, I. et al. Identification of the tumour transition states occurring during EMT. Nature 556, 463–468. https://doi.org/10.1038/s41586-018-0040-3 (2018).
Kisoda, S. et al. Prognostic value of partial EMT-related genes in head and neck squamous cell carcinoma by a bioinformatic analysis. Oral Dis. https://doi.org/10.1111/odi.13351 (2020).
Yu, M. R., Kim, H. J. & Park, H. R. Fusobacterium nucleatum accelerates the progression of colitis-associated colorectal cancer by promoting EMT. Cancers (Basel). https://doi.org/10.3390/cancers12102728 (2020).
Harrandah, A. M., Chukkapalli, S. S., Bhattacharyya, I., Progulske-Fox, A. & Chan, E. K. L. Fusobacteria modulate oral carcinogenesis and promote cancer progression. J. Oral. Microbiol. 13, 1849493. https://doi.org/10.1080/20002297.2020.1849493 (2020).
Yokoyama, K. et al. Reverse correlation of E-cadherin and snail expression in oral squamous cell carcinoma cells in vitro. Oral Oncol. 37, 65–71. https://doi.org/10.1016/s1368-8375(00)00059-2 (2001).
Nguyen, P. T. et al. The FGFR1 inhibitor PD173074 induces mesenchymal–epithelial transition through the transcription factor AP-1. Br. J. Cancer 109, 2248–2258. https://doi.org/10.1038/bjc.2013.550 (2013).
Abiko, Y., Sato, T., Mayanagi, G. & Takahashi, N. Profiling of subgingival plaque biofilm microflora from periodontally healthy subjects and from subjects with periodontitis using quantitative real-time PCR. J. Periodontal Res. 45, 389–395. https://doi.org/10.1111/j.1600-0765.2009.01250.x (2010).
Preza, D. et al. Microarray analysis of the microflora of root caries in elderly. Eur. J. Clin. Microbiol. Infect. Dis. 28, 509–517. https://doi.org/10.1007/s10096-008-0662-8 (2009).
Zhang, L., Liu, Y., Zheng, H. J. & Zhang, C. P. The oral microbiota may have influence on oral cancer. Front. Cell. Infect. Microbiol. 9, 476. https://doi.org/10.3389/fcimb.2019.00476 (2020).
Kudo, Y. et al. Oral environment and cancer. Genes Environ. 38, 13. https://doi.org/10.1186/s41021-016-0042-z (2016).
Bolz, J., Dosa, E., Schubert, J. & Eckert, A. W. Bacterial colonization of microbial biofilms in oral squamous cell carcinoma. Clin. Oral Investig. 18, 409–414. https://doi.org/10.1007/s00784-013-1007-2 (2014).
Nagy, K. N., Sonkodi, I., Szoke, I., Nagy, E. & Newman, H. N. The microflora associated with human oral carcinomas. Oral Oncol. 34, 304–308 (1998).
Schmidt, B. L. et al. Changes in abundance of oral microbiota associated with oral cancer. PLoS ONE 9, e98741. https://doi.org/10.1371/journal.pone.0098741 (2014).
Han, Y. W. et al. Interactions between periodontal bacteria and human oral epithelial cells: Fusobacterium nucleatum adheres to and invades epithelial cells. Infect. Immun. 68, 3140–3146. https://doi.org/10.1128/Iai.68.6.3140-3146.2000 (2000).
Gur, C. et al. Binding of the Fap2 protein of Fusobacterium nucleatum to human inhibitory receptor TIGIT protects tumors from immune cell attack. Immunity 42, 344–355. https://doi.org/10.1016/j.immuni.2015.01.010 (2015).
Castellarin, M. et al. Fusobacterium nucleatum infection is prevalent in human colorectal carcinoma. Genome Res. 22, 299–306. https://doi.org/10.1101/gr.126516.111 (2012).
Kostic, A. D. et al. Genomic analysis identifies association of Fusobacterium with colorectal carcinoma. Genome Res. 22, 292–298. https://doi.org/10.1101/gr.126573.111 (2012).
Bullman, S. et al. Analysis of Fusobacterium persistence and antibiotic response in colorectal cancer. Science 358, 1443. https://doi.org/10.1126/science.aal5240 (2017).
Yang, Y. et al. Fusobacterium nucleatum increases proliferation of colorectal cancer cells and tumor development in mice by activating toll-like receptor 4 signaling to nuclear factor-kappab, and up-regulating expression of MicroRNA-21. Gastroenterology 152, 851–866 e824. https://doi.org/10.1053/j.gastro.2016.11.018 (2017).
Li, Y. Y. et al. Association of Fusobacterium nucleatum infection with colorectal cancer in Chinese patients. World J. Gastroenterol. 22, 3227–3233. https://doi.org/10.3748/wjg.v22.i11.3227 (2016).
Yan, X., Liu, L., Li, H., Qin, H. & Sun, Z. Clinical significance of Fusobacterium nucleatum, epithelial–mesenchymal transition, and cancer stem cell markers in stage III/IV colorectal cancer patients. Oncol. Targets Ther. 10, 5031–5046. https://doi.org/10.2147/OTT.S145949 (2017).
Abdulkareem, A. A., Shelton, R. M., Landini, G., Cooper, P. R. & Milward, M. R. Potential role of periodontal pathogens in compromising epithelial barrier function by inducing epithelial–mesenchymal transition. J. Periodontal Res. 53, 565–574. https://doi.org/10.1111/jre.12546 (2018).
Milward, M. R. et al. Differential activation of NF-kappaB and gene expression in oral epithelial cells by periodontal pathogens. Clin. Exp. Immunol. 148, 307–324. https://doi.org/10.1111/j.1365-2249.2007.03342.x (2007).
Lu, Y. C., Yeh, W. C. & Ohashi, P. S. LPS/TLR4 signal transduction pathway. Cytokine 42, 145–151. https://doi.org/10.1016/j.cyto.2008.01.006 (2008).
Li, H., Li, Y., Liu, D. & Liu, J. LPS promotes epithelial-mesenchymal transition and activation of TLR4/JNK signaling. Tumour Biol. 35, 10429–10435. https://doi.org/10.1007/s13277-014-2347-5 (2014).
Zhao, L. et al. LPS-induced epithelial–mesenchymal transition of intrahepatic biliary epithelial cells. J. Surg. Res. 171, 819–825. https://doi.org/10.1016/j.jss.2010.04.059 (2011).
Puram, S. V. et al. Single-cell transcriptomic analysis of primary and metastatic tumor ecosystems in head and neck cancer. Cell 171, 1611–1624 e1624, https://doi.org/10.1016/j.cell.2017.10.044 (2017).
Acknowledgements
Not applicable.
Funding
This work was supported in part by grants-in-aid from the Ministry of Education, Science and Culture of Japan [grant numbers 19H03853 and 19K19315].
Author information
Authors and Affiliations
Contributions
Y.K. conceived and designed the study. S.W., N.F., Y.M., S.K., K.Y., K.Y. and H.Y. performed the research and statistical analysis. K.O. and N.I. reviewed data and interpretation. N.F. and Y.K. drafted the paper. Y.K. and N.I. edited and revised the paper. All authors read and approved the final manuscript.
Corresponding author
Ethics declarations
Competing interests
The authors declare no competing interests.
Additional information
Publisher's note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if changes were made. The images or other third party material in this article are included in the article's Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article's Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
Shao, W., Fujiwara, N., Mouri, Y. et al. Conversion from epithelial to partial-EMT phenotype by Fusobacterium nucleatum infection promotes invasion of oral cancer cells. Sci Rep 11, 14943 (2021). https://doi.org/10.1038/s41598-021-94384-1
Received:
Accepted:
Published:
DOI: https://doi.org/10.1038/s41598-021-94384-1
- Springer Nature Limited
This article is cited by
-
MiR-455-5p suppresses PDZK1IP1 to promote the motility of oral squamous cell carcinoma and accelerate clinical cancer invasion by regulating partial epithelial-to-mesenchymal transition
Journal of Experimental & Clinical Cancer Research (2023)