Abstract
Human Vγ9Vδ2 T cells recognize pyrophosphates produced by microbes and transformed cells and play a role in anti-infective immunity and tumor surveillance. Toll-like receptors (TLR) are pattern recognition receptors in innate immune cells which sense microbial structures including nucleic acids. Given that γδ T cells are in clinical development for application in cellular cancer immunotherapy and TLR ligands have potent adjuvant activity, we investigated the co-stimulatory role of selected TLR ligands in γδ T-cell activation. Here we have used recently described RNA ligands for TLR7 and TLR8 together with Vγ9Vδ2 T-cell specific pyrophosphate antigens to analyze the rapid cytokine induction in Vδ2 T cells as well as the accessory cell requirements. While TLR8- as well as TLR7/8-specific RNA did not induce IFN-γ in Vδ2 T cells on their own, they provided strong co-stimulation for Vδ2 T cells within peripheral blood mononuclear cells in the presence of additional T-cell receptor activation. In contrast, TLR7 ligands were ineffective. Purified γδ T cells did not directly respond to TLR8 co-stimulation but required the presence of monocytes. Further experiments revealed a critical role of IL-1β and IL-18, and to a slightly lesser extent of IL-12p70, in the co-stimulation of Vδ2 T cells by TLR8 and TLR7/8 RNA ligands. Results of intracellular cytokine expression were validated by ELISA analysis of cytokines in cell culture supernatants. The cell context-dependent adjuvant activity of TLR8 and TLR7/8 RNA ligands described here might be important for the future optimization of γδ T-cell based cancer immunotherapy.
Similar content being viewed by others
Introduction
Approximately 2–5% of CD3+ T cells in the peripheral blood carry a γδ T-cell receptor (TCR) rather than the conventional αβ TCR. In the blood of adult donors, the majority of γδ T cells express Vγ9 paired with Vδ2, for simplicity referred to as Vδ2 throughout this study1,2. Vδ2 T cells recognize phosphorylated metabolites of isoprenoid biosynthesis required for cholesterol synthesis and protein prenylation. Such pyrophosphates, collectively termed phosphoantigens (pAg), are intermediates of the non-mevalonate pathway used by many bacteria and parasites, but are also generated in the eukaryotic mevalonate pathway. Microbial pAg such as (E)-4-Hydroxy-3-methyl-but-2-enyl pyrophosphate (HMBPP) stimulate human Vδ2 T cells at nanomolar concentrations, whereas micromolar concentrations of eukaryotic pAg like isopentenyl pyrophosphate (IPP) are required for activation of the very same Vδ2 T cells3,4. Activation of Vδ2 T cells by microbial or eukaryotic pAg requires the presence of butyrophilin (BTN) transmembrane molecules, specifically BTN3A1 and BTN2A15,6,7. Healthy cells produce insufficient amounts of the pAg IPP to activate γδ T cells. Many transformed cells, however, have a dysregulated mevalonate pathway leading to increased accumulation of IPP, which then triggers the activation of Vδ2 T cells8. As a consequence, many solid tumors and leukemias/lymphomas are recognized and killed by γδ T cells. Importantly, the sensitivity of tumor cells to lysis by Vδ2 T cells can be strongly increased by nitrogen-containing aminobisphosphonates like zoledronate which interfere with the mevalonate pathway leading to accumulation of IPP9. Zoledronate is also a potent and selective stimulus for Vδ2 T-cell expansion when added to peripheral blood mononuclear cells (PBMC), due to the zoledronate-triggered production of IPP in monocytes10. Given the additional advantage of their HLA-independence (i.e., application across HLA barriers is possible11), there is an increasing interest to apply γδ T cells in cancer immunotherapy12,13,14.
The activation and differentiation of γδ T cells is regulated by co-stimulatory signals and the cytokine milieu. While human γδ T cells have the capacity to acquire functional phenotypes resembling Th1, Th2, Th9, Th17 cells and others, ex vivo isolated Vδ2 T cells are usually prone to produce mainly interferon-γ (IFN-γ) and tumor necrosis factor-α (TNF-α)15,16,17. The effector activity of γδ T cells is modulated by innate immune cells like monocytes, macrophages and dendritic cells (DC) activated by multiple pattern recognition receptors. In this regard, Toll-like receptors (TLR) play a central role as sensors of microbial products, resulting in the context-dependent production of pro-inflammatory and anti-inflammatory cytokines, or type I interferons. Not surprisingly, γδ T-cell activation and differentiation is also modulated by TLR ligands18,19. γδ T cells themselves can express certain TLR, and direct effects of some TLR ligands on human and mouse γδ T-cell activation have been reported20,21,22,23.
We recently studied possible effects of TLR7 and TLR8 ligands on the activation of human Vδ2 T cells. Both TLR7 and TLR8 are endosomal receptors and recognize single-stranded microbial RNA as their natural ligand24. However, for both receptors non-RNA ligands mainly of the imidazoquinoline compound class have been described, such as Imiquimod (TLR7) and Resiquimod (TLR7/8)25. We observed that Resiquimod (but not Imiquimod) per se stimulated some IFN-γ production in Vδ2 T cells within the total population of PBMC, and co-stimulated IFN-γ production in response to the Vδ2 T-cell specific pAg HMBPP. At the same time, non-RNA TLR8 ligands like Resiquimod or Motolimod inhibited the proliferative expansion of Vδ2 T cells in the presence of monocytes26. Mechanistically, we found that a substantial proportion of monocytes died in response to the imidazoquinoline TLR ligands, thereby providing strong co-stimulation for γδ T-cell IFN-γ production but insufficient support for their cellular expansion26.
γδ T cells are considered to share features of innate and adaptive immunity. Due to their independence of antigen processing for TCR-mediated responsiveness, their activation is rapidly modulated by signals from innate immune cells. To investigate the modulation of γδ T-cell activation by TLR7 and TLR8 ligands more physiological than imidazoquinoline compounds, we made use of RNA ligands for TLR7 and TLR8 mimicking viral ssRNA27,28,29 to re-evaluate the role of these TLR in Vδ2 T-cell activation, with a focus on the role of monocytes and selected cytokines.
Materials and methods
Isolation of cell populations
Leukocyte concentrates of healthy adult blood donors were obtained from the Institute of Transfusion Medicine, University Hospital Schleswig–Holstein (Kiel, Germany). Written informed consent was obtained from all donors. The research was conducted in accordance with the Declaration of Helsinki and was approved by the relevant institutional review boards (ethic committee of the Medical Faculty of the University of Kiel, Germany; code number: D546/16). PBMC were isolated by Ficoll-Hypaque density gradient centrifugation. γδ T cells were purified from PBMC by positive magnetic selection using the anti-TCRγ/δ micro-Bead Kit from Miltenyi Biotec (Bergisch Gladbach, Germany) following the instructions of the company. To increase the purity of γδ T cells, two consecutive magnetic columns were applied. The purity of isolated γδ T cells was > 97%. Monocytes were isolated from PBMC by negative isolation using the Pan Monocyte Isolation Kit (Miltenyi Biotec) or the EasySep monocyte isolation kit (Stem Cell Technologies, Cologne, Germany) following the instructions of the companies. Negatively isolated monocytes contained > 92% CD14+ monocytes and < 0.2% contaminating CD3+ T cells as determined by flow cytometry.
Reagents
The following reagents were obtained from Invivogen (Toulouse, France): TL8-506 (TLR8 ligand), Resiquimod (TLR7/8 ligand), ssRNA40 (TLR8 RNA ligand), ssRNA41 (inactive control for ssRNA40), CU-CPT9a (TLR8 inhibitor)30, neutralizing anti-IL-1β antibody (mabg-hil1b-3), neutralizing anti-IL-18 antibody (mabg-hil18-3). Neutralizing anti-IL-12p70 antibody (MAB219) was purchased from R&D Systems (Bio-Techne, Wiesbaden, Germany). Human recombinant cytokines were obtained as follows: IL-1β and IL-12 were from ImmunoTools (Friesoythe, Germany), IL-18 from MBL (Biozol, Eching, Germany), IL-2 (Proleukin) was kindly provided by Novartis (Basel Switzerland). The TLR8 agonist Motolimod (VTX-2337) was purchased from Sellekchem (Houston, TX, USA). Phytohemagglutinin (PHA) was obtained from Sigma Aldrich (Schnelldorf, Germany). The Vγ9Vδ2-selective pAg (E)-4-Hydroxy-3-methyl-but-2-enyl pyrophosphate (HMBPP) was purchased from Echelon Biosciences (Salt Lake City, UT, USA). The following RNA ligands for TLR 7 and TLR8 have been previously described27,28,29 and were synthesized by Biomers.net (Ulm, Germany): R805 (TLR7), R2152 and R2196 (TLR8), 9.2s (TLR7/8), polyCA (negative inert control RNA). RNA ligands were complexed with low MW poly-arginine (pArg; Sigma Aldrich) before adding to cell cultures. In control experiments, the maximal final concentration of pArg (2 µg/mL) did not exert any effect on γδ T-cell activation. Transfectants expressing TLR7 (HEK-blue-hTLR7; hkb-htlr7), TLR8 (HEK-blue-hTLR8; hkb-htlr8) were obtained from Invivogen.
Cell cultures
PBMC (4 × 105 per well) or purified γδ T cells (0.5–1 × 105 per well) with or without purified monocytes (1 × 105 per well) were cultured in wells of 96-well round bottom microtiter plates (Nunc; Thermo Fisher Scientific, Waldham, MA, USA). Complete culture medium was RPMI 1640 (Thermo Fisher Scientific) supplemented with antibiotics (100 U/mL penicillin, 100 µg/mL streptomycin) and 10% of heat-inactivated low endotoxin fetal bovine serum (Bio&Sell, Feucht, Germany). Where indicated, cell cultures were supplemented with 10 ng/mL of IL-1β, 10 ng/mL of IL-12, 20 ng/mL of IL-18, or 5 µg/mL of neutralizing anti-cytokine antibodies. Vγ9Vδ2 T-cell lines were established from PBMC containing 2–3% CD3+Vδ2+ γδ T cells as described31. Briefly, PBMC were stimulated with 2.5 μM zoledronate (Novartis) and 50 IU/mL IL-2. IL-2 was added every other day, and cultures were split on day 7 and day 9. After 12 days, such γδ T-cell lines contained > 90% CD3+Vδ2+ γδ T cells. γδ T-cell lines were seeded at 2 × 105 cells per well in complete medium supplemented with 10 IU/mL IL-2. Cell cultures were stimulated or not with TLR ligands in the absence or additional presence of 1 nM HMBPP, and were incubated for 24 h at 370C in a humidified atmosphere of 5% CO2 in air. For measurement of intracellular cytokines, 3 μM monensin was added during the last 4 h to prevent cytokine secretion.
Flow cytometry
The following mAb were obtained from BD Biosciences (Heidelberg, Germany): anti-CD3-PE/APC/BV605 (clone SK7), anti-CD14-FITC/APC (clone MoP9), anti-IFN-γ-PE or -PE/Cy7 (clone 4S.B3), anti-Granzyme B-PE-CF954 (clone GB11), anti-TNF-α-PE (clone MAb 11). Anti-Vδ2-FITC (clone IMMU389) was obtained from Beckman Coulter (Krefeld, Germany), anti-hTLR7-PE and anti-hTLR8-AF647 were purchased from R&D Systems. For cell surface staining, cells were washed, stained for 20 min on ice with mAb, washed twice, and resuspended in 1% paraformaldehyde. For intracellular staining, cells were permeabilized in Cytofix/Cytoperm buffer (BD Biosciences) before staining with fluorochrome-conjugated mAb. Final antibody concentrations were used according to respective data sheets. All analyses were measured on a FACS Calibur or LSR Fortessa cytometer (BD Biosciences), using the software CellQuest Pro and DIVA (Data-Interpolating Variational Analysis) for acquisition respectively, and FlowJo v10.6.1 software for data analysis.
Quantification of cytokines in cell culture supernatants
IFN-γ and Granzyme-B (GrB) in cell culture supernatants were quantified using Human IFN-γ (DY285B) or GrB (DY2906) DuoSet ELISA kits from R&D Systems, following the instructions of the company. Cytokines including TNF-α, IL-1β, IL-12p70 and IL-18 were measured by Luminex Multiplex assay (R&D Systems) according to the instructions of the company.
Statistical analysis
Statistical comparisons were made between groups using one-or two-way ANOVA analysis and Dunnett´s multiple comparison test against respective internal controls. All analyses were done with the Graphpad Prism 8 software. Levels of significance were set as * p < 0.05, ** p < 0.01, *** p < 0.001, and **** p < 0.0001.
Results
Expression of TLR7 and TLR8
We analyzed expression patterns of TLR7 and TLR8 by flow cytometry in peripheral blood leukocyte subsets, i.e. monocytes, γδ T cells, neutrophils as well as NK cells. For comparison, we used HEK cells stably transfected with TLR7 or TLR8, respectively. As shown in a representative experiment (Suppl. Fig. S1), TLR7 was weakly expressed, with monocytes and neutrophils expressing slightly higher levels than γδ T cells and NK cells. TLR8 was detected in monocytes, neutrophils and NK cells, in line with published studies on the functional expression of TLR8 in these cells32,33,34,35,36. In this donor, γδ T cells expressed very low levels of TLR8 as determined by Δ MFI (MFI TLR8 minus MFI isotype control). A summary of several experiments performed with different healthy blood donors is presented for TLR7 in Fig. 1a and for TLR8 in Fig. 1b. Here, MFI of isotype controls have not been subtracted. Overall, monocytes expressed same levels of TLR8 like the HEK-TLR8 transfectants, and both expressed significantly higher levels of TLR8 in comparison to other analyzed immune cell populations.
Expression of TLR7 and TLR8 in immune cells. Purified monocytes, γδ T cells, neutrophils and NK cells, as well as TLR7- and TLR8-transfected HEK cells were stained for intracellular analysis of TLR7 and TLR8 expression. Results are depicted as mean ± SD of median fluorescence intensity (MFI) of specific antibody staining of three to seven experiments with different healthy blood donors. (a) TLR7, (b) TLR8. Statistical significance is indicated with * p < 0.05, ** p < 0.01, **** p < 0.0001. ns, not significant.
Co-stimulatory activity of TLR8 and TLR7/8 but not TLR7 RNA ligands
PBMC were activated with various TLR subset-specific RNA ligands and for comparison with well characterized non-RNA small molecule ligands, in the absence or presence of the Vγ9Vδ2 T-cell specific phosphoantigen HMBPP for simultaneous TCR activation. After 24 h, intracellular expression of IFN-γ was analyzed by flow cytometry with a gate set on Vδ2 T cells. Results presented in Suppl. Fig. S2 indicate that neither TLR7-specifc RNA pG805 (as well as the inactive control RNA pCA37) nor TLR7-specific imidazoquinoline ligand Imiquimod had any co-stimulatory activity (TLR ligands without HMBPP: gray histograms; TLR ligands together with HMBPP: open histograms). In contrast, non-RNA TLR8 ligands TL8-506 and Motolimod significantly enhanced the weak HMBPP-induced IFN-γ expression (Suppl. Fig. S3). Two different TLR8-specific RNA ligands (ssRNA40, R2152) strongly co-stimulated the HMBPP-induced IFN-γ expression, as did the TLR7/8-specific RNA 9.2s, while a third TLR8-specific RNA (R2196) was less active (Suppl. Fig. S3). The well-established imidazoquinoline TLR7/8 agonist Resiquimod was less active when compared to 9.2s, mainly due to different kinetics (see below). Overall, TLR8 RNA ligands strongly enhanced IFN-γ in Vδ2 T cells in the presence of the TCR stimulus HMBPP but showed only weak activity and only at higher concentrations (2–4 µg/mL) in the absence of HMBPP (compare gray histograms in Suppl. Fig. S3). Based on the dose titrations presented, we selected optimal concentrations for subsequent experiments (4 μg/mL R2152 and 9.2s, 2 μg/mL ssRNA40 and Resiquimod).
Next, we performed time course studies to follow the co-stimulatory effect of TLR8 ligands over time. In these experiments, PBMC were cultured for 6 and 24 h in the presence or absence of TLR ligands and HMBPP, and intracellular IFN-γ expression was measured within Vδ2 γδ T cells (Fig. 2a) and within CD3-negative cells in the lymphocyte gate (Fig. 2b). Figure 2a illustrates that Resiquimod exerted higher co-stimulation on HMBPP-activated γδ T cells at the earlier time point when compared to 24 h, whereas all three TLR8 and TLR7/8 RNA ligands were much more active at 24 h. In line with published reports34,38, we also observed IFN-γ expression induced by TLR ligands only (i.e., in the absence of HMBPP) within CD3-negative lymphocytes, most likely NK cells (Fig. 2b). The potent co-stimulatory activity of TLR8 RNA ligands on the IFN-γ induction in Vδ2 T cells within PBMC activated for 24 h with HMBPP was validated in a total of eight donors (Fig. 2c). Moreover, the co-stimulatory effect of the TLR ligands was clearly dependent on TLR8, as shown by the effect of the selective inhibitor CU-CPT9a30 at both 6 and 24 h of activation (Fig. 3).
Kinetics of IFN-γ induction in γδ T cells and CD3-negative lymphocytes. PBMC were cultured in the presence or absence of 1 nM HMBPP and the indicated TLR ligands. After 6 and 24 h, the intracellular expression of IFN-γ was analyzed with a gate set on (a) CD3+Vδ2+ γδ T cells, or (b) CD3-negative lymphocytes (i.e., mainly NK cells). Representative histograms are shown in (a) and (b). A summary of eight experiments is presented in (c). Results are expressed as mean fluorescence intensity (MFI) ± SD. Statistical significance is indicated with * p < 0.05, ** p < 0.01.
Co-stimulation by RNA ligands is TLR8-dependent. PBMC were activated with HMBPP in the presence or absence of TLR8 ligands and additional presence or absence of 10 µM TLR8 inhibitor CU-CPT9a. Intracellular expression of IFN-γ in CD3+Vδ2+ γδ T cells was analyzed after 6 (upper panel) and 24 h (lower panel). Gray histograms: without CU-CPT9a, open histograms: with CU-CPT9a. One out of two experiments with similar results is shown.
Role of endogenous cytokines
In the experiments presented so far, we described the co-stimulatory effect of TLR8 RNA ligands on the IFN-γ induction in Vδ2 T cells within PBMC stimulated with the pAg HMBPP. Monocytes comprise a substantial proportion of PBMC and are known to express TLR8 (Fig. 1) and to produce a range of cytokines in response to TLR8 activation, some of which are important regulators of T-cell differentiation28,32,33,34,38,39. In the context of γδ T-cell activation, IL-1β, IL-12p70 and IL-18 are of particular interest. IL-1β has multiple effects in early T-cell activation40, and IL-18 is a crucial factor in the regulation of IFN-γ induction41. IL-12p70 on the other hand is a key cytokine in the differentiation of Th1 T cells32 which is the primary differentiation pathway of ex vivo isolated human γδ T cells42. We have previously reported that monocytes secrete IL-1β in response to TLR8 ligands ssRNA40 and Resiquimod26. Together with IL-1β and TNF-α, we also detected IL-12p70 and IL-18 in the supernatants of purified monocytes activated by TLR8 RNA ligand ssRNA40 (as well as by Resiquimod) (Supplemental Table 1).To address the potential contribution of these cytokines, we added neutralizing antibodies against IL-1β, IL-18 and IL-12p70 to PBMC activated with HMBPP in the absence or presence of TLR8 ligands. Again, the intracellular cytokine expression in Vδ2 T cells was measured after 24 h. In addition to IFN-γ we also analyzed Granzyme B (GrB) which is a major effector molecule of cytotoxic γδ T cells43. Results of a representative experiment are depicted in Fig. 4a (IFN-γ) and Fig. 4c (GrB). The expression of the cytokines in the absence of added antibodies (control) is shown in the lowest histogram for both cytokines. As before, there was a clear costimulatory effect on IFN-γ and GrB induction by TLR8 ligands R2152 and ssRNA40, and by TLR7/8 ligand 9.2s, but not by the inactive control ssRNA41 (Fig. 4a,c). In contrast to IFN-γ (and TNF-α; not shown), a major proportion of Vδ2 T cells already expressed GrB in the absence of added TLR8 ligands, but the active ligands (and not the inactive control ssRNA41) clearly further co-stimulated GrB expression (Fig. 4c). The addition of neutralizing anti-cytokine antibodies reduced (anti-IL-12p70) or abolished (anti-IL-1β, anti-IL-18) the co-stimulatory effect of TLR8 RNA ligands on IFN-γ (Fig. 4a) and TNF-α (not shown) production. While the HMBPP-induced GrB expression in Vδ2 T cells (“Medium” in Fig. 4c) was not affected by anti-cytokine antibodies, the additional co-stimulatory effect of the TLR8 ligands was also abolished, most notably with anti-IL-1β. A summary of four experiments displaying the mean fluorescence intensity (MFI) and statistical analysis is shown for IFN-γ in Fig. 4b and for GrB in Fig. 4d. Note that MFI is displayed on a logarithmic scale, and the effect of all three anti-cytokine antibodies was highly significant (p < 0.0001) for IFN-γ. Taken together, these results indicate that all three cytokines contribute to the co-stimulation of cytokine induction in Vδ2 T cells by TLR8 RNA ligands within PBMC.
Modulation of cytokine induction in Vδ2 T cells by anti-cytokine antibodies. PBMC were activated with HMBPP in the presence or absence of TLR8 ligands and additional presence or absence of 5 µg/mL of neutralizing anti-cytokine antibodies as indicated. Intracellular expression of IFN-γ (a,b) and GrB (c,d) in CD3+Vδ2+ γδ T cells was analyzed after 24 h. The lower histograms in each panel of (a) and (c) show the upregulated cytokine expression in the absence of anti-cytokine antibodies (“controls”). (a), (c) representative histograms; (b), (d) Summary of four experiments. Results are expressed as mean fluorescence intensity on a logarithmic scale (MFI) ± SD. Statistical significance is indicated with * p < 0.05, ** p < 0.01, *** p < 0.001, **** p < 0.0001. ns, not significant.
Purified γδ T cells require monocytes for co-stimulation by TLR8 RNA ligands
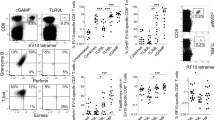
Next, we investigated the potential responsiveness of freshly isolated γδ T cells to co-stimulation with TLR8 RNAs. To this end, γδ T cells were purified by magnetic MACS sorting and stimulated for 24 h with HMBPP in the absence or presence of TLR8 ligands and recombinant cytokines IL-1β, IL-12p70, or IL-18. Under these conditions, no substantial induction of IFN-γ (Fig. 5a) or TNF-α (not shown) was observed, except for IL-18 which had a minor effect on IFN-γ induction, which was not further increased by the additional presence of IL-1β (Fig. 5a, top histograms). Again, high expression of GrB was also detected in the purified γδ T cells, which however was neither modulated by TLR8 ligands nor by the added cytokines (Fig. 5b). Together, these results indicate that purified γδ T cells are not directly co-stimulated by TLR8 RNA ligands, in line with the low TLR8 expression detected by flow cytometry. However, when monocytes isolated by negative MACS selection were added back, the co-stimulatory effect of R2152, ssRNA40 and 9.2s was restored as shown in the “control” histograms of a representative experiment in Fig. 5c. The co-stimulatory function of monocytes is at least partly due to TLR8-induced secretion of IL-1β, IL-18 or IL-12p70 as suggested by the blocking effect of the respective neutralizing antibodies (Fig. 5c). IL-18 is a key factor for IFN-γ induction41 (in fact it has been initially described as “γ-Interferon-inducing factor”). While the data in Fig. 5a indicated that IL-18 does not directly affect IFN-γ induction in isolated γδ T cells, it might still do so in a broader cellular context. To address this question, we analyzed IFN-γ expression in Vδ2 T cells within PBMC depleted of CD14+ monocytes and activated by HMBPP in the absence or presence of TLR8 ligands. The results shown in Fig. 5d indicate that the exogenous supply of IL-18 (and to a lesser extent of IL-12) indeed co-stimulated IFN-γ in HMBPP-activated γδ T cells, whereas the TLR8 ligands did not exert such co-stimulatory activity, due to the absence of monocytes in the CD14-depleted PBMC cultures. To corroborate the results obtained by intracellular flow cytometry, we measured the release of secreted cytokines IFN-γ and GrB in cell culture supernatants by ELISA. In these experiments, we compared PBMC, purified γδ T cells, and purified γδ T cells reconstituted with purified monocytes, each stimulated with TLR8 ligands only or with additional HMBPP activation. The results of three to four independent experiments are presented in Fig. 6. In PBMC, the active ligands R2152, ssRNA40 and 9.2s strongly induced IFN-γ (Fig. 6a) and GrB (Fig. 6b), both in the absence (gray columns) and in the presence (open columns) of HMBPP. The potent IFN-γ and GrB secretion in PBMC in the absence of HMBPP is most likely due to the activation of NK cells which are known producers of both cytokines, and are activated in a monocyte-dependent manner by TLR8 RNA ligands34,38. In line with the intracellular FACS analysis, isolated γδ T cells did neither secrete IFN-γ nor GrB. Only in the presence of monocytes in combination with the TCR stimulus HMBPP was a significant enhancing effect of active TLR8 RNAs on IFN-γ production observed, while Resiquimod showed little effect (Fig. 6a). Similarly, GrB secretion in γδ T cells was restored when monocytes were added back. Again, co-stimulation by R2152, ssRNA40 and 9.2s was observed in the additional presence of HMBPP. Baseline secretion of GrB (in the absence of HMBPP) was not enhanced by TLR8 ligands (Fig. 6b).
Role of monocytes in co-stimulation of γδ T cells by TLR8 ligands. 100.000 purified γδ T cells alone (a,b), or together with 100.000 purified monocytes (c), or 400.000 CD14-depleted PBMC (d) were activated with HMBPP in the presence or absence of TLR8 ligands as indicated. Recombinant cytokines IL-1β (10 ng/mL), IL-12 (10 ng/mL), IL-18 (20 ng/mL (a,b,d) or 5 µg/mL of neutralizing anti-cytokine antibodies (c) were added as indicated. Intracellular expression of IFN-γ (a,c,d) and GrB (b) in CD3+Vδ2+ γδ T cells was analyzed after 24 h. The lower histograms in each panel show the IFN-γ/GrB expression in the absence of added cytokines (a,b,d) or anti-cytokine antibodies (c). Histograms of one representative out of five (a,b,c) or two (d) experiments are shown.
Co-stimulation of purified γδ T cells by TLR8 RNA ligands requires monocytes and TCR activation. 400.000 PBMC, 100.000 purified γδ T cells, and 100.000 purified γδ T cells reconstituted with 100.000 monocytes, were cultured in the absence (gray columns) or presence of HMBPP (open columns) and the absence or additional presence of TLR8 ligands. After 24 h, cell culture supernatants were collected and analyzed by ELISA for IFN-γ (a) and GrB (b). All ELISAs were performed on two independent replicates in each experiment. Mean ± SD of three to four independent experiments are shown. Statistical significance is indicated with * p < 0.05, ** p < 0.01, *** p < 0.001.
The presented results indicate that freshly isolated γδ T cells are not directly co-stimulated by active TLR8 RNA ligands but require the additional presence of monocytes. Next, we asked whether pre-activated (in contrast to resting) γδ T cells might perhaps directly respond to TLR8 ligand co-stimulation. To this end, we analyzed short-term Vδ2 γδ T-cell lines which had been generated by initial stimulation with zoledronate and repeated exposure to IL-2. In comparison to circulating freshly isolated γδ T cells, expanded γδ T-cell lines expressed higher levels of TLR8 (Fig. 7a). γδ T-cell lines were then cultured for 24 h in the absence or presence of R2152 or 9.2s and without or with additional HMBPP. As shown in Fig. 7b, the RNA ligands did not induce IFN-γ secretion on their own. In the presence of HMBPP, the γδ T-cell lines secreted IFN-γ, but again the levels were not significantly modulated by the TLR8 RNA ligands.
Lack of direct co-stimulation of activated γδ T cells by TLR8 RNA ligands. Short-term expanded γδ T-cell lines were generated by stimulation of PBMC with zoledronate and IL-2 and repeated addition of IL-2. After 14 days, γδ T-cell lines comprised > 94% CD3+Vδ2+ T cells. (a) Intracellular TLR8 expression (open histogram), isotype control (shaded histogram). (b) Expanded γδ T cells were cultured for 24 h in the absence or presence of 1 nM HMBPP and TLR8 RNAs R2152 or 9.2s as indicated. IFN-γ in cell culture supernatants was quantified by ELISA. All ELISAs were performed on two independent replicates in each experiment. Mean ± SD of six independent experiments are shown. Statistical significance is indicated with *** p < 0.001. ns, not significant.
Discussion
The endosomal TLR7 and TLR8 which are mainly expressed in innate immune cells, are well characterized sensors of single-stranded viral and bacterial RNA. While the functional expression of TLR8 in monocytes is undisputed28,32,38, the functional expression of TLR7 is less clear28. In fact, functional TLR7 expression was more attributed to plasmacytoid DC (pDC) rather than monocytes28. However, more recent studies also indicate that TLR7 and TLR8 activate distinct pathways in monocytes during RNA virus infection, supporting a concept of ligand-specific regulation36. In addition to synthetic small molecules like Motolimod (VTX-2337), TL8-506, or Resiquimod, TLR8 specifically senses viral, bacterial, parasite (e.g., Plasmodium falciparum) and related synthetic RNA sequences34,39,44. Recently, it was discovered that TLR8 actually recognizes degradation products resulting from processing of natural or synthetic RNA molecules by endolysosomal endoribonucleases RNase T2 and RNase 229,45. In view of their strong adjuvant-like activation of the innate immune arm, TLR7/8 ligands are in clinical studies mainly for oncological indications46. As such, TLR and other pattern recognition receptor ligands might be also valuable tools to enhance the efficacy of γδ T-cell cancer immunotherapy. Multiple approaches of γδ T-cell application in cancer immunotherapy are in development including adoptive transfer of in vitro expanded γδ T cells as well as selective in vivo activation of γδ T cells by antibodies or bispecific γδ T-cell engagers12,13,14,47. Most strategies will require additional adjuvants to counteract the immunosuppressive tumor micromilieu and/or to enhance the entry of immune cells including γδ T cells into cold tumors48. Along this line, it is important to explore the co-stimulation of γδ T cells by defined TLR ligands.
In this study, we used the rapid cytokine induction as a read-out to define the co-stimulatory activity of TLR7 and TLR8 RNA ligands. Previous studies have shown that ligands for TLR3, TLR4 and TLR9 co-stimulate IFN-γ induction in Vδ2 T cells within the PBMC in a monocyte- or immature DC-dependent manner49,50,51. Short-term expanded Vδ2 T cells were also found to directly respond to TLR2 ligand co-stimulation52, and we have previously reported direct co-stimulation of purified γδ T cells by TLR2 ligands Pam2CSK4 and FSL-1 and upregulation of TLR2 following TCR activation53. We also reported co-stimulation of γδ T cells by TLR3 ligand poly(I:C), in agreement with the detectable TLR3 expression in freshly isolated human γδ T cells20,21. We now observed a potent co-stimulatory activity of TLR8 RNA ssRNA40 and R215229 as well as TLR7/8-specific RNA 9.2s27,28 on IFN-γ expression in Vδ2 T cells within PBMC stimulated with the pAg HMBPP. Interestingly, both the time course kinetics and the intensity of co-stimulation differed between the well characterized non-RNA TLR7/8 ligand Resiquimod and RNA ligands. The increased intracellular IFN-γ expression of HMBPP-activated γδ T cells in the presence of Resiquimod was already evident after 6 h and less obvious after 24 h, whereas the strong co-stimulatory activity of RNA ligands occurred after 24 h (Fig. 2a). The more potent activity of RNA ligands in comparison to Resiquimod also resulted in much higher levels of secreted IFN-γ and GrB measured in cell culture supernatants (Fig. 6). While the molecular explanation for the stronger co-stimulatory activity of TLR8 RNA ligands in comparison to Resiquimod requires further investigation, our results suggest that RNA ligands might be more suitable to boost γδ T-cell activation also in vivo. In contrast, TLR7-specific RNA as well as other established TLR7 ligands like Imiquimod did not have such co-stimulatory activity. However, TLR7 ligands might still modulate γδ T cell effector functions through alternative pathways, for instance by increasing the susceptibility of tumor cells to γδ T-cell mediated lysis54. In line with published data34,38, we also noticed activation of CD3-negative cells (most likely NK cells) in PBMC within the lymphocyte gate by TLR8 RNA ligands (Fig. 2b). In view of the known accessory cell dependency of TLR co-stimulation in other systems and the potent cytokine induction in monocytes by TLR8 ligands28,32,34,36,38,49,51, we also assumed indirect (i.e., accessory cell dependent) activation of Vδ2 T cells by TLR8 RNA ligands. This is supported by the very weak TLR8 (and TLR7) expression as determined by flow cytometry in γδ T cells when compared to monocytes. Furthermore, TLR8 RNA ligands did not co-stimulate cytokine expression in purified γδ T cells, neither in the absence (not shown) nor in the presence of TCR stimulation with HMBPP. While monocytes can produce in a stimulus-dependent manner a large variety of cytokines including TNF-α, CCL3/MIP-1α and type I interferon, we focused our attention on the important monocyte cytokines IL-1β, IL-12 and IL-18. Using neutralizing antibodies, we showed that each of these cytokines contributes to the co-stimulation of cytokine-producing Vδ2 T cells within the total PBMC population, although with slightly different potency. Considering IFN-γ, there was no statistical difference between the inhibitory effect of the anti-cytokine antibodies, even though anti-IL-12p70 was slightly less active (Fig. 4b). In the case of GrB, the inhibitory effect of anti-IL-12p70 was less significant compared to anti-IL-1β and anti-IL-18 when RNA ligands R2152 or 9.2s were used for activation (Fig. 4d). Interestingly, however, none of the three cytokines could restore the co-stimulatory effect of TLR8 RNA ligands when purified γδ T cells were activated with HMBPP, neither for IFN-γ (Fig. 5a) nor for TNF-α (not shown). Only in the case when purified γδ T cells were reconstituted with purified monocytes did we observe again the co-stimulatory activity of TLR8 RNA ligands (Fig. 5c). These results clearly demonstrate that cytokine induction in isolated Vδ2 γδ T cells cannot be elicited in the absence of monocytes (or perhaps other accessory cells like immature DC); neither HMBPP alone, nor the additional presence of TLR8 RNA ligands and/or IL-1β, IL-12 or IL-18 was able to significantly induce IFN-γ or TNF-α expression in purified Vδ2 T cells. Further experiments were designed to obtain more insight into the role of exogenous cytokines in the TLR8 RNA ligand co-stimulation. To this end, we analyzed IFN-γ induction in Vδ2 T cells within CD14 (i.e. monocyte-)-depleted PBMC. In contrast to purified γδ T cells reconstituted with monocytes, the CD14-depleted PBMC contain γδ T cells and cells other than monocytes (e.g., CD4+ T cells) which can also “present” HMBPP and thereby activate γδ T cells in the presence of cytokines like IL-1855. In this setting, we found that indeed exogenous IL-18 (and to a lesser extent IL-12) can co-stimulate IFN-γ expression in HMBPP-activated Vδ2 T cells, in the absence of TLR8 ligand co-stimulation (due to the lack of monocytes) (Fig. 5d). These results confirm that IL-18 and to a lesser extent IL-12 are important regulators of γδ T-cell activation and proliferation56,57 but underscore the requirement of additional activation signals.
Constitutive expression of perforin and serine proteases like GrB in circulating γδ T cells is well documented58. GrB and additional cytotoxic effector proteins including granulysin are important mediators of the effector function of Vδ2 γδ T cells to lyse Plasmodium falciparum parasites and tumor cells59,60,61. Importantly, Plasmodium falciparum parasites produce pAg which activate Vδ2 T cells62. Since RNA from Plasmodium falciparum-infected erythrocytes can activate TLR834, the infection with Plasmodium falciparum parasites reflects a pathological condition where the results of our current in vitro studies might be directly relevant in vivo. As expected, we noticed strong expression of GrB in Vδ2 T cells both when analyzed within the PBMC or in isolated γδ T cells. Nevertheless, the active TLR8 RNA ligands further increased GrB expression in Vδ2 T cells within HMBPP-activated PBMC but again not in purified γδ T cells (Figs. 5,6). Interestingly, the additional co-stimulatory effect by TLR8 RNA ligands, but not the constitutive GrB expression, was abolished by neutralizing anti-IL-1β antibody (Fig. 4c,d). Like IFN-γ, GrB was secreted into cell culture supernatants when PBMC were activated only by TLR8 RNA ligands. This was also observed with purified γδ T cells reconstituted with monocytes, however at much lower levels. Taking together our results from intracellular flow cytometry and detection of secreted cytokines in culture supernatants, we conclude that TLR8 RNA ligands induce IFN-γ and GrB production within PBMC in NK cells (in a monocyte-dependent manner34,38) with additional contribution of γδ T cells as suggested by the increased release in the presence of HMBPP. Furthermore, purified γδ T cells require TCR activation (in our experiments by HMBPP) and the additional presence of monocytes to become sensitive to the potent co-stimulatory activity of TLR8 RNA ligands.
In contrast to the lack of direct effects on γδ T cells reported here, TLR8 ligands might exert direct co-stimulatory activity on other T-cell populations such as CD4 T cells or regulatory T cells (Treg). While the reported TLR8 expression in CD4 T cells is inconsistent63,64,65, a recent study provided clear evidence for a direct co-stimulatory activity of various TLR8 ligands on purified human CD4 T cells65. Moreover, since TLR8 ligation has been shown to revert the suppressive activity of Treg64, we have to consider that TLR8 ligands (and presumably ligands for other pattern recognition receptors as well) may modulate T-cell subsets differentially and in a microenvironment context-specific manner. Taken together, there is no doubt that TLR8 RNA ligands are highly potent co-activators of various immune cells, but the requirement of accessory cells (e.g., monocytes), additional activation signals (e.g., TCR stimulation) and specific cytokines (e.g., IL-1β, IL-18, IL-12p70) may vary between the analyzed immune cell populations (e.g., γδ T cells versus NK cells).
TLR ligands are in the focus of interest as adjuvants in vaccine development and cancer therapy46,66,67. Currently, the website https://www.clinicaltrials.gov/ lists only clinical studies with non-RNA TLR7 and/or TLR8 ligands. However, there is strong evidence that RNA ligands are potent activators of innate immunity and in consequence co-stimulators of adaptive immunity as well. At the translational level, it may require optimization of pharmacological formulation for optimal delivery of such ligands e.g. to the tumor microenvironment. The results of our present study clearly indicate that TLR8 RNA ligands provide potent co-stimulation to human γδ T cells. In view of the raising attention to bring γδ T cells into clinical application14, we expect that our findings will help to improve the efficacy of γδ T-cell based cancer immunotherapy.
Abbreviations
- BTN:
-
Butyrophilin
- GrB:
-
Granzyme B
- HMBPP:
-
(E)-4-Hydroxy-3-methyl-but-2-enyl pyrophosphate
- IFN-γ:
-
Interferon-γ
- pAg:
-
Phosphoantigen
- PBMC:
-
Peripheral blood mononuclear cells
- TCR:
-
T-cell receptor
- TLR:
-
Toll-like receptor(s)
- TNF-α:
-
Tumor necrosis factor-α
References
Vantourout, P. & Hayday, A. Six-of-the-best: unique contributions of gammadelta T cells to immunology. Nat. Rev. Immunol. 13, 88–100 (2013).
Hinz, T. et al. Identification of the complete expressed human TCR V gamma repertoire by flow cytometry. Int. Immunol. 9, 1065–1072 (1997).
Morita, C. T. et al. Structural features of nonpeptide prenyl pyrophosphates that determine their antigenicity for human gamma delta T cells. J. Immunol. 167, 36–41 (2001).
Hintz, M. et al. Identification of (E)-4-hydroxy-3-methyl-but-2-enyl pyrophosphate as a major activator for human gammadelta T cells in Escherichia coli. FEBS Lett. 509, 317–322 (2001).
Harly, C. et al. Key implication of CD277/butyrophilin-3 (BTN3A) in cellular stress sensing by a major human γδ T-cell subset. Blood 120, 2269–2279 (2012).
Rigau, M. et al. Butyrophilin 2A1 is essential for phosphoantigen reactivity by γδ T cells. Science 367, 5516 (2020).
Karunakaran, M. M. et al. Butyrophilin-2A1 directly binds germline-encoded regions of the Vγ9Vδ2 TCR and is essential for phosphoantigen sensing. Immunity 52, 487–498 (2020).
Gruenbacher, G. & Thurnher, M. Mevalonate metabolism in immuno-oncology. Front. Immunol. 8, 1714 (2017).
Gober, H. J. et al. Human T cell receptor gammadelta cells recognize endogenous mevalonate metabolites in tumor cells. J. Exp. Med. 197, 163–168 (2003).
Roelofs, A. J. et al. Peripheral blood monocytes are responsible for gammadelta T cell activation induced by zoledronic acid through accumulation of IPP/DMAPP. Br. J. Haematol. 144, 245–250 (2009).
Xu, Y. et al. Allogeneic Vγ9Vδ2 T-cell immunotherapy exhibits promising clinical safety and prolongs the survival of patients with late-stage lung or liver cancer. Cell. Mol. Immunol. 18, 427–439 (2021).
Silva-Santos, B., Mensurado, S. & Coffelt, S. B. γδ T cells: pleiotropic immune effectors with therapeutic potential in cancer. Nat. Rev. Cancer. 19, 392–404 (2019).
Sebestyen, Z., Prinz, I., Déchanet-Merville, J., Silva-Santos, B. & Kuball, J. Translating gammadelta (γδ) T cells and their receptors into cancer cell therapies. Nat. Rev. Drug Discov. 19, 169–184 (2020).
Kabelitz, D., Serrano, R., Kouakanou, L., Peters, C. & Kalyan, S. Cancer immunotherapy with γδ T cells: many paths ahead of us. Cell. Mol. Immunol. 17, 925–939 (2020).
Kabelitz, D. & He, W. The multifunctionality of human Vgamma9Vdelta2 gammadelta T cells: clonal plasticity or distinct subsets?. Scand. J. Immunol. 76, 213–222 (2012).
Caccamo, N. et al. Differentiation, phenotype, and function of interleukin-17-producing human Vγ9Vδ2 T cells. Blood 118, 129–138 (2011).
Peters, C., Häsler, R., Wesch, D. & Kabelitz, D. Human Vdelta2 T cells are a major source of interleukin-9. Proc. Natl. Acad. Sci. USA 113, 12520–12525 (2016).
Wesch, D., Peters, C., Oberg, H. H., Pietschmann, K. & Kabelitz, D. Modulation of gammadelta T cell responses by TLR ligands. Cell. Mol. Life Sci. 68, 2357–2370 (2011).
Collins, C., Shi, C., Russell, J. Q., Fortner, K. A. & Budd, R. C. Activation of gamma delta T cells by Borrelia burgdorferi is indirect via a TLR- and caspase-dependent pathway. J. Immunol. 181, 2392–2398 (2008).
Pietschmann, K. et al. Toll-like receptor expression and function in subsets of human gammadelta T lymphocytes. Scand. J. Immunol. 70, 245–255 (2009).
Wesch, D. et al. Direct costimulatory effect of TLR3 ligand poly(I:C) on human gamma delta T lymphocytes. J Immunol. 176, 1348–1354 (2006).
Li, M. et al. Upregulation of Intestinal Barrier Function in Mice with DSS-Induced Colitis by a Defined Bacterial Consortium Is Associated with Expansion of IL-17A Producing Gamma Delta T Cells. Front Immunol. 8, 824 (2017).
Schwacha, M. G. et al. Dermal γδ T-cells can be activated by mitochondrial damage-associated molecular patterns. PLoS ONE 11, 8993 (2016).
Hartmann, G. Nucleic acid immunity. Adv. Immunol. 133, 121–169 (2017).
Chi, H. et al. Anti-tumor activity of toll-like receptor 7 agonists. Front. Pharmacol. 8, 304 (2017).
Serrano, R., Wesch, D. & Kabelitz, D. Activation of human γδ T cells: Modulation by toll-like receptor 8 ligands and role of monocytes. Cells 9, 713 (2020).
Hornung, V. et al. Sequence-specific potent induction of IFN-alpha by short interfering RNA in plasmacytoid dendritic cells through TLR7. Nat. Med. 11, 263–270 (2005).
Ablasser, A. et al. Selection of molecular structure and delivery of RNA oligonucleotides to activate TLR7 versus TLR8 and to induce high amounts of IL-12p70 in primary human monocytes. J. Immunol. 182, 6824–6833 (2009).
Ostendorf, T. et al. Immune sensing of synthetic, bacterial, and protozoan RNA by toll-like receptor 8 requires coordinated processing by RNase T2 and RNase 2. Immunity 52, 591–605 (2020).
Zhang, S. et al. Small-molecule inhibition of TLR8 through stabilization of its resting state. Nat. Chem. Biol. 14, 58–64 (2018).
Peters, C., Kouakanou, L., Oberg, H. H., Wesch, D. & Kabelitz, D. In vitro expansion of Vγ9Vδ2 T cells for immunotherapy. Methods Enzymol. 631, 223–237 (2020).
Bekeredjian-Ding, I. et al. T cell-independent, TLR-induced IL-12p70 production in primary human monocytes. J. Immunol. 176, 7438–7446 (2006).
Eigenbrod, T., Pelka, K., Latz, E., Kreikemeyer, B. & Dalpke, A. H. TLR8 senses bacterial RNA in human monocytes and plays a nonredundant role for recognition of streptococcus pyogenes. J. Immunol. 195, 1092–1099 (2015).
Coch, C. et al. Human TLR8 senses RNA from Plasmodium falciparum-infected red blood cells which is uniquely required for the IFN-γ response in NK cells. Front. Immunol. 10, 371 (2019).
Makni-Maalej, K. et al. TLR8, but not TLR7, induces the priming of the NADPH oxidase activation in human neutrophils. J. Leukoc. Biol. 97, 1081–1087 (2015).
de Marcken, M., Dhaliwal, K., Danielsen, A. C., Gautron, A. S. & Dominguez-Villar, M. TLR7 and TLR8 activate distinct pathways in monocytes during RNA virus infection. Sci. Signal. 12(605), 1347 (2019).
Glas, M. et al. Targeting the cytosolic innate immune receptors RIG-I and MDA5 effectively counteracts cancer cell heterogeneity in glioblastoma. Stem Cells. 31, 1064–1074 (2013).
Berger, M. et al. TLR8-driven IL-12-dependent reciprocal and synergistic activation of NK cells and monocytes by immunostimulatory RNA. J. Immunother. 32, 262–271 (2009).
Bergstrøm, B. et al. TLR8 Senses Staphylococcus aureus RNA in Human Primary Monocytes and Macrophages and Induces IFN-β Production via a TAK1-IKKβ-IRF5 Signaling Pathway. J. Immunol. 195, 1100–1111 (2015).
Van Den Eeckhout, B., Tavernier, J. & Gerlo, S. Interleukin-1 as Innate Mediator of T Cell Immunity. Front. Immunol. 11, 621931. https://doi.org/10.3389/fimmu.2020.621931 (2021).
Kaplanski, G. Interleukin-18: Biological properties and role in disease pathogenesis. Immunol. Rev. 281, 138–153 (2018).
Wesch, D., Glatzel, A. & Kabelitz, D. Differentiation of resting human peripheral blood gamma delta T cells toward Th1- or Th2-phenotype. Cell. Immunol. 212, 110–117 (2001).
Peters, C. et al. TGF-β enhances the cytotoxic activity of Vδ2 T cells. Oncoimmunology. 8, e1522471. https://doi.org/10.1080/2162402X.2018.1522471 (2018).
Liu, G. & Gack, M. U. Distinct and Orchestrated Functions of RNA Sensors in Innate Immunity. Immunity 53, 26–42 (2020).
Greulich, W. et al. TLR8 is a sensor of RNase T2 degradation products. Cell 179, 1264–1275 (2019).
Frega, G. et al. Trial Watch: experimental TLR7/TLR8 agonists for oncological indications. Oncoimmunology. 9, 1796002 (2020).
Oberg, H. H. et al. Bispecific antibodies enhance tumor-infiltrating T cell cytotoxicity against autologous HER-2-expressing high-grade ovarian tumors. J. Leukoc. Biol. 107, 1081–1095 (2020).
Wesch, D., Kabelitz, D. & Oberg, H. H. Tumor resistance mechanisms and their consequences on γδ T cell activation. Immunol. Rev. 298, 84–98 (2020).
Rothenfusser, S. et al. Distinct CpG oligonucleotide sequences activate human gamma delta T cells via interferon-alpha/-beta. Eur. J. Immunol. 31, 3525–3534 (2001).
Kunzmann, V., Kretzschmar, E., Herrmann, T. & Wilhelm, M. Polyinosinic-polycytidylic acid-mediated stimulation of human gammadelta T cells via CD11c dendritic cell-derived type I interferons. Immunology 112, 369–377 (2004).
Devilder, M. C., Allain, S., Dousset, C., Bonneville, M. & Scotet, E. Early triggering of exclusive IFN-gamma responses of human Vgamma9Vdelta2 T cells by TLR-activated myeloid and plasmacytoid dendritic cells. J. Immunol. 183, 3625–3633 (2009).
Deetz, C. O. et al. Gamma interferon secretion by human Vgamma2Vdelta2 T cells after stimulation with antibody against the T-cell receptor plus the Toll-Like receptor 2 agonist Pam3Cys. Infect. Immun. 74, 4505–4511 (2006).
Peters, C., Oberg, H. H., Kabelitz, D. & Wesch, D. Phenotype and regulation of immunosuppressive Vδ2-expressing γδ T cells. Cell. Mol. Life Sci. 7, 1943–1960 (2014).
Shojaei, H. et al. Toll-like receptors 3 and 7 agonists enhance tumor cell lysis by human gammadelta T cells. Cancer Res. 69, 8710–8717 (2009).
Nerdal, P. T. et al. Butyrophilin 3A/CD277-Dependent activation of human γδ T cells: Accessory cell capacity of distinct leukocyte populations. J. Immunol. 197, 3059–3068 (2016).
Yang, R. et al. IL-12 expands and differentiates human Vγ2Vδ2 T effector cells producing antimicrobial cytokines and inhibiting intracellular mycobacterial growth. Front. Immunol. 10, 913 (2019).
Schilbach, K., Welker, C., Krickeberg, N., Kaißer, C., Schleicher, S., Hashimoto, H. In the Absence of a TCR Signal IL-2/IL-12/18-Stimulated γδ T Cells Demonstrate Potent Anti-Tumoral Function Through Direct Killing and Senescence Induction in Cancer Cells. Cancers (Basel). 12, 130 (2020).
Troye-Blomberg, M. et al. Human gamma delta T cells that inhibit the in vitro growth of the asexual blood stages of the Plasmodium falciparum parasite express cytolytic and proinflammatory molecules. Scand. J. Immunol. 50, 642–650 (1999).
Hernández-Castañeda, M. A. et al. γδ T Cells Kill Plasmodium falciparum in a Granzyme- and Granulysin-Dependent Mechanism during the Late Blood Stage. J. Immunol. 204, 1798–1809 (2020).
Junqueira, C. et al. γδ T cells suppress Plasmodium falciparum blood-stage infection by direct killing and phagocytosis. Nat. Immunol. 22, 347–357 (2021).
Oberg, H. H. et al. Tribody [(HER2)2xCD16] Is More Effective Than Trastuzumab in Enhancing γδ T Cell and Natural Killer Cell Cytotoxicity Against HER2-Expressing Cancer Cells. Front. Immunol. 9, 814 (2018).
Liu, C. et al. Vγ9Vδ2 T cells proliferate in response to phosphoantigens released from erythrocytes infected with asexual and gametocyte stage Plasmodium falciparum. Cell. Immunol. 334, 11–19 (2018).
Caron, G. et al. Direct stimulation of human T cells via TLR5 and TLR7/8: flagellin and R-848 up-regulate proliferation and IFN-gamma production by memory CD4+ T cells. J. Immunol. 175, 1551–1557 (2005).
Peng, G. et al. Toll-like receptor 8-mediated reversal of CD4+ regulatory T cell function. Science 309, 1380–1384 (2005).
Meås, H. Z. et al. Sensing of HIV-1 by TLR8 activates human T cells and reverses latency. Nat. Commun. 11, 147 (2020).
Dowling, D. J. Recent Advances in the Discovery and Delivery of TLR7/8 Agonists as Vaccine Adjuvants. Immunohorizons. 2, 185–197 (2018).
Michaelis, K. A. et al. The TLR7/8 agonist R848 remodels tumor and host responses to promote survival in pancreatic cancer. Nat. Commun. 10, 4682 (2019).
Acknowledgements
We are very grateful to Monika Kunz for expert technical assistance.
Funding
Open Access funding enabled and organized by Projekt DEAL. This work was supported by grants the Wilhelm Sander-Stiftung (Grant 2018.045.1 to D.K.). R.S. is the recipient of a long-term fellowship from the German Academic Exchange Service (DAAD). G.H. received funding by the Deutsche Forschungsgemeinschaft (DFG, German Research Foundation) under Germany's Excellence Strategy - EXC2151 - 390873048 and TRR237, and by DZIF TTU IICH 07.834.00.
Author information
Authors and Affiliations
Contributions
R.S., D.W. and D.K. designed the experiments, R.S. performed most experiments, C.P. contributed to analysis of FACS results, C.C. and G.H. designed RNA ligands, D.K. wrote a first draft of the manuscript, all authors contributed to the discussion and approved the final version of the manuscript.
Corresponding author
Ethics declarations
Competing interests
The authors declare no competing interests.
Additional information
Publisher's note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if changes were made. The images or other third party material in this article are included in the article's Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article's Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
Serrano, R., Coch, C., Peters, C. et al. Monocyte-dependent co-stimulation of cytokine induction in human γδ T cells by TLR8 RNA ligands. Sci Rep 11, 15231 (2021). https://doi.org/10.1038/s41598-021-94428-6
Received:
Accepted:
Published:
DOI: https://doi.org/10.1038/s41598-021-94428-6
- Springer Nature Limited