Abstract
This study evaluated acute cardiac stress after a high-intensity interval training session in patients with type 2 diabetes (T2D) versus healthy controls. High intensity aerobic exercise was performed by 4 × 4-min intervals (90–95% of maximal heart rate), followed by a ramp protocol to peak oxygen uptake. Echocardiography was performed before and 30 min after exercise. Holter electrocardiography monitored heart rhythms 24 h before, during, and 24 h after the exercise. Left atrial end-systolic volume, peak early diastolic mitral annular velocity, and the ratio of peak early to late diastolic mitral inflow velocity were reduced by approximately 18%, 15%, and 31%, respectively, after exercise across groups. Left ventricular end-diastolic wall thickness was the only echo parameter that significantly differed between groups in response to exercise. The T2D group had a rate of supraventricular extrasystoles per hour that was 265% greater than that of the controls before exercise, which remained higher after exercise. A single exhaustive exercise session impaired left ventricular diastolic function in both groups. The findings also indicated impaired right ventricular function in patients with T2D after exercise.
ClinicalTrials.gov Identifier: NCT02998008.
Similar content being viewed by others
Introduction
Type 2 diabetes (T2D) is an increasingly prevalent condition worldwide and is likely to reach pandemic levels within the coming decades1. The condition is characterized by high blood glucose and abnormal insulin regulation and is strongly linked to obesity and inactivity. Several complications are associated with the disease, such as kidney disease, retinopathy, cardiovascular disease, and diabetic cardiomyopathy2. Low cardiorespiratory fitness (maximal oxygen uptake; VO2max), one of the strongest predictors of cardiovascular death, is common in patients with T2D3, who are more prone to arrhythmias and their complications such as an increased risk of stroke in those with atrial fibrillation3, and cognitive impairment in older adults4.
Clinical studies associated diabetes with left ventricular (LV) dysfunction independent of other heart diseases1. Myocardial metabolism depends on a sufficient energy substrate provided by fatty acids and glucose during physical exercise. There is a fine-tuned balance in healthy individuals with a dynamic variation in the energy source that depends on the heart’s workload and the exercise intensity5. However, this substrate flexibility is significantly impaired in patients with T2D due to insulin deficiency. Therefore, the metabolism depends more on the oxidation of fatty acids, reducing cardiac efficiency6,7,8. Several studies have reported that efficiency of diabetic hearts is further reduced, which cannot be explained by only the reduced substrate flexibility7,9. This reduction is ascribed to a certain extent to increased oxygen consumption by non-contractile processes, such as increased mitochondrial uncoupling, production of reactive oxygen species10,11, impaired excitation–contraction coupling and Ca2+ handling12,13. These changes can be prevented by exercise training14,15.
Despite numbers of studies showing beneficial effects by exercise, there are also studies showing impairment of the myocardium after vigorous prolonged exercise. A study from the North See Race showed elevated troponin levels after prolonged vigorous exercise among well-trained athletes16. There are increasing reports of elevated cardiac troponin (cTn) I and T (TnT) levels, reflecting myocardial cell damage17, after exercise interventions. Studies have reported reduced contractility, increased cardiac injury biomarkers and reduced right ventricular (RV) and LV ejection fraction (EF) after long periods of high-intensity training18,19,20,21,22,23,24. In most cases, the effects are transient; however, persistent changes such as the development of fibrosis have occurred in patients exposed to extreme amounts of training combined with a predisposition for cardiac dysfunction20.
Aim of the study
There is still much to learn regarding the heart’s response to exercise, both in individuals with T2D and those predisposed to ischemic heart disease. The present study aimed to investigate cardiac function and volume responses, biomarkers of cardiac stress, and arrhythmias following a session of high-intensity exhaustive exercise in patients with T2D compared with healthy individuals. We hypothesized that acute exercise training could provoke greater cardiac stress that would manifest with more pronounced cardiac dysfunction in patients with T2D than in healthy individuals. We expected both groups to have elevated TnT levels and indications of impaired cardiac function following exhaustive exercise, with potentially more prominent findings in the RV.
Results
Physical characteristics and baseline blood parameters
The mean age was 56 years in both groups. Except from glycated hemoglobin (HbA1c), blood glucose, and insulin C peptide levels, there was no difference between T2D and healthy controls in physical characteristics or blood parameters at baseline (Table 1). In the T2D group, HbA1c levels were significantly higher (33%), glucose levels were 57% higher, and insulin C peptide levels were 50% higher. No other baseline parameters differed between the groups at baseline.
Response to cardiopulmonary exercise test (CPET)
VO2peak was significantly lower in the T2D group compared to controls (33.1 ± 5.8 ml kg−1 min−1 and 44.0 ± 6.6 ml min–1 kg–1, respectively, p < 0.01) (Fig. 1A). Minute ventilation (VE) and the ventilatory CO2 per minute (VCO2) was also significantly reduced in the diabetes group compared to the controls (Fig. 1B,C). The peak heart rate was similar in the two groups with 181 ± 12 beats min−1 in the T2D group and 175 ± 10 beats min−1 in the control group (Fig. 1D).
Baseline data from cardiopulmonary exercise tests between the controls and type 2 diabetes (T2D) group. (A) Peak oxygen uptake (VO2peak) displayed in ml min–1 kg–1; (B) minute ventilation peak (VEpeak) displayed in L min−1; (C) ventilatory CO2 per minute (VCO2) displayed in L min−1; (D) peak heart rate (HRpeak) displayed in beats per min (bpm). Data presented with box and whiskers with minimum to maximum values. p values are indicated in figure. Control: n = 7, T2D: n = 7.
Change in blood samples after exercise
Despite the individual changes observed in several of the measured blood parameters, there were no statistical significant differences in response to exercise between the groups.
Glucose
Glucose levels were expected to decrease in the T2D group following exercise but remained constant (8.6 mmol/L pre-exercise, 8.2 mmol/L post-exercise and 8.6 mmol/L 24 h post-exercise). In the control group, the glucose levels were significantly lower than those in the T2D group but did not change over the different time points (5.4 mmol/L pre-exercise, 5.3 mmol/L post-exercise and 6.2 mmol/L 24 h post-exercise (Fig. 2A,B).
Blood sample data from baseline (Pre) and 1 h and 24 h post-exercise. (A) Glucose in the control group; (B) glucose in the T2D group; (C) Troponin T (TnT) in the control group; (D) TnT in the T2D group. Presented with individual data at each time-point. The detection limit for TnT was 10 ng/L. p values between T2D and control are indicated. Control: n = 7, T2D: n = 7.
Troponin T
All of the control group participants had TnT values < 10 ng/L before the exercise training. Two participants of the T2D group had higher values (13 ng/L and 11 ng/L), while the rest had values < 10 ng/L. Three participant in the T2D group had TnT ≥ 10 ng/L after the exercise. Two participants in the T2D group had serum TnT levels that remained elevated after 24 h. Two participants in the control group had elevated TnT levels exceeding 10 ng/L post-exercise; the participant with the highest measured TnT level (20 ng/L) remained above 10 ng/L 24 h post-exercise (Fig. 2C,D).
Baseline cardiac function in T2D and controls
The T2D group had smaller mean baseline RV end-diastolic diameter (36.4 ± 5.9 mm for T2D vs. 45.9 ± 4.2 mm for control; p < 0.01 (Table 2). There were no other statistically significant differences between the two groups at baseline (before exercise training).
Cardiac responses to exhaustive exercise in T2D and controls
The only parameter with a statistically significant change from baseline to after exhaustive exercise between groups was end-diastolic intraventricular septum thickness (1.5 mm increase in controls, 0.3 mm reduction in the T2D group; p < 0.05).
Despite the limited intergroup differences in response to exercise, there were statistically significant changes within each groups in several echocardiography parameters (Table 2).
There was a statistically significant reduction in early diastolic mitral annular velocity (e´), reaching 1.4 cm/s in the control group (p < 0.05) and 0.8 cm/s in the T2D group (p < 0.05) when measured by color tissue Doppler, with the pulsed-wave tissue Doppler measurements showing similar findings (Appendix Table A.1). The peak systolic mitral annular velocity was not significant different. The corresponding mitral inflow peak early diastolic velocity (E) was lower after exercise in both groups (− 13.6 cm/s in the control group [p < 0.05] and − 12.2 cm/s in the T2D group [p = 0.1]).
The LV end-diastolic posterior wall thickness increased in the control group after exercise (p < 0.05), while no significant change appeared in the T2D group. A non-significant post-exercise reduction in LV end-diastolic volume compared with baseline was observed in the controls (− 11.4 ml, p = 0.13) and T2D group (− 10.1 ml, p = 0.16). A similar finding was present when analyzing three-dimensional recordings (Appendix Table A.2 and A.3).
There were no differences in the two groups in systolic fractional shortening after exercise. LV EF was > 3.4%-points lower in both groups after exercise, but the differences were not statistically significant. However, in the patients with elevated TnT, LV EF was reduced by 6.7% after exercise (p < 0.05). The early to late peak diastolic mitral inflow velocity (E/A ratio) was significantly reduced by 0.4 in both groups post exercise (p < 0.05).
As a measure of RV function, the tricuspid annular plane systolic excursion (TAPSE) was − 2.2 mm lower in the T2D group (p < 0.05) and − 3.3 in the control group (not statistically significant). Peak early diastolic tricuspid annular velocity was also reduced from baseline to post-exercise in the T2D group (− 1.8 mm, p < 0.05) but was not significantly changed in the control group (− 1.3 mm, p = 0.08).
The left atrial end-systolic volume was significantly reduced from baseline to post-exercise in the T2D group (− 10.8 ml, p < 0.05) and controls (− 13.9 ml, p < 0.05). RV echocardiography detected no changes in either group.
Heart rate during echocardiography did not differ significantly between the groups before or after exercise, but it was significantly higher in the control group during the post-exercise testing (65 ± 13 and 83 ± 14 bpm [p < 0.05] and 69 ± 12 and 79 ± 8 bpm for the controls and T2D group, respectively).
Interestingly, sub-study analyses on echocardiography recordings performed on individuals with post-exercise elevated TnT (independent of the study group) displayed more significant post-exercise deterioration on cardiac function (Appendix Table A.4).
Holter electrocardiogram
There were significantly more premature supraventricular extrasystoles (SVES) and ventricular extrasystoles (VES) in the T2D group at baseline (Fig. 3). The T2D group also exhibited more premature ventricular beats after exercise; however, the exercise did not the number of premature beats.
Holter electrocardiography. (A) Supraventricular extrasystoles (SVES) per hour (Control: n = 7, T2D: n = 7) and (B) ventricular extrasystoles (VES) per hour (Control: n = 7, T2D: n = 6). Data presented with box and whiskers with minimum to maximum values. Pre represents the complete period 24 h before exercise and Post represents the complete period 24 h after termination of exercise. No statistical differences within groups from pre- to post-exercise was observed. p values are indicated.
Discussion
The present study demonstrated statistically significant differences in cardiorespiratory fitness level between the T2D group and controls; however, there were no consistent differences in the cardiac response to exercise training. Interestingly, after exhaustive exercise, both groups had significantly altered e’, E/A ratios, and left atrial end-systolic volumes. These findings indicate that a single session of exhaustive high intensity exercise training affects the hearts of patients with T2D and healthy controls, causing at least intermittent impaired function.
We found that e’ and the E/A ratio were significantly lower in both groups from baseline to post-exercise. Therefore, these changes indicate impaired LV diastolic function after exhaustive exercise in both groups. Diastolic dysfunction refers to disturbed LV relaxation25. Similar findings in terms of E/A ratio have occurred after marathon participation with much longer duration26,27,28. Acute adaptations, indicating post-exercise cardiac dysfunction, is further supported by increased LV end-diastolic posterior wall thickness (p = 0.02) and somewhat increased end-diastolic intraventricular septum thickness (p ≤ 0.09) in the control group. This change might reflect post-exercise myocardial edema or increased blood volume in the myocardium. Exercised-induced muscle damage in other muscles has shown an inflammation-like response after exercise, and the finding could indicate a similar mechanism in the myocardium29.
Interestingly, these alterations did not appear in the T2D group. The reason for the change in the parameters in the control group and not in the T2D group remains unclear and needs further investigation. However, the lower mitral blood flow velocity (E) and smaller left atrial volumes could indicate that e’ and E/A changes might be partly due to a reduced post-exercise preload.
Peak early diastolic tricuspid annular velocities and TAPSE were reduced after exercise but were only statistically significant in the T2D group, which might indicate RV dysfunction. Based on previous findings, we expected more pronounced changes in RV after exhaustive exercise18,19,30,31. However, our results did not indicate more severe changes in the RV than in the LV. This finding might be partly because of the relatively short duration of the exercise training. Although conducted at high intensity, the duration was short compared to previous reports18,19,31. Exercise duration has been linked to the degree of RV impairment, where longer durations appear to cause greater impairment31. The study by La Gerche et al. hypothesized that long-term processes such as fibrosis might contribute to the development of RV dysfunction31.
The acute changes observed after exercise training at high intensity are normally transient. La Gerche found a transient increase in RV volume and a decline in RV function after three to 11 h of exercise, and most patients recover within a week20,31. Unfortunately, we did not follow up our population with echocardiograms 24 h after exercise. However, our data showing a decline of TnT levels 24 h after exercise could indicate that the modest systolic and diastolic dysfunction is restored within a relatively short time.
Several studies have reported increased cardiac troponin levels after short and long exercise sessions32,33,34. There is a broad agreement that cardiac impairment following exercise training is greatest in the least trained22,35. The T2D group had a statistically significant 25% lower VO2peak than the age-matched controls, which corresponds to previously reported values of cardiorespiratory fitness in this patient group36. This reduction in cardiorespiratory fitness has been associated with a two-fold increased risk of cardiovascular mortality among patients with T2D37. Myers et al. showed a 12% increase in survival with a 1 metabolic equivalent (~ 3.5 ml kg−1 min−1) improvement in VO2peak38. The present study found a substantial ~ 3 metabolic equivalent (11 ml kg−1 min−1) difference. The difference in cardiorespiratory fitness was further supported by the echocardiographic findings of numerically smaller LVs and RVs in patients with T2D. A greater increase in TnT would be expected in the T2D group because their VO2peak was significantly lower than the controls, demonstrating that the patients with T2D had a significantly lower fitness level. In the North Sea study, a TnT increase was also associated with a higher load of occult obstructive coronary artery disease39. Since the T2D group displayed lower aerobic capacity, reduced cardiac function, and a higher load of cardiovascular risk factors than the control group, we wanted to determine whether the T2D group had a more severe post-exercise increase in TnT.
In contrast to our assumption, only a few of the included patients presented with elevated TnT post-exercise. There were no differences between the patients with T2D and the healthy controls. The previously mentioned studies detected increases far above 14 ng/L, which is the cut-off for myocardial infarction17. The discrepancy between our results and those of other studies might be due to the differences in exercise duration and total workload over time, with previous studies employing relatively high-intensity exercise over hours. A recent study showed that troponin elevation is probably more closely linked to intensity than duration40. A plausible explanation for our findings is that both groups were exposed to the same relatively high-intensity exercise. Notwithstanding, there was an increase in TnT in five participants, three of whom were in the T2D group. Interestingly, those with elevated TnT (independent of group) had more severely impaired cardiac function indications. Several authors suggested that increased troponin levels after exercise could be caused by a physiological response that causes leakage of the unbound free form of troponins from the cytosol during exercise due to membrane damage, not necrosis, including destruction of the contractile apparatus that is common after myocardial infarction41.
There were significantly more premature SVES and VES in the T2D group at baseline, agreeing with previous related studies. That might result from changes caused by T2D and the effects of common comorbidities such as hypertension on the heart and autonomic nervous system42,43. There was no further effect of exercise on number of premature beats.
T2D is characterized by hyperglycemia, commonly diagnosed by elevated HbA1c levels. Hyperglycemia is a significant risk factor for cardiovascular disease. Engaging in exercise training improves glucose uptake and insulin sensitivity for several hours, depending on the exercise intensity and duration44. The exercise intensity determines the use of substrates available during exercise. Higher intensities depend on utilizing glucose, while up to approximately 60% intensities result in greater fat oxidation45, which could be important for the glucose regulation commonly observed after exercise. Postprandial glycemic function has been reported to improve acutely after exercise, and high-intensity exercise has been reported to have greater and more lasting effects46,47,48. However, we did not use continuous glucose monitoring in our study and cannot confirm nor exclude similar results. There was no change in glucose after exercise in any of the groups. HbA1c was measured only during screening to confirm the presence of T2D.
Study strengths and limitations
The main limitation of this pilot study is the small sample size, and the results obtained should be considered carefully and serve as a fundament for further studies. The patients with T2D also presented with relatively mild symptoms of diabetes. This population typically has body mass indices (BMI) > 30, while our participants had a mean BMI of 28. CPET displayed the largest differences between the groups. Before the study, there were doubts about whether the T2D group would be able to perform maximal effort during CPET. However, there was no significant difference in the respiratory exchange ratio between the controls and the T2D group. Also, the echocardiographic examinations were performed at rest, and stress echocardiography might have been a better-suited measure to determine cardiac performance differences. The blinding for group assignment and time in the echocardiographic analyses constitutes one of the study’s strengths. The highly relevant methods for exploring acute responses to exhaustive exercise in patients with T2D and healthy individuals constitute another of the study’s strengths.
Conclusion
The present study found no major differences in the cardiac response to acute exhaustive exercise between the patients with T2D and the healthy controls. After exercise training, both groups had reduced cardiac function, displayed by reduced e’ and the E/A ratio, indicating LV diastolic function. Following exercise, there were no consistent differences between the T2D and control groups in cardiac troponin release. Despite the significantly greater number of premature SVES and VES in the T2D group than in the control group, exercise did not alter the electrophysiological parameters from baseline. The comprehensive and blinded echocardiographic and electrophysiological analyses provided valuable information regarding the acute cardiac responses to high-intensity training in patients with T2D versus healthy controls and provided hypotheses for future research.
Methods
Subjects
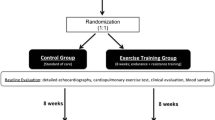
The study included age-matched subjects with T2D (n = 7) and healthy controls (n = 7). In total, 15 men volunteered for the study; one person was excluded due to a lack of parameters confirming T2D. Inclusion criteria were an age > 30 years and confirmed T2D accompanied by elevated HbA1C and glucose levels. The patients with T2D were on optimal medication advised from their medical doctors (Individual medications and history of T2D included in Appendix Table A.5) None of the T2D presented with diabetic complications (retinopathy, nephropathy, neuropathy, etc.). All participants provided written informed consent before data collection. The Regional Committee for Medical Research Ethics Central Norway approved this study (REC ID 2016/1596), which complied with the statement of ethical principles for medical research outlined in the Declaration of Helsinki. All methods were performed under the relevant guidelines. The study is registered in ClinicalTrials.gov Identifier: NCT02998008 (First posted: 20/12/2016).
Test procedure and protocols
Participant registration and timeline
Day 1
All participants completed a questionnaire from a physician evaluating their health status and medical consent for training and CPET. Blood pressure was measured following 10 min of rest while seated in a chair. Three tests were performed and the mean result of the latter two was used. The participants had their height measured in cm and then underwent an Inbody scan (Inbody, AU). They subsequently underwent Holter electrocardiogram (ECG) monitoring of the cardiac electrical activity 24 h before, during, and 24 h after the exercise. Lastly, a blood sample was collected from the participants at the end of day 1.
Day 2
Echocardiography was first performed immediately before the single session of exhaustive exercise consisting of a 4 × 4-min interval exercise and one final bout performed as a ramp protocol to assess VO2peak. After the exercise all participants rested for 30 min before undergoing the second echocardiography. At the end of day 2, a second blood sample was collected 30 min after the second echocardiography.
Day 3
Participants concluded their Holter ECG monitoring, and a final blood sample was collected 24 h after the exercise test.
Interval training and CPET
The exercise was performed as a 4 × 4-min high-intensity interval training. The intervals were conducted at approximately 90% of VO2peak and were followed by 2-min breaks with active recovery at 60%. We then added a fifth interval performed as a ramp protocol with speed and/or inclination increments to measure VO2peak. The CPET to measure VO2peak was performed at the NeXt Move core facility at the Norwegian University of Science and Technology. All participants were regularly offered water during and after exercise to prevent hypovolemia. Given that patients with T2D sometimes have physical limitations, experienced personnel determined the best individual CPET regimen during a 6-min warm-up on the treadmill (Woodway PPS55, USA Inc., Waukesha, WI, USA), by detecting functional walking or running speed and inclination, as well as subjective moderate aerobic intensity based on rated perceived exertion (RPE Borg scale 6–20). Participants were then fitted with a heart rate monitor (H7, Polar Electro, Kempele, Finland) and facemask (7450 Series V2 CPET mask, Hans Rudolph Inc., Shawnee, KS, USA). Work economy measurements were performed during an initial 4-min period at a fixed submaximal workload serving as an extended warm-up.
VO2max was defined using the following criteria: (1) VO2 levelling off (< 2 ml min–1 kg–1) despite the increased workload and (2) respiratory exchange ratio ≥ 1.05. If these criteria were not met, the term VO2peak was used. A participants’s VO2peak was defined as the mean of the three successive highest VO2 measurements recorded during the CPET. For simplicity, the term VO2peak is used for all patients.
An individualized ramp protocol was used until either exhaustion or fulfilment of the criteria for VO2max or VO2peak. The workload was gradually increased, and gas measurements were recorded every tenth second using a mixing chamber ergospirometry system (Metalyzer II, Cortex Biophysik Gmbh, Leipzig, Germany).
Echocardiography
Echocardiographic recordings and analyses of the different chambers followed the recommendation by the American and European societies of Echocardiography49. An experienced cardiologist performed transthoracic echocardiography, and all participants were examined in the left-lateral decubitus position. A Vivid E95 scanner was employed with a phased-array transducer (M5S) (GE Ultrasound, Horten, Norway). Echocardiographic data were stored digitally and analyzed after end of study inclusion by the same cardiologist. All echocardiograms were acquired with the operator blinded to group assignment to avoid any bias in the analyses. All analyses were performed by the same operator blinded to group assignment and whether the echocardiogram was recorded before or after the exhaustive exercise session. All measurements reflect the mean of three cardiac cycles, as recommended for patients in sinus rhythm. The measurements are reported as absolute values and not indexed to body surface area.
Grey-scale two-dimensional views were recorded from the parasternal border in short- and long-axis, and the apical position in four-chamber, two-chamber, and long-axis views. Separate recordings were made to optimize the volumetric measurements of the specific chambers and avoid foreshortening and misalignment. Linear measurements of the LV myocardium and dimensions were done in parasternal long-axis recordings at end-diastole and end-systole immediately below the level of the mitral valve leaflet tips. The fractional shortening was calculated by the change in LV size divided by the end-diastolic size. Left atrial and LV volumes were measured by the summation of discs method in four- and two-chamber views by tracing of the endocardial border. LV EF was calculated as the percentage of blood volume ejected during systole using biplane method of disc summation (Simpson’s method). The area-length method estimated right atrial and RV volumes from RV-focused four-chamber views. The RV dimension was measured in RV-focused four-chamber views at the basal and mid-ventricular levels. TAPSE was measured by reconstructed motion mode aligned to the movement of the basal RV free wall. Recordings were performed in color-coded Doppler mode through all valvular orifices and vessels to identify conditions such as regurgitation and stenosis.
Spectral Doppler with a sample volume recorded blood flow; (a) at tip of the mitral leaflet and in the presence of mitral regurgitation aligned to the regurgitant jet, (b) in the distal LV outflow tract, (c) through the aortic valve, (d) at tip of the tricuspid valve and in presence of tricuspid regurgitation aligned to the regurgitant jet, and (e) in the RV outflow tract. Care was taken to align the ultrasound beam to the blood flow direction for all measurements. The mitral inflow peak early (E) and late (A) diastolic velocities and the early diastolic deceleration time was measured, and the E/A ratio was calculated.
Color tissue Doppler cine-loops were recorded in the apical four-chamber, two-chamber and long-axis, and RV-focused view. Target frame rate for the color tissue Doppler recordings was 100 fps. Care was taken to align the ultrasound beam to the myocardial wall. Peak systolic (S’) and early diastolic (e’) mitral annular velocities were measured at the base of the six myocardial walls by color tissue Doppler, and the average values are used as measurements of the LV myocardial velocities. Pulsed-wave tissue Doppler velocity curves were recorded from the basal part of the left and right ventricle, at the septal and lateral points (near the insertion of the mitral valve) and from the RV free wall (near the insertion of the tricuspid valve). e’ was measured at the base of the septal and anterolateral wall by pulsed-wave tissue Doppler and the average was used for calculation of the E/e’ ratio. The peak systolic and early diastolic tricuspid annular velocities were measured by color tissue Doppler and pulse-wave Doppler, in the basal part of the right ventricular free wall.
Biochemical analysis
Blood samples were analyzed following standard operating procedures at St. Olavs Hospital. Glucose, HbA1c, total cholesterol, low density lipoprotein LDL cholesterol, TnT and insulin C peptide were all obtained before the training. Glucose and TnT were also obtained 1 h and 24 h post-exercise.
Body composition and weight
Body composition was measured using the validated bioelectrical impedance unit, Inbody 720 (Biospace, Seoul, Korea)50. In this machine, four pairs of electrodes are implanted into the handles and floor scale of the analyzer. Before testing, participants fast for a minimum of two hours and are encouraged to go to the toilet right before using the scale. The participants stood for 5 min before entering the scale and were barefoot. Due to the electrical impulse, people with pacemaker were not tested. Height, age, and sex were plotted om the scale display. After two minutes, weight (kg), BMI, muscle mass (kg), bodyfat percentage, and visceral fat (cm2) were measured by the scale. The device was auto calibrated once a week with the machine turned off.
Heart rhythm
A 48-h ambulatory, continuous ECG recording (DigiTrak XT, Phillips Healthcare, Andover, MA) was used 24 h before, during, and 24 h after the exercise session. Supraventricular and ventricular premature beats and arrhythmias were counted by the vendor-specific software but manually controlled by a trained physician.
Statistical analysis
A two-tailed Mann–Whitney test (unpaired samples) was applied to compare the changes from baseline to post-exercise between the groups (T2D and control). To compare the changes from baseline to post-exercise within each group, we used a two-tailed Wilcoxon matched-pairs signed-rank test, with exact p values. Heart rhythm measured using Holter electrocardiography monitoring was analyzed by Mann–Whitney two-tailed test (exact p values) at basline and post-exercise. Differences in TnT and glucose levels in the blood samples between T2D and control at baseline and at 1 h and 24 h post-exercise was performed using a mixed-effect model for repeated measures corrected with Šídák's multiple comparisons test. With TnT as a cardiac stress marker, we performed separate sub-analyses to determine the cardiac function response to exercise in individuals increased TnT levels. Data from the individuals with increased TnT levels (i.e., TnT > 10 ng/L) were therefore analyzed as a separate population using two-tailed Wilcoxon matched-pairs signed rank test, with exact p values. All analyses was performed using GraphPad Prism (version 9.3.1). p values < 0.05 were considered significant.
Ethics approval
The Regional Committee for Medical Research Ethics Central Norway approved this study (REC ID 2016/1596), which complied with the ethical ethical principles for medical research outlined in the Declaration of Helsinki. All methods were performed under the relevant guidelines and in agreement with the approval from the ethical committee. The study is registered in ClinicalTrials.gov Identifier: NCT02998008 (First posted: 20/12/2016).
Data availability
The datasets analyzed during the current study are available from the corresponding author on reasonable request.
References
Fang, Z. Y., Prins, J. B. & Marwick, T. H. Diabetic cardiomyopathy: Evidence, mechanisms, and therapeutic implications. Endocr. Rev. 25, 543–567. https://doi.org/10.1210/er.2003-0012 (2004).
Zhuo, X., Zhang, P. & Hoerger, T. J. Lifetime direct medical costs of treating type 2 diabetes and diabetic complications. Am. J. Prevent. Med. 45, 253–261. https://doi.org/10.1016/j.amepre.2013.04.017 (2013).
Cosentino, F. et al. 2019 ESC Guidelines on diabetes, pre-diabetes, and cardiovascular diseases developed in collaboration with the EASD: The Task Force for diabetes, pre-diabetes, and cardiovascular diseases of the European Society of Cardiology (ESC) and the European Association for the Study of Diabetes (EASD). Eur. Heart J. 41, 255–323. https://doi.org/10.1093/eurheartj/ehz486 (2019).
Mone, P. et al. Correlation of physical and cognitive impairment in diabetic and hypertensive frail older adults. Cardiovasc. Diabetol. 21, 10. https://doi.org/10.1186/s12933-021-01442-z (2022).
Stanley, W. C. & Chandler, M. P. Energy metabolism in the normal and failing heart: Potential for therapeutic interventions. Heart Fail. Rev. 7, 115–130 (2002).
van den Brom, C. E. et al. Altered myocardial substrate metabolism is associated with myocardial dysfunction in early diabetic cardiomyopathy in rats: Studies using positron emission tomography. Cardiovasc. Diabetol. 8, 39. https://doi.org/10.1186/1475-2840-8-39 (2009).
Mather, K. J. et al. Assessment of myocardial metabolic flexibility and work efficiency in human type 2 diabetes using 16-[18F]fluoro-4-thiapalmitate, a novel PET fatty acid tracer. Am. J. Physiol. Endocrinol. Metab. 310, E452-460. https://doi.org/10.1152/ajpendo.00437.2015 (2016).
Anderson, E. J. et al. Substrate-specific derangements in mitochondrial metabolism and redox balance in the atrium of the type 2 diabetic human heart. J. Am. Coll. Cardiol. 54, 1891–1898. https://doi.org/10.1016/j.jacc.2009.07.031 (2009).
Buchanan, J. et al. Reduced cardiac efficiency and altered substrate metabolism precedes the onset of hyperglycemia and contractile dysfunction in two mouse models of insulin resistance and obesity. Endocrinology 146, 5341–5349. https://doi.org/10.1210/en.2005-0938 (2005).
Boudina, S. et al. Reduced mitochondrial oxidative capacity and increased mitochondrial uncoupling impair myocardial energetics in obesity. Circulation 112, 2686–2695. https://doi.org/10.1161/circulationaha.105.554360 (2005).
Boudina, S. et al. Mitochondrial energetics in the heart in obesity-related diabetes: Direct evidence for increased uncoupled respiration and activation of uncoupling proteins. Diabetes 56, 2457–2466. https://doi.org/10.2337/db07-0481 (2007).
Stølen, T. O. et al. Interval training normalizes cardiomyocyte function, diastolic Ca2+ control, and SR Ca2+ release synchronicity in a mouse model of diabetic cardiomyopathy. Circ. Res. 105, 527–536. https://doi.org/10.1161/circresaha.109.199810 (2009).
Pereira, L. et al. Calcium signaling in diabetic cardiomyocytes. Cell Calcium 56, 372–380. https://doi.org/10.1016/j.ceca.2014.08.004 (2014).
Hafstad, A. D., Boardman, N. & Aasum, E. How exercise may amend metabolic disturbances in diabetic cardiomyopathy. Antioxid. Redox Signal 22, 1587–1605. https://doi.org/10.1089/ars.2015.6304 (2015).
Baekkerud, F. H. et al. High intensity interval training ameliorates mitochondrial dysfunction in the left ventricle of mice with type 2 diabetes. Cardiovasc. Toxicol. https://doi.org/10.1007/s12012-019-09514-z (2019).
Kleiven, O. et al. Occult obstructive coronary artery disease is associated with prolonged cardiac troponin elevation following strenuous exercise. Eur. J. Prevent. Cardiol. https://doi.org/10.1177/2047487319852808 (2019).
Thygesen, K. et al. Third universal definition of myocardial infarction. J. Am. Coll. Cardiol. 60, 1581–1598. https://doi.org/10.1016/j.jacc.2012.08.001 (2012).
Claessen, G. et al. Right ventricular fatigue developing during endurance exercise: An exercise cardiac magnetic resonance study. Med. Sci. Sports Exerc. 46, 1717–1726. https://doi.org/10.1249/mss.0000000000000282 (2014).
Elliott, A. D. & La Gerche, A. The right ventricle following prolonged endurance exercise: Are we overlooking the more important side of the heart? A meta-analysis. Br. J. Sports Med. 49, 724–729. https://doi.org/10.1136/bjsports-2014-093895 (2015).
La Gerche, A., Connelly, K. A., Mooney, D. J., MacIsaac, A. I. & Prior, D. L. Biochemical and functional abnormalities of left and right ventricular function after ultra-endurance exercise. Heart 94, 860–866. https://doi.org/10.1136/hrt.2006.101063 (2008).
Mousavi, N. et al. Relation of biomarkers and cardiac magnetic resonance imaging after marathon running. Am. J. Cardiol. 103, 1467–1472. https://doi.org/10.1016/j.amjcard.2009.01.294 (2009).
Neilan, T. G. et al. Myocardial injury and ventricular dysfunction related to training levels among nonelite participants in the Boston marathon. Circulation 114, 2325–2333. https://doi.org/10.1161/circulationaha.106.647461 (2006).
Oxborough, D. et al. Dilatation and dysfunction of the right ventricle immediately after ultraendurance exercise: exploratory insights from conventional two-dimensional and speckle tracking echocardiography. Circ. Cardiovasc. Imaging 4, 253–263. https://doi.org/10.1161/circimaging.110.961938 (2011).
Trivax, J. E. et al. Acute cardiac effects of marathon running. J. Appl. Physiol. (Bethesda, MD, 1985) 108, 1148–1153. https://doi.org/10.1152/japplphysiol.01151.2009 (2010).
Leite-Moreira, A. F. Current perspectives in diastolic dysfunction and diastolic heart failure. Heart 92, 712–718. https://doi.org/10.1136/hrt.2005.062950 (2006).
George, K. et al. Mitral annular myocardial velocity assessment of segmental left ventricular diastolic function after prolonged exercise in humans. J. Physiol. 569, 305–313. https://doi.org/10.1113/jphysiol.2005.095588 (2005).
Oxborough, D. et al. The impact of marathon running upon ventricular function as assessed by 2D, Doppler, and tissue-Doppler echocardiography. Echocardiography 23, 635–641. https://doi.org/10.1111/j.1540-8175.2006.00282.x (2006).
Serrano Ostariz, E. et al. Post-exercise left ventricular dysfunction measured after a long-duration cycling event. BMC Res. Notes 6, 211. https://doi.org/10.1186/1756-0500-6-211 (2013).
Peake, J. M., Neubauer, O., Della Gatta, P. A. & Nosaka, K. Muscle damage and inflammation during recovery from exercise. J. Appl. Physiol. 1985(122), 559–570. https://doi.org/10.1152/japplphysiol.00971.2016 (2017).
La Gerche, A. et al. Disproportionate exercise load and remodeling of the athlete’s right ventricle. Med. Sci. Sports Exerc. 43, 974–981. https://doi.org/10.1249/MSS.0b013e31820607a3 (2011).
La Gerche, A. et al. Exercise-induced right ventricular dysfunction and structural remodelling in endurance athletes. Eur. Heart J. 33, 998–1006. https://doi.org/10.1093/eurheartj/ehr397 (2012).
Airaksinen, K. E. J. Cardiac troponin release after endurance exercise: Still much to learn. J. Am. Heart Assoc. 9, e015912. https://doi.org/10.1161/jaha.120.015912 (2020).
Bjørkavoll-Bergseth, M. et al. Duration of elevated heart rate is an important predictor of exercise-induced troponin elevation. J. Am. Heart Assoc. 9, e014408. https://doi.org/10.1161/jaha.119.014408 (2020).
Aakre, K. M. & Omland, T. Physical activity, exercise and cardiac troponins: Clinical implications. Prog. Cardiovasc. Dis. 62, 108–115. https://doi.org/10.1016/j.pcad.2019.02.005 (2019).
Shave, R. et al. Exercise-induced cardiac troponin T release: A meta-analysis. Med. Sci. Sports Exerc. 39, 2099–2106. https://doi.org/10.1249/mss.0b013e318153ff78 (2007).
Hollekim-Strand, S. M. et al. High-intensity interval exercise effectively improves cardiac function in patients with type 2 diabetes mellitus and diastolic dysfunction: A randomized controlled trial. J. Am. Coll. Cardiol. 64, 1758–1760. https://doi.org/10.1016/j.jacc.2014.07.971 (2014).
Go, A. S. et al. Heart disease and stroke statistics–2014 update: A report from the American Heart Association. Circulation 129, e28–e292. https://doi.org/10.1161/01.cir.0000441139.02102.80 (2014).
Myers, J. et al. Exercise capacity and mortality among men referred for exercise testing. N. Engl. J. Med. 346, 793–801. https://doi.org/10.1056/NEJMoa011858 (2002).
Skadberg, O. et al. The cardiac troponin response following physical exercise in relation to biomarker criteria for acute myocardial infarction; the North Sea Race Endurance Exercise Study (NEEDED) 2013. Clin. Chim. Acta 479, 155–159. https://doi.org/10.1016/j.cca.2018.01.033 (2018).
Marshall, L. et al. Effect of exercise intensity and duration on cardiac troponin release. Circulation 141, 83–85. https://doi.org/10.1161/circulationaha.119.041874 (2020).
Gresslien, T. & Agewall, S. Troponin and exercise. Int. J. Cardiol. 221, 609–621. https://doi.org/10.1016/j.ijcard.2016.06.243 (2016).
Huang, S. H. et al. The presence of ectopic atrial rhythm predicts adverse cardiovascular outcomes in a large hospital-based population. Heart Rhythm 17, 967–974. https://doi.org/10.1016/j.hrthm.2020.01.024 (2020).
Sajeev, J. K. et al. Association between excessive premature atrial complexes and cryptogenic stroke: Results of a case–control study. BMJ Open 9, e029164. https://doi.org/10.1136/bmjopen-2019-029164 (2019).
Colberg, S. R. Physical activity: the forgotten tool for type 2 diabetes management. Front. Endocrinol. (Lausanne) 3, 70. https://doi.org/10.3389/fendo.2012.00070 (2012).
Kränkel, N. et al. Exercise training to reduce cardiovascular risk in patients with metabolic syndrome and type 2 diabetes mellitus: How does it work?. Eur. J. Prevent. Cardiol. 26, 701–708. https://doi.org/10.1177/2047487318805158 (2019).
Little, J. P., Jung, M. E., Wright, A. E., Wright, W. & Manders, R. J. Effects of high-intensity interval exercise versus continuous moderate-intensity exercise on postprandial glycemic control assessed by continuous glucose monitoring in obese adults. Appl. Physiol. Nutr. Metab. 39, 835–841. https://doi.org/10.1139/apnm-2013-0512 (2014).
Oberlin, D. J. et al. One bout of exercise alters free-living postprandial glycemia in type 2 diabetes. Med. Sci. Sports Exerc. 46, 232–238. https://doi.org/10.1249/MSS.0b013e3182a54d85 (2014).
Wormgoor, S. G., Dalleck, L. C., Zinn, C., Borotkanics, R. & Harris, N. K. High-intensity interval training is equivalent to moderate-intensity continuous training for short- and medium-term outcomes of glucose control, cardiometabolic risk, and microvascular complication markers in men with type 2 diabetes. Front. Endocrinol. (Lausanne) 9, 475. https://doi.org/10.3389/fendo.2018.00475 (2018).
Lang, R. M. et al. Recommendations for cardiac chamber quantification by echocardiography in adults: An update from the American Society of Echocardiography and the European Association of Cardiovascular Imaging. J. Am. Soc. Echocardiogr. 28, 1-39.e14. https://doi.org/10.1016/j.echo.2014.10.003 (2015).
McLester, C. N., Nickerson, B. S., Kliszczewicz, B. M. & McLester, J. R. Reliability and agreement of various inbody body composition analyzers as compared to dual-energy X-ray absorptiometry in healthy men and women. J. Clin. Densitom. 23, 443–450. https://doi.org/10.1016/j.jocd.2018.10.008 (2020).
Acknowledgements
The performance of 4x4-min interval training and testing of VO2max was provided by NeXt Move, Norwegian University of Science and Technology (NTNU). NeXt Move is funded by the Faculty of Medicine at NTNU and Central Norway Regional Health Authority.”
Funding
The Liaison Committee between the Central Norway Regional Health Authority (RHA) and the Norwegian University of Science and Technology (NTNU). No relation to the industry exists. The funding source had no role in the study design, data collection, analysis, interpretation, or manuscript writing. Open access funding provided by Norwegian University of Science and Technology.
Author information
Authors and Affiliations
Contributions
Conceptualization, M.A.H.; methodology: H.O.N., K.L., R.H.G., A.E.T., V.M., H.O.N.I., S.M.H.-S., H.D., M.A.H.; formal analysis, H.O.N., K.L., R.H.G., A.E.T., V.M., H.O.N.I., H.D., M.A.H.; investigation: H.O.N., K.L., R.H.G., A.E.T., V.M., H.O.N.I., S.M.H.-S., H.D., M.A.H.; resources: M.A.H.; writing—original draft preparation: H.O.N., R.H.G.; writing—review and editing: H.O.N., K.L., R.H.G., A.E.T., V.M., H.O.N.I., S.M.H.-S., H.D., M.A.H.; supervision: H.D., M.A.H. project administration, M.A.H.; funding acquisition, M.A.H. All authors have read and agreed to the published version of the manuscript.
Corresponding author
Ethics declarations
Competing interests
The authors declare no competing interests.
Additional information
Publisher's note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if changes were made. The images or other third party material in this article are included in the article's Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article's Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
Ness, H.O., Ljones, K., Gjelsvik, R.H. et al. Acute effects of high intensity training on cardiac function: a pilot study comparing subjects with type 2 diabetes to healthy controls. Sci Rep 12, 8239 (2022). https://doi.org/10.1038/s41598-022-12375-2
Received:
Accepted:
Published:
DOI: https://doi.org/10.1038/s41598-022-12375-2
- Springer Nature Limited