Abstract
Upright computed tomography (CT) provides physiologically relevant images of daily life postures (sitting and standing). The volume of the human airway in sitting or standing positions remains unclear, and no clinical study to date has compared the inspiratory and expiratory airway volumes and luminal areas among standing, sitting, and supine positions. In this prospective study, 100 asymptomatic volunteers underwent both upright (sitting and standing positions) and conventional (supine position) CT during inspiration and expiration breath-holds and the pulmonary function test (PFT) within 2 h of CT. We compared the inspiratory/expiratory airway volumes and luminal areas on CT among the three positions and evaluated the correlation between airway volumes in each position on CT and PFT measurements. The inspiratory and expiratory airway volumes were significantly higher in the sitting and standing positions than in the supine position (inspiratory, 4.6% and 2.5% increase, respectively; expiratory, 14.9% and 13.4% increase, respectively; all P < 0.001). The inspiratory and expiratory luminal areas of the trachea, bilateral main bronchi, and average third-generation airway were significantly higher in the sitting and standing positions than in the supine position (inspiratory, 4.2‒10.3% increases, all P < 0.001; expiratory, 6.4‒12.8% increases, all P < 0.0001). These results could provide important clues regarding the pathogenesis of orthopnea. Spearman’s correlation coefficients between the inspiratory airway volume on CT and forced vital capacity and forced expiratory volume in 1 s on PFT were numerically higher in the standing position than in the supine position (0.673 vs. 0.659 and 0.669 vs. 0.643, respectively); however, no statistically significant differences were found. Thus, the airway volumes on upright and conventional supine CT were moderately correlated with the PFT measurements.
Similar content being viewed by others
Explore related subjects
Discover the latest articles, news and stories from top researchers in related subjects.Introduction
Humans are in an upright (sitting or standing) position during daytime hours; however, most of the 3-dimensional diagnostic imaging techniques, such as magnetic resonance imaging or computed tomography (CT), are performed in a supine position. Thus, the volume of the human airway in the sitting or standing position is still unclear. Chest radiography is the most common imaging examination performed in the upright position1; however, chest radiography provides 2-dimensional images that do not accurately depict the airway volume.
An upright 320-detector-row CT scanner has recently been developed to assess the 3-dimensional anatomy of a human in the upright position2. This upright CT scanner provides physiologically relevant images of daily life postures, such as sitting and standing positions, and enables the acquisition of volume data of the entire chest (isotropic 0.5-mm voxel size) in about 5 seconds3,4. A previous study compared the inspiratory and expiratory lung and lobe volumes among standing, sitting, and supine positions3. However, to the best of our knowledge, no clinical study to date has compared both the inspiratory and expiratory airway volumes and luminal areas among the three positions. We hypothesized that the inspiratory and expiratory airway volumes and luminal areas will be different between the upright (sitting and standing) and supine positions because of the different directions of gravity in relation to the chest in these positions. We also hypothesized that upright CT airway volume will be more strongly associated than supine CT with the measurements on the pulmonary function test (PFT) because the PFT is performed in the upright position.
The purpose of this study was to compare the inspiratory and expiratory airway volumes and luminal areas on CT among the standing, sitting, and supine positions and to determine the correlation between the airway volumes in each position on CT and measurements on the PFT.
Methods
Study population
This prospective study was approved by the Keio University School of Medicine Ethics Committee (No. 20160384). All participants provided written informed consent (UMIN Clinical Trials Registry [UMIN-CTR]: UMIN000026586). All methods were performed in accordance with the relevant guidelines and regulations. In addition, informed consent was obtained to publish the images in an online open access publication. From June 2017 to August 2018, 100 asymptomatic volunteers from a volunteer recruitment company were enrolled in this study. To ensure that normal whole-body anatomy was evaluated, volunteers with a history of diabetes, dyslipidemia, hypertension, dysuria, and smoking; those who had any type of symptoms; those who were pregnant or possibly pregnant; and those who were currently undergoing treatment or had undergone surgery were excluded from the study. The data of the 100 included volunteers had been analyzed for different purposes in a previous study that evaluated lung and lobe volumes3 but not airway volume.
CT imaging protocol
All participants underwent both upright body trunk low-radiation-dose CT in standing (Fig. 1A) and sitting positions with arms down at their sides (Fig. 1B), performed using an upright 320-detector-row CT (prototype TSX-401R, Canon Medical Systems, Otawara, Japan)2,3,4, and conventional body trunk low-radiation-dose CT in the supine position with arms raised (Fig. 1C), performed using a 320-detector-row CT (Aquilion ONE, Canon Medical Systems), within 2 h on the same day. The participants were scanned in the three positions during both deep-inspiration breath-hold and expiration breath-hold (at the end-tidal expiration, near functional residual capacity on PFT), as described in previous studies3,5. The order of standing, sitting and supine CT was not randomized.
Upright CT examination in the standing position (A), upright CT examination in the sitting position (B), and conventional CT examination in the supine position (C). Upright CT examinations in the standing position (A) and sitting position (B) were performed with the subject’s arms down during both deep inspiration breath-hold and expiration breath-hold. Conventional CT in the supine position (C) was performed with the subject’s arms raised during both deep inspiration breath-hold and expiration breath-hold. CT computed tomography.
All CT examinations were unenhanced and performed with automatic exposure control using a noise index of 24 for a slice thickness of 5 mm (tube current range, 10–350 mA)3. Other scanning parameters were the same for standing, sitting, and supine CT scans: peak tube voltage, 100 kVp; rotation speed, 0.5 s; slice collimation, 0.5 mm × 80; and pitch factor, 0.8133. The series of contiguous 0.5-mm-thick images was reconstructed with Adaptive Iterative Dose Reduction 3D (Canon Medical Systems)6.
Pulmonary function test
All participants underwent PFTs within 2 h of CT examinations on the same day. The PFT was performed with the participants in a stable condition while sitting, using a spirometer (Chestac-8900, Chest M.I., Tokyo, Japan) in accordance with ATS/European Respiratory Society recommendations7,8. The total lung capacity and residual volume were measured using the multi-breath helium dilution method. The predicted values of the spirometric measurements were derived from the guidelines of the Japanese Respiratory Society9.
Airway volume measurements on CT
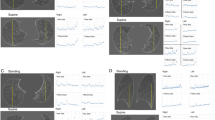
Airway volume measurements for all 100 volunteers in the three positions were performed by two radiologists, in consensus, with 15 (Y.YA.) and 7 (Y.YO.) years of experience using a commercially available workstation (Synapse Vincent, Fuji Film Co., Ltd., Tokyo, Japan)3,4,10,11,12,13,14,15. This workstation incorporates a computer-aided detection system and automatically extracts the entire airway tree (from the trachea to all bilateral airways with lumen diameters of more than approximately 1.5 mm), which was defined as the airway volume (Fig. 2)3,4,10,11,12,13,14,15. In addition, all branches of the third- to sixth-generation airways in all segments were manually identified by tracking from the third to sixth generation13,15,16. The cross-sectional images perpendicular to the longitudinal center line of the lumen were generated for each branch, and the luminal areas in the middle-third portion were automatically measured and averaged10,13,15. The mean luminal area for each generation airway was calculated in all segments10,15. All measurements were performed in a blinded and randomized manner. During all the measurements, the radiologists were also blinded to patient characteristics and PFT results. The airway volume changes from expiration to inspiration on CT, and the ratio of inspiratory airway volume to expiratory airway volume were calculated.
Statistical analysis
The data are presented as mean ± standard deviation. A paired t test was performed to analyze the differences in the airway volumes and luminal areas among standing, sitting, and supine positions; the differences in the airway volume changes from expiration to inspiration among the three positions; and the differences in the ratio of inspiratory airway volume to expiratory airway volume among the three positions. Bonferroni correction was used for multiple comparisons. The difference in age between women and men was assessed using Student’s t test. The associations between the airway volumes on CT in each position and the measurements on the PFT were evaluated using Spearman’s rank correlation test. Paired correlation coefficients (PFT measurements vs. airway volumes on CT among the three positions) were compared using a mixed-effect model with Bonferroni correction for multiple comparisons (e.g. across all PFT measurements and three positions). The significance level for all tests was 5% (two-sided). All data were analyzed using a commercially available software program (JMP version 12; SAS Institute Inc, Cary, NC, USA).
Results
Participant characteristics
The clinical characteristics of all the participants (n = 100) are shown in Table 1. No significant difference was found in age between the men and women (44.9 ± 10.0 years vs. 48.0 ± 11.9 years, P = 0.210).
Airway volumes on CT in standing, sitting, and supine positions
The inspiratory airway volumes were significantly higher in the sitting and standing positions than in the supine position (4.6% and 2.5% increase, respectively; both P < 0.004) (Table 2). The expiratory airway volumes were significantly higher in the sitting and standing positions than in the supine position (14.9% and 13.4% increase, respectively; both P < 0.0001). The inspiratory airway volumes were significantly higher in the sitting position than in the standing position (2.0%; P = 0.0072). No significant difference was found in the expiratory airway volumes between the sitting and standing positions (P = 0.0898).
Airway volume changes from expiration to inspiration on CT in standing, sitting, and supine positions
The airway volume changes from expiration to inspiration in the sitting and standing positions were significantly lower than those in the supine position (17.0 ± 7.8 and 16.3 ± 7.3 mL, respectively vs. 20.1 ± 10.4 mL; both P < 0.0001). No significant difference was found in the airway volume change from expiration to inspiration between the sitting and standing positions (P = 0.2181).
Ratio of inspiratory airway volume to expiratory airway volume in standing, sitting, and supine positions
The ratios of inspiratory airway volumes to expiratory airway volumes in the sitting and standing positions were significantly lower than those in the supine position (1.40 ± 0.18 and 1.39 ± 0.19, respectively vs. 1.53 ± 0.25; both P < 0.0001). No significant difference was found in the ratio of inspiratory airway volume to expiratory airway volume between the sitting and standing positions (P = 0.9359).
Airway luminal areas on CT in standing, sitting, and supine positions
The inspiratory airway luminal areas of the trachea, bilateral main bronchi, and average third-, fourth-, fifth-, and sixth-generation airway were significantly higher in the sitting and standing positions than those in the supine position (4.2‒11.0% increases, all P < 0.006) (Table 3). The expiratory luminal areas of the trachea, bilateral main bronchi, and average third-generation airway were significantly higher in the sitting and standing positions than those in the supine position (6.4‒12.8% increases, all P < 0.0001) (Table 3). No significant differences were found in the inspiratory or expiratory airway luminal areas of the trachea, bilateral main bronchi, or average third-, fourth-, fifth-, or sixth-generation airways between the sitting and standing positions (Table 3).
Associations between airway volumes on CT in standing, sitting, and supine positions and measurements on PFT
Spearman’s coefficients (ρ) for the correlation between airway volumes on CT and measurements on the PFT are shown in Table 4. The coefficients for the correlation between the inspiratory airway volumes on CT and the measurements on the PFT were numerically higher in the standing position than in the supine position, with regard to vital capacity (0.681 vs. 0.660), forced vital capacity (0.673 vs. 0.659), forced expiratory volume in 1 s (0.669 vs. 0.643), inspiratory capacity (0.640 vs. 0.632), residual volume (0.558 vs. 0.546), functional residual capacity (0.607 vs. 0.585), and total lung capacity (0.726 vs. 0.709) (Table 4); however, no significant differences were found among these correlation coefficients between the standing and supine positions (all P > 0.0797). The coefficients for the correlation between the inspiratory airway volumes on CT and the measurements on the PFT were numerically higher in the sitting position than in the supine position, with regard to vital capacity (0.667 vs. 0.660), forced vital capacity (0.662 vs. 0.65), residual volume (0.573 vs. 0.546), functional residual capacity (0.629 vs. 0.585), and total lung capacity (0.721 vs. 0.709) (Table 4); however, no significant differences were found among these correlation coefficients between the sitting and supine positions (all P > 0.0938). The correlation coefficients between the inspiratory airway volumes on CT and the measurements on the PFT were numerically higher in the supine position than in the sitting position, with regard to forced expiratory volume in 1 s (0.643 vs. 0.641) and inspiratory capacity (0.632 vs. 0.604) (Table 4); however, no significant differences were found in these two correlation coefficients between the supine and sitting positions (all P > 0.3922).
Discussion
To the best of our knowledge, this is the first study to show the differences in the airway volumes on CT among standing, sitting, and supine positions. Our study showed that the inspiratory and expiratory airway volumes as well as luminal areas of the trachea, bilateral main bronchi, and average third-generation airway were significantly higher in the sitting and standing positions than in the supine position. These findings are noteworthy because the results could provide important clues regarding the pathogenesis of orthopnea. In patients with chronic obstructive pulmonary disease (COPD), breathing discomfort can become amplified in the supine position (i.e. orthopnea)17,18. However, the precise mechanisms of orthopnea are still unknown18. Eltayara et al. reported that increased airway resistance in the supine position due to a lower end-expiratory lung volume probably plays a role in the genesis of orthopnea17. Considering our results, the increased airway resistance in the supine position due to a lower expiratory airway volume could also play a role in the development of orthopnea.
One possible reason for the difference in airway volume and luminal area between the upright (sitting and standing positions) and supine positions would be due to the difference in the direction of gravity. Several previous studies have reported that gravity affects the airway and chest19,20,21,22,23,24. Beaumont et al. reported that gravity affects the airway area and lung volume during parabolic flight using the acoustic reflection method and inductance plethysmography19. Elliott et al. evaluated the effect of spaceflight on sleep-disordered breathing and concluded that gravity plays an important role in the genesis of apneas, hypopneas, and snoring in healthy subjects20. In addition, it has been reported that gravity is associated with atelectasis22 and affects the chest wall mechanics23,24.
Our study also showed that the correlations between the inspiratory airway volume on CT and the measurements on the PFT tended to be higher in the standing position than in the supine position, although no statistically significant differences were found. This may be because PFTs are conducted in the upright position, and the direction of the thorax in PFTs corresponds to that in the upright CT rather than that in the conventional supine CT3,4,25. Furthermore, it is reported that the body position influences the results of PFTs26,27,28.
A previous study reported that the inspiratory airway luminal areas of the trachea, bilateral main bronchi, and average third-generation airway were larger in the standing than in the supine position15. Our results were, to some extent, consistent with these results; however, our study firstly evaluated inspiratory and expiratory airway luminal areas in the sitting position, the expiratory airway luminal areas in the upright position in an asymptomatic volunteer cohort, and the volume of the whole airway with lumen diameters of more than approximately 1.5 mm, which would be more reflective of the overall condition of the airway. Another previous study reported that the airway volume in the right upper and middle-lower lobes on conventional supine CT were correlated with the forced expiratory volume in 1 s in patients with COPD (correlation coefficient, 0.41)14; however, the authors assessed only the airway volume in the right lung and did not assess the left airway. We believe that measuring only the right airway may not allow overall lung function to be assessed. Actually, the correlation coefficient between the airway volume (whole bilateral airway) in the standing position and the forced expiratory volume in 1 s in this study was 0.669, relatively higher than that in the previous study (0.41)14. Whole airway volume in the standing position could be used as a new clinical indicator to evaluate the therapeutic effect or disease severity, and future studies investigating the correlation between airway volumes on upright CT and clinical findings in patient cohorts are needed.
The current study had some limitations. First, we included only 100 asymptomatic participants at a single institution, and further studies with large samples sizes at multiple centers are required to confirm these preliminary findings. Second, in this study, although the radiologists evaluated the CT images in a blinded and randomized manner, they could recognize, to some extent, the positions of the participants because of the presence or absence of a CT scanner table. However, the airway volume measurements were automated by using a commercially available workstation; thus, observer bias is considered to be negligible4. Third, conventional supine CT was performed with the arms raised in this study, whereas upright (standing and sitting) CT was performed with the arms down; thus, the form of the chest would have been slightly different between the upright and supine positions, which may have influenced the results of this study. However, we believe that standing or sitting with the arms down is the natural standing or sitting posture for human beings.
Conclusions
The inspiratory and expiratory airway volumes and luminal areas of the trachea, bilateral main bronchi, and average third-generation airway were significantly higher in the sitting and standing positions than in the supine position, which could provide important clues regarding the pathogenesis of orthopnea. The airway volumes on both upright and conventional supine CT were moderately correlated with the PFT measurements.
Data availability
The datasets generated during and/or analyzed during the current study are available from the corresponding author on reasonable request.
References
Schaefer-Prokop, C., Neitzel, U., Venema, H. W., Uffmann, M. & Prokop, M. Digital chest radiography: An update on modern technology, dose containment and control of image quality. Eur. Radiol. 18, 1818–1830. https://doi.org/10.1007/s00330-008-0948-3 (2008).
Jinzaki, M. et al. Development of upright computed tomography with area detector for whole-body scans: Phantom study, efficacy on workflow, effect of gravity on human body, and potential clinical impact. Investig. Radiol. 55, 73–83. https://doi.org/10.1097/RLI.0000000000000603 (2020).
Yamada, Y. et al. Comparison of inspiratory and expiratory lung and lobe volumes among supine, standing and sitting positions using conventional and upright CT. Sci. Rep. 10, 16203. https://doi.org/10.1038/s41598-020-73240-8 (2020).
Yamada, Y. et al. Differences in lung and lobe volumes between supine and standing positions scanned with conventional and newly developed 320-detector-row upright CT: Intra-individual comparison. Respiration 99, 598–605. https://doi.org/10.1159/000507265 (2020).
Bhatt, S. P. et al. Association between expiratory central airway collapse and respiratory outcomes among smokers. JAMA 315, 498–505. https://doi.org/10.1001/jama.2015.19431 (2016).
Yamada, Y. et al. Dose reduction in chest CT: Comparison of the adaptive iterative dose reduction 3D, adaptive iterative dose reduction, and filtered back projection reconstruction techniques. Eur. J. Radiol. 81, 4185–4195. https://doi.org/10.1016/j.ejrad.2012.07.013 (2012).
Miller, M. R. et al. Standardisation of spirometry. Eur. Respir. J. 26, 319–338. https://doi.org/10.1183/09031936.05.00034805 (2005).
Graham, B. L. et al. Standardization of spirometry 2019 update. An Official American Thoracic Society and European Respiratory Society Technical Statement. Am. J. Respir. Crit. Care Med. 200, e70–e88. https://doi.org/10.1164/rccm.201908-1590ST (2019).
The Committee of Pulmonary Physiology JRS. Forced expiratory curve, flow volume curve and peak flow. In The Clinical Respiratory Function Test (eds. The Committee of Pulmonary Physiology JRS) 312–321 (Medical Review, 2016).
Chubachi, S. et al. Differences in airway lumen area between supine and upright computed tomography in patients with chronic obstructive pulmonary disease. Respir. Res. 22, 95. https://doi.org/10.1186/s12931-021-01692-1 (2021).
Iwano, S. et al. Pulmonary lobar volumetry using novel volumetric computer-aided diagnosis and computed tomography. Interact. Cardiovasc. Thorac. Surg. 17, 59–65. https://doi.org/10.1093/icvts/ivt122 (2013).
Kitano, M. et al. Lobar analysis of collapsibility indices to assess functional lung volumes in COPD patients. Int. J. Chron. Obstruct. Pulmon. Dis. 9, 1347–1356. https://doi.org/10.2147/copd.s72616 (2014).
Tanabe, N. et al. Direct evaluation of peripheral airways using ultra-high-resolution CT in chronic obstructive pulmonary disease. Eur. J. Radiol. 120, 108687. https://doi.org/10.1016/j.ejrad.2019.108687 (2019).
Tanabe, N. et al. Associations of airway tree to lung volume ratio on computed tomography with lung function and symptoms in chronic obstructive pulmonary disease. Respir. Res. 20, 77. https://doi.org/10.1186/s12931-019-1047-5 (2019).
Matsumoto, S. et al. Difference in the airway luminal area between the standing and supine positions using upright and conventional computed tomography. Clin. Anat. 34, 1150–1156. https://doi.org/10.1002/ca.23763 (2021).
Nishimoto, K. et al. Relationship between fraction of exhaled nitric oxide and airway morphology assessed by three-dimensional CT analysis in asthma. Sci. Rep. 7, 10187. https://doi.org/10.1038/s41598-017-10504-w (2017).
Eltayara, L., Ghezzo, H. & Milic-Emili, J. Orthopnea and tidal expiratory flow limitation in patients with stable COPD. Chest 119, 99–104. https://doi.org/10.1378/chest.119.1.99 (2001).
Elbehairy, A. F. et al. Mechanisms of orthopnoea in patients with advanced COPD. Eur. Respir. J. 57, 2000754. https://doi.org/10.1183/13993003.00754-2020 (2021).
Beaumont, M. et al. Gravity effects on upper airway area and lung volumes during parabolic flight. J. Appl. Physiol. 84, 1639–1645. https://doi.org/10.1152/jappl.1998.84.5.1639 (1998).
Elliott, A. R. et al. Microgravity reduces sleep-disordered breathing in humans. Am. J. Respir. Crit. Care Med. 164, 478–485. https://doi.org/10.1164/ajrccm.164.3.2010081 (2001).
Joosten, S. A., O’Driscoll, D. M., Berger, P. J. & Hamilton, G. S. Supine position related obstructive sleep apnea in adults: Pathogenesis and treatment. Sleep Med. Rev. 18, 7–17. https://doi.org/10.1016/j.smrv.2013.01.005 (2014).
Woodring, J. H. & Reed, J. C. Types and mechanisms of pulmonary atelectasis. J. Thorac. Imaging 11, 92–108. https://doi.org/10.1097/00005382-199621000-00002 (1996).
Bettinelli, D. et al. Effect of gravity on chest wall mechanics. J. Appl. Physiol. 92, 709–716. https://doi.org/10.1152/japplphysiol.00644.2001 (2002).
Liu, S. B., Wilson, T. A. & Schreiner, K. Gravitational forces on the chest wall. J. Appl. Physiol. 70, 1506–1510. https://doi.org/10.1152/jappl.1991.70.4.1506 (1991).
Yamada, Y. et al. Comparison of lung, lobe, and airway volumes between supine and upright computed tomography and their correlation with pulmonary function test in patients with chronic obstructive pulmonary disease. Respiration. 101, 1110–1120. https://doi.org/10.1159/000527067 (2022).
Blair, E. & Hickam, J. B. The effect of change in body position on lung volume and intrapulmonary gas mixing in normal subjects. J. Clin. Investig. 34, 383–389. https://doi.org/10.1172/jci103086 (1955).
Katz, S., Arish, N., Rokach, A., Zaltzman, Y. & Marcus, E. L. The effect of body position on pulmonary function: A systematic review. BMC Pulm. Med. 18, 159. https://doi.org/10.1186/s12890-018-0723-4 (2018).
Meysman, M. & Vincken, W. Effect of body posture on spirometric values and upper airway obstruction indices derived from the flow-volume loop in young nonobese subjects. Chest 114, 1042–1047. https://doi.org/10.1378/chest.114.4.1042 (1998).
Acknowledgements
This study was supported by Japan Society for the Promotion of Science (JSPS) KAKENHI (grant numbers JP17H04266, JP17K16482, and JP20K08056), Uehara Memorial Foundation, Takeda Science Foundation, and Canon Medical Systems (Otawara, Japan). The authors would like to acknowledge all of the volunteers for their willingness to participate in the study. The authors thank Dr. Keiichi Narita, Dr. Takehiro Nakahara, Naomi Tamaki, Yoko Tauchi, and Kyoko Komatsu for their valuable assistance.
Author information
Authors and Affiliations
Contributions
Y.Yamada, M.Y., and M.J. were responsible for the conception or design of the work; Y.Yamada, M.Y., Y.Yokoyama, S.M., A.T. and Y.N. were responsible for the acquisition of data; Y.Yamada, M.Y., S.C., Y.Yokoyama and T.A. analyzed and interpreted the data; and Y.Yamada, M.Y., S.C., Y.Yokoyama, S.M., A.T., Y.N., M.M., T.A., K.F. and M.J. drafted and revised the paper for important intellectual content. All authors have approved the manuscript for submission.
Corresponding authors
Ethics declarations
Competing interests
Masahiro Jinzaki received a grant from Canon Medical Systems. However, Canon Medical Systems was not involved in the design and conduct of the study; in the collection, analysis, and interpretation of the data; or in the preparation, review, and approval of the manuscript. The remaining authors (Y.Yamada, M.Y., S.C., Y.Yokoyama, S.M., A.T., Y.N., M.M., T.A., and K.F.) have no conflicts of interest to declare.
Additional information
Publisher's note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if changes were made. The images or other third party material in this article are included in the article's Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article's Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
Yamada, Y., Yamada, M., Chubachi, S. et al. Comparison of inspiratory and expiratory airway volumes and luminal areas among standing, sitting, and supine positions using upright and conventional CT. Sci Rep 12, 21315 (2022). https://doi.org/10.1038/s41598-022-25865-0
Received:
Accepted:
Published:
DOI: https://doi.org/10.1038/s41598-022-25865-0
- Springer Nature Limited
This article is cited by
-
Differences in lung attenuation gradients between supine and standing positions in healthy participants on conventional/supine and upright computed tomography
Scientific Reports (2024)
-
Upright CT-based evaluation of the effects of posture on skull-base reconstruction after endoscopic endonasal surgery
Scientific Reports (2024)