Abstract
Pregnant women are at high risk for iron deficiency anemia due to increased nutrient requirements during pregnancy. Despite high coverage of iron and folic acid supplementation (IFAS), low compliance is reported. The study aimed to assess compliance with IFAS and its associated factors among antenatal care (ANC) attendees in Wondo District, Southern Ethiopia. A facility-based cross-sectional study was conducted among 400 pregnant women. Pregnant women were selected through systematic random sampling. Pre-tested structured questionnaire was used to collect data through face to face interview. Data were entered into Epi-info and exported to Statistical Package for Social Sciences for analysis. The variables with p-value < 0.25 in the bivariable analysis were entered into the multivariable logistic regression model. P values less than 0.05 were considered significant. Results were reported as crude and adjusted odds ratios with 95% confidence intervals. The prevalence of compliance to IFAS was (177, 44.3%). Factors significantly associated with compliance to IFAS were maternal age ≥ 25 years [AOR 2.27, 95% CI (1.21, 4.28)], maternal education [AOR 2.62, 95% CI (1.43, 4. 79)], husband's education [AOR 3.60, 95% CI (2.07, 6.25)], knowledge of anemia [AOR 4.40, 95% CI (2.65, 7.30)], and knowledge of IFA [AOR 2.21, 95% CI (1.40, 3.50)]. This study showed that compliance to IFAS was low. Maternal age, maternal education, husband's education, knowledge about anemia and iron folic acid was found to be significantly associated with adherence to IFAS. Emphasis should be placed on young, uneducated mothers and their husbands.
Similar content being viewed by others
Explore related subjects
Discover the latest articles, news and stories from top researchers in related subjects.Introduction
Compliance refers to the act of conforming to the recommendations made by the provider with respect to timing, dosage, and frequency of medication taking. Therefore, compliance is the extent to which a client acts in accordance with the prescribed interval and dose of a dosing regimen1. Anemia is a condition in which the oxygen-carrying capacity of red blood cells is insufficient to meet the physiological needs of the body2. It is a global public health problem affecting nearly two billion people, despite the global introduction of iron and folic acid and their provision through antenatal care programs3. It affects more than 32 million pregnant women worldwide and contributes to 20% of maternal deaths4 Iron deficiency is the most common and widespread nutritional disorder in the world and is a major public health problem in both developed and developing countries5. Pregnant women in particular are at high risk for iron deficiency anemia due to their high nutrient requirements during pregnancy6. Preventive measures include daily iron and folic acid supplementation to reduce the risk of low birth weight, neural tube defects, and maternal anemia and iron deficiency during pregnancy7.
Globally, an estimated 41.8% of pregnant women are anemic, and at least half of this burden is thought to be due to iron deficiency, with the remainder due to conditions such as folate, vitamin B12 or vitamin A deficiency, chronic inflammation, parasitic infections and inherited disorders7. Iron deficiency anemia during pregnancy is associated with an increased risk of low maternal weight gain, preterm labor and placenta previa, premature rupture of membranes, cardiac arrest and bleeding, decreased resistance to infection, poor cognitive development, and reduced work capacity6,8. Similarly, the effects of iron deficiency anemia on the fetus and newborn are increased risk of prematurity, low birth weight, and fetal distress, which contribute to perinatal morbidity and mortality6,9,10,11.
Iron supplementation has been a major strategy in low and middle-income countries including Ethiopia to reduce iron deficiency anemia during pregnancy12. In Ethiopia, IFA is supplemented free of charge during antenatal care follow up. Despite the implementation of IFAS in Ethiopia, anemia remains responsible for the majority of maternal morbidity and mortality13. Therefore, compliance to IFAS is critically needed. Compliance to iron and folic acid supplementation (IFAS) is defined based on the woman's self-report of the number of IFA tablets taken in the previous 7 days, which was used as a proxy estimate of recommended (90 + days) iron folic acid compliance. In this case, pregnant mothers who took ≥ 4 tablets per week were considered compliant14.
National Nutrition Program II is being designed and implemented in Ethiopia to prevent and treat anemia during pregnancy15. This program aims to reduce the prevalence of anemia in pregnant women from 22 to 14% by 2020. This goal includes providing iron sulfate and folic acid to all pregnant women16. According to the national standard, the recommended dose in Ethiopia is 300–325 mg of ferrous sulfate and 400 µg of folic acid once a day for at least 90 days of prenatal period, preferably with a meal12. But as the national data and most studies show, compliance is still below the standard. For example, the 2019 Ethiopia Mini Demographic Health Survey (EMDHS) report found that among 3,927 pregnant women in the past five years, 60% took iron folic acid (IFA) tablets during pregnancy, and 11% took them for the recommended period of 90 or more days17.
Recent studies conducted in Ethiopia have reported prevalence of IFAS compliance ranging from 38.3% in Shala District18 to 92.4% in Robe town Southeast Ethiopia19. However, the Kanungu District study in Uganda reported the lowest prevalence of 22.37% compared to the most recent studies conducted in Ethiopia20. This shows the variation from one location to another in Ethiopia and the huge differences from country to country, which necessitates site-specific prevalence studies.
Previous studies have shown that education, maternal age, family income, place of residence, early initiation of ANC, frequency of ANC, history of anemia, counseling for IFAS during pregnancy, knowledge of anemia, and knowledge of IFAS were associated with adherence compliance to IFAS8,21,22,23,24,25,26,27,28. However, recent studies conducted in Ethiopia and Uganda found no significant association between sociodemographic variables and IFAS adherence18,20,29,30. Nevertheless, socio-demographic variables are important determinants of compliance to IFAS as shown in the previous studies.
According to the Wondo District Health Office statistics report, the level of iron and folic acid supplementation among pregnant women in the district was 99%. However, the level of compliance with IFA in the district has not yet been assessed. Determining the level of compliance with IFA and identifying the factors responsible for compliance in the district could make a significant contribution to improving the health status of pregnant women and newborns. Therefore, this study aimed to assess the compliance with IFAS and its associated factors among pregnant women in Wondo District of Oromia, Southern Ethiopia.
Methods
Study setting, period and participants
A facility-based cross-sectional study was conducted among pregnant women in Wondo District, Southern Ethiopia. According to district health office administrative report, the total number of women of reproductive age groups and pregnant women in the district were estimated to be 26,183 and 4,105 respectively. Among pregnant women attending ANC clinic at health centers, 97% were supplemented with IFA tablet31. The study was conducted from August 16 to October 30, 2019.
All pregnant women attending ANC and previously supplemented with iron and folic acid tablets at the facilities at least one week prior to the data collection period were our source population. Pregnant women who were previously supplemented with iron and folic acid tablets at least one week prior to data collection, who came to the health facility during the data collection period, were systematically selected for the study population.
Inclusion and exclusion criteria
Inclusion criteria for this study were pregnant women who had at least one ANC visit at a health facility and were supplemented with IFA tablets at least one week prior to data collection.
Pregnant women who came for the first antenatal visit, those who could not hear and/or speak and those with mental disorder were excluded from the study.
Sample size determination and Sampling procedure
The minimum sample size required was calculated using the single population proportion formula, assuming 95% CI, 5% margin of error, and a proportion of 39.2% from the study in Misha district of Hadiya zone23. Finally, considering 10% for possible non-response, a sample size of 402 was estimated to meet the objectives.
The study was conducted in three health centers namely Busa, Shasha and Bachil located in Wondo district. Out of 853 pregnant mothers attending ANC clinic in the three health centers, 830 (97%) were supplemented with IFA within two months and fifteen days. The calculated sample was distributed among these health centers in proportion to the number of women attending ANC and supplemented IFA during the data collection period. Finally, systematic random sampling technique was used to include 402 participants in the study using the interval (K = 2) for each health center. Lottery method was used to select the random starting number and 1 was drawn and odd numbers of participants were interviewed after receiving ANC service.
Data collection
Data were collected using a structured questionnaire adapted from a study conducted in Dabre Tabor General Hospital32. It consisted of six parts: socio-demographic characteristics of participants, pregnancy and health status characteristics, knowledge of IFA supplementation, compliance question, knowledge of anemia, health facility related factor (S2). Knowledge questions were checked for reliability and the result of Cronbach's alpha was equal to 0.7.
Measurement of variables
Our dependent variable for the current study was IFAS compliance, which is a dichotomous variable.
Compliance
This was measured based on the woman's self-report of the number of IFA tablets taken in the previous 7 days, which was used as a proxy estimate of recommended (90 + days) iron folic acid compliance. In this case, pregnant mothers who took ≥ 4 tablets per week were considered compliant14.
Knowledge of anemia
Women's knowledge of anemia was assessed by five multiple-choice questions asking about signs and symptoms of anemia, possible causes of anemia, groups susceptible to anemia, and prevention of anemia. The correct answer for each item was scored as "1" and the incorrect answer was scored as "0". The items were then summed and the mean was calculated. If the pregnant women scored above the mean, they have good knowledge and if the pregnant women scored below the mean, they have poor knowledge27.
Knowledge of IFAs
Women's knowledge of IFA supplementation was assessed by four multiple-choice questions asking about the benefits of IFA, frequency of use, duration of use, and side effects. The correct answer for each item was scored as "1" and the incorrect answer was scored as "0". The items were then summed and the mean was calculated. If the pregnant women scored above the mean, they had good knowledge and if the pregnant women scored below the mean, they had poor knowledge27.
Data analysis
Data were checked for completeness and consistency, coded and entered into EPI-info version 7.2 and exported to SPSS version 21 for analysis. Univariate analysis was performed for each variable by describing frequencies (percentages) for categorical variables and means (standard deviation) for continuous variables. Binary logistic regression analysis was performed for each independent variable with the outcome variable. A variable with a p-value < 0.25 in the bivariate test was considered a candidate for multivariable logistic regression analysis. Finally, a multivariable logistic regression model was performed to determine the independent variables of IFA compliance status. Adjusted odds ratios with corresponding 95% confidence intervals were calculated to determine the strength of the association. All tests were two-tailed and a p-value < 0.05 was considered statistically significant.
Ethics approval and consent to participate
Prior to the actual data collection process, the Madda Walabu University Ethical Review Committee approved the study protocol with reference number MWU/950/12 E.C. Additional written permission was obtained from the West Arsi Zonal Health Office and the Wondo District Health Office on a step-by-step basis. Subjects were informed of the purpose of the study and were assured of privacy and confidentiality of their responses. Written informed consent was obtained from all the participants and or their legal guardians. Assent was obtained from women under 18 years of age, and their husbands were asked for consent. The study adhered to the tenets of the Declaration of Helsinki.
Results
Socio-demographic characteristics
A total of 400 participants were involved in the study with a response rate of 99%. The reason for non-response was refusal. The age of the study participants ranged from 16 to 43 years with a mean age of 28.68 (± 5.89 SD) years. Most had no formal education (185, 46.2%), lived in rural areas (301, 75.3%), and were Protestant in religion (183, 45.8%). Almost three quarters (296, 74.0%) of the study participants had more than 6 family members (Table 1).
Obstetrics and health related characteristics
Among the respondents, (220, 55%) were tested for anemia and (48, 21.8%) of them were anemic during the current pregnancy. Most of the pregnant women, (249, 62.2%) visited antenatal care follow-up for 3–4 times, while (151, 37.8%) had 2 antenatal care visits in the health institution during the current pregnancy.
Knowledge status of respondents on Anemia and Benefit of IFAS
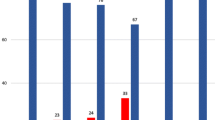
About (222, 55.5%) of the respondents had good knowledge about anemia whereas (178, 44.5%) had poor knowledge about anemia. Regarding the knowledge about the benefits of IFAS, (213, 53.2%) of the respondents had good knowledge while (187, 46.8%) had poor knowledge about IFAS. (Fig. 1).
Health facility related characteristics
More than half (210, 52.5%) were counseled on IFA during their visits. The majority (222, 55.5%) of respondents needed 30 min or less to reach the nearest health facility from their home (Table 2).
Compliance status to IFA supplementation
From the total of 400 participants enrolled in this study, (117, 44.3%) with 95% CI of (39.0%, 50.0%) of the pregnant women were compliant with IFA, that is, took IFA tablets for ≥ 4 days/week in the previous one week before the study.
Factors associated with compliance to IFA among pregnant women
Binary and multivariable logistic regression was done to identify factors associated with compliance to IFA supplementation. First, sixteen factors were analyzed by using binary logistic regression. Among them, maternal age ≥ 25 years [COR 2.47, 95% CI (1.45,4.18)], maternal primary education [COR 1.91, 95% CI (1.50,3.16)], husband primary education [COR 2. 77, 95% CI (1.70,4.52)], husband's secondary education and above [COR 2.38, 95% CI (1.42,3.99)], counseling on IFA [COR 1.28, 95% CI (0.86,1.90)], knowledge of IFA [COR 2. 08 95% CI (1.39,3.12)], knowledge of anemia [COR 3.2795% CI (2.15,4.97)], gestational age at 1st ANC [COR 1.28, 95% CI (0.87,1.91)], number of ANC visits [COR 1. 60, 95% CI (1.06,2.42)] and time from home to health facility [COR 1.27, 95% CI (0.85,1.89)] had p-value < 0.25 and were selected for multivariable analysis.
Multivariable analysis revealed that five predictors were significantly associated with IFA supplementation. Pregnant mothers whose age was ≥ 25 years were 2.27 times more likely to adhere to IFAS than pregnant mothers whose age was < 25 years (AOR 2.27, 95% CI (1.21, 4.28)). The odds of compliance to IFAS were 2.62 times higher among participants whose educational status was primary education [AOR 2.62, 95% CI (1.43, 4.79)] compared to study participants who were illiterate. And those study participants whose husbands had an educational status of primary education were 3.60 [AOR 3.60, 95% CI (2.07, 6.25)] and secondary education and above were 2.52 [AOR 2.52, 95% CI (1.40, 4.52)] times more likely to comply with IFAS as compared to those study subjects whose husbands had no formal education. Pregnant mothers who had good knowledge about IFA supplementation were 2.21 times more likely to be compliant with IFA supplementation as compared to those who had poor knowledge about IFA supplementation (AOR 2.21, 95% CI (1.40, 3.50)). Pregnant mothers who had good knowledge about anemia were 4.40 times more likely to comply with IFA supplementation compared to those who had poor knowledge (AOR 4.40, 95% CI (2.65, 7.30)) (Table 3).
Discussion
This study was conducted to assess compliance with IFAS and identify factors associated with it among pregnant women in Wondo District of Oromia Region. Among 400 pregnant women who participated in the study, (177, 44.3%) were compliant to IFA supplementation. This finding is higher than the findings of the study conducted in Mecha District, Northwest Ethiopia (20.4%)27, Afar Region, Mille and Assaita Districts 22.9%33, Shalla district 38.3%18, Lay Armachiho Health Centers (28.5%)22 and the study conducted in Kanungu District, Uganda (22.37%)20. This may be related to increased knowledge of pregnant women about anemia and IFA supplementation over time. The educational level of the study participants and their husbands may also have increased compliance in our study. On the other hand, the result of compliance with IFA found in this study was lower than the result found in Assella city which was 59.8%, which was 59.8%16 , the study in Burji district Segen zone 51.4%14, Zinder 68%8, Simada district , North West Ethiopia (67.6%)29, Debay Tilat Gen district North West Ethiopia (52.8)34, Dire Dawa city (71.8%)30and the study done in South India 64.7%35. This inconsistency may be due to cultural, socioeconomic, and geographic differences from place to place. For example, in the Diredawa study, slightly less than half of the participants were government employees, and being an employee may have increased their awareness of IFA30. Another reason may be that the majority of our study participants were from rural areas and pregnant women may not receive information from the health center, and women in rural areas were probably less educated than those in urban areas. The timing of the study is another possible reason for the observed difference.
This study revealed that maternal educational status had a significant association with compliance to IFAS. Pregnant women with primary education were 2.62 times more likely to adhere to IFAS than pregnant women with no formal education. This finding is supported by other studies conducted in Mecha District, North west Ethiopia, Nigeria21,22 and Indonesia21,26,27,36. This is also similar to the study from the Philippines, where better education led to compliance with IFAS37. This may be because educated women are likely to have better knowledge and access to information about iron deficiency anemia and its treatment, the benefits of supplements, and pregnancy in general. Again, it may be related to the notion that education is more likely to increase women's awareness of micronutrient deficiencies and ways to overcome them. It may also be related to the fact that educated women are more likely to adhere to health care interventions, such as IFA, that provide better care for both the infant and the mother.
Participant`s husband`s educational status was also one of the significantly associated factor, those participant`s whose husband`s educational status was primary level were 3.60 times, secondary level and above were 2.52 times more compliant than those participant`s whose husband had no formal education. This finding is consistent with the study conducted in Indonesia36. The likely explanation could be that partner support from educated partners may have helped women to adhere to IFAS. Educated husbands may have been aware of IFAS and encouraged their partners to take the tablets without interruption as recommended by health workers. Encouragement from husbands may thus motivate women to continue taking the tablets.
Women aged ≥ 25 years were 2.27 times more likely to be compliant with IFAS than women of younger age (< 25 years). The reason for this may be that older women may be more concerned about their health and pregnancy outcomes and may have had better experiences with prevention and treatment of iron deficiency anemia. This finding is consistent with a study in India that found that older women (> 25 years) were more compliant than younger and this finding is also consistent with the study in Ethiopia23. However, some recent studies conducted in Ethiopia found no significant association between socio-demographic variables (age, mother's education, and in our case, husband's education) and IFAS adherence18,29,30,34.
Good knowledge of anemia was significantly associated with compliance to IFAS among pregnant women, where pregnant women with good knowledge of anemia were 4.40 times more likely to adhere to IFAS than those with poor knowledge of anemia This finding is similar with the studies conducted in North Wollo zone24, Western Amhara, Mecha district27 and Dire Dawa city30. The probable reason could be the fact that knowledge helps women to have awareness about prevention and treatment of anemia by taking iron folate supplement during pregnancy.
Knowledge of IFAS was also associated with women's adherence to iron and folic acid supplementation in studies conducted in Kenya, Hawasa City, Dire Dawa City, Debay Tilat Gen District North West Ethiopia, and Debre tabor General Hospital6,30,32,34,38. Similarly, knowledge of iron and folic acid supplementation was associated with adherence to iron and folic acid supplementation in this study. This may be because knowledge helps women understand the benefits of taking the supplement and the consequences of not taking the supplement for the mother and fetus during pregnancy, labor and delivery.
The strength of this study is that we used a relatively large sample and the response rate was high. However, the study is prone to social desirability bias because the outcome variable depends on mothers' self-report. This may underestimate or overestimate compliance. In addition, recall bias is another concern. We tried to minimize this by collecting information on reported IFA intake within 7 days prior to the interview. Despite the limitations, the current study identified valuable variables for intervention.
Conclusions
The results of this study showed that pregnant mothers' compliance to IFAS was 44.3%, and factors such as maternal age, maternal education, husband's education, knowledge of anemia, and knowledge of IFAS were found to be significantly associated with compliance to IFAS during pregnancy. Compliance to prenatal iron and folic acid is still low in the district and does not yet meet WHO recommendations, despite the usefulness of this health program to combat iron deficiency anemia. Therefore, district health offices should collaborate with education offices to improve the educational status of women and men. Comprehensive nutrition education and health promotion programs in health facilities should focus on the importance of ANC follow-up and adherence to IFA tablets, which in turn will improve pregnant mothers' knowledge of anemia and the benefits of IFA tablets. Special attention should be given to young mothers under the age of 25.
Data availability
The datasets used and/or analysed during the current study are included within the manuscript and the detail are uploaded as supplementary files.
Change history
26 January 2024
A Correction to this paper has been published: https://doi.org/10.1038/s41598-024-52765-2
References
Cramer, J. A. et al. Medication compliance and persistence: Terminology and definitions. Value Health 11, 44–77 (2008).
Gernand, A. D., Schulze, K. J., Stewart, C. P., West, K. P. & Christian, P. Micronutrient deficiencies in pregnancy worldwide: Health effects and prevention. Nat. Rev. Endocrinol. 12, 274–289. https://doi.org/10.1038/nrendo.2016.37 (2016).
Akibu, M. et al. Adherence to prenatal iron-folic acid supplementation in low-and middle-income countries (LMIC): A protocol for systematic review and meta-analysis. Syst. Rev. 7, 1–5 (2018).
Birhanu, Z. et al. Ethiopian women’s perspectives on antenatal care and iron-folic acid supplementation: Insights for translating global antenatal calcium guidelines into practice. Maternal Child Nutr. 14, e12424 (2018).
Organization, W. H. Guidelines on Food Fortification with Micronutrients (World Health Organization, 2006).
Kassa, Z. Y., Awraris, T., Daba, A. K. & Tenaw, Z. Compliance with iron folic acid and associated factors among pregnant women through pill count in Hawassa city, South Ethiopia: A community based cross-sectional study. Reprod. Health 16, 1–8 (2019).
WHO. Guideline: Daily Iron and Folic Acid Supplementation in Pregnant Women (WHO, 2012).
Begum, K. et al. Prevalence of and factors associated with antenatal care seeking and adherence to recommended iron-folic acid supplementation among pregnant women in Zinder, Niger. Maternal Child Nutr. 14, e12466 (2018).
Begum, S. Factors associated with adherence to Iron Folic acid supplementations during Pregnancy in Uttar Pradesh. Indian J. Maternal Child Health 14(2), 8 (2012).
Ogundipe, O. et al. Factors associated with prenatal folic acid and iron supplementation among 21,889 pregnant women in Northern Tanzania: A cross-sectional hospital-based study. BMC Public Health 12, 1–10 (2012).
Stephen, G. et al. Anaemia in pregnancy: Prevalence, risk factors, and adverse perinatal outcomes in Northern Tanzania. Anemia 2018, 1846280 (2018).
Niguse, W. & Murugan, R. Determinants of adherence to iron folic acid supplementation among pregnant women attending antenatal clinic in Asella Town, Ethiopia. Int. J. Ther. Appl. 35, 60–67 (2018).
Gashaw et al. Adherence to Iron and Folic Acid Supplement and Associated Factors among AntenatalCare Attendant Mothers In Lay Armachiho Health Centers, Northwest, Ethiopia, 2017 (2018).
Boti, N. et al. Adherence to Iron-Folate supplementation and associated factors among Pastoralist’s pregnant women in Burji districts, Segen area People’s zone, southern Ethiopia: Community-based cross-sectional study. Int. J. Reprod. Med. 2018, 1–8 (2018).
ETHIOPIA, F. D. R. O. National nutrition program-II. (Addis Ababa Ethiopia 2016).
Niguse, W. Adherence rate to iron folic acid supplementation among pregnant women. bioRxiv 2019, 535534 (2019).
ICF., E. P. H. I. E. E. A. Ethiopia Mini Demographic and Health Survey 2019: Key Indicators (EPHI and ICF, 2019).
Kedir Obsa, A., Tegene, Y. & Gebretsadik, A. Iron and folic acid supplementation compliance and associated factors among pregnant women attending antenatal clinic in Shalla District, Southwest Ethiopia: A cross-sectional study. J. Nutr. Metab. 2021, 1–7 (2021).
Beressa, G., Lencha, B., Bosha, T. & Egata, G. Utilization and compliance with iron supplementation and predictors among pregnant women in Southeast Ethiopia. Sci. Rep. 12, 16253. https://doi.org/10.1038/s41598-022-20614-9 (2022).
Nimwesiga, C., Murezi, M. & Taremwa, I. M. Adherence to iron and folic acid supplementation and its associated factors among pregnant women attending antenatal care at Bwindi Community Hospital Western Uganda. Int. J. Reprod. Med. 2021, 1–10 (2021).
Adanikin, A. I., Awoleke, J. O., Olofinbiyi, B. A., Adanikin, P. O. & Ogundare, O. R. Routine iron supplementation and anaemia by third trimester in a Nigerian hospital. Ethiop. J. Health Sci. 25, 305–312 (2015).
Agegnehu, G., Atenafu, A., Dagne, H. & Dagnew, B. Adherence to iron and folic acid supplement and associated factors among antenatal care attendant mothers In Lay Armachiho Health Centers, Northwest Ethiopia, 2017. bioRxiv 2018, 493916 (2018).
Arega Sadore, A., Abebe Gebretsadik, L. & Aman Hussen, M. Compliance with iron-folate supplement and associated factors among antenatal care attendant mothers in Misha District, South Ethiopia: Community based cross-sectional study. J. Environ. Public Health 2015, 1–7 (2015).
Demis, A., Geda, B., Alemayehu, T. & Abebe, H. Iron and folic acid supplementation adherence among pregnant women attending antenatal care in North Wollo Zone northern Ethiopia: Institution based cross-sectional study. BMC Res. Notes 12, 1–7 (2019).
Neupane, N., Sharma, S. & Kaphle, H. P. Factors affecting compliance of iron and folic acid among pregnant women attaining Western Regional Hospital, Pokhara, Nepal. Int. J. Res. Curr. Dev. 1, 43–47 (2015).
Nisar, Y. B., Dibley, M. J. & Aguayo, V. M. Iron-folic acid supplementation during pregnancy reduces the risk of stunting in children less than 2 years of age: A retrospective cohort study from Nepal. Nutrients 8, 67 (2016).
Taye, B., Abeje, G. & Mekonen, A. Factors associated with compliance of prenatal iron folate supplementation among women in Mecha district, Western Amhara: A cross-sectional study. Pan Afr. Med. J. 20, 4894 (2015).
Yadav, K. D., Yadav, U. N., Wagle, R. R., Thakur, D. N. & Dhakal, S. Compliance of iron and folic acid supplementation and status of anaemia during pregnancy in the Eastern Terai of Nepal: Findings from hospital based cross sectional study. BMC Res. Notes 12, 1–6 (2019).
Mekonnen, A., Alemnew, W., Abebe, Z. & Demissie, G. D. Adherence to iron with folic acid supplementation among pregnant women attending antenatal care in public health centers in simada district, northwest ethiopia: Using health belief model perspective. Patient Preference Adherence 15, 843 (2021).
Solomon, Y., Sema, A. & Menberu, T. Adherence and associated factors to iron and folic acid supplementation among pregnant women attending antenatal care in public hospitals of Dire Dawa Eastern Ethiopia. Eur. J. Midwifery 5, 1–7 (2021).
Statistics, W. D. H. O. Wondo District Health Office Statistics (2018).
Gebremariam, A. D., Tiruneh, S. A., Abate, B. A., Engidaw, M. T. & Asnakew, D. T. Adherence to iron with folic acid supplementation and its associated factors among pregnant women attending antenatal care follow up at Debre Tabor General Hospital, Ethiopia, 2017. PLoS ONE 14, e0210086 (2019).
Gebre, A., Debie, A., Berhane, A. & Redddy, P. S. Determinants of compliance to iron-folic acid supplementation among pregnant women in pastoral communities of Afar region: The cases of mille and assaita districts, Afar, Etiopia-2015. Med. Res. Chronicles 4, 352–362 (2017).
Demisse, B., Temesgen, H., Dessie, B. & Kassa, G. M. Adherence status to iron with folic acid supplementation and associated factors among pregnant women receiving antenatal care at public health facilities in Northwest Ethiopia. SAGE Open Med. 9, 20503121211049936 (2021).
Mithra, P. et al. Compliance with iron-folic acid (IFA) therapy among pregnant women in an urban area of south India. Afr. Health Sci. 14, 255–260 (2014).
Wiradnyani, L. A. A., Khusun, H., Achadi, E. L., Ocviyanti, D. & Shankar, A. H. Role of family support and women’s knowledge on pregnancy-related risks in adherence to maternal iron–folic acid supplementation in Indonesia. Public Health Nutr. 19, 2818–2828 (2016).
Felipe-Dimog, E. B., Yu, C.-H., Ho, C.-H. & Liang, F.-W. Factors influencing the compliance of pregnant women with iron and folic acid supplementation in the Philippines: 2017 Philippine Demographic and health survey analysis. Nutrients 13, 3060 (2021).
Juma, M. Predictors of optimum antenatal iron-folate supplementation in a low resource rural set-up in Eastern Kenya. J. Public Health Epidemiol. 7, 337–345 (2015).
Acknowledgements
Our thanks go to Wondo district health office. We also thank our data collectors and supervisors for their commitment throughout the research work. We would like to thank our study participants for their time and willingness to participate in our study.
Author information
Authors and Affiliations
Contributions
B.L. Participated in formulation of the research question, design of the study, supervision, carried out data analysis, write up and drafted the manuscript. T.M. Conceptualization of the study, formulated the research question, designed data collection tool, supervised data collection, participated in data analysis and reviewed the manuscript. A.M., S.D., D.Y. and G.B.: Participated in the formulation of the research question, design of the study, data analysis, and write up and reviewing the manuscript.
Corresponding author
Ethics declarations
Competing interests
The authors declare no competing interests.
Additional information
Publisher's note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
The original online version of this Article was revised: The original version of this Article contained an error in the order of the author names, which was incorrectly given as Bikila Lencha, Taye Mengistu, Ashenafi Mekonnen, Sisay Degno, Daniel Yohannis and Girma Beressa.
Supplementary Information
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if changes were made. The images or other third party material in this article are included in the article's Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article's Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
Mengistu, T., Lencha, B., Mekonnen, A. et al. Compliance to iron folic acid supplementation and its associated factors among pregnant women attending Antenatal clinic in Wondo district: a cross-sectional study. Sci Rep 13, 17468 (2023). https://doi.org/10.1038/s41598-023-44577-7
Received:
Accepted:
Published:
DOI: https://doi.org/10.1038/s41598-023-44577-7
- Springer Nature Limited