Abstract
Age-related macular degeneration (AMD) is one of the leading causes of blindness. AMD is currently incurable; the best solution is to prevent its occurrence. To develop drugs for AMD, it is crucial to have a model system that mimics the symptoms and mechanisms in patients. It is most important to develop safer and more effective anti-AMD drug. In this study, the dose of A2E and the intensity of blue light were evaluated to establish an appropriate atrophic in vitro model of AMD and anti-AMD effect and therapeutic mechanism of Codonopsis lanceolata. The experimental groups included a control group an AMD group treated with A2E and blue light, a lutein group treated with 25 μM lutein after AMD induction, and three groups treated with different doses of C. lanceolata (10, 20, and 50 μg/mL) after AMD induction. Intrinsic apoptotic pathway (Bcl-2 family), anti-oxidative system (Keap1/Nrf2/HO-1 antioxidant response element), and anti-carbonyl effect (4-hydroxynonenal [4-HNE]) were evaluated using immunofluorescence, MTT, TUNEL, FACS, and western blotting analyses. A2E accumulation in the cytoplasm of ARPE-19 cells depending on the dose of A2E. Cell viability of ARPE-19 cells according to the dose of A2E and/or blue light intensity. The population of apoptotic or necrotic cells increased based on the A2E dose and blue light intensity. Codonopsis lanceolata dose-dependently prevented cell death which was induced by A2E and blue light. The antiapoptotic effect of that was caused by activating Keap1/Nrf2/HO-1 pathway, suppressing 4-HNE, and modulating Bcl-2 family proteins like increase of antiapoptotic proteins such as Bcl-2 and Bcl-XL and decrease of proapoptotic protein such as Bim. Based on these findings, 30 μM A2E and 20 mW/cm2 blue light on adult retinal pigment epithelium-19 cells was an appropriate condition for AMD model and C. lanceolata shows promise as an anti-AMD agent.
Similar content being viewed by others
Introduction
Age-related macular degeneration (AMD) is a condition where the central vision is gradually lost as a result of aging. It is one of the leading causes of blindness worldwide1. In a meta-analysis conducted by the Wang group in 2022, the annual incidence of early and late AMD was found to be 1.59% and 0.23%, respectively. The study also projected that by 2050, the number of individuals affected by early and late AMD would reach 39.05 million and 6.41 million, respectively2. Another meta-analysis conducted in the United States revealed that the prevalence of AMD in individuals aged 40 years and older was 1.47%, while in women aged 80 years and older, it reached 15%3. This indicates a significant increase in the incidence of AMD with age. Furthermore, it is concerning that the population aged 60 years and older is projected to rapidly increase from 12% in 2015 to 22% in 20504.
The bis-retinoid N-retinyl-N-retinylidene ethanolamine (A2E) is a type of lipofuscin that is fluorescent. During aging, it accumulates in various parts of the body, including neurons, cardiac muscle, and the retinal pigment epithelium (RPE)5. Exposure to blue light (415–455 nm) can stimulate damage to RPE cells through oxidative stress, ultimately leading to the development of AMD6. There are several risk factors that can contribute to the development of AMD such as aging, tobacco smoking, cataract surgery, family health history, and being overweight7,8. AMD can be classified into two types: atrophic AMD (85–90%), which is characterized by the presence of drusen and hyperpigmentation, and neovascular AMD (10–15%), which is characterized by the development of choroidal neovascularization following RPE cell death9.
The treatments for AMD are categorized into three types: device-based treatment (prophylactic laser therapy and photodynamic therapy), anti-inflammatory drug treatment (corticosteroids and nonsteroidal anti-inflammatory drugs), and anti-vascular endothelial growth factor (anti-VEGF) treatment (VEGF antibody, aptamer, and tyrosine kinase inhibitor)10. However, each approach has adverse effects. Device-based treatment can lead to macular edema and retinovascular disease11,12, while anti-inflammatory drug treatment can cause hypertension, insulin resistance, insomnia, skin thinning, and gastric ulceration13. Anti-VEGF treatment, specifically through intravitreal injection, carries the risk of bleeding and infection14.
Because of various adverse effects of AMD medication it is necessary to develop a safe and effective anti-AMD drug. In order to evaluate the anti-AMD effect and examine the therapeutic mechanisms of drug candidates, it is crucial to establish an appropriate model system. The cell-based AMD model can be classified into two types: A2E combined with blue light induction, and chemical induction. Several studies have explored the relationship between A2E dose and blue light intensity. For example, one study used 20 μM A2E and 0.04 mW/cm2 blue light for 48 h15, while others used 25 μM A2E and 4.43 mW/cm2 blue light for 30 min16, 100 μM A2E and 0.4 mW/cm2 blue light for 20 min, or 35 mW/cm2 blue light for 60 sec17. Many chemical stimulators that can induce AMD have been studied, including cigarette smoke18, H2O219, KBrO320, and NaIO321. However, the advantages and disadvantages of each model are still unclear, and it is necessary to determine the differences among them.
Codonopsis lanceolata (C. lanceolata)has been used as a culinary ingredient and traditional medicinal material in Asia (Korea, China, and Japan) for a significant period of time. Recently, several biological effects of C. lanceolata have been reported, including its anti-proliferative effect on HT-29 colon cancer cells22, anti-obesity and anti-hyperlipidemia effects23, anti-hepatitis effect24, anti-inflammatory effect25, and anti-asthmatic effect26.
In this study, an appropriate in vitro model of AMD was suggested to effectively develop anti-AMD drugs. This model depended on the A2E and blue light treatment. Furthermore, the anti-AMD effect of C. lanceolata, along with its mechanism, was evaluated.
Materials and methods
A2E synthesis
A2E was synthesized according to Parish’s method27. Briefly, all-trans-retinal (100 mg, 352 mM) and 9.5 mg of ethanolamine (155 mM) were dissolved in 3.0 mL of ethanol (EtOH). Then, 9.3 µL of acetic acid (155 mM) was added, and the mixture was reacted at 120 rpm at room temperature in the dark for 48 h (Fig. 1A). To evaluate the purity of the synthetic A2E, liquid chromatography was conducted using a Waters Alliance 2695 HPLC system with a photodiode array detector. The analytic conditions are described in Table 1.
N-retinylidene-N-retinyl-ethanolamine (A2E) synthesis and the light intensity of the manufactured blue light transilluminator. (A) The scheme of A2E synthesis. (B) The result of A2E synthesis. Synthetic A2Es consisted of one A2E and two A2E isotypes. (C) The intensity of the blue light transilluminator. The peak wavelength of the irradiated light was 454.6 nm, with the majority of light falling within the range of blue light.
Manufacturing and intensity measurement of blue light transilluminator
The blue light emitting diodes (LEDs, Sumbulbs, 12 V Blue Light, Shenzhen, China) were used for the blue light transilluminator. The light intensity and wavelength were tested using the NeoLight PL5000 (PIMACS, Kyunggi, Korea), the Programmable AC Power Source 61,052 (Chroma ATE Inc., Taoyuan, Taiwan), and the Voltech PM3000A Universal Power Analyzer (Advanced Test Equipment Corp. CA, USA) by Korea Photonic Technology Institute (KOPTI, Gwangju, Korea). The analytical condition was maintained at 25.1 ± 0.6 °C and 51.8 ± 1.5% relative humidity.
In vitro study schedule including sample collecting
In this study, several cell culture protocols were utilized (Fig. 2). The 3-[4,5-dimethylthiazole-2-yl]-2,5-diphenyltetrazolium bromide (MTT) assay (VWR Life Science, OH, USA, 76,022–152) was performed to assess cell viability. Fluorescence activated cell sorting (FACS) analysis was conducted to determine the population of apoptotic cells. The immunofluorescence (IF) assay was used to analyze terminal deoxynucleotidyl transferase dUTP nick end labeling (TUNEL) staining for apoptotic cell status, as well as A2E auto-fluorescence and activation of the anti-oxidative system, Kelch-like ECH-associated protein 1 (Keap1)/nuclear factor erythroid-2-related factor 2 (Nrf2)/heme oxygenase-1 (HO-1) pathway. Western blotting was performed to examine the apoptotic pathway (B cell lymphoma 2 (Bcl-2) family), mitogen-activated protein kinase (MAPK), and indicators of oxidative stress (Keap1/Nrf2/HO-1) and carbonyl stress (4-hydroxynonenal (4-HNE)). Figure 6 provides a detailed description of the specific parameters for each assay.
Analysis of the accumulation and cytotoxicity of A2E in ARPE-19 cells
The adult retinal pigment epithelium (ARPE-19) cell line was purchased from the American Type Culture Collection (ATCC, Manassas, VA, USA, CRL-2302™) and maintained in Dulbecco’s modified eagle medium (DMEM, Gibco, 12,100,046) containing 10% fetal bovine serum (FBS, Gibco, Waltham, MA, USA, 30,067,334) and 1% penicillin. To evaluate the level of A2E accumulation in ARPE-19 cells, a confocal laser scanning microscope (Nanoscope systems, K1-Fluo, Daejeon, Korea) was used. The nucleus was counter-stained with 4',6-diamidino-2-phenylindole (DAPI, Thermo Fisher, Waltham, MA, USA, 62,247). A range of A2E concentrations from 0 to 40 μM was used and confirmed at 488 nm.
To measure the cytotoxicity of synthetic A2E on ARPE-19 cells, the cells were seeded at a density of 2 × 103 cells per well. After 36 h, various doses of A2E (0, 10, 20, 30, and 40 μM) were administered. Then, 24 h after A2E treatment, three levels of blue light intensity (0, 20, and 40 mW/cm2) were applied for 15 min. After 24 h, an MTT assay was conducted to evaluate the cytotoxicity of A2E and/or blue light in ARPE-19 cells, and the results were obtained using a Multiskan SkyHigh Microplate Spectrophotometer (Thermo Fisher Scientific, Waltham, MA, USA).
The analysis of apoptosis pathway of ARPE-19 cells by A2E and/or blue light
The abundance of apoptotic ARPE-19 cells depending on the dose of synthetic A2E and/or the intensity of blue light was measured using IF, TUNEL staining, and FACS analysis. Based on the MTT assay and A2E accumulation, the doses of A2E and the intensity of blue light were confirmed as 0, 30, or 40 μM A2E and 0, 20, or 40 mW/cm2 blue light.
For the FACS analysis, Invitrogen Alex Fluor 488 apoptosis detection kit (Invitrogen, Waltham, MA, USA, R37174) was used. The cells were harvested using trypsin (Gibco, 25,200,056). Single cells were washed, stained using Alex Fluor 488 and propidium iodide from the kit, and the results were acquired using Guava Easycyte (Millipore, Burlington, MA, USA).
For the TUNEL assay, the Click-iT™ Plus TUNEL assay kit (Invitrogen, C10618) was used. A2E cells were treated under the same conditions regarding A2E dose and/or blue light intensity. The media was discarded, and the attached cells were washed with phosphate buffered saline (PBS, Lonza, Walkersville, MD, USA, BE17-517Q). The cells were then fixed with 4% formaldehyde (Daejung, Siheung-si, Gyeonggi-do, Korea, P2031) in PBS. After fixation, 0.25% Triton X-100 (Sigma-Aldrich, Saint Louis, MO, USA, 9036–19-5) in PBS was added, and the cells were stained following the manufacturer’s guidelines. Finally, the images were obtained using a K1-Fluo confocal microscope (Nanoscope systems).
The analysis of carbonyl stress and oxidative stress on ARPE-19 cells by A2E and/or blue light
Carbonyl stress and oxidative stress were assessed using western blotting. To evaluate the carbonyl stress induced by A2E and/or blue light, the representative carbonyl stress-induced metabolite, 4-HNE (abcam, Ab46545), was analyzed. Oxidative stress analysis was conducted using primary antibodies for Nrf2 (Invitrogen, PA5-27,882) and HO-1 (Invitrogen, PA5-77,833).
Preparation and analysis of C. lanceolata extract and active compounds
The root of C. lanceolata was obtained from Wellphyto Co. (Gwangju, Korea) and deposited at Mokpo National University (MNUCSS-CL-01). To extract the active compounds, 20 g of dried C. lanceolata root was subjected to hot water extraction at 100 ℃ for 4 h. The resulting extract was freeze-dried. In our previous study28, lobetylin was confirmed as an active compound in C. lanceolata. This study was conducted to comply with the IUCN Policy Statement on Research involving Species at Risk of Extinction and the Convention on the Trade in Endangered Species of Wild Fauna and Flora.
Analysis of the anti-cytotoxic and anti-apoptotic effects of C. lanceolata in an in vitro model of AMD
All in vitro experiments were performed as shown in Fig. 2. To determine the proper concentration of C. lanceolata for this study, five doses of C. lanceolata (5, 10, 25, 50, and 100 μM) were tested, along with a normal control group (CON; 0 μM A2E and 20 mW/cm2 blue light), an induction control group (A2E; 30 μM A2E and 20 mW/cm2 blue light), and a positive control group (Lutein; 30 μM A2E, 20 mW/cm2 blue light, and 25 μM lutein). At 12 h after seeding ARPE-19 cells in a 96-well plate (2 × 103 cell/well), the reagents were administered. At 24 h after C. lanceolata treatment, A2E was added to each well, excluding the normal control group. At 24 h after A2E addition, each well was irradiated with 20 mW/cm2 blue light for 15 min. Finally, 24 h after blue light irradiation, the MTT assay was conducted to evaluate the anti-cytotoxic effect of C. lanceolata.
The anti-apoptotic effect of C. lanceolata was measured using IF for TUNEL staining and FACS analysis. The experimental groups included the CON, A2E, Lutein, and three doses of C. lanceolata (10, 25, 50 μg/mL) groups. A2E was applied 24 h after seeding the ARPE-19 cells, and blue light was irradiated after 48 h and after 72 h. The cells were harvested using trypsin to evaluate apoptosis. The subsequent steps were the same for IF, TUNEL, and FACS analyses.
Analysis of suppression effect of C. lanceolata on three stresses
The anti-apoptotic mechanism of the Bcl-2 family pathway was evaluated using primary antibodies against Bcl-2 (Santa Cruz Biotechnology, sc-7382), B-cell lymphoma-extra large (Bcl-XL, Invitrogen, PA5-17805), and Bcl-2 interacting mediator of cell death (Bim, Santa Cruz Biotechnology, sc-374358). The results of were obtained using Davinch-WesternTM (Davinch-K, Seoul, Korea).
To evaluate the anti-apoptotic effect of C. lanceolata, the changes in the Keap1/Nrf2/HO-1 pathway and 4-HNE levels were assessed using western blotting and IF. Primary antibodies for Keap1 (Invitrogen, PA5-99,434), Nrf2 (Invitrogen, PA5-27,882), HO-1 (Invitrogen, PA5-77,833), and 4-HNE (abcam, Ab46545) were used.
Statistics
The results are expressed as the mean ± standard deviation (SD). Following one-way analysis of variance (ANOVA) analysis, Dunnett’s multiple comparison was conducted. Differences with p values below 0.05 were considered significant.
Results
A2E synthesis and the light wavelength of a self-manufactured transilluminator
As shown in Fig. 1A, 352 mM all-trans-retinal and 155 mM ethanolamine were dissolved in 3.0 mL of EtOH. Then, 155 mM acetic acid was added to the mixture, and they were reacted through centrifugation at 120 rpm at room temperature in the dark for 48 h (Fig. 1A). After the reaction, three types of A2E were synthesized and verified using liquid chromatographic analysis. One A2E was found approximately at 12 min (retention time), while two A2E isotypes (Iso-A2Es) were found around 14 min and 16 min (Fig. 1B). The analytical conditions are presented in Table 1. The most effective light for AMD induction is blue light, which has a wavelength range of 400–500 nm29. The self-manufactured blue light transilluminator used in this study mainly emitted blue light within this range, with a peak of the wavelength of 454.6 nm (Fig. 1C).
A2E permeated into ARPE-19 cells and the population of dead cells increased depending on both A2E and blue light
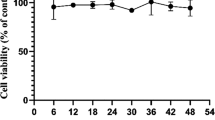
A2E, when reacted with blue light, induces AMD and exhibits autofluorescence30. To evaluate the level of A2E permeation in the cytoplasm, an IF assay was performed after treatment with 0, 10, 20, 30, or 40 μM A2E. In treatments with 10 μM A2E or less, the green color was unclear. However, in treatments with 20 μM A2E or more, green spots could be clearly detected in the cytoplasm (Fig. 3A). A2E decreased cell viability from 100 ± 7.75% in the 0 μM treatment group to 83.4 ± 9.50% in the 40 μM treatment group (Fig. 3B and Table 2) without blue light treatment. Co-treatment with A2E and blue light dose-dependently increased cytotoxicity. Under 20 mW/cm2 blue light illumination, the viabilities in the 30 μM and 40 μM A2E treatment groups were 73.5 ± 9.91% and 72.5 ± 8.89%, respectively. Under 40 mW/cm2 blue light exposure, the viabilities in the 30 μM and 40 μM A2E treatment groups were only 68.1 ± 6.96% and 63.2 ± 7.17%, respectively. Based on these results, the optimal condition was determined to be 30 μM A2E treatment with 20 mW/cm2 blue light illumination.
Cytotoxicity and A2E accumulation in adult retinal pigment epithelial (ARPE)-19 cells, depending on the dose of A2E and the intensity of blue light. (A) A2E accumulation in the cytoplasm of ARPE-19 cells depending on the dose of A2E. A clear presence of A2E in the cytoplasm was observed, particularly at a dose of 20 μM A2E. Scale bar, 50 μm. Magnification, 1000 × . (B) Cell viability of ARPE-19 cells according to the dose of A2E and/or blue light intensity. N = 6. The results are presented as the mean ± standard deviation (SD). *, p < 0.05; **, p < 0.001 compared to 0 μM A2E. $, p < 0.05; $$ p < 0.01 compared to 10 μM A2E. #, p < 0.05; ##, p < 0.001 compared to 20 μM A2E.
A2E and blue light induces apoptosis in ARPE-19 cells via Nrf2/HO-1 pathway and carbonyl stress
To analyze the apoptotic effect of A2E and/or blue light treatment, TUNEL assay was performed followed by IF analysis (Fig. 4A). The results were similar to those observed in cell viability tests (Fig. 3B). A2E treatment dose-dependently increased the number of apoptotic cells. Under 20 mW/cm2 blue light illumination, 30 μM or 40 μM A2E treatment induced cell apoptosis, particularly resulting in irregular cell morphology. Similar results were obtained with 40 mW/cm2 blue light treatment. To confirm cell death caused by A2E and blue light, FACS analysis was conducted (Table 3). A2E treatment alone dose-dependently increased the population of dead cells, including necrotic cells, from about 5.1 ± 0.68% in the 0 μM A2E treatment group to 23.4 ± 3.50% in the 40 μM A2E treatment group. Co-treatment with A2E and blue light also dose-dependently increased the number of dead cells. Specifically, after 30 μM A2E treatment with 20 mW/cm2 blue light exposure, the population of apoptotic cells was 21.6 ± 0.072%. Accordingly, this condition was selected as the AMD cell model. Although there are many factors that induce cell death, oxidative and carbonyl stress are among the important ones31. To examine the effect of treatment with A2E, blue light, or their combination on oxidative and carbonyl stress, the levels of oxidative stress markers, such as the Nrf2/HO-1 pathway and the carbonyl stress marker 4-HNE were measured (Fig. 4B). Without blue light treatment, an upregulation of 4-HNE due to A2E treatment was observed. However, under 20 mW/cm2 blue light treatment, A2E treatment suppressed the Nrf2/HO-1 pathway but increased the level of 4-HNE in a dose-dependent manner.
Apoptosis, oxidative stress, and carbonyl stress in ARPE-19 cells depending on the level of A2E and the intensity of blue light. (A) The results of the TUNEL assay for ARPE-19 cell death at various doses of A2E and/or blue light intensities. Scale bar, 50 μm. Magnification, 1000 × . (B) The results of apoptosis-related pathway analysis. N = 3.
C. lanceolata prevented cell death induced by A2E and blue light in a dose-dependent manner
To measure the preventive effect of C. lanceolata against cytotoxicity induced by A2E and blue light, an MTT assay was performed (Fig. 5A). Co-treatment with 30 μM A2E and 20 mW/cm2 blue light increased the population of dead ARPE-19 cells, but 25 μM lutein treatment prevented their cytotoxicity. Although only in the 100 μg/mL C. lanceolata treatment group, the live cell percentage was similar to that in the 25 μM lutein treatment group, C. lanceolata treatment resulted an increasing trend of live cell population depending on the dose. A2E and blue light co-treatment significantly induced cell death compared to the control, but C. lanceolata treatment dose-dependently decreased the level of apoptosis (green) caused by A2E and blue light co-treatment (Fig. 4B). To confirm the result of the IF assay (Fig. 5B), the anti-apoptotic effect of C. lanceolata was analyzed using FACS (Table 4). Compared to the result in the control group (the population of total apoptotic cells, 5.8 ± 2.37%), A2E and blue light co-treatment induced a higher amount of cell death (10.4 ± 2.90%), but C. lanceolata treatment dose-dependently prevented A2E and blue light-induced cell death. In particular, the population of dead cells in the 50 μg/mL C. lanceolata treatment group (5.0 ± 1.83%) was similar to that in the control group. Compared to the population of normal cells in the 25 μM lutein treatment group (82.2 ± 0.95%), the population in the 25 μg/mL C. lanceolata treatment group was 83.5 ± 2.03%, indicating that the normal cell percentage in the lutein treatment group was similar to that in the 25 μg/mL C. lanceolata treatment group.
Codonopsis lanceolata prevented cell death induced by A2E and blue light. (A) C. lanceolata dose-dependently ameliorated cell death induced by A2E and blue light (N = 3). *, p < 0.05; **, p < 0.001 compared to CON; $, p < 0.05 compared to the A2E and blue light treatment group; #, p < 0.05 compared to the lutein treatment group. (B) C. lanceolata dose-dependently suppressed RPE-19 cell apoptosis induced by A2E and blue light (green spot). Scale bar, 50 μm. Magnification, 1000 × .
C. lanceolata prevented apoptosis in ARPE-19 cells by increasing Bcl-2 and Bcl-XL and decreasing Bim, stimulating the activation of the Keap1/Nrf2/HO-1, and downregulating 4-HNE
The results shown in Fig. 5 suggested that C. lanceolata prevented apoptosis in ARPE-19 cells, which was caused by co-treatment with A2E and blue light. The Bcl-2 family includes anti-apoptotic proteins, such as Bcl-2 and Bcl-xL, as well as the pro-apoptotic protein Bim32. We analyzed the Bcl-2 family proteins to investigate the anti-apoptotic mechanism of C. lanceolata (Fig. 6A). Co-treatment with A2E and blue light regulated the levels of Bcl-2 family proteins by downregulating Bcl-2 and Bcl-XL and upregulating Bim. However, C. lanceolata suppressed this effect in a dose-dependent manner, increasing Bcl-2 and Bcl-XL levels while decreasing Bim expression (Fig. 6A). Keap1/ Nrf2/ HO-1 pathway plays an important role in the anti-oxidative system. Under normal conditions, Keap1 and Nrf2 are bound together in the cytoplasm. However, when cells are stressed, Nrf2 separates from Keap1 and translocates to the nucleus, acting as a transcription factor for HO-133. C. lanceolata increased the expression levels of Keap1, Nrf2, and HO-1 proteins in a dose-dependent manner and effectively reduced the level of 4-HNE (Fig. 6B). To confirm the activation of the Keap1/Nrf2/HO-1 pathway, an IF assay was performed (Fig. 6C and D). In the A2E group, the expression level of Nrf2 in the nucleus was lower compared to the control group. However, similar to lutein treatment, C. lanceolata treatment dose-dependently increased the expression of Nrf2 in the nucleus (Fig. 6C). Similarly, the expression of Keap1 and HO-1 were dose-dependently increased in the cytoplasm (Fig. 6D), consistent with the results of western blotting in the C. lanceolata treatment group. Overall, these results indicate that C. lanceolata effectively activated the Keap1/Nrf2/HO-1 pathway.
Codonopsis lanceolata regulated the apoptosis of ARPE-19 cells through the activation of the Keap1/Nrf2/HO-1 pathway and the suppression of 4-HNE. (A) C. lanceolata modulated the Bcl-2 family, increasing the levels of the antiapoptotic proteins Bcl-2 and Bcl-XL, while decreasing the level of the proapoptotic protein Bim (N = 3). (B) C. lanceolata treatment activated the anti-oxidative Keap1/Nrf2/HO-1 pathway but decreased the expression of 4-HNE in a dose-dependent manner (N = 3). (C) C. lanceolata treatment stimulated the expression of nuclear Nrf2, which functions as a transcription factor for HO-1 (green spots). (D) C. lanceolata treatment dose-dependently induced the expressions of Keap1 and HO-1. Scale bar, 50 μm. Magnification, 1000 × .
Discussion
AMD is one of the leading causes of blindness worldwide1, and it is closely associated with aging. The global population of aging individuals is rapidly increasing4. According to the stage of AMD, medications can be divided into two types: treatments for atrophic and neovascular AMD. The therapeutic method for neovascular AMD includes laser or anti-VEGF treatment, which aims to inhibit angiogenesis in the choroidal area10. The purpose of atrophic AMD treatment is to prevent the death of RPE cells and is associated with eliminating various factors-related to apoptosis, such as oxidative stress, inflammation, and carbonyl stress. Current medications have various adverse effects such as macular edema, retinovascular disease, hypertension, insulin resistance, insomnia, skin thinning, gastric ulceration, eye bleeding, and increased risk of infection11,12,13,14. Due to these adverse effects, there is a need for new AMD drugs based on the type of AMD such as atrophic or neovascular AMD that are both more effective and safer. For successful drug development, it is crucial to establish an appropriate AMD model system.
Depending on the time of occurrence and angiogenesis in the choroidal area, AMD can be classified into two types: atrophic and neovascular AMD. The main difference between them is that atrophic AMD is caused by the death of RPE cells in the early stage. While neovascular AMD occurs due to angiogenesis in the choroidal area after RPE cell death9. The initiation of AMD is believed to involve the death of RPE cells, which can be caused by oxidative stress, inflammation, and carbonyl stress31. There are various reactive oxygen species (ROS), including hydroxyl radical (OH·), hydroxide ion (HO-), triplet oxygen (3O2), superoxide anion (O2·−), peroxide ion (O22−), hydrogen peroxide (H2O2), and nitric oxide (NO·)34. The ROS related to AMD occurrence have been identified as OH·35, O2·−36, and H2O237. However, the relationship between NO· levels and AMD occurrence is unclear, as controversial results exist, such as upregulation38 and down-regulation39 in AMD patients. Oxidative stress and inflammation are deeply related to the development of several pathologies34, as inflammatory cells stimulate oxidative stress40 and ROS induce an increase in proinflammatory gene expression41. The Keap1/Nrf2 ARE is one of the representative anti-oxidative systems. It can control not only oxidative stress but also inflammation through the NF-κB pathway. This pathway is suggested as a good therapeutic target against many diseases, such as cancer, diabetes, inflammatory disease, and respiratory disease42,43. Carbonyl stress refers to the negative process in several parts of the bio-organism, such as protein, plasma membrane, and DNA, that is caused by carbonyl compounds generated through non-oxidative mechanisms44. Some carbonylation-related metabolites, such as 4-HNE45, trans-4-hydroxy-2-hexenal (4-HHE)46, and malondialdehyde (MDA)47, stimulate the occurrence of AMD. Apoptosis can be classified into extrinsic and intrinsic pathways32. The extrinsic pathway is initiated by the interaction of transmembrane receptors and ligands, such as tumor necrosis factor receptor 1 (TNFR1)/TNF-α, FasR/FasL, and death receptors (DRs)/tumor necrosis-related apoptosis-inducing ligand (TRAIL)48,49,50. The intrinsic pathway is deeply connected to mitochondrial changes, which can be positively or negatively controlled by Bcl-2 family proteins but is not related to death receptors51. Bcl-2 family proteins include anti-apoptotic proteins, such as Bcl-2, Bcl-extra (Bcl-x), and Bcl-xL, and pro-apoptotic proteins, such as Bcl-2 associated X (Bax), Bcl-2 antagonist/killer 1 (Bak), and Bim.
The atrophic AMD is initiated by the death of RPE cells, which is caused by oxidative stress, inflammation, and carbonyl stress. Although there are many risk factors, such as aging, tobacco smoking, cataract surgery, family history, and overweight, the proximate and major factor is believed to be the epoxide type of A2E, which is produced by A2E and blue light6. However, it is unclear what level of A2E and intensity of blue light are required to induce an in vitro AMD model. From various studies, the level of A2E has been reported to range from 20 to 100 μM, and the intensity of blue light has been tested from 0.04 to 35 mW/cm215,16,17. To investigate similar conditions in bio-organisms with atrophic AMD, we evaluated the permeability of A2E to the cytoplasm and the relationship between RPE cell death and A2E level/blue light intensity (Figs. 3 and 4). A2E was found to pass through the cell membrane in a dose-dependent manner (Fig. 3A), and its cytotoxic effect on ARPE-19 cells increased with the level of A2E in the cytoplasm and the intensity of blue light (Fig. 3B). The population of apoptotic cells was increased in a dose-dependent manner with A2E and blue light treatment, but the number of necrotic cells also increased (Fig. 4A and Table 3). Taking into account both the number of apoptotic and necrotic cells, the combination of 30 μM A2E treatment and 20 mW/cm2 blue light transillumination was selected as the best in vitro AMD model condition. To confirm the apoptosis-related oxidative stress and carbonyl stress pathway, several factors were analyzed. Under 30 μM A2E treatment and 20 mW/cm2 blue light transillumination, the Nrf2/HO-1 anti-oxidative system was suppressed and the level of 4-HNE was increased in ARPE-19 cells (Fig. 4B). These results indicate that ARPE-19 cell death is induced by Nrf2/HO-1 anti-oxidative system-related oxidative and carbonyl stress (Figs. S1, S3, S3) .
While developing potential synthetic chemicals against atrophic AMD is an option, natural products that have been used as culinary and/or medicinal materials for a long time can be another alternative, as they may be relatively safe if they have been consumed as edible substances for a prolonged period. However, before considering them as candidates, their therapeutic mechanisms, such as anti-oxidation, anti-inflammation, and/or anti-carbonylation for preventing RPE cell death, should be confirmed. C. lanceolata is a culinary/medicinal material that has been used for a long time in Asia and has been reported to have biological effects, such as anti-hepatitis24, anti-inflammatory25, and anti-asthmatic effects26. These observations suggest that C. lanceolata has anti-inflammatory and immune modulation effects. In this study, we evaluated the anti-apoptotic effect of C. lanceolata on RPE cells by analyzing apoptosis-related factors, such as oxidative and carbonyl stress. C. lanceolata dose-dependently decreased the level of apoptosis in ARPE-19 cells induced by A2E and blue light co-treatment (Fig. 5B & Table 4). When comparing the anti-apoptotic potency between C. lanceolata and lutein (positive control drug), the normal cell population in 25 μM lutein treatment was 82.2 ± 0.95% and in 25 μg/mL C. lanceolata treatment was 83.5 ± 2.03%. As the comparison of 25 μM lutein and 25 μg/mL C. lanceolata treatment did not indicate a statistically significant difference, the anti-apoptotic potency of C. lanceolata was assumed to be similar to that of lutein. Based on its anti-apoptotic potency, we assessed the involvement of the Bcl-2 family-related intrinsic apoptosis pathway, the Keap1/Nrf2 anti-oxidative system, and carbonyl stress (Fig. 6). As shown in Fig. 5A, C. lanceolata effectively modulated the Bcl-2 family by increasing the levels of anti-apoptotic Bcl-2 proteins, such as Bcl-2 and Bcl-XL, while decreasing that of the pro-apoptotic protein, Bim. C. lanceolata not only stimulated the Keap1/Nrf2/HO-1 ARE pathway (Fig. 6B–D) but also inhibited the expression of 4-HNE (Fig. 6B).
Conclusion
Based on these results, we obtained two findings. First, we found that the appropriate condition for an in vitro model of AMD is the treatment of ARPE-19 cells with 30 μM A2E and transillumination with 20 mW/cm2 blue light. This combination effectively induced oxidative and carbonyl stress, leading to the death of ARPE-19 cells. Second, we found that C. lanceolata shows promise as an anti-AMD agent. It effectively suppressed cellular stresses through Nrf2/HO-1 ARE activation and 4-HNE suppression, ultimately preventing apoptosis by deactivating the intrinsic apoptosis pathway.
Data availability
All data and material in this manuscript will be made available on request to corresponding author.
References
Jonas, J. B. et al. Updates on the epidemiology of age-related macular degeneration. Asia-Pac J. Ophthalmol. 6, 493–497 (2017).
Wang, Y. et al. Global incidence, progression, and risk factors of age-related macular degeneration and projection of disease statistics in 30 years: A modeling study. Gerontol. 68, 721–735 (2022).
The Eye Diseases Prevalence Research Group. Prevalence of age-related macular degeneration in the United States. Arch. Ophthalmol. 122, 564–572 (2004).
World Health Organization, Ageing and health. https://www.who.int/news-room/fact-sheets/detail/ageing-and-health. Accessed 26th Jan 2023 (2023).
Crouch, R. K., Koutalos, Y., Kono, M., Schey, K. & Ablonczy, Z. A2E and lipofuscin. Prog. Mol. Biol. Transl. Sci. 134, 449–463 (2015).
Lamb, L. E. & Simon, J. D. A2E: A component of ocular lipofuscin. Photochem. Photobiol. 79(2), 127–136 (2004).
Chakravarthy, U. et al. Clinical risk factors for age-related macular degeneration: A systematic review and meta-analysis. BMC Ophthalmol. 10, 31 (2010).
Zhang, Q. Y. et al. Overweight, obesity and risk of age-related macular degeneration. Invest. Ophthalmol. Vis. Sci. 57, 1276–1283 (2016).
Bhutto, I. & Lutty, G. Understanding age-related macular degeneration (AMD): Relationships between the photoreceptor/retinal pigment epithelium/Bruch’s membrane/choriocapillaris complex. Mol. Aspects Med. 33, 295–317 (2012).
Cho, Y. K., Park, D. H. & Jeon, I. C. Medication trends for age-related macular degeneration. Int. J. Mol. Sci. 22, 11837 (2021).
Mainster, M. A. & Reichal, E. Transpupillary thermotherapy for age-related macular degeneration: Long-pulse photocoagulation, apoptosis, and heat shock proteins. Ophthalmic Surg. Lasers 31, 359–373 (2000).
Bresnick, G. H. Diabetic maculopathy. A critical review highlighting diffuse macular edema. Ophthalmology 90, 1301–1317 (1983).
Kapugi, M. & Cunningham, K. Corticosteroids. Orthop. Nurs. 38, 336–339 (2019).
Falavarjani, K. G. & Nguyen, Q. D. Adverse events and complications associated with intravitreal injection of anti-VEGF agents: A review of literature. Eye 27, 787–794 (2013).
Moon, J. et al. Blue light effect on retinal pigment epithelial cells by display devices. Integr. Biol. 9(5), 436–443 (2017).
Alaimo, A. et al. Toxicity of blue led light and A2E is associated to mitochondrial dynamics impairment in ARPE-19 cells: Implications for age-related macular degeneration. Arch. Toxicol. 93, 1401–1415 (2019).
Sparrow, J. R. & Cai, B. Blue light-induced apoptosis of A2E-containing RPE: Involvement of caspase-3 and protection by Bcl-2. Invest. Ophthalmol. Vis. Sci. 42(6), 1356–1362 (2001).
Govindaraju, V. K., Bodas, M. & Vij, N. Cigarette smoke induced autophagy-impairment regulates AMD pathogenesis mechanisms in ARPE-19 cells. PLoS ONE 12(8), e0182420 (2017).
Hanus, J. et al. Induction of necrotic cell death by oxidative stress in retinal pigment epithelial cells. Cell Death Dis. 4, e965 (2013).
Kuo, S. C. et al. Potassium bromate-induced cell model of age-related macular degeneration in vitro. Mol. Med. Rep. 23(3), 216 (2021).
Aung, K. H., Liu, H., Ke, Z., Jiang, S. & Huang, J. Glabridin attenuates the retinal degeneration induced by sodium iodate in vitro and in vivo. Front. Pharmacol. 11, 566699 (2020).
Wang, L., Xu, M. L., Hu, J. H., Rasmussen, S. K. & Wang, M. H. Codonopsis laceolata extract induces G1/G1 arrest and apoptosis in human colon tumor HT-29 cells—involvement of ROS generation and polyamine depletion. Food Chem. Toxicol. 49, 149–154 (2011).
Lee, J. S. et al. Codonopsis laceolata extract prevents diet-induced obesity in C57BL/6 mice. Nutrients 6, 4663–4677 (2014).
Cha, A. et al. Antilipogenic and anti-inflammatory activities of Codonopsis laceolata in mice hepatic tissues after chronic ethanol feeding. J. Biomed. Biotechnol. 2012, 141395 (2012).
Lee, Y. G. et al. Regulatory effects of Codonopsis laceolata on macrophage-mediated immune responses. J. Ethnopharmacol. 112, 180–188 (2007).
Bok, S. H., Han, K. M., Boo, H. O., Cho, S. S. & Park, D. H. Codonopsis laceolata water extract ameliorates asthma severity by inducing Th2 cells’ and pulmonary epithelial cells’ apoptosis via NF-κB/COX-2 pathway. Processes 10, 1249 (2022).
Parish, C. A., Hashimoto, M., Nakanishi, K., Dillon, J. & Janet, S. Isolation and one-step preparation of A2E and iso-A2E, fluorophores from human retinal pigment epithelium. Proc. Natl. Acad. Sci. USA 95(25), 14609–14613 (1998).
Song, S. Y. et al. Standardization of diploid Codonopsis laceolata root extract as an anti-hyperuricemic source. Processes 9, 2065 (2021).
Taylor, H. R. et al. Visible light and risk of age-related macular degeneration. Trans. Am. Ophthalmol. Soc. 88, 163–173 (1990).
Sparrow, J. R., Parish, C. A., Hashimoto, M. & Nakanishi, K. A2E, a lipofuscin fluorophore, in human retinal pigmented epithelial cells in culture. Invest. Ophthalmol. Vis. Sci. 40(12), 2988–2995 (1999).
Cho, Y. K. et al. The age-related macular degeneration (AMD)-preventing mechanism of natural products. Processes 10, 678 (2022).
Elmore, S. Apoptosis: A review of programmed cell death. Toxicol. Pathol. 35(4), 495–516 (2007).
Loboda, A., Damulewicz, M., Pyza, E., Jozkowicz, A. & Dulak, J. Role of Nrf2/HO-1 system in development, oxidative stress response and diseases: An evolutionarily conserved mechanism. Cell Mol. Life Sci. 73, 3221–3247 (2016).
Biswas, S. K. Does the interdependence between oxidative stress and inflammation explain the antioxidant paradox?. Oxid. Med. Cell Longev. 2016, 5698931 (2016).
Imammura, T. et al. Hydroxyl radicals cause fluctuation in intracellular ferrous ion levels upon light exposure during photoreceptor cell death. Exp. Eye Res. 129, 24–30 (2014).
Marie, M. et al. Light action spectrum on oxidative stress and mitochondrial damage in A2E-loaded retinal pigment epithelium cells. Cell Death. Dis. 9(3), 287 (2018).
Kaczara, P., Sarna, T. & Burke, J. M. Dynamics of H2O2 availability to ARPE-19 cultures in models of oxidative stress. Free Radic. Biol. Med. 48, 1064–1070 (2010).
Evereklioglu, C. et al. Nitric oxide and lipid peroxidation are increased and associated with decreased antioxidant enzyme activities in patients with age-related macular degeneration. Documenta. Ophthalmol. 106, 129–136 (2003).
Totan, Y. et al. Plasma malondialdehyde and nitric oxide levels in age related macular degeneration. Br. J. Ophthalmol. 85, 1426–1428 (2001).
Collins, T. Acute and Chronic Inflammation. In Robbins Pathologic Basis of Disease (eds Cotran, R. S. et al.) 50–88 (W.B. Saunders, 1999).
Flohe, L., Brigelius-Flohe, R., Saliou, C., Traber, M. G. & Packer, L. Redox regulation of NF-κB activation. Free Radical Bio. Med. 22(6), 1115–1126 (1997).
de Freitas, S. M. et al. The Keap1/Nrf2-ARE pathway as a pharmacological target for chalcones. Molecules 23, 1803 (2018).
Lu, M. C., Ji, J. A., Jiang, Z. Y. & You, Q. D. The Keap1-Nrf2-ARE pathway as a potential preventive and therapeutic target: An update. Med. Res. Rev. 36, 924–963 (2016).
Zoccali, C., Mallamaci, F. & Tripepi, G. AGEs and carbonyl stress: Potential pathogenetic factors of long-term uraemic complications. Nephrol. Dial. Transplant 15(Suppl 2), 7–11 (2000).
Kauppinen, A. H. et al. Oxidative stress activates NLRP3 inflammasomes in ARPE-19 cells-Implications for age-related macular degeneration (AMD). Immunol. Lett. 147, 29–33 (2012).
Long, E. K. & Picklo, M. J. Sr. Trans-4-hydroxy-2-hexenal, a product of n-3 fatty acid peroxidation: Make some room HNE…. Free Radic. Biol. Med. 49(1), 1–8 (2010).
Pinna, A., Boscia, F., Paligiannis, P., Carru, C. & Zinellu, A. Malondialdehyde levels in patients with age-related macular degeneration: A systematic review and meta-analysis. Retina 40(2), 195–203 (2020).
Chicheportiche, Y. et al. TWEAK, a new secreted ligand in the tumor necrosis factor family that weakly induces apoptosis. J. Biol. Chem. 272, 32401–32410 (1997).
Ashkenazi, A. & Dixit, V. M. Death receptors: Signaling and modulation. Science 281, 1305–1308 (1998).
Suliman, A., Lam, A., Datta, R. & Srivastava, R. K. Intracellular mechanisms of TRAIL: Apoptosis through mitochondrial-dependent and -independent pathways. Oncogene 20, 2122–2133 (2001).
Cory, S. & Adams, J. M. The Bcl2 family: Regulators of the cellular life-or-death switch. Nat. Rev. Cancer 2, 647–656 (2002).
Acknowledgements
C. lanceolata root was donated by Dr. Hee-Ock Boo, CEO in Wellphyto Co. (Gwangju, Korea).
Funding
This work was supported by the National Research Foundation of Korea (NRF) grant funded by the Korea government (MSIT) (No. 2022R1A5A8033794).
Author information
Authors and Affiliations
Contributions
First two authors, SY.L. and YK.C. equally contributed to this study, and they shared first authorship. Description of the first manuscript: SY.L. and YK.C. Experiment and protocol: SY.L., YK.C., CS.B., G.K., and MJ.L.. Conceptualization: IC.J., SS.C. and DH.P. Write and revisions: DH.P. All authors approved the submitted version.
Corresponding authors
Ethics declarations
Competing interests
The authors declare no competing interests.
Additional information
Publisher's note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if changes were made. The images or other third party material in this article are included in the article's Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article's Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
Lee, SY., Cho, YK., Bae, CS. et al. Oxidative and carbonyl stress induced AMD and Codonopsis lanceolata ameliorates AMD via controlling oxidative and carbonyl stress. Sci Rep 14, 16322 (2024). https://doi.org/10.1038/s41598-024-67044-3
Received:
Accepted:
Published:
DOI: https://doi.org/10.1038/s41598-024-67044-3
- Springer Nature Limited