Abstract
The increasing infodemic, changes in the media landscape, and the COVID-19 pandemic have rendered healthcare professionals’ involvement in social media (SoMe) of urgent need. However, research efforts to understand the opinions, needs, and concerns of healthcare professionals (HCP) tackling this new responsibility have been limited, despite being necessary for designing efficient support for them. In this article we look at varying opinions and attitudes published by HCPs towards the use of SoMe as a tool to communicate health-related information to the public: How did their attitudes develop since the decade preceding the COVID-19 outbreak and what were their main expressed concerns over the years. We conducted a qualitative review of editorials published on this topic in academic journals since 2010 by searching five databases up to December 2022. Thirty-eight (38) articles met the selection criteria. Nineteen (19) expressed a positive attitude, and Nineteen (19) expressed a negative or cautious attitude. Based on the results, the research period (2010–2022) was divided into three stages: 2010–2015, 2016–2018, and 2019–2022. Attitudes in the first stage were positive, the middle was at almost a tie, and the last retreated to negative. The most common concerns cited regarding SoMe use by HCPs are negative effects on physician–patient relationships, HCPs’ professional image, patient privacy, the quality of the information provided, conflict of interest declarations, ethical and legal risks, the perception of medical consensus, limited resources, and competing with entertainment. The editorial opinions of HCPs towards professional SoMe use express shifting hesitancies. The earlier optimism succeeded in an era (pre-2010) of cautioning against engaging with SoMe. Concerns in the first stage were mainly related to HCP´s behavior and use of SoMe. The last phase’s concerns were more oriented toward SoMe platforms, their design, dynamics, and effect on public discourse, with the escalating infodemic and COVID-19 pandemic.
Similar content being viewed by others
Explore related subjects
Discover the latest articles, news and stories from top researchers in related subjects.Introduction
In 2020 the World Health Organization declared that the infodemic has become one of the top 10 health risks in the world, just after the COVID-19 outbreak (World Health Organization, 2020). The COVID-19 pandemic spotlighted the parallel infodemic that had been developing for years (Eysenbach, 2002), accelerated by the growing influence of misinformation and disinformation on social media platforms (Zaidi et al., 2021). Pandemic and vaccine-related information for viruses such as COVID-19 need to be adequately communicated to all segments of society in order for the Healthcare institutions’ containment plans to work (Mach et al., 2021). This makes the demand for varying communication approaches and platforms higher (Berg et al., 2021; Krawiec et al., 2021). As people increasingly seek health information online (Ducrot et al., 2021), Social Media (SoMe) is among the most common sources people resort to, despite varying degrees of trust in the information provided through them (Sun et al., 2019). Communication analysts have studied health information-seeking patterns and trends, in order to better inform health and media institutions and strategies. These investigations and available data clearly indicate that the trend of seeking health-related information on SoMe continues to be on the rise (Park et al., 2018). The COVID-19 pandemic contributed further to that (Mangono et al., 2021; Su et al., 2021).
SoMe accounts have become a main source of information for news producers worldwide (Pole and Gulyas, 2015). Primary sources, whether they be officials, celebrities, scientists, or key actors, can now be “harvested” from their verified SoMe accounts, rather than sought out and interviewed. Both the primary sources and the audience know this, which contributes to further accelerating the process of de-mediating information (Fontaine et al., 2018) and mainstreaming-mediated information prosumers (Bruns, 2005; Johnston, 2016). The challenges discussed by Pole and Gulyas in 2015 (Mangono et al., 2021) to the exclusivity of the traditional gate-keeper role of journalists are manifesting in how it’s being negotiated in an evolving and constant dialog between actors, audience, and reporters (Qualman, 2013).
In the case of complex scientific information, this may sometimes be viewed as a positive development, bearing in mind that journalists are not always able to command and communicate the latest health research findings with the same level of accuracy that healthcare professionals (HCPs) can have (Qualman, 2013).
However, in this media market, the fastest ones to step in to supply the increasing demand were not always necessarily the best qualified to do so (Zarocostas, 2020). This has been demonstrated by the often modest or poor quality of health information online, according to quality assessment research conducted by HCPs (Bernard et al., 2007). That problem seems to worsen in audiovisual resources, where the majority of video producers seem to be laypersons with regard to health information (Döring and Conde, 2021).
Today, celebrities and influencers commenting on public and global issues unrelated to their area of professional expertise have come to be heard by millions of followers (Gottlieb and Dyer, 2020), despite those followers’ varying perceptions of the credibility of the information and/or opinions they convey (Ducrot et al., 2021). To make things worse, recent research has suggested that false information travels faster and reaches a wider audience on SoMe than accurate information (Qualman, 2013). Research on misinformation has repeatedly pointed to how difficult it is to correct, forget or “undo” the effects of misinformation once it reaches the audience (Sui et al., 2021).
This led many voices from inside and outside the medical community to call upon medical and healthcare professionals to play an active role, confronting misinformation and disinformation and providing the public with more reliable information on this issue on the platforms where they are seeking it (O’Connor and Murphy, 2020; Zaidi et al., 2021).
The combination of the increasing infodemic, the changes in media dynamics and landscape with the appearance of a pandemic of the scale of COVID-19 has made HCPs’ contribution and involvement in SoMe communication of urgent need. HCPs, on the other hand, have expressed varying attitudes (Chari and Akpojivi, 2021; Drude et al., 2021) toward this new responsibility.
In this article we take a closer look at the attitudes and opinions formally published by HCPs and academics towards the use of SoMe as a tool to communicate health-related information directly with the public: How those attitudes have been developing since the decade preceding the COVID-19 outbreak, paying close attention to the concerns and hesitancies they have expressed. The aim is to inform efforts to develop strategies and plans to mitigate those concerns, with the hope that that will effectively help and encourage HCPs venturing into SoMe and resolve their hesitancies.
Our understanding of what constitutes the ¨medical community¨ in this context is based on the compound understanding of the following terms and dynamics: “Community”, “online community”, “communities of practice” and real to digital community transitioning. We find ourselves leaning towards Cobigo´s definition of community (Cobigo et al., 2016) as a group of people that interact and support each other, and are bounded by shared experiences or characteristics, a sense of belonging, and often by their physical proximity. We value Stanoevska-Slabeva´s description of online communities (Stanoevska-Slabeva, 2002) as being characterized by strong relationships between participants, community-specific structure and modes of discourse, common vocabulary, common meaning, shared history, community rituals, continuity of communication and a common on-line meeting space. We rely on Wenger´s definition of communities of practice (Wenger, 1998) as groups of people who share a passion for something that they know how to do, and who interact regularly in order to learn how to do it better. We also favor the very sincere Webster’s Dictionary definition of the medical community (Webster-Dictionary, 2023) as the body of individuals who are qualified to practice medicine. Our understanding of the evolution of “real” face-to-face communities into digital communities has been informed by the work of Diez-Bosch that has found that the three key elements of building consolidated online communities are content, services, and social networks where open debate is facilitated (Díez-Bosch et al., 2018).
To get a sense of what the professional attitudes within this roughly defined community are and how they have been developing, we chose to review the literature format designed to express professional opinions in this field of knowledge: Editorial articles, as well as opinion and commentary articles.
While acknowledging that this medium has limited quantitative representative value of the overall medical community opinions and practices, we find it to be one that holds a highly esteemed qualitative value, in that it articulates detailed opinions, that are of enough importance and urgency to their holders to motivate them to undergo the lengthy process of academic journal publication, in order to voice them out to their fellow professionals. It has limited potential for generalizing results, but it helps us understand how the argument of the attitude is constructed.
Objectives
General objectives
This editorial review aims to trace how formally expressed attitudes by members of the HCP community have been developing towards the use of SoMe by individual HCPs, as a tool for communicating health-related information, advice, and the latest research findings to the public directly, without the mediation of media professionals. It does not look at health institutions and their official communication officers and SoMe accounts, but rather at the efforts of individual HCPs themselves. The varying uses of SoMe in iHealth, information & knowledge sharing, networking, promotion and overall professional development have been attracting the attention of HCPs and institutions worldwide for many years (Rukavina et al., 2021). More recently, the potential of SoMe to monitor and forecast the development of virus spread in cases of pandemics is also gaining momentum, raising interest and questions both technical, legal and ethical. However, in this paper, the focus is exclusively on the use of SoMe by HCPs that address an open audience with information to help educate, engage and raise public awareness on varying health issues and the latest scientific research developments. Attitudes are assessed by whether or not they are optimistic and favorable toward this use.
Specific objectives
-
Determine if views expressed in editorials have a positive view or a negative/cautious view of this use of SoMe by HCPs. Although most editorials are well-balanced articles that do not look at only one side of the coin but are aware of both positive and negative aspects of the issue, however, as opinion pieces often do, they can and do elaborate more on the perspective they adopt.
-
List the most common contributors to the cautious/negative views, as expressed through concern issues mentioned in those editorials, that arise with the use of SoMe by HCPs. We have assumed that the more often a concern is mentioned, the more likely it is to be shared among a large proportion of the HCP community, or perhaps the more serious its hazards are viewed in the practice of HCPs. Thus, the concern list is organized in order of most commonly cited to least cited concerns.
Methodology
Through expressed opinions in editorial, opinion, and commentary articles of English language academic publications, this editorial review attempts to trace the development of the medical community’s formally expressed attitudes towards the use of SoMe to communicate with the public. The reasons for choosing these types of articles are three-fold. First, they are written by accredited professionals in the field, speaking from a position of verified experience, and willing to undergo the lengthy publication process to address the issue raised. Second, they are published in journals that value the accuracy of the information and peer review approvals, and yet, thirdly, they are also articles that do not limit themselves to data but are designed to be the place where authors explicitly express their opinions and attitudes, as well as their reasoning for it and make their stance officially acknowledged. Whilst we are aware that surveys and questionnaires may be more quantitively representative, opinions in them are sought out, not expressed on purpose by their owners, and are often quantified separately from their motifs, which then may or may not be answered and/or processed in predominantly open-ended questions. This has enabled us to also delve deeper into the main concerns behind those opinions, as explicitly presented by their owners, to better understand how they were constructed. Yet we find it is important to note the limitations on the accurate representation that editorials and opinion pieces give rise to, exactly for being most commonly authored by seasoned professionals and not by a representative sample of the HCP community.
Initially, our main review questions were centered specifically around the use of the video format on SoMe, to understand the medical community’s attitude towards the use of video explanations and video blogs (or vlogs), on social media by healthcare professionals to communicate health-related information to the public.
However, after developing the appropriate Boolean syntax, using it in seven databases, and filtering the results through the necessary selection process, only eight editorial articles on the subject were found. This very limited number encouraged us to broaden our search to explore the use of SoMe in general, regardless of format.
Thus, the main review question became: “How have the medical community’s expressed attitudes towards the use of social media by healthcare professionals to communicate health-related information to the public developed since the decade preceding the COVID-19 outbreak?”
Search
To answer that, we used the Boolean syntax: (Healthcare professional OR doctor OR nurse) AND (social media OR Twitter OR Facebook OR YouTube OR Instagram OR TikTok). It was elaborated and tailored to be used in 5 academic databases (Scopus, PubMed, Psychology and Behavioural Sciences Collection, MEDLINE, Communication and Mass Media Complete). Filters were applied to limit the search to the years 2010–2022, and the articles to peer-reviewed, editorial, opinion or commentary articles only. The search was carried out in both titles and abstracts of articles, and it was last updated in December 2022.
The reason for selecting those SoMe platforms (Facebook, YouTube, Instagram and TikTok) is that they were the top 4 ranked in 2022 (Statista, 2022) that offer the chance of following a public figure or person outside of the direct personal contact circle (WhatsApp and WeChat were excluded). Twitter was added to them because it is often cited as the platform most used by HCPs (Jackson et al., 2018).
Selection
The results from the five databases were cross-checked for duplications and filtered again on the Rayyan review tool to include at least one of the following keywords in their title or abstract (Social Media, Twitter, Facebook, Instagram, YouTube, TikTok, infodemic, video, disinformation, misinformation). The filtered articles underwent title and abstract screening. Given the fact that many editorials did not have an abstract in the databases, the full article was screened when no abstract was available.
Only articles that discussed the use of SoMe by HCPs communicating health-related information to the public were included in the detailed narrative review. Excluded were articles that discussed other uses of SoMe by HCPs (as a research tool, for inter-medical information sharing or networking within the medical community, for advertising or self-promotion), articles that discussed health-related information on other non-SoMe platforms or only mentioned SoMe as a backdrop or context for their main focus theme, and articles that discussed health-related information on SoMe that are not provided by HCPs or not aimed at the public (wrong combination) or that discuss the regulation or the monitoring of the use of SoMe for health-related information sharing. Additionally, a few articles that were not medically related were also excluded.
Analysis
Articles that passed the title and abstract screening underwent a qualitative content analysis in three stages: The first was the overall attitude labeling stage; a deductive analysis (Kibiswa, 2019) whereby the articles were categorized into 1 of 3 pre-determined categories (Positive attitude, cautious attitude, and negative attitude) after undergoing a review by the three authors, followed by a discussion to determine and conclude any disagreement in the categorization decisions. Articles were considered as having a positive attitude toward HCPs’ professional use of SoMe if they expressed optimism about this practice, explained its benefits and/or encouraged HCPs to engage in it. They were considered cautious if they expressed both optimism and concerns and concluded on a careful nuanced note. Articles were considered negative if they expressed ample and/or strong concerns about engagement in this practice and concluded on a pessimistic/worried note.
The next step was tracing out the different stages of the study period through an inductive analysis whereby an open categorization process was used based on the emerging themes observed in the initial first of the review. Those thematic categories are The level of technical knowledge about SoMe platforms (that the authors have or that the authors assume the readers possess), the promoted aspects of the use of SoMe in a professional healthcare function, commonly recurring issues addressed, and the consideration given to the quality of the content shared on those platforms and their developing dynamics.
Later, a close reading of the articles permitted the identification of relevant content and its assigning under the four established analysis categories, the results are demonstrated in Table 2, with 1 example quote provided as evidence for each category and stage. From the grouping of content into the 4 thematic categories we were able to construct the temporal patterns that lead us to establish the three research stages.
The third stage of analysis done was also an inductive analysis of open categorization that led to extracting, organizing and observing the development trajectory of the most common concerns about HCPs’ use of SoMe that were mentioned in the selected articles. Special attention was made here to the effects the COVID-19 pandemic had on the issue, and an additional table (Table 6) was dedicated to it.
Results
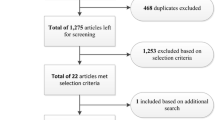
The sifting process resulted in finding 38 articles that met the selection criteria. They are presented visually here as a flow diagram in Fig. 1.
The total number of articles labeled as having a positive overall attitude towards HCPs’ use of SoMe to communicate with the public was 19, while the other 19 were labeled as having a cautious or negative attitude.
Included articles are distributed according to the study stage and attitude as per Table 1. The increase in the average number of published articles on the topic per year according to the three-stage distribution and the shifts in the positive to cautious/negative article ratios compared to the total number of articles per stage are visualized in Fig. 2.
The included articles are detailed by name, stage, publication year, author, attitude and a quote expressing the attitude orientation in Table 2.
As explained earlier, the research period (2010–2022) was divided into three stages according to the content development of four thematic categories: The first stage is 2010–2015, the second is 2016–2018 and the third is 2019–2022.
Table 3 presents the four thematic categories and their content development accompanied by a single quote from each stage that we found best exemplifies the characteristics detected in that stage.
Articles in the first stage tended to be somewhat exploratory in how they introduced the topic of SoMe use in healthcare and demonstrated simple technical knowledge of the platforms, often explaining basic concepts to their readers, such as what an SMS is or a blog or a tweet. Many of them seemed most fascinated by the outreach of SoMe and the unprecedented speed with which users can broadcast directly to huge numbers of people. Oftentimes they spoke from an exploratory perspective, introducing the platforms and their tools and functions, and invited their readers to join, discover and benefit from the new advantages those tools offer. Little attention was given here to the quality of the content shared on those platforms or the platform design consequences on the dynamics of the discourses.
In the 2nd stage, the technical knowledge was slightly more advanced, no longer introducing the platforms but rather commenting on good or bad experiences using them, new achievements reached or problems faced over time with their use. They generally assumed more knowledge in their readers and discussed practical issues that can face by those embarking recently on using them in a professional context. More attention was given here to the content quality and the emerging dynamics that were starting to clarify, both positive and negative.
In the 3rd stage, many authors had come a long way in developing technical know-how, not only of the average-user tools but also of advanced content creator issues, and platform design and management issues. Few articles entertained a novel user with simple technical introductions. Articles here started discussing issues resulting from specific aspects of the tools, and how they can be solved. Attention was given to the complexity of the problems that had crystallized. Solution approaches varied very much, unlike the initial stage which suggested little more than guidelines and rulebooks. The quality of the content shared and the role of platform design in pushing, promoting, sidelining or challenging different types of content and content sources became a very recurring concern in this stage. Advice given to HCPs here was more related to mitigating negative platform dynamics by collective, institutional and global negotiation and advocacy efforts than to managing security settings to maintain information privacy as had been the case previously. The scale of the approach toward the use of SoMe in public health communication had expanded remarkably.
As for the most common concerns cited in those articles as negative effects of the use of SoMe by HCPs, they are listed in Table 4, ordered by frequency, and distribution over the study period stages. Table 5 presents a detailed list of those concerns, the articles that mentioned them with one quote from each article for each concern.
Finally, Table 6 is dedicated specifically to the COVID-19 pandemic repercussions on the infodemic and public health communication concerns as expressed by the selected articles.
Discussion
To understand the development of the HCP’s formally expressed attitudes towards the use of SoMe to inform the public on health-related issues, we looked closely at editorials from the decade preceding the outbreak of COVID-19 that discuss this topic and traced an increase in hesitancy towards SoMe.
Unfortunately, we were unable to find previous editorial review articles on this subject to cross-check our findings with and draw comparisons. Thus, we decided to use opinion and attitude survey research as cross-checking references to measure how coherent our findings are with available research on the subject. We take a look at several surveys conducted since 2010 among HCPs concerning their attitudes towards professional SoMe use and compare their findings with those of our editorial review. One of the most orienting survey findings to our study is that of the age denominator: Repeatedly, throughout all three stages, surveys have noticed clear differences in SoMe attitudes between younger and senior generations of HCPs (Bellini et al., 2020; Casà et al., 2021; Adilman et al., 2016; Brown et al., 2014; Wagner et al., 2018; Keller et al., 2014).
This helps us contextualize our findings and gives a more optimistic view: younger generations are more likely to use SoMe in general, and they are more likely to use it in a more nuanced and technically advanced manner. Their overall attitudes tend to be more positive than those of their seniors. Taking into consideration that editorial articles are often written by seasoned professionals with some years of experience behind them (Freda and Kearney, 2005; Leslie and Hemmings, 2020), this might indicate that the reality and future of HCP’s attitudes towards SoMe are brighter than the numbers in our review indicate. On the other hand, this also draws our attention again to the question of representation amongst HCPs and the limitations of editorial articles as accurate reflections of the opinions, attitudes and concerns of the medical community in general.
Survey research has also concluded that the main concerns behind SoMe hesitancy among HCP are personal and patient privacy and security concerns (Adilman et al., 2016), legal concerns (Brown et al., 2014), lack of perceived value of SoMe (Wagner et al., 2018), time constraints (Keller et al., 2014), as well as worries over a possible deterioration of accountability, professional image, confidentiality, and professional boundaries (Rukavina et al., 2021)
Our discussion is presented using the same three-stage-order we have established in our results section, based on its findings.
The initial stage: This stage was slightly cautious but generally positive. Privacy, decorum, reputation and relationship boundaries were the first concerns to be discussed in editorials in the earlier stages of SoMe use by the HCP’s community. Those were not new concerns in the world of HC communication, of course, they simply took on a new shape with the use of the new technology. The initial stage concerns tended to be more logical in nature: Based on the problems one would anticipate could potentially occur with the use of SoMe, according to the somewhat simple understanding of SoMe functions and dynamics that was readily available back then. It may serve well to remember here that this was the era when many senior professionals were still discovering what SoMe is, as well as its advantages and disadvantages. This is reflected in survey findings from this stage, where results in Australia for example in 2014 indicated that one-quarter of surveyed doctors did not use any social media websites at all, and only 1 of the entire sample of 187 respondents had used social media (eg, Twitter or Facebook) to communicate with patients.
It can thus be assumed that some forecasting might have been needed at this stage as many questions remained open for development and experience to answer them. So, it is not surprising that most of those concerns had been re-applied from the pre-SoMe communication era to the post-SoMe era.
One might consider any hesitancy at this stage as a normal part of the discovery process, where the 2014 survey-based research (Brown et al., 2014) found that “few doctors were able to adequately protect their information online…. The older participants were, the less likely they were to know how to remove photos of themselves they wouldn’t want patients to see. No participant aged over 65 years knew how to do this”. It concluded that it has found “a surprising reluctance to engage with the new media despite the demands of the community.”
Also worth noting is that a good deal of focus was centered around how HCPs used those platforms, or rather “behaved” on them: Should they befriend patients, should they have separate professional and private accounts, should they address wrong or misleading health information they come across, etc… Little attention was paid in this stage to how the public used SoMe for health-related information, or how the platforms were designed and functioned. Popular narratives, patient content sharing and debate dynamics were viewed in a similar way to waiting-room patient-chit-chat. The underlying assumption there being that the digitalization of the format was the only new aspect.
We repeatedly came across articles that referred to a pre-existing institutional hesitancy towards the use of SoMe as something that is frowned upon and deemed unnecessary and perhaps even inappropriate in an HCP context (Ho, 2014; Trethewey, 2020; Zaidi et al., 2021). References to strict guidelines quoted more cautioning and alarm than encouragement and sharing of know-how. A military physician article (Balog et al., 2012) even dated the shift by year in a perfect match to our study phase initiation in 2010: ¨The Department of Defense’s (DoD’s) decision to open social media access to military members in February 2010 signals a major shift in policy.¨. This was more clearly noted in positive attitude articles of this stage that expressed some level of frustration with the old-school mindset. So, we decided to take a closer look into pre-2010 editorials and were only able to find 2, quite negative, articles discussing the matter (Dossey, 2009; Freshwater, 2009).
This lack of publication might be translated as a lack of interest in or disregard of the matter, perhaps. That added to the negative attitude in the only found articles, and to the repeated references from post-2010 articles, all indicate that the pre-2010 era had probably been a stage of early hesitancy. However, the very limited number of articles means we have little evidence to go by. Thus, we maintain it as a hypothesis in need of further exploration.
The middle stage: The near tie between positive and cautious/negative attitudes in this stage make it a stage of gradual transitioning.
A certain amount of practice and know-how seems to have gradually spread. This is reflected in the slight increase in technical details discussed, and the self-promotional or celebrative tone in some articles announcing new SoMe achievements in HC practice and knowledge-sharing activities. In those articles, the focus is on the new opportunities and potential SoMe can open up, as well as sharing experiences and the latest advancements achieved by HCPs that have taken up one platform or the other. On the other hand, some articles started to comment on the content of public discourse and narratives and to question the structures of SoMe platforms and their effect with deeper technical knowledge. The more optimistic articles in this stage tended to express a simpler view of the technology, and often labeled the public discourse as empowering users and creating support networks and communities amongst patients.
In this phase, SoMe was no longer viewed as a tool to simply socialize casually with friends and family and its professional uses increased in many fields, gaining it more value and stance in society as a whole. In survey research, several papers in this stage expressed the justification of the research carried out to be the need to improve HCP’s participation in professional SoMe (Adilman et al., 2016) use by understanding their attitudes towards SoMe and the concerns behind their hesitancy to engage more actively with it (Wagner et al., 2018).
The more serious implications of SoMe developments had not yet created many scandals or panic. According to a study on the spread of Health-related misinformation on SoMe, it was the controversy around SoMe’s role in the election of the previous US president Donald Trump in 2016 that marked the end of well-intentioned naïveté in many people´s relationship with SoMe (Wang et al., 2019) and the starting point of much controversy, concerns and hesitancies. This falls rather neatly within our 3 stage division dates. It was the year 2017 in which the term “fake news” was selected word of the year by the Collins Dictionary (2017). The clearer reflection that had on published peer-reviewed editorials in this review seemed to have staggered a year behind, till past 2018, perhaps due to the lengthy publication processes in peer-review journals.
News of voter fraud in the USA (Shane, 2017) and other countries (Euronews, 2017), bots (Baraniuk, 2017) and troll industry (Bradshaw and Howard, 2017; Walker, 2017), user data commerce and leaks of industry-scale privacy breaches (Cadwalladr and Graham-Harrison, 2018), as well as algorithm ̈dilemmas ̈ (Orlowski and Rhodes, 2020) that highlight instances of contradiction between financial gains from increased usage volume and social & civil rest, all contributed to ushering in the age of wide infodemic concerns.
The third stage: A clear advance was noted in the level of sophistication of various categories of the analysis in this stage.
It’s a phase characterized by more complex, more nuanced concerns by professionals with a deeper technical understanding of SoMe platform dynamics, algorithms and commercial interests, as well as legal dilemmas and political consequences. The concerns voiced here are very well informed in comparison with those of the initial phase, yet they are less likely to consider withdrawal, abstinence or minimizing SoMe use and engagement as a solution.
In this stage, the focus had shifted off of each individual HCP’s usage of SoMe towards a more collective perspective on the issues of concern. The health-related content that is being shared on SoMe platforms by laypersons became a matter of mounting concern in this phase. The public discourse and the pseudo-science, conspiracy theories or post-truth narratives gaining momentum with algorithms that favor engagement over content quality took center stage, and many of the solutions suggested by the editorials were a result of analyzing the complex factors at play: Commercial interests of SoMe platforms and the legal and ethical complexity of regulating them, cross-border politics and influence over the world wide web, new concerns over SoMe addiction, dependencies and echo-chambers arguably worsened by the COVID-19 quarantine, etc.
Amidst all that, the attention given to the contributions of individual HCPs battling the infodemic was now seen within a much wider and more complex context. Calls were no longer for mere guidelines each hospital or university should set for its staff and trainees as was the case in the initial phase, but rather for inclusive strategies created and implemented with institutional partners from other fields, such as media enterprises, political bodies and activists, data scientists and SoMe platforms management, in addition to global and national health organizations. The call for further training developed into a call for curriculum changes to educate the upcoming generations of HCPs on SoMe use as a regular and challenging part of their work. This was also reflected in several survey research conclusions expressing concern about digital literacy and the competence of current and future HCPs (Casà et al. 2021; Rukavina et al., 2021).
Limitations
The age denominator effect
Since editorial authors are often senior professionals as we have seen, and statistical surveys have confirmed younger HCPs expressing more positive and engaged attitudes towards SoMe use, this could indicate that the reality of the community’s attitudes is more optimistic than is reflected in an editorial review.
The lack of interest in discussing the video format in editorials might also be due to that format being notoriously used by and aimed toward younger users.
The gender gap
Most (ca. 65%) editorials included were written by men, and the content of most of them did not report on nor discuss any differences encountered between male and female HCPs. In comparison with surveys, where gender demographics are routinely considered, a recent study on online harassment and career advancement (Woitowich et al., 2021) said 1 in 6 female HCPs were harassed, while male counterparts reported benefitting from increased opportunities and networking as a result of their SoMe activities.
Representation and reality of practice
In addition to the obvious age and gender factors, many other factors are at play and should be accounted for when distinguishing our article sample authors from the entirety of the medical community. A more in-depth exploration of those factors and the question of representation within the medical community is needed. It is also worth noting that the relationship between opinions, attitudes and concerns in articles with actions and practice in real life is not a simple linear one. Exactly how those attitudes may reflect on the reality of HCP´s use of SoMe remains a question to explore in further research.
Sample size
The somewhat limited number of articles included in this review demands caution in drawing firm generalizations. This was mitigated to a certain extent by the comparison with survey research results.
Also worth noting is the fluid nature of the 3-stage system this review results have been organized in. There were rare instances of exceptionally advanced articles in the first stage, or simplistic ones in the final stage. However, the review here expressed the overall trend in those phases, while being aware that a shift of a few years forward or back can occur for some authors.
During the database search, the Boolean syntax was amended according to each database search engine system and filter. As many synonyms to HCPs as possible were used in most of them, and yet many other synonyms, certainly specialties, were not included. Citation threading later revealed that many editorials included only the name of the narrow specialization (cardiologist, dermatologist, psychiatrist, etc.) which prevented even a very elaborate Boolean syntax from finding them. Future research could perhaps benefit from the use of citation threading (reverse research).
Conclusion
We conclude that the editorial opinions of HCPs towards professional SoMe use can be seen to bare shifting hesitancies and concerns. However, the earlier SoMe hesitancy (SoMeH) sensed in the pre-2010 era and noted in the concerns cited in the initial stage (2010–2015) could have had somewhat different underlying reasons, such as lack of knowledge and experience, in comparison with the later stage (2019–2022) hesitancy and concerns that were based on well-informed research on global developments in the world of SoMe, infodemic and COVID-19. The orientation of the hesitancy shifted over the years from being mainly preoccupied with the way HCPs used SoMe and the content they shared on it, to worrying about the medium itself; SoMe platform design, algorithms, non-HCP user-generated content and the discourse dynamics that emerged. This was exacerbated by the Covid-19 pandemic when concerns sounded notably stronger alarm tones. The middle stage balance can be considered as that of transition, a coming-of-age of sorts when newly acquired skills started helping mitigate some of the initial stage concerns and the new wave of problems had just begun to loom.
Better, safer and more effective HCP engagement with SoMe and contribution to the fight against the infodemic could benefit from better understanding the attitudes, concerns and hesitancies of HCPs. Understanding can help mitigation, aid and training strategies and programs on local, national and global levels create better plans to integrate millions of HCPs worldwide in the much-needed, and complex-designed, efforts against health misinformation and disinformation feeding the infodemic.
Further research is needed that focuses more clearly on HCPs’ use of SoMe to address the general public, as most research reviewed in this article discussed various SoMe uses by HCPs. Also needed is more focus on specific aspects of HCP use of SoMe to address the public, such as platform-specific research or format-specific research, as the current literature largely assumes written or text-based communication, with little attention to visual material and almost ignores audiovisual and video blogging (vlogging) formats.
Data availability
The data that support the findings of this study were derived from the databases (Scopus, PubMed, Psychology and Behavioural Sciences Collection, MEDLINE, Communication and Mass Media Complete) available in the public domain
References
Abrams EM, Greenhawt M (2020) Mitigating Misinformation and Changing the Social Narrative. J Allergy and Clin Immunol Pract. https://doi.org/10.1016/j.jaip.2020.08.007
Adilman R, Rajmohan Y, Brooks E, Urgoiti GR, Chung C, Hammad N et al. (2016) Social media use among physicians and trainees: results of a national medical oncology physician survey. J Oncol Pract 12(1):e52–60
Ahmed OH, Weiler R, Schneiders AG, McCrory P, Sullivan SJ (2015) Top tips for social media use in sports and exercise medicine: doing the right thing in the digital age. BR J Sports Med. https://doi.org/10.1136/bjsports-2014-094395
Antonoff MB (2015) Thoracic Surgery Social Media Network: bringing thoracic surgery scholarship to Twitter. J Thorac Cardiovasc Surg 150:292–3. https://doi.org/10.1016/j.jtcvs.2015.06.006
Balog EK, Warwick AB, Randall VF, Kieling MC (2012) Medical professionalism and social media: the responsibility of military medical personnel. Mil Med 177(2):123–124
Baraniuk C (2017) The “creepy Facebook AI” story that captivated the media. https://www.bbc.com/news/technology-40790258. Accessed 1 July 2022
Bellini MI, Parisotto C, Dor FJMF, Kessaris N (2020) Social Media use among transplant professionals in Europe: a cross-sectional study from the European Society of Organ Transplantation. Exp Clin Transplant 18(2):169–76
Bennett K, Berlin NL, MacEachern MP, Buchman SR, Preminger BA, Vercler CJ (2018) Discussion: The Ethical and Professional Use of Social Media in Surgery: A Systematic Review of the Literature. Plast Reconstr Surg. https://doi.org/10.1097/PRS.0000000000004692
Berg SH, O’Hara JK, Shortt MT, Thune H, Brønnick KK, Lungu DA et al. (2021) Health authorities’ health risk communication with the public during pandemics: a rapid scoping review. BMC Public Health 21(1):1–23
Bernard A, Langille M, Hughes S, Rose C, Leddin D, Veldhuyzen van Zanten S (2007) A systematic review of patient inflammatory bowel disease information resources on the World Wide Web. Am J Gastroenterol 102:2070–7
Bradshaw S, Howard PN (2017) Troops, Trolls and Troublemakers: a global inventory of organized Social Media manipulation. http://governance40.com/wp-content/uploads/2018/11/Troops-Trolls-and-Troublemakers.pdf Accessed 1 Jul 2022
Brown J, Ryan C, Harris A (2014) How doctors view and use social media: a national survey. J Med Internet Res. https://doi.org/10.2196/jmir.3589
Bruns A (2005) Gatewatching: collaborative online news production. Peter Lang Publishing, New York
Cadwalladr C, Graham-Harrison E (2018) Revealed: 50 million Facebook profiles harvested for Cambridge Analytica in major data breach. https://www.theguardian.com/news/2018/mar/17/cambridge-analytica-facebook-influence-us-election Accessed 1 Jul 2022
Camm CF (2012) Should doctors be more careful with social media? Ann Med. Surg. https://doi.org/10.1016/S2049-0801(12)70003-1
Campbell I, Rudan I (2020) Helping global health topics go viral online. J Global Health. https://doi.org/10.7189/jogh.10.010101
Casà C, Marotta C, di Pumpo M, Cozzolino A, D’Aviero A, Frisicale EM et al. (2021) COVID-19 and digital competencies among young physicians: are we (really) ready for the new era? A national survey of the Italian Young Medical Doctors Association. Ann Dell’Ist Super Sanita 57(1):1–6
Cataldi JR, O’Leary ST, Leary STO (2021) Addressing vaccine concerns: a hopeful path forward for vaccine confidence. Am J Public Health 111(4):556–8
Chari T, Akpojivi U (2021) Media and global pandemics: continuities and discontinuities. JAMS. https://doi.org/10.1386/jams_00050_2
Cobigo V, Martin L, Mcheimech R (2016) Understanding community. Can J Disabil Stud. https://doi.org/10.15353/cjds.v5i4.318
Collier R. (2018) Containing health myths in the age of viral misinformation. CMAJ. https://doi.org/10.1503/cmaj.180543
Díez-Bosch M, Micó-Sanz J, Sabaté-Gauxachs A (2018) Construction of online communities based on consolidated face-to-face communities. The case of Catholic church on the Internet. Prof Inf. https://doi.org/10.3145/epi.2018.nov.09
Dorfman RG, Vaca EE, Fine NA, Schierle CF (2017) Discussion: The Ethics of Sharing Plastic Surgery Videos on Social Media: Systematic Literature Review, Ethical Analysis, and Proposed Guidelines. Plastic and Reconstructive Surgery. https://doi.org/10.1097/PRS.0000000000003695
Döring N, Conde M (2021) Sexual health information on social media: a systematic scoping review. Bundesgesundheitsbl Gesundheitsforsch Gesundheitsschutz 64:1416–29
Dossey L (2009) Plugged in: at what price? The perils and promises of electronic communication. J Sci Heal. https://doi.org/10.1016/j.explore.2009.06.006
Drude KP (2021) Introduction to the special edition on social media. J Technol Behav Sci. https://doi.org/10.1007/s41347-021-00217-3
Ducrot P, Montagni I, Nguyen Thanh V, Serry AJ, Richard JB (2021) Evolution of online health-related information seeking in France from 2010 to 2017: results from nationally representative surveys. J Med Internet Res 23(4 Apr):e18799
Euronews (2017) Fraud, fakes and photoshops…. the online war over the Catalan referendum. Euronews. https://www.euronews.com/2017/10/02/fakes-and-questionable-votes-the-polemics-of-the-catalan-referendum Accessed 1 July 2022
Eysenbach G (2002) Infodemiology: the epidemiology of (mis)information. Am J Med 113(9):763–765
Eysenbach G (2020) How to fight an infodemic: the four pillars of infodemic management. J Med Internet Res. https://doi.org/10.2196/21820
Fagherazzi G, Goetzinger C, Rashid MA, Aguyayo GA, Huiart L (2020) Digital health strategies to fight COVID-19 worldwide: challenges, recommendations, and a Call for Papers. J Med Internet Res. https://doi.org/10.2196/19284
Fake news Collins Dictionary (2017) https://blog.collinsdictionary.com/language-lovers/collins-2017-word-of-the-year-shortlist/ Accessed 29 May 2022
Fontaine G, Lavallée A, Maheu-Cadotte MA, Bouix-Picasso J, Bourbonnais A (2018) Health science communication strategies used by researchers with the public in the digital and social media ecosystem: a systematic scoping review protocol. BMJ Open 8:e019833–e019833
Freda MC, Kearney M (2005) An international survey of nurse editors’ roles and practices. J Nurs Scholar. https://doi.org/10.1111/j.1547-5069.2005.00006.x
Freshwater F (2009) Internet communication and education. J Plast Reconstr Aesthet Surg. https://doi.org/10.1016/j.bjps.2009.04.009
Gardner JM (2017) How Angiosarcoma and Facebook changed my life. Arch Pathol Lab Med 141:188. https://doi.org/10.5858/arpa.2016-0447-ED
Goitz RJ (2021) CORR Insights (R): Most YouTube Videos About Carpal Tunnel Syndrome Have the Potential to Reinforce Misconceptions. Clin Orthop Relat Res. https://doi.org/10.1097/CORR.0000000000001896
Gottlieb M, Dyer S (2020) Information and disinformation: social media in the COVID-19 crisis. Acad Emerg Med. https://doi.org/10.1111/acem.14036
Grant R (2017) Public health professionals urgently need to develop more effective communications strategies. Am J Public Health. https://doi.org/10.2105/AJPH.2017.303738
Hill J. (2019) Medical misinformation: Vet the message! Heart Rhythm. https://doi.org/10.1111/pace.13616
Hill JA, Agewall S, Baranchuk A, Booz GW, Borer JS, Camici PG et al (2019) Medical misinformation: vet the message! Heart Rhythm. https://doi.org/10.1016/j.hrthm.2018.12.030
Ho K (2014) Harnessing the social web for health and wellness: issues for research and knowledge translation. J Med Internet Res. https://doi.org/10.2196/jmir.2969
Ho K. et al. (2014) Harnessing the social web for health and wellness: issues for research and knowledge translation. J Med Internet Res. https://doi.org/10.2196/jmir.2969
Jackson J, Gettings S, Metcalfe A (2018) “The power of Twitter”: using social media at a conference with nursing students. Nurse Educ Today. https://doi.org/10.1016/j.nedt.2018.06.017
Johnston L (2016) Social news=journalism evolution? Digit Journalism. https://doi.org/10.1080/21670811.2016.1168709
Jones C, Hayter M (2013) Editorial: social media use by nurses and midwives: a “recipe for disaster” or a “force for good”? J Clin Nurs. https://doi.org/10.1111/jocn.12406
Katz A (2019) Social media and scholarly publication: what is the connection? Oncol Nurs Forum. https://doi.org/10.1188/19.ONF.517-518
Keller B, Labrique A, Jain KM, Pekosz A, Levine O (2014) Mind the gap: social media engagement by public health researchers. J Med Internet Res 16:1–8
Kibiswa N (2019) Directed Qualitative Content Analysis (DQlCA): a tool for conflict analysis. Qual Rep 24(8):2059–2079
Krawiec JM, Piaskowska OM, Piesiewicz PF, Białaszek W (2021) Tools for public health policy: nudges and boosts as active support of the law in special situations such as the COVID-19 pandemic. Glob Health. https://doi.org/10.1186/s12992-021-00782-5
Leininger L, Albrecht S, Buttenheim A, Dowd J, Ritter A, Simanek A, Valentino M, Jones M (2022) Fight Like a Nerdy Girl: The Dear Pandemic Playbook for Combating Health Misinformation. A J Health Promotion. https://doi.org/10.1177/08901171211070956
Mach K. et al. (2021) News media coverage of COVID-19 public health and policy information. HSSC. https://doi.org/10.1057/s41599-021-00900-z
Mangono T, Smittenaar P, Caplan Y, Huang VS, Sutermaster S, Kemp H et al. (2021) Information-seeking patterns during the COVID-19 pandemic across the United States: longitudinal analysis of Google Trends Data. J Med Internet Res 23(5 May):e22933
McCarthy C, DeCamp M, McEvoy J (2018) Social Media and Physician Conflict of Interest. A J of Medicine. https://doi.org/10.1016/j.amjmed.2018.02.011
McLean R, Shirazian S (2018) Women and kidney disease: a Twitter conversation for one and all. Kidney Int Rep. https://doi.org/10.1016/j.ekir.2018.05.001
O’Connor C, Murphy M (2020) Going viral: doctors must combat fake news in the fight against Covid-19. Ir Med J 113(5):85–85
Orlowski J, Rhodes L (2020) Exposure labs. The social dilemma. https://www.thesocialdilemma.com Accessed 1 Jul 2022
Park JH, Christman MP, Linos E, Rieder EA (2018) Dermatology on Instagram: an analysis of hashtags. J Drugs Dermatol 17:482–484
Pole K, Gulyas A (2015) Global social journalism study. https://doi.org/10.13140/RG.2.1.4031.6968
Qualman E (2013) Socialnomics: how social media transforms the way we live and do business, 2nd edn. John Wiley & Sons, New Jersey
Queen D, Harding K (2014) Social media can revolutionise health care provider–patient relationship. Int Wound J https://doi.org/10.1111/iwj.12268
Ratzan Scott C (2011) Our new “social” communication age in health. J Health Commun. https://doi.org/10.1080/10810730.2011.610220
Rossi M (2020) Editorial Commentary: YouTube Meniscus Videos Have Poor Reliability and Quality: Videos Uploaded by Physicians Are Evidence-Based Superior and Show Few “Dislikes”. J Arthroscopic & Related Surgery. https://doi.org/10.1016/j.arthro.2019.10.006
Rukavina TV, Viskić J, Poplašen LM, Relić D, Marelić M, Jokic D et al. (2021) Dangers and benefits of social media on e-professionalism of health care professionals: scoping review. J Med Internet Res 23(11):1–25
Salik JR (2020) From cynic to advocate: the use of Twitter in cardiology. J Am Coll Cardiol 76:623–627. https://doi.org/10.1016/j.jacc.2020.06.050
Scott J (2021) Managing the infodemic about COVID-19: strategies for clinicians and researchers. Acta Psychiatr Scand 143(5):377–9
Shane S (2017) The fake Americans Russia created to influence the election. https://www.nytimes.com/2017/09/07/us/politics/russia-facebook-twitter-election.html. Accessed 1 July 2022
Shaun W. Russian troll factory paid US activists to help fund protests during election. https://www.theguardian.com/world/2017/oct/17/russian-troll-factory-activists-protests-us-election. Accessed 1 July 2022
Leslie K, Hemmings Jr HC (2020) Excellence in editorials: fulfilling their critical role in the medical literature. Br J Anaesth. https://doi.org/10.1016/j.bja.2020.06.061
Stanoevska-Slabeva K (2002) Toward a community-oriented design of Internet platforms. Int J Electron Commer 6(3):71–95
Statista (2022) Most used social media. Statista. https://www.statista.com/statistics/272014/global-social-networks-ranked-by-number-of-users/. Accessed 18 Dec 2022
Su Z, McDonnell D, Wen J, Kozak M, Abbas J, Šegalo S et al. (2021) Mental health consequences of COVID-19 media coverage: the need for effective crisis communication practices. Glob Health. https://doi.org/10.1186/s12992-020-00654-4
Sui YJ, Zhang B, Sui Y, Zhang B (2021) Determinants of the perceived credibility of rebuttals concerning health misinformation. IJERPH. https://doi.org/10.3390/ijerph18031345
Sun Y, Zhang Y, Gwizdka J, Trace CB (2019) Consumer evaluation of the quality of online health information: systematic literature review of relevant criteria and indicators. J Med Internet Res 21:e12522
Sylow L (2021) Three challenges of being a scientist in an age of misinformation. J Physiology. https://doi.org/10.1113/JP281434
Thorp HH (2021) Public debate is good for science. Science. https://doi.org/10.1126/science.abg4685
Trethewey SP (2020) Strategies to combat medical misinformation on social media. Postgrad Med J. https://doi.org/10.1136/postgradmedj-2019-137201
Varghese TK, Entwistle JW, Mayer JE, Moffatt-Bruce SD, Sade RM, Blitzer D, et al. (2019) Ethical standards for cardiothoracic surgeons’ participation in social media. Ann Thora Surg. https://doi.org/10.1016/j.athoracsur.2019.04.003
Wagner JP, Cochran AL, Jones C, Gusani NJ, Varghese TK, Attai DJ (2018) Professional use of social media among surgeons: results of a multi-institutional study. J Surg Educ. https://doi.org/10.1016/j.jsurg.2017.09.008
Walker S (2017) Russian troll factory paid US activists to help fund protests during election. The Guardian. https://www.theguardian.com/world/2017/oct/17/russian-troll-factory-activists-protests-us-election. Accessed 1 July 2022
Wang Y, McKee M, Torbica A, Stuckler D (2019) Systematic literature review on the spread of health-related misinformation on social media. Soc Sci Med. https://doi.org/10.1016/j.socscimed.2019.112552
Webster-Dictionary (2023) Definition of medical community by Webster’s Online Dictionary. https://www.webster-dictionary.org/definition/medical%20community. Accessed 15 Mar 2023
Wenger E (1998) Communities of practice: learning, meaning, and identity. Cambridge University Press, Cambridge
Woitowich NC, Arora VM, Pendergrast T, Gottlieb M, Seth Trueger N, Jain S (2021) Gender differences in physician use of social media for professional advancement. JAMA Netw Open. https://doi.org/10.1001/jamanetworkopen.2021.9834
World Health Organisation (2020) 10 global health issues to track in 2021. WHO. https://www.who.int/news-room/spotlight/10-global-health-issues-to-track-in-2021. Accessed 5 Apr 2022
Zaidi AU, Glaros AK, Weyand AC (2021) Navigating a new terrain: how Twitter is changing hematologists. Blood Adv 5(1):277–8
Zarocostas J (2020) How to fight an infodemic. Lancet 395(10225):676
Acknowledgements
The authors confirm there has been no significant financial support for this work that could have influenced its outcome.
Author information
Authors and Affiliations
Contributions
MD-B, LA and LR-R conceived and designed the methodology. LA searched and selected the articles included in the revision. MD-B, LA and LR-R analyzed the research results. LA wrote the first draft of the manuscript. LR-R and MD-B corrected and collaborated in the final revision of the article. The authors approved the final version of the article.
Corresponding authors
Ethics declarations
Competing interests
The authors declare no competing interests.
Ethical approval
This paper is based on publicly available documents and has not collected any personal, sensitive, or confidential information nor contains any studies with human participants and therefore has not required prior approval from any ethics committee.
Informed consent
This article does not contain any studies with human participants performed by any of the authors.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons license, and indicate if changes were made. The images or other third party material in this article are included in the article’s Creative Commons license, unless indicated otherwise in a credit line to the material. If material is not included in the article’s Creative Commons license and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this license, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
Alhafez, L., Rubio-Rico, L. & Diez-Bosch, M. Healthcare professionals’ editorial opinions on communicating with the public: shifting social media hesitancies. Humanit Soc Sci Commun 10, 343 (2023). https://doi.org/10.1057/s41599-023-01820-w
Received:
Accepted:
Published:
DOI: https://doi.org/10.1057/s41599-023-01820-w
- Springer Nature Limited