Abstract
Background
Brain metastases (BMs) are the most frequent intracranial tumours associated with poor clinical outcomes. Radiotherapy is essential in the treatment of these tumours, although the optimal radiation strategy remains controversial. The present study aimed to assess whether whole brain radiation therapy with a simultaneous integrated boost (WBRT + SIB) provides any therapeutic benefit over WBRT alone.
Methods
We included and retrospectively analysed 82 patients who received WBRT + SIB and 83 who received WBRT alone between January 2012 and June 2021. Intracranial progression-free survival (PFS), local tumour control (LTC), overall survival (OS), and toxicity were compared between the groups.
Results
Compared to WBRT alone, WBRT + SIB improved intracranial LTC and PFS, especially in the lung cancer subgroup. Patients with high graded prognostic assessment score or well-controlled extracranial disease receiving WBRT + SIB had improved intracranial PFS and LTC. Moreover, WBRT + SIB also improved the long-term intracranial tumour control of small cell lung cancer patients. When evaluating toxicity, we found that WBRT + SIB might slightly increase the risk of radiation-induced brain injury, and that the risk increased with increasing dosage. However, low-dose WBRT + SIB had a tolerable radiation-induced brain injury risk, which was lower than that in the high-dose group, while it was comparable to that in the WBRT group.
Conclusions
WBRT + SIB can be an efficient therapeutic option for patients with BMs, and is associated with improved intracranial LTC and PFS. Furthermore, low-dose WBRT + SIB (biologically effective dose [BED] ≤ 56 Gy) was recommended, based on the acceptable risk of radiation-induced brain injury and satisfactory tumour control.
Trial registration
Retrospectively registered.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Brain metastases (BMs) are the most common intracranial malignancy, with an incidence of approximately 8.3–14.3 per 100,000 people [1, 2]. Approximately 10–30% of cancer patients develop brain metastases during the course of the disease [3, 4]. For patients with malignant tumours, once BMs are observed, the disease is considered to have progressed to an advanced stage, and is frequently linked with a poor prognosis [2]. The median overall survival (OS) of patients with BMs receiving only symptomatic relief treatments is 1–2 months [5], and approximately 20–30% of patients die due to poor intracranial tumour control [6].
Currently, the primary treatments for brain metastases are surgery, radiation therapy, chemotherapy, targeted therapy, and immunotherapy [7]. For decades, whole brain radiation therapy (WBRT) has been utilised as the standard treatment option to relieve most patients’ symptoms and prolong their survival by several months [8, 9]. This is especially true for patients who are not suitable candidates for general surgery or stereotactic radiosurgery (SRS) [10]. According to the results of several studies, however, WBRT provides poor control of existing metastases [11, 12]. Therefore, WBRT plus a lesion-targeting radiation boost has been introduced as an effective strategy for improved tumour control [13,14,15,16,17,18,19]. This included three boost schemes: WBRT + SRS, WBRT with a simultaneous integrated boost (WBRT + SIB), and WBRT with sequential integrated boost (WBRT + SEB). Compared with others, WBRT + SIB does not prolong the overall duration of radiation, and requires only one radiation treatment plan [14]. Having a single treatment plan helps us confirm the dose to the organs at risk (OARs), and further reduces radiation therapy-related toxicities. Moreover, WBRT + SIB could be used to treat large-diameter tumours, for which SRS is not an option [20]. Studies on WBRT + SIB are still limited, although several small-scale retrospective studies have reported potential survival benefits for WBRT + SIB over WBRT [19, 21, 22]. WBRT + SIB, however, has not been extensively analysed in selected populations, such as small cell lung cancer (SCLC) patients, and research on toxicities and dose selection remains limited. The present study, therefore, aimed to evaluate whether WBRT + SIB provides any therapeutic benefit over WBRT alone.
Materials and methods
Patient selection
A total of 499 patients who underwent brain radiotherapy in our department between January 2012 and June 2021 were identified and retrospectively analysed. The treatment plans for all enrolled patients were comprehensively determined by physicians based on recommendations from National Comprehensive Cancer Network (NCCN) guidelines [23], the number and location of brain metastases, and the general condition of the patients. In this study, we applied consistent inclusion and exclusion criteria for patient selection. The patient inclusion criteria were as follows: 1) primary solid tumour confirmed pathologically, with contrast-enhanced computed tomography (CT)- or magnetic resonance imaging (MRI)-verified BMs (no limitation on the number of BMs); 2) age ≥ 18 years; and 3) undergoing brain radiation. Prior surgery for BMs was allowed only if the patient experienced a postoperative relapse. The exclusion criteria were as follows: 1) undergoing either SRS or stereotactic radiation therapy (SRT); 2) undergoing prophylactic cranial irradiation (PCI); 3) undergoing two-dimensional radiation therapy; 4) previous intracranial radiation; and 5) inadequate follow-up imaging for at least 3 months. The following factors from each patient were analysed: age, sex, smoking status, drinking status, Karnofsky Performance Scale (KPS), pathological tumour type, number of BMs, extracranial disease status, extracranial metastases, presence or absence of meningeal or liver metastases, surgery before radiation, systemic treatment, radiotherapy dosages, dose fraction regimens, biologically effective dose (BED), radiotherapy technique, gross target volume (GTV), clinical target volume (CTV), planning gross target volume (PGTV), planning target volume (PTV), sum of the longest diameter of the BMs, treatment-related toxicities and date of initial treatment, BM diagnosis, first day of radiation treatment, intracranial progression, and death or final follow-up visit. Furthermore, a prognostic index, the Graded Prognostic Assessment (GPA), was calculated for each patient, which was the sum of scores (0, 0.5, and 1.0) for four factors: age, KPS, extracranial metastases, and number of BMs [24].
Radiotherapy strategy
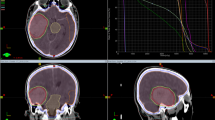
To ensure reproducibility, all patients were placed in a supine position, in a custom-made thermoplastic mask, and underwent a simulation CT scan of the entire head, using a 3- or 5-mm slice thickness. The CT scans were then merged with available contrast-enhanced T1-weighted MRI sequences. The target delineation criteria for both groups were the same: GTV was defined as brain metastases; CTV was defined as the whole brain tissue; PGTV was defined as GTV plus 5-mm margins; and PTV was defined as CTV plus 5-mm margins. The OARs were also delineated, primarily including the brainstem, eyes, lenses, optic chiasma, and optic nerves. Radiotherapy was delivered using intensity-modulated radiation therapy (IMRT), volumetric-modulated arc therapy (VMAT), or three-dimensional conformal radiotherapy (3D-CRT). For patients who underwent WBRT + SIB, the prescribed dose to the PTV was 25–37.5 Gy in 10–20 fractions, and the simultaneous boost to the PGTV was 35–52.5 Gy in 10–20 fractions (5 fractions per week). The dose for WBRT alone was 30 Gy in 10 fractions to the PTV (5 fractions per week) without further dose escalation.
Follow-up
Follow-up examinations included brain MRI or CT, physical examinations, and toxicity evaluations conducted at least every 3 months for the first 2 years, and every 6 months thereafter, according to clinical protocol. Responses to treatment were assessed by experienced radiologists using the Response Assessment in Neuro-Oncology Brain Metastases (RANO-BM) criteria [25]. Toxicity was scored using the Common Toxicity Criteria Adverse Events version 5.0 (CTCAE v.5.0).
Study endpoints
The primary endpoints of the present study were intracranial progression-free survival (PFS) and local tumour control (LTC). Intracranial PFS was defined as the time from the first day of radiation exposure to intracranial progression (including both the progression of irradiated BMs and the appearance of new lesions), death from any cause, or the final follow-up visit. Intracranial LTC was evaluated from the first day of radiation exposure to intracranial local tumour progression (only including progression of irradiated BMs), death, or the final follow-up visit. Progression was defined as a relative increase of the sum of the longest diameters of the BMs of ≥20% from the baseline, according to the RANO-BM criteria. Treatment-related modifications, such as radiation necrosis, were not regarded as local failures.
The secondary endpoints of the present study were OS and radiation-related toxicity. OS was defined as the time from the first day of radiation exposure to death or final follow-up. Radiation-induced brain injury was diagnosed by experienced radiologists using MRI and magnetic resonance spectroscopy (MRS). The survival and toxicity data were obtained from hospital records or direct correspondence with the referring physician or relatives of patients.
Statistical analysis
Descriptive characteristics were analysed using the chi-squared and Fisher’s exact tests, and continuous variables were evaluated using the t-test and Mann-Whitney U test. A propensity score matching (PSM) analysis was conducted with logistic regression considering the following: sex, GPA scores, primary tumour type, and number of BMs. We employed the Kaplan-Meier method, log-rank test, and landmark survival analyses to compare intracranial PFS, LTC, and OS among different groups. Specifically, Competing Risk analyses, accounting for deaths unrelated to intracranial tumour progression as competing risks, were particularly utilized to assess intracranial PFS and LTC across the groups. Univariate and multivariate analyses were performed using the Cox regression models. Additionally, the factors with P < 0.2 in univariate analysis were included in the multivariate analysis. A receiver operating characteristic (ROC) curve was used to assess toxicity. PSM analysis and stratified analysis were utilized to control and adjust for potential allocation bias, enhancing the internal validity of this study. SPSS (version 26.0), R (version 4.1.2), RStudio, and GraphPad Prism (version 9.3.0) were used for the analyses. All P-values were two-sided, with P < 0.05. considered statistically significant.
Results
Patients
A total of 165 patients were included for analysis in the present study: 82 in the WBRT + SIB group, and 83 in the WBRT group. The baseline characteristics of the two groups are shown in Table 1. Notably, the WBRT group had a higher proportion of breast cancer patients (16.9% vs. 1.2%), leading to imbalances in sex and primary tumour type (P = 0.004 and P < 0.001, respectively). Furthermore, the WBRT + SIB group exhibited higher GPA scores compared to the WBRT group (69.6% with GPA ≥ 2 vs. 51.8%; P = 0.017). All other characteristics were well-balanced between the two groups. Subsequently, after conducting a PSM analysis, the patient characteristics were re-evaluated and presented in Table 1, demonstrating that all characteristics were well-balanced. Details concerning radiotherapy-related characteristics can be found in Supplementary Table 1.
Intracranial PFS, LTC, and OS
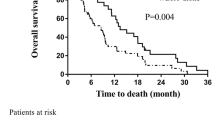
For all patients, the cumulative incidence of local intracranial progression was significantly lower in the WBRT + SIB group, leading to a significantly longer intracranial local tumour control (LTC) period (P = 0.023; Fig. 1A). Similarly, WBRT + SIB also slightly prolonged patients’ intracranial progression-free survival (PFS), although not reaching statistical significance (P = 0.076; Fig. 1B). However, there were no significant benefits in overall survival (OS) for the WBRT + SIB group compared to WBRT alone (P = 0.180; Fig. 1C). Of note, the survival outcomes after PSM analysis were consistent with the aforementioned results, showing that the WBRT + SIB group achieved significantly longer intracranial LTC and PFS (P = 0.006 and 0.042, respectively; Figs. 1D, E), but still no improvement in overall survival (P = 0.662; Fig. 1F).
Comparison of intracranial local tumour control (LTC) (A), intracranial progression-free survival (PFS) (B), and overall survival (OS) (C) between whole brain radiation therapy with a simultaneous integrated boost (WBRT + SIB) and whole brain radiation therapy (WBRT) in all patients using competing risk analyses. Comparison of intracranial LTC (D), intracranial PFS (E), and OS (F) between WBRT + SIB and WBRT after propensity score matching (PSM) using competing risk analyses. Comparison of intracranial LTC (G), intracranial PFS (H), and OS (I) between WBRT + SIB and WBRT in the lung cancer subgroup using competing risk analyses
Then we conducted additional survival analyses in the lung cancer subgroup, which included 68 patients receiving WBRT and 76 patients receiving WBRT + SIB. The results indicated that the WBRT + SIB group had a dramatically improved intracranial LTC and PFS compared with the WBRT group (P = 0.002 and 0.009, respectively; Figs. 1G, H). There was no significant difference, however, in terms of OS (P = 0.323; Fig. 1I).
Besides, the intracranial LTC and PFS curves presented in Fig. 1A, B, D, E, G, and H were further analysed using the Kaplan-Meier method, as demonstrated in Supplementary Fig. 1. The outcomes remained consistent with the earlier results.
Predictive factors of intracranial PFS, LTC, and OS
As shown in Supplementary Table 2, univariate analysis revealed that treatment method, extracranial disease control, and GPA score had substantial impacts on intracranial PFS in the lung cancer subgroup (P = 0.021, 0.172, and 0.029, respectively). Furthermore, multivariate analysis indicted that treatment with WBRT+SIB was an independent influencing factor strongly associated with increased intracranial PFS compared to WBRT alone (P = 0.026).
Similarly, we further examined the factors that influenced LTC and OS in the lung cancer subgroup, and found that treatment methods and GPA scores were the major contributing factors to intracranial LTC (P = 0.044 and 0.054, respectively; Supplementary Table 3). Multivariate analysis of OS revealed that pathological type non-small cell lung cancer (NSCLC), well-controlled extracranial disease, and higher GPA were associated with increased OS (P = 0.004, 0.004, and 0.02, respectively; Supplementary Table 4).
Stratified analysis
To minimise the impact of other predictive factors and the difference in baseline GPA scores, stratified analyses was performed by dividing lung cancer patients with BMs into groups based on GPA scores, extracranial disease control, and pathological tumour type. The relevant information regarding the subgroups is presented in Supplementary Table 5.
The results of the stratified analysis indicated that WBRT + SIB dramatically increased intracranial PFS and LTC in patients with a GPA ≥ 2 or stable extracranial disease, when compared to WBRT alone (P = 0.055, 0.008, 0.005, and 0.002, respectively; Figs. 2A, B, C, D), whereas patients with a GPA < 2 or active extracranial disease saw no benefit from WBRT + SIB vs. WBRT alone (P = 0.184, 0.323, 0.533, and 0.353, respectively; Figs. 2E, F, G, H). All the results of the stratified analysis were reconfirmed through the Kaplan-Meier method, as illustrated in Supplementary Fig. 2.
Comparison of intracranial progression-free survival (PFS) (A) and local tumour control (LTC) (B) for WBRT and WBRT + SIB in lung cancer patients with a graded prognostic assessment (GPA) score ≥ 2 using competing risk analyses. Comparison of intracranial PFS (C) and LTC (D) for WBRT and WBRT + SIB in lung cancer patients with stable extracranial disease (ED) using competing risk analyses. Comparison of intracranial PFS (E) and LTC (F) for WBRT and WBRT + SIB in lung cancer patients with a GPA < 2 using competing risk analyses. Comparison of intracranial PFS (G) and LTC (H) for WBRT and WBRT + SIB in lung cancer patients with active ED using competing risk analyses
Additionally, NSCLC patients who underwent treatment with WBRT + SIB exhibited notable improvements in both intracranial PFS and LTC (P = 0.019 and 0.015, respectively; Figs. 3A, B). For small cell lung cancer (SCLC) patients, however, we found no remarkable differences in intracranial PFS or LTC between the two groups (P = 0.264 and 0.096, respectively; Figs. 3C, D). Consistent results were obtained through the Kaplan-Meier method, as depicted in Supplementary Fig. 3. Then we further conducted landmark survival analysis, we did find that treatment with WBRT + SIB significantly improved the long-term intracranial PFS and LTC (> 5 months) of SCLC patients (P = 0.025 and 0.024, respectively; Figs. 3E, F), although no such improvement was seen in short-term survival (P = 0.146 and 0.119, respectively; Fig. 3E, F).
Comparison of intracranial progression-free survival (PFS) (A) and local tumour control (LTC) (B) for WBRT and WBRT + SIB in non-small cell lung cancer patients (NSCLC) using competing risk analyses. Comparison of intracranial PFS (C) and LTC (D) for WBRT and WBRT + SIB in small cell lung cancer (SCLC) patients using competing risk analyses. Landmark analysis of intracranial PFS (E) and LTC (F) in SCLC patients receiving WBRT + SIB and WBRT (cutoff time = 5 months)
Toxicity
As shown in Table 2, the majority of the patients included in the present study experienced radiotherapy-related toxicities, which primarily involved nausea, vomiting, dizziness, headache, radiation-induced brain injury, or other central nervous system (CNS) symptoms. The incidence of grade 3 or worse adverse events in the WBRT + SIB and WBRT groups was 0 vs. 2.4% (P = 0.497) for headache, 1.2 vs. 1.2% (P > 0.999) for dizziness, 1.2 vs. 0% (P = 0.497) for radiation-induced brain injury, and 0 vs. 2.4% (P = 0.497) for leukopenia, respectively.
Additionally, when evaluating the incidence of radiation-induced brain injury, there were 8 cases (9.8%), including 1 case of grade 3 radiation-induced brain injury, in the WBRT + SIB group, whereas the WBRT group reported only 2 cases (2.4%), neither of which were grade 3. The incidence of radiation-induced brain injury was higher in the WBRT + SIB group for all grades (grades 1 to 3, P = 0.992, 0.207, and 0.497, respectively; Fig. 4A), and the same was seen for overall risk (P = 0.099; Fig. 4A). We further explored the association between the risk of radiation-induced brain injury and the booster dosage administered in the WBRT + SIB group, and found that the risk rose with an increased dosage (area under the curve [AUC] = 0.755; Fig. 4B). Moreover, to determine the optimal dose for WBRT + SIB therapy, we separated the patients into two subgroups: low-dose (BED ≤56 Gy) and high-dose (BED > 56 Gy), and found that low-dose WBRT + SIB had a lower incidence of radiation-induced brain injury than high-dose WBRT + SIB (P = 0.020). Additionally, no significant difference was found when compared with WBRT alone (P > 0.999).
Discussion
In the present study, we found that when utilised as the first-line treatment for BMs, WBRT + SIB resulted in better intracranial tumour control than WBRT alone. Furthermore, low-dose WBRT + SIB (BED ≤56 Gy) was preferred to high-dose WBRT + SIB because of the association between the boost dosage and the incidence of radiation-induced brain injury.
Although WBRT is still considered the standard treatment option for BMs, the median intracranial PFS after such treatment among patients with multiple BMs is only approximately 5–7 months [18, 26]. In the present study, we discovered that WBRT + SIB could prolong the intracranial LTC of existing metastases, which was also reflected in the slightly improved intracranial PFS. And after PSM analysis, the survival outcomes were consistent with these results, showing that the WBRT + SIB group achieved significantly longer intracranial LTC and PFS without baseline differences between the two groups. Moreover, to minimise the impact of baseline differences in sex and primary tumour type, further analysis was performed in the lung cancer subgroup, in which we found that lung cancer patients treated with WBRT + SIB demonstrated greater improvements in intracranial PFS and LTC. Univariate and multivariate analyses also indicated that the treatment method (WBRT vs. WBRT + SIB) was an independent prognostic factor for patients’ intracranial PFS and LTC.
The results of the present study were consistent with those of Popp et al. [18], who evaluated 124 patients with at least 4 BMs from various primary tumour types (excluding SCLC) treated with an average of 35 Gy WBRT or 30 Gy WBRT with 42 or 51 Gy SIB in 12 fractions. They found that WBRT + SIB was associated with improved intracranial PFS and OS than WBRT. The results of the present study, however, did not indicate any improvement in survival benefits in the WBRT + SIB group, even after PSM analysis, which might be attributed to the following factors: 1) more patients experienced meningeal metastasis in the WBRT + SIB group than the WBRT group (5.8 vs. 0%); 2) there was a lower proportion of targeted therapy in the WBRT + SIB group than the WBRT group (25.0 vs. 28.8%); and 3) there was a lower incidence of salvage therapy (brain radiation or surgery, 9.6 vs. 19.2%) in the WBRT + SIB group compared to the WBRT group. In fact, the benefit of WBRT + SIB treatment on survival remains controversial. In line with our results, several studies have shown that the dose escalation strategy did not improve patient survival compared with WBRT alone [15, 27, 28].
On the other hand, the existence of brain metastases had a profound impact on both the quality of life (QOL) and neurological status of patients [29]. Research suggested that employing WBRT-alone for brain metastases offers limited benefits in terms of both QOL and neurological status [30,31,32,33,34]. Conversely, dose escalation strategies like SRS demonstrated clear advantages [12]. Notably, our study highlighted that WBRT+SIB treatment significantly enhances intracranial local tumour control, effectively delaying brain tumour progression and recurrence in patients with brain metastases. This implies that, despite the absence of an OS advantage compared to WBRT-alone treatment, WBRT+SIB treatment may still hold potential benefits in terms of enhancing QOL and neurological status. However, owing to the retrospective nature of this study, we have been unable to access relevant information for analysis. Further research is imperative to substantiate these aspects.
Univariate analysis in the present study revealed that both GPA and extracranial disease contributed to the control of intracranial tumours. In previous studies, they were recognised as independent influencing factors for intracranial PFS, which is consistent with the findings of the present study [15, 27]. Additionally, due to the retrospective nature of this study, a certain degree of allocation bias may exist, mainly arising from decisions made by physicians or patients. Consequently, the WBRT + SIB group in this study exhibited higher baseline GPA scores than the WBRT group. To minimize the impact of these factors, except for the previous PSM analysis, we also conducted a stratified analysis within the lung cancer subgroup. The results presented patients with a GPA ≥ 2 and stable extracranial disease had substantially improved intracranial PFS and LTC following WBRT + SIB treatment compared to WBRT alone, while patients with a GPA < 2 and active extracranial disease exhibited no therapeutic benefit. This implies that, despite differences in baseline characteristics, WBRT + SIB treatment provided a clear advantage in terms of intracranial tumour local control, especially in the population with high GPA scores and stable extracranial disease. For patients with a GPA < 2 and active extracranial disease, the stratified analysis did not reveal a clear therapeutic benefit. We hypothesize that this could be attributed to the fact that patients with poor prognostic factors, such as low KPS, multiple BMs, or extracranial metastases are more likely to have shorter survival times [24, 35], and the advantage of WBRT + SIB over WBRT in terms of intracranial tumour local control is not obvious in that limited time. These findings further support the use of WBRT + SIB in patients with improved baseline conditions.
On the other hand, we first reported SCLC patients with BMs who underwent WBRT + SIB had improved intracranial PFS and LTC at long-term survival (> 5 months). Available research on WBRT + SIB in SCLC patients is limited, with only one small retrospective study demonstrating that WBRT + SIB prolonged OS compared to WBRT alone [22]. Although SCLC patients have a high risk of BMs, which are rarely isolated and characterised by early intracranial dissemination [22, 36], the findings of the present study suggest the use of WBRT + SIB treatment in SCLC patients for better long-term intracranial tumour control. Additionally, added benefits of LTC were also seen in NSCLC patients following WBRT + SIB treatment, consistent with earlier studies [27].
In terms of adverse events, there was no significant difference in the occurrence of grade 3 or higher toxicities between the two groups; however, we discovered that radiation-induced brain injury occurred more frequently in the WBRT + SIB group (overall, 9.8 vs. 2.4%). Furthermore, we noticed that the incidence of radiation-induced brain injury increased as the BED administered increased. One study reported a radiation necrosis incidence of approximately 3.2% following WBRT + SIB treatment [18], which was slightly lower than what we observed in the present study. It may be attributed to the different definitions between radiation necrosis and radiation-induced brain injury, as well as the utilization of distinct diagnostic methods in the study. The confirmation of radiation necrosis relied on pathological examination, whereas we diagnosed radiation-induced brain injury using MRI and MRS. [37,38,39]. Therefore, the findings of the present study indicate that treatment with WBRT + SIB, particularly high-dose, may increase the risk of radiation-induced brain injury. And this risk was found to be significantly lower following low-dose (BED ≤56 Gy) WBRT + SIB than high-dose WBRT + SIB, and was equivalent to that of WBRT alone. Moreover, using both competing risk analyses and the Kaplan-Meier approach, we found no difference in intracranial tumour control between the low- and high-dose WBRT + SIB groups. (P = 0.654, 0.471, 0.532, and 0.365, respectively; Supplementary Figs. 4A, B, C, D). Therefore, the results of the present study confirmed that low-dose WBRT + SIB treatment could allow for better intracranial tumour control while simultaneously minimising the risk of radiation-induced brain injury. Based on our findings, we recommend 30 Gy in 10 fractions for PTV, and 40 Gy in 10 fractions for PGTV.
The present study had several limitations. Firstly, due to the retrospective nature of this study, researchers were unable to randomly control the allocation process of participants, leading to potential allocation bias, such as the imbalance in baseline GPA scores between the two treatment groups. Despite significant efforts to mitigate this bias through methods like PSM analysis and stratified analyses, the study results may still be influenced. Second, there was no evaluation of the patients’ quality of life and neurological status, due to the absence of corresponding data. Third, because this was a small retrospective study with inherent biases, the findings should be verified in future prospective studies.
Conclusions
In conclusion, treatment with WBRT + SIB may improve intracranial tumour control in patients with BMs compared to WBRT alone, particularly in the lung cancer subgroup. Patients with higher GPA scores and well-controlled extracranial disease undergoing WBRT + SIB had improved intracranial PFS and LTC than those undergoing WBRT alone. Moreover, the use of WBRT + SIB also led to better long-term intracranial control in SCLC patients. The results of the present study demonstrated that treatment with WBRT + SIB might increase the risk of radiation-induced brain injury, with that risk being proportional to the boost dosage. Low-dose WBRT + SIB (BED ≤56 Gy) showed good tumour control and an acceptable risk of radiation-induced brain injury; therefore, low-dose WBRT + SIB should be considered for patients with BMs, although further prospective studies are needed to validate our findings.
Availability of data and materials
The datasets used and/or analysed during the current study are available from the corresponding author on reasonable request.
Abbreviations
- BMs:
-
brain metastases
- WBRT + SIB:
-
whole brain radiation therapy with a simultaneous integrated boost
- WBRT:
-
whole brain radiation therapy
- PFS:
-
progression-free survival
- LTC:
-
local tumour control
- OS:
-
overall survival
- BED:
-
biologically effective dose
- SRS:
-
stereotactic radiosurgery
- WBRT + SEB:
-
whole brain radiation therapy with sequential integrated boost
- OARs:
-
organs at risk
- SCLC:
-
small cell lung cancer
- NCCN:
-
National Comprehensive Cancer Network
- CT:
-
computed tomography
- MRI:
-
magnetic resonance imaging
- SRT:
-
stereotactic radiation therapy
- PCI:
-
prophylactic cranial irradiation
- KPS:
-
karnofsky performance scale
- GTV:
-
gross target volume
- CTV:
-
clinical target volume
- PGTV:
-
planning gross target volume
- PTV:
-
planning target volume
- GPA:
-
graded prognostic assessment
- IMRT:
-
intensity-modulated radiation therapy
- VMAT:
-
volumetric-modulated arc therapy
- 3D-CRT:
-
three-dimensional conformal radiotherapy
- RANO-BM:
-
neuro-oncology brain metastases
- CTCAE v.5.0:
-
common toxicity criteria adverse events version 5.0
- MRS:
-
magnetic resonance spectroscopy
- PSM:
-
propensity score matching
- ROC:
-
receiver operating characteristic
- NSCLC:
-
non-small cell lung cancer
- CNS:
-
central nervous system
- QOL:
-
quality of life.
References
Nayak L, Lee EQ, Wen PY. Epidemiology of brain metastases. Curr Oncol Rep. 2012;14(1):48–54.
Valiente M, Ahluwalia MS, Boire A, et al. The evolving landscape of brain metastasis. Trends Cancer. 2018;4(3):176–96.
Frisk G, Svensson T, Backlund LM, et al. Incidence and time trends of brain metastases admissions among breast cancer patients in Sweden. Br J Cancer. 2012;106(11):1850–3.
Goncalves PH, Peterson SL, Vigneau FD, et al. Risk of brain metastases in patients with nonmetastatic lung cancer: analysis of the metropolitan Detroit surveillance, epidemiology, and end results (SEER) data. Cancer. 2016;122(12):1921–7.
Weissman DE. Glucocorticoid treatment for brain metastases and epidural spinal cord compression: a review. J Clin Oncol. 1988;6(3):543–51.
Gu L, Qing S, Zhu X, et al. Stereotactic radiation therapy (SRT) for brain metastases of multiple primary tumors: a single institution retrospective analysis. Front Oncol. 2019;9:1352.
Suh JH, Kotecha R, Chao ST, et al. Current approaches to the management of brain metastases. Nat Rev Clin Oncol. 2020;17(5):279–99.
Kocher M, Soffietti R, Abacioglu U, et al. Adjuvant whole-brain radiotherapy versus observation after radiosurgery or surgical resection of one to three cerebral metastases: results of the EORTC 22952-26001 study. J Clin Oncol. 2011;29(2):134–41.
Nieder C, Spanne O, Mehta MP, et al. Presentation, patterns of care, and survival in patients with brain metastases: what has changed in the last 20 years? Cancer. 2011;117(11):2505–12.
Vogelbaum MA, Brown PD, Messersmith H, et al. Treatment for brain metastases: ASCO-SNO-ASTRO guideline. J Clin Oncol. 2022;40(5):492–516.
Tsao MN, Xu W, Wong RK, et al. Whole brain radiotherapy for the treatment of newly diagnosed multiple brain metastases. Cochrane Database Syst Rev. 2018;1(1):CD003869.
Brown PD, Jaeckle K, Ballman KV, et al. Effect of radiosurgery alone vs radiosurgery with whole brain radiation therapy on cognitive function in patients with 1 to 3 brain metastases: a randomized clinical trial. JAMA. 2016;316(4):401–9.
Borghetti P, Pedretti S, Spiazzi L, et al. Whole brain radiotherapy with adjuvant or concomitant boost in brain metastasis: dosimetric comparison between helical and volumetric IMRT technique. Radiat Oncol. 2016;11:59.
Qing D, Zhao B, Zhou YC, et al. Whole-brain radiotherapy plus sequential or simultaneous integrated boost for the treatment of a limited number of brain metastases in non-small cell lung cancer: a single-institution study. Cancer Med. 2020;9(1):238–46.
Lin B, Huang D, Du H, et al. Whole-brain radiation therapy with simultaneous integrated boost versus whole-brain radiation therapy plus stereotactic radiosurgery for the treatment of brain metastasis from lung Cancer. Front Oncol. 2021;11:631422.
Zhou L, Liu J, Xue J, et al. Whole brain radiotherapy plus simultaneous in-field boost with image guided intensity-modulated radiotherapy for brain metastases of non-small cell lung cancer. Radiat Oncol. 2014;9:117.
Aoyama H, Shirato H, Tago M, et al. Stereotactic radiosurgery plus whole-brain radiation therapy vs stereotactic radiosurgery alone for treatment of brain metastases: a randomized controlled trial. JAMA. 2006;295(21):2483–91.
Popp I, Rau S, Hintz M, et al. Hippocampus-avoidance whole-brain radiation therapy with a simultaneous integrated boost for multiple brain metastases. Cancer. 2020;126(11):2694–703.
Du TQ, Li X, Zhong WS, et al. Brain metastases of lung cancer: comparison of survival outcomes among whole brain radiotherapy, whole brain radiotherapy with consecutive boost, and simultaneous integrated boost. J Cancer Res Clin Oncol. 2021;147(2):569–77.
Linskey ME, Andrews DW, Asher AL, et al. The role of stereotactic radiosurgery in the management of patients with newly diagnosed brain metastases: a systematic review and evidence-based clinical practice guideline. J Neuro-Oncol. 2010;96(1):45–68.
Dobi A, Fodor E, Maraz A, et al. Boost irradiation integrated to whole brain radiotherapy in the Management of Brain Metastases. Pathol Oncol Res. 2020;26(1):149–57.
Sun H, Xu L, Wang Y, et al. Additional radiation boost to whole brain radiation therapy may improve the survival of patients with brain metastases in small cell lung cancer. Radiat Oncol. 2018;13(1):250.
Nabors LB, Portnow J, Ahluwalia M, et al. Central nervous system cancers, version 3.2020, NCCN clinical practice guidelines in oncology. J Natl Compr Cancer Netw. 2020;18(11):1537–70.
Sperduto PW, Berkey B, Gaspar LE, et al. A new prognostic index and comparison to three other indices for patients with brain metastases: an analysis of 1,960 patients in the RTOG database. Int J Radiat Oncol Biol Phys. 2008;70(2):510–4.
Lin NU, Lee EQ, Aoyama H, et al. Response assessment criteria for brain metastases: proposal from the RANO group. Lancet Oncol. 2015;16(6):e270–8.
Brown PD, Gondi V, Pugh S, et al. Hippocampal avoidance during whole-brain radiotherapy plus Memantine for patients with brain metastases: phase III trial NRG oncology CC001. J Clin Oncol. 2020;38(10):1019–29.
Lu F, Hou Y, Xia Y, et al. Survival and intracranial control outcomes of whole-brain radiotherapy (WBRT) alone versus WBRT plus a radiotherapy boost in non-small-cell lung cancer with brain metastases: a single-institution retrospective analysis. Cancer Manag Res. 2019;11:4255–72.
Andrews DW, Scott CB, Sperduto PW, et al. Whole brain radiation therapy with or without stereotactic radiosurgery boost for patients with one to three brain metastases: phase III results of the RTOG 9508 randomised trial. Lancet. 2004;363(9422):1665–72.
Achrol AS, Rennert RC, Anders C, et al. Brain metastases. Nat Rev Dis Primers. 2019;5(1):5.
Mulvenna P, Nankivell M, Barton R, et al. Dexamethasone and supportive care with or without whole brain radiotherapy in treating patients with non-small cell lung cancer with brain metastases unsuitable for resection or stereotactic radiotherapy (QUARTZ): results from a phase 3, non-inferiority, randomised trial. Lancet. 2016;388(10055):2004–14.
Steinmann D, Paelecke-Habermann Y, Geinitz H, et al. Prospective evaluation of quality of life effects in patients undergoing palliative radiotherapy for brain metastases. BMC Cancer. 2012;12:283.
Caissie A, Nguyen J, Chen E, et al. Quality of life in patients with brain metastases using the EORTC QLQ-BN20+2 and QLQ-C15-PAL. Int J Radiat Oncol Biol Phys. 2012;83(4):1238–45.
Pulenzas N, Khan L, Tsao M, et al. Fatigue scores in patients with brain metastases receiving whole brain radiotherapy. Support Care Cancer. 2014;22(7):1757–63.
Li B, Yu J, Suntharalingam M, et al. Comparison of three treatment options for single brain metastasis from lung cancer. Int J Cancer. 2000;90(1):37–45.
Sperduto PW, Kased N, Roberge D, et al. Summary report on the graded prognostic assessment: an accurate and facile diagnosis-specific tool to estimate survival for patients with brain metastases. J Clin Oncol. 2012;30(4):419–25.
Gong L, Wang QI, Zhao L, et al. Factors affecting the risk of brain metastasis in small cell lung cancer with surgery: is prophylactic cranial irradiation necessary for stage I-III disease? Int J Radiat Oncol Biol Phys. 2013;85(1):196–200.
Ali FS, Arevalo O, Zorofchian S, et al. Cerebral radiation necrosis: incidence, pathogenesis, diagnostic challenges, and future opportunities. Curr Oncol Rep. 2019;21(8):66.
Hollingworth W, Medina LS, Lenkinski RE, et al. A systematic literature review of magnetic resonance spectroscopy for the characterization of brain tumors. AJNR Am J Neuroradiol. 2006;27(7):1404–11.
Chao ST, Ahluwalia MS, Barnett GH, et al. Challenges with the diagnosis and treatment of cerebral radiation necrosis. Int J Radiat Oncol Biol Phys. 2013;87(3):449–57.
Acknowledgements
We thank for the supports of Prof. Zhiyong Yuan and Prof. Lujun Zhao.
Funding
This study was funded by National Natural Science Foundation of China (No. 81602565 and 82073348), National Outstanding Youth Science Fund Project of National Natural Science Foundation of China (No. 82102835) and Tianjin Key Medical Discipline (Specialty) Construction Project (TJYXZDXK-009A).
Author information
Authors and Affiliations
Contributions
KZ, and TZ designed this study and wrote the main manuscript. KZ, TZ, ZG, FZ, JL, YL, YL and XW performed development of methodology, review and revision of the paper. KZ, TZ, ZG, FZ, JL, YL, YL, XW, XC, WZ and XC collected and analyzed the clinical data. WZ, QP and PW provided statistical and material support. QP and PW performed funding acquisition and project administration. All authors read and approved the final manuscript.
Corresponding authors
Ethics declarations
Ethics approval and consent to participate
The study was approved by the ethics committee of Tianjin Medical University Cancer Institute and Hospital (BC2023045). Since it is a retrospective study that presents no risks to the participants’ health or economic well-being, the ethics committee of Tianjin Medical University Cancer Institute and Hospital granted an exemption from obtaining informed consent.
All the methods performed in this study were in accordance with the guidelines stated in the ‘Ethics Approval and Consent to Participate’ statement provided above.
Consent for publication
Not applicable.
Competing interests
The authors declare no competing interests.
Additional information
Publisher’s Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Additional file 1.
Supplementary Table 1 - 5.
Additional file 2.
Supplementary Fig. 1 Comparison of intracranial local tumour control (LTC) (A) and progression-free survival (PFS) (B) between whole brain radiation therapy with a simultaneous integrated boost (WBRT + SIB) and whole brain radiation therapy (WBRT) in all patients using Kaplan-Meier method. Comparison of intracranial LTC (C) and PFS (D) between WBRT + SIB and WBRT after propensity score matching (PSM) using Kaplan-Meier method. Comparison of intracranial LTC (E) and PFS (F) between WBRT + SIB and WBRT in the lung cancer subgroup using Kaplan-Meier method.
Additional file 3.
Supplementary Fig. 2 Comparison of intracranial progression-free survival (PFS) (A) and local tumour control (LTC) (B) for WBRT and WBRT + SIB in lung cancer patients with a graded prognostic assessment (GPA) score ≥ 2 using Kaplan-Meier method. Comparison of intracranial PFS (C) and LTC (D) for WBRT and WBRT + SIB in lung cancer patients with stable extracranial disease (ED) using Kaplan-Meier method. Comparison of intracranial PFS (E) and LTC (F) for WBRT and WBRT + SIB in lung cancer patients with a GPA < 2 using Kaplan-Meier method. Comparison of intracranial PFS (G) and LTC (H) for WBRT and WBRT + SIB in lung cancer patients with active ED using Kaplan-Meier method.
Additional file 4.
Supplementary Fig. 3 Comparison of intracranial progression-free survival (PFS) (A) and local tumour control (LTC) (B) for WBRT and WBRT + SIB in non-small cell lung cancer patients (NSCLC) using Kaplan-Meier method. Comparison of intracranial PFS (C) and LTC (D) for WBRT and WBRT + SIB in small cell lung cancer (SCLC) patients using Kaplan-Meier method.
Additional file 5.
Supplementary Fig. 4 Comparison of intracranial progression-free survival (PFS) (A) and local tumour control (LTC) (B) for low-dose and high-dose WBRT + SIB group using competing risk analyses. Comparison of intracranial PFS (C) and LTC (D) for low-dose and high-dose WBRT + SIB group using Kaplan-Meier method.
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if changes were made. The images or other third party material in this article are included in the article's Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article's Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by/4.0/. The Creative Commons Public Domain Dedication waiver (http://creativecommons.org/publicdomain/zero/1.0/) applies to the data made available in this article, unless otherwise stated in a credit line to the data.
About this article
Cite this article
Zhang, K., Zhang, T., Guo, Z. et al. Adding simultaneous integrated boost to whole brain radiation therapy improved intracranial tumour control and minimize radiation-induced brain injury risk for the treatment of brain metastases. BMC Cancer 23, 1240 (2023). https://doi.org/10.1186/s12885-023-11739-9
Received:
Accepted:
Published:
DOI: https://doi.org/10.1186/s12885-023-11739-9