Abstract
Background
A recent survey revealed that extensive off-label use of sugammadex in pediatric anesthesia deserved particular attention. The present study with trial sequential analysis (TSA) aimed to evaluate the effects of sugammadex for antagonizing neuromuscular blockade (NMB) in pediatric patients, and to investigate whether the findings achieved the required information size to draw conclusions.
Methods
PubMed, Embase, Cochrane Library and China National Knowledge Infrastructure (CNKI) were searched from inception to April 2021. All randomized controlled trials used sugammadex as reversal agent in pediatric patients were enrolled. Time from NMB reversal to recovery of the train-of-four ratio (TOFr) to 0.9 and extubation time were considered as co-primary outcomes, and incidences of adverse events were considered as secondary outcomes. Grading of Recommendations Assessment, Development, and Evaluation (GRADE) system was used to rate the quality of evidences.
Results
Data from 18 studies involving 1,065 pediatric patients were acquired. The results revealed that use of sugammadex was associated with shorter duration from administration of reversal agents to TOFr > 0.9 (MD = -14.42, with 95% CI [-17.08, -11.75]) and shorter interval from reversal from NMB to extubation (MD = -13.98, with 95% CI [-16.70, -11.26]) compared to control groups. TSA also indicated that the current sample sizes were sufficient with unnecessary further trials. Analysis of secondary outcomes indicated that administration of sugammadex was associated with less incidence of postoperative nausea and vomiting (PONV), bradycardia, and dry mouth compared to control groups.
Conclusion
Considering of satisfactory and rapid neuromuscular blockade reversal with low incidences of adverse events, sugammadex might be considered as the preferred option for children in clinical anesthesia practice compared to acetylcholinesterase inhibitors. However, overall low-quality evidences in present study rated by GRADE system indicated that superiority of sugammadex employed in pediatric patients needs to be confirmed by more studies with high quality and large sample size in future.
Similar content being viewed by others
Introduction
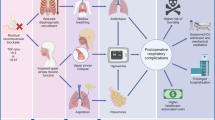
The wide use of neuromuscular blocking agents (NMBAs) has revolutionized clinical anesthetic practice. It produces rapid profound skeletal muscle relaxation, provides convenient tracheal intubation, and improves surgical operating conditions [1]. However, it exposes patients to the risks of residual neuromuscular blockade (NMB) including postoperative pulmonary diseases and respiratory complications (pulmonary atelectasis, decreased oxygen saturation, upper airway obstruction) [2, 3], and leads to reintubation and excess length of stay.
Before sugammadex arrived on the scene, neostigmine, one of acetylcholinesterase inhibitors, was routinely used to competitively reverse the blockade of non-depolarizing muscle relaxants (e.g. rocuronium). However, application of neostigmine gives rise to various negative effects including bradycardia, hypersalivation, and bronchoconstriction. Therefore, to antagonize muscarinic side-effects, anticholinergics (e.g. atropine, glycopyrrolate) are recommended to be administered in a mixture with neostigmine. In addition, due to an absence of ability to reverse the blockade from rocuronium immediately, use of neostigmine may increase risks of post-operative residual neuromuscular block [4,5,6].
As the first non-competitive antagonist for the reversal of NMB, sugammadex, a modified γ-cyclodextrin, features its unique mechanism different from the mechanism of acetylcholinesterase inhibitors. It rapidly encapsulates rocuronium or vecuronium by one-to-one molecular binding, provides fast and predictable reversal effects of NMB, and decreases the incidence of residual block efficiently [7,8,9]. Since the first-in-man clinical research in 2005 [10], sugammadex has been used extensively in surgical practice for adult patients in recent years [11]. Simultaneously, although the drug package insert evidently declares that “the safety and efficacy of sugammadex in pediatric patients have not been established” [12], according to recent studies [13, 14] and a latest survey [15], this novel agent has been frequently used in pediatric anesthesia, especially among anesthesiologists with fewer years of practice.
In an effort to evaluate the effects of sugammadex on pediatric patients, Won et al. [16] and Liu et al. [17] conducted the relevant meta-analyses, and both of two studies demonstrated its effective and rapid profiles in reversing NMB. However, authors described that included studies still lacking sufficient information. It also requires more evidences to draw the reliable conclusions.
Therefore, on the basis of combining the latest evidences in various regions, we conducted the present updated meta-analysis by reviewing RCTs (randomized controlled trials) to compare the efficacy and safety between sugammadex and acetylcholinesterase inhibitors, so as to accumulate more information about the use of sugammadex for antagonizing rocuronium-induced NMB in pediatric patients. And the trial sequential analysis (TSA) was also performed to determine whether the findings achieved the required information size to draw the conclusions.
The present meta-analysis was performed in accordance with the recommendations in the Preferred Reporting Items for Systematic Reviews and Meta-Analyses (PRISMA) statement [18] and the guidelines described in the Cochrane Handbook.
Methods
Search strategy
Two independent authors (BL and QZ) searched PubMed, Embase, Cochrane Library, and CNKI (China National Knowledge Infrastructure) databases up to April 24, 2021. Moreover, we considered potentially useful studies in Google Scholar as additional sources of information. The search terms we used included infant, child, adolescent, sugammadex, org 25,969, bridion and randomized controlled trial (Appendix S1). Only human studies were involved, and there were no restrictions of language.
Eligibility criteria
The studies meeting the following conditions were selected for further analysis:
Participants
The patients were the pediatric patients (< 18 years old) who experienced different surgical and diagnostic procedures.
Intervention and comparison
Using sugammadex (regardless of administration doses) versus acetylcholinesterase inhibitors or placebo as reversal agent.
Outcome measures
Given that rapid recovery from NMB to a train-of-four (TOF) ratio of 0.9, short duration from reversal injection to extubation, and limited adverse effects were considered as the ideal characteristics of a reversal agent [19], the co-primary outcomes were as follows: (a) time from NMB reversal to recovery of the TOF ratio to 0.9, (b) extubation time. And incidences of adverse events were considered as secondary outcomes.
Study design
Randomized controlled trials with no language limitations.
Data extraction, and assessment of the risk of bias
Two authors (BL and QZ) conducted the data extraction and identified quality and eligibility of studies. After removing the duplicates from different databases, those obviously irrelevant records were excluded by titles and abstracts screening. The full texts of the remaining studies were obtained and perused. To collect the general characteristics of enrolled studies, a table was designed and filled by us (Table 1). The risk of bias in RCTs was evaluated by the Cochrane risk of bias tool [20], using the following domains: random sequence generation (generation of the randomization sequence), allocation concealment, blinding of outcome assessment, incomplete outcome data, and selective reporting. All articles could have the following domain classifications: high risk of bias, low risk of bias, uncertain risk (without information for judgment). Any disagreements were resolved by consensus through discussion.
Grading the quality of evidence
Assessment of quality of evidence and strength of recommendations was conducted by using the Grading of Recommendations Assessment, Development, and Evaluation (GRADE) methodology [39]. The quality of outcomes was independently assessed by two authors (BL and QZ). On the basis of risk of bias, inconsistency, indirectness, imprecision, and publication bias, the quality was classified as high, moderate, low, or very low. The GRADE profiler (version 3.6) software was used.
Statistical analysis
Statistical analyses were performed by using Review Manager software (Version 5.3.3, the Cochrane Collaboration 2014, the Nordic Cochrane Centre). Mean difference (MD) with 95% confidence interval (CI) were used to estimate continuous variables, and risk ratio (RR) with 95% confidence interval (CI) and the Mantel–Haenszel method (fixed or random models) were used to analyze dichotomous data. The I-squared (I2) test was chosen to weigh the impact of heterogeneity on the results. If significant heterogeneity (present at I2 > 50%) existed, the sensitivity analysis was performed by omitting each study individually, and the random effects model was chosen; otherwise, the fixed-effects model was chosen. Publication bias were evaluated by using Begg's test and Egger’s test if the number of included studies exceeds 10. Evaluation was performed using version 1.2.4 of the metabias program, Stata/MP 12.0 for Windows (StataCorp LP, 4905 Lakeway Drive, College Station, TX 77,845, USA). A P value < 0.05 was considered statistically significant.
Sparse data and the repeated significance testing with new studies updating may lead to type-1 errors (false-positive outcomes) and type-2 errors (false-negative outcomes) of meta-analyses. To eliminate the risks from type-1 and type-2 errors, Trial sequential analysis (TSA), which can adjust the statistical threshold by controlling P value and widening confidence intervals, was performed by us. TSA can estimate the required information size (RIS) and trial sequential monitoring boundaries. The cumulative Z curve entering the futility area or crossing the trial sequential monitoring boundary may indicate that the present evidences of intervention effects are at a sufficient level, and further trials will be unnecessary. Otherwise, evidences are insufficient to draw the conclusion if Z curve does not cross any boundaries or reach the RIS [40]. And the TSA was performed using Trial Sequential Analysis Viewer Software (version 0.9.5.10 beta; http://www.ctu.dk/tsa).
Results
Literature search results
After screening in databases and additional sources of information, a total of 187 relevant items were identified initially. 65 duplicate records were removed, and 96 records were excluded by titles and abstracts reviewing. In these 96 excluded items, 49 were studies conducted in adult patients, 20 were protocols or registered trials, 11 were reviews, 9 were irrelevant studies, 3 were conferences news, 2 were case reports or letters, 2 were previous systematic reviews published in 2016 and in 2017. And then 8 items were excluded by full-text screening, five of them reported the uncorrelated outcomes, and three of them were owing to the inappropriate comparisons. Eventually, 18 studies were chosen in consequent analysis [21,22,23,24,25,26,27,28,29,30,31,32,33,34,35,36,37,38]. The process of literatures identification is described in PRISMA flowchart (Fig. 1).
Basic characteristics of enrolled studies
The enrolled studies were published from 2009 to 2020, and a total of 1,065 eligible pediatric patients (ages ranged from 7 days to 18 years) were included in analysis. The outcome “time interval from administration of reversal agents to train-of-four ratio” was reported in 17 studies [21,22,23,24,25,26,27,28,29,30,31, 33,34,35,36,37,38], and the outcome “extubation time” was reported in 14 studies [23,24,25, 28,29,30,31,32,33,34,35,36,37,38]. 0.6 mg/kg rocuronium was given in all patients except patients in Veiga RG et al. study [22] (Rocuronium 0.45 mg/kg). And most of studies focused on evaluation in sugammadex versus combination of acetylcholinesterase inhibitors and anticholinergics, only two studies compared sugammadex with placebo. The main characteristics of all enrolled studies were summarized in Table 1.
Risk of bias assessment
We used Cochrane Collaboration’s risk of bias tool to evaluate the validity and quality of these enrolled studies [20]. In random sequence generation domain, 12 studies had low risk [21, 25, 27,28,29,30,31,32,33,34, 36, 37], and 6 studies had unclear risk [22,23,24, 26, 35, 38]. In allocation concealment domain, 6 studies had low risk of bias [21, 26, 29, 30, 32, 34], and 12 studies had unclear risk [22,23,24,25, 27, 28, 31, 33, 35,36,37,38]. Ten studies had low risk of bias [21, 24, 26, 28, 30,31,32,33,34, 36] and rest of studies had unclear risk of bias [22, 23, 25, 27, 29, 35, 37, 38] in blinding of participants and personnel domain. One study had a high risk of bias [28], 9 studies had low risk of bias [21, 24, 26, 30,31,32,33,34, 36], and 8 studies had unclear risk [22, 23, 25, 27, 29, 35, 37, 38] in blinding of outcome assessment domain. Sixteen studies had low risk of bias in incomplete outcome data [21, 23, 25,26,27,28,29,30,31,32,33,34,35,36,37,38] and rest of studies had unclear risk of bias [22, 24]. In selective reporting domain, 16 studies had low risk [21, 23,24,25,26,27,28,29,30,31, 33,34,35,36,37,38], and two studies had unclear risk of bias [22, 32].
Primary outcome 1: time interval from administration of reversal agents to train-of-four ratio (TOFr) > 0.9
Seventeen studies including 995 pediatric patients described the time from NMB reversal to recovery of the TOF ratio to 0.9. The I2 of 99% indicated that substantial heterogeneity was existed, but the source could not be attributed clearly to one particular study by sensitivity analysis; thus, the random effects model was used. According to present analysis with larger sample size, the use of sugammadex was associated with significantly shorter duration from administration of reversal agents to TOFr > 0.9 compared to traditional acetylcholinesterase inhibitors or placebo (MD -14.42 with 95% CI [-17.08, -11.75], P < 0.00001, I2 = 99%) (Fig. 2A). Publication bias was detected in analysis by both Begg's test (P = 0.001) and Egger's test (P = 0.000) (Fig. 4A). In order to estimate and adjust for the number and outcomes of missing studies, we performed Duval's trim and fill method [41] by using version 1.0.5 of the metatrim program, Stata/MP 12.0 for Windows (StataCorp LP, 4905 Lakeway Drive, College Station, TX 77,845, USA). The trim-and-fill method showed no trimming performed and data unchanged. The information about trim and fill procedure was provided in Appendix S2. The outcome of TSA indicated that the cumulative Z curves crossed the conventional boundary, trial sequential monitoring boundary, and also the required information size (calculated as 358). It revealed that the sample size of patients was enough, and further studies would be unlikely to change the conclusion (Fig. 2B). According to GRADE summary of findings table, the quality of evidence for this outcome was low. It might be resulted from inconsistency (I2 > 50%) and existed publication bias (Table S1).
A Forest plot depicting the meta-analysis for the outcome “time interval from administration of reversal agents to train-of-four ratio (TOFr) > 0.9” for sugammadex versus controls; B Trial sequential analysis for the outcome “time interval from administration of reversal agents to train-of-four ratio (TOFr) > 0.9”. Notes: Green + dot, low risk of bias; yellow ? dot, unclear risk of bias; red—dot, high risk of bias. (Abbreviations: CI, Confidence interval)
Primary outcome 2: extubation time
A total of 14 studies involving 883 pediatric patients reported the duration from NMB reversal to extubation. By the same token, I2 of 99% existed the significant heterogeneity. However, all attempts to reduce the value of I2 to below 50% by excluding one single study were not successful in sensitivity analysis, therefore, the random effects model was used by us. The use of sugammadex was associated with shorter interval from reversal from NMB to extubation compared to acetylcholinesterase inhibitors or placebo (MD -13.98 with 95% CI [-16.70, -11.26], P < 0.00001, I2 = 99%) (Fig. 3A). However, results from Begg's test (P = 0.002) and Egger’s test (P = 0.000) indicated that publication bias was existed in the analysis (Fig. 4B). Duval's trim and fill method was conducted, and results showed no trimming performed and data unchanged. The information about trim and fill procedure was provided in Appendix S2. The result from TSA indicated that with a required information size of 747, firm evidence was in place in favor of sugammadex (Fig. 3B). The GRADE summary of findings table indicated that quality of evidence for present outcome was low. Inconsistency (I2 > 50%) and publication bias may be considered as main factors (Table S1).
A Forest plot depicting the meta-analysis for the outcome “extubation time” for sugammadex versus controls; B Trial sequential analysis for the outcome “extubation time”. Notes: Green + dot, low risk of bias; yellow ? dot, unclear risk of bias; red—dot, high risk of bias. (Abbreviations: CI, Confidence interval)
Secondary outcomes
Adverse effects including postoperative nausea and vomiting (PONV), bradycardia, pain, spasm, dry mouth, apnea, and oxygen desaturation were considered as our secondary outcomes. The results indicated that use of sugammadex was associated with significantly lower incidence of PONV (RR = 0.30; 95%CI: 0.20 to 0.46), bradycardia (RR = 0.09; 95%CI: 0.02 to 0.46), and dry mouth (RR = 0.14; 95%CI: 0.05 to 0.38) compared to acetylcholinesterase inhibitors or placebo. For other adverse effects, no significant differences were found between the two groups. The results of publication bias were (P = 0.088, Begg’s test and P = 0.004, Egger’s test) (Fig. 4C), however, the trim-and-fill method to adjust for funnel plot asymmetry showed no trimming performed and data unchanged. Owing to absence of statistical heterogeneity (I2 < 50%) in secondary outcomes, the fixed-effects model was used. The details of secondary outcomes were demonstrated in Table 2. The results from GRADE summary of table revealed that quality of evidence for most of secondary outcomes was low and imprecision (lack of events number) was served as the main reason. The details were provided in Table S1.
Discussion
The meta-analyses conducted by Won et al. [16] and Liu et al. [17] included RCTs published during 2016–2017 and demonstrated the superiority of sugammadex in providing rapid recovery in children. However, limited sample size (253 patients and 575 patients individually) of the two studies and increasing clinical applications of sugammadex in recent years prompted us to update the research.
Our present study evaluated a total of 18 RCTs enrolled over 1000 pediatric patients. The results indicated that administration of sugammadex in children was associated with shorter duration from administration of reversal agents to TOFr > 0.9 and shorter interval from reversal from NMB to extubation compared to acetylcholinesterase inhibitors or placebo. It confirmed and strengthened the findings of previous meta-analyses. And TSA results from our present study about the co-primary outcomes indicated that the present evidences of anticipated intervention effects were sufficient.
As one of main adverse effects appeared in post-anaesthesia care units (PACU), PONV after general anaesthesia may be resulted from multiple causative factors, such as inhalational anaesthesia and perioperative opioids use [42]. The study conducted by Liu et al. [17] described no difference in incidence of nausea and vomiting between sugammadex group and control group. However, the present study with a larger sample size demonstrated that the application of sugammadex was associated with significantly lower incidence of PONV in pediatric patients compared to control group.
According to previous retrospective analysis and review [14, 43], bradycardia, one of significant adverse effects of NMB reversal agents, was found more commonly in neostigmine patients than in sugammadex patients. The results of our present study suggested that incidence of both bradycardia and dry mouth was significant lower in sugammadex patients, and no difference was found in occurrence of pain, bronchospasm, laryngospasm, apnea and oxygen desaturation between two groups. Regrettably, even though we performed a thorough search including several international and one Chinese database, the sample size of most secondary outcomes was still limited, and it was insufficient to draw reliable conclusions.
Another limitation from our present study was the widespread low quality in outcomes exhibited by GRADE approach evaluation, which resulted from publication bias, inconsistency (high heterogeneity) and imprecision (lack of events number). The results of Begg's test and Egger's test indicated that publication bias were existed in several outcomes. However, the trim-and-fill method to adjust for funnel plot asymmetry revealed no trimming performed and data unchanged. Actually, publication bias should be considered as one major difficulty in systematic reviews. The researches with statistically significant results were tend to be the ones accepted for publication rather than studies with inconclusive outcomes or with no obvious treatment effects [44]. Therefore, the review of published studies might be identified as a biased selection of the researches, and sometimes the problems from publication bias were inevitable. Therefore, to overcome the problems, we conducted a thorough search for grey literature from websites “http://www.greylit.org/” and “http://greyguide.isti.cnr.it/” by using key terms “sugammadex” or “bridion” or “25,969” or “361LPM2T56” (Accessed 6 April 2022). However, no results were found. In addition, the attempts to reduce high heterogeneity by excluding one single study were failed in sensitivity analysis, and it led us to use random effects models for meta-analysis.
Conclusion
Although detected heterogeneity was considerable in primary outcomes, the results of present study demonstrated that the use of sugammadex was associated with more rapid reversal of rocuronium-induced neuromuscular blockade when compared with control groups. And TSA provided firm evidence in favor of sugammadex for primary outcomes. However, overall low-quality evidences evaluated by GRADE system demonstrated that superiority of sugammadex in providing adequate efficacy and safety of NMB reversal in children needs to be confirmed by more studies with high quality and large sample size in future.
Availability of data and materials
All data generated or analysed during this study are included in this published article [and its supplementary information files].
Abbreviations
- TSA:
-
Trial sequential analysis
- NMB:
-
Neuromuscular blockade
- TOFr:
-
Train-of-four ratio
- GRADE:
-
Grading of recommendations assessment, development, and evaluation
- PONV:
-
Postoperative nausea and vomiting
- NMBAs:
-
Neuromuscular blocking agents
- RCTs:
-
Randomized controlled trials
- CNKI:
-
China National Knowledge Infrastructure
- MD:
-
Mean difference
- CI:
-
Confidence interval
- RR:
-
Risk ratio
- RIS:
-
Required information size
- PACU:
-
Post-anaesthesia care units
References
Murphy GS. Neuromuscular monitoring in the perioperative period. Anesth Analg. 2018;126:464–8.
Murphy GS, Brull SJ. Residual neuromuscular block: lessons unlearned. Part I: definitions, incidence, and adverse physiologic effects of residual neuromuscular block. Anesth Analg. 2010;111(1):120–8.
Grosse-Sundrup M, Henneman JP, Sandberg WS, Bateman BT, Uribe JV, Nguyen NT, et al. Intermediate acting non-depolarizing neuromuscular blocking agents and risk of postoperative respiratory complications: prospective propensity score matched cohort study. BMJ. 2012;15(345):e6329. https://doi.org/10.1136/bmj.e6329.
Abrishami A, Ho J, Wong J, Yin L, Chung F. Sugammadex, a selective reversal medication for preventing postoperative residual neuromuscular blockade. Cochrane Database Syst Rev. 2009;4:CD007362.
Kirkegaard-Nielsen H, Helbo-Hansen HS, Lindholm P, Severinsen IK, Bülow K. Time to peak effect of neostigmine at antagonism of atracurium- or vecuronium-induced neuromuscular block. J Clin Anesth. 1995;7:635–9.
Kirkegaard-Nielsen H, Helbo-Hansen HS, Lindholm P, Severinsen IK, Pedersen HS, Jensen EW. Optimum time for neostigmine reversal of atracurium-induced neuromuscular blockade. Can J Anaesth. 1996;43:932–8.
Bom A, Bradley M, Cameron K, Clark JK, Van Egmond J, Feilden H, et al. A novel concept of reversing neuromuscular block: chemical encapsulation of rocuronium bromide by a cyclodextrin-based synthetic host. Angew Chem Int Ed Engl. 2002;41(2):265–70.
Caldwell J. Sugammadex: past, present and future. Adv Anaesth. 2011;29:19–27.
Moore E, Hunter J. The new neuromuscular blocking agents: do they offer any advantages? Br J Anaesth. 2001;87(6):912–25.
Gijsenbergh F, Ramael S, Houwing N, van Iersel T. First human exposure of Org 25969, a novel agent to reverse the action of rocuronium bromide. Anesthesiology. 2005;103(4):695–703.
Hristovska AM, Duch P, Allingstrup M, Afshari A. Efficacy and safety of sugammadex versus neostigmine in reversing neuromuscular blockade in adults. Cochrane Database Syst Rev. 2017;8(8):CD012763.
Merck.com. Highlights of prescribing information BRIDION® (sugammadex) Injection, for intravenous use Initial U.S. Approval. 2015. Available at: https://www.merck.com/product/usa/pi_circulars/b/bridion/bridion_pi.pdf. Accessed 24 Oct 2020
Tobias JD. Current evidence for the use of sugammadex in children. Paediatr Anaesth. 2017;27(2):118–25.
Tobias JD. Sugammadex: Applications in Pediatric Critical Care. J Pediatr Intensive Care. 2020;9(3):162–71.
Faulk DJ, Austin TM, Thomas JJ, Strupp K, Macrae AW, Yaster M. A Survey of the Society for Pediatric Anesthesia on the Use, Monitoring, and Antagonism of Neuromuscular Blockade. Anesth Analg. 2021. https://doi.org/10.1213/ANE.0000000000005386.
Won YJ, Lim BG, Lee DK, Kim H, Kong MH, Lee IO. Sugammadex for reversal of rocuronium-induced neuromuscular blockade in pediatric patients: A systematic review and meta-analysis. Medicine (Baltimore). 2016;95(34):e4678.
Liu G, Wang R, Yan Y, Fan L, Xue J, Wang T. The efficacy and safety of sugammadex for reversing postoperative residual neuromuscular blockade in pediatric patients: A systematic review. Sci Rep. 2017;7(1):5724.
Moher D, Liberati A, Tetzlaff J, Altman DG. Preferred reporting items for systematic reviews and meta-analyses: the PRISMA statement. BMJ. 2009;339:b2535.
Kopman AF, Yee PS, Neuman GG. Relationship of the train-of-four fade ratio to clinical signs and symptoms of residual paralysis in awake volunteers. Anesthesiology. 1997;86:765–71.
Higgins JP, Thomas J, Chandler J, Cumpston M, Li T, Page MJ, Welch VA. Cochrane Handbook for systematic reviews of interventions version 6.0, vol. 4. 2019. p. 64–75.
Plaud B, Meretoja O, Hofmockel R, Raft J, Stoddart PA, van Kuijk JH, et al. Reversal of rocuronium-induced neuromuscular blockade with sugammadex in pediatric and adult surgical patients. Anesthesiology. 2009;110(2):284–94. https://doi.org/10.1097/ALN.0b013e318194caaa (PMID: 19194156).
Veiga R, Carceles B, Dominguez S, Lopez F, Orozco M, Alvarez-Gomez J. Sugammadex reversal efficacy and security vs neostigmine in the rocuronium-induced neuromuscular blockade in paediatric patients:10AP3-5. Eur J Anaesthesiol. 2011;28:153.
Alvarez-Gomez JA, Baron M, Ruiz GV, et al. Efficacy and safety of the reversal with sugammadex from deep rocuronium-induced neuromuscular blockade in children. 2012. (http://www.asaabstracts.com/strands/asaabstracts/abstract.htm?year=2012&index=16&absnum=2981).
Gaona D, Carceles M, Veiga G, Lopez R, Mejia J, Asensi P. Efficacy and safety of the reversal with sugammadex in deep neuromuscular blockade induced by rocuronium in pediatrics. Br J Anaesth. 2012;108(S2):308–9.
Kara T, Ozbagriacik O, Turk HS, Isil CT, Gokuc O, Unsal O, et al. Sugammadex versus neostigmine in pediatric patients: a prospective randomized study. Rev Bras Anestesiol. 2014;64(6):400–5.
Ozgün C, Cakan T, Baltacı B, Başar H. Comparison of reversal and adverse effects of sugammadex and combination of - Anticholinergic-Anticholinesterase agents in pediatric patients. J Res Med Sci. 2014;19(8):762–8.
Ghoneim AA, El Beltagy MA. Comparative study between sugammadex and neostigmine in neurosurgical anesthesia in pediatric patients. Saudi J Anaesth. 2015;9(3):247–52.
El Sayed M, Hassan S. Does sugammadex facilitate recovery after outpatient tonsillectomy in children? Egyt J Anesth. 2016;32(4):447–50.
Güzelce D, Kendigelen P, Tütüncü A, Kaya G, Altintas F. Comparison of sugammadex and neostigmine in terms of time to extubation in pediatrics. Med Bull Haseki. 2016;54:207–11.
Mohamad Zaini RH, Penny Tevaraj JM, Wan Hassan WN, et al. Comparison between the efficacy of neostigmine versus sugammadex for reversal of rocuronium induced neuromuscular blockade in paediatric patients. Anesth Analg. 2016;123:329.
Ammar AS, Mahmoud KM, Kasemy ZA. A comparison of sugammadex and neostigmine for reversal of rocuronium-induced neuromuscular blockade in children. Acta Anaesthesiol Scand. 2017;61(4):374–80.
Korkmaz MO, Sayhan H, Guven M. Does sugammadex decrease the severity of agitation and complications in pediatric patients undergoing adenotonsillectomy? Saudi Med J. 2019;40(9):907–13.
An J, Lee JH, Kim E, Woo K, Kim H, Lee D. Comparison of sugammadex and pyridostigmine bromide for reversal of rocuronium-induced neuromuscular blockade in short-term pediatric surgery: a prospective randomized study. Anesthesia and Pain Medicine. 2019;14(3):288–93.
Hussein AA, Hegazy MM, Elramely MA, Mohamed AG. Sugammadex versus neostigmine in pediatric cancer patients undergoing outpatient surgical procedures. Int J Res Pharm Sci. 2020;11(2):2741–6.
Li XB, Jiang Y, Zhang WP, Zhang RF, Li J, Wei R. Effects of sugammadex on postoperative respiratory management in children with congenital heart disease: a randomized controlled study. Biomed Pharmacother. 2020;127:110180.
Li L, Jiang Y, Zhang W. Sugammadex for Fast-Track Surgery in Children Undergoing Cardiac Surgery: A Randomized Controlled Study. J Cardiothorac Vasc Anesth. 2021;35(5):1388–92.
Hu J, Peng Z, Wang L, Zhang R, Bai J. A comparison of sugammadex and neostigmine for reversal of rocuronium-induced neuromuscular blockade undergoing laparoscopic inguinal hernia repair in children. Int J Anesth Resus. 2020;41(6):550–4. https://doi.org/10.3760/cma.j.cn321761-20190722-00049.Chinese.
Jiang Y, Wei R, Zhang R, Zheng J. Efficacy and safety of sugammadex in reversing rocuronium-induced neuromuscular blockade in children post elective tonsillectomy. Pharm Clin Res. 2020;02:139–41. https://doi.org/10.13664/j.cnki.pcr.2020.02.015.Chinese.
Guyatt GH, Oxman AD, Schünemann HJ, Tugwell P, Knottnerus A. GRADE guidelines: a new series of articles in the Journal of Clinical Epidemiology. J Clin Epidemiol. 2011;64:380–2.
Holst LB, Petersen MW, Haase N, Perner A, Wetterslev J. Restrictive versus liberal transfusion strategy for red blood cell transfusion: systematic review of randomised trials with meta-analysis and trial sequential analysis. BMJ. 2015;350:h1354.
Duval S, Tweedie R. Trim and fill: a simple funnel-plot–based method of testing and adjusting for publication bias in meta-analysis. Biometrics. 2000;56(2):455–63.
Apfel CC, Stoecklein K, Lipfert P. PONV: a problem of inhalational anaesthesia? Best Pract Res Clin Anaesthesiol. 2005;19(3):485–500.
Gaver RS, Brenn BR, Gartley A, Donahue BS. Retrospective analysis of the safety and efficacy of sugammadex versus neostigmine for the reversal of neuromuscular blockade in children. Anesth Analg. 2019;129(4):1124–9.
Copas JB, Shi JQ. A sensitivity analysis for publication bias in systematic reviews. Stat Methods Med Res. 2001;10(4):251–65.
Acknowledgements
Not applicable.
Funding
The present study was supported by the Science and Technology Plan Project of Sichuan Province (2020YFS0035).
Author information
Authors and Affiliations
Contributions
Bingchen Lang, Lu Han, Lingli Zhang and Qin Yu helped contributed to the conception and design of the study, and write the manuscript; Lingli Zhang, Qin Yu, and Zhijun Jia provided the administrative support; Bingchen Lang, Qianqian Zhang and Shouming Chen contributed to collection and analysis of data; Linan Zeng, Liang Huang, Lingli Zhang and Qin Yu participated in the critical review of the manuscript; All authors read and approved the final manuscript.
Corresponding authors
Ethics declarations
Ethics approval and consent to participate
Not applicable.
Consent for publication
Not applicable.
Competing interests
The authors declare that they have no competing interests.
Additional information
Publisher’s Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if changes were made. The images or other third party material in this article are included in the article's Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article's Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by/4.0/. The Creative Commons Public Domain Dedication waiver (http://creativecommons.org/publicdomain/zero/1.0/) applies to the data made available in this article, unless otherwise stated in a credit line to the data.
About this article
Cite this article
Lang, B., Han, L., Zeng, L. et al. Efficacy and safety of sugammadex for neuromuscular blockade reversal in pediatric patients: an updated meta-analysis of randomized controlled trials with trial sequential analysis. BMC Pediatr 22, 295 (2022). https://doi.org/10.1186/s12887-022-03288-0
Received:
Accepted:
Published:
DOI: https://doi.org/10.1186/s12887-022-03288-0