Abstract
Background
Anaplastic thyroid carcinoma (ATC) is the most aggressive subtype of thyroid cancer. In this study, we used a three-dimensional in vitro system to evaluate the effect of a dual MEK/Aurora kinase inhibitor, BI-847325 anticancer drug, on several cellular and molecular processes involved in cancer progression.
Methods
Human ATC cell lines, C643 and SW1736, were grown in alginate hydrogel and treated with IC50 values of BI-847325. The effect of BI-847325 on inhibition of kinases function of MEK1/2 and Aurora kinase B (AURKB) was evaluated via Western blot analysis of phospho-ERK1/2 and phospho-Histone H3 levels. Sodium/iodide symporter (NIS) and thyroglobulin (Tg), as two thyroid-specific differentiation markers, were measured by qRT-PCR as well as flow cytometry and immunoradiometric assay. Apoptosis was assessed by Annexin V/PI flow cytometry and BIM, NFκB1, and NFκB2 expressions. Cell cycle distribution and proliferation were determined via P16, AURKA, and AURKB expressions as well as PI and CFSE flow cytometry assays. Multidrug resistance was evaluated by examining the expression of MDR1 and MRP1. Angiogenesis and invasion were investigated by VEGF expression and F-actin labeling with Alexa Fluor 549 Phalloidin.
Results
Western blot results showed that BI-847325 inhibits MEK1/2 and AURKB functions by decreasing phospho-ERK1/2 and phospho-Histone H3 levels. BI-847325 induced thyroid differentiation markers and apoptosis in ATC cell lines. Inversely, BI-847325 intervention decreased multidrug resistance, cell cycle progression, proliferation, angiogenesis, and invasion at the molecular and/or cellular levels.
Conclusion
The results of the present study suggest that BI-857,325 might be an effective multi-targeted anticancer drug for ATC treatment.
Similar content being viewed by others
Background
Anaplastic thyroid carcinoma (ATC) is one of the most lethal malignancies, with a median survival rate of six months. In general, surgical- and radioiodine-based therapeutic procedures are not effective, and ATC patients have poor prognoses with high morbidity and mortality. At present, there is no standard therapy for ATC, and the patientsʼ survival rate has not improved for decades [1, 2].
Considerable progress has been made in identifying genetic changes and signaling pathways, involved in the invasiveness of ATC. Several new therapies that target the relevant pathways are currently undergoing clinical trials [1]. In ATC, most genetic mutations, importantly BRAFV600E, affect the MEK/ERK signaling pathway [3]. Activation of the Mitogen-Activated Protein Kinase (MAPK) Pathway plays a key role in the regulation of the cell cycle, apoptosis, proliferation, differentiation, invasion, angiogenesis, and drug resistance [4, 5]. At present, genetic-based targeted therapy is the most promising curative plan in ATC. A wide range of inhibitors have been discovered against the main effectors of the MAPK pathway that demonstrate anticancer potential by suppressing the growth of tumor cells both in vitro and in vivo [1]. Since MEK is the downstream effector of BRAF, MEK inhibition is an effective strategy to block the reactivation of the MAPK pathway in ATC. In 2018, Dabrafenib, a BRAF inhibitor, in combination with Trametinib, a MEK inhibitor, were approved by the Food and Drug Administration (FDA) for the treatment of ATC patients with the BRAFV600E mutation [6, 7].
In addition to genetic alterations, the ability of high proliferation, a hallmark of cancers, is thought to represent a major driving force in ATC progression and poor prognosis [8]. A number of mitotic kinases with irregular expression in malignant thyroid tissues are involved in the growth of thyroid tumors. These include three members of the Aurora kinase family (AURKA, AURKB, and AURKC), serin/thereonine kinases that regulate multiple aspects of tumor growth and progression [9]. In recent years, a wide range of Aurora kinase inhibitors have been developed that have shown promising antitumor effects against ATC in preclinical studies [10].
At present, several hybrid compounds are introduced for cancer treatment that are multi-target in nature due to simultaneously interfering with different signaling pathways involved in cancer development [11, 12]. BI-847325, a selective dual MEK/Aurora kinase inhibitor, is one of the multi-target anticancer drugs [13]. This hybrid compound may reduce the risk of adverse drug reactions and side effects [13,14,15]. However, despite the acceptable safety profile of BI-847325, its development has been halted due to insufficient drug exposure at the maximum tolerated dose (MTD) to achieve MEK inhibition in cancers such as liver, kidney, breast, and melanoma [16].
The microenvironment is an emerging concept in cancer biology that is shown to dramatically alter not only the behavior of tumor cells but also drug responses. However, most in vitro studies testing drug effects on cancer cells use two-dimensional (2D) cell culture protocols. In a traditional 2D culture system, adherent tumor cells are attached to the plastic surface of a Cell Culture Flask or Flat Petri Dish and grown as a monolayer. This routine method of cell culture has advantages such as simple maintenance and cost-effectiveness, but it also has the disadvantage of incompetence in simulating the tumor microenvironment [17]. Indeed, three-dimensional (3D) cell culture models better mimic the natural tumor microenvironment such as physiological gradient, cell-cell communications, and cell-matrix interactions. Therefore, 3D cell culture systems have an important role in the discovery of anticancer drugs. In recent years, the use of 3D models in cancer research has substantially increased [18, 19].
In the present study, the effect of dual MEK/Aurora kinase inhibitor BI-847325 on the key biological processes involved in cancer progression including cell cycle, apoptosis, proliferation, differentiation, invasion, angiogenesis, and drug resistance was evaluated using a 3D in vitro ATC model at the molecular and/or cellular levels.
Materials and methods
2D cell culture
Human ATC cell lines, C643 and SW1736, were purchased from Cell Lines Service (CLS, Germany). Both of the cell lines were cultured according to the providerʼs instruction.
3D cell culture and cytotoxicity assay
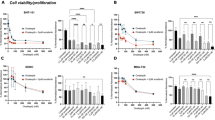
C643 and SW1736 ATC cell lines were grown in the alginate hydrogel [20, 21]. The cytotoxic effect of BI-847325 (Adooq Bioscience, Irvine, CA, USA, Cat. No.: A15762) on 3D-cultured cells was measured in 24, 48, and 72 h by MTT [3-(4,5-dimethylthiazolyl-2)-2,5-diphenyltetrazolium bromide] assay. The half-maximal inhibitory concentration (IC50) of BI-847325 anticancer drug was calculated in 3D cell culture system for each ATC cell line as previously described [20, 21].
Cell cycle assay
The spheroids were pre-cultured before BI-847325 treatment. Then, C643 and SW1736 cell lines were treated with 15 µM and 34 µM concentrations (IC50 values) of BI-847325 for 48 h, respectively. Cells were revived from the alginate scaffold using sodium citrate (55 mM, 10 mM HEPES, pH 7.4) as previously explained [22] and analyzed through the Cell Cycle Assay Kit (Abcam, Cambridge, USA) according to the manufactureʼs protocol. Cell cycle distribution for each cell line was evaluated by flow cytometry using BD FACSCalibur. The percentage of cells in the G0/G1, S, and G2/M phases was determined using FlowJo software.
Apoptosis assay
Treated cells with IC50 values of BI-847325 were revived from the hydrogel scaffold. For apoptosis assay, the Annexin V-FITC Apoptosis Detection Kit (Invitrogen, Carlsbad, CA, USA) was used. The apoptotic cells were detected and quantified by flow cytometry using BD FACSCalibur. The data was analyzed using FlowJo software.
Cell proliferation assay
Before alginate encapsulation and treatment, cells were labeled using CellTrace™ CFSE Cell Proliferation Kit (Invitrogen, Carlsbad, CA, USA) according to the manufactureʼs instruction. The proliferation capacity of C643 and SW1736 was measured by flow cytometry using BD FACSCalibur after treatment with IC50 values of BI-847325 and decapsulation. The proliferation data were analyzed using FlowJo software.
Flow cytometric detection of sodium/iodide symporter (NIS)
The cell lines were treated with IC50 values of BI-847325 and removed from the scaffold after 48 h. The amount of NIS protein was assessed using the anti-human NIS antibody (Abcam, Cambridge, UK, Cat. No.: ab17795) by flow cytometry according to the manufactureʼs protocol. Isotype control antibody (mouse IgG1, Abcam, Cambridge, UK) was used under the same condition. The relative expression of NIS protein was determined using FlowJo software by comparing the mean fluorescence intensity between treated and untreated cells.
Immunoradiometric assay (IRMA)
Culture condition, treatment, and decapsulation have been described above. Before h-thyroglobulin (Tg) measurement, cell lines were physically lyzed by sonication with 15-W power for 30 s with consecutive 1 s ON and 1 s OFF power (Bandelin, model HD3100). The amount of Tg protein was measured by IRMA Kit (Isotopes Co., Ltd. (IZOTOP), Budapest, Hungary), based on the manufactureʼs guideline.
Invasion assay
Invasion of pre- and post-treatment of C643 and SW1736 ATC cell lines was evaluated following fixation of alginate-encapsulated cells with 4% paraformaldehyde. The nuclei and actin filaments were stained with DAPI and Alexa Fluor™ 549 Phalloidin (Invitrogen, Carlsbad, CA, USA), respectively. Then, the stained cells were imaged by the fluorescence microscopy.
Western blotting assay
After decapsulating the cells from the hydrogel, protein extraction and Western blotting were carried out as described by Eslami et al. [23]. The following primary antibodies were used to confirm the inhibitory effect of BI-847325 on the function of MEK1/2 and AURKB kinases in the treated cell lines: Total p44/42 MAPK (ERK1/2), Phosphorylated p44/42 MAPK (ERK1/2)Thr202/Tyr204, Histone H3, Phospho-Histone H3 (Ser10) (Cell Signaling Technologies, UK, Cat. No.: #9102, #4370, #4499, #53,348, respectively), and β-actin (PADZA, Tehran, Iran, Cat. No.: MM114). Secondary antibodies included HRP-conjugated goat anti-rabbit IgG and HRP-conjugated goat anti-mouse IgG were a kind gift from Dr. Mohammad Reza Nejadmoghaddam (Avicenna Research Institute, Tehran, Iran).
Quantitative real-time PCR (qRT-PCR) assay
Treated cells with IC50 values of BI-847325 were removed from the alginate scaffold after 48 h. RNA isolation, complementary DNA (cDNA) synthesis, and qRT-PCR were performed as previously described [22]. Changes in mRNA expression were normalized to β-actin. The primer sequences are listed in Table 1.
Statistical analysis
All the experiments except Western blot were performed two times. Data were analyzed using GraphPad Prism software (GraphPad PRISM V 5.0) and presented as means ± standard deviation (SD). The gene expression analyses were done using 2–∆∆Ct method. Two-way ANOVA was used for the statistical analysis of the cell cycle and apoptosis experiments. The statistical significance of other assays was determined by t-test. Statistical significances are expressed as p < .05 (*); p < .01 (**); p < .001 (***); p < .0001 (****).
Results
qRT-PCR
BI-847325 regulated cell cycle and proliferation through upregulation of P16 and downregulation of AURKA and AURKB
The expression of P16, as a suppressor of cell cycle progression at the G1/S checkpoint [24], was measured after BI-847325 treatment on C643 and SW1736 cell lines. As shown in Fig. 1A and B, the expression of P16 was significantly upregulated after treatment in both ATC cell lines. Also, the expression of key regulators of the G2/M transition of the mitotic cell cycle, AURKA [25] and AURKB [26], were evaluated following treatment. The data showed that the expression of AURKA was significantly decreased in comparison with untreated control in C643 and SW1736. However, the expression of AURKB was merely downregulated SW1736 cell line (Fig. 1A and B).
The effect of BI-847325 on the expression of different inspected genes in C643 and SW1736 ATC cell lines. A The expression of AURKA, MDR1, MRP1, NFκB2, and VEGF genes was significantly decreased in C643 cell line. The expression of P16 and BIM as well as NIS and Tg genes was significantly increased in this cell line. All the expressions were compared to the untreated control 48 h after treatment with 15 µM of BI-847325. B The expression of AURKA, AURKB, MDR1, MRP1, NFκB1, NFκB2, and VEGF genes was significantly decreased in SW1736 cell line. The expression of P16 and BIM as well as NIS and Tg genes was significantly increased in this cell line. All the expressions were compared to the untreated control 48 h after treatment with 34 µM of BI-847325. Statistical significances are expressed as p < .05 (*); p < .01 (**); p < .001 (***); p < .0001 (****). C Gplot heatmap of gene expression data in C643 and SW1736 ATC cell lines. The differences between the gene expression profile of AURKA, AURKB, MDR1, MRP1, NFκB1, NFκB2, VEGF, P16, BIM, NIS, and Tg in C643 and SW1736 are shown as color-coded: crimson for upregulated and dark blue for downregulated genes
BI-847325 induced apoptosis and necrosis via upregulation of BIM and downregulation of NFκB1 and NFκB2
Inhibition of MEK activity was shown to regulate the expression of pro-apoptotic gene BIM and anti-apoptotic genes NFκB1 and NFκB2. As shown in Fig. 1A and B, the expression of BIM was significantly upregulated by BI-847325 treatment in both ATC cell lines. Reversely, the expression of NFκB2 was significantly decreased following treatment in the two cell lines. However, the expression of NFκB1 was significantly downregulated by BI-847325 just in SW1736 cell line. It should be noted that the expression of AURKA and AURKB genes, which are also involved in inducing apoptosis, decreased after treatment as mentioned above.
BI-847325 decreased multidrug resistance through downregulation of MDR1 and MRP1
Suppression of MAPK signaling pathway activity by BI-847325 treatment could significantly decrease the expression of MDR1 and MRP1 genes in C643 and SW1736 ATC cell lines (Fig. 1A and B).
BI-847325 induced redifferentiation via upregulation of NIS and Tg
To evaluate the amount of differentiation in C643 and SW1736 cells following drug intervention, the expressions of NIS and Tg, as two thyroid-specific differentiation markers, were measured. The qRT-PCR results showed that the expressions of both genes were significantly increased in BI-847325 treated cells in comparison with the control (Fig. 1A and B).
BI-847325 decreased angiogenesis through downregulation of VEGF
Inhibition of the MEK/ERK pathway was shown to decrease the expression of VEGF gene. As shown in Fig. 1A and B, the expression of VEGF was significantly downregulated following BI-847325 treatment in C643 and SW1736 ATC cell lines.
The differences in the gene expression patterns of all measured genes in C643 and SW1736 cells are shown in Fig. 1C.
Flow cytometry and IRMA
BI-847325 regulated cell cycle
Changes in the cell cycle distribution induced after BI-847325 treatment were evaluated by cellular DNA content and cell cycle profiling using flow cytometry. The treatment of ATC cells caused different results in cell cycle phase distribution in each cell line (Fig. 2A–D). BI-847325 decreased the number of cells in the G0/G1 and S phases in C643 and SW1736 cells and increased the accumulation of cells in G2/M just in C643 cell line. Moreover, as shown in Fig. 2A–D, BI-847325 significantly induced apoptosis, which was measured by the proportion of sub-G1 cells compared to the controls. Flow cytometry analysis further confirmed the related data in mRNA levels of P16, AURKA, and AURKB genes concerning the effect of BI-843,725 anticancer drug on the cell cycle regulation.
The effect of BI-847325 on the cell cycle distribution, apoptosis, and proliferation in C643 and SW1736 ATC cell lines. A, B After 48 h of drug intervention, C643 and SW1736 cells were subjected to cell cycle analysis by PI flow cytometry. The percentage of cells in sub-G1, G0/G1, S, and G2/M phases are indicated for each cell line. The untreated cells were considered as control. C, D Representative histogram of cell cycle analysis based on flow cytometry in 48 h after BI-847325 treatment of C643 and SW1736 compared to untreated cells as control. E, F Apoptosis assessment using Annexin V/PI flow cytometry in BI-847325 treated cells in comparison with untreated cells as control. G, H Graphical representation of early apoptosis, late apoptosis, and necrosis based on flow cytometry in 48 h after BI-847325 treatment of C643 and SW1736 compared to untreated cells as control. Cellular proliferation of untreated and treated cells was measured using flow cytometry 48 h after treatment. I, J CFSE histograms for C643 and SW1736. Orange histograms show 18 h after labeling, which confirms labeled but non-proliferating cells. K The diagram shows significantly higher fluorescence intensity and consequently lower proliferation in treated ATC cell lines compared to untreated cells. Statistical significances are expressed as p < .05 (*); p < .01 (**); p < .001 (***); p < .0001 (****)
BI-847325 induced apoptosis
The inhibition of the MAPK signaling pathway and the members of Aurora kinase family may lead to the induction of apoptosis. The ability of BI-847325 to cause apoptotic/necrotic cell death in ATC cell lines was analyzed using flow cytometry. Treatment of C643 and SW1736 caused different results in each cell line. As shown in Fig. 2E–H, BI-847325 treatment resulted in significant induction of death in two ATC cell lines, 67% in C643 and 35.7% in SW1736. Flow cytometry analysis of cellular apoptosis further confirmed the obtained data concerning the effect of BI-847325 on cell death via transcript-level regulation of apoptotic-/necrotic-associated genes including BIM, NFκB1, NFκB2, AURKA, and AURKB as well as the increased number of cells in sub-G1.
BI-847325 decreased cell proliferation
MEK/ERK signaling pathway and Aurora kinase family play an important role in the regulation of ATC cell proliferation. Therefore, flow cytometry assay was performed to determine the effect of dual MEK/Aurora kinase inhibitor BI-847325 on cell proliferation. As shown in Fig. 2I–K, the treatment with BI-847325 resulted in a significant reduction of cell proliferation in C643 and SW1736 cell lines. Moreover, as mentioned above, changes in the expression of proliferation-related genes were consistent with the results at the cellular level.
BI-847325 induced cell redifferentiation
To investigate whether BI-847325 could influence the differentiation of ATC cells, the expressions of NIS and Tg genes were measured by qRT-PCR. Furthermore, flow cytometry assay and IRMA were used to evaluate the protein levels of NIS and Tg, respectively. Inhibition of MAPK pathway by BI-847325 significantly enhanced transcriptomic levels of NIS and Tg in C643 and SW1736 cell lines, as described above. Moreover, flow cytometry results showed that the NIS protein was significantly upregulated by BI-847325 treatment in C643 cell line. However, the protein level of NIS was not significantly increased after treatment in SW1736 cells (Fig. 3A–C). Also, IRMA results were further confirmed the elevated level of Tg in the treated cells in comparison with the untreated control in both cell lines, although this increase was not significant (Fig. 3D). This may be related to the difference in the expression level of NIS after treatment in the two cell lines (Fig. 1C). The different observations at the cellular and molecular levels in each of the cell lines give us a wide view concerning the genetic background difference of C643 and SW1736 ATC cell lines [27,28,29,30].
The effect of BI-847325 on the protein levels of NIS and Tg in C643 and SW1736 ATC cell lines. NIS was quantified by flow cytometry 48 h after BI-847325 treatment. The Representative histograms indicate the FITC unspecific background fluorescence (isotype) and the level of NIS protein Pre- and post-treatment in C643 A and SW1736 B. C Graphical representation of the protein level of NIS based on flow cytometry in 48 h after BI-847325 treatment of ATC cell lines compared to untreated cells as control. Tg was measured using IRMA assay 48 h after BI-847325 treatment. D The concentration of Tg protein is indicated for C643 and SW1736 cells. Statistical significances are expressed as p < .05 (*); p < .01 (**); p < .001 (***); p < .0001 (****)
F-actin labeling
BI-847325 decreased invasion by reducing F-actin network formation
To assess the effect of BI-847325 on the invasiveness of ATC cells, F-actin labeling was used to determine BI-847325-induced actin cytoskeleton remodeling. The result showed that the formation of F-actin network in cell invasion was significantly decreased following inhibition of the MEK/ERK pathway and Aurora kinase family in C643 and SW1736 cell lines (Fig. 4A–C).
The effect of BI-847325 on invasion of ATC cell lines as well as inhibition of the kinases function of MEK1/2 and AURKB. Alexa Fluor 549 Phalloidin staining was performed to investigate changes in the invasiveness of C643 A and SW1736 B 48 h after BI-847325 treatment. The nuclei were also stained simultaneously with DAPI (A-B, magnification = 400X, Scale bar = 50 μm). C The proportion of cell invading is indicated for C643 and SW1736. Statistical significances are expressed as p < .05 (*); p < .01 (**); p < .001 (***); p < .0001 (****). D This hybrid compound decreased the function of MEK1/2 and AURKB by reducing the levels of phospho-ERK1/2 and phospho-Histone H3 in C643 and SW1736 cell lines. Uncropped immunoblots are shown in Additional file 1: Fig. S1
Western blotting
BI-847325 inhibited the kinases function of MEK1/2 and AURKB
The phosphorylated form of ERK1/2 and Histone H3 are upregulated in ATC and contribute to the highly aggressive behavior of this tumor. The effect of BI-847325 on inhibition of kinases function of MEK1/2 and AURKB in ATC cell lines was examined by Western blot assay. The results confirmed that the treatment with BI-847325 decreased the levels of phospho-ERK1/2 and phospho-Histone H3, without altering protein expression (Fig. 4D).
Discussion
In this study, to evaluate the anticancer effect of BI-847325 on ATC, various biological processes associated with cancer progression including drug resistance, differentiation, angiogenesis, invasion, apoptosis, cell cycle, and proliferation were examined at the molecular and/or cellular levels (Fig. 5).
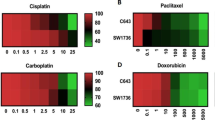
Currently, a multimodal therapeutic approach including surgery followed by chemotherapy is used for ATC patients. Unfortunately, genotoxic drugs such as Doxorubicin are not very efficient against ATC. Therefore, molecular targeted drugs including tyrosine kinase inhibitors are recommended for more effective treatment of patients with ATC. However, the prognosis of patients is poor and mortality from this cancer remains a major challenge worldwide [1]. Chemotherapy studies have shown that Doxorubicin, as single-agent or in combination, produces response rates between 15% and 25% [31, 32]. Several mechanisms have been proposed in relation to Doxorubicin drug resistance. One of the most important of them is the overexpression of ATP-binding cassette transporters such as MDR1 and MRP1 [33]. Studies have shown that the expression of these multidrug resistance genes can be regulated by the MEK/ERK signaling pathway in ATC [34]. As the results of this study show, the treatment with targeted anticancer drug BI-847325 could reduce the expression of multidrug resistance genes, MDR1 and MRP1, in ATC cell lines (Fig. 1). Hence, it is expected that the modified cells with reduced drug resistance capacity are more sensitive to anticancer drugs. However, further studies at the cellular and tumoral levels are needed to confirm this molecular finding.
As evidence has shown, during the development of ATC, thyroid cells lose their differentiation and consequently the expression of NIS and Tg, as two differentiation markers of thyrocytes. Therefore, ATC patients do not respond to radioiodine ablation as the mainstay of treatment for differentiated thyroid cancer, due to decreased expression of NIS [35,36,37,38]. Any drug intervention that leads to the expression of NIS can be considered as a candidate for chemotherapy of ATC by inducing redifferentiation and providing the basis for treatment with radioiodine [39,40,41]. Therefore, NIS and Tg, whose expression is regulated by the MAPK pathway [42], were evaluated to assess the degree of differentiation induced in ATC cells by BI-847325. BI-847325 had the potential to increase the expression of NIS and Tg at the transcript and protein levels and may produce cells that are more sensitive to radioactive iodine therapy (Figs. 1 and 3). Therefore, it can be considered as an effective multi-targeted anticancer drug for the treatment of ATC and other radioiodine-refractory thyroid cancers.
Angiogenesis and actin cytoskeleton organization also play an important role in tumor progression and invasion of ATC [43, 44]. Angiogenesis is affected by vascular endothelial growth factor (VEGF), and studies have shown that the expression of VEGF gene is upregulated in thyroid cancer, especially in ATC. Tyrosine kinase inhibitors of VEGF receptors are currently used as targeted therapies for ATC patients [43, 45, 46]. The treatment of ATC cell lines with BI-847325 may decrease tumor angiogenesis by reducing VEGF expression (Fig. 1). Han et al. demonstrated that the MAPK pathway regulates actin organization and cell invasion [47]. In addition, research has shown that three members of the Aurora kinase family (AURKA, AURKB, and AURKC) play an important role in cancer cell migration and tumor progression [48,49,50]. Simultaneous inhibition of the MEK/ERK pathway and Aurora kinase family by BI-847325 remodeled the actin filament network and reduced ATC cell invasion (Fig. 4 A-C). However, further studies are needed to determine the role of Aurora kinases in the organization of actin filaments.
As mentioned, MAPK signaling is one of the most important intracellular pathways involved in ATC development and progression [51]. This signaling pathway reduces cell death by altering the expression of genes involved in the apoptotic process such as BIM, NFκB1, NFκB2, AURKA, and AURKB, thereby increasing tumor growth [52,53,54,55]. Also, studies have shown that the Aurora kinase family is involved in tumor progression by suppressing apoptosis [56, 57]. Selective inhibitors of AURKA, AURKB, and AURKC can induce apoptosis in ATC cells [58, 59]. For instance, Bonnemains et al. indicated that VX-680 increased apoptosis by inhibiting the function of AURKA, AURKB, and AURKC in different ATC cell lines [59]. Inhibition of MEK/ERK pathway by BI-847325 increased the expression of pro-apoptotic gene BIM and decreased anti-apoptotic genes NFκB1 and NFκB2 as well as AURKA and AURKB in ATC cells (Fig. 1). The treatment with BI-847325, a dual MEK/Aurora kinase inhibitor, also induced apoptosis at the cellular level (Fig. 2E–H) by decreasing the function of AURKA, AURKB, and AURKC in addition to regulating the expression of apoptotic genes. Phadke et al. showed that BI-847325 treatment regulated the expression of Mcl-1 and BIM and consequently induced apoptosis in melanoma cell lines [60].
Moreover, in our previous study, we determined the effect of BI-847325 anticancer drug on the molecular mechanisms that regulate MALAT1-related genes in ATC. The results of this study suggested that BI-847325 could be effective against ATC by regulating the genes involved in cell cycle and apoptosis including MALAT1 and its downstream genes such as Mcl-1, miR-363-3p, and cyclin D1 [22].
Evidence has shown that RAS/RAF/MEK/ERK pathway and Aurora kinase family are also involved in cell cycle and proliferation [5, 9]. Activation of the MAPK signaling pathway as a result of mutations occurring in the RAS and BRAF genes can lead to rapid tumor progression and poor prognosis of ATC [61]. Over the past decade, our knowledge about the molecular details that control cell cycle and proliferation has improved. Hence, it has been shown that different genes such as P16, AURKA, and AURKB play an important role in tumor growth in ATC [9, 62,63,64]. Lee et al. demonstrated that the P16 tumor suppressor, which inhibits cell cycle progression, is undetectable in 24 of 27 ATC tissues [65, 66]. Moreover, Wiseman et al. using immunohistochemistry (IHC) and tissue microarray (TMA) found that the AURKC is one of the five molecular targets most frequently expressed in 32 ATC patients’ tissue samples [67]. Baldini et al. showed that selective AURKA and AURKB inhibitors have therapeutic potential for ATC due to suppression of cell proliferation as well as induction of apoptosis and G2/M phase arrest [10]. Chromatin compaction in G2/M is mediated by Histone H3 phosphorylation. AURKB promotes mitosis and cell division by increasing the phosphorylation of Histone H3 in serine 10 [68] while AURKB inhibitors decrease cell proliferation by reducing this phosphorylation [69]. Consistent with the findings of Phadke et al. [60], the results of this study showed that the treatment with BI-847325 could reduce phosphorylation of Histone H3 in serine 10 in ATC cell lines (Fig. 4D). Also, Sorrentino et al. showed that AURKB overexpressed in ATC cells and its inhibition by RNA interference or AURK inhibitor can reduce cell growth [70]. Because the expressions of P16, AURKA, and AURKB genes are regulated by the MAPK pathway [54, 55, 71], BI-847325 as a dual MEK/Aurora kinase inhibitor significantly increased P16 expression in both ATC cell lines. This anticancer drug also decreased the expression and function of key regulators of cell cycle and proliferation, AURKA, AURKB, and AURKC, resulting in cell cycle arrest and reduced cell proliferation (Fig. 2A–D and I–K). It should be noted that the ATC cell lines used in this study have mutations in the MAPK pathway i.e. RAS mutation [C643] and BRAFV600E mutation [SW1736] [20] and, therefore their different responses to BI-847325 at the cellular and molecular levels may be related to their different genetic backgrounds.
Overall, BI-847325 can be suggested as an anticancer drug for the treatment of ATC patients due to its regulatory effects on key biological processes associated with cancer progression.
Conclusion
In conclusion, the results of this study showed that BI-857,325 has the potential to be considered as an effective multi-targeted anticancer drug for the treatment of ATC. BI-847325 intervention induced the thyroid-specific differentiation markers including NIS and Tg as well as apoptosis in ATC cell lines. Moreover, targeted therapy with BI-847325 reduced invasion, angiogenesis, proliferation, cell cycle progression, and multidrug resistance at the molecular and/or cellular levels. In addition, BI-847325 decreased the function of MEK1/2 and AURKB by decreasing the levels of phospho-ERK1/2 and phospho-Histone H3. However, further experiments using xenograft transplant tumors and ATC animal models are needed to confirm the findings of this study on the response of ATC tumors to BI-847325 anticancer drug in vivo. Also, the use of additional complementary assays to determine the details of the regulatory mechanisms of this hybrid compound on the biological processes involved in cancer progression can help to better understand the effects of BI-847325.
.
Availability of data and materials
The datasets generated and/or analyzed during the current study are available from the corresponding author upon reasonable request.
Abbreviations
- 2D:
-
Two-dimensional
- 3D:
-
Three-dimensional
- ATC:
-
Anaplastic Thyroid Cancer
- AURKA:
-
Aurora Kinase A
- AURKB:
-
Aurora Kinase B
- AURKC:
-
Aurora Kinase C
- BIM:
-
BCL2 Like 11
- IC50 :
-
Half-Maximal Inhibitory Concentration
- IHC:
-
Immunohistochemistry
- IRMA:
-
Immunoradiometric assay
- MALAT1:
-
Metastasis Associated Lung Adenocarcinoma Transcript 1
- MAPK:
-
Mitogen-Activated protein kinase
- Mcl-1:
-
Myeloid cell leukemia sequence 1
- MDR1:
-
ATP Binding Cassette Subfamily B Member 1
- MRP1:
-
ATP Binding Cassette Subfamily C Member 1
- NFκB1:
-
Nuclear Factor Kappa B Subunit 1
- NFκB2:
-
Nuclear Factor Kappa B Subunit 2
- NIS:
-
Sodium/Iodide Symporter
- P16:
-
Cyclin Dependent Kinase Inhibitor 2 A
- qRT-PCR:
-
quantitative Real-Time Polymerase Chain Reaction
- Tg:
-
Thyroglobulin
- TMA:
-
Tissue microarray
- VEGF:
-
Vascular endothelial growth factor
References
Saini S, Tulla K, Maker AV, Burman KD, Prabhakar BS. Therapeutic advances in anaplastic thyroid cancer: a current perspective. Mol Cancer. 2018;17(1):1–14.
Lin B, Ma H, Ma M, Zhang Z, Sun Z, Hsieh I-y, et al. The incidence and survival analysis for anaplastic thyroid cancer: a SEER database analysis. Am J translational Res. 2019;11(9):5888.
Pozdeyev N, Rose MM, Bowles DW, Schweppe RE. Molecular therapeutics for anaplastic thyroid cancer. In: Pozdeyev N, Rose MM, Bowles DW, Schweppe RE, editors. Seminars in cancer biology. Amsterdam: Elsevier; 2020.
McCubrey JA, Steelman LS, Chappell WH, Abrams SL, Wong EW, Chang F, et al. Roles of the Raf/MEK/ERK pathway in cell growth, malignant transformation and drug resistance. Biochim et Biophys Acta (BBA)-Molecular Cell Res. 2007;1773(8):1263–84.
Guo YJ, Pan WW, Liu SB, Shen ZF, Xu Y, Hu LL. ERK/MAPK signalling pathway and tumorigenesis. Experimental and Therapeutic Medicine. 2020;19(3):1997–2007.
Subbiah V, Kreitman RJ, Wainberg ZA, Cho JY, Schellens JH, Soria JC, et al. Dabrafenib and trametinib treatment in patients with locally advanced or metastatic BRAF V600–mutant anaplastic thyroid cancer. J Clin Oncol. 2018;36(1):7.
U.S. Food and Drug Administration. FDA approves dabrafenib plus trametinib for anaplastic thyroid cancer with BRAF V600E mutation. 2018. www.fda.gov/Drugs/InformationOnDrugs/ApprovedDrugs/ucm606708.htm. Accessed 7 Sept 2022
Salvatore G, Nappi TC, Salerno P, Jiang Y, Garbi C, Ugolini C, et al. A cell proliferation and chromosomal instability signature in anaplastic thyroid carcinoma. Cancer Res. 2007;67(21):10148–58.
Baldini E, Sorrenti S, D’Armiento E, Prinzi N, Guaitoli E, Favoriti P, et al. Aurora kinases: new molecular targets in thyroid cancer therapy. Clin Ter. 2012;163(6):e457-62.
Baldini E, Tuccilli C, Prinzi N, Sorrenti S, Antonelli A, Gnessi L, et al. Effects of selective inhibitors of Aurora kinases on anaplastic thyroid carcinoma cell lines. Endocr Relat Cancer. 2014;21(5):797–811.
Savonarola A, Palmirotta R, Guadagni F, Silvestris F. Pharmacogenetics and pharmacogenomics: role of mutational analysis in anti-cancer targeted therapy. Pharmacogenomics J. 2012;12(4):277–86.
Miteva-Marcheva NN, Ivanov HY, Dimitrov DK, Stoyanova VK. Application of pharmacogenetics in oncology. Biomark Res. 2020;8(1):1–10.
Sini P, Gürtler U, Zahn SK, Baumann C, Rudolph D, Baumgartinger R, et al. Pharmacological profile of BI 847325, an orally bioavailable, ATP-competitive inhibitor of MEK and Aurora kinases. Mol Cancer Ther. 2016;15(10):2388–98.
Makhoba XH, Viegas C Jr, Mosa RA, Viegas FP, Pooe OJ. Potential impact of the multi-target drug approach in the treatment of some complex diseases. Drug Design Dev Ther. 2020;14:3235.
Szumilak M, Wiktorowska-Owczarek A, Stanczak A. Hybrid drugs—a strategy for overcoming anticancer drug resistance? Molecules. 2021;26(9):2601.
Schöffski P, Aftimos P, Dumez H, Deleporte A, De Block K, Costermans J, et al. A phase I study of two dosing schedules of oral BI 847325 in patients with advanced solid tumors. Cancer Chemother Pharmacol. 2016;77(1):99–108.
Kapałczyńska M, Kolenda T, Przybyła W, Zajączkowska M, Teresiak A, Filas V, et al. 2D and 3D cell cultures–a comparison of different types of cancer cell cultures. Archi Med Sci. 2018;14(4):910–9.
Jensen C, Teng Y. Is it time to start transitioning from 2D to 3D cell culture? Front Mol Biosci. 2020;7:33.
Langhans SA. Three-dimensional in vitro cell culture models in drug discovery and drug repositioning. Front Pharmacol. 2018;9:6.
Samimi H, Sohi AN, Irani S, Arefian E, Mahdiannasser M, Fallah P, et al. Alginate-based 3D cell culture technique to evaluate the half-maximal inhibitory concentration: an in vitro model of anticancer drug study for anaplastic thyroid carcinoma. Thyroid Res. 2021;14(1):1–9.
Samimi H, Haghpanah V, Irani S, Fallah P, Arefian E, Soleimani M. Determination of ATP-Competitive inhibitor drug toxicity in anaplastic thyroid Cancer based on cell characteristics and Three-Dimensional Cell Culture. Modares J Biotechnol. 2019;10(3):503–9.
Samimi H, Haghpanah V, Irani S, Arefian E, Sohi AN, Fallah P, et al. Transcript-level regulation of MALAT1-mediated cell cycle and apoptosis genes using dual MEK/Aurora kinase inhibitor “BI-847325” on anaplastic thyroid carcinoma. DARU J Pharm Sci. 2019;27(1):1–7.
Eslami A, Lujan J. Western blotting: sample preparation to detection. JoVE (Journal of Visualized Experiments). 2010;44.
Bruce JL, Hurford RK Jr, Classon M, Koh J, Dyson N. Requirements for cell cycle arrest by p16INK4a. Mol Cell. 2000;6(3):737–42.
Willems E, Dedobbeleer M, Digregorio M, Lombard A, Lumapat PN, Rogister B. The functional diversity of Aurora kinases: a comprehensive review. Cell Div. 2018;13(1):1–17.
Kassardjian A, Rizkallah R, Riman S, Renfro SH, Alexander KE, Hurt MM. The transcription factor YY1 is a novel substrate for Aurora B kinase at G2/M transition of the cell cycle. PLoS ONE. 2012;7(11):e50645.
Pilli T, Prasad KV, Jayarama S, Pacini F, Prabhakar BS. Potential utility and limitations of thyroid cancer cell lines as models for studying thyroid cancer. Thyroid. 2009;19(12):1333–42.
Samimi H, Fallah P, Sohi AN, Tavakoli R, Naderi M, Soleimani M, et al. Precision medicine approach to anaplastic thyroid cancer: advances in targeted drug therapy based on specific signaling pathways. Acta Medica Iranica. 2017;55:200–8.
Meireles AM, Preto A, Rocha AS, Rebocho AP, Máximo V, Pereira-Castro I, et al. Molecular and genotypic characterization of human thyroid follicular cell carcinoma–derived cell lines. Thyroid. 2007;17(8):707–15.
Landa I, Pozdeyev N, Korch C, Marlow LA, Smallridge RC, Copland JA, et al. Comprehensive genetic characterization of human thyroid cancer cell lines: a validated panel for preclinical studies. Clin Cancer Res. 2019;25(10):3141–51.
Perri F, Di Lorenzo G, Scarpati GDV, Buonerba C. Anaplastic thyroid carcinoma: a comprehensive review of current and future therapeutic options. World J Clin Oncol. 2011;2(3):150.
Cabanillas ME, Zafereo M, Gunn GB, Ferrarotto R. Anaplastic thyroid carcinoma: treatment in the age of molecular targeted therapy. J Oncol Pract. 2016;12(6):511–8.
Zheng X, Cui D, Xu S, Brabant G, Derwahl M. Doxorubicin fails to eradicate cancer stem cells derived from anaplastic thyroid carcinoma cells: characterization of resistant cells. Int J Oncol. 2010;37(2):307–15.
Abbasifarid E, Sajjadi-Jazi SM, Beheshtian M, Samimi H, Larijani B, Haghpanah V. The role of ATP-binding cassette transporters in the chemoresistance of anaplastic thyroid cancer: a systematic review. Endocrinology. 2019;160(8):2015–23.
Ragazzi M, Ciarrocchi A, Sancisi V, Gandolfi G, Bisagni A, Piana S. Update on anaplastic thyroid carcinoma: morphological, molecular, and genetic features of the most aggressive thyroid cancer. Int J Endocrinol. 2014;2014:790834.
da Silva TN, Limbert E, Leite V. Poorly differentiated thyroid carcinoma patients with detectable thyroglobulin levels after initial treatment show an increase in mortality and disease recurrence. Eur thyroid J. 2018;7(6):313–8.
Akagi T, Luong Q, Gui D, Said J, Selektar J, Yung A, et al. Induction of sodium iodide symporter gene and molecular characterisation of HNF3 β/FoxA2, TTF-1 and C/EBP β in thyroid carcinoma cells. Br J Cancer. 2008;99(5):781–8.
Carvalho DP, Ferreira AC. The importance of sodium/iodide symporter (NIS) for thyroid cancer management. Arquivos Brasileiros de Endocrinologia & Metabologia. 2007;51:672–82.
Lamartina L, Anizan N, Dupuy C, Leboulleux S, Schlumberger M. Redifferentiation-facilitated radioiodine therapy in thyroid cancer. Endocrine-related Cancer. 2021;28(10):T179-T91.
Hong CM, Ahn B-C. Redifferentiation of radioiodine refractory differentiated thyroid cancer for reapplication of I-131 therapy. Front Endocrinol. 2017;8:260.
Choi YJ, Lee J-E, Ji HD, Lee B-R, Lee SB, Kim KS, et al. Tunicamycin as a novel redifferentiation agent in radioiodine therapy for anaplastic thyroid cancer. Int J Mol Sci. 2021;22(3):1077.
Fu H, Cheng L, Jin Y, Cheng L, Liu M, Chen L. MAPK inhibitors enhance HDAC inhibitor-induced redifferentiation in papillary thyroid cancer cells harboring BRAFV600E: an in vitro study. Mol Therapy-Oncolytics. 2019;12:235–45.
Soh EY. Implication of angiogenesis in thyroid Cancer. Korean J Endocr Surg. 2002;2(1):1–4.
Montero-Conde C, Martin-Campos J, Lerma E, Gimenez G, Martinez-Guitarte J, Combalia N, et al. Molecular profiling related to poor prognosis in thyroid carcinoma. Combining gene expression data and biological information. Oncogene. 2008;27(11):1554–61.
Enokida T, Tahara M. Management of VEGFR-Targeted TKI for thyroid Cancer. Cancers. 2021;13(21):5536.
Porter A, Wong DJ. Perspectives on the treatment of advanced thyroid cancer: approved therapies, resistance mechanisms, and future directions. Front Oncol. 2021. https://doi.org/10.3389/fonc.2020.592202.
Han M-Y, Kosako H, Watanabe T, Hattori S. Extracellular signal-regulated kinase/mitogen-activated protein kinase regulates actin organization and cell motility by phosphorylating the actin cross-linking protein EPLIN. Mol Cell Biol. 2007;27(23):8190–204.
Baldini E, D’Armiento M, Ulisse S. A new aurora in anaplastic thyroid cancer therapy. Int J Endocrinol. 2014;2014:816430.
Wu X, Liu J-m, Song H-h, Yang Q-k, Ying H, Tong W-l, et al. Aurora-B knockdown inhibits osteosarcoma metastasis by inducing autophagy via the mTOR/ULK1 pathway. Cancer Cell Int. 2020;20(1):1–14.
Bejar JF, DiSanza Z, Quartuccio SM. The oncogenic role of meiosis-specific Aurora kinase C in mitotic cells. Exp Cell Res. 2021;407(2):112803.
Milosevic Z, Pesic M, Stankovic T, Dinic J, Milovanovic Z, Stojsic J, et al. Targeting RAS-MAPK-ERK and PI3K-AKT-mTOR signal transduction pathways to chemosensitize anaplastic thyroid carcinoma. Translational Res. 2014;164(5):411–23.
Balmanno K, Cook S. Tumour cell survival signalling by the ERK1/2 pathway. Cell Death Differentiation. 2009;16(3):368–77.
Ahmed KM, Dong S, Fan M, Li JJ. Nuclear factor-κB p65 inhibits mitogen-activated protein kinase signaling pathway in radioresistant breast cancer cells. Mol Cancer Res. 2006;4(12):945–55.
Marampon F, Gravina GL, Popov VM, Scarsella L, Festuccia C, La Verghetta ME, et al. Close correlation between MEK/ERK and Aurora-B signaling pathways in sustaining tumorigenic potential and radioresistance of gynecological cancer cell lines. Int J Oncol. 2014;44(1):285–94.
Furukawa T, Kanai N, Shiwaku H, Soga N, Uehara A, Horii A. AURKA is one of the downstream targets of MAPK1/ERK2 in pancreatic cancer. Oncogene. 2006;25(35):4831–9.
Du R, Huang C, Liu K, Li X, Dong Z. Targeting AURKA in Cancer: molecular mechanisms and opportunities for Cancer therapy. Mol Cancer. 2021;20(1):1–27.
Huang D, Huang Y, Huang Z, Weng J, Zhang S, Gu W. Relation of AURKB over-expression to low survival rate in BCRA and reversine-modulated aurora B kinase in breast cancer cell lines. Cancer Cell Int. 2019;19(1):1–13.
Baldini E, Tuccilli C, Prinzi N, Sorrenti S, Antonelli A, Gnessi L, et al. The dual Aurora kinase inhibitor ZM447439 prevents anaplastic thyroid cancer cell growth and tumorigenicity. J Biol Regul Homeost Agents. 2013;27(3):705–15.
Arlot-Bonnemains Y, Baldini E, Martin B, Delcros J-G, Toller M, Curcio F, et al. Effects of the Aurora kinase inhibitor VX-680 on anaplastic thyroid cancer-derived cell lines. Endocrine-related Cancer. 2008;15(2):559–68.
Phadke MS, Sini P, Smalley KS. The novel ATP-competitive MEK/Aurora kinase inhibitor BI-847325 overcomes acquired BRAF inhibitor resistance through suppression of Mcl-1 and MEK expression. Mol Cancer Ther. 2015;14(6):1354–64.
Piscazzi A, Costantino E, Maddalena F, Natalicchio MI, Gerardi AMT, Antonetti R, et al. Activation of the RAS/RAF/ERK signaling pathway contributes to resistance to sunitinib in thyroid carcinoma cell lines. J Clin Endocrinol Metabolism. 2012;97(6):E898–906.
Khatami F, Larijani B, Heshmat R, Keshtkar A, Mohammadamoli M, Teimoori-Toolabi L, et al. Meta-analysis of promoter methylation in eight tumor-suppressor genes and its association with the risk of thyroid cancer. PLoS ONE. 2017;12(9):e0184892.
Smallridge RC, Marlow LA, Copland JA. Anaplastic thyroid cancer: molecular pathogenesis and emerging therapies. Endocrine-related Cancer. 2009;16(1):17–44.
Ulisse S, Delcros JG, Baldini E, Toller M, Curcio F, Giacomelli L, et al. Expression of Aurora kinases in human thyroid carcinoma cell lines and tissues. Int J Cancer. 2006;119(2):275–82.
Lee J-J, Au AY, Foukakis T, Barbaro M, Kiss N, Clifton-Bligh R, et al. Array-CGH identifies cyclin D1 and UBCH10 amplicons in anaplastic thyroid carcinoma. Endocrine-related Cancer. 2008;15(3):801–15.
Sheikkholeslami S, Zarif-Yeganeh M, Farashi S, Azizi F, Kia SK, Teimoori-Toolabi L, et al. Promoter methylation of tumor suppressors in thyroid carcinoma: a systematic review. Iran J Public Health. 2021;50(12):2461–72.
Wiseman SM, Masoudi H, Niblock P, Turbin D, Rajput A, Hay J, et al. Anaplastic thyroid carcinoma: expression profile of targets for therapy offers new insights for disease treatment. Ann Surg Oncol. 2007;14(2):719–29.
Moura DS, Campillo-Marcos I, Vázquez-Cedeira M, Lazo PA. VRK1 and AURKB form a complex that cross inhibit their kinase activity and the phosphorylation of histone H3 in the progression of mitosis. Cell Mol Life Sci. 2018;75(14):2591–611.
Borah NA, Reddy MM. Aurora kinase B inhibition: a potential therapeutic strategy for cancer. Molecules. 2021;26(7):1981.
Sorrentino R, Libertini S, Pallante PL, Troncone G, Palombini L, Bavetsias V, et al. Aurora B overexpression associates with the thyroid carcinoma undifferentiated phenotype and is required for thyroid carcinoma cell proliferation. J Clin Endocrinol Metabolism. 2005;90(2):928–35.
Wen-Sheng W. ERK signaling pathway is involved in p15 INK4b/p16 INK4a expression and HepG2 growth inhibition triggered by TPA and Saikosaponin a. Oncogene. 2003;22(7):955–63.
Acknowledgements
The authors would like to thanks Ms. Mahla Esfandiari and Ms. Zahra Gohari for their technical assistance. The authors are thankful to Dr. Mohammad Reza Nejadmoghaddam for providing the secondary antibodies used in this study. Also, the authors thank Dr. Simzar Hosseinzadeh, for her helpful suggestions and advice.
Funding
This research did not receive any specific grant from funding agencies in the public, commercial, or not-for-profit sectors.
Author information
Authors and Affiliations
Contributions
VH and HS designed the study; HS and RT performed the experiments. HS contributed to data acquisition and interpreted the data as well as wrote the first draft of the manuscript; PF, MAS. and MN analyzed data; ANS supervised 3D cell culture in alginate hydrogel and MTT assay. All authors read and approved the final manuscript.
Corresponding author
Ethics declarations
Ethics approval and consent to participate
Not applicable.
Consent for publication
Not applicable.
Competing interests
The authors declare that they have no conflict of interest.
Additional information
Publisher’s Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary information
Additional file 1: Figure S1.
Uncropped immunoblots on X-ray film and PVDF membrane for the western blot bands are presented in Fig. 4 (D). The molecular weight marker was loaded on each gel. All samples were run into 2 gels, one for β-actin and the other one for the rest of the antibodies (4 antibodies). Following immunoblotting, the blot used for 4 antibodies was cut into 4 parts, 2 upper parts were probed with ERK1/2 and phospho-ERK1/2 antibodies, and 2 lower parts were probed with Histone H3 and phospho-Histone H3 antibodies. The molecular weight markers are not shown on some of the cut blots.
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if changes were made. The images or other third party material in this article are included in the article's Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article's Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by/4.0/. The Creative Commons Public Domain Dedication waiver (http://creativecommons.org/publicdomain/zero/1.0/) applies to the data made available in this article, unless otherwise stated in a credit line to the data.
About this article
Cite this article
Samimi, H., Tavakoli, R., Fallah, P. et al. BI-847325, a selective dual MEK and Aurora kinases inhibitor, reduces aggressive behavior of anaplastic thyroid carcinoma on an in vitro three-dimensional culture. Cancer Cell Int 22, 388 (2022). https://doi.org/10.1186/s12935-022-02813-6
Received:
Accepted:
Published:
DOI: https://doi.org/10.1186/s12935-022-02813-6